National Aspergillosis Centre Video Recordings

NAC Monthly Patient Meetings
The NAC monthly patient meetings provide a friendly, supportive, and informative space for anyone living with aspergillosis or related conditions. Hosted by the National Aspergillosis Centre (NAC), these sessions bring together patients, carers, and healthcare professionals to:
-
share personal experiences
-
ask questions in a safe environment
-
hear the latest updates on treatments, research, and self-care strategies
🎥 Watch past sessions
Our YouTube channel now has 87 recordings, covering everything from expert talks to personal patient stories. Whatever your stage in the journey — newly diagnosed or managing your condition for years — you’ll find something helpful and relatable.
Recent Highlights
-
September — Explored how Artificial Intelligence can support patients in finding trustworthy information. We also answered community questions about biologic medications, looking at what research tells us about their long-term effectiveness in asthma and ABPA.
-
August — Focused on new biologics for severe asthma, discussing why they don’t always work for everyone, and why some patients see benefits fade over time.
-
July — Shared updates from the British Thoracic Society meeting in Manchester, plus further insights into what the future may hold for biologic treatments.
💡 Whether you want practical advice, the latest medical updates, or simply the chance to connect with others who truly understand your journey, the NAC monthly meetings are here for you.
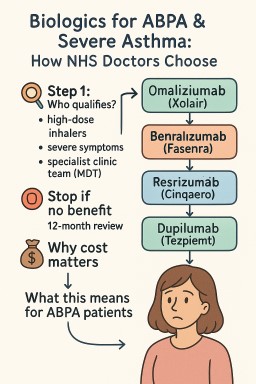
💊 Biologics for ABPA & Severe Asthma: How NHS Doctors Choose
Biologics are modern injection or infusion treatments that target the immune system. They can help people with Allergic Bronchopulmonary Aspergillosis (ABPA) by reducing inflammation, cutting down on steroid use, and lowering flare-ups.
In the UK, consultants must follow NICE (National Institute for Health and Care Excellence) guidance, which sets both clinical criteria and cost-effectiveness rules.
🔎 Step 1: Who qualifies?
-
You must already be on high-dose inhalers and still have severe symptoms.
-
Decisions are made by a specialist severe asthma / ABPA clinic team (MDT).
-
Blood tests, flare history, and steroid use are all considered.
🧭 Step 2: Which biologic?
Consultants match the drug to the type of inflammation you have:
| Pathway / Clues | Possible Biologic | Notes |
|---|---|---|
| IgE-allergic (allergic tests positive, high IgE) | Omalizumab (Xolair) | Works best if perennial allergies are driving symptoms. |
| Eosinophilic (high eosinophil counts, frequent flare-ups, or long-term steroid use) | Mepolizumab (Nucala) or Benralizumab (Fasenra) | NHS requires doctors to choose the least-expensive if both fit. |
| Eosinophils ≥400 + frequent flare-ups | Reslizumab (Cinqaero, IV drip) | Less used, but an option if IV therapy is acceptable. |
| Still severe after above / not eligible | Dupilumab (Dupixent) | Also helps if you have eczema or nasal polyps. |
| Any type, severe with ≥3 flare-ups or on daily steroids | Tezepelumab (Tezspire) | Works even if blood tests don’t show high eosinophils or IgE. |
🛑 Step 3: Stop if no benefit
NICE requires a 12-month review.
-
If your flare-ups or daily steroid dose haven’t fallen enough (usually by ≥50%), treatment should stop.
💷 Why cost matters
-
The NHS only funds biologics judged “cost-effective.”
-
If two drugs are equally suitable, consultants must use the least-expensive one.
-
This doesn’t mean you won’t get the right drug — but sometimes doctors must justify why one biologic is better for you personally.
📌 What this means for ABPA patients
-
ABPA is not directly covered by NICE guidance, but the same biologics are often used if you also meet asthma criteria.
-
Main goals:
-
Reduce oral steroids (prednisolone) and their side-effects.
-
Control flare-ups and lung damage.
