Why Antifungal Drug Interactions Matter — and How AntifungalInteractions.org Can Help

Key points
- Antifungal medicines used in aspergillosis can interact with many common medicines and supplements.
- Some interactions are mild, while others can significantly affect drug levels or side effects.
- Interactions may involve steroids, inhalers, antibiotics, heart medicines, acid suppressants and herbal supplements.
- Patients should always tell healthcare teams about all medicines, vitamins and supplements they take.
- AntifungalInteractions.org is a specialist resource designed to help healthcare professionals and patients understand potential antifungal interactions.
Why do antifungal interactions matter so much?
The antifungal medicines used to treat aspergillosis are powerful and highly specialised drugs. They are extremely important in controlling fungal disease, but many also affect the way the body processes other medicines.
This is particularly true for azole antifungals such as:
- itraconazole,
- voriconazole,
- posaconazole,
- isavuconazole.
These medicines are processed through enzyme systems in the liver, especially the cytochrome P450 system. Unfortunately, many other medicines also use these same pathways.
This means antifungals can sometimes:
- increase levels of other medicines,
- reduce levels of other medicines,
- increase side effects,
- affect liver function,
- change how well treatments work.
Because aspergillosis patients often take several medicines at the same time, interactions become particularly important.
Common medicines that may interact with antifungals
Not every interaction is dangerous, and many medicines can still be used safely with careful monitoring. However, some combinations require dose adjustments or additional caution.
Steroids and inhalers
Many patients with allergic bronchopulmonary aspergillosis (ABPA), severe asthma or bronchiectasis take steroid medicines.
Interactions can occur with:
- prednisolone,
- methylprednisolone,
- inhaled steroids such as fluticasone or budesonide.
Azole antifungals can increase steroid exposure, potentially increasing the risk of side effects such as:
- weight gain,
- skin thinning,
- high blood sugar,
- adrenal suppression,
- mood changes.
Heart medicines
Some antifungals can affect heart rhythm or interact with medicines used for:
- high blood pressure,
- irregular heartbeat,
- blood thinning,
- cholesterol management.
This is one reason doctors and pharmacists carefully review medication lists before starting antifungal treatment.
Acid suppressants
Medicines used for acid reflux or stomach protection may affect how well some antifungals are absorbed.
This includes:
- omeprazole,
- lansoprazole,
- esomeprazole,
- antacid preparations.
In some cases, antifungal levels may become too low to work effectively.
Antibiotics and other anti-infective medicines
Some antibiotics and antifungals can interact in ways that increase side effects or affect the electrical activity of the heart.
This is particularly important in people already taking multiple medicines.
Supplements and herbal remedies
Patients are often surprised that supplements may also interact with antifungals.
Potential concerns include:
- CBD oil or cannabis products,
- St John’s Wort,
- high-dose vitamins,
- herbal sleep remedies,
- sports supplements.
“Natural” products can still affect liver enzyme systems and may alter medicine levels.
What is AntifungalInteractions.org?
AntifungalInteractions.org is a specialist online interaction checker designed specifically for antifungal medicines.
The site was developed to help healthcare professionals identify and manage potential interactions involving antifungal drugs.
It is widely used internationally and is regularly updated by specialist pharmacy experts.
Why is it useful?
General drug references do not always provide detailed fungal-specific interaction guidance.
AntifungalInteractions.org focuses specifically on antifungal medicines and often provides:
- more detailed interaction information,
- clearer explanations of risks,
- practical management advice,
- colour-coded interaction severity ratings.
This can help patients better understand why clinicians sometimes adjust medicines, order blood tests or recommend monitoring.
Can patients use the website themselves?
Yes — many patients find it useful for understanding their treatment better.
However, it is important not to interpret interaction checkers without context.
An interaction warning does not automatically mean:
- a medicine combination is unsafe,
- treatment must stop,
- harm will definitely occur.
Many interactions can be safely managed by:
- dose adjustments,
- blood test monitoring,
- timing changes,
- careful clinical supervision.
What should patients do?
Patients should try to keep an up-to-date list of:
- prescription medicines,
- inhalers,
- vitamins,
- supplements,
- CBD or cannabis products,
- over-the-counter medicines.
It is particularly important to mention supplements or herbal remedies because these are easily overlooked during clinic visits.
Do not stop medicines without advice
One of the most important messages is that patients should not stop antifungal medicines or other prescribed treatments based only on an online interaction checker.
Antifungal treatment decisions are often carefully balanced against:
- severity of fungal disease,
- lung function,
- other illnesses,
- alternative treatment options.
Healthcare teams can often safely manage interactions once they are aware of them.
The bottom line
Drug interactions are an important part of antifungal treatment, particularly for people living with aspergillosis who may already take several medicines.
AntifungalInteractions.org is an excellent specialist resource that can help patients and healthcare professionals better understand these interactions.
However, online interaction checkers should support discussions with healthcare professionals rather than replace them.
Useful link
Visit AntifungalInteractions.org
BNF to check any other medication interactions
Author and review information
Prepared as general educational information for people affected by aspergillosis and related lung conditions.
This article does not replace personalised medical advice.
Last reviewed: May 2026
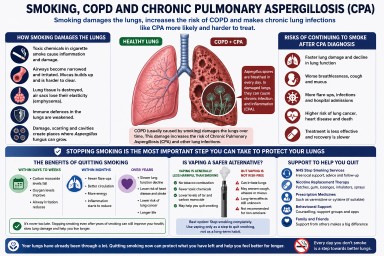
CBD Oil, Cannabis and Aspergillosis: Safety, Quality and Drug Interactions

Key points
- Some people with chronic illnesses report that CBD or cannabis products help with pain, anxiety, sleep or wellbeing.
- Evidence for benefit in aspergillosis itself remains limited.
- Smoking or vaping cannabis may irritate the lungs and may not be suitable for people with respiratory disease.
- CBD and cannabis products can interact with antifungal medicines and steroids.
- Product quality varies greatly, especially with over-the-counter or online products.
- Always let your healthcare team or pharmacist know about any CBD or cannabis products you are using.
Why this topic comes up
People living with aspergillosis often cope with long-term symptoms such as fatigue, chronic cough, breathlessness, pain or chest discomfort, anxiety, poor sleep, steroid side effects and reduced quality of life.
Because of this, discussions about CBD oil, cannabis or “medical marijuana” occasionally appear in patient groups and online communities. Some people report that these products help them cope better with symptoms or improve sleep and wellbeing.
At the same time, there are important safety issues that people with respiratory fungal disease should be aware of, particularly around lung irritation, product quality and drug interactions.
CBD and cannabis are not the same thing
CBD: cannabidiol
CBD, or cannabidiol, is one of the compounds found in cannabis plants. CBD products usually contain little or no THC, or tetrahydrocannabinol, the chemical responsible for the “high” associated with cannabis.
CBD products may be sold as oils, capsules, gummies, creams, drinks or food supplements. CBD is generally less intoxicating than THC-containing cannabis products.
Cannabis or marijuana
Cannabis products may contain varying amounts of THC. THC is more strongly associated with intoxication, impaired concentration, sedation, anxiety or panic, hallucinations or paranoia in some people, and impaired driving or coordination.
Different cannabis products can vary enormously in strength and purity.
What conditions have good evidence for medical cannabis?
Cannabis-based medicines are prescribed in some situations where evidence is reasonably strong.
In the UK, prescription cannabinoid medicines are mainly used for certain severe forms of epilepsy, chemotherapy-related nausea and vomiting, and muscle spasticity in multiple sclerosis. There is also ongoing research into chronic pain and palliative care use.
However, evidence for benefit in aspergillosis, bronchiectasis, asthma, allergic bronchopulmonary aspergillosis (ABPA) or chronic pulmonary aspergillosis (CPA) remains limited.
This does not mean that people never feel benefit. Some clearly do. But respiratory fungal disease is not currently one of the better-established medical indications.
Lung safety concerns in aspergillosis
This is probably the most important issue for many aspergillosis patients.
Smoking cannabis
Smoking any substance exposes the lungs to heat, particulates, irritants and combustion products.
For people who already have asthma, bronchiectasis, chronic lung infection, airway inflammation or fungal lung disease, this may worsen symptoms such as coughing, wheezing, chest tightness, mucus production or breathlessness.
Vaping
Some people assume vaping is automatically safer than smoking, but this is not always true.
Vaping can still irritate the airways and lungs, and the long-term effects are not fully understood. For people with fragile or inflamed lungs, clinicians are often cautious about recommending inhaled cannabis products of any kind.
Contamination and quality problems
One important issue is that cannabis and CBD products are not all produced to the same standards.
Product quality can vary greatly
Some products may contain more or less CBD or THC than stated, contain contaminants, contain pesticides or solvents, or vary significantly between batches.
This is especially true for unregulated products purchased online or from unofficial sources.
Mould contamination
Cannabis products can occasionally become contaminated with moulds, including Aspergillus species.
This is particularly concerning for immunocompromised patients, transplant patients, people on long-term steroids, and people with chronic lung disease.
Although this appears uncommon, it is one reason respiratory specialists are often cautious about smoked cannabis products in fungal disease patients.
Drug interactions: a very important issue
Many antifungal medicines are processed through liver enzyme systems that can also be affected by CBD or cannabis compounds. This means interactions are possible.
Antifungal medicines of concern
Potential interactions may occur with antifungals such as:
- itraconazole
- voriconazole
- posaconazole
- isavuconazole
These medicines already require careful monitoring because blood levels can vary significantly between people.
Adding CBD or cannabis products may potentially alter antifungal levels, liver metabolism or side-effect risks.
