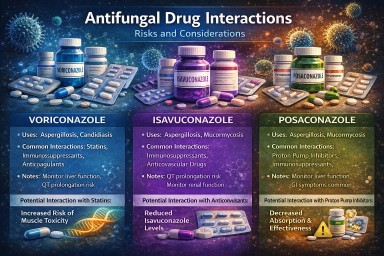
Why Antifungal Drug Interactions Matter — and How AntifungalInteractions.org Can Help

Key points
- Antifungal medicines used in aspergillosis can interact with many common medicines and supplements.
- Some interactions are mild, while others can significantly affect drug levels or side effects.
- Interactions may involve steroids, inhalers, antibiotics, heart medicines, acid suppressants and herbal supplements.
- Patients should always tell healthcare teams about all medicines, vitamins and supplements they take.
- AntifungalInteractions.org is a specialist resource designed to help healthcare professionals and patients understand potential antifungal interactions.
Why do antifungal interactions matter so much?
The antifungal medicines used to treat aspergillosis are powerful and highly specialised drugs. They are extremely important in controlling fungal disease, but many also affect the way the body processes other medicines.
This is particularly true for azole antifungals such as:
- itraconazole,
- voriconazole,
- posaconazole,
- isavuconazole.
These medicines are processed through enzyme systems in the liver, especially the cytochrome P450 system. Unfortunately, many other medicines also use these same pathways.
This means antifungals can sometimes:
- increase levels of other medicines,
- reduce levels of other medicines,
- increase side effects,
- affect liver function,
- change how well treatments work.
Because aspergillosis patients often take several medicines at the same time, interactions become particularly important.
Common medicines that may interact with antifungals
Not every interaction is dangerous, and many medicines can still be used safely with careful monitoring. However, some combinations require dose adjustments or additional caution.
Steroids and inhalers
Many patients with allergic bronchopulmonary aspergillosis (ABPA), severe asthma or bronchiectasis take steroid medicines.
Interactions can occur with:
- prednisolone,
- methylprednisolone,
- inhaled steroids such as fluticasone or budesonide.
Azole antifungals can increase steroid exposure, potentially increasing the risk of side effects such as:
- weight gain,
- skin thinning,
- high blood sugar,
- adrenal suppression,
- mood changes.
Heart medicines
Some antifungals can affect heart rhythm or interact with medicines used for:
- high blood pressure,
- irregular heartbeat,
- blood thinning,
- cholesterol management.
This is one reason doctors and pharmacists carefully review medication lists before starting antifungal treatment.
Acid suppressants
Medicines used for acid reflux or stomach protection may affect how well some antifungals are absorbed.
This includes:
- omeprazole,
- lansoprazole,
- esomeprazole,
- antacid preparations.
In some cases, antifungal levels may become too low to work effectively.
Antibiotics and other anti-infective medicines
Some antibiotics and antifungals can interact in ways that increase side effects or affect the electrical activity of the heart.
This is particularly important in people already taking multiple medicines.
Supplements and herbal remedies
Patients are often surprised that supplements may also interact with antifungals.
Potential concerns include:
- CBD oil or cannabis products,
- St John’s Wort,
- high-dose vitamins,
- herbal sleep remedies,
- sports supplements.
“Natural” products can still affect liver enzyme systems and may alter medicine levels.
What is AntifungalInteractions.org?
AntifungalInteractions.org is a specialist online interaction checker designed specifically for antifungal medicines.
The site was developed to help healthcare professionals identify and manage potential interactions involving antifungal drugs.
It is widely used internationally and is regularly updated by specialist pharmacy experts.
Why is it useful?
General drug references do not always provide detailed fungal-specific interaction guidance.
AntifungalInteractions.org focuses specifically on antifungal medicines and often provides:
- more detailed interaction information,
- clearer explanations of risks,
- practical management advice,
- colour-coded interaction severity ratings.
