Weekly Aspergillosis Research Update April - May 2026
Search term: aspergillosis
Period covered: late April–early May 2026
Key highlights this week
- Diagnostics: new evidence for pentraxin-3 and airway galactomannan testing.
- Treatment: voriconazole dosing may be difficult during ECMO and needs close monitoring.
- Resistance: azole-resistant Aspergillus fumigatus detected around patient homes in Brazil.
- Transplant medicine: aspergillosis remains the dominant invasive mould infection after lung transplantation.
- Future therapies: early laboratory work identifies a possible new antifungal drug target.
1. New diagnostic marker: pentraxin-3 for invasive pulmonary aspergillosis
Sun C et al. Diagnostic value of pentraxin 3 in plasma and bronchoalveolar lavage fluid for invasive pulmonary aspergillosis in non-neutropenic patients: a prospective multicenter clinical study. Emerging Microbes & Infections, 2026.
View on PubMed – PMID: 42054395
This prospective multicentre study looked at pentraxin-3 in blood and bronchoalveolar lavage fluid as a diagnostic marker for invasive pulmonary aspergillosis in patients who are not neutropenic.
Why it matters: diagnosing invasive aspergillosis can be especially difficult in patients outside the classic high-risk groups. This study supports the wider move toward combining tests and biomarkers rather than relying on one result alone.
2. Galactomannan testing in tracheobronchial aspirates after lung transplant
Monforte A et al. Diagnostic value of galactomannan in tracheobronchial aspirate for Aspergillus infection in lung transplant recipients (the GALACTBAS study). Journal of Clinical Microbiology, 2026.
View on PubMed – PMID: 42059612
This study assessed whether galactomannan testing in tracheobronchial aspirates can help diagnose Aspergillus infection in lung transplant recipients.
Why it matters: aspergillosis after lung transplantation often involves the airways. Testing airway samples may support earlier diagnosis and may sometimes be less invasive than deeper lung sampling.
3. Voriconazole levels may vary during ECMO
Yusuff H et al. Time-varying voriconazole clearance during extracorporeal membrane oxygenation. Antimicrobial Agents and Chemotherapy, 2026.
View on PubMed – PMID: 42059809
This paper looked at voriconazole clearance in critically ill patients receiving extracorporeal membrane oxygenation (ECMO).
Why it matters: voriconazole is commonly used to treat invasive aspergillosis, but drug levels can be unpredictable in critical illness. This supports the importance of therapeutic drug monitoring so dosing can be adjusted safely and effectively.
4. Azole-resistant Aspergillus found around patient homes in Brazil
de Barros Rodrigues DK et al. Environmental circulation of Aspergillus fumigatus with reduced susceptibility to agricultural triazole in Brazil: clonal dissemination of potentially resistant genotypes. Mycoses, 2026.
View on PubMed – PMID: 42037564
This study investigated environmental Aspergillus fumigatus around the homes of two patients with suspected aspergillosis caused by resistant isolates.
Why it matters: the findings add to concern that antifungal resistance can arise and circulate in the environment, including through exposure to agricultural triazoles. This is important because azole resistance can make aspergillosis harder to treat.
5. Invasive mould infections after lung transplantation: aspergillosis dominates
Pennington KM et al. Impact of invasive mold infection-coded diagnoses on utilization, costs, and mortality after lung transplantation. Chest, 2026.
View on PubMed – PMID: 42061698
This study assessed invasive mould infection-coded diagnoses after lung transplantation. Aspergillosis was the most common invasive mould infection reported.
Why it matters: lung transplant recipients remain among the highest-risk groups for severe aspergillosis. The study reinforces the need for prevention, early recognition, rapid diagnosis and specialist management.
6. A possible new antifungal target in Aspergillus fumigatus
Storer ISR et al. A protein-protein interaction inhibitor arrests the cell cycle in Aspergillus fumigatus. mBio, 2026.
View on PubMed – PMID: 42053292
This laboratory study explored a compound that interferes with protein-protein interactions and can arrest the cell cycle in Aspergillus fumigatus.
Why it matters: current antifungal options remain limited, and resistance is a growing problem. Early-stage work like this may help identify future antifungal drug classes.
7. Diabetes and fungal infection risk
Kaur H et al. Fungal infections in diabetes mellitus. Indian Journal of Medical Microbiology, 2026.
View on PubMed – PMID: 42061613
This review discusses fungal infections in people with diabetes, including mucormycosis, aspergillosis and cryptococcosis.
Why it matters: diabetes can affect immune function and increase susceptibility to some infections. For patients with existing lung disease, good diabetes management may be one part of reducing overall infection risk.
8. Aspergillosis during cancer immunotherapy
Niravath P et al. A Phase II Study of Docetaxel and Pembrolizumab plus Interleukin 12 Gene Therapy in Nonmetastatic, Anthracycline-Refractory Triple-Negative Breast Cancer (INTEGRAL). Clinical Cancer Research, 2026.
View on PubMed – PMID: 41661218
This cancer therapy study includes a reported case of pulmonary aspergillosis and respiratory failure during treatment.
Why it matters: modern cancer treatments can alter infection risk in complex ways. Aspergillosis should remain on the radar in patients who become unwell during or after intensive cancer therapy.
Other papers noted this week
- Canakinumab safety pharmacovigilance analysis – relevant to biologic therapy safety and infection monitoring. PMID: 41998856
- Canine sinonasal radiotherapy study – includes nasal aspergillosis in dogs, but is mainly veterinary/radiotherapy focused. PMID: 42007656
- Mucormycosis retrospective study – relevant to invasive fungal disease burden but not directly focused on aspergillosis. PMID: 42050055
Overall message
This week’s papers show how aspergillosis research is moving in several important directions at once: better diagnostic markers, more personalised antifungal dosing, growing concern about environmental resistance, and continued recognition of high-risk groups such as transplant recipients, critically ill patients and people with complex immune or metabolic conditions.
For patients, the main message is that aspergillosis is a complex condition and testing or treatment decisions often need specialist interpretation. No single test result tells the whole story; clinicians usually combine symptoms, scans, culture results, biomarkers and risk factors before deciding on diagnosis and treatment.
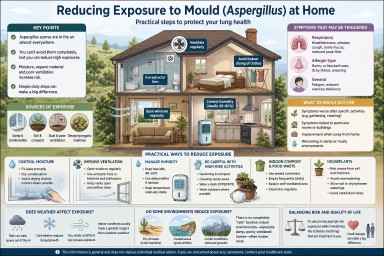
Reducing Exposure to Mould (Aspergillus) at Home
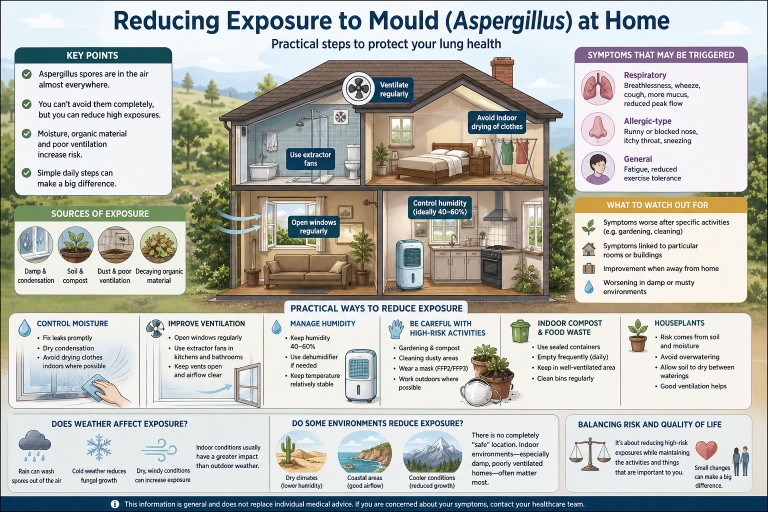
Audience: Patients with aspergillosis (including Allergic Bronchopulmonary Aspergillosis and Chronic Pulmonary Aspergillosis), carers, and non-specialist cliniciansIf you have aspergillosis, reducing exposure to environmental moulds such as Aspergillus can help minimise symptoms and reduce the risk of flare-ups.This guide brings together practical, evidence-informed advice based on environmental studies and clinical experience at specialist centres such as the National Aspergillosis Centre (Manchester, UK).