Steroids and other medicines
Interactions may also occur with prednisolone, methylprednisolone, opioid pain medicines, sleeping tablets, antidepressants and anti-anxiety medicines.
Possible effects may include increased sedation, dizziness, falls, confusion, liver irritation or worsening side effects.
This does not automatically mean the products are unsafe, but it does mean healthcare teams should know about them.
“Natural” does not always mean low risk
Many patients understandably assume that CBD products are “gentle” or “natural.”
However, natural products can still interact with prescription medicines, doses may be inconsistent, some products are poorly regulated, and side effects can still occur.
This is especially important in aspergillosis because patients are often already taking multiple medicines, including antifungals and steroids.
Why patients may still be interested
Despite the uncertainties, it is understandable why some patients explore these products.
People sometimes report improvement in sleep, anxiety, pain, appetite, overall wellbeing or coping with chronic illness. These experiences are real and important to acknowledge respectfully.
At present, however, there is still limited high-quality research specifically in aspergillosis and chronic fungal lung disease.
Practical safety advice
If someone chooses to use CBD or cannabis products, it is sensible to:
- tell their healthcare team or pharmacist,
- mention all supplements and oils being used,
- watch for new side effects after starting,
- avoid assuming “natural” means risk-free,
- be especially cautious with smoked or inhaled products,
- avoid driving or hazardous activities if feeling impaired.
When to seek medical advice
Medical review is important if new symptoms appear after starting CBD or cannabis products, especially:
- worsening breathlessness,
- severe drowsiness,
- confusion,
- hallucinations,
- jaundice,
- severe dizziness,
- palpitations,
- fever or worsening chest symptoms.
The bottom line
CBD and cannabis products are becoming more widely discussed in chronic illness communities, including among people with aspergillosis.
Some people report benefits for sleep, anxiety or quality of life, and there are a small number of medical conditions where prescription cannabis-based medicines are supported by stronger evidence.
However, for aspergillosis patients, important concerns remain around lung irritation, mould contamination, product quality, and interactions with antifungal medicines and steroids.
Because of this, healthcare teams are usually cautious and prefer open discussion rather than patients using these products without medical awareness.
Further information
- NHS guidance on medical cannabis
- Specialist pharmacist advice on antifungal interactions
- Specialist pharmacist advice on steroid interactions
- National Aspergillosis Centre resources on antifungal medicines
Author and review information
Prepared for aspergillosis patients and carers as general educational information. This article is not intended to replace personalised medical advice.
Last reviewed: May 2026
Weekly Aspergillosis Research Update 18th May 2026
This update is written for patients, carers and non-specialists. It is not medical advice, but it may help explain why specialist assessment, careful monitoring and joined-up care are so important in aspergillosis.
Key points
- Aspergillosis is not one single illness. It includes allergic, chronic and invasive forms, each needing different assessment and treatment.
- Several recent papers show that Aspergillus disease often develops where the lungs are already vulnerable, damaged or scarred.
- Invasive aspergillosis remains mainly a concern for people who are severely unwell or immunocompromised.
- Antifungal resistance, drug interactions and access to specialist fungal diagnostics continue to be important themes.
- Some papers describe unusual or experimental approaches, but these should not be seen as standard treatment unless recommended by a specialist team.
1. Aspergillosis can develop in already damaged lungs
One recent case report described chronic pulmonary aspergillosis complicated by a bacterial lung abscess inside a lung cavity. The patient was successfully treated with percutaneous drainage, where fluid or infected material is drained through the skin using imaging guidance, alongside medical care.
Another recent paper examined aspergillosis complicating idiopathic pulmonary fibrosis. Idiopathic pulmonary fibrosis is a serious lung-scarring condition. This paper is important because fungal infection in people with fibrotic lung disease remains relatively understudied.
A separate review on the gut-lung axis in people with cystic fibrosis on CFTR modulators also reflects the growing interest in how long-term lung disease, airway microbes, inflammation and wider body systems interact. This is not only about Aspergillus, but it is relevant to understanding why airway infections and immune responses can vary between patients.
Why this matters: Aspergillus can sometimes take advantage of areas of lung that are already damaged by previous infection, cavities, scarring, bronchiectasis, chronic obstructive pulmonary disease, tuberculosis, cystic fibrosis, fibrosis or other long-term lung conditions. This does not mean everyone with lung damage will develop aspergillosis, but it does explain why doctors may investigate new or worsening symptoms carefully.
2. Nutritional health and immune resilience
A paper on aspergillosis in anorexia nervosa reported two cases and reviewed previous published cases. Severe malnutrition can affect the immune system, making some infections more likely or harder to recover from.
Why this matters: nutrition is part of immune resilience. This does not mean that poor diet directly causes aspergillosis, but severe undernutrition may reduce the body’s ability to respond to infection. For patients living with chronic illness, maintaining nutrition, weight and muscle strength can be an important part of overall care.
3. Invasive aspergillosis remains a serious infection in high-risk groups
Several papers this week focused on invasive aspergillosis. These included a 12-year retrospective cohort study of invasive aspergillosis in children, a review of invasive mould infections in children, and a case report of pulmonary aspergillosis following severe fever with thrombocytopenia syndrome.
Other papers reported invasive Aspergillus disease in very specific high-risk settings, including extensive facial tissue necrosis after paediatric peripheral blood stem cell transplantation and a Chinese-language report on bronchoscopic interventional therapy for invasive pulmonary aspergillosis.
Why this matters: invasive aspergillosis is different from allergic bronchopulmonary aspergillosis and chronic pulmonary aspergillosis. It usually occurs in people who are severely unwell or whose immune system is significantly weakened. It is a medical emergency and requires urgent specialist care.
For patients and families, it is useful to understand that the word aspergillosis covers several different diseases. The outlook, urgency and treatment plan can be very different depending on which form is present.
4. Better diagnosis depends on awareness and laboratory capacity
A French multicentre survey looked at laboratory capacity for diagnosing fungal infections. This type of research is important because diagnosis does not depend only on the doctor thinking of fungal disease. It also depends on access to the right laboratory tests, fungal culture, antigen testing, molecular testing, susceptibility testing and specialist interpretation.
Another paper on primary ciliary dyskinesia in children included aspergillosis among the infections and differential diagnoses clinicians may need to consider when assessing complex chronic respiratory symptoms. Although this was not primarily an aspergillosis paper, it reinforces the wider point that fungal disease can be part of a broader diagnostic picture in patients with long-term airway problems.
Why this matters: delays in diagnosing aspergillosis are common. Improving diagnosis means improving the whole pathway: clinical awareness, access to tests, expert laboratories and specialist teams who can interpret complex results.
5. Antifungal resistance remains an important issue
A review on a One Health approach to antifungal resistance in allergic bronchopulmonary aspergillosis highlighted the wider problem of antifungal resistance. A One Health approach recognises that human health, animal health and the environment are connected.
Aspergillus species live widely in the environment. Resistance may emerge not only through medical antifungal use, but also through environmental exposure to antifungal compounds used in agriculture or other settings.
Why this matters: antifungal resistance can make treatment more difficult. This is one reason why specialist teams may request fungal cultures, susceptibility testing, antifungal drug-level monitoring or treatment changes. It is also why antifungals should be used carefully and monitored properly.
6. Drug interactions are a practical safety issue
One paper examined possible drug interactions between midostaurin and posaconazole in people with a type of acute myeloid leukaemia. Although this is a specialist cancer-treatment paper, it illustrates a wider issue that is relevant to many patients taking antifungal medicines.
Azole antifungals such as itraconazole, voriconazole, posaconazole and isavuconazole can interact with other medicines. These interactions may affect antifungal levels, side effects or the levels of other medicines.
Why this matters: patients taking antifungals should tell their doctor and pharmacist about all prescribed medicines, over-the-counter medicines, inhalers, herbal products and supplements. Monitoring is part of safe antifungal treatment.
7. New or alternative antifungal approaches are being explored
One case report described pulmonary aspergillosis treated with oral amphotericin B, known as MAT2203, in a patient with human immunodeficiency virus-related cryptococcal meningitis. This is interesting because amphotericin B is usually given intravenously, and oral formulations are being explored for specific situations.
A Scite literature check also highlighted recent specialist papers on endoscopic liposomal amphotericin B therapy in semi-invasive pulmonary aspergillosis and newer antifungal approaches such as manogepix. These were not central to the PubMed list used for this update, but they support the wider message that antifungal research is active.
Why this matters: research into new ways of treating Aspergillus infection is active. This is encouraging, especially for difficult cases where standard antifungal treatment is limited by resistance, side effects or interactions. However, case reports and early-stage studies should not be seen as proof that a treatment is ready for routine use.
8. Allergic bronchopulmonary aspergillosis guidance continues to evolve
A Chinese-language expert consensus paper considered the diagnosis and treatment of allergic bronchopulmonary aspergillosis with integrated traditional Chinese and western medicine. This is not directly applicable to UK practice, but it reflects the continued international interest in improving diagnosis and management of allergic bronchopulmonary aspergillosis.
Why this matters: allergic bronchopulmonary aspergillosis can be difficult to diagnose because it overlaps with asthma, bronchiectasis, mucus plugging, raised immunoglobulin E and eosinophilic inflammation. Different countries and specialist groups continue to refine how they classify and manage the condition.
9. Laboratory science continues to improve understanding of Aspergillus
One paper investigated Aspergillus fumigatus morphogenesis and pathogenesis through a putative lipid transporter called ArvA. This is laboratory-based science rather than an immediate patient-care paper.
Why this matters: basic science helps researchers understand how Aspergillus grows, adapts and interacts with the immune system. Over time, this type of work may help identify new treatment targets or explain why some infections behave differently from others.
