🧾 Rezafungin: A New Antifungal Being Trialled for CPA
Some people with chronic pulmonary aspergillosis (CPA) have trouble tolerating standard antifungal medications. Commonly used drugs like voriconazole and posaconazole can cause serious side effects such as hallucinations, liver enzyme disturbances, or gut problems. When these medications can’t be used, options become limited.
A new antifungal, rezafungin, is now being studied as a possible treatment for CPA — especially in people who can't tolerate azoles. It is not yet approved for aspergillosis, but a major clinical trial is under way.
🧬 What Is Rezafungin?
Rezafungin is part of a newer group of antifungal drugs called echinocandins. These work by weakening the fungal cell wall — a very different mechanism to azole drugs like itraconazole or voriconazole.
Key features:
-
Given as a weekly intravenous (IV) drip
-
Long-acting: stays in the body for days after each dose
-
Designed to provide high drug levels in the lungs and bloodstream
-
Early studies show less frequent side effects than with some older antifungals
It is already licensed for treatment of Candida bloodstream infections but is being studied now for CPA.
🧪 Current Research: Trial for CPA
A clinical trial is currently recruiting people with CPA who:
-
Cannot take azole antifungals because of side effects or resistance
-
Need alternative or combination therapy
This trial (called REZAFUNGin Efficacy and Safety for Aspergillus – CPA) is being conducted in the UK and internationally. The goal is to test whether rezafungin is safe and effective in CPA patients who have few remaining options.
🔗 View the clinical trial (NCT06794554)
📊 What Have Previous Studies Found?
While studies in CPA are just beginning, previous trials in other fungal infections provide important clues:
✅ Phase 2 & 3 Studies (Candida Infections)
-
Rezafungin was found to be as effective as daily echinocandins (like caspofungin)
-
Once-weekly dosing worked just as well as daily treatment
-
Side effects were mild, and liver toxicity was rare
-
No CNS side effects (like hallucinations) were reported
🧫 Laboratory Evidence
-
Rezafungin is active against Aspergillus fumigatus, including some azole-resistant strains
-
It reaches good levels in lung tissue — an important feature for CPA
-
May be used alone or with another antifungal in complex cases
🩺 Case Example
A recent case report described successful treatment of chronic pulmonary aspergillosis using rezafungin plus voriconazole in a patient with resistant infection (Oxford University Press, 2024).
⚠️ Is Rezafungin Available Now?
Not yet. Rezafungin is only available for CPA:
-
Through a clinical trial, or
-
By special approval for compassionate use in selected cases
It is not currently licensed for aspergillosis in the UK or elsewhere.
💬 What Should I Discuss with My Doctor?
If you're considering participation in a clinical trial or if standard treatments have failed, you might ask:
-
Am I eligible for the rezafungin CPA trial?
-
What are the benefits and risks of trying this treatment?
-
Will I still need other antifungals (e.g. azoles or amphotericin)?
-
How often will I need blood tests and hospital visits?
-
Will this help if I have azole resistance or liver side effects?
📌 Summary
Rezafungin is a new antifungal drug being tested for people with chronic pulmonary aspergillosis who cannot take older treatments. It offers once-weekly dosing and early signs suggest a favourable safety profile, including in patients with liver concerns or those who had side effects from azoles.
Although not yet widely available, it may offer hope for people with limited options. If you or someone you know is struggling with antifungal intolerance, you may wish to speak to your medical team about the CPA clinical trial or explore compassionate access routes.
👉 Learn more or check trial sites:
🔗 https://clinicaltrials.gov/study/NCT06794554
Cyber Safety for Aspergillosis Patients: Supplement to UK NCSC Advice
This guide builds on the official UK Government cybersecurity advice for families and individuals (www.ncsc.gov.uk/section/advice-guidance/you-your-family) and adds patient-specific tips for people with aspergillosis.
Feeling overwhelmed?
You're not alone. The internet and phone landscape can feel like a minefield, especially when you're trying to manage your health too. No one expects you to become an expert in cybersecurity overnight. The aim of this guide isn’t to scare you — it’s to help you take small, realistic steps to protect yourself.
Just like with your health, doing the basics well goes a long way. You don’t need to memorise everything — focus on:
- Using strong passwords (or a password manager)
- Being cautious with texts, links, and phone calls
- Asking for help when something doesn’t feel right
- Always accept updates on your phone, browser, or computer when offered — these often fix known security problems and help keep you protected.
It's okay to stop and ask: “Does this sound right?” If in doubt, check with someone you trust.
Top Scam Red Flags
Watch out for these common signs that something could be a scam:
- You’re told to act urgently or keep it secret
- You’re offered money, discounts, prizes or help out of the blue
- You’re asked to click a link or open an attachment in a message
- A caller claims to be from the bank, NHS, government, or police, but something feels off
- You’re told the second part of a message will come from a different number or address
- You’re asked to confirm personal, financial or password information
- You’re asked to download software or apps to “fix” your device
- You’re pressured to stay on the phone or not call anyone else
If in doubt, hang up, delete, or double check with someone you trust.
1. Protecting Your NHS and Medical Accounts
- Use strong, unique passwords for your NHS login, GP apps (e.g. Patient Access, myGP), or hospital portals.
- Enable two-factor authentication (2FA) wherever it’s offered.
- Never share your NHS login or codes with anyone.
