Understanding Steroids, Cortisol, ACTH and Adrenal Suppression in Aspergillosis
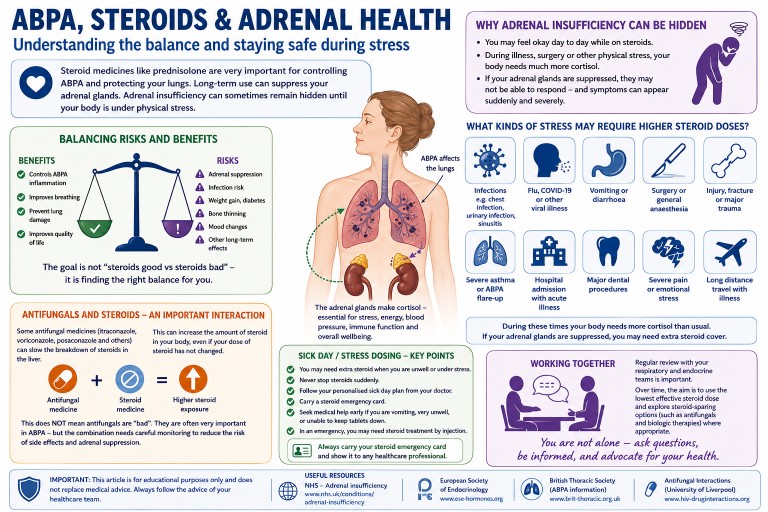
For people with Allergic Bronchopulmonary Aspergillosis (ABPA), severe asthma and other forms of aspergillosis, steroid treatment can be both extremely helpful and medically complicated.
Many patients are prescribed corticosteroids such as prednisolone or methylprednisolone to control inflammation, improve breathing and reduce the risk of lung damage. These medicines can be very effective. However, repeated or long-term steroid treatment can also affect the body’s natural hormone system, especially the adrenal glands.
Some patients are told:
- “Your cortisol is low.”
- “Your ACTH level is abnormal.”
- “You may have adrenal suppression.”
- “This may be steroid withdrawal.”
- “The blood tests are difficult to interpret.”
This can be worrying and confusing, especially when symptoms are severe but the explanation is not straightforward.
This article explains why adrenal problems can occur in some people with aspergillosis and severe asthma, why blood tests such as cortisol and ACTH can be difficult to interpret, and why steroid treatment sometimes involves a careful balance between benefit and risk.
Key points summary
- Steroid medicines can reduce the body’s own natural cortisol production.
- This is called adrenal suppression or adrenal insufficiency.
- Symptoms may overlap with aspergillosis, asthma, infection, fatigue or steroid withdrawal.
- Blood tests such as cortisol and ACTH can be difficult to interpret.
- Inhaled steroids and antifungal medicines can also influence steroid effects.
- Long-term prednisolone is generally avoided where possible, but it may still be necessary for some patients.
- Patients should not stop or reduce steroids suddenly without medical advice.
- Severe symptoms such as collapse, vomiting, dehydration, confusion or severe weakness require urgent medical advice.
Contents
- What do the adrenal glands do?
- What are cortisol and ACTH?
- Why are steroids used in ABPA and aspergillosis?
- Are steroids only meant for short-term use?
- How steroids affect the body’s natural hormone system
- What is adrenal suppression?
- Why symptoms can be difficult to recognise
- Why blood tests can become confusing
- The role of inhaled steroids
- Antifungal medicines and steroid interactions
- Steroid withdrawal versus adrenal insufficiency
- What kinds of stress may require higher steroid doses?
- When should patients seek urgent medical advice?
- Frequently asked questions
- Final thoughts
What do the adrenal glands do?
The adrenal glands are small glands that sit above the kidneys. They produce several important hormones, including cortisol.
Cortisol helps the body:
- respond to stress,
- maintain blood pressure,
- regulate energy levels,
- support immune function,
- and cope with illness or infection.
The body carefully controls cortisol levels through a hormone signalling system involving the brain, the pituitary gland and the adrenal glands.
What are cortisol and ACTH?
ACTH stands for adrenocorticotropic hormone.
The pituitary gland in the brain releases ACTH to tell the adrenal glands to produce cortisol.
This system normally works as a feedback loop:
- When cortisol is low, ACTH usually rises.
- When cortisol is high, ACTH usually falls.
Cortisol levels naturally change during the day and are usually highest in the early morning. This is one reason why many cortisol blood tests are taken around 9am.
Why are steroids used in ABPA and aspergillosis?
In Allergic Bronchopulmonary Aspergillosis (ABPA) and some severe asthma conditions, the immune system reacts strongly to Aspergillus fungi.
This can cause:
- airway inflammation,
- wheezing,
- coughing,
- mucus plugging,
- breathlessness,
- worsening lung function,
- and repeated flare-ups.
Steroids such as prednisolone are often used because they reduce inflammation quickly and effectively.
Some patients may need:
- short courses during flare-ups,
- repeated courses,
- long-term low-dose treatment,
- inhaled steroid therapy,
- antifungal treatment,
- or biologic medicines to reduce the need for oral steroids.
For many patients, steroids are not optional or casual medicines. They may be essential treatments used to control serious inflammation and protect lung function.
Are steroids only meant for short-term use?
Patients sometimes hear that prednisolone was “only designed for short-term use”. This is understandable, because modern medical practice tries to avoid long-term steroid treatment where possible.
Long-term oral corticosteroids can cause significant side effects, including:
- adrenal suppression,
- diabetes or worsening blood sugar control,
- osteoporosis and fracture risk,
- increased infection risk,
- cataracts or glaucoma,
- muscle weakness,
- skin thinning and bruising,
- weight gain,
- sleep disturbance,
- and mood or mental health effects.
For this reason, doctors usually aim to use steroids at the lowest effective dose for the shortest safe time.
However, it is also important not to oversimplify this message. Some people with ABPA, severe asthma or other inflammatory lung conditions do need longer-term steroid treatment because the disease itself can be dangerous if not controlled.
In some patients, the risk of uncontrolled lung inflammation may outweigh the risks of steroid treatment, at least for a period of time.
Modern care increasingly tries to reduce steroid exposure by using other approaches where appropriate, such as:
- antifungal treatment,
- biologic medicines for severe asthma or ABPA-type inflammation,
- careful monitoring of lung function and blood tests,
- gradual steroid tapering,
- bone protection where needed,
- diabetes monitoring,
- and regular review of whether the steroid dose can be reduced.
The key message is not that patients have done anything wrong by needing steroids. The key message is that long-term steroid treatment deserves careful monitoring, honest discussion and regular review.
Patient reassurance: If you have needed prednisolone for ABPA or severe asthma, this does not mean you have failed or made a poor choice. It usually means your medical team has been trying to control a potentially serious inflammatory condition. The aim is to balance benefit and risk as safely as possible.
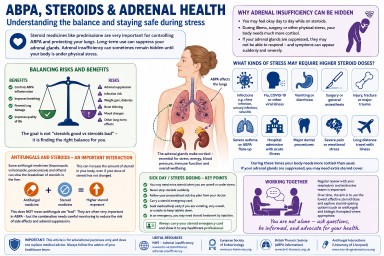
Balancing risks and benefits
One of the hardest parts of long-term steroid treatment is that two important things can be true at the same time:
- steroids can cause serious side effects,
- and steroids can also prevent serious lung damage and dangerous flare-ups.
Patients sometimes feel guilty, frustrated or frightened when they hear about the risks of prednisolone. Others may feel judged for “still being on steroids”.
However, many people with ABPA or severe asthma did not choose steroids lightly. Steroids are often prescribed because uncontrolled inflammation itself can damage the lungs, worsen bronchiectasis, increase hospital admissions and significantly reduce quality of life.
Modern respiratory care increasingly tries to reduce steroid exposure where possible using:
- antifungal therapy,
- biologic medicines,
- careful monitoring,
- gradual tapering plans,
- and better recognition of steroid side effects.
But for some patients, steroids may still remain an important part of treatment, even if the goal is eventually to reduce the dose.
The most helpful approach is usually not “steroids are good” or “steroids are bad”, but rather:
- What dose is truly needed?
- Can the dose be safely reduced?
- Are side effects being monitored properly?
- Are there alternative treatments available?
- And is the patient being listened to when symptoms change?
This balanced approach is increasingly recognised as one of the most important parts of caring for people with severe asthma and aspergillosis.
How steroids affect the body’s natural hormone system
Steroid medicines act in ways that are similar to natural cortisol.
When the body senses steroid medication in the bloodstream, it may reduce its own ACTH production. Over time, this can mean:
- ACTH falls,
- the adrenal glands become less active,
- and natural cortisol production decreases.
Doctors sometimes describe this as the adrenal glands “going to sleep”.
This is called:
- adrenal suppression,
- steroid-induced adrenal insufficiency,
- or hypothalamic-pituitary-adrenal axis suppression.
What is adrenal suppression?
Adrenal suppression means the body may not produce enough cortisol when it is needed.
This can become especially important during:
- infection,
- surgery,
- injury,
- severe stress,
- or rapid steroid reduction.
Some patients develop symptoms gradually. Others notice problems when trying to reduce steroid doses.
Because cortisol is part of the body’s stress response, people with adrenal insufficiency may need specific medical advice about what to do during illness, vomiting, surgery or severe infection.
Why symptoms can be difficult to recognise
Symptoms of adrenal suppression can overlap with many other conditions common in people with aspergillosis, ABPA or severe asthma.
Possible symptoms include:
- profound tiredness,
- weakness,
- dizziness,
- sweating,
- shakiness,
- nausea,
- muscle aches,
- low mood,
- brain fog,
- reduced exercise tolerance,
- poor recovery after illness,
- or feeling suddenly much worse after reducing steroids.
