Depemokimab – a new long-acting treatment for severe asthma: what aspergillosis patients need to know
A new medicine called depemokimab is being reviewed by European and UK regulators as a possible treatment for severe eosinophilic (type-2) asthma. Many people with aspergillosis-related conditions – especially allergic bronchopulmonary aspergillosis (ABPA) and severe asthma with fungal sensitisation (SAFS) – also have this type of inflammation, so new options are always important.
⭐ What is depemokimab?
Depemokimab is a biologic treatment, similar to medicines like mepolizumab or benralizumab, but designed to last much longer in the body. It blocks interleukin-5 (IL-5), one of the key signals that drives eosinophils – a type of white blood cell involved in allergy, asthma and ABPA flares.
⭐ What makes it different?
The most important difference is how rarely it needs to be taken.
Current biologics for type-2 asthma are given every 4, 6 or 8 weeks.
Depemokimab is designed to be taken twice a year – only once every six months.
For many people, this could mean:
-
Fewer injections
-
More steady asthma control
-
Less disruption to daily life
-
A treatment that’s easier to stick with over time
In clinical trials, depemokimab also helped to:
-
Reduce asthma attacks
-
Lower the need for oral steroids
-
Improve symptoms in people with chronic sinusitis and nasal polyps, which commonly affects ABPA and SAFS patients
⭐ Is this a treatment for ABPA or CPA?
Not specifically.
Depemokimab is not a treatment for the Aspergillus fungus itself and it does not replace antifungal medicines.
However, for people whose asthma drives their ABPA symptoms, better asthma control can mean:
-
fewer flare-ups
-
better breathing
-
less need for steroids
-
reduced pressure on already damaged airways
So while it is not an antifungal, it may become another option in the toolkit for managing asthma linked to aspergillosis.
⭐ When might this be available in the UK?
Depemokimab is currently under review by European regulators.
In the UK, the NICE appraisal for NHS use is underway, with a decision expected in March 2026.
If approved, it could become available on the NHS sometime in 2026.
⭐ What should patients do now?
At this stage:
-
There is no action needed from patients.
-
Your asthma or ABPA team will be the first to know when new biologics are approved.
-
If you already receive a biologic (e.g., mepolizumab, benralizumab, omalizumab, dupilumab), there is no change to your treatment plan.
-
If you struggle with frequent injections or poor asthma control, your clinician may consider depemokimab in the future once approved.
Mycotoxins in Damp Homes: Are They a Hidden Cause of Chronic Illness?
The internet is full of claims that “toxic mould” and “mycotoxins” in damp homes cause chronic fatigue, brain fog, immune disorders, or long-term poisoning.
These stories are frightening — but they are also misleading.
This article explains what mycotoxins are, what risks are real, and why blaming them can delay proper diagnosis and treatment.
1. What Are Mycotoxins?
Mycotoxins are chemicals produced by some fungi. Certain mycotoxins can be harmful — but usually in situations completely different from normal household mould.
Examples include:
-
Aflatoxin in contaminated food crops (mainly in tropical regions)
-
Ochratoxin A in poorly stored grains
-
Trichothecenes from water-damaged materials in rare extreme cases
In UK homes, airborne mycotoxin levels are generally extremely low.
2. Can Mycotoxins in Homes Cause Chronic Illness?
The scientific consensus from WHO, UKHSA, CDC, and NICE is:
No — not at the levels found in typical damp or mouldy houses.
Mycotoxins mainly cause illness by eating contaminated food, not by breathing small amounts in the air.
Symptoms linked to damp homes — fatigue, cough, wheeze, headaches — are usually caused by:
-
Allergens (dust mites, spores)
-
Irritants
-
Cold, damp air
-
Bacteria
-
Volatile organic compounds (VOCs)
-
Poor ventilation
-
Existing asthma or lung disease
These symptoms are real, but they are not mycotoxin poisoning.
3. Why the Myth Persists
Online sources often promote the idea of “mould toxicity” because:
-
It offers a simple explanation for complex symptoms
-
Private companies sell expensive testing kits
-
Influencers share personal stories
-
It feels empowering to “identify” a hidden cause
But most testing marketed as “mycotoxin screening” is not medically valid and often gives false positives.
4. The Real Harm: Misdiagnosis and Delayed Treatment
This is crucial.
People who believe they have “mycotoxin illness” may delay getting proper medical assessment for:
-
ABPA (Allergic Bronchopulmonary Aspergillosis)
-
CPA (Chronic Pulmonary Aspergillosis)
-
SAFS (Severe Asthma with Fungal Sensitisation)
-
Bronchiectasis
-
NTM lung disease
-
Adrenal insufficiency
-
Asthma deterioration
Some conditions worsen without correct treatment, and the delay can be significant.
People may also spend large amounts of money on:
-
Detox supplements
-
“Mould inspections”
-
Repeated home fogging or ozone treatments
-
House moves
-
Throwing away belongings
-
Private “mycotoxin tests”
These rarely help — and often worsen stress and isolation.
5. When Should Someone Be Concerned About Mycotoxins? (Very Rare Cases)
Significant mycotoxin exposure is possible only in:
-
Buildings with severe, long-term water damage
-
Homes where black mould covers large areas and ventilation is extremely poor
-
Certain workplaces (grain stores, composting facilities)
Even then, the main health effects involve irritation and asthma, not systemic poisoning.
6. If You Do Have ABPA, CPA, or Asthma — Home Improvements Can Help
Not because they remove toxins, but because they improve air quality:
-
Lower humidity (40–60%)
-
Fix damp problems
-
Improve ventilation
-
Use HEPA air filters
-
Reduce dust and allergens
-
Clean or replace heavily contaminated soft furnishings
These steps support better respiratory control, particularly in people already living with lung disease.
Key Message
Mycotoxins in UK homes are not a hidden cause of chronic illness.
Believing otherwise can delay diagnosis and treatment of real, treatable conditions such as ABPA, CPA, asthma, and bronchiectasis.
Improving your home environment helps — but it supports lung health, it does not “detox” mycotoxins.
Understanding Aspergillosis Through Imaging: A Guide for Patients and Non-Specialist Clinicians
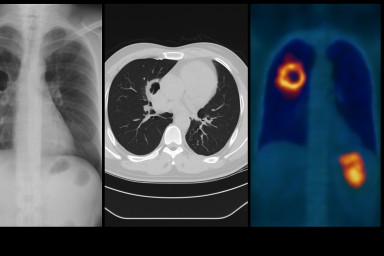
Imaging — especially chest X-ray and high-resolution CT (HRCT) — is one of the most important tools for recognising, diagnosing and monitoring aspergillosis. Because the condition can affect the lungs in very different ways, seeing what is happening inside the chest is essential for both patients and clinicians.
This guide explains why imaging matters, how it is used, and provides links to trusted resources that show what aspergillosis looks like on scans.
