Potential respiratory hazards of fungal exposure in the residential indoor environment: a systematic review (2025)
Summary of the 2025 Systematic Review for Non-Specialists & Patients
Read full paper here: Potential respiratory hazards of fungal exposure in the residential indoor environment: a systematic review - ScienceDirect
What was this review about?
This review looked at all the scientific evidence from 1990–2025 on how indoor fungi (moulds) in homes affect people’s breathing and general respiratory health. It examined 94 studies, mapping out where fungi come from, which species appear most often, and how they affect the lungs, nose, throat, and immune system.
Key Findings in Plain Language
1. The biggest sources of indoor mould are dampness and building damage
Homes with water leaks, damp walls, damaged materials and poor ventilation are the most common sources of fungi—especially Aspergillus and Penicillium. These thrive in wet building materials, bathrooms, kitchens, drains, air-conditioning systems and even water dispensers.
2. Indoor fungi are strongly linked to a wide range of respiratory symptoms
Across many countries, indoor fungal exposure was associated with:
-
Asthma and asthma flare-ups
-
Allergic rhinitis (blocked or runny nose)
-
Chronic cough and throat irritation
-
Adenoid enlargement in children
-
Hypersensitivity pneumonitis (allergic inflammation of the lungs)
-
Reduced lung function
-
Even pulmonary haemorrhage in rare cases
The review shows that even everyday exposure—not just visibly mouldy homes—can worsen respiratory health.
3. Some fungi are more strongly associated with illness
Important associations include:
-
Aspergillus → asthma symptoms, COPD exacerbations, throat irritation, hypersensitivity reactions
-
Penicillium → asthma, allergic rhinitis, hypersensitivity pneumonitis
-
Alternaria → childhood asthma risk
-
Candida & Fusarium → present in wet areas such as bathrooms and may affect vulnerable individuals
4. The geographic picture is uneven
Most research comes from high-income, temperate countries. There are major evidence gaps in tropical and subtropical regions, where humidity is high and fungal exposure is likely worse. This limits current global understanding of risk.
5. Prevention works — but public awareness is low
Simple actions (cleaning, improved ventilation, addressing leaks, correct humidity ranges) can radically reduce fungal burden. One study showed 80–90% reduction in airborne mould counts after residents were given basic remediation advice.
What’s New or Important in This 2025 Review?
1. A fully integrated “source → species → disease → location” map
The review is the first to link fungal sources, the exact fungi found, the diseases they cause, and where the evidence comes from, creating a multi-layered evidence map. This helps identify:
-
Which household features pose the highest risk
-
Which fungi are clinically most important
-
Where research gaps exist
2. Highlights the major global research imbalance
It emphasises that very little evidence exists from low-income and tropical areas—where exposure may be far more severe. This is a call for equity and better global surveillance.
3. Shows that fungi may affect more than the lungs
The review notes new evidence that fungal exposure may also influence neurological and immune-mediated symptoms, suggesting mould exposure could have broader health effects than traditionally recognised.
4. Identifies major gaps in identifying which fungal species cause harm
Many studies only measure “mould level” without identifying the fungus. The review argues for better fungal detection technologies, such as:
-
Portable real-time samplers
-
Multi-omics (DNA, RNA, metabolites)
-
Long-term cohort studies
These tools could finally clarify which fungi cause which illnesses.
5. Strong emphasis on emerging technologies for prevention
Including:
-
UV and photocatalytic TiO₂ devices
-
Improved antifungal cleaning agents
-
Building materials designed to resist mould growth
-
Volcanic minerals and clays that absorb harmful compounds
Why This Review Matters (for Patients, Carers, and Clinicians)
1. It shows mould is not “just an allergy problem”
Indoor fungi can worsen or trigger asthma, COPD, hypersensitivity pneumonitis, chronic sinus issues, and may even influence immune and neurological health. This validates patient experiences where damp homes worsen symptoms.
2. It provides strong evidence for housing-related health advocacy
Patients can use this to:
-
Request landlord repairs
-
Support home assessments
-
Advocate for rehousing if severe mould is present
-
Justify humidifier/dehumidifier use, and ventilation improvements
3. It highlights the importance of early remediation
Even simple cleaning and remediation steps can dramatically reduce mould burden and symptoms—important for families, vulnerable groups, and those with chronic lung disease.
4. It gives clinicians a clearer evidence base
Respiratory teams can use this to:
-
Recognise when housing contributes to disease flare-ups
-
Understand which conditions are most strongly linked to indoor fungi
-
Make better-informed referrals for environmental health assessments
5. It builds a scientific foundation for future guidelines
The authors point out that national building codes, indoor air quality policies, and public health guidance lag behind the evidence—and this review is intended to inform future regulation.
