Lung Bleeding (Haemoptysis) in Aspergillosis: What It Means and What to Expect
 Last reviewed: March 2026
Last reviewed: March 2026Audience: Patients, carers, and non-specialist healthcare professionals
Applies to: Chronic Pulmonary Aspergillosis (CPA), bronchiectasis, and related lung conditions
Key Points
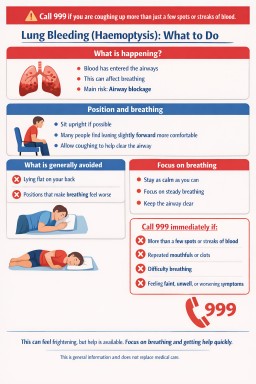
- Coughing up more than a few spots or streaks of blood is a medical emergency
- If bleeding is heavier or affects breathing, call 999 immediately
- The main immediate risk is airway blockage, not just blood loss
- Emergency care focuses on keeping airways clear and protecting breathing
- Some general positioning approaches are commonly used in healthcare settings
- This page provides general information only and is not a substitute for medical care
Table of Contents
- What is haemoptysis?
- Why can it happen in aspergillosis?
- Why does it feel so frightening?
- When is it an emergency?
- What happens during emergency care?
- While waiting for help (general guidance)
- Why positioning matters
- Understanding airway safety
- What is generally avoided
- What happens after hospital care?
- Medications such as tranexamic acid
- Common questions
- When to seek medical help
What is haemoptysis?
Haemoptysis means coughing up blood from the lungs or airways. This can range from small streaks in sputum to larger bleeds.
In people with Chronic Pulmonary Aspergillosis (CPA) and related lung conditions, haemoptysis can occur due to changes in lung structure and blood vessels.
Why can it happen in aspergillosis?
- Areas of lung damage (such as cavities) may develop
- Blood vessels in these areas can become fragile
- Inflammation may increase susceptibility to bleeding
Not all patients will experience haemoptysis, but awareness is important.
Why does it feel so frightening?
Many patients describe a strong sensation of being unable to breathe during a lung bleed.
This can occur because blood enters the airways, which may interfere with airflow. Even small amounts in the wrong place can feel overwhelming.
This reaction is common and understandable.
When is it an emergency?
NHS guidance advises calling 999 if you are coughing up more than just a few spots or streaks of blood.
Call 999 immediately if:
- You are coughing up more than just a few spots or streaks of blood
- You are coughing up repeated mouthfuls or clots
- You have difficulty breathing
- You feel faint, unwell, or symptoms are worsening
Small streaks or flecks of blood should still be checked by a healthcare professional, but larger or increasing amounts should be treated as an emergency.
What happens during emergency care?
Emergency responders and hospital teams focus on:
- Supporting breathing (for example, with oxygen)
- Monitoring vital signs
- Identifying the source of bleeding
- Protecting unaffected areas of the lung where possible
In some cases, procedures such as bronchial artery embolisation may be used to control bleeding.
While waiting for help (general guidance)
If you are waiting for emergency services to arrive, general first-aid principles often focus on maintaining comfort and supporting breathing.
- If possible, try to remain in a position that feels easiest for breathing
- Many patients find that being upright or slightly forward is more comfortable
- Try to keep the airway clear by allowing coughing if needed
The priority is to seek urgent medical help rather than attempting to manage the situation alone.
In an emergency, it may not be possible to adopt an “ideal” position—focus on calling for help.
Why positioning matters
In healthcare settings, positioning is sometimes used to help:
- Keep airways as clear as possible
- Reduce the spread of blood within the lungs
- Maintain breathing while further treatment is arranged
This is based on general principles of lung anatomy and airflow. The aim is not to stop bleeding, but to support breathing.
Many people find it easier to breathe when upright or leaning slightly forward. This may help fluid move out through the mouth rather than further back into the main airways.
Understanding airway safety
In situations where there is bleeding (or sometimes vomiting), the main concern is keeping the airway clear so that air can move in and out of the lungs.
Fluid in the airway can interfere with breathing, which is why emergency care focuses on maintaining airway clearance as well as treating the underlying cause.
Positions that allow fluid to move out of the mouth rather than back into the airway are generally preferred. Many people find being upright or slightly forward helps with this.
If someone becomes unable to remain upright, is very drowsy, or is vomiting, placing them on their side (recovery position) may help keep the airway clear while waiting for emergency services.
This information is general and does not replace emergency care. Always call 999 if symptoms are severe.
What is generally avoided
In clinical practice, certain positions are usually avoided because they may make breathing more difficult.
- Lying flat on the back
- Positions that feel like they worsen breathing
If you feel unsure, prioritise comfort and breathing while waiting for help.
What happens after hospital care?
After an episode of haemoptysis, your clinical team may:
- Investigate the cause of bleeding
- Review your current treatment
- Discuss whether any preventative measures are appropriate
If you have experienced haemoptysis, it may be helpful to ask your team whether you need an individualised plan.
Medications such as tranexamic acid
Some patients may be prescribed tranexamic acid to help reduce bleeding.
If you have been given this medication with clear instructions, it may be intended for use during bleeding episodes. It should only be taken exactly as directed by your clinical team.
Tranexamic acid does not replace the need to seek urgent medical help. If you are coughing up more than a few spots or streaks of blood, or feel unwell or breathless, call 999.
If you are unsure whether to take it during an episode, seek urgent medical advice.
Common Questions
Is coughing up blood always serious?
Any new or unexplained bleeding should be assessed. Larger amounts require urgent attention.
Can I manage this at home?
Significant haemoptysis should not be managed at home. Always seek urgent medical help.
Will it happen again?
This varies between individuals. Your specialist team can advise based on your condition.
When to seek medical help
Call 999 immediately if:
- You are coughing up more than just a few spots or streaks of blood
- You have difficulty breathing
- You feel faint, unwell, or symptoms are worsening
Seek medical advice urgently (NHS 111 or GP) if:
- You notice new or increasing blood in sputum
- You have recurrent or ongoing minor bleeding
Important safety note
This information is for general education only and does not replace medical advice. In an emergency, always seek immediate professional care.
