Diagnosis
[et_pb_section fb_built="1" _builder_version="4.19.1" _module_preset="default" custom_margin="|-66px||1px||" custom_padding="0px||3px|0px||" hover_enabled="0" global_colors_info="{}" theme_builder_area="post_content" width="100%" sticky_enabled="0"][et_pb_row _builder_version="4.19.1" _module_preset="default" global_colors_info="{}" theme_builder_area="post_content"][et_pb_column type="4_4" _builder_version="4.19.1" _module_preset="default" global_colors_info="{}" theme_builder_area="post_content"][et_pb_text _builder_version="4.19.1" _module_preset="default" global_colors_info="{}" theme_builder_area="post_content"]
Accurate diagnosis has never been straightforward for aspergillosis, but modern tools are being developed rapidly and are now improving the speed and accuracy of diagnosis. A patient presenting at the clinic will first be asked to give a history of the symptoms that they have noticed. Depending on this history a number of tests may be requested from the following list:
- A blood test
- X-rays or CT scan of the chest
- A skin test to measure sensitivity to Aspergillus allergens
- Culture and analysis of a sputum (mucus) sample
- Culture of tissue fluids e.g. lung fluid (called BAL)
- A bronchoscopy – where a flexible tube is passed down into the lungs while under sedation.
- A sample or biopsy of a tissue mass (if present) in a lung cavity
[/et_pb_text][et_pb_divider color="#000000" divider_style="dotted" _builder_version="4.19.1" _module_preset="default" width="80%" module_alignment="center" global_colors_info="{}" theme_builder_area="post_content"][/et_pb_divider][et_pb_text _builder_version="4.19.1" _module_preset="default" global_colors_info="{}" theme_builder_area="post_content"]
What do the tests show?
Blood tests: Antibodies against Aspergillus proteins can be measured in a patient’s blood and this indicates if the patient may have an Aspergillus infection – this is done using an enzyme-linked immunosorbent assay (ELISA), such as the ImmunoCAP® Specific IgE Blood Test.. A positive result means that antibodies to the fungus have been detected. A positive test result is also a useful marker for later comparisons to assess efficiency of treatment. Occasionally a false positive result may occur which is why a number of different tests are used in diagnosing aspergillosis. Sometimes markers of allergy to Aspergillus are positive in the blood. A test for a particular fungal molecule sometimes found in the blood – called the galactomannan test may also be carried out on a blood sample.
Other tests include blood count, plasma viscosity and C-reactive protein, which may indicate inflammation – such markers usually improve on treatment so a baseline level is helpful. Liver and kidney function tests are important as liver function can be abnormal on antifungal drugs. Also, some aspergillosis patients may have low levels of a substance called mannose binding lectin (MBL) and display abnormal genes for this protein.
A chest X-ray allows visualisation of the inside of the lungs and may identify an abnormality such as any lung cavities – formed as a result of another underlying disease or infection, or if a fungal ball (aspergilloma) is present. A more advanced cross sectional picture of the lungs may be needed, in which case computer tomography (CT) might be necessary. The procedure relies on X-rays to produce a detailed image. You will need to lie still on a narrow table, which slides into the centre of the CT scanner where the X-rays rotate around you. A scan normally takes only a few minutes.
A skin test where a small needle is used to scratch the surface of the skin can be used to detect whether a patient has circulating IgE antibodies specific for Aspergillus. This is a more common test if you have asthma or ABPA. A positive result indicates that the patient is sensitised to Aspergillus. See immune system.
A sample of sputum, other tissue fluids or tissue biopsies may be sent to the laboratory to be cultured, in order to see if it is possible to grow Aspergillus from the sample. Scientists use a special culture plate to grow moulds, and if any does grow they often use a microscope to confirm the type of mould. Another way of detecting Aspergillus is with a sensitive molecular testing method.
A bronchoscopy is a procedure where a flexible tube is passed into the lungs to view the lung and airways – the patient is sedated during the procedure. Samples of the lung tissue or fluids can be biopsied through the bronchoscope for examination in the laboratory by culture and molecular tests, if needed. See more.
Biopsies are small samples of tissue taken from infected areas (e.g. lung, sinus) that are either sliced thinly, stained and examined under a microscope, or are placed on nutrient media that allows any fungus present to grow – the fungus can then be identified.
The results of the above tests are then considered together and if aspergillosis is confirmed a suitable treatment regime will be started.
[/et_pb_text][et_pb_divider color="#000000" divider_style="dotted" _builder_version="4.19.1" _module_preset="default" width="80%" module_alignment="center" custom_margin="7px||11px|||" custom_padding="9px|||||" global_colors_info="{}" theme_builder_area="post_content"][/et_pb_divider][et_pb_text _builder_version="4.19.1" _module_preset="default" global_colors_info="{}" theme_builder_area="post_content"]
Symptoms:
Symptoms can be widely different depending on the type of aspergillosis that a patient may have. For instance one patient with an aspergilloma may have few symptoms or just a cough, another may cough up large quantities of blood (haemoptysis) and require urgent medical attention The following is a general list of some of the symptoms which aspergillosis patients can experience – but there is a large variation between patients.
