Aspergillosis & Asthma: When Risks Peak Through the Year
Many people living with aspergillosis, asthma, or bronchiectasis notice that their symptoms change with the seasons.
This is no coincidence — environmental factors such as temperature, humidity, pollen, spores, and viral infections all vary through the year, and these can strongly influence both lung health and allergic or fungal disease.
Understanding these patterns can help you plan ahead, reduce exposure, and know when to take extra care.
🌸 Spring: Pollen and Early Spore Season
As temperatures rise, tree pollen (especially birch, oak, and plane) and Aspergillus spores begin to increase in outdoor air.
For people with Allergic Bronchopulmonary Aspergillosis (ABPA) or Severe Asthma with Fungal Sensitisation (SAFS), this can trigger cough, wheeze, and chest tightness.
-
Keep an eye on Met Office pollen and spore forecasts.
-
Open windows on dry days, but check for signs of mould indoors, especially around windows and bathrooms.
-
If you notice symptoms flaring every spring, let your respiratory team know — small medication adjustments may help.
📊 Data source: Met Office spore count data.
☀️ Summer: Soil, Compost, and Renovation Hazards
Warm, humid conditions mean fungi thrive — especially outdoors.
Compost heaps, garden soil, and grass cuttings can release very high levels of Aspergillus spores.
People with chronic lung disease, ABPA, or Chronic Pulmonary Aspergillosis (CPA) are at greater risk of exacerbations during this period.
-
If gardening or using compost, wear gloves and an FFP2/FFP3 mask.
-
Avoid turning compost heaps or cleaning bird feeders if you are immunocompromised.
-
Keep home humidity below 60% and ventilate well during warm spells.
🪴 Source: Protective mask and compost safety advice.
🍂 Autumn: Damp Homes and Viral Load
As the weather cools, we close windows and turn on heating — trapping moisture indoors.
This increases damp and mould growth, particularly in poorly ventilated areas.
At the same time, colds, flu, and RSV infections surge, all of which can make fungal or allergic conditions worse.
-
Use a dehumidifier and ensure air can circulate behind furniture.
-
Check for leaks, condensation, or cold corners.
-
Stay up to date with flu and COVID vaccinations if eligible.
💧 Source: Aspergillosis.org damp guidance.
❄️ Winter: Indoor Season and Medication Review
Outdoor spore levels are lowest in winter, but indoor exposure dominates — from bathrooms, humidifiers, and heating systems.
Viral infections remain a major trigger for asthma and ABPA flare-ups, and antifungal or steroid treatments may need review.
-
Keep homes warm but ventilated where possible.
-
Review your treatment plan with your clinical team, especially if you’re using steroids or biologics.
-
Contact your GP or specialist early if you notice an increase in cough, breathlessness, or mucus plugs.
🧭 Key Takeaway
Aspergillosis and asthma flare-ups often follow the seasons:
| Season | Main Risks | Take Action |
|---|---|---|
| Spring | Pollen, outdoor spores | Monitor counts, check home for mould |
| Summer | Compost, soil, renovation dust | Use masks/gloves, avoid heavy exposure |
| Autumn | Damp homes, viruses | Dehumidify, ventilate, manage infections |
| Winter | Indoor air, viruses | Keep warm, review treatment |
By spotting your personal pattern, you and your care team can plan ahead — reducing exacerbations and staying well all year.
🫁 Understanding Chronic Cough in Aspergillosis
What the latest British Thoracic Society statement means for you
🌬️ Why This Matters
If you live with aspergillosis, Allergic Bronchopulmonary Aspergillosis (ABPA), or bronchiectasis, coughing can dominate your life. It’s tiring, painful, and socially awkward — especially when people assume it means infection.
Doctors used to see cough as just a symptom of another problem, but the British Thoracic Society (BTS) Clinical Statement on Chronic Cough in Adults (2023) recognises something new:
For many people, a cough can become a condition in its own right — caused by airway and nerve hypersensitivity, not just infection.
This matters for aspergillosis patients because fungal allergy and inflammation make the airways especially sensitive.
💡 What Is “Chronic Cough”?
A chronic cough is one lasting eight weeks or more.
It may be:
-
Dry – little or no mucus
-
Productive – thick sputum (common in bronchiectasis or chronic aspergillosis)
-
Triggered by dust, cold air, perfume, or strong scents
For people with aspergillosis, several overlapping causes may exist:
-
Fungal colonisation or infection
-
Allergic inflammation (ABPA)
-
Bronchiectasis and mucus retention
-
Reflux or post-nasal drip
-
Nerve hypersensitivity
This is why one treatment rarely fixes everything — different “treatable traits” must be addressed together.
🧬 Why It Happens
1️⃣ The Hypersensitive Cough Reflex
People with aspergillosis often develop overactive airway nerves — so normal irritants like dust, scent, or cold air trigger coughing fits.
This “cough reflex hypersensitivity” happens because:
-
Ongoing inflammation damages the airway lining.
-
Nerve endings in the throat and lungs become over-responsive.
-
Even mild triggers set off powerful reflexes.
This is a real physiological process, not psychological.
It’s why cough can continue even when infection is under control.
2️⃣ Treatable Traits – Finding the Real Drivers
| Treatable Trait | What It Means | What Helps |
|---|---|---|
| Airway infection or colonisation | Persistent fungi or bacteria | Antifungal or antibiotic therapy, sputum tests |
| Allergic inflammation | ABPA or asthma-type airway swelling | Corticosteroids, biologics (e.g., mepolizumab, benralizumab) |
| Cough reflex hypersensitivity | Overactive airway nerves | Speech therapy, nerve-modulating medication |
| Airway clearance problems | Mucus that’s hard to shift | Physiotherapy, saline or mucolytic therapy |
| Reflux or postnasal drip | Acid or sinus drainage irritation | Reflux management, ENT care |
Identifying these traits helps your clinician personalise treatment.
💊 Medications That Can Cause or Worsen Cough
The BTS statement highlights that some medicines can trigger or amplify chronic cough — especially in people with already-sensitive lungs.