10. A note of caution about non-standard treatments
One paper reported follow-up of a previous aspergillosis case treated with oxygen-ozone therapy. This should be interpreted very cautiously. Pulmonary aspergillosis usually requires specialist assessment and, when treatment is needed, evidence-based antifungal therapy and monitoring.
Important: patients should not stop prescribed antifungal treatment or replace it with non-standard approaches without discussion with their specialist clinical team.
What this means for patients
This week’s research shows again that aspergillosis is complex. It can be allergic, chronic or invasive. It can affect people with asthma, cystic fibrosis, damaged lungs, weakened immune systems or severe underlying illness. It may require imaging, blood tests, sputum tests, bronchoscopy, antifungal drug monitoring and careful review by experienced clinicians.
The most useful message for patients is that persistent or worsening symptoms should be taken seriously, especially in people with known lung disease or immune problems. Good communication with healthcare teams, careful monitoring and specialist fungal expertise remain central to safe care.
When to seek medical advice
People living with aspergillosis or long-term lung disease should seek medical advice if they notice:
- new or worsening breathlessness
- coughing up blood
- persistent fever or night sweats
- unexplained weight loss
- worsening fatigue or weakness
- new chest pain
- symptoms that are not improving despite treatment
- possible side effects from antifungal medicines
Urgent medical help is needed for severe breathlessness, significant coughing up of blood, confusion, collapse, severe chest pain or rapidly worsening symptoms.
References and papers included in this update
- Okazaki Y, Shirata M, Koma K, et al. Chronic pulmonary aspergillosis complicated by a lung abscess within a pulmonary cavity successfully treated with percutaneous drainage: A case report.
Internal Medicine. 2026. - Mercier A, Loridant S, Tetart M, et al. Aspergillosis in anorexia nervosa: a report of two cases and review of the literature.
BMC Infectious Diseases. 2026. - Gutierrez-Perez C, Jones JT, Puerner CTS, et al. Insights into Aspergillus fumigatus morphogenesis and pathogenesis through the putative lipid transporter ArvA.
mSphere. 2026. - Greydanus DE, Bhave SY, Ashok N, Goel A. Primary ciliary dyskinesia in pediatric persons: A microscopic movement malady.
Disease-a-Month. 2026. - Lai X, Gao Q, Wu L. A 56-Year-Old Male Farmer From China With Severe Fever With Thrombocytopenia Syndrome and Pulmonary Aspergillosis: A Case Report and Review of Literature.
American Journal of Case Reports. 2026. - Morio F, Alanio A, Boukris-Sitbon K, et al. Assessing Laboratory Capacity for Diagnosis of Fungal Infections in France: A Multicentre survey within the SINFONI Network.
Medical Mycology. 2026. - Falcon RMG, Asedillo KFY, Gilo AJG, et al. One health approach to management of antifungal resistance in allergic bronchopulmonary aspergillosis.
Molecular Biology Reports. 2026. - Kagimu E, Senkoro E, Gakuru J, et al. Pulmonary Aspergillosis Treated With Oral Amphotericin B (MAT2203) in a Patient With HIV-Related Cryptococcal Meningitis.
Clinical Case Reports. 2026. - Lefranc M, Ramel E, Marsh R, et al. Towards a gut-lung axis role in pwCF on CFTR modulators: rationale, clinical evidence and perspectives.
Journal of Cystic Fibrosis. 2026. - Bermudez J, Debray MP, Uzunhan Y, et al. Aspergillosis complicating idiopathic lung fibrosis: a multicentric series.
Respiratory Medicine. 2026. - Franzini M, Valdenassi L, Chirumbolo S. Follow up of a previous aspergillosis case report treated with oxygen-ozone therapy, reporting clinical remission of the lung fungal infection.
International Immunopharmacology. 2026. - Karaman A, Cengiz AB, Aykac K, et al. Evaluation of the Clinical Characteristics and Survival of Pediatric Patients with Invasive Aspergillosis: A 12-year Retrospective Cohort Study.
Mycopathologia. 2026. - Joisten CS, Mellinghoff SC, Seidel D, et al. Clinical impact of potential drug-drug interactions between midostaurin and posaconazole in FLT3-mutated AML.
Antimicrobial Agents and Chemotherapy. 2026. - Lim H, Kim MW, Lee JW. Delayed Anterolateral Thigh Free Flap Reconstruction for Extensive Buccal-Midfacial Necrosis Caused by Invasive Aspergillosis After Pediatric PBSCT: A 7-Year Follow-Up.
Journal of Craniofacial Surgery. 2026. - Warris A, Rojo P, Groll AH, Arrieta AC. Invasive mold infections in the pediatric setting: current status and new developments.
Expert Review of Anti-Infective Therapy. 2026. - Li J, Cai CL, Zhao LN, Wang YH, Mu XD. Clinical analysis of comprehensive bronchoscopic interventional therapy for invasive pulmonary aspergillosis.
Zhonghua Jie He He Hu Xi Za Zhi. 2026. - Allergy Committee of Chinese Association of Integrative Medicine. Expert consensus on the diagnosis and treatment of allergic bronchopulmonary aspergillosis with integrated traditional Chinese and western medicine: 2026 edition.
Zhonghua Yi Xue Za Zhi. 2026.
Editor’s note
This article is based mainly on a PubMed search for recent aspergillosis papers. Each reference links to its PubMed record where readers can view the abstract, journal details and, where available, links to free full text. A brief Scite search was also used to identify related recent papers and research themes, but the main patient-facing interpretation has been written from the PubMed results listed above.
Last reviewed: May 2026
Aspergillosis Trust: Supporting People Affected by Aspergillosis

Raising Awareness of Aspergillosis
One of the Trust’s most important roles is increasing awareness of aspergillosis among:
- Patients and carers
- Healthcare professionals
- Researchers
- Policy makers
- The wider public
This includes helping people better understand conditions such as:
- ABPA (Allergic Bronchopulmonary Aspergillosis)
- CPA (Chronic Pulmonary Aspergillosis)
- Aspergilloma
- Invasive aspergillosis
- Severe asthma with fungal sensitisation (SAFS)
By promoting education and awareness, the Trust helps support earlier recognition and diagnosis of fungal disease.
Patient Support and Community
Living with aspergillosis can be physically and emotionally challenging. Many patients experience fatigue, breathlessness, anxiety, long treatment journeys and uncertainty about the future.
The Aspergillosis Trust helps provide:
- Patient-focused information
- Community support
- Awareness campaigns
- Educational events
- Opportunities for patient involvement
The charity also helps patients connect with others who understand the realities of living with chronic fungal disease, reducing feelings of isolation and helping people feel supported.
Supporting Research and Advocacy
The Trust actively supports research into aspergillosis and fungal disease, while also advocating for better services and greater recognition of fungal infections within healthcare systems.
This includes:
- Supporting patient participation in research
- Raising awareness of diagnostic delays
- Promoting better understanding of chronic fungal disease
- Working alongside clinicians, researchers and respiratory organisations
- Supporting international awareness activities
The organisation has collaborated with specialist centres, patient groups and international respiratory organisations to strengthen awareness and improve education around aspergillosis.
Working Together with the Wider Respiratory Community
The Aspergillosis Trust is part of a growing international effort to improve fungal disease awareness and patient support.
This includes collaboration and engagement with organisations such as:
- European Lung Foundation (ELF)
- European Respiratory Society (ERS)
- Specialist respiratory and infectious disease centres
- Patient advocacy organisations
- Researchers working in fungal disease and respiratory medicine
These partnerships help ensure that the experiences of people living with aspergillosis are represented within wider respiratory healthcare discussions.
Differences Between the Aspergillosis Trust and National Aspergillosis Centre Patient Support
The Aspergillosis Trust and the National Aspergillosis Centre (NAC) both play extremely important roles in supporting people affected by aspergillosis, but they are different types of organisations with different responsibilities and strengths. In many ways, they complement one another.
The National Aspergillosis Centre (NAC)
The National Aspergillosis Centre is an NHS Highly Specialised Service based at Wythenshawe Hospital in Manchester. It is a specialist clinical centre commissioned to diagnose, treat and manage complex aspergillosis cases — particularly Chronic Pulmonary Aspergillosis (CPA).
The NAC provides:
- Specialist medical diagnosis and treatment
- Advice and Guidance to clinicians across the UK
- Monitoring of antifungal therapy
- Clinical investigations and testing
- Research programmes
- Patient education resources
- NHS-supported patient support meetings and moderated support groups
The NAC CARES team (Community, Awareness, Research, Education and Support) runs:
- The patient information website aspergillosis.org
- Weekly Microsoft Teams meetings
- Educational webinars
- Facebook and online support communities
- Research participation activities
- World Aspergillosis Day educational events
Because the NAC is part of the NHS, its information tends to be strongly clinically focused and evidence-based, with close involvement from specialist doctors, nurses, pharmacists and researchers.
The Aspergillosis Trust
The Aspergillosis Trust is a patient-led charity rather than a clinical NHS service. It was created by patients and carers affected by aspergillosis to improve awareness, advocacy and community support.
The Trust focuses particularly on:
- Raising public and professional awareness
- Patient advocacy
- Representing the patient voice
- Community support
- Campaigning for earlier diagnosis and better recognition
- Helping reduce isolation among patients and carers
Because it is patient-led, the Trust brings a particularly strong lived-experience perspective. Many people find this valuable because the charity is run by people who directly understand the emotional, practical and social impact of living with aspergillosis.