- weight loss
- fatigue
- fever
- cough
- coughing blood (haemoptysis)
- breathlessness
A patient with some of these symptoms may not have aspergillosis – in fact it is unlikely, unless the person has a poor immune system (eg. following cancer therapy, organ transplantation). If a person has not responded to several doses of antibiotics and has a weakened immune system then tests for aspergillosis should be considered.
[/et_pb_text][/et_pb_column][/et_pb_row][/et_pb_section]
Loneliness and Aspergillosis
[et_pb_section fb_built="1" _builder_version="4.19.1" _module_preset="default" custom_padding="0px||0px|8px||" global_colors_info="{}" theme_builder_area="post_content" custom_margin="|59px||42px||"][et_pb_row _builder_version="4.19.1" _module_preset="default" custom_margin="50px|auto|50px|30px|true|false" global_colors_info="{}" theme_builder_area="post_content"][et_pb_column type="4_4" _builder_version="4.19.1" _module_preset="default" global_colors_info="{}" theme_builder_area="post_content"][et_pb_text _builder_version="4.19.1" _module_preset="default" custom_margin="|-124px||||" custom_padding="|0px||||" global_colors_info="{}" theme_builder_area="post_content"]
Believe it or not, loneliness is as bad for your health as obesity, air pollution or physical inactivity. Some studies put loneliness as equivalent to smoking 15 cigarettes per day.
In a recent poll in our Facebook patient group for people with chronic forms of aspergillosis 40% stated that they were lonely more than once per week and 75% of those stated that they were lonely every day. In total 73% recorded loneliness at least occasionally.
We also asked people who care for aspergillosis patients the same questions and this time 56% stated that they were lonely more than once per week, with 78% lonely at least occasionally.
Give those two poll results, are people lonely because they have a chronic illness that might restrict their socialising, and are they lonely because they look after someone with a chronic illness?
The level of loneliness in the general population in the UK is currently at 45%, so there are clearly more people who are lonely in both groups affected by aspergillosis (73% and 78%). Furthermore, 30% of those people who have chronic aspergillosis in our poll were lonely every day, which compares poorly with national statistics that show the number of people in the general population who are lonely as frequently as every day is only 5%.
Conclusion: There are six times as many people with chronic aspergillosis that are lonely every day compared with the general UK population!
Loneliness is clearly a big problem for people who either have chronic aspergillosis or care for someone with chronic aspergillosis.
What can we do about this?
Firstly, awareness of the problem is a big step forward. Awareness of its far-reaching consequences for our mental and physical health may provide some incentive to take action to try to change things. The campaign to end Loneliness (https://www.campaigntoendloneliness.org/the-facts-on-loneliness/) has found that those affected can be of all ages/genders/able or disabled/chronically ill or not and they aim to inspire everyone to connect and communities to come together to help. Nobody should be without company who wants it.
They also provide a lot of useful hints and tips on how to reduce your loneliness (https://www.campaigntoendloneliness.org/feeling-lonely/ ), how to connect with others a bit better, and reduce your health risks – if nothing else at the moment we all could do with getting together to keep warm! Regardless of why you feel lonely, we can all find a way to make connections no matter how fleeting – they all count.
Here at the National Aspergillosis Centre we hold weekly meetings for all patients both here in the UK and abroad
Zoom meetings are a casual and fun way to chat with fellow aspergillosis travelers and NAC staff (Tuesdays 2-3pm GMT and Thursdays 10 – 11am GMT) in which you can just sit and listen to us all chatting for an hour – all you need is a smartphone/tablet/laptop to join us.
The meetings are private so we do not give instructions on how to join on a public page such as this. For directions on how to get involved join one of the following groups and we will get back to you:
Of course some people are entirely happy on their own
[/et_pb_text][/et_pb_column][/et_pb_row][/et_pb_section]
Doing a disability assessment
[et_pb_section fb_built="1" _builder_version="4.19.1" _module_preset="default" global_colors_info="{}" theme_builder_area="post_content"][et_pb_row _builder_version="4.19.1" _module_preset="default" global_colors_info="{}" theme_builder_area="post_content"][et_pb_column type="4_4" _builder_version="4.19.1" _module_preset="default" global_colors_info="{}" theme_builder_area="post_content"][et_pb_text _builder_version="4.19.1" _module_preset="default" global_colors_info="{}" theme_builder_area="post_content"]
In order to claim government help for living with a disability you will have to complete a disability assessment. This can be a stressful and demanding experience, so we have gathered some helpful tips from those who have already been through the process.

Keep all of your medical records and letters and make sure you have access to online records and appointments. On the day of the interview, take a copy of all the paperwork with you, so you can refer to it if needed.