Why Imaging Matters in Aspergillosis
Aspergillosis affects the lungs deep within the airway and lung tissue. Many of these changes cannot be detected by a stethoscope or blood tests alone. Imaging helps detect:
-
mucus plugging
-
bronchiectasis (damaged widened airways)
-
cavities (holes) in the lungs
-
fungal balls (aspergillomas)
-
inflammation and consolidation
-
scarring or fibrosis
-
signs of haemoptysis risk
In Allergic Bronchopulmonary Aspergillosis (ABPA), imaging may show mucus impaction or central bronchiectasis.
In Chronic Pulmonary Aspergillosis (CPA), it may show cavities, thickened cavity walls, or a fungus ball.
In invasive aspergillosis, imaging can detect early nodules, the “halo sign”, or rapidly progressing changes.
Understanding these patterns helps clinicians choose the right treatment at the right time, and helps patients make sense of what is happening in their lungs.
Key Online Resources for Aspergillosis Imaging
Radiopaedia – Open Radiology Reference
One of the clearest, most comprehensive imaging resources available.
-
Pulmonary aspergillosis overview:
https://radiopaedia.org/articles/pulmonary-aspergillosis?lang=gb -
Invasive pulmonary aspergillosis:
https://radiopaedia.org/articles/invasive-pulmonary-aspergillosis?lang=gb -
Aspergilloma (fungal ball):
https://radiopaedia.org/articles/aspergilloma?lang=gb
Why it’s useful:
Radiopaedia shows real CT and X-ray examples from multiple patients, helping you understand what radiologists look for and how different forms of aspergillosis appear on imaging.
Peer-Reviewed Pictorial Reviews
These academic reviews provide side-by-side CT examples of the full spectrum of disease, written in an accessible style and extremely useful for both patients and clinicians.
-
Imaging Spectrum in Chronic Pulmonary Aspergillosis (Garg et al., 2022)
https://pmc.ncbi.nlm.nih.gov/articles/PMC9833062/ -
Pictorial Essay: Forms of Pulmonary Aspergillosis (Tamkevičiūtė et al., 2024)
(abstract) https://www.ejradiology.com/article/S0720-048X%2824%2900006-8/abstract
These explain in pictures:
-
how cavities form
-
how aspergillomas look
-
early vs late changes
-
how ABPA patterns differ from CPA
-
what stable vs progressive disease looks like
They are especially helpful for GPs, respiratory trainees, and nurses learning to interpret fungal disease imaging.
Classic RSNA Radiographics Review (Franquet et al.)
A foundational article describing radiologic patterns in allergic, chronic and invasive aspergillosis.
Although technical, this remains a reference standard for understanding how fungal disease presents on CT.
National Aspergillosis Centre (UK) – Patient-Friendly Information
Clear explanations of why imaging is needed, how CT is used, and what typical findings mean.
-
Chronic Pulmonary Aspergillosis (CPA):
https://mft.nhs.uk/wythenshawe/services/infectious-diseases/national-aspergillosis-centre/about-aspergillosis/chronic-pulmonary-aspergillosis-cpa/
These pages are ideal for newly diagnosed patients, people preparing for CT scans, and clinicians who want a quick overview.
Asthma + Lung UK – General Aspergillosis Overview
Patient-friendly explanations of the different types of aspergillosis, diagnosis and treatment.
Includes mention of imaging when relevant.
How Imaging Guides Clinical Decisions
1. Confirming the Diagnosis
Different forms of aspergillosis look different on scans:
-
ABPA may show “finger-in-glove” mucus plugging or central bronchiectasis.
-
CPA requires a cavity seen on imaging for >3 months.
-
Aspergilloma is a fungal ball sitting within a cavity.
-
Invasive disease shows nodules, halo signs, or rapidly evolving infiltrates.
Without CT imaging, these distinctions cannot reliably be made.
2. Checking for Complications
Imaging detects:
-
new cavities
-
cavity wall thickening
-
risk of haemoptysis (bleeding)
-
pleural thickening
-
fibrosis
-
co-existing infections
These findings often trigger urgent or proactive treatment modifications.
3. Monitoring Progression and Treatment Response
Symptoms alone are not enough. Imaging shows whether:
-
disease is stable or progressing
-
antifungal treatment is working
-
inflammation is reducing
-
mucus plugging is clearing
-
new areas are becoming involved
This is why people with CPA or ABPA may have repeat CT scans, usually every 6–12 months or when symptoms worsen.
Using These Resources Safely
These resources are not for self-diagnosis. Instead, they help:
-
patients understand their own scan reports
-
GPs recognise when to refer to a specialist
-
hospital teams spot aspergillosis in complex or unclear cases
-
nurses and allied health professionals visualise lung changes
-
clinicians communicate findings more clearly
Imaging must always be interpreted by a trained radiologist or specialist team, but these materials help demystify the process.
Summary
Imaging is central to the diagnosis and management of aspergillosis. Whether you are a patient trying to understand your scans, a GP seeing a complex chest X-ray, or a hospital clinician assessing breathlessness, these imaging resources provide clear, trustworthy examples.
By learning what different patterns look like — mucus plugging, cavities, aspergillomas, fibrosis or invasive changes — non-specialists can make more confident decisions, and patients can better understand their condition.
The Chief Medical Officer’s Annual Report 2025: Infections
What this document is
The Chief Medical Officer’s Annual Report 2025: Infections is a major national review produced by the Chief Medical Officer for England, Professor Chris Whitty. It is a comprehensive, 371-page assessment of:
-
Current infectious disease threats in England
-
How infections are changing (ageing population, travel, globalisation, antimicrobial resistance)
-
What the NHS, public health services, and government need to do to protect the public
-
Key topics including vaccines, fungal infections, infection in older adults, housing, climate change and more
It includes contributions from national experts—including a full chapter dedicated to fungal infections (section 4.2) and others that touch on issues highly relevant to aspergillosis patients (vaccination, antimicrobial resistance, respiratory infections, housing, and vulnerable populations)
cmo-annual-report-2025-infectio…
Why it is published
The report is published each year to:
1. Advise Government
It sets out the CMO’s expert recommendations on how England should prepare for current and future infection threats, including pandemics, AMR, and emerging fungal pathogens.
2. Influence NHS planning and investment
The report highlights weaknesses in the system and proposes reforms.
This year’s report strongly emphasises:
-
Better infection services
-
Stronger surveillance
-
Improving vaccine uptake
-
Protecting older adults (now the group with most infection-related deaths)
-
Expanding superspecialist expertise—including fungal disease expertise
3. Inform clinicians, researchers, and public health professionals
It provides a current consensus on infectious disease trends, evidence, and priorities.
Chapters are written by leading UK experts in each field (e.g., fungal infections, antimicrobial resistance, vaccines, imported infections)
4. Educate the public and third-sector organisations
The report is open-access and intended to help the public understand why infection preparedness matters and why actions like vaccination, stewardship, and early diagnosis are essential.
