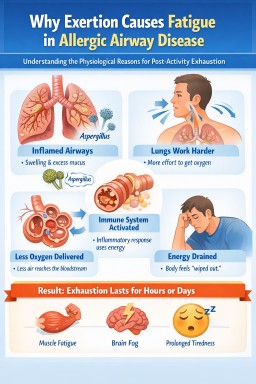
Managing fatigue and energy in aspergillosis and allergic fungal lung disease
Key points
- Many people with aspergillus-related lung conditions experience extreme tiredness after physical or mental exertion.
- This fatigue can last hours or even several days.
- Breathing, immune activity, inflammation and sometimes hormone imbalance all use extra energy.
- Activity can temporarily increase airway inflammation and mucus.
- Managing energy carefully (“spoon theory”) can help prevent fatigue crashes.
Contents
- Why people with lung disease feel exhausted after exertion
- What is happening in the lungs and body
- Managing energy: the “spoon theory”
- Practical ways to manage energy
- Nutrition and adrenal health
- Warning signs you are running out of energy
- Why fatigue in lung disease is different from normal tiredness
- Daily energy management checklist
- Can this fatigue be treated?
- When to talk to your doctor
Why people with lung disease feel exhausted after exertion
Healthy lungs have a large reserve capacity. When we exercise or do physical work, breathing becomes deeper and faster, but the lungs can usually cope easily.
In people with aspergillosis or allergic airway disease, the airways may already be:
- inflamed
- narrowed
- filled with mucus
- sensitive to allergens such as Aspergillus fumigatus
When the body demands more oxygen during activity, the lungs must work much harder to supply it. Activities that seem minor to other people may therefore require much greater effort from the body.
What is happening in the lungs and body?
Inflamed airways
Many aspergillus-related conditions involve inflammation in the airways. The immune system releases chemicals that cause:
- swelling of airway walls
- increased mucus production
- greater airway sensitivity
During exertion, breathing becomes faster and deeper, which can irritate these inflamed airways further.
Mucus affecting airflow
Inflamed airways often produce extra mucus. This mucus can partly block airflow and lead to:
- coughing
- wheezing
- breathlessness
- uneven airflow within the lungs
This may reduce how efficiently oxygen enters the bloodstream. Doctors sometimes refer to this as ventilation–perfusion mismatch.
Breathing uses more energy
In healthy people, breathing uses only a small fraction of the body's energy. In lung disease, breathing may require much more effort.
Additional muscles may assist breathing, including:
- chest muscles
- neck muscles
- shoulder muscles
These muscles can become fatigued during activity, just like leg muscles after exercise.
Immune system activity
If the immune system reacts to fungal proteins or allergens, it releases signalling chemicals called cytokines. These chemicals can produce symptoms similar to mild illness, including fatigue, brain fog and muscle aches.
Delayed inflammation after activity
Some people notice that fatigue appears later rather than immediately. Physical effort can trigger inflammation that develops over 12–48 hours, increasing mucus production, airway irritation and tiredness.
This explains why people sometimes feel worse the day after a busy day.
Managing energy: the “spoon theory”
Many people with chronic illness find it helpful to think about their energy using the idea of spoon theory.
In this idea:
- each spoon represents a small unit of energy
- you start the day with a limited number of spoons
- each activity uses some of those spoons
Because breathing and inflammation already use energy, people with lung disease may begin the day with fewer spoons available.
Example of spoon use
| Activity | Possible energy use |
|---|---|
| Getting dressed | 1 spoon |
| Showering | 2–3 spoons |
| Cooking a meal | 2 spoons |
| Doctor’s appointment | 3–4 spoons |
| Busy social day | Many spoons |
If too many spoons are used early in the day, the body may run out of energy, leading to exhaustion lasting hours or even days.
Practical ways to manage energy
Plan activities around your best time of day
| Time of day | Suggested activities |
|---|---|
| Morning | Errands or appointments |
| Midday | Light household tasks |
| Afternoon | Quieter activities |
| Evening | Rest and recovery |
Break tasks into smaller steps
Large tasks can overwhelm the lungs and muscles. Instead of doing everything at once:
- clean one room at a time
- cook in stages
- prepare things earlier in the day
Use the 50–70% rule
Try to stop activity when you reach about half to two-thirds of your limit. Stopping early often prevents the fatigue crash that can occur later.
Use breathing techniques
Pursed-lip breathing
- breathe in through your nose
- breathe out slowly through gently pursed lips
Rhythmic breathing
Match breathing with movement, for example when climbing stairs.
Keep mucus moving
Mucus increases the work of breathing. Helpful strategies include:
- airway clearance techniques
- staying well hydrated
- gentle movement
- using inhalers or nebulisers as prescribed
Maintain gentle regular activity
Although exertion can cause fatigue, complete inactivity can worsen the problem. Gentle activity such as walking or pulmonary rehabilitation exercises helps maintain muscle strength.
Protect sleep
- maintain a regular sleep routine
- clear mucus before bedtime if needed
- avoid heavy exertion late in the evening
Nutrition and adrenal health
Nutrition and energy
Good nutrition helps support energy levels. Helpful strategies include:
- eating regular meals
- including protein for muscle repair (eggs, fish, dairy, beans or nuts)
- eating complex carbohydrates for steady energy
- drinking enough fluids
Some people find that smaller, more frequent meals reduce breathlessness compared with large meals.
Important nutrients
- protein
- vitamin D
- iron
- B vitamins
Doctors may check for deficiencies if fatigue is severe.