These symptoms may also occur with:
- an ABPA flare,
- asthma worsening,
- lung infection,
- chronic illness,
- poor sleep,
- anxiety,
- or steroid withdrawal.
This overlap is one reason why patients can feel frustrated or uncertain. Symptoms are real, even when the cause is difficult to pin down.
Why blood tests can become confusing
Many patients expect blood tests to give clear answers, but cortisol and ACTH results are often complicated.
Several things can affect results:
- time of day,
- recent steroid use,
- the type of steroid used,
- inhaled steroid dose,
- recent dose reductions,
- illness or stress,
- laboratory methods,
- and antifungal medicines.
Typical patterns
In classic steroid-induced adrenal suppression:
- cortisol is low,
- and ACTH is low or “inappropriately normal”.
This happens because steroid medication suppresses ACTH production.
However, real-life cases are not always straightforward. Some patients may have recently reduced steroids, missed doses, changed steroid type, used high-dose inhaled steroids, or taken antifungal medicines that alter steroid metabolism.
In some situations, endocrinologists may need repeated testing or dynamic tests such as a Synacthen test to understand whether the adrenal glands can respond properly.
It is important that patients do not try to interpret cortisol or ACTH results in isolation. The result needs to be understood alongside symptoms, medication history, timing of the sample and the clinical situation.
The role of inhaled steroids
Many people assume inhaled steroids only affect the lungs.
Inhaled steroids usually have fewer whole-body effects than long-term oral steroids, but high doses can sometimes contribute to adrenal suppression, especially when combined with:
- long-term or repeated oral steroid courses,
- azole antifungal medicines,
- other medicines that affect steroid metabolism,
- or individual differences in how medicines are processed.
This does not mean inhaled steroids are unsafe or should be stopped suddenly. For many people with asthma or ABPA, inhaled steroids are an important part of keeping airway inflammation under control.
It does mean that total steroid exposure should be reviewed carefully, especially in patients with symptoms suggestive of adrenal suppression.
Antifungal medicines and steroid interactions
This is an especially important issue in aspergillosis.
Antifungal medicines such as:
- itraconazole,
- voriconazole,
- posaconazole,
- and isavuconazole
can interact with other medicines, including corticosteroids.
Some azole antifungals slow the breakdown of steroids in the liver. This can increase the body’s exposure to steroid medication, meaning that even doses which initially appear moderate may sometimes behave more like higher doses inside the body.
This interaction may increase the risk of:
- adrenal suppression,
- Cushing-like side effects,
- weight gain,
- skin thinning,
- easy bruising,
- high blood sugar,
- muscle weakness,
- or hormonal imbalance.
The interaction can be particularly important in patients taking:
- oral prednisolone or methylprednisolone,
- high-dose inhaled steroids,
- multiple steroid preparations together,
- or repeated steroid courses over time.
Some patients tolerate steroid treatment reasonably well for long periods before antifungal medicines are added. Endocrine problems may then become more noticeable later, especially during:
- infection,
- surgery,
- vomiting or diarrhoea,
- major physical stress,
- rapid steroid reduction,
- or severe asthma or ABPA flare-ups.
This can feel as though adrenal insufficiency has appeared “suddenly” or “out of nowhere”, when in reality the adrenal glands may have been partially suppressed for some time.
Why adrenal insufficiency may only become obvious during illness or stress
Some patients with steroid-related adrenal suppression cope reasonably well during normal day-to-day life, especially while still taking regular steroids. However, the problem may become much more noticeable when the body faces significant physical stress.
Under normal circumstances, the body rapidly increases cortisol production during severe illness or injury. If the adrenal glands cannot respond properly, symptoms may suddenly become much more severe.
Patients sometimes describe:
- “crashing” during an infection,
- extreme exhaustion,
- severe weakness,
- dizziness or collapse,
- poor recovery after illness,
- or feeling suddenly unable to cope physically.
This does not mean every severe illness in an ABPA patient is caused by adrenal insufficiency. Infections, inflammation and lung disease themselves are often the major problem. However, adrenal suppression can sometimes contribute to deterioration and may only reveal itself during periods of stress or acute illness.
This is one reason why some patients are given “sick day rules”, emergency steroid cards or advice about temporary steroid dose increases during illness.
Importantly, this does not mean antifungal medicines are “bad” or should be avoided. In many patients, antifungal treatment significantly improves ABPA control and may eventually help reduce steroid exposure overall. The important message is that these combinations require awareness, monitoring and careful medical supervision.
Patients should never stop antifungal or steroid medicines suddenly without medical advice.
Steroid withdrawal versus adrenal insufficiency
Steroid withdrawal and adrenal insufficiency can feel very similar.
Steroid withdrawal
When steroid doses are reduced, the body may take time to adjust. Patients can temporarily feel unwell even if the adrenal glands are slowly recovering.
Adrenal insufficiency
Adrenal insufficiency means the body cannot produce enough cortisol to meet its needs.
Symptoms may overlap considerably. Recovery can sometimes take weeks or months, and in some patients longer.
For many patients, one of the hardest parts is that they may “look well” externally while feeling exhausted internally.
It is important that symptoms are not dismissed simply because they are difficult to measure.
What kinds of stress may require higher steroid doses?
Patients who have adrenal insufficiency or significant adrenal suppression may sometimes be advised to temporarily increase steroid doses during periods of physical stress. This is often called following “sick day rules”.
The body normally produces extra cortisol during stress, illness or injury. If the adrenal glands cannot respond properly, extra steroid medication may sometimes be needed to prevent serious illness.
Examples of situations that may place significant stress on the body include:
- high fever or significant infection,
- chest infection or pneumonia,
- vomiting or diarrhoea,
- COVID-19 or influenza,
- major dental treatment or surgery,
- fractures or significant injury,
- general anaesthetic procedures,
- severe asthma attacks or ABPA flare-ups,
- hospital admission with acute illness,
- or severe physical exhaustion associated with illness.
The exact advice varies between patients depending on:
- whether adrenal insufficiency has been formally diagnosed,
- the steroid dose currently being taken,
- how suppressed the adrenal glands are thought to be,
- other medical conditions,
- and guidance from endocrine or respiratory specialists.
Some patients are provided with:
- specific “sick day rules”,
- an emergency steroid card,
- medical alert jewellery,
- or emergency hydrocortisone injection kits.
Patients should only adjust steroid doses according to the advice provided by their medical team. If severe vomiting, collapse, confusion, inability to keep medication down or major deterioration occurs, urgent medical advice is needed.
When should patients seek urgent medical advice?
Patients should seek urgent medical help if they experience:
- collapse,
- fainting,
- severe vomiting,
- inability to keep steroid medication down,
- severe dehydration,
- confusion,
- severe weakness,
- very low blood pressure,
- or sudden major deterioration during illness.
These symptoms can occasionally indicate adrenal crisis, which is a medical emergency.
Patients who have been told they are at risk of adrenal insufficiency should follow the emergency and “sick day” advice given by their endocrine or respiratory team.
Frequently asked questions
Does everyone taking steroids develop adrenal suppression?
No. Risk depends on factors such as dose, duration, repeated courses, inhaled steroid dose, other medicines and individual sensitivity.
Can adrenal function recover?
Yes. Many patients gradually recover adrenal function over time, although recovery speed varies.
Are inhaled steroids safer than tablets?
Inhaled steroids usually have fewer whole-body effects than long-term oral steroids, but high doses can still contribute to adrenal suppression in some patients, especially when combined with certain antifungal medicines.
Why do I feel worse when reducing steroids?
This can happen for several reasons. The underlying lung disease may flare, the body may be adjusting to lower steroid levels, or cortisol production may not yet have recovered.
Does needing long-term prednisolone mean something has gone wrong?
Not necessarily. Long-term prednisolone is usually avoided where possible because of side effects, but some patients need it to control serious inflammation. The aim is regular review, careful monitoring and dose reduction when it is safe.
Should I stop steroids because of this risk?
No patient should stop prescribed steroids suddenly unless specifically advised by their medical team. Sudden withdrawal can be dangerous, especially if the body’s own cortisol production is suppressed.
Final thoughts
Adrenal suppression and steroid-related hormone problems are recognised complications of corticosteroid treatment.
For patients with aspergillosis, ABPA and severe asthma, the situation can become especially complex because:
- steroid treatment may be medically necessary,
- symptoms overlap with many other conditions,
- antifungal medicines may interact with steroids,
- inhaled steroids may add to total steroid exposure,
- and blood tests are not always straightforward.
Patients sometimes feel frustrated because their symptoms are difficult to explain or measure clearly. However, these experiences are recognised by clinicians and researchers, and steroid-related adrenal problems are increasingly acknowledged as important and sometimes under-recognised.
The goal is not to create fear of steroids. The goal is to use them carefully, monitor them properly, reduce them when possible, and support patients through the difficult process of balancing disease control with treatment side effects.
Suggested internal links
- ABPA treatment overview
- Steroid side effects
- Antifungal drug interactions
- Fatigue and aspergillosis
- Severe asthma and biologics
- Living with long-term aspergillosis
- Mental wellbeing and chronic illness
- Aspergillosis.org Knowledge Hub
References and further reading
When was this article last reviewed?
Last reviewed: May 2026
Author and review information
Prepared for patient education and support purposes.
This article is intended for general educational use and should not replace personalised medical advice from a healthcare professional.
