Talking to Friends and Family about Aspergillosis
[et_pb_section fb_built="1" admin_label="section" _builder_version="4.16" global_colors_info="{}" theme_builder_area="post_content" custom_padding="1px||1px||true|false"][et_pb_row admin_label="row" _builder_version="4.16" background_size="initial" background_position="top_left" background_repeat="repeat" global_colors_info="{}" theme_builder_area="post_content"][et_pb_column type="4_4" _builder_version="4.16" custom_padding="|||" global_colors_info="{}" custom_padding__hover="|||" theme_builder_area="post_content"][et_pb_text admin_label="Text" _builder_version="4.16" background_size="initial" background_position="top_left" background_repeat="repeat" global_colors_info="{}" theme_builder_area="post_content"]
It can be hard to talk to friends and family about aspergillosis. As a rare disease, few people know about it, and some of the medical terms can be quite confusing. If you’ve been recently diagnosed, you might still be getting to grips with the disease for yourself, and learning about how it will affect your life. You might also run into preconceptions or assumptions about fungal disease that aren’t particularly helpful.
All in all, these are tricky waters to navigate, so here are some things to consider before talking to someone about aspergillosis for the first time.
- Get to grips with aspergillosis yourself first. Particularly if you’ve recently been diagnosed.
You might not ever know all the answers, but having an understanding of your type, your treatment and what aspergillosis means for you will help.
- Pick a good time and place. Being able to talk one-to-one, in a place where you won’t be interrupted, is a good first step.
It’s also a good idea to choose a time when neither of you will have to rush off. Pop the kettle on and settle in.
- Be patient. Your loved one or friend probably won’t have heard of aspergillosis before, and might struggle with the different medical words, so give them time to digest what you have told them and ask questions if they need to.
Try not to get frustrated if they don’t react in the way that you’d hoped. They might be very sad, when what you need right now is someone to be strong. Or they might brush it off or make light of it, when you want them to understand that aspergillosis is a serious disease. Often people need time to go away and think before coming back with offers of support, or with more questions – let them know that that’s ok.
- Be open and honest. Talking to someone you care for about the disease is not easy, but it’s important that you explain how aspergillosis is likely to affect you. You might feel tempted to downplay things, but being honest can help in managing your friend or family member’s expectations in the future.
Some people find the Spoon Theory helpful in explaining chronic illness. In short, spoons represent the energy needed to get daily tasks (getting dressed, showering, washing up etc.) done. People without chronic illness have an unlimited number of spoons each day. But people with a disease like aspergillosis only get, say, 10 spoons on a ‘good’ day. Using this example can help to explain how living with aspergillosis effects all areas of life.
- Let them in. If you are talking to someone close to you, inviting them to learn more or share some of your experiences can be very helpful. You might want to invite them to come to an appointment with you, or visit a local support meeting.
If they want to learn more, or ask questions you don’t know the answer to, useful resources are available online. For example, did you know that we have a Facebook group just for family, friends and carers of people with aspergillosis? Lots of pages on this website can also be very helpful, so feel free to pass on the link (https://aspergillosis.org/).
- Be yourself – you are not your disease. There is so much more to you than aspergillosis, and your friends and family should know that too. But talking about it could mean that you get a little bit more support or understanding from those closest to you, which is never a bad thing.