- Always go directly to the official app or website, not through links in emails or texts.
2. Beware of Scams
- Scams can take many forms — phone calls, emails, texts, or fake websites.
- Be especially wary of anyone offering money, discounts, prizes, or urgent deals.
- Criminals may pose as trusted organisations like your bank, utility provider, government, or even the NHS.
- As a general principle: if something seems too good to be true — such as offers of free money, major discounts, prizes, or miracle cures — it almost certainly isn't real. Be suspicious of anything that promises unusually high benefits for little or no effort.
- If in doubt, forward suspicious messages to [email protected] (Link) or speak to someone you trust before taking action.
3. Using Online Support Groups Safely
- Facebook groups and forums can be great for connection, but don’t post:
- Your address, phone number, or full date of birth
- Photos of prescriptions or test results
- Don’t click links shared by strangers, even if they seem friendly.
- Moderators or admins should never ask for sensitive personal details.
4. Shopping and Donations
- Be cautious when buying medical supplies or donating online.
- Stick to trusted UK pharmacies and charities.
- Watch for copycat sites that look like legitimate health organisations.
5. Email, Phone & Text Safety
- Don’t click on links or open attachments in messages claiming to be from the NHS, unless you were expecting them.
- Never share passwords or bank details over email or text.
- Never give out your account numbers or passwords, especially if someone is trying to rush or pressure you.
- Scam texts can fake NHS or GOV.UK addresses — check official sites if unsure.
- Even texts or emails that appear to come from your bank can be faked. A common red flag is a message saying that a second text or email will come from a different number or sender — ask yourself why a genuine organisation would do this. Real authorities go to great lengths to be verifiable.
- If someone calls and tries to rush or scare you, hang up and call back using an official number from the NHS or your GP’s website.
- If in doubt — or even as a general principle — hang up and call a number you can verify yourself, such as:
- The number printed on the back of your bank card
- The official website of a company or authority (searched independently)
- Avoid using any contact information provided by the caller or in a suspicious message — treat it as untrustworthy until confirmed.
- To check a suspicious link in a text, don’t click — instead, search for the organisation’s website directly or ask someone you trust.
6. If You're Shielding or Vulnerable
- You may be more targeted by scams pretending to offer:
- COVID-19 test kits, antifungal treatments, or priority delivery slots
- Access to urgent medical appointments or services
- Verify any offer with your NHS care team before taking action.
7. Keeping Your Devices Safe
- Install antivirus and keep your phone/tablet/computer updated.
- Always accept software updates — they patch security flaws that criminals may try to exploit.
- Set devices to auto-lock and use a passcode or fingerprint.
- Avoid using public Wi-Fi for medical logins or financial information.
Do You Still Need Antivirus?
- Windows PCs: Yes — always install antivirus. Microsoft Defender (built-in) is good and free. You can also consider free versions of AVG, Avast, or Bitdefender.
- Mac computers: Less targeted, but still recommended. Free options include Avira or Sophos Home.
- Android phones: A good idea, especially if you install apps outside the Play Store. Try Bitdefender or AVG.
- iPhones/iPads: Antivirus apps aren’t usually needed if you keep iOS updated and install apps only from the App Store.
Whichever device you use, updates and cautious browsing are just as important as antivirus software.
8. Best Ways to Use Strong Passwords
Cyber security can be time-consuming and even irritating — but as malicious activity becomes more sophisticated, it’s worth the effort. Consider using different levels of passwords for different kinds of accounts:
- Low-level passwords for things like newsletters or forums
- High-level, strong passwords for NHS, banking, or health-related logins
Make Passwords Long and Unique
- Use at least 12 characters, mixing letters, numbers, and symbols
- Avoid personal info like names or birthdates
Use a Password Manager
- Tools like Bitwarden, 1Password, or Apple Keychain securely store passwords
- You only need to remember one master password
Use Passphrases for Important Accounts
- Combine random words to create a memorable but strong password, like:
Correct!Horse-Battery!Staple99
Turn On Two-Factor Authentication (2FA)
- Adds a second layer of protection, such as a code from your phone
- 2FA ties your account to a specific device (like your phone), meaning a criminal would need access to that device as well as your password to break in
Use a Unique Password for Every Account
- Never reuse passwords
Avoid These Mistakes
| Mistake | Better Option |
|---|---|
| Reusing passwords | Use a password manager |
| Writing them down | Use encrypted storage |
| Adding "123" to a word | Use unrelated, random words/symbols |
When to Change Passwords
- If your account may have been hacked
- If the same password is used elsewhere
Is It Safe to Use Chrome or Other Browser Autofill?
Using Chrome, Firefox, Safari, or Edge to autofill logins can be safe with the right precautions:
- Your device should be private and locked with a passcode or fingerprint
- Your browser and operating system should be kept fully up to date
- You should avoid storing logins for sensitive accounts (e.g. banking, NHS login)
Risks to consider:
- Passwords stored in browsers can be accessed by malware or rogue extensions
- If someone gets access to your device, they may access saved logins
Safer Alternative:
- Use a dedicated password manager (like Bitwarden, 1Password, or Dashlane)
- These offer stronger security and are harder for malware or hackers to access
If you do use browser autofill, protect your device and account with:
- Two-factor authentication for your Google, Apple, or Microsoft account
- A strong device password or biometric lock
9. Finding the Happy Medium
Cybersecurity doesn’t have to take over your life — the key is to find a realistic balance between staying safe and staying sane:
- Focus on protecting your most important accounts first — especially NHS, email, banking, and anything medical
- Don’t ignore warning signs, but don’t feel you have to be perfect with every app or device
- Use automation where possible (e.g. password managers, browser autofill, device lock)
- Ask for help if you’re unsure — carers, family members, or digital support charities can assist
Think of it like seatbelts — you hope you never need them, but they’re worth the hassle when something goes wrong.
