The Power of Keeping a Health Diary When You Have Aspergillosis

Last reviewed: June 2026
Audience: People living with aspergillosis, families and carers
Key points
- A health diary can help you understand symptoms, triggers and changes over time.
- It can be especially useful if you experience fatigue, brain fog or memory problems.
- It can make clinic appointments more focused and productive.
- A diary may show progress that is hard to notice day to day.
- The best diary is simple, quick and realistic to keep using.
Contents
- Why keep a health diary?
- How it can help with aspergillosis
- Brain fog and memory
- Spotting patterns and triggers
- Using your diary at appointments
- The psychological benefit
- Simple diary template
- Common questions
- When to seek medical advice
Why keep a health diary?
Living with aspergillosis often means symptoms change from day to day. Some days may be manageable. Others may involve more coughing, breathlessness, fatigue, sinus symptoms, poor sleep or medication side effects.
Because these changes can happen gradually, it can be difficult to remember exactly when symptoms started, whether they are getting better or worse, or what might have triggered them.
A health diary gives you a simple record of what is happening over time. It can help you, your family and your healthcare team see patterns that may not be obvious from memory alone.
How a diary can help with aspergillosis
People with aspergillosis may find it useful to record:
- Cough
- Breathlessness
- Fatigue
- Sputum or phlegm
- Wheeze
- Sinus symptoms
- Sleep quality
- Exercise or walking distance
- Mood and wellbeing
- Medication changes
- Possible side effects
You may also want to note possible triggers, such as damp or mould exposure, pollen, dusty environments, changes in weather, respiratory infections, stress, travel or changes in medication.
Brain fog and memory
Many people with long-term lung conditions describe episodes of brain fog. This may feel like forgetfulness, poor concentration, difficulty finding words, feeling mentally slower than usual, or feeling as though your head is “empty”.
Brain fog can have many possible causes, including fatigue, poor sleep, infection, inflammation, stress, anxiety, pain, medication side effects, low oxygen levels or other health problems.
A diary acts as an external memory. Instead of trying to remember when something changed, you can look back and see what was happening at the time.
Spotting patterns and triggers
| What you record | What it may help show |
|---|---|
| Symptoms | Whether cough, breathlessness or fatigue are improving or worsening |
| Sleep | Whether poor sleep is linked to worse symptoms |
| Exercise | What level of activity is manageable |
| Weather | Whether heat, humidity, cold air or storms affect symptoms |
| Environment | Possible links with damp, mould, dust or pollen |
| Medication | Possible benefits, side effects or changes during dose reduction |
| Infections | Early warning signs or repeated patterns |
Using your diary at appointments
Healthcare professionals may ask questions such as:
- When did your symptoms start?
- Are they getting better or worse?
- Have you noticed any triggers?
- Have you changed any medication recently?
- How far can you walk now compared with before?
- Have you had any infections or courses of antibiotics?
These questions are not always easy to answer from memory, especially when you are tired or anxious. A diary can help you give clearer, more accurate information.
You may find it useful to bring a short summary to your appointment, such as:
- Three things that have improved
- Three things that have worsened
- Any medication changes
- Your main questions for the appointment
Sometimes the diary tells a different story
When you have had a difficult few days, it can feel as though nothing is improving. A diary may show that the wider picture is more encouraging.
For example, you may feel:
“Nothing has changed.”
But your diary may show:
- You are walking further than three months ago
- You are sleeping better
- You have had fewer chest infections
- You are coughing less at night
- You are doing more social activities
Equally, a diary can show gradual deterioration that might otherwise be missed. Both types of information can be useful.
The psychological benefit
Chronic illness can feel unpredictable. A diary can help restore a sense of control by changing the question from:
“Why do I feel awful?”
to:
“What changed recently?”
This can reduce uncertainty and help you feel more involved in your care.
A diary can also become a record of resilience. It may include difficult days, but it can also capture walks completed, holidays taken, family events attended, personal goals reached and challenges overcome.
Keep it simple
Many people stop keeping a diary because they try to record too much. A simple diary is usually more useful than a complicated one.
A daily entry might take less than two minutes and include:
- Symptoms, scored from 0 to 10
- Energy level, scored from 0 to 10
- Sleep quality
- Exercise or activity
- Medication changes
- Anything unusual
Consistency matters more than detail.
Paper, phone or app?
There is no single correct way to keep a diary. You could use:
- A notebook
- A printed diary sheet
- A phone notes app
- A calendar
- Voice notes
- A spreadsheet
- A symptom tracking app
- A fitness tracker or smartwatch
The best diary is the one you will actually use.
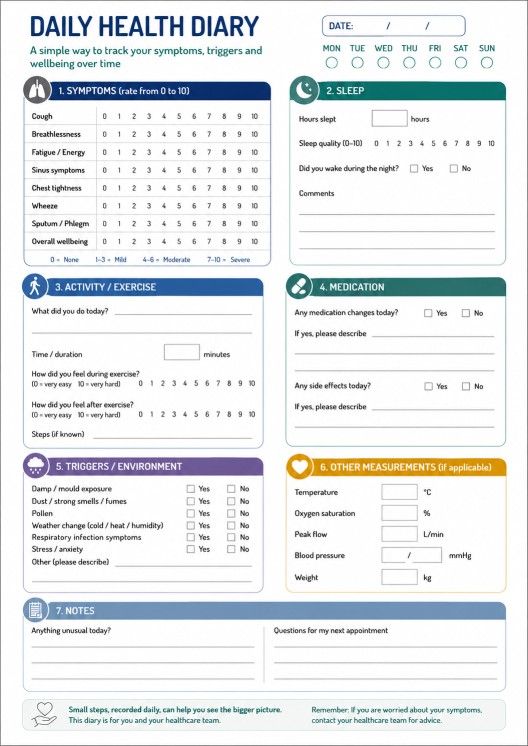
Simple diary template
Daily health diary
Date: __________________________
Symptoms, 0–10
Cough: ______
Breathlessness: ______
Fatigue: ______
Sinus symptoms: ______
Overall wellbeing: ______
Sleep
Hours slept: ______
Sleep quality, 0–10: ______
Activity
Exercise or activity today:
__________________________________________________
Medication
Any medication changes or side effects?
__________________________________________________
Notes
Anything unusual today?
__________________________________________________
__________________________________________________
Daily Diary - PDF downloadable
Common questions
Do I need to write every day?
No. Some people write daily. Others only record changes, flare-ups, medication changes or important events.
What if I forget for a few days?
That is very common. Simply restart when you remember. A diary does not have to be perfect to be useful.
Should I record test results?
You can if you find it helpful. Some people record blood results, oxygen saturations, lung function, weight, clinic letters or medication levels. Do not worry if this feels too much. A simple symptom diary is still useful.
Can a diary replace medical advice?
No. A diary is a tool to support conversations with your healthcare team. It should not be used to diagnose or treat symptoms without medical advice.
When to seek medical advice
Seek medical advice promptly if you experience:
- Sudden or significant worsening of breathlessness
- Coughing up large amounts of blood
- Persistent fever
- Severe chest pain
- New confusion or rapidly worsening brain fog
- Weakness, speech problems, facial drooping or visual changes
- Symptoms that are worsening quickly or feel unusual for you
If you are unsure, contact your healthcare team, NHS 111, your GP, or emergency services depending on severity.
Further information
- Living with aspergillosis
- Fatigue and aspergillosis
- Exercise and aspergillosis
- Mental wellbeing and aspergillosis
Author and review information
This article is provided for general educational support for people affected by aspergillosis. It is not a substitute for medical advice from your own healthcare team.
Prepared for: Aspergillosis.org
Last reviewed: June 2026
Do You Carry Your Aspergillosis Information With You?

New NHS Plans Could Help in Future – But What About Today?
The UK government is currently debating plans for a new NHS “single patient record” system. The aim is to allow authorised healthcare professionals to access important information from GP surgeries, hospitals, community services and other parts of the NHS more easily.
If implemented successfully, this could reduce the need for patients to repeatedly explain their medical history and could help emergency departments, ambulance crews and other healthcare professionals see important information such as diagnoses, medications, allergies and previous treatment.
For people living with aspergillosis and other long-term respiratory conditions, this could be especially valuable. However, these changes will take time to develop and introduce. For now, patients remain one of the most important links between different parts of the healthcare system.
Why This Matters for Aspergillosis Patients
Many people with aspergillosis receive care from several different services, including:
- General Practitioners (GPs)
- Local respiratory teams
- Specialist nurses
- Hospital clinics
- Emergency departments
- Pharmacists
- Community healthcare teams
- Specialist centres such as the National Aspergillosis Centre
Healthcare records are not always immediately available to every professional involved in your care. This means there may be times when you need to explain:
- What type of aspergillosis you have
- Which medications you take
- Any important allergies or serious drug reactions
- Whether you have adrenal insufficiency or take long-term steroids
- Who your specialist team is
- What previous treatments you have received
Having this information readily available can save time and may help healthcare professionals make decisions more quickly and safely.
What Information Should You Carry?
 You do not need to carry your entire medical record. A simple one-page health summary is usually enough.
You do not need to carry your entire medical record. A simple one-page health summary is usually enough.
1. Your Diagnosis
List your main diagnoses clearly. Examples include:
- Allergic Bronchopulmonary Aspergillosis (ABPA)
- Chronic Pulmonary Aspergillosis (CPA)
- Severe Asthma with Fungal Sensitisation (SAFS)
- Aspergillus Bronchitis
- Bronchiectasis
- Severe Asthma
- Chronic Obstructive Pulmonary Disease (COPD)
2. Your Current Medications
Include all current treatments, particularly:
- Antifungal medications, such as itraconazole, voriconazole, posaconazole or isavuconazole
- Steroid tablets
- Hydrocortisone replacement therapy
- Biologic therapies
- Inhalers
- Oxygen therapy
- Antibiotics you are currently taking
Try to keep this list up to date.
3. Drug Allergies and Serious Reactions
This is one of the most important sections. Include any known allergies or serious reactions, for example:
- Penicillin allergy
- Prednisolone allergy
- Previous severe drug reactions
- Medicines you have been told to avoid
4. Steroid or Adrenal Information
If you have adrenal insufficiency or are taking long-term steroid treatment, make this very clear.
I have adrenal insufficiency and may require emergency steroid treatment if seriously unwell.
Many patients already carry a steroid emergency card. If you have been advised to carry one, continue to carry it at all times.
5. Specialist Contact Information
Include:
- Consultant name
- Hospital or specialist centre
- Clinic or specialist nurse contact details, if available
6. Emergency Contact
Include:
- Name
- Relationship
- Telephone number
An Important Extra Note for Aspergillosis Patients
Many antifungal medications interact with other medicines. If you take itraconazole, voriconazole, posaconazole or isavuconazole, consider including the following statement on your health summary:
I take an azole antifungal medication. Please check for potential drug interactions before prescribing new medicines.
This simple statement may help avoid medication-related problems.
If You Are a National Aspergillosis Centre Patient: Using myMFT
If you are a patient of the National Aspergillosis Centre (NAC), you may already have access to some of your hospital information through the myMFT patient portal.
myMFT is the patient portal used by Manchester University NHS Foundation Trust (MFT), which includes Wythenshawe Hospital and the National Aspergillosis Centre.
Depending on the services you use, myMFT may allow you to:
- View MFT appointment details
- Access clinic letters
- Keep track of important test results, letters and health information
- Attend online video consultations
- Use proxy access to help manage a family member’s healthcare, with consent
Many patients find it useful to keep copies of important clinic letters on their phone or tablet. This can be particularly helpful if you attend another hospital, visit your GP, travel away from home or need emergency treatment.
myMFT does not replace a future NHS-wide patient record, but it can provide access to important information that may help you and your healthcare professionals manage your care more effectively.
Find out more about myMFT on the Manchester University NHS Foundation Trust website.
For Patients Not Under the National Aspergillosis Centre
If you are not an NAC or MFT patient, your local hospital may have its own patient portal or online record system. Ask your hospital clinic, respiratory team or GP surgery whether you can access clinic letters, appointment information or test results online.
You may also be able to use the NHS App to manage parts of your healthcare, depending on your GP surgery and local NHS services.
Find out more about the NHS App.
You may also find it useful to know your NHS number. You do not need to know your NHS number to receive NHS care, but it can be helpful when contacting services or completing forms.
Where Should You Keep Your Information?
Many patients choose to:
- Save a copy on their mobile phone
- Keep a printed copy in their wallet or handbag
- Store it alongside their steroid emergency card
- Keep a copy with travel documents
- Share a copy with family members or carers
- Keep copies of important clinic letters on their phone or tablet
The best system is the one that is easy to access when needed.
Printable options (Word documents):
Looking Ahead
The proposed NHS single patient record could eventually make it easier for healthcare professionals to access important information quickly and safely.
For patients with rare conditions such as aspergillosis, that could improve continuity of care, reduce delays and reduce the need to repeatedly explain complex medical histories.
Until then, carrying a simple summary of your condition remains one of the easiest and most effective ways to help healthcare professionals understand your health needs and provide appropriate care.
Key Points
- Carry a simple one-page health summary.
- Include diagnoses, medications, allergies and specialist contacts.
- Clearly state if you have adrenal insufficiency or take long-term steroids.
- Mention azole antifungal treatment and potential drug interactions.
- National Aspergillosis Centre patients may be able to access clinic information through myMFT.
- Patients outside MFT should ask whether their own hospital has a patient portal.
- Keep important information on your phone and consider carrying a printed copy.
- A future NHS single patient record may improve information sharing, but patients remain an important source of information today.
Common Questions
Do I need to carry all my clinic letters?
No. A concise one-page summary is usually more useful in an emergency. However, keeping copies of important clinic letters on your phone can be helpful.
What if I am treated at more than one hospital?
This is one of the main reasons to carry a health summary. Different healthcare providers may not always have immediate access to the same information.
Is this only useful in emergencies?
No. It can also help during GP appointments, outpatient visits, travel, planned hospital admissions and when seeing healthcare professionals unfamiliar with aspergillosis.
What if I am a National Aspergillosis Centre patient?
Consider registering for myMFT and keeping important clinic letters available on your phone or tablet for easy access.
What if I am not an NAC patient?
Ask your own hospital or respiratory clinic whether they offer a patient portal. You can also check what information is available through the NHS App.
When to Seek Medical Advice
Seek urgent medical advice if you experience:
- Significant worsening of breathlessness
- Chest pain
- Coughing up significant amounts of blood
- Symptoms of adrenal crisis if you have adrenal insufficiency
- Severe allergic reactions to medications
- Rapid deterioration in your respiratory symptoms
If you need emergency help, call 999. For urgent medical advice in the UK, use NHS 111.
Useful Links
- myMFT patient portal – Manchester University NHS Foundation Trust
- NHS App
- Find your NHS number
- Aspergillosis information and support
Frequently Asked Questions
What information should an aspergillosis patient carry in an emergency?
Patients should consider carrying a summary of their diagnosis, medications, allergies, steroid or adrenal information, specialist contacts and emergency contact details.
Should people with aspergillosis carry a medication list?
Yes. Many aspergillosis patients take antifungal medicines, steroids, biologic therapies and inhalers. An up-to-date medication list can help avoid prescribing errors and drug interactions.
What is myMFT?
myMFT is the patient portal used by Manchester University NHS Foundation Trust. It allows eligible patients to access appointments, clinic letters, test results and other healthcare information.
Can aspergillosis patients access their records online?
Some patients can access records through services such as myMFT, local hospital portals or the NHS App, depending on where they receive care.
What is the NHS single patient record?
The proposed NHS single patient record aims to improve information sharing between healthcare providers so patients do not need to repeatedly explain their medical history.
Author: National Aspergillosis Centre Patient Support Team
Reviewed by: National Aspergillosis Centre
Last reviewed: June 2026
Important: This article is intended for information only and should not replace advice from your healthcare team.
Exercise and Aspergillosis: How Physical Activity Can Improve Breathing, Strength and Wellbeing
Key points
- Exercise is one of the most helpful non-drug tools for many people living with aspergillosis.
- Regular physical activity can improve breathlessness, strength, stamina, mood, confidence and quality of life.
- The best approach is usually little and often, rather than occasional intensive exercise.
- Do not compare yourself with others. Everyone has different lungs, treatments, fitness levels and limits.
- Respiratory physiotherapists and pulmonary rehabilitation programmes can help you exercise safely and confidently.
- Walking, cycling, swimming, rowing, gentle yoga, Tai Chi and singing can all be useful, depending on the individual.
- People with aspergillosis should take extra care around mould-heavy environments such as compost, leaf mould, sheds and building dust.
Contents
- Why exercise matters in aspergillosis
- The activity and breathlessness cycle
- Benefits of exercise
- Specific issues for aspergillosis patients
- How to start safely
- Activities that may help
- Pulmonary rehabilitation and physiotherapy
- The golden rule: little and often
- What clinicians want patients to know
- Real-life examples
- When to seek medical advice
- Frequently asked questions
- Related articles and further support
Why exercise matters in aspergillosis
Living with aspergillosis can be physically and emotionally challenging. Breathlessness, coughing, fatigue, disturbed sleep, medication side effects and reduced confidence can all make it tempting to become less active.
Unfortunately, becoming less active can make symptoms feel worse over time. Muscles weaken, fitness falls, balance may worsen and everyday activities such as walking, climbing stairs, shopping or playing with grandchildren can become harder.
This process is often called deconditioning. It does not mean the symptoms are imaginary. It means the body has lost some of its ability to cope with activity.
The encouraging news is that exercise can help reverse part of this process.
Exercise cannot cure aspergillosis, but it can help the body use oxygen more efficiently, strengthen muscles, improve confidence and make daily life easier.
Importantly, people may feel better and do more even when their lung function tests do not change very much.
The activity and breathlessness cycle
Many people with chronic lung disease become trapped in a difficult cycle:
The deconditioning cycle
Breathlessness → Less activity → Loss of fitness → More breathlessness → Even less activity
Exercise helps by creating a healthier cycle:
The rebuilding cycle
Gentle activity → Stronger muscles → More confidence → Easier daily tasks → Better quality of life
This is why small, regular activity can be so powerful. The aim is not to force the lungs to work harder. The aim is to help the whole body work better.
Benefits of exercise
Improved breathlessness
Exercise may make you breathless while you are doing it, but regular activity often reduces breathlessness during everyday tasks. This happens because muscles become stronger and more efficient, so they need less effort to perform the same activity.
More energy
Many patients report feeling less tired once they build a regular routine. Exercise uses energy in the short term, but over time it can improve stamina and reduce the effort needed for daily life.
Stronger muscles
Long-term illness, hospital admissions, inactivity and corticosteroid treatment can all contribute to muscle weakness. Strength exercises can help rebuild leg strength, improve balance and support independence.
Better mood and confidence
Living with aspergillosis can affect mental wellbeing. Exercise can help reduce anxiety, stress and low mood. It can also restore a sense of control and achievement.
Improved bone health
This is especially important for people who have taken long-term corticosteroids. Weight-bearing activity and strength training can help protect bone strength and reduce the risk of osteoporosis.
Better daily function
For many patients, the most important benefit is practical: being able to walk further, climb stairs more easily, go shopping, travel, garden, socialise or enjoy family life with more confidence.
Specific issues for aspergillosis patients
Avoiding high mould exposure
Aspergillus is commonly found in soil, compost, decaying vegetation, damp buildings and dust. Some activities can expose people to large numbers of fungal spores.
Activities that may increase exposure include:
- Handling compost
- Turning soil
- Clearing leaf piles
- Wood chipping
- Spreading bark or mulch
- Cleaning sheds, garages, lofts or basements
- Working around mouldy materials
- Construction or demolition environments
Outdoor exercise such as walking, cycling and running is generally encouraged. However, it is sensible to avoid places where mould, compost, dust or decaying vegetation are being heavily disturbed.
Some people may choose to wear a well-fitting FFP2 or FFP3 mask for unavoidable dusty or mould-heavy tasks, but avoidance is usually better where possible.
Haemoptysis: coughing blood
People with Chronic Pulmonary Aspergillosis (CPA), lung cavities or aspergillomas may sometimes cough blood. This is called haemoptysis.
If you have recent, recurrent or significant haemoptysis, discuss exercise with your respiratory team. Most routine activity remains safe for many people, but vigorous exertion may need to be paused or modified during periods of active bleeding.
Oxygen levels
Some people with aspergillosis also have bronchiectasis, Chronic Obstructive Pulmonary Disease (COPD), fibrosis, previous tuberculosis damage or other lung scarring. In these situations, oxygen levels may fall during exertion even when resting oxygen levels are normal.
If breathlessness feels out of proportion, or if you notice unusually low oxygen saturations during activity, discuss this with your respiratory team. You may benefit from an exercise assessment or pulmonary rehabilitation referral.
Fatigue and boom-and-bust activity
Aspergillosis-related fatigue can be different from normal tiredness. It may be influenced by chronic inflammation, active infection, poor sleep, anxiety, medication side effects and reduced fitness.
Many patients experience a boom-and-bust pattern:
Good day → Do too much → Several days recovering
Regular, steady activity is usually more helpful than occasional bursts of intensive effort.
Steroid-related muscle weakness
People who have taken long-term corticosteroids may develop muscle weakness, particularly around the thighs and hips. This can make standing from a chair, climbing stairs and walking uphill more difficult.
Strength exercises such as sit-to-stands, step-ups and resistance band work can be particularly helpful.
Adrenal insufficiency
Some patients who have used long-term corticosteroids develop adrenal insufficiency. These patients should understand their sick day rules and discuss unusually strenuous exercise, endurance events or major hikes with their healthcare team.
Most routine gentle or moderate exercise is safe, but unusually demanding activity may require additional planning.
Asthma, ABPA and exercise symptoms
Many people with Allergic Bronchopulmonary Aspergillosis (ABPA) also have asthma. Exercise can sometimes trigger wheeze, cough or chest tightness.
This does not usually mean exercise should be avoided. Good asthma control, appropriate inhaler use, gradual warm-up and pacing can make a major difference. Speak to your healthcare team if exercise regularly triggers asthma symptoms.
How to start safely
Start from where you are
Your starting point is your starting point. It does not matter what someone else can do. If you can only walk for two or three minutes, that is still a valid place to begin.
Use the talk test
During moderate exercise, you should usually be able to speak in short sentences. If you cannot speak at all, you may be pushing too hard.
Build gradually
Small increases are usually safer and more sustainable than sudden changes. For example, increasing a walk from five minutes to six or seven minutes may be more helpful than trying to double it immediately.
Plan rest periods
Rest is not failure. Many people with lung disease do better with short bursts of activity separated by planned rests.
Track progress gently
Some patients find it motivating to keep a simple record of walks, steps, strength exercises or how breathless they feel. The aim is encouragement, not pressure.
A simple beginner example
Example starter plan
- Week 1–2: Walk for 5 minutes most days, or less if needed.
- Week 3–4: Add one or two minutes when comfortable.
- Week 5–6: Add gentle strength exercises, such as sit-to-stands.
- Ongoing: Continue gradual increases, with rest days when needed.
This is only an example. Some people will need to start lower, while others may safely start higher.
Activities that may help
The best exercise is usually the one you enjoy and can keep doing regularly.
Walking
Walking is one of the simplest and most effective activities. It requires no special equipment, can be adapted to most fitness levels and is easy to build gradually.
Cycling
Cycling, including use of a stationary exercise bike, can improve stamina while placing less strain on the joints than running.
Swimming
Swimming can be helpful because the water supports body weight. However, some people with asthma find chlorinated pools trigger symptoms.
Rowing
Rowing machines can provide both cardiovascular and strength benefits. Start gently and focus on technique.
Strength training
Strength training does not have to mean heavy weights. Useful exercises may include:
- Sit-to-stands from a chair
- Step-ups
- Wall push-ups
- Resistance bands
- Light hand weights
Gentle yoga and Tai Chi
Many patients enjoy gentle yoga or Tai Chi because they combine movement, balance, breathing awareness, posture and relaxation. Chair-based versions may be useful for people with reduced mobility.
Singing
Singing may not sound like exercise, but many people with lung conditions find it helpful. It can support breathing control, posture, confidence, social connection and respiratory muscle coordination.
Some patients enjoy local choirs or Singing for Lung Health groups.
Pulmonary rehabilitation and physiotherapy
You do not have to do this alone.
A respiratory physiotherapist can help assess your current ability and design a programme that suits your symptoms, fitness level and goals.
A specialist physiotherapist may help with:
- Breathlessness management
- Pacing strategies
- Strength and stamina building
- Airway clearance techniques where appropriate
- Confidence around movement
- Safe return to activity after illness
Pulmonary rehabilitation
Pulmonary rehabilitation is a structured programme that usually combines supervised exercise, education, breathing techniques and self-management advice.
Many people with chronic lung disease describe pulmonary rehabilitation as one of the most helpful interventions they have received.
If you have ongoing breathlessness, reduced exercise tolerance or loss of confidence, ask your GP, respiratory consultant, specialist nurse or physiotherapist whether pulmonary rehabilitation may be suitable for you.
The golden rule: little and often
Exercise with aspergillosis: the golden rule
Little and often is usually better than a lot all at once.
Do not compare yourself with other people, including other aspergillosis patients.
Everyone has different lungs, different treatments, different ages and different levels of fitness.
Focus on your own starting point and your own progress.
Do not try to keep up with others. You do you.
One of the biggest traps is comparing yourself with other patients. Someone else may complete a long-distance walk, climb a mountain, run a race or cycle hundreds of miles. That can be inspiring, but it should not become your target.
Instead, ask yourself:
Am I a little stronger, fitter or more confident than I was a few months ago?
Success may mean:
- Walking for five minutes when previously you could only manage three
- Climbing stairs more comfortably
- Shopping with less breathlessness
- Doing light gardening safely
- Enjoying a holiday more easily
- Playing with children or grandchildren
- Needing fewer rests during ordinary daily tasks
These achievements matter.
For most people living with aspergillosis, consistency beats intensity.
What clinicians want patients to know
Exercise is not about pushing through at all costs
Healthcare professionals usually want patients to remain as active as safely possible, but that does not mean ignoring symptoms or forcing yourself to keep up with others.
The safest approach is usually to build gradually, pace yourself and ask for help when symptoms change.
Exercise should support your life, not punish your body.
Real-life examples
The person who walks five minutes a day
For someone recovering from illness or a hospital admission, a five-minute daily walk may be a major achievement. If that becomes six minutes, then eight minutes, that is progress.
The person who completes a long-distance walk
Some people with aspergillosis manage major challenges such as long-distance walking routes. These stories can be inspiring, but they are not a standard everyone else must meet.
The person who joins a singing group
For some patients, a singing group may be more enjoyable and sustainable than a gym. Singing can support breathing control and confidence while also providing social contact.
The person who returns to gardening carefully
Gardening can be enjoyable and active, but compost, leaf mould and disturbed soil may contain high levels of fungal spores. Some patients adapt by avoiding compost handling, asking for help with mould-heavy tasks, wearing protective masks where appropriate, and choosing lower-risk gardening activities.
When to seek medical advice
Stop exercising and seek medical advice if you experience:
- Chest pain
- Severe or unusual breathlessness
- Dizziness or fainting
- Significant haemoptysis, meaning coughing blood
- Sudden worsening of symptoms
- New palpitations or heart rhythm symptoms
- Oxygen levels much lower than usual, if you monitor them
- Exercise tolerance that suddenly falls without an obvious reason
Always speak to your healthcare team if you are unsure whether exercise is safe for you, especially if your symptoms have recently changed.
Frequently asked questions
Can I exercise if I have aspergillosis?
Yes, many people with aspergillosis benefit from regular physical activity. Exercise should be adapted to your symptoms, fitness level and medical conditions. Ask your healthcare team for advice if you have severe breathlessness, recent haemoptysis or unstable symptoms.
Can exercise improve breathlessness?
Yes. Exercise can improve muscle efficiency, stamina and confidence. This can reduce breathlessness during everyday activities, even if lung function test results do not change significantly.
What is the best exercise for Allergic Bronchopulmonary Aspergillosis?
There is no single best exercise for Allergic Bronchopulmonary Aspergillosis. Walking, cycling, swimming, gentle yoga, strength training and pulmonary rehabilitation can all be helpful. The best activity is one you can do safely and regularly.
Can pulmonary rehabilitation help aspergillosis patients?
Many people with chronic respiratory symptoms, bronchiectasis or reduced exercise tolerance benefit from pulmonary rehabilitation. It combines supervised exercise, education, breathing techniques and self-management support.
Should people with aspergillosis avoid gardening?
Not necessarily, but some gardening activities can expose people to high levels of Aspergillus spores. Handling compost, turning soil, clearing leaves and working with mulch may carry higher exposure. Lower-risk gardening activities may be more suitable for some patients.
Can exercise help steroid-related muscle weakness?
Yes. Strength exercises can help rebuild muscle strength lost through long-term corticosteroid treatment, illness or inactivity. Simple exercises such as sit-to-stands, step-ups and resistance bands can be useful.
Is singing useful for people with lung disease?
Many people with lung disease find singing helpful for breathing control, posture, confidence and social connection. Some areas offer Singing for Lung Health groups.
Should I exercise when I am tired?
Gentle movement may help on some tired days, but severe fatigue may mean your body needs rest. Pacing is important. Try to avoid repeated boom-and-bust cycles where you do too much on a good day and then need several days to recover.
Take-home message
Exercise is one of the most powerful tools available to help people living with aspergillosis maintain independence, strength and quality of life.
Move more, but move at your own pace.
Find something you enjoy.
Ask for help when you need it.
Little and often beats heroic efforts.
Do not compare yourself with others.
You do you.
Related articles
You may also find these aspergillosis.org articles helpful:
- Why Am I Breathless When My Oxygen Levels Are Normal?
- Physiotherapy for Aspergillosis
- Living with Aspergillosis
- Managing Fatigue in Aspergillosis
- Steroids and Adrenal Insufficiency
- Bronchiectasis and Aspergillosis
- What is Allergic Bronchopulmonary Aspergillosis (ABPA)?
- What is Chronic Pulmonary Asprgillosis (CPA)?
Further support and information
Author and review information
Author: Graham Atherton, National Aspergillosis Centre
Medical review: National Aspergillosis Centre Clinical Team
Last reviewed: June 2026
This article provides general information and should not replace advice from your own healthcare team.
Specialist Evidence Briefing: Aspergillus Serology for CPA Diagnosis: Why Assay Choice, Cut-Offs and Confirmatory Testing Matter
Key points
- CPA diagnosis remains challenging because symptoms and radiology overlap with tuberculosis, non-tuberculous mycobacterial disease, bronchiectasis, chronic obstructive pulmonary disease, malignancy and other chronic lung disorders.
- Aspergillus immunoglobulin G (IgG) testing is a cornerstone of CPA diagnosis, but performance varies between assays.
- Cut-off selection affects sensitivity and specificity, with important consequences for both missed CPA and overdiagnosis.
- Confirmatory or complementary testing, such as Western blot in selected situations, may help clarify difficult or borderline cases.
- The paper is directly relevant to specialist respiratory, infectious diseases and mycology services because diagnostic reliability affects referral pathways, antifungal prescribing and case definition.
The paper
Bigot J, Gibert C, Millet N, et al. Aspergillus serology for chronic pulmonary aspergillosis diagnosis: optimization of an enzyme-linked immunosorbent assay kit and assessment of a Western blot kit performance. Journal of Clinical Microbiology. Published 28 May 2026. doi:10.1128/jcm.00182-26.
Why this paper matters
CPA is a progressive and potentially fatal chronic lung infection that usually occurs in patients with underlying structural lung damage. Diagnosis depends on combining clinical symptoms, characteristic radiology and evidence of Aspergillus infection or immune response.
In practice, Aspergillus serology is often the decisive test. A positive Aspergillus IgG result can support the diagnosis when imaging and symptoms are compatible. A negative result can reduce diagnostic probability. But serology is not absolute. Different assays use different antigen preparations, platforms and reporting units. This means that results from one laboratory may not be directly comparable with results from another.
This paper is therefore important because it addresses a real-world diagnostic problem: how to optimise Aspergillus serological testing so that it performs reliably in the diagnosis of CPA.
Clinical background: why CPA serology is difficult
CPA often develops in patients with structurally abnormal lungs. Common underlying conditions include previous pulmonary tuberculosis, non-tuberculous mycobacterial infection, chronic obstructive pulmonary disease, bronchiectasis, sarcoidosis, prior lung surgery and other cavitary lung diseases.
These same conditions can also cause chronic symptoms and abnormal imaging without CPA. This creates a diagnostic grey zone. Patients may have cavities, pleural thickening, fibrosis, bronchiectasis, chronic cough, haemoptysis or weight loss for reasons other than Aspergillus disease.
Aspergillus IgG testing is therefore valuable because it provides evidence of an immune response to Aspergillus. However, it must be interpreted in context. A positive result does not, by itself, prove active CPA. A negative result does not always fully exclude CPA, particularly if clinical suspicion remains high.
What the study evaluates
The paper evaluates two related aspects of CPA serology:
- Optimisation of an enzyme-linked immunosorbent assay (ELISA) kit for Aspergillus serology in CPA diagnosis.
- Assessment of Western blot kit performance, potentially as a complementary or confirmatory approach.
This is clinically relevant because ELISA-based Aspergillus IgG testing is widely used in diagnostic pathways, while Western blot may offer additional qualitative information in selected cases. The practical question is whether assay optimisation and confirmatory testing improve diagnostic performance enough to change specialist practice.
Why assay cut-offs matter
The choice of diagnostic cut-off is not a technical detail; it changes clinical classification.
| Cut-off strategy | Likely effect | Clinical risk |
|---|---|---|
| Lower cut-off | Higher sensitivity | More false positives and possible overdiagnosis |
| Higher cut-off | Higher specificity | More false negatives and missed CPA |
| Population-specific cut-off | Potentially better clinical performance | May reduce comparability between centres |
| Single universal cut-off | Simpler implementation | May perform poorly across different populations |
In a specialist CPA service, false negatives may delay antifungal treatment and referral. False positives may lead to unnecessary anxiety, additional imaging, prolonged antifungal therapy and avoidable toxicity. The correct balance depends on the clinical setting, disease prevalence and consequences of diagnostic error.
Where Western blot may fit
Western blot testing may be useful where ELISA results are borderline, discordant with imaging, or difficult to interpret in patients with complex lung disease. It may also be useful as a complementary method in diagnostic algorithms, depending on availability and validated performance.
However, Western blot should not be seen as a simple replacement for ELISA. Its value depends on whether it adds diagnostic clarity beyond standard serology, whether it is reproducible between laboratories, and whether clinicians know how to act on the result.
Clinical interpretation: serology is supportive, not standalone
For specialists, the key principle remains:
Aspergillus serology supports the diagnosis of CPA but does not diagnose CPA in isolation.
A robust CPA diagnosis requires integration of:
- compatible symptoms, usually chronic cough, weight loss, fatigue, breathlessness or haemoptysis;
- compatible imaging, particularly cavities, pleural thickening, pericavitary infiltrates, fungal ball, nodules or progressive fibrosis;
- mycological or immunological evidence, especially Aspergillus IgG;
- exclusion or recognition of alternative and co-existing diagnoses, including active tuberculosis, non-tuberculous mycobacterial disease, malignancy and bacterial bronchiectasis.
Implications for specialist services
This paper supports the need for carefully governed CPA serology pathways. Specialist centres and diagnostic laboratories should consider:
- which Aspergillus IgG assay is used locally;
- what cut-off is applied and how it was validated;
- whether borderline zones should be reported rather than simple positive/negative categories;
- how results are interpreted in high-risk structural lung disease populations;
- whether confirmatory testing is available for selected cases;
- how serology is integrated with CT findings and microbiology;
- whether local reports include interpretive comments to reduce misuse.
Suggested diagnostic reporting approach
Rather than reporting Aspergillus serology as a binary answer, laboratories and specialist services may benefit from a more interpretive model:
| Result category | Possible interpretation | Suggested action |
|---|---|---|
| Clearly negative | CPA less likely, but not impossible if clinical suspicion is high | Review imaging and alternative diagnoses; repeat if disease evolves |
| Borderline or low positive | Uncertain significance | Correlate with CT, symptoms, cultures and prior results; consider repeat or confirmatory testing |
| Clearly positive | Supports CPA in the right clinical/radiological context | Assess full CPA criteria and consider specialist referral or treatment discussion |
| Discordant result | Serology conflicts with clinical picture | Reassess diagnosis, assay limitations and possibility of co-existing disease |
Relevance to post-tuberculosis lung disease
This paper is particularly relevant when considered alongside recent evidence that CPA may be detected during or soon after pulmonary tuberculosis treatment. In post-tuberculosis lung disease, cavities and chronic radiological abnormalities are common, but not all symptoms are due to active TB or permanent scarring.
Reliable Aspergillus serology is therefore essential. If the assay cut-off is poorly calibrated, clinicians may either miss CPA in symptomatic patients with cavities or overdiagnose CPA in patients with structural lung damage but no active Aspergillus disease.
Relevance to bronchiectasis and non-tuberculous mycobacterial disease
Patients with bronchiectasis or non-tuberculous mycobacterial lung disease may also have chronic symptoms, mucus production, recurrent infection, radiological change and occasional Aspergillus isolation. Aspergillus serology can be useful in identifying CPA, but positive results must be interpreted carefully because these patients often have complex chronic airway disease.
For this group, assay performance and cut-off choice may substantially affect diagnostic confidence.
Implications for antifungal stewardship
Improved CPA serology has direct stewardship implications. Antifungal treatment for CPA is often prolonged and requires monitoring for toxicity, drug interactions and therapeutic drug levels. Overdiagnosis can expose patients to unnecessary azoles. Underdiagnosis can allow progressive cavitary disease, haemoptysis and loss of lung function.
More reliable serological testing can therefore support both earlier treatment in true CPA and avoidance of unnecessary therapy in patients who do not meet diagnostic criteria.
Evidence strength
| Question | Evidence strength | Comment |
|---|---|---|
| Is Aspergillus IgG central to CPA diagnosis? | Strong | Recognised in major CPA diagnostic guidance |
| Do different assays and cut-offs affect performance? | Strong | Well-recognised practical issue in CPA serology |
| Can assay optimisation improve diagnostic classification? | Likely | This paper directly addresses optimisation, but local validation remains important |
| Should Western blot replace ELISA? | Not established | More likely to be complementary or confirmatory in selected cases |
| Should serology alone determine CPA treatment? | No | Must be interpreted with symptoms, imaging and microbiology |
Practical take-home messages for specialists
- Know which Aspergillus IgG assay your laboratory uses.
- Know the cut-off and whether it has been validated for CPA.
- Be cautious with borderline results.
- Do not diagnose CPA on serology alone.
- Do not dismiss CPA solely because one serological test is negative if the clinical and CT picture is highly suggestive.
- Consider repeat or complementary testing when results are discordant.
- Integrate serology with CT, symptoms, sputum fungal culture/PCR and assessment for tuberculosis or non-tuberculous mycobacteria.
Conclusion
This paper is a timely reminder that CPA diagnosis depends not only on whether Aspergillus serology is performed, but on how well the assay is optimised, how cut-offs are selected and how results are interpreted. For specialist services, improved serology can strengthen diagnostic confidence, support earlier recognition of CPA and reduce unnecessary antifungal treatment.
The broader implication is clear: CPA diagnostic pathways need standardised, validated and clinically interpreted Aspergillus serology, not isolated positive or negative blood test results.
References
- Bigot J, Gibert C, Millet N, et al. Aspergillus serology for chronic pulmonary aspergillosis diagnosis: optimization of an enzyme-linked immunosorbent assay kit and assessment of a Western blot kit performance.
Journal of Clinical Microbiology. Published 28 May 2026.
doi:10.1128/jcm.00182-26.
PubMed - Denning DW, Cadranel J, Beigelman-Aubry C, et al. Chronic pulmonary aspergillosis: rationale and clinical guidelines for diagnosis and management.
European Respiratory Journal. 2016;47(1):45-68.
doi:10.1183/13993003.00583-2015.
PubMed - Patterson TF, Thompson GR, Denning DW, et al. Practice guidelines for the diagnosis and management of aspergillosis: 2016 update by the Infectious Diseases Society of America.
Clinical Infectious Diseases. 2016;63(4):e1-e60.
doi:10.1093/cid/ciw326.
PubMed
Commercial Aspergillus fumigatus real-time PCR for invasive pulmonary aspergillosis: specialist evidence briefing
Why this paper matters
Invasive pulmonary aspergillosis remains difficult to diagnose early, particularly in patients with haematological malignancy, haematopoietic stem cell transplantation, intensive chemotherapy, corticosteroid exposure or profound immunosuppression. Culture is insensitive, histology is often unavailable, and radiology is not specific. Galactomannan has become a central biomarker, but performance varies by specimen type, antifungal exposure, host group and disease stage.
Aspergillus PCR has long been promising, but implementation has been limited by assay heterogeneity, extraction differences, target selection, contamination concerns, and variable interpretation across centres. A clinically evaluated commercial real-time PCR assay is therefore important because commercialisation may improve standardisation, reproducibility and adoption outside specialist mycology laboratories.
Clinical context
The diagnosis of IPA is usually probabilistic. Clinicians combine:
- host factors, such as neutropenia, haematological malignancy, transplantation or corticosteroid exposure;
- compatible imaging, especially nodules, halo sign, cavitation or infarct-like lesions on computed tomography;
- mycological evidence, including galactomannan, culture, microscopy, PCR or lateral-flow assays;
- clinical course and response to antifungal therapy.
In this setting, a commercial Aspergillus fumigatus real-time PCR assay could support earlier diagnosis, improve confidence in probable IPA classification, and potentially reduce unnecessary empirical antifungal treatment when used as part of a diagnostic algorithm.
Main finding
The paper evaluates a commercial Aspergillus fumigatus real-time PCR assay for the diagnosis of invasive pulmonary aspergillosis in patients with haematological malignancies. The clinical relevance lies in validating a defined assay in a high-risk population where early diagnosis directly affects antifungal timing and survival.
The specialist significance is not simply that PCR “works”. The key question is whether a commercial PCR assay offers sufficiently reliable analytical and clinical performance to be used alongside galactomannan and imaging in routine pathways.
What is genuinely new?
The novelty is likely to sit in one or more of the following areas:
- evaluation of a specific commercial assay rather than an in-house laboratory-developed test;
- clinical validation in a defined haematology population;
- comparison against established diagnostic categories such as proven/probable IPA;
- assessment of analytical performance, including limit of detection, reproducibility or specificity;
- potential contribution to standardisation of Aspergillus PCR implementation.
This is not a new concept in principle: Aspergillus PCR has been studied for many years. What is more clinically useful is the transition from heterogeneous in-house assays towards assays that can be validated, quality-assured and compared across centres.
Relationship to existing evidence
Recent reviews of molecular fungal diagnostics emphasise that PCR can improve the diagnosis of invasive fungal disease but remains limited by standardisation, assay availability and interpretation. A 2025 review in Diagnostics noted that PCR is sensitive and specific for invasive fungal disease, but that implementation remains constrained by limited standardisation, few commercial options, and lack of clear guidance for interpreting results.
That surrounding evidence makes this type of paper important. Commercial PCR assays do not automatically solve diagnostic uncertainty, but they can reduce one major barrier: between-laboratory variability.
Strengths to look for in the paper
- Clearly defined patient population, especially haematological malignancy or transplant subgroups.
- Use of accepted case definitions for proven, probable and possible IPA.
- Separate analytical and clinical performance assessment.
- Comparison with galactomannan, culture and radiology.
- Evaluation by specimen type, especially bronchoalveolar lavage fluid versus blood.
- Consideration of antifungal exposure before sampling.
- Reporting of sensitivity, specificity, positive predictive value and negative predictive value.
Limitations and cautions
PCR performance depends strongly on specimen type. Bronchoalveolar lavage fluid generally provides a higher organism burden than blood in IPA, but it is more invasive and may not be feasible in unstable or thrombocytopenic patients. Blood PCR is less invasive but may be less sensitive, especially in localised airway-invasive disease.
False positives may arise from colonisation, contamination or detection of non-invasive airway presence. False negatives may occur with low fungal burden, prior antifungal therapy, sampling timing, extraction inefficiency or inhibitors. A positive PCR result should therefore not be interpreted in isolation.
A further issue is species coverage. A narrowly targeted Aspergillus fumigatus assay may perform well for A. fumigatus but could miss non-fumigatus Aspergillus species or cryptic species with different susceptibility patterns. In haematology patients, that may matter for epidemiology and antifungal resistance surveillance.
Clinical implications
For specialist services, the likely implication is that commercial Aspergillus PCR should be considered as part of a multi-modal diagnostic pathway rather than as a standalone rule-in or rule-out test.
A practical diagnostic model might include:
- early CT imaging in high-risk patients with persistent fever or respiratory symptoms;
- serum galactomannan in appropriate host groups;
- bronchoalveolar lavage where clinically safe;
- BAL galactomannan, fungal culture, microscopy and Aspergillus PCR;
- azole resistance testing or sequencing where Aspergillus is detected;
- multidisciplinary interpretation with haematology, infectious diseases, respiratory and mycology input.
Implications for antifungal stewardship
A validated commercial PCR assay may support earlier targeted antifungal therapy, but also more confident de-escalation when combined with negative biomarkers and low radiological probability. The stewardship value depends on pathway design. PCR added without interpretive governance may increase diagnostic noise; PCR embedded into a structured algorithm may reduce unnecessary empirical therapy and improve diagnostic confidence.
Implications for UK specialist mycology services
For UK centres, this type of paper supports the case for:
- standardised fungal PCR pathways;
- clear reporting language for positive and negative results;
- integration with antifungal stewardship rounds;
- external quality assessment participation;
- reflex testing for resistance where feasible;
- collaboration between local laboratories and specialist mycology reference services.
Evidence strength
| Question | Evidence strength | Comment |
|---|---|---|
| Can Aspergillus PCR detect fungal DNA in clinical specimens? | Strong | Longstanding molecular evidence |
| Can PCR support IPA diagnosis? | Moderate to strong | Best when combined with host, imaging and biomarker data |
| Are commercial assays ready for routine use? | Emerging | Depends on assay validation, specimen type and pathway integration |
| Can PCR alone rule in or rule out IPA? | No | Should not be used in isolation |
Conclusion
Commercial Aspergillus real-time PCR assays represent an important step towards standardised molecular diagnosis of invasive pulmonary aspergillosis. Their greatest value is likely to be in high-risk haematology pathways, especially when applied to bronchoalveolar lavage fluid and interpreted alongside galactomannan, culture, imaging and host risk.
The clinical message is not that PCR replaces existing tests. Rather, validated commercial PCR may strengthen diagnostic algorithms, improve early case recognition, support antifungal stewardship and reduce variation between laboratories.
References
- Gibert C, Bigot J, et al. Clinical and analytical evaluation of a commercial Aspergillus fumigatus real-time PCR assay for the diagnosis of invasive pulmonary aspergillosis in patients with hematological malignancies.
Journal details to confirm from PubMed record.
PubMed - Brown L, Cruciani M, Morton O, et al. The molecular diagnosis of invasive fungal diseases with a focus on PCR.
Diagnostics. 2025;15(15):1909.
doi:10.3390/diagnostics15151909.
PubMed - Patterson TF, Thompson GR, Denning DW, et al. Practice guidelines for the diagnosis and management of aspergillosis: 2016 update by the Infectious Diseases Society of America.
Clinical Infectious Diseases. 2016;63(4):e1-e60.
doi:10.1093/cid/ciw326.
PubMed
Research significance summary for specialists: Chronic pulmonary aspergillosis during tuberculosis treatment: emerging evidence, diagnostic pitfalls and implications for TB pathways
Why this matters
CPA remains substantially under-recognised in people with current or previous pulmonary tuberculosis. The clinical overlap is considerable: cough, haemoptysis, weight loss, fatigue, cavitation and progressive radiological change can be attributed to TB relapse, treatment failure, non-tuberculous mycobacterial infection, bacterial bronchiectasis, malignancy or post-TB lung disease.
For TB programmes and respiratory services, the practical question is no longer simply whether CPA occurs after TB. The question is whether there should be defined triggers for CPA assessment during TB treatment, particularly when symptoms persist despite microbiologically effective therapy.
The traditional model: CPA after tuberculosis
The conventional model is well established:
- Pulmonary tuberculosis causes cavitation, fibrosis, bronchiectasis and pleural distortion.
- Residual cavities may persist after microbiological cure.
- Aspergillus conidia can colonise these abnormal airspaces.
- In some patients, colonisation progresses to simple aspergilloma, chronic cavitary pulmonary aspergillosis or chronic fibrosing pulmonary aspergillosis.
This model is supported by older post-TB aspergilloma studies and by modern CPA burden estimates. Bongomin’s review of post-tuberculosis CPA highlights residual pulmonary cavities as a major risk substrate and summarises classic British data in which Aspergillus precipitins and aspergillomas increased over time after treated pulmonary TB.
The newer question: can CPA be present or emerge during TB treatment?
Several recent prospective studies suggest that CPA may be detected during the active TB treatment pathway, not only years after treatment completion.
1. Jha et al. 2024: serial CPA assessment during treatment of newly diagnosed PTB
Jha and colleagues conducted a prospective study of newly detected pulmonary tuberculosis cases and assessed CPA at baseline and at the end of anti-tubercular therapy. Of 255 initially recruited patients, 158 completed follow-up. The authors reported CPA at baseline and at end-of-treatment, with 23 of 158 assessed patients diagnosed with CPA at completion of TB therapy.
The study is important because it examined serial Aspergillus IgG changes and CPA incidence during the course of anti-tubercular therapy. The authors reported proven CPA in approximately 7% at baseline and 14.6% at end-of-treatment, broadly comparable with earlier Indonesian longitudinal data.
However, interpretation requires caution. Not all patients underwent HRCT at end-of-treatment, follow-up attrition was substantial, and the distinction between incident CPA, pre-existing CPA, transient Aspergillus immune response and radiological overlap with active TB remains difficult.
2. APICAL Indonesia study: CPA in patients treated for pulmonary TB
The APICAL study by Setianingrum and colleagues was a prospective longitudinal study in Indonesia. It investigated CPA in patients treated for pulmonary tuberculosis and reported CPA at baseline and at the end of TB therapy. Jha et al. cite APICAL as reporting 7.9% CPA at baseline and 13.3% at the end of TB therapy when proven and probable CPA were combined.
This study is one of the key pieces of evidence that the TB–CPA relationship is not purely post-treatment. CPA may be present within the treatment period, particularly where patients have cavitary disease or persistent symptoms.
3. Uganda study: persistent symptoms after two months of TB therapy
Namusobya and colleagues studied patients with microbiologically confirmed drug-sensitive PTB who had persistent respiratory symptoms after two months of standard anti-TB therapy. CPA was defined using persistent symptoms, suggestive radiology and evidence of Aspergillus infection, including Aspergillus IgG/IgM immunochromatographic testing and/or culture.
The study found CPA in around 20% of participants with persistent symptoms after the intensive phase of TB treatment. This is particularly relevant to clinical practice because two months is a natural review point in TB treatment pathways. Persistent symptoms at that stage are often interpreted as delayed recovery, adherence problems, drug resistance or alternative bacterial infection. CPA should be added to that differential in selected patients.
4. Ghana prospective follow-up: mainly post-treatment, but relevant to timing
Ocansey and colleagues followed patients after pulmonary TB treatment and found CPA emerging by the end of treatment and increasing further six months later. The study reported an overall 12-month CPA incidence of 10.7% among resurveyed patients, with 3% at end-of-treatment and 7.4% six months post-treatment.
This supports a continuum model: CPA risk may begin during active disease or treatment and continue after TB completion, especially in those with residual cavities.
Possible biological and diagnostic explanations
Detection of CPA during TB therapy may reflect more than one phenomenon. These categories are clinically important because they have different implications.
| Scenario | Interpretation | Clinical implication |
|---|---|---|
| Pre-existing CPA misdiagnosed as TB | CPA may mimic smear-negative or clinically diagnosed TB | Review microbiological confirmation and imaging; avoid repeated empiric TB treatment where evidence is weak |
| True PTB–CPA co-disease at diagnosis | Both Mycobacterium tuberculosis and Aspergillus-related disease are present | Requires parallel diagnostic reasoning and careful drug interaction management |
| Incident CPA during treatment | Aspergillus disease develops in newly formed or persistent cavities | Consider CPA if symptoms persist or imaging progresses despite adequate TB treatment |
| Colonisation or transient serological positivity | Aspergillus detected without established progressive CPA | Repeat assessment and avoid over-treatment unless full CPA criteria are met |
| Post-TB lung disease with later CPA | Classic pathway: CPA develops months to years after TB treatment | Long-term awareness in patients with residual cavities, haemoptysis or chronic symptoms |
Diagnostic criteria: why timing is difficult
Most CPA definitions require compatible symptoms, radiology and mycological or immunological evidence over at least three months. That creates difficulty during TB therapy because active PTB itself can produce prolonged symptoms and cavitary radiology.
Guideline-consistent CPA diagnosis generally requires:
- chronic respiratory or systemic symptoms, usually for at least three months;
- compatible imaging, such as one or more cavities, pleural thickening, pericavitary infiltrates, fungal ball, progressive fibrosis or nodules;
- microbiological or immunological evidence of Aspergillus infection, especially raised Aspergillus IgG;
- exclusion of alternative diagnoses, including active TB, non-tuberculous mycobacterial disease, malignancy and other chronic infections.
In active TB, the exclusion criterion is problematic because TB and CPA can genuinely co-exist. Therefore, rather than using “active TB” to exclude CPA automatically, clinicians may need to ask whether the observed course is fully explained by TB alone.
When should CPA be considered during TB treatment?
CPA assessment should be considered during TB treatment when one or more of the following are present:
- persistent cough, haemoptysis, weight loss, fatigue or breathlessness after the intensive phase of TB treatment;
- persistent or enlarging cavities despite microbiological response to anti-TB therapy;
- new intracavitary material or suspected fungal ball;
- pleural thickening or pericavitary infiltrates that progress despite TB treatment;
- repeatedly negative TB microbiology despite a clinical label of TB relapse;
- history of previous TB or other structural lung disease;
- unexplained haemoptysis after apparent TB response;
- patients being considered for repeat TB treatment without strong microbiological confirmation.
Suggested diagnostic approach
A pragmatic diagnostic approach in specialist respiratory or infectious disease settings could include:
- Confirm TB status: review baseline microbiology, GeneXpert/NAAT, culture, drug susceptibility and treatment response.
- Repeat imaging: CT is preferable to chest radiography where CPA is suspected, particularly to assess cavities, fungal ball, pleural thickening and pericavitary progression.
- Request Aspergillus IgG: a positive result is a major diagnostic component, though not sufficient alone.
- Send respiratory samples: fungal culture and/or Aspergillus PCR where available; also reassess for TB and non-tuberculous mycobacteria.
- Assess duration and trajectory: progressive symptoms or radiology over three months strengthens CPA diagnosis.
- Review differential diagnoses: malignancy, bacterial bronchiectasis, NTM, lung abscess, vasculitis and other chronic infections.
- Discuss complex cases with a specialist mycology or CPA centre: especially if antifungal therapy is being considered during rifampicin-based TB treatment.
Treatment implications and drug interactions
If CPA is diagnosed during TB therapy, management is complicated by major drug interactions. Rifampicin is a potent enzyme inducer and substantially reduces exposure to many triazole antifungals, including itraconazole, voriconazole and posaconazole. Co-administration is generally problematic and may render azole therapy ineffective.
Specialist input is therefore essential. Management may require:
- review of TB regimen and treatment phase;
- therapeutic drug monitoring for azoles where used;
- careful liver function monitoring;
- assessment of haemoptysis risk;
- consideration of timing of antifungal initiation;
- multidisciplinary discussion involving TB, respiratory, infectious diseases, pharmacy and mycology teams.
In some cases, observation and reassessment may be appropriate if CPA criteria are incomplete and the patient is clinically improving. In others, particularly with progressive cavitary disease, haemoptysis or strong Aspergillus IgG positivity, earlier specialist intervention may be justified.
What do guidelines currently say?
ERS/ESCMID
The ERS/ESCMID CPA guideline recognises tuberculosis as a major underlying condition for CPA and defines CPA using chronic symptoms, compatible radiology and Aspergillus evidence, typically over at least three months. It supports Aspergillus IgG as a central diagnostic test and recommends long-term oral triazole therapy for symptomatic or progressive chronic cavitary disease.
IDSA
The IDSA aspergillosis guideline similarly defines chronic cavitary pulmonary aspergillosis by at least three months of symptoms or progressive radiographic abnormalities, compatible cavitary disease, microbiological or serological evidence of Aspergillus, and minimal immunocompromise. It explicitly notes that CPA may complicate underlying pulmonary diseases, including tuberculosis and non-tuberculous mycobacterial infection.
BTS
The British Thoracic Society 2025 Clinical Statement on Aspergillus-related chronic lung disease provides current UK best-practice framing for diagnosis and management of chronic Aspergillus lung disease. Its publication reflects increasing recognition that Aspergillus-related chronic lung disease requires specific diagnostic pathways, antifungal stewardship and specialist respiratory-mycology collaboration.
WHO TB guidance
WHO TB guidance focuses on TB diagnosis, drug susceptibility, treatment regimens, monitoring, treatment failure and public health control. CPA is not yet embedded as a routine screening component of standard TB treatment pathways. This creates a gap between TB programme algorithms and emerging evidence from fungal disease studies.
Evidence strength
| Question | Evidence strength | Comment |
|---|---|---|
| Does TB predispose to CPA? | Strong | Consistent epidemiological, radiological and mechanistic evidence |
| Does CPA occur after TB treatment? | Strong | Well-established, especially with residual cavities |
| Can CPA be detected during TB treatment? | Moderate | Supported by prospective studies from Indonesia, Uganda and India |
| Does CPA truly begin during treatment rather than being pre-existing? | Uncertain | Requires better baseline CT, serial mycology and longer follow-up |
| Should all TB patients be screened for CPA? | Insufficient evidence | Targeted testing in high-risk or persistently symptomatic patients is more defensible |
| Does early CPA detection during TB treatment improve outcomes? | Unproven | Needs prospective interventional studies |
Implications for TB and respiratory services
The emerging evidence supports a targeted CPA assessment trigger within TB pathways, rather than universal screening at present.
A reasonable specialist position would be:
In patients receiving treatment for pulmonary tuberculosis, persistent symptoms, haemoptysis or non-resolving/progressive cavitary disease after the intensive phase should prompt consideration of CPA, especially where TB microbiology is negative or improving and imaging remains suspicious.
This is particularly relevant in high TB burden countries, but also in low TB burden settings where patients with previous TB, migrant health histories or unexplained cavitary disease may be seen in respiratory clinics.
Research priorities
- Prospective studies with baseline and serial CT imaging in microbiologically confirmed PTB.
- Serial Aspergillus IgG titres, fungal culture and molecular testing during TB therapy.
- Clear separation of proven CPA, probable CPA, Aspergillus colonisation and transient seropositivity.
- Studies of CPA screening at two months versus end-of-treatment versus six months post-treatment.
- Outcome studies assessing whether early CPA recognition reduces haemoptysis, lung destruction, retreatment for TB or mortality.
- Health-economic modelling of targeted CPA testing in TB programmes.
Conclusion
The evidence base is moving from a simple post-TB model towards a continuum model of TB-associated CPA. In this model, Aspergillus-related disease may be present at TB diagnosis, emerge during therapy, become apparent at treatment completion, or develop later in post-TB lung disease.
For specialists, the key implication is not that every patient with TB requires CPA screening. Rather, CPA should be actively considered when the clinical trajectory is not adequately explained by TB alone, particularly in patients with cavitation, haemoptysis, persistent symptoms or poor radiological resolution.
Embedding a CPA assessment trigger into TB follow-up pathways may reduce misdiagnosis, repeated empirical TB treatment and delayed antifungal management. The evidence is not yet definitive, but it is strong enough to justify specialist awareness, targeted testing and further prospective research.
References
-
Bongomin F. Post-tuberculosis chronic pulmonary aspergillosis: An emerging public health concern.
PLOS Pathogens. 2020;16(8):e1008742.
doi:10.1371/journal.ppat.1008742.
PubMed -
Denning DW, Cadranel J, Beigelman-Aubry C, et al. Chronic pulmonary aspergillosis: rationale and clinical guidelines for diagnosis and management.
European Respiratory Journal. 2016;47(1):45-68.
doi:10.1183/13993003.00583-2015.
PubMed -
Jha D, Kumar U, Meena VP, et al. Chronic pulmonary aspergillosis incidence in newly detected pulmonary tuberculosis cases during follow-up.
Mycoses. 2024;67(5).
doi:10.1111/myc.13747.
PubMed -
Namusobya M, Bongomin F, Mukisa J, et al. Chronic pulmonary aspergillosis in patients with active pulmonary tuberculosis with persisting symptoms in Uganda.
Mycoses. 2022;65(6):625-634.
doi:10.1111/myc.13444.
PubMed -
Ocansey B, Otoo B, Gbadamosi H, et al. Importance of Aspergillus-specific antibody screening for diagnosis of chronic pulmonary aspergillosis after tuberculosis treatment: a prospective follow-up study in Ghana.
Journal of Fungi. 2022;9(1):26.
doi:10.3390/jof9010026.
PubMed -
Patterson TF, Thompson GR, Denning DW, et al. Practice guidelines for the diagnosis and management of aspergillosis: 2016 update by the Infectious Diseases Society of America.
Clinical Infectious Diseases. 2016;63(4):e1-e60.
doi:10.1093/cid/ciw326.
PubMed -
Setianingrum F, Rozaliyani A, Adawiyah R, et al. A prospective longitudinal study of chronic pulmonary aspergillosis in pulmonary tuberculosis in Indonesia (APICAL).
Thorax. 2022;77(8):821-828.
doi:10.1136/thoraxjnl-2020-216464.
PubMed
Aspergillosis Research Update: Earlier Diagnosis, Better Testing and New Treatment Possibilities

Research update covering mid-May to early June 2026
Key points
- New research suggests Aspergillus infection may develop during tuberculosis treatment, rather than only years afterwards.
- A large cystic fibrosis registry study has improved understanding of who is most at risk of developing Allergic Bronchopulmonary Aspergillosis (ABPA).
- A case report highlights that ABPA can occasionally cause severe mucus plugging and even lung collapse.
- New studies continue to improve testing for Chronic Pulmonary Aspergillosis (CPA), including Aspergillus antibody tests.
- Several papers evaluated newer diagnostic tools including PCR, galactomannan, lateral flow testing and metagenomic sequencing.
- Researchers are increasingly exploring treatments that support the immune system, rather than only targeting the fungus directly.
Introduction
The last two weeks have seen a wide range of new aspergillosis research covering diagnosis, risk factors, immune responses and future treatment possibilities.
A clear theme emerging from recent studies is the move towards earlier diagnosis and more personalised approaches to care. Researchers are also increasingly investigating how the immune system interacts with Aspergillus and whether improving immune function could become part of future treatment strategies.
Can Aspergillus infection begin during tuberculosis treatment?
One of the most interesting studies came from Peru, where researchers investigated Aspergillus infection among patients receiving treatment for pulmonary tuberculosis.
Traditionally, doctors have believed that Chronic Pulmonary Aspergillosis often develops months or years after tuberculosis causes lung damage. However, this study raises the possibility that Aspergillus infection may sometimes emerge during active tuberculosis treatment itself.
This finding is important because CPA is a recognised complication of tuberculosis worldwide. If future studies confirm these findings, clinicians may need to monitor some tuberculosis patients more closely for signs of fungal infection much earlier than previously thought.
Large registry study improves understanding of ABPA risk
Researchers in Turkey analysed data from a national cystic fibrosis registry to examine how often Allergic Bronchopulmonary Aspergillosis develops and which patients are most likely to be affected.
Large registry studies are valuable because they include information from many patients over extended periods of time. This allows researchers to identify patterns that smaller studies may miss.
The study helps improve understanding of how frequently ABPA develops, which patients appear to be at greatest risk, and which factors may be associated with disease development.
ABPA can sometimes cause severe airway blockage
A striking case report described a patient whose ABPA presented with complete collapse of one lung and respiratory failure.
Although uncommon, this case highlights an important aspect of ABPA that many patients already recognise from personal experience: mucus plugging can sometimes become severe.
In ABPA, inflammation causes excessive mucus production within the airways. In some cases, thick mucus plugs can partially or completely block sections of the lung.
Improved blood tests for Chronic Pulmonary Aspergillosis
Researchers have reported new work aimed at improving Aspergillus antibody testing for Chronic Pulmonary Aspergillosis.
Diagnosis of CPA often depends on a combination of symptoms, CT scan findings, evidence of Aspergillus infection and Aspergillus antibody testing. Current blood tests are useful but not perfect. Improving their accuracy could help reduce missed diagnoses and improve confidence when diagnosing CPA.
New diagnostic technologies continue to advance
PCR testing
A clinical evaluation of a commercial Aspergillus fumigatus PCR test in patients with haematological malignancies examined how accurately the test identifies invasive pulmonary aspergillosis.
Metagenomic sequencing
Researchers also published a systematic review and meta-analysis examining metagenomic next-generation sequencing for invasive pulmonary aspergillosis.
This technology analyses genetic material from all organisms present in a sample rather than looking for a single pathogen. Although currently expensive and not widely available, it may play an increasing role in future fungal diagnostics.
Lateral flow testing
Another study evaluated a lateral flow device designed to detect Aspergillus antigens. These tests could eventually help make fungal diagnostics faster and more accessible.
New insights into galactomannan testing
Researchers investigated whether comparing galactomannan levels in bronchial washing samples and blood samples could improve diagnosis of pulmonary aspergillosis.
Galactomannan is one of the most widely used fungal biomarkers. Refining how it is interpreted may improve diagnostic accuracy and help clinicians distinguish between infection and other conditions.
Could future treatment involve strengthening the immune system?
Some of the most exciting research focused on immune-based therapies. Rather than directly targeting Aspergillus, researchers are exploring ways to improve the body's ability to fight infection.
Anti-PD-1 and interferon-gamma
A study examined emerging evidence for anti-PD-1 therapy and interferon-gamma as adjunctive immunotherapy in invasive mould infections.
These approaches aim to reverse immune exhaustion and improve natural antifungal responses. They remain experimental, but they represent an important future direction.
Enhancing neutrophil function
Another study examined how G-CSF may improve neutrophil activity during Aspergillus fumigatus infection.
Neutrophils are among the body's most important immune cells for controlling Aspergillus. Improving their function could potentially help patients whose immune systems struggle to clear fungal infections.
Therapeutic drug monitoring remains important
A case report highlighted how voriconazole blood levels changed significantly as inflammation improved during treatment.
This reinforces an important principle already recognised by specialist centres: antifungal drug levels can change over time, and therapeutic drug monitoring remains an important part of safe and effective treatment.
What does this mean for patients?
Several themes stand out from this fortnight's research.
First, researchers continue to focus heavily on earlier diagnosis. Better blood tests, improved PCR methods, lateral flow devices and sequencing technologies all aim to identify aspergillosis more accurately and more quickly.
Second, there is growing interest in understanding which patients are most at risk of developing aspergillosis. This may eventually lead to more personalised monitoring and earlier intervention.
Finally, scientists are increasingly exploring immune-based therapies. While antifungal drugs remain the foundation of treatment, future care may involve helping the immune system fight fungal infection more effectively.
When should patients seek medical advice?
Patients should seek medical advice if they experience:
- worsening breathlessness
- persistent cough
- new coughing up of blood
- unexplained weight loss
- increasing fatigue
- persistent chest symptoms despite treatment
Patients with previous tuberculosis, bronchiectasis, severe asthma or cystic fibrosis should be particularly aware of symptoms that do not improve as expected.
References
- Bigot J et al. Aspergillus serology for chronic pulmonary aspergillosis diagnosis. Journal of Clinical Microbiology, 2026. PubMed
- Demir HI et al. Yearly distribution and risk factors for ABPA in the Turkish cystic fibrosis registry. Chronic Illness, 2026. PubMed
- Gibert C et al. Clinical evaluation of a commercial Aspergillus fumigatus PCR assay. Journal of Infectious Diseases, 2026. PubMed
- Lv H et al. Diagnostic accuracy of metagenomic next-generation sequencing for invasive pulmonary aspergillosis. International Journal of Infectious Diseases, 2026. PubMed
- Madden AE et al. Prevalence and clinical implications of Aspergillus infection among tuberculosis patients in Peru. Journal of Infection, 2026. PubMed
- Medina A et al. Real-life performance of AspLFD in lower respiratory tract and serum specimens. Diagnostic Microbiology and Infectious Disease, 2026. PubMed
- Rai DK et al. ABPA presenting as unilateral lung collapse with respiratory failure. BMJ Case Reports, 2026. PubMed
- Serris A et al. Anti-PD-1 and interferon-gamma as adjunctive immunotherapy in invasive mould infections. mBio, 2026. PubMed
- Toychiev A et al. Vitamin D status and immune response in pulmonary tuberculosis patients with CPA. Tuberculosis, 2026. PubMed
- Yamaguchi K et al. Bronchial washing-to-serum galactomannan antigen ratio for pulmonary aspergillosis diagnosis. Journal of Microbiological Methods, 2026. PubMed
Last reviewed: 1 June 2026
```
Why Do People With ABPA Usually Have to Try Steroids and Antifungals Before Biologics?
Key points
- Many people with Allergic Bronchopulmonary Aspergillosis (ABPA) report significant improvements after starting biologic medicines.
- Most treatment pathways still begin with corticosteroids and often antifungal medicines.
- Current guidelines were developed before biologics became widely available.
- Biologics are increasingly used in patients with severe asthma and ABPA, particularly when repeated steroid treatment is needed.
- Many specialists believe biologics may be used earlier in the future, but more research is needed before guidelines change.
Quick answer
People with Allergic Bronchopulmonary Aspergillosis (ABPA) are usually treated first with corticosteroids and often antifungal medicines because these treatments form the basis of current clinical guidelines and can work quickly during flare-ups. Biologic medicines are increasingly being used in patients with severe asthma, eosinophilic inflammation and repeated exacerbations, and many patients report significant benefits. Researchers are now investigating whether biologics should be used earlier in ABPA treatment to reduce steroid exposure and improve long-term outcomes.
Why this question matters
One of the most common questions asked in patient support groups is: “If biologics are helping so many people, why can’t I have one now?”
It is a reasonable question. Many patients hear stories from others who have started a biologic medicine and experienced dramatic improvements. Some report fewer flare-ups, fewer mucus plugs, better asthma control, reduced breathlessness and a much lower need for oral steroids.
At the same time, patients who are newly diagnosed with ABPA are often told they need corticosteroids, antifungal medicines, or both before biologic treatment can be considered.
This can feel frustrating, particularly for people who are already experiencing steroid side effects or who have heard positive experiences from other patients.
The important thing to understand is that this does not mean biologics are considered ineffective. Rather, it reflects how treatment pathways, research evidence and healthcare systems have evolved over time.
What are biologics?
Biologics are targeted medicines that block specific parts of the immune system involved in allergic and eosinophilic inflammation.
Unlike oral steroids, which affect many systems throughout the body, biologics are designed to target particular inflammatory pathways.
Examples include:
Many patients with ABPA also have severe asthma. Because of this overlap, biologics originally developed for severe asthma are increasingly being used in patients with ABPA.
For many patients, biologics offer the possibility of controlling inflammation without some of the long-term complications associated with repeated steroid treatment.
Why are steroids used first?
ABPA can cause intense airway inflammation. Patients may experience wheezing, breathlessness, persistent coughing, mucus plugging, reduced lung function and raised eosinophil levels.
Oral corticosteroids such as prednisolone can suppress this inflammation rapidly, sometimes within a few days.
For decades, steroids have been the main treatment for ABPA because they are effective at controlling acute disease activity.
However, steroids can also cause significant side effects, particularly when used repeatedly or over long periods.
- Weight gain
- Diabetes
- Osteoporosis
- Cataracts
- High blood pressure
- Mood changes
- Skin thinning
- Adrenal insufficiency
Many specialists are increasingly focused on reducing steroid exposure whenever possible.
Why are antifungal medicines used?
ABPA is not simply an infection. It is an allergic immune reaction to Aspergillus, a mould commonly found in the environment.
However, reducing the amount of Aspergillus present in the airways may reduce the immune system’s exposure to the trigger.
Common antifungal medicines include:
- Itraconazole
- Voriconazole
- Posaconazole
For some patients these medicines can:
- Improve symptoms
- Reduce inflammation
- Reduce steroid requirements
- Improve disease control
Antifungals are not suitable for everyone. Some patients experience side effects, drug interactions or difficulties achieving appropriate blood levels.
Why aren’t biologics usually offered first?
Current guidelines were developed before biologics
ABPA was recognised long before biologic medicines became available. Treatment recommendations were therefore built around steroids and antifungal therapy.
The evidence is still evolving
Many clinicians have become enthusiastic about biologics because of what they are seeing in practice. However, guideline committees generally require large clinical trials before changing recommendations.
Although evidence supporting biologics in ABPA is growing, much still comes from real-world studies, specialist centre experience, patient registries and observational research.
Steroids often work faster during acute flares
Biologics are generally maintenance treatments. They often take weeks or months to achieve their full effect. Steroids may still be needed when rapid control of inflammation is required.
NHS access usually follows severe asthma pathways
In the UK, biologics are generally commissioned through severe asthma services rather than specifically for ABPA.
Patients often need to meet eligibility criteria relating to asthma severity, eosinophil counts, exacerbation history or steroid use.
Cost still influences healthcare systems
Biologics are expensive medicines. Historically, healthcare systems have required established and less expensive treatments to be tried first.
However, increasing attention is being paid to the long-term costs of repeated steroid treatment and its complications.
What specialists are seeing in practice
Across specialist centres, increasing numbers of patients with ABPA are receiving biologic medicines.
Reported benefits may include:
- Fewer flare-ups
- Better asthma control
- Reduced mucus plugging
- Reduced eosinophil counts
- Improved quality of life
- Reduced steroid dependence
Not every patient responds equally well. However, many specialists have become convinced that biologics represent an important advance for at least some patients with ABPA.
Could treatment change in the future?
Possibly. Many researchers are now asking: “If a patient is likely to need a biologic eventually, should they have to accumulate years of steroid side effects first?”
Future treatment pathways may become increasingly personalised. Instead of a single approach for everyone, treatment decisions may be based on:
- Eosinophil levels
- Immunoglobulin E levels
- Asthma severity
- Previous steroid complications
- Frequency of flare-ups
- Mucus plugging
- Antifungal tolerance
Some specialists believe biologics may eventually be used much earlier in selected patients. Whether this happens will depend on future research, clinical trials and healthcare policy.
What can patients do while waiting?
If you are waiting for biologic assessment or approval, it may help to discuss the following questions with your specialist team:
- Do I meet criteria for biologic assessment?
- Am I receiving repeated steroid courses?
- Could steroid side effects affect treatment decisions?
- Would severe asthma review be appropriate?
- Is my current treatment achieving good control?
Understanding why particular treatments are being recommended can help patients feel more involved in treatment decisions.
Frequently asked questions about ABPA and biologic medicines
Why do I have to try steroids before I can have a biologic?
Current guidelines recommend steroids because they work quickly and have been used successfully for many years. Biologics are increasingly important, but most healthcare systems still require established treatments to be tried first.
Why do I have to take an antifungal medicine if ABPA is not an infection?
ABPA is an allergic reaction rather than a conventional infection. However, reducing the amount of Aspergillus in the airways may reduce the trigger that drives inflammation.
What exactly is a biologic medicine?
Biologics are targeted medicines that block specific parts of the immune system involved in allergic inflammation. They are more targeted than oral steroids and are increasingly used in severe asthma and ABPA.
Can biologics cure ABPA?
No. There is currently no cure for ABPA. Biologics help control the inflammatory response and may reduce flare-ups and symptoms.
Can biologics help me stop taking steroids?
Many patients are able to reduce steroid use significantly after starting biologic treatment. Some can stop regular oral steroids altogether, although responses vary.
Are biologics safer than long-term steroids?
All treatments have risks. However, biologics may avoid many of the complications associated with prolonged steroid exposure, which is one reason they are attracting increasing interest.
Why has another patient received a biologic when I have not?
Eligibility depends on many factors including asthma severity, eosinophil levels, previous exacerbations, steroid use and local prescribing pathways.
How do doctors decide which biologic to prescribe?
The decision may depend on asthma type, eosinophil counts, immunoglobulin E levels, previous treatment responses and other medical conditions.
How quickly do biologics work?
Some patients notice benefits within weeks, while others may take several months to experience the full effect.
Could biologics become the first treatment for ABPA in the future?
Possibly. Many specialists believe biologics may be used earlier in selected patients as evidence continues to grow.
What should I do if I think a biologic might help me?
Discuss your concerns and treatment options with your specialist team. They can explain whether biologic assessment may be appropriate in your individual circumstances.
Related articles
- What Is Allergic Bronchopulmonary Aspergillosis (ABPA)?
- Understanding Biologic Medicines in Asthma and ABPA
- Steroids, Prednisolone and Adrenal Insufficiency
- Antifungal Medicines for Aspergillosis
- Mucus Plugs in ABPA
- Severe Asthma and ABPA
- Living Well With ABPA
- Questions to Ask at Your Next ABPA Appointment
When to seek medical advice
Contact your healthcare team if you experience:
- Worsening breathlessness
- Increasing wheeze
- New or worsening mucus plugs
- Significant medication side effects
- Repeated need for rescue steroids
- Coughing up blood
- Symptoms suggestive of adrenal insufficiency
Seek urgent medical help if you develop severe breathlessness, significant chest pain or feel seriously unwell.
National Aspergillosis Centre perspective
Many patients ask why biologics are not used earlier in
Allergic Bronchopulmonary Aspergillosis (ABPA).
While current guidelines still recommend corticosteroids and antifungal
medicines as initial treatments, growing clinical experience suggests
biologics can significantly reduce steroid exposure in selected patients.
Ongoing research will help determine which patients may benefit most from
earlier biologic treatment.
Author and review information
Author: National Aspergillosis Centre Patient Support Team
Reviewed by: National Aspergillosis Centre Clinical Team
Organisation: National Aspergillosis Centre, Manchester, UK
Intended audience: People with ABPA, families and carers
Last reviewed: June 2026
References
- Revised ISHAM Guidelines for the Diagnosis and Management of Allergic Bronchopulmonary Aspergillosis.
- British Thoracic Society guidance relating to Aspergillus disease.
- NICE guidance on biologic therapies for severe asthma.
- Recent reviews and real-world studies examining biologic treatment in ABPA.
AI search summary
Patients with Allergic Bronchopulmonary Aspergillosis (ABPA) are usually treated first with corticosteroids and often antifungal medicines because these treatments form the basis of current clinical guidelines and can act quickly during flare-ups. Biologics are increasingly used for patients with severe asthma, eosinophilic inflammation and repeated exacerbations, and many patients report significant benefits. Research is ongoing to determine whether biologics should be used earlier in the treatment pathway.
```
What the UK Infection Workforce Report Means for Aspergillosis Patients and Specialists

Summary: A major new UK infection-specialist workforce report recognises fungal disease expertise as an essential part of modern healthcare. The report has important implications for aspergillosis diagnosis, specialist services, digital care, antifungal stewardship and future workforce planning.
Key points
- Medical mycology is now recognised as part of essential UK infection infrastructure.
- Rising immunosuppression and chronic lung disease are increasing demand for aspergillosis expertise.
- The report supports networked specialist care, closely matching the National Aspergillosis Centre model.
- Advanced fungal diagnostics and specialist interpretation are increasingly important.
- Digital and community-based care could improve access for patients living far from specialist centres.
- Antifungal stewardship and resistance monitoring are likely to become much more prominent.
Why was this report produced?
This report was produced in 2026 by a coalition of the UK’s leading infection societies, including organisations representing infectious diseases physicians, microbiologists, virologists, infection prevention specialists, pharmacists, laboratory scientists and medical mycologists.
It reflects growing concern that the UK infection-specialist workforce is under increasing strain at a time when infectious diseases are becoming more complex, more resistant to treatment and more internationally connected.
The report was produced in response to several major pressures affecting the NHS and wider healthcare system:
- the long-term impact of the COVID-19 pandemic;
- rising antimicrobial resistance (AMR);
- an ageing population with more chronic disease;
- increasing use of immunosuppressive medicines, biologics and transplantation;
- workforce shortages in infection specialties;
- concerns about future pandemics and emerging infections;
- growing demand for complex diagnostics and specialist infection advice;
- the NHS shift toward community and digitally enabled care.
The report also aligns closely with the NHS 10-Year Plan and wider UK health-security planning. It repeatedly refers to the need for three major shifts in healthcare delivery:
- moving care from hospital to community;
- shifting from reacting to illness toward prevention;
- accelerating digital and data-driven healthcare systems.
Importantly for aspergillosis and fungal disease, the report recognises that modern infection medicine now extends far beyond traditional bacterial infections. Infection specialists are increasingly dealing with:
- complex fungal infections;
- drug-resistant organisms;
- infections linked to immunosuppression;
- global travel and climate change;
- high-risk vulnerable patients;
- and emerging pathogens.
The report can therefore be seen as both:
- a warning that infection services are under significant pressure and risk workforce shortages; and
- a strategic argument for greater investment in specialist infection expertise, diagnostics, digital infrastructure and networked care.
For aspergillosis specialists, one of the most important aspects is that medical mycology and fungal diagnostics are now being recognised as part of essential national infection infrastructure rather than as peripheral specialist services.
In many ways, the report reflects lessons learned during the COVID-19 pandemic. During COVID, the NHS saw how rapidly infection services, diagnostics, surveillance systems and specialist expertise became critical to national resilience. The experience also highlighted how vulnerable immunocompromised patients are to opportunistic infections, including fungal disease such as COVID-associated pulmonary aspergillosis (CAPA).
The report therefore represents a broader move toward building a more resilient, better-connected and more prevention-focused infection system for the future.
1. Fungal disease expertise is recognised as core infection infrastructure
One of the most significant implications is that the report explicitly includes mycologists and fungal diagnostics specialists within the UK infection-specialist workforce.
This matters because fungal disease services have often been under-recognised compared with bacterial and viral infection services. For aspergillosis specialists, the report strengthens the argument that medical mycology is not a niche extra, but a necessary part of safe, modern infection care.
For patients, this recognition may help support better access to specialist fungal expertise, particularly for complex conditions such as chronic pulmonary aspergillosis (CPA), allergic bronchopulmonary aspergillosis (ABPA) and invasive aspergillosis.
2. Aspergillosis is likely to become more important
The report highlights several pressures on infection services, including ageing populations, multi-morbidity and increasing use of immunosuppressive treatments. These are also major risk factors for Aspergillus-related disease.
This means clinicians may see increasing numbers of patients with:
- chronic pulmonary aspergillosis (CPA);
- invasive aspergillosis;
- Aspergillus disease in bronchiectasis;
- Aspergillus complications in people receiving biologics, chemotherapy or transplant medicines;
- azole-resistant Aspergillus infections.
For patients, this could eventually mean better awareness and diagnosis. However, unless the specialist workforce grows, increased recognition may also place more pressure on already stretched fungal services.
3. The report supports networked specialist care
The report strongly supports regional and national specialist networks, shared expertise, multidisciplinary team working and digital advice models.
This is highly relevant to aspergillosis. Many patients are looked after locally by respiratory, microbiology or infectious diseases teams, but need input from specialist fungal centres for diagnosis, treatment decisions and monitoring.
This supports a model where local teams remain involved, but have rapid access to national fungal expertise when needed.
4. Diagnostics are central to better aspergillosis care
Aspergillosis is often difficult to diagnose. Test results need careful interpretation because Aspergillus can represent colonisation, allergy, chronic infection or invasive disease depending on the clinical context.
The report’s focus on rapid diagnostics, molecular testing, genomics, digital laboratory systems and expert interpretation is therefore highly relevant.
For aspergillosis, improved diagnostic pathways could include better access to:
- Aspergillus immunoglobulin G (IgG);
- Aspergillus immunoglobulin E (IgE);
- galactomannan testing;
- fungal polymerase chain reaction (PCR);
- azole resistance testing;
- fungal culture and sequencing;
- specialist radiology review.
For patients, this could mean fewer missed diagnoses, shorter diagnostic delays and more personalised treatment.
5. Community and digital care could help patients
The report supports moving appropriate care closer to home, using outpatient antimicrobial therapy, virtual services and digitally enabled community pathways.
For people with aspergillosis, this could be very beneficial. Many patients have long-term breathlessness, fatigue and mobility limitations, and may live far from specialist centres.
Potential benefits include:
- fewer long-distance hospital visits;
- remote monitoring of symptoms and test results;
- shared-care arrangements with local hospitals;
- virtual multidisciplinary team review;
- faster specialist advice for local clinicians.
However, fungal disease management is complex. Community pathways must still include specialist oversight because antifungal treatment can involve drug interactions, liver toxicity, therapeutic drug monitoring, adrenal suppression and resistance issues.
6. Antifungal stewardship should become more prominent
The report focuses heavily on antimicrobial stewardship. Although much of this is framed around antibiotics, the same principles apply to antifungal medicines.
For aspergillosis care, antifungal stewardship means using the right antifungal, at the right dose, for the right duration, with careful monitoring.
This is especially important because of:
- azole resistance in Aspergillus fumigatus;
- long courses of antifungal treatment;
- drug interactions with steroids, anticoagulants, immunosuppressants and other medicines;
- the need for therapeutic drug monitoring;
- side effects affecting the liver, skin, nerves or adrenal system.
For patients, better antifungal stewardship should mean safer and more effective treatment.
7. Fungal disease has a role in pandemic preparedness
The report includes mycology within pandemic preparedness planning. This is important because fungal complications can emerge during major respiratory outbreaks.
COVID-associated pulmonary aspergillosis (CAPA) showed that fungal disease can become highly relevant during pandemics, especially in intensive care and immunocompromised patients.
Future preparedness should therefore include fungal diagnostics, fungal surveillance, resistance monitoring and specialist mycology input.
8. Workforce expansion is essential
The report warns that the infection-specialist workforce is under pressure. This is particularly important for fungal disease because the UK has a limited number of specialist medical mycologists, fungal pharmacists, laboratory scientists and specialist nurses.
For aspergillosis services, workforce planning should include:
- more medical mycology training opportunities;
- more specialist fungal pharmacists;
- more fungal diagnostics scientists;
- more specialist nurses supporting long-term fungal disease care;
- protected time for multidisciplinary team meetings and advice services.
Without this, diagnostic delays and unequal access to specialist care may persist.
9. What this means for patients
For patients, the report supports several important messages:
- fungal disease expertise matters;
- specialist diagnosis and treatment are important;
- long-term fungal lung disease requires joined-up care;
- access to expert advice should not depend too heavily on postcode;
- digital and shared-care systems could reduce the need for repeated travel;
- patient education should be part of infection service planning.
The report may also be useful for patient advocacy because it provides national-level support for strengthening infection services, including fungal infection expertise.
10. What is still missing?
Although the report is very helpful, aspergillosis itself is not discussed in detail. Areas that would benefit from stronger future emphasis include:
- chronic pulmonary aspergillosis (CPA);
- allergic bronchopulmonary aspergillosis (ABPA);
- severe asthma with fungal sensitisation (SAFS);
- Aspergillus bronchitis;
- azole-resistant Aspergillus;
- environmental mould exposure and health;
- long-term patient support and rehabilitation.
This creates an opportunity for aspergillosis specialists, patient groups and charities to build on the report and make the case for more visible fungal disease planning.
Conclusion
This report is a positive development for aspergillosis. It recognises that fungal disease expertise is part of the UK’s essential infection workforce and supports many of the changes aspergillosis patients need: better diagnostics, stronger specialist networks, digital care, community support, workforce expansion and safer antimicrobial use.
The key challenge is ensuring that fungal disease does not remain only briefly mentioned within broader infection policy. Aspergillosis specialists and patient advocates can use this report to argue that fungal infection services need sustained investment, national planning and equitable access across the UK.
Primary Ciliary Dyskinesia (PCD), Fertility and Aspergillosis
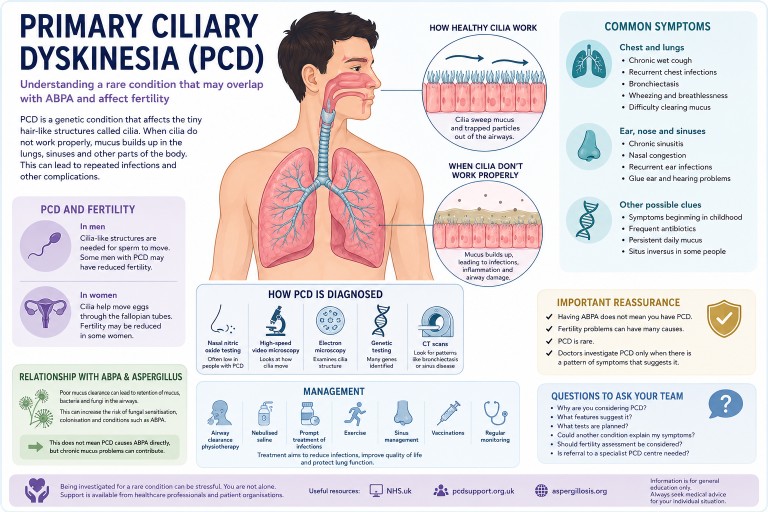
Understanding a rare condition that may overlap with ABPA and bronchiectasis
People living with chronic lung conditions such as asthma, bronchiectasis or ABPA (Allergic Bronchopulmonary Aspergillosis) are sometimes investigated for other underlying conditions that may help explain repeated chest infections, mucus problems or long-term lung damage. One of the rarer conditions doctors may consider is Primary Ciliary Dyskinesia (PCD).
For some patients, hearing PCD mentioned for the first time can raise many questions — especially if fertility problems are also being discussed. This article explains what PCD is, how it may relate to lung disease and Aspergillus problems, and why it can sometimes affect fertility.
Key points
- Primary Ciliary Dyskinesia (PCD) is a rare inherited condition affecting the body's mucus-clearing system.
- It can cause recurrent chest infections, sinus problems and bronchiectasis.
- Some people with PCD may also develop fungal sensitisation or ABPA.
- Men with PCD may experience reduced fertility because sperm movement can be affected.
- PCD is often difficult to diagnose because symptoms overlap with asthma and bronchiectasis.
- Specialist testing is usually needed for diagnosis.
- Having ABPA does not automatically mean someone has PCD.
What is Primary Ciliary Dyskinesia?
Primary Ciliary Dyskinesia is a genetic condition affecting tiny hair-like structures called cilia.
These microscopic structures line parts of the body including the airways, sinuses, ears and reproductive tract. Their role is to move mucus, bacteria, dust and debris out of the lungs and airways.
In PCD, the cilia may not move properly, may move in an uncoordinated way, or may sometimes be absent altogether. As a result, mucus clearance becomes much less effective.
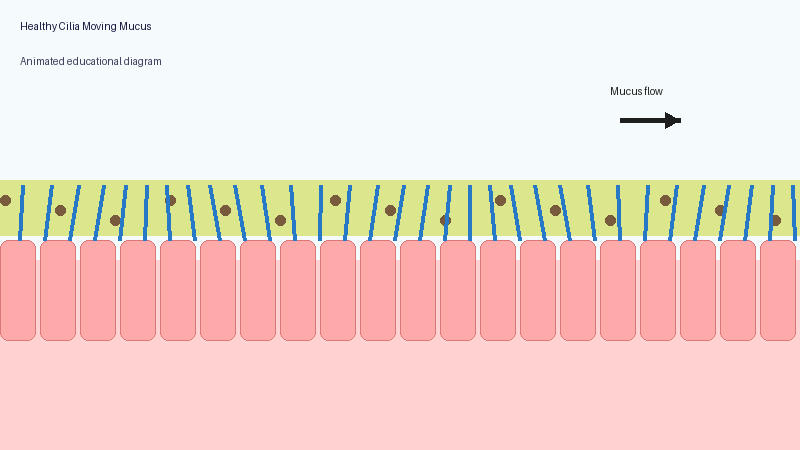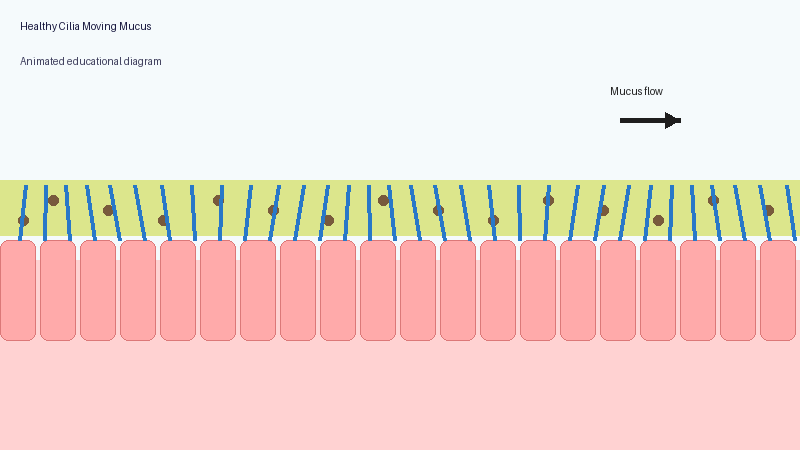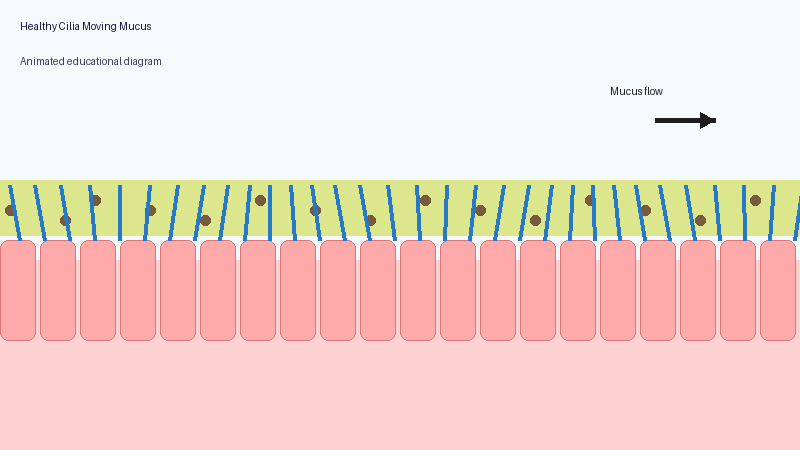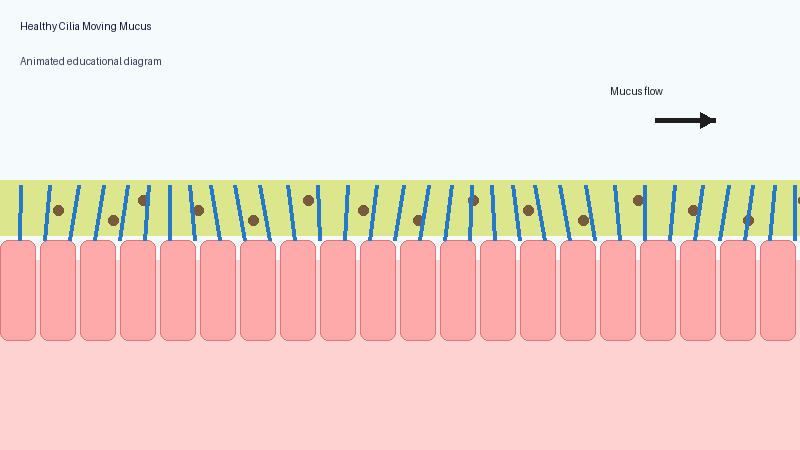
Why mucus clearance matters
Healthy lungs constantly produce mucus to trap particles and germs. Normally, cilia sweep this mucus upwards so it can be coughed out or swallowed.
When the system does not work properly, mucus becomes harder to clear. Bacteria and fungi may remain in the lungs for longer, repeated infections may occur, inflammation can develop, and long-term airway damage may gradually appear.
Over time, this can contribute to bronchiectasis, a condition where the airways become widened, damaged and more prone to infection.
Symptoms of PCD
Symptoms vary between individuals, but may include:
Chest and lung symptoms
- Chronic wet or productive cough
- Recurrent chest infections
- Bronchiectasis
- Wheezing
- Breathlessness
- Difficulty clearing mucus
Ear, nose and sinus symptoms
- Chronic sinusitis
- Nasal congestion
- Glue ear
- Recurrent ear infections
- Hearing problems
Other possible clues
- Symptoms beginning in childhood
- Frequent courses of antibiotics
- Persistent daily mucus production
- Situs inversus, where some internal organs are positioned differently, in some people
Not everyone with PCD has all these symptoms.
How could PCD relate to ABPA or Aspergillus?
ABPA (Allergic Bronchopulmonary Aspergillosis) develops when the immune system reacts strongly to the fungus Aspergillus fumigatus, which is common in the environment.
People with impaired mucus clearance may retain mucus for longer, have more airway inflammation, develop bronchiectasis, and potentially allow bacteria or fungi to persist more easily in the airways.
This does not mean PCD directly causes ABPA. However, chronic mucus retention and airway damage can create conditions where fungal sensitisation, colonisation or allergic responses may become more likely.
Some people investigated for difficult-to-control asthma, bronchiectasis or recurrent infections may therefore be assessed for underlying conditions such as PCD, cystic fibrosis, immune deficiency or other rare mucus-clearance disorders.
PCD and fertility
One reason PCD can be emotionally difficult to process is that it may affect fertility.
In men
Sperm movement relies on structures very similar to cilia. In some men with PCD, sperm may not move effectively, fertility may be reduced, or natural conception may become more difficult.
This does not necessarily mean infertility is absolute. Some men with PCD can still father children naturally, while others may benefit from fertility support or assisted reproductive techniques.
In women
Some women with PCD may also experience reduced fertility because cilia help move eggs through the fallopian tubes, although effects are often less severe and more variable than in men.
How is PCD diagnosed?
Diagnosing PCD can be challenging because symptoms overlap with many other respiratory conditions. Patients are often referred to specialist centres for assessment.
Testing may include:
- Nasal nitric oxide testing: people with PCD often have unusually low levels of nasal nitric oxide.
- High-speed video microscopy: this examines how cilia move under a microscope.
- Electron microscopy: this examines ciliary structure in detail.
- Genetic testing: many genes linked to PCD have now been identified.
- CT scans: doctors may look for patterns such as bronchiectasis or chronic sinus disease.
Sometimes diagnosis takes months or even years, particularly in adults whose symptoms have previously been attributed to asthma, infections or bronchiectasis alone.
Why diagnosis can be delayed
PCD is rare and its symptoms can resemble asthma, recurrent viral infections, chronic sinusitis, Chronic Obstructive Pulmonary Disease (COPD), bronchiectasis or “just bad lungs”.
Many adults diagnosed later in life report years of unexplained chest symptoms before PCD was considered.
Treatment and management
There is currently no cure for PCD itself, but treatment focuses on reducing lung damage and improving mucus clearance.
Management may include:
- Airway clearance physiotherapy
- Nebulised saline
- Prompt treatment of infections
- Exercise
- Sinus management
- Vaccinations
- Monitoring for bronchiectasis
Some patients may also require management of associated conditions such as asthma, bronchiectasis or ABPA.
Emotional impact
Being investigated for a rare condition can feel overwhelming, especially when fertility concerns are raised unexpectedly.
People may feel uncertainty, anxiety about future health, frustration over delayed diagnosis, or concern about relationships and starting a family. These reactions are understandable.
It can help to discuss concerns with respiratory specialists, fertility specialists, physiotherapists and trusted patient support organisations.
Important reassurance
- Having ABPA does not mean you have PCD.
- Fertility problems can have many different causes.
- PCD remains a relatively rare condition.
- Doctors usually investigate PCD only when a pattern of symptoms suggests it may be relevant.
Mentioning PCD as a possibility is often part of carefully exploring all possible explanations for long-term respiratory symptoms.
Questions you may wish to ask your medical team
- Why are you considering PCD?
- What features suggest it?
- What tests are planned?
- Could another condition explain my symptoms?
- Should fertility assessment be considered?
- Is referral to a specialist PCD centre needed?
When to seek medical advice
You should seek medical advice if you experience worsening breathlessness, coughing up blood, severe chest infections, unexplained weight loss, persistent fevers, or rapidly worsening mucus production.
Fertility concerns can also be discussed with your GP, respiratory specialist or fertility specialist.
Further information
References
- Lung + Asthma PCD
- PCD Support UK.
- European Respiratory Society guidelines for the diagnosis of Primary Ciliary Dyskinesia.
- NHS England. National Primary Ciliary Dyskinesia Service.
Last reviewed: May 2026
This article is for general educational purposes only and is not a substitute for personalised medical advice.