🔑 Key Points
- Aspergillus spores are present in the air almost everywhere.
- Complete avoidance is not possible—focus on reducing higher-level exposures.
- The most important drivers are moisture, organic decay, and disturbance.
- Indoor exposure is often more important than outdoor exposure.
- Simple environmental and behavioural changes can significantly reduce risk.
🌍 Where does mould exposure come from?
Aspergillus is a common environmental mould. It grows on organic material and releases microscopic spores into the air.
Common sources include:
- Damp walls, ceilings, and condensation
- Soil, compost, and plant material
- Dust and poorly ventilated spaces
- Food waste and decaying organic matter
Spores are always present at low levels. Problems arise when concentrations increase, particularly in enclosed or damp environments.
⚖️ Who is most affected?
Reducing exposure is particularly relevant for people with:
- Allergic Bronchopulmonary Aspergillosis (ABPA)
- Chronic Pulmonary Aspergillosis (CPA)
- Asthma or bronchiectasis
- Reduced immune function
Individual sensitivity varies. Some people notice clear environmental triggers, while others are less affected by day-to-day variation.
⚠️ What symptoms can mould exposure trigger?
Exposure may trigger or worsen symptoms by increasing airway inflammation or allergic responses.
Respiratory symptoms
- Increased breathlessness
- Wheezing or chest tightness
- Persistent or worsening cough
- Increased or thicker mucus
- Reduced peak flow (if monitored)
Allergic-type symptoms
- Nasal congestion or runny nose
- Itchy throat
- Sneezing
General symptoms
- Fatigue
- Reduced exercise tolerance
In ABPA, exposure may contribute to flare-ups. In CPA, changes may be more gradual.
👀 What should you watch out for?
Patterns are often more informative than single exposures.
- Symptoms worsening after specific activities (e.g. gardening, cleaning)
- Symptoms linked to particular rooms or buildings
- Improvement when away from home
- Worsening in damp or musty environments
Keeping a simple symptom diary can sometimes help identify triggers.
Important: Not all symptoms are due to mould exposure—other factors such as infection or asthma control may also play a role.
🏠 Reducing mould in your home
1. Control moisture (most important factor)
- Fix leaks promptly (pipes, roofs, windows)
- Dry condensation from windows and walls
- Avoid prolonged indoor drying of clothes where possible
Moisture is the key driver of mould growth—reducing it addresses the root cause.
2. Improve ventilation
- Open windows regularly (even short periods can help)
- Use extractor fans in kitchens and bathrooms
- Avoid blocking vents or airflow pathways
Ventilation removes spores and reduces humidity at the same time.
3. Manage condensation
- Maintain a relatively stable indoor temperature
- Use lids when cooking
- Consider dehumidifiers in problem areas
🌬️ Ventilation, filtration and humidity
Ventilation (first priority)
Ventilation is usually the most effective intervention because it removes airborne spores and reduces moisture.
Dehumidifiers
Dehumidifiers reduce indoor humidity (target around 40–60%), making conditions less favourable for mould growth.
HEPA air purifiers
HEPA filters can remove airborne particles, including fungal spores. However, they do not address the source of mould and are best used alongside other measures.
Practical approach: address moisture and ventilation first, then consider additional filtration if needed.
🌦️ Does weather affect mould exposure?
- Rain can reduce airborne spores by washing them out of the air
- Cold conditions reduce fungal growth
- Dry, windy weather can increase exposure by disturbing dust and soil
However, indoor conditions usually have a greater impact than outdoor weather.
🌍 Do some environments reduce exposure?
Some environments may be associated with lower exposure:
- Dry climates (lower humidity)
- Coastal areas (good airflow and dilution)
- Cooler conditions (reduced fungal growth)
There is no completely “safe” location, and indoor conditions often matter more than geography.
🌿 Activities and exposure
Some activities can temporarily increase exposure:
- Gardening or handling compost
- Cleaning dusty areas
- Handling stored materials
Precautions:
- Wear a well-fitted mask (FFP2 or FFP3)
- Carry out dusty tasks outdoors where possible
- Avoid enclosed, poorly ventilated spaces
🗑️ Indoor compost bins and food waste
Food waste provides an ideal environment for mould growth.
Risk increases when waste is stored indoors for prolonged periods, particularly in warm conditions.
- Empty bins frequently (ideally daily)
- Use sealed containers
- Keep in well-ventilated areas
- Clean bins regularly
🌱 Houseplants
The main risk comes from soil and moisture rather than the plant itself.
👉 Read full guide on houseplants and aspergillosis
⚖️ Balancing risk and quality of life
It is important to balance exposure reduction with maintaining normal daily activities.
- Gardening can often continue with precautions
- Houseplants can often be kept safely
- Focus on reducing higher-risk exposures rather than avoiding everything
⚠️ When to seek medical advice
- Increasing breathlessness
- Worsening cough or mucus
- Reduced peak flow
- Symptoms clearly linked to environment
Seek urgent advice for:
- Rapid breathlessness
- Chest pain
- Coughing blood
📚 Further reading
👩⚕️ Author & Review
Developed using patient questions and reviewed in line with National Aspergillosis Centre practice (Manchester, UK).
This information is general and does not replace individual medical advice.
Houseplants and Aspergillosis: Do You Need to Get Rid of Them?

Audience: Patients with aspergillosis (including Allergic Bronchopulmonary Aspergillosis), carers, and non-specialist cliniciansHouseplants are a common concern for people with
aspergillosis, particularly those with
Allergic Bronchopulmonary Aspergillosis (ABPA).If you’ve asked this question, you’re not alone—many patients raise it in our
patient questions and discussions.
🔑 Key Points
- Houseplants can be a source of Aspergillus spores, mainly from soil.
- Most people with ABPA do not need to remove all plants.
- The main risk comes from damp soil and disturbance.
- Simple precautions can significantly reduce exposure.
- How plants are cared for matters more than the type of plant.
Contents
- Why houseplants can be a problem
- How big is the risk?
- Do houseplants clean the air?
- Can I safely keep my plants?
- How to reduce risk
- Are some plants lower risk?
- When to consider removing plants
- Common questions
- When to seek medical advice
- References
🌱 Why can houseplants be a problem?
Aspergillus is a common environmental mould found in:
- Soil and compost
- Decaying plant material
- Damp indoor environments
For people with Allergic Bronchopulmonary Aspergillosis (ABPA), inhaling spores can trigger airway inflammation, wheeze, cough, and breathlessness.
The main risk comes from soil rather than the plant itself.
⚖️ How big is the risk?
The risk varies depending on:
- How stable your condition is
- The number of plants
- Ventilation in your home
- How plants are maintained
Specialist centres such as the National Aspergillosis Centre (NAC) recommend a
risk reduction approach rather than complete avoidance.
You can read more in our guide to
reducing mould exposure.
Important: There is limited direct research linking houseplants to worsening ABPA. Advice is based on environmental studies and clinical experience.
🌿 Do houseplants clean the air?
You may have heard that houseplants “clean the air.” This idea comes from laboratory studies, including research by
:contentReference[oaicite:0]{index=0}, conducted in sealed environments.
In real homes, the effect is minimal.
- Very large numbers of plants would be needed
- Ventilation has a much greater impact
- Soil may introduce Aspergillus spores
For a broader explanation, see our
aspergillosis overview.
Bottom line: Plants may improve wellbeing, but they are not an effective air-cleaning strategy.
