🛡️ How Your Care is Changing: Understanding Antimicrobial Stewardship
A guide for patients with aspergillosis and chronic lung conditions
If you're being treated for chronic pulmonary aspergillosis (CPA), ABPA, or any long-term lung condition, you might notice changes in the way doctors use antifungal and antibiotic medicines. These changes are part of a worldwide effort to tackle antimicrobial resistance (AMR) — and to make sure the right treatment is used, in the right place, for the right reason.
💬 What is Antimicrobial Stewardship?
Antimicrobial stewardship (AMS) means using antifungal and antibiotic medications responsibly, so they work better now and stay effective for the future.
It’s about:
-
Using the right medication
-
In the right place
-
For the right reason
-
At the right dose and duration
This helps ensure patients get better faster, and we all stay protected from drug-resistant infections.
🔬 What Is Antimicrobial Resistance?
Antimicrobial resistance (AMR) happens when bacteria or fungi evolve and stop responding to medicines that used to work. This makes infections:
-
Harder to treat
-
More likely to come back
-
More dangerous for people with lung or immune conditions
There are two major types:
-
Antibiotic resistance (bacteria)
-
Antifungal resistance (fungi, including Aspergillus fumigatus)
💊 Antibiotics: Broad vs Narrow Spectrum
Doctors aim to use targeted antibiotics wherever possible. Here’s how they differ:
| Type | Description | Examples | Used For |
|---|---|---|---|
| Broad-spectrum | Kills a wide range of bacteria | Co-amoxiclav, meropenem, ceftriaxone | Sepsis, serious infections |
| Narrow-spectrum | Targets specific bacteria | Penicillin, nitrofurantoin, flucloxacillin | Simple infections |
🧪 Doctors may start with broad-spectrum drugs in emergencies but switch to narrow-spectrum when test results are available — this is called de-escalation.
🦠 Antifungal Resistance and Aspergillosis
People with CPA or ABPA are often treated with antifungals like:
-
Itraconazole
-
Voriconazole
-
Posaconazole
-
Isavuconazole
But fungi can develop resistance, especially when:
-
Medications are used long-term
-
Fungi are exposed to azole sprays on crops and flowers
You may inhale resistant spores from:
-
Compost, potting soil, or garden centres
-
Fresh flowers (especially imported ones)
🏥 What Might You Notice in Hospital?
✅ Shorter or targeted treatment
-
You may be on 5–7 days of antibiotics/antifungals
-
Switch from IV to tablets happens earlier once you're stable
✅ Treatment reviews
-
Your medication will be reviewed within 48–72 hours
-
Changes may be made based on lab results
✅ More testing
-
Blood, sputum, or biopsy samples help identify infections and resistance
-
Ensures you get the right treatment
✅ Specialist involvement
-
An infection or respiratory consultant may review your case if resistant infection is suspected
✅ Infection control
-
You may notice:
-
No fresh flowers
-
HEPA filters in some wards
-
Staff using extra precautions to prevent airborne infections
-
🏡 What Might You Notice From Your GP?
✅ More specific prescribing
-
GPs are less likely to give antibiotics “just in case”
-
More narrow-spectrum choices based on the suspected infection
✅ Diagnostic support
-
GPs may send sputum or urine samples before prescribing
-
May test your blood for antifungal levels (TDM)
✅ Home safety advice
You may be advised to:
-
Avoid indoor compost or plant pots
-
Wear FFP2/FFP3 masks when gardening
-
Keep indoor air well ventilated
🧬 New Antifungals Being Protected for Patient Use
Several antifungals are in development and being reserved just for medical use (not agriculture), including:
| Drug | What it is | Why it matters |
|---|---|---|
| Rezafungin | Weekly IV echinocandin | Long-lasting for serious infections |
| Ibrexafungerp | First oral alternative to azoles | Trials for aspergillosis |
| Olorofim | New class (DHODH inhibitor) | Active against resistant Aspergillus |
| Opelconazole | Inhaled antifungal | Direct treatment to the lungs |
| Fosmanogepix | Novel target | Works against drug-resistant fungi |
🧠 What This All Means for You
These changes are about:
-
Better outcomes — faster recovery with fewer side effects
-
Preventing resistance — protecting future treatments
-
More personalised care — based on test results and your condition
✅ What You Can Do
| Action | Why It Helps |
|---|---|
| Take medications exactly as prescribed | Prevents underdosing and resistance |
| Don’t stop treatment early | Even if you feel better |
| Ask if your treatment has been reviewed | Encourages early switch or adjustment |
| Use a mask and gloves for gardening | Reduces spore exposure |
| Avoid fresh flowers and compost indoors | Especially in bedrooms or when unwell |
| Report any new or worsening symptoms | Resistance may be developing |
| Ask about resistance testing if you’re not improving | Labs can check fungal response |
| Stay informed and speak up | You’re part of the stewardship solution |
📌 In Summary: Stewardship in Action
Antimicrobial stewardship is not about doing less — it's about doing things more precisely.