A Simple Way to Think About the Difference
| NAC Patient Support | Aspergillosis Trust |
|---|---|
| NHS specialist clinical service | Independent patient charity |
| Led by healthcare professionals and NHS staff | Led by patients and carers |
| Focus on diagnosis, treatment, education and research | Focus on advocacy, awareness and peer support |
| Provides specialist clinical expertise | Provides lived-experience support |
| Closely linked to NHS care pathways | Represents the broader patient community |
| Produces medically reviewed educational resources | Amplifies the patient voice and patient needs |
How They Work Together
Importantly, these organisations are not competitors. They often collaborate closely on awareness campaigns, patient education, World Aspergillosis Day activities, webinars, conferences and research engagement.
Many patients benefit from engaging with both:
- The NAC for specialist medical expertise and educational resources
- The Aspergillosis Trust for advocacy, lived experience and broader patient community support
Together, they help create a stronger support network for people living with aspergillosis.
Why Patient Participation Matters
Patient experience is one of the most valuable resources in improving understanding of aspergillosis.
People living with aspergillosis often understand challenges that are not always visible in clinical appointments, including:
- Diagnostic delays
- Fatigue and fluctuating symptoms
- Treatment side effects
- Emotional impact
- Difficulties accessing information and support
By sharing experiences and becoming involved in awareness and advocacy activities, patients and carers can help improve understanding and support for others.
Participation does not need to be overwhelming. It can include:
- Sharing experiences confidentially
- Joining online discussions or support groups
- Supporting awareness campaigns
- Attending educational events
- Helping improve patient information
- Participating in surveys or research projects
Even small contributions can help improve awareness and care for future patients.
How to Learn More or Get Involved
- Aspergillosis Trust Website
- European Lung Foundation Aspergillosis Pages
- National Aspergillosis Centre Resources
The Aspergillosis Trust demonstrates the importance of patient-led advocacy in rare and under-recognised diseases. Through education, awareness and community support, the charity helps ensure that people living with aspergillosis are better informed, better supported and increasingly heard.
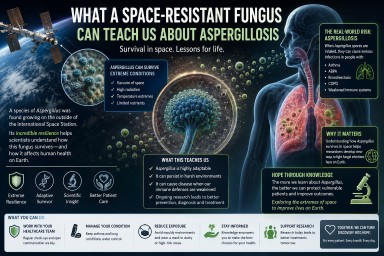
What a Space-Resistant Fungus Can Teach Us About Aspergillosis
A recent Smithsonian article described how a microscopic fungus survived conditions designed to sterilise spacecraft. At first glance, this might sound like a story about space exploration rather than human health. But for people living with aspergillosis, it carries an important and surprisingly positive message.
Fungi are remarkable survivors
The article describes research showing that some Aspergillus spores can survive extreme conditions, including harsh radiation, dryness and cleaning procedures. This does not mean that aspergillosis patients need to worry about “space fungi”. Instead, it highlights something patients and specialists already understand very well: fungi are extraordinarily resilient organisms.
Aspergillus spores are common in the environment. They can be found in soil, compost, decaying leaves, dust, damp buildings and sometimes even very clean environments. Most people breathe in small numbers of spores every day without becoming ill, because their lungs and immune system clear them effectively.
For people with lung disease, asthma, immune system problems or damaged lung tissue, however, Aspergillus can sometimes cause illness. This includes conditions such as chronic pulmonary aspergillosis, allergic bronchopulmonary aspergillosis and severe asthma with fungal sensitisation.
A positive message for patients
One positive message from this research is that aspergillosis is not caused by weakness, poor hygiene or personal failure. Fungi are genuinely formidable organisms. If some fungal spores can survive environments as extreme as those used in space research, it becomes easier to understand why completely avoiding Aspergillus in everyday life is difficult.
This can be reassuring for patients who feel frustrated when symptoms persist despite doing “everything right”. It is not that they are failing. It is that fungal biology is complex, and fungal exposure is part of the natural world.
Why this matters emotionally
Many people with aspergillosis say they feel misunderstood. They may hear comments such as:
- “It’s only mould.”
- “Surely it should have cleared by now.”
- “Why are you still worrying about it?”
Stories like this help show that fungi are not simple or trivial. They are ancient, adaptable and scientifically fascinating organisms. Aspergillosis is therefore not “just mould exposure”; it is a real medical condition involving a complex interaction between the fungus, the lungs and the immune system.
Science is taking fungi more seriously
Another encouraging message is that fungi are attracting more scientific attention. Researchers are studying fungal survival, environmental spread, resistance to treatment, and the ways fungi interact with humans and indoor environments.
This matters because better understanding can lead to better diagnosis, better treatment and better prevention. In recent years, fungal medicine has already benefited from improvements in CT scanning, fungal blood tests, respiratory samples, antifungal treatments and biologic medicines for some allergic forms of disease.
Resilience goes both ways
The story also offers a useful reflection: fungi are resilient, but so are patients.
Many people living with aspergillosis adapt to long-term symptoms, hospital appointments, uncertainty, fatigue and treatment decisions. They continue to work, care for families, attend support groups, learn about their condition and help others understand fungal disease.
That resilience deserves recognition.
What patients can take from this
- Aspergillus is difficult to avoid completely, so exposure reduction should be realistic rather than perfectionist.
- Persistent symptoms are not a personal failure; fungal diseases can be complex and long-lasting.
- Fungal science is advancing, and aspergillosis is increasingly recognised as an important medical condition.
- Patients’ experiences are valid, even when others do not fully understand them.
When to seek medical advice
People with aspergillosis or suspected aspergillosis should seek medical advice if they develop worsening breathlessness, coughing up blood, unexplained weight loss, persistent fever, chest pain, a major change in sputum, or a significant deterioration in day-to-day symptoms.
Anyone already under specialist care should follow their agreed care plan and contact their clinical team if symptoms change significantly.
Further reading
- Smithsonian Magazine: fungus surviving spacecraft sterilisation conditions
- Aspergillosis.org: patient information and support
Last reviewed: May 2026
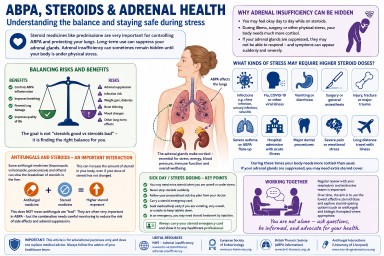
Understanding Steroids, Cortisol, ACTH and Adrenal Suppression in Aspergillosis
For people with Allergic Bronchopulmonary Aspergillosis (ABPA), severe asthma and other forms of aspergillosis, steroid treatment can be both extremely helpful and medically complicated.
Many patients are prescribed corticosteroids such as prednisolone or methylprednisolone to control inflammation, improve breathing and reduce the risk of lung damage. These medicines can be very effective. However, repeated or long-term steroid treatment can also affect the body’s natural hormone system, especially the adrenal glands.
Some patients are told:
- “Your cortisol is low.”
- “Your ACTH level is abnormal.”
- “You may have adrenal suppression.”
- “This may be steroid withdrawal.”
- “The blood tests are difficult to interpret.”
This can be worrying and confusing, especially when symptoms are severe but the explanation is not straightforward.
This article explains why adrenal problems can occur in some people with aspergillosis and severe asthma, why blood tests such as cortisol and ACTH can be difficult to interpret, and why steroid treatment sometimes involves a careful balance between benefit and risk.
Key points summary
- Steroid medicines can reduce the body’s own natural cortisol production.
- This is called adrenal suppression or adrenal insufficiency.
- Symptoms may overlap with aspergillosis, asthma, infection, fatigue or steroid withdrawal.
- Blood tests such as cortisol and ACTH can be difficult to interpret.
- Inhaled steroids and antifungal medicines can also influence steroid effects.
- Long-term prednisolone is generally avoided where possible, but it may still be necessary for some patients.
- Patients should not stop or reduce steroids suddenly without medical advice.
- Severe symptoms such as collapse, vomiting, dehydration, confusion or severe weakness require urgent medical advice.
Contents
- What do the adrenal glands do?
- What are cortisol and ACTH?
- Why are steroids used in ABPA and aspergillosis?
- Are steroids only meant for short-term use?
- How steroids affect the body’s natural hormone system
- What is adrenal suppression?
- Why symptoms can be difficult to recognise
- Why blood tests can become confusing
- The role of inhaled steroids
- Antifungal medicines and steroid interactions
- Steroid withdrawal versus adrenal insufficiency
- What kinds of stress may require higher steroid doses?
- When should patients seek urgent medical advice?
- Frequently asked questions
- Final thoughts
What do the adrenal glands do?
The adrenal glands are small glands that sit above the kidneys. They produce several important hormones, including cortisol.
Cortisol helps the body:
- respond to stress,
- maintain blood pressure,
- regulate energy levels,
- support immune function,
- and cope with illness or infection.
The body carefully controls cortisol levels through a hormone signalling system involving the brain, the pituitary gland and the adrenal glands.
What are cortisol and ACTH?
ACTH stands for adrenocorticotropic hormone.
The pituitary gland in the brain releases ACTH to tell the adrenal glands to produce cortisol.
This system normally works as a feedback loop:
- When cortisol is low, ACTH usually rises.
- When cortisol is high, ACTH usually falls.
Cortisol levels naturally change during the day and are usually highest in the early morning. This is one reason why many cortisol blood tests are taken around 9am.
Why are steroids used in ABPA and aspergillosis?
In Allergic Bronchopulmonary Aspergillosis (ABPA) and some severe asthma conditions, the immune system reacts strongly to Aspergillus fungi.
This can cause:
- airway inflammation,
- wheezing,
- coughing,
- mucus plugging,
- breathlessness,
- worsening lung function,
- and repeated flare-ups.
Steroids such as prednisolone are often used because they reduce inflammation quickly and effectively.
Some patients may need:
- short courses during flare-ups,
- repeated courses,
- long-term low-dose treatment,
- inhaled steroid therapy,
- antifungal treatment,
- or biologic medicines to reduce the need for oral steroids.