Who Does This Help Most?
Patients with:
-
Asthma
-
Allergic bronchopulmonary aspergillosis (ABPA)
-
Aspergillus bronchitis
-
COPD (especially those with fungal-associated exacerbations)
-
Hypersensitivity pneumonitis
-
Children with recurrent respiratory infections
-
Anyone living in damp, mouldy, water-damaged, or poorly ventilated homes
Clinicians:
Respiratory physicians, GPs, ENT specialists, allergists, immunologists.
Policy & Housing Professionals:
Public health teams, environmental health officers, social landlords, housing associations.
Researchers:
Those developing diagnostics, fungal exposure studies, indoor air quality monitoring, or patient-centred environmental interventions.
What to do if you think you’ve been given the wrong dose of a medication
Advice for people living with aspergillosis
Most of the time, prescriptions are correct and safe. However, people with aspergillosis often have complex medical needs, and it is not unusual for treatment to differ from standard “one-size-fits-all” dosing. This means that occasionally, a prescription may not match what you usually receive or what your specialist has recommended.
If something doesn’t look right, it is reasonable — and responsible — to pause and check.
Why this can happen
Prescribing in GP surgeries and hospitals is usually done using electronic systems with preset doses and durations. These defaults are designed for the average patient and for common infections.
People with aspergillosis may:
-
need longer or higher-dose treatment
-
be taking interacting medicines (for example antifungals or steroids)
-
have been advised by a specialist to follow a non-standard plan
If this information is not clearly visible at the time of prescribing, the prescriber may reasonably select a default option that is not quite right for you. This is a system issue, not a personal failure.
Signs that a prescription may need checking
You might want to query a prescription if:
-
the dose or duration is different from what you usually receive
-
it does not match what your specialist discussed
-
it seems very short for a significant infection
-
the pharmacist queries it
-
you feel significantly worse after starting it
You do not need to know what the “correct” dose should be to ask for a review.
What to do — step by step
1. Do not ignore your concern
If something feels wrong, it is appropriate to pause and ask for clarification.
2. Speak to the pharmacist
Pharmacists are trained to spot dosing and duration issues. Ask:
-
“Does this look right for someone with my condition?”
-
“Could you check this against my previous prescriptions or clinic letters?”
Pharmacists can often contact the prescriber directly.
3. Contact the prescriber for a check
You can say:
-
“I have a long-term lung condition and usually need non-standard dosing.”
-
“Could this be checked against my specialist advice?”
This is a safety check, not a complaint.
4. Use trusted information sources
In the UK, the British National Formulary (BNF) lists usual doses and important side effects. You are not expected to interpret this alone, but it can help you explain your concern clearly.
5. If you are unsure, do not start or continue without advice
If you are worried about dose, duration, or side effects, seek medical advice urgently rather than continuing in uncertainty.
Why this matters for aspergillosis patients
In people with chronic lung disease:
-
under-dosing can lead to treatment failure or relapse
-
short courses may increase the risk of resistance
-
symptoms may worsen and be misinterpreted as disease progression
From an antimicrobial stewardship (AMS) perspective, the right dose and duration are just as important as avoiding unnecessary antibiotics.
This is about partnership, not blame
Most prescribing issues happen because:
-
systems default to standard settings
-
clinicians work under extreme time pressure
-
complex information is not always easy to see
Good care depends on patients, prescribers and pharmacists working together.
If safety depends on the patient spotting an error, the system needs improving — not the patient.
Key take-home message
If a prescription doesn’t look right for you, it is reasonable to ask for it to be checked.
Asking for clarification protects you and supports safer care for everyone.
Aspergillosis Patient Conference 2025 – summary and recording

The Aspergillosis Patient Conference 2025 took place online on 29 November 2025. The event was co-organised and co-presented by the National Aspergillosis Centre (NAC) and The Aspergillosis Trust, in collaboration with the European Lung Foundation (ELF).
The free conference brought together people living with aspergillosis, carers, patient advocates, clinicians and researchers from across Europe and beyond. Its focus was firmly patient-centred, combining clinical expertise with lived experience to improve understanding, awareness and care.
🎥 The full conference recording is now available to watch online, enabling anyone who missed the live event to benefit from the sessions and discussions.
What the conference covered
Across the programme, speakers explored:
-
What aspergillosis is and the different forms it can take
-
Symptoms and diagnostic challenges, including delays in recognition
-
Current treatment and management approaches
-
Living with aspergillosis, shared directly by patients
-
What needs to improve, including awareness, education and access to specialist care
Live questions, polling and discussion ensured that patient priorities and real-world concerns shaped the conversation throughout.