-
-
Evidence supports omalizumab, mepolizumab, benralizumab, and dupilumab in ABPA; tezepelumab has less data so far.
✅ Bottom line:
Biologics can be life-changing for ABPA patients, but the NHS pathway means the choice depends on your blood results, flare history, steroid needs — and cost-efficiency rules. If one option doesn’t work, another may still be possible.
Information on Allergic BronchoPulmonary Aspergillosis (ABPA) / SAFS – For Family and Friends
Print out or share electronically
WHAT IT IS
ABPA (Allergic Bronchopulmonary Aspergillosis) and SAFS (Severe Asthma with Fungal Sensitisation) are allergic reactions to a common fungus, Aspergillus. In some people with asthma, the immune system overreacts to spores in the air, causing inflammation, swelling, and mucus plugs in the lungs.
WHAT IT'S NOT
-
Not contagious – you can't catch it.
-
Not poor hygiene – Aspergillus is everywhere in the air.
-
Not the patient's fault – flare-ups happen because of the condition, not something they did or didn't do.
WHY AREN'T OTHERS AFFECTED?
Most people's lungs clear these spores easily. In ABPA/SAFS the immune system reacts too strongly – more likely with long-standing asthma, severe allergies, damaged airways (e.g., bronchiectasis), or a genetic tendency. It's not weakness or lifestyle choices – often just lung history and bad luck.
TYPICAL SYMPTOMS
-
Wheezing, cough (sometimes with mucus plugs)
-
Breathlessness
-
Severe fatigue
-
Sometimes coughing up blood
WORST SYMPTOMS
-
Mucus plugs – thick, sticky clumps blocking airways, making breathing suddenly harder.
-
Intense coughing – can be exhausting, cause chest pain, and disrupt sleep.
TREATMENT
-
Anti-inflammatory medicines (often steroids)
-
Antifungals to reduce Aspergillus in the airways
-
Biologics for severe asthma/allergic inflammation
-
Monitoring with blood tests, breathing tests, and scans
THE REALITY
This condition can dominate daily life. On bad days the person may not be able to do much at all. Energy and breathing can change day-to-day (even hour-to-hour). If plans are cancelled, it isn't a lack of interest – it's the illness. Flare-ups can also make people feel short-tempered – a natural reaction to frustration, not a lack of care. Many people also live with a constant awareness of environmental risks – weighing up every new place or activity for dust, damp, or spores. This can feel exhausting and may lead them to avoid situations that others wouldn’t think twice about.
LOOKING AHEAD
-
With good control – Many people manage their symptoms well, reduce flare-ups, and keep active with the right treatment and avoidance of triggers.
-
Risks – Without good control, repeated flare-ups can slowly damage the lungs and lead to bronchiectasis.
-
Change over time – Some improve and need less treatment; others have ongoing ups and downs. Early action on flare-ups makes a big difference.
ENVIRONMENTAL TRIGGERS & PROTECTION
Some people with ABPA or SAFS have to avoid dust, mould, strong smells, smoke, and damp places – these can trigger flare-ups. Activities like gardening, compost turning, or DIY can be risky because they release fungal spores into the air. Wearing a well-fitting mask (e.g., FFP2/FFP3) can help reduce exposure – it's about staying well, not being antisocial.
HOW FRIENDS AND FAMILY CAN BEST HELP
-
Be flexible with plans – energy and breathing can change suddenly; last-minute cancellations aren't personal.
-
Help avoid triggers – choose low-dust, low-mould venues and activities.
-
Support treatment routines – lifts to appointments, collecting prescriptions, or reminders if welcome.
-
Listen without judgement – let them share symptoms and frustrations.
-
Encourage safe activities – suggest hobbies and outings with low environmental risk.
-
Show affection and reassurance – a hug, a kind message, or checking in can mean a lot.