Adrenal insufficiency
Some patients who have taken long-term steroid medications may develop adrenal insufficiency. The adrenal glands normally produce cortisol, which helps regulate energy and stress responses.
Symptoms may include:
- severe fatigue
- dizziness
- muscle weakness
- difficulty recovering after exertion
Patients with adrenal insufficiency usually take hydrocortisone replacement therapy and should follow their doctor’s advice carefully.
Warning signs you are running out of energy
- breathing becomes faster or more difficult
- increased coughing or mucus
- arms or legs feel heavy
- dizziness or weakness
- difficulty concentrating
- chest tightness or wheezing
When these warning signs appear, it is usually best to stop and rest before continuing.
Why fatigue in lung disease is different from normal tiredness
Fatigue in lung disease is not simply normal tiredness. Several factors occur at the same time:
- breathing requires more energy
- the immune system may be active
- oxygen exchange may be less efficient
- nutrition and hormone balance may influence recovery
Because of this combination, fatigue may appear suddenly and last longer than expected.
Daily energy management checklist
Pacing and activity
- spread activities across the day
- stop before exhaustion
- plan demanding tasks when energy is highest
- allow recovery time after busy days
Breathing and airway care
- use breathing techniques during exertion
- perform airway clearance if needed
- take inhalers or nebulisers as prescribed
- stay well hydrated
Nutrition and medication
- eat regular meals
- include protein for muscle strength
- take medications as prescribed
- follow sick-day rules if you have adrenal insufficiency
Sleep and recovery
- maintain a regular sleep routine
- clear mucus before bedtime
- rest when warning signs appear
Can this fatigue be treated?
Fatigue associated with aspergillosis, allergic fungal airway disease, or severe asthma can sometimes be improved when the underlying causes are treated. Because several different processes contribute to fatigue, treatment usually focuses on improving multiple factors rather than a single cure.
Treating airway inflammation
Inflammation in the airways is one of the major contributors to fatigue. When the airways are inflamed:
- breathing requires more effort
- mucus production increases
- oxygen exchange becomes less efficient
Treatments aimed at reducing airway inflammation may include:
- Inhaled corticosteroids – commonly used in asthma to reduce inflammation directly in the airways.
- Antifungal therapy – in some patients, reducing fungal growth can reduce immune activation and inflammation.
- Biologic therapies – newer treatments that target specific immune pathways involved in allergic and inflammatory lung disease.
Biologic treatments
Biologics are one of the most promising areas of treatment for severe asthma and allergic airway disease. These medications target specific parts of the immune system that drive inflammation.
| Biologic | Target | Effect |
|---|---|---|
| Omalizumab | IgE | Reduces allergic inflammation |
| Mepolizumab / Benralizumab | IL-5 pathway | Reduces eosinophilic inflammation |
| Dupilumab | IL-4 / IL-13 | Reduces type-2 inflammation |
| Tezepelumab | TSLP | Blocks upstream inflammatory signalling |
Some patients with conditions such as allergic bronchopulmonary aspergillosis (ABPA) or severe asthma report improvements in breathlessness, symptoms and overall energy levels when inflammation is better controlled.
Improving mucus clearance
Mucus in the airways increases the work of breathing and can contribute to fatigue. Strategies that may help include:
- airway clearance techniques
- physiotherapy
- maintaining good hydration
- using prescribed inhalers or nebulisers correctly
Treating other contributing factors
Fatigue can also be worsened by other health issues that are common in chronic lung disease, such as:
- iron deficiency
- vitamin deficiencies
- poor sleep
- adrenal insufficiency
- muscle deconditioning
Addressing these factors can sometimes improve overall energy levels.
Pulmonary rehabilitation
Pulmonary rehabilitation programmes combine exercise training, breathing techniques and education about pacing activities. These programmes can improve muscle efficiency and exercise tolerance, and many patients report reduced fatigue and improved quality of life.
Future treatments
Research into inflammatory lung diseases is advancing rapidly. New biologic drugs and other targeted therapies are being developed that may improve control of airway inflammation.
Researchers are also studying how the lung microbiome (bacteria and fungi living in the airways) influences inflammation. In the future, this may lead to more personalised treatments for patients with fungal-related lung disease.
Inflammatory fatigue
Researchers are increasingly recognising that chronic inflammatory diseases can cause a form of fatigue sometimes called “inflammatory fatigue.”
In these conditions, immune signalling chemicals released during inflammation can affect the brain and energy metabolism. Similar patterns of fatigue are seen in diseases such as rheumatoid arthritis and inflammatory bowel disease.
This may help explain why some treatments that reduce inflammation — including biologic therapies — can improve fatigue even when lung function measurements change only modestly.
Interrupting the fatigue cycle
Treatment aims to interrupt the cycle that can develop in chronic lung disease:
Airway inflammation
↓
Breathing requires more effort
↓
More energy used by respiratory muscles
↓
Immune system activity
↓
Reduced overall energy and fatigue
By improving airway inflammation, mucus clearance, muscle strength and overall health, many patients find their energy levels become more manageable.
When to talk to your doctor
Seek medical advice if:
- fatigue becomes progressively worse
- breathlessness increases
- new symptoms appear such as chest pain or coughing up blood
- fatigue prevents normal daily activities
A reassuring message
Many people with aspergillosis or allergic airway disease worry that exhaustion means their condition is worsening.
In most cases it reflects the extra energy required for breathing, inflammation and immune activity. Learning to pace activity can help people live more comfortably with chronic lung disease.
Author: National Aspergillosis Centre information team
Review: Clinical review recommended
Last reviewed: 2026