Breathe deeply at the Asthma + Lung UK Garden

Asthma + Lung UK’s “Breathing Space Garden” at the RHS Chelsea Flower Show is a beautiful reminder of how much our surroundings can affect our lungs, our wellbeing, and our ability to pause and breathe.
Designed by award-winning garden designer Angus Thompson, the garden is inspired by the Japanese idea of yohaku no bi — “the beauty of empty space”. It brings together calming woodland planting, flowing water, accessible design, and quiet areas for rest, reflection, yoga, and tai chi.
The planting has been chosen with lung health in mind, using low-allergen species, soft textures, resilient trees, and calming green spaces that offer a gentler environment for people with sensitive lungs.
For people living with aspergillosis, asthma, chronic obstructive pulmonary disease (COPD), bronchiectasis, and other lung conditions, this message is especially powerful. Clean air, reduced stress, accessible outdoor spaces, and thoughtful planting can all help people feel more comfortable and supported.
Importantly, the garden will continue to make a difference after Chelsea. It is due to be permanently relocated to the Breathing Space lung rehabilitation centre in Rotherham, where it will support people living with lung conditions for years to come.
RHS Chelsea Flower Show: 19–23 May 2026
Read more from Asthma + Lung UK
Physiotherapy for Aspergillosis: Breathing, Mucus Clearance and Keeping Active
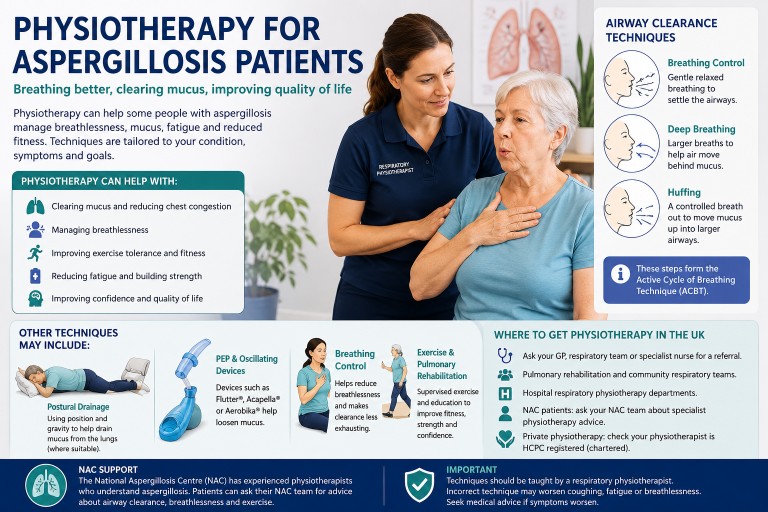
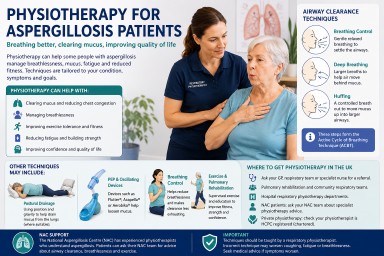
Physiotherapy can be an important part of supportive care for some people living with aspergillosis. It does not treat the fungal infection itself, but it can help with breathlessness, mucus clearance, strength, fitness, posture, fatigue and confidence with activity.
This may be especially helpful for people with Chronic Pulmonary Aspergillosis (CPA), Allergic Bronchopulmonary Aspergillosis (ABPA), Severe Asthma with Fungal Sensitisation (SAFS), Aspergillus bronchitis, bronchiectasis, asthma, Chronic Obstructive Pulmonary Disease (COPD), or lung damage from previous infection.
Key points
- Physiotherapy can help some aspergillosis patients manage mucus, breathlessness and reduced activity.
- Airway clearance techniques may be useful when mucus is difficult to clear.
- The Active Cycle of Breathing Technique (ACBT) is commonly used in respiratory physiotherapy.
- Other approaches include huffing, breathing control, postural drainage, airway clearance devices, exercise training and pulmonary rehabilitation.
- Technique matters — airway clearance should ideally be taught by a respiratory physiotherapist.
- National Aspergillosis Centre (NAC) patients can ask for advice from experienced physiotherapists who understand aspergillosis.
Contents
- Why physiotherapy matters in aspergillosis
- Airway clearance and mucus management
- Active Cycle of Breathing Technique (ACBT)
- Other physiotherapy techniques
- Pulmonary rehabilitation and exercise
- Breathing retraining and breathlessness
- Where to get physiotherapy in the UK
- Useful NHS videos and guides
- When to seek medical advice
Why physiotherapy matters in aspergillosis
Many people with aspergillosis have underlying lung conditions that affect how the lungs clear mucus, expand during breathing and cope with exertion. Long-term illness can also lead to muscle weakness, reduced fitness and loss of confidence with activity.
Common problems include:
- thick or persistent mucus
- frequent coughing
- breathlessness on exertion
- fatigue
- reduced walking distance
- weakness after illness or hospital admission
- poor posture from chronic breathlessness or coughing
- anxiety around breathing
- dysfunctional breathing patterns
Physiotherapy aims to improve function and quality of life. It is often most useful when it is personalised to the patient’s lung condition, symptoms, fitness level and treatment plan.
Airway clearance and mucus management
Some people with aspergillosis produce mucus every day. This is particularly common in people who also have bronchiectasis, asthma, Aspergillus bronchitis or repeated chest infections.
Mucus that remains in the lungs can contribute to:
- blocked or narrowed airways
- more coughing
- chest tightness
- breathlessness
- fatigue
- recurrent infections
Respiratory physiotherapists can teach airway clearance techniques to help move mucus from smaller airways towards larger airways, where it can be cleared more easily by huffing or coughing.
Active Cycle of Breathing Technique (ACBT)
ACBT stands for Active Cycle of Breathing Technique. It is one of the most commonly used airway clearance methods in respiratory physiotherapy.
It usually includes three parts:
- Breathing control – gentle relaxed breathing to settle the airways.
- Deep breathing exercises – larger breaths to help air move behind mucus.
- Huffing – a controlled breath out through an open mouth to move mucus upwards.
ACBT can often be adapted depending on symptoms, oxygen levels, energy, breathlessness and the amount of mucus being produced.
Other physiotherapy techniques
Huffing
A huff is a controlled breath out through an open mouth and throat. It can move mucus without the effort of repeated hard coughing. Many patients find huffing less exhausting than forceful coughing.
Postural drainage
Postural drainage uses body position and gravity to help drain mucus from different parts of the lungs. It may not be suitable for everyone, especially people with reflux, severe breathlessness, frailty, oxygen requirements or certain heart and lung complications.
Positive Expiratory Pressure and oscillating devices
Some patients may be advised to use airway clearance devices such as Flutter®, Acapella® or Aerobika®. These devices create resistance or vibration during breathing out, helping to loosen mucus and keep the airways open.
Breathing control
Breathing control can help settle the breathing pattern, reduce panic during breathlessness and make airway clearance less tiring.
Posture and mobility work
Chronic coughing and breathlessness can affect posture. Physiotherapy may include stretching, shoulder mobility, chest wall movement, gentle strengthening and exercises to improve comfort when breathing.
Fatigue management and pacing
Fatigue is common in aspergillosis. Physiotherapists may help patients pace activities, avoid “boom and bust” patterns, and gradually rebuild function without triggering prolonged exhaustion.
Pulmonary rehabilitation and exercise
Pulmonary rehabilitation is a structured programme of exercise and education for people with long-term lung disease who experience breathlessness. NHS England describes pulmonary rehabilitation as an exercise and education programme for people with lung disease who have symptoms of breathlessness.
Programmes may include:
- supervised exercise
- walking or cycling
- strength training
- breathing advice
- education about managing long-term lung disease
- confidence-building around activity
For aspergillosis patients, pulmonary rehabilitation may be particularly useful when breathlessness, weakness or reduced activity are affecting daily life.
