When ‘chest infections’ don’t respond: when to suspect ABPA or CPA (Clinical perspective)
Patients presenting with recurrent “chest infections” that do not respond to antibiotics are common in primary and secondary care. In a subset of these cases, the underlying cause may not be bacterial, but related to fungal disease or immune-mediated responses to Aspergillus.
This article summarises when to suspect allergic bronchopulmonary aspergillosis (ABPA) or chronic pulmonary aspergillosis (CPA), and how to move from repeated empirical treatment to a more structured diagnostic approach.
Key clinical message
Repeated antibiotic-treated exacerbations with limited response, particularly when symptoms improve with steroids and then relapse, should prompt reconsideration of the diagnosis.
When to suspect ABPA or CPA
Consider aspergillosis-related disease in patients with:
- Recurrent “chest infections” with poor or inconsistent antibiotic response
- Steroid-responsive symptoms with relapse on reduction or cessation
- Persistent or unexplained radiological abnormalities
- Underlying lung disease:
- Asthma
- Bronchiectasis
- Chronic obstructive pulmonary disease (COPD)
- Previous tuberculosis or lung damage
- Raised or previously documented abnormalities in:
- Total IgE
- Eosinophils
- Aspergillus-specific markers (if previously tested)
These features are not diagnostic in isolation but should raise suspicion when seen together.
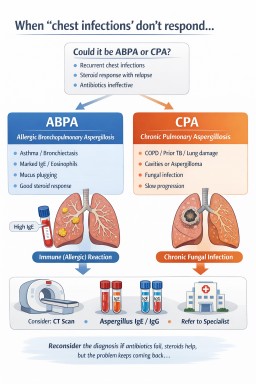
ABPA vs CPA: clinical distinction
| Feature | ABPA | CPA |
|---|---|---|
| Primary mechanism | Immune-mediated (allergic) | Chronic fungal infection |
| Typical background | Asthma, bronchiectasis | Structural lung disease, prior TB, COPD |
| Steroid response | Often marked | Variable (may improve symptoms but not disease) |
| Antibiotic response | Limited | Limited |
| Radiology | Mucus plugging, bronchiectasis | Cavities, fungal balls, fibrosis |
Common pitfalls in practice
- Repeated empirical antibiotics despite poor response
- Short courses of steroids without a long-term management plan
- Reliance on chest X-ray alone in persistent or atypical cases
- Failure to recognise patterns across multiple consultations or admissions
These patterns can lead to prolonged diagnostic delay, which is well described in CPA and ABPA.
Suggested diagnostic approach
1. Reassess the working diagnosis
When standard treatment fails, explicitly reconsider whether the presentation remains consistent with bacterial infection.
2. Imaging
- Escalate from chest X-ray to CT thorax where appropriate
- Look for:
- Cavitation
- Fungal ball (aspergilloma)
- Mucus plugging
- Bronchiectasis
3. Blood tests
- Total IgE
- Eosinophil count
- Aspergillus-specific IgE and IgG (where available)
4. Microbiology / further testing
Depending on context, consider sputum culture, fungal markers, or specialist input.
The steroid–relapse pattern
A common clinical scenario:
Exacerbation → steroids → improvement → relapse
This should raise suspicion of an underlying inflammatory or fungal-driven process rather than recurrent bacterial infection alone.
When to consider referral
Referral to a specialist centre (e.g. National Aspergillosis Centre, Manchester) may be appropriate where:
- Diagnosis remains uncertain
- Symptoms are persistent or progressive despite treatment
- Antifungal therapy is being considered or not tolerated
- Radiology suggests CPA or complex disease
Referral decisions should be made in the context of overall patient condition, comorbidities, and goals of care.
Why diagnosis is often delayed
- Overlap with common respiratory conditions
- Partial response to standard therapies
- Fragmentation across care settings
- Limited exposure to aspergillosis in routine practice
Recognising the pattern is often the key step in reducing delay.
Practical takeaways
- If antibiotics are not working, reconsider the diagnosis
- If steroids repeatedly improve symptoms, ask why
- Use CT imaging to clarify persistent abnormalities
- Aim for a clear, shared management plan
Guidelines and further reading
- British Thoracic Society. Clinical Statement on Aspergillus-related chronic lung disease
- ISHAM Working Group. Guidelines for ABPA diagnosis and management
- Denning DW et al. Chronic pulmonary aspergillosis guidelines
Further professional resources
Aspergillosis.org – Information for healthcare professionals
This article is intended for educational purposes and should be interpreted in the context of individual clinical judgement.
When ‘chest infections’ don’t respond: when to suspect ABPA or CPA (Patient guide)
Patients presenting with recurrent “chest infections” that do not respond to antibiotics are common in primary and secondary care. In a subset of these cases, the underlying cause may not be bacterial, but related to fungal disease or immune-mediated responses to Aspergillus.