🌿 Can I safely keep my houseplants?
In many cases, yes.
Many people with ABPA keep houseplants without problems when their condition is stable and plants are well maintained.
However, some individuals are more sensitive, so a personalised approach is important.
✅ How to reduce your risk
1. Manage the soil carefully
- Avoid constantly damp compost
- Allow the top layer to dry between watering
- Consider lower-organic substrates (e.g. clay pebbles)
Tip from patients: Adding a layer of stones or gravel on top of the soil can reduce disturbance during watering and may help limit release of fungal spores.
2. Avoid disturbing soil indoors
- Repot plants outside if possible
- Wear a well-fitted mask (FFP2 or FFP3)
3. Maintain good plant hygiene
- Remove dead leaves promptly
- Avoid visible mould growth
- Do not allow stagnant water
4. Choose locations carefully
- Keep plants out of bedrooms
- Ensure good ventilation
5. Personal hygiene after handling plants
- Wash hands after handling soil or compost
- Avoid touching your face before cleaning hands
- Consider changing clothes after heavy gardening
- Ventilate the area after indoor plant work
These steps form part of a wider approach to
reducing environmental exposure.
🌿 Are some plants lower risk for ABPA?
There is no strong evidence that specific plants are “safe” or “unsafe.” The main risk comes from soil and moisture.
Some setups may be lower risk in practice:
- Hydroponic or semi-hydroponic plants
- Plants that prefer drier conditions (e.g. succulents)
- Well-maintained plants with minimal decaying material
Important: Any plant can become higher risk if soil becomes damp or mouldy.
If unsure, you may wish to review
clinical guidance or discuss with your care team.
🚩 When should I consider removing plants?
- Symptoms worsen after watering or handling plants
- Visible mould in soil
- Frequent flare-ups
- Clinical advice recommends stricter avoidance
Some people remove plants temporarily during unstable periods and reintroduce them later.
❓ Common questions
Are leaves dangerous?
No—the main risk comes from soil and decaying material.
Is outdoor gardening riskier?
Yes, due to higher exposure. Wearing a mask is recommended.
Do air purifiers help?
HEPA filters may reduce airborne particles, but evidence specific to ABPA is limited.
⚠️ When to seek medical advice
- Increasing breathlessness or wheeze
- Worsening cough or mucus
- Reduced peak flow
- Symptoms linked to specific environments
Do not change treatment without medical advice.
📚 References & Further Reading
- What is aspergillosis?
- Reducing exposure to mould
- World Health Organization – Indoor air quality guidance
- UK Health Security Agency – Damp and mould health risks
👩⚕️ Author & Review
Developed for patient education in line with UK specialist practice (National Aspergillosis Centre, Manchester).
This information is general and does not replace individual medical advice.
Looking for more answers? Visit our
patient questions hub.
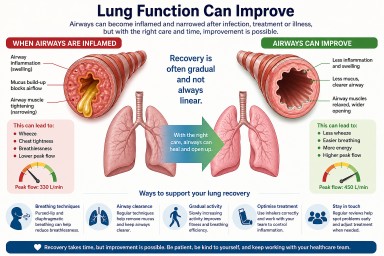
Can Lung Function Improve After Infection or Treatment?
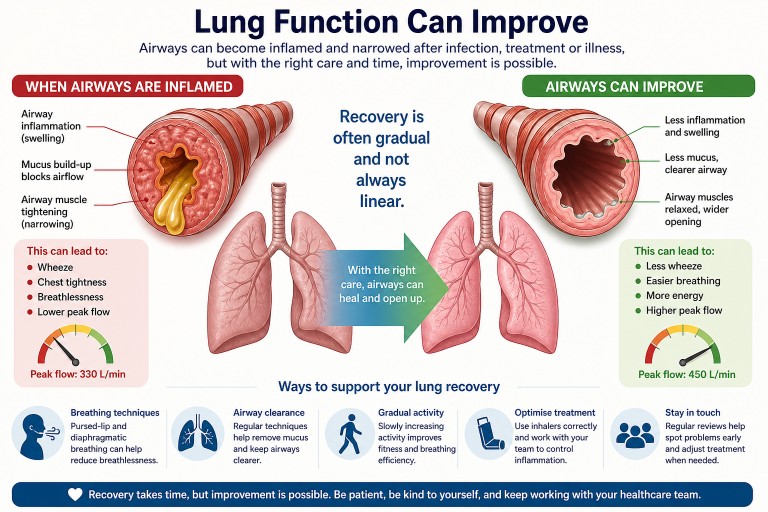
Last reviewed: May 2026
Audience: Patients, carers, and non-specialists
Key Points
- Lung function often can improve after infections, chemotherapy, or inflammation—but recovery may take weeks to months.
- A drop in peak flow usually reflects airway narrowing, inflammation, or mucus, not always permanent damage.
- Normal oxygen levels (e.g. 95–100%) are reassuring and suggest gas exchange is still working well.
- Symptoms like breathlessness and wheeze can persist even while the lungs are gradually recovering.
- If symptoms are not improving, further assessment may help identify treatable causes.
Contents
- Can lung function recover?
- Why has my lung function dropped?
- Why does recovery feel slow or “stuck”?
- What might help?
- Breathing techniques in detail
- When might further tests be needed?
- Common questions
- When to seek medical advice
Can lung function recover?
In many cases, yes—lung function can improve after a significant illness such as a chest infection, chemotherapy, or inflammation affecting the airways.
However, recovery is often gradual and not always straightforward. It may take:
- Several weeks after an infection
- Several months after more severe illness or treatment
It is also common for symptoms to fluctuate during recovery rather than steadily improve.
Why has my lung function dropped?
A reduction in peak flow or increased breathlessness does not always mean permanent damage. Common causes include:
- Airway inflammation (swelling inside the breathing tubes)
- Mucus build-up, which can block airflow
- Airway narrowing or spasm, similar to asthma
- Post-infectious sensitivity (airways remain irritated after infection)
- Reduced fitness after illness (deconditioning)
In some patients, conditions such as Allergic Bronchopulmonary Aspergillosis (ABPA) or other airway diseases can contribute to ongoing symptoms.
Important: If oxygen levels remain normal (for example, around 97%), this suggests that the lungs are still transferring oxygen effectively, which is reassuring.
Why does recovery feel slow or “stuck”?
Many people feel frustrated because they are doing everything “right” but not seeing improvement. This is very common.
Possible reasons include:
- Residual mucus that is difficult to clear
- Ongoing low-level inflammation
- Airways that remain sensitive after infection
- Effects of steroid treatment, especially during dose changes
- Fatigue and reduced activity levels
Recovery can happen slowly in the background, even when symptoms remain noticeable.
What might help?
Different approaches may support recovery. These should be discussed with your clinical team where appropriate.
1. Airway clearance
- Regular airway clearance techniques can help remove mucus
- Some people benefit from devices that assist mucus clearance
2. Breathing techniques
Breathing techniques can help reduce breathlessness and improve control. A more detailed guide is provided below.
3. Gradual activity
- Slowly increasing activity levels can rebuild strength
- Pacing is important—avoid pushing too hard too quickly
4. Optimising treatment
- Ensuring inhaler technique is correct
- Reviewing whether airway inflammation is fully controlled
Breathing Techniques in Detail
Breathing techniques can help reduce breathlessness, improve airflow, and make breathing feel more controlled—especially when airways are inflamed or narrowed.
They do not treat the underlying condition directly, but they can improve symptoms, confidence, and daily activity.
Pursed-Lip Breathing
What it does: Helps keep airways open for longer during breathing out, reducing air trapping and easing breathlessness.
How to do it:
- Breathe in slowly through your nose (about 2 seconds)
- Purse your lips (as if whistling)
- Breathe out slowly through your lips (about 4 seconds)
- Keep the breath out gentle, not forced
When to use it:
- During breathlessness
- With activity (e.g. walking, stairs)
- To regain control of breathing
Tip: Aim for a longer out-breath than in-breath.