Breathing retraining and breathlessness
Some people feel very breathless even when oxygen levels are normal or near normal. This can happen because breathlessness is influenced by airway inflammation, muscle effort, anxiety, breathing pattern, air trapping and the brain’s perception of breathing discomfort.
Breathing retraining may include:
- slower, calmer breathing
- diaphragmatic breathing
- pursed-lip breathing
- relaxation techniques
- coordinating breathing with walking, stairs or other activity
These techniques can be especially useful for patients who feel frightened by breathlessness or who have developed an inefficient breathing pattern.
Where to get physiotherapy in the UK
Access to physiotherapy varies across the UK, but patients with long-term lung disease may be able to obtain support through several routes.
1. Through your GP or respiratory team
Your GP, respiratory consultant, specialist nurse or hospital team may be able to refer you to a respiratory physiotherapist, community respiratory team or pulmonary rehabilitation service.
2. Through pulmonary rehabilitation services
Many local NHS pulmonary rehabilitation services accept referrals for people with chronic respiratory disease, including conditions such as Chronic Obstructive Pulmonary Disease (COPD), bronchiectasis, asthma, interstitial lung disease and other long-term breathing problems. Some services accept GP referrals, hospital referrals or self-referrals, but criteria vary locally.
3. Through community respiratory teams
Some areas have community respiratory teams that provide assessment, education, pulmonary rehabilitation, breathlessness support, oxygen-related advice and airway clearance support.
4. Through hospital respiratory physiotherapy departments
Hospital respiratory physiotherapists often support patients during admissions, after exacerbations, or through specialist outpatient respiratory clinics.
5. Through the National Aspergillosis Centre
National Aspergillosis Centre (NAC) patients can ask their NAC team whether specialist physiotherapy advice would be helpful. NAC has experienced physiotherapists who understand aspergillosis and the particular problems patients may face, including mucus clearance, breathlessness, fatigue, reduced fitness and co-existing lung disease.
6. Private physiotherapy
Some patients choose to see a private physiotherapist. The NHS advises that private physiotherapists should be chartered and registered with the Health and Care Professions Council (HCPC). The Chartered Society of Physiotherapy provides a “Find a Physio” directory that can be searched by location and specialty.
Useful UK links:
- National Aspergillosis Centre Physiotherapy
- NHS: Physiotherapy
- NHS England: Pulmonary rehabilitation
- Chartered Society of Physiotherapy: Find a physiotherapist
- Association of Chartered Physiotherapists in Respiratory Care
Useful NHS videos and guides
The following NHS resources may help patients understand airway clearance techniques. They should not replace individual advice from a respiratory physiotherapist.
Royal Free London NHS Foundation Trust – Active Cycle of Breathing
A clear patient-focused demonstration of ACBT.
Watch: Active Cycle of Breathing – Royal Free London NHS Foundation Trust
NHS Greater Glasgow & Clyde – Active Cycle of Breathing
A detailed demonstration from respiratory physiotherapy services.
Watch: Respiratory Physiotherapy Service – Active Cycle of Breathing
University College London Hospitals NHS Foundation Trust – breathing and airway clearance videos
UCLH has a useful set of patient information videos covering breathing exercises and airway clearance.
Watch: UCLH patient information videos – breathing exercises
UCLH – How to clear phlegm from your chest
A short, practical NHS video explaining how ACBT can help clear phlegm.
Watch: How to clear phlegm from your chest – ACBT
Cambridge University Hospitals NHS Foundation Trust
A patient information page explaining airway clearance and ACBT.
Read: Airway clearance – Active Cycle of Breathing Technique
Hull University Teaching Hospitals NHS Trust
A detailed patient leaflet on ACBT as a secretion clearance technique.
Read: Active Cycle of Breathing Technique – secretion clearance
University Hospitals Plymouth NHS Trust
A step-by-step patient guide to breathing control, thoracic expansion exercises and huffing.
Read: Active Cycle of Breathing Technique
When to seek medical advice
Airway clearance techniques should ideally be taught by a respiratory physiotherapist. Incorrect technique may sometimes worsen coughing, fatigue, airway irritation or breathlessness.
Seek medical advice urgently if you develop:
- new or worsening coughing of blood
- sudden worsening breathlessness
- chest pain
- fever or signs of infection
- dizziness or fainting
- significant oxygen desaturation
- rapid deterioration after starting a new exercise or airway clearance routine
Summary
Physiotherapy can be an important supportive treatment for some people with aspergillosis. It may help with mucus clearance, breathlessness, posture, fatigue, strength, confidence and activity levels.
Techniques such as ACBT, huffing, breathing control, postural drainage, airway clearance devices and pulmonary rehabilitation can all help selected patients. The best approach depends on the person’s symptoms, underlying lung condition and overall health.
For NAC patients, specialist physiotherapy advice is available from professionals experienced in aspergillosis care. If mucus clearance, breathlessness or reduced activity are becoming difficult, it is worth asking the NAC team whether physiotherapy input may help.
Medical note: This article is for general information only. It does not replace advice from your doctor, specialist nurse or respiratory physiotherapist. Airway clearance and exercise plans should be tailored to the individual patient.
Last reviewed: May 2026
When Breathlessness Feels Severe — Even When Oxygen Levels Look “Normal”

Many people living with aspergillosis, severe asthma, bronchiectasis, or other chronic lung conditions describe a confusing and sometimes frightening experience:
“My oxygen saturations are normal, my peak flow is reasonable, there’s little wheeze, but I still feel like I’m drowning.”
This can be distressing for patients and frustrating for carers. Some people feel that because their oxygen levels or breathing tests appear “acceptable”, their symptoms are not fully understood.
Importantly, severe breathlessness can occur even when standard measurements such as oxygen saturations and peak flow readings appear relatively normal.
This does not mean the symptoms are imaginary or “all in the mind”. Breathlessness is complex and can have many different causes.
Why Breathlessness Is More Complicated Than Oxygen Levels
When doctors or nurses assess breathing problems, they often check:
- Oxygen saturation levels (sats)
- Peak flow readings
- Respiratory rate
- Presence of wheeze
- Chest sounds
These are all important. However, they do not always reflect how breathless a person feels.
Some people with chronic respiratory illness may have:
- Normal oxygen saturations
- Reasonable peak flow readings
- Little visible wheeze
- Minimal mucus production
…yet still experience intense sensations of:
- air hunger
- tight chest
- difficulty taking a satisfying breath
- feeling unable to “fill the lungs”
- panic associated with breathing
- extreme fatigue from breathing effort
What Can Cause This?
Breathlessness in aspergillosis and chronic lung disease is often caused by several factors happening together.
Inflammation and Airway Sensitivity
Conditions such as Allergic Bronchopulmonary Aspergillosis (ABPA), Severe Asthma with Fungal Sensitisation (SAFS), bronchiectasis, and Chronic Pulmonary Aspergillosis (CPA) can all cause inflamed and hypersensitive airways.
The lungs may feel irritated or tight even if oxygen exchange remains relatively preserved.
Small Airways Dysfunction
Some breathing problems occur in the smaller airways of the lungs and may not always show clearly on basic tests such as peak flow.
Patients can feel significant chest tightness or air trapping despite “good numbers”.
Muscle Fatigue
Breathing takes muscular effort. Chronic respiratory illness can place a long-term strain on the chest wall and breathing muscles, leading to exhaustion and increased awareness of breathing.
Mucus and Airflow Changes
Even relatively small amounts of mucus or airway narrowing can create sensations of chest heaviness or difficulty moving air.
Breathing Pattern Dysfunction (Dysfunctional Breathing)
This is increasingly recognised in people with chronic respiratory illness.