It’s how your healthcare team makes sure you receive:
The right medication, in the right place, for the right reason.
🔗 Want to Learn More?
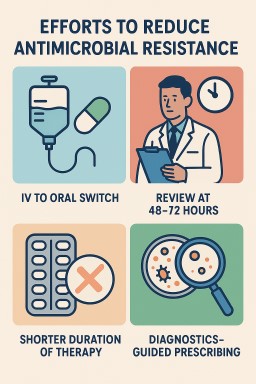
💊 General Strategies to Reduce Antimicrobial Resistance in Clinical Practice
1. IV to Oral Switch (IVOS)
One of the most effective and safe interventions in antimicrobial stewardship.
🔁 Why switch from IV to oral early?
-
Reduces complications (e.g. line infections, thrombosis)
-
Lowers costs and bed-days
-
Improves patient comfort and mobility
-
Oral options (e.g. ciprofloxacin, fluconazole, linezolid) are highly bioavailable, often matching IV efficacy
✅ When is IVOS appropriate?
-
Clinical improvement seen
-
Source controlled
-
Oral route available and tolerated
-
Suitable oral alternative exists
NHS guidance: "Start smart – then focus" encourages early IVOS reviews within 48–72 hours of antibiotic initiation.
2. "Start Smart – Then Focus" (UK NHS Framework)
This key NHS antimicrobial policy includes:
-
Start Smart: Prescribe antibiotics appropriately from the beginning
-
Then Focus:
-
Review at 48–72 hours
-
Consider stop, switch, change, or continue
-
Document clearly in records
-
Supported by NICE guidelines and UKHSA audits
3. Shorter Duration of Therapy
For many infections, shorter courses (e.g. 5–7 days instead of 10–14) are now preferred.
Examples:
-
Community-acquired pneumonia: 5 days
-
Pyelonephritis: 7 days
-
Cellulitis: 5–7 days
This reduces resistance pressure and side effects.
4. Diagnostics-Guided Prescribing
-
Procalcitonin and CRP tests can help distinguish bacterial from viral infections
-
Rapid PCR, MRSA, or blood culture diagnostics guide targeted therapy
The aim is avoid empirical broad-spectrum antibiotics where possible.
5. Restricted Prescribing Policies
-
Certain high-risk drugs (e.g. carbapenems, vancomycin, antifungals) are restricted to ID approval
-
Antimicrobials are tiered by risk (e.g. traffic light systems) to encourage narrow-spectrum use
6. Antimicrobial Stewardship Teams (ASTs)
Multidisciplinary teams:
-
Lead on stewardship strategy
-
Audit antimicrobial use
-
Provide decision support for complex cases
-
Educate staff and update local formularies
In the NHS, stewardship is a CQUIN target (incentivised performance indicator).
7. Education and Behaviour Change
-
Mandatory AMS training for junior doctors and prescribers
-
Behavioural nudges in electronic prescribing systems (e.g. default shorter durations, alert for IVOS)
8. Surveillance and Reporting
-
ePAMS+, ESPAUR, and PHE Fingertips dashboards track:
-
Prescribing by hospital/unit
-
Resistance trends
-
Audit compliance with IVOS, duration, and documentation
-
9. Patient-Facing Initiatives
-
"Antibiotic Guardian" and leaflets explaining viral vs bacterial infections
-
Empowering patients to ask:
"Do I really need antibiotics? When can I switch to tablets?"