References
- NHS. Coughing up blood (haemoptysis): https://www.nhs.uk/symptoms/coughing-up-blood/
- European Respiratory Society and interventional radiology guidance on haemoptysis
Author and review
Author: National Aspergillosis Centre (Patient Education Team)
Review: Specialist clinicians, Manchester University NHS Foundation Trust
Next review due: March 2027
Why Headaches Can Occur in Aspergillosis
Last reviewed: March 2026
Key Points
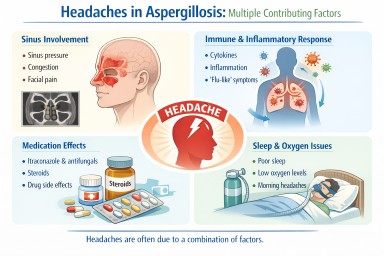
- Headaches are relatively common in people living with aspergillosis, but they usually have multiple contributing causes.
- Common causes include sinus involvement, inflammation, sleep disturbance, and medication effects.
- Antifungal medicines such as itraconazole may improve some symptoms indirectly but can also occasionally cause headaches.
- Patterns (timing, location, triggers) can help identify likely causes, but headaches are rarely due to one factor alone.
- New, severe, or unusual headaches should always be assessed by a healthcare professional.
Table of Contents
- Overview
- Sinus involvement (common cause)
- Inflammation and immune response
- Allergic-type responses (e.g. ABPA)
- Medication effects
- Sleep disturbance and night symptoms
- Breathing and oxygen levels
- General health factors
- Understanding headache patterns
- Common questions
- When to seek medical advice
- Summary
- Author and review
- References
Overview
Many people living with aspergillosis report headaches at some point during their illness. These headaches can vary in type, severity, and timing, and may be confusing—especially when they change over time or seem linked to treatment.
In most cases, headaches are not caused by a single factor. Instead, they reflect a combination of:
- local effects (such as sinus pressure)
- immune system activity
- medication effects
- sleep and general health factors
Understanding these different contributors can help make sense of symptoms and support more informed discussions with your clinical team.
Sinus involvement (common cause)
When Aspergillus affects the sinuses (sometimes called fungal sinusitis), this can directly cause headaches.
This happens because:
- sinus drainage becomes blocked
- pressure builds up in the sinus cavities
- the lining of the sinuses becomes inflamed
Typical features:
- pain or pressure in the forehead, cheeks, or behind the eyes
- worsening when bending forward
- a feeling of fullness or congestion
This is one of the most direct ways aspergillosis can lead to headaches.
Inflammation and immune response
Even when the sinuses are not directly involved, the body’s immune response to fungal material can cause systemic effects.
The immune system releases signalling molecules (such as cytokines) that can:
- increase inflammation
- affect blood vessels
- trigger headache pathways
This type of headache can feel similar to a “flu-like” or inflammatory headache.
Allergic-type responses (e.g. ABPA)
In conditions such as Allergic Bronchopulmonary Aspergillosis (ABPA), the immune system reacts strongly to Aspergillus.
This may involve:
- allergic pathways
- histamine and related mediators
- ongoing airway inflammation
Possible symptoms:
- head pressure or discomfort
- fluctuating headaches
- a “foggy” or unwell feeling
These headaches are often less clearly localised than sinus-related pain.
Medication effects
Some treatments used in aspergillosis can contribute to headaches.
Antifungal medications (e.g. itraconazole):
- headache is a recognised side effect in some people
- effects vary between individuals
Steroids (if prescribed):
- can affect sleep and mood
- may influence blood pressure
- can indirectly contribute to headaches
Medication effects can sometimes overlap with disease-related symptoms, making patterns harder to interpret.
Sleep disturbance and night symptoms
Sleep disruption is common in chronic lung conditions.
Possible contributors include:
- night-time coughing
- breathlessness
- discomfort or anxiety
Poor sleep can lead to:
- morning headaches
- increased sensitivity to pain
- fatigue-related headaches
Breathing and oxygen levels
In some people with more advanced lung involvement:
- oxygen levels may be slightly reduced
- breathing effort may increase
This can contribute to:
- morning headaches
- fatigue and cognitive symptoms
Not all patients experience this, but it is an important factor in some cases.
General health factors
Headaches can also be influenced by general aspects of living with a long-term condition:
- dehydration
- fatigue
- reduced activity levels
- stress or anxiety
These factors can contribute to tension-type headaches or make other headache types more noticeable.
Understanding headache patterns
Looking at patterns can sometimes help identify likely contributors.
- Facial pressure worse on bending: may suggest sinus involvement
- Early morning headaches: may relate to sleep or breathing patterns
- Fluctuating or “wave-like” symptoms: may reflect inflammation or immune activity
- New headaches after starting medication: may be treatment-related
However, these are general observations only and do not replace clinical assessment.
Headaches in Aspergillosis: Interactive Decision Aid
This tool helps patients and carers think about common patterns that can contribute to headaches in aspergillosis. It does not diagnose the cause of a headache.
It is designed to support discussion with a healthcare professional and highlight possible contributors such as sinus involvement, inflammation, medication effects, sleep disturbance, and breathing-related factors.
1. Where is the pain mainly felt?
2. When is it most noticeable?
3. What does it feel like?
4. What other features are present?
5. Are there any red flags?
Possible contributors
This panel highlights common patterns only. It is not a diagnosis and does not replace medical assessment.
Common questions
Are headaches a recognised symptom of aspergillosis?
They can occur, but are usually indirect and caused by associated factors such as sinus disease or inflammation.
Can antifungal treatment improve headaches?
In some cases, yes—if symptoms are linked to fungal-related inflammation. However, antifungals can also occasionally cause headaches as a side effect.
Are “histamine-type” headaches part of aspergillosis?
Some patients describe symptoms in this way, but the underlying mechanism is often more complex than histamine alone.
Why do my headaches change over time?
This is common and may reflect changes in inflammation, treatment, sleep, or overall health.
When to seek medical advice
You should seek medical advice if you experience:
- new or unusually severe headaches
- headaches that are worsening over time
- neurological symptoms (e.g. vision changes, weakness, confusion)
- fever, neck stiffness, or other concerning symptoms
If you are unsure whether your headaches are related to aspergillosis, treatment, or another cause, it is important to discuss this with your healthcare team.