When breathing becomes difficult over months or years, people may unconsciously develop altered breathing patterns, including:
- rapid shallow breathing
- upper chest breathing
- frequent sighing
- over-breathing (hyperventilation)
- muscle tension around the chest and neck
This can worsen symptoms and create a vicious cycle where the sensation of breathlessness becomes amplified.
Symptoms may include:
- air hunger
- dizziness
- tingling
- tight chest
- panic sensations
- difficulty “switching off” breathing awareness
Importantly, this does not mean the illness is psychological or “not real”. Dysfunctional breathing can happen alongside genuine lung disease.
Why Inhalers Sometimes Seem to Help Less
Reliever inhalers such as salbutamol (Ventolin) are designed mainly to relax tightened airways.
If breathlessness is being driven partly by breathing pattern dysfunction, muscle fatigue, inflammation, hypersensitivity, or air trapping, inhalers may not always provide dramatic relief.
This can be confusing and upsetting for patients.
“But My Tests Are Normal…”
Many patients feel frustrated, frightened, or even dismissed when told that oxygen levels, peak flow readings, or chest examinations are “fine” despite severe breathlessness.
Normal oxygen saturations are reassuring in terms of immediate danger, but they do not always reflect the full experience of chronic respiratory illness.
Breathlessness is influenced by many factors including inflammation, airway sensitivity, breathing effort, muscle fatigue, anxiety associated with struggling to breathe, and altered breathing patterns.
Because of this, some people may feel profoundly breathless even when routine measurements appear relatively stable.
It can sometimes help to explain symptoms in practical, functional terms, such as:
- “I become breathless walking across the room.”
- “I recover much more slowly than usual.”
- “This feels much worse than my normal baseline.”
- “I feel exhausted by the effort of breathing.”
- “Breathing exercises seem to help settle things.”
These descriptions may help healthcare professionals understand how symptoms are affecting day-to-day life, rather than focusing only on oxygen levels or peak flow numbers.
Some patients also find it helpful to ask questions such as:
- Could breathing pattern dysfunction be contributing?
- Would respiratory physiotherapy help?
- Would pulmonary rehabilitation be appropriate?
- How should I judge when symptoms need urgent assessment?
Importantly, severe breathlessness should never simply be ignored. New, worsening, or unusual symptoms still require proper medical assessment.
At the same time, many people with chronic lung disease experience very real symptoms that are not always fully reflected by routine measurements alone.
Why Breathlessness Can Feel So Frightening
The sensation of breathlessness is created by the brain interpreting signals from the lungs, breathing muscles, chest wall, blood chemistry, and nervous system.
This means that the feeling of “not getting enough air” is not determined only by oxygen levels.
In chronic lung disease, several things can trigger the sensation of breathlessness, including:
- inflamed or sensitive airways
- extra effort needed to move air in and out
- air trapping in the lungs
- muscle fatigue
- rapid or shallow breathing
- stress hormones released during breathing distress
- heightened awareness of breathing sensations
When breathing becomes uncomfortable, the body naturally responds with anxiety and adrenaline. This is a protective survival response.
Unfortunately, this can sometimes create a cycle:
breathlessness → anxiety → faster breathing → more chest tightness → worse breathlessness
This does not mean symptoms are “psychological”. The physical sensation is real, but the body’s alarm systems can unintentionally amplify it.
What Can Help During an Episode of Breathlessness?
Different techniques help different people, and severe or rapidly worsening symptoms should always be medically assessed. However, some patients find the following approaches helpful during episodes of distressing breathlessness:
Slow the Breathing Rate
Trying to slow breathing gently can help reduce over-breathing and chest tightness.
Some people find it helpful to:
- breathe in gently through the nose
- breathe out slowly through pursed lips
- focus on making the out-breath longer than the in-breath
Use a Recovery Position
Sitting forward slightly with the arms supported on knees or a table can sometimes reduce the work of breathing.
Reduce Panic and “Air Hunger”
Trying to fight for bigger and bigger breaths can sometimes worsen symptoms.
Some patients find it more helpful to focus on:
- gentle breathing rhythm
- relaxing the shoulders and neck
- slowing breathing rather than deepening it
- focusing attention away from the chest where possible
Use Prescribed Treatments Appropriately
Follow the advice provided by your healthcare team regarding inhalers, nebulisers, airway clearance, or rescue medication.
If inhalers are not helping as expected, this should be discussed with a respiratory specialist rather than simply increasing use repeatedly.
Know Your “Usual” Pattern
Many patients find it useful to learn the difference between:
- their “usual” chronic breathlessness
- breathing pattern dysfunction or over-breathing episodes
- symptoms suggesting infection or acute deterioration
This can help patients feel more confident recognising when urgent medical assessment may be needed.
Can Breathing Retraining Help?
Some patients find breathing retraining exercises very helpful, especially when guided by:
- respiratory physiotherapists
- specialist breathing services
- pulmonary rehabilitation teams
- asthma nurse specialists
Breathing retraining may include:
- slowing breathing rate
- diaphragmatic (“belly”) breathing
- nasal breathing techniques
- recovery breathing positions
- relaxation techniques
- paced activity and pacing strategies
Some NHS respiratory teams recommend online breathing resources and guided exercises to help patients recognise and manage over-breathing patterns.
These approaches are usually intended to work alongside medical treatment — not instead of it.
Living With an “Invisible” Symptom
One of the hardest aspects of chronic breathlessness is that outward signs may not always match how severe symptoms feel internally.
Many patients report feeling dismissed when oxygen levels are normal or when tests appear “better than expected”.
The experience of breathlessness is real, even when routine measurements do not fully explain it.
This is one reason why specialist respiratory assessment can be important in complex conditions such as aspergillosis.
When to Seek Medical Help
You should seek urgent medical advice if breathlessness is:
- suddenly worsening
- associated with chest pain
- causing blue lips or fingertips
- associated with falling oxygen saturations
- accompanied by fever or signs of infection
- causing confusion or severe exhaustion
- significantly different from your usual symptoms
Even if previous episodes have been related to breathing pattern dysfunction, new or worsening symptoms should still be medically assessed.
Further Support
You may also find these resources helpful:
Last reviewed: May 2026
Produced by: National Aspergillosis Centre CARES Team / Aspergillosis Website
Mental Health Awareness Week: Supporting the Emotional Impact of Aspergillosis

Mental Health Awareness Week is a reminder that health is not only physical.
For people living with aspergillosis, and for the family members and carers who support them,
the emotional impact of a long-term lung condition can be significant.
Aspergillosis can bring uncertainty, fatigue, breathlessness, repeated appointments,
medication changes, worries about test results, and concerns about the future.
It is understandable that some people experience anxiety, low mood, frustration,
isolation, or disturbed sleep.
Carers may also feel under pressure. Supporting someone with a chronic illness can be rewarding,
but it can also be tiring and emotionally demanding. Looking after your own mental health is not selfish;
it helps you continue to support the person you care about.
Small steps can help
- Talk to someone you trust about how you are feeling.
- Stay connected with friends, family, or peer support groups.
- Pace your activities and allow time for rest.
- Try gentle movement if this is safe and manageable for you.
- Write down worries or questions before appointments.
- Ask your healthcare team for support if anxiety, low mood, or stress is affecting daily life.
You are not alone
Many people with aspergillosis find it helpful to speak with others who understand what it is like
to live with a rare fungal lung condition. Peer support can reduce isolation and help patients and carers
feel more informed and understood.
The National Aspergillosis Centre and associated patient organisations provide support, information,
and opportunities to connect with others affected by aspergillosis:
- Aspergillosis support resources for families and carers
- Weekly aspergillosis support meetings
- Aspergillosis Support Facebook group
When to seek help
If you are feeling persistently overwhelmed, very low, anxious, unable to cope,
or if your mental health is affecting your day-to-day life, please speak to your GP,
specialist nurse, or healthcare team. Mental health support is an important part of healthcare.