Speakers and perspectives
The conference featured a broad range of patient advocates and clinical experts, including:
-
People with lived experience of chronic pulmonary aspergillosis (CPA) and allergic bronchopulmonary aspergillosis (ABPA)
-
Representatives from NAC, The Aspergillosis Trust and the ELF Aspergillosis Patient Advisory Group
-
Respiratory physicians, infectious disease specialists and researchers involved in European clinical guidelines and research
This mix ensured that sessions reflected both medical best practice and day-to-day patient realities.
Who the recording is useful for
The on-demand recording is particularly valuable for:
-
People living with aspergillosis and related lung conditions
-
Family members, carers and supporters
-
Healthcare professionals seeking a patient-focused overview
-
Patient organisations and advocates working in respiratory or fungal disease
Why this conference matters
Aspergillosis remains under-diagnosed and poorly understood, despite its significant impact on health and quality of life. This conference highlighted:
-
The importance of patient voices in education and guideline development
-
The need for earlier diagnosis and clearer care pathways
-
The value of collaboration between specialist centres, patient charities and European organisations
By making the recording freely available, NAC, The Aspergillosis Trust and ELF have ensured the conference continues to support patients, carers and professionals well beyond the live event.
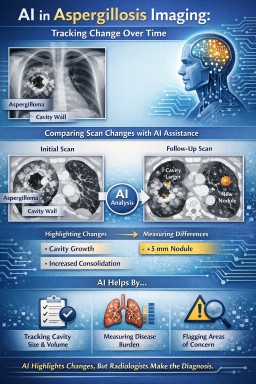
The role of AI in imaging follow-up for aspergillosis
Aspergillosis is not a single disease, but a spectrum of related conditions, including allergic bronchopulmonary aspergillosis (ABPA), chronic pulmonary aspergillosis (CPA), aspergilloma, subacute invasive aspergillosis, and Aspergillus bronchitis. Across this spectrum, imaging plays a central role in assessment, monitoring, and treatment planning.
Artificial intelligence (AI) is increasingly being explored in chest imaging as a supportive tool, particularly in the follow-up of chronic and complex lung disease. Its potential value in aspergillosis lies not in making diagnoses, but in consistent, data-driven image comparison.
Why aspergillosis is challenging for imaging interpretation
Imaging findings in aspergillosis are often:
-
Non-specific, overlapping with tuberculosis, non-tuberculous mycobacterial lung disease, lung cancer, vasculitis, and post-infectious scarring
-
Heterogeneous, even within the same patient
-
Slowly evolving, making change difficult to judge by eye
-
Mixed with other lung disease, such as bronchiectasis, asthma, fibrosis, or emphysema
For these reasons, imaging must always be interpreted in full clinical context and often benefits from specialist multidisciplinary discussion.
Where AI may add particular value
AI does not “know” that it is looking at aspergillosis. Instead, it compares imaging data directly, without assumptions about diagnosis. This can be helpful in several areas relevant to aspergillosis:
1. Consistent comparison of serial scans
AI can compare computed tomography (CT) scans over time using the same criteria each time, helping to:
-
Detect subtle interval change in cavities or nodules
-
Measure changes in cavity size, wall thickness, or internal content
-
Identify progression or stability that may be difficult to judge visually
This is particularly useful in chronic pulmonary aspergillosis, where progression may be slow and subtle.
2. Objective measurement of disease burden
AI can assist with:
-
Quantifying cavity volume or consolidation
-
Measuring extent of bronchiectasis or mucus plugging
-
Tracking changes following antifungal treatment or airway clearance
Objective measurements may help reduce subjectivity when monitoring response to treatment.
3. Highlighting areas for closer review
AI systems can flag areas of change or abnormality for radiologist attention. This may act as a “second set of eyes”, particularly in busy services, but does not replace expert review.
What AI cannot do in aspergillosis
It is important to be clear about the limitations:
-
AI cannot diagnose aspergillosis
-
AI cannot distinguish colonisation from active disease
-
AI cannot integrate symptoms, immune status, serology, or microbiology
-
AI cannot judge clinical significance or treatment need
For example, a change in cavity appearance may reflect active disease, treatment response, bacterial infection, bleeding, or simple movement of intracavitary material. Only expert clinical interpretation can determine significance.
Why radiologist expertise remains essential
In aspergillosis, small imaging changes can have very different meanings depending on context. Radiologists bring:
-
Experience in recognising mimics and artefacts
-
Understanding of treatment-related change
-
Ability to communicate uncertainty and recommend next steps
-
Integration of imaging with wider clinical information
AI may improve consistency and sensitivity, but responsibility for interpretation and reporting remains with the radiologist.