Useful Links
- UK NCSC advice for individuals & families - constantly updated and UK government verified: https://www.ncsc.gov.uk/section/advice-guidance/you-your-family
- Report phishing emails: [email protected]
Remember: Your health is private and valuable. Treat your medical and personal information like you would your bank details. Stay cautious, ask questions, and when in doubt, ask a trusted health professional or carer.
💊 Staying Safe on Long-Term Treatment for Aspergillosis
(Steroids and Azole Antifungal Medicines)
If you're living with aspergillosis, your treatment plan may include long-term antifungals (e.g. itraconazole, voriconazole, posaconazole, or isavuconazole) and sometimes oral steroids like prednisolone. These medicines can be essential in managing your symptoms and preventing long-term lung damage.
But like all strong medicines, they need to be monitored closely—and you should be part of every treatment decision.
🗣️ You Should Be Involved in Every Medication Decision
NHS and NICE guidance recommend that:
-
Medicines should be reviewed regularly
-
Reviews should include the patient’s voice
-
Decisions to continue, stop, or adjust a medicine should be made together
🔗 NICE Medicines Optimisation Guidance:
https://www.nice.org.uk/guidance/ng5
⚠️ Why Regular Reviews Matter – Especially with Steroids and Azoles
Azole antifungals and steroids are powerful tools for treating aspergillosis, but they can cause side effects—especially if taken for long periods. Regular reviews help ensure you're getting the benefit of treatment without unnecessary risk.
🧪 Azole Antifungals Used in Aspergillosis
| Drug | Brand name(s) | Notes |
|---|---|---|
| Itraconazole | Sporanox | Common first-line; blood level monitoring needed |
| Voriconazole | Vfend | May affect vision, liver; used in severe cases |
| Posaconazole | Noxafil | Often well tolerated; used if others don’t suit |
| Isavuconazole | Cresemba | Newer; fewer interactions and side effects |
These antifungals can interact with many other medicines. The British National Formulary (BNF) lists over 300 interactions for itraconazole alone.
🧠 What About Prednisolone?
Prednisolone is a steroid that helps reduce inflammation but may cause side effects like:
-
Weight gain, diabetes, mood swings
-
Eye problems (e.g. cataracts)
-
Bone thinning (osteoporosis)
-
Adrenal insufficiency—where the body stops making enough natural steroid hormone
This is why lowest dose for the shortest time is best, and stopping should always be gradual and supervised.
🔁 What If You Can’t Stop These Medications?
In ABPA or chronic pulmonary aspergillosis, long-term antifungals or steroids may be the only effective treatment for now. That’s okay—what matters is staying safe and supported.
Here’s how your team should help:
-
✅ Use the lowest effective dose
-
✅ Monitor side effects and blood levels (especially for itraconazole and voriconazole)
-
✅ Watch for liver, nerve, adrenal, or eye problems
-
✅ Consider switching antifungals if side effects develop
-
✅ Look into steroid-sparing options (e.g. biologics like omalizumab or benralizumab for ABPA—though not yet widely approved)
👥 What If You’re Experiencing a Side Effect?
Here’s an example of a positive, patient-led conversation:
Patient:
"Since starting itraconazole, I’ve had tingling in my feet and some burning pain at night. I’m worried it’s the medicine."
Doctor:
"Thank you for bringing this up. That’s important. Let’s review your timing and symptoms. Itraconazole can sometimes cause nerve issues—let’s check your drug level and liver tests, and talk about adjusting the dose or switching antifungals."
Patient:
"Is it dangerous to stop suddenly?"
Doctor:
"No, not if done with supervision from your doctor—we’ll make any changes carefully and monitor you throughout. I’ll schedule follow-up, and please get in touch if anything worsens."
✅ You deserve to be listened to. Never ignore a side effect or worry that you’re being a nuisance—your body knows when something isn’t right.
🔎 Who Should You Talk To?
Here’s who to contact depending on the concern:
| Type of Concern | Best First Contact | Why |
|---|---|---|
| Side effects (e.g. nausea, mood, tingling) | GP or clinical pharmacist | Pharmacists are medication experts and often easier to access than specialists |
| Drug interactions | Pharmacist | They can check for dangerous combinations |
| Monitoring (e.g. blood tests, drug levels) | Specialist team | Usually manages antifungals and steroid tapering |
| Suspected allergy or adrenal issues | GP or endocrinologist referral | For detailed hormone testing or allergy support |
| General concerns or you're unsure who to ask | GP | They can coordinate referrals and advice |
🧩 What If You React Differently Than Expected?
Rare side effects do happen—including steroid allergy or intolerance, or nerve pain from azoles. You might feel dismissed, especially if the reaction is unusual or not in the textbook.