📦 Summary Table: Key Interventions
| Strategy | Purpose |
|---|---|
| IV to Oral Switch | Reduce IV duration, speed discharge |
| Review at 48–72 hrs | Reassess need, de-escalate if possible |
| Shorter therapy courses | Lower resistance pressure |
| Targeted diagnostics | Support narrow-spectrum prescribing |
| Prescribing restrictions | Protect last-resort antimicrobials |
| Stewardship teams | Oversee, audit, educate |
| Surveillance & feedback | Monitor trends, guide policy |
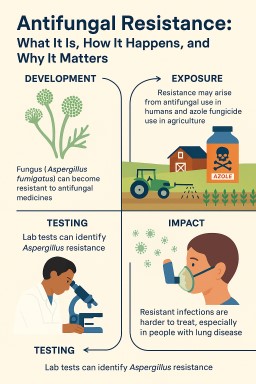
🦠 Antifungal Resistance: What It Is, How It Happens, and Why It Matters
Antifungal resistance is a growing global health threat, especially for people with lung conditions like chronic pulmonary aspergillosis (CPA) or allergic bronchopulmonary aspergillosis (ABPA). Just like bacteria can become resistant to antibiotics, fungi like Aspergillus fumigatus can develop resistance to antifungal drugs — making infections harder or even impossible to treat.
🔍 What Is Antifungal Resistance?
Antifungal resistance occurs when fungi evolve in ways that allow them to survive exposure to medications that used to kill them or stop their growth. This makes standard treatments less effective and increases the risk of:
-
Treatment failure
-
Prolonged illness
-
More severe infections
-
Increased hospital stays and costs
-
Higher death rates in vulnerable patients
🧬 How Does It Develop?
Fungi become resistant through genetic changes, often due to:
-
Long-term antifungal treatment in patients
-
Widespread environmental exposure to antifungal chemicals — especially azoles used on crops
Once resistance develops, the fungus may stop responding to key drugs like:
-
Itraconazole
-
Voriconazole
-
Posaconazole
-
Isavuconazole
These are the mainstays of treatment for aspergillosis and other serious fungal infections.
🌾 The Role of Agriculture: A Hidden Driver
Many resistant strains of Aspergillus don’t develop in people — they develop in the environment, especially in farmland and flower production areas.
Why?
The azole fungicides used on crops are chemically very similar to the azoles used in human medicine. They target the same fungal enzyme (CYP51, involved in cell wall formation). Fungi exposed repeatedly to these sprays can adapt — and the resulting resistant spores can:
-
Survive in soil, compost, and plant debris
-
Be carried on the wind
-
Be inhaled by people — especially those with weakened lungs or immune systems
High-risk areas include:
-
Grain farming (wheat, barley, maize)
-
Fruit production (apples, grapes, citrus)
-
Ornamental flowers (e.g., roses, tulips, chrysanthemums) — especially when imported or mass-grown
-
Garden centres and potting compost
🏠 Exposure at Home: Flowers, Soil, and More
People may unknowingly bring resistant Aspergillus spores into their homes through:
-
Fresh cut flowers (especially from florists using treated imports)
-
Potting compost or stored bulbs
-
Uncovered soil and plant material indoors
This is particularly dangerous for those with lung conditions, suppressed immunity, or recent surgery.
Practical tips:
-
Avoid keeping fresh flowers or pot plants in bedrooms or living areas
-
Use gloves and masks (FFP2 or FFP3) when handling soil or compost
-
Ventilate indoor spaces after gardening
💊 What’s Being Done: Medical, Policy, and Drug Development
1. Reserving drugs for clinical use
New antifungal drugs with novel mechanisms are being designed exclusively for medical use. Some are already approved or in late clinical trials:
| Drug | Type / Mechanism | Status | Notes |
|---|---|---|---|
| Rezafungin | Echinocandin (IV, once-weekly) | Approved 2023 (US/EU) | For Candida, with long half-life |
| Ibrexafungerp | Oral glucan synthase inhibitor | Approved 2021 (US) | Active against resistant Candida, in trials for Aspergillus |
| Oteseconazole | Oral tetrazole | Approved 2022 (US) | Less toxicity, fewer interactions |
| Olorofim | Pyrimidine synthesis inhibitor | Late trials | First in class, active against Aspergillus |
| Fosmanogepix | GWT1 enzyme inhibitor | Trials | New target, good against multi-drug resistant fungi |
| Opelconazole | Inhaled azole | Trials | Direct lung delivery, potential for aspergillosis |
Many of these drugs are being deliberately withheld from agriculture to protect their effectiveness.