A balanced way to think about AI in aspergillosis imaging
In aspergillosis, artificial intelligence is best viewed as a tool that highlights and measures change, rather than one that explains or diagnoses it. Its strength lies in consistency; its limitation lies in lack of clinical understanding.
Used appropriately, AI may support safer and more consistent follow-up for people living with aspergillosis, while expert radiology and specialist clinical care remain central to diagnosis and management.
When treatment itself causes harm: an important message for people with aspergillosis
For most people, following medical advice is the safest and most appropriate course of action. However, for some people living with aspergillosis or other long-term lung conditions, treatment itself can occasionally cause harm — particularly when adverse drug reactions are not recognised early.
Aspergillosis often requires long-term or repeated courses of medication, sometimes alongside treatment for co-existing infections or other conditions. Because symptoms of aspergillosis can overlap with medication side effects, new or worsening problems may be assumed to be part of the illness rather than a reaction to treatment.
Why this can be difficult to recognise
People with aspergillosis may:
-
already experience fatigue, breathlessness, pain, or neurological symptoms
-
take multiple medicines at the same time
-
have fluctuating symptoms due to infection, inflammation, or treatment response
This makes it harder to distinguish disease activity from drug-related effects.
The importance of recognising adverse drug reactions
Some medicines commonly used in people with lung disease can, in a small number of individuals, cause serious or long-lasting side effects. These reactions may develop gradually or worsen with continued use.
Examples (not exhaustive) include:
-
Antibiotics – tendon, nerve, gastrointestinal, cardiac or immune-related effects
-
Antifungal medicines – liver toxicity, neurological symptoms, skin reactions, drug interactions
-
Steroids – bone loss, adrenal suppression, mood changes, infection risk
-
Immunosuppressive or biologic therapies – infection risk, immune dysregulation, inflammatory reactions
Not everyone experiences these effects, and many people take these medicines safely. However, when significant new symptoms appear after starting or changing treatment, they should be actively reassessed.
Why knowledge of medication side effects matters
Patients are not expected to diagnose themselves. However, having a basic awareness of known serious side effects can help patients recognise when something may not be right.
In the UK, trusted sources such as the British National Formulary (BNF) list both common and rare but serious adverse effects for prescribed medicines, and drug:drug interactions which are particularly significant for antifungal medications. Reviewing this information can support informed discussions with healthcare professionals, particularly if symptoms worsen rather than improve.
Checking authoritative sources is not about challenging clinical expertise or stopping treatment independently. It is about ensuring that potential drug reactions are considered alongside disease progression.
A balanced message for patients and clinicians
Safe care depends on partnership. This means:
-
patients feeling able to report side effects clearly and repeatedly if needed
-
clinicians remaining alert to drug reactions, especially when symptoms are atypical or progressive
-
being willing to pause, review, and reconsider treatment when outcomes are not as expected
Early recognition of adverse drug reactions can reduce the risk of long-term or permanent harm.
Take-home message
If treatment is making you feel significantly worse, and the symptoms do not feel right for you, it is reasonable to ask for reassessment — even if the treatment is commonly used or usually well tolerated.
Being informed, listened to, and reviewed promptly helps ensure safer care for people living with aspergillosis.
Using Radiopaedia and Online Imaging Resources Safely: What Expert Patients and Non-Specialist Clinicians Need to Know
Online radiology education platforms such as Radiopaedia (see aspergillosis images here) have transformed access to medical knowledge. They provide high-quality explanations of imaging findings, annotated examples, and differential diagnoses that are invaluable for learning, teaching, and patient empowerment.
For expert patients living with long-term conditions, and for non-specialist clinicians working outside radiology, these resources can greatly improve understanding of scan reports and discussions with healthcare teams. However, it is important to understand what these tools can – and cannot – do.
Radiopaedia is an educational resource, not a diagnostic service
Radiopaedia is designed to teach pattern recognition and radiological reasoning, not to provide individual diagnoses. The cases shown are curated examples, often with classic features, and are presented without the full clinical complexity that accompanies real patients.
Real-world imaging interpretation requires integration of:
-
Clinical history and symptoms
-
Laboratory results (for example inflammatory markers, microbiology, immunology)
-
Prior imaging and disease progression
-
Treatment history and response
-
Knowledge of common mimics and incidental findings
This clinical synthesis cannot be replicated by reviewing example images alone.
Why expert radiologist review still matters
For many diagnoses, there is no substitute for a radiologist formally reviewing and interpreting the imaging.
This is particularly true when:
-
Findings are subtle or evolving
-
Multiple conditions coexist (for example bronchiectasis, infection, scarring, and inflammation together)
-
Imaging appearances overlap between diseases
-
Treatment decisions depend on small but important changes over time
Radiologists are trained to recognise not only “textbook” appearances, but also atypical, incomplete, or misleading patterns, and to weigh uncertainty appropriately in their reports.