Diaphragmatic (Belly) Breathing
What it does: Encourages more efficient breathing using the diaphragm rather than upper chest muscles.
How to do it:
- Sit or lie comfortably
- Place one hand on your chest, one on your abdomen
- Breathe in through your nose and allow your abdomen to rise
- Breathe out slowly (through pursed lips if helpful)
Tip: Keep shoulders relaxed and avoid lifting the chest.
Breathing Control (for flare-ups)
- Pause and rest
- Breathe slowly through the nose
- Breathe out gently through relaxed or pursed lips
- Release tension in shoulders and neck
Helpful positions:
- Sitting leaning forward with arms supported
- Standing leaning on a surface
“Blow as You Go”
Use during activity:
- Breathe in before effort
- Breathe out during effort (e.g. standing up, climbing)
This helps prevent breath-holding and reduces strain.
Important: These techniques should feel comfortable and controlled. If symptoms worsen, stop and rest.
When might further tests be needed?
If symptoms are persistent, worsening, or not improving as expected, your clinical team may consider:
- Spirometry (lung function tests)
- Imaging such as a chest CT scan
- Assessment for:
- Airway inflammation
- Bronchiectasis
- Fungal-related lung disease
Common Questions
Does a drop in peak flow mean permanent damage?
No. Peak flow mainly reflects how open your airways are and can improve with treatment.
Why do I feel breathless if my oxygen levels are normal?
Breathlessness is often caused by airway narrowing or inefficient breathing, not low oxygen.
Can lungs fully recover?
Some people return to their previous baseline. Others improve significantly but may not reach exactly the same level.
When to seek medical advice
- Worsening breathlessness
- Increasing wheeze or chest tightness
- New or persistent cough
- Changes in sputum (including blood)
- No improvement over time
If symptoms suddenly worsen, seek urgent medical attention.
Final Thoughts
A drop in lung function after infection or treatment can feel worrying, but it often reflects treatable airway changes. Improvement is possible, although recovery may take time.
Staying in contact with your healthcare team helps ensure that any ongoing issues are identified and managed appropriately.
References & Further Reading
- British Thoracic Society (BTS) guidance
- European Respiratory Society (ERS) patient resources
- National Aspergillosis Centre patient information
This article is for general information only and does not replace medical advice. Always consult your healthcare team.
ABPA or Steroid Side Effects? Understanding Symptoms During Long-Term Treatment
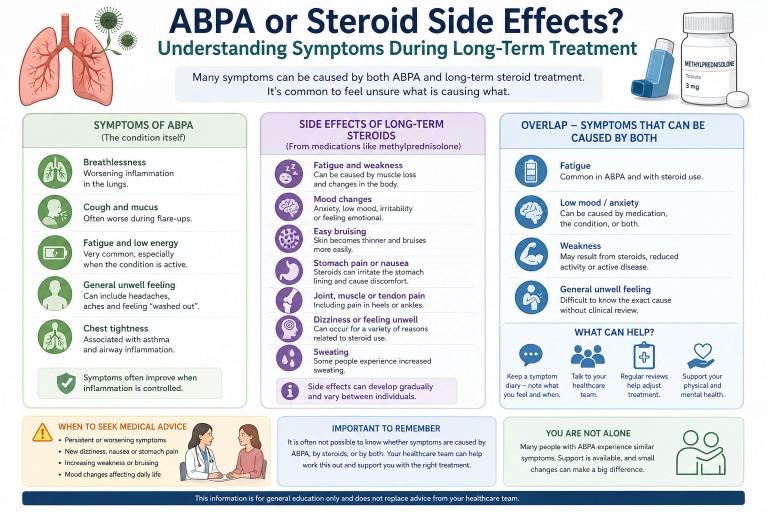

Last reviewed: April 2026
Many people living with Allergic Bronchopulmonary Aspergillosis (ABPA) who take long-term steroids find it difficult to tell whether their symptoms are caused by the condition or the treatment.
Symptoms in ABPA can come from both the condition and long-term steroid treatment. Fatigue, weakness, mood changes, and general unwellness are common to both, making it difficult to identify a single cause without clinical review.
This is especially true for people taking corticosteroids such as methylprednisolone or prednisolone.

---
Key Points
- ABPA and steroid treatment can cause overlapping symptoms.
- Fatigue, low mood, and general unwellness can come from either the condition or medication.
- Long-term corticosteroid use can cause additional side effects.
- It is common to feel unsure what is causing symptoms.
- Ongoing or worsening symptoms should be discussed with your healthcare team.
---
Why is it hard to tell the difference?
ABPA is an immune-driven lung condition that causes inflammation. Treatment often includes corticosteroids such as methylprednisolone or prednisolone, which reduce inflammation but can also affect many systems in the body.
This means that:
- The disease itself can cause symptoms
- The treatment can also cause symptoms
As a result, people often experience a combination of both.
---
Symptoms caused by ABPA
ABPA commonly affects the lungs but can also cause more general symptoms.
- Fatigue and low energy
- Breathlessness
- Cough and mucus production
- Chest tightness
- General feeling of being unwell
Fatigue can be particularly prominent, especially during flare-ups.
---
Side effects of long-term steroids
Corticosteroids such as methylprednisolone are highly effective treatments, but long-term use can lead to a range of side effects.
- Fatigue and weakness (including muscle loss)
- Mood changes (anxiety, low mood, irritability)
- Easy bruising (skin becomes thinner)
- Stomach irritation or pain
- Dizziness or feeling unwell
- Sweating
- Bone or joint discomfort
Learn more about treatment approaches in aspergillosis treatment options.
---
Where symptoms overlap
Some symptoms can be caused by both ABPA and steroid treatment, making them difficult to interpret.
| Symptom | Possible cause |
|---|---|
| Fatigue | ABPA inflammation or steroid effects |
| Low mood / anxiety | Medication effects or impact of chronic illness |
| Weakness | Muscle loss from steroids or reduced activity |
| General unwell feeling | Both |
This overlap is one of the most challenging aspects of long-term management.
🔎 Not sure what’s causing your symptoms?
Many people with ABPA feel exactly the same—this overlap is one of the most common challenges during long-term treatment.
---
Understanding specific symptoms
Some symptoms are more commonly linked to treatment effects:
- Easy bruising – often related to steroid use
- Heel or ankle pain – may relate to tendon or joint effects
- Stomach pain – can be linked to steroid irritation
Other symptoms, such as fatigue, dizziness, and nausea, may have multiple possible causes.
Because of this, it is often not possible to attribute symptoms to a single cause without clinical review.
---
When to seek medical advice
You should contact your healthcare team if you experience:
- Persistent or worsening fatigue
- New dizziness or nausea
- Ongoing stomach pain
- Increasing weakness
- Mood changes affecting daily life
These symptoms do not necessarily indicate a serious problem, but they may mean that treatment or support needs to be reviewed.
---
Summary
In ABPA, symptoms such as fatigue, weakness, and low mood can arise from both the condition and its treatment. Long-term steroid use can add additional effects, making it difficult to distinguish between causes.
If symptoms are persistent or worsening, it is important to discuss them with your healthcare team so that appropriate adjustments or support can be considered.
---
Further Reading
- Allergic Bronchopulmonary Aspergillosis (ABPA)
- Treatment of Aspergillosis
- Weight Loss and Weakness in Aspergillosis
---
Author & Review
Prepared for aspergillosis.org to support patient understanding. Content reflects current clinical knowledge and patient-reported experience.
Disclaimer
This information is for general education only and does not replace advice from your healthcare team.