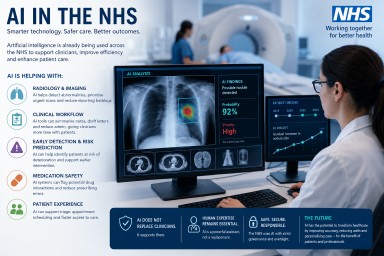
Artificial Intelligence (AI) in the NHS: Promise, Progress and the Future of Healthcare
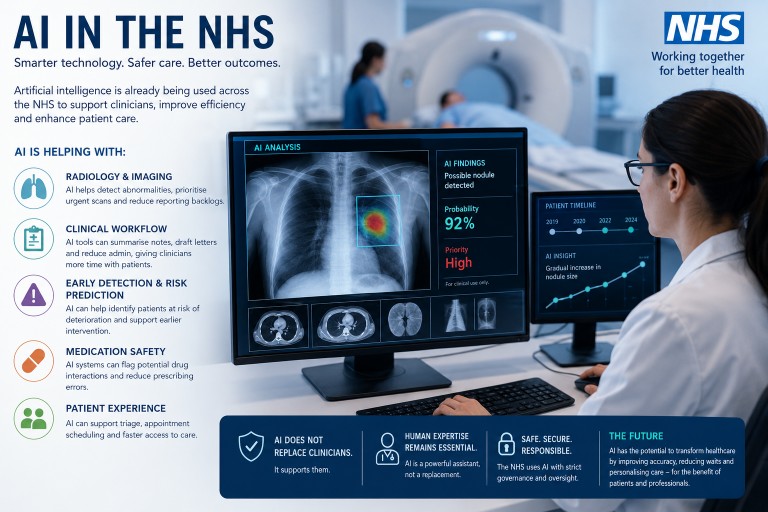
Artificial intelligence (AI) is no longer a futuristic idea within the NHS. AI technologies are already being used in some areas of healthcare across the UK, particularly in radiology, diagnostics, administration and workflow support. However, the reality is more nuanced than many headlines suggest.
At present, AI in the NHS is best understood as a collection of promising technologies being introduced gradually, cautiously and under clinical oversight. Some NHS trusts are using several AI-assisted systems routinely, while others have little or no operational AI deployment beyond pilot projects.
The direction of travel is clear: AI is likely to become an increasingly important part of healthcare over the next decade. However, the NHS is moving carefully because healthcare is a high-risk environment where mistakes can have serious consequences.
What Does AI Mean in Healthcare?
In healthcare, AI usually refers to computer systems that can analyse large amounts of data and identify patterns more quickly or consistently than humans alone.
Examples include:
- Analysing medical scans
- Helping detect cancers or fractures
- Supporting diagnosis
- Summarising clinic consultations
- Reducing paperwork
- Predicting patient deterioration
- Helping prioritise urgent cases
- Supporting medication safety checks
Importantly, most NHS AI systems are currently designed to support clinicians rather than replace them.
AI in NHS Radiology
Radiology is currently one of the biggest areas of AI development within the NHS.
AI systems are being used or trialled to help analyse:
- Chest X-rays
- CT scans
- MRI scans
- Mammograms
- Retinal photographs
- Dermatology images
AI is particularly attractive in radiology because the NHS faces:
- Large radiologist shortages
- Increasing imaging demand
- Growing reporting backlogs
- Rising complexity of scans
How AI Is Currently Used
Most NHS radiology AI systems currently operate in one of three ways:
1. AI as a “Second Reader”
The scan is interpreted by a radiologist, while AI acts as an additional safety check.
AI may flag:
- Possible lung nodules
- Fractures
- Brain bleeds
- Abnormal mammograms
- Signs of stroke
The human clinician still makes the final decision.
2. Prioritisation (“Triage”)
AI can rapidly review scans and move potentially urgent cases higher in the reporting queue.
This may help speed up treatment for:
- Stroke
- Pulmonary embolism
- Pneumothorax (collapsed lung)
- Intracranial bleeding
3. Identifying Likely Normal Scans
Some AI systems are being studied to identify scans that appear very likely to be normal.
The aim is to allow radiologists to focus more attention on:
- Abnormal scans
- Complex cases
- Uncertain findings
However, this remains an area of careful evaluation and regulation.
Does AI Sometimes Perform Better Than Humans?
In certain narrow and repetitive tasks, AI can sometimes outperform humans or help reduce specific types of errors.
AI can be very good at:
- Detecting tiny abnormalities
- Maintaining consistency
- Working without fatigue
- Rapid image analysis
- Comparing huge numbers of images
Humans can become:
- Tired
- Distracted
- Overloaded
- Inconsistent under pressure
For example, AI may detect very small lung nodules or subtle fractures that could potentially be overlooked during a busy reporting session.
However, AI also has important weaknesses.
AI may struggle with:
- Rare diseases
- Complex clinical context
- Unusual anatomy
- Poor-quality scans
- Unexpected combinations of disease
Importantly, AI and humans often make different kinds of mistakes.
The emerging evidence suggests that:
Human + AI is often better than either alone.
Will Radiologists Be Replaced?
At present, the NHS does not view AI as a replacement for radiologists.
Instead, AI is mainly being introduced as:
- A support tool
- A safety net
- A prioritisation system
- A workflow assistant
Radiologists still provide:
- Clinical judgement
- Contextual interpretation
- Decision-making
- Communication
- Management of uncertainty
In the foreseeable future, radiology is likely to become increasingly AI-assisted but still human-led.
Longitudinal Analysis: One of the Most Exciting Future Possibilities
One of the most promising future applications of AI is longitudinal analysis.
This means comparing:
- Current scans
- Previous scans
- Blood tests
- Lung function
- Medications
- Clinical notes
- Symptoms
- Outcomes over time
Humans are not particularly good at consistently recognising very subtle changes across years of imaging and clinical data.
AI could potentially become extremely powerful at:
- Tracking disease progression
- Measuring tumour growth
- Monitoring fibrosis
- Quantifying cavity enlargement
- Identifying treatment response
- Predicting future deterioration
This could be especially valuable in chronic diseases such as:
- Chronic Pulmonary Aspergillosis (CPA)
- Bronchiectasis
- Chronic Obstructive Pulmonary Disease (COPD)
- Interstitial lung disease
- Cancer
In the future, AI may help move medicine from:
“What does this scan show today?”
towards:
“What is happening over time, and what is likely to happen next?”
AI Beyond Radiology
AI Clinical Documentation
The NHS is increasingly exploring AI systems that can generate:
- Clinic letters
- Consultation summaries
- Medical notes
- Coding suggestions
These “AI scribes” may help reduce administrative burden and allow clinicians to spend more time with patients.
AI Triage Systems
Some NHS services now use AI-assisted triage systems to:
- Route patient requests
- Identify urgent problems
- Prioritise appointments
- Support NHS App workflows
Medication Safety
AI may eventually help identify:
- Drug interactions
- Prescribing errors
- Missed monitoring
- Unsafe medication combinations
Operational Efficiency
The NHS is also exploring AI for:
- Appointment scheduling
- Referral management
- Staff rostering
- Reducing missed appointments
- Managing workflow
Why AI Adoption Is Uneven Across the NHS
AI adoption currently varies considerably across the NHS.
Some trusts use multiple AI systems routinely, while others have minimal deployment.
This variation is influenced by:
- Funding differences
- IT infrastructure
- Digital maturity
- Research partnerships
- Clinical confidence
- Procurement complexity
- Availability of evidence
Large teaching hospitals and academic centres often adopt new technologies earlier than smaller hospitals.
As a result, current NHS AI deployment is best described as:
Selective, cautious and evolving.
Why the NHS Is Proceeding Carefully
The NHS is naturally cautious about AI because healthcare is fundamentally different from many other industries.
Mistakes can have serious consequences, including:
- Missed cancers
- Delayed diagnosis
- Medication harm
- Unsafe treatment decisions
For this reason, NHS AI systems generally require:
- Clinical validation
- Governance review
- Safety monitoring
- Regulatory approval
- Human oversight
- Ongoing audit
There is also awareness that:
- commercial hype can exceed evidence,
- real-world NHS workflows are complex,
- and some AI systems may not perform as well outside carefully controlled studies.
Potential Risks and Concerns
Although AI has enormous potential, there are also important concerns.
Patient Safety
AI systems can make mistakes and may occasionally be confidently wrong.
Bias
If training data is incomplete or biased, AI performance may vary between different patient groups.
Loss of Human Contact
Some patients worry that healthcare could become less personal if technology replaces human interaction.
Data Privacy
AI systems often require access to large healthcare datasets, raising understandable questions about confidentiality and data governance.
The Likely Future
The most likely future is probably not:
“AI replaces doctors.”
Instead, it is more likely to be:
“Clinicians increasingly work alongside AI systems.”
AI may gradually become another routine layer of healthcare infrastructure, much as:
- electronic patient records,
- CT scanners,
- MRI scanners,
- and digital pathology systems
became normal parts of modern medicine.
Over time, patients may benefit from:
- Earlier diagnosis
- Safer systems
- More personalised medicine
- Faster reporting
- Reduced waiting times
- Better chronic disease monitoring
However, successful implementation will depend heavily on:
- careful governance,
- good evidence,
- clinical oversight,
- public trust,
- and maintaining the human side of healthcare.
A Balanced Summary
AI in the NHS is already real, but still at an early stage of adoption.
Current use is best described as:
Promising applications in partial use, being introduced gradually and carefully while safety, effectiveness and governance continue to be evaluated.
The NHS is unlikely to move recklessly because healthcare carries high stakes. Instead, adoption will probably continue incrementally, with evidence and clinical confidence building over time.
If implemented wisely, AI has the potential to become one of the most important developments in modern healthcare — not by replacing clinicians, but by helping them deliver safer, faster and more personalised care.
