The Power of Keeping a Health Diary When You Have Aspergillosis

Last reviewed: June 2026
Audience: People living with aspergillosis, families and carers
Key points
- A health diary can help you understand symptoms, triggers and changes over time.
- It can be especially useful if you experience fatigue, brain fog or memory problems.
- It can make clinic appointments more focused and productive.
- A diary may show progress that is hard to notice day to day.
- The best diary is simple, quick and realistic to keep using.
Contents
- Why keep a health diary?
- How it can help with aspergillosis
- Brain fog and memory
- Spotting patterns and triggers
- Using your diary at appointments
- The psychological benefit
- Simple diary template
- Common questions
- When to seek medical advice
Why keep a health diary?
Living with aspergillosis often means symptoms change from day to day. Some days may be manageable. Others may involve more coughing, breathlessness, fatigue, sinus symptoms, poor sleep or medication side effects.
Because these changes can happen gradually, it can be difficult to remember exactly when symptoms started, whether they are getting better or worse, or what might have triggered them.
A health diary gives you a simple record of what is happening over time. It can help you, your family and your healthcare team see patterns that may not be obvious from memory alone.
How a diary can help with aspergillosis
People with aspergillosis may find it useful to record:
- Cough
- Breathlessness
- Fatigue
- Sputum or phlegm
- Wheeze
- Sinus symptoms
- Sleep quality
- Exercise or walking distance
- Mood and wellbeing
- Medication changes
- Possible side effects
You may also want to note possible triggers, such as damp or mould exposure, pollen, dusty environments, changes in weather, respiratory infections, stress, travel or changes in medication.
Brain fog and memory
Many people with long-term lung conditions describe episodes of brain fog. This may feel like forgetfulness, poor concentration, difficulty finding words, feeling mentally slower than usual, or feeling as though your head is “empty”.
Brain fog can have many possible causes, including fatigue, poor sleep, infection, inflammation, stress, anxiety, pain, medication side effects, low oxygen levels or other health problems.
A diary acts as an external memory. Instead of trying to remember when something changed, you can look back and see what was happening at the time.
Spotting patterns and triggers
| What you record | What it may help show |
|---|---|
| Symptoms | Whether cough, breathlessness or fatigue are improving or worsening |
| Sleep | Whether poor sleep is linked to worse symptoms |
| Exercise | What level of activity is manageable |
| Weather | Whether heat, humidity, cold air or storms affect symptoms |
| Environment | Possible links with damp, mould, dust or pollen |
| Medication | Possible benefits, side effects or changes during dose reduction |
| Infections | Early warning signs or repeated patterns |
Using your diary at appointments
Healthcare professionals may ask questions such as:
- When did your symptoms start?
- Are they getting better or worse?
- Have you noticed any triggers?
- Have you changed any medication recently?
- How far can you walk now compared with before?
- Have you had any infections or courses of antibiotics?
These questions are not always easy to answer from memory, especially when you are tired or anxious. A diary can help you give clearer, more accurate information.
You may find it useful to bring a short summary to your appointment, such as:
- Three things that have improved
- Three things that have worsened
- Any medication changes
- Your main questions for the appointment
Sometimes the diary tells a different story
When you have had a difficult few days, it can feel as though nothing is improving. A diary may show that the wider picture is more encouraging.
For example, you may feel:
“Nothing has changed.”
But your diary may show:
- You are walking further than three months ago
- You are sleeping better
- You have had fewer chest infections
- You are coughing less at night
- You are doing more social activities
Equally, a diary can show gradual deterioration that might otherwise be missed. Both types of information can be useful.
The psychological benefit
Chronic illness can feel unpredictable. A diary can help restore a sense of control by changing the question from:
“Why do I feel awful?”
to:
“What changed recently?”
This can reduce uncertainty and help you feel more involved in your care.
A diary can also become a record of resilience. It may include difficult days, but it can also capture walks completed, holidays taken, family events attended, personal goals reached and challenges overcome.
Keep it simple
Many people stop keeping a diary because they try to record too much. A simple diary is usually more useful than a complicated one.
A daily entry might take less than two minutes and include:
- Symptoms, scored from 0 to 10
- Energy level, scored from 0 to 10
- Sleep quality
- Exercise or activity
- Medication changes
- Anything unusual
Consistency matters more than detail.
Paper, phone or app?
There is no single correct way to keep a diary. You could use:
- A notebook
- A printed diary sheet
- A phone notes app
- A calendar
- Voice notes
- A spreadsheet
- A symptom tracking app
- A fitness tracker or smartwatch
The best diary is the one you will actually use.
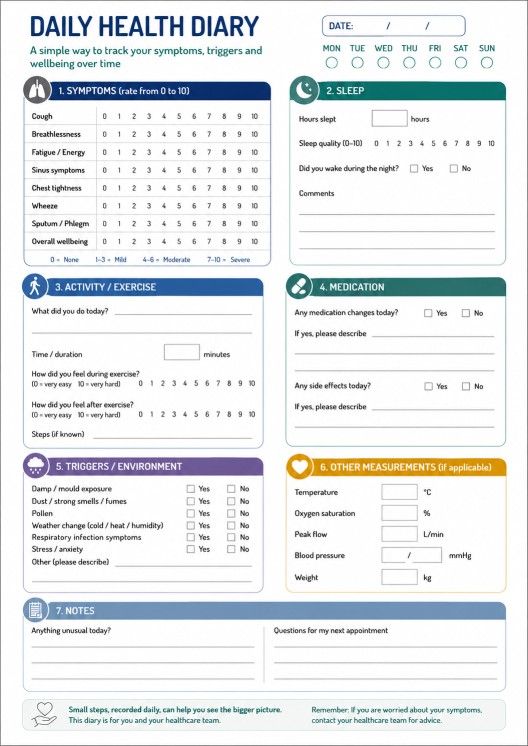
Simple diary template
Daily health diary
Date: __________________________
Symptoms, 0–10
Cough: ______
Breathlessness: ______
Fatigue: ______
Sinus symptoms: ______
Overall wellbeing: ______
Sleep
Hours slept: ______
Sleep quality, 0–10: ______
Activity
Exercise or activity today:
__________________________________________________
Medication
Any medication changes or side effects?
__________________________________________________
Notes
Anything unusual today?
__________________________________________________
__________________________________________________
Daily Diary - PDF downloadable
Common questions
Do I need to write every day?
No. Some people write daily. Others only record changes, flare-ups, medication changes or important events.
What if I forget for a few days?
That is very common. Simply restart when you remember. A diary does not have to be perfect to be useful.
Should I record test results?
You can if you find it helpful. Some people record blood results, oxygen saturations, lung function, weight, clinic letters or medication levels. Do not worry if this feels too much. A simple symptom diary is still useful.
Can a diary replace medical advice?
No. A diary is a tool to support conversations with your healthcare team. It should not be used to diagnose or treat symptoms without medical advice.
When to seek medical advice
Seek medical advice promptly if you experience:
- Sudden or significant worsening of breathlessness
- Coughing up large amounts of blood
- Persistent fever
- Severe chest pain
- New confusion or rapidly worsening brain fog
- Weakness, speech problems, facial drooping or visual changes
- Symptoms that are worsening quickly or feel unusual for you
If you are unsure, contact your healthcare team, NHS 111, your GP, or emergency services depending on severity.
Further information
- Living with aspergillosis
- Fatigue and aspergillosis
- Exercise and aspergillosis
- Mental wellbeing and aspergillosis
Author and review information
This article is provided for general educational support for people affected by aspergillosis. It is not a substitute for medical advice from your own healthcare team.
Prepared for: Aspergillosis.org
Last reviewed: June 2026
Do You Carry Your Aspergillosis Information With You?

New NHS Plans Could Help in Future – But What About Today?
The UK government is currently debating plans for a new NHS “single patient record” system. The aim is to allow authorised healthcare professionals to access important information from GP surgeries, hospitals, community services and other parts of the NHS more easily.
If implemented successfully, this could reduce the need for patients to repeatedly explain their medical history and could help emergency departments, ambulance crews and other healthcare professionals see important information such as diagnoses, medications, allergies and previous treatment.
For people living with aspergillosis and other long-term respiratory conditions, this could be especially valuable. However, these changes will take time to develop and introduce. For now, patients remain one of the most important links between different parts of the healthcare system.
Why This Matters for Aspergillosis Patients
Many people with aspergillosis receive care from several different services, including:
- General Practitioners (GPs)
- Local respiratory teams
- Specialist nurses
- Hospital clinics
- Emergency departments
- Pharmacists
- Community healthcare teams
- Specialist centres such as the National Aspergillosis Centre
Healthcare records are not always immediately available to every professional involved in your care. This means there may be times when you need to explain:
- What type of aspergillosis you have
- Which medications you take
- Any important allergies or serious drug reactions
- Whether you have adrenal insufficiency or take long-term steroids
- Who your specialist team is
- What previous treatments you have received
Having this information readily available can save time and may help healthcare professionals make decisions more quickly and safely.