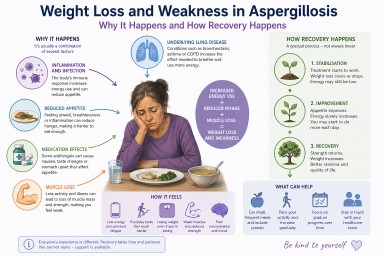
Weight Loss and Weakness in Aspergillosis: Why It Happens, How It Feels, and What Helps Recovery
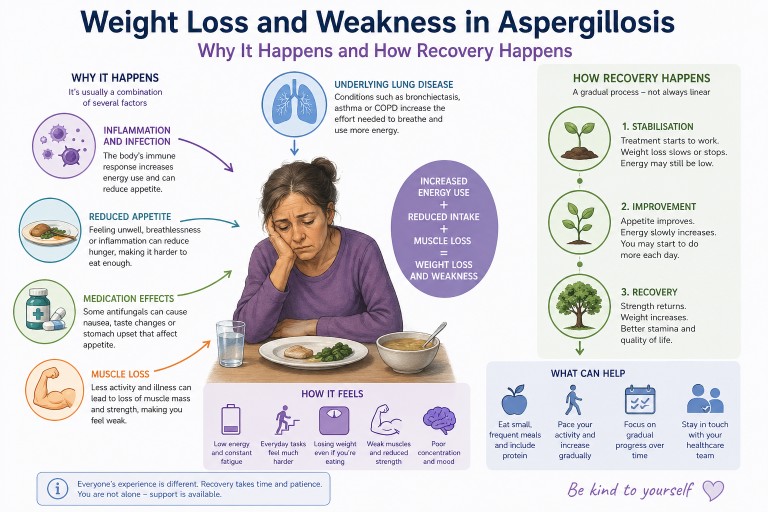
Last reviewed: April 2026
Unexpected weight loss and severe weakness are among the most worrying symptoms people report after being diagnosed with aspergillosis. Many describe feeling unlike themselves—physically drained, thinner than they have ever been, and struggling with everyday activities.
This article explains why this happens, what is going on in the body, and what recovery typically looks like.
---
Key Points
- Weight loss and fatigue are common in aspergillosis, particularly early in the illness or during flare-ups.
- They are usually caused by a combination of inflammation, increased energy use, reduced appetite, and muscle loss.
- Medication side effects can contribute but are rarely the main cause.
- Many people improve over time, but recovery is usually gradual and can take weeks to months.
- Stabilising weight is often the first important step before regaining strength.
---
Contents
- Why does aspergillosis cause weight loss?
- What is happening inside the body?
- Which types of aspergillosis are affected?
- Why does it feel so severe?
- Does it get better?
- What can help day to day?
- Nutrition and rebuilding strength
- When to seek medical advice
- Common questions
---
Why does aspergillosis cause weight loss?
Weight loss in aspergillosis is rarely due to a single cause. Instead, it is usually the result of several overlapping processes.
1. Increased energy use (hypermetabolism)
When the body is dealing with infection or inflammation, it requires more energy. This is sometimes described as a hypermetabolic state.
- The immune system is active and consumes energy
- The body produces inflammatory signals
- Breathing effort may increase
This means you may be burning more calories than usual—even at rest.
2. Reduced appetite
Many people notice they are eating less, sometimes without realising it. This may be due to:
- Feeling unwell or fatigued
- Shortness of breath when eating
- Changes in appetite driven by inflammation
3. Medication effects
Some treatments can affect appetite or digestion. For example:
- Antifungal medications such as itraconazole or voriconazole may cause nausea or taste changes
- Steroids may increase appetite but can also contribute to muscle weakness over time
Medication effects vary widely and are usually only part of the overall picture.
4. Muscle breakdown
During illness, the body may break down muscle to meet energy needs. This can happen quickly, especially if activity levels fall.
This leads to:
- Loss of strength
- Reduced stamina
- A feeling of being “weak” rather than just lighter
5. Underlying lung disease
Many people with aspergillosis also have conditions such as bronchiectasis, asthma, or chronic obstructive pulmonary disease (COPD). These can increase the effort required for breathing and contribute to ongoing energy use.
---
What is happening inside the body?
Several biological processes contribute to weight loss and fatigue:
- Inflammatory signalling: The immune system releases chemical signals that affect metabolism and appetite
- Catabolism: The body breaks down tissues (including muscle) to release energy
- Energy imbalance: More energy is used than consumed
This combination can make weight loss feel rapid and difficult to control.
---
Which types of aspergillosis are affected?
These symptoms are most commonly seen in:
- Chronic Pulmonary Aspergillosis (CPA)
- Allergic Bronchopulmonary Aspergillosis (ABPA), particularly during flare-ups
However, not everyone experiences weight loss, and severity varies.
---
Why does it feel so severe?
Many people describe this stage as one of the most difficult parts of their illness. This is because several factors are happening at once:
- Physical energy is reduced
- Muscle strength has declined
- The body is under ongoing stress
- Recovery has not yet begun
This can make everyday activities—such as walking, cooking, or even eating—feel unusually difficult.
---
Does it get better?
In many cases, yes—there is gradual improvement over time, especially once treatment begins to control the condition.
Recovery often follows a pattern:
- Initial phase: weight loss and severe fatigue
- Stabilisation: weight loss slows or stops
- Recovery: gradual return of strength and energy
This process is usually slow and uneven, with good and bad days.
---
What can help day to day?
1. Focus on maintaining nutrition
- Eat small amounts regularly rather than large meals
- Choose foods that are easy to prepare and eat
- Include protein to support muscle maintenance
2. Pace activity carefully
- Gentle movement can help maintain strength
- Avoid pushing too hard, as this can worsen fatigue
- Increase activity gradually as energy improves
3. Look at trends over time
It can be helpful to focus on gradual changes such as:
- Weight stabilising
- Small improvements in energy
---
Nutrition and rebuilding strength
Recovery often happens in stages:
- Stage 1: Stabilising weight
- Stage 2: Gradually increasing intake
- Stage 3: Rebuilding muscle and strength
Regaining muscle mass takes time and usually follows once the underlying condition is better controlled.
---
When to seek medical advice
You should contact your healthcare team if you experience:
- Continued or rapid weight loss
- Increasing weakness
- Difficulty eating or swallowing
- New or worsening symptoms
This may indicate the need for additional support or adjustment of treatment.
---
Common questions
Is weight loss just due to poor appetite?
No. Reduced appetite is only one factor. Increased energy use and muscle loss are also important contributors.
Are medications the main cause?
Medications can contribute, but they are rarely the main reason for weight loss.
Will I regain my strength?
Many people do regain strength over time, although recovery is usually gradual.
Why does recovery take so long?
The body needs time to reduce inflammation, restore energy balance, and rebuild muscle.
---
Summary
Weight loss and weakness in aspergillosis are common and can feel severe, particularly early in the illness. They are usually caused by a combination of increased energy use, reduced appetite, muscle loss, and underlying lung disease.
Although recovery can take time, many people improve gradually as treatment takes effect.
---
Further Reading
- Chronic Pulmonary Aspergillosis (CPA)
- Allergic Bronchopulmonary Aspergillosis (ABPA)
- Treatment of Aspergillosis
---
Author & Review
Prepared for aspergillosis.org to support patient understanding. Content reflects current clinical knowledge and patient-reported experience.
Disclaimer
This page is for general information only and does not replace advice from your healthcare team.
Weekly Aspergillosis Research Update: Week ending 27 April 2026
Highlights this week
- Occupational aspergillosis: workplace exposure to Aspergillus highlighted in a national study.
- ABPA and biologics: early evidence for tezepelumab in allergic bronchopulmonary aspergillosis.
- Mucus plugging: important mechanism in ABPA, bronchiectasis and chronic lung disease.
- Invasive disease: new analysis of antifungal treatment strategies.
- Resistance: ongoing global surveillance of antifungal susceptibility.
Occupational non-invasive aspergillosis
A French national multicentre study reviewed occupational cases of non-invasive aspergillosis over more than 20 years.