Try and keep a diary of all of your symptoms and the effects that they have on your life for a few months before your assessment. Symptoms that may have become routine for you are still severe and need to be mentioned. “Mention every little niggle”.
Speak to Citizens Advice, or the equivalent in other countries, as they are experienced in navigating the large amounts of paperwork and helping you prepare for the interview. Often people are in a difficult emotional state when trying to fill in assessments, and having the support from a third party is a big help.
When asked about your symptoms and how your condition affects your life, think about how you are on your worst days. A ‘good’ day to you almost certainly still involves many wearing symptoms, so make sure you don’t accidentally gloss over anything.
If you’re in the UK, look at subscribing to the Benefits and Work website. They have guides to applying for UK disability benefits, and some of our patients have found their diary templates and wording examples very useful.
Look or ask for tips from others on the Aspergillosis Facebook support group. Also join groups such as The ESA DLA UC & PIP Survival Guide, or the equivalent in other countries.
If you don’t get all you need from your first interview, appeal. Some departments have targets to reach for the first interview, but on appeal you may be more likely to succeed. Even if that’s not the case, you will be better prepared the second time around.
Ensuring aspergillosis is recognised as a severe health condition: As aspergillosis is such a rare condition, those drawing up disability guidelines may not be familiar with the disease. The more people know about aspergillosis, the better! The best way to do this in the UK is to get in touch with your local MP and ask them to check with the Minister of State for Disabled People, Health and Work, to ensure that aspergillosis is included as a long-term, incurable, debilitating condition. Refer your MP to the National Aspergillosis Centre for more information. The more people advocating for aspergillosis patients, the more well-known and understood a condition it will become.
For more information:
Last Updated on June 19, 2019
[/et_pb_text][/et_pb_column][/et_pb_row][/et_pb_section]
Finding an advocate
[et_pb_section fb_built="1" _builder_version="4.19.1" _module_preset="default" width="100%" custom_padding="3px|0px|1px|||" hover_enabled="0" global_colors_info="{}" theme_builder_area="post_content" sticky_enabled="0"][et_pb_row _builder_version="4.19.1" _module_preset="default" custom_padding="22px|2px|22px|2px|true|true" global_colors_info="{}" theme_builder_area="post_content"][et_pb_column type="4_4" _builder_version="4.19.1" _module_preset="default" global_colors_info="{}" theme_builder_area="post_content"][et_pb_text _builder_version="4.19.1" _module_preset="default" global_colors_info="{}" theme_builder_area="post_content"]
If you have concerns with how your condition is being managed, or any questions about aspergillosis and its treatment, you may find yourself needing speak up on behalf of yourself. Most people will be able to do this for themselves, or with help from family and friends, but some may need an independent advocate to help them express their wishes and make informed decisions about their condition. Here are our tips for advocating for yourself, or finding an independent advocate.

Phone your consultant’s secretary or a specialist respiratory nurse from your team (emails sometimes get buried). Use Relay if you struggle with hearing.
Contact the Patient Advice and Liaison Service (PALS) team at your local hospital. PALS will be able to help you answer questions and resolve any concerns you have about your healthcare.
Get in touch with an advocate via your local council or a disability organisation such as VoiceAbility.
Keep pushing until you get what you need.
For more information, see the NHS advice on getting someone to speak up for you
[/et_pb_text][/et_pb_column][/et_pb_row][/et_pb_section]
Managing breathlessness
[et_pb_section fb_built="1" _builder_version="4.19.1" _module_preset="default" global_colors_info="{}" theme_builder_area="post_content"][et_pb_row _builder_version="4.19.1" _module_preset="default" custom_margin="4px|auto|4px|auto|true|false" global_colors_info="{}" theme_builder_area="post_content"][et_pb_column type="4_4" _builder_version="4.19.1" _module_preset="default" global_colors_info="{}" theme_builder_area="post_content"][et_pb_text _builder_version="4.19.1" _module_preset="default" hover_enabled="0" global_colors_info="{}" theme_builder_area="post_content" sticky_enabled="0"]
Breathlessness
Breathlessness is simply defined as ‘feeling that you are out of breath’, and most of us are familiar with that sensation when we once ran around as children or in later years climbing hills or rushing for a bus. In this context it is of course a completely normal reaction to exertion and we are comfortable with it because we can control it.
However when we feel breathless and we haven’t exerted ourselves it is very different matter. We no longer feel in control and one result is that our anxiety levels rise. Once we start getting anxious the feeling can spiral to panic, which will only make things worse as this itself can cause breathlessness. It is much easier to breath if we keep as calm as possible.
Breathlessness can come on suddenly (as an acute attack) or gradually. It can stay for a long time and become a chronic condition. In order to avoid excessive anxiety it is important that the people affected (patients and carer) are put back into control of the situation, and that is what your doctor will do. It is therefore important that you inform your doctor about any unexpected bouts of breathlessness. (NB your doctor refers to breathlessness as dyspnoea).