What Information Should You Carry?
 You do not need to carry your entire medical record. A simple one-page health summary is usually enough.
You do not need to carry your entire medical record. A simple one-page health summary is usually enough.
1. Your Diagnosis
List your main diagnoses clearly. Examples include:
- Allergic Bronchopulmonary Aspergillosis (ABPA)
- Chronic Pulmonary Aspergillosis (CPA)
- Severe Asthma with Fungal Sensitisation (SAFS)
- Aspergillus Bronchitis
- Bronchiectasis
- Severe Asthma
- Chronic Obstructive Pulmonary Disease (COPD)
2. Your Current Medications
Include all current treatments, particularly:
- Antifungal medications, such as itraconazole, voriconazole, posaconazole or isavuconazole
- Steroid tablets
- Hydrocortisone replacement therapy
- Biologic therapies
- Inhalers
- Oxygen therapy
- Antibiotics you are currently taking
Try to keep this list up to date.
3. Drug Allergies and Serious Reactions
This is one of the most important sections. Include any known allergies or serious reactions, for example:
- Penicillin allergy
- Prednisolone allergy
- Previous severe drug reactions
- Medicines you have been told to avoid
4. Steroid or Adrenal Information
If you have adrenal insufficiency or are taking long-term steroid treatment, make this very clear.
I have adrenal insufficiency and may require emergency steroid treatment if seriously unwell.
Many patients already carry a steroid emergency card. If you have been advised to carry one, continue to carry it at all times.
5. Specialist Contact Information
Include:
- Consultant name
- Hospital or specialist centre
- Clinic or specialist nurse contact details, if available
6. Emergency Contact
Include:
- Name
- Relationship
- Telephone number
An Important Extra Note for Aspergillosis Patients
Many antifungal medications interact with other medicines. If you take itraconazole, voriconazole, posaconazole or isavuconazole, consider including the following statement on your health summary:
I take an azole antifungal medication. Please check for potential drug interactions before prescribing new medicines.
This simple statement may help avoid medication-related problems.
If You Are a National Aspergillosis Centre Patient: Using myMFT
If you are a patient of the National Aspergillosis Centre (NAC), you may already have access to some of your hospital information through the myMFT patient portal.
myMFT is the patient portal used by Manchester University NHS Foundation Trust (MFT), which includes Wythenshawe Hospital and the National Aspergillosis Centre.
Depending on the services you use, myMFT may allow you to:
- View MFT appointment details
- Access clinic letters
- Keep track of important test results, letters and health information
- Attend online video consultations
- Use proxy access to help manage a family member’s healthcare, with consent
Many patients find it useful to keep copies of important clinic letters on their phone or tablet. This can be particularly helpful if you attend another hospital, visit your GP, travel away from home or need emergency treatment.
myMFT does not replace a future NHS-wide patient record, but it can provide access to important information that may help you and your healthcare professionals manage your care more effectively.
Find out more about myMFT on the Manchester University NHS Foundation Trust website.
For Patients Not Under the National Aspergillosis Centre
If you are not an NAC or MFT patient, your local hospital may have its own patient portal or online record system. Ask your hospital clinic, respiratory team or GP surgery whether you can access clinic letters, appointment information or test results online.
You may also be able to use the NHS App to manage parts of your healthcare, depending on your GP surgery and local NHS services.
Find out more about the NHS App.
You may also find it useful to know your NHS number. You do not need to know your NHS number to receive NHS care, but it can be helpful when contacting services or completing forms.
Where Should You Keep Your Information?
Many patients choose to:
- Save a copy on their mobile phone
- Keep a printed copy in their wallet or handbag
- Store it alongside their steroid emergency card
- Keep a copy with travel documents
- Share a copy with family members or carers
- Keep copies of important clinic letters on their phone or tablet
The best system is the one that is easy to access when needed.
Printable options (Word documents):
Looking Ahead
The proposed NHS single patient record could eventually make it easier for healthcare professionals to access important information quickly and safely.
For patients with rare conditions such as aspergillosis, that could improve continuity of care, reduce delays and reduce the need to repeatedly explain complex medical histories.
Until then, carrying a simple summary of your condition remains one of the easiest and most effective ways to help healthcare professionals understand your health needs and provide appropriate care.
Key Points
- Carry a simple one-page health summary.
- Include diagnoses, medications, allergies and specialist contacts.
- Clearly state if you have adrenal insufficiency or take long-term steroids.
- Mention azole antifungal treatment and potential drug interactions.
- National Aspergillosis Centre patients may be able to access clinic information through myMFT.
- Patients outside MFT should ask whether their own hospital has a patient portal.
- Keep important information on your phone and consider carrying a printed copy.
- A future NHS single patient record may improve information sharing, but patients remain an important source of information today.
Common Questions
Do I need to carry all my clinic letters?
No. A concise one-page summary is usually more useful in an emergency. However, keeping copies of important clinic letters on your phone can be helpful.
What if I am treated at more than one hospital?
This is one of the main reasons to carry a health summary. Different healthcare providers may not always have immediate access to the same information.
Is this only useful in emergencies?
No. It can also help during GP appointments, outpatient visits, travel, planned hospital admissions and when seeing healthcare professionals unfamiliar with aspergillosis.
What if I am a National Aspergillosis Centre patient?
Consider registering for myMFT and keeping important clinic letters available on your phone or tablet for easy access.
What if I am not an NAC patient?
Ask your own hospital or respiratory clinic whether they offer a patient portal. You can also check what information is available through the NHS App.
When to Seek Medical Advice
Seek urgent medical advice if you experience:
- Significant worsening of breathlessness
- Chest pain
- Coughing up significant amounts of blood
- Symptoms of adrenal crisis if you have adrenal insufficiency
- Severe allergic reactions to medications
- Rapid deterioration in your respiratory symptoms
If you need emergency help, call 999. For urgent medical advice in the UK, use NHS 111.
Useful Links
- myMFT patient portal – Manchester University NHS Foundation Trust
- NHS App
- Find your NHS number
- Aspergillosis information and support
Frequently Asked Questions
What information should an aspergillosis patient carry in an emergency?
Patients should consider carrying a summary of their diagnosis, medications, allergies, steroid or adrenal information, specialist contacts and emergency contact details.
Should people with aspergillosis carry a medication list?
Yes. Many aspergillosis patients take antifungal medicines, steroids, biologic therapies and inhalers. An up-to-date medication list can help avoid prescribing errors and drug interactions.
What is myMFT?
myMFT is the patient portal used by Manchester University NHS Foundation Trust. It allows eligible patients to access appointments, clinic letters, test results and other healthcare information.
Can aspergillosis patients access their records online?
Some patients can access records through services such as myMFT, local hospital portals or the NHS App, depending on where they receive care.
What is the NHS single patient record?
The proposed NHS single patient record aims to improve information sharing between healthcare providers so patients do not need to repeatedly explain their medical history.
Author: National Aspergillosis Centre Patient Support Team
Reviewed by: National Aspergillosis Centre
Last reviewed: June 2026
Important: This article is intended for information only and should not replace advice from your healthcare team.
Exercise and Aspergillosis: How Physical Activity Can Improve Breathing, Strength and Wellbeing
Key points
- Exercise is one of the most helpful non-drug tools for many people living with aspergillosis.
- Regular physical activity can improve breathlessness, strength, stamina, mood, confidence and quality of life.
- The best approach is usually little and often, rather than occasional intensive exercise.
- Do not compare yourself with others. Everyone has different lungs, treatments, fitness levels and limits.
- Respiratory physiotherapists and pulmonary rehabilitation programmes can help you exercise safely and confidently.
- Walking, cycling, swimming, rowing, gentle yoga, Tai Chi and singing can all be useful, depending on the individual.
- People with aspergillosis should take extra care around mould-heavy environments such as compost, leaf mould, sheds and building dust.
Contents
- Why exercise matters in aspergillosis
- The activity and breathlessness cycle
- Benefits of exercise
- Specific issues for aspergillosis patients
- How to start safely
- Activities that may help
- Pulmonary rehabilitation and physiotherapy
- The golden rule: little and often
- What clinicians want patients to know
- Real-life examples
- When to seek medical advice
- Frequently asked questions
- Related articles and further support
Why exercise matters in aspergillosis
Living with aspergillosis can be physically and emotionally challenging. Breathlessness, coughing, fatigue, disturbed sleep, medication side effects and reduced confidence can all make it tempting to become less active.
Unfortunately, becoming less active can make symptoms feel worse over time. Muscles weaken, fitness falls, balance may worsen and everyday activities such as walking, climbing stairs, shopping or playing with grandchildren can become harder.