Useful Resources and Further Reading
- NHS England: Artificial Intelligence and Machine Learning
- NHS AI Lab
- NHS AI Knowledge Repository
- NICE: Evidence Standards Framework for Digital Health Technologies
- UK Government: AI Opportunities Action Plan
- Royal College of Radiologists: Artificial Intelligence
- British Institute of Radiology: Artificial Intelligence Special Interest Group
- The Health Foundation: How Could AI Improve the NHS?
- The King’s Fund: Artificial Intelligence and the NHS
- Nature: Artificial Intelligence in Healthcare Collection
- The Lancet Digital Health
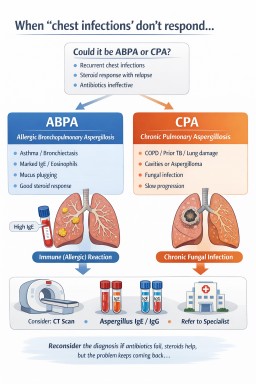
When ‘chest infections’ don’t respond: when to suspect ABPA or CPA (Patient guide)
Patients presenting with recurrent “chest infections” that do not respond to antibiotics are common in primary and secondary care. In a subset of these cases, the underlying cause may not be bacterial, but related to fungal disease or immune-mediated responses to Aspergillus.
This article summarises when to suspect allergic bronchopulmonary aspergillosis (ABPA) or chronic pulmonary aspergillosis (CPA), and how to move from repeated empirical treatment to a more structured diagnostic approach.
Key clinical message
Repeated antibiotic-treated exacerbations with limited response, particularly when symptoms improve with steroids and then relapse, should prompt reconsideration of the diagnosis.
When to suspect ABPA or CPA
Consider aspergillosis-related disease in patients with:
- Recurrent “chest infections” with poor or inconsistent antibiotic response
- Steroid-responsive symptoms with relapse on reduction or cessation
- Persistent or unexplained radiological abnormalities
- Underlying lung disease:
- Asthma
- Bronchiectasis
- Chronic obstructive pulmonary disease (COPD)
- Previous tuberculosis or lung damage
- Raised or previously documented abnormalities in:
- Total IgE
- Eosinophils
- Aspergillus-specific markers (if previously tested)
These features are not diagnostic in isolation but should raise suspicion when seen together.
ABPA vs CPA: clinical distinction
| Feature | ABPA | CPA |
|---|---|---|
| Primary mechanism | Immune-mediated (allergic) | Chronic fungal infection |
| Typical background | Asthma, bronchiectasis | Structural lung disease, prior TB, COPD |
| Steroid response | Often marked | Variable (may improve symptoms but not disease) |
| Antibiotic response | Limited | Limited |
| Radiology | Mucus plugging, bronchiectasis | Cavities, fungal balls, fibrosis |
Common pitfalls in practice
- Repeated empirical antibiotics despite poor response
- Short courses of steroids without a long-term management plan
- Reliance on chest X-ray alone in persistent or atypical cases
- Failure to recognise patterns across multiple consultations or admissions
These patterns can lead to prolonged diagnostic delay, which is well described in CPA and ABPA.
Suggested diagnostic approach
1. Reassess the working diagnosis
When standard treatment fails, explicitly reconsider whether the presentation remains consistent with bacterial infection.
2. Imaging
- Escalate from chest X-ray to CT thorax where appropriate
- Look for:
- Cavitation
- Fungal ball (aspergilloma)
- Mucus plugging
- Bronchiectasis
3. Blood tests
- Total IgE
- Eosinophil count
- Aspergillus-specific IgE and IgG (where available)
4. Microbiology / further testing
Depending on context, consider sputum culture, fungal markers, or specialist input.
The steroid–relapse pattern
A common clinical scenario:
Exacerbation → steroids → improvement → relapse
This should raise suspicion of an underlying inflammatory or fungal-driven process rather than recurrent bacterial infection alone.
When to consider referral
Referral to a specialist centre (e.g. National Aspergillosis Centre, Manchester) may be appropriate where:
- Diagnosis remains uncertain
- Symptoms are persistent or progressive despite treatment
- Antifungal therapy is being considered or not tolerated
- Radiology suggests CPA or complex disease
Referral decisions should be made in the context of overall patient condition, comorbidities, and goals of care.
Why diagnosis is often delayed
- Overlap with common respiratory conditions
- Partial response to standard therapies
- Fragmentation across care settings
- Limited exposure to aspergillosis in routine practice
Recognising the pattern is often the key step in reducing delay.
Practical takeaways
- If antibiotics are not working, reconsider the diagnosis
- If steroids repeatedly improve symptoms, ask why
- Use CT imaging to clarify persistent abnormalities
- Aim for a clear, shared management plan
Guidelines and further reading
Which guideline should I use?
In UK practice, the British Thoracic Society (BTS) statement provides the most directly applicable clinical guidance. The ISHAM guidelines offer detailed international consensus, particularly for ABPA. Both are complementary and widely used.
- British Thoracic Society (BTS)
Clinical Statement on Aspergillus-related chronic pulmonary disease
UK guidance covering diagnosis and management of ABPA, CPA, and related conditions.
View BTS clinical statement
- International Society for Human and Animal Mycology (ISHAM)
Revised clinical practice guidelines for allergic bronchopulmonary aspergillosis/mycoses
International consensus guidance on diagnosis, classification, and management of ABPA.
View ISHAM guideline (European Respiratory Journal)
- Chronic Pulmonary Aspergillosis (CPA) guidelines
Denning DW et al. Chronic pulmonary aspergillosis: rationale and clinical guidelines for diagnosis and management
View PubMed record
Further professional resources
For clinician-focused guidance, referral pathways, and educational material:
https://aspergillosis.org/information-for-professionals/
This article is intended for educational purposes and should be interpreted in the context of individual clinical judgement.
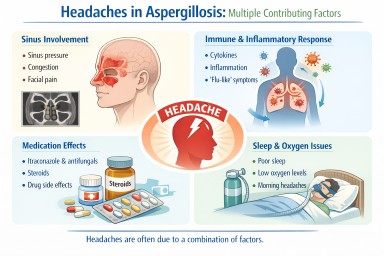
Why Headaches Can Occur in Aspergillosis
Last reviewed: March 2026
Key Points
- Headaches are relatively common in people living with aspergillosis, but they usually have multiple contributing causes.
- Common causes include sinus involvement, inflammation, sleep disturbance, and medication effects.
- Antifungal medicines such as itraconazole may improve some symptoms indirectly but can also occasionally cause headaches.
- Patterns (timing, location, triggers) can help identify likely causes, but headaches are rarely due to one factor alone.
- New, severe, or unusual headaches should always be assessed by a healthcare professional.
Table of Contents
- Overview
- Sinus involvement (common cause)
- Inflammation and immune response
- Allergic-type responses (e.g. ABPA)
- Medication effects
- Sleep disturbance and night symptoms
- Breathing and oxygen levels
- General health factors
- Understanding headache patterns
- Common questions
- When to seek medical advice
- Summary
- Author and review
- References
Overview
Many people living with aspergillosis report headaches at some point during their illness. These headaches can vary in type, severity, and timing, and may be confusing—especially when they change over time or seem linked to treatment.
In most cases, headaches are not caused by a single factor. Instead, they reflect a combination of:
- local effects (such as sinus pressure)
- immune system activity
- medication effects
- sleep and general health factors
Understanding these different contributors can help make sense of symptoms and support more informed discussions with your clinical team.
Sinus involvement (common cause)
When Aspergillus affects the sinuses (sometimes called fungal sinusitis), this can directly cause headaches.
This happens because:
- sinus drainage becomes blocked
- pressure builds up in the sinus cavities
- the lining of the sinuses becomes inflamed
Typical features:
- pain or pressure in the forehead, cheeks, or behind the eyes
- worsening when bending forward
- a feeling of fullness or congestion
This is one of the most direct ways aspergillosis can lead to headaches.
Inflammation and immune response
Even when the sinuses are not directly involved, the body’s immune response to fungal material can cause systemic effects.
The immune system releases signalling molecules (such as cytokines) that can:
- increase inflammation
- affect blood vessels
- trigger headache pathways
This type of headache can feel similar to a “flu-like” or inflammatory headache.
Allergic-type responses (e.g. ABPA)
In conditions such as Allergic Bronchopulmonary Aspergillosis (ABPA), the immune system reacts strongly to Aspergillus.
This may involve:
- allergic pathways
- histamine and related mediators
- ongoing airway inflammation
Possible symptoms:
- head pressure or discomfort
- fluctuating headaches
- a “foggy” or unwell feeling
These headaches are often less clearly localised than sinus-related pain.
Medication effects
Some treatments used in aspergillosis can contribute to headaches.
Antifungal medications (e.g. itraconazole):
- headache is a recognised side effect in some people
- effects vary between individuals
Steroids (if prescribed):
- can affect sleep and mood
- may influence blood pressure
- can indirectly contribute to headaches
Medication effects can sometimes overlap with disease-related symptoms, making patterns harder to interpret.
Sleep disturbance and night symptoms
Sleep disruption is common in chronic lung conditions.
Possible contributors include:
- night-time coughing
- breathlessness
- discomfort or anxiety
Poor sleep can lead to:
- morning headaches
- increased sensitivity to pain
- fatigue-related headaches
Breathing and oxygen levels
In some people with more advanced lung involvement:
- oxygen levels may be slightly reduced
- breathing effort may increase
This can contribute to:
- morning headaches
- fatigue and cognitive symptoms
Not all patients experience this, but it is an important factor in some cases.
General health factors
Headaches can also be influenced by general aspects of living with a long-term condition:
- dehydration
- fatigue
- reduced activity levels
- stress or anxiety
These factors can contribute to tension-type headaches or make other headache types more noticeable.