Why it matters: workplace exposure (dust, compost, damp buildings, waste handling) may contribute to disease in some patients and should be considered in clinical history-taking.
Reference: Michel A et al.
PMID: 42033338
Tezepelumab in allergic bronchopulmonary aspergillosis
A small 4-patient case series explored the use of tezepelumab in allergic bronchopulmonary aspergillosis (ABPA) with severe asthma.
Why it matters: adds to growing interest in biologics for ABPA, particularly where steroid burden is high. Evidence remains early and limited.
Reference: Sanz-Sanjosé B et al.
PMID: 42017435
Mucus plugging in chronic lung disease
A narrative review examined mucus plugging in chronic obstructive lung diseases and bronchiectasis, including ABPA.
Why it matters: mucus plugs can block airways, worsen breathlessness, and contribute to infection risk and scan abnormalities.
Reference: Schou C et al.
PMCID: PMC13103984
Invasive aspergillosis treatment
A systematic review and network meta-analysis compared antifungal treatment regimens for invasive aspergillosis.
Why it matters: invasive aspergillosis remains a high-mortality infection; early diagnosis and optimal antifungal therapy are critical. Triazoles and other antifungals remain central to management. :contentReference[oaicite:0]{index=0}
Reference: Gu Q et al.
PMID: 42012594
Natural killer cells and resistant Aspergillus
A laboratory study demonstrated antifungal activity of human natural killer cells against azole-resistant Aspergillus fumigatus.
Why it matters: improves understanding of immune defence mechanisms and may inform future therapies.
Reference: Namie H et al.
PMID: 42012259
Antifungal susceptibility surveillance
A multicentre Taiwan study examined susceptibility patterns of clinical Aspergillus isolates (2021–2023).
Why it matters: resistance patterns vary geographically, influencing antifungal treatment choices.
Reference: Hsieh M et al.
PMID: 42012212
Invasive aspergillosis in severe viral illness
A study explored invasive pulmonary aspergillosis complicating severe fever with thrombocytopenia syndrome.
Why it matters: reinforces the link between severe illness, immune disruption, and risk of invasive aspergillosis.
Reference: Du Q et al.
PMID: 42032512
Lower-priority or indirect papers
Veterinary study (canine nasal aspergillosis)
Primarily a veterinary oncology study with limited relevance to human disease.
Reference:
PMID: 42007656
Canakinumab pharmacovigilance
Focuses on drug safety rather than aspergillosis.
Reference:
PMID: 41998856
Overall message
This week’s research highlights the wide scope of aspergillosis—from environmental and occupational exposure to allergic disease, invasive infection, antifungal resistance, and immune responses. The most relevant developments for patients remain ABPA biologics, mucus plugging, and antifungal resistance trends.
Patient note
This summary is for general information only and does not replace medical advice. Always discuss treatment decisions with your specialist team.
Damp Homes, Indoor Air and Health: What a Recent Evidence Review Tells Us

Summary: A recent rapid review by researchers from the Health and Safety Executive examined evidence on microbiological hazards in buildings, including moulds, bacteria and viruses. The review highlights that dampness, poor ventilation and building design can all affect indoor air quality and respiratory health.
Key points
- People spend much of their time indoors, so indoor air quality can strongly affect health.
- Damp indoor conditions increase the risk of mould growth and musty odours.
- Common indoor moulds include Aspergillus, Penicillium and Cladosporium.
- Dampness and visible or hidden mould are linked with asthma, rhinitis, wheeze and other respiratory symptoms.
- Ventilation is one of the most important ways to reduce moisture and dilute airborne contaminants.
- Improving energy efficiency is important, but very airtight homes still need adequate ventilation.
Contents
- Why indoor air matters
- What the review found
- Damp, mould and lung health
- Aspergillus and aspergillosis
- Ventilation and building design
- What can help reduce risk?
- Help us understand damp homes and health
- When to seek medical advice
Why indoor air matters
Most of us spend a large amount of time indoors — at home, at work, or in public buildings. The air inside buildings can contain particles from many sources, including dust, mould spores, bacteria, viruses, cooking, cleaning products, pets and outdoor air entering the home.
The recent review, Exposure Risks from Microbiological Hazards in Buildings and Their Control — A Rapid Review of the Evidence, looked at evidence for harmful microorganisms in indoor air and on surfaces, and how building design, ventilation and moisture affect exposure.
What the review found
The review found strong evidence that microorganisms can be present in indoor air and on surfaces. These include fungi, bacteria and viruses. The evidence was strongest for the role of dampness and poor ventilation in increasing the risk of indoor mould growth and respiratory health effects.
The review’s main conclusions included:
- Airborne allergenic fungi are well documented in indoor air.
- Damp conditions increase mould growth and mouldy odours indoors.
- Dampness and mould are associated with respiratory ill health, including asthma, rhinitis and wheezing.
- Penicillium, Aspergillus and Cladosporium are commonly detected in damp buildings.
- Infectious viruses and bacteria can also be detected in indoor air and on surfaces.
- Ventilation is a key control measure for reducing moisture and diluting airborne contaminants.
Damp, mould and lung health
Dampness is one of the most important drivers of indoor mould growth. Moisture can come from leaks, condensation, flooding, poor insulation, inadequate heating, drying clothes indoors, cooking, showering, or poor ventilation.
When dampness persists, mould can colonise indoor materials such as plasterboard, wallpaper, wood, carpets, soft furnishings and settled dust. Mould may be visible, but it can also grow in hidden areas such as behind furniture, inside wall cavities, behind wallpaper, under flooring, or around poorly ventilated cold surfaces.
Exposure to damp and mould has been linked with:
- Wheezing
- Asthma symptoms or asthma worsening
- Rhinitis and nasal symptoms
- Cough
- Respiratory infections
- Worsening symptoms in people with existing lung disease
Importantly, the review notes that the relationship between indoor microorganisms and health is complex. Risk depends on the type of organism, the level of exposure, the building conditions and the susceptibility of the person exposed.
Aspergillus and aspergillosis
Aspergillus is a common mould found in the environment. Most people inhale Aspergillus spores every day without becoming ill. However, some people are more vulnerable, including those with asthma, bronchiectasis, chronic lung disease, weakened immune systems, or previous lung damage.
In susceptible people, exposure to Aspergillus may contribute to conditions such as allergic bronchopulmonary aspergillosis (ABPA), severe asthma with fungal sensitisation (SAFS), aspergillus bronchitis, or chronic pulmonary aspergillosis (CPA). The home environment is not the only source of exposure, but damp indoor spaces may increase the amount of fungal material a person breathes in.
This does not mean that every damp home causes aspergillosis, or that every person exposed to mould will become ill. It does mean that reducing dampness, improving ventilation and addressing visible or hidden mould are sensible steps for respiratory health.
Ventilation and building design
One of the strongest messages from the review is that ventilation is central to controlling indoor microbiological risk. Ventilation helps by:
- Removing moisture from indoor air
- Reducing condensation
- Diluting airborne mould spores and other particles
- Reducing the build-up of infectious aerosols
- Improving overall indoor air quality
The review also highlights an important modern problem. Homes are increasingly designed or retrofitted to be more airtight and energy efficient. This can improve warmth and reduce energy use, but if ventilation is inadequate, moisture and airborne contaminants may accumulate indoors.
In other words, insulation and energy efficiency are important, but they need to be balanced with effective ventilation and moisture control.
What can help reduce risk?
The review does not suggest that one single action solves all indoor air problems. Instead, it supports a combined approach.
1. Reduce moisture
- Repair leaks promptly.
- Check roofs, gutters, pipes and window seals.
- Use extractor fans in kitchens and bathrooms where available.
- Avoid drying clothes indoors where possible, or ventilate well if you do.
- Reduce condensation on windows and cold walls.
2. Improve ventilation
- Use trickle vents if fitted.
- Open windows when safe and practical.