Who reads it
The report is widely used across:
Government
-
Department of Health and Social Care
-
UKHSA
-
Cabinet Office (emergency planning)
-
Local authorities
NHS and clinical services
-
Infectious disease physicians
-
Respiratory teams
-
Microbiology and virology specialists
-
Primary care networks
-
ICS / ICB teams planning local services
Researchers and academic institutions
It sets the direction for future research and funding priorities, including for fungal disease and AMR.
Charities, patient organisations and advocates
Groups representing people with chronic, infectious, or respiratory illness read the report to understand system-level changes and advocate for patient needs.
Industry and diagnostics developers
They monitor future needs for antifungals, vaccines, and diagnostic tools.
Why this report is important for aspergillosis patients
Several aspects of the 2025 report directly relate to people with ABPA, CPA, SAFS or Aspergillus bronchitis.
1. Fungal infections are recognised as a major emerging threat
The report includes a dedicated chapter on fungal infections (section 4.2), describing:
-
Rising antifungal resistance
-
Expanding fungal threats globally
-
The importance of specialist mycology expertise
-
The risks from agricultural fungicides
-
The need for improved surveillance and diagnostics
This formal recognition strengthens the case for specialised centres like the National Aspergillosis Centre.
2. It highlights the need for superspecialists in rare and imported infections—including fungal disease
The CMO states that England requires:
“superspecialists to provide advice on and management of infections including… rarer [infections] such as fungal infections.”
cmo-annual-report-2025-infectio…
This directly supports the role and expansion of the NHS mycology services, which Aspergillus patients rely on for accurate diagnosis and treatment.
**3. It reinforces the importance of antimicrobial and antifungal stewardship
For people with aspergillosis, this matters because:
-
Resistance to azoles is rising—and the report explicitly mentions agricultural fungicides as part of the problem.
-
Stewardship ensures patients receive appropriate antifungals, monitored carefully and adjusted safely.
-
It argues for more drug development, which is essential because current antifungal options are limited.
4. It emphasises diagnosing infection in older adults
Older adults are increasingly vulnerable to infections and complications, especially respiratory ones.
The report stresses that:
-
Infection in older adults often has more serious consequences
-
Early diagnosis is essential
-
Access to specialist care must improve
Since many aspergillosis patients are older with complex lung disease, this section validates the need for better recognition and earlier referral.
5. Housing and damp are recognised as infection risks
The chapter Housing and Infection (section 7.2) discusses how substandard housing—including damp and mould—drives respiratory illness.
Although not Aspergillus-specific, it gives important public health backing for patients needing remediation and better housing conditions.
6. The report strengthens the case for national fungal surveillance
Key recommendations include:
-
Improving surveillance of antimicrobial and antifungal resistance
-
Better mapping of emerging pathogens
-
More research into fungal diseases
These system-level improvements directly benefit aspergillosis patients by helping earlier detection and better treatment options.
7. It raises awareness of fungal disease at national level
Simply being included in a flagship CMO report is important.
It means:
-
Policymakers can no longer overlook fungal infections
-
Funding for mycology services becomes easier to justify
-
Clinicians across the NHS will become more aware of CPA, ABPA and related diseases
-
It helps reduce the years-long diagnostic delays many patients face
In short — why Aspergillus patients should care
The 2025 CMO Annual Report is one of the most influential documents shaping future infectious disease strategy in England. For aspergillosis patients, it is important because:
✓ Fungal infections are explicitly highlighted as a growing threat
✓ Specialist mycology services are recognised as essential
✓ Antifungal resistance is identified as a major risk requiring action
✓ Better diagnosis and monitoring of at-risk groups is encouraged
✓ Housing, climate, age and vulnerability—all major issues for patients—are addressed
✓ It strengthens the case for investment in NAC and wider mycology networks
This report can be used by patient groups, NAC advocates, and healthcare professionals to press for:
-
More referrals
-
Better awareness among GPs and respiratory teams
-
Expanded mycology diagnostic capacity
-
Greater research funding
-
Better antifungal stewardship
-
National fungal surveillance
🌍 THE MICROBIOME REVOLUTION
How gut and lung microbiota are transforming the way we diagnose, treat and understand infection in aspergillosis

For decades, infection was seen through a simple lens:
Find the organism → treat the organism → infection cured.
But modern microbiome research has shown that this view is too narrow—especially for chronic lung diseases such as aspergillosis, bronchiectasis, ABPA, SAFS and CPA.
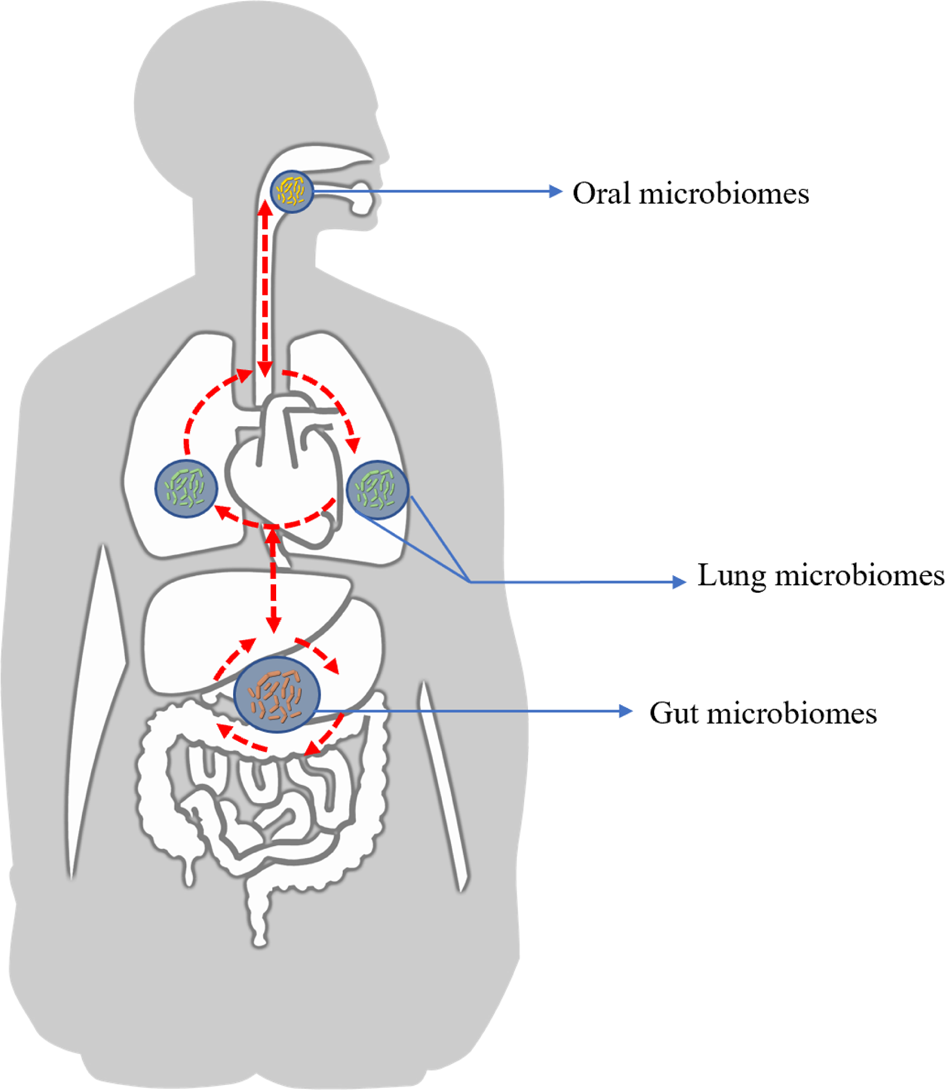
We now understand that the:
-
lungs,
-
gut,
-
sinuses,
-
skin, and even
-
CPA cavities
contain complex microbial ecosystems (bacteria, fungi, viruses, archaea) that interact dynamically with each other and with your immune system.