This article summarises when to suspect allergic bronchopulmonary aspergillosis (ABPA) or chronic pulmonary aspergillosis (CPA), and how to move from repeated empirical treatment to a more structured diagnostic approach.
Key clinical message
Repeated antibiotic-treated exacerbations with limited response, particularly when symptoms improve with steroids and then relapse, should prompt reconsideration of the diagnosis.
When to suspect ABPA or CPA
Consider aspergillosis-related disease in patients with:
- Recurrent “chest infections” with poor or inconsistent antibiotic response
- Steroid-responsive symptoms with relapse on reduction or cessation
- Persistent or unexplained radiological abnormalities
- Underlying lung disease:
- Asthma
- Bronchiectasis
- Chronic obstructive pulmonary disease (COPD)
- Previous tuberculosis or lung damage
- Raised or previously documented abnormalities in:
- Total IgE
- Eosinophils
- Aspergillus-specific markers (if previously tested)
These features are not diagnostic in isolation but should raise suspicion when seen together.
ABPA vs CPA: clinical distinction
| Feature | ABPA | CPA |
|---|---|---|
| Primary mechanism | Immune-mediated (allergic) | Chronic fungal infection |
| Typical background | Asthma, bronchiectasis | Structural lung disease, prior TB, COPD |
| Steroid response | Often marked | Variable (may improve symptoms but not disease) |
| Antibiotic response | Limited | Limited |
| Radiology | Mucus plugging, bronchiectasis | Cavities, fungal balls, fibrosis |
Common pitfalls in practice
- Repeated empirical antibiotics despite poor response
- Short courses of steroids without a long-term management plan
- Reliance on chest X-ray alone in persistent or atypical cases
- Failure to recognise patterns across multiple consultations or admissions
These patterns can lead to prolonged diagnostic delay, which is well described in CPA and ABPA.
Suggested diagnostic approach
1. Reassess the working diagnosis
When standard treatment fails, explicitly reconsider whether the presentation remains consistent with bacterial infection.
2. Imaging
- Escalate from chest X-ray to CT thorax where appropriate
- Look for:
- Cavitation
- Fungal ball (aspergilloma)
- Mucus plugging
- Bronchiectasis
3. Blood tests
- Total IgE
- Eosinophil count
- Aspergillus-specific IgE and IgG (where available)
4. Microbiology / further testing
Depending on context, consider sputum culture, fungal markers, or specialist input.
The steroid–relapse pattern
A common clinical scenario:
Exacerbation → steroids → improvement → relapse
This should raise suspicion of an underlying inflammatory or fungal-driven process rather than recurrent bacterial infection alone.
When to consider referral
Referral to a specialist centre (e.g. National Aspergillosis Centre, Manchester) may be appropriate where:
- Diagnosis remains uncertain
- Symptoms are persistent or progressive despite treatment
- Antifungal therapy is being considered or not tolerated
- Radiology suggests CPA or complex disease
Referral decisions should be made in the context of overall patient condition, comorbidities, and goals of care.
Why diagnosis is often delayed
- Overlap with common respiratory conditions
- Partial response to standard therapies
- Fragmentation across care settings
- Limited exposure to aspergillosis in routine practice
Recognising the pattern is often the key step in reducing delay.
Practical takeaways
- If antibiotics are not working, reconsider the diagnosis
- If steroids repeatedly improve symptoms, ask why
- Use CT imaging to clarify persistent abnormalities
- Aim for a clear, shared management plan
Guidelines and further reading
Which guideline should I use?
In UK practice, the British Thoracic Society (BTS) statement provides the most directly applicable clinical guidance. The ISHAM guidelines offer detailed international consensus, particularly for ABPA. Both are complementary and widely used.
- British Thoracic Society (BTS)
Clinical Statement on Aspergillus-related chronic pulmonary disease
UK guidance covering diagnosis and management of ABPA, CPA, and related conditions.
View BTS clinical statement
- International Society for Human and Animal Mycology (ISHAM)
Revised clinical practice guidelines for allergic bronchopulmonary aspergillosis/mycoses
International consensus guidance on diagnosis, classification, and management of ABPA.
View ISHAM guideline (European Respiratory Journal)
- Chronic Pulmonary Aspergillosis (CPA) guidelines
Denning DW et al. Chronic pulmonary aspergillosis: rationale and clinical guidelines for diagnosis and management
View PubMed record
Further professional resources
For clinician-focused guidance, referral pathways, and educational material:
https://aspergillosis.org/information-for-professionals/
This article is intended for educational purposes and should be interpreted in the context of individual clinical judgement.