- Use mechanical ventilation systems correctly.
- Keep air bricks and vents clear.
- Make sure extractor fans are working effectively.
3. Deal with mould safely
- Small areas of surface mould may be cleaned carefully using appropriate household methods.
- Large, persistent or recurring mould usually needs the underlying damp problem fixed.
- People with significant lung disease, immune suppression or severe symptoms should avoid heavy mould disturbance and seek advice.
4. Reduce dust reservoirs
- Regular cleaning can reduce settled dust and spores.
- HEPA-filter vacuum cleaners may be helpful for some households.
- Hard flooring may be easier to keep dust-free than carpets in high-risk situations.
5. Consider air filtration where appropriate
Portable high-efficiency particulate air (HEPA) filters may help reduce airborne particles in some settings. They are not a substitute for fixing damp or improving ventilation, but they may be a useful additional measure for some people.
Help us understand damp homes and health
The evidence linking damp homes, mould and respiratory health is strong, but there are still important unanswered questions. We need to better understand how different homes, building types, ventilation patterns and damp conditions affect people’s health in real life.
The National Aspergillosis Centre is running a UK citizen science study looking at damp homes and health.
We are inviting people to register their interest in taking part.
The study is open to people with and without lung conditions, and to people living in homes with or without damp or mould. This comparison is important because it helps researchers understand which factors are most strongly linked with health outcomes.
Register your interest in the damp homes and health study
Taking part may involve completing a questionnaire and, at a later stage, providing a dust sample from your home. The information gathered will help improve understanding of indoor environments and respiratory health.
When to seek medical advice
Please seek medical advice if you have:
- New or worsening breathlessness
- Chest pain
- Coughing up blood
- Persistent fever
- Repeated chest infections
- Rapidly worsening asthma symptoms
- Unexplained weight loss or severe fatigue
If you already have aspergillosis, asthma, bronchiectasis, chronic obstructive pulmonary disease (COPD), immune suppression, or another lung condition, it is worth discussing any significant damp or mould exposure with your healthcare team.
Common questions
Can mould affect health even if I cannot see it?
Yes. Hidden mould or dampness may still affect indoor air quality. A musty smell, persistent condensation or symptoms that worsen in a particular room may suggest a problem.
Does all mould cause aspergillosis?
No. Mould exposure is common, and most people do not develop aspergillosis. Aspergillosis usually occurs when exposure combines with individual susceptibility, such as asthma, bronchiectasis, immune suppression or existing lung damage.
Is ventilation always good?
Ventilation is usually important for reducing moisture and improving indoor air quality. However, the best approach depends on the building, outdoor conditions and the person’s health. Ventilation should not replace fixing leaks or removing sources of damp.
Can air purifiers solve damp and mould problems?
No. Air purifiers may reduce airborne particles, but they do not remove the source of moisture or mould growth. Damp problems need to be addressed at source.
Summary
This recent evidence review reinforces a practical message: indoor air quality matters. Dampness, poor ventilation and mould growth are not simply cosmetic housing problems — they can affect respiratory health, especially in people with asthma, aspergillosis or other lung conditions.
The most effective approach is to reduce moisture, improve ventilation, remove mould sources where possible and understand how buildings influence exposure. Research such as the UK damp homes and health study will help build better evidence for patients, clinicians, housing providers and policymakers.
References and further reading
- Beswick A, Crook B, Gosling B, et al. Exposure Risks from Microbiological Hazards in Buildings and Their Control — A Rapid Review of the Evidence. Atmosphere. 2025;16:1243. doi:10.3390/atmos16111243.
- Damp homes and health study — register your interest
- Aspergillosis.org — patient and carer information
Article type: Patient and public information
Last reviewed: April 2026
Based on: Recent evidence review of microbiological hazards in buildings and their control.
Can Aspergillosis Be Cured? Understanding Treatment, Control, and Long-Term Therapy
Last reviewed: April 2026
Key points
- Aspergillosis is caused by fungi from the Aspergillus group.
- Most people breathe in Aspergillus spores regularly without becoming ill.
- In some people, damaged airways, lung cavities, mucus plugs, or immune responses allow the fungus or fungal material to persist.
- Antifungal treatment may aim to cure, but in many cases the goal is long-term control.
- Steroids can reduce harmful inflammation in allergic disease, but they can also reduce the body’s ability to clear fungus.
Table of contents
- Overview
- Why breathing in spores does not usually cause disease
- Why aspergillosis can be hard to clear
- Infection and ABPA: different reasons for persistence
- Do steroids influence this?
- Control vs cure
- Common antifungal treatments
- Why you may not hear many success stories
- When to seek medical advice
- Common questions
Overview
It is very common for people diagnosed with aspergillosis to feel worried when they read that others have been taking antifungal medication for months or even years.
This can lead to an understandable question:
“Does treatment actually work, or will I have this forever?”
The answer is more nuanced than a simple yes or no. Different forms of aspergillosis behave differently, and treatment goals vary depending on the condition.
Two of the most common conditions are:
- Allergic Bronchopulmonary Aspergillosis (ABPA) – an allergic immune reaction to Aspergillus in the airways
- Chronic Pulmonary Aspergillosis (CPA) – a long-term fungal infection, usually in areas of damaged lung tissue
Understanding this difference is key to understanding why treatment may continue for a long time.
If you would like a more detailed explanation of how these conditions are diagnosed and managed, see our guides to chronic pulmonary aspergillosis (CPA) and allergic bronchopulmonary aspergillosis (ABPA).
Why breathing in spores does not usually cause disease
Aspergillus spores are present in the environment, including air, soil, compost, dust, and decaying vegetation. Most people breathe in small numbers of these spores regularly without becoming ill.
In healthy lungs, spores are usually cleared by the immune system and by the normal cleaning mechanisms of the airways.
This means:
- Exposure to Aspergillus is common
- Most exposure does not lead to disease
- Aspergillosis usually develops only when there are additional risk factors, such as lung damage, mucus trapping, or altered immune responses
So it is not accurate to think of most patients as being “constantly reinfected”. A better way to think about it is that some lungs provide conditions where Aspergillus, or fungal material, can persist and continue to cause problems.
Why aspergillosis can be hard to clear
Aspergillosis can be difficult to clear for several reasons. These include the structure of the lungs, the biology of the fungus, limitations of drug penetration, and the way the immune system responds.
1. Damaged lung tissue can provide protected spaces
In CPA, Aspergillus often grows in areas of abnormal lung, such as cavities, scarred tissue, or areas affected by bronchiectasis.
These areas can act as protected spaces where the fungus is harder for the immune system and antifungal medicines to reach.
2. Thick mucus can trap fungus and fungal material
In airway diseases such as asthma, bronchiectasis, and ABPA, thick mucus can trap spores, hyphae, and fungal fragments.
This trapped material can continue to stimulate inflammation even when the fungus is not invading lung tissue.
3. Antifungal medicines may suppress rather than sterilise
Antifungal medications can reduce fungal activity and help prevent progression, but they may not always remove every trace of fungus from damaged lung spaces or mucus-filled airways.
For this reason, success is often measured by:
- Improved symptoms
- Stabilised weight and energy
- Fewer flare-ups
- Stable or improved scans
- Prevention of further lung damage
Infection and ABPA: different reasons for persistence
Chronic pulmonary aspergillosis: persistence of infection
In chronic pulmonary aspergillosis, the problem is fungal growth in damaged lung tissue.
- Lung cavities provide spaces where fungus can grow
- Drug penetration may be limited
- The immune system may not fully clear infection
Allergic bronchopulmonary aspergillosis: persistence of reaction
In ABPA, the main issue is an exaggerated immune response.
- Mucus traps fungal material
- Small amounts can trigger strong reactions
- Inflammation leads to more mucus
Do steroids influence this?
Yes. Steroids can be helpful but must be used carefully.
In ABPA, they reduce inflammation but may also reduce fungal clearance.