This can help patients better understand why clinicians sometimes adjust medicines, order blood tests or recommend monitoring.
Can patients use the website themselves?
Yes — many patients find it useful for understanding their treatment better.
However, it is important not to interpret interaction checkers without context.
An interaction warning does not automatically mean:
- a medicine combination is unsafe,
- treatment must stop,
- harm will definitely occur.
Many interactions can be safely managed by:
- dose adjustments,
- blood test monitoring,
- timing changes,
- careful clinical supervision.
What should patients do?
Patients should try to keep an up-to-date list of:
- prescription medicines,
- inhalers,
- vitamins,
- supplements,
- CBD or cannabis products,
- over-the-counter medicines.
It is particularly important to mention supplements or herbal remedies because these are easily overlooked during clinic visits.
Do not stop medicines without advice
One of the most important messages is that patients should not stop antifungal medicines or other prescribed treatments based only on an online interaction checker.
Antifungal treatment decisions are often carefully balanced against:
- severity of fungal disease,
- lung function,
- other illnesses,
- alternative treatment options.
Healthcare teams can often safely manage interactions once they are aware of them.
The bottom line
Drug interactions are an important part of antifungal treatment, particularly for people living with aspergillosis who may already take several medicines.
AntifungalInteractions.org is an excellent specialist resource that can help patients and healthcare professionals better understand these interactions.
However, online interaction checkers should support discussions with healthcare professionals rather than replace them.
Useful link
Visit AntifungalInteractions.org
BNF to check any other medication interactions
Author and review information
Prepared as general educational information for people affected by aspergillosis and related lung conditions.
This article does not replace personalised medical advice.
Last reviewed: May 2026
AntifungalInteractions.org – A Specialist Resource for Safer Antifungal Treatment
Last reviewed: April 2026
Managing antifungal medications can be complex. Many antifungal drugs interact with other medicines, foods, and even supplements.
To support both patients and healthcare professionals, a dedicated resource is available:
AntifungalInteractions.org.
Key Points
- A specialist database focused specifically on antifungal drug interactions
- More detailed and targeted than general resources such as the British National Formulary (BNF)
- Includes guidance designed for both healthcare professionals and patients
- Regularly updated (typically several times per month)
- Maintained by an experienced clinical pharmacist and prescriber
- Owned and supported by the Fungal Infection Trust
What is AntifungalInteractions.org?
AntifungalInteractions.org is a dedicated online database designed to help users understand how antifungal medications interact with:
- Other prescribed drugs
- Over-the-counter medications
- Herbal supplements
- Certain foods and drinks
Unlike general drug reference tools, this resource focuses specifically on antifungal medicines, making it particularly useful for conditions such as aspergillosis, where treatment often involves long-term or complex therapy.
Why This Resource Matters
1. Antifungal drugs are complex
Common antifungal medications such as azoles (e.g. itraconazole, voriconazole, posaconazole) are known to interact with many other drugs.
These interactions can:
- Increase side effects
- Reduce treatment effectiveness
- Require dose adjustments or monitoring
2. General resources may not go far enough
Widely used tools like the British National Formulary (BNF) are essential, but they are designed for broad use across all medicines.
AntifungalInteractions.org provides:
- More detailed interaction explanations
- Practical interpretation of risk
- Condition-specific relevance
3. It supports informed discussions
The database is not a replacement for clinical advice, but it can help patients and clinicians:
- Prepare for consultations
- Understand potential risks
- Ask more informed questions
Who Maintains the Database?
AntifungalInteractions.org is maintained by:
Saarah Niazi-Ali
MPharm, PG Cert (General Pharmacy Practice), PG Dip (Advanced Clinical Pharmacy Practice),
Independent Pharmacist Prescriber, Non-Medical Prescribing (Level 7), Final Medical Signatory
The database is updated frequently—typically 3–4 times per month, often on a weekly basis—ensuring that information remains current and clinically relevant.