This process is often called deconditioning. It does not mean the symptoms are imaginary. It means the body has lost some of its ability to cope with activity.
The encouraging news is that exercise can help reverse part of this process.
Exercise cannot cure aspergillosis, but it can help the body use oxygen more efficiently, strengthen muscles, improve confidence and make daily life easier.
Importantly, people may feel better and do more even when their lung function tests do not change very much.
The activity and breathlessness cycle
Many people with chronic lung disease become trapped in a difficult cycle:
The deconditioning cycle
Breathlessness → Less activity → Loss of fitness → More breathlessness → Even less activity
Exercise helps by creating a healthier cycle:
The rebuilding cycle
Gentle activity → Stronger muscles → More confidence → Easier daily tasks → Better quality of life
This is why small, regular activity can be so powerful. The aim is not to force the lungs to work harder. The aim is to help the whole body work better.
Benefits of exercise
Improved breathlessness
Exercise may make you breathless while you are doing it, but regular activity often reduces breathlessness during everyday tasks. This happens because muscles become stronger and more efficient, so they need less effort to perform the same activity.
More energy
Many patients report feeling less tired once they build a regular routine. Exercise uses energy in the short term, but over time it can improve stamina and reduce the effort needed for daily life.
Stronger muscles
Long-term illness, hospital admissions, inactivity and corticosteroid treatment can all contribute to muscle weakness. Strength exercises can help rebuild leg strength, improve balance and support independence.
Better mood and confidence
Living with aspergillosis can affect mental wellbeing. Exercise can help reduce anxiety, stress and low mood. It can also restore a sense of control and achievement.
Improved bone health
This is especially important for people who have taken long-term corticosteroids. Weight-bearing activity and strength training can help protect bone strength and reduce the risk of osteoporosis.
Better daily function
For many patients, the most important benefit is practical: being able to walk further, climb stairs more easily, go shopping, travel, garden, socialise or enjoy family life with more confidence.
Specific issues for aspergillosis patients
Avoiding high mould exposure
Aspergillus is commonly found in soil, compost, decaying vegetation, damp buildings and dust. Some activities can expose people to large numbers of fungal spores.
Activities that may increase exposure include:
- Handling compost
- Turning soil
- Clearing leaf piles
- Wood chipping
- Spreading bark or mulch
- Cleaning sheds, garages, lofts or basements
- Working around mouldy materials
- Construction or demolition environments
Outdoor exercise such as walking, cycling and running is generally encouraged. However, it is sensible to avoid places where mould, compost, dust or decaying vegetation are being heavily disturbed.
Some people may choose to wear a well-fitting FFP2 or FFP3 mask for unavoidable dusty or mould-heavy tasks, but avoidance is usually better where possible.
Haemoptysis: coughing blood
People with Chronic Pulmonary Aspergillosis (CPA), lung cavities or aspergillomas may sometimes cough blood. This is called haemoptysis.
If you have recent, recurrent or significant haemoptysis, discuss exercise with your respiratory team. Most routine activity remains safe for many people, but vigorous exertion may need to be paused or modified during periods of active bleeding.
Oxygen levels
Some people with aspergillosis also have bronchiectasis, Chronic Obstructive Pulmonary Disease (COPD), fibrosis, previous tuberculosis damage or other lung scarring. In these situations, oxygen levels may fall during exertion even when resting oxygen levels are normal.
If breathlessness feels out of proportion, or if you notice unusually low oxygen saturations during activity, discuss this with your respiratory team. You may benefit from an exercise assessment or pulmonary rehabilitation referral.
Fatigue and boom-and-bust activity
Aspergillosis-related fatigue can be different from normal tiredness. It may be influenced by chronic inflammation, active infection, poor sleep, anxiety, medication side effects and reduced fitness.
Many patients experience a boom-and-bust pattern:
Good day → Do too much → Several days recovering
Regular, steady activity is usually more helpful than occasional bursts of intensive effort.
Steroid-related muscle weakness
People who have taken long-term corticosteroids may develop muscle weakness, particularly around the thighs and hips. This can make standing from a chair, climbing stairs and walking uphill more difficult.
Strength exercises such as sit-to-stands, step-ups and resistance band work can be particularly helpful.
Adrenal insufficiency
Some patients who have used long-term corticosteroids develop adrenal insufficiency. These patients should understand their sick day rules and discuss unusually strenuous exercise, endurance events or major hikes with their healthcare team.
Most routine gentle or moderate exercise is safe, but unusually demanding activity may require additional planning.
Asthma, ABPA and exercise symptoms
Many people with Allergic Bronchopulmonary Aspergillosis (ABPA) also have asthma. Exercise can sometimes trigger wheeze, cough or chest tightness.
This does not usually mean exercise should be avoided. Good asthma control, appropriate inhaler use, gradual warm-up and pacing can make a major difference. Speak to your healthcare team if exercise regularly triggers asthma symptoms.
How to start safely
Start from where you are
Your starting point is your starting point. It does not matter what someone else can do. If you can only walk for two or three minutes, that is still a valid place to begin.
Use the talk test
During moderate exercise, you should usually be able to speak in short sentences. If you cannot speak at all, you may be pushing too hard.
Build gradually
Small increases are usually safer and more sustainable than sudden changes. For example, increasing a walk from five minutes to six or seven minutes may be more helpful than trying to double it immediately.
Plan rest periods
Rest is not failure. Many people with lung disease do better with short bursts of activity separated by planned rests.
Track progress gently
Some patients find it motivating to keep a simple record of walks, steps, strength exercises or how breathless they feel. The aim is encouragement, not pressure.
A simple beginner example
Example starter plan
- Week 1–2: Walk for 5 minutes most days, or less if needed.
- Week 3–4: Add one or two minutes when comfortable.
- Week 5–6: Add gentle strength exercises, such as sit-to-stands.
- Ongoing: Continue gradual increases, with rest days when needed.
This is only an example. Some people will need to start lower, while others may safely start higher.
Activities that may help
The best exercise is usually the one you enjoy and can keep doing regularly.
Walking
Walking is one of the simplest and most effective activities. It requires no special equipment, can be adapted to most fitness levels and is easy to build gradually.
Cycling
Cycling, including use of a stationary exercise bike, can improve stamina while placing less strain on the joints than running.
Swimming
Swimming can be helpful because the water supports body weight. However, some people with asthma find chlorinated pools trigger symptoms.
Rowing
Rowing machines can provide both cardiovascular and strength benefits. Start gently and focus on technique.
Strength training
Strength training does not have to mean heavy weights. Useful exercises may include:
- Sit-to-stands from a chair
- Step-ups
- Wall push-ups
- Resistance bands
- Light hand weights
Gentle yoga and Tai Chi
Many patients enjoy gentle yoga or Tai Chi because they combine movement, balance, breathing awareness, posture and relaxation. Chair-based versions may be useful for people with reduced mobility.
Singing
Singing may not sound like exercise, but many people with lung conditions find it helpful. It can support breathing control, posture, confidence, social connection and respiratory muscle coordination.
Some patients enjoy local choirs or Singing for Lung Health groups.
Pulmonary rehabilitation and physiotherapy
You do not have to do this alone.
A respiratory physiotherapist can help assess your current ability and design a programme that suits your symptoms, fitness level and goals.
A specialist physiotherapist may help with:
- Breathlessness management
- Pacing strategies
- Strength and stamina building
- Airway clearance techniques where appropriate
- Confidence around movement
- Safe return to activity after illness
Pulmonary rehabilitation
Pulmonary rehabilitation is a structured programme that usually combines supervised exercise, education, breathing techniques and self-management advice.
Many people with chronic lung disease describe pulmonary rehabilitation as one of the most helpful interventions they have received.
If you have ongoing breathlessness, reduced exercise tolerance or loss of confidence, ask your GP, respiratory consultant, specialist nurse or physiotherapist whether pulmonary rehabilitation may be suitable for you.
The golden rule: little and often
Exercise with aspergillosis: the golden rule
Little and often is usually better than a lot all at once.
Do not compare yourself with other people, including other aspergillosis patients.
Everyone has different lungs, different treatments, different ages and different levels of fitness.
Focus on your own starting point and your own progress.
Do not try to keep up with others. You do you.
One of the biggest traps is comparing yourself with other patients. Someone else may complete a long-distance walk, climb a mountain, run a race or cycle hundreds of miles. That can be inspiring, but it should not become your target.
Instead, ask yourself:
Am I a little stronger, fitter or more confident than I was a few months ago?
Success may mean:
- Walking for five minutes when previously you could only manage three
- Climbing stairs more comfortably
- Shopping with less breathlessness
- Doing light gardening safely
- Enjoying a holiday more easily
- Playing with children or grandchildren
- Needing fewer rests during ordinary daily tasks
These achievements matter.
For most people living with aspergillosis, consistency beats intensity.