Summary
Headaches in people with aspergillosis are usually caused by a combination of factors rather than a single issue.
The most common contributors include:
- sinus involvement
- immune and inflammatory responses
- sleep disturbance
- medication effects
Understanding patterns and changes over time can be helpful, but medical assessment is important if symptoms are new, severe, or concerning.
Author and review
Prepared for: aspergillosis.org
Audience: Patients and non-specialist readers
Important: This article is for general information only and does not replace individual medical advice.
References
- Patterson TF et al. (2016). Practice Guidelines for the Diagnosis and Management of Aspergillosis.
PMID: 27365388 - Denning DW et al. (2016). Chronic pulmonary aspergillosis guidelines.
PMID: 26699723 - Chakrabarti A et al. (2009). Fungal sinusitis: a categorization and definitional schema.
PMID: 19522756
Why Do My “Histamine” Headaches Improve on Itraconazole?
Last reviewed: March 2026
Key Points
- Itraconazole is an antifungal medicine. It is not an antihistamine.
- Some people notice that symptoms such as headaches, flushing, or a “histamine-type” feeling become shorter or less intense after starting treatment.
- This is most likely because itraconazole reduces the fungal burden and the immune response it triggers, rather than blocking histamine directly.
- Symptoms that happen in the early hours of the morning may also be influenced by the body’s natural day-night rhythm.
- Changes in symptoms can be helpful clues, but headaches can have more than one cause.
Table of Contents
- Overview
- What is itraconazole and how does it work?
- What do people mean by “histamine dump” headaches?
- Why might symptoms improve on itraconazole?
- Why do symptoms often happen at night?
- Does this mean histamine is the main problem?
- Common questions
- When to seek medical advice
- Summary
- Author and review
- References
Overview
Some people taking itraconazole for non-lung or lung forms of aspergillosis notice that symptoms they describe as “histamine-type” symptoms, such as headaches, flushing, pressure, or a general sense of inflammatory overload, become shorter or less severe.
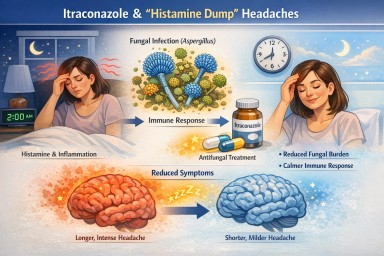
A typical pattern might be:
- Symptoms start overnight, for example, around 2 am
- Symptoms previously lasted most of the day
- Symptoms are now settling much earlier after starting treatment
This can be confusing, especially when the symptoms feel similar to a histamine reaction. The important point is that itraconazole does not work like an antihistamine, but it can reduce symptoms indirectly if a fungal process is contributing to them.
What is itraconazole and how does it work?
Itraconazole is an antifungal medicine used to treat infections caused by fungi such as Aspergillus.
It works by interfering with the production of ergosterol, an essential part of the fungal cell membrane. This weakens the fungus and helps reduce fungal growth and survival in the body.
As the fungal burden falls, the immune system may be less strongly stimulated, and that can lead to a reduction in inflammation-related symptoms.
So although itraconazole does not block histamine directly, it may reduce the underlying trigger that is causing the body to react.
What do people mean by “histamine dump” headaches?
“Histamine dump” is not a formal medical diagnosis, but some patients use it as a practical way of describing symptoms such as:
- sudden headaches, especially overnight or early in the morning
- flushing or a feeling of heat
- pressure in the head or sinuses
- a sense of being “wired”, agitated, or unwell
These symptoms may involve histamine, but they can also reflect broader inflammation, immune activation, mast cell activity, or other signalling chemicals in the body.
Why might symptoms improve on itraconazole?
If itraconazole is helping, it is most likely doing so indirectly. There are several possible reasons for this.
1. Reduced fungal burden
If fungal material in the body is reduced, there may be less for the immune system to react to. That can mean less inflammatory signalling overall.
2. Reduced immune activation
Fungi can stimulate the immune system in ways that lead to inflammation and, in some people, histamine-related symptoms. If antifungal treatment lowers that stimulus, symptoms may become less intense or settle more quickly.
3. Shorter inflammatory response
Some people find that the symptom still begins, but does not “run on” for as long. For example, a headache that used to last from 2am until late afternoon may now settle by 5am.
Why do symptoms often happen at night?
The body has a natural circadian rhythm, a 24-hour cycle that affects hormones, inflammation, sleep, and immune activity.
- Some inflammatory signals can be more noticeable overnight
- Cortisol rises in the early morning, and helps suppress inflammation
Does this mean histamine is the main problem?
Not necessarily. Symptoms may involve multiple pathways, including immune response to fungi, general inflammation, mast cell activity, and sinus pressure.
Common questions
Does itraconazole act like an antihistamine?
No. It does not block histamine receptors.
Why are my symptoms improving but not gone?
This is common and may reflect partial control of the underlying trigger.
Does this prove Aspergillus is the cause?
No. It suggests a possible link but does not confirm causation.
Will symptoms continue to improve?
Possibly, but responses vary between individuals.
When to seek medical advice
- new or severe headaches
- neurological symptoms (vision, speech, balance)
- worsening or persistent symptoms
- concerns about medication side effects
Summary
Itraconazole does not directly affect histamine but may reduce symptoms by lowering fungal burden and immune activation.
Author and review
Prepared for: aspergillosis.org
Audience: Patients and non-specialist readers
Important: This does not replace individual medical advice.
References
- Patterson TF, Thompson GR 3rd, Denning DW, et al. (2016).
Practice Guidelines for the Diagnosis and Management of Aspergillosis.
View on PubMed (PMID: 27365388) - Denning DW et al. (2016).
Chronic pulmonary aspergillosis guidelines.
View on PubMed (PMID: 26699723) - Barnes PJ, Adcock IM (2009).
Circadian rhythm in airway disease.
View on PubMed (PMID: 19336589) - Stone KD et al. (2010).
IgE, mast cells, and eosinophils.
View on PubMed (PMID: 20176269)
Why Join an Online Support Group if You Have Aspergillosis?
You are not alone with aspergillosis
Join a friendly online support meeting — no pressure, just listen if you prefer.
Many patients find that even attending once helps them feel more reassured, informed, and supported.