If you feel at immediate risk of harming yourself, or you do not feel safe,
seek urgent help by calling emergency services or going to your nearest emergency department.
More information about Mental Health Awareness Week is available from the
Mental Health Foundation
Your mental health matters. Support, understanding, and connection can make a difference.
Weekly aspergillosis research update: papers published 4–12 May 2026
This week’s PubMed search for aspergillosis identified several new papers relevant to aspergillosis diagnosis, treatment, host-pathogen biology, allergic bronchopulmonary aspergillosis (ABPA), invasive pulmonary aspergillosis (IPA), and chronic pulmonary aspergillosis (CPA).
Key themes this week
- Bronchoscopic intervention in invasive pulmonary aspergillosis: a Chinese clinical analysis reports on bronchoscopic features and interventional therapy in IPA.
- ABPA guidance and imaging: one expert consensus paper and one adult asthma imaging study add to the ABPA literature.
- Diagnostics: new papers discuss galactomannan biology, metagenomic next-generation sequencing, and radiological assessment.
- Complex invasive fungal infection: several case-based reports highlight diagnostic difficulty in mixed or unusual fungal infections.
- Antifungal pharmacology: a real-life cohort study examines isavuconazole pharmacokinetics and pharmacodynamics.
Allergic bronchopulmonary aspergillosis (ABPA)
Expert consensus on ABPA diagnosis and treatment using integrated traditional Chinese and western medicine
Allergy Committee of Chinese Association of Integrative Medicine.
Zhonghua Yi Xue Za Zhi. 2026 May 12;106(17):1678-1695.
doi: 10.3760/cma.j.cn112137-20260101-00001
PMID: 42103676
This Chinese expert consensus addresses diagnosis and treatment of allergic bronchopulmonary aspergillosis. The abstract notes that ABPA is a hypersensitivity lung disease triggered by sensitisation to Aspergillus fumigatus or other Aspergillus species, with reported incidence of 1.0–3.5% in asthma patients and 7–15% in cystic fibrosis patients.
Why it matters: Although this is a Chinese-language consensus document and includes integrated traditional Chinese and western medicine approaches, it may still be useful to track because international consensus documents can show how ABPA recognition and management are evolving globally.
Radiological manifestations of ABPA in adult asthmatic patients
Wahab F, Hussain Babar T, Nadeem SF, Amin Z, Sarwar S, Ahmad S, Wahab A, Mukhtar S.
Monaldi Archives for Chest Disease. 2026 May 7. Online ahead of print.
doi: 10.4081/monaldi.2026.3648
PMID: 42099257
This paper focuses on radiological findings in adults with asthma and allergic bronchopulmonary aspergillosis. The PubMed abstract describes ABPA as developing through type I or type III hypersensitivity reactions to filamentous fungi such as Aspergillus.
Why it matters: Imaging remains central to recognising ABPA complications such as bronchiectasis, mucus plugging and other structural airway changes. Papers that improve recognition of radiological patterns may help reduce diagnostic delay in patients labelled as having difficult asthma alone.
Invasive pulmonary aspergillosis (IPA) and complex fungal infection
Clinical analysis of comprehensive bronchoscopic interventional therapy for invasive pulmonary aspergillosis
Li J, Cai CL, Zhao LN, Wang YH, Mu XD.
Zhonghua Jie He He Hu Xi Za Zhi. 2026 May 12;49(5):555-560.
doi: 10.3760/cma.j.cn112147-20250719-00420
PMID: 42108177
This Chinese-language clinical analysis investigates bronchoscopic features of invasive pulmonary aspergillosis and summarises the clinical efficacy of comprehensive bronchoscopic interventional therapy. Underlying conditions in the reported cases included diabetes mellitus and haematological malignancy.
Why it matters: Bronchoscopy can contribute both diagnostically and therapeutically in selected patients with IPA, particularly where airway obstruction, fungal plaques, necrotic material or local complications are present. This paper may be of interest to clinicians managing complex IPA cases.
Fatal triple co-infection with Aspergillus, Mucorales and Nocardia in aplastic anaemia
Sadeghi Borkehim S, Azhdari Tehrani H, Javandoust Gharehbagh F, Kord M, Azimi M, Alavi Darazam I.
BMC Infectious Diseases. 2026 May 9.
doi: 10.1186/s12879-026-13190-0
PMID: 42106631
This case report describes a fatal triple co-infection involving Aspergillus, Mucorales and Nocardia in a patient with aplastic anaemia.
Why it matters: In severely immunocompromised patients, invasive fungal disease may not occur in isolation. Mixed infections can complicate diagnosis, delay targeted treatment and require broader microbiological investigation than would be needed for a single-pathogen infection.
Cladribine treatment in pulmonary Langerhans cell histiocytosis complicated by invasive aspergillosis
Piekarczyk P, Pajer M, Kupis W, Wojda E, Nowicka U, Radzikowska E.
Polish Archives of Internal Medicine. 2026 May 4. Online ahead of print.
doi: 10.20452/pamw.17292
PMID: 42100864
This free article reports cladribine treatment in a young patient with isolated progressive pulmonary Langerhans cell histiocytosis complicated by invasive aspergillosis. No abstract was available in the PubMed record.
Why it matters: This appears to be a highly specialised case, but it highlights the intersection between rare lung disease, immunomodulatory treatment and risk of invasive fungal infection.
Invasive pulmonary aspergillosis in an apparently immunocompetent host
Beeravolu HR, Ghewade B, Alone V, Mummaneni R, Patil PA.
Respiratory Medicine Case Reports. 2026 Apr 27;61:102425. eCollection 2026.
doi: 10.1016/j.rmcr.2026.102425
PMID: 42088316
This case report describes invasive pulmonary aspergillosis in an immunocompetent host. Although IPA classically occurs in immunocompromised patients, the authors note that it can occasionally occur without obvious immunosuppression, which may contribute to diagnostic delay.
Why it matters: Case reports of IPA in apparently immunocompetent patients should be interpreted cautiously, but they are useful reminders that clinical context, imaging, microbiology and disease trajectory all matter when assessing possible invasive fungal infection.
Diagnostics, biomarkers and fungal biology
Structure and biosynthetic mechanisms of galactomannans in filamentous fungi
Oka T, Kadooka C, Tanaka Y, Hira D.
Biochimica et Biophysica Acta - General Subjects. 2026 May 7;1870(8):130960. Online ahead of print.
doi: 10.1016/j.bbagen.2026.130960
PMID: 42105885
This review focuses on galactomannans in filamentous fungi. Galactomannan contains mannose and galactofuranose; galactofuranose is absent in humans and is clinically important because galactomannan detection is used in the diagnosis of invasive pulmonary aspergillosis.
Why it matters: Galactomannan is one of the best-known fungal biomarkers in aspergillosis diagnostics. Understanding its structure and biosynthesis helps explain both the value and limitations of galactomannan-based testing.
Metagenomic next-generation sequencing for severe influenza complicated by invasive pulmonary aspergillosis
Niu S, Guo L, Li Z, Liu Y, Zhao L.
Frontiers in Cellular and Infection Microbiology. 2026 Apr 21;16:1746504. eCollection 2026.
doi: 10.3389/fcimb.2026.1746504
PMID: 42093770
This study evaluates the diagnostic performance of metagenomic next-generation sequencing for detecting invasive pulmonary aspergillosis in patients with severe influenza.
Why it matters: Influenza-associated pulmonary aspergillosis is increasingly recognised in critically ill patients. Rapid molecular methods such as metagenomic next-generation sequencing may help identify fungal infection earlier, although interpretation requires care because detection of fungal DNA does not always prove invasive disease.
Antifungal treatment and pharmacology
Real-life pharmacokinetics and pharmacodynamics of isavuconazole
Guidi M, Couchepin J, Reinhold I, Kronig I, Neofytos D, Schreiber PW, André P, Buclin T, Lamoth F.