Governance and Ownership
The resource is owned and supported by the Fungal Infection Trust, a UK-based organisation dedicated to improving the understanding, diagnosis, and treatment of fungal diseases.
This ensures that the database:
- Remains focused on patient benefit
- Is aligned with specialist fungal disease care
- Supports both clinical practice and patient education
Who Is It For?
Patients and carers
- To better understand their medications
- To check for potential interactions
- To support conversations with their clinical team
Healthcare professionals
- Infectious disease specialists
- Respiratory clinicians
- Pharmacists
- GPs managing complex patients
It is particularly valuable for clinicians managing conditions such as:
- Chronic pulmonary aspergillosis (CPA)
- Allergic bronchopulmonary aspergillosis (ABPA)
- Other fungal infections requiring long-term antifungal therapy
How Does It Compare to Other Resources?
| Feature | AntifungalInteractions.org | General Drug References (e.g. BNF) |
|---|---|---|
| Focus | Antifungal-specific | All medicines |
| Level of detail | High (specialist) | Moderate (broad coverage) |
| Patient-friendly explanations | Yes | Limited |
| Update frequency | Frequent (monthly/weekly) | Regular but broader scope |
Important Notes for Patients
While this database is a valuable resource, it should be used appropriately:
- Do not stop or change medication based on what you read
- Always discuss concerns with your doctor, pharmacist, or specialist team
- Use the information to support—not replace—medical advice
When to Seek Medical Advice
Contact your healthcare provider if you:
- Start a new medication while on antifungal treatment
- Experience new or worsening side effects
- Are unsure whether a supplement or food is safe
- Have been advised of a potential interaction
Summary
AntifungalInteractions.org is a highly valuable, specialist resource that fills an important gap in antifungal care.
Its combination of:
- Expert clinical oversight
- Frequent updates
- Patient-accessible explanations
- Specialist focus
makes it an important tool for both patients and healthcare professionals managing fungal disease.
Further Reading
- British National Formulary (BNF)
- Aspergillosis treatment guidance (aspergillosis.org)
Author & Review
Prepared for Aspergillosis patient and healthcare education.
Content aligned with UK specialist practice and reviewed for clarity and safety.
Voriconazole interactions: what patients need to know
Key points
- Voriconazole interacts with many medicines.
- It affects several liver enzyme pathways, including CYP3A4, CYP2C19, and CYP2C9.
- Its behaviour can vary more from one person to another than some other azoles.
- Some medicines can make voriconazole stronger, while others can make it less effective.
- Visual side effects and sensitivity to sunlight are well recognised with voriconazole.
What is voriconazole?
Voriconazole is an azole antifungal often used in serious fungal infections, including aspergillosis. It can be very effective, but it also has a relatively complex interaction profile.
Why voriconazole interacts with so many medicines
Voriconazole affects several liver enzyme systems, including CYP3A4, CYP2C19, and CYP2C9. It can increase the levels of some medicines, while some other medicines can lower voriconazole levels and reduce its effectiveness.
Because voriconazole metabolism varies between patients, the same combination can affect people differently.
The interaction groups most likely to matter
Steroids
Voriconazole can increase exposure to some steroids, including inhaled steroids, which may increase the risk of steroid side effects.
Medicines that reduce voriconazole levels
Some medicines, including certain anti-seizure medicines and rifampicin-type antibiotics, can reduce voriconazole levels so much that the antifungal may not work properly.
Blood thinners
Some blood thinners may become stronger when taken with voriconazole, increasing bleeding risk.
Heart rhythm medicines
Voriconazole can contribute to QT prolongation, so combinations with other medicines that affect heart rhythm may be particularly important.
Statins
Some statins can become stronger when taken with voriconazole, increasing the risk of muscle side effects.
Immunosuppressants
Medicines such as tacrolimus and ciclosporin can rise significantly with voriconazole and often require specialist monitoring and dose adjustment.