Why Join an Online Support Group if You Have Aspergillosis?
Living with aspergillosis can feel isolating. Many people go for years without meeting another person with the same condition. Family and friends may be supportive, but they may not fully understand what it is like to live with breathlessness, fatigue, treatment side effects, uncertainty, or repeated hospital visits.
That is one reason online support groups can be so valuable. They bring people together who understand, often immediately, many of the challenges that aspergillosis can bring.
Key points
- Online support groups reduce isolation and help patients feel understood
- They offer shared experience alongside emotional support
- They improve confidence and understanding of the condition
- They help patients feel better prepared for appointments
- They are flexible — you can simply listen if you prefer
What changes when people join a support group?
Before joining
- Feeling alone with the condition
- Uncertainty about symptoms
- Limited practical advice
- Low confidence at appointments
- Worry about the future
After joining
- Connection with others who understand
- Better understanding of the condition
- Practical day-to-day coping ideas
- More confidence asking questions
- Feeling more supported and reassured
Why aspergillosis can feel so isolating
Aspergillosis is a relatively rare condition, and many patients never meet someone else with the same diagnosis. Online support groups help bridge that gap by creating a shared space for understanding and connection.
1. You realise you are not alone
Hearing others describe similar symptoms and challenges can be immediately reassuring and reduce feelings of isolation.
2. Shared experience can be deeply reassuring
Support groups provide practical, real-world insight into managing fatigue, pacing, work, and daily life.
3. You may understand your condition better
Listening to others and accessing shared resources helps build confidence and understanding.
4. It can help you feel more confident at appointments
Patients often feel better prepared and more able to ask the right questions.
5. Emotional support matters too
These groups provide encouragement, understanding, and a sense of belonging.
What happens in a typical online support session?
- Friendly welcome — no pressure to speak
- Open discussion — share or listen
- Optional topics — such as fatigue or treatment experiences
- Flexible participation — camera and microphone optional
- Safe, moderated space
Many people attend their first session just to listen — and that is completely fine.
What patients often say
“I wish I had joined sooner. Just hearing others talk made a huge difference.”
“I didn’t speak in my first meeting, but it really helped just listening.”
“It helped me understand my condition and feel more confident.”
Thinking of joining?
You can attend once, listen, and decide if it feels helpful. There is no obligation to continue.
View meeting times and book here:
https://aspergillosis.org/support-meetings/
Meetings are held online using Microsoft Teams. You will receive a joining link after booking.
Bottom line
Online support groups offer connection, reassurance, and understanding. They cannot replace medical care, but they can make living with aspergillosis feel more manageable and less lonely.
Please note: These groups are for support and shared experience. They do not replace advice from your own doctor or specialist team.
Donating Your Body for Medical Research in the UK
This is an uncommon request, but it can be very helpful to researchers. There is no compulsion at all to consider body donation. It is entirely a personal choice. Many people will decide that it is not for them, and that is completely understandable. For those who do wish to explore it, however, body donation can make an important contribution to medical education, training, and research.
What does body donation mean?
In the UK, donating your body means leaving it after death to a medical school or other appropriately licensed institution for anatomical examination, education, training, or research.
You cannot usually donate your body specifically to “aspergillosis research” alone. However, donation may still support work that is highly relevant to people affected by aspergillosis, including:
- lung disease
- infection
- immune responses
- medical training in complex respiratory illness
The most important point: consent must be given in advance
Under UK law, body donation must be arranged before death. This means:
- you must give written consent
- the consent must usually be witnessed
- your family cannot normally make this decision for you after you die
How to arrange body donation
- Choose a medical school
You need to contact a medical school directly. Most only accept donations from their local area. - Request an information pack
The school will explain its process, send consent forms, and set out any restrictions. - Complete the consent forms
Keep copies with your important papers and let your family know your wishes. - Tell your next of kin or executor
They will usually need to contact the medical school promptly after death.
Important to understand
- Not every donation can be accepted. Even if you have registered, a medical school may not be able to accept the body in every circumstance.
- A backup funeral plan is important.
- Body donation is separate from organ donation. They are different systems and require separate arrangements.
Can I ask for donation to help lung or aspergillosis-related research?
You can certainly explain that your interest is in supporting research and education relevant to lung disease, infection, or aspergillosis. However, you cannot usually guarantee exactly how a donated body will be used. Even so, donation may still support education and research that benefits future patients with complex respiratory and fungal conditions.
Where to start: Human Tissue Authority
The best first step is the Human Tissue Authority (HTA), which provides UK guidance and a way to identify the correct medical school for your postcode.
Examples of medical school body donation pages
Please note: contact details and catchment arrangements can change, so it is wise to confirm current information directly on each medical school’s website.
- University of Manchester
Body donation / bequeathals information - University of Liverpool
Human Anatomy Resource Centre body donation page
Email: [email protected]
Tel: 0151 794 5442 - University of Leeds
Bequests information
Email: [email protected]
Tel: 0113 343 4297
Final thought
Donating your body for medical education or research is an unusual and deeply personal decision. There is absolutely no obligation to consider it. But for those who do, it can be a generous and lasting way to support future learning, better care, and research that may help people living with serious conditions, including aspergillosis.
Last reviewed: March 2026
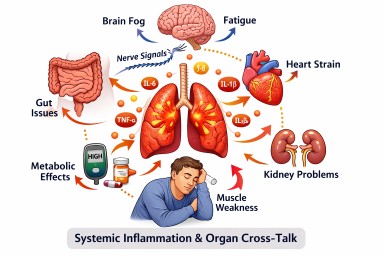
How Inflammation in One Part of the Body Can Affect the Rest of the Body
Last reviewed: 24 March 2026
Audience: Patients, families, and non-specialist clinicians
Author: Aspergillosis.org editorial team
Many people think of inflammation as something that stays in one place: a painful joint, an inflamed lung, an irritated sinus, or a bowel flare. In reality, inflammation is often a whole-body process. Signals released at one site can travel through the blood, nervous system, and immune system, influencing other organs and changing how the body feels and functions overall.
This helps explain why a local health problem can sometimes lead to symptoms that seem much broader, such as fatigue, poor concentration, low mood, loss of appetite, aches, disturbed sleep, or worsening of other long-term conditions.