For many patients, steroids are not optional or casual medicines. They may be essential treatments used to control serious inflammation and protect lung function.
Are steroids only meant for short-term use?
Patients sometimes hear that prednisolone was “only designed for short-term use”. This is understandable, because modern medical practice tries to avoid long-term steroid treatment where possible.
Long-term oral corticosteroids can cause significant side effects, including:
- adrenal suppression,
- diabetes or worsening blood sugar control,
- osteoporosis and fracture risk,
- increased infection risk,
- cataracts or glaucoma,
- muscle weakness,
- skin thinning and bruising,
- weight gain,
- sleep disturbance,
- and mood or mental health effects.
For this reason, doctors usually aim to use steroids at the lowest effective dose for the shortest safe time.
However, it is also important not to oversimplify this message. Some people with ABPA, severe asthma or other inflammatory lung conditions do need longer-term steroid treatment because the disease itself can be dangerous if not controlled.
In some patients, the risk of uncontrolled lung inflammation may outweigh the risks of steroid treatment, at least for a period of time.
Modern care increasingly tries to reduce steroid exposure by using other approaches where appropriate, such as:
- antifungal treatment,
- biologic medicines for severe asthma or ABPA-type inflammation,
- careful monitoring of lung function and blood tests,
- gradual steroid tapering,
- bone protection where needed,
- diabetes monitoring,
- and regular review of whether the steroid dose can be reduced.
The key message is not that patients have done anything wrong by needing steroids. The key message is that long-term steroid treatment deserves careful monitoring, honest discussion and regular review.
Patient reassurance: If you have needed prednisolone for ABPA or severe asthma, this does not mean you have failed or made a poor choice. It usually means your medical team has been trying to control a potentially serious inflammatory condition. The aim is to balance benefit and risk as safely as possible.
Balancing risks and benefits
One of the hardest parts of long-term steroid treatment is that two important things can be true at the same time:
- steroids can cause serious side effects,
- and steroids can also prevent serious lung damage and dangerous flare-ups.
Patients sometimes feel guilty, frustrated or frightened when they hear about the risks of prednisolone. Others may feel judged for “still being on steroids”.
However, many people with ABPA or severe asthma did not choose steroids lightly. Steroids are often prescribed because uncontrolled inflammation itself can damage the lungs, worsen bronchiectasis, increase hospital admissions and significantly reduce quality of life.
Modern respiratory care increasingly tries to reduce steroid exposure where possible using:
- antifungal therapy,
- biologic medicines,
- careful monitoring,
- gradual tapering plans,
- and better recognition of steroid side effects.
But for some patients, steroids may still remain an important part of treatment, even if the goal is eventually to reduce the dose.
The most helpful approach is usually not “steroids are good” or “steroids are bad”, but rather:
- What dose is truly needed?
- Can the dose be safely reduced?
- Are side effects being monitored properly?
- Are there alternative treatments available?
- And is the patient being listened to when symptoms change?
This balanced approach is increasingly recognised as one of the most important parts of caring for people with severe asthma and aspergillosis.
How steroids affect the body’s natural hormone system
Steroid medicines act in ways that are similar to natural cortisol.
When the body senses steroid medication in the bloodstream, it may reduce its own ACTH production. Over time, this can mean:
- ACTH falls,
- the adrenal glands become less active,
- and natural cortisol production decreases.
Doctors sometimes describe this as the adrenal glands “going to sleep”.
This is called:
- adrenal suppression,
- steroid-induced adrenal insufficiency,
- or hypothalamic-pituitary-adrenal axis suppression.
What is adrenal suppression?
Adrenal suppression means the body may not produce enough cortisol when it is needed.
This can become especially important during:
- infection,
- surgery,
- injury,
- severe stress,
- or rapid steroid reduction.
Some patients develop symptoms gradually. Others notice problems when trying to reduce steroid doses.
Because cortisol is part of the body’s stress response, people with adrenal insufficiency may need specific medical advice about what to do during illness, vomiting, surgery or severe infection.
Why symptoms can be difficult to recognise
Symptoms of adrenal suppression can overlap with many other conditions common in people with aspergillosis, ABPA or severe asthma.
Possible symptoms include:
- profound tiredness,
- weakness,
- dizziness,
- sweating,
- shakiness,
- nausea,
- muscle aches,
- low mood,
- brain fog,
- reduced exercise tolerance,
- poor recovery after illness,
- or feeling suddenly much worse after reducing steroids.
These symptoms may also occur with:
- an ABPA flare,
- asthma worsening,
- lung infection,
- chronic illness,
- poor sleep,
- anxiety,
- or steroid withdrawal.
This overlap is one reason why patients can feel frustrated or uncertain. Symptoms are real, even when the cause is difficult to pin down.
Why blood tests can become confusing
Many patients expect blood tests to give clear answers, but cortisol and ACTH results are often complicated.
Several things can affect results:
- time of day,
- recent steroid use,
- the type of steroid used,
- inhaled steroid dose,
- recent dose reductions,
- illness or stress,
- laboratory methods,
- and antifungal medicines.
Typical patterns
In classic steroid-induced adrenal suppression:
- cortisol is low,
- and ACTH is low or “inappropriately normal”.
This happens because steroid medication suppresses ACTH production.
However, real-life cases are not always straightforward. Some patients may have recently reduced steroids, missed doses, changed steroid type, used high-dose inhaled steroids, or taken antifungal medicines that alter steroid metabolism.
In some situations, endocrinologists may need repeated testing or dynamic tests such as a Synacthen test to understand whether the adrenal glands can respond properly.
It is important that patients do not try to interpret cortisol or ACTH results in isolation. The result needs to be understood alongside symptoms, medication history, timing of the sample and the clinical situation.
The role of inhaled steroids
Many people assume inhaled steroids only affect the lungs.
Inhaled steroids usually have fewer whole-body effects than long-term oral steroids, but high doses can sometimes contribute to adrenal suppression, especially when combined with:
- long-term or repeated oral steroid courses,
- azole antifungal medicines,
- other medicines that affect steroid metabolism,
- or individual differences in how medicines are processed.
This does not mean inhaled steroids are unsafe or should be stopped suddenly. For many people with asthma or ABPA, inhaled steroids are an important part of keeping airway inflammation under control.
It does mean that total steroid exposure should be reviewed carefully, especially in patients with symptoms suggestive of adrenal suppression.
Antifungal medicines and steroid interactions
This is an especially important issue in aspergillosis.
Antifungal medicines such as:
- itraconazole,
- voriconazole,
- posaconazole,
- and isavuconazole
can interact with other medicines, including corticosteroids.
Some azole antifungals slow the breakdown of steroids in the liver. This can increase the body’s exposure to steroid medication, meaning that even doses which initially appear moderate may sometimes behave more like higher doses inside the body.
This interaction may increase the risk of:
- adrenal suppression,
- Cushing-like side effects,
- weight gain,
- skin thinning,
- easy bruising,
- high blood sugar,
- muscle weakness,
- or hormonal imbalance.
The interaction can be particularly important in patients taking:
- oral prednisolone or methylprednisolone,
- high-dose inhaled steroids,
- multiple steroid preparations together,
- or repeated steroid courses over time.
Some patients tolerate steroid treatment reasonably well for long periods before antifungal medicines are added. Endocrine problems may then become more noticeable later, especially during:
- infection,
- surgery,
- vomiting or diarrhoea,
- major physical stress,
- rapid steroid reduction,
- or severe asthma or ABPA flare-ups.
This can feel as though adrenal insufficiency has appeared “suddenly” or “out of nowhere”, when in reality the adrenal glands may have been partially suppressed for some time.
Why adrenal insufficiency may only become obvious during illness or stress
Some patients with steroid-related adrenal suppression cope reasonably well during normal day-to-day life, especially while still taking regular steroids. However, the problem may become much more noticeable when the body faces significant physical stress.
Under normal circumstances, the body rapidly increases cortisol production during severe illness or injury. If the adrenal glands cannot respond properly, symptoms may suddenly become much more severe.
Patients sometimes describe:
- “crashing” during an infection,
- extreme exhaustion,
- severe weakness,
- dizziness or collapse,
- poor recovery after illness,
- or feeling suddenly unable to cope physically.
This does not mean every severe illness in an ABPA patient is caused by adrenal insufficiency. Infections, inflammation and lung disease themselves are often the major problem. However, adrenal suppression can sometimes contribute to deterioration and may only reveal itself during periods of stress or acute illness.
This is one reason why some patients are given “sick day rules”, emergency steroid cards or advice about temporary steroid dose increases during illness.
Importantly, this does not mean antifungal medicines are “bad” or should be avoided. In many patients, antifungal treatment significantly improves ABPA control and may eventually help reduce steroid exposure overall. The important message is that these combinations require awareness, monitoring and careful medical supervision.
Patients should never stop antifungal or steroid medicines suddenly without medical advice.
Steroid withdrawal versus adrenal insufficiency
Steroid withdrawal and adrenal insufficiency can feel very similar.
Steroid withdrawal
When steroid doses are reduced, the body may take time to adjust. Patients can temporarily feel unwell even if the adrenal glands are slowly recovering.
Adrenal insufficiency
Adrenal insufficiency means the body cannot produce enough cortisol to meet its needs.
Symptoms may overlap considerably. Recovery can sometimes take weeks or months, and in some patients longer.
For many patients, one of the hardest parts is that they may “look well” externally while feeling exhausted internally.
It is important that symptoms are not dismissed simply because they are difficult to measure.
What kinds of stress may require higher steroid doses?