JAC-Antimicrobial Resistance. 2026 May 5;8(3):dlag071. eCollection 2026 Jun.
doi: 10.1093/jacamr/dlag071
This paper reports real-life pharmacokinetic and pharmacodynamic data for isavuconazole, an antifungal used in invasive aspergillosis and mucormycosis.
Why it matters: Real-world pharmacology studies are important because antifungal exposure can vary between patients. Better understanding of drug levels, exposure-response relationships and clinical outcomes may help refine antifungal monitoring and dosing strategies.
Aspergillus species, virulence and non-human disease
Pathogenic mechanisms of Aspergillus lentulus infection in Galleria mellonella
Zhang L, Ji M, Hasimu H, Abliz P.
Mycopathologia. 2026 May 9;191(3):51.
doi: 10.1007/s11046-026-01072-7
PMID: 42105125
This experimental study investigates pathogenic mechanisms of Aspergillus lentulus infection using Galleria mellonella larvae, focusing on oxidative stress and tissue damage.
Why it matters: Aspergillus lentulus is a clinically important cryptic species within the Aspergillus fumigatus complex and may show reduced susceptibility to some antifungals. Model systems such as Galleria mellonella can help explore fungal virulence mechanisms before moving into more complex models.
Antemortem diagnosis of aspergillosis in a gentoo penguin
Matsumoto N, Itoh M, Toyotome T, Watanabe K, Yamada M, Hagino K, Neo S, Yamada K.
Journal of Veterinary Medical Science. 2026 May 7. Online ahead of print.
doi: 10.1292/jvms.25-0377
PMID: 42091553
This veterinary case report describes antemortem diagnosis of aspergillosis in a gentoo penguin using computed tomography and air sac fluid aspiration.
Why it matters: Aspergillosis is an important disease in birds, particularly captive penguins. Although not directly relevant to human clinical care, veterinary aspergillosis studies can contribute to understanding host susceptibility, environmental exposure and diagnostic approaches across species.
Related respiratory and microbiome research
The gut microbiome in cystic fibrosis
Marsh R, Tricker JM, Delhaes L, Bomberger JM, van der Gast C.
Journal of Cystic Fibrosis. 2026 May 9. Online ahead of print.
doi: 10.1016/j.jcf.2026.05.003
PMID: 42108153
This review discusses recent findings and future opportunities relating to the gut microbiome in cystic fibrosis.
Why it matters: This is not primarily an aspergillosis paper, but cystic fibrosis is an important context for allergic bronchopulmonary aspergillosis and airway fungal colonisation. Microbiome research may eventually help clarify how bacterial, fungal and host factors interact in chronic airway disease.
Summary
This week’s most directly relevant papers include new work on bronchoscopic management of invasive pulmonary aspergillosis, ABPA consensus and imaging, galactomannan biology, molecular diagnosis in influenza-associated pulmonary aspergillosis, and real-world isavuconazole pharmacology. Several case reports also underline the continuing diagnostic difficulty of invasive fungal disease, particularly in complex or immunocompromised patients.
Join our UK Citizen Science Project on Damp Homes and Health

Many people living with aspergillosis, asthma and chronic lung disease tell us they are worried about damp, mould and housing conditions — but often struggle to know:
- whether their home really has a problem
- who to trust for advice
- whether mould testing is reliable
- and what effective remediation should involve.
There is currently considerable uncertainty around indoor mould assessment, air sampling and interpretation of results. Many patients report difficulty obtaining clear, independent advice or meaningful remediation.
At the same time, we still know surprisingly little about the real-life health impact of living in damp homes across the UK.
A UK Citizen Science Project
We are supporting a UK citizen science project exploring how damp homes may affect health, including respiratory health and conditions such as aspergillosis.
Citizen science projects involve members of the public helping researchers and healthcare communities better understand real-world problems by sharing experiences and observations.
You do not need to have diagnosed aspergillosis to take part.
We are interested in hearing from people:
- living in damp or mouldy homes
- living in homes without damp
- with respiratory conditions
- and without respiratory conditions.
The initial registration takes about 1 minute and simply records your interest in the project.
Why this matters
By taking part, you may help improve understanding of:
- damp homes and respiratory disease
- mould exposure
- indoor air quality
- housing conditions
- challenges with mould assessment and remediation
- and the wider health impact of dampness in UK homes.
We hope the project will help patients, clinicians, housing professionals and researchers better understand:
- how people experience damp homes in real life
- the difficulties many people face obtaining reliable advice
- the limitations of current mould assessment approaches
- and what practical interventions may genuinely improve health and quality of life.
Related information
You can also read our practical guide discussing damp homes, mould testing, remediation and tenant support:
Read our guide to damp, mould and aspergillosis
Find out more or register your interest
Damp Homes and Health Study UK
Please share this project with:
- patients and carers
- healthcare professionals
- housing professionals
- damp and mould specialists
- environmental health professionals
- researchers
- and anyone interested in improving understanding of damp homes and health.
Damp, Mould and Aspergillosis: A Practical Guide for Patients Worried About Their Home
People with aspergillosis, asthma, bronchiectasis, chronic lung disease, allergies, or a weakened immune system are often understandably concerned about whether dampness or mould in the home could be affecting their health.
This guide explains:
- what signs to look for
- what practical steps may help
- the limitations of mould air testing
- who is most likely to provide reliable professional help
- and what support may be available for tenants.
Key points
- Dampness and mould can matter for people with respiratory disease.
- The most important question is usually: why is moisture present?
- Air sampling and mould spore counts have major limitations and should not be relied on alone.
- A “normal” air test does not reliably prove that a home is free from damp or hidden mould.
- The best assessments usually focus on building defects, condensation, ventilation, leaks and moisture sources.
- For complex problems, experienced chartered building professionals and occupational/environmental hygienists are often more useful than simple “mould testing” services.
- Dust and dirt accumulation may contribute to mould growth and respiratory irritation, especially in damp environments.
- Recent UK housing guidance increasingly recognises the health impact of damp and mould.
Why damp and mould matter
Fungi are a normal part of the environment. Tiny fungal spores are present in outdoor air, soil, gardens, compost and many indoor spaces. Most people breathe in small numbers of spores every day without becoming ill.
However, persistent dampness indoors can allow mould growth to increase. This may worsen irritation, allergy, asthma symptoms or respiratory symptoms in some people.
People who may be more sensitive include those with:
- Allergic Bronchopulmonary Aspergillosis (ABPA)
- Chronic Pulmonary Aspergillosis (CPA)
- Severe Asthma with Fungal Sensitisation (SAFS)
- bronchiectasis
- Chronic Obstructive Pulmonary Disease (COPD)
- cystic fibrosis
- severe asthma
- significant allergies
- or a weakened immune system.
Signs your home may have a damp problem
Visible signs
- black, green or white mould growth
- condensation on windows
- damp patches
- peeling wallpaper or paint
- bubbling plaster
- staining on walls or ceilings
- warped wood
- persistent condensation
Smell
A persistent musty, earthy or “damp” smell can sometimes indicate hidden moisture or mould growth, even when little is visible.
Possible building causes
- leaks from roofs, gutters or plumbing
- poor ventilation
- condensation
- cold external walls
- thermal bridging
- rising damp
- penetrating damp
- blocked air vents
- drying clothes indoors without enough ventilation.
Can dust and dirt make mould problems worse?
Yes. Accumulated dust and dirt can sometimes contribute to indoor mould problems, especially when combined with moisture or high humidity.
Dust is not simply “dirt” — it often contains:
- skin cells
- textile fibres
- pollen
- bacteria
- fungal spores
- organic material
- and microscopic debris.
When dust accumulates in damp or poorly ventilated areas, it can provide nutrients that allow mould growth to establish more easily on surfaces.