Understanding headache patterns
Looking at patterns can sometimes help identify likely contributors.
- Facial pressure worse on bending: may suggest sinus involvement
- Early morning headaches: may relate to sleep or breathing patterns
- Fluctuating or “wave-like” symptoms: may reflect inflammation or immune activity
- New headaches after starting medication: may be treatment-related
However, these are general observations only and do not replace clinical assessment.
Headaches in Aspergillosis: Interactive Decision Aid
This tool helps patients and carers think about common patterns that can contribute to headaches in aspergillosis. It does not diagnose the cause of a headache.
It is designed to support discussion with a healthcare professional and highlight possible contributors such as sinus involvement, inflammation, medication effects, sleep disturbance, and breathing-related factors.
1. Where is the pain mainly felt?
2. When is it most noticeable?
3. What does it feel like?
4. What other features are present?
5. Are there any red flags?
Possible contributors
This panel highlights common patterns only. It is not a diagnosis and does not replace medical assessment.
Common questions
Are headaches a recognised symptom of aspergillosis?
They can occur, but are usually indirect and caused by associated factors such as sinus disease or inflammation.
Can antifungal treatment improve headaches?
In some cases, yes—if symptoms are linked to fungal-related inflammation. However, antifungals can also occasionally cause headaches as a side effect.
Are “histamine-type” headaches part of aspergillosis?
Some patients describe symptoms in this way, but the underlying mechanism is often more complex than histamine alone.
Why do my headaches change over time?
This is common and may reflect changes in inflammation, treatment, sleep, or overall health.
When to seek medical advice
You should seek medical advice if you experience:
- new or unusually severe headaches
- headaches that are worsening over time
- neurological symptoms (e.g. vision changes, weakness, confusion)
- fever, neck stiffness, or other concerning symptoms
If you are unsure whether your headaches are related to aspergillosis, treatment, or another cause, it is important to discuss this with your healthcare team.
Summary
Headaches in people with aspergillosis are usually caused by a combination of factors rather than a single issue.
The most common contributors include:
- sinus involvement
- immune and inflammatory responses
- sleep disturbance
- medication effects
Understanding patterns and changes over time can be helpful, but medical assessment is important if symptoms are new, severe, or concerning.
Author and review
Prepared for: aspergillosis.org
Audience: Patients and non-specialist readers
Important: This article is for general information only and does not replace individual medical advice.
References
- Patterson TF et al. (2016). Practice Guidelines for the Diagnosis and Management of Aspergillosis.
PMID: 27365388 - Denning DW et al. (2016). Chronic pulmonary aspergillosis guidelines.
PMID: 26699723 - Chakrabarti A et al. (2009). Fungal sinusitis: a categorization and definitional schema.
PMID: 19522756
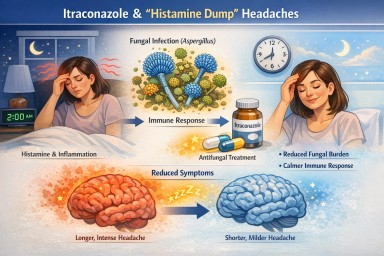
Why Do My “Histamine” Headaches Improve on Itraconazole?
Last reviewed: March 2026
Key Points
- Itraconazole is an antifungal medicine. It is not an antihistamine.
- Some people notice that symptoms such as headaches, flushing, or a “histamine-type” feeling become shorter or less intense after starting treatment.
- This is most likely because itraconazole reduces the fungal burden and the immune response it triggers, rather than blocking histamine directly.
- Symptoms that happen in the early hours of the morning may also be influenced by the body’s natural day-night rhythm.
- Changes in symptoms can be helpful clues, but headaches can have more than one cause.
Table of Contents
- Overview
- What is itraconazole and how does it work?
- What do people mean by “histamine dump” headaches?
- Why might symptoms improve on itraconazole?
- Why do symptoms often happen at night?
- Does this mean histamine is the main problem?
- Common questions
- When to seek medical advice
- Summary
- Author and review
- References
Overview
Some people taking itraconazole for non-lung or lung forms of aspergillosis notice that symptoms they describe as “histamine-type” symptoms, such as headaches, flushing, pressure, or a general sense of inflammatory overload, become shorter or less severe.
A typical pattern might be:
- Symptoms start overnight, for example, around 2 am
- Symptoms previously lasted most of the day
- Symptoms are now settling much earlier after starting treatment
This can be confusing, especially when the symptoms feel similar to a histamine reaction. The important point is that itraconazole does not work like an antihistamine, but it can reduce symptoms indirectly if a fungal process is contributing to them.
What is itraconazole and how does it work?
Itraconazole is an antifungal medicine used to treat infections caused by fungi such as Aspergillus.
It works by interfering with the production of ergosterol, an essential part of the fungal cell membrane. This weakens the fungus and helps reduce fungal growth and survival in the body.
As the fungal burden falls, the immune system may be less strongly stimulated, and that can lead to a reduction in inflammation-related symptoms.
So although itraconazole does not block histamine directly, it may reduce the underlying trigger that is causing the body to react.
What do people mean by “histamine dump” headaches?
“Histamine dump” is not a formal medical diagnosis, but some patients use it as a practical way of describing symptoms such as:
- sudden headaches, especially overnight or early in the morning
- flushing or a feeling of heat
- pressure in the head or sinuses
- a sense of being “wired”, agitated, or unwell
These symptoms may involve histamine, but they can also reflect broader inflammation, immune activation, mast cell activity, or other signalling chemicals in the body.
Why might symptoms improve on itraconazole?
If itraconazole is helping, it is most likely doing so indirectly. There are several possible reasons for this.
1. Reduced fungal burden
If fungal material in the body is reduced, there may be less for the immune system to react to. That can mean less inflammatory signalling overall.
2. Reduced immune activation
Fungi can stimulate the immune system in ways that lead to inflammation and, in some people, histamine-related symptoms. If antifungal treatment lowers that stimulus, symptoms may become less intense or settle more quickly.
3. Shorter inflammatory response
Some people find that the symptom still begins, but does not “run on” for as long. For example, a headache that used to last from 2am until late afternoon may now settle by 5am.
Why do symptoms often happen at night?
The body has a natural circadian rhythm, a 24-hour cycle that affects hormones, inflammation, sleep, and immune activity.
- Some inflammatory signals can be more noticeable overnight
- Cortisol rises in the early morning, and helps suppress inflammation
Does this mean histamine is the main problem?
Not necessarily. Symptoms may involve multiple pathways, including immune response to fungi, general inflammation, mast cell activity, and sinus pressure.
Common questions
Does itraconazole act like an antihistamine?
No. It does not block histamine receptors.
Why are my symptoms improving but not gone?
This is common and may reflect partial control of the underlying trigger.
Does this prove Aspergillus is the cause?
No. It suggests a possible link but does not confirm causation.
Will symptoms continue to improve?
Possibly, but responses vary between individuals.
When to seek medical advice
- new or severe headaches
- neurological symptoms (vision, speech, balance)
- worsening or persistent symptoms
- concerns about medication side effects
Summary
Itraconazole does not directly affect histamine but may reduce symptoms by lowering fungal burden and immune activation.
Author and review
Prepared for: aspergillosis.org
Audience: Patients and non-specialist readers
Important: This does not replace individual medical advice.
References
- Patterson TF, Thompson GR 3rd, Denning DW, et al. (2016).
Practice Guidelines for the Diagnosis and Management of Aspergillosis.
View on PubMed (PMID: 27365388) - Denning DW et al. (2016).
Chronic pulmonary aspergillosis guidelines.
View on PubMed (PMID: 26699723) - Barnes PJ, Adcock IM (2009).
Circadian rhythm in airway disease.
View on PubMed (PMID: 19336589) - Stone KD et al. (2010).
IgE, mast cells, and eosinophils.
View on PubMed (PMID: 20176269)
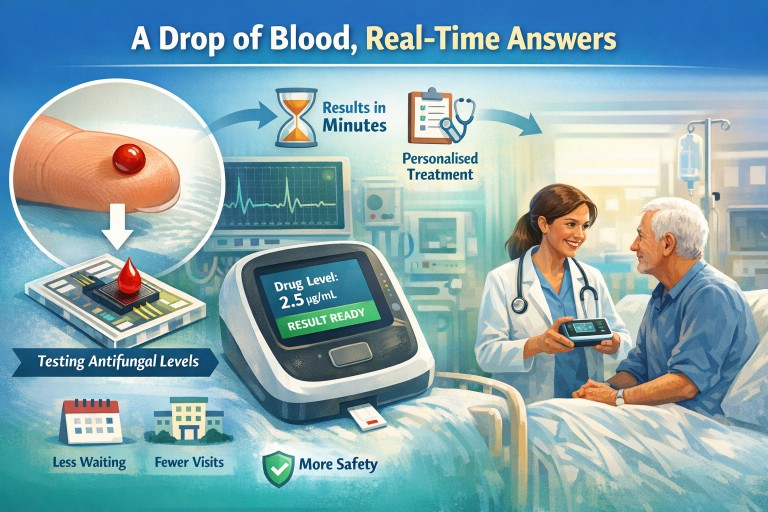
A Drop of Blood, Real-Time Answers
Last reviewed: 20 March 2026
Audience: Patients, carers, families, and non-specialists
Topic: Point-of-care monitoring of antifungal drug levels
New bedside testing for antifungal drugs — and why patients welcome it
For many people taking antifungal medicines, blood tests are an important part of care. These tests help doctors check whether the amount of medicine in the body is too low, too high, or about right.