You are entitled to:
-
A proper medication review
-
A second opinion
-
Referral to pharmacy, allergy, or endocrine clinics
-
Kind, respectful care from professionals who take you seriously
True reactions are rare—but not imaginary. Speak up, document what you notice, and ask for help.
📚 Stay Informed with Reliable Sources
-
BNF (British National Formulary): https://bnf.nice.org.uk
-
NICE Guidance: https://www.nice.org.uk
-
Cochrane Reviews (independent evidence summaries):
https://www.cochrane.org/evidence/
🤝 Final Word
If you're on long-term treatment for aspergillosis, you're not failing—you're managing a difficult condition with strength and persistence. What matters is that you’re:
-
Heard
-
Supported
-
Included in every decision
You are the expert in how your body feels—and when your voice is part of the team, the care is always better.
🫁 Mucus Plugging in Aspergillosis: What It Is, Why It Happens, and What It Means
For patients with ABPA, CPA, Aspergillus bronchitis, or asthma
🔍 What Is a Mucus Plug?
A mucus plug is a thick clump of sticky mucus that becomes trapped in your lungs. It can block airways, cause coughing, and make breathing more difficult. In people with aspergillosis, this is common — but the type, location, and cause of the mucus can vary.
🧪 What Causes Mucus Plugging?
Your lungs naturally make mucus to protect against germs and irritants. But in fungal or allergic lung disease, this mucus may:
-
Be produced in excess
-
Become too thick or sticky
-
Get trapped due to airway damage
Aspergillosis-related causes include:
-
ABPA (Allergic Bronchopulmonary Aspergillosis) – inflammation causes thick, sticky mucus
-
Aspergillus bronchitis – fungus lives in mucus, producing biofilms
-
CPA (Chronic Pulmonary Aspergillosis) – may lead to mucus due to structural damage
-
Bronchiectasis – airways are widened and can no longer clear mucus properly
🧬 Are All Mucus Plugs the Same?
No. Mucus plugs vary in colour, texture, cause, and treatment. Here's how they differ:
| Type of Plug | What You Might See | What It Could Mean | Common in... |
|---|---|---|---|
| Sticky, stringy | Clear/yellow, like glue | Allergic inflammation | ABPA, asthma |
| Rubbery or solid | Brown, rubbery, “slug-like” | Allergic + fungal mix | ABPA, Aspergillus bronchitis |
| Green or smelly | Thick, foul-smelling | Infection (bacteria) | Bronchiectasis |
| Foamy or frothy | Clear/white, bubbly | Non-infectious irritation | COPD, asthma |
| Black or speckled | May contain fungal specks | Fungal growth | CPA, fungal bronchitis |
🖼️ What Do Mucus Plugs Look Like on a CT Scan?
Below are real examples of CT scan findings showing mucus plugging in different forms of aspergillosis and related conditions.
🧷 1. Finger-in-glove sign (ABPA)
Mucus in large airways appears like fingers inside a glove. This is common in allergic fungal airway disease.
➡ Seen in: ABPA, bronchiectasis with fungal colonisation
📍 Note: Branching tubular opacities filled with mucus.
🌿 2. Tree-in-bud pattern
Small airway blockage — plugs in the tiniest branches of the lungs. Common in infection, inflammation, and Aspergillus bronchitis.
➡ Seen in: Aspergillus bronchitis, asthma, CPA with superinfection
📍 Note: Tiny dots and lines in a tree-like shape.
🧱 3. Lung collapse (atelectasis) from plug
A large mucus plug can block a main airway, causing collapse of part of the lung.
➡ Seen in: Severe ABPA, CPA, patients with weakened cough reflex
📍 Note: Whiteout of part of lung where plug is blocking airflow.
📸 Example CT Findings

1. Bronchiectasis + mucus plug
Area in the left lower lung shows dilated bronchi filled with mucus—classic for bronchiectasis with mucoid impaction

2. Extensive bronchiectasis with plugs
Widespread thick-walled airway dilatation accompanied by mucus plugs (black arrows) and consolidation (black arrowheads)

3. Luminal plugging in small airways
Subtle luminal opacities in peripheral bronchi—the “tree‑in‑bud” pattern common in asthma, COPD, and infections.

4. Atelectasis (part of the lung has collapsed or isn’t fully inflating) due to mucus plugging
Consolidation and small airway blockage leading to lung collapse, highlighted by arrows in the upper lobe.
💡 Clinical Takeaways
| Feature | What it indicates |
|---|---|
| Mucoid impaction | Large airway fungal/allergic plugs (e.g., ABPA) or bronchiectasis |
| Tree‑in‑bud | Small-airway infection/inflammation (e.g., TB, PCD, asthma) |
| Atelectasis | Complete blockage, leading to collapse and consolidation |
| Persistent luminal plugs | Associated with worse airflow obstruction and symptoms in COPD/asthma |
✅ Next Steps / Applications
-
These CT examples are valuable for educational use—they illustrate the different patterns seen in mucus plugging across disease types.
-
Radiologists often use these signs to help diagnose and tailor management (infection, allergy, structural lung disease).
-
If your patients or students need simplified visuals, these scans paired with annotations (e.g., arrows, labels) can make great teaching tools.
🧠 What Does It Feel Like?
People often say:
“It felt like something was stuck and wouldn’t come out.”
“I finally coughed up a rubbery strand — like glue.”