Patients who have adrenal insufficiency or significant adrenal suppression may sometimes be advised to temporarily increase steroid doses during periods of physical stress. This is often called following “sick day rules”.
The body normally produces extra cortisol during stress, illness or injury. If the adrenal glands cannot respond properly, extra steroid medication may sometimes be needed to prevent serious illness.
Examples of situations that may place significant stress on the body include:
- high fever or significant infection,
- chest infection or pneumonia,
- vomiting or diarrhoea,
- COVID-19 or influenza,
- major dental treatment or surgery,
- fractures or significant injury,
- general anaesthetic procedures,
- severe asthma attacks or ABPA flare-ups,
- hospital admission with acute illness,
- or severe physical exhaustion associated with illness.
The exact advice varies between patients depending on:
- whether adrenal insufficiency has been formally diagnosed,
- the steroid dose currently being taken,
- how suppressed the adrenal glands are thought to be,
- other medical conditions,
- and guidance from endocrine or respiratory specialists.
Some patients are provided with:
- specific “sick day rules”,
- an emergency steroid card,
- medical alert jewellery,
- or emergency hydrocortisone injection kits.
Patients should only adjust steroid doses according to the advice provided by their medical team. If severe vomiting, collapse, confusion, inability to keep medication down or major deterioration occurs, urgent medical advice is needed.
When should patients seek urgent medical advice?
Patients should seek urgent medical help if they experience:
- collapse,
- fainting,
- severe vomiting,
- inability to keep steroid medication down,
- severe dehydration,
- confusion,
- severe weakness,
- very low blood pressure,
- or sudden major deterioration during illness.
These symptoms can occasionally indicate adrenal crisis, which is a medical emergency.
Patients who have been told they are at risk of adrenal insufficiency should follow the emergency and “sick day” advice given by their endocrine or respiratory team.
Frequently asked questions
Does everyone taking steroids develop adrenal suppression?
No. Risk depends on factors such as dose, duration, repeated courses, inhaled steroid dose, other medicines and individual sensitivity.
Can adrenal function recover?
Yes. Many patients gradually recover adrenal function over time, although recovery speed varies.
Are inhaled steroids safer than tablets?
Inhaled steroids usually have fewer whole-body effects than long-term oral steroids, but high doses can still contribute to adrenal suppression in some patients, especially when combined with certain antifungal medicines.
Why do I feel worse when reducing steroids?
This can happen for several reasons. The underlying lung disease may flare, the body may be adjusting to lower steroid levels, or cortisol production may not yet have recovered.
Does needing long-term prednisolone mean something has gone wrong?
Not necessarily. Long-term prednisolone is usually avoided where possible because of side effects, but some patients need it to control serious inflammation. The aim is regular review, careful monitoring and dose reduction when it is safe.
Should I stop steroids because of this risk?
No patient should stop prescribed steroids suddenly unless specifically advised by their medical team. Sudden withdrawal can be dangerous, especially if the body’s own cortisol production is suppressed.
Final thoughts
Adrenal suppression and steroid-related hormone problems are recognised complications of corticosteroid treatment.
For patients with aspergillosis, ABPA and severe asthma, the situation can become especially complex because:
- steroid treatment may be medically necessary,
- symptoms overlap with many other conditions,
- antifungal medicines may interact with steroids,
- inhaled steroids may add to total steroid exposure,
- and blood tests are not always straightforward.
Patients sometimes feel frustrated because their symptoms are difficult to explain or measure clearly. However, these experiences are recognised by clinicians and researchers, and steroid-related adrenal problems are increasingly acknowledged as important and sometimes under-recognised.
The goal is not to create fear of steroids. The goal is to use them carefully, monitor them properly, reduce them when possible, and support patients through the difficult process of balancing disease control with treatment side effects.
Suggested internal links
- ABPA treatment overview
- Steroid side effects
- Antifungal drug interactions
- Fatigue and aspergillosis
- Severe asthma and biologics
- Living with long-term aspergillosis
- Mental wellbeing and chronic illness
- Aspergillosis.org Knowledge Hub
References and further reading
When was this article last reviewed?
Last reviewed: May 2026
Author and review information
Prepared for patient education and support purposes.
This article is intended for general educational use and should not replace personalised medical advice from a healthcare professional.
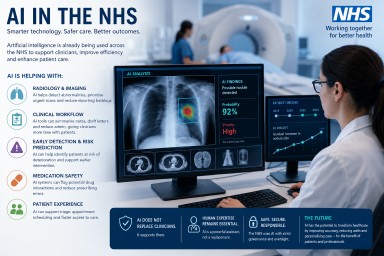
Artificial Intelligence (AI) in the NHS: Promise, Progress and the Future of Healthcare
Artificial intelligence (AI) is no longer a futuristic idea within the NHS. AI technologies are already being used in some areas of healthcare across the UK, particularly in radiology, diagnostics, administration and workflow support. However, the reality is more nuanced than many headlines suggest.
At present, AI in the NHS is best understood as a collection of promising technologies being introduced gradually, cautiously and under clinical oversight. Some NHS trusts are using several AI-assisted systems routinely, while others have little or no operational AI deployment beyond pilot projects.
The direction of travel is clear: AI is likely to become an increasingly important part of healthcare over the next decade. However, the NHS is moving carefully because healthcare is a high-risk environment where mistakes can have serious consequences.
What Does AI Mean in Healthcare?
In healthcare, AI usually refers to computer systems that can analyse large amounts of data and identify patterns more quickly or consistently than humans alone.
Examples include:
- Analysing medical scans
- Helping detect cancers or fractures
- Supporting diagnosis
- Summarising clinic consultations
- Reducing paperwork
- Predicting patient deterioration
- Helping prioritise urgent cases
- Supporting medication safety checks
Importantly, most NHS AI systems are currently designed to support clinicians rather than replace them.
AI in NHS Radiology
Radiology is currently one of the biggest areas of AI development within the NHS.
AI systems are being used or trialled to help analyse:
- Chest X-rays
- CT scans
- MRI scans
- Mammograms
- Retinal photographs
- Dermatology images
AI is particularly attractive in radiology because the NHS faces:
- Large radiologist shortages
- Increasing imaging demand
- Growing reporting backlogs
- Rising complexity of scans
How AI Is Currently Used
Most NHS radiology AI systems currently operate in one of three ways:
1. AI as a “Second Reader”
The scan is interpreted by a radiologist, while AI acts as an additional safety check.
AI may flag:
- Possible lung nodules
- Fractures
- Brain bleeds
- Abnormal mammograms
- Signs of stroke
The human clinician still makes the final decision.
2. Prioritisation (“Triage”)
AI can rapidly review scans and move potentially urgent cases higher in the reporting queue.
This may help speed up treatment for:
- Stroke
- Pulmonary embolism
- Pneumothorax (collapsed lung)
- Intracranial bleeding
3. Identifying Likely Normal Scans
Some AI systems are being studied to identify scans that appear very likely to be normal.
The aim is to allow radiologists to focus more attention on:
- Abnormal scans
- Complex cases
- Uncertain findings
However, this remains an area of careful evaluation and regulation.
Does AI Sometimes Perform Better Than Humans?
In certain narrow and repetitive tasks, AI can sometimes outperform humans or help reduce specific types of errors.
AI can be very good at:
- Detecting tiny abnormalities
- Maintaining consistency
- Working without fatigue
- Rapid image analysis
- Comparing huge numbers of images
Humans can become:
- Tired
- Distracted
- Overloaded
- Inconsistent under pressure
For example, AI may detect very small lung nodules or subtle fractures that could potentially be overlooked during a busy reporting session.
However, AI also has important weaknesses.
AI may struggle with:
- Rare diseases
- Complex clinical context
- Unusual anatomy
- Poor-quality scans
- Unexpected combinations of disease
Importantly, AI and humans often make different kinds of mistakes.
The emerging evidence suggests that:
Human + AI is often better than either alone.
Will Radiologists Be Replaced?
At present, the NHS does not view AI as a replacement for radiologists.
Instead, AI is mainly being introduced as:
- A support tool
- A safety net
- A prioritisation system
- A workflow assistant
Radiologists still provide:
- Clinical judgement
- Contextual interpretation
- Decision-making
- Communication
- Management of uncertainty
In the foreseeable future, radiology is likely to become increasingly AI-assisted but still human-led.
Longitudinal Analysis: One of the Most Exciting Future Possibilities
One of the most promising future applications of AI is longitudinal analysis.
This means comparing:
- Current scans
- Previous scans
- Blood tests
- Lung function
- Medications
- Clinical notes
- Symptoms
- Outcomes over time
Humans are not particularly good at consistently recognising very subtle changes across years of imaging and clinical data.
AI could potentially become extremely powerful at:
- Tracking disease progression
- Measuring tumour growth
- Monitoring fibrosis
- Quantifying cavity enlargement
- Identifying treatment response
- Predicting future deterioration
This could be especially valuable in chronic diseases such as:
- Chronic Pulmonary Aspergillosis (CPA)
- Bronchiectasis
- Chronic Obstructive Pulmonary Disease (COPD)
- Interstitial lung disease
- Cancer
In the future, AI may help move medicine from:
“What does this scan show today?”
towards:
“What is happening over time, and what is likely to happen next?”
AI Beyond Radiology
AI Clinical Documentation
The NHS is increasingly exploring AI systems that can generate:
- Clinic letters
- Consultation summaries
- Medical notes
- Coding suggestions
These “AI scribes” may help reduce administrative burden and allow clinicians to spend more time with patients.
