When Symptoms Are Real but Answers Are Not: Understanding Uncertainty
Last reviewed: 18 March 2026
Key points
- Many people experience a period where symptoms are real but no clear diagnosis has been made.
- This can sometimes feel like being told “nothing is wrong” or “it is all in your head”.
- In most cases, this reflects uncertainty in the system, not disbelief from clinicians.
- Conditions such as aspergillosis can take time to become recognisable.
- Physical and psychological factors can overlap—but unexplained symptoms are still real symptoms.
- Clear communication and ongoing review are key to moving forward.
The experience many patients describe
During a long diagnostic journey, many people reach a point where they hear phrases such as:
- “Your tests are normal”
- “We can’t find anything serious”
- “It may be stress or anxiety contributing”
Even when these words are carefully chosen, they can feel like:
“Nothing is wrong” or “it’s all in my head”
This can be one of the most difficult parts of the journey—especially when symptoms are ongoing, disruptive, and clearly real.
Why this happens
This situation usually reflects the limits of current medical systems rather than a lack of concern.
Tests do not always give clear answers
Modern medicine relies heavily on tests. But for many conditions—including chronic pulmonary aspergillosis (CPA)—tests may:
- be negative early on
- show unclear or borderline results
- require interpretation over time
This creates a gap between:
- what the patient is experiencing
- what can currently be measured
Medicine is designed to provide answers
Clinicians are trained to explain symptoms and reassure patients. When no clear diagnosis is available, they may turn to explanations such as:
- stress
- anxiety
- functional symptoms
These are real and valid factors—but if introduced too early, they can feel like the search has stopped.
Time pressure
Short consultations can mean:
- less time to explain uncertainty
- less opportunity to validate patient experience
- simplified explanations that lose nuance
What doctors mean vs what patients hear

Often, the issue is not what is said—but how it is understood.
| What may be said | What may be heard |
|---|---|
| “Your tests are normal” | “Nothing is wrong” |
| “We haven’t found a cause yet” | “There is no cause” |
| “Stress may be contributing” | “It’s all in your head” |
Understanding this gap can help both patients and clinicians move forward more constructively.
A critical clarification
Not having a diagnosis is not the same as not having a disease.
Unexplained symptoms are still real symptoms.
Medicine does not always have immediate answers—especially for conditions that develop slowly or do not fit standard patterns.
Physical and psychological overlap
It is important to take a balanced view.
- Physical illness can lead to anxiety, fatigue, and distress
- Anxiety can worsen physical symptoms such as breathlessness
This relationship is two-way, not either/or.
The problem arises when psychological explanations replace further investigation, rather than sitting alongside it.
Why this matters in aspergillosis
Conditions such as aspergillosis often:
- develop gradually
- have non-specific symptoms
- require multiple tests over time
This makes periods of uncertainty more likely, particularly before a diagnosis such as allergic bronchopulmonary aspergillosis (ABPA) or CPA is confirmed.
You can read more about this in Why Aspergillosis Is So Hard to Diagnose.
What patients can do
- Keep a record of symptoms and how they change over time
- Ask what the current working diagnosis is
- Ask when the situation should be reviewed
- Share concerns clearly, but remain open to different explanations
Helpful questions include:
- “What else could this be?”
- “What would make you reconsider the diagnosis?”
- “When should we review this again?”
A shared understanding
This situation is not about:
- patients being dismissed
- clinicians not caring
It reflects a deeper reality:
Medicine does not always have immediate answers—especially for complex or evolving conditions.
The goal is to keep the process open, respectful, and moving forward.
Common questions
Does this mean doctors think I’m imagining symptoms?
No. It usually reflects uncertainty rather than disbelief.
Can stress really affect physical symptoms?
Yes—but this should not stop appropriate medical investigation.
What should I do if I feel dismissed?
Ask for clarification, a review plan, or a second opinion if needed.
Related pages
Managing fatigue and energy in aspergillosis and allergic fungal lung disease
Key points
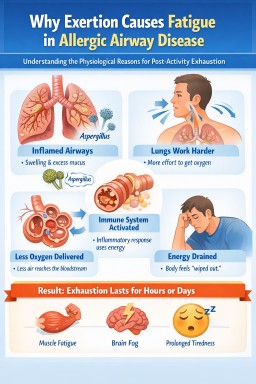
- Many people with aspergillus-related lung conditions experience extreme tiredness after physical or mental exertion.
- This fatigue can last hours or even several days.
- Breathing, immune activity, inflammation and sometimes hormone imbalance all use extra energy.
- Activity can temporarily increase airway inflammation and mucus.
- Managing energy carefully (“spoon theory”) can help prevent fatigue crashes.
Contents
- Why people with lung disease feel exhausted after exertion
- What is happening in the lungs and body
- Managing energy: the “spoon theory”
- Practical ways to manage energy
- Nutrition and adrenal health
- Warning signs you are running out of energy
- Why fatigue in lung disease is different from normal tiredness
- Daily energy management checklist
- Can this fatigue be treated?
- When to talk to your doctor
Why people with lung disease feel exhausted after exertion
Healthy lungs have a large reserve capacity. When we exercise or do physical work, breathing becomes deeper and faster, but the lungs can usually cope easily.
In people with aspergillosis or allergic airway disease, the airways may already be:
- inflamed
- narrowed
- filled with mucus
- sensitive to allergens such as Aspergillus fumigatus
When the body demands more oxygen during activity, the lungs must work much harder to supply it. Activities that seem minor to other people may therefore require much greater effort from the body.
What is happening in the lungs and body?
Inflamed airways
Many aspergillus-related conditions involve inflammation in the airways. The immune system releases chemicals that cause:
- swelling of airway walls
- increased mucus production
- greater airway sensitivity
During exertion, breathing becomes faster and deeper, which can irritate these inflamed airways further.
Mucus affecting airflow
Inflamed airways often produce extra mucus. This mucus can partly block airflow and lead to:
- coughing
- wheezing
- breathlessness
- uneven airflow within the lungs
This may reduce how efficiently oxygen enters the bloodstream. Doctors sometimes refer to this as ventilation–perfusion mismatch.
Breathing uses more energy
In healthy people, breathing uses only a small fraction of the body's energy. In lung disease, breathing may require much more effort.
Additional muscles may assist breathing, including:
- chest muscles
- neck muscles
- shoulder muscles
These muscles can become fatigued during activity, just like leg muscles after exercise.
Immune system activity
If the immune system reacts to fungal proteins or allergens, it releases signalling chemicals called cytokines. These chemicals can produce symptoms similar to mild illness, including fatigue, brain fog and muscle aches.
Delayed inflammation after activity
Some people notice that fatigue appears later rather than immediately. Physical effort can trigger inflammation that develops over 12–48 hours, increasing mucus production, airway irritation and tiredness.
This explains why people sometimes feel worse the day after a busy day.
Managing energy: the “spoon theory”
Many people with chronic illness find it helpful to think about their energy using the idea of spoon theory.
In this idea:
- each spoon represents a small unit of energy
- you start the day with a limited number of spoons
- each activity uses some of those spoons
Because breathing and inflammation already use energy, people with lung disease may begin the day with fewer spoons available.
Example of spoon use
| Activity | Possible energy use |
|---|---|
| Getting dressed | 1 spoon |
| Showering | 2–3 spoons |
| Cooking a meal | 2 spoons |
| Doctor’s appointment | 3–4 spoons |
| Busy social day | Many spoons |
If too many spoons are used early in the day, the body may run out of energy, leading to exhaustion lasting hours or even days.
Practical ways to manage energy
Plan activities around your best time of day
| Time of day | Suggested activities |
|---|---|
| Morning | Errands or appointments |
| Midday | Light household tasks |
| Afternoon | Quieter activities |
| Evening | Rest and recovery |
Break tasks into smaller steps
Large tasks can overwhelm the lungs and muscles. Instead of doing everything at once:
- clean one room at a time
- cook in stages
- prepare things earlier in the day
Use the 50–70% rule
Try to stop activity when you reach about half to two-thirds of your limit. Stopping early often prevents the fatigue crash that can occur later.
Use breathing techniques
Pursed-lip breathing
- breathe in through your nose
- breathe out slowly through gently pursed lips
Rhythmic breathing
Match breathing with movement, for example when climbing stairs.
Keep mucus moving
Mucus increases the work of breathing. Helpful strategies include:
- airway clearance techniques
- staying well hydrated
- gentle movement
- using inhalers or nebulisers as prescribed
Maintain gentle regular activity
Although exertion can cause fatigue, complete inactivity can worsen the problem. Gentle activity such as walking or pulmonary rehabilitation exercises helps maintain muscle strength.
Protect sleep
- maintain a regular sleep routine
- clear mucus before bedtime if needed
- avoid heavy exertion late in the evening
Nutrition and adrenal health
Nutrition and energy
Good nutrition helps support energy levels. Helpful strategies include:
- eating regular meals
- including protein for muscle repair (eggs, fish, dairy, beans or nuts)
- eating complex carbohydrates for steady energy
- drinking enough fluids
Some people find that smaller, more frequent meals reduce breathlessness compared with large meals.
Important nutrients
- protein
- vitamin D
- iron
- B vitamins
Doctors may check for deficiencies if fatigue is severe.
Adrenal insufficiency
Some patients who have taken long-term steroid medications may develop adrenal insufficiency. The adrenal glands normally produce cortisol, which helps regulate energy and stress responses.
Symptoms may include:
- severe fatigue
- dizziness
- muscle weakness
- difficulty recovering after exertion
Patients with adrenal insufficiency usually take hydrocortisone replacement therapy and should follow their doctor’s advice carefully.