[/et_pb_text][/et_pb_column][/et_pb_row][/et_pb_section]
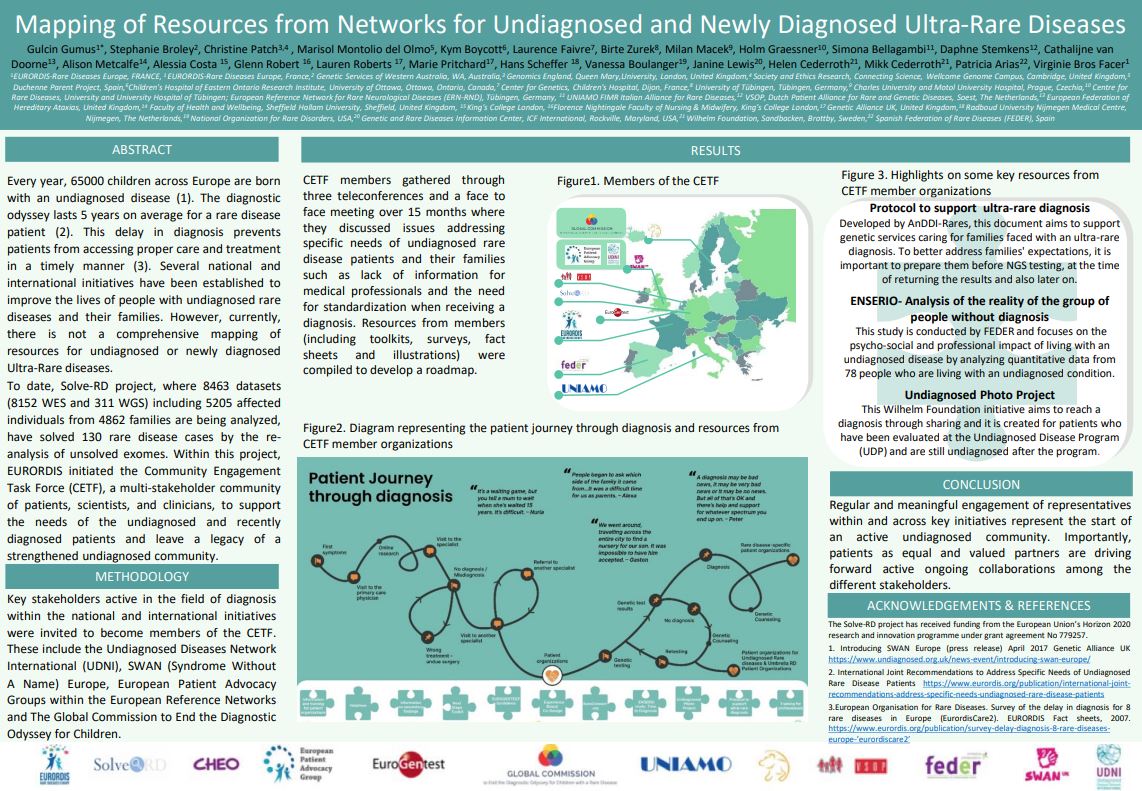
Rare disease patient journey to diagnosis
[et_pb_section fb_built="1" _builder_version="4.16" global_colors_info="{}" theme_builder_area="post_content"][et_pb_row _builder_version="4.16" background_size="initial" background_position="top_left" background_repeat="repeat" global_colors_info="{}" theme_builder_area="post_content"][et_pb_column type="4_4" _builder_version="4.16" custom_padding="|||" global_colors_info="{}" custom_padding__hover="|||" theme_builder_area="post_content"][et_pb_text _builder_version="4.16" background_size="initial" background_position="top_left" background_repeat="repeat" global_colors_info="{}" theme_builder_area="post_content"]
A map aspergillosis patients may be all too familiar with!
https://twitter.com/eurordis/status/1269906129364156416
[/et_pb_text][/et_pb_column][/et_pb_row][/et_pb_section]
ISHAM Award for Prof Malcolm Richardson
[et_pb_section fb_built="1" admin_label="section" _builder_version="4.16" global_colors_info="{}" theme_builder_area="post_content" custom_padding="0px||0px||true|false"][et_pb_row admin_label="row" _builder_version="4.16" background_size="initial" background_position="top_left" background_repeat="repeat" global_colors_info="{}" theme_builder_area="post_content"][et_pb_column type="4_4" _builder_version="4.16" custom_padding="|||" global_colors_info="{}" custom_padding__hover="|||" theme_builder_area="post_content"][et_pb_text admin_label="Text" _builder_version="4.16" background_size="initial" background_position="top_left" background_repeat="repeat" global_colors_info="{}" theme_builder_area="post_content"] Founded in 1954, the International Society for Human and Animal Mycology (ISHAM) is a large worldwide organisation that represents and supports all doctors and researchers that have an interest in Medical Mycology - which includes aspergillosis as well as all fungal disease.