“Once it cleared, I could breathe better instantly.”
🧼 How Are Mucus Plugs Treated?
Treatment depends on the underlying cause:
✅ Medications
-
Steroids – reduce inflammation in ABPA and asthma
-
Antifungals – lower fungal load (e.g., itraconazole, posaconazole)
-
Mucolytics – thin mucus (e.g., carbocisteine, hypertonic saline)
-
Antibiotics – treat bacterial infections
✅ Airway Clearance Techniques
-
Respiratory physio – helps you learn how to shift mucus
-
Devices – flutter valve, PEP mask, Acapella
-
Inhaled/nebulised therapy – opens airways and loosens plugs
⚠️ Always speak to your clinical team before starting a new technique.
🧪 Can Coughing Up a Plug Help Diagnosis?
Yes! If you cough up a rubbery, large, or unusual plug, it can be:
-
Tested for fungus, bacteria, or allergy cells (eosinophils)
-
Sent for culture to detect Aspergillus
-
Helpful in guiding or confirming diagnosis of ABPA or Aspergillus bronchitis
👣 Key Points for Aspergillosis Patients
| Question | Answer |
|---|---|
| Is mucus plugging common? | Yes, especially in ABPA, CPA, and bronchiectasis |
| Are all mucus plugs the same? | No – they vary in size, shape, colour, and cause |
| What should I do if I cough one up? | Tell your doctor – it may be useful to test |
| Can it be seen on scans? | Yes – CT can show where plugs are and how severe |
| Can it be treated? | Yes – treatments include steroids, antifungals, mucolytics, and physio |
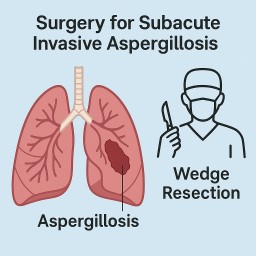
When Antifungals Fail: One Patient’s Recovery from Subacute Invasive Aspergillosis After Surgery
Subacute Invasive Aspergillosis (SAIA) is a rare and serious lung infection caused by the Aspergillus fungus. It often affects people who are immunocompromised—whether due to illness or medications like immunosuppressants—and typically sits between chronic and acute invasive forms in severity.
🧬 A Patient's Story from Australia
“I was diagnosed with SAIA after being treated with immunosuppressants for an autoimmune condition. Over seven months, I tried three different antifungal medications—but the infection persisted. I was still producing thick mucus and felt systemically unwell, almost like I had a constant infection running through me.
Four weeks ago, I underwent a wedge resection—a type of surgery where the affected part of my lung was removed. Since then, my symptoms have completely resolved. I’m no longer coughing or feeling septic.
My infectious diseases specialist plans to keep me on posaconazole for 12 months, with monthly galactomannan blood tests to catch any recurrence early.
I’ve found there’s very little published about surgery for SAIA, so I hope my experience might help others.”
🧪 What Is SAIA?
SAIA is a slowly progressive lung infection that develops over weeks to months. Unlike acute invasive aspergillosis, which moves quickly, SAIA often occurs in people with some degree of immune suppression but who aren’t completely immunocompromised.
It can present with:
-
Persistent cough
-
Low-grade fever
-
Fatigue
-
Mucus production
-
Progressive lung damage
Standard treatment involves long-term antifungal therapy, often with drugs like:
-
Itraconazole
-
Voriconazole
-
Posaconazole
But in some cases—like this patient’s—antifungal therapy alone isn’t enough.
🛠️ When Is Surgery Used for SAIA?
Surgery, including wedge resection, may be considered when:
-
Antifungal medications are not effective
-
The infection is localized to one part of the lung
-
There is persistent or worsening lung damage
-
Patients are fit enough to undergo surgery
🔍 What Does the Evidence Say?
Although not commonly performed, surgery for aspergillosis is documented in medical literature, especially in cases of:
-
Chronic pulmonary aspergillosis (CPA)
-
Fungal nodules
-
Subacute forms like SAIA
Key studies:
-
A U.S. study of >100,000 aspergillosis cases found that only 4.8% underwent surgery, usually for treatment failure or severe complications.
-
A Chinese study of 85 CPA patients showed a relapse rate of only 7% post-surgery, with most patients improving dramatically.
-
A UK case series described 30 patients having lung resections over 15 years, showing surgery is safe and effective when performed in experienced centres.
🔄 What Happens After Surgery?
Even after a successful resection, follow-up antifungal treatment is often continued to prevent recurrence. Monitoring usually includes:
-
Regular imaging (CT scans)
-
Galactomannan blood tests (to detect fungal components)
-
Symptom tracking
This is typically guided by a multidisciplinary team involving infectious diseases, respiratory, and thoracic surgery specialists.
🎯 Key Takeaways
-
SAIA is uncommon, and when antifungals fail, surgery can be life-changing.
-
Wedge resection is a lung-sparing procedure that removes just the infected portion, offering good outcomes when the disease is localised.
-
Ongoing antifungal therapy and monitoring are critical to long-term success.
-
Your story adds to a growing but still limited body of knowledge and may help inform future treatment decisions and encourage further research.
If you are a patient or clinician navigating SAIA and struggling with antifungal treatment, this story may offer hope—and a reminder that surgical options, though rarely needed, can be effective when used judiciously.