MORE INFORMATION & SUPPORT
National Aspergillosis Centre (UK): https://mft.nhs.uk/wythenshawe/services/infectious-diseases/national-aspergillosis-centre/
Patient information & community: https://aspergillosis.org
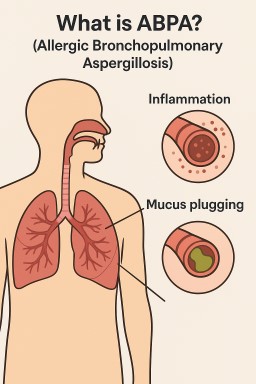
📘 What is ABPA? (Allergic Bronchopulmonary Aspergillosis)
Patient handout for A&E staff who ask what aspergillosis is.
What is ABPA?
ABPA is an allergic lung condition caused by the immune system overreacting to the fungus Aspergillus. It mainly affects people with asthma or cystic fibrosis.
When Aspergillus spores are inhaled, most people clear them without issue. In ABPA, the immune system sees these spores as dangerous and mounts a strong inflammatory response. This leads to asthma-like symptoms, mucus plugging, and can result in permanent lung damage (bronchiectasis) if left untreated.
Symptoms
-
Worsening breathlessness
-
Wheezing, chest tightness
-
Coughing up thick, often brown mucus
-
Fever, fatigue, or feeling generally unwell
-
Unintentional weight loss (advanced cases)
Diagnosis
-
History of asthma or cystic fibrosis
-
High IgE levels and positive Aspergillus-specific IgE
-
Eosinophilia (raised white blood cells)
-
Sputum culture or PCR positive for Aspergillus
-
Chest imaging showing mucus plugging or bronchiectasis
Treatment
-
Oral corticosteroids (e.g. prednisolone) to reduce inflammation
-
Antifungal medication (e.g. itraconazole) to lower fungal burden
-
Biologic therapies (e.g. omalizumab or benralizumab) in some patients
-
Regular monitoring by respiratory or infectious diseases specialists
Key Points for A&E:
✅ ABPA is an allergic lung disease, not a classical infection
✅ Can present with severe asthma, mucus plugging, or type 2 respiratory failure
✅ Requires early recognition and often systemic steroids and antifungal therapy
✅ Take bloods (IgE, eosinophils, CRP), consider chest imaging, and review oxygen status
📍 For specialist support:
National Aspergillosis Centre (NAC)
🏥 Wythenshawe Hospital, Manchester University NHS Foundation Trust
🌐 NAC homepage on MFT website https://mft.nhs.uk/wythenshawe/services/infectious-diseases/national-aspergillosis-centre/
🌐 www.aspergillosis.org
📞 Daytime contact: 0161 291 2891 or 0161 291 4362
📞 Urgent out-of-hours: Call Wythenshawe switchboard on 0161 998 7070
📢 Ask for the on-call Infectious Diseases Consultant
🫁 Is It an ABPA Flare or a Bronchiectasis Flare? How to Tell the Difference
If you have aspergillosis, especially ABPA (Allergic Bronchopulmonary Aspergillosis) and bronchiectasis, it can be hard to know which one is flaring up when your lungs feel worse. They often overlap — but there are some clues that can help.
🔍 How the Two Conditions Are Different
| Feature | ABPA Flare (Allergic Reaction to Aspergillus) | Bronchiectasis Flare (Infection in Damaged Airways) |
|---|---|---|
| Main cause | Your immune system reacting to Aspergillus | Infection in widened, inflamed airways |
| Symptoms you may notice | - Chest tightness or wheezing - Thick, sticky mucus - Feeling more tired - Occasional low-grade fever |
- Wet cough with more sputum - Sputum changes colour (green/yellow) - Fever, chills, or general unwell feeling |
| How it starts | May come on gradually or after exposure to damp/mould | Often starts after a cold or virus |
| What helps most | Steroids (inhaled or oral), sometimes biologics | Antibiotics and chest physiotherapy |
| What tests may show | - Raised IgE or eosinophils - CT may show mucus plugs |
- Raised CRP or white cells - Sputum may grow bacteria or fungus |
| What to ask your doctor | “Is my IgE or eosinophil count up?” | “Do I need a sputum test or antibiotics?” |
🧭 What Can You Do as a Patient?