Causes
Acute attack
A sudden attack will require you to see a doctor quickly, as it often requires immediate treatment. People who have asthma, chronic obstructive pulmonary disease (COPD) or heart failure are usually well prepared by their doctors, with an action plan that includes starting treatment before the clinician arrives. If it is new to you seek medical assistance without delay.
In a group of people who have aspergillosis, there is often asthma, COPD and infection (pneumonia and bronchitis) to consider. The British Lung Foundation list the following common causes:
- A flare-up of asthma: You might feel your chest is tight or feel you are wheezing rather than being short of breath.
- A flare-up of COPD: You might feel more out of breath and tired than normal and your usual ways to control your breathlessness don’t work so well.
- A pulmonary embolism. This is when you have clots in your lung arteries that have travelled from other parts of your body, usually your legs or arms. These clots can be very small and cause acute breathlessness. More clots can get released over a long time and cause your feeling of breathlessness to get worse, and eventually you might have daily long-term breathlessness.
- Lung infections such as pneumonia and bronchitis.
- Pneumothorax (also called collapsed lung)
- Pulmonary oedema or effusion or fluid in your lungs. This might be due to the failure of your heart to pump fluid around efficiently or due to liver disease, cancer or infection. It can also cause long-term breathlessness, but this can be reversed once the cause is known.
- A heart attack (also called a coronary artery thrombosis)
- Cardiac arrhythmia. This is an abnormal heart rhythm. You might feel your heart misses beats or you might experience palpitations.
- Hyperventilation or a panic attack.
Long term (chronic) breathlessness
Chronic breathlessness is usually a symptom of an underlying chronic condition such as asthma, Allergic Bronchopulmonary Aspergillosis (ABPA), Chronic Pulmonary Aspergillosis (CPA), obesity and more. The British Lung Foundation list the following common causes:
- Chronic obstructive pulmonary disease (COPD)
- Heart failure. This can be due to problems with the rhythm, valves or cardiac muscles of your heart.
- Interstitial lung disease (ILD), including idiopathic pulmonary fibrosis (IPF). These are conditions where inflammation or scar tissue builds up in your lungs.
- Allergic alveolitis, which is an allergic lung reaction to certain dusts you breathe in.
- Industrial or occupational lung diseases such as asbestosis, which is caused by being exposed to asbestos.
- Bronchiectasis. This is when your bronchial tubes are scarred and distorted leading to a build-up of phlegm and chronic coughing.
- Muscular dystrophy or myasthenia gravis, which causes muscle weakness.
- Anaemia and kidney disease.
- Being obese, lacking fitness, and feeling anxious or depressed can also cause you to feel short of breath. You might often have these issues alongside other conditions. Treating them is a vital part of treating your breathlessness.
Diagnosing breathlessness
Your doctor will want to discover what is causing your breathlessness and, as you can see above, there are many possibilities so diagnosis can take some time. In a group of people with aspergillosis the list is much shorter but your doctor will still need to be sure he has found the correct cause. There are several useful tips on the BLF website for people going to see their doctor for the first time with breathlessness, including recording the sorts of activity that make you breathless on a phone with a camera and showing the recordings to your doctor.
NOTE if you are a chronic breathlessness patient you will sometimes be asked to score your level of breathlessness from 1-5 by using this scale:
| Grade | Degree of breathlessness related to activities |
| 1 | Not troubled by breathlessness except on strenuous exercise |
| 2 | Short of breath when hurrying on the level or walking up a slight hill |
| 3 | Walks slower than most people on the level, stops after a mile or so, or stops after 15 minutes walking at own pace |
| 4 | Stops for breath after walking about 100 yards or after a few minutes on level ground |
| 5 | Too breathless to leave the house, or breathless when undressing |
Managing Breathlessness
Once the cause of your breathlessness has been established, you and your doctor can work together to get control of your breathing back. Things you can do include (from BLF website):
- If you smoke, get help to quit. There is very good evidence that seeing someone who is trained to help people stop smoking, as well as taking regular nicotine replacement and/or anti-craving medicines, increases your chance of being a long-term non-smoker.
- Get a flu jab every year.
- Try some breathing techniques. There are various techniques that you can use to help you control your breathing. If you practise these and use them every day, they will help you when you are active and getting breathless. They will also help you manage if you get short of breath suddenly. Some examples are:
– Blow as you go: breathe out when you are making a big effort, such as standing up, stretching or bending.
– Pursed-lips breathing: breathe out with your lips pursed as if you were whistling. - Be more physically active. Physical activity could be walking, gardening, walking the dog, housework or swimming as well as going to a gym. Read the NHS guide on seated exercising.
- If you have a lung condition, you can be referred to a pulmonary rehabilitation (PR) programme by your doctor, and if you have a heart problem there are cardiac rehabilitation services too. These classes help you to get control over your breathlessness, get you fitter and are also lots of fun.