Founded in 1954, the International Society for Human and Animal Mycology (ISHAM) is a large worldwide organisation that represents and supports all doctors and researchers that have an interest in Medical Mycology - which includes aspergillosis as well as all fungal disease.
Fungal diseases are generally not given the attention that they deserve from medical authorities so it is vital that diagnostics and research are supported internationally, especially where health services, so the work of ISHAM is particularly valuable.
The immense contribution of medical mycology diagnostics specialist and former Director of the Mycology Reference Centre Manchester Prof Malcolm Richardson to the work of ISHAM has been recognised at the recent ISHAM conference in New Delhi, September 2022.[/et_pb_text][/et_pb_column][/et_pb_row][/et_pb_section]
Mycology Reference Centre Manchester Director (retired) Prof Malcolm Richardson Honoured
[et_pb_section fb_built="1" admin_label="section" _builder_version="4.16" global_colors_info="{}" theme_builder_area="post_content" custom_padding="7px||7px||true|false"][et_pb_row admin_label="row" _builder_version="4.16" background_size="initial" background_position="top_left" background_repeat="repeat" global_colors_info="{}" theme_builder_area="post_content"][et_pb_column type="4_4" _builder_version="4.16" custom_padding="|||" global_colors_info="{}" custom_padding__hover="|||" theme_builder_area="post_content"][et_pb_text admin_label="Text" _builder_version="4.16" background_size="initial" background_position="top_left" background_repeat="repeat" global_colors_info="{}" theme_builder_area="post_content"]

The British Society for Medical Myology (BSMM) has a long and distinguished history in the advancement of education and the promotion of research in all branches of medical and veterinary mycology over the last 69 years (www.bsmm.org), so it is a great honour to be elected to be its President. Prof Richardson follows an illustrious list of fellow medical mycologists who have served as President of BSMM since 1964.
Professor Malcolm Richardson built and ran the highly specialised mycology laboratories at the Mycology Reference Centre Manchester since its inception alongside the National Aspergillosis Centre at the Manchester University NHS FT in 2009 until his retirement in 2020, and still serves the centre as its Consultant Clinical Scientist in Medical Mycology. He has an extensive list of publications, positions and achievements - for more details click here.
Prof Richardson commented "I feel very honoured to be elected as President, having been a BSMM member for 50 years", and it is particularly fitting that the Presidency comes to Manchester as the annual scientific meeting of the BSMM is to take place in the city in May 2023.
[/et_pb_text][/et_pb_column][/et_pb_row][/et_pb_section]
Why does someone with chronic disease feel so tired?
[et_pb_section fb_built="1" _builder_version="4.18.0" _module_preset="default" custom_padding="7px||93px|||" global_colors_info="{}" theme_builder_area="post_content" custom_margin="|-29px||-30px||"][et_pb_row _builder_version="4.18.0" _module_preset="157b2edb-eee9-4384-8648-c0e491cc6118" custom_padding="11px||70px||false|" hover_enabled="0" global_colors_info="{}" theme_builder_area="post_content" box_shadow_style="none" sticky_enabled="0"][et_pb_column type="4_4" _builder_version="4.18.0" _module_preset="default" global_colors_info="{}" theme_builder_area="post_content"][et_pb_video src="https://www.youtube.com/watch?v=ML_NL8EdhCc" _builder_version="4.18.0" _module_preset="default" custom_margin="||2px|||" custom_padding="30px|30px|30px|30px|false|false" global_colors_info="{}" theme_builder_area="post_content"][/et_pb_video][et_pb_text _builder_version="4.18.0" _module_preset="default" text_font_size="15px" global_colors_info="{}" theme_builder_area="post_content"]
Ashley explains how fatigue affects your psychological wellbeing, and how to manage thoughts and feelings.
[/et_pb_text][et_pb_text _builder_version="4.18.0" _module_preset="default" custom_padding="|1px||1px|false|true" global_colors_info="{}" theme_builder_area="post_content"]
Most people with a chronic illness will be all too familiar with how tired it makes them feel. Fatigue is a prominent and debilitating symptom of aspergillosis and recent research is starting to show why this is.