What clinicians want patients to know
Exercise is not about pushing through at all costs
Healthcare professionals usually want patients to remain as active as safely possible, but that does not mean ignoring symptoms or forcing yourself to keep up with others.
The safest approach is usually to build gradually, pace yourself and ask for help when symptoms change.
Exercise should support your life, not punish your body.
Real-life examples
The person who walks five minutes a day
For someone recovering from illness or a hospital admission, a five-minute daily walk may be a major achievement. If that becomes six minutes, then eight minutes, that is progress.
The person who completes a long-distance walk
Some people with aspergillosis manage major challenges such as long-distance walking routes. These stories can be inspiring, but they are not a standard everyone else must meet.
The person who joins a singing group
For some patients, a singing group may be more enjoyable and sustainable than a gym. Singing can support breathing control and confidence while also providing social contact.
The person who returns to gardening carefully
Gardening can be enjoyable and active, but compost, leaf mould and disturbed soil may contain high levels of fungal spores. Some patients adapt by avoiding compost handling, asking for help with mould-heavy tasks, wearing protective masks where appropriate, and choosing lower-risk gardening activities.
When to seek medical advice
Stop exercising and seek medical advice if you experience:
- Chest pain
- Severe or unusual breathlessness
- Dizziness or fainting
- Significant haemoptysis, meaning coughing blood
- Sudden worsening of symptoms
- New palpitations or heart rhythm symptoms
- Oxygen levels much lower than usual, if you monitor them
- Exercise tolerance that suddenly falls without an obvious reason
Always speak to your healthcare team if you are unsure whether exercise is safe for you, especially if your symptoms have recently changed.
Frequently asked questions
Can I exercise if I have aspergillosis?
Yes, many people with aspergillosis benefit from regular physical activity. Exercise should be adapted to your symptoms, fitness level and medical conditions. Ask your healthcare team for advice if you have severe breathlessness, recent haemoptysis or unstable symptoms.
Can exercise improve breathlessness?
Yes. Exercise can improve muscle efficiency, stamina and confidence. This can reduce breathlessness during everyday activities, even if lung function test results do not change significantly.
What is the best exercise for Allergic Bronchopulmonary Aspergillosis?
There is no single best exercise for Allergic Bronchopulmonary Aspergillosis. Walking, cycling, swimming, gentle yoga, strength training and pulmonary rehabilitation can all be helpful. The best activity is one you can do safely and regularly.
Can pulmonary rehabilitation help aspergillosis patients?
Many people with chronic respiratory symptoms, bronchiectasis or reduced exercise tolerance benefit from pulmonary rehabilitation. It combines supervised exercise, education, breathing techniques and self-management support.
Should people with aspergillosis avoid gardening?
Not necessarily, but some gardening activities can expose people to high levels of Aspergillus spores. Handling compost, turning soil, clearing leaves and working with mulch may carry higher exposure. Lower-risk gardening activities may be more suitable for some patients.
Can exercise help steroid-related muscle weakness?
Yes. Strength exercises can help rebuild muscle strength lost through long-term corticosteroid treatment, illness or inactivity. Simple exercises such as sit-to-stands, step-ups and resistance bands can be useful.
Is singing useful for people with lung disease?
Many people with lung disease find singing helpful for breathing control, posture, confidence and social connection. Some areas offer Singing for Lung Health groups.
Should I exercise when I am tired?
Gentle movement may help on some tired days, but severe fatigue may mean your body needs rest. Pacing is important. Try to avoid repeated boom-and-bust cycles where you do too much on a good day and then need several days to recover.
Take-home message
Exercise is one of the most powerful tools available to help people living with aspergillosis maintain independence, strength and quality of life.
Move more, but move at your own pace.
Find something you enjoy.
Ask for help when you need it.
Little and often beats heroic efforts.
Do not compare yourself with others.
You do you.
Related articles
You may also find these aspergillosis.org articles helpful:
- Why Am I Breathless When My Oxygen Levels Are Normal?
- Physiotherapy for Aspergillosis
- Living with Aspergillosis
- Managing Fatigue in Aspergillosis
- Steroids and Adrenal Insufficiency
- Bronchiectasis and Aspergillosis
- What is Allergic Bronchopulmonary Aspergillosis (ABPA)?
- What is Chronic Pulmonary Asprgillosis (CPA)?
Further support and information
Author and review information
Author: Graham Atherton, National Aspergillosis Centre
Medical review: National Aspergillosis Centre Clinical Team
Last reviewed: June 2026
This article provides general information and should not replace advice from your own healthcare team.
CBD Oil, Cannabis and Aspergillosis: Safety, Quality and Drug Interactions

Key points
- Some people with chronic illnesses report that CBD or cannabis products help with pain, anxiety, sleep or wellbeing.
- Evidence for benefit in aspergillosis itself remains limited.
- Smoking or vaping cannabis may irritate the lungs and may not be suitable for people with respiratory disease.
- CBD and cannabis products can interact with antifungal medicines and steroids.
- Product quality varies greatly, especially with over-the-counter or online products.
- Always let your healthcare team or pharmacist know about any CBD or cannabis products you are using.
Why this topic comes up
People living with aspergillosis often cope with long-term symptoms such as fatigue, chronic cough, breathlessness, pain or chest discomfort, anxiety, poor sleep, steroid side effects and reduced quality of life.
Because of this, discussions about CBD oil, cannabis or “medical marijuana” occasionally appear in patient groups and online communities. Some people report that these products help them cope better with symptoms or improve sleep and wellbeing.
At the same time, there are important safety issues that people with respiratory fungal disease should be aware of, particularly around lung irritation, product quality and drug interactions.
CBD and cannabis are not the same thing
CBD: cannabidiol
CBD, or cannabidiol, is one of the compounds found in cannabis plants. CBD products usually contain little or no THC, or tetrahydrocannabinol, the chemical responsible for the “high” associated with cannabis.
CBD products may be sold as oils, capsules, gummies, creams, drinks or food supplements. CBD is generally less intoxicating than THC-containing cannabis products.
Cannabis or marijuana
Cannabis products may contain varying amounts of THC. THC is more strongly associated with intoxication, impaired concentration, sedation, anxiety or panic, hallucinations or paranoia in some people, and impaired driving or coordination.
Different cannabis products can vary enormously in strength and purity.
What conditions have good evidence for medical cannabis?
Cannabis-based medicines are prescribed in some situations where evidence is reasonably strong.
In the UK, prescription cannabinoid medicines are mainly used for certain severe forms of epilepsy, chemotherapy-related nausea and vomiting, and muscle spasticity in multiple sclerosis. There is also ongoing research into chronic pain and palliative care use.
However, evidence for benefit in aspergillosis, bronchiectasis, asthma, allergic bronchopulmonary aspergillosis (ABPA) or chronic pulmonary aspergillosis (CPA) remains limited.
This does not mean that people never feel benefit. Some clearly do. But respiratory fungal disease is not currently one of the better-established medical indications.
Lung safety concerns in aspergillosis
This is probably the most important issue for many aspergillosis patients.
Smoking cannabis
Smoking any substance exposes the lungs to heat, particulates, irritants and combustion products.
For people who already have asthma, bronchiectasis, chronic lung infection, airway inflammation or fungal lung disease, this may worsen symptoms such as coughing, wheezing, chest tightness, mucus production or breathlessness.
Vaping
Some people assume vaping is automatically safer than smoking, but this is not always true.
Vaping can still irritate the airways and lungs, and the long-term effects are not fully understood. For people with fragile or inflamed lungs, clinicians are often cautious about recommending inhaled cannabis products of any kind.
Contamination and quality problems
One important issue is that cannabis and CBD products are not all produced to the same standards.
Product quality can vary greatly
Some products may contain more or less CBD or THC than stated, contain contaminants, contain pesticides or solvents, or vary significantly between batches.
This is especially true for unregulated products purchased online or from unofficial sources.
Mould contamination
Cannabis products can occasionally become contaminated with moulds, including Aspergillus species.
This is particularly concerning for immunocompromised patients, transplant patients, people on long-term steroids, and people with chronic lung disease.
Although this appears uncommon, it is one reason respiratory specialists are often cautious about smoked cannabis products in fungal disease patients.
Drug interactions: a very important issue
Many antifungal medicines are processed through liver enzyme systems that can also be affected by CBD or cannabis compounds. This means interactions are possible.
Antifungal medicines of concern
Potential interactions may occur with antifungals such as:
- itraconazole
- voriconazole
- posaconazole
- isavuconazole
These medicines already require careful monitoring because blood levels can vary significantly between people.
Adding CBD or cannabis products may potentially alter antifungal levels, liver metabolism or side-effect risks.
Steroids and other medicines
Interactions may also occur with prednisolone, methylprednisolone, opioid pain medicines, sleeping tablets, antidepressants and anti-anxiety medicines.