🔹 ACE Inhibitors (Blood pressure or heart disease)
Examples: Ramipril, Lisinopril, Enalapril, Perindopril
-
Can cause a dry, tickly cough due to bradykinin build-up.
-
Happens in ~1 in 5 users, sometimes months after starting.
-
GP can switch to a similar drug (ARB – e.g., losartan) that doesn’t cause cough.
🔹 Beta Blockers (Heart or migraine medicines)
Examples: Atenolol, Propranolol, Bisoprolol
-
May tighten airways, worsening wheeze or cough.
-
Safer “lung-selective” versions exist but should still be monitored.
🔹 Inhalers
Examples: Fluticasone, Budesonide, Salbutamol
-
Can irritate the throat if used without a spacer or if technique is poor.
-
Always rinse or gargle after use, and ask your pharmacist to review inhaler technique.
🔹 Antifungal or Reflux Medicines
-
Antifungals (itraconazole, voriconazole) don’t directly cause cough, but reflux or nausea can trigger coughing indirectly.
-
PPIs (omeprazole, lansoprazole) usually help reflux-related cough, but long-term use should be reviewed regularly.
🔹 Other Drugs
-
Amiodarone, methotrexate, and some biologics can rarely cause cough due to lung inflammation.
-
Nasal sprays or lozenges with menthol/alcohol may irritate already-sensitive airways.
💬 If you suspect a medicine is contributing, don’t stop it suddenly — speak to your doctor or pharmacist first.
They can review interactions using the
👉 BNF Interactions Checker – NICE Medicines Guidance.
🔍 How Doctors Assess Chronic Cough
BTS recommends a structured pathway:
-
Basic tests: chest X-ray, spirometry, bloods (eosinophils, IgE), FeNO if available.
-
Further tests: CT scan, allergy or sputum studies if initial tests are abnormal.
-
Trait-based review: identifying overlapping issues — fungal, allergic, nerve-related, or reflux-related.
-
Specialist referral: to a Cough Clinic or Aspergillosis Centre if symptoms persist.
🧴 Pharmacists: Your Safety Specialists
Pharmacists — hospital or community — are crucial for managing long-term cough and medication safety:
-
Check for cough-inducing drugs or interactions.
-
Advise on best timing for antifungal and steroid doses.
-
Help switch to fragrance-free personal or cleaning products.
-
Liaise with your GP and consultant to fine-tune treatment.
🧭 Regular medication reviews every few months can prevent small problems becoming major triggers.
💬 How It Feels — and Why It’s Misunderstood
People with aspergillosis often describe:
“A tickle that turns into a spasm I can’t stop.”
“People think I’m ill, but it’s just the air or perfume.”
This happens because your airway nerves and immune cells are already primed.
Coughing doesn’t mean you’re infectious — it’s your body’s protective reflex in overdrive.
🩺 What Helps Most
-
Optimise your aspergillosis and ABPA treatment.
-
Cough-control physiotherapy or speech therapy for nerve-related cough.
-
Airway clearance techniques for mucus.
-
Identify and avoid irritants: perfume, smoke, strong detergents, cold air.
-
Ask about biologics if inflammation remains active despite steroids.
-
Use nerve-modulating medicines only under specialist advice.
🧘 Emotional Health Matters Too
Living with a chronic cough can cause anxiety, embarrassment, and isolation.
Support from counsellors, CBT therapists, or patient groups helps manage this stress — and can actually reduce cough frequency through better relaxation and breathing control.
🌱 Key Takeaway
Chronic cough in aspergillosis isn’t “just a symptom” — it’s often a mix of airway inflammation, fungal allergy, nerve hypersensitivity, and sometimes side effects of medicines.
The good news is that every contributing factor is treatable once identified — and cough can improve significantly with the right combination of medical, physical, and environmental care.
🔗 Trusted Resources
💼 Aspergillosis, Scent Sensitivity, and the Workplace
Understanding why everyday environments can trigger coughing — and what you can do about it
🌫️ When the Air Itself Feels Unsafe
Many people living with aspergillosis, Allergic Bronchopulmonary Aspergillosis (ABPA), or severe allergies feel anxious about returning to offices or shared spaces.
It isn’t the job that’s difficult — it’s the environment.
Dusty desks, neglected air vents, cold air-conditioning, and strong perfumes can all trigger coughing or wheezing.
Even a few minutes in a scented or dusty room can leave you coughing for hours — and explaining (again) that you’re not contagious.
If this sounds familiar, you’re not being oversensitive — you’re reacting to real biological triggers.
🧬 Why These Reactions Happen
1️⃣ Chemical Irritants and Perfumes
Perfumes, air fresheners, and cleaning sprays release volatile organic compounds (VOCs) such as limonene, linalool, and formaldehyde.
In sensitive lungs, these cause irritation and inflammation of the airways.
-
Research shows VOCs can provoke coughing, wheezing, and chest tightness in people with asthma or allergic airway disease.
-
These chemicals also activate airway nerve endings (trigeminal and vagal nerves) that trigger coughing reflexes — even when no infection or allergy is present.
This is known as neurogenic inflammation — a real, measurable process that makes you cough within seconds of exposure.
2️⃣ Damaged or Sensitive Airways
People with aspergillosis, bronchiectasis, or ABPA already have inflamed, scarred, or hypersensitive airways.
The airway lining (epithelium) is fragile and “leaky,” letting irritants trigger inflammation more easily.
Cough receptors are overactive, so small exposures — to scent, dust, or cold air — produce a big response.
Doctors call this airway hyperreactivity or irritant-induced cough reflex hypersensitivity.
It’s not psychological — it’s your lungs doing too good a job of protecting themselves.
3️⃣ Immune System Over-Response
Because aspergillosis and ABPA involve Type-2 immune inflammation (involving eosinophils and Th2 cytokines), your body’s defence cells are already primed.
When you inhale perfumes, dust, or fungal spores, those same immune pathways may flare up — releasing histamine and other inflammatory chemicals.