2. Policy & regulation
-
The “One Health” approach is gaining ground: it recognises the links between human, animal, and environmental health.
-
Some countries are monitoring soil and air for resistant fungi (e.g. Netherlands, UK).
-
Campaigns are underway to regulate or ban agricultural use of triazoles that drive cross-resistance.
-
Hospitals increasingly restrict fresh flowers in high-risk wards to protect immunocompromised patients.
🧭 What Needs to Happen Next
-
Tighter coordination between agricultural and medical authorities to regulate antifungal use
-
Incentives for developing safer, non-cross-reactive fungicides for farming
-
Increased global surveillance of resistant fungi in both clinical and environmental settings
-
Patient and public education about the risks and how to reduce exposure
🧠 What Patients Can Do
If you live with aspergillosis, chronic lung disease, or weakened immunity:
✅ Take your antifungal medicine exactly as prescribed
✅ Don’t stop or change treatment without medical advice
✅ Ask about resistance testing if symptoms worsen
✅ Avoid exposure to soil, compost, and fresh flowers
✅ Use respiratory protection (FFP2/FFP3 masks) in dusty or mouldy environments
✅ Advocate for better public policies on antifungal stewardship
🔗 Want to Learn More?
Telecare Devices and the UK Digital Switchover: What Aspergillosis Patients and Carers Need to Know
Background By the end of 2025, traditional landline telephone networks in the UK will be phased out and replaced by digital (VoIP) systems delivered via broadband. This national "Digital Switchover" affects anyone using landline-based devices, including many telecare systems vital to people with chronic illnesses like chronic pulmonary aspergillosis (CPA), ABPA, and SAFS.
This document provides clear guidance for aspergillosis patients and carers concerned about how this change affects telecare equipment such as fall alarms, pendant buttons, and GPS trackers.
Why This Matters for Aspergillosis Patients Many people with aspergillosis rely on telecare to remain safe at home. These may include:
- Fall detectors
- Emergency pendant alarms
- Door sensors
- GPS trackers
- Daily wellbeing check-in devices
These systems were typically connected to analogue landlines. Once the switch to digital phone lines is made, some older devices may stop working correctly unless they are upgraded or adapted.
What Changes with the Digital Switchover?
| Feature | Current (Analogue Landline) | Future (Digital via Broadband) |
|---|---|---|
| Phone line works during power cuts | Yes | No (unless battery backup is added) |
| Telecare devices plug into phone socket | Yes | Only with compatible router or adapter |
| Works independently of broadband | Yes | No, relies on internet connection |
Common Concerns and Solutions
- "Will my current telecare alarm still work?"
- Possibly not. Many older alarms won't function over digital broadband lines.
- Solution: Ask your alarm provider if your device is VoIP compatible or if they can supply a digital-ready or cellular version.
- "Will full fibre broadband stop my telecare from working?"
- Not automatically, but older devices may be incompatible.
- Solution: If switching to full fibre, ensure your telecare system can plug into the new router or ask about an analogue telephone adapter (ATA) with battery backup.
- "What happens during a power cut?"
- Digital lines go down unless you have a UPS (Uninterruptible Power Supply) or the telecare device is cellular-based.
- "Can I upgrade to something more future-proof?"
- Yes. Many councils and private providers now offer mobile-enabled alarms with built-in SIM cards and GPS.
- These do not rely on landlines or home Wi-Fi.
What You Should Do Now
- Contact your telecare provider
- Ask if your current device is digital-compatible.
- Request upgrade options if needed.
- Speak to your broadband provider
- Let them know you use telecare. Ask about battery backup or compatibility.
- Contact your local Adult Social Care team
- Many councils are offering free or subsidised upgrades to digital or mobile telecare.
- Test your system
- Before and after switching broadband providers, run a test call with your alarm provider.