Key points
- Inflammation is not always confined to one organ or body part.
- Inflamed tissues release chemical messengers that can circulate throughout the body.
- The brain, heart, kidneys, liver, gut, lungs, and immune system all communicate with one another.
- This “cross-talk” can be helpful in short-term illness, but harmful when inflammation becomes prolonged.
- Ongoing inflammation is linked with fatigue, brain fog, low mood, cardiovascular strain, and worsening of other chronic diseases.
Table of contents
- What is inflammation?
- Why inflammation does not always stay local
- How the body communicates during inflammation
- Common whole-body effects of inflammation
- Why this matters in lung disease and aspergillosis
- Acute inflammation versus chronic inflammation
- What can help?
- When to seek medical advice
- Common questions
- References
What is inflammation?
Inflammation is part of the body’s defence system. It is one of the ways the immune system responds to infection, injury, irritation, allergens, or tissue damage. In the short term, inflammation is often helpful. It can help the body fight infection, clear damaged tissue, and begin repair.
But inflammation can also become too strong, too prolonged, or poorly controlled. When that happens, the effects may no longer stay limited to the original problem area.
Why inflammation does not always stay local
When tissue becomes inflamed, immune cells release small signalling proteins called cytokines and other inflammatory mediators. These act like chemical messages. Some stay nearby, but many enter the bloodstream and influence distant organs.
This is why inflammation in one part of the body can sometimes cause:
- tiredness or exhaustion
- feeling unwell or “washed out”
- poor concentration or “brain fog”
- worsening appetite
- sleep disruption
- higher strain on the heart or kidneys
- worsening of other inflammatory conditions
Researchers increasingly describe this as systemic inflammation or organ cross-talk. In other words, organs do not operate in isolation. They are part of an interconnected network.
How the body communicates during inflammation
1. Chemical messengers in the blood
Inflamed tissues can release cytokines such as interleukin-6 (IL-6), interleukin-1 beta (IL-1β), and tumour necrosis factor alpha (TNF-α). These may affect blood vessels, metabolism, the brain, the heart, and other immune cells.
These signals are useful during short-term illness, but if they remain elevated they may contribute to chronic symptoms and long-term health effects.
2. Organ-to-organ immune cross-talk
Modern immunology shows that the gut, liver, lungs, brain, heart, kidneys, and bone marrow can influence one another through immune signalling. A problem in one organ may therefore alter immune behaviour somewhere else.
This can be protective, but it can also become part of a vicious circle, especially in chronic disease.
3. Nerve signalling between the body and brain
Inflammation is not communicated only by blood. The nervous system also plays a role. Signals from inflamed tissues can travel through nerves, including the vagus nerve, to the brain. The brain then responds by adjusting immune activity and body-wide stress responses.
This helps explain why inflammation can affect fatigue, mood, motivation, sleep, and mental clarity.
4. Stress, hormones, and metabolism
Inflammation also interacts with the body’s hormonal and metabolic systems. This can influence energy use, blood sugar regulation, muscle strength, and appetite. Over time, chronic inflammation may put extra strain on the cardiovascular and kidney systems.
Common whole-body effects of inflammation
Fatigue
One of the most common effects of inflammation is fatigue. This is not simply feeling sleepy. It can be a profound lack of physical and mental energy. Many chronic inflammatory illnesses are associated with this kind of exhaustion.
Brain fog and mood changes
Inflammatory signals can affect the brain, contributing to reduced concentration, slowed thinking, low motivation, anxiety, or low mood. This does not mean symptoms are “all in the mind”. It means that immune activity can influence brain function.
Heart and blood vessel effects
Inflammation can make blood vessels less healthy over time and may contribute to a higher cardiovascular risk. This is one reason why long-standing inflammatory diseases are often linked to heart and circulatory problems.
Kidney effects
The kidneys are sensitive to inflammatory stress. In some conditions, long-term systemic inflammation can contribute to kidney damage or worsen existing kidney disease. Kidney disease itself can also increase inflammation, creating a two-way relationship.
Muscle weakness and reduced stamina
Ongoing inflammation can alter how muscles use energy and recover after activity. This may contribute to weakness, reduced exercise tolerance, and slower recovery after exertion.
Why this matters in lung disease and aspergillosis
For people with chronic lung conditions, including some forms of aspergillosis, inflammation in the airways or lungs may have effects beyond breathing alone. The lungs are not separate from the rest of the body.
Inflammation in the lungs may contribute to:
- general fatigue
- poor stamina
- sleep disruption
- brain fog
- loss of appetite
- worsening of other conditions
This can be especially relevant for people living with long-term inflammatory lung disease, repeated infections, allergic inflammation, or complex treatment burdens.
It is also one reason why patients sometimes feel that their symptoms are “bigger” than what would be expected from the lungs alone. Often, that experience is real and biologically plausible.
Acute inflammation versus chronic inflammation
Acute inflammation
This is the short-term response seen with infection, injury, or a sudden flare. It may cause fever, pain, swelling, and marked tiredness. Usually, it settles when the trigger is controlled.
Chronic inflammation
This is lower-grade or persistent inflammation that continues over time. It may be driven by chronic infection, immune dysregulation, ongoing tissue damage, obesity, autoimmune disease, long-term lung disease, or other medical problems. Chronic inflammation is often less dramatic but may have broader long-term effects.
What can help?
The right approach depends on the underlying cause. Broadly, management focuses on:
- identifying and treating the cause of inflammation where possible
- controlling infections or allergic triggers
- optimising treatment of the underlying disease
- supporting sleep, nutrition, and pacing of activity
- monitoring the effects on other organs when relevant
There is rarely a single quick fix for chronic inflammation. Good management usually means looking at the whole person, not just the inflamed organ.
When to seek medical advice
Please seek medical advice if inflammation-related symptoms are worsening or if you develop:
- new or severe breathlessness
- chest pain
- confusion or marked drowsiness
- new swelling, reduced urine output, or signs of dehydration
- persistent fevers
- rapid decline in energy, mobility, or daily functioning
If symptoms are sudden, severe, or alarming, seek urgent medical help.
Common questions
Does inflammation always damage the whole body?
No. Short-term, controlled inflammation is a normal and useful response. Problems are more likely when inflammation is severe, repeated, or persistent.