That’s why even non-allergic triggers can cause coughing or breathlessness.
4️⃣ Combined Triggers
Reactions are often additive.
Dust, perfume, cold air, and low humidity can act together:
-
VOCs stick to dust particles and linger.
-
Cold air increases nerve sensitivity.
-
Mould fragments or Aspergillus spores amplify inflammation.
So what seems like “just perfume” may actually be a cocktail of irritants acting on already-inflamed lungs.
💬 The Social Challenge
Explaining a chronic cough can feel awkward.
Colleagues often assume it means infection — and that’s stressful when you’re already managing symptoms.
You shouldn’t have to justify your condition, but some people find it helps to have a short, calm explanation ready:
“I have a long-term lung condition that makes me cough when the air is dusty or scented — it’s not infectious.”
If you’re comfortable, let HR or Occupational Health know so they can help set expectations and prevent misunderstandings.
🏥 Your Rights and Reasonable Adjustments (UK)
Under the Equality Act 2010, aspergillosis and severe environmental allergies can qualify as a disability because they substantially affect daily life.
That means employers have a legal duty to make reasonable adjustments, such as:
-
A clean, fragrance-free workspace
-
Portable air purifier or improved ventilation
-
Flexible or hybrid working
-
Adjusting temperature or airflow
-
Asking cleaning teams to use low-VOC products
Occupational Health can formalise these requests confidentially so you’re not seen as a “complainer.”
👉 Equality Act 2010 – Reasonable Adjustments (GOV.UK)
👉 ACAS Guidance on Long-Term Health Conditions
🧴 Pharmacists: The Unsung Safety Specialists
Your hospital or local pharmacist is an important ally.
They can:
-
Review all your medicines for interactions or side effects that might worsen coughing.
-
Advise how to take antifungals (e.g., with food, not with antacids).
-
Suggest fragrance-free personal care or cleaning products.
-
Liaise with your GP or hospital consultant if medication changes are needed.
You can also use the official
👉 BNF Interactions Checker (NICE Medicines Guidance)
to look up possible drug interactions — but always confirm findings with your pharmacist.
🏡 Considering Remote or Hybrid Work
If triggers are unavoidable in your current workplace, remote or hybrid work may be a safe and realistic alternative.
A Fit Note from your consultant or GP can recommend home working as a health adjustment.
When searching for jobs, look for roles described as remote, home-based, or flexible — many NHS, charity, and tech employers are now supportive of this.
🧘 Managing the Emotional Side
Anxiety about returning to work is natural.
Many people find that anticipating exposure — and potential misunderstanding — is almost as stressful as the symptoms themselves.
Talking to your consultant or GP about counselling or CBT for health anxiety can help you build confidence and coping strategies.
Peer support from others with chronic respiratory disease can be just as powerful — you’re not alone in feeling this way.
🌱 Key Takeaways
-
Reactions to perfume, dust, and cold air are real physiological responses, not oversensitivity.
-
They occur because inflamed airways and primed immune systems are hypersensitive to chemical and physical irritants.
-
Simple environmental changes — plus understanding from employers and colleagues — can make a huge difference.
-
Pharmacists, doctors, and occupational-health teams can help you manage medicines and advocate for a safe workspace.
You deserve an environment that helps you stay well — not one that forces you to prove you’re not sick.
Further Reading
-
“Airway Hyperresponsiveness in Asthma: Its Measurement and Clinical Significance” (PMC full-text) — a detailed review of what airway hyper-responsiveness (AHR) is, how it happens, and why it matters. Link
-
“Cough Hypersensitivity” (PDF patient leaflet, UK NHS trust) — explains how the airway nerves become too sensitive, what triggers are, and how the cycle of cough can develop. Link
⚠️ Omeprazole and PPIs: What’s Behind the Recent Warning?
Recently, several newspapers – including The Mirror – reported that a “BBC doctor” had issued a warning to anyone taking omeprazole, a commonly prescribed drug for acid reflux and heartburn.
So, is this something new, or just another media scare? Let’s look at what the evidence actually says – and what it means if you’re living with aspergillosis, bronchiectasis, or other chronic lung diseases.
💊 What Are PPIs?
Proton Pump Inhibitors (PPIs) such as omeprazole, lansoprazole, and esomeprazole are medicines that reduce stomach acid.
They’re often used to:
-
Treat reflux, indigestion, or stomach ulcers
-
Protect the stomach from irritation caused by anti-inflammatory drugs or steroids
They’re very effective and widely prescribed — millions of people in the UK take them every day.
⚠️ Why the Headlines?
The recent news stories stem from a discussion on BBC Morning Live, where GP Dr Punam Krishan highlighted the potential long-term side effects of PPIs.
Although these aren’t “new discoveries”, they serve as an important reminder that long-term PPI use should be reviewed regularly.
🧠 What the Evidence Shows
Research over the past decade has shown that taking PPIs for a long time or at high doses can lead to several possible side effects:
| Possible Issue | What Happens | Why It Matters |
|---|---|---|
| Infections | Higher risk of gut infections such as Clostridioides difficile and bacterial overgrowth | Stomach acid normally helps kill harmful bacteria; reducing it alters the balance |
| Changes in gut microbiome | Loss of protective “friendly” bacteria | May influence digestion, immunity, and inflammation |
| Reduced absorption of nutrients | Low magnesium, iron, or vitamin B12 | Can lead to tiredness, cramps, or anaemia |
| Bone health | Slightly higher risk of fractures with very long-term use | May relate to calcium absorption |
| Kidney and heart effects (rare) | Observed in some studies | Still being researched |
Most of these risks are small, and for many people the benefits outweigh them — but it’s still important to make sure you’re taking the lowest effective dose and that your doctor reviews the need for it periodically.