Summary As the UK phases out analogue landlines, it's essential for patients and carers to act early. Ensuring your telecare system is compatible with digital broadband will help maintain your independence and safety. Monitoring your oxygen saturation may also support early detection of lung health changes.
Resources for Further Help
- Aspergillosis Patient Support
- Aspergillus & Aspergillosis Resources
- Ofcom Digital Switchover Advice
- Your local council’s Adult Social Care department
If you have questions or need help contacting the right services, the National Aspergillosis Centre support team can guide you.
📄 Why Might My Posaconazole Levels Be Undetectable?
Understanding Antifungal Monitoring in Aspergillosis Treatment
If you’re taking posaconazole to treat Aspergillus-related conditions like ABPA (Allergic Bronchopulmonary Aspergillosis) or CPA (Chronic Pulmonary Aspergillosis), your doctor may ask for blood tests to check if the drug is reaching the right levels in your body.
Sometimes, those tests come back showing “undetectable” or “very low” levels, even when you’ve been taking the medication exactly as prescribed.
This can be worrying — but there are several common reasons this happens, and it doesn’t always mean the medicine isn’t working or that you’ve done something wrong.
❓ What Is Posaconazole?
Posaconazole is an antifungal medicine used to treat infections caused by the Aspergillus fungus. It comes in tablet, liquid, or IV forms. Most people take the tablet once a day — often for many weeks or months.
To work properly, the drug needs to reach a certain level in your bloodstream. This is why your team may request a blood test to check how well your body is absorbing it.
🔍 Reasons Your Posaconazole Levels May Be Low or Undetectable
1. Not Enough Fat in Your Diet
Posaconazole needs some fat in your meal to be absorbed properly — especially the liquid version.
Try to take it with a meal that includes:
-
Dairy (cheese, yoghurt, full-fat milk)
-
Eggs, nuts, or oily fish
-
A little olive oil or butter in cooking
Tip: Never take it on an empty stomach!
2. Other Medications or Supplements
Some medications and remedies can reduce how well posaconazole is absorbed, including:
-
Proton pump inhibitors (e.g. omeprazole, lansoprazole)
-
Antacids
-
Rifampicin
-
Herbal supplements like St John’s Wort
Let your doctor or pharmacist know about everything you take — even vitamins and over-the-counter products.
3. Timing of the Blood Test
The blood test should be taken just before your next dose (called a trough level).
If it’s taken too early (after a fresh dose), or too late (if you missed a dose), it may give a misleading result.
4. Problems with Absorption
Some medical conditions can make it harder for your body to absorb medications, including:
-
Coeliac disease
-
Crohn’s or colitis
-
Chronic diarrhoea or digestive issues
If you have any of these, your doctor may suggest an alternative form — like switching from liquid to tablet or tablet to IV.
5. Lab or Sample Error
Occasionally, there may be a problem with the blood sample — like a delay in handling, or a lab processing issue. In that case, your team may simply repeat the test.
✅ What You Can Do
✔️ Take your medicine with food (especially with fat)
✔️ Tell your team about other medications
✔️ Check which form you’re taking (tablets are usually better absorbed than the liquid)
✔️ Ask when your blood test should be done
✔️ Don’t panic if the result is low — just repeat the test with support from your team
🩺 Why This Matters
Getting the right amount of posaconazole in your body is essential to:
-
Help clear fungal infection
-
Prevent it from spreading
-
Reduce symptoms like coughing, breathlessness, and mucus
-
Avoid the risk of fungal resistance
💬 Talk to Your Healthcare Team
If you’re concerned about your levels or not feeling better, don’t stop your medication — contact your team. There may be a simple fix like adjusting your dose, changing the form of medicine, or switching how and when you take it.
📘 For more information
Visit: www.aspergillosis.org
Or speak to your GP, pharmacist, or specialist team.
Article 4: Why This New Information on Biofilms Can Be Reassuring — Not Frightening
💬 A Message to Patients: Why This New Information Can Be Reassuring — Not Frightening
We understand that learning about things like biofilms, the lung microbiome, or how different bugs work together might feel a little overwhelming or even alarming. These topics are complex and unfamiliar to many.
But we want you to know: this science is already improving care for people with aspergillosis — and you don’t need to understand every detail for it to help you.