Sedatives and some mental health medicines
Some sedatives and psychiatric medicines can become stronger when combined with voriconazole, increasing the risk of drowsiness, confusion, or other side effects.
Voriconazole-specific issues patients should know
Visual changes
Temporary visual disturbances are well recognised with voriconazole. Patients may notice blurred vision, brighter vision, or changes in colour perception.
Photosensitivity
Voriconazole can increase sensitivity to sunlight. Patients should use sensible sun protection and report new skin changes, especially during long-term treatment.
Variable drug levels
Voriconazole levels can vary between patients, which is one reason some teams use therapeutic drug monitoring in selected situations.
What patients should do in practice
- Tell your clinical team and pharmacist that you are taking voriconazole.
- Check before starting new medicines, including over-the-counter or herbal products.
- Report visual changes, significant sensitivity to sunlight, or a change in symptoms after a medicine change.
- Do not change treatment without advice.
When to seek medical advice
Seek medical advice urgently for severe bleeding, fainting, severe palpitations, marked confusion, or rapid worsening after a medicine change.
Important
This page is educational and does not list every interaction. For a full check, use the BNF interaction checker or speak to a pharmacist or clinician.
References
Itraconazole interactions: what patients need to know
Key points
- Itraconazole can interact with many other medicines.
- It usually does this by affecting liver enzymes, especially CYP3A4.
- Some combinations need careful monitoring, while others are best avoided.
- Capsules and liquid formulations are not handled by the body in exactly the same way.
- This page highlights the interactions most likely to matter to people with aspergillosis.
What is itraconazole?
Itraconazole is an azole antifungal used in aspergillosis and other fungal infections. It has a relatively high interaction burden, so medicine checks are especially important before starting it and whenever another medicine is added, stopped, or changed.
Why itraconazole interacts with so many medicines
Itraconazole can increase the levels of some other medicines by affecting liver enzymes, especially CYP3A4. This means that some medicines may become stronger than intended, which can increase the risk of side effects or toxicity.
The interaction groups most likely to matter
Steroids and inhalers
This is one of the most important groups for many aspergillosis patients, especially those with asthma or allergic bronchopulmonary aspergillosis. Itraconazole can increase exposure to some steroids, including inhaled steroids, which may increase the risk of steroid side effects.
Possible symptoms to report: unusual weight gain, easy bruising, increased facial rounding, mood changes, worsening blood sugar control, weakness, or marked fatigue.
Statins
Some statins can become much stronger when taken with itraconazole. This can increase the risk of muscle toxicity.
Possible symptoms to report: new muscle pain, muscle weakness, or dark urine.
Blood thinners
Itraconazole can increase the effect of some blood thinners, which may raise bleeding risk.
Possible symptoms to report: unusual bruising, bleeding that is hard to stop, black stools, vomiting blood, or coughing up much more blood than usual.
Heart and rhythm medicines
Some combinations can increase the risk of serious heart rhythm problems. Itraconazole is also used cautiously in people with a history of ventricular dysfunction or heart failure unless the infection is serious.
Possible symptoms to report: fainting, palpitations, marked dizziness, increasing ankle swelling, or worsening breathlessness.
Sleeping tablets, sedatives, and some mental health medicines
Some sedatives and psychotropic medicines can become stronger when combined with itraconazole, increasing the risk of drowsiness, confusion, falls, or breathing problems.
Immunosuppressants
Medicines such as tacrolimus and ciclosporin can rise significantly when taken with itraconazole and usually need specialist monitoring.
Medicines that can make itraconazole less effective
Some medicines lower itraconazole levels, which means the antifungal may not work as well. This can happen with some anti-seizure medicines, rifampicin-type antibiotics, and some antiviral medicines.
Acid-reducing medicines and itraconazole capsules
Reduced stomach acid can lower the absorption of itraconazole capsules. This means reflux medicines, antacids, and some acid-suppressing treatments can affect how well the capsules work. The liquid formulation behaves differently and should not be treated as interchangeable with capsules.