🛡️ Understanding Your Risk: Aspergillosis, Steroids, and the Immune System
If you’ve been diagnosed with an Aspergillus-related condition, such as chronic pulmonary aspergillosis (CPA), ABPA, or a fungal ball (aspergilloma), you might wonder:
“Am I immunocompromised? And do steroids or biologics put me at more risk?”
The answers depend on your underlying health, medications, and how your body responds to Aspergillus.
🌍 Aspergillus is Common — But Not Harmless
Aspergillus is a type of mould found everywhere — in soil, air, and dust. Most people breathe it in daily without problems. But in some people, it can:
-
Trigger an allergic reaction (ABPA or fungal sinusitis)
-
Cause infection in damaged lungs (CPA or aspergilloma)
-
Spread aggressively in those with very weak immune systems (invasive aspergillosis)
Understanding your level of immune defence helps explain your risk and how your treatment should be managed.
🧬 Levels of Immunocompromise: What They Mean
Immunosuppression isn't black-and-white — it's a spectrum. Here's how it applies to people with or at risk of aspergillosis:
🔴 High-Level Immunosuppression (High Risk)
-
Recent chemotherapy or bone marrow transplant
-
Stem cell or organ transplant
-
Severe neutropenia (very low white blood cell count)
-
High-dose steroids (e.g. ≥20 mg prednisolone daily for weeks)
-
Uncontrolled HIV/AIDS
-
Intensive care or mechanical ventilation
🧠 These people are at risk of serious, fast-spreading infections — including invasive aspergillosis (IA), which is rare but life-threatening.
🟠 Moderate Immunosuppression (Common in Aspergillosis Patients)
-
Long-term low-to-moderate steroids (e.g. <10–15 mg prednisolone)
-
Biologics for asthma (e.g. omalizumab, benralizumab)
-
Chronic lung disease (COPD, bronchiectasis, asthma)
-
Diabetes, malnutrition, or genetic immune traits
-
Previous TB, sarcoidosis, or other lung damage
🧠 This group is at greater risk of chronic forms of aspergillosis — especially CPA, ABPA, and aspergillus bronchitis.
🟢 Low or No Immunosuppression (Low Risk)
-
People with well-controlled asthma or sinusitis
-
Those on occasional short courses of steroids
-
No major lung or immune conditions
🧠 This group is unlikely to develop aspergillosis.
💊 What if You Already Have Aspergillosis?
If you’ve been diagnosed with CPA, ABPA, aspergilloma, or sinus disease caused by Aspergillus, some treatments may still increase your vulnerability if not carefully managed.
❗ Steroids (e.g. Prednisolone)
-
Help control inflammation (especially in ABPA)
-
But also suppress immunity, making it easier for Aspergillus to grow
-
Can worsen CPA or increase risk of bleeding in aspergilloma
-
Risk rises with higher doses and longer courses
🟠 If steroids are needed, they should usually be combined with antifungal medication (like itraconazole or voriconazole) to keep fungal growth in check.
❗ Biologics for Asthma (e.g. Omalizumab, Mepolizumab)
-
Target allergic inflammation without broadly suppressing the immune system
-
Don’t usually increase the risk of invasive fungal infections
-
May slightly alter how your immune system responds to Aspergillus
🟠 Biologics can be helpful in ABPA and severe asthma, but regular monitoring is still important.
🔍 Summary Table: Common Risk Factors and What They Mean
| Factor | What It Does | What to Watch For |
|---|---|---|
| Long-term steroids | Suppress immune cells, reduce inflammation | Use with antifungals; monitor closely |
| Biologics for asthma | Modulate immune pathways (e.g. IgE, IL-5) | Safe in most; watch for subtle effects |
| TB, sarcoid, or other lung scarring | Leaves cavities that allow fungal growth | Regular scans and blood tests |
| Diabetes or malnutrition | Affects immune function and tissue repair | Keep well-managed |
| Low white blood cells (neutropenia) | Limits ability to fight fungal infection | Urgent action needed if fever or unwell |
| Lung diseases (COPD, asthma, bronchiectasis) | Reduce local lung defences | Increases risk of CPA, ABPA, or colonisation |
✅ What Can You Do to Stay Safe?
-
Take antifungals as prescribed, especially if you're on steroids or biologics
-
Avoid unnecessary long-term steroid use — use the lowest dose for the shortest time
-
Report new or worsening symptoms early — especially breathlessness, coughing blood, fatigue, or sinus pain
-
Have regular follow-ups with your respiratory or infectious diseases team
-
Don’t stop any medication suddenly — especially steroids — without medical advice
💬 Final Reassurance
Having aspergillosis doesn’t mean you’re severely immunocompromised — but some treatments can increase your risk if not managed carefully. With the right balance of antifungals, asthma treatments, and medical support, many people live well with ABPA, CPA, and related conditions.
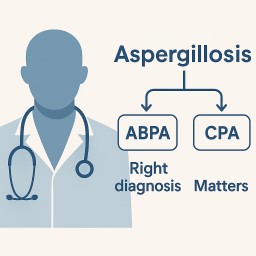
🩺 Why an Accurate Diagnosis Matters in Aspergillosis
If you've been told you have aspergillosis — or one of its forms like ABPA or CPA — you may wonder:
"Why does the exact diagnosis matter?"
Isn’t treatment just treatment?