If you are breathless due to loss of fitness, ask your GP or practice nurse about local referral schemes that support people who want to be more active. - Drink and eat healthily and manage your weight. Your doctor can help you work out what your healthy weight should be. If you are carrying excess weight you will require more effort to breathe and move around, and it will be more difficult to get control over your feelings of breathlessness.
If you have diabetes, ask about educational events to help you to manage your weight and eat a more balanced diet. Your GP or practice nurse can help you to find healthy eating support services. - Get treatment if you feel stressed or anxious. If your area doesn’t have a dedicated breathlessness clinic that provides this help, ask your GP to refer you to a counsellor or clinical psychologist who will be able to help. Sometimes medicines can help too, so talk to your GP about this.
- Use the right medication in the right way.- Some breathlessness is treated with inhalers. If you have an inhaler make sure somebody regularly checks you know how to use it correctly. Don’t be afraid to ask to try different types if you can’t get on with the one you have. Use them as they have been prescribed to you. Ask your doctor or nurse for a written description of how to manage your lung condition.
- If you take tablets, capsules or liquids to control your breathing make sure you know why you are taking them and ask your health care professional or pharmacist if you don’t. If your breathlessness is due to heart failure you might need to adjust your treatment according to your weight and how much your ankles swell. Make sure you that have a written plan that you understand.
- If you have COPD, you might have a rescue pack so you can start treatment early if you have a flare-up. This must always come with a written action plan that you understand and agree with.
Can oxygen help?
Evidence shows that oxygen will not help your breathlessness if your blood oxygen levels are normal. But if you have a condition that means that the level of oxygen in your blood is low, oxygen treatment can make you feel better and live longer.
Your GP can refer you for advice and tests. You should see a specialist team to assess your needs and ensure you use oxygen safely. They will monitor your use of oxygen and change your prescription as your needs change. Never use oxygen without specialist advice.
Further information:
[/et_pb_text][/et_pb_column][/et_pb_row][/et_pb_section]
Sex and breathlessness
[et_pb_section fb_built="1" _builder_version="4.19.1" _module_preset="default" custom_padding="0px|||0px||" global_colors_info="{}" theme_builder_area="post_content"][et_pb_row _builder_version="4.19.1" _module_preset="default" custom_margin="4px|auto|4px|auto|true|false" custom_padding="40px|4px|13px|4px|false|true" global_colors_info="{}" theme_builder_area="post_content"][et_pb_column type="4_4" _builder_version="4.19.1" _module_preset="default" global_colors_info="{}" theme_builder_area="post_content"][et_pb_text _builder_version="4.21.0" _module_preset="default" hover_enabled="0" global_colors_info="{}" theme_builder_area="post_content" sticky_enabled="0"]
Breathlessness is often a major feature of pulmonary aspergillosis and we provide instructions on how to regain control over breathlessness on another page of this website.
Sadly breathlessness leaves many of its patients highly anxious about any exertion that may bring on the sensation of losing control again. This is a problem as exercise is a very good way to help relieve breathlessness and is one way we manage living with it.
Not surprisingly this can also have a major impact on the enjoyment of sex, as sex often involves significant exertion! Thankfully the British Lung Foundation offer detailed support to help people concerned with enjoying a full sex life while having a chronic lung condition and we replicate their work here:
Sex is an important part of life for many people, and this doesn’t have to change because you or your partner has a lung condition. It’s normal to worry about getting tired or out of breath. However, both you and your partner should take responsibility for your sexual relationship, so it’s important to talk to each other about your concerns and wishes and remain open-minded
How much energy will I need?
Sexual activity, including intercourse, oral sex and masturbation, requires energy. As with all physical activity, you will need to use your heart, lungs and muscles.
You might need to breathe more frequently and your heart rate and blood pressure might go up for a short time. This is the same for everyone. They return to normal levels quickly, so don’t worry if this happens. The energy you use during orgasm is similar to the energy needed to climb stairs or take a brisk walk.
Remember that some changes in your sex life are just part of getting older and not because of your lung condition. Slower erections and delayed orgasms are normal in middle age and later life.
There are a number of ways to be intimate with your partner that are less physically demanding, including hugging and touching.
When is the best time to have sex?
Have sex when you feel rested and your breathing feels comfortable. This is likely to be when your medication is most effective and your energy levels are not too low, so you may need to plan ahead. However, don’t change your normal habits if this is stressful for you or your partner
Be comfortable and relaxed. If you are too cold or too hot, you won’t be relaxed. If you’re feeling stressed or tired, having sex could intensify these feelings. All of this could make your breathing more difficult. It’s also advisable to avoid sexual activity after a heavy meal or drinking alcohol. Your breathing might be more strained if you have a full stomach and feel bloated. Alcohol can decrease your sexual function and make it more difficult for men to get an erection. This could make you or your partner more anxious.
How can I prepare for having sex?
You might want to try coughing up phlegm before you have sex, or avoid having sex in the morning when many people cough up more phlegm.