Imaging patterns are rarely diagnostic in isolation
Many imaging features are non-specific. For example:
-
Cavities can be caused by infection, inflammation, malignancy, or prior disease
-
Nodules may represent infection, scarring, inflammation, or benign change
-
Mucus plugging can occur in asthma, infection, allergic disease, or chronic airway disease
Educational resources often present differential diagnoses clearly, but deciding which diagnosis applies to a specific patient requires clinical judgment and experience.
A particular note for chronic lung and fungal disease
In complex conditions such as chronic lung disease, allergic lung disease, or fungal infections, imaging interpretation is especially nuanced. Appearances may change slowly, fluctuate with treatment, or overlap with other long-standing abnormalities.
Small changes that are significant to a specialist team may appear minor or ambiguous when viewed without context. Conversely, dramatic-looking findings may represent stable or inactive disease.
This is why specialist radiology input, often alongside multidisciplinary discussion, remains essential.
How expert patients and clinicians should use Radiopaedia
Used appropriately, Radiopaedia can:
-
Improve understanding of scan terminology
-
Help frame informed questions for clinicians
-
Support education and shared decision-making
-
Aid non-specialists in recognising when further advice is needed
It should not be used to:
-
Self-diagnose based on image similarity
-
Override formal radiology reports
-
Draw conclusions without clinical correlation
The key message
Radiopaedia and similar platforms are powerful educational tools. They enhance knowledge, confidence, and communication. But for many diagnoses, they complement rather than replace expert radiologist assessment.
The safest and most effective approach is to use educational resources alongside formal imaging reports, specialist input, and clinical discussion — not instead of them.
Beyond guidelines: what do I need to know when dealing with fungal diagnostics?
Cornelia Lass-Flörl. Clinical Microbiology and Infection (2025)
Why this paper matters
Diagnosing invasive fungal infections (including aspergillosis) remains difficult in real-world practice. Guidelines exist, but patients and clinicians often experience confusing or apparently conflicting test results. This narrative review explains why that happens and how results should be interpreted in context, particularly for Aspergillus infections.
Key messages relevant to aspergillosis
1. Your immune system strongly affects test results
The paper clearly explains that diagnostic tests behave very differently depending on immune status:
-
In neutropenic or heavily immunosuppressed patients, antigen tests such as galactomannan tend to perform better, while antibody tests often fail.
-
In immunocompetent or non-neutropenic patients, including many with chronic pulmonary aspergillosis (CPA), Aspergillus IgG antibody tests are often positive and clinically useful.
This helps explain why some patients are told their blood tests are “negative” despite ongoing disease.
2. Where the sample comes from matters
For lung aspergillosis:
-
Bronchoalveolar lavage (BAL) samples are far more informative than blood.
-
Blood cultures are usually unhelpful for Aspergillus, as the fungus rarely circulates in the bloodstream.
-
A positive sputum culture may represent colonisation rather than infection, especially in people without severe immune suppression.
This reinforces an important patient message: a single test result is rarely enough.
3. Antifungal treatment can hide infection
Starting antifungal therapy early can:
-
Make cultures negative
-
Reduce antigen levels (e.g. galactomannan)
-
Complicate microscopy interpretation
This explains why some patients experience false reassurance from negative tests after treatment has already begun. Serial testing and clinical judgement are often more informative than a single result.
4. False positives and cross-reactivity are common
The review highlights important pitfalls:
-
β-D-glucan can be positive due to bacterial infections or medical materials, not just fungi
-
Galactomannan can cross-react with other fungi (e.g. Fusarium)
-
Mixed infections can occur in immunosuppressed patients
This supports a cautious interpretation of “positive” results and explains why clinicians may hesitate to diagnose aspergillosis based on one test alone.
5. Colonisation vs infection is a central challenge
A particularly relevant section for aspergillosis patients explains:
-
Aspergillus can live in airways without causing invasive disease
-
Diagnosis relies on combining symptoms, imaging, risk factors, and multiple tests
This reflects the lived experience of many patients with bronchiectasis, asthma, or chronic lung disease.
Strengths of the paper
-
Written by a leading international mycology expert
-
Pragmatic and clinically grounded
-
Explains why guidelines don’t always fit individual patients
-
Particularly strong on Aspergillus diagnostics, including CPA and invasive disease
Limitations
-
Focuses mainly on invasive fungal infections; allergic and chronic syndromes are discussed less
-
Aimed primarily at clinicians and laboratories, not patients
Take-home message for patients
There is no single “definitive” test for aspergillosis. Results depend on immune status, sample type, timing, and prior treatment. Negative tests do not always mean absence of disease, and positive tests do not always mean active infection.