-
📝 Keep a symptom diary – especially note changes in:
-
Sputum colour or amount
-
Wheezing or chest tightness
-
Tiredness or sleep quality
-
-
🧪 Ask for the right tests:
-
Blood tests like IgE and eosinophils for ABPA
-
CRP, white blood count, and sputum tests for bronchiectasis
-
-
🩺 Don’t guess or self-treat – steroids and antibiotics work in different ways, and using the wrong one can make things worse or mask important signs.
💬 Final Thought
It's very common for people with aspergillosis to feel confused by flare-ups — you're not alone. Learning to spot your own patterns, and getting support from your specialist team, can make a real difference.
🧵 Why Am I Getting More “Plugs” This July?
A message for aspergillosis patients
July is often a time when people with aspergillosis feel a bit better — but sometimes, things don’t go quite to plan. If you’ve suddenly started getting more mucus “plugs” or are struggling to clear your chest, here are some possible reasons:
🔍 Common Reasons for More Mucus or Plugs in Summer
| Possible Cause | Why it might affect you now |
|---|---|
| Fungal spores are high | July and August bring very high outdoor levels of Aspergillus, Cladosporium, and other moulds – especially on dry, windy days or after cutting grass. These can trigger inflammation and more mucus. |
| Pollen season continues | Even though tree pollen has gone, grass, weed, and cereal pollen are still in the air. These can worsen symptoms for people with ABPA or asthma. |
| Humidity or storms | Sudden weather changes, humid air, or storms can make breathing more difficult and mucus harder to shift. Some people call this "thunderstorm asthma." |
| Air pollution (ozone) | Sunny weather increases ozone and air pollution – both can irritate your airways. |
| Low-level infection or flare-up | If your mucus is thicker, darker, or smells different, it might be a sign of a fungal or bacterial flare-up, even without a high temperature. |
| Hydration or medication changes | Less water, skipping nebulisers, or changes in routine can make mucus stickier. |
| Blocked sinuses | Post-nasal drip from fungal sinusitis can make it feel like mucus is always sitting in your throat or upper chest. |
✅ What You Can Do
-
Drink more fluids, especially warm water or squash
-
Use saline in your nebuliser to loosen thick mucus
-
Do your chest clearance exercises more often – flutter device, ACBT, or huffing
-
Don’t skip antifungals, inhalers, or mucolytics like carbocisteine
-
Consider a nasal rinse if your sinuses feel blocked
-
Keep windows closed on high spore or high pollen days
-
Speak to your team if things don’t settle – you may need a review or antibiotics
⚠️ When to Get Checked
-
You're coughing up yellow, green or brown mucus
-
Mucus smells bad or has blood in it
-
You feel more breathless or more tired
-
You’ve needed to increase your nebuliser use
💬 You're Not Alone
Many patients with aspergillosis get more mucus at this time of year — even when the sun’s out! Don’t assume it’s “just the weather.” Sometimes it’s a sign that your lungs or sinuses are reacting to invisible spores in the air.
Biologics and Long Term Side Effects
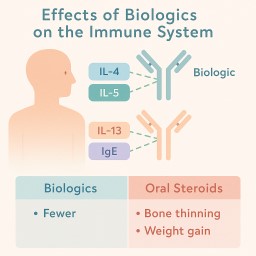
✅ What Are Biologics?
Biologics are targeted treatments made from living cells. They work by blocking parts of the immune system that cause inflammation — for example:
-
IL-4, IL-5, IL-13: linked to eosinophilic inflammation
-
IgE: linked to allergies and ABPA
They are not immunosuppressants like steroids or chemotherapy, but rather immune modulators.
💊 Long-Term Side Effects – What Do We Know?