What patients should do in practice
- Keep a current medicines list and bring it to appointments.
- Tell clinicians and pharmacists if you are taking itraconazole.
- Ask specifically about inhalers, steroid tablets, statins, blood thinners, and reflux treatment.
- Do not change doses or stop medicines without advice.
- If your itraconazole formulation changes, ask whether it should be taken with food or on an empty stomach.
When to seek medical advice
Seek urgent medical advice for severe bleeding, black stools, vomiting blood, severe muscle pain, fainting, marked palpitations, or rapidly worsening breathlessness.
Important
This page is not a full interaction database. For a complete medicine-by-medicine check, use the BNF interaction checker or speak to a pharmacist or clinician.
References
Amphotericin B interactions: what patients need to know
Key points
- Amphotericin B comes in different formulations, and they are not interchangeable.
- Its main interaction risks are different from the azoles.
- The most important problems are usually kidney stress, low potassium, low magnesium, and additive toxicity with other medicines.
- These risks matter most with intravenous treatment.
- If you hear “amphotericin B”, it is important to know which formulation is being used.
What is amphotericin B?
Amphotericin B is an antifungal used mainly for serious fungal infections. In modern UK practice this often means liposomal amphotericin B, but conventional amphotericin B deoxycholate is also a recognised formulation.
Why amphotericin B interactions are different from azoles
Unlike azole antifungals, amphotericin B does not mainly cause medicine interactions through liver enzymes. Its most important interaction risks usually relate to kidney injury, low potassium, low magnesium, and infusion-related effects.
The interaction groups most likely to matter
Other medicines that can damage the kidneys
This is one of the most important groups. Combining amphotericin B with other nephrotoxic medicines can increase the risk of kidney injury.
Diuretics, steroids, and other medicines that lower potassium
Amphotericin B can lower potassium, and some other medicines can make this worse. This may increase the risk of weakness, cramps, or heart rhythm problems.
Digoxin and heart-rhythm-sensitive situations
Low potassium caused by amphotericin B can make digoxin-related toxicity more likely and may increase the importance of electrolyte monitoring.
Flucytosine
When combined with flucytosine, specialist monitoring may be needed because toxicity can increase.
Some cancer medicines and intensive hospital treatments
In hospital, additive toxicity with other intensive treatments may be particularly important, especially where kidneys and electrolytes are already under strain.
White blood cell transfusions
Acute lung reactions are a recognised specialist concern if amphotericin B is given during or soon after leukocyte transfusions.
Why the formulations matter
Amphotericin B formulations are not interchangeable. Conventional amphotericin B deoxycholate and liposomal amphotericin B have different dosing, different handling by the body, and different safety profiles. Using the wrong formulation in the wrong dose has caused serious and even fatal errors.
In general, liposomal amphotericin B is less nephrotoxic than conventional amphotericin B deoxycholate, but it still requires careful monitoring.
What patients should do in practice
- Ask which amphotericin B formulation is being used.
- Tell the clinical team about all medicines, especially kidney-risk medicines, diuretics, steroids, and digoxin.
- Expect blood tests to monitor kidney function, potassium, and magnesium during intravenous treatment.
- Report weakness, reduced urine output, worsening swelling, palpitations, or marked dizziness.
When to seek medical advice
Seek urgent medical help for severe breathlessness, fainting, major palpitations, or a rapid deterioration during treatment.
Important
This page is educational and does not list every possible interaction. Amphotericin B treatment is usually managed by specialist teams, especially when given intravenously.
References
Isavuconazole interactions: what patients need to know
Key points
- Isavuconazole can interact with other medicines, but its interaction profile is often less complex than older azoles.
- It mainly interacts through CYP3A4.
- Some medicines can increase isavuconazole levels, while others can reduce its effectiveness.
- It has an important difference from some other azoles: it can shorten the QT interval.