Warning signs you are running out of energy
- breathing becomes faster or more difficult
- increased coughing or mucus
- arms or legs feel heavy
- dizziness or weakness
- difficulty concentrating
- chest tightness or wheezing
When these warning signs appear, it is usually best to stop and rest before continuing.
Why fatigue in lung disease is different from normal tiredness
Fatigue in lung disease is not simply normal tiredness. Several factors occur at the same time:
- breathing requires more energy
- the immune system may be active
- oxygen exchange may be less efficient
- nutrition and hormone balance may influence recovery
Because of this combination, fatigue may appear suddenly and last longer than expected.
Daily energy management checklist
Pacing and activity
- spread activities across the day
- stop before exhaustion
- plan demanding tasks when energy is highest
- allow recovery time after busy days
Breathing and airway care
- use breathing techniques during exertion
- perform airway clearance if needed
- take inhalers or nebulisers as prescribed
- stay well hydrated
Nutrition and medication
- eat regular meals
- include protein for muscle strength
- take medications as prescribed
- follow sick-day rules if you have adrenal insufficiency
Sleep and recovery
- maintain a regular sleep routine
- clear mucus before bedtime
- rest when warning signs appear
Can this fatigue be treated?
Fatigue associated with aspergillosis, allergic fungal airway disease, or severe asthma can sometimes be improved when the underlying causes are treated. Because several different processes contribute to fatigue, treatment usually focuses on improving multiple factors rather than a single cure.
Treating airway inflammation
Inflammation in the airways is one of the major contributors to fatigue. When the airways are inflamed:
- breathing requires more effort
- mucus production increases
- oxygen exchange becomes less efficient
Treatments aimed at reducing airway inflammation may include:
- Inhaled corticosteroids – commonly used in asthma to reduce inflammation directly in the airways.
- Antifungal therapy – in some patients, reducing fungal growth can reduce immune activation and inflammation.
- Biologic therapies – newer treatments that target specific immune pathways involved in allergic and inflammatory lung disease.
Biologic treatments
Biologics are one of the most promising areas of treatment for severe asthma and allergic airway disease. These medications target specific parts of the immune system that drive inflammation.
| Biologic | Target | Effect |
|---|---|---|
| Omalizumab | IgE | Reduces allergic inflammation |
| Mepolizumab / Benralizumab | IL-5 pathway | Reduces eosinophilic inflammation |
| Dupilumab | IL-4 / IL-13 | Reduces type-2 inflammation |
| Tezepelumab | TSLP | Blocks upstream inflammatory signalling |
Some patients with conditions such as allergic bronchopulmonary aspergillosis (ABPA) or severe asthma report improvements in breathlessness, symptoms and overall energy levels when inflammation is better controlled.
Improving mucus clearance
Mucus in the airways increases the work of breathing and can contribute to fatigue. Strategies that may help include:
- airway clearance techniques
- physiotherapy
- maintaining good hydration
- using prescribed inhalers or nebulisers correctly
Treating other contributing factors
Fatigue can also be worsened by other health issues that are common in chronic lung disease, such as:
- iron deficiency
- vitamin deficiencies
- poor sleep
- adrenal insufficiency
- muscle deconditioning
Addressing these factors can sometimes improve overall energy levels.
Pulmonary rehabilitation
Pulmonary rehabilitation programmes combine exercise training, breathing techniques and education about pacing activities. These programmes can improve muscle efficiency and exercise tolerance, and many patients report reduced fatigue and improved quality of life.
Future treatments
Research into inflammatory lung diseases is advancing rapidly. New biologic drugs and other targeted therapies are being developed that may improve control of airway inflammation.
Researchers are also studying how the lung microbiome (bacteria and fungi living in the airways) influences inflammation. In the future, this may lead to more personalised treatments for patients with fungal-related lung disease.
Inflammatory fatigue
Researchers are increasingly recognising that chronic inflammatory diseases can cause a form of fatigue sometimes called “inflammatory fatigue.”
In these conditions, immune signalling chemicals released during inflammation can affect the brain and energy metabolism. Similar patterns of fatigue are seen in diseases such as rheumatoid arthritis and inflammatory bowel disease.
This may help explain why some treatments that reduce inflammation — including biologic therapies — can improve fatigue even when lung function measurements change only modestly.
Interrupting the fatigue cycle
Treatment aims to interrupt the cycle that can develop in chronic lung disease:
Airway inflammation
↓
Breathing requires more effort
↓
More energy used by respiratory muscles
↓
Immune system activity
↓
Reduced overall energy and fatigue
By improving airway inflammation, mucus clearance, muscle strength and overall health, many patients find their energy levels become more manageable.
When to talk to your doctor
Seek medical advice if:
- fatigue becomes progressively worse
- breathlessness increases
- new symptoms appear such as chest pain or coughing up blood
- fatigue prevents normal daily activities
A reassuring message
Many people with aspergillosis or allergic airway disease worry that exhaustion means their condition is worsening.
In most cases it reflects the extra energy required for breathing, inflammation and immune activity. Learning to pace activity can help people live more comfortably with chronic lung disease.
Author: National Aspergillosis Centre information team
Review: Clinical review recommended
Last reviewed: 2026
Using AI Safely When You Have Aspergillosis
Artificial intelligence (AI) tools (for example, ChatGPT and other “medical chatbots”) can help people living with aspergillosis understand information, prepare for appointments, and feel more confident asking questions.
Used well, AI can be like a helpful explainer.
Used badly, it can be misleading — especially for conditions like aspergillosis where treatment decisions are complex.
This page explains what is safe, what is not safe, and how to use AI in a way that supports (not replaces) your clinical team.
Who is this page for?
This guidance is for people affected by:
-
Chronic Pulmonary Aspergillosis (CPA)
-
Allergic Bronchopulmonary Aspergillosis (ABPA)
-
Severe Asthma with Fungal Sensitisation (SAFS)
-
Aspergillus bronchitis
-
Other long-term Aspergillus-related lung problems
A simple rule that keeps you safe
AI should improve your understanding — it should not change your treatment.
If an AI tool suggests starting, stopping, or changing medication, do not act on it without speaking to your clinician.
What AI is good for
AI tools are usually helpful for:
Explaining medical words in plain language
Examples:
-
“What is Aspergillus Immunoglobulin G (IgG)?”
-
“What does ‘eosinophils’ mean?”
-
“What is a CT scan finding such as ‘cavity’ or ‘bronchiectasis’?”
Understanding medicines (general information)
AI can explain:
-
What a medicine is for
-
How it works in the body
-
Common side effects (in general terms)
-
Why monitoring is needed
This can be helpful for antifungal medicines such as itraconazole, voriconazole, posaconazole, and isavuconazole.
Preparing for appointments
AI can help you create a list of questions, for example:
-
“What monitoring do I need while on antifungals?”
-
“What symptoms should prompt urgent review?”
-
“How do we judge whether treatment is working?”
Summarising research articles
If you paste a paragraph from a paper (or describe it), AI can often translate it into patient-friendly language.
(Always remember: AI can sometimes get details wrong — see below.)
Organising your story
Many people find it useful to ask AI to format:
-
A timeline of symptoms
-
A list of medicines and dates
-
A short “what I want from this appointment” summary
This can make consultations more productive.
What AI is NOT safe for
AI should not be used for:
Diagnosis
Aspergillosis diagnosis usually depends on a careful combination of:
-
Symptoms and clinical history
-
Imaging (often computed tomography, CT)
-
Blood tests
-
Sputum tests / microbiology
-
Sometimes bronchoscopy results
AI cannot reliably “diagnose” from symptoms or a single test result.
Treatment decisions
Do not use AI to decide:
-
Whether you should start or stop antifungals
-
Steroid doses or tapering plans
-
Whether you “should” try biologics (for example, omalizumab)
-
Whether a side effect is safe to ignore
These decisions must be individualised and clinician-led.
Urgent situations
If you have worsening breathlessness, fever, chest pain, or coughing blood (haemoptysis), seek medical advice urgently.
AI is not an emergency service.
Why aspergillosis needs extra caution
Aspergillosis care can be complicated because:
-
Some antifungal medicines have important drug interactions
-
Blood levels may need monitoring (therapeutic drug monitoring)
-
Side effects can overlap with symptoms of lung disease
-
Different Aspergillus-related conditions can look similar but need different management
AI tools can also:
-
Over-generalise from asthma guidance
-
Confuse chronic disease with invasive disease
-
“Hallucinate” (invent) facts, references, or confident-sounding explanations
-
Be out of date
Privacy and confidentiality: what not to share with AI
To protect your privacy, avoid typing in:
-
Your full name
-
Date of birth
-
NHS number
-
Home address
-
Phone number
-
Identifiable clinic letters or reports (unless anonymised)
A safer way to write questions
Instead of pasting an entire letter, use a summary like:
“Adult with chronic lung disease, on itraconazole 200 mg daily, recent CT shows cavities, asking about monitoring and side effects.”
That’s usually enough for education and planning questions.
A safe “4-step” way to use AI
-
Ask AI to explain (terms, tests, general concepts)
-
Ask AI to help you prepare questions
-
Discuss those questions with your clinician
-
Only change treatment after clinical advice
A quick safety checklist
Before trusting an AI answer, ask:
-
Is this general education, or is it telling me what I should do?
-
Does it recommend changing my medicine or dose?
-
Does it mention checking interactions or monitoring?
-
Does it conflict with my current plan?
-
Is this situation urgent?