AI Triage Systems
Some NHS services now use AI-assisted triage systems to:
- Route patient requests
- Identify urgent problems
- Prioritise appointments
- Support NHS App workflows
Medication Safety
AI may eventually help identify:
- Drug interactions
- Prescribing errors
- Missed monitoring
- Unsafe medication combinations
Operational Efficiency
The NHS is also exploring AI for:
- Appointment scheduling
- Referral management
- Staff rostering
- Reducing missed appointments
- Managing workflow
Why AI Adoption Is Uneven Across the NHS
AI adoption currently varies considerably across the NHS.
Some trusts use multiple AI systems routinely, while others have minimal deployment.
This variation is influenced by:
- Funding differences
- IT infrastructure
- Digital maturity
- Research partnerships
- Clinical confidence
- Procurement complexity
- Availability of evidence
Large teaching hospitals and academic centres often adopt new technologies earlier than smaller hospitals.
As a result, current NHS AI deployment is best described as:
Selective, cautious and evolving.
Why the NHS Is Proceeding Carefully
The NHS is naturally cautious about AI because healthcare is fundamentally different from many other industries.
Mistakes can have serious consequences, including:
- Missed cancers
- Delayed diagnosis
- Medication harm
- Unsafe treatment decisions
For this reason, NHS AI systems generally require:
- Clinical validation
- Governance review
- Safety monitoring
- Regulatory approval
- Human oversight
- Ongoing audit
There is also awareness that:
- commercial hype can exceed evidence,
- real-world NHS workflows are complex,
- and some AI systems may not perform as well outside carefully controlled studies.
Potential Risks and Concerns
Although AI has enormous potential, there are also important concerns.
Patient Safety
AI systems can make mistakes and may occasionally be confidently wrong.
Bias
If training data is incomplete or biased, AI performance may vary between different patient groups.
Loss of Human Contact
Some patients worry that healthcare could become less personal if technology replaces human interaction.
Data Privacy
AI systems often require access to large healthcare datasets, raising understandable questions about confidentiality and data governance.
The Likely Future
The most likely future is probably not:
“AI replaces doctors.”
Instead, it is more likely to be:
“Clinicians increasingly work alongside AI systems.”
AI may gradually become another routine layer of healthcare infrastructure, much as:
- electronic patient records,
- CT scanners,
- MRI scanners,
- and digital pathology systems
became normal parts of modern medicine.
Over time, patients may benefit from:
- Earlier diagnosis
- Safer systems
- More personalised medicine
- Faster reporting
- Reduced waiting times
- Better chronic disease monitoring
However, successful implementation will depend heavily on:
- careful governance,
- good evidence,
- clinical oversight,
- public trust,
- and maintaining the human side of healthcare.
A Balanced Summary
AI in the NHS is already real, but still at an early stage of adoption.
Current use is best described as:
Promising applications in partial use, being introduced gradually and carefully while safety, effectiveness and governance continue to be evaluated.
The NHS is unlikely to move recklessly because healthcare carries high stakes. Instead, adoption will probably continue incrementally, with evidence and clinical confidence building over time.
If implemented wisely, AI has the potential to become one of the most important developments in modern healthcare — not by replacing clinicians, but by helping them deliver safer, faster and more personalised care.
Useful Resources and Further Reading
- NHS England: Artificial Intelligence and Machine Learning
- NHS AI Lab
- NHS AI Knowledge Repository
- NICE: Evidence Standards Framework for Digital Health Technologies
- UK Government: AI Opportunities Action Plan
- Royal College of Radiologists: Artificial Intelligence
- British Institute of Radiology: Artificial Intelligence Special Interest Group
- The Health Foundation: How Could AI Improve the NHS?
- The King’s Fund: Artificial Intelligence and the NHS
- Nature: Artificial Intelligence in Healthcare Collection
- The Lancet Digital Health
Living With Aspergillosis: When Others Do Not Fully Understand How You Feel

Living with aspergillosis can affect far more than the lungs. Many patients have symptoms that are difficult to explain, difficult to measure, and difficult for other people to fully understand.
Breathlessness, fatigue, coughing, chest tightness, sleep disruption, anxiety during flare-ups, medication side effects, and uncertainty about the future can all become part of daily life. These symptoms may fluctuate from day to day, and people may appear well at times even when they are struggling.
This can leave patients feeling misunderstood, dismissed, or even blamed for focusing too much on their health.
Key points
- Symptoms of aspergillosis and chronic lung disease are real, even when they are invisible to others.
- Feeling anxious, frustrated, or preoccupied with health is understandable when symptoms affect daily life.
- Validation from family, friends, and clinicians can reduce distress.
- Finding meaningful things to do beyond illness can also help patients cope.
- The aim is balance: being heard and supported, while also protecting quality of life.
Why aspergillosis can be hard for others to understand
Many people with chronic pulmonary aspergillosis (CPA), allergic bronchopulmonary aspergillosis (ABPA), severe asthma, bronchiectasis, or other long-term lung conditions live with symptoms that are not always visible.
A patient may look well, speak normally, or have reasonable oxygen levels at rest, but still experience severe fatigue, breathlessness on exertion, anxiety during breathing difficulty, or a long recovery after simple activities.
Symptoms may also fluctuate. Someone may manage an activity one day but be unable to do the same thing the next. This inconsistency can be confusing for family, friends, employers, and sometimes even healthcare professionals.
“Stop obsessing” is usually not helpful
Patients with chronic illness are sometimes told to “stop obsessing” about their health. This may be said with good intentions, but it can feel dismissive.
Patients may hear:
“You are making too much of this.”
or:
“It is all in your head.”
In reality, many patients are not choosing to focus on illness. The illness is already demanding attention through symptoms, medication routines, appointments, uncertainty, and changes to daily life.
However, there is also a useful point hidden inside the poor wording. Constantly monitoring every symptom can become exhausting and may increase anxiety. The better message is not “stop obsessing”, but:
“Your symptoms are real, but you also deserve space in your life that is not only about illness.”
Validation matters
Validation means recognising that a person’s experience is real and understandable. It does not mean agreeing that every symptom is dangerous, or that every worry needs urgent medical action.
Useful validating phrases include:
- “I believe you.”
- “That sounds exhausting.”
- “I know this affects much more than people can see.”
- “How is today compared with your usual baseline?”
- “What would help you most today?”
Validation can reduce distress. When patients feel dismissed, they may feel driven to repeat themselves, seek reassurance, or prove how unwell they are. When they feel heard, they may find it easier to step back from constant symptom monitoring and focus on other parts of life.
The mind and body interact
Breathlessness is not just a physical sensation. It can trigger fear very quickly. This is a normal human response: breathing difficulty naturally makes the brain more alert to danger.
This does not mean symptoms are imaginary. It means chronic respiratory illness affects the whole person: physically, emotionally, socially, and psychologically.
Anxiety, uncertainty, poor sleep, and repeated flare-ups can all increase awareness of symptoms. At the same time, genuine physical symptoms can increase anxiety. The two can reinforce each other.
Recognising this interaction can help patients and clinicians work together without blame.
Finding something else to think about can help
For many patients, finding meaningful activities beyond illness is genuinely helpful. This might include hobbies, gentle exercise, time outdoors, music, crafts, reading, gardening, photography, volunteering, family activities, or peer support.
This is not the same as ignoring illness. It is a way of protecting identity and quality of life.
The aim is not to deny symptoms, but to prevent illness becoming the only focus of every day.
“Your illness is real, but it should not be allowed to take over every part of who you are.”
What families and friends can do
Family members and friends may not be able to fully understand what chronic aspergillosis feels like. They do not need perfect understanding to be supportive.
Helpful support includes:
- believing the person’s symptoms are real;
- recognising that fatigue and breathlessness may not be visible;
- avoiding dismissive comments;
- asking what would help rather than assuming;
- understanding that symptoms may fluctuate;
- encouraging enjoyable activities without pressuring the person to “push through”.
Less helpful comments include:
- “You look fine.”
- “You were able to do it yesterday.”
- “You need to stop thinking about it.”
- “Everyone gets tired.”
What clinicians may be trying to say
Sometimes clinicians may say things such as “try not to focus on it too much” because they believe further tests or treatments may not currently help. They may be trying to avoid unnecessary antibiotics, steroids, scans, or procedures.
That can be a reasonable clinical concern, but the message needs to be communicated carefully.
A better way to say it might be:
“I believe your symptoms are real and distressing. We will continue to look for changes that need treatment. At the same time, some symptoms may persist despite treatment, so we also need to support your quality of life.”
This keeps the patient heard, while also being honest about the limits of medical treatment.
Practical ways to find balance
- Use structured symptom tracking: a brief daily note may be more helpful than constant checking.
- Know your baseline: understanding what is normal for you makes changes easier to spot.
- Agree an action plan: ask your healthcare team what changes should prompt medical advice.
- Protect non-illness time: plan small, realistic activities that are not centred on health.
- Use peer support carefully: support groups can reduce isolation, but try to avoid constant comparison or fear-based searching.
- Ask for emotional support: counselling, psychological therapies, pulmonary rehabilitation, or breathing physiotherapy may help some people.
When to seek medical advice
This article is general information and does not replace medical advice. Patients should seek medical help if they experience significant or worrying change, especially:
- worsening breathlessness;
- falling oxygen saturations if they monitor them;
- new or worsening chest pain;
- coughing up blood;
- high fever, rigors, or signs of serious infection;
- new confusion, fainting, or severe weakness;
- rapid deterioration from their usual baseline;
- symptoms that feel different from their usual pattern.
If symptoms are severe or rapidly worsening, urgent medical help should be sought.
Final thought
Living with aspergillosis can be physically and emotionally demanding. Patients deserve to be believed, heard, and supported. At the same time, they also deserve help to build a life that is not entirely defined by illness.
A helpful message for patients, families, and clinicians is:
“Your illness is real. Your distress is understandable. You deserve support. And you also deserve a life with meaning, connection, and moments of relief beyond illness.”