✅ Examples of How Biofilm Awareness Is Already Helping Patients
🧪 1. Combined Treatment for Coinfection
People who have both Aspergillus and Pseudomonas infections are now more likely to be:
-
Tested for both microbes
-
Given combination therapy (e.g. antifungals + inhaled antibiotics)
This reduces the risk of persistent symptoms and lowers the chance of hospital admission.
🌬 2. Inhaled Therapies That Reach Biofilms
Doctors are now using or trialling inhaled medications that can:
-
Reach fungal and bacterial biofilms more directly
-
Work even when oral drugs can’t penetrate
For example, inhaled colistin or tobramycin is used in bronchiectasis; inhaled antifungals (like opelconazole) are in trials for aspergillosis.
💡 3. Chest Physiotherapy and Mucus Clearance
Biofilm research has shown that many infections hide in thick mucus. So, clearing mucus isn't just for comfort — it’s a critical part of treatment.
-
More patients now receive airway clearance devices
-
Some are referred for specialist physiotherapy to support this
🧼 4. Better Infection Control in Hospital
Because we understand that biofilms form on equipment and even in hospital air systems, specialist centres like NAC use:
-
HEPA-filtered rooms
-
Strict protocols to prevent airborne contamination
This lowers the risk of acquiring new fungal infections during hospital stays.
📊 5. More Personalised Care
Some patients now receive tailored treatment plans based on:
-
Sputum cultures that show which organisms are present
-
Whether biofilm-forming species are involved
-
Coexisting inflammation, allergies, or colonisation patterns
This is a big shift from one-size-fits-all prescriptions.
💬 Final Reassurance
These discoveries don’t mean there’s something worse going on. They mean that:
Doctors now understand more
Treatments are becoming more precise
We can often treat fewer times, more effectively
You're not alone — and you're not expected to keep up with every detail. This information helps your care team make better choices for you, reduce flare-ups, and improve quality of life. And that’s what really matters.
📝 Article 3: When Microbes Work Together – Aspergillus, Pseudomonas, and Lung Inflammation
🤝 Not all microbes are rivals — some collaborate
Recent research shows that Aspergillus fumigatus and Pseudomonas aeruginosa can cooperate, particularly in people with weakened lungs or structural damage (e.g. from bronchiectasis, CF, or CPA).
Examples of how they interact:
-
Pseudomonas produces toxins (phenazines) that sometimes stimulate Aspergillus growth in low doses
-
Aspergillus produces substances like gliotoxin that weaken immune responses and protect both microbes
-
Both can form mixed biofilms, making them more drug-resistant and more inflammatory
⚠️ Clinical implications:
Coinfection with Aspergillus and Pseudomonas is associated with:
-
Worse lung function in CF, bronchiectasis, CPA
-
More frequent exacerbations and hospital admissions
-
Longer recovery times and lower quality of life
🧠 Why is this important for treatment?
Doctors are now:
-
Testing for multiple microbes during exacerbations
-
Using combination therapy — antifungals and antibiotics together
-
Supporting the immune system with:
-
Airway clearance
-
Nutrition
-
Steroid balancing (not too much, not too little)
-
🧬 New tools on the horizon:
-
Drugs that block microbial signalling (quorum sensing)
-
Microbiome profiling to predict flare-ups
-
Biofilm-dissolving agents in development
-
Inhaled antifungals under trial (e.g. opelconazole)
🌟 Final Summary: A Shift in Perspective
| Old Approach | New, Holistic Approach |
|---|---|
| Target a single infection | Understand the whole lung ecosystem |
| Treat only during active infection | Focus on prevention, balance, resilience |
| One-size-fits-all antibiotic use | Tailored therapy, minimise microbiome damage |
| Ignore biofilms | Disrupt biofilms and support mucus clearance |
| Fungal and bacterial issues separate | Recognise synergy and co-infection |
📝 Article 2: The Lung Microbiome – More Than Just Aspergillus
🌱 What is the lung microbiome?
The lung microbiome is the collection of bacteria, fungi, and viruses that naturally live in your respiratory system. For a long time, lungs were thought to be sterile — we now know that they host complex microbial communities, even in healthy people.