This paper strongly supports the multidisciplinary, experience-based approach used in specialist centres such as the National Aspergillosis Centre.
Aspergillus Updates week 51
1. Immunodeficiency, rare syndromes & aspergillosis risk
Standing Still: A Case of Stiff Person Syndrome and Common Variable Immunodeficiency
Khazar et al., Cureus, 2025
Summary
-
Describes a rare coexistence of Stiff Person Syndrome (SPS) and Common Variable Immunodeficiency (CVID).
-
Highlights autoimmune–immunodeficiency overlap and diagnostic complexity.
Why it matters
-
CVID is a recognised risk factor for recurrent infections and chronic lung disease, including bronchiectasis and chronic pulmonary aspergillosis (CPA).
-
Reinforces the need for multisystem thinking when patients present with neurological and respiratory symptoms.
Limitations
-
Single case; no fungal infection reported.
-
Indirect relevance to aspergillosis but important for risk stratification.
Beyond Cystic Fibrosis: Recognising Shwachman–Diamond Syndrome in the Respiratory Clinic
Yang et al., Respirology Case Reports, 2025
Summary
-
Emphasises misdiagnosis of Shwachman–Diamond syndrome (SDS) as cystic fibrosis.
-
Includes discussion of allergic bronchopulmonary aspergillosis (ABPA) in the differential.
Why it matters
-
Reinforces that non-CF genetic syndromes can present with:
-
Bronchiectasis
-
Recurrent infection
-
ABPA-like features
-
-
Highly relevant to adult respiratory clinics and late diagnoses.
Clinical takeaway
-
ABPA should prompt consideration of underlying immune or genetic disease, not just asthma or CF.
2. Genetics & structural lung disease
Exome sequencing reanalysis identifies a novel CFAP54 variant in primary ciliary dyskinesia
Li et al., Frontiers in Medicine, 2025
Summary
-
Identifies a new likely pathogenic CFAP54 variant.
-
Expands the phenotypic spectrum of Primary Ciliary Dyskinesia (PCD).
Relevance to aspergillosis
-
PCD → impaired mucociliary clearance → chronic infection, bronchiectasis, and secondary fungal disease.
-
ABPA and CPA are increasingly recognised in non-CF bronchiectasis populations.
Strength
-
Genotype–phenotype correlation strengthens diagnostic confidence.
Limitation
-
Aspergillosis not a primary focus, but highly relevant to long-term respiratory outcomes.
3. Haematology, malignancy & invasive aspergillosis
Mixed-Phenotype Acute Leukemia Transforming into AML-M4
Alhayek et al., Cureus, 2025
Summary
-
Case of evolving leukemia complicated by pancytopenia, invasive pulmonary aspergillosis (IPA), and COVID-19.
Key points
-
Illustrates real-world stacked risk:
-
Neutropenia
-
Chemotherapy
-
Viral infection
-
IPA
-
Clinical relevance
-
Strong reminder that IPA often emerges during diagnostic or therapeutic transitions, not just during induction chemotherapy.
Invasive fungal infections in haematologic diseases: evidence, challenges, and practice
Cho et al., Blood Research, 2025 – Review
Summary
-
Comprehensive overview of invasive aspergillosis, candidiasis, and mucormycosis.
-
Covers diagnostics, antifungal resistance, and treatment strategies.
Strengths
-
Practical, guideline-aligned.
-
Emphasises individualised risk assessment and early treatment.
Gap
-
Limited discussion of long-term survivors and post-IPA chronic complications (e.g. CPA).
4. Imaging & diagnostics
CT Pulmonary Angiography in invasive pulmonary aspergillosis
Tian, Future Microbiology, 2025
Summary
-
Explores the role of CT pulmonary angiography (CTPA) in detecting angioinvasion.
Why it matters
-
Vascular occlusion and infarction are hallmarks of IPA.
-
CTPA may improve diagnostic confidence when standard CT is equivocal.
Limitations
-
Case-based evidence.
-
Needs integration into diagnostic algorithms.
Sequential serum galactomannan as an outcome marker
Többen et al., Int J Infect Dis, 2025
Summary
-
Registry-based exploratory analysis of serial galactomannan (GM).
Key finding
-
Trends in GM may correlate with treatment response, not just diagnosis.
Clinical importance
-
Supports GM as a monitoring biomarker, though interpretation remains complex.
Caution
-
Not reliable in all patient groups (e.g. non-neutropenic, antifungal pre-exposure).
5. Chronic pulmonary aspergillosis & structural disease
Molecular epidemiology of Aspergillus species in CPA (South India)
Spruijtenburg et al., Medical Mycology, 2025
Summary
-
Describes species diversity and genetic variation in CPA patients.