Possible effects may include increased sedation, dizziness, falls, confusion, liver irritation or worsening side effects.
This does not automatically mean the products are unsafe, but it does mean healthcare teams should know about them.
“Natural” does not always mean low risk
Many patients understandably assume that CBD products are “gentle” or “natural.”
However, natural products can still interact with prescription medicines, doses may be inconsistent, some products are poorly regulated, and side effects can still occur.
This is especially important in aspergillosis because patients are often already taking multiple medicines, including antifungals and steroids.
Why patients may still be interested
Despite the uncertainties, it is understandable why some patients explore these products.
People sometimes report improvement in sleep, anxiety, pain, appetite, overall wellbeing or coping with chronic illness. These experiences are real and important to acknowledge respectfully.
At present, however, there is still limited high-quality research specifically in aspergillosis and chronic fungal lung disease.
Practical safety advice
If someone chooses to use CBD or cannabis products, it is sensible to:
- tell their healthcare team or pharmacist,
- mention all supplements and oils being used,
- watch for new side effects after starting,
- avoid assuming “natural” means risk-free,
- be especially cautious with smoked or inhaled products,
- avoid driving or hazardous activities if feeling impaired.
When to seek medical advice
Medical review is important if new symptoms appear after starting CBD or cannabis products, especially:
- worsening breathlessness,
- severe drowsiness,
- confusion,
- hallucinations,
- jaundice,
- severe dizziness,
- palpitations,
- fever or worsening chest symptoms.
The bottom line
CBD and cannabis products are becoming more widely discussed in chronic illness communities, including among people with aspergillosis.
Some people report benefits for sleep, anxiety or quality of life, and there are a small number of medical conditions where prescription cannabis-based medicines are supported by stronger evidence.
However, for aspergillosis patients, important concerns remain around lung irritation, mould contamination, product quality, and interactions with antifungal medicines and steroids.
Because of this, healthcare teams are usually cautious and prefer open discussion rather than patients using these products without medical awareness.
Further information
- NHS guidance on medical cannabis
- Specialist pharmacist advice on antifungal interactions
- Specialist pharmacist advice on steroid interactions
- National Aspergillosis Centre resources on antifungal medicines
Author and review information
Prepared for aspergillosis patients and carers as general educational information. This article is not intended to replace personalised medical advice.
Last reviewed: May 2026
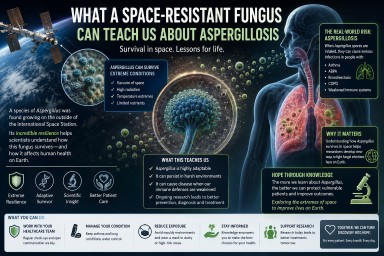
What a Space-Resistant Fungus Can Teach Us About Aspergillosis
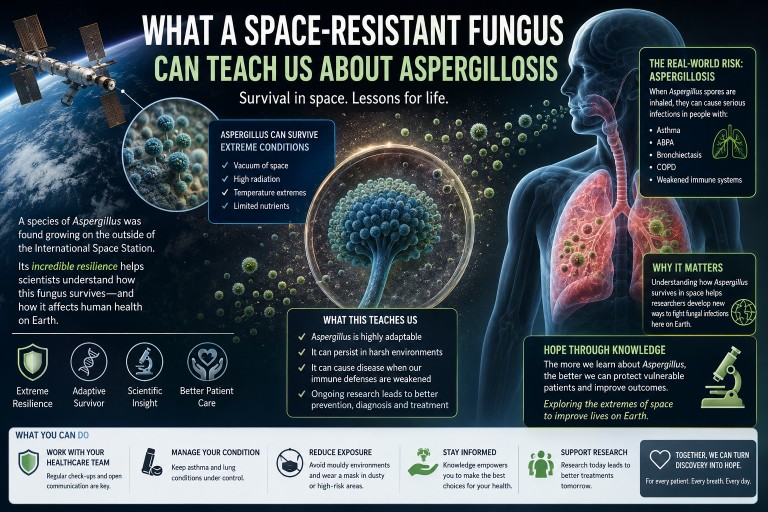
A recent Smithsonian article described how a microscopic fungus survived conditions designed to sterilise spacecraft. At first glance, this might sound like a story about space exploration rather than human health. But for people living with aspergillosis, it carries an important and surprisingly positive message.
Fungi are remarkable survivors
The article describes research showing that some Aspergillus spores can survive extreme conditions, including harsh radiation, dryness and cleaning procedures. This does not mean that aspergillosis patients need to worry about “space fungi”. Instead, it highlights something patients and specialists already understand very well: fungi are extraordinarily resilient organisms.
Aspergillus spores are common in the environment. They can be found in soil, compost, decaying leaves, dust, damp buildings and sometimes even very clean environments. Most people breathe in small numbers of spores every day without becoming ill, because their lungs and immune system clear them effectively.
For people with lung disease, asthma, immune system problems or damaged lung tissue, however, Aspergillus can sometimes cause illness. This includes conditions such as chronic pulmonary aspergillosis, allergic bronchopulmonary aspergillosis and severe asthma with fungal sensitisation.
A positive message for patients
One positive message from this research is that aspergillosis is not caused by weakness, poor hygiene or personal failure. Fungi are genuinely formidable organisms. If some fungal spores can survive environments as extreme as those used in space research, it becomes easier to understand why completely avoiding Aspergillus in everyday life is difficult.
This can be reassuring for patients who feel frustrated when symptoms persist despite doing “everything right”. It is not that they are failing. It is that fungal biology is complex, and fungal exposure is part of the natural world.
Why this matters emotionally
Many people with aspergillosis say they feel misunderstood. They may hear comments such as:
- “It’s only mould.”
- “Surely it should have cleared by now.”
- “Why are you still worrying about it?”
Stories like this help show that fungi are not simple or trivial. They are ancient, adaptable and scientifically fascinating organisms. Aspergillosis is therefore not “just mould exposure”; it is a real medical condition involving a complex interaction between the fungus, the lungs and the immune system.
Science is taking fungi more seriously
Another encouraging message is that fungi are attracting more scientific attention. Researchers are studying fungal survival, environmental spread, resistance to treatment, and the ways fungi interact with humans and indoor environments.
This matters because better understanding can lead to better diagnosis, better treatment and better prevention. In recent years, fungal medicine has already benefited from improvements in CT scanning, fungal blood tests, respiratory samples, antifungal treatments and biologic medicines for some allergic forms of disease.
Resilience goes both ways
The story also offers a useful reflection: fungi are resilient, but so are patients.
Many people living with aspergillosis adapt to long-term symptoms, hospital appointments, uncertainty, fatigue and treatment decisions. They continue to work, care for families, attend support groups, learn about their condition and help others understand fungal disease.
That resilience deserves recognition.
What patients can take from this
- Aspergillus is difficult to avoid completely, so exposure reduction should be realistic rather than perfectionist.
- Persistent symptoms are not a personal failure; fungal diseases can be complex and long-lasting.
- Fungal science is advancing, and aspergillosis is increasingly recognised as an important medical condition.
- Patients’ experiences are valid, even when others do not fully understand them.
When to seek medical advice
People with aspergillosis or suspected aspergillosis should seek medical advice if they develop worsening breathlessness, coughing up blood, unexplained weight loss, persistent fever, chest pain, a major change in sputum, or a significant deterioration in day-to-day symptoms.
Anyone already under specialist care should follow their agreed care plan and contact their clinical team if symptoms change significantly.
Further reading
- Smithsonian Magazine: fungus surviving spacecraft sterilisation conditions
- Aspergillosis.org: patient information and support
Last reviewed: May 2026
Living With Aspergillosis: When Others Do Not Fully Understand How You Feel

Living with aspergillosis can affect far more than the lungs. Many patients have symptoms that are difficult to explain, difficult to measure, and difficult for other people to fully understand.
Breathlessness, fatigue, coughing, chest tightness, sleep disruption, anxiety during flare-ups, medication side effects, and uncertainty about the future can all become part of daily life. These symptoms may fluctuate from day to day, and people may appear well at times even when they are struggling.
This can leave patients feeling misunderstood, dismissed, or even blamed for focusing too much on their health.
Key points
- Symptoms of aspergillosis and chronic lung disease are real, even when they are invisible to others.
- Feeling anxious, frustrated, or preoccupied with health is understandable when symptoms affect daily life.
- Validation from family, friends, and clinicians can reduce distress.
- Finding meaningful things to do beyond illness can also help patients cope.
- The aim is balance: being heard and supported, while also protecting quality of life.
Why aspergillosis can be hard for others to understand
Many people with chronic pulmonary aspergillosis (CPA), allergic bronchopulmonary aspergillosis (ABPA), severe asthma, bronchiectasis, or other long-term lung conditions live with symptoms that are not always visible.