👨⚕️ What research and experience show:
| Biologic | Used for | Long-term safety known? | Side effects most reported |
|---|---|---|---|
| Omalizumab (Xolair) | Allergic asthma, ABPA | 20+ years of use | Injection site reactions, headache, very rare anaphylaxis |
| Mepolizumab (Nucala) | Eosinophilic asthma, CPA | 10+ years | Fatigue, headache, shingles (rare), mild infections |
| Benralizumab (Fasenra) | Severe asthma, CPA | ~6–7 years | Headache, pharyngitis, injection site issues |
| Dupilumab (Dupixent) | Asthma, eczema, nasal polyps | 6–8 years | Eye dryness/redness, cold sores, joint pain (rare) |
| Tezepelumab (Tezspire) | Severe asthma | ~2 years | Sore throat, joint pain, injection site reactions |
⚠️ Possible Long-Term Concerns (but rare)
-
Infections: Some concern about slightly increased risk of herpes zoster (shingles) or respiratory viruses, but overall risk is very low compared to steroids.
-
Immunogenicity: Your body might develop antibodies to the drug over time, reducing its effect — this is more a loss of benefit, not a dangerous side effect.
-
Cancer risk: No consistent evidence linking asthma/ABPA biologics to cancer.
-
Unknowns: Because some biologics are new (e.g. tezepelumab), we don't yet have 20-year data — but so far the safety profile is reassuring.
🩺 Compared to Oral Steroids
| Treatment | Side Effects Over Time |
|---|---|
| Steroids (e.g. prednisolone) | Weight gain, diabetes, infections, bone thinning, cataracts, adrenal suppression |
| Biologics | Mostly minor – injection site pain, headache, mild infection risk, rare allergic reaction |
So in most cases, biologics reduce the need for steroids and therefore reduce long-term harm.
💬 Patient Experience
Most patients report:
-
Improved quality of life
-
Reduced asthma/ABPA attacks
-
Fewer hospital visits
-
Very few stop due to side effects
✅ Summary
| Question | Answer |
|---|---|
| Do biologics have long-term side effects? | Usually mild and rare; mostly injection reactions or mild infections |
| Are they safer than long-term steroids? | Yes, especially over years |
| Should I be worried? | Not usually — but always monitor with your team |
| How long have they been used? | 6–20+ years, depending on the biologic, with very good safety data |
😷 Coping With Masks: Advice for People With Aspergillosis Who Struggle to Wear One
For people living with aspergillosis, asthma, or other lung conditions, wearing a facemask can sometimes feel uncomfortable — even frightening. You may feel like you can’t breathe properly, become hot or anxious, or feel claustrophobic. Some patients avoid masks altogether, even when they want to wear one to protect themselves from spores, pollution, or infection.
This guide is here to reassure you: you are not alone, and there are ways to make mask-wearing safer and more comfortable.
🫁 "I Can’t Breathe in a Mask" – Is This Normal?
Yes — many people with respiratory conditions feel this way. But here’s what the science tells us:
✅ For most people, even those with chronic lung disease, oxygen levels are not reduced by wearing a mask
❌ The feeling of not getting enough air is often caused by:
-
Anxiety or shallow breathing
-
The heat and humidity under the mask
-
The sensation of restricted airflow, not actual oxygen deprivation
💡 Helpful Tips If You Find Masks Difficult to Wear
1. Practise in a calm setting
Start wearing your mask for short periods at home, where you feel safe. Use calming breathing (slow in through the nose, out through the mouth). This helps your brain and lungs get used to the sensation.
2. Choose a mask that suits your needs
Different types of masks feel very different to wear.
| Problem | Suggested Mask |
|---|---|
| Feels suffocating or hot | Structured FFP2 or duckbill-style masks (keep shape off your face) |
| Claustrophobic | Surgical masks (lighter and looser fitting) |
| Strong reactions to smells or pollution | FFP2/FFP3 masks or Vogmask with carbon filter |
| Sweat or overheating | Lightweight cotton or disposable masks with cooling fabric or filter inserts |
3. Use your inhaler beforehand (if prescribed)
Some people with asthma or ABPA find wearing a mask easier after using their reliever inhaler (blue) 10–15 minutes beforehand.