Can one inflamed organ affect another?
Yes. There is now strong evidence that organs influence one another through immune, vascular, metabolic, and nerve-based pathways.
Can inflammation cause fatigue even if blood tests are not dramatically abnormal?
Yes. Symptoms and blood markers do not always match perfectly. Some people experience substantial fatigue and other systemic symptoms even when routine blood tests are only mildly abnormal or intermittently raised.
Is this relevant to chronic lung disease?
Yes. Lung inflammation can have effects that go beyond breathing, including fatigue, reduced stamina, and wider body effects.
References
- Dou J, et al. The Interplay of Cross-Organ Immune Regulation in Inflammation and Cancer. MedComm. 2025.
- Jin H, Li M, et al. A body–brain circuit that regulates body inflammatory responses. Nature. 2024.
- Katkenov N, et al. Systematic Review on the Role of IL-6 and IL-1β in Cardiovascular Diseases. Journal of Cardiovascular Development and Disease. 2024.
- Nowak KL, et al. Targeting Inflammation in CKD. Current Opinion in Nephrology and Hypertension. 2025.
- Paganin W, et al. Inflammatory biomarkers in depression: a scoping review. 2024.
- Mehta NN, et al. IL-6 and Cardiovascular Risk: A Narrative Review. 2024.
- Che H, et al. Organ cross-talk: molecular mechanisms, biological functions and therapeutic opportunities. 2026.
Disclaimer: This article is for general information and education. It is not a substitute for personalised medical advice. If you are worried about worsening symptoms, new symptoms, or the effect of inflammation on your health, speak to your clinical team.
Building fitness with Aspergillosis
Last reviewed: 20 March 2026
Audience: Patients, carers, families, and non-specialists
Applies to: Allergic bronchopulmonary aspergillosis (ABPA), chronic pulmonary aspergillosis (CPA), Aspergillus bronchitis, severe asthma with fungal sensitisation (SAFS)
Why it feels so hard — and how to improve safely
Key points
- Feeling exhausted after activity is common in aspergillosis and does not mean you are failing.
- Breathlessness and fatigue are often due to lung changes, not just “lack of fitness”.
- Pushing too hard can make symptoms worse — pacing is essential.
- Small, steady increases in activity are more effective than big efforts.
- Respiratory physiotherapy can make a major difference.
- Some patients (e.g. with cavities or haemoptysis) need tailored, cautious approaches.
Why exercise feels so difficult
Many people with aspergillosis find that even simple activity can feel exhausting.
This is not just about fitness. It is often due to changes in how the lungs and body work, including:
- Inflamed or narrowed airways
- Mucus affecting airflow
- Reduced oxygen transfer
- Increased effort needed to breathe
In addition:
- Long-term illness can reduce muscle strength
- Treatments such as steroids may affect weight and energy
- Many people experience post-exertional fatigue (feeling worse after activity)
This means your body is working harder than it used to — even for everyday tasks.
Why “just doing more” can backfire
It is natural to think that pushing harder will improve fitness. However, in aspergillosis this often leads to a cycle:
- Doing too much on a “good day”
- Feeling exhausted afterwards
- Needing longer recovery
- Losing confidence
This is sometimes called a “boom and bust” cycle.
The goal is not to push harder — it is to build steadily and sustainably.
A safer way to build fitness
1. Find your baseline
Start with what you can do without feeling completely exhausted afterwards.
This may be much less than you expect — and that is normal.
2. Use the 70–80% rule
Only do about 70–80% of what you feel capable of.
This helps prevent setbacks and allows gradual improvement.
3. Break activity into smaller chunks
Short sessions (e.g. 10–15 minutes) with rest in between are often easier than one long effort.
4. Use breathing control
Pursed-lip breathing:
- Breathe in through your nose
- Breathe out slowly through pursed lips
This helps keep airways open and reduces breathlessness.
5. Add gentle strength work
Improving muscle strength can reduce breathlessness and improve stamina.
- Sit-to-stand from a chair
- Light squats (with support)
- Step-ups
Start small — 2–3 times per week is enough.
The role of respiratory physiotherapy
Respiratory physiotherapy can be one of the most helpful supports available.
A respiratory physiotherapist can help with:
- Breathing techniques to reduce breathlessness
- Airway clearance to manage mucus
- Tailored exercise plans at the right pace
- Confidence in what is safe to do
You may be offered this as pulmonary rehabilitation.
If you have not been referred, it is worth asking your GP or specialist team.
⚠️ Important safety advice (including bleeding risk)
Exercise is helpful for many people with aspergillosis — but it is not always appropriate to increase activity without guidance.
Be especially cautious if you have:
- Coughing up blood (haemoptysis) — current or recent
- An aspergilloma (fungal ball)
- Lung cavities
- A recent flare or worsening symptoms
Why this matters
In some forms of aspergillosis, blood vessels in the lungs can become fragile. Strain or increased pressure in the chest can increase the risk of bleeding.
When to stop and seek advice
- Coughing up blood (even small amounts)
- Sudden increase in breathlessness
- Chest pain or tightness
- Feeling significantly worse after activity
How to exercise more safely (if stable)
- Keep activity gentle and controlled
- Avoid heavy lifting or straining
- Avoid holding your breath during exertion
- Build activity gradually
If you are unsure, seek advice from your specialist team or a respiratory physiotherapist before increasing activity.
What progress really looks like
Improvement is rarely a straight line.
- Some days will be better than others
- Setbacks are common
- Progress may be slow but meaningful
This is normal in chronic lung conditions.
When to seek medical advice
Contact your healthcare team if you experience:
- New or worsening breathlessness
- Changes in cough or sputum
- Chest pain
- Coughing up blood
- Severe or persistent fatigue
Final message
Living with aspergillosis changes how your body responds to activity.
But improvement is possible — with the right approach.
Build slowly, pace yourself, and get the right support — especially from a respiratory physiotherapist.
In one sentence
Exercise can help — but it must be paced, personalised, and safe for your type of aspergillosis.
Author: Graham Atherton and ChatGPT draft support
For review by: National Aspergillosis Centre
Note: This article is for general information and does not replace medical advice.