We are often asked why someone with aspergillosis feels so tired and up till now our usual answer would be that when your immune system is working hard it tires you out much like if you had run a km or two that day – the effort needed is similar and you are exhausted. Recent research gives us a slightly different picture. As your body responds to an infection one of the things that your immune system can do is to directly put you to sleep to help your recovery!
Molecules called cytokines are produced in response to inflammation (eg infection) and one of their functions is to stimulate drowsiness and sleep. Furthermore once asleep your immune system really gets to work on the infection – focusing your energy on fighting the infection, and promoting fever.
We are aware that some medications make good sleep difficult/impossible at times and anxiety plays its part too. If you mention this to your GP you may get a referral to one of the many NHS Sleep clinics in the UK who can help problems with getting asleep/staying asleep https://www.nhs.uk/…/Sleep-Medicine/LocationSearch/1888
Hints and tips for getting a good sleep
Hints and tips on how to manage the psychological impact of fatigue
[/et_pb_text][/et_pb_column][/et_pb_row][/et_pb_section]
The importance of detecting cancer early
[et_pb_section fb_built="1" admin_label="section" _builder_version="4.18.0" custom_padding="5px||5px|||" global_colors_info="{}" theme_builder_area="post_content"][et_pb_row admin_label="row" _builder_version="4.16" background_size="initial" background_position="top_left" background_repeat="repeat" custom_margin="|-33px||21px||" custom_padding="5px|0px||||" global_colors_info="{}" theme_builder_area="post_content"][et_pb_column type="4_4" _builder_version="4.16" custom_padding="|||" global_colors_info="{}" custom_padding__hover="|||" theme_builder_area="post_content"][et_pb_text admin_label="Text" _builder_version="4.16" background_size="initial" background_position="top_left" background_repeat="repeat" custom_margin="-41px|-146px||||" global_colors_info="{}" theme_builder_area="post_content"]
Our focus at the National Aspergillosis Centre is to raise awareness and support those with aspergillosis. Still, it is vital as an NHS organisation that we raise awareness of other conditions because, sadly, a diagnosis of aspergillosis does not make you impervious to everything else, and a chronic illness has the potential to mask the symptoms of other conditions like cancer.
The ever-growing pressure on the NHS, increased waiting times, a growing reluctance amongst many to seek medical attention, and a lack of understanding of the common symptoms of many cancers are all factors that can lead to an extended diagnostic interval, which in turn reduces treatment options. Therefore, earlier recognition of symptoms by patients is crucial in mitigating other factors that delay diagnosis.
It is important to note that not all alarm symptoms are cancer. Still, cancer incidence and mortality projections estimate that 1 in 2 people in the UK will be diagnosed with cancer in their lifetime(1), so last week at our monthly patient meeting, we talked about cancer and the most common symptoms. Inspired by the incredible work of the late Dame Deborah James on raising awareness and breaking down the taboo attached to bowel cancer, we have compiled the content from that talk into one article.
What is Cancer?
Cancer starts in our cells.
Usually, we have just the right number of each type of cell. This is because cells produce signals to control how much and how often the cells divide.
If any of these signals are faulty or missing, cells might start to grow and multiply too much and form a lump called a tumour.
Cancer Research UK, 2022
Cancer Statistics
- Every two minutes, someone in the UK is diagnosed with cancer.
- Breast, prostate, lung and bowel cancers together accounted for over half (53%) of all new cancer cases in the UK in 2016-2018.
- Half (50%) of people diagnosed with cancer in England and Wales survive their disease for ten years or more (2010-11).
- Cancer is the cause of 27-28% of all deaths in England in a typical year.
Experts believe abdominal cancers - throat, stomach, bowel, pancreatic, ovarian - and urological cancers - prostate, kidney and bladder - are the most likely to go unrecognised.

The above chart shows cancer diagnoses by stage for some cancers in 2019 (the most current data). The stage of cancer relates to the size of the tumour and how far it has spread. Diagnosis at a later stage is related to lower survival.