A new type of technology is being developed to do this much more quickly, using just a single drop of blood placed onto a specialised chip. Instead of sending blood away to a laboratory and waiting days for a result, this kind of test may be able to provide an answer much more quickly, sometimes during the clinic visit itself.
Patients in a recent focus group responded very positively to this idea. They welcomed not only the technology itself, but also what it could mean for their care: less waiting, less uncertainty, fewer trips to hospital, and more personalised treatment.
Key points
- A new test can measure antifungal drug levels from a drop of blood.
- The blood is placed on a specialised chip containing tiny sensors.
- Results may be available much faster than standard laboratory testing.
- This could help doctors adjust treatment more quickly and more precisely.
- Patients in a focus group strongly welcomed the technology.
- Reported benefits included less anxiety, fewer hospital visits, and more confidence in treatment decisions.
What is this new test?
This is a type of point-of-care test. That means it is designed to be used close to the patient, such as in a clinic or at the bedside, rather than sending the sample away to a central laboratory.
In this case, the aim is to measure the level of an antifungal drug in the blood from a very small sample, sometimes just a finger-prick drop. The drop of blood is placed onto a specialised chip. That chip contains tiny channels and sensors that can detect the amount of drug present.
People sometimes describe this type of system as a “lab on a chip” because it performs some of the work of a laboratory in a very small device.
How does the technology work?
The exact science varies between devices, but the general idea is similar.
- A small blood sample is taken.
This may be from a finger prick rather than a larger blood draw. - The blood is placed onto a specialised chip.
The chip is designed to handle a tiny volume of blood. - The blood moves through microscopic channels.
These channels guide the sample to the parts of the chip that do the measurement. - Sensors on the chip detect the antifungal drug.
These sensors are designed to recognise the drug or react to it in a measurable way. - A reader produces a result.
A connected device reads the signal from the chip and estimates the drug level.
Some systems use electrical signals, some use light, and some use chemical reactions. Patients do not need to understand all the engineering details to understand the main point: the chip is acting like a mini laboratory.
A simple way to think about it is this:
Instead of sending your blood sample to a distant laboratory, this technology brings part of the laboratory to your fingertip.
Why do antifungal drug levels matter?
Some antifungal medicines need careful monitoring because the “right” level can be quite important.
If the drug level is too low, the medicine may not work well enough. If the drug level is too high, side effects may become more likely.
This can be especially relevant for antifungal drugs such as:
- itraconazole
- voriconazole
- posaconazole
Drug levels can vary from person to person for many reasons, including:
- how well the body absorbs the medicine
- interactions with other medicines
- differences in liver function and metabolism
- changes in health over time
At present, monitoring usually involves sending blood to a laboratory. That works, but it can mean delays. Results may not come back quickly enough to guide decisions during the clinic appointment itself.
A faster bedside test could help clinicians make treatment decisions more quickly and could support more personalised care.
What did patients say about it?
In the patient focus group, this technology was widely welcomed. Patients were not only interested in the novelty of the test. They also recognised several practical benefits that could make day-to-day care easier and safer.
1. Faster results could reduce anxiety
Many patients described the stress of waiting for test results. Waiting can create a sense of uncertainty: Is the treatment working? Is the dose correct? Are side effects more likely?
A test that gives much quicker results was seen as reassuring. Instead of waiting days, patients liked the idea of getting answers much sooner, possibly while still in clinic.
2. Fewer visits could reduce the burden of care
For many people with chronic lung conditions or long-term illness, going to hospital is not a small task. Travel, parking, breathlessness, fatigue, mobility problems, and long waits can make even a short appointment exhausting.
Patients felt that a faster and simpler test could reduce some of this burden, especially if it could be built into a normal appointment or eventually be offered closer to home.
3. More personalised dosing felt important
Patients often understand from experience that medicines do not affect everyone in the same way. One person may tolerate a treatment well, while another may have side effects or absorb the medicine differently.
Because of this, patients valued the idea that treatment could be adjusted based on their own measured drug level, rather than relying only on standard dosing. This gave a stronger sense that care was being tailored to the individual.
4. Closer monitoring gave reassurance about safety
Antifungal drugs can be very helpful, but patients also know that some of them can have side effects and interactions. That can make treatment feel worrying, especially over longer periods.
Patients said that being able to check drug levels more quickly and more easily could help them feel safer. It suggested that treatment was being watched closely rather than left unchecked between appointments.
5. Immediate results could help patients feel more involved
Another important theme was involvement. Patients often feel that blood is taken, results disappear into the system, and decisions come later without much real-time discussion.
By contrast, a bedside result creates the possibility of discussing the number there and then. Patients felt this could help them better understand their treatment and feel more involved in decisions about dose changes and ongoing care.
6. It seemed to fit better with real life
Patients repeatedly emphasised that long-term treatment has to fit around real lives, not just clinic systems. Many welcomed the idea of a test that was quicker, simpler, and potentially more convenient.
In that sense, what patients welcomed was not just a chip or a machine, but a model of care that felt more responsive and more human-centred.
What could this mean for future care?
If this technology proves accurate, reliable, and affordable, it could support a different way of monitoring antifungal treatment.
Possible future benefits could include:
- drug level testing during the clinic appointment itself
- faster dose adjustment when levels are too high or too low
- closer monitoring when starting or changing treatment
- fewer repeat visits just to check blood levels
- potential future use in community settings or, one day, at home
It is important to be realistic. New technologies must be carefully tested before they become routine. They need to be shown to be accurate, dependable, and practical in real healthcare settings.
Even so, patients clearly recognised the potential. For them, this is not just about speed. It is about moving toward care that is:
- more responsive
- more personalised
- more convenient
- less anxiety-provoking
Common questions
Is this available now?
Usually not as a routine test in most healthcare settings. It is still being developed and studied, although interest in this type of monitoring is growing.
Will this replace ordinary blood tests?
Not immediately. Standard laboratory testing is still important. New bedside systems may first be used alongside existing methods while they are being evaluated and introduced.
Would this work for every antifungal drug?
Not necessarily. Some devices may be designed for specific drugs first. Wider use would depend on the technology and the evidence supporting it.
Could this be used at home?
Possibly one day, but that is likely to depend on how reliable, affordable, and easy to use the technology becomes. For now, clinic or bedside use is the more immediate possibility.
Why is a drop-of-blood test appealing to patients?
Because it may mean quicker answers, less uncertainty, fewer hospital trips, and more confidence that treatment decisions are based on what is happening in their own body.
When to seek medical advice
You should contact your healthcare team if you:
- develop new or worsening side effects from your antifungal medicine
- feel your treatment is not helping
- have concerns about drug interactions with other medicines
- are unsure whether to continue, stop, or change your medication
A new bedside test could support treatment decisions, but it would not replace medical advice. Symptoms, scans, blood tests, and clinical review would still matter.
Final thoughts
This new chip-based bedside technology may sound futuristic, but the reason patients welcomed it is very straightforward.
They saw the possibility of care that is faster, clearer, safer, and better adapted to real life.
In other words, this is about more than measuring a drug level from a drop of blood. It is about moving away from delayed, one-size-fits-all monitoring and toward real-time, personalised, patient-centred care.
In one sentence
A tiny chip and a drop of blood could help doctors adjust antifungal treatment more quickly — and patients believe that could make care less stressful, less burdensome, and more personal.
Author: Graham Atherton and ChatGPT draft support
For review by: National Aspergillosis Centre / relevant clinical or research reviewer
Note: This article is for general information and should not be used as a substitute for medical advice.
When Symptoms Are Real but Answers Are Not: Understanding Uncertainty
Last reviewed: 18 March 2026
Key points
- Many people experience a period where symptoms are real but no clear diagnosis has been made.
- This can sometimes feel like being told “nothing is wrong” or “it is all in your head”.
- In most cases, this reflects uncertainty in the system, not disbelief from clinicians.
- Conditions such as aspergillosis can take time to become recognisable.
- Physical and psychological factors can overlap—but unexplained symptoms are still real symptoms.
- Clear communication and ongoing review are key to moving forward.
The experience many patients describe
During a long diagnostic journey, many people reach a point where they hear phrases such as:
- “Your tests are normal”
- “We can’t find anything serious”
- “It may be stress or anxiety contributing”
Even when these words are carefully chosen, they can feel like:
“Nothing is wrong” or “it’s all in my head”
This can be one of the most difficult parts of the journey—especially when symptoms are ongoing, disruptive, and clearly real.
Why this happens
This situation usually reflects the limits of current medical systems rather than a lack of concern.
Tests do not always give clear answers
Modern medicine relies heavily on tests. But for many conditions—including chronic pulmonary aspergillosis (CPA)—tests may:
- be negative early on
- show unclear or borderline results
- require interpretation over time
This creates a gap between:
- what the patient is experiencing
- what can currently be measured
Medicine is designed to provide answers
Clinicians are trained to explain symptoms and reassure patients. When no clear diagnosis is available, they may turn to explanations such as:
- stress
- anxiety
- functional symptoms
These are real and valid factors—but if introduced too early, they can feel like the search has stopped.
Time pressure
Short consultations can mean:
- less time to explain uncertainty
- less opportunity to validate patient experience
- simplified explanations that lose nuance
What doctors mean vs what patients hear

Often, the issue is not what is said—but how it is understood.
| What may be said | What may be heard |
|---|---|
| “Your tests are normal” | “Nothing is wrong” |
| “We haven’t found a cause yet” | “There is no cause” |
| “Stress may be contributing” | “It’s all in your head” |
Understanding this gap can help both patients and clinicians move forward more constructively.
A critical clarification
Not having a diagnosis is not the same as not having a disease.
Unexplained symptoms are still real symptoms.
Medicine does not always have immediate answers—especially for conditions that develop slowly or do not fit standard patterns.