If any answer worries you: pause and ask your care team.
Example prompts patients can use safely
You can copy/paste these into an AI tool:
-
“Explain Chronic Pulmonary Aspergillosis (CPA) in plain language.”
-
“What questions should I ask about long-term itraconazole treatment?”
-
“What monitoring is commonly recommended for antifungal medicines?”
-
“Can you help me write a one-page symptom and medication summary for my clinic appointment?”
-
“Here is a paragraph from a research paper — can you summarise it in patient-friendly language and list any uncertainties?”
Tip: If you want a more cautious response, add:
“Please be conservative and tell me what you’re unsure about.”
Signs an AI answer may be unreliable
Be cautious if the AI:
-
Sounds very confident but gives no clear reasoning
-
Gives exact doses or taper schedules
-
Claims “this is definitely ABPA/CPA” from limited information
-
Provides references you cannot find elsewhere
-
Dismisses side effects, interactions, or monitoring
-
Encourages you to delay medical care
Final reminder
AI can be a helpful tool for understanding and preparing — but it is not a substitute for a specialist team.
If you are unsure, or something feels wrong, it is always reasonable to contact your clinician, specialist nurse, or GP.
Medical disclaimer
This page is for general information only and is not medical advice. Always follow the guidance of your healthcare team, especially regarding diagnosis, medicines, and urgent symptoms.
Travelling with Aspergillosis: A Comprehensive Guide to Safe and Stable Travel
This guide is for people living with:
- Chronic Pulmonary Aspergillosis (CPA)
- Allergic Bronchopulmonary Aspergillosis (ABPA)
- Severe asthma (including fungal sensitisation)
- Bronchiectasis
- Fibrotic or structurally abnormal lung disease
Most people with stable disease can travel successfully. The goal is not restriction — it is risk reduction through preparation, environmental awareness, and early action if symptoms change.
Contents
- 1. Understanding Travel Risk in Aspergillosis
- 2. Coordinating With Your Medical Team
- 3. Assessing Stability Before Travel
- 4. Choosing a Destination: Environmental Determinants
- 5. Regional Risk Patterns Explained
- 6. Air Pollution & AQI Monitoring
- 7. Heat, Humidity & Hydration Physiology
- 8. Travel Insurance & Disclosure
- 9. Medication Planning & Contingency Prescriptions
- 10. Specific Considerations for Azole Antifungals
- 11. Air Travel: Physiology & Fit-to-Fly
- 12. Cabin Dryness & Post-Flight Irritation
- 13. Travelling with Oxygen
- 14. Accommodation Risk Reduction
- 15. High-Spore & Dust Exposure Environments
- 16. Infection Prevention
- 17. Haemoptysis Planning
- 18. Red Flag Symptoms
- 19. Advanced Planning Checklist
1. Understanding Travel Risk in Aspergillosis
Travel risk arises from four domains:
- Structural lung vulnerability (cavities, fibrosis, bronchiectasis)
- Inflammatory instability (ABPA activity, asthma control)
- Environmental exposure (humidity, dust, pollution)
- Healthcare accessibility (if deterioration occurs)
Travel is usually safe when disease is stable and exposures are predictable.
2. Coordinating With Your Medical Team
Respiratory Clinic
- Review recent imaging (particularly in CPA)
- Assess haemoptysis history
- Consider fit-to-fly testing if oxygen saturation borderline
- Discuss standby rescue medication
GP
- Ensure medication supply exceeds travel duration
- Provide updated medication summary
- Support vaccination review
- Assist with insurance documentation
3. Assessing Stability Before Travel
Delay travel if within 4–6 weeks of:
- Significant haemoptysis
- Escalating breathlessness
- Recent hospital admission
- New antifungal initiation
Stable inflammatory markers and symptom plateau are reassuring.
4. Choosing a Destination: Environmental Determinants
Key determinants:
- Humidity: promotes indoor mould growth
- Flood history: water damage increases fungal load
- Air pollution: triggers bronchospasm
- Dust burden: irritates inflamed airways
- Healthcare infrastructure: safety net if unwell
5. Regional Risk Patterns Explained
Lower Overall Respiratory Stress
- Scandinavia
- New Zealand
- Canada (outside wildfire season)
Cooler climates limit mould growth; strong building codes reduce damp housing.
Moderate Risk
- Mediterranean Europe
Generally safe when stable; monitor wildfire smoke and heat stress.
Higher Respiratory Stress
- Tropical monsoon climates
- Flood-prone regions
- Highly polluted megacities
- Dust storm zones
Humidity increases fungal proliferation; particulate pollution worsens airway inflammation.
6. Air Pollution & AQI Monitoring
Air pollution can exacerbate cough, bronchospasm, breathlessness and fatigue in people with chronic lung disease. In some urban environments, pollution may pose a greater day-to-day risk than fungal exposure.
The most widely used measure of air quality is the Air Quality Index (AQI), which combines several pollutants into a single score.
Key Pollutants That Matter in Lung Disease
- PM2.5 – fine particulate matter small enough to penetrate deep into the lungs
- PM10 – larger inhalable particles
- Ozone (O₃) – irritates airways, especially in heat
- Nitrogen dioxide (NO₂) – associated with traffic pollution
PM2.5 is particularly important in aspergillosis and severe asthma because it can:
- Trigger airway inflammation
- Increase mucus production
- Worsen bronchospasm
- Reduce exercise tolerance
Reliable Air Quality Monitoring Resources
These sites provide real-time data and forecasts:
- World Air Quality Index (WAQI)
https://waqi.info
Interactive global map with live AQI data for cities worldwide. - IQAir (AirVisual)
https://www.iqair.com
Detailed pollutant breakdowns, 7-day forecasts and wildfire smoke tracking. - UK Daily Air Quality Index (DEFRA)
https://uk-air.defra.gov.uk
Official UK monitoring network with health advice bands.
These platforms also offer mobile apps, which are useful for checking conditions while travelling.
How to Interpret AQI in Practical Terms
| AQI | Category | Practical Advice for Lung Conditions |
|---|---|---|
| 0–50 | Good | Ideal conditions for outdoor activity |
| 51–100 | Moderate | Usually safe; monitor symptoms |
| 101–150 | Unhealthy for sensitive groups | Reduce strenuous outdoor activity; consider indoor plans |
| 151–200 | Unhealthy | Limit time outdoors; avoid exertion |
| 200+ | Very Unhealthy/Hazardous | Stay indoors with filtered air if possible |
For many patients with CPA, ABPA or severe asthma, an AQI above 100 warrants caution. Above 150, limiting outdoor exposure is advisable.
Wildfire Smoke
Wildfire smoke contains high concentrations of PM2.5 and organic particulates. Even patients who are stable at home may experience:
- Increased cough
- Chest tightness
- Increased sputum production
- Fatigue
If travelling during wildfire season:
- Check AQI daily
- Plan indoor activities when levels are elevated
- Use air-conditioned or filtered indoor environments
- Carry rescue inhalers
Urban Pollution vs Rural Dust
Urban areas are more affected by traffic-related pollutants (NO₂, PM2.5), while rural or desert areas may present dust exposure. Both can aggravate inflamed airways.
The risk is cumulative. Short exposure is usually tolerated; prolonged high-level exposure increases the likelihood of symptom flare.
Key principle: checking AQI before and during travel is one of the simplest and most effective risk-reduction steps for people with chronic lung disease.
7. Heat, Humidity & Hydration Physiology
Hot climates place additional physiological stress on people with chronic lung disease.
Why Heat Matters
In warm environments, the body increases sweating and respiratory water loss to regulate temperature. This leads to:
- Increased insensible fluid loss (fluid lost through breathing and skin)
- Reduced plasma volume if intake is inadequate
- Thickening of airway secretions
In bronchiectasis and chronic pulmonary aspergillosis (CPA), mucus clearance is already impaired. Dehydration increases mucus viscosity, making sputum:
- Harder to expectorate
- More likely to stagnate in damaged airways
- Potentially more prone to secondary infection
Patients may notice thicker sputum, increased cough, or chest tightness in hot weather.
Humidity: Helpful or Harmful?
Humidity has mixed effects:
- Moderate humidity can help prevent airway drying.
- High humidity can increase environmental mould growth, particularly indoors if ventilation is poor.
In tropical or monsoon climates, poorly ventilated buildings may have higher fungal spore burdens due to damp conditions.
Heat, Fatigue & Breathlessness
Heat increases cardiovascular demand. The heart works harder to dissipate heat, which can:
- Increase perceived breathlessness
- Increase fatigue
- Reduce exercise tolerance
This does not necessarily indicate worsening lung disease — but it can feel similar.
Hydration Strategy
Practical recommendations:
- Begin hydrating the day before travel
- Drink fluids regularly rather than waiting for thirst
- Aim for pale straw-coloured urine
- Increase intake during flights and hot excursions
Limit:
- Excess alcohol (diuretic effect)
- High caffeine intake
Additional Practical Measures
- Plan outdoor activity early morning or evening
- Rest during peak heat (midday)
- Use air-conditioned environments when available
- Continue airway clearance routines while travelling
Key principle: in chronic lung disease, hydration supports mucus clearance and reduces avoidable exacerbation risk during hot weather.
8. Travel Insurance & Full Medical Disclosure
Travel insurance is not a formality — it is a critical safety net for people with chronic lung disease.