Understanding the Journey to Diagnosis (Start Here)
Last reviewed: 18 March 2026
Key points
- Aspergillosis can be difficult to diagnose because symptoms often overlap with more common illnesses.
- Long diagnostic journeys are common in many chronic and uncommon conditions, not just aspergillosis.
- Uncertainty does not mean symptoms are unreal.
- Diagnosis often becomes clearer over time, as symptoms, scans, tests, and patterns build up.
- Good communication, ongoing review, and specialist input can make a major difference.
Why we created this series
People living with aspergillosis often tell us that the hardest part was not only the illness itself, but the time before they had an answer. Many describe repeated symptoms, multiple appointments, courses of treatment that only partly helped, and a growing sense that something still did not fit.
This experience is common in conditions such as chronic pulmonary aspergillosis (CPA) and allergic bronchopulmonary aspergillosis (ABPA), but it is also seen much more widely across medicine.
We created this series to help make sense of that process in a way that is:
- clear and accessible for patients and carers
- respectful of clinicians working within complex systems
- honest about uncertainty, delay, and emotional impact
- useful for improving understanding on both sides
The articles in this series
1. Why Aspergillosis Is So Hard to Diagnose
This article explains why aspergillosis can be difficult to recognise, why medicine usually starts with more common explanations, and how diagnosis often depends on patterns building up over time rather than one single test.
Best for: understanding the overall process and why delays can happen.
2. When Symptoms Are Real but Answers Are Not: Understanding Uncertainty
This article looks at the emotional and communication side of the diagnostic journey, including why patients may feel unheard, what clinicians may mean when they speak cautiously, and why unexplained symptoms are still real symptoms.
Best for: understanding uncertainty, communication gaps, and the experience of not yet having answers.
3. Why Diagnosis Can Take Time — and Why You Are Not Alone
This article places the diagnostic journey in a wider context, showing that long paths to diagnosis are common in many chronic and complex conditions, and offering reassurance that patients are not alone in this experience.
Best for: reassurance, perspective, and recognising that this journey is shared by many others.
Who may find this series helpful
This series may be useful if you are:
- a patient with ongoing respiratory symptoms and no clear diagnosis yet
- a carer or family member trying to understand what your loved one is going through
- a person recently diagnosed with aspergillosis and looking back on a long journey
- a general practitioner, respiratory clinician, nurse, or allied health professional wanting to better understand the patient perspective
It may also help people with other chronic conditions, because many of the same themes—uncertainty, overlap of symptoms, repeated reassessment, and eventual recognition—are seen across a wide range of illnesses.
When to seek medical advice
Seek medical advice if you have ongoing or worsening symptoms that are not improving as expected, especially if they keep returning or no longer fit the original explanation.
Seek urgent medical advice if you have symptoms such as:
- coughing up blood
- rapidly worsening breathlessness
- new chest pain
- significant unexplained weight loss
- high fever or signs of severe infection
If you already have an underlying lung condition and your usual treatment no longer seems to be working, it is reasonable to ask whether the diagnosis needs to be reviewed.
Related resources
Why Diagnosis Can Take Time — and Why You Are Not Alone
Last reviewed: 18 March 2026
Key points
- Long diagnostic journeys are common in many chronic and rare conditions—not just aspergillosis.
- Delays do not mean your symptoms were not real or important.
- Diagnosis often becomes clear over time, as patterns develop.
- Many patients go through similar experiences before reaching answers.
- Specialist centres play an important role when conditions are complex.
You are not alone in this
One of the most important things to understand is this:
Long and difficult diagnostic journeys are common—especially in chronic or complex illness.
Many people living with conditions such as chronic pulmonary aspergillosis (CPA) or allergic bronchopulmonary aspergillosis (ABPA) describe months or years of symptoms before a clear diagnosis was made.
This experience, while frustrating, is not unusual—and it does not mean your care has failed.
This happens in many conditions
Aspergillosis is not unique in this respect.
Similar diagnostic journeys are seen in:
- chronic lung diseases
- autoimmune conditions
- rare infections
- conditions with overlapping symptoms (e.g. fatigue syndromes)
In all of these, the same pattern often occurs:
- early symptoms are non-specific
- common conditions are treated first
- tests may initially be normal
- the true pattern only becomes clear over time
Why time helps diagnosis
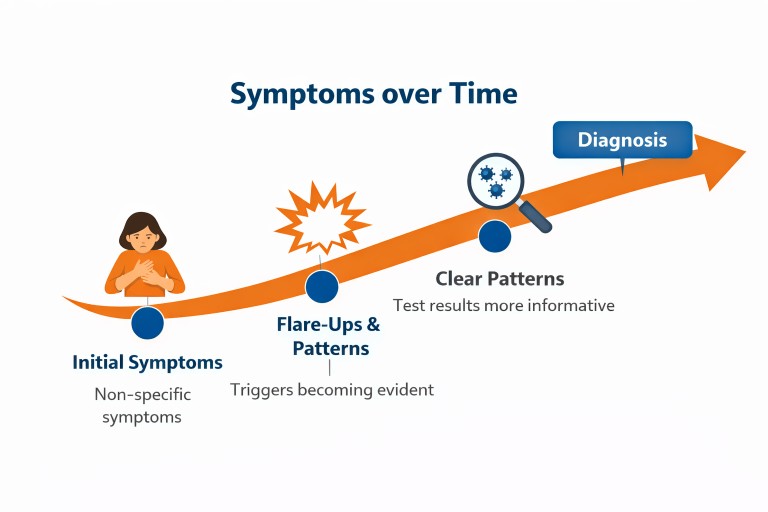
Although it can feel like delay, time often provides essential information.
Patterns emerge
- symptoms become more consistent
- flare-ups follow recognisable triggers
- response to treatment becomes clearer
Tests become more informative
- changes appear on imaging (e.g. CT scans)
- blood markers become more clearly abnormal
- microbiology results become more consistent
What was unclear early on can become much more visible later.
The turning point
Many patients describe a moment when things begin to change:
- symptoms no longer fit common conditions
- treatments stop working as expected
- a clinician recognises a pattern
This is often the point where less common diagnoses—including aspergillosis—are considered.
The role of specialist centres
Complex conditions are often best diagnosed in specialist centres with experience in that field.