Rather than being passive passengers, these microbes shape inflammation, immunity, symptoms, resistance, treatment response and overall wellbeing.
This is why microbiome science is truly revolutionising how clinicians think about infection.
🧬 1. What is a microbiome?
A microbiome is the entire community of microorganisms living in a particular environment, plus all the genes, chemicals, signals and interactions that exist between them.
Healthy microbiomes are:
-
diverse
-
stable
-
environmentally balanced
-
dominated by harmless or beneficial species
Disease-associated microbiomes are:
-
less diverse
-
unstable
-
dominated by a few harmful organisms
-
deeply involved in inflammation
This imbalance is called dysbiosis.
🫁 2. The lung microbiome: complex, dynamic, and vital
The lungs are not sterile—they contain a delicate, low-density microbiome.
In health, microbes drift in and out through:
-
breathing
-
micro-aspiration
-
mucociliary clearance
The “healthy lung microbiota” remains balanced because airflow and immune regulation prevent any single species from dominating.
In disease (aspergillosis, bronchiectasis, ABPA, SAFS, CPA), the situation changes:
-
thick mucus traps microbes
-
reduced airflow produces stagnant zones
-
inflammation increases microbial stickiness
-
biofilms form
-
pathogens dominate
-
microbial diversity drops
-
chronic inflammation becomes self-sustaining
This drives persistent symptoms even when cultures appear negative.
🍽️ 3. The gut microbiome: our “second immune system”

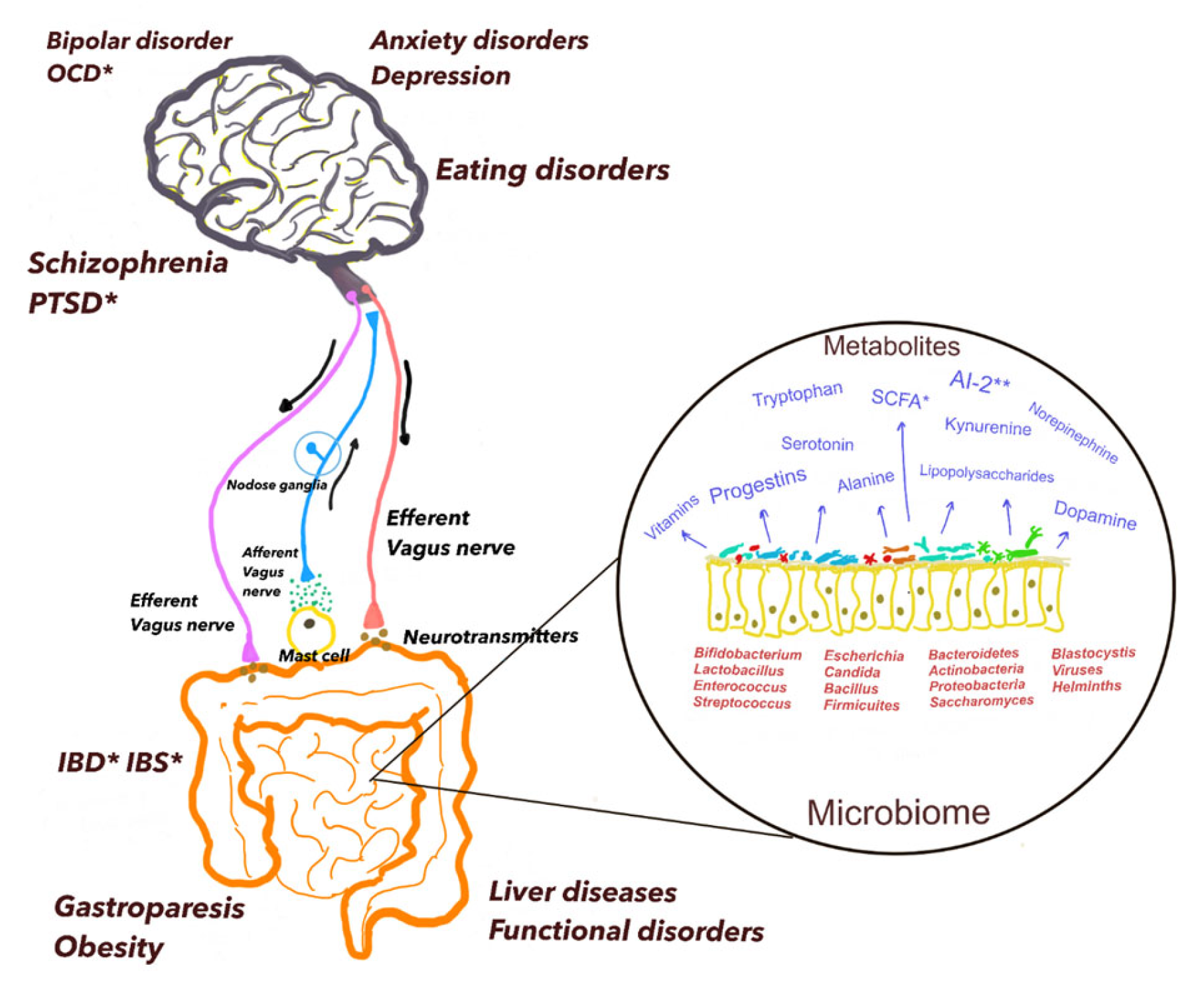
The gut contains trillions of bacteria, fungi and viruses.
Far from being limited to digestion, the gut microbiome influences:
-
immune development
-
inflammation control
-
IgE responses
-
eosinophils
-
energy levels
-
weight regulation
-
steroid responsiveness
-
susceptibility to infection
-
mental wellbeing
Up to 70% of your immune system is shaped by gut microbes.
This means:
Gut health directly affects lung health, including risk and severity of aspergillosis-related disease.
🔄 4. The Gut–Lung Axis: how the two microbiomes talk to each other
The gut and lungs are connected through a biochemical “highway” known as the gut–lung axis.