4. Take breaks when needed
If you’re in a safe place (like outdoors, away from people), it’s okay to briefly lift your mask and take a few calm breaths — especially if you're struggling. You don't need to wear it all the time to benefit.
5. Try alternatives in low-risk settings
If you genuinely can’t tolerate a mask:
-
Wear one only in crowded indoor areas (shops, clinics, transport)
-
Consider using a face shield over a mask or in short exposures (note: shields protect others less)
-
Maintain distance and ventilation in mask-free spaces
🔁 Don’t Let One Bad Experience Stop You
Struggling to wear a mask doesn’t mean you’ve failed — it just means you need to try something different. Many patients find that with the right mask and some breathing strategies, they can use one when it matters most.
Remember, even wearing a mask for short periods (e.g. clinic waiting room, pharmacy queue) offers valuable protection.
🧠 Why It Matters for Aspergillosis
People with aspergillosis often need to avoid airborne risks like:
-
Fungal spores (especially Aspergillus fumigatus)
-
Pollution and chemicals
-
Viral infections that could worsen lung damage
Wearing a well-fitting FFP2 or FFP3 mask, especially in higher-risk situations, is one of the best ways to reduce exposure.
🤝 You're Not Alone
If you feel overwhelmed, isolated, or panicked when wearing a mask — you are not alone. Many others in the aspergillosis community feel the same way. With time, support, and the right mask, it often gets easier.
📝 Summary: What You Can Try
-
✅ Practise wearing a mask at home for short periods
-
✅ Try structured masks (like FFP2 duckbill) for better airflow
-
✅ Use a reliever inhaler beforehand if needed
-
✅ Take short breaks if it becomes too uncomfortable
-
✅ Don’t wear a mask all the time — just when it matters most
🛡️ FFP2/FFP3 Mask Use in Aspergillosis: Summary
| Mask Type | Who Might Use It | When It's Used |
|---|---|---|
| FFP2 (95% filtration) | Some patients with CPA, ABPA, or SAFS, especially during flares or hospital visits | During travel on public transport, clinic waiting rooms, visiting building sites, or dust exposure |
| FFP3 (99% filtration) | Patients who are severely immunocompromised (e.g. post-transplant, on chemotherapy, or high-dose steroids) | In high-risk environments: hospital construction, building work nearby, or heavy dust/mould exposure |
✅ When Masks Might Be Advisable
-
During hospital visits, particularly in winter or during flu/COVID waves
-
If you're immunosuppressed, e.g. taking long-term steroids or biologics
-
When exposed to mouldy buildings, compost, building work, or flood damage
-
In crowded indoor environments where infection risk is high
❌ When They’re Usually Not Needed
-
Day-to-day life in a clean, dry home environment
-
Low-risk outdoor activity (e.g. walking in the park)
-
If your asthma/ABPA/CPA is stable and you're not immunocompromised
🗣️ What the National Aspergillosis Centre Recommends
-
Use FFP2 masks when entering environments likely to have airborne fungal spores
-
FFP3 masks may be offered for high-risk medical procedures or when severely immunocompromised
-
Masks are one part of a broader protection strategy, which includes:
-
Good indoor air quality (HEPA filters, ventilation)
-
Avoidance of dusty environments
-
Prompt treatment of fungal infections
-
🌬️ Living with Asthma and Aspergillosis: Understanding the Overlap, the Immune System, and the Right Treatment
If you live with asthma and have been told you also have aspergillosis, such as ABPA (Allergic Bronchopulmonary Aspergillosis) or SAFS (Severe Asthma with Fungal Sensitisation), your situation is more complex than most people realise.
This guide explains:
-
The different types of asthma
-
How aspergillosis complicates asthma
-
The role of eosinophils, IgE, and the immune system
-
Why some people don’t have “typical” symptoms (like wheeze)
-
What treatments are available — and how to personalise your care
🧠 Asthma Isn’t One Disease
Asthma is a condition where the airways (breathing tubes) become:
-
Inflamed (swollen and irritated)
-
Overreactive to certain triggers (allergens, cold air, infection, etc.)