If you use an inhaler to open up your airways, called a bronchodilator, try taking one or two puffs before starting sexual activity as this may relieve shortness of breath and wheezing during sex.
Some people also find that oxygen increases stamina. If you use oxygen at home, using it before sexual activity might help to prevent you from getting short of breath.
How will my treatment affect my sex life?
Some medications can cause a decline in your sex drive or sexual function. If this is a problem for you, talk to your GP, respiratory nurse or health care professional for advice.
Using a steroid inhaler or taking steroids through a nebuliser can cause oral thrush, a type of infection in the mouth. This might make you feel less inclined to have sex or be intimate. It’s a good idea to speak to your GP, respiratory nurse or health care professional if you get a lot of thrush infections.
Some medications, such as antibiotics, might also increase the risk of genital thrush. It’s important to make sure thrush infections are properly treated, and avoid having sex until the infection has cleared up.
Oxygen treatment
If you use oxygen at home, you might find that you feel self-conscious or uncomfortable using it during sexual activity. However, it is perfectly safe to have sex while using oxygen, so talk to your partner about your concerns.
Oxygen can be delivered through a tube attached to a face mask, but if you need to use oxygen while having sex you might feel more comfortable using a nasal cannula (two very small plastic tubes that are placed into each nostril, enabling you to breathe the oxygen in through your nose).
If you have been advised to use a different setting of oxygen for activity, make sure you use the oxygen at this level during sexual activity too.
Non-invasive ventilation
Many people who use non-invasive ventilation (NIV) overnight to help them to breathe find that it affects sexual activity. However, it is perfectly safe to have sex and to be intimate while on NIV, so there is no reason why you can’t use your ventilator during sexual activity if it is suitable for you and your partner.
What if I get short of breath during sex?
All types of physical activity, including sex, can cause you to become slightly out of breath. This is nothing to be worried about, and your breathing will return to normal. Trying to relax will help.
If you become very short of breath during sex, try pausing to take some slow, deep breaths. Your GP, respiratory nurse or health care professional should be able to advise you about breathing techniques to manage your breathlessness. These often have the added benefit of helping you to relax.
As with any activity, taking regular and frequent rests can also be helpful. For example, try changing positions or taking turns with sexual activity. You should also stop to take your reliever inhaler if you need to.
Sexual positions
It’s important to keep your diaphragm free and avoid weighing down on your chest. You might find it more comfortable to use positions that need less energy to maintain. Here are some suggestions for both heterosexual and same-sex couples:
British Lung Foundation
[/et_pb_text][et_pb_image src="https://aspergillosis.org/wp-content/uploads/2023/02/sex_and_breathlessness_positions_BLF.jpg" title_text="sex_and_breathlessness_positions_BLF" _builder_version="4.19.5" _module_preset="default" global_colors_info="{}" theme_builder_area="post_content"][/et_pb_image][et_pb_text _builder_version="4.19.5" _module_preset="default" global_colors_info="{}" theme_builder_area="post_content"]
Try both partners lying on their sides, either facing each other (example 1) or with one partner behind the other (example 2).
If you prefer one partner being on top, it might be better for the partner who has a lung condition to take the lower position, as it tends to require less activity. It’s important that the person on top doesn’t press down on their partner’s chest (example 3).
You could try one partner kneeling on the floor, bending over with their chest resting on the bed (example 4).
One partner sitting on the edge of the bed with their feet on the floor, with the other kneeling on the floor in front, might be comfortable (example 5).
Finally, remember that holding each other, hugging, kissing and caressing can also be fulfilling expressions of love and affection, and require less energy (example 6).
All forms of intimacy should be enjoyable and fun, so having a sense of humour and being able to laugh with your partner will help. Talking about any difficulties either you or your partner is experiencing is also important. Be prepared to try different ways to express your affection and tell each other what feels good.
Read the full BLF article complete with downloadable leaflets
[/et_pb_text][/et_pb_column][/et_pb_row][/et_pb_section]
Managing Chronic Pain
[et_pb_section fb_built="1" _builder_version="4.19.1" _module_preset="default" custom_padding="3px|||2px||" global_colors_info="{}" theme_builder_area="post_content"][et_pb_row column_structure="3_5,2_5" _builder_version="4.21.0" _module_preset="default" custom_margin="45px|auto|5px|auto|false|false" global_colors_info="{}" theme_builder_area="post_content"][et_pb_column type="3_5" _builder_version="4.21.0" _module_preset="default" global_colors_info="{}" theme_builder_area="post_content"][et_pb_text _builder_version="4.21.0" _module_preset="default" custom_margin="|-51px||||" custom_padding="|41px||||" global_colors_info="{}" theme_builder_area="post_content"]
Chronic pain is common amongst people with chronic respiratory diseases, and also amongst their carers; in fact it is one of the most common reasons for both to visit the doctor. At one time your doctor’s response might have been simple – check that the cause of the pain should clear up with intervention and then prescribe painkiller drugs to help the patient cope with the short period of pain. If the predicted period of pain is not going to be short they might continue to give you painkillers, but after a certain point we know that two things start to happen:
- The painkillers will start giving you side effects, some of which can be serious (eg. depression). The longer you are on the painkillers, and the higher the dose, the worse this can get.