Physical and psychological overlap
It is important to take a balanced view.
- Physical illness can lead to anxiety, fatigue, and distress
- Anxiety can worsen physical symptoms such as breathlessness
This relationship is two-way, not either/or.
The problem arises when psychological explanations replace further investigation, rather than sitting alongside it.
Why this matters in aspergillosis
Conditions such as aspergillosis often:
- develop gradually
- have non-specific symptoms
- require multiple tests over time
This makes periods of uncertainty more likely, particularly before a diagnosis such as allergic bronchopulmonary aspergillosis (ABPA) or CPA is confirmed.
You can read more about this in Why Aspergillosis Is So Hard to Diagnose.
What patients can do
- Keep a record of symptoms and how they change over time
- Ask what the current working diagnosis is
- Ask when the situation should be reviewed
- Share concerns clearly, but remain open to different explanations
Helpful questions include:
- “What else could this be?”
- “What would make you reconsider the diagnosis?”
- “When should we review this again?”
A shared understanding
This situation is not about:
- patients being dismissed
- clinicians not caring
It reflects a deeper reality:
Medicine does not always have immediate answers—especially for complex or evolving conditions.
The goal is to keep the process open, respectful, and moving forward.
Common questions
Does this mean doctors think I’m imagining symptoms?
No. It usually reflects uncertainty rather than disbelief.
Can stress really affect physical symptoms?
Yes—but this should not stop appropriate medical investigation.
What should I do if I feel dismissed?
Ask for clarification, a review plan, or a second opinion if needed.
Related pages
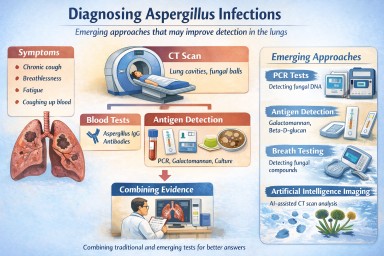
Clinical Trials and Emerging Diagnostics for Aspergillus Infections
How new diagnostic technologies may improve detection of Aspergillus lung infections
Last reviewed: March 2026
Author: Graham Atherton
Key points
- Diagnosing Aspergillus lung infections can be challenging because symptoms often resemble other lung diseases.
- Doctors usually combine CT scans, blood tests and microbiology tests to make a diagnosis.
- Researchers are developing new diagnostics that detect fungal DNA, fungal molecules, or drug-resistant strains.
- Emerging tools include PCR tests, antigen detection, rapid tests, sequencing technologies and artificial intelligence imaging.
- This page focuses on Aspergillus infections rather than allergic conditions such as Allergic Bronchopulmonary Aspergillosis, Severe Asthma with Fungal Sensitisation, or Aspergillus bronchitis.
- Many of these newer technologies are being studied in clinical trials and research programmes worldwide.
Table of contents
- 1. Important note: infection vs allergy
- 2. Why better diagnostics are needed
- 3. How Aspergillus infections are diagnosed today
- 4. Detecting the immune response vs detecting the fungus
- 5. Simple diagram: two ways of looking for Aspergillus disease
- 6. DNA testing (PCR diagnostics)
- 7. Fungal antigen detection
- 8. Rapid diagnostic tests
- 9. Breath diagnostics
- 10. Sequencing technologies and the lung microbiome
- 11. Detecting antifungal resistance
- 12. Artificial intelligence and CT imaging
- 13. Flowchart: how doctors diagnose chronic Aspergillus infection
- 14. The future diagnostic pathway
- 15. Common questions patients ask
- 16. When to seek medical advice
- 17. References
1. Important note: infection vs allergy
This article focuses on diagnosing Aspergillus infections of the lungs, particularly:
- Chronic Pulmonary Aspergillosis
- Aspergillus nodules
- Aspergilloma (fungal ball)
- Subacute invasive aspergillosis
These conditions involve the fungus growing in lung tissue or in pre-existing lung cavities.
This is different from allergic Aspergillus disease, such as:
- Allergic Bronchopulmonary Aspergillosis (ABPA)
- Severe Asthma with Fungal Sensitisation (SAFS)
- Aspergillus bronchitis (which overlaps with airway disease rather than the classic cavity-forming infections discussed here)
In allergic disease, diagnosis focuses more on immune reactions, such as IgE antibodies, eosinophils, allergy testing and markers of Type 2 inflammation.
This page therefore focuses mainly on diagnostics for Aspergillus infection rather than allergy. A separate article can cover immune diagnostics in allergic Aspergillus disease.
2. Why better diagnostics are needed
Chronic Pulmonary Aspergillosis often develops in people who already have damaged lungs, for example from:
- tuberculosis
- Chronic Obstructive Pulmonary Disease
- bronchiectasis
- sarcoidosis
- previous severe lung infections
- lung surgery
Symptoms may include:
- chronic cough
- breathlessness
- fatigue
- weight loss
- coughing up blood
- chest discomfort
These symptoms are not specific, meaning they can occur in many other lung diseases.
Aspergillus is also very common in the environment, so detecting it in sputum does not always mean it is causing disease. Sometimes it may simply be present without invading tissue or causing progressive damage.
For these reasons, diagnosing chronic aspergillosis usually requires multiple tests interpreted together, rather than relying on one result alone.
3. How Aspergillus infections are diagnosed today
Doctors usually combine three main types of evidence.
| Diagnostic method | What it shows |
|---|---|
| CT scan | Structural lung changes such as cavities, nodules or fungal balls |
| Blood tests | The body's immune response to Aspergillus |
| Microbiology tests | Evidence of the fungus itself |
The most important blood test for many patients with Chronic Pulmonary Aspergillosis is Aspergillus IgG antibodies.
CT scans are also critical because they can reveal features such as:
- lung cavities
- fungal balls
- nodules
- thickened cavity walls
- progressive lung destruction or scarring
Microbiology may include sputum culture, bronchoscopy samples, microscopy, molecular testing and antigen detection.
No single test is perfect. Doctors usually look at the whole picture: symptoms, scan findings, blood tests, microbiology, and how things change over time.
4. Detecting the immune response vs detecting the fungus
Some diagnostic tests detect how the body reacts to Aspergillus, while others try to detect the fungus itself.
Immune response tests
Examples include:
- Aspergillus IgG antibodies
- general inflammatory markers
These tests show that the immune system has encountered Aspergillus, but they do not always prove that the fungus is currently active, growing, or causing ongoing damage.
Direct fungal detection
Other tests look for components of the fungus itself.
| Test | What it detects |
|---|---|
| PCR | Aspergillus DNA |
| Galactomannan | Fungal cell wall molecules |
| Beta-D-glucan | Fungal structural components |
| Culture | Growth of the fungus in the laboratory |
These tests can sometimes provide more direct evidence that fungal material is present.
Why not rely only on the immune response?
Immune-response tests are extremely useful, but they are indirect. They tell us what the body is doing, not necessarily what the fungus is doing at that moment.
Antibodies may remain raised for quite a long time, may change only slowly, and may vary from person to person. Some patients also produce weaker immune responses than others.
By contrast, tests that detect fungal DNA or fungal cell wall components may sometimes give a better sense that fungal material is actually present in the lungs.
The footprints analogy
A useful way to understand this difference is:
- Immune response tests are like seeing footprints in the snow – they show that someone has been there.
- Direct fungal tests are like seeing the person themselves – they show that the organism is present.
In practice, doctors usually combine both kinds of evidence to make the diagnosis more reliable.
5. Simple diagram: two ways of looking for Aspergillus disease
Two broad diagnostic approaches
| Approach | Examples | Main question |
|---|---|---|
| Looking for the body's response | Aspergillus IgG, inflammation markers | Has the immune system reacted to Aspergillus? |
| Looking for the fungus itself | PCR, galactomannan, Beta-D-glucan, culture | Is fungal material present? |
| Looking for damage caused in the lungs | CT scan | Has Aspergillus or another disease caused structural lung change? |
This is why diagnosis is usually based on a combination of evidence rather than any single test.
6. DNA testing (PCR diagnostics)
Polymerase Chain Reaction, usually shortened to PCR, detects the DNA of Aspergillus fungi.
These tests can be performed on samples such as:
- sputum
- bronchoscopy samples
- lung tissue
Advantages of PCR include:
- faster results than fungal culture
- detection of very small amounts of fungus
- possible detection even when cultures are negative
However, PCR also has challenges. It may detect fungal material even when it is not clearly causing disease, and methods are not yet fully standardised across all laboratories.
Even so, PCR is one of the most important emerging tools in fungal diagnostics and is increasingly used in specialist centres.
7. Fungal antigen detection
Some tests look for molecules released by fungal cells. These are often called antigen tests.
Galactomannan
Galactomannan is a molecule found in the cell wall of Aspergillus.
It is already widely used in diagnosing invasive aspergillosis and is being studied more closely in chronic forms of disease as well.
Beta-D-glucan
Beta-D-glucan is a structural component found in the cell walls of many fungi.
Raised levels can suggest fungal infection somewhere in the body, although it is not specific for Aspergillus alone.
Researchers are interested in how these markers might be used alongside CT, antibody testing and PCR to improve accuracy.
8. Rapid diagnostic tests
Researchers are also developing rapid antigen tests that can detect fungal molecules within minutes.
These tests work in a similar way to a simple strip test and may offer:
- quick results
- minimal laboratory equipment
- possible use in clinics with fewer resources
These tests are promising, but they still need careful evaluation to show how accurate and reliable they are in real patients with chronic Aspergillus disease.
9. Breath diagnostics
Fungi release small chemicals called volatile organic compounds. Some experimental devices aim to detect these compounds in exhaled breath.