Breast Cancer - Symptoms
- A lump or thickening in the breast which is different to the rest of the breast tissue
- Continuous breast pain in one part of the breast or armpit
- One breast becomes larger or lower/higher than the other breast
- Changes to the nipple - turning inward or changes shape or position
- Puckering or dimpling to the breast
- Swelling under the armpit or around the collarbone
- A rash on or around the nipple
- Discharge from one or both nipples
For more information visit:
https://www.breastcanceruk.org.uk/
https://www.cancerresearchuk.org/about-cancer/breast-cancer
Kidney Cancer - Symptoms
- Blood in the urine
- Low back pain on one side not through injury
- A lump on the side or lower back
- Fatigue
- Loss of appetite
- Unexplained weight loss
- Fever that is not caused by an infection and that doesn't go away
For more information visit:
https://www.nhs.uk/conditions/kidney-cancer/symptoms/
https://www.cancerresearchuk.org/about-cancer/kidney-cancer/symptoms
Lung cancer
The symptoms of lung cancer can be particularly hard to differentiate for patients with aspergillosis. It is important to report any new symptoms, such as a change to a long-term cough, weight loss and chest pain to your GP or specialist consultant.
Symptoms
- A persistent cough that doesn't go away after 2/3 weeks
- A change in your long-term cough
- Increased and persistent breathlessness
- Coughing up blood
- An ache or pain in the chest or shoulder
- Repeated or persistent chest infection
- Loss of appetite
- Fatigue
- Weight loss
- Hoarsness
For more information visit:
https://www.nhs.uk/conditions/lung-cancer
https://www.cancerresearchuk.org/about-cancer/lung-cancer
Ovarian Cancer - Symptoms
- Persistent bloating
- Feeling full quickly
- Loss of appetite
- Changes in bowel habits
- Unexplained weight loss
- Pelvic or abdominal pain
- Needing to wee more frequently
- Fatigue
For more information visit:
https://www.nhs.uk/conditions/ovarian-cancer/
Pancreatic Cancer
Some of the symptoms of pancreatic cancer can closely resemble those of bowel conditions such as irritable bowel. See your GP if your symptoms change, get worse, or do not feel normal for you.
Symptoms
- Yellowing to the whites of your eyes or skin (jaundice)
- Itchy skin, darker pee and paler poo than usual
- Loss of appetite
- Fatigue
- Fever
Other symptoms can affect your digestion, such as:
- Nausea and vomiting
- Changes in bowel habits
- Stomach and/or back pain
- Indigestion
- Bloating
For more information visit:
https://www.nhs.uk/conditions/pancreatic-cancer
https://www.cancerresearchuk.org/about-cancer/pancreatic-cancer
https://www.pancreaticcancer.org.uk/
Prostate Cancer - Symptoms
- Urinating more frequently, often during the night (nocturia)
- Increased urgency to urinate
- Urine hesitancy (difficulty starting to urinate)
- Difficulty in passing urine
- Weak flow
- Feeling that your bladder has not emptied fully
- Blood in urine or semen
For more information visit:
https://www.nhs.uk/conditions/prostate-cancer
https://www.cancerresearchuk.org/about-cancer/prostate-cancer
Skin Cancer
Patients who are on antifungal medication are at an increased risk of developing skin cancer, therefore it is important to understand the symptoms and take adequate precautions with sun exposure to reduce the risk.
Symptoms
There are three main types of skin cancer:
- Malignant Melanoma
- Basal Cell Carcinoma (BCC)
- Squamous Cell Carcinoma (SCC)
Broadly, the signs are (shown in the image below):
BCC
- Flat, raised or dome-shaped spot
- Pearly or skin-coloured
SCC
- Raised, crusty or scaly
- Sometimes ulcerated
Melanoma
- An abnormal mole that is asymmetrical, irregular and has multiple colours

For more information visit:
https://www.cancerresearchuk.org/about-cancer/skin-cancer
https://www.nhs.uk/conditions/melanoma-skin-cancer/
https://www.nhs.uk/conditions/non-melanoma-skin-cancer/
Throat Cancer
Throat cancer is a general term that means cancer that starts in the throat, however, Doctors don't generally use it. This is because there are different types of cancer which can affect the area of the throat.