Why it matters
-
Highlights:
-
Geographic variation
-
Potential antifungal resistance implications
-
-
Supports species-level identification in CPA.
Strength
-
Strong laboratory–clinical interface.
Advanced pulmonary sarcoidosis
Spagnolo et al., Seminars in Respiratory and Critical Care Medicine, 2025
Summary
-
Reviews complications of advanced sarcoidosis, including:
-
Bronchiectasis
-
Pulmonary hypertension
-
Chronic pulmonary aspergillosis
-
Key point
-
CPA should be actively considered, not viewed as rare, in fibrotic sarcoidosis.
Rezafungin OPAT for chronic pulmonary aspergillosis
Law et al., JAC Antimicrobial Resistance, 2025
Summary
-
First real-world case of rezafungin used via outpatient parenteral therapy for CPA.
-
Includes a health-economic assessment.
Why this is important
-
CPA treatment options are limited.
-
Weekly dosing may:
-
Reduce hospital burden
-
Improve quality of life
-
Caution
-
Single case; echinocandins are not standard CPA therapy.
-
Best viewed as salvage or niche use.
6. Tracheobronchial & atypical aspergillosis
Tracheobronchial Aspergillosis Mimicking Pseudotumour
Castillo Gamboa et al., Clinical Case Reports, 2025
Summary
-
Rare presentation of tracheobronchial aspergillosis masquerading as malignancy.
Clinical lesson
-
Endobronchial disease can be missed or mislabelled.
-
Supports biopsy and fungal testing when appearances are atypical.
7. Immunology, inflammation & host–pathogen interaction
PANoptosis in pathogen infection and systemic disease
Cai et al., Cell Biology and Toxicology, 2025 – Review
Summary
-
Reviews PANoptosis (pyroptosis, apoptosis, necroptosis) in infections.
Relevance
-
Aspergillus is discussed as a trigger of complex inflammatory cell death pathways.
-
May help explain:
-
Severe tissue damage
-
Dysregulated inflammation in IPA
-
Translational value
-
Still mechanistic; clinical applications remain distant.
PD-1 / PD-L1 immune checkpoint in fungal infections
Zheng et al., Virulence, 2025 – Review
Summary
-
Explores immune exhaustion in ABPA, CPA, and IPA.
Key insight
-
Checkpoint pathways may:
-
Contribute to chronic infection persistence
-
Become future adjunctive immunotherapies
-
Important caution
-
Immune checkpoint modulation carries significant risk in fungal disease.
8. Antimicrobial stewardship & prophylaxis
Procalcitonin-guided antibiotics in RSV and influenza
Hessels et al., BMJ Open Respiratory Research, 2025
Finding
-
Reduced antibiotic use without increased fungal infection risk.
Relevance
-
Important reassurance that stewardship does not increase IPA risk in viral respiratory infections.
Letermovir prophylaxis post-HSCT
Kimura et al., J Infect Chemother, 2025
Key result
-
Letermovir did not increase invasive aspergillosis or candidemia risk.
Clinical reassurance
-
Supports ongoing antiviral prophylaxis strategies in transplant patients.
9. Experimental antifungals
Berberine suppresses Aspergillus fumigatus growth
Wang et al., ACS Infectious Diseases, 2025
Summary
-
Demonstrates antifungal activity via:
-
Mitochondrial fragmentation
-
Reactive oxygen species
-
Hog1-MAPK activation
-
-
Reduced fungal burden in a murine IPA model.
Important caution
-
Pre-clinical only.
-
Not a supplement recommendation for patients.
Overall themes & take-home messages
Key trends this week
-
Increasing recognition of rare immunodeficiency and genetic syndromes behind chronic lung disease.
-
Better understanding of non-classical aspergillosis presentations.
-
Strong interest in immune modulation, biomarkers, and novel therapies.
-
Continued need for early diagnosis, especially in haematology and advanced lung disease.
For clinical practice
-
Think beyond labels (asthma, CF, cancer).
-
Revisit diagnoses when disease behaves atypically.
-
CPA and ABPA remain under-recognised but increasingly documented across conditions.
If you’d like, I can:
-
Turn this into a NAC weekly research digest
-
Produce patient-safe summaries of selected papers
-
Extract figures and learning points for teaching or the Knowledge Hub
Aspergillosis Trust – A Community for Patients
The Aspergillosis Trust is a patient-led charity dedicated to helping people affected by aspergillosis and supporting the wider community of patients, carers, families, and friends. It exists to make life with aspergillosis easier by *raising awareness, sharing information, and bringing people together so no one has to go through this alone. *Aspergillosis Trust Charity
Although aspergillosis is a rare condition, the Trust’s vision is simple and powerful: to make aspergillosis widely recognised so it can be diagnosed earlier, treated more effectively, and better understood — by health professionals and the general public alike.