How the gut affects the lungs
Gut bacteria produce metabolites such as:
-
short-chain fatty acids (SCFAs) — e.g., butyrate
-
tryptophan metabolites
-
bile-acid derivatives
These travel in the bloodstream and regulate:
-
airway inflammation
-
Th2/Th17 immune responses
-
IgE and eosinophils
-
neutrophil activity
-
mucus production
-
tolerance to allergens (including fungal allergens)
-
steroid responsiveness
Low SCFA levels are linked to:
-
more severe asthma
-
worse fungal sensitisation
-
increased ABPA flares
-
poorer lung function
-
difficulty clearing infection
How lung disease affects the gut
Chronic respiratory disease increases:
-
gut permeability (“leaky gut”)
-
microbiota disruption
-
systemic inflammation
-
digestive symptoms
-
fatigue
-
candida overgrowth
Steroids and antibiotics worsen this further.
This creates a self-reinforcing circle of inflammation and dysbiosis.
🧱 5. Biofilms: microbial fortresses driving persistent disease
Biofilms are communities of microbes encased in a sticky protective matrix.
In aspergillosis and bronchiectasis, biofilms:
-
make organisms up to 100–1000× more resistant to treatment
-
protect microbes from the immune system
-
allow bacteria and fungi to communicate and collaborate
-
swap resistance genes
-
support mixed infections (e.g., Aspergillus + Pseudomonas)
-
cause chronic symptoms even with “negative” cultures
Biofilms also change the immune system’s behaviour, driving long-term inflammation.
🔬 6. What microbiome research has revealed so far
A. Infection is rarely a single organism
Microbiomes show that infections are polymicrobial ecosystems, not isolated pathogens.
B. Diversity = resilience
Higher microbial diversity is linked to:
-
better lung stability
-
fewer flare-ups
-
lower inflammation
Low diversity correlates with:
-
severe disease
-
CPA progression
-
ABPA flares
-
worse bronchiectasis outcomes
C. Microbiome patterns can predict future illness
Research shows that flare-ups often follow:
-
a drop in diversity
-
an increase in dominant pathogens
-
changes in fungal–bacterial interactions
D. Treatment responses are microbiome-dependent
The presence of certain bacteria can make Aspergillus:
-
grow faster
-
form stronger biofilms
-
resist antifungals
-
provoke more inflammation
🫁🌱 7. What patients can do to support their lung microbiota
Just as dietary fibre supports gut microbes, there are practical steps that support a healthier lung microbial ecosystem.
These steps do not introduce microbes into the lungs; instead, they improve the environment the microbiota lives in.
⭐ 1. Keep airways clear — the foundation of lung microbial health
Biofilms and harmful microbes thrive in stagnant mucus.
Effective clearance techniques:
-
Active Cycle of Breathing Techniques (ACBT)
-
Autogenic drainage
-
Oscillating devices (Flutter, Acapella, Aerobika)
-
Nebulised saline (3–7%)
-
Huffing and controlled coughing
Clearer airways → more airflow → better microbial balance.
⭐ 2. Hydration
Hydration thins mucus, improves ciliary function, and weakens biofilms.
⭐ 3. Use inhalers correctly & control inflammation
Inflamed, narrowed airways promote dysbiosis.
Good control of:
-
asthma
-
ABPA
-
eosinophilia
reduces microbial imbalance.
⭐ 4. Improve sinus health
The sinuses drip microbes into the lungs all day long.
Sinus care (saline rinses, nasal steroids) supports lung microbiota stability.
⭐ 5. Avoid unnecessary antibiotics
Antibiotics disrupt:
-
lung microbiota
-
gut microbiota
-
fungal–bacterial balance
-
biofilm behaviour
Use them when needed — but avoid repeated unnecessary courses.
⭐ 6. Exercise
Exercise increases airflow and clearance, helping shift the lung microbiome toward a healthier, more diverse state.
⭐ 7. Reduce smoke and indoor pollutants
Pollutants:
-
paralyse cilia
-
thicken mucus
-
promote pathogenic microbes
-
reduce diversity
HEPA filtration, ventilation, and smoke avoidance all help.
⭐ 8. Manage reflux (GORD)
Micro-aspiration introduces stomach contents into the lungs, disrupting the lung microbiota.
Treating reflux supports lung microbial homeostasis.
⭐ 9. Support your gut microbiota
A healthy gut → more SCFAs → improved lung immunity → a more balanced lung microbiome.
Helpful for gut health:
-
fibre-rich foods
-
diverse diet
-
fermented foods (if tolerated)
-
avoiding unnecessary antibiotics
-
reducing alcohol
-
managing stress
🩺 8. What this means for the future of aspergillosis care
Within 5–10 years, we may routinely use:
-
microbiome sequencing in clinic
-
AI-designed “ecosystem maps” of the lungs
-
targeted therapies for mixed infections
-
inhaled agents that break down biofilms
-
gut-directed therapies to help lung disease
-
personalised airway clearance plans
-
microbial diversity scores to predict flares
This could:
-
reduce exacerbations
-
minimise antibiotic and antifungal exposure
-
improve quality of life
-
slow CPA progression
-
improve steroid responsiveness
-
reduce hospital admissions
🧠 9. Key takeaways
-
You have two important microbiomes that matter for aspergillosis:
the lung microbiome and the gut microbiome. -
They communicate through the gut–lung axis.
-
Dysbiosis (imbalance) increases inflammation and worsens fungal disease.
-
Biofilms make infections far more resistant and persistent.
-
Patients can support their lung microbiota through lifestyle steps, especially:
-
airway clearance
-
hydration
-
exercise
-
sinus care
-
avoiding unnecessary antibiotics
-
supporting gut health
-
-
Microbiome science is transforming future diagnosis and treatment strategies.
Verified UK Resources for Damp, Mould & Health
Here is a short, reliable, UK-verified list of resources for people worried about damp, mould and health. Each link is trustworthy, evidence-based, and not influenced by companies selling testing or “mycotoxin cleanses”.
1. NICE – Damp and Mould Guidelines
This guideline covers indoor air quality in residential buildings. It aims to raise awareness of the importance of good air quality in people's homes and how to achieve this.
🔗 https://www.nice.org.uk/guidance/NG149
2. UK Health Security Agency (UKHSA) – Damp & Mould Health Guidance
The most authoritative public health guidance used by councils, housing providers, and clinicians.
Includes:
-
How mould affects health
-
Who is at higher risk
3. Shelter – Tenant Rights on Damp and Mould
For renters needing practical, legal steps to get repairs done.
🔗Damp and mould in private rented homes
🔗Damp and mould in council and housing association homes
4. Citizens Advice – Step-by-Step Action for Damp Problems
Simple language, includes letter templates for landlords.
🔗 https://www.citizensadvice.org.uk/housing/repairs-and-housing/repairs-and-housing-conditions/whos-responsible-for-repairs/repairs-damp/
5. Housing Ombudsman – Damp & Mould Guidance for Social Housing
Very helpful for council and housing association tenants dealing with delays or poor responses.