🫁 Why It Matters for Aspergillosis and Lung Conditions
If you have aspergillosis, bronchiectasis, or Primary Ciliary Dyskinesia (PCD), there are extra reasons to think carefully about long-term PPI use:
-
Microbiome connections: The gut and lungs are linked through what’s called the gut–lung axis. Disturbances in gut bacteria can affect immune responses elsewhere in the body — possibly including the lungs.
-
Infection control: PPIs can slightly increase the risk of bacterial or fungal overgrowth in the gut. While this doesn’t directly cause lung infection, it may influence the body’s balance between helpful and harmful microbes.
-
Medication interactions: Some antifungal medicines (like itraconazole or posaconazole) rely on stomach acidity for absorption — so PPIs can reduce their effectiveness. Your specialist will usually time doses or adjust medication accordingly.
-
Reflux and aspiration: On the other hand, reflux itself can worsen lung disease if acid is inhaled into the lungs — so stopping PPIs suddenly can make things worse. Always discuss any change with your doctor first.
🩺 What You Can Do
If you take omeprazole or another PPI:
-
Check why you’re on it – Is it for reflux, ulcer protection, or another reason?
-
Review the dose and duration – Many people can step down to a lower dose or switch to on-demand use once symptoms are controlled.
-
Don’t stop suddenly – Stopping PPIs abruptly can cause a rebound in acid production and make symptoms flare.
-
Ask about alternatives – Some people can switch to H2-blockers (e.g. ranitidine-type medicines), or use lifestyle changes such as avoiding late meals, raising the bedhead, and reducing caffeine or alcohol.
-
Discuss with your specialist team – Particularly if you’re also on antifungal or antibiotic treatments, as interactions can occur.
🧩 Key Takeaway
The recent headlines about omeprazole are not new, but they highlight a genuine issue:
PPIs are very useful drugs — but long-term use should always be reviewed to make sure the benefits outweigh the risks.
For most people, there’s no need to panic.
Just make sure you:
-
Use the lowest effective dose
-
Review your need for PPIs at least once a year
-
Discuss any concerns with your respiratory or gastroenterology team
🔗 Useful References
-
NHS Guidance: Proton Pump Inhibitors – Risks and Review Advice
-
PrescQIPP PPI Safety Review (UK 2023) – Long-term safety and deprescribing guidance
-
Gut (BMJ): Proton pump inhibitors and gut microbiota: cause for concern? (Gut 2016;65:740–748)
🏠 Awaab’s Law: What It Means for Social Housing Tenants
Awaab’s Law is one of the most important housing reforms in years.
It aims to protect tenants from damp, mould and unsafe living conditions — problems that can seriously affect health, especially for people with asthma, bronchiectasis or fungal lung disease.
The law starts to take effect in October 2025 and is named in memory of Awaab Ishak, a two-year-old who tragically died from prolonged exposure to damp and mould in a housing association flat in Rochdale.
His case led to new, legally enforceable time limits for social landlords to investigate and repair health hazards in rented homes.
📜 Where the Law Comes From
Awaab’s Law forms part of the Social Housing (Regulation) Act 2023.
It adds a new legal duty (Section 10A) to the Landlord and Tenant Act 1985, requiring every social landlord to comply with “prescribed requirements” about how quickly hazards must be investigated and repaired.
These rules are set out in the Awaab’s Law Regulations, published on GOV.UK, and enforced by the Regulator of Social Housing.
👥 Who the Law Covers
Awaab’s Law applies to:
-
Social landlords in England, such as housing associations and local authorities
-
Tenants living in social housing under secure, assured, or introductory tenancy agreements
Awaab’s Law does not yet apply to:
-
Private landlords or the private rented sector (PRS)
-
Owner-occupiers or leaseholders
The Government has confirmed that lessons from this law will inform future private-rented-sector reforms.
(Official source: GOV.UK – Awaab’s Law Guidance)
🏘️ What Is Social Housing?
Social housing is housing owned or managed by public or not-for-profit organisations and rented out at below-market rates to people in housing need.
It provides secure, long-term homes and is regulated by the Regulator of Social Housing.
(Official source: Regulator of Social Housing – GOV.UK)
🧱 Who Provides It
-
Local authorities (councils) – council housing
-
Housing associations – independent, not-for-profit registered providers
-
Charitable or community landlords – smaller providers that must still meet national standards
These organisations are known as registered providers under the Housing and Regeneration Act 2008.
💰 How Social Housing Differs from Other Tenancies
| Feature | Social Housing | Private Rented Housing | Shared Ownership / Leasehold |
|---|---|---|---|
| Who owns it | Council / housing association | Private landlord / company | Part tenant part provider |
| Rent level | Below market (50–80%) | Market rate | Rent on unsold share + mortgage |
| Tenancy type | Secure / assured (long-term) | Assured shorthold (short-term) | Leasehold ownership |
| Regulation | Regulator of Social Housing | Local authority & housing law | Leasehold law |
| Repair standards | Decent Homes Standard + Awaab’s Law | General HHSRS duties | As defined in lease |
| Who qualifies | Based on housing need | Anyone meeting market criteria | Specific financial criteria |
⚙️ What Landlords Must Do Under Awaab’s Law
Social landlords must:
-
Investigate reported hazards quickly
-
Provide written findings after inspection
-
Repair and make safe within legal deadlines
-
Offer temporary accommodation if the home cannot be made safe in time
These duties cover damp and mould and any emergency hazard posing serious risk to health or safety.
🕒 Timeframes Landlords Must Follow
| Stage | Time Allowed | Example |
|---|---|---|
| Emergency hazard | Make safe immediately / within 24 hours | Gas leak, severe mould, electrical fault |
| Significant hazard | Investigate within 10 working days | Damp, cold, structural issues |
| Tenant update | Written summary within 3 working days | Explain findings + repairs |
| If not safe in time | Provide alternative accommodation | Until repairs complete |
(Source: GOV.UK – Draft Guidance)
💬 Why Mould and Damp Matter
Damp and mould are common and dangerous in UK housing and can worsen or trigger asthma, ABPA, CPA, and COPD.
The English Housing Survey (2023) found 1 in 10 social homes had damp or mould problems.