Why the Trust Matters to You
Shared Experience and Support
The Aspergillosis Trust understands what it’s like to live with a rare lung condition because it’s run by patients and carers themselves. This means the insights and support it offers come from real experience, not just medical textbooks. It connects people who have walked similar paths, helping reduce isolation and fostering practical encouragement.
Information You Can Use
The Trust supports people around the world by providing information, resources, and real and virtual support networks. Whether you’re newly diagnosed or navigating long-term treatment, the Trust’s curated links, articles, and connections can help you find reliable answers and understand your options.Charity Commission
Raising Awareness and Understanding
By amplifying patient voices and sharing stories, the Trust helps increase understanding of aspergillosis among doctors, nurses, and healthcare teams. This awareness work helps ensure more people are referred for specialist care sooner, leading to better outcomes.
Where Community Meets Practical Help
-
The Trust offers a network of support and encouragement for people living with aspergillosis.
-
It provides curated links and resources to help you find information relevant to your situation.
-
Through awareness campaigns and shared patient stories, it works to improve understanding and recognition of aspergillosis among clinicians and the public.
Whether you’re looking for knowledge, community, or reassurance that others understand what you’re going through, the Aspergillosis Trust is a valuable companion on your journey.
For more about how to connect or get support, you can visit their website or reach out directly via their contact page.
Why Exposure to Aspergillus (e.g., in a Damp Home) Does Not Usually Mean You Have Aspergillosis
Many people worry that finding mould in a home means they are at serious risk of aspergillosis. This fear is understandable, especially when you have respiratory symptoms. But the truth is:
Exposure to Aspergillus is extremely common, and aspergillosis is rare.
Here’s why most people who encounter Aspergillus never develop disease — and what to look out for if you are at risk.
1. Aspergillus Is Everywhere — Even in Healthy Homes
Aspergillus spores are naturally present in the environment. We breathe them in every day from:
-
Soil, leaves, compost
-
Outdoor air
-
Dust and ventilation systems
-
Older or damp buildings
These spores are so widespread that avoiding them completely is impossible.
The good news is:
For most people, breathing in Aspergillus spores does not cause illness.
The airways and immune system are excellent at clearing them quickly and safely.
2. Damp Homes Increase Exposure — Not Disease
A damp or mouldy home may contain higher levels of spores, but this generally causes:
-
Irritation of the airways
-
Worsening of asthma or allergies
-
Coughing or wheezing
-
Musty smells and reduced air quality
These symptoms can feel unpleasant, but damp housing does not usually cause aspergillosis.
Most health effects of damp homes are related to allergens and irritants, not fungal disease.
3. Aspergillosis Develops Only in Vulnerable People
To develop aspergillosis, a person usually needs underlying risk factors such as:
-
Asthma, bronchiectasis, COPD, or previous TB
-
Weakened immune system
(e.g., due to chemotherapy, high-dose steroids, immunosuppressants) -
A strong allergic tendency (as in Allergic Bronchopulmonary Aspergillosis — ABPA)
Even among these groups, only a minority develop disease.
Exposure alone is not enough.
4. Why Some People Think Exposure “Caused” Their Illness
For people who later develop ABPA or chronic aspergillosis, a first major flare often follows:
-
Living in a damp home
-
Decorating or renovating
-
Gardening or composting
-
Clearing mould or dust
This can give the impression the exposure caused the disease.
In reality:
Exposure usually triggers or reveals an underlying condition — it does not create it.
Underlying immune or lung problems were already present long before the flare.
5. When to Seek Medical Review
See a doctor if you have:
-
A chronic wet cough
-
Mucus plugging
-
Breathlessness that gets worse over months
-
Coughing up blood
-
Repeated chest infections
-
Worsening asthma control
-
Unexplained weight loss
These may indicate ABPA, chronic pulmonary aspergillosis (CPA), or other lung disease.
6. Environmental Improvements Can Still Help
If you have ABPA, CPA, or asthma, improving home conditions can reduce flare-ups:
-
Lower humidity (40–60%)
-
Improve ventilation
-
Repair damp or leaks
-
Use HEPA air filtration
-
Clean or replace old soft furnishings if heavily contaminated
These steps reduce asthma triggers and airway irritation — not because they “remove Aspergillus entirely”, but because they create a healthier breathing environment.
Key Message
Exposure to Aspergillus is normal.
Disease is uncommon and depends on underlying health — not on exposure alone.
Damp homes can trigger symptoms but rarely cause aspergillosis.