This is particularly common:
- behind furniture placed against cold walls
- around windows
- on curtains and blinds
- inside wardrobes
- under beds
- around ventilation grilles
- and in areas with condensation.
For people with asthma, allergy or aspergillosis, heavy dust accumulation may also worsen irritation or respiratory symptoms independently of visible mould.
Symptoms that may be triggered or worsened
Damp or mould exposure may contribute to:
- coughing
- wheezing
- chest tightness
- breathlessness
- increased sputum
- nasal irritation
- sinus symptoms
- eye irritation
- fatigue
- worsening asthma control
- increased allergy symptoms.
Symptoms may be more noticeable in certain rooms, overnight, during winter, after rainfall, or when ventilation is poor.
However, symptoms alone cannot prove that mould exposure is the cause. Many respiratory conditions can cause similar symptoms, so medical advice is important if symptoms are worsening.
Should you get air testing done?
Many companies offer indoor air sampling, mould spore counts or fungal testing. Patients often hope this will provide reassurance or proof that a home is safe.
Unfortunately, air sampling has important limitations.
Limitations of air sampling
- There are no universally agreed “safe” mould spore levels for homes.
- Results can vary enormously throughout the day.
- Outdoor air can strongly influence indoor results.
- Cleaning, vacuuming, opening windows or walking around can alter results.
- A short air sample may not represent usual exposure.
- Hidden damp or mould may not show up in an air sample.
- A “normal” air test does not reliably prove that a building is free from damp or mould problems.
Air sampling may sometimes be useful when carried out by experienced specialists as part of a wider investigation. However, it should not be used as the only basis for deciding whether a home is safe or whether remediation has worked.
What usually matters most?
The key question is usually:
Why is moisture present in the home?
Without moisture, significant mould growth usually cannot continue. Therefore, the most important step is to identify and correct the source of dampness.
This may involve:
- repairing leaks
- improving ventilation
- reducing condensation
- correcting insulation or thermal bridging problems
- repairing gutters, roofs or plumbing
- addressing overcrowding or excessive indoor humidity.
What you can do yourself
Improve ventilation
- Use extractor fans in bathrooms and kitchens.
- Open windows when practical and safe.
- Do not block air vents.
- Ventilate after showering, cooking or drying clothes.
Reduce indoor humidity
- Dry clothes outdoors where possible.
- Use lids on pans while cooking.
- Avoid drying clothes on radiators without ventilation.
- Consider a humidity monitor.
- Aim to avoid persistently high indoor humidity.
A dehumidifier may help reduce humidity in some situations, but it does not fix the underlying cause of dampness if there is a leak, structural defect or ventilation problem.
Reduce dust accumulation
- Clean regularly using methods that minimise dust disturbance.
- Pay particular attention to hidden or poorly ventilated areas.
- Move furniture slightly away from cold external walls where possible.
- Reduce clutter that traps dust and moisture.
- Wash soft furnishings and curtains regularly if practical.
Clean small areas carefully
Small areas of surface mould can sometimes be cleaned carefully using appropriate cleaning products. Avoid dry brushing or actions that disturb mould and release spores into the air.
People with significant lung disease, severe asthma, severe allergy or aspergillosis may prefer somebody else to carry out cleaning to reduce exposure.
Large, recurring or hidden mould problems usually need professional assessment.
Who is most likely to provide reliable help?
The most useful professionals are usually those who investigate the building and the source of moisture, not just the air.
For complex damp or mould problems, more robust help may come from:
- experienced chartered building surveyors
- building pathology specialists
- chartered building engineers
- occupational hygienists
- environmental hygienists with experience in indoor air quality and moisture assessment.
Relevant UK professional bodies
- Royal Institution of Chartered Surveyors (RICS)
- Chartered Institute of Building (CIOB)
- Chartered Association of Building Engineers (CABE)
- British Occupational Hygiene Society (BOHS)
Some damp and remediation companies may also be associated with the Property Care Association (PCA). This may indicate relevant industry training, but membership alone does not guarantee expertise. Experience and independence still matter.
Is impartial advice available?
Sometimes. People are often unsure where to obtain trustworthy, independent advice about damp and mould.
Possible sources of impartial guidance may include:
- local council Environmental Health departments
- housing officers (for tenants)
- Citizens Advice services
- NHS guidance
- UK Health Security Agency (UKHSA) guidance
- recognised professional bodies.
Local councils may sometimes inspect severe housing conditions, particularly where:
- children or vulnerable adults are involved
- landlords are failing to act
- there is extensive visible mould
- or housing conditions may present health hazards.
Support varies considerably between areas, and services are often stretched, but councils can sometimes require landlords to take action where housing conditions are unsafe.
Awaab’s Law and what it may mean for tenants
For people living in rented accommodation, especially social housing, recent changes in UK housing law may provide stronger protection where damp and mould problems are affecting health.
Awaab’s Law was introduced following the death of two-year-old Awaab Ishak in Rochdale after prolonged exposure to severe mould in social housing.
The law strengthens expectations that social landlords:
- investigate damp and mould complaints promptly
- assess potential risks to health
- carry out repairs within defined timescales
- and respond more urgently where vulnerable people are involved.
This is particularly important for people with:
- aspergillosis
- asthma
- bronchiectasis
- Chronic Obstructive Pulmonary Disease (COPD)
- cystic fibrosis
- or weakened immune systems.
What tenants should do
If you are concerned about damp or mould in rented accommodation, it may help to:
- report problems formally and in writing where possible
- keep photographs and dates
- record repeated complaints
- document worsening conditions
- keep copies of correspondence
- retain relevant medical letters if symptoms are worsening.
Where severe respiratory disease is present, medical evidence may help demonstrate vulnerability and the need for urgent action.
Important limitations
Awaab’s Law does not mean that every mould problem becomes an emergency or that all homes can be repaired immediately. Housing shortages, structural problems, funding limitations and contractor delays still affect what can be achieved.
However, the law has strengthened the expectation that damp and mould complaints should be taken seriously and addressed promptly, particularly where vulnerable people are affected.
NICE guidance and UK guidance
The National Institute for Health and Care Excellence (NICE) has increasingly recognised the importance of indoor air quality and housing conditions in respiratory health.
In addition, the UK Health Security Agency (UKHSA) has published major guidance emphasising that:
- damp and mould should be addressed promptly
- visible mould should not be ignored
- people with respiratory disease may be more vulnerable
- and simply blaming lifestyle alone is often inappropriate.
Recent UK guidance has increasingly shifted away from treating damp and mould purely as cosmetic issues, recognising their potential health impacts — especially for vulnerable people.
Questions to ask before paying for an assessment
- What qualifications and experience do you have in damp, mould and building moisture problems?
- Are you independent, or do you also sell remediation work?
- Will you investigate moisture sources, ventilation and building defects?
- Will I receive a written report explaining the likely cause?
- How will you decide whether remediation has worked?
- Will you explain the limitations of any air sampling?
- Do you use air sampling as part of a wider assessment, or as the main test?
Be cautious if...
- the assessment mainly consists of a quick air sample
- dramatic health claims are made
- the report presents spore counts as a simple “safe/unsafe” result
- expensive remediation is recommended immediately
- the company creates pressure to buy treatment packages
- there is little attention to leaks, condensation, ventilation or building defects.
How do you know remediation has worked?
Success should usually be judged by practical outcomes, including:
- visible mould has been removed safely
- the source of moisture has been corrected
- damp patches are drying out
- musty smells have reduced
- ventilation has improved
- humidity is better controlled
- mould does not quickly return
- symptoms improve over time, where mould exposure was contributing.
Repeat air sampling alone is not a reliable way to prove that a home is safe.