More information can be found here: https://www.macmillan.org.uk/cancer-information-and-support/head-and-neck-cancer/throat-cancer
General symptoms
- Sore throat
- Ear pain
- Lump in the neck
- Difficulty swallowing
- Change in your voice
- Unexplained weight loss
- A cough
- Shortness of breath
- A feeling of something stuck in the throat
For more information visit:
https://www.nhs.uk/conditions/head-and-neck-cancer/
Bladder Cancer - Symptoms
- Increased urination
- Urgency to urinate
- A burning sensation when passing urine
- Pelvic pain
- Flank pain
- Abdominal pain
- Unexplained weight loss
- Leg swelling
For more information visit:
https://www.nhs.uk/conditions/bladder-cancer/
https://www.cancerresearchuk.org/about-cancer/bladder-cancer
Bowel Cancer - Symptoms
- Bleeding from the bottom and/or blood in poo
- A persistent and unexplained change in bowel habit
- Unexplained weight loss
- Fatigue
- A pain or lump in the stomach
For more information visit:
https://www.bowelcanceruk.org.uk/about-bowel-cancer/
https://www.cancerresearchuk.org/about-cancer/bowel-cancer
(1)Smittenaar CR, Petersen KA, Stewart K, Moitt N. Cancer incidence and mortality projections in the UK until 2035. Br J Cancer 2016 Oct 25;115(9):1147-1155
[/et_pb_text][/et_pb_column][/et_pb_row][/et_pb_section]
Aspergillosis and Fatigue
[et_pb_section fb_built="1" _builder_version="4.18.0" _module_preset="default" custom_padding="3px||2px|||" global_colors_info="{}"][et_pb_row _builder_version="4.18.0" _module_preset="default" custom_padding="30px|30px|30px|30px|true|true" hover_enabled="0" global_colors_info="{}" box_shadow_style="preset1" sticky_enabled="0"][et_pb_column type="4_4" _builder_version="4.18.0" _module_preset="default" global_colors_info="{}"][et_pb_text _builder_version="4.18.0" _module_preset="default" global_colors_info="{}"]
People who have chronic respiratory illness frequently state that one of the main symptoms that they find difficult to cope with is perhaps one that doesn’t leap to mind as a major problem for most of us who do not have a chronic illness – fatigue.
Time and time again people who have aspergillosis mention how exhausted it makes them feel, and here at the National Aspergillosis Centre we have determined that fatigue is a major component of chronic pulmonary aspergillosis (CPA – see Al-Shair et. al. 2016) and that the impact of aspergillosis on a patients quality of life correlated well with the level of fatigue suffered.
There are many possible causes of fatigue in the chronically ill: it could partly be a result of the energy that the immune system of a patient puts into fighting off the infection, it could partly be a consequence of some of the medication taken by people who are chronically ill and possibly even the result of undiagnosed health problems such as anaemia, hypothyroidism, low cortisol or infection (e.g. long COVID).
Because of the many possibilities that cause fatigue, your first step in trying to improve the situation is to go and see your doctor who can check for all common causes of fatigue. Once you have established that there are no other possible hidden causes you might read through this article on fatigue produced by NHS Scotland containing lots of food for thought and suggestions to improve your fatigue.
[/et_pb_text][/et_pb_column][/et_pb_row][/et_pb_section]
Singing for lung health
[et_pb_section fb_built="1" admin_label="section" _builder_version="4.16" global_colors_info="{}" theme_builder_area="post_content" custom_padding="11px||11px||true|false"][et_pb_row admin_label="row" _builder_version="4.16" background_size="initial" background_position="top_left" background_repeat="repeat" global_colors_info="{}" theme_builder_area="post_content"][et_pb_column type="4_4" _builder_version="4.16" custom_padding="|||" global_colors_info="{}" custom_padding__hover="|||" theme_builder_area="post_content"][et_pb_text admin_label="Text" _builder_version="4.16" background_size="initial" background_position="top_left" background_repeat="repeat" global_colors_info="{}" theme_builder_area="post_content"]The breath control needed to sing can also help people who have lung disease breathe better and can help lift mood too which is vitally important for our health and quality of life.
Want to try therapeutic singing?