Mould exposure can cause:
-
Asthma flare-ups and new respiratory infections
-
Worsening of fungal lung disease
-
Eye, throat, and skin irritation
Awaab’s Law recognises that poor building design and ventilation, not “tenant lifestyle,” are usually to blame.
🏘️ Why Shared and Multiple-Occupancy Homes Are Higher Risk
Buildings converted into Houses in Multiple Occupation (HMOs) are prone to damp and mould because they:
-
House many people in small spaces
-
Were often converted without proper ventilation or insulation
-
Rely on multiple tenants to report and manage repairs
HMOs are mainly in the private rented sector and not covered by Awaab’s Law.
They are regulated separately under the Housing Act 2004 and inspected by councils using the Housing Health and Safety Rating System (HHSRS).
These homes frequently house students, low-income workers, and people with chronic illness, making damp-related respiratory illnesses a particular concern.
🧱 Why HMOs Need Stronger Oversight
Local authorities can issue Improvement Notices or prosecute landlords for neglecting repairs, but Awaab’s Law’s fixed deadlines do not yet apply.
Government statements indicate future reforms will extend similar protections to private and HMO tenants.
💬 Why This Matters for Health
For anyone with chronic lung disease (ABPA, CPA, asthma, bronchiectasis), damp and mould can trigger flare-ups and new infections.
Awaab’s Law now forces social landlords to act promptly within set legal time limits.
Tenants can:
-
Use the landlord’s complaints procedure
-
Contact the Housing Ombudsman Service
-
Report serious risks to the Regulator of Social Housing or local council
🏛️ Does Awaab’s Law Apply to MOD, NHS, and Other Service Housing?
No — not directly.
Awaab’s Law covers registered social housing providers in England (local authorities and housing associations).
It does not extend to housing owned or managed by the Ministry of Defence (MOD), NHS Trusts, or other public-service employers, unless they are formally registered social landlords (which is rare).
| Housing Type | Covered by Awaab’s Law? | Notes |
|---|---|---|
| Council / Housing Association Homes | ✅ Yes | Registered providers under the Regulator of Social Housing |
| Private Rented Sector | ❌ No (not yet) | May be included in future reforms |
| MOD (Service Family Accommodation) | ❌ No | Managed by Defence Infrastructure Organisation; standards set by policy, not law |
| NHS Staff Accommodation | ❌ No | Governed by occupational licence terms and health & safety law |
| University or Key Worker Housing | ❌ No | Treated as private or institutional housing |
| Charitable / Supported Housing | ⚠️ Sometimes | Only if registered with the Regulator of Social Housing |
These providers must still maintain safe conditions under Health and Safety law, but they do not yet have the same legal repair timescales as social landlords.
The Government has stated that principles from Awaab’s Law may be used to improve MOD and NHS housing standards in future.
(Sources: legislation.gov.uk, GOV.UK – Awaab’s Law Guidance, Parliament.uk HCWS423)
🧩 Summary
| Key Point | What It Means |
|---|---|
| Who it covers | Tenants in social housing (England only) |
| What it covers | Damp, mould, and serious health hazards |
| When it starts | From 27 October 2025 |
| Who it excludes | Private, MOD, NHS and service housing |
| Why it matters | Protects tenants from unsafe homes and poor health |
| Who enforces it | Regulator of Social Housing / Local Authorities |
| Official sources | GOV.UK / legislation.gov.uk / Parliament.uk |
🔗 Official References
🌿 Aspergillosis in the Sinuses (Allergic Fungal Rhinosinusitis – AFRS)
It’s quite possible for Aspergillus to affect both the lungs and the sinuses.
The sinuses are small air-filled spaces behind the nose, eyes, and cheeks that normally drain mucus freely. When Aspergillus spores become trapped there, they can trigger an allergic or inflammatory reaction — rather like ABPA in the lungs.
This allergic form is called Allergic Fungal Rhinosinusitis (AFRS).
It isn’t a contagious infection — it’s an overreaction of the immune system to fungal spores. Over time, it can lead to thick mucus, nasal blockage, and sometimes nasal polyps.
🩵 Common symptoms
-
Persistent nasal congestion or blockage
-
Thick or sticky mucus (sometimes with brown or dark flecks)
-
Reduced or lost sense of smell
-
Facial pressure, pain, or fullness (especially around the eyes or cheeks)
-
Post-nasal drip (mucus running down the throat)
-
Fatigue or worsening asthma symptoms
🔬 Diagnosis
-
CT scan of the sinuses – shows thickened or blocked areas
-
Nasal endoscopy – a tiny camera used to look inside
-
Fungal culture or microscopy from mucus samples
-
Blood tests – sometimes show raised total IgE or Aspergillus-specific IgE
💊 Treatment
-
Topical nasal steroids (sprays or rinses) or short courses of oral steroids to reduce inflammation
-
Saline rinses to help keep the sinuses clear
-
ENT surgery if sinuses are blocked or filled with thick fungal debris
-
Antifungal medication in some cases, especially if fungal growth is confirmed
🌸 The Main Types of Aspergillus Sinus Disease
There are several recognised types of sinus aspergillosis. Most people with ABPA or asthma experience only the allergic form (AFRS).
1️⃣ Allergic Fungal Rhinosinusitis (AFRS)
-
Caused by an allergic reaction to Aspergillus
-
Leads to inflammation, thick mucus, and polyps
-
Non-invasive – the fungus stays on the surface
-
Managed with steroids, nasal rinses, and sometimes surgery
✅ This is the type most relevant for ABPA patients.
2️⃣ Fungal Ball (Mycetoma)
-
A clump of fungus (usually A. fumigatus) in a single sinus, often the cheek (maxillary) sinus
-
Common in otherwise healthy people
-
Causes chronic congestion or facial pain
-
Treated surgically – antifungals rarely needed
-
Not allergic and not invasive
3️⃣ Invasive Aspergillus Sinusitis
-
Rare, seen mostly in people with severely weakened immunity (e.g., chemotherapy, bone marrow transplant, uncontrolled diabetes)
-
The fungus invades surrounding tissue and blood vessels
-
Causes severe facial pain, swelling, fever, sometimes affecting the eyes
-
Needs urgent treatment with antifungal drugs and surgery
⚠️ Very rare in people with ABPA or CPA.