When to seek medical advice
People with aspergillosis or other lung conditions should seek medical advice if they experience:
- worsening breathlessness
- coughing blood
- rapidly worsening asthma symptoms
- fever or signs of infection
- unexplained weight loss
- significant deterioration in chest symptoms
- new or worsening fatigue with chest symptoms.
If symptoms appear linked to a damp or mouldy environment, discuss this with your healthcare team. They may not be able to assess the building, but they can help assess your health and whether your respiratory condition is changing.

Related information on Aspergillosis.org
- Reducing mould exposure
- Damp homes and health study
- What is aspergillosis?
- Living with aspergillosis
- Patient information hub
Useful resources
- UK Health Security Agency: Damp and mould guidance
- NICE: Indoor air quality at home
- NICE: Excess winter deaths and illness and the health risks associated with cold homes
- UK Government: Awaab’s Law factsheet
- Shelter UK: Damp and mould in rented homes
- Citizens Advice: Housing disrepair
Sir David Attenborough at 100: Inspiring Wonder in Nature and Fungi

Celebrating 100 years of Sir David Attenborough and his extraordinary contribution to understanding nature, fungi and the living world.Today marks the 100th birthday of David Attenborough — a remarkable milestone for someone who has spent a lifetime helping the world see nature differently.
For many of us interested in fungi and aspergillosis, his work has also helped shine a light on a kingdom of life that was too often overlooked. Through documentaries exploring fungi, moulds, forests and hidden ecosystems, he helped bring the extraordinary world of fungi into homes around the globe — revealing not just beauty, but the vital role fungi play in life on Earth.
At a time when awareness of fungal disease and environmental mould exposure remains so important, that contribution matters greatly.
Happy 100th Birthday Sir David — and thank you for a century of curiosity, education and wonder.
Blue inhalers, combination inhalers and aspergillosis: what patients need to know
Blue reliever inhalers, such as salbutamol or Ventolin, remain important medicines and can be lifesaving during asthma symptoms or an asthma attack. However, asthma guidelines have changed because doctors now recognise that relying too heavily on a blue inhaler can be a sign that the underlying airway inflammation is not being well controlled.
What is a blue inhaler?
A blue inhaler usually contains a medicine called a short-acting beta2 agonist, often shortened to SABA. Salbutamol is the best-known example.
These inhalers work quickly by relaxing the muscles around the airways. This can relieve wheeze, chest tightness and breathlessness within minutes. However, a blue inhaler does not treat the airway inflammation that often drives asthma symptoms.
You can read more about reliever inhalers from Asthma + Lung UK.
Why are asthma guidelines changing?
Asthma is not just a condition of narrowed airways. It is also an inflammatory condition. A reliever inhaler may make breathing feel easier for a short time, but if inflammation is not treated, asthma may remain poorly controlled.
Frequent use of a blue reliever inhaler can therefore be a warning sign. It may mean that asthma treatment needs reviewing, especially if someone is needing their reliever often, waking at night, having flare-ups, or finding their normal activities limited.
The updated NICE/BTS/SIGN asthma guideline supports greater use of treatment plans that combine symptom relief with anti-inflammatory treatment.
What are AIR and MART inhalers?
Some patients are now prescribed a combination inhaler that contains:
- a fast-acting reliever medicine to open the airways
- an inhaled corticosteroid to reduce inflammation
These approaches are known as:
- AIR – Anti-Inflammatory Reliever
- MART – Maintenance and Reliever Therapy
With these plans, the combination inhaler may be used when symptoms occur. In MART, it is also used regularly every day as maintenance treatment.
The important difference is that when symptoms increase, the patient receives more anti-inflammatory treatment as well as more reliever medicine. This aims to reduce the cycle of worsening symptoms, repeated blue inhaler use, and untreated inflammation.
Useful patient information is available from Asthma + Lung UK on AIR inhalers and MART inhalers.
Does this mean everyone should stop using their blue inhaler?
No. This is the most important point.
The new guidance does not mean that every patient must immediately stop using a blue inhaler. It also does not mean that blue inhalers are “bad” or banned.
For many people, nothing will change straight away. Some patients will remain on their current inhalers. Others may be changed to an AIR or MART plan after review by their GP, asthma nurse or respiratory specialist.
Will some patients have their blue inhaler taken away?
Sometimes, but not always.
If a patient is moved onto an AIR or MART plan, their combination inhaler may become both their preventer and their reliever. In that situation, they may no longer routinely need a separate blue inhaler.
However, some patients may still keep a blue inhaler as backup, and others may continue with separate preventer and reliever inhalers. This depends on the individual patient, their diagnosis, their inhalers, and their asthma action plan.
Not all combination inhalers can be used as relievers. Only specific inhalers containing a fast-acting medicine such as formoterol are suitable for AIR or MART use. Patients should only use inhalers in this way if they have been specifically prescribed and instructed to do so.
Why this is more complicated for aspergillosis patients
People with aspergillosis-related lung disease often have more complex respiratory problems than standard asthma alone.
This may include:
- ABPA (Allergic Bronchopulmonary Aspergillosis)
- severe asthma with fungal sensitisation
- bronchiectasis
- mucus plugging
- chronic airway infection or fungal colonisation
- reduced lung reserve or scarring
For these patients, breathlessness is not always caused by asthma-type inflammation alone. It may also be related to mucus, infection, bronchiectasis, fungal activity, or structural lung damage.
This means that simply taking more inhaler may not always address the real cause of worsening symptoms.
Steroids: useful but needing balance
Inhaled corticosteroids can be very helpful in asthma and ABPA because they reduce airway inflammation. Good control of inflammation may reduce symptoms, flare-ups and the need for oral steroid courses.
However, steroid exposure also needs careful management in aspergillosis patients. Higher steroid doses may increase the risk of side effects such as oral thrush and, in some situations, may affect the balance between inflammation control and fungal growth.
This does not mean patients should avoid inhaled steroids. It means that treatment should be individualised and reviewed by a clinician who understands the patient’s full lung condition.
What should aspergillosis patients do?
- Do not stop your blue inhaler suddenly if it has been prescribed for you.
- Do not change your preventer or steroid inhaler without medical advice.
- Check your own asthma action plan. Make sure you know which inhaler is for daily prevention and which one is for symptoms.
- Ask whether your combination inhaler is suitable for AIR or MART use. Do not assume that all combination inhalers can be used this way.
- Request a review if you are using your reliever inhaler frequently, symptoms are worsening, or you are unsure what to do.
When to seek urgent help
Seek urgent medical help if your breathlessness is severe, your reliever is not helping as expected, you are struggling to speak in full sentences, your lips or fingers look blue, or your symptoms are rapidly worsening.
Follow your personal asthma action plan. If you think you are having an asthma attack, do not delay seeking emergency help.
The key message
The new guidance is not simply about “taking away blue inhalers”. It is about recognising that asthma symptoms often reflect airway inflammation, and that some patients do better when symptom relief and anti-inflammatory treatment are given together.
For people with aspergillosis, the message is especially important: inhaler treatment should be reviewed in the context of the whole lung condition, not changed because of a headline.
If you are unsure about your inhalers, speak to your GP, asthma nurse, respiratory consultant or aspergillosis team.