- It is still essential to check new medicines carefully.
What is isavuconazole?
Isavuconazole is a newer azole antifungal used in invasive aspergillosis and some other serious fungal infections. It is often seen as having a more predictable interaction profile than some older azoles, but it still has important interactions.
Why isavuconazole interacts with other medicines
Isavuconazole is mainly linked to CYP3A4. This means some medicines can become stronger when combined with it, while other medicines can lower isavuconazole levels and reduce its effectiveness.
The interaction groups most likely to matter
Medicines that reduce isavuconazole effectiveness
Some medicines, including rifampicin-type antibiotics and certain anti-seizure drugs, can lower isavuconazole levels and may make treatment ineffective.
Steroids
Some steroid levels may rise with isavuconazole, although the interaction pattern is often less intense than with some older azoles.
Immunosuppressants
Medicines such as tacrolimus and ciclosporin may increase and usually need specialist review and monitoring.
Blood thinners
Some blood thinners may become stronger, increasing bleeding risk.
Statins
Some statin levels may increase, which can raise the risk of muscle side effects.
Important isavuconazole-specific points
QT shortening
Unlike several other azole antifungals, isavuconazole can shorten the QT interval. This is an important difference and should be considered when other heart medicines are being reviewed.
Generally simpler interaction profile
Compared with itraconazole and voriconazole, isavuconazole is often considered a little easier to manage in patients taking several medicines, although checks are still essential.
What patients should do in practice
- Tell your pharmacist or clinician if you are taking isavuconazole.
- Check before starting prescription, over-the-counter, or herbal medicines.
- Ask specifically about anti-seizure drugs, antibiotics, blood thinners, and heart medicines.
- Do not stop or change medicines without advice.
When to seek medical advice
Seek medical advice urgently for severe bleeding, fainting, severe palpitations, severe muscle pain, or rapid worsening after a medicine change.
Important
This page is educational and not a complete interaction database. For a full check, use the BNF interaction checker or speak to a pharmacist or clinician.
References
- BNF: isavuconazole monograph and interactions
- UK isavuconazole SmPCs - not available
Posaconazole interactions: what patients need to know
Key points
- Posaconazole can interact with other medicines, although its interaction pattern is often a little simpler than itraconazole or voriconazole.
- It mainly interacts through CYP3A4 inhibition.
- Important interaction groups include immunosuppressants, steroids, blood thinners, and some heart medicines.
- Some medicines can reduce posaconazole levels and make treatment less effective.
- Tablets and oral suspension are not interchangeable in the same way.
What is posaconazole?
Posaconazole is an azole antifungal used in aspergillosis and in some high-risk patients for prevention of fungal infection. It is often seen as somewhat easier to manage than some older azoles, but important interactions still exist.
Why posaconazole interacts with other medicines
Posaconazole mainly affects CYP3A4, a key liver enzyme involved in handling many medicines. This means some drugs can become stronger, while some combinations can lower posaconazole levels and make it less effective.
The interaction groups most likely to matter
Steroids
Posaconazole can increase exposure to some steroids, including inhaled or oral steroids, which may increase the risk of steroid side effects.
Immunosuppressants
Medicines such as tacrolimus and ciclosporin can rise significantly with posaconazole and usually need close specialist monitoring.
Blood thinners
Some blood thinners may become stronger, increasing bleeding risk.
Statins
Some statins can rise in level, increasing the risk of muscle problems.
Heart rhythm medicines
Some combinations can increase the risk of heart rhythm problems and need careful review.
Medicines that reduce posaconazole effectiveness
Some medicines, including rifampicin-type antibiotics and certain anti-seizure drugs, can lower posaconazole levels and may make treatment less effective.
Posaconazole formulations and absorption
Posaconazole comes in different forms, including tablets, oral suspension, and infusion. The oral suspension and tablets are not handled identically by the body and should not be assumed to be interchangeable dose-for-dose without clinical advice.