-
Narrowed and often filled with mucus, making breathing difficult
But not everyone with asthma has the same cause, symptoms, or treatment response. Asthma actually includes many subtypes — and understanding your type is key to getting the right care.
🧬 Common Asthma Types in Aspergillosis
| Asthma Type | Cause / Trigger | Key Features |
|---|---|---|
| Allergic asthma | IgE-driven allergy to pollen, dust, pets, fungi | Common in early-life asthma |
| Eosinophilic asthma | High levels of eosinophils (a white blood cell) | Often adult-onset and hard to control |
| SAFS | Allergy to fungi (especially Aspergillus) | Severe, steroid-resistant asthma |
| ABPA | Allergic reaction to Aspergillus growing in lungs | Very high IgE, eosinophils, mucus, lung damage |
| Cough-variant asthma | Inflammation without wheeze | Dry cough as the only symptom |
| “Silent” asthma | Reduced or absent warning signs | No wheeze, may present with fatigue, cough or breathlessness only |
🫢 New Section: What Is “Silent Asthma”?
“Silent asthma” is not an official medical term, but it’s used to describe:
-
Asthma without the classic wheeze (often just cough or tightness)
-
Or where asthma attacks happen suddenly, without clear warning
This is important because:
-
People may not realise they have asthma
-
Diagnosis may be delayed or missed
-
Flare-ups can be severe or even life-threatening
-
It may occur in people with fungal asthma, ABPA, or airway damage
Silent asthma is especially relevant in:
-
Older adults
-
People with ABPA or SAFS
-
People with cough-variant asthma
-
Anyone whose asthma doesn’t “sound” typical
🧪 Tests like FeNO, spirometry, and blood eosinophil counts are vital for confirming what’s really happening inside the lungs — even if symptoms are subtle.
🔬 Why ABPA Adds Complexity
If you have ABPA, the asthma symptoms are made worse by:
-
A hypersensitive immune reaction to Aspergillus fumigatus
-
Mucus plugging and blocked airways
-
Lung damage (bronchiectasis) that doesn’t improve with inhalers alone
-
A mix of allergic and eosinophilic inflammation
Key signs include:
-
Extremely high IgE levels
-
Raised eosinophils
-
Positive blood tests for Aspergillus
-
Lung CT scan changes
💊 Treatment Options Based on Asthma Type
| Treatment | Used For |
|---|---|
| Inhaled corticosteroids (ICS) | All types, first-line |
| Antifungal medications | ABPA, SAFS |
| Oral steroids (e.g. prednisolone) | ABPA flares, severe asthma |
| Biologics (e.g. mepolizumab, omalizumab) | Severe allergic or eosinophilic asthma |
| Chest physiotherapy | Mucus clearance in ABPA or bronchiectasis |
Each treatment is tailored based on whether your asthma is driven by:
-
IgE (allergy)
-
Eosinophils (inflammation)
-
Fungal exposure or colonisation
📍 What to Discuss with Your Healthcare Team
If you:
-
Have asthma that isn’t well controlled
-
Need frequent steroids
-
Have a chronic cough, thick mucus, or lung damage
-
Have high IgE or eosinophils
-
Or don’t wheeze, but still get breathless or fatigued…
… it’s important to ask your doctor:
-
Could I have ABPA or SAFS?
-
Is there a fungal or eosinophilic component to my asthma?
-
Should I be tested for Aspergillus allergy or IgE?
-
Am I a candidate for biologics or antifungals?
✅ Final Takeaway
Asthma with aspergillosis is more than just “bad asthma” — it’s a complex condition involving allergy, inflammation, fungal exposure, and in some cases, permanent airway changes. Some patients don’t experience wheeze — this is called “silent asthma,” and it deserves just as much attention.
You don’t have to manage this alone — and there are now targeted treatments that can help reduce symptoms, prevent damage, and improve quality of life.