When purchasing insurance, you must declare all pre-existing medical conditions. This typically includes:
- Chronic Pulmonary Aspergillosis (CPA)
- Allergic Bronchopulmonary Aspergillosis (ABPA)
- Severe asthma
- Bronchiectasis
- Pulmonary fibrosis
- Long-term steroid therapy
- Adrenal insufficiency (if present)
- Oxygen use (even if only occasional)
Why Full Disclosure Matters
If you fail to declare a relevant condition, the insurer may:
- Refuse to cover medical treatment abroad
- Decline repatriation costs
- Refuse to reimburse cancelled flights or accommodation
- Invalidate the entire policy
This applies even if the emergency appears unrelated. Insurers may review your full medical history during a claim.
What Insurers Typically Ask
You may be asked:
- Have you been hospitalised in the past 12 months?
- Have you had medication changes recently?
- Have you had haemoptysis?
- Are you awaiting tests or investigations?
- Are you on long-term steroids?
Answer these questions carefully and honestly.
Policies and Stability
Some insurers will decline cover if:
- You have been hospitalised recently
- You are awaiting investigations
- Your condition is considered unstable
This is another reason to travel during a period of clinical stability.
European Travel (UK Patients)
If travelling within Europe, ensure you carry:
- Your GHIC (Global Health Insurance Card)
However, GHIC does not replace travel insurance. It may not cover:
- Private healthcare
- Mountain rescue
- Repatriation to the UK
Practical Tips
- Purchase insurance as soon as you book travel
- Keep written confirmation of declared conditions
- Carry the insurer’s emergency contact number with you
- Inform the insurer early if you require hospital care abroad
In summary: full disclosure protects you. Insurance is only effective if the insurer understands your medical background from the outset.
9. Medication Planning & Contingency Prescriptions
- Carry 1–2 weeks extra supply
- Bring medications in original packaging
- Carry clinic letter
- Consider written rescue plan
10. Specific Considerations for Azole Antifungals
Azoles have significant drug–drug interactions.
- Inform any clinician abroad you are taking an azole
- Avoid grapefruit
- Be aware of sun sensitivity (voriconazole)
- Take itraconazole with food
11. Air Travel: What Actually Happens in the Cabin?
Commercial aircraft cabins are pressurised to simulate an altitude of approximately 6,000–8,000 feet (1,800–2,400 metres).
This means the partial pressure of oxygen is lower than at sea level. For healthy individuals this causes only a small drop in oxygen saturation (typically 3–4%).
Are Most People with Aspergillosis OK to Fly?
Yes — most stable patients fly without difficulty.
People who are:
- Clinically stable
- Not oxygen-dependent
- Without recent haemoptysis
- With resting oxygen saturations ≥95%
generally tolerate commercial flights well, including medium and long-haul travel.
Many patients report anxiety before their first flight after diagnosis, but in stable disease, significant problems are uncommon.
Who Should Consider Fit-to-Fly Testing?
Assessment may be appropriate if you have:
- Resting oxygen saturation consistently below 95%
- Advanced pulmonary fibrosis
- Extensive cavitation
- Significant breathlessness at minimal exertion
- Recent clinical deterioration
The test commonly used is a Hypoxic Challenge Test (HCT), which simulates cabin oxygen conditions to determine whether supplemental oxygen is required during flight.
Where would I have a Hypoxic Challenge Test (HCT)?
In the UK, a Hypoxic Challenge Test is usually arranged through a hospital respiratory physiology department.
You cannot book this test directly. It must be requested by:
- Your respiratory consultant or clinic, or
- Occasionally your GP (who would refer you to a hospital service)
The test is typically performed in:
- A hospital lung function laboratory
- A respiratory physiology unit
- A specialist respiratory centre
During the test, you breathe a gas mixture containing a lower oxygen concentration (usually around 15%) to simulate aircraft cabin conditions. Your oxygen saturation is monitored continuously. If levels fall below safe thresholds, in-flight oxygen may be recommended.
Do Most People Need This Test?
No. Many stable patients with normal resting oxygen saturation (typically ≥95%) do not require hypoxic challenge testing.
The test is generally considered if you:
- Have resting oxygen saturation below 95%
- Have advanced pulmonary fibrosis
- Are already using oxygen
- Have significant exertional desaturation
If you are unsure, ask your respiratory team whether assessment is appropriate for you.
Symptoms During Flight: What Is Normal?
Mild symptoms that can occur in stable patients include:
- Slight increase in breathlessness on walking the aisle
- Fatigue
- Dry cough (often due to low humidity)
These are usually temporary and not dangerous.
Severe symptoms (marked breathlessness at rest, chest pain, dizziness, confusion) are uncommon and require crew notification.
Anxiety vs Physiological Breathlessness
It is very common for people with chronic lung disease to experience heightened awareness of their breathing during flights. The enclosed environment, reduced cabin pressure and awareness of altitude can all increase anxiety.
Anxiety-related breathlessness typically presents as:
- A sensation of not getting a “satisfying” breath
- Chest tightness without wheeze
- Rapid breathing (hyperventilation)
- Tingling in fingers or lips
- Light-headedness
Hyperventilation lowers carbon dioxide levels in the blood. This can cause dizziness, tingling and a feeling of air hunger — even when oxygen levels are normal.
Physiological hypoxia (true low oxygen levels) is less common in stable patients who have been assessed as fit to fly. When it occurs, it is more likely in those with advanced fibrosis, low baseline oxygen saturations, or recent instability.
Features more suggestive of physiological compromise include:
- Persistent breathlessness at rest
- Worsening cyanosis (bluish lips or fingers)
- Marked fatigue or confusion
- Objective low oxygen saturation if measured
For patients who have undergone fit-to-fly assessment and been cleared to travel, significant in-flight hypoxia is uncommon.
Practical Strategies
- Use slow, paced breathing (e.g. inhale for 4 seconds, exhale for 6 seconds)
- Focus on extended exhalation to reduce hyperventilation
- Keep shoulders relaxed and posture upright
- Avoid repeatedly “checking” your breathing
- Remind yourself that mild symptoms are common and expected
Understanding the difference between anxiety-related breathlessness and true hypoxia can significantly reduce distress during flight.
Deep Vein Thrombosis (DVT) Risk
Chronic lung disease does not automatically increase DVT risk, but long-haul immobility does.
General advice:
- Move legs regularly
- Stay hydrated
- Avoid excess alcohol
12. Cabin Dryness & Post-Flight Airway Irritation
Cabin humidity is typically 10–20% (normal indoor comfort is 40–60%).
Low humidity can:
- Dry airway lining
- Reduce mucociliary clearance
- Thicken secretions
- Trigger cough or mild bronchospasm
This is often why people feel they have “caught a cold” the day after flying. In most cases, it is airway irritation rather than infection.
How to Reduce Dryness Effects
- Hydrate well before and during flight
- Limit alcohol and caffeine
- Use isotonic saline nasal spray
- Continue preventer inhalers
- Keep rescue inhaler accessible
- Avoid direct overhead air vents blowing onto your face
- Consider mask use — masks increase humidity of inhaled air
Symptoms typically settle within 24–48 hours.
When to Seek Advice After Flying
Seek medical advice if you develop:
- Progressively worsening breathlessness
- Persistent fever
- Significant haemoptysis
- Chest pain
In stable patients, serious in-flight deterioration is uncommon.
12. Cabin Dryness & Post-Flight Irritation
Cabin humidity is 10–20%.
Dry air:
- Reduces mucociliary clearance
- Thickens secretions
- Triggers cough
- Irritates airways
Hydration and saline sprays reduce symptoms. Post-flight irritation commonly lasts 24–48 hours and does not necessarily indicate infection.
13. Travelling with Oxygen
Confirm airline device approval and battery duration. Plan well in advance.
14. Accommodation Risk Reduction
Request:
- Hard flooring
- No damp odour
- No renovation dust
- Pet-free rooms
Chains Often Reported as Allergy-Conscious
- Hyatt
- Hilton
- Marriott
- Scandic
- Premier Inn
Newer business hotels often have better HVAC filtration.
15. High-Spore & Dust Exposure Environments
- Compost handling
- Construction sites
- Flood-damaged buildings
- Agricultural dust
Avoid heavy inhalation exposure.
16. Infection Prevention
- Hand hygiene
- Avoid close contact with visibly unwell individuals
- Maintain vaccination schedule
17. Haemoptysis Planning
If you have a history of haemoptysis:
- Know your previous pattern
- Carry clinic contact details
- Seek urgent care if volume increases significantly
18. Red Flag Symptoms
- Increasing breathlessness
- New or worsening haemoptysis
- Persistent fever
- Severe chest pain
19. Advanced Planning Checklist
- Travel when stable
- Plan with GP and respiratory clinic
- Carry documentation
- Monitor AQI
- Hydrate on flights
- Avoid damp & heavy dust
- Know red flags
With preparation, most people with stable aspergillosis travel safely and successfully.
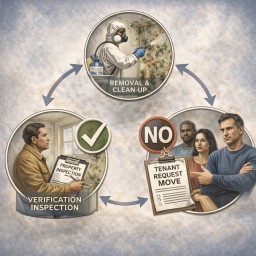
Remediation, verification, and refusal to move you
Home › Knowledge Hub › Damp, mould and aspergillosis › Remediation & refusal to move
If remediation is done but symptoms persist or worsen, the key question becomes: has the home been demonstrated to be safe to occupy?
What “good remediation” should include
- Cause fixed: leak/ingress/defect repaired, not just cleaned.
- Drying: adequate drying time and moisture checks.
- Material decisions: water-damaged porous materials removed where needed.
- Safe work: dust/spore spread controlled (important for medically vulnerable households).
- Verification: documented checks that work is complete and the home is safe.