You may be lucky and find a lung health group locally, however, you don't have to leave your home to benefit (sessions are run on Zoom), AND you don't have to be a patient either as the groups are also open to carers.
The Asthma & Lung Health charity has published a page giving some useful information on how you can find a singing group in your area.[/et_pb_text][/et_pb_column][/et_pb_row][/et_pb_section]
Monkeypox outbreak
[et_pb_section fb_built="1" admin_label="section" _builder_version="4.16" global_colors_info="{}" theme_builder_area="post_content"][et_pb_row admin_label="row" _builder_version="4.16" background_size="initial" background_position="top_left" background_repeat="repeat" global_colors_info="{}" theme_builder_area="post_content" custom_margin="11px|auto|11px|auto|true|false"][et_pb_column type="4_4" _builder_version="4.16" custom_padding="|||" global_colors_info="{}" custom_padding__hover="|||" theme_builder_area="post_content"][et_pb_text admin_label="Text" _builder_version="4.16" background_size="initial" background_position="top_left" background_repeat="repeat" global_colors_info="{}" theme_builder_area="post_content"]
What is Monkeypox?
How is monkeypox spread?
Symptoms
- fever
- headache
- muscle aches
- backache
- swollen lymph nodes
- shivering
- exhaustion
[/et_pb_text][/et_pb_column][/et_pb_row][/et_pb_section]
Drug Induced Photosensitivity
What is drug-induced photosensitivity?
Photosensitivity is the abnormal or heightened reaction of the skin when exposed to ultraviolet (UV) radiation from the sun. This leads to skin that has been exposed to the sun without protection becoming burnt, and in turn, this can increase the risk of developing skin cancer.
There are several medical conditions like lupus, psoriasis and rosacea that can increase a person's sensitivity to ultraviolet light. A more comprehensive list of known conditions can be found here.
Drug-induced photosensitivity is the most common type of skin-related adverse drug reaction and can occur as a result of topical and oral medications. Reactions happen when a component of the medication combines with UV radiation during sun exposure, causing a phototoxic reaction that appears as severe sunburn, identified by swelling, itchiness, profuse redness and in the worst cases, blistering and oozing.
Patients taking antifungal medications, in particular, Voriconazole and Itraconazole (the former being more widely known for causing reactions), are often aware of the increased risks of photosensitivity; however, these are not the only drugs that can induce an abnormal response to UV exposure. Other drugs that have been reported to cause photosensitivity are:
- NSAIDs (Ibuprofen (oral and topical), naproxen, aspirin)
- Cardiovascular medication (furosemide, ramipril, amlodipine, nifedipine, amiodarone, clopidogrel – just a few)
- Statins (simvastatin)
- Psychotropic drugs (olanzapine, clozapine, fluoxetine, citalopram, sertraline – just a few)
- Antibacterial medications (ciprofloxacin, tetracycline, doxycycline)
It is essential to note that the above list is not exhaustive, and reported reactions range from rare to frequent. If you think a medication other than your antifungal is causing a reaction to the sun, speak to your pharmacist or GP.
How to protect yourself
In most cases, patients can't stop taking the medication that can predispose them to photosensitivity. Staying out of the sun isn't always possible either - quality of life is always an important consideration; therefore, extra care should be taken to protect their skin while outside.
There are two types of protection:
- Chemical
- Physical
Chemical protection is in the form of sunscreen and sunblock. However, it is important to remember that sunscreen and sunblock are not the same. Sunscreen is the most common type of sun protection, and it works by filtering the sun's UV rays, but some still get through. Sunblock reflects the rays away from the skin and prevents them from penetrating it. When buying sunscreen, look for a sun protection factor (SPF) of 30 or above to protect against UVB and at least a UVA protection rating of 4 stars.
Physical protection
- NHS guidance advises staying in the shade when the sun is strongest, which in the UK is between 11am and 3pm from March to October
- Use a sunshade or umbrella
- A wide-brimmed hat that shades the face, neck and ears
- Long-sleeved tops, trousers and skirts made of close-weave fabrics that stop sunlight from penetrating
- Sunglasses with wraparound lenses and wide arms that conform to the British Standard
- UV protective clothing
Links to further information