🔗 https://www.housing-ombudsman.org.uk/damp-and-mould/
6. Awaab’s Law Information (Housing Ombudsman)
Sets strict deadlines for social landlords to investigate and fix reported damp/mould.
🔗 https://www.housing-ombudsman.org.uk/centre-for-learning/key-topics/awaabs-law/
7. Asthma + Lung UK – Mould and Breathing Problems
Good for people with asthma, COPD, ABPA or bronchiectasis.
Practical tips and when to seek medical help.
🔗 https://www.asthmaandlung.org.uk/blog/advice-support/know-your-rights-what-do-if-you-have-damp-mould-rented-home
8. London Fire Brigade – Safe Use of Dehumidifiers & Ventilation Advice
Useful because many people misuse heaters or dehumidifiers while trying to “dry out” a home.
🔗https://www.london-fire.gov.uk/safety/
9. Royal Institution of Chartered Surveyors
The Royal Institution of Chartered Surveyors (RICS) is the global professional body setting standards for land, property, construction and the built environment. Its members help ensure that buildings and infrastructure are safe, well-managed and sustainable, providing trusted expertise for governments, industry and the public.
https://www.rics.org/consumer-guides/damp-and-mould
Optional extras (carefully chosen):
World Health Organization – Indoor Dampness & Health Review
A global evidence assessment → helps debunk myths about “toxic mould” testing.
🔗 https://www.who.int/publications/i/item/9789289041683
Important reassurance you can give people
These sources are aligned on three key points:
✔ Mould exposure can worsen asthma, allergies and respiratory illness.
Especially in children, older adults, and people with chronic lung conditions (like ABPA, CPA, bronchiectasis).
✔ Mycotoxins in UK homes are not a common cause of chronic, systemic illness.
Reputable agencies (NHS, UKHSA, WHO) do not support “mycotoxin testing” or expensive “detox” treatments.
✔ Fixing the building is the most important treatment.
Ventilation, reducing humidity, removing contaminated soft furnishings, and remediation are the real interventions.
Aspergillosis Research Highlights — Week in Review (Last 7 Days: Week 50)
Seven key publications: pathogenicity, diagnostics, resistance, treatment, maxillofacial disease, and ABPA in COPD.
1. Comparative Overview of A. fumigatus, A. flavus, and A. niger
Rafique et al., J Infect Public Health, 2025
DOI: 10.1016/j.jiph.2025.103070
What this adds
-
A major comparative review (2000–2025) of the three most clinically relevant Aspergillus species.
-
Highlights broad clinical spectrum: allergy → chronic disease → invasive aspergillosis.
-
Identifies species-specific concerns:
-
A. fumigatus: globally dominant, rapidly evolving triazole resistance.
-
A. flavus: important in warmer climates; high aflatoxin relevance.
-
A. niger: relatively lower virulence but significant in sinus disease.
-
-
Public health message: surveillance gaps persist, especially for non-fumigatus species.
Why it matters
A strong reference paper supporting the WHO prioritisation of Aspergillus, and reinforcing the need for:
-
Better diagnostics
-
Species-level identification
-
Environmental resistance monitoring
2. GFP Fusion Protein Proteolysis in A. fumigatus
Paul & Moye-Rowley, G3 (Bethesda), 2025
DOI: 10.1093/g3journal/jkaf295
What this adds
-
Fundamental molecular biology study revealing regulated degradation pathways of green fluorescent protein (GFP) fusion proteins inside A. fumigatus.
-
Demonstrates how the fungus controls protein turnover under stress conditions.
Why it matters
-
Advances tools for fungal cell biology.
-
Supports drug development by clarifying pathways involved in stress response and antifungal tolerance.
-
Reinforces WHO’s classification of A. fumigatus as one of the four most critical fungi to study.
3. ABPA in COPD: Case Series + Review
Ren et al., BMC Pulmonary Medicine, 2025
DOI: 10.1186/s12890-025-04027-8
What this adds
-
11 COPD cases with confirmed Allergic Bronchopulmonary Aspergillosis — highlighting:
-
Under-recognition in COPD
-
Overlap with chronic bronchitis/bronchiectasis symptoms
-
Frequent misdiagnosis as recurrent infections or COPD exacerbations
-
-
Provides diagnostic guidance and a literature synthesis.
Why it matters
-
Significant implications for case finding across the UK.
-
Supports NAC messaging: ABPA is not only an asthma disease.
-
Reinforces need for:
-
IgE/IgG screening
-
Early CT imaging
-
Awareness among COPD teams and primary care
-
4. EL219: Next-Generation Polyene Antifungal
Youssef et al., AAC, 2025
DOI: 10.1128/aac.01400-25
What this adds
-
Animal model evidence that EL219, a modern polyene, is effective against:
-
Triazole-susceptible A. fumigatus
-
Azole-resistant isolates
-
Difficult species (A. lentulus, A. calidoustus)
-
Why it matters
-
Highly relevant to rising global antifungal resistance.
-
Early indication that EL219 may fill a clinical gap similar to (or complementary to) olorofim and fosmanogepix.
-
Suggests strong activity even in immunosuppressed models.
5. Misidentification & Triazole Resistance in Aspergillus tubingensis
Wang et al., JAMA Network Open, 2025
DOI: 10.1001/jamanetworkopen.2025.43630
What this adds
-
Large Southern California population study showing:
-
Frequent misidentification of A. tubingensis as A. niger.
-
Notable azole resistance rates in correctly identified isolates.
-
-
Stresses need for genomic sequencing or MALDI-TOF with updated libraries.
Why it matters
-
Strong evidence that misidentification leads to:
-
Inappropriate antifungal therapy
-
Poor outcomes
-
-
Supports calls for expanded diagnostic reference services such as MRCM.
6. 50-Year Review of Oral Fungal Infections in Thailand
Kosanwat et al., Clinical Oral Investigations, 2025
DOI: 10.1007/s00784-025-06685-8
What this adds
-
Longitudinal study: 29% of deep infections involved aspergillosis.
-
Mean age 62 → older adults most affected.
-
Many cases were mucormycosis, histoplasmosis, or aspergillosis presenting late.
Why it matters
-
Shows that oral/maxillofacial fungal disease remains under-recognised globally.
-
Relevant to dental teams → better imaging + biopsy protocols needed.
-
May help NAC/CARES identify referral pathways from dental medicine.
7. Management of Maxillary Sinus Aspergillosis with Implants
Khoury et al., Int J Oral Implantol, 2025
What this adds
-
Real-world 3–10 year follow-up of 11 patients.
-
Standardised approach:
-
Surgical clearance
-
Antifungal therapy
-
Successful implant-prosthetic rehabilitation
-
Why it matters
-
Demonstrates excellent long-term outcomes when sinus aspergillosis is properly treated.