Further support and reading
If you are living with aspergillosis and feel that others do not fully understand what you are going through, these resources may help. They offer information about long-term illness, mental wellbeing, breathlessness, invisible symptoms, and patient support.
- Aspergillosis patient support
Information about support meetings, patient resources, and ways to connect with others affected by aspergillosis. - NHS Talking Therapies
NHS support for people experiencing anxiety, depression, or emotional distress, including people living with long-term health conditions. - Asthma + Lung UK: Living with a lung condition
Practical information on living with breathlessness, fatigue, flare-ups, and the emotional effects of lung disease. - Chronic Illness Inclusion
A UK organisation focused on the experiences of people living with chronic, energy-limiting, and often invisible conditions. - The Patients Association: Long-term conditions
Advice and information for people managing long-term health conditions and navigating healthcare conversations.
Important: If your symptoms suddenly worsen, you develop severe breathlessness, chest pain, coughing up blood, confusion, fainting, or signs of serious infection, seek urgent medical advice. In the UK, call NHS 111 for urgent advice or 999 in an emergency.
European Lung Foundation (ELF): Giving Patients a Voice in Respiratory Health

What makes ELF particularly valuable is that it is genuinely patient-led. Patients and carers are not simply consulted occasionally; they actively help shape educational resources, awareness campaigns, research priorities and clinical guideline discussions.
ELF and Aspergillosis
One particularly important area of ELF’s work is its commitment to supporting people affected by aspergillosis and other fungal lung diseases.
The ELF Aspergillosis Information Hub provides accessible, reliable information about:
- ABPA (Allergic Bronchopulmonary Aspergillosis)
- CPA (Chronic Pulmonary Aspergillosis)
- Aspergilloma
- Invasive aspergillosis
- Symptoms and diagnosis
- Treatment approaches
- Living with long-term fungal disease
- Patient experiences and support
The ELF Aspergillosis Patient Advisory Group
ELF has also established a dedicated Aspergillosis Patient Advisory Group, bringing together people from across Europe with direct lived experience of aspergillosis.
The group works alongside clinicians and researchers to improve awareness, encourage earlier diagnosis, develop patient education, influence research priorities and support better long-term care.
Why Patient Participation Matters
Aspergillosis is still under-recognised in many countries, and many patients experience long delays before receiving a diagnosis. Patient involvement can help change this.
By sharing experiences, joining discussions and supporting awareness activities, patients and carers can help improve understanding of fungal lung disease, strengthen educational materials, support newly diagnosed patients and raise awareness among healthcare professionals and the public.
Not everyone needs to become a public speaker or campaigner. Participation can include joining online meetings, completing surveys, sharing experiences confidentially, reviewing patient information, supporting awareness campaigns online or helping identify what matters most to patients.
Ways to Get Involved
- Visit the ELF Aspergillosis Information Hub
- Learn about the ELF Aspergillosis Patient Advisory Group
- Explore the ELF Patient Organisation Network
- Support the Healthy Lungs for Life campaign
- Watch ELF videos on YouTube
A Shared Effort
ELF demonstrates that respiratory healthcare works best when patients, carers, clinicians and researchers work together as partners.
For people affected by aspergillosis, involvement in organisations like ELF can help transform personal experience into something that improves understanding, care and support for others across Europe and beyond.
Every patient story, question, survey response and conversation contributes to building greater awareness of aspergillosis and improving the future of care.
Smoking, COPD and Chronic Pulmonary Aspergillosis (CPA)
Many people diagnosed with Chronic Pulmonary Aspergillosis (CPA) also have Chronic Obstructive Pulmonary Disease (COPD). One of the strongest shared risk factors between the two conditions is cigarette smoking.
Smoking does not directly “cause” Aspergillus infection in the same way a virus or bacteria causes disease. However, it can create the lung damage and immune dysfunction that make CPA more likely to develop and harder to control.
Why smoking matters in CPA and COPD
Smoking damages the lungs over many years by:
- Destroying normal lung tissue and airways
- Causing chronic inflammation
- Reducing the lungs’ ability to clear mucus, dust and fungal spores
- Damaging the tiny hair-like structures called cilia that normally sweep organisms out of the airways
- Weakening local immune defence inside the lungs
- Increasing emphysema, cavities, scarring and bronchiectasis — all environments where Aspergillus can grow more easily
People breathe in Aspergillus spores every day. Healthy lungs usually remove them without difficulty. Damaged lungs are different. In COPD, especially severe COPD, spores can remain trapped in damaged airways and cavities, increasing the risk of long-term fungal colonisation or infection.
Is smoking causal?
The relationship is complex, but in many patients smoking is likely to be an important contributing cause.
Smoking contributes to:
- COPD development
- Structural lung damage
- Reduced immune clearance
- Increased infection risk
- Faster lung decline
All of these increase vulnerability to CPA.
Smoking is therefore not simply an associated factor. In many patients it is part of the chain of events that eventually leads to CPA developing.
Not every smoker develops CPA, and not every person with CPA has smoked. Some people develop CPA after tuberculosis, severe pneumonia, sarcoidosis, asthma, bronchiectasis, lung surgery or other lung diseases. However, smoking substantially increases risk because it accelerates lung injury and reduces the lungs’ resilience.
Why continuing to smoke after CPA diagnosis is dangerous
Once CPA is established, continuing to smoke can make management much harder.
Smoking may:
- Accelerate further lung destruction
- Worsen breathlessness and cough
- Increase mucus production
- Increase flare-ups and infections
- Reduce physical fitness and oxygen levels
- Reduce quality of life
- Increase hospital admissions
- Make COPD progression faster
- Increase risk of lung cancer alongside CPA
- Make recovery from infections slower
Many patients with CPA already have limited lung reserve. Continuing to smoke can progressively reduce the remaining healthy lung tissue.
“The damage is already done” — is stopping still worthwhile?
Yes. This is one of the commonest and most understandable feelings among long-term smokers with lung disease. However, stopping smoking can still help, even after significant lung damage has already occurred.
Within days to weeks
- Carbon monoxide levels fall
- Oxygen delivery improves
- Airways may become less irritated
- Some coughing and mucus clearance may improve
Within months
- COPD flare-ups may reduce
- Circulation improves
- Physical activity may become easier
- Inflammation begins to reduce
Over years
- Lung function decline slows
- Risk of heart disease and stroke falls
- Risk of lung cancer gradually decreases
- Survival improves compared with continued smoking
For people with CPA, preserving remaining lung function is critical. Slowing further structural damage may help stabilise disease, and antifungal treatment works best in lungs that are not being continually injured by smoke.
Is vaping a safer alternative?
Many patients ask whether vaping, or using e-cigarettes, is a safer option than smoking cigarettes.
Current evidence suggests that vaping is likely to be substantially less harmful than smoking tobacco cigarettes because vaping avoids the combustion process that produces tar, carbon monoxide and many toxic chemicals found in cigarette smoke.
For smokers who are unable to stop nicotine completely, switching entirely from smoking to vaping may reduce harm.
However, vaping is not risk-free.
Vaping aerosols can still irritate the lungs and may contain:
- Fine particles
- Flavouring chemicals
- Heating by-products
- Nicotine
- Other airway irritants
Some people with CPA, COPD, asthma or bronchiectasis report:
- Increased cough
- Throat irritation
- Chest tightness
- Wheeze
- Increased mucus symptoms
Long-term effects of vaping are still being studied.
For patients with CPA, the safest option for lung health is probably:
- Stop smoking cigarettes completely
- Use vaping only if it helps avoid returning to smoking
- Gradually reduce vaping if possible
A common problem is “dual use” — continuing to smoke while also vaping. This usually provides much less benefit than stopping cigarettes completely.
While nicotine itself is addictive, most of the major smoking-related lung damage comes from the toxic products created by burning tobacco.
For many patients, switching from smoking to vaping may still represent an important positive step if it helps them move away from cigarettes permanently.
Nicotine addiction is powerful
Many people with CPA and COPD have smoked for decades. Stopping is rarely simply a matter of willpower. Nicotine is strongly addictive, and smoking often becomes linked to stress relief, routine, anxiety management and social habits.
Patients should not feel ashamed if stopping is difficult. Repeated attempts are normal. Many successful quitters tried several times before succeeding permanently.
What can help?
Support works better than trying alone.
Options include:
- NHS stop smoking services
- Nicotine replacement therapy, such as patches, gum, sprays or lozenges
- Prescription medicines such as varenicline or cytisine, if suitable
- Behavioural support and counselling
- Gradual reduction plans
- Vape or e-cigarette transition strategies in selected patients
- Family and peer support
For many people with severe lung disease, stopping smoking is one of the most important treatments available — alongside inhalers, oxygen, physiotherapy and antifungal medication.
A realistic but important message
Patients with CPA often already live with fatigue, cough, breathlessness and anxiety about the future. Smoking may feel comforting in the short term, but it usually continues the cycle of lung injury that helped create the problem in the first place.
Stopping smoking cannot reverse established CPA, but it may:
- Slow further lung decline
- Improve day-to-day symptoms
- Improve response to treatment
- Preserve independence longer
- Reduce complications
- Improve long-term survival
Even small improvements in lung health can matter enormously when lung reserve is limited.
When to seek medical advice
Patients with CPA, COPD or other lung disease should seek medical advice if they:
- Become significantly more breathless
- Develop chest pain
- Cough up increasing amounts of blood
- Notice worsening wheeze or mucus production
- Develop fevers or signs of infection
- Feel unable to cope with smoking withdrawal symptoms alone
Stopping smoking is often difficult, but healthcare professionals can offer support and treatment options that improve the chances of success.