🤝 Specialist care
If you have lung aspergillosis (such as ABPA or CPA) and start noticing more nasal congestion, sinus pressure, or post-nasal drip, it’s sensible to mention it to your respiratory or mycology team.
At the National Aspergillosis Centre (NAC), sinus disease is often co-managed by ENT surgeons, respiratory physicians, and mycology specialists, ensuring coordinated care.
With the right combination of treatments — and early recognition of symptoms — most people find their sinus symptoms improve, and controlling sinus inflammation can even help with overall breathing and energy.
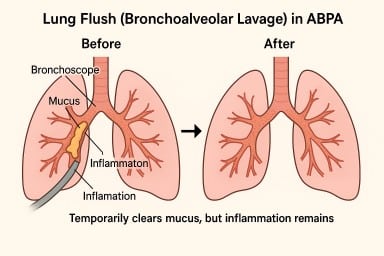
🫁 “Lung Flush” (Bronchoalveolar Lavage) in ABPA – What It Is and Why It Brings Only Short-Term Relief
A lung flush (also called a bronchoalveolar lavage, or BAL) isn’t a regular treatment for Allergic Bronchopulmonary Aspergillosis (ABPA), but it’s sometimes used selectively in NHS hospitals.
💧 What Happens During a Lung Flush
It’s done during a bronchoscopy, where a thin, flexible tube is passed through the nose or mouth into the lungs.
A small amount of sterile saline is washed into part of the lung and then gently suctioned back out.
The fluid is tested for:
-
Aspergillus growth or DNA
-
Other infections (bacteria, fungi, viruses)
-
Signs of inflammation or allergic activity
You’re given local anaesthetic and light sedation, so you stay comfortable but sleepy. Most people go home the same day.
🧪 Main Purpose – Diagnosis
In most ABPA cases, a lavage is done to find out what’s causing symptoms – whether they’re due to Aspergillus, another infection, or ongoing inflammation.
The results help doctors fine-tune treatment, such as adjusting antifungal doses or deciding if a biologic drug might help.
🫁 Sometimes Used to Clear Mucus
In certain situations – especially when thick mucus plugs are blocking airways or causing part of a lung to collapse – doctors may use lavage as a therapeutic “flush.”
This can wash out sticky secretions and temporarily improve airflow, helping physiotherapy and medication work more effectively.
It’s usually a short, day-case procedure, and most people feel back to normal after a day or two.
⚠️ Why It’s Only Short-Term Relief
Although lavage can clear mucus, ABPA is caused by an allergic immune reaction, not by the mucus itself.
Unless that reaction is controlled with:
-
Corticosteroids (to reduce inflammation),
-
Antifungal drugs (to lower the fungal load), or
-
Biologic injections (to block allergy pathways),
…the lungs will continue to produce thick, sticky mucus, which can re-accumulate within days or weeks.
So while a “lung flush” can make breathing easier in the short term, the effect is temporary – like clearing a blocked drain while the tap is still running.
⚠️ Risks and After-Effects
A bronchoscopy with lavage is generally safe, but it is still an invasive procedure. Possible effects include:
-
Temporary sore throat, cough, or hoarseness (common)
-
Mild bleeding or streaks of blood in sputum for a short time
-
Low oxygen levels during or after the procedure (monitored carefully)
-
Chest tightness, infection, or fever – uncommon but possible
-
Bronchospasm (airway narrowing) in people with very sensitive lungs, which is why it’s done in a hospital with respiratory support available
Because of these small but real risks, the NHS uses lavage only when the benefits outweigh the downsides – for example, when mucus is causing serious blockage or when test results will change management.
💬 In Summary
A “lung flush” can temporarily clear mucus and ease breathing, but it doesn’t stop ABPA’s underlying allergic inflammation.
The mucus often returns unless that inflammation is brought under control with long-term medical treatment.
It’s a useful tool when needed, but not something done regularly or lightly.
🌿 Why do I get thick, yellow mucus in the morning?
Many people with asthma, ABPA (allergic bronchopulmonary aspergillosis) or sinus problems notice that first thing in the morning they cough up or “hook out” very thick, sticky, yellow mucus from the back of the throat or nose.
It can feel like glue — stringy, rubbery, and slow to move.
The good news is:
👉 This doesn’t automatically mean that Aspergillus fungus is growing in your sinuses.
💧 Why it happens
At night, mucus naturally becomes thicker because:
-
You breathe more through your mouth while sleeping, which dries the nose and throat.
-
Mucus sits still instead of draining, so it concentrates and thickens.
-
If you already have sinus inflammation or allergies, your mucus glands make even more.
-
It often drains down the back of the throat (post-nasal drip), where it collects until morning.
This combination makes for a lumpy, sticky “plug” that only shifts once you’re up and moving around.
🧠 When might fungus be involved?
If the sinuses become colonised with Aspergillus or another fungus, there are usually extra clues, such as:
-
Blocked nose or pressure that doesn’t improve with sprays or rinses
-
One-sided pain or discharge
-
Dark, rubbery, or green-grey plugs rather than yellow mucus
-
Loss of smell
-
CT or endoscopy showing thick debris or “fungal balls”
If these are present, an ENT specialist can look directly into the sinuses and, if needed, take a small sample for fungal culture or order a CT scan.
🩺 What helps most people
You can often manage the morning mucus with simple measures:
-
Saline nasal rinses (like Sterimar, NeilMed, or salt-water sprays) — thin mucus and wash out allergens or fungal dust.
-
Warm fluids or gentle steam to moisten airways.
-
Topical nasal steroid sprays (if prescribed) — reduce swelling and mucus production.
-
Plenty of hydration through the day.