Red flags (“bad remediation”)
- Paint over staining or “mould spray” only
- No drying plan, no moisture measurements
- No documentation of what was removed/replaced
- Work that creates dust without protection/containment
- Refusal to provide any meaningful post-remediation checks
If symptoms worsen after remediation
Worsening symptoms can occur if contaminated materials were disturbed or if damp persists behind walls/floors. This is a strong indicator that the hazard may not be resolved.
Actions:
- Document symptoms and healthcare visits (Page 3 template).
- Ask landlord for written evidence of safety and remediation details.
- Request escalation to Environmental Health if unresolved.
If the landlord refuses to move you (decant)
Use this framing:
- The issue is not “repairs completed” — it is safety and health risk.
- Ask: “What evidence shows the home is safe to occupy?”
Template request for temporary alternative accommodation
Subject: Request for temporary alternative accommodation (health risk / damp and mould) Hello [Name/Team], Despite remediation work, we are experiencing ongoing damp/mould concerns and worsening health symptoms in a clinically vulnerable household. Please provide written evidence that the home is safe to occupy, including: - confirmation the moisture source has been resolved, - evidence of drying/moisture checks, - what materials were removed/replaced, - what post-remediation checks were completed. Given the uncertainty around safety and the health impacts, we are requesting temporary alternative accommodation until the property can be demonstrated to be safe to occupy. Kind regards, [Name]
If you return “under protest”
If you have no alternative but to return, keep it in writing:
We are returning to the property due to lack of alternative accommodation. We do not accept that the damp/mould hazard has been resolved and will continue to document health impacts and seek independent assessment.
Trials, systematic reviews, and state-of-the-science reviews from ~2016–2026 on damp housing, mould, and health
Executive summary (what 10 years of evidence consistently shows)
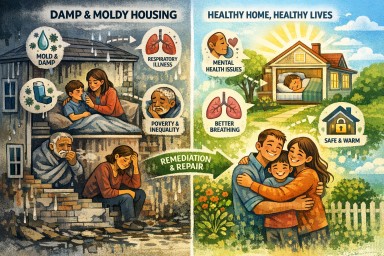
1) Damp and mouldy housing is a causal driver of respiratory disease
-
Strong, repeated associations with asthma incidence, asthma exacerbations, wheeze, chronic cough, and poorer lung function, especially in children.
-
Effects persist across countries, climates, and housing systems.
-
Evidence is strongest for asthma and allergic respiratory disease, but extends to bronchitis, infections, and symptom burden in people with existing lung disease.
2) Health effects are dose-related, not binary
-
Risk increases with extent, persistence, and visibility of dampness/mould (patch size, odour, condensation, repeated water damage).
-
No safe threshold has been identified → “any dampness matters.”
3) Mental health impacts are now well-established
-
Damp and mould exposure is associated with depression, anxiety, stress, sleep disturbance, and reduced wellbeing.
-
Pathways are both biological (inflammation, immune activation) and psychosocial (lack of control, stigma, housing insecurity).
4) Children are disproportionately affected
-
Strong paediatric evidence links damp homes to asthma development, poorer asthma control, and higher healthcare use.
-
Early-life exposure appears particularly important.
5) Damp housing is a marker of structural inequality
-
Concentrated in low-income, overcrowded, poorly maintained, or privately rented housing.
-
Acts as a health inequality amplifier, not just an environmental exposure.
6) Remediation works—but prevention works better
-
Interventions that fix the building (leaks, insulation, ventilation) improve symptoms.
-
Education alone is insufficient if the housing defect remains.
Thematic synthesis of the literature
1. Respiratory health (strongest evidence base)
Consistent findings across reviews (2016–2025):
-
Dampness and mould exposure increases:
-
Asthma onset in children
-
Asthma severity and exacerbations
-
Wheeze, cough, breathlessness
-
-
Associations hold even after adjusting for smoking, socioeconomic status, and outdoor pollution.
Key insight
Damp housing is not merely an “asthma trigger” — it is a risk factor for developing disease, especially in childhood.
2. Childhood lung health (very strong, clinically relevant)
-
Paediatric reviews emphasise that clinicians routinely see children whose symptoms are driven or sustained by housing conditions.
-
Poor housing undermines:
-
Controller medication effectiveness
-
Self-management plans
-
Long-term lung development
-
Clinical implication
Asking about housing conditions should be as routine as asking about pets or smoking in paediatric respiratory clinics.
3. Mental health and wellbeing (rapidly strengthening evidence)
Recent state-of-the-science reviews conclude:
-
Damp and mould exposure is associated with:
-
Depression
-
Anxiety
-
Psychological distress
-
-
Effects persist even when respiratory disease is accounted for.
Mechanisms proposed
-
Chronic inflammation and immune signalling
-
Sleep disruption
-
Loss of control and “housing stress”
-
Fear for children’s health
Important shift
Damp housing is no longer viewed as purely a respiratory issue—it is a whole-person health exposure.
4. Measurement and exposure assessment (important but imperfect)
What works reasonably well
-
Visual inspection and standard dampness indices
-
Structured questionnaires (especially for asthma cohorts)
-
ERMI (Environmental Relative Moldiness Index) as a research tool
What does NOT yet exist
-
A clinically agreed safe exposure threshold
-
A single test that rules exposure in or out
Consensus
Absence of a perfect test does not mean absence of harm.
5. Built environment, ventilation, and remediation
Clinical trials and housing intervention studies show:
-
Improved ventilation and moisture control:
-
Reduces indoor humidity
-
Improves reported physical and mental health
-
-
Poorly executed energy efficiency measures can worsen damp if ventilation is not addressed.
Critical point
“Warmth without ventilation” is a known failure mode.
6. Housing as a social determinant of health
Major public health frameworks now explicitly define healthy housing as:
-
Warm
-
Dry
-
Well-ventilated
-
Free from mould and toxins
-
Secure and accessible
Shift in framing
Damp housing is not an individual lifestyle issue—it is a system-level health determinant.
What the evidence does not support (important for countering misinformation)
-
No convincing evidence that:
-
“Detox” supplements treat mould exposure
-
Binding agents reverse health effects
-
Genetic susceptibility alone explains illness without exposure
-
-
Evidence strongly favours environmental remediation, not biomedical “workarounds”.
Implications for practice, policy, and patient support
For clinicians
-
Ask about damp and mould explicitly.
-
Document housing conditions when symptoms are unexplained or refractory.
-
Support patients with letters or reports—this is evidence-based advocacy, not speculation.
For public health & housing services
-
Damp housing remediation is preventive medicine.
-
Children’s respiratory health and mental health outcomes justify investment.
For patients
-
Symptoms are not imagined.
-
The problem is the building, not personal failure.
-
Improvement often requires structural change, not just treatment escalation.
Bottom line (10-year consensus)
Damp and mouldy housing causes avoidable disease, worsens inequality, and undermines medical care.
Fixing homes is one of the most effective—and underused—public health interventions available.
References
-
Bentley R, Mason K, Jacobs D, Blakely T, Howden-Chapman P, Li A, Adamkiewicz G, Reeves A.
Housing as a social determinant of health: a contemporary framework. Lancet Public Health. 2025;10(10):e855–e864. doi:10.1016/S2468-2667(25)00142-2. PMID: 40953578. -
Moorcroft C, Whitehouse A, Grigg J.
Damp and mouldy home: impact on lung health in childhood. Archives of Disease in Childhood. 2025;110(6):419–421. doi:10.1136/archdischild-2023-326035. PMID: 39814530. -
Gatto MR, Mansour A, Li A, Bentley R.
A state-of-the-science review of the effect of damp- and mold-affected housing on mental health. Environmental Health Perspectives. 2024;132(8):086001. doi:10.1289/EHP14341. PMID: 39162373. -
Patti MA, Henderson NB, Phipatanakul W, Jackson-Browne M.
Recommendations for clinicians to combat environmental disparities in pediatric asthma. Chest. 2024;166(6):1309–1318. doi:10.1016/j.chest.2024.07.143. PMID: 39059578. -
Punyadasa D, Adderley NJ, Rudge G, Nagakumar P, Haroon S.
Self-reported questionnaires to assess indoor home environmental exposures in asthma patients: a scoping review. BMC Public Health. 2024;24:2915. doi:10.1186/s12889-024-20418-8. PMID: 39434085. -
Kozajda A, Miśkiewicz E.
Exposure to bioaerosol in the residential environment. Medycyna Pracy. 2024;75(6):545–560. doi:10.13075/mp.5893.01508. PMID: 39688367. -
Vesper SJ.
The development and application of the Environmental Relative Moldiness Index (ERMI). Critical Reviews in Microbiology. 2025;51(2):285–295. doi:10.1080/1040841X.2024.2344112. PMID: 38651788. -
Nabaweesi R, Hanna M, Muthuka JK, Samuels AD, Brown V, Schwartz D, Ekadi G.
The built environment as a social determinant of health. Primary Care. 2023;50(4):591–599. doi:10.1016/j.pop.2023.04.012. PMID: 37866833. -
Grant TL, Wood RA.
The influence of urban exposures and residence on childhood asthma. Pediatric Allergy and Immunology. 2022;33(5):e13784. doi:10.1111/pai.13784. PMID: 35616896. -
Coulburn L, Miller W.
Prevalence, risk factors and impacts related to mould-affected housing: an Australian integrative review. International Journal of Environmental Research and Public Health. 2022;19(3):1854. doi:10.3390/ijerph19031854. PMID: 35162876. -
Wimalasena NN, Chang-Richards A, Wang KI, Dirks KN.