A patient may look well, speak normally, or have reasonable oxygen levels at rest, but still experience severe fatigue, breathlessness on exertion, anxiety during breathing difficulty, or a long recovery after simple activities.
Symptoms may also fluctuate. Someone may manage an activity one day but be unable to do the same thing the next. This inconsistency can be confusing for family, friends, employers, and sometimes even healthcare professionals.
“Stop obsessing” is usually not helpful
Patients with chronic illness are sometimes told to “stop obsessing” about their health. This may be said with good intentions, but it can feel dismissive.
Patients may hear:
“You are making too much of this.”
or:
“It is all in your head.”
In reality, many patients are not choosing to focus on illness. The illness is already demanding attention through symptoms, medication routines, appointments, uncertainty, and changes to daily life.
However, there is also a useful point hidden inside the poor wording. Constantly monitoring every symptom can become exhausting and may increase anxiety. The better message is not “stop obsessing”, but:
“Your symptoms are real, but you also deserve space in your life that is not only about illness.”
Validation matters
Validation means recognising that a person’s experience is real and understandable. It does not mean agreeing that every symptom is dangerous, or that every worry needs urgent medical action.
Useful validating phrases include:
- “I believe you.”
- “That sounds exhausting.”
- “I know this affects much more than people can see.”
- “How is today compared with your usual baseline?”
- “What would help you most today?”
Validation can reduce distress. When patients feel dismissed, they may feel driven to repeat themselves, seek reassurance, or prove how unwell they are. When they feel heard, they may find it easier to step back from constant symptom monitoring and focus on other parts of life.
The mind and body interact
Breathlessness is not just a physical sensation. It can trigger fear very quickly. This is a normal human response: breathing difficulty naturally makes the brain more alert to danger.
This does not mean symptoms are imaginary. It means chronic respiratory illness affects the whole person: physically, emotionally, socially, and psychologically.
Anxiety, uncertainty, poor sleep, and repeated flare-ups can all increase awareness of symptoms. At the same time, genuine physical symptoms can increase anxiety. The two can reinforce each other.
Recognising this interaction can help patients and clinicians work together without blame.
Finding something else to think about can help
For many patients, finding meaningful activities beyond illness is genuinely helpful. This might include hobbies, gentle exercise, time outdoors, music, crafts, reading, gardening, photography, volunteering, family activities, or peer support.
This is not the same as ignoring illness. It is a way of protecting identity and quality of life.
The aim is not to deny symptoms, but to prevent illness becoming the only focus of every day.
“Your illness is real, but it should not be allowed to take over every part of who you are.”
What families and friends can do
Family members and friends may not be able to fully understand what chronic aspergillosis feels like. They do not need perfect understanding to be supportive.
Helpful support includes:
- believing the person’s symptoms are real;
- recognising that fatigue and breathlessness may not be visible;
- avoiding dismissive comments;
- asking what would help rather than assuming;
- understanding that symptoms may fluctuate;
- encouraging enjoyable activities without pressuring the person to “push through”.
Less helpful comments include:
- “You look fine.”
- “You were able to do it yesterday.”
- “You need to stop thinking about it.”
- “Everyone gets tired.”
What clinicians may be trying to say
Sometimes clinicians may say things such as “try not to focus on it too much” because they believe further tests or treatments may not currently help. They may be trying to avoid unnecessary antibiotics, steroids, scans, or procedures.
That can be a reasonable clinical concern, but the message needs to be communicated carefully.
A better way to say it might be:
“I believe your symptoms are real and distressing. We will continue to look for changes that need treatment. At the same time, some symptoms may persist despite treatment, so we also need to support your quality of life.”
This keeps the patient heard, while also being honest about the limits of medical treatment.
Practical ways to find balance
- Use structured symptom tracking: a brief daily note may be more helpful than constant checking.
- Know your baseline: understanding what is normal for you makes changes easier to spot.
- Agree an action plan: ask your healthcare team what changes should prompt medical advice.
- Protect non-illness time: plan small, realistic activities that are not centred on health.
- Use peer support carefully: support groups can reduce isolation, but try to avoid constant comparison or fear-based searching.
- Ask for emotional support: counselling, psychological therapies, pulmonary rehabilitation, or breathing physiotherapy may help some people.
When to seek medical advice
This article is general information and does not replace medical advice. Patients should seek medical help if they experience significant or worrying change, especially:
- worsening breathlessness;
- falling oxygen saturations if they monitor them;
- new or worsening chest pain;
- coughing up blood;
- high fever, rigors, or signs of serious infection;
- new confusion, fainting, or severe weakness;
- rapid deterioration from their usual baseline;
- symptoms that feel different from their usual pattern.
If symptoms are severe or rapidly worsening, urgent medical help should be sought.
Final thought
Living with aspergillosis can be physically and emotionally demanding. Patients deserve to be believed, heard, and supported. At the same time, they also deserve help to build a life that is not entirely defined by illness.
A helpful message for patients, families, and clinicians is:
“Your illness is real. Your distress is understandable. You deserve support. And you also deserve a life with meaning, connection, and moments of relief beyond illness.”
Further support and reading
If you are living with aspergillosis and feel that others do not fully understand what you are going through, these resources may help. They offer information about long-term illness, mental wellbeing, breathlessness, invisible symptoms, and patient support.
- Aspergillosis patient support
Information about support meetings, patient resources, and ways to connect with others affected by aspergillosis. - NHS Talking Therapies
NHS support for people experiencing anxiety, depression, or emotional distress, including people living with long-term health conditions. - Asthma + Lung UK: Living with a lung condition
Practical information on living with breathlessness, fatigue, flare-ups, and the emotional effects of lung disease. - Chronic Illness Inclusion
A UK organisation focused on the experiences of people living with chronic, energy-limiting, and often invisible conditions. - The Patients Association: Long-term conditions
Advice and information for people managing long-term health conditions and navigating healthcare conversations.
Important: If your symptoms suddenly worsen, you develop severe breathlessness, chest pain, coughing up blood, confusion, fainting, or signs of serious infection, seek urgent medical advice. In the UK, call NHS 111 for urgent advice or 999 in an emergency.
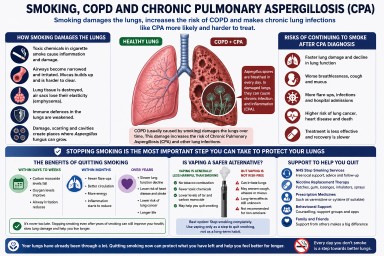
Smoking, COPD and Chronic Pulmonary Aspergillosis (CPA)
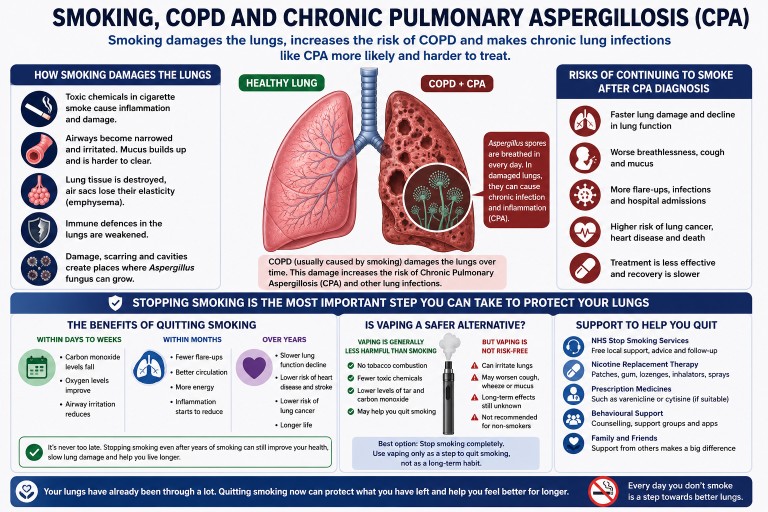
Many people diagnosed with Chronic Pulmonary Aspergillosis (CPA) also have Chronic Obstructive Pulmonary Disease (COPD). One of the strongest shared risk factors between the two conditions is cigarette smoking.
Smoking does not directly “cause” Aspergillus infection in the same way a virus or bacteria causes disease. However, it can create the lung damage and immune dysfunction that make CPA more likely to develop and harder to control.
Why smoking matters in CPA and COPD
Smoking damages the lungs over many years by:
- Destroying normal lung tissue and airways
- Causing chronic inflammation
- Reducing the lungs’ ability to clear mucus, dust and fungal spores
- Damaging the tiny hair-like structures called cilia that normally sweep organisms out of the airways
- Weakening local immune defence inside the lungs
- Increasing emphysema, cavities, scarring and bronchiectasis — all environments where Aspergillus can grow more easily
People breathe in Aspergillus spores every day. Healthy lungs usually remove them without difficulty. Damaged lungs are different. In COPD, especially severe COPD, spores can remain trapped in damaged airways and cavities, increasing the risk of long-term fungal colonisation or infection.