-
Avoid over-using decongestant sprays, which can make congestion worse in the long run.
If mucus stays thick, coloured, or difficult to clear for more than a few weeks — or you develop sinus pressure, pain, or smell loss — ask for a review by your ENT or respiratory team.
🟢 Key message
Thick yellow mucus in the morning is usually a sign of dryness and overnight build-up, not an active fungal infection.
Regular rinsing, good hydration, and controlling sinus inflammation usually keep things under control.
Fungal colonisation is much less common — and when it happens, there are usually other warning signs that your clinician can check.
Understanding and Controlling Your Immune System
How your immune system works
Your immune system is your body’s built-in defence and repair network.
It protects you from infection, clears away damaged cells, and helps you heal after illness or injury. But it’s also connected to almost every part of the body — your brain, gut, hormones, and even mood.
When finely balanced, it keeps you healthy. When it becomes over- or under-active, it can cause inflammation, allergies, or long-term conditions such as ABPA or asthma.
🧠 1. Brain and nerves
-
Normal role: Immune cells in the brain (called microglia) keep nerve circuits healthy and remove damaged cells.
-
When things go wrong: Too much inflammation can cause fatigue, “brain fog,” anxiety, or depression — feelings many people experience during infection or flare-ups. Long-term inflammation is linked to memory problems and slower recovery after illness.
❤️ 2. Heart and blood vessels
-
Normal role: Immune cells repair vessel walls and help wounds heal.
-
When things go wrong: Chronic inflammation can thicken arteries (atherosclerosis) or cause rare problems like vasculitis, which affects blood flow. Balancing inflammation helps protect heart and circulation health.
🫁 3. Lungs and airways
-
Normal role: The immune system protects your lungs from germs, clears dust, and repairs tissue after irritation.
-
When things go wrong:
-
In asthma or ABPA, the immune system overreacts to harmless triggers such as Aspergillus spores, pollen, or dust, causing airway swelling, mucus build-up, and breathlessness.
-
In CPA, parts of the immune system struggle to clear fungal infection effectively, leading to chronic inflammation and tissue damage.
Keeping the immune response balanced — not too weak, not too strong — is the key to long-term lung health.
-
🍽️ 4. Gut and digestion
-
Normal role: About 70% of your immune cells live in the gut, where they keep a healthy balance of bacteria and prevent harmful microbes leaking into the bloodstream.
-
When things go wrong: Stress, poor diet, or antibiotics can disrupt this balance, increasing inflammation.
A varied, fibre-rich diet and, in some cases, probiotics can help the gut “educate” the immune system.
💪 5. Muscles, joints, and repair
-
Normal role: Immune cells clear damaged tissue and stimulate repair after exercise or illness.
-
When things go wrong: If the immune system stays “switched on,” joints and muscles can ache or feel weak.
Fatigue in aspergillosis may be partly due to ongoing low-level inflammation.
🧬 6. Hormones and metabolism
-
Normal role: Hormones like cortisol and adrenaline help keep inflammation under control.
-
When things go wrong:
-
Overactive inflammation can worsen insulin resistance, weight changes, and tiredness.
-
Autoimmune problems can affect glands like the thyroid or adrenal glands (Addison’s disease).
Managing stress, sleep, and diet all help the immune-hormonal balance.
-
🩸 7. Blood and bone marrow
-
Normal role: The immune system is built in the bone marrow, producing white cells, red cells, and platelets.
-
When things go wrong: Excessive inflammation raises blood markers such as CRP or eosinophils, often seen during ABPA flare-ups or infection.
Monitoring these levels helps your specialist adjust treatment safely.
🦴 8. Skin and mucous membranes
-
Normal role: Acts as the body’s first barrier, with immune cells ready to seal wounds or fight germs.
-
When things go wrong: Eczema, psoriasis, and slow-healing wounds can occur when immune balance is disturbed — sometimes as side effects of steroids or other medications.
⚖️ 9. The balance between defence and tolerance
The most important job of your immune system is to tell friend from foe — to destroy invaders but leave your own body unharmed.
-
If it overreacts, you get allergies or autoimmune disease.
-
If it underreacts, infections can take hold more easily.
-
In aspergillosis, both problems can occur together: too little defence against fungus, but too much inflammation once the fungus is detected.
🧩 How Medicine Is Learning to Control the Immune System Better
In the past, we only had blunt tools — like steroids — to “calm” inflammation. These saved lives but also caused side effects.
Today, science is learning to control the immune system more precisely, using targeted treatments, cell therapies, and even lifestyle tools that work with your body’s own defences.
🎯 1. Targeted biologic drugs
These are antibodies made in the lab that block one specific immune signal instead of suppressing everything.
Examples used in asthma and ABPA:
-
Mepolizumab and benralizumab block interleukin-5 (IL-5), reducing eosinophil-driven inflammation.
-
Dupilumab blocks IL-4 and IL-13 pathways, calming allergic inflammation.
Other biologics (like infliximab, tocilizumab, and omalizumab) target immune messengers involved in arthritis, eczema, or autoimmune disease.
💉 2. Vaccines and immune training
Vaccines “teach” the immune system to respond safely and efficiently.
New approaches — such as mRNA vaccines — can be updated quickly and may in future be used to retrain the immune system in chronic diseases, allergies, and even cancer.
⚙️ 3. Immune cell therapies and genetic repair
Researchers can now rebuild parts of the immune system:
-
CAR-T cell therapy modifies a patient’s own T cells to find and destroy cancer.
-
T-reg therapy expands the body’s natural “peacekeeping” cells to prevent autoimmune attack.
-
Gene editing (CRISPR) aims to correct inherited immune problems or fine-tune overactive responses.
🧠 4. Neuro-immune and stress control
Because the brain and immune system constantly talk, therapies that reduce stress or stimulate specific nerves can influence inflammation.
-
Vagus nerve stimulation devices can reduce gut and joint inflammation.
-
Mindfulness, relaxation, and gentle exercise lower stress hormones and improve immune balance — especially in asthma or ABPA, where stress can trigger flares.