In chronic infection, steroids can increase the risk of persistence or progression.
Monitoring and drug interactions are important during treatment.
Control vs cure: what is the goal?
For many people, the realistic goal is:
- Stability rather than eradication
- Reduced symptoms
- Prevention of progression
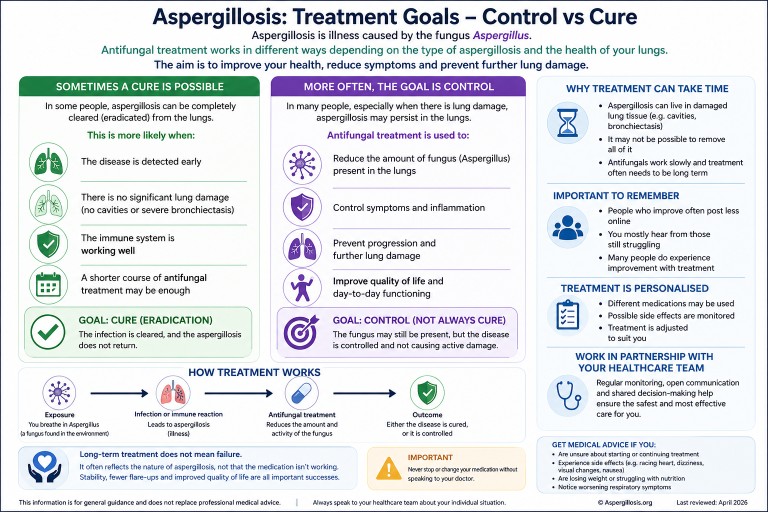
Common antifungal treatments
- Itraconazole
- Voriconazole
- Posaconazole
These treatments are selected based on individual factors and require monitoring.
Why don’t I hear many success stories?
People who improve often post less, while those still struggling are more visible in forums.
When to seek medical advice
- Uncertainty about treatment
- Side effects
- Weight loss
- Worsening symptoms
Common questions
Can aspergillosis be cured?
Sometimes, but often it is managed long-term.
Are people constantly reinfected?
No. Most people clear spores regularly without issue.
Why is ABPA difficult to treat?
Because of ongoing immune reactions and mucus trapping.
Further reading
- Chronic Pulmonary Aspergillosis (CPA)
- Allergic Bronchopulmonary Aspergillosis (ABPA)
- Antifungal medicines
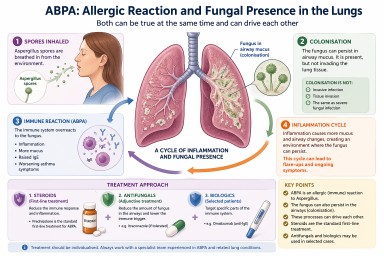
ABPA: Allergic Reaction or Fungal Presence in the Lungs?
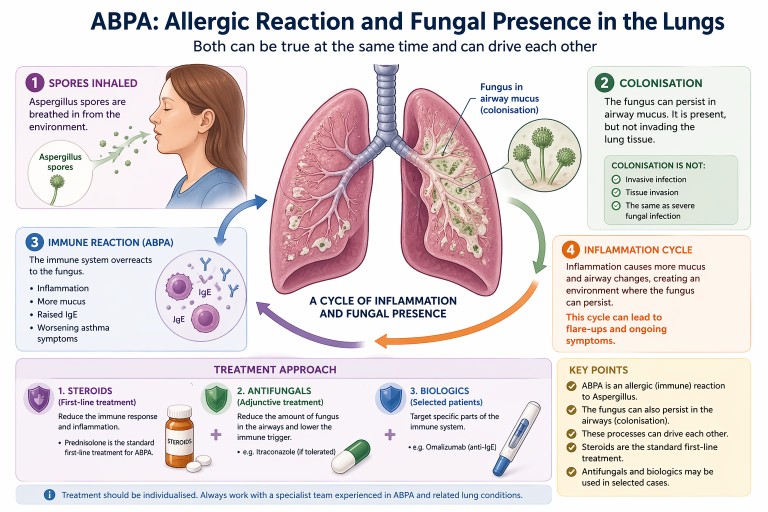
Allergic Bronchopulmonary Aspergillosis (ABPA) can be confusing. It is often described as an allergic condition, yet patients may also be told there is “fungus in the lungs”.
In reality, both can be true at the same time.
Key points
- ABPA is primarily an allergic (immune) reaction to Aspergillus
- The fungus can also persist in the airways (colonisation)
- Colonisation is not the same as invasive infection
- Steroids are the standard first-line treatment
- Antifungals and biologics may be used in selected cases
What is ABPA?
ABPA is a condition where the immune system overreacts to a common environmental fungus, most often Aspergillus fumigatus.
For a full introduction, see our guide to
what is ABPA.
This leads to:
- airway inflammation
- increased mucus production
- worsening asthma symptoms
- raised Immunoglobulin E (IgE) levels
If you are unfamiliar with IgE, see
our explanation of IgE.
Importantly, ABPA is not an invasive fungal infection. The lungs are reacting to fungal material rather than being invaded by it.
Can the fungus live in the lungs?
Yes—this is an important nuance.
In people with conditions such as:
- asthma
- bronchiectasis
the structure of the airways can allow Aspergillus to persist in mucus within the airways. This is known as colonisation.
Colonisation means:
- the fungus is present in airway mucus
- it may grow at low levels locally
- it does not invade lung tissue
This is very different from serious invasive fungal infections seen in severely immunocompromised patients.
How ABPA and colonisation interact
ABPA and colonisation are best understood as part of a spectrum of Aspergillus-related lung disease.
They can interact in a cycle:
- Aspergillus spores are inhaled
- The fungus persists in airway mucus
- The immune system reacts strongly (ABPA)
- Inflammation leads to more mucus production
- This creates an environment where the fungus can persist
This cycle can contribute to:
- recurrent flare-ups
- ongoing inflammation
- persistently raised IgE levels
Standard treatment: steroids
Oral corticosteroids are the traditional first-line treatment for ABPA.
Steroids such as prednisolone are used because they:
- reduce airway inflammation
- suppress the allergic immune response
- improve symptoms such as breathlessness and cough
- help control flare-ups
Learn more in our guide to
steroids and aspergillosis.
Where do antifungals fit in?
Antifungal medications such as itraconazole are often used as an additional (adjunctive) treatment rather than the primary therapy.
The aim is to:
- reduce the amount of fungus present in the airways
- lower the trigger for the immune response
- sometimes allow a reduction in steroid dose
For more detail, see our
antifungal treatments guide.
Biologic treatments
Biologic therapies such as omalizumab (anti-IgE) are increasingly used in some patients, particularly when:
- symptoms are difficult to control
- steroid side effects are significant
- there is severe asthma alongside ABPA
Read more about
biologics in asthma and ABPA.
Why results and symptoms may not match
Some people with ABPA may feel relatively well but still have:
- raised IgE levels
- evidence of fungal presence in the airways
This is because blood tests reflect underlying immune activity, which does not always match how a person feels day to day.
Why treatment is individualised
Although steroids are the standard treatment, management is often tailored to the individual. This is because people may also have:
- asthma
- bronchiectasis
- difficulty tolerating antifungal medications
- side effects from long-term steroid use
Specialist teams balance these factors when planning treatment.
When to seek medical advice
People with ABPA should seek medical review if they experience:
- worsening breathlessness
- increased cough or sputum
- new or persistent chest symptoms
- possible medication side effects
Treatment decisions should always be made with a clinician experienced in managing Aspergillus-related lung disease.
Summary
- ABPA is primarily an allergic condition
- The fungus can also persist in the airways (colonisation)
- These processes can drive each other
- Steroids are the standard first-line treatment
- Antifungals and biologics may be used in selected cases
Last reviewed: April 2026
Prepared by: National Aspergillosis Centre (patient information resource)