Further reading
Dry Mouth, Aspergillosis and Dental Health
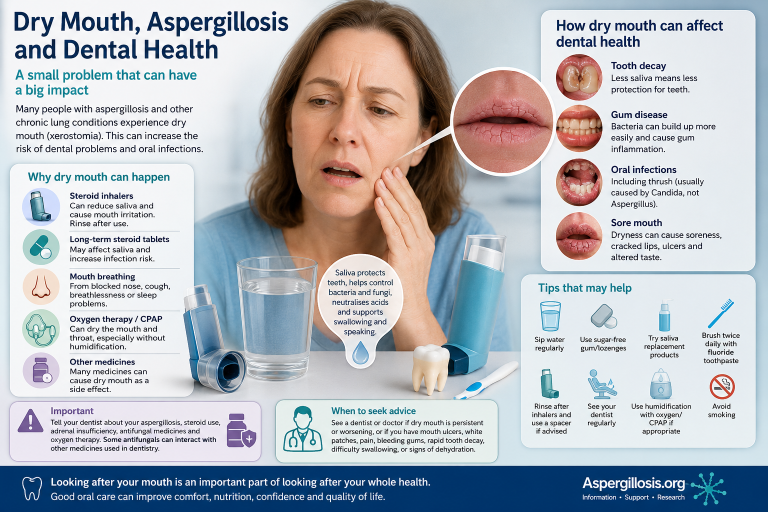
Why oral health problems may be more common than many patients expect
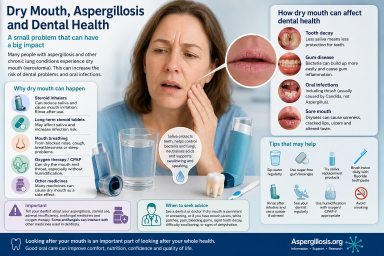
People living with aspergillosis often focus understandably on symptoms such as breathlessness, coughing, fatigue, wheezing or chest infections. However, many patients also notice problems affecting the mouth, throat and teeth — particularly dry mouth, soreness, altered taste and worsening dental health.
Although Aspergillus itself does not usually directly infect the mouth, the wider effects of chronic respiratory disease, medications and long-term treatment can sometimes have a significant impact on oral health and wellbeing.
Key points
- Dry mouth is commonly reported by patients with chronic respiratory disease and aspergillosis.
- Saliva is important for protecting teeth and gums.
- Steroid inhalers, mouth breathing and oxygen therapy can all contribute to dryness.
- Long-term dry mouth may increase the risk of tooth decay, gum disease and oral infections.
- Good oral hygiene and regular dental care are especially important.
- Dentists should be informed about antifungal medications and steroid treatment.
Why does dry mouth happen?
Dry mouth, sometimes called xerostomia, occurs when the mouth does not produce enough saliva or when saliva does not protect the mouth as effectively as usual.
Saliva plays several important roles. It helps protect teeth from decay, controls bacteria and fungi, reduces acidity in the mouth, supports swallowing and speech, and protects the delicate tissues inside the mouth.
When saliva levels fall, patients may notice:
- a sticky or dry feeling in the mouth;
- waking with a dry mouth;
- difficulty swallowing dry foods;
- sore gums, tongue or throat;
- bad breath;
- cracked lips;
- increased thirst;
- altered taste;
- mouth soreness or burning.
Why might aspergillosis patients be affected?
In many cases, the problem is not caused directly by Aspergillus itself. Instead, several factors linked to respiratory disease and treatment may combine together.
Steroid inhalers
Inhaled corticosteroids are commonly used in asthma, Allergic Bronchopulmonary Aspergillosis (ABPA), severe eosinophilic lung disease and other respiratory conditions.
These medicines are important and should not be stopped without medical advice, but they can sometimes contribute to mouth irritation, dryness, hoarseness, oral thrush and throat discomfort.
Using a spacer device, where appropriate, and rinsing the mouth after inhaler use may help reduce some local side effects.
Long-term steroid tablets
Some patients with aspergillosis or severe asthma have taken oral steroid tablets such as prednisolone, sometimes for prolonged periods. Long-term steroid exposure may affect immunity and can increase the risk of infections such as oral thrush.
Some patients may also develop adrenal suppression or adrenal insufficiency after prolonged steroid exposure. Patients with known adrenal insufficiency should make sure their dentist and healthcare team are aware before significant dental treatment or procedures.
Mouth breathing
Many people with chronic respiratory disease breathe through their mouth more often, especially overnight. This may happen because of blocked nose, sinus disease, breathlessness, coughing, asthma symptoms or poor sleep.
Over time, regular mouth breathing can dry the mouth and throat, especially during the night.
Oxygen therapy and CPAP
Supplemental oxygen and continuous positive airway pressure (CPAP) devices may dry the upper airways, particularly if humidification is not used.
Some patients notice dry lips, sore throat, dry nose, thick mucus or increased mouth discomfort overnight.
Medication side effects
A number of commonly prescribed medicines may contribute to dry mouth. These can include antihistamines, antidepressants, some pain medicines, bronchodilators and some blood pressure medicines.
The combined effect of several medicines may become significant, especially in people managing complex long-term health conditions.
Why does dry mouth matter for dental health?
Dry mouth is more than simply uncomfortable. Saliva normally helps protect the teeth and gums. Without enough saliva, plaque bacteria can grow more easily, acids remain in contact with teeth for longer, enamel may weaken and gums may become inflamed.
Some patients are surprised by how quickly dental problems can develop after periods of illness, long-term treatment or persistent dry mouth.
Possible problems include:
- tooth decay;
- gum disease;
- sensitive teeth;
- mouth ulcers;
- oral thrush;
- cracked lips;
- denture discomfort;
- difficulty eating or speaking comfortably.
Oral thrush and fungal infections
Patients with aspergillosis sometimes worry that oral fungal infections mean Aspergillus is spreading in the mouth. In most cases, oral thrush is caused by Candida yeast rather than Aspergillus.
Symptoms of oral thrush may include white patches, soreness, redness, altered taste, painful swallowing or cracking at the corners of the mouth.
Steroid inhalers and dry mouth can both increase the risk of thrush. Patients should seek medical or dental advice if symptoms persist or recur.
Important information for dentists
Patients should inform their dentist about:
- their aspergillosis diagnosis;
- inhaled or oral steroid use;
- adrenal insufficiency or adrenal suppression;
- antifungal medicines;
- oxygen therapy or CPAP use;
- significant breathlessness or difficulty lying flat.
This is important because some antifungal medicines, including itraconazole, voriconazole and posaconazole, can interact with other medicines. Dentists and doctors can help check for possible interactions when procedures, antibiotics, pain relief or sedation are being considered.
Practical tips that may help
Some patients find the following measures helpful:
- sip water regularly;
- avoid excessive alcohol and caffeine;
- use sugar-free gum or lozenges if suitable;
- ask a pharmacist or dentist about saliva replacement sprays, gels or mouthwashes;
- rinse the mouth after steroid inhalers;
- use a spacer device if recommended;
- brush twice daily with fluoride toothpaste;
- clean between teeth if able;
- attend regular dental reviews;
- avoid smoking;
- discuss persistent symptoms with a GP, dentist, pharmacist or specialist team.
Patients using oxygen or CPAP may wish to ask their respiratory team whether humidification is appropriate.
When to seek medical or dental advice
Seek advice if dry mouth is persistent, worsening or causing problems with eating, sleeping, swallowing or speaking.
Medical or dental review is particularly important if there are mouth ulcers, white patches, bleeding gums, rapid tooth decay, severe soreness, repeated oral thrush, signs of dehydration, dizziness or marked weakness.
Patients with adrenal insufficiency, severe respiratory disease or complex medication regimens should make sure healthcare professionals are aware before major dental procedures.
A commonly overlooked part of chronic illness
Living with aspergillosis often involves managing far more than lung symptoms alone. Dry mouth and dental health problems may seem minor at first, but over time they can affect comfort, nutrition, sleep, confidence, communication and overall quality of life.
Recognising these issues early may help patients seek support sooner and reduce longer-term complications.
Further information
Author and review information
Prepared by: National Aspergillosis Centre CARES Team / Aspergillosis Website Editorial Team
Last reviewed: May 2026
References and further reading
- NHS information on dry mouth and oral thrush.
- Dental and oral medicine guidance on xerostomia and prevention of tooth decay.
- Respiratory guidance on inhaled corticosteroids and inhaler technique.
- Medicines information for azole antifungals and corticosteroids.