🌿 5. Microbiome and metabolic balance
Your gut bacteria, diet, and metabolism shape immune health.
-
A high-fibre, plant-based diet produces short-chain fatty acids that calm inflammation.
-
Probiotic and prebiotic therapies are being studied to restore immune tolerance.
-
Metabolic drugs such as metformin are showing anti-inflammatory effects beyond diabetes care.
🧩 6. Re-teaching immune tolerance
The ultimate goal is to re-educate the immune system so it stops attacking harmless things.
-
Allergen immunotherapy exposes the body to small, increasing doses of allergens to reduce sensitivity.
-
Nanoparticle and peptide therapies are being developed to signal to immune cells that “this is safe,” switching off allergic or autoimmune responses without weakening defences.
👤 7. Personalised immune medicine
Every person’s immune system behaves differently.
-
New blood and genetic tests (“immune phenotyping”) help doctors match patients to the best biologic or antifungal treatment.
-
Artificial intelligence is being used to model individual immune systems — predicting who will respond best to certain drugs.
-
In the future, “immune profiles” may be as common as cholesterol or blood pressure checks.
💬 Living with Aspergillosis: What This Means for You
-
You’re not powerless. Understanding your immune system helps you work with your doctors to find the best balance of antifungal, biologic, and anti-inflammatory treatments.
-
Lifestyle still matters. Stress control, exercise, nutrition, and infection avoidance (e.g. clean air, low mould exposure) all influence immune stability.
-
New hope. Research is rapidly advancing — turning immune control from a guessing game into a precise science.
The same breakthroughs that transformed cancer and autoimmune care are now informing treatments for allergic and fungal lung disease.
🩺 In summary
Your immune system touches every part of your body — lungs, gut, brain, hormones, and skin.
In aspergillosis, it can become both under-protective and over-reactive, creating the delicate balance specialists are trying to restore.
Modern medicine is learning to tune the immune system like an orchestra, not silence it — calming inflammation when it harms you, and strengthening defence when you need it most.
The future of aspergillosis care lies in immune precision — treating not just infection, but the whole system that responds to it.
🌿 Covid-19 and ABPA / Bronchiectasis: What Patients Need to Know
Many patients with ABPA, bronchiectasis, and asthma ask:
“If I test positive for Covid, am I at higher risk, and do I need antivirals or steroids?”
“Is Covid still a dangerous infection now that everyone has had it many times?”
Here’s what’s important right now.
🎯 Why you may be at higher risk
Having ABPA, bronchiectasis, or asthma doesn’t guarantee severe illness, but it does put you at higher risk compared to the average healthy adult. This means you are more likely to experience:
-
More severe Covid illness – infections can trigger worse chest symptoms (wheeze, shortness of breath, cough).
-
Secondary infections – bronchiectasis makes it easier for bacteria to grow in mucus after a viral infection.
-
Flares of existing disease – Covid can set off asthma attacks or ABPA flare-ups.
-
Slower recovery – fatigue, breathlessness, and extra sputum can last longer.
⚠️ Important: “Higher risk” does not mean you will definitely become very unwell. Many people with chronic lung disease still have mild Covid and recover fully at home.
✅ Current Covid treatments in the UK (2025)
-
Antivirals / monoclonal antibodies
-
People with conditions like ABPA, bronchiectasis, or severe asthma may be eligible for medicines such as Paxlovid or Molnupiravir.
-
These must usually be started within 5 days of symptoms or a positive test.
-
Access is through the NHS Covid Medicines Delivery Unit (CMDU), often arranged via NHS 111 or your GP.
-
-
Steroids
-
Oral steroids (prednisolone) are not routinely given for Covid unless oxygen levels drop, or you already take them for your lung condition.
-
If your asthma/ABPA flares, follow your specialist’s guidance on when to start rescue steroids.
-
-
Antibiotics
-
Covid is viral, so antibiotics don’t treat it directly.
-
But if your doctor suspects a bacterial infection (e.g. in bronchiectasis), they may prescribe something like doxycycline.
-
🧾 Practical steps if you test positive
-
Call NHS 111 or your GP: Tell them you have ABPA/bronchiectasis/asthma and ask about referral for antivirals.
-
Monitor symptoms closely:
-
Use a pulse oximeter if you have one (seek help if oxygen ≤94%).
-
Watch for worsening breathlessness, chest pain, or confusion.
-
-
Keep safe at home: Ventilate rooms, use masks if possible, and wash hands often — though once exposed, focus mainly on monitoring and treatment.
🚨 When to seek urgent help
-
Severe shortness of breath
-
Oxygen levels ≤92–94%
-
Chest pain, confusion, or sudden collapse
→ Call 999
❓ Is Covid still dangerous in 2025?
Why it feels less dangerous now
-
Vaccination and immunity: Most people have had jabs and multiple infections, so later bouts are usually milder.
-
Variants: Current strains spread more easily but often cause less pneumonia than the original virus.
-
Better treatments: Antivirals and steroids (when needed) are widely available.
Why it can still be dangerous
-
Vulnerable groups: People with lung disease, weakened immunity, or older age are still more likely to need hospital care.
-
Exacerbations: Even mild Covid can set off asthma or ABPA flares, or worsen bronchiectasis infections.
-
Long Covid: Some people continue to develop fatigue, breathlessness, or brain fog lasting weeks to months.
-
Hospital admissions: Lower than during the pandemic, but NHS hospitals still see severe cases every winter.
👉 In summary: For most healthy people, Covid now feels like a bad cold or flu. For people with ABPA, bronchiectasis, or severe asthma, it can still be a dangerous infection — which is why monitoring and access to antivirals remain important.
✅ Key message
With ABPA and bronchiectasis, you are more vulnerable to complications from Covid. Most people still recover at home, but you may be eligible for antivirals. Steroids are only used if your underlying condition flares or if your oxygen drops. Stay alert, act quickly if symptoms worsen, and reach out for NHS support as soon as you test positive.