If successful, breath testing could provide:
- completely non-invasive testing
- rapid screening
- repeat testing over time without invasive procedures
This remains an early and experimental field, but it is attractive because it could make testing much easier for patients.
10. Sequencing technologies and the lung microbiome
Modern sequencing technologies can analyse all microbial DNA in a sample.
This means they may identify:
- fungi
- bacteria
- viruses
These approaches may help doctors understand mixed infections and the broader lung microbiome, especially in people with bronchiectasis or complex chronic lung disease.
In the future, sequencing may help explain why some patients have persistent symptoms or repeated flares involving more than one organism.
11. Detecting antifungal resistance
Some strains of Aspergillus fumigatus have developed resistance to azole antifungal drugs.
Newer diagnostic tests can detect genetic mutations linked to drug resistance, especially in the CYP51A gene.
Earlier detection of resistance could help doctors:
- choose effective antifungal drugs sooner
- avoid ineffective treatment
- improve long-term outcomes
This is an important area of research because antifungal resistance is a growing international concern.
12. Artificial intelligence and CT imaging
Artificial intelligence is increasingly being explored as a way to analyse CT scans more precisely.
These systems may eventually help doctors:
- detect subtle lung changes earlier
- measure cavity size or progression more consistently
- monitor disease over time
- compare scans more accurately
Artificial intelligence is unlikely to replace expert radiologists or specialist teams, but it may become a useful support tool.
13. Flowchart: how doctors diagnose chronic Aspergillus infection
Typical diagnostic pathway
Symptoms
persistent cough, breathlessness, fatigue, weight loss, coughing up blood
↓
CT scan
looking for cavities, fungal balls, nodules, scarring or progressive damage
↓
Blood tests
especially Aspergillus IgG and general inflammatory markers
↓
Microbiology
sputum, bronchoscopy, culture, PCR, antigen tests
↓
Clinical interpretation
combining symptoms, imaging, blood tests and microbiology
↓
Diagnosis and follow-up
deciding whether this is infection, colonisation, another lung condition, or mixed disease
This flowchart is simplified, but it shows the basic principle: diagnosis depends on combining evidence.
14. The future diagnostic pathway
In the future, diagnosing Aspergillus infection may involve several rapid tests used together.
A possible pathway could look like this:
Symptoms → CT scan → fungal antigen test → PCR confirmation → resistance testing
This approach could allow:
- faster diagnosis
- more personalised treatment
- earlier detection of complications
- better treatment monitoring
The aim is not necessarily to replace older tests, but to make the whole diagnostic process earlier, clearer and more precise.
15. Common questions patients ask
Why can Aspergillus infection take time to diagnose?
Because no single test can confirm the disease on its own. Doctors usually need to combine scan findings, blood tests, microbiology and the clinical history.
Why do some tests detect antibodies while others detect the fungus?
Antibody tests show how the immune system has reacted. Molecular and antigen tests try to show whether fungal material is present. Both are useful, but they answer slightly different questions.
Why is a CT scan so important?
A CT scan shows whether there is structural lung damage such as cavities, nodules or fungal balls. This helps doctors judge whether Aspergillus is likely to be causing disease rather than simply being present.
Are these new diagnostics available now?
Some are already used in specialist centres, but many are still being evaluated in clinical trials and research studies.
Will these newer tests replace existing blood tests?
Probably not completely. More likely, they will be used alongside existing tests to improve accuracy and speed.
16. When to seek medical advice
You should seek medical advice if you have symptoms such as:
- persistent cough
- worsening breathlessness
- unexplained fatigue
- weight loss
- coughing up blood
- new or worsening chest pain
These symptoms can have many causes, but they should be assessed properly, especially if you already have underlying lung disease.
17. References
- Denning DW, Cadranel J, Beigelman-Aubry C, Ader F, Chakrabarti A, Blot S, Ullmann AJ, Dimopoulos G, Lange C; European Society for Clinical Microbiology and Infectious Diseases and European Respiratory Society. Chronic pulmonary aspergillosis: rationale and clinical guidelines for diagnosis and management. Eur Respir J. 2016 Jan;47(1):45-68. doi: 10.1183/13993003.00583-2015. PMID: 26699723.
- Kosmidis C, Denning DW. The clinical spectrum of pulmonary aspergillosis. Thorax. 2015 Mar;70(3):270-7. doi: 10.1136/thoraxjnl-2014-206291. Epub 2014 Oct 29. PMID: 25354514.
- Takazono T, Izumikawa K. Recent Advances in Diagnosing Chronic Pulmonary Aspergillosis. Front Microbiol. 2018 Aug 17;9:1810. doi: 10.3389/fmicb.2018.01810. PMID: 30174658; PMCID: PMC6107790.
Author and review information
This page is intended for patients, carers, and non-specialist clinicians. It provides general educational information and should not replace individual medical advice.
Systemic fungal infections: why speed, diagnosis and stewardship matter
Systemic fungal infections — including aspergillosis, candidiasis, cryptococcosis, mucormycosis and pneumocystis pneumonia — are medical emergencies. When diagnosis or treatment is delayed, mortality rises sharply. This comprehensive review brings together current understanding of how these infections arise, why they are so difficult to diagnose, and what is needed to improve outcomes.
Why fungal infections are often missed
Unlike many bacterial infections, systemic fungal infections can be hard to confirm quickly. Fungal organisms are often present in low numbers, may be released intermittently into the bloodstream, and can be difficult to grow in standard cultures. As a result, no single test is usually sufficient, and clinicians often need a combination of imaging, cultures, antigen tests, molecular tests (PCR), and histopathology.
Because delay can be fatal, antifungal treatment is frequently started on clinical suspicion alone — especially in critically ill or immunocompromised patients. The paper emphasises that this approach is often necessary, but it must be paired with a clear diagnostic strategy.
Antifungal stewardship: knowing when to stop
A central message of the paper is that diagnostic tests are just as important for stopping treatment as for starting it. Antifungal drugs can be toxic, interact with many other medicines, and drive antifungal resistance if used unnecessarily.
The authors stress that:
-
Diagnostic results should be actively reviewed
-
Antifungal therapy should be stopped or stepped down if infection is not supported by evidence
-
This approach protects patients and preserves antifungal effectiveness
Antifungal resistance is a growing threat
Antifungal resistance is no longer rare. The review highlights:
-
Azole resistance in Aspergillus, including cryptic species
-
Rising resistance in several Candida species
-
The global spread of multidrug-resistant Candida auris
Because of this, the authors recommend that all clinically relevant fungal isolates are identified to species level and tested for antifungal susceptibility wherever possible. Making assumptions about drug sensitivity is increasingly unsafe.
Aspergillosis: a broad spectrum of disease
The paper clearly outlines the many forms of aspergillosis, ranging from:
-
Allergic disease (such as allergic bronchopulmonary aspergillosis)
-
Chronic pulmonary aspergillosis, often in people with underlying lung damage
-
Subacute and acute invasive disease, particularly in immunocompromised or critically ill patients
Importantly, the review notes that aspergillosis is not limited to severely immunocompromised people. Chronic and subacute forms often occur in individuals with structural lung disease who are otherwise immunocompetent.
Climate change and emerging fungal risks
One of the most forward-looking sections of the paper addresses how climate change and natural disasters are altering fungal disease patterns. Rising environmental temperatures, flooding, storms and environmental disruption are:
-
Increasing exposure to environmental fungi
-
Enabling fungi to adapt to higher temperatures
-
Contributing to outbreaks after natural disasters and trauma
-
Expanding fungal diseases into new geographic regions
The authors argue that fungal infections must be considered part of future public health and healthcare resilience planning.
Key take-home messages
-
Systemic fungal infections are time-critical medical emergencies
-
Diagnosis usually requires multiple tests, not a single result
-
Early antifungal treatment is often necessary — but must be reviewed
-
Diagnostics are essential for safe antifungal stewardship
-
Antifungal resistance is a real and growing problem
-
Climate change is reshaping fungal epidemiology and risk
Free access to the full article
Elsevier has provided free access to the full paper for a limited time (no registration required):
👉 https://authors.elsevier.com/a/1mZqR4qdNoJLH2
🗓️ Available until 28 March 2026
This article is recommended reading for patients wanting a deeper understanding of fungal disease, as well as clinicians, microbiology teams, and healthcare planners.
Can blood tests help predict if chronic pulmonary aspergillosis will come back?
This study from the National Aspergillosis Centre (NAC) looked at people with chronic pulmonary aspergillosis (CPA) who had completed antifungal treatment and asked a simple question:
Can blood tests tell us who is more likely to relapse after treatment stops?
What the researchers did
Doctors reviewed patients with CPA who had:
-
Taken antifungal treatment for at least 6 months
-
Stopped treatment because they were clinically stable
They then followed these patients to see who stayed well and who relapsed, and compared this with their blood test results at the time treatment stopped.
What they found
-
About 1 in 4 patients had a relapse after stopping treatment
-
People whose Aspergillus IgG blood test was still high at the end of treatment were much more likely to relapse
-
Patients whose IgG level had fallen to a lower level did not relapse in this study
-
Signs of Aspergillus allergy or sensitisation also increased relapse risk
-
CT scan appearances and treatment length alone were not reliable predictors
Why this matters for patients
This means that:
-
Blood tests may help doctors decide when it is safe to stop treatment
-
Some people may need closer follow-up or longer treatment
-
Follow-up can be more personalised, rather than “one size fits all”
Importantly, a relapse does not mean treatment failed — it reflects how persistent this infection can be in damaged lungs.
Key takeaway
A simple blood test at the end of treatment may help predict who needs closer monitoring for CPA relapse.
This research supports a more individualised approach to long-term CPA care.