- Some painkillers – especially those used to treat severe pain – start to lose their effectiveness if given over several weeks
[/et_pb_text][/et_pb_column][et_pb_column type="2_5" _builder_version="4.21.0" _module_preset="default" global_colors_info="{}" theme_builder_area="post_content"][et_pb_image src="https://aspergillosis.org/wp-content/uploads/2023/05/managechronpain.jpg" title_text="managechronpain" align="right" _builder_version="4.21.0" _module_preset="default" custom_margin="|||-15px||" global_colors_info="{}" theme_builder_area="post_content"][/et_pb_image][/et_pb_column][/et_pb_row][et_pb_row _builder_version="4.21.0" _module_preset="default" custom_margin="12px|auto|8px|auto|false|false" global_colors_info="{}" theme_builder_area="post_content"][et_pb_column type="4_4" _builder_version="4.21.0" _module_preset="default" global_colors_info="{}" theme_builder_area="post_content"][et_pb_text _builder_version="4.21.0" _module_preset="default" global_colors_info="{}" theme_builder_area="post_content"]
Nowadays doctors are more likely to try and encourage patients to remain active, to remain at work and, depending on the source of the pain, might well recommend strengthening exercises (improved muscle tone and strength case help support a painful joint). This also helps the patient to socialise, reduces anxiety and the risk of depression, and can even reduce the pain itself.
But wait! You might ask: Won’t moving a painful joint cause more damage and therefore more pain? If done under medical supervision this is unlikely, and overall the pain usually improves and the dose of painkillers is reduced.
Find out more at: NHS – Managing chronic pain
[/et_pb_text][/et_pb_column][/et_pb_row][et_pb_row _builder_version="4.19.1" _module_preset="default" custom_margin="16px|auto|-5px|auto|false|false" custom_padding="31px|4px|40px|4px|false|true" global_colors_info="{}" theme_builder_area="post_content"][et_pb_column type="4_4" _builder_version="4.19.1" _module_preset="default" global_colors_info="{}" theme_builder_area="post_content"][et_pb_text _builder_version="4.21.0" _module_preset="default" global_colors_info="{}" theme_builder_area="post_content"]
But what about the chest pain often experienced by people with respiratory illness?
Firstly it is important to stress that all chest pain needs to be examined by a doctor as there are several possible causes and some causes need immediate attention e.g. heart attack!
Some chest pain comes from sore bones, muscles and joints so, as we cannot avoid moving our chests during breathing, we tend to reduce movement for a while and take painkillers until the pain is reduced. But, just as written above, your doctor may start to use a variety of approaches to keep your chest moving, build up the muscles to help prevent future pain, and reduce painkiller dose – the same as with any other joint pain.
Find out more at: NHS Chest pain
How can I reduce my dose of painkillers?
There are several techniques that will help you feel more in control of the amount of pain you are in – some are mentioned in the above link, managing chronic pain. Several exploit a little known fact about pain, which most of us will take some convincing of. Our pain is not generated by injury, it is generated by our brains as a defensive mechanism. That suggests that the amount of pain we feel is not inevitable, we might be able to control it a little by using our brains!
Not convinced? Try watching this video recommended by one of our patients, which helped her understand that we can do something to reduce our pain, and possibly even reduce our dose of painkillers.
[/et_pb_text][et_pb_video src="https://www.youtube.com/watch?v=5p6sbi_0lLc" _builder_version="4.19.1" _module_preset="default" global_colors_info="{}" theme_builder_area="post_content"][/et_pb_video][/et_pb_column][/et_pb_row][/et_pb_section]
Recognising and avoiding depression
[et_pb_section fb_built="1" _builder_version="4.19.1" _module_preset="default" custom_margin="-32px|||||" custom_padding="28px|||0px||" global_colors_info="{}" theme_builder_area="post_content"][et_pb_row _builder_version="4.19.1" _module_preset="default" custom_padding="3px|3px|3px|3px|true|true" global_colors_info="{}" theme_builder_area="post_content"][et_pb_column type="4_4" _builder_version="4.19.1" _module_preset="default" global_colors_info="{}" theme_builder_area="post_content"][et_pb_text _builder_version="4.19.1" _module_preset="default" custom_margin="|-50px||-54px||" global_colors_info="{}" theme_builder_area="post_content"]
People who have chronic illnesses such as ABPA & CPA are very vulnerable to anxiety and depression. These are not superficial illnesses in themselves, and they can be very serious and even life threatening in some cases, if neglected. It is important that we remove the stigma that has long been a part of depression – partly from those who would seek to devalue people who suffer from depression, and partly from the people themselves. Depression is very common.