Actually, no. In aspergillosis, getting the right diagnosis makes a huge difference to your care, safety, and long-term health.
This article explains why an accurate diagnosis is essential – not just for treatment, but also for recovery, monitoring, access to specialist care, and living well with the condition.
🔍 What Are ABPA and CPA?
Both ABPA and CPA are caused by the Aspergillus mould, but they affect the body in very different ways:
| Condition | Description |
|---|---|
| ABPA (Allergic Bronchopulmonary Aspergillosis) | An allergic reaction to Aspergillus in the lungs. Most common in people with asthma or cystic fibrosis. |
| CPA (Chronic Pulmonary Aspergillosis) | A chronic lung infection with Aspergillus. Often seen in people with damaged lungs (e.g. past TB, COPD, bronchiectasis). |
Because the symptoms can overlap (like coughing, mucus, or fatigue), it's not always easy to tell them apart — but the treatments are completely different.
🎯 Why Accurate Diagnosis is So Important
1. ✅ Get the Right Treatment
Different types of aspergillosis need very different medicines.
| Diagnosis | Main Treatment | Notes |
|---|---|---|
| ABPA | Steroids (e.g. prednisolone), sometimes antifungals (like itraconazole) | Helps control inflammation and allergy |
| CPA | Long-term antifungals (e.g. itraconazole, voriconazole, posaconazole) | Steroids may make CPA worse |
A wrong diagnosis can lead to the wrong treatment — and that can delay recovery or cause harm.
2. 📆 Plan Your Long-Term Care
Each condition has its own journey:
-
ABPA tends to flare up and settle down, often alongside asthma.
-
CPA is usually chronic and progressive, slowly damaging the lungs if untreated.
Knowing your diagnosis helps your doctors decide:
-
How often to scan your lungs (CT or X-rays)
-
What blood tests to monitor (e.g. IgE for ABPA, IgG for CPA)
-
How long to continue medication
-
What symptoms need urgent review
3. ⚠️ Avoid Side Effects and Harm
If you're given steroids for the wrong condition (e.g. CPA), they can:
-
Weaken your immune system
-
Let the fungal infection get worse
-
Increase the risk of diabetes, weight gain, or bone thinning
And if you’re given antifungals for ABPA without treating the allergy side, you might still keep having flare-ups.
A correct diagnosis helps your team weigh up risks and benefits — and adjust safely.
4. 🏥 Access the Right Specialist Services
In the UK, some treatments are only available for specific diagnoses:
-
Biologic drugs like omalizumab or mepolizumab are only available for severe ABPA under strict NHS criteria.
-
Long-term antifungal treatment for CPA is provided by highly specialised services, such as the National Aspergillosis Centre in Manchester.
Without the right diagnosis on record, access to these treatments may be delayed or blocked.
5. 🧭 Understand What to Expect
An accurate diagnosis helps you understand:
-
What symptoms are normal, and what should be reported
-
Whether your condition is likely to get better, stay the same, or slowly worsen
-
What lifestyle changes, home monitoring, or support groups might help
It also allows your care team to link you to others with similar conditions — for advice, reassurance, and shared experiences.
🧪 What Tests Help Make the Diagnosis?
Your specialist may request:
-
Blood tests (e.g. IgE, IgG antibodies to Aspergillus)
-
CT scans to look at the shape of your lungs
-
Sputum or bronchoscopy samples to grow or detect the fungus
-
Breathing tests (lung function) to assess airflow and trapping
These help build a full picture — no one test is enough on its own.
💬 In Summary
“Aspergillosis” is an umbrella term — but the exact type you have really matters.
Getting the correct diagnosis helps ensure:
-
🧬 You get the most effective treatment
-
📊 You avoid unnecessary harm
-
📆 You have the right follow-up plan
-
🧠 You understand your condition better
-
🩺 You can access the right NHS services
If you're not sure which type of aspergillosis you have — or you feel your diagnosis hasn’t been reviewed in a while — speak to your GP or respiratory team.
🫁 Understanding Bronchiectasis, COPD, and Aspergillosis: What Patients Need to Know
Living with a lung condition can be confusing — especially when the symptoms of bronchiectasis, COPD, and aspergillosis are so similar. This guide explains the differences, how they are diagnosed, and why many people are wrongly diagnosed (or underdiagnosed) at first.
🌬️ What Are These Conditions?
Bronchiectasis
A condition where the airways become damaged, widened, and scarred, often from past infections, immune problems, or conditions like ABPA or CPA. This makes it hard to clear mucus, leading to regular infections.
COPD (Chronic Obstructive Pulmonary Disease)
A group of conditions — including emphysema and chronic bronchitis — that cause narrowed airways and damaged air sacs. Most often caused by smoking or long-term exposure to fumes or dust.