In practice, the tablets tend to be more predictable than the suspension.
What patients should do in practice
- Tell your pharmacist or clinician if you are taking posaconazole.
- Ask about new medicines, especially blood thinners, steroids, statins, and heart medicines.
- If your formulation changes, ask whether there are any special instructions.
- Do not stop or swap medicines without advice.
When to seek medical advice
Seek medical advice urgently for severe bleeding, fainting, major palpitations, severe muscle pain, or rapid worsening after a medicine change.
Important
This page does not list every interaction. For a full check, use the BNF interaction checker or speak to a pharmacist or clinician.
References
Antifungal drug interactions: what patients with aspergillosis need to know
Key points
- Antifungal medicines can interact with other medicines, including inhalers, steroid tablets, blood thinners, heart medicines, cholesterol tablets, and some over-the-counter or herbal products.
- The azole antifungals usually interact by affecting how the liver handles medicines.
- Amphotericin B is different: its main interaction risks are more often linked to kidneys, potassium, magnesium, and infusion-related effects.
- This page gives an overview. It does not list every interaction.
- For a full medicine-by-medicine check, use the BNF interaction checker or ask a pharmacist or clinician.
Why interactions matter in aspergillosis
People with aspergillosis often take more than one medicine. This may include inhalers, steroid tablets, medicines for reflux, antibiotics, pain relief, blood pressure treatment, blood thinners, cholesterol tablets, and drugs for other long-term conditions. That means medicine checks are especially important whenever an antifungal is started, stopped, or changed.
How the main antifungals differ
Most long-term interaction questions in aspergillosis involve the azole antifungals: itraconazole, voriconazole, posaconazole, and isavuconazole. These mainly interact because they affect liver enzymes, especially CYP3A4, although some also affect CYP2C9 and CYP2C19.
Amphotericin B behaves differently. Its most important risks are usually kidney stress, low potassium, low magnesium, and additive toxicity with other medicines rather than classic liver-enzyme interactions.
Quick comparison table
| Antifungal | Main interaction pattern | Typical complexity | Important extra point |
|---|---|---|---|
| Itraconazole | Strong enzyme-based interactions, especially CYP3A4 | High | Capsules and liquid are not handled by the body in the same way |
| Voriconazole | Complex enzyme-based interactions involving several CYP pathways | High | More variable between patients; visual side effects and photosensitivity are well recognised |
| Posaconazole | Mainly CYP3A4-related interactions | Moderate | Tablets and oral suspension are not interchangeable in the same way |
| Isavuconazole | Mainly CYP3A4-related interactions, usually less complex than older azoles | Lower to moderate | Can shorten the QT interval |
| Amphotericin B | Kidney, potassium, magnesium, and infusion-related interaction risks | Different rather than simpler | Formulations are not interchangeable |
Individual antifungal guides
- Itraconazole interactions: what patients need to know
- Voriconazole interactions: what patients need to know
- Posaconazole interactions: what patients need to know
- Isavuconazole interactions: what patients need to know
- Amphotericin B interactions: what patients need to know
What patients should do in practice
- Keep an up-to-date list of all medicines, including inhalers, creams, over-the-counter medicines, supplements, and herbal products.
- Tell your doctor, nurse, pharmacist, or hospital team that you are taking an antifungal.
- Do not start, stop, or swap medicines on your own because of something you have read online.
- Ask specifically about new medicines, steroid changes, reflux treatment, blood thinners, cholesterol medicines, and heart medicines.
When to seek medical advice
Seek medical advice promptly if symptoms change after a medicine is started, stopped, or changed. Seek urgent help for severe bleeding, fainting, severe muscle pain, marked palpitations, rapidly worsening breathlessness, severe drowsiness, or a sudden significant decline in your health.
Important
This resource is educational. It does not replace personalised advice from your clinical team, GP, or pharmacist, and it is not a complete interaction database.