-
Practical implications for:
-
ENT surgeons
-
Oral surgeons
-
Implant dentistry
-
-
Supports inclusion of aspergillosis in sinus disease differential diagnosis.
Cross-Cutting Themes Emerging This Week
1. Under-recognition and misidentification
-
ABPA in COPD
-
Misidentified A. tubingensis
-
Asymptomatic sinus disease
-
Oral/maxillofacial deep fungal infections
→ Key NAC message: We are missing cases in primary care, COPD clinics, ENT, and dentistry.
2. Antifungal resistance remains a central threat
-
Contemporary reviews of species-specific resistance patterns
-
EL219’s promise against resistant species
-
Misidentification leading to incorrect susceptibility assumptions
3. Need for better diagnostics and reference centres
-
Species-level identification is essential
-
Supports arguments for expansion of MRCM-style national services
4. The clinical spectrum is broad
From allergy (ABPA in COPD) → chronic sinus disease → deep oral infections → invasive pulmonary aspergillosis.
This reinforces the message: aspergillosis is multi-specialty, not confined to respiratory medicine.
Weekly NAC/MRCM Take-Home Messages
-
COPD teams should screen for ABPA more frequently—especially in patients with recurrent “infective exacerbations.”
-
Species-level identification is increasingly important; misidentification contributes to treatment failure.
-
New antifungals like EL219 show promise against resistant strains including A. lentulus.
-
Dental and ENT teams need better awareness: sinus and oral fungal infections remain overlooked but treatable.
-
Global reviews show growing public health significance of Aspergillus species—aligning with WHO priorities.
Biofilms: what they are, why they cause persistent infection, and how research is changing treatment
1. What exactly is a biofilm?
A biofilm is a structured community of microbes—bacteria, fungi, or a mixture—that attaches to a surface and produces a self-generated protective matrix.
The building blocks
Biofilms contain:
-
Cells: e.g., Aspergillus fumigatus, Pseudomonas aeruginosa, Staphylococcus aureus
-
Extracellular polymeric substances (EPS):
-
Sticky sugars (polysaccharides)
-
Proteins
-
DNA released from dead cells (eDNA)
-
Lipids
These form the thick “slime” layer.
-
Microbial ‘specialisation’
Within a biofilm, microbes change behaviour:
-
Some become slow-growing persister cells, which survive drug exposure.
-
Others produce signalling molecules (“quorum sensing”) to coordinate defence systems.
-
The deeper layers become low-oxygen and acidic, making antifungals and antibiotics less effective.
Where do biofilms form in lung disease?
-
In bronchiectatic airways, where mucus stagnates
-
Around Aspergillus cavities in chronic pulmonary aspergillosis (CPA)
-
In mucus plugs in ABPA
-
In sinuses of patients with chronic fungal sinusitis
-
On medical devices (catheters, stents)
2. Why biofilms create so many problems
Biofilm problem 1: Immense drug resistance
Microbes in biofilms can be 100–1,000× more tolerant to antifungals/antibiotics.
This is due to:
-
EPS matrix blocking drug penetration
-
Slow metabolic rate → drugs that target growth become less effective
-
Persister cells surviving even high doses
-
Enzymes in the biofilm breaking down drugs
Aspergillus biofilms show increased resistance to:
-
Azoles (itraconazole, voriconazole)
-
Amphotericin B
-
Echinocandins to a lesser extent
Pseudomonas biofilms resist:
-
Ciprofloxacin
-
Colistin (partially)
-
Beta-lactams
This helps explain your recent comment about Pseudomonas now being resistant even though you haven’t used ciprofloxacin for years—biofilms drive spontaneous resistance through evolution, stress responses, and gene exchange.
Biofilm problem 2: Immune evasion
Immune cells (neutrophils, macrophages) cannot easily penetrate the EPS layer.
This leads to:
-
Incomplete clearance → long-term infection
-
Chronic inflammation → lung damage, fatigue
-
Continuous mucus production triggered by inflammation
For Aspergillus, the fungus can switch genes on/off to avoid immune detection when it grows as a biofilm-like sheet rather than as airborne spores.
Biofilm problem 3: Mixed infections behave differently
When bacteria and fungi coexist, they interact:
-
Pseudomonas produces molecules that stimulate Aspergillus regrowth, or vice versa
-
Each organism’s biofilm strengthens the other
-
Mixed biofilms activate more intense inflammation
-
They can shift the entire lung microbiome into a more disease-promoting “ecology”
This is why people with bronchiectasis or ABPA often experience:
-
Frequent exacerbations
-
Slow recovery
-
Mucus plugging
-
Worsening lung function over time
3. Why people with aspergillosis and bronchiectasis are especially vulnerable
Stagnant mucus
Biofilms love:
-
Thick mucus
-
Low airflow
-
Damp surfaces
All of which are present in:
-
Bronchiectasis
-
ABPA (due to mucus plugging)
-
Chronic pulmonary aspergillosis
-
Severe asthma with fungal sensitisation (SAFS)
Altered immunity
Long-term steroid use, high IgE, eosinophilia, and chronic inflammation all influence how readily biofilms form and how well the immune system can clear them.
Frequent antibiotic/antifungal exposure
This shapes the microbial community in a way that makes biofilms more likely and more resistant.
4. What we are doing to tackle biofilms
A. Current clinical strategies
1. Airway clearance is the single most effective biofilm disruptor
Physiotherapy techniques that help:
-
ACTs (Active Cycle of Breathing Techniques)
-
Oscillating devices (Flutter, Acapella)
-
Postural drainage
-
Autogenic drainage
-
Saline nebulisation
These physically remove biofilms, which no drug can fully achieve alone.
2. Nebulised therapies
-
Hypertonic saline (3–7%) helps break down mucus and destabilise the EPS matrix
-
Inhaled antibiotics (tobramycin, colistin, aztreonam) target bacterial biofilms
-
Nebulised antifungals are being explored, though not yet standard care
3. Anti-inflammatory control
Steroids/biologics help reduce airway swelling and mucus stasis, indirectly reducing biofilm formation.
4. Managing comorbidities
-
Reducing reflux
-
Improving sinus clearance
-
Treating asthma aggressively
All reduce the “fuel” available to biofilms.
B. Research and innovation
1. New antifungals with anti-biofilm activity
-
Olorofim
-
Fosmanogepix
-
Ibrexafungerp
These show better penetration and less susceptibility to biofilm-related resistance.
2. Quorum sensing blockers
Compounds that prevent microbes from “communicating” so they cannot coordinate a biofilm. In trials for Pseudomonas.
3. Enzymes to dissolve the biofilm matrix
Research into:
-
DNases
-
Polysaccharide-breaking enzymes
-
Surfactants
These aim to weaken the EPS “scaffolding”.
4. Microbiome-based approaches
Understanding how lung microbial ecosystems shift in disease could allow:
-
Removal of harmful species
-
Strengthening protective species
-
Reducing biofilm formation overall
5. Combination therapies
Antifungal + antibiotic + mucolytic
is likely the future for patients with mixed fungal–bacterial biofilms.