In people with chronic lung conditions like CPA, ABPA, asthma, bronchiectasis, and cystic fibrosis, the lung microbiome can become unbalanced. Certain harmful microbes may overgrow, while beneficial ones disappear.
🤝 Why is this important?
The balance of microbes in your lungs affects:
-
How your immune system responds
-
Whether inflammation is triggered or controlled
-
How easily infections take hold
In aspergillosis patients:
-
Disruption of the microbiome may encourage fungal growth
-
Frequent antibiotics (for chest infections) can kill good bacteria, giving fungi and drug-resistant bacteria an advantage
-
Some microbes may protect against Aspergillus or help modulate inflammation
This is particularly important during flare-ups and exacerbations.
🧪 What are researchers doing?
Lung microbiome research is growing rapidly. Scientists are:
-
Identifying "protective" microbes that might reduce disease severity
-
Studying how antibiotics, steroids, and antifungals alter the microbiome
-
Investigating faecal or airway microbiota transplants in severe lung disease
-
Developing tests that detect imbalances in lung flora before symptoms worsen
💡 What can you do as a patient?
-
Avoid unnecessary or repeated broad-spectrum antibiotics unless clearly needed
-
Use airway clearance techniques to keep mucus and debris low
-
Ask your clinician if your sputum cultures test for both bacteria and fungi
-
Consider probiotics cautiously, though evidence for lung benefit is still limited
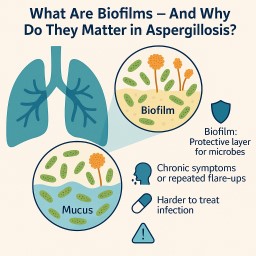
📝 Article 1: What Are Biofilms – And Why Do They Matter in Aspergillosis?
🧫 What is a biofilm?
A biofilm is a protective layer that microorganisms (like fungi and bacteria) create when they stick to a surface — such as the inside of airways, lung cavities, or medical devices. They secrete a sticky matrix of sugars, proteins, and DNA that holds them together and shields them from harm.
In aspergillosis, Aspergillus fumigatus forms biofilms on:
-
Mucus in the lungs
-
Cavities or damaged tissue (e.g. in CPA)
-
Surfaces of bronchial airways, especially in people with asthma or bronchiectasis
Pseudomonas aeruginosa, a bacterium often found alongside Aspergillus, also forms biofilms — and they can even form mixed (dual-species) biofilms together.
❗Why does this matter?
Biofilms protect the microbes inside by:
-
Blocking immune cells from reaching them
-
Preventing antibiotics or antifungals from penetrating the biofilm
-
Allowing microbes to go dormant, then reactivate later
This is one reason why infections in aspergillosis patients can become chronic, relapse frequently, or be very hard to fully clear.
People with CPA, ABPA, SAFS, or fungal bronchitis may experience:
-
Repeated flare-ups or infections despite treatment
-
Persistent coughing, breathlessness, or mucus production
-
Ongoing inflammation in the lungs, even when cultures are negative
🛠 How are biofilms treated?
Current options include:
1. Antifungals and antibiotics
-
Standard antifungals (like voriconazole, posaconazole, isavuconazole) can sometimes penetrate biofilms, but often require longer or higher doses.
-
Inhaled antibiotics (e.g. nebulised colistin or tobramycin) are used in bronchiectasis and can help break into bacterial biofilms.
-
Combined therapy (targeting both bacteria and fungi) may be used in patients with co-infection.
2. Disrupting the biofilm
-
DNase (Pulmozyme) in cystic fibrosis breaks up sticky DNA in mucus where biofilms form.
-
Future treatments aim to use enzymes, surfactants, or nanoparticles to dismantle biofilms.
3. Clearing mucus and infected secretions
-
Chest physiotherapy, postural drainage, and devices like the Acapella® or Flutter® help remove secretions where biofilms sit.
-
Bronchoscopy is occasionally used to clear dense mucus plugs.