In the UK, the National Aspergillosis Centre provides:
- expert multidisciplinary assessment
- access to specialist diagnostics
- experience in recognising patterns of disease
Referral to a specialist centre is often a key step in reaching a diagnosis.
The emotional impact
Long periods without answers can be deeply challenging.
Patients often describe:
- frustration and uncertainty
- feeling unheard or misunderstood
- loss of confidence in their own body
These reactions are entirely understandable.
Your experience is valid—even if the diagnosis took time to emerge.
Moving forward
Once a diagnosis is made, many patients feel a sense of relief—even if treatment is still needed.
A diagnosis provides:
- an explanation for symptoms
- a direction for treatment
- a clearer future plan
Even before diagnosis, it is important to remember:
You are still on a pathway—just not always a straight one.
Common questions
Does a long delay mean something was missed?
Not necessarily. Many conditions are only diagnosable once they have developed further.
Should I have been referred earlier?
Sometimes earlier referral is helpful, but it usually depends on how symptoms evolve over time.
Is this unique to aspergillosis?
No—this pattern is seen across many chronic and rare conditions.
Related pages
Why Aspergillosis Is So Hard to Diagnose
Last reviewed: 18 March 2026
Key points
- Aspergillosis is often difficult to diagnose because its symptoms can look very similar to those of more common conditions.
- Diagnosis usually depends on several pieces of evidence being brought together, rather than one simple test.
- Doctors are trained to consider common conditions first, because this is usually the safest and most efficient approach.
- This approach works well for many patients, but it can delay recognition of conditions such as aspergillosis.
- Delays are often caused by the way healthcare systems are organised, not by lack of care or effort from individual clinicians.
- Patients can help by keeping a clear record of symptoms, tests, treatments, and how things have changed over time.
Why diagnosis can be difficult
Aspergillosis is not a single illness but a group of conditions caused by Aspergillus, a mould commonly found in the environment. These include:
- Allergic bronchopulmonary aspergillosis (ABPA)
- Chronic pulmonary aspergillosis (CPA)
- Other airway and colonisation-related conditions
Diagnosis usually depends on combining:
- symptoms over time
- CT scan findings
- blood tests (including immunological tests)
- sputum microbiology
- clinical history
There is rarely a single “yes or no” test, which is why diagnosis can take time.
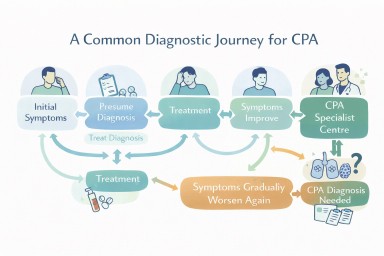
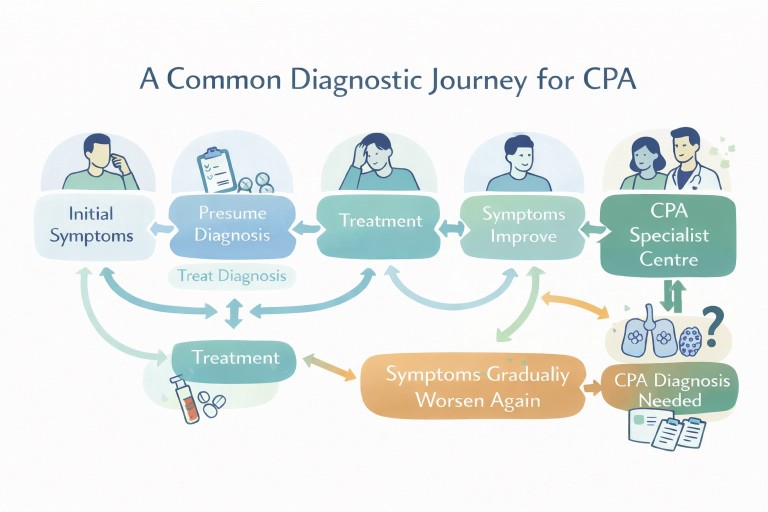
What the patient journey often looks like
Early symptoms
Symptoms such as cough, breathlessness, fatigue, or sputum are common across many conditions including bronchiectasis, asthma, and infection.
Treatment for common conditions
Initial treatment often includes antibiotics, inhalers, or steroids. These are appropriate first steps based on clinical guidelines such as those from the British Thoracic Society (BTS).
Ongoing symptoms
When symptoms persist or return, further investigation is usually needed.
The turning point
At some stage, fungal disease may be considered and tests for Aspergillus are performed.
Why doctors tackle common conditions first
Why do doctors start with common conditions?
Doctors treat common diseases first, prioritizing efficiency, patient safety, and high-probability outcomes. This approach, considering the most likely diagnosis first, helps manage patient health efficiently and effecctively before investigating rare or complex conditions.
This approach is safe and effective for most people, but conditions like aspergillosis can sit outside these usual pathways.
Where delays can happen
Overlap of symptoms
Symptoms overlap with many conditions, including tuberculosis and lung cancer.
No single definitive test
Diagnosis often requires combining multiple test results rather than relying on one.
Gradual disease progression
Conditions such as CPA may evolve over months or years.
Multiple conditions
Patients may have more than one lung condition at the same time.
Why this is often about the system, not the individual doctor
Healthcare systems are designed to manage large numbers of patients efficiently and safely. This means prioritising common conditions first.
However, aspergillosis often requires specialist input. In the UK, this may include referral to the National Aspergillosis Centre, which provides expert assessment and management.
International guidance from organisations such as ESCMID (European Society of Clinical Microbiology and Infectious Diseases) also highlights the complexity of fungal diseases.
What patients can do
- Keep a record of symptoms and treatments
- Ask when diagnosis should be reviewed
- Discuss whether further tests are needed
- Use trusted information sources such as our diagnosis guide
A more balanced way to think about delay
Diagnosis is often not a single event but a process that unfolds over time.
The goal is to recognise patterns earlier and ensure patients who need specialist input are identified sooner.
Common questions
Why was I treated for other conditions first?
Because those conditions are more common and more likely.
Should I ask about aspergillosis?
Yes, especially if symptoms are persistent or unusual—but it should be part of a broader discussion.
When to seek medical advice
- Persistent or worsening symptoms
- Coughing up blood
- Unexplained weight loss