Is smoking causal?
The relationship is complex, but in many patients smoking is likely to be an important contributing cause.
Smoking contributes to:
- COPD development
- Structural lung damage
- Reduced immune clearance
- Increased infection risk
- Faster lung decline
All of these increase vulnerability to CPA.
Smoking is therefore not simply an associated factor. In many patients it is part of the chain of events that eventually leads to CPA developing.
Not every smoker develops CPA, and not every person with CPA has smoked. Some people develop CPA after tuberculosis, severe pneumonia, sarcoidosis, asthma, bronchiectasis, lung surgery or other lung diseases. However, smoking substantially increases risk because it accelerates lung injury and reduces the lungs’ resilience.
Why continuing to smoke after CPA diagnosis is dangerous
Once CPA is established, continuing to smoke can make management much harder.
Smoking may:
- Accelerate further lung destruction
- Worsen breathlessness and cough
- Increase mucus production
- Increase flare-ups and infections
- Reduce physical fitness and oxygen levels
- Reduce quality of life
- Increase hospital admissions
- Make COPD progression faster
- Increase risk of lung cancer alongside CPA
- Make recovery from infections slower
Many patients with CPA already have limited lung reserve. Continuing to smoke can progressively reduce the remaining healthy lung tissue.
“The damage is already done” — is stopping still worthwhile?
Yes. This is one of the commonest and most understandable feelings among long-term smokers with lung disease. However, stopping smoking can still help, even after significant lung damage has already occurred.
Within days to weeks
- Carbon monoxide levels fall
- Oxygen delivery improves
- Airways may become less irritated
- Some coughing and mucus clearance may improve
Within months
- COPD flare-ups may reduce
- Circulation improves
- Physical activity may become easier
- Inflammation begins to reduce
Over years
- Lung function decline slows
- Risk of heart disease and stroke falls
- Risk of lung cancer gradually decreases
- Survival improves compared with continued smoking
For people with CPA, preserving remaining lung function is critical. Slowing further structural damage may help stabilise disease, and antifungal treatment works best in lungs that are not being continually injured by smoke.
Is vaping a safer alternative?
Many patients ask whether vaping, or using e-cigarettes, is a safer option than smoking cigarettes.
Current evidence suggests that vaping is likely to be substantially less harmful than smoking tobacco cigarettes because vaping avoids the combustion process that produces tar, carbon monoxide and many toxic chemicals found in cigarette smoke.
For smokers who are unable to stop nicotine completely, switching entirely from smoking to vaping may reduce harm.
However, vaping is not risk-free.
Vaping aerosols can still irritate the lungs and may contain:
- Fine particles
- Flavouring chemicals
- Heating by-products
- Nicotine
- Other airway irritants
Some people with CPA, COPD, asthma or bronchiectasis report:
- Increased cough
- Throat irritation
- Chest tightness
- Wheeze
- Increased mucus symptoms
Long-term effects of vaping are still being studied.
For patients with CPA, the safest option for lung health is probably:
- Stop smoking cigarettes completely
- Use vaping only if it helps avoid returning to smoking
- Gradually reduce vaping if possible
A common problem is “dual use” — continuing to smoke while also vaping. This usually provides much less benefit than stopping cigarettes completely.
While nicotine itself is addictive, most of the major smoking-related lung damage comes from the toxic products created by burning tobacco.
For many patients, switching from smoking to vaping may still represent an important positive step if it helps them move away from cigarettes permanently.
Nicotine addiction is powerful
Many people with CPA and COPD have smoked for decades. Stopping is rarely simply a matter of willpower. Nicotine is strongly addictive, and smoking often becomes linked to stress relief, routine, anxiety management and social habits.
Patients should not feel ashamed if stopping is difficult. Repeated attempts are normal. Many successful quitters tried several times before succeeding permanently.
What can help?
Support works better than trying alone.
Options include:
- NHS stop smoking services
- Nicotine replacement therapy, such as patches, gum, sprays or lozenges
- Prescription medicines such as varenicline or cytisine, if suitable
- Behavioural support and counselling
- Gradual reduction plans
- Vape or e-cigarette transition strategies in selected patients
- Family and peer support
For many people with severe lung disease, stopping smoking is one of the most important treatments available — alongside inhalers, oxygen, physiotherapy and antifungal medication.
A realistic but important message
Patients with CPA often already live with fatigue, cough, breathlessness and anxiety about the future. Smoking may feel comforting in the short term, but it usually continues the cycle of lung injury that helped create the problem in the first place.
Stopping smoking cannot reverse established CPA, but it may:
- Slow further lung decline
- Improve day-to-day symptoms
- Improve response to treatment
- Preserve independence longer
- Reduce complications
- Improve long-term survival
Even small improvements in lung health can matter enormously when lung reserve is limited.
When to seek medical advice
Patients with CPA, COPD or other lung disease should seek medical advice if they:
- Become significantly more breathless
- Develop chest pain
- Cough up increasing amounts of blood
- Notice worsening wheeze or mucus production
- Develop fevers or signs of infection
- Feel unable to cope with smoking withdrawal symptoms alone
Stopping smoking is often difficult, but healthcare professionals can offer support and treatment options that improve the chances of success.
Mental Health Awareness Week: Supporting the Emotional Impact of Aspergillosis

Mental Health Awareness Week is a reminder that health is not only physical.
For people living with aspergillosis, and for the family members and carers who support them,
the emotional impact of a long-term lung condition can be significant.
Aspergillosis can bring uncertainty, fatigue, breathlessness, repeated appointments,
medication changes, worries about test results, and concerns about the future.
It is understandable that some people experience anxiety, low mood, frustration,
isolation, or disturbed sleep.
Carers may also feel under pressure. Supporting someone with a chronic illness can be rewarding,
but it can also be tiring and emotionally demanding. Looking after your own mental health is not selfish;
it helps you continue to support the person you care about.
Small steps can help
- Talk to someone you trust about how you are feeling.
- Stay connected with friends, family, or peer support groups.
- Pace your activities and allow time for rest.
- Try gentle movement if this is safe and manageable for you.
- Write down worries or questions before appointments.
- Ask your healthcare team for support if anxiety, low mood, or stress is affecting daily life.
You are not alone
Many people with aspergillosis find it helpful to speak with others who understand what it is like
to live with a rare fungal lung condition. Peer support can reduce isolation and help patients and carers
feel more informed and understood.
The National Aspergillosis Centre and associated patient organisations provide support, information,
and opportunities to connect with others affected by aspergillosis:
- Aspergillosis support resources for families and carers
- Weekly aspergillosis support meetings
- Aspergillosis Support Facebook group
When to seek help
If you are feeling persistently overwhelmed, very low, anxious, unable to cope,
or if your mental health is affecting your day-to-day life, please speak to your GP,
specialist nurse, or healthcare team. Mental health support is an important part of healthcare.
If you feel at immediate risk of harming yourself, or you do not feel safe,
seek urgent help by calling emergency services or going to your nearest emergency department.
More information about Mental Health Awareness Week is available from the
Mental Health Foundation
Your mental health matters. Support, understanding, and connection can make a difference.
Blue inhalers, combination inhalers and aspergillosis: what patients need to know
Blue reliever inhalers, such as salbutamol or Ventolin, remain important medicines and can be lifesaving during asthma symptoms or an asthma attack. However, asthma guidelines have changed because doctors now recognise that relying too heavily on a blue inhaler can be a sign that the underlying airway inflammation is not being well controlled.
What is a blue inhaler?
A blue inhaler usually contains a medicine called a short-acting beta2 agonist, often shortened to SABA. Salbutamol is the best-known example.
These inhalers work quickly by relaxing the muscles around the airways. This can relieve wheeze, chest tightness and breathlessness within minutes. However, a blue inhaler does not treat the airway inflammation that often drives asthma symptoms.
You can read more about reliever inhalers from Asthma + Lung UK.
Why are asthma guidelines changing?
Asthma is not just a condition of narrowed airways. It is also an inflammatory condition. A reliever inhaler may make breathing feel easier for a short time, but if inflammation is not treated, asthma may remain poorly controlled.
Frequent use of a blue reliever inhaler can therefore be a warning sign. It may mean that asthma treatment needs reviewing, especially if someone is needing their reliever often, waking at night, having flare-ups, or finding their normal activities limited.
The updated NICE/BTS/SIGN asthma guideline supports greater use of treatment plans that combine symptom relief with anti-inflammatory treatment.
What are AIR and MART inhalers?
Some patients are now prescribed a combination inhaler that contains:
- a fast-acting reliever medicine to open the airways
- an inhaled corticosteroid to reduce inflammation
These approaches are known as:
- AIR – Anti-Inflammatory Reliever
- MART – Maintenance and Reliever Therapy
With these plans, the combination inhaler may be used when symptoms occur. In MART, it is also used regularly every day as maintenance treatment.