5. Key takeaways
-
Biofilms are highly organised microbial fortresses that are difficult for drugs and the immune system to reach.
-
They cause persistent infection, inflammation, and drug resistance.
-
In aspergillosis and bronchiectasis, they play a central role in ongoing symptoms and flare-ups.
-
Airway clearance remains the cornerstone of treatment today.
-
New antifungals, antibiofilm agents, and microbiome therapies offer real hope for breaking biofilm-related disease cycles.
Why do some people cough up long, tube-shaped pieces of mucus?
In several chronic lung conditions, the airways can become inflamed and produce thick mucus.
When this mucus sits in the bronchial tubes, it can sometimes harden into a cast shaped exactly like the airway.
People often describe these casts as:
-
long, ribbon-like or “snakeskin” pieces
-
rubbery or stretchy
-
white, yellow, or green
-
shaped like the inside of a tube
Coughing one up can feel dramatic but is usually a sign that your lungs are finally able to clear a blockage.
What does it mean if a cast has black flecks or dark spots?
This can look alarming, but several common, mostly harmless explanations exist.
1. Old or dried blood
Tiny amounts of bleeding from irritated airways can dry and turn:
red → brown → black
This often appears as tiny black dots or threads.
2. Inhaled particles
Dust, soot, pollution, or smoke can get trapped in mucus deeper in the lungs and show up as dark specks.
3. Debris from infection or inflammation
Long-standing inflammation can cause:
-
darkened mucus fragments
-
tiny bits of fungal, bacterial or biofilm material
-
oxidised (darkened) mucus layers
These often look like pepper-like flecks and are not dangerous on their own.
4. Oxidation or ageing of thick mucus
When mucus sits for a long time before it is coughed out, it can become darker in spots.
When this is usually not worrying
Black flecks are often harmless when:
-
the amount is small
-
the colour change is occasional
-
you feel better after coughing the cast out
-
there is no new increase in blood, fever, or breathlessness
-
this fits your usual pattern of mucus plugging
Most people with chronic airway disease experience occasional colour changes in mucus.
When to mention it to your doctor
You should let your team know if:
-
black flecks keep appearing repeatedly
-
you cough up more blood than usual
-
your breathing worsens suddenly
-
your sputum smells different
-
you have fever or chest pain
-
casts become bigger, more frequent, or harder to clear
These changes do not always mean something serious, but they are worth checking.
Why do casts form in the first place?
Conditions that can cause airway casts include:
-
Bronchiectasis
-
ABPA (Allergic Bronchopulmonary Aspergillosis)
-
Severe or eosinophilic asthma
-
Chronic infections, including fungal or bacterial
-
COPD with mucus hypersecretion
Inflammation makes mucus thicker, and narrowed airways make it harder to clear.
Over time, mucus can mould itself into the shape of the airway — becoming a cast.
What to do if you cough one up
-
Stay calm — this often brings relief.
-
Take note of its colour and size.
-
Hydrate well to thin mucus.
-
Continue your usual airway-clearance technique (physio, nebulisers, saline, etc.)
-
Let your team know if it is unusual for you.
Final reassurance
Coughing up a long, tube-like piece of mucus can feel shocking, but in most cases it simply means your lungs are clearing a blocked area.
Black flecks are usually:
-
old blood
-
trapped dust or soot
-
dried mucus debris
Most of the time, these findings are not dangerous, but they can give useful clues about airway inflammation.
**Understanding Your Immune System:
A Simple Guide for Aspergillillosis Patients and Carers**
Part of the Aspergillosis Immune System Knowledge Hub
(See also: Articles 2, 3, and 4)
When you live with aspergillosis, asthma, bronchiectasis, or fungal allergy, the immune system plays a major role in your symptoms and how your condition behaves. This article explains the key parts of the immune system in a clear, accessible way.
🧬 1. B Cells — the Antibody Makers
B cells produce antibodies, which act like “tags” that help the immune system recognise germs.
They make different types, including:
-
IgE — triggers allergy
-
IgG — provides long-term immunity and helps diagnose chronic infection
-
IgA — protects the nose, throat, and gut
In Aspergillosis:
-
ABPA: B cells overproduce IgE against Aspergillus.
-
CPA: High Aspergillus IgG helps confirm chronic infection.
-
SAFS/Bronchitis: Mixed or subtle antibody patterns.
🧠 2. T Cells — the Immune System’s Directors
T cells guide and regulate the immune response.
Types include:
-
Helper T cells (Th cells): tell B cells what antibodies to make
-
Killer T cells: destroy infected or damaged cells
-
Regulatory T cells: calm the immune system and prevent over-reaction
In Aspergillosis:
-
ABPA: Helper T cells become overactive, driving allergic inflammation.
-
CPA: T cells attempt to control fungal growth but cannot fully clear it.
🟡 3. IgE — the Allergy Antibody
IgE causes:
-
wheezing
-
swelling
-
itching
-
mucus production
-
allergic reactions
In ABPA, IgE levels become very high because the body incorrectly treats Aspergillus as a major allergen.
🟢 4. IgG — the Memory and Detection Antibody
IgG helps the immune system remember past infections.
A raised Aspergillus IgG level is one of the main tests for CPA.
🔥 5. Mast Cells — the Alarm Cells
Mast cells sit in the lungs, nose, sinuses, skin, and gut.
When triggered (often by IgE), they release:
-
histamine
-
leukotrienes
-
inflammatory chemicals
This causes:
-
wheezing
-
chest tightness
-
mucus production
-
itching or burning sensations
-
coughing
They are very active in ABPA and severe asthma.
🌈 6. Histamine — Why Symptoms Feel the Way They Do
Histamine release leads to:
-
swelling and redness
-
increased mucus
-
nerve irritation → itch, tickle, burning
-
airway narrowing → wheeze and breathlessness
This explains why flare-ups can feel sudden or “out of proportion” to test results.
🧩 7. Putting It Together: Immune Pathways in Aspergillosis
| Condition | Dominant Antibody | Key Cells | Symptoms Driven By |
|---|---|---|---|
| ABPA | Very high IgE | Mast cells, eosinophils | Allergy, mucus, flare-ups |
| CPA | Raised IgG | T cells, macrophages | Chronic inflammation, cavities |
| SAFS/Allergic asthma | IgE ± eosinophils | Mast cells, eosinophils | Wheeze, mucus, sensitivity |
| Aspergillus bronchitis | Variable | Neutrophils, airway cells | Cough, sputum, recurring infections |
Understanding these pathways helps you and your clinical team choose the right treatments.
Next articles:
- **Understanding your immune system
- How the Immune System Knows “Self”
- What Happens in Autoimmune Disease (Addison’s Explained)
- Eosinophils and Type-2 Inflammation in Aspergillosis
- **Where Do All These Immune Cells Live, and Where Are They Made?