🔬 Looking ahead:
Researchers are studying:
-
Drugs that target the biofilm matrix directly
-
Ways to prevent biofilms from forming in the first place
-
New diagnostic tools that detect biofilm presence
📁 Coping with Steroid Side Effects and Finding Balance: A Guide for Aspergillosis Patients
Living with chronic forms of aspergillosis—such as chronic pulmonary aspergillosis (CPA), allergic bronchopulmonary aspergillosis (ABPA), severe asthma with fungal sensitisation (SAFS), or Aspergillus bronchitis—often means taking corticosteroids like prednisolone or hydrocortisone. These powerful medicines can be life-saving, but they also come with physical and emotional side effects, especially at high doses or when taken over long periods.
This guide is here to support you with practical tips, patient stories, and advice on reducing steroids while maintaining your quality of life.
🔊 What Do Steroids Do?
Steroids reduce inflammation and calm overactive immune responses. They're commonly used in aspergillosis to:
- Manage allergic reactions (e.g. in ABPA)
- Control lung inflammation
- Treat adrenal insufficiency or steroid withdrawal symptoms
🔁 Why Reducing Steroids Can Be So Difficult
Steroids are very effective but also powerful. Tapering the dose can cause:
- Return of pain, fatigue, breathing problems, or inflammation
- Steroid withdrawal symptoms (fatigue, low mood, joint pain)
- Adrenal suppression if the body has stopped making its own cortisol
Many patients report:
“I reduced by 1mg and everything fell apart.” “I want to be on less, but life is unbearable when I try.”
You are not failing. Finding the right dose is a balance between lowering risks and keeping your life manageable.
🛋 Common Side Effects and What You Can Do
| Side Effect | Tips to Cope |
|---|---|
| Increased appetite | Plan balanced meals, high-fibre snacks, drink water, be kind to yourself |
| Weight gain / swelling | Gentle movement, reduce salt, try pressotherapy (discuss with your team) |
| Mood swings or anxiety | Talk about it, track your feelings, ask about counselling or peer support |
| Insomnia | Avoid caffeine late, consider timing of dose, try a calming bedtime routine |
| "Moon face" / puffiness | Often fades when dose is reduced; hydrate and moisturise |
| Muscle/joint pain or weakness | Gentle stretches, walking, low-impact activity, speak to a physio if needed |
| Bruising/thin skin | Moisturise, protect from bumps, avoid strong detergents |
| Raised blood sugar | Eat regularly, reduce sugary drinks, ask about monitoring if concerned |
| Bone thinning | Ask about calcium, vitamin D, or bone-protecting medications |
| Adrenal suppression | Never stop suddenly; always taper with a doctor's guidance |
👥 Real Patient Stories and Analogies
🐻 Alison's Bears
“There are two bears inside me. Prednisone Bear is wild and wants to eat and sleep and snap. But Rusty McTravel Bear is my real self—gentle, curious, slowly trying to get back on the road. I’ve learned to recognise the first and nurture the second.”
🏎️ The Revving Car
“Being on steroids sometimes feels like a car with the engine revving but the brakes on. You’re buzzing, but you’re stuck. Try easing the brakes: take a walk, make tea, do something simple to use the energy.”
🚩 Finding Your Balance: When Less Isn't Always Better
✅ Go slow
- Taper in small steps—as little as 0.5–1mg at a time
- Wait several weeks between reductions
✅ Keep a steroid diary
- Note dose, mood, sleep, symptoms, activity
- This helps identify your "minimum effective dose"
✅ Accept that a small maintenance dose may be necessary
- You are not failing if you need 2mg, 5mg, or 7.5mg long-term
- The goal is a life worth living, not perfection
✅ Ask about alternatives
- Inhaled steroids, antifungals, or biologics might help reduce systemic steroid use
✅ Consider adrenal testing
- Especially if you feel unwell during tapering or on low doses
🛏️ Other Strategies That May Help
- Pressotherapy for leg pain and swelling
- Mindfulness or breathing exercises for anxiety or insomnia
- Peer support (online or in person)
- Short-term plans: some patients use a "rescue dose" plan for flare-ups
- Talk to your care team: never reduce on your own without guidance
💼 Summary
Reducing or living with steroids is not just about doses. It’s about protecting your body and your sense of self. If a small daily dose keeps you functioning, that is not weakness—it’s balance.
You are not alone. Many in the aspergillosis community are navigating this same path.
“The right dose is the one where I can breathe, move, smile — and still feel like myself.”