The important difference is that when symptoms increase, the patient receives more anti-inflammatory treatment as well as more reliever medicine. This aims to reduce the cycle of worsening symptoms, repeated blue inhaler use, and untreated inflammation.
Useful patient information is available from Asthma + Lung UK on AIR inhalers and MART inhalers.
Does this mean everyone should stop using their blue inhaler?
No. This is the most important point.
The new guidance does not mean that every patient must immediately stop using a blue inhaler. It also does not mean that blue inhalers are “bad” or banned.
For many people, nothing will change straight away. Some patients will remain on their current inhalers. Others may be changed to an AIR or MART plan after review by their GP, asthma nurse or respiratory specialist.
Will some patients have their blue inhaler taken away?
Sometimes, but not always.
If a patient is moved onto an AIR or MART plan, their combination inhaler may become both their preventer and their reliever. In that situation, they may no longer routinely need a separate blue inhaler.
However, some patients may still keep a blue inhaler as backup, and others may continue with separate preventer and reliever inhalers. This depends on the individual patient, their diagnosis, their inhalers, and their asthma action plan.
Not all combination inhalers can be used as relievers. Only specific inhalers containing a fast-acting medicine such as formoterol are suitable for AIR or MART use. Patients should only use inhalers in this way if they have been specifically prescribed and instructed to do so.
Why this is more complicated for aspergillosis patients
People with aspergillosis-related lung disease often have more complex respiratory problems than standard asthma alone.
This may include:
- ABPA (Allergic Bronchopulmonary Aspergillosis)
- severe asthma with fungal sensitisation
- bronchiectasis
- mucus plugging
- chronic airway infection or fungal colonisation
- reduced lung reserve or scarring
For these patients, breathlessness is not always caused by asthma-type inflammation alone. It may also be related to mucus, infection, bronchiectasis, fungal activity, or structural lung damage.
This means that simply taking more inhaler may not always address the real cause of worsening symptoms.
Steroids: useful but needing balance
Inhaled corticosteroids can be very helpful in asthma and ABPA because they reduce airway inflammation. Good control of inflammation may reduce symptoms, flare-ups and the need for oral steroid courses.
However, steroid exposure also needs careful management in aspergillosis patients. Higher steroid doses may increase the risk of side effects such as oral thrush and, in some situations, may affect the balance between inflammation control and fungal growth.
This does not mean patients should avoid inhaled steroids. It means that treatment should be individualised and reviewed by a clinician who understands the patient’s full lung condition.
What should aspergillosis patients do?
- Do not stop your blue inhaler suddenly if it has been prescribed for you.
- Do not change your preventer or steroid inhaler without medical advice.
- Check your own asthma action plan. Make sure you know which inhaler is for daily prevention and which one is for symptoms.
- Ask whether your combination inhaler is suitable for AIR or MART use. Do not assume that all combination inhalers can be used this way.
- Request a review if you are using your reliever inhaler frequently, symptoms are worsening, or you are unsure what to do.
When to seek urgent help
Seek urgent medical help if your breathlessness is severe, your reliever is not helping as expected, you are struggling to speak in full sentences, your lips or fingers look blue, or your symptoms are rapidly worsening.
Follow your personal asthma action plan. If you think you are having an asthma attack, do not delay seeking emergency help.
The key message
The new guidance is not simply about “taking away blue inhalers”. It is about recognising that asthma symptoms often reflect airway inflammation, and that some patients do better when symptom relief and anti-inflammatory treatment are given together.
For people with aspergillosis, the message is especially important: inhaler treatment should be reviewed in the context of the whole lung condition, not changed because of a headline.
If you are unsure about your inhalers, speak to your GP, asthma nurse, respiratory consultant or aspergillosis team.
Further reading
Houseplants and Aspergillosis: Do You Need to Get Rid of Them?

Audience: Patients with aspergillosis (including Allergic Bronchopulmonary Aspergillosis), carers, and non-specialist cliniciansHouseplants are a common concern for people with
aspergillosis, particularly those with
Allergic Bronchopulmonary Aspergillosis (ABPA).If you’ve asked this question, you’re not alone—many patients raise it in our
patient questions and discussions.
🔑 Key Points
- Houseplants can be a source of Aspergillus spores, mainly from soil.
- Most people with ABPA do not need to remove all plants.
- The main risk comes from damp soil and disturbance.
- Simple precautions can significantly reduce exposure.
- How plants are cared for matters more than the type of plant.
Contents
- Why houseplants can be a problem
- How big is the risk?
- Do houseplants clean the air?
- Can I safely keep my plants?
- How to reduce risk
- Are some plants lower risk?
- When to consider removing plants
- Common questions
- When to seek medical advice
- References
🌱 Why can houseplants be a problem?
Aspergillus is a common environmental mould found in:
- Soil and compost
- Decaying plant material
- Damp indoor environments
For people with Allergic Bronchopulmonary Aspergillosis (ABPA), inhaling spores can trigger airway inflammation, wheeze, cough, and breathlessness.
The main risk comes from soil rather than the plant itself.
⚖️ How big is the risk?
The risk varies depending on:
- How stable your condition is
- The number of plants
- Ventilation in your home
- How plants are maintained
Specialist centres such as the National Aspergillosis Centre (NAC) recommend a
risk reduction approach rather than complete avoidance.
You can read more in our guide to
reducing mould exposure.
Important: There is limited direct research linking houseplants to worsening ABPA. Advice is based on environmental studies and clinical experience.
🌿 Do houseplants clean the air?
You may have heard that houseplants “clean the air.” This idea comes from laboratory studies, including research by
:contentReference[oaicite:0]{index=0}, conducted in sealed environments.
In real homes, the effect is minimal.
- Very large numbers of plants would be needed
- Ventilation has a much greater impact
- Soil may introduce Aspergillus spores
For a broader explanation, see our
aspergillosis overview.
Bottom line: Plants may improve wellbeing, but they are not an effective air-cleaning strategy.
🌿 Can I safely keep my houseplants?
In many cases, yes.
Many people with ABPA keep houseplants without problems when their condition is stable and plants are well maintained.
However, some individuals are more sensitive, so a personalised approach is important.
✅ How to reduce your risk
1. Manage the soil carefully
- Avoid constantly damp compost
- Allow the top layer to dry between watering
- Consider lower-organic substrates (e.g. clay pebbles)
Tip from patients: Adding a layer of stones or gravel on top of the soil can reduce disturbance during watering and may help limit release of fungal spores.
2. Avoid disturbing soil indoors
- Repot plants outside if possible
- Wear a well-fitted mask (FFP2 or FFP3)
3. Maintain good plant hygiene
- Remove dead leaves promptly
- Avoid visible mould growth
- Do not allow stagnant water
4. Choose locations carefully
- Keep plants out of bedrooms
- Ensure good ventilation
5. Personal hygiene after handling plants
- Wash hands after handling soil or compost
- Avoid touching your face before cleaning hands
- Consider changing clothes after heavy gardening
- Ventilate the area after indoor plant work
These steps form part of a wider approach to
reducing environmental exposure.
🌿 Are some plants lower risk for ABPA?
There is no strong evidence that specific plants are “safe” or “unsafe.” The main risk comes from soil and moisture.
Some setups may be lower risk in practice:
- Hydroponic or semi-hydroponic plants
- Plants that prefer drier conditions (e.g. succulents)
- Well-maintained plants with minimal decaying material
Important: Any plant can become higher risk if soil becomes damp or mouldy.
If unsure, you may wish to review
clinical guidance or discuss with your care team.
🚩 When should I consider removing plants?
- Symptoms worsen after watering or handling plants
- Visible mould in soil
- Frequent flare-ups
- Clinical advice recommends stricter avoidance
Some people remove plants temporarily during unstable periods and reintroduce them later.
❓ Common questions
Are leaves dangerous?
No—the main risk comes from soil and decaying material.
Is outdoor gardening riskier?
Yes, due to higher exposure. Wearing a mask is recommended.
Do air purifiers help?
HEPA filters may reduce airborne particles, but evidence specific to ABPA is limited.
⚠️ When to seek medical advice
- Increasing breathlessness or wheeze
- Worsening cough or mucus
- Reduced peak flow
- Symptoms linked to specific environments
Do not change treatment without medical advice.
📚 References & Further Reading
- What is aspergillosis?
- Reducing exposure to mould
- World Health Organization – Indoor air quality guidance
- UK Health Security Agency – Damp and mould health risks
👩⚕️ Author & Review
Developed for patient education in line with UK specialist practice (National Aspergillosis Centre, Manchester).
This information is general and does not replace individual medical advice.
Looking for more answers? Visit our
patient questions hub.