Recognising Depression – Common Symptoms
The mental health charity, Mind, has produced this extensive guide to understanding depression. It’s full of useful information and contacts, so is well worth a read if you think you, or someone you know, might be experiencing the symptoms of depression. Some of the most common symptoms they identify are copied below:

This NHS page also gives a good overview of depression; recognising the symptoms in yourself, and the various treatment options available.
Depression and chronic illness
This WikiHow article is very good at describing how we can fight back against depression due to chronic illness – the first part of which is acceptance, and then developing your personal tools to beat depression. Building effective personal management tools is very important in this battle; apathy or lack of acceptance will contribute to making depression worse, because if we fail to recognise the symptoms (in ourselves or others), we will fail to build our defences against it.
[/et_pb_text][/et_pb_column][/et_pb_row][/et_pb_section]
Plugs and Slugs
[et_pb_section fb_built="1" _builder_version="4.19.1" _module_preset="default" width="100%" custom_padding="|18px||||" hover_enabled="0" global_colors_info="{}" theme_builder_area="post_content" sticky_enabled="0"][et_pb_row _builder_version="4.18.0" _module_preset="default" custom_margin="|auto||84px||" custom_padding="7px|0px|7px|0px|true|true" global_colors_info="{}" theme_builder_area="post_content"][et_pb_column type="4_4" _builder_version="4.18.0" _module_preset="default" global_colors_info="{}" theme_builder_area="post_content"][et_pb_text _builder_version="4.18.0" _module_preset="default" global_colors_info="{}" theme_builder_area="post_content"]
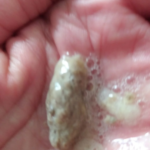
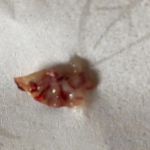
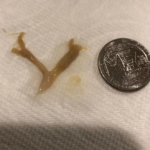
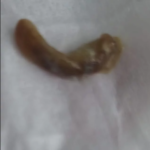
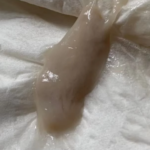
People who have aspergillosis tend to cough up characteristic mucoid plugs often when being given oral steroids. These can take many shapes and forms and be different colours depending on what they contain – some can have hard objects within them, others can be very thick/hard on general consistency.
These can be a helpful sign for a diagnosis, so we thought is would be useful if we collected a small library of images for clinicians to refer to, which we will publish here. Patients could also use them to show to your doctor as examples of the kind of thing they are also coughing up.
Images have helpfully been donated by members of the National Aspergillosis Support UK Facebook group.
Contact us if you have examples you would like us to include.
[/et_pb_text][et_pb_toggle title="Aspergillosis plugs ‘n slugs (Click here to show images)" open_toggle_text_color="#000000" _builder_version="4.18.0" _module_preset="default" title_text_color="#000000" title_font="|600|||||||" global_colors_info="{}" theme_builder_area="post_content"]
[/et_pb_toggle][/et_pb_column][/et_pb_row][/et_pb_section]
Living with CPA and ABPA
[et_pb_section fb_built="1" _builder_version="4.18.0" _module_preset="default" global_colors_info="{}" theme_builder_area="post_content" custom_padding="8px||2px|||"][et_pb_row _builder_version="4.18.0" _module_preset="_initial" custom_margin="-21px|auto||auto||" global_colors_info="{}" theme_builder_area="post_content" custom_padding="40px|0px|40px|0px|true|true"][et_pb_column type="4_4" _builder_version="4.18.0" _module_preset="default" global_colors_info="{}" theme_builder_area="post_content"][et_pb_text _builder_version="4.18.0" _module_preset="default" global_colors_info="{}" theme_builder_area="post_content"]
Gwynedd was formally diagnosed with CPA and ABPA at the National Aspergillosis Centre in 2012. Below she lists some of the symptoms she experiences and what she has found helpful in managing the conditions.
These symptoms fluctuate and can be very insignificant until a flare-up occurs. Then they can be severe enough to alter what I can do in a day.
- Tightening of the chest and or upper airway.
- Inflammation can be felt as heat and a 'zingyness' in my chest.
- Pain and discomfort over my back in my lungs.
Self-help
- A healthy diet, as recommended by the dietetic society or as guided by a consultant or specialist nurse.
- Extra protein where one is underweight.
- Exercise is essential for my mental well-being and helps me with chest clearing.
My local respiratory consultant firmly believes in the benefits of Yoga and slower breathing to help with chest clearance and relaxation, which reduces inflammation and anxiety and aids the immune system.
Anxiety is a side effect of ABPA & CPA as both conditions are debilitating, and fluctuations occur seemingly with no warning. It is not unreasonable to feel anxious about this diagnosis. Treatments help, as do lifestyle changes.
[/et_pb_text][/et_pb_column][/et_pb_row][/et_pb_section]