Housing risk factors associated with respiratory disease: a systematic review. International Journal of Environmental Research and Public Health. 2021;18(6):2815. doi:10.3390/ijerph18062815. PMID: 33802036. -
Ali SH, Foster T, Hall NL.
The relationship between infectious diseases and housing maintenance in Indigenous Australian households. International Journal of Environmental Research and Public Health. 2018;15(12):2827. doi:10.3390/ijerph15122827. PMID: 30545014. -
Wolkoff P.
Indoor air humidity, air quality, and health – an overview. International Journal of Hygiene and Environmental Health. 2018;221(3):376–390. doi:10.1016/j.ijheh.2018.01.015. PMID: 29398406. -
Mendell MJ, Kumagai K.
Observation-based metrics for residential dampness and mold with dose–response relationships to health: a review. Indoor Air. 2017;27(3):506–517. doi:10.1111/ina.12342. PMID: 27663473. -
Francisco PW, Jacobs DE, Targos L, Dixon SL, Breysse J, Rose W, Cali S.
Ventilation, indoor air quality, and health in homes undergoing weatherization: a randomized trial. Indoor Air. 2017;27(2):463–477. doi:10.1111/ina.12325. PMID: 27490066. -
Barnes CS, Horner WE, Kennedy K, Grimes C, Miller JD.
Home assessment and remediation. Journal of Allergy and Clinical Immunology: In Practice. 2016;4(3):423–431.e15. doi:10.1016/j.jaip.2016.01.006. PMID: 27157934. -
Chew GL, Horner WE, Kennedy K, Grimes C, Barnes CS, Phipatanakul W, Larenas-Linnemann D, Miller JD.
Procedures to assist health care providers to determine when home assessments for potential mold exposure are warranted. Journal of Allergy and Clinical Immunology: In Practice. 2016;4(3):417–422.e2. doi:10.1016/j.jaip.2016.01.013. PMID: 27021632. -
Vesper S, Wymer L.
The relationship between Environmental Relative Moldiness Index values and asthma. International Journal of Hygiene and Environmental Health. 2016;219(3):233–238. doi:10.1016/j.ijheh.2016.01.006. PMID: 26861576.
How to Ask Fewer, Better Questions in Appointments
Focusing on what matters most to you—without feeling you’re wasting time
Many patients and carers worry about “asking too much” in clinic. Appointments are short, clinicians are busy, and you may already have a long list of questions in your head. The aim isn’t to stop asking questions—it’s to ask the right ones, at the right time, in the right way.
Here are practical strategies that help you stay focused, feel heard, and make the most of limited time.
1. Decide your Top 3 priorities before you go
Before the appointment, write down everything you’re thinking about. Then circle just three things that matter most right now.
Good priorities are usually:
-
A symptom that is new, worsening, or frightening
-
A treatment issue that affects daily life (side-effects, adherence, cost, function)
-
A decision you need to make soon
If it doesn’t change what happens in the next few weeks, it may not need airtime today.
If you remember only one thing: appointments are for decisions, not encyclopaedias.
2. Separate “need to know” from “nice to know”
It’s easy to mix curiosity with urgency.
Need to know (ask now):
-
Is this symptom important?
-
Is this treatment still right for me?
-
What should I do if X happens?
-
Are we monitoring the right things?
Nice to know (park for later):
-
Mechanisms, pathways, emerging research
-
Rare side-effects without symptoms
-
“What if” scenarios far in the future
Keep a “parking list” for later reading or discussion.
3. Frame questions around impact, not theory
Clinicians work best when questions are grounded in real life.
Instead of:
-
“I read a paper saying X might affect Y…”
Try:
-
“I’m noticing X in daily life—does that change what we do?”
-
“Is this symptom something you’d want to investigate?”
This signals relevance and helps clinicians triage quickly.
4. Ask one question at a time
Long, multi-part questions feel overwhelming and are easy to partially answer.
Break them down:
-
First: Is this important?
-
Then (if yes): What do we do about it?
-
Then (if needed): What should I watch for?
You’ll often find later questions become unnecessary once the first is answered.
5. Use the “Is this something we should…” test
This single phrase keeps questions concise and respectful of time:
-
“Is this something we should investigate?”
-
“Is this something that changes treatment?”
-
“Is this something I should worry about?”
A clear yes/no (or not yet) is often all you need.
6. Accept that not everything fits in one appointment
It’s okay—and normal—to say:
-
“I know we may not have time today—what should I prioritise?”
-
“Which of these matters most from your point of view?”
This shows partnership, not passivity.
If something needs more time, ask how best to handle it:
-
Another appointment
-
A nurse specialist
-
Written advice
-
Monitoring and review later
7. Bring written notes (but don’t read them all out)
A short list helps you stay focused under pressure.
Tip:
-
Highlight your top 3
-
Tick them off as they’re addressed
-
If time runs out, you still covered what mattered most
8. For carers: ask on behalf, not over
Carers often worry about dominating the conversation.
Helpful approaches:
-
Ask the patient first: “What do you most want answered today?”
-
Step in only if something important is being missed
-
Offer to follow up questions outside the appointment if possible
9. Reassure yourself: clinicians don’t expect perfection
You are not expected to:
-
Understand everything
-
Ask the “right” questions every time
-
Cover your entire condition in one visit
Good clinicians prefer:
a focused conversation
over
a rushed, overloaded one
10. A simple closing question that saves time
If time is tight, end with:
-
“Is there anything you think I should have asked but didn’t?”
This often surfaces the most important point of all.
The takeaway
You are not wasting time by asking questions—you’re wasting time by asking too many unfocused ones.
Clarity, prioritisation, and relevance help everyone:
-
You leave with answers that matter
-
Clinicians can make better decisions
-
Anxiety is reduced, not fuelled
Does when I eat cause fat gain if I have adrenal insufficiency?
Many people with adrenal insufficiency worry that eating at the “wrong time” — especially later in the day — will automatically cause weight gain or “steroid belly”.
This is understandable, but it’s important to separate myths from what actually happens in the body.
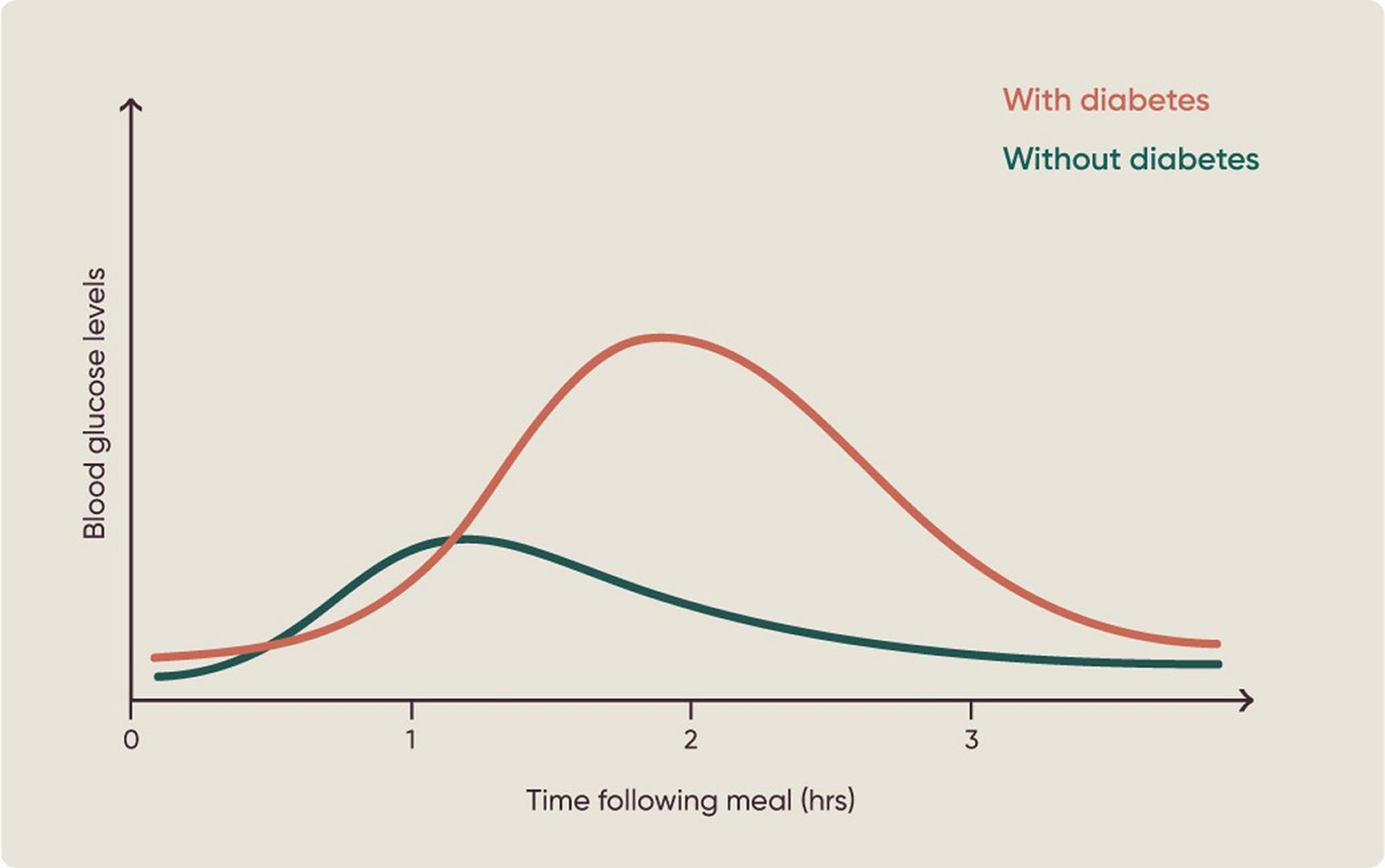

What doctors mean by “glucose response”
When clinicians or researchers talk about glucose response, they mean:
How your blood sugar rises and falls after eating
It does not mean that sugar is instantly being turned into fat.