Aspergillosis
An infection or allergic reaction caused by the fungus Aspergillus. Types include:
-
ABPA (allergic bronchopulmonary aspergillosis) — mostly in asthma or bronchiectasis
-
CPA (chronic pulmonary aspergillosis) — causes lung cavities and fungal balls
-
Aspergillus bronchitis — low-grade infection in people with bronchiectasis
🔄 Shared Symptoms
All three can cause:
| Symptom | Bronchiectasis | COPD | Aspergillosis |
|---|---|---|---|
| Chronic cough | ✅ | ✅ | ✅ |
| Sputum (phlegm) | ✅ (often a lot) | ✅ (varies) | ✅ (sticky, sometimes brown) |
| Breathlessness | ✅ | ✅ | ✅ |
| Recurrent infections | ✅ | ✅ | ✅ |
| Fatigue | ✅ | ✅ | ✅ |
| Wheezing | Sometimes | ✅ | ✅ in ABPA |
| Coughing blood (haemoptysis) | ✅ | ⚠️ | ✅ (especially in CPA) |
Because the symptoms are so similar, many people with aspergillosis are first told they have COPD or bronchiectasis until further tests are done.
🖥️ How Are They Diagnosed?
🧪 Tests Used
| Test | Helps Diagnose |
|---|---|
| Spirometry (lung function) | COPD or asthma (airflow obstruction) |
| High-resolution CT scan | Bronchiectasis, CPA, emphysema |
| Aspergillus IgG & IgE blood tests | CPA (IgG), ABPA (IgE) |
| Sputum culture or PCR | Finds Aspergillus or bacterial infections |
| Eosinophil count | High in ABPA |
| Chest X-ray | May show cavities, but CT is better |
🫁 CT Scan Signs: What Do Radiologists Look For?
| Feature | Bronchiectasis | COPD | CPA / Aspergillosis |
|---|---|---|---|
| Airway shape | Widened, thickened (signet-ring sign) | Narrowed or normal | May have overlapping bronchiectasis |
| Lung tissue | Scarring, mucus plugging | Blackened areas (emphysema) | Cavities, fungal balls, fibrosis |
| Mucus | Often present | Sometimes present | Mucus or fungus in airways |
| Other signs | Tree-in-bud, cystic changes | Air trapping, flattened diaphragm | Thickened cavity walls, pleural changes |
💨 What Are Air Trapping and Hyperinflation?
These are signs that air is getting stuck in the lungs — common in asthma, COPD, ABPA, and sometimes CPA.
🔹 Air trapping
Air gets into the lungs but can’t get out fully. You may feel like you can’t finish exhaling.
-
Seen on CT scan as dark areas during breathing out.
-
Lung function tests show high residual volume (RV).
-
Common in asthma, ABPA, bronchiectasis, and COPD.
🔹 Hyperinflation
The lungs are permanently overfilled with air, even when you’re not trying to breathe in.
-
Seen on CT/X-ray as large lungs, flattened diaphragm, and horizontal ribs.
-
Lung function shows high total lung capacity (TLC).
-
Common in emphysema, severe asthma, and ABPA.
Why it matters: Both conditions make breathing harder and less efficient, especially when active. Treatment like inhalers, antifungals, airway clearance, or biologics may help.
💊 Treatment Approaches
| Treatment | Bronchiectasis | COPD | Aspergillosis |
|---|---|---|---|
| Airway clearance physiotherapy | ✅ Essential | Sometimes | ✅ Often vital |
| Antibiotics | ✅ Regularly used | During flares | ✅ For Aspergillus bronchitis/CPA |
| Inhalers (bronchodilators) | Sometimes helpful | ✅ Core treatment | ✅ In ABPA if asthma is present |
| Steroids | In flares or ABPA | ✅ Often | ✅ In ABPA |
| Antifungals (e.g. itraconazole, voriconazole) | ❌ Not routine | ❌ | ✅ Main treatment for CPA/ABPA |
| Pulmonary rehab | ✅ | ✅ | ✅ May help fatigue/breathlessness |
| Oxygen | Rare | ✅ In advanced disease | ✅ In some advanced cases |
🧠 Why It’s Complicated
Many patients are misdiagnosed at first:
-
Aspergillosis can develop on top of COPD or bronchiectasis
-
A long delay in diagnosis is common
-
Some people have all three conditions, or overlapping features (e.g. COPD + ABPA)
That’s why blood tests and CT scans are so important — symptoms alone aren’t enough.
✅ Summary Table
| Feature | Bronchiectasis | COPD | Aspergillosis |
|---|---|---|---|
| Cause | Infection, immune issues | Smoking, pollutants | Fungal allergy or infection |
| Airway problem | Widened, mucus-filled | Narrowed, damaged sacs | Cavities, fungus growth or allergy |
| Diagnostic test | CT scan | Spirometry | CT + Aspergillus IgG/IgE |
| Key treatment | Clearance + antibiotics | Inhalers, steroids | Antifungals ± steroids |
💬 What Should I Ask My Doctor?
-
Could my symptoms be due to more than one condition?
-
Have I had a CT scan and Aspergillus blood tests?
-
Should I be seen by a specialist centre (e.g. for ABPA or CPA)?
-
Am I using the right inhalers or physiotherapy?
-
Could I benefit from a sputum test or antifungal treatment?
🫁 Airway Clearance in Aspergillosis: A Patient Guide
Managing mucus to breathe easier, stay healthier, and feel more in control
💡 Why Is Mucus Clearance Important?
If you’re living with a condition like chronic pulmonary aspergillosis (CPA), allergic bronchopulmonary aspergillosis (ABPA), or aspergillus bronchitis, you may experience ongoing mucus build-up in your lungs. This can:
-
Make breathing harder
-
Trap infection
-
Cause inflammation and damage
-
Trigger coughing, wheeze or breathlessness
Airway clearance techniques (ACTs) help