Inhalers and Nebulisers
Inhalers and nebulisers are medical devices that turn liquid medicines into a fine mist with small droplets that can be inhaled into the lungs. This helps to concentrate the medication where it needs to be, while reducing the amount of side effects you experience.
Inhalers
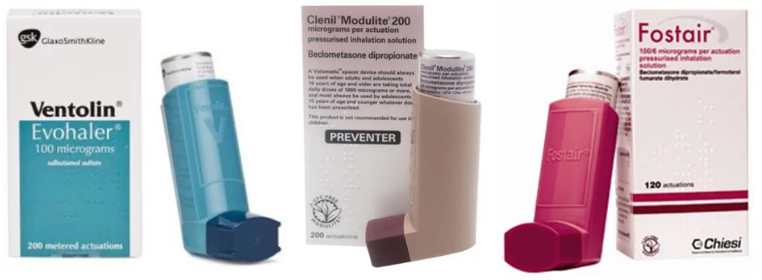
Hand-held inhalers are commonly used for mild to moderate asthma. A reliever (usually blue) contains Ventolin, which opens up the airways during an asthma attack. A preventer (often brown) contains a corticosteroid (e.g. beclomethasone), which are taken daily to reduce inflammation in the lungs and reduce the risk of an attack happening. Inhalers are small and portable, but some people find them fiddly and prefer to use a spacer cylinder.
Ask your doctor or pharmacist to show you how to use your inhaler effectively. To check whether an inhaler needs replacing, pull out the metal canister and shake – you should be able to feel liquid sloshing around inside it.
- Read more at asthma.org.uk
Nebulisers
Nebulisers are electrical appliances that deliver higher doses of medications into your lungs through a mask, which is useful when patients are too ill or unable to use handheld inhalers, or when the medication is not available in inhaler form. Nebulisers can deliver medication such as Ventolin, saline (to loosen mucus), antibiotics (e.g. colicin) or antifungals, although some must be delivered through a mouthpiece because they can leak around a mask and get into the eyes.

Nebulisers used at the National Aspergillosis Centre:
Jet nebulisers use compressed gas (air or oxygen) to atomise medication or saline, and are suitable for sticky medications. These are driven by a compressor (eg. Medix Econoneb), which draws air (or oxygen) in and pushes it through a filter and into the nebuliser chamber. The two types of jet nebuliser used at the National Aspergillosis Centre are simple jet nebulisers (eg. Microneb III) and breath-assisted nebulisers (eg. Pari LC sprint).
Simple jet nebulisers deliver medication at a constant rate until it runs out, whether you are breathing in or out – therefore not all of the medication will be delivered to your airways . The droplet size produced by simple jet nebulisers is also larger than that produced by breath-assisted nebulisers, so the medication is not delivered as far down into your lungs. This is useful for medications such as bronchodilators (eg. Ventolin), which target the smooth muscle in your airways, and therefore do not need to reach as far down as your alveoli.
Breath-assisted nebulisers have a valve which shuts when you inspire, stopping medication leaking out of the nebuliser while you breath in, so less medication is wasted. The droplets produced are also smaller, meaning that they can reach further down your airways. Therefore the breath-assisted nebuliser is used for antibiotic and antifungal medication, so they can reach the smallest, furthest parts of your airways.
Other nebulisers:
Vibrating mesh nebulisers use a rapidly-vibrating crystal to vibrate a metal plate with holes in (a bit like a tiny sieve). The vibration forces the medication through the holes in the plate, generating a mist of small droplets. Small, portable versions of vibrating mesh nebulisers are available, however they are not used by the NAC as they cannot be used with many of the medications prescribed to our patients, and are not always very robust.
Like vibrating mesh nebulisers, ultrasonic nebulisers use a rapidly-vibrating crystal; however, instead of pushing the droplets through pores in a metal plate, the crystal vibrates the medication directly. This breaks the liquid into droplets at its surface, and this mist can be breathed in by the patient. Ultrasonic nebulisers are not suitable for certain medications and aren’t traditionally used in the home setting.
For more information:
- Read this article by Prescribing in Practice for more technical detail.
- Read more at the British Lung Foundation
If your doctor recommends you to use nebulised medication then your care team may be able to arrange for you to borrow one without charge from the hospital and show you how to use it. However, if this is not possible then you may have to buy your own. It is important to follow the cleaning instructions that the nebuliser comes with, and replace masks and tubing every 3 months.