A rise in blood glucose after eating is normal and happens in everyone.
Does eating later in the day automatically turn food into fat?
No.
Fat gain does not happen because of a single meal or snack — or because you ate at a particular time.
In most people:
-
Carbohydrates are first used for energy
-
Extra glucose is stored as glycogen in muscles and liver
-
Only repeated excess intake over time contributes to fat gain
Eating in the evening does not automatically cause fat storage.
Where insulin fits in (without the fear)
Eating raises blood glucose, which triggers insulin.
Insulin:
-
Helps move glucose into cells
-
Replenishes energy stores
-
Temporarily pauses fat burning
This pause is normal and reversible.
Insulin does not automatically create body fat.
Fat gain happens when:
-
Total calorie intake is consistently higher than needs
-
Steroid replacement is higher than required
-
This pattern continues over weeks or months
Why people with adrenal insufficiency feel confused about this
With adrenal insufficiency:
-
Cortisol replacement is taken in doses, not continuously
-
Symptoms, stress, poor sleep, or illness can affect appetite and energy
-
Some people are prone to low blood sugar, especially later in the day
Because of this:
-
Rigid food timing rules can make symptoms worse
-
Skipping meals or avoiding evening snacks can increase fatigue, dizziness, or night-time symptoms
A safer way to think about meal timing
Instead of strict rules, think in patterns:
-
Some people feel best with:
-
Larger meals earlier in the day
-
Lighter evenings
-
-
Others need:
-
A small evening snack
-
Protein or fat to keep blood sugar stable overnight
-
Both can be correct.
What matters most is:
-
How you feel
-
Whether your energy is stable
-
Whether sleep and symptoms improve
What usually matters more than timing
For people with adrenal insufficiency, weight changes are most often related to:
-
Total daily steroid dose
-
Repeated or prolonged stress dosing
-
Reduced activity due to illness or fatigue
-
Menopause, ageing, or other medical conditions
Food timing plays a much smaller role.
Key reassurance
If a food timing rule makes you feel worse, it is not the right rule for you.
-
A single glucose rise does not cause fat gain
-
Eating later does not automatically lead to weight gain
-
Safety, symptom control, and adequate steroid replacement come first
Please remember
Never change steroid dose or meal patterns intended to prevent hypoglycaemia without medical advice.
Underdosing steroids is far more dangerous than eating at the “wrong” time.
Take-home message
Focus on stability, nourishment, and feeling well — not fear of timing.
Hydrocortisone dosing in adrenal insufficiency
Why adrenal insufficiency can happen in people with aspergillosis
Many people with aspergillosis, particularly those with asthma-related conditions such as allergic bronchopulmonary aspergillosis (ABPA) or more severe chronic lung disease, need treatment with steroid medicines at some point. These treatments — often essential to control inflammation, protect the lungs, and improve breathing — may include repeated or long-term courses of steroids such as prednisolone.
When steroid treatment is used over time, it can reduce the body’s own production of cortisol by the adrenal glands. In some people, the adrenal glands do not fully recover, leading to adrenal insufficiency. Cortisol is a vital hormone that helps the body manage energy, illness, infection, and physical stress. When it cannot be made reliably, hydrocortisone replacement is needed to keep the body safe and functioning.
In this situation, hydrocortisone is prescribed to replace the cortisol your body can no longer make, usually after prednisolone has been reduced or stopped, or when prednisolone is no longer needed to control lung inflammation but adrenal support is still required.
Adrenal insufficiency in people with aspergillosis is not a failure and not something you have caused. It is a recognised consequence of necessary treatment for a serious, long-term condition. With the right information, a personalised dosing plan, and medical support, adrenal insufficiency can be managed safely alongside aspergillosis.
A patient guide to everyday (basal) dosing, higher-dose needs, and short-term stress dosing
If you take hydrocortisone because you have adrenal insufficiency, understanding how your dose works — both day to day and during illness or stress — is essential for your safety and wellbeing.
This guide explains:
-
What your basal (everyday) dose is for
-
Why some people need higher basal doses
-
When and how stress dosing is used — and why it is short term
-
Why some doctors may hesitate — and how to work safely with them
-
Where to find trusted patient and clinician resources
Very important first point ❗
Any changes to your hydrocortisone dose must be agreed in advance with a doctor or specialist nurse who knows your adrenal insufficiency.
This includes:
-
Your usual daily dose
-
Your stress-dosing (“sick day”) plan
-
Emergency injection instructions
This guide does not replace medical advice.
It is designed to help you understand your treatment and communicate clearly with healthcare professionals.
1) Your basal (everyday) hydrocortisone dose
What the basal dose is for
Your basal dose is the hydrocortisone you take on an ordinary day, when you are not ill or under unusual stress. Its purpose is to:
-
Replace the cortisol your body cannot make reliably
-
Support normal daily function (energy, blood pressure, mood)
-
Help your body feel stable and safe
-
Reduce the risk of chronic under-replacement
It is replacement, not treatment for inflammation.
A key point many patients are not told
Being consistently under-replaced does not help adrenal recovery.
Ongoing symptoms such as:
-
Constant exhaustion
-
Dizziness or nausea on standing
-
Brain fog or low mood
-
Poor tolerance of everyday stress
-
Frequent “crashes” or infections
can delay recovery, not speed it. Stability supports healing.
What doctors usually mean by a “physiological” dose
Most adults naturally produce the equivalent of about 15–25 mg of hydrocortisone per day.
Doctors aim for a dose in this range and adjust for:
-
Body size
-
Activity level
-
Other medical conditions
-
Individual response
This is replacement, not “high-dose steroids”.
How basal hydrocortisone is usually taken
To mimic the body’s natural rhythm, doses are often split:
-
A larger dose in the morning
-
Smaller doses later in the day
-
Avoiding late evening doses where possible
This supports:
-
Energy and blood pressure
-
Sleep
-
Mood and concentration
Signs your basal dose may be too low
Tell your doctor if you have persistent:
-
Severe fatigue despite rest
-
“Wired but empty” feeling
-
Dizziness, nausea, or salt craving
-
Poor concentration or memory
-
Low mood or anxiety
-
Frequent need for rescue or stress doses
These symptoms matter even if blood tests look reassuring.
Blood tests are only part of the picture
Cortisol and ACTH tests:
-
Help with diagnosis
-
Are less helpful for adjusting daily dose
-
Do not always reflect how well you function
Doctors experienced with adrenal insufficiency rely heavily on how you feel and cope day to day.
The right balance
Rather than “as low as possible,” a safer aim is:
Low enough to avoid overtreatment, but high enough to live a stable, functional life.
Living in constant deficit is not success.
2) When a higher basal dose may be appropriate
Some people with adrenal insufficiency — particularly those with chronic illness — may genuinely need a higher basal hydrocortisone dose (for example 25–30 mg/day).
This does not automatically mean overtreatment.
Well-recognised examples include:
Chronic inflammatory lung disease (including ABPA)
-
Ongoing airway inflammation and immune activation
-
Recurrent infective or inflammatory flares
-
The body may never be in a true “resting” state
-
Standard doses may leave patients under-replaced
-
A stable higher dose can reduce repeated stress dosing and improve daily function
Frequent infections or slow recovery
-
Repeated illness or prolonged recovery
-
Frequent “temporary” stress dosing just to cope with everyday life
Long-standing steroid-induced adrenal insufficiency
-
Years of prednisolone or similar treatment
-
Deep suppression of the adrenal system
Larger body size or higher metabolic demand
-
Cortisol needs vary with body size and activity
Autonomic symptoms or low blood pressure
-
Postural dizziness or faintness
-
Often benefit from a higher morning dose
Clinical clue:
If someone repeatedly needs stress dosing just to manage ordinary days, their basal dose may be too low for their current physiology.
Important reassurance
-
Higher basal doses can be appropriate, temporary, or longer-term
-
They do not automatically prevent recovery
-
Ongoing inflammation and repeated physiological stress suppress recovery more than adequate replacement
-
Doses should always be prescribed, documented, and reviewed
3) Stress dosing — when your body temporarily needs more
What stress dosing means
A healthy body automatically makes more cortisol during:
-
Illness or infection
-
Fever
-
Vomiting or diarrhoea
-
Injury or trauma
-
Severe pain
-
Surgery or medical procedures
-
Major physical stress
If you have adrenal insufficiency:
➡️ your body cannot do this, so doctors prescribe stress dosing in advance as part of your safety plan.
Stress dosing is essential — but it is short term
Stress dosing is meant to last only as long as the stress lasts.
It covers a temporary increase in need, not your everyday requirements.
What “short term” usually means
Stress dosing may last:
-
24–48 hours for minor illness or fever
-
Several days for infections or recovery from injury
-
During and immediately after surgery or procedures
Your doctor should advise:
-
When to increase
-
How much to increase
-
When and how to return to your usual dose
Why stress dosing should not continue indefinitely
If higher doses are needed for longer, something usually needs review:
-
Infection or inflammation has not settled
-
The basal dose may be too low
-
Another medical problem is present
If stress dosing is still needed after the original stress has passed, it’s time to talk to your doctor.
Stepping back down safely
-
Doctors usually advise returning to baseline
-
Sometimes a 1–2 day step-down is used
-
You should not remain on stress doses “just in case”
Stress dosing does NOT:
-
Stop adrenal recovery
-
Mean you are “failing”
-
Cause long-term harm when used correctly
Not stress dosing can:
-
Make you seriously unwell
-
Delay recovery
-
Lead to adrenal crisis


4) Why some doctors seem hesitant
Doctors outside endocrinology (GPs, A&E, ward teams):
-
Are trained to minimise steroid use
-
Often think of steroids only as anti-inflammatory drugs
-
May rarely manage adrenal insufficiency
What they may not realise immediately:
Your hydrocortisone is replacing a missing hormone — it is essential, not extra.
5) How to advocate safely (with medical backing)
It is appropriate to say:
“I have adrenal insufficiency. My doctor has advised stress dosing during illness to prevent adrenal crisis.”
If you have them, show:
-
Your Steroid Emergency Card
-
A written stress-dosing plan
-
A clinic letter or summary
6) Trusted resources & further support (with links)
The following organisations provide reliable, clinician-endorsed information on adrenal insufficiency, hydrocortisone replacement, stress dosing, and emergency care.
They are widely recognised by NHS endocrinology teams and safe to share with patients, families, and healthcare professionals.
UK patient and professional resources
Addison’s Disease Self-Help Group (ADSHG)
Website: https://www.addisonsdisease.org.uk
What it offers:
-
Clear explanations of basal vs stress dosing
-
Patient-friendly sick-day rules
-
Emergency hydrocortisone injection guidance
-
Downloadable patient leaflets used in NHS clinics
-
Webinars, helpline, and peer support
Why it’s useful:
ADSHG explicitly supports individualised dosing and crisis prevention.
Society for Endocrinology
Steroid Emergency Card & adrenal crisis guidance:
https://www.endocrinology.org/clinical-practice/steroid-emergency-card/
Why it’s useful:
-
Highly trusted by doctors, A&E, and ward teams
-
Clear professional wording that reassures non-specialists
-
Supports rapid decision-making in emergencies
NHS (England)
Steroid Emergency Card information:
https://www.nhs.uk/conditions/steroid-emergency-card/
Why it’s useful:
-
Official NHS backing
-
Useful for legitimacy in emergency or inpatient settings
International patient resources (useful supplements)
Endocrine Society
Patient information on adrenal insufficiency:
https://www.endocrine.org/patient-engagement/endocrine-library/adrenal-insufficiency
Why it’s useful:
-
Clear explanations of cortisol physiology
-
Conservative, authoritative tone
-
Helpful for patients seeking international consensus
National Adrenal Diseases Foundation (NADF)
Website: https://www.nadf.us
What it offers:
-
Practical sick-day rules
-
Emergency preparedness guidance
-
Injection training resources
Particularly helpful for patients with long-standing adrenal insufficiency or frequent illness.
Resources especially relevant for ABPA & chronic lung disease
National Aspergillosis Centre
Website: https://mft.nhs.uk/wythenshawe/services/infectious-diseases/national-aspergillosis-centre/
Why it’s relevant:
-
Specialist centre where ABPA and adrenal insufficiency often overlap
-
Supports personalised care plans in complex disease
Aspergillosis Trust
Website: https://www.aspergillosistrust.org
Why it’s useful:
-
Patient-focused education and advocacy
-
Helps explain the chronic physiological stress of ABPA
-
Supports conversations about higher basal hydrocortisone needs
Quick-access patient checklist (phone / wallet)
Patients are encouraged to keep:
-
Steroid Emergency Card
-
Sick-day rules (ADSHG)
-
Personal stress-dosing plan (agreed with doctor)
-
Clinic letter or summary
Many patients keep photos of these documents on their phone for emergencies.
Final reassurance
These resources support — not replace — medical advice.
They exist to help patients stay safe, informed, and confident when managing hydrocortisone and communicating with healthcare professionals.
**Pain Perception and Aspergillosis:
Why It Matters — and What Help Is Available**
Living with aspergillosis—whether Chronic Pulmonary Aspergillosis (CPA), Allergic Bronchopulmonary Aspergillosis (ABPA), Aspergillus bronchitis, or Severe Asthma with Fungal Sensitivity (SAFS)—can mean coping with symptoms that change day to day.
Pain, breathlessness, muscle aches, fatigue and joint discomfort are common. What many people don’t realise is that how the body perceives and processes pain plays a major role in how these symptoms feel — and how well they can be managed.
Understanding pain perception doesn’t mean your symptoms aren’t real. It means understanding why pain behaves the way it does in chronic illness — and how to gain more control.
1. Why pain perception matters in aspergillosis
Pain is produced by the nervous system, and is influenced by:
-
Inflammation in the lungs or sinuses
-
Muscle strain from coughing or altered breathing
-
Reduced fitness after flare-ups
-
Long-term corticosteroid use
-
Adrenal insufficiency
-
Stress, uncertainty, poor sleep, and emotional load
Pain is therefore a mix of bodily changes and how the brain interprets signals.
Both are real. Both deserve attention.
2. Muscle changes and increased sensitivity
People with aspergillosis may experience:
-
Weakened rib, back, and shoulder muscles
-
Reduced leg strength
-
Joint instability
-
Muscle fatigue leading to higher pain sensitivity
Everyday movements can feel more painful, and pain can worsen breathlessness. Many people fall into a cycle: flare-up → rest → muscle weakening → more pain → more breathlessness → more rest.
Understanding this cycle helps break it.
3. Stress, sleep and emotions influence pain
Pain becomes stronger when:
-
You are tired
-
You feel anxious, unsafe, or overwhelmed
-
Your symptoms are unpredictable
-
You have recently been in hospital
-
You are caring for someone who is unwell
This does not mean pain is psychological.
It means the nervous system becomes more alert, so signals feel louder.
Carers experience this too.
4. Why understanding pain helps you manage symptoms
Learning about pain perception helps you:
-
Pace activity wisely
-
Avoid panic when symptoms spike
-
Identify muscular vs inflammatory discomfort
-
Communicate clearly with clinicians
-
Reduce stress-driven symptom amplification
-
Prevent flare-ups by calming the nervous system
It’s not about ignoring symptoms — it’s about understanding them so you can respond safely and confidently.
5. NHS resources that can help
Below are useful links recommended across NHS pain services.
🔹 NHS self-help guidance on long-term pain
These pages offer practical advice on managing persistent pain, pacing, movement, and everyday strategies:
How to get NHS help for your pain
https://www.nhs.uk/live-well/pain/how-to-get-nhs-help-for-your-pain/
10 ways to reduce pain
https://www.nhs.uk/live-well/pain/10-ways-to-ease-pain/
These guides are suitable for people with chest pain, muscular pain, fatigue and inflammation linked to lung disease.
🔹 NHS Pain Management Programmes (PMP)
Many NHS Trusts run Pain Management Programmes. These provide a combination of physiotherapy, psychology, pacing education, flare-up planning, and medication review.
Examples of NHS PMP resources:
Royal Orthopaedic Hospital – PMP information
https://roh.nhs.uk/services-information/pain-management/pain-management-programme
Ashford & St Peter’s Hospitals – Pain Management Programme
https://www.ashfordstpeters.nhs.uk/the-pain-management-programme
Gloucestershire Hospitals – Pain Management Options
https://www.gloshospitals.nhs.uk/our-services/services-we-offer/pain-management-service/management-options-pain/
Speak to your GP or specialist team if you want a referral.
🔹 The Pain Toolkit (NHS-endorsed self-management booklet)
Widely used by NHS pain services and physiotherapy teams.
PDF:
https://www.nhsfife.org/media/c349s6xo/nhs-fife-pain-toolkit.pdf
This guide covers pacing, flare-up planning, problem-solving, emotional wellbeing and shared decision-making.
🔹 NHS Talking Therapies (for stress-related pain amplification)
If stress, anxiety or sleep disturbance are worsening your pain, NHS Talking Therapies services can help.
Find your local service here:
https://www.nhs.uk/service-search/mental-health/find-a-psychological-therapies-service/
These services support people with long-term physical conditions as well as mood and anxiety problems.
🔹 Physiotherapy & pulmonary rehabilitation
These services help with:
-
Breathing pattern retraining
-
Strengthening ribs, shoulders, back, hips, and knees
-
Improving stamina and reducing breathlessness
-
Reducing muscle pain and improving posture
Ask your GP, respiratory consultant, or specialist nurse for a referral.
6. What patients and carers can start today
✔ Notice pain patterns
Track fatigue, sleep, activity, stress, and symptoms.
✔ Practice pacing
Spread tasks through the day. Avoid pushing hard on “good days” — it often leads to flare-ups.
✔ Gentle strengthening
Even small daily exercises protect joints, support breathing and lower pain sensitivity.
✔ Reduce nervous-system overload
Breathing exercises, grounding, relaxation and mindfulness calm the system that amplifies pain.
✔ Seek help early
If pain changes or worries you, involve your GP or specialist team.
✔ Carers: protect your wellbeing
Carers benefit from pacing, strengthening and psychological support just as much as patients.
7. When to seek medical review
Contact your GP or specialist team urgently if you experience:
-
Sudden new chest pain
-
Pain with fever or coughing up blood
-
Pain that stops you breathing normally
-
Severe muscle weakness
-
Persistent flare-ups despite treatment
-
Symptoms suggesting adrenal problems
Pain in aspergillosis is real, but also manageable. With the right understanding and NHS-supported tools, you can reduce flare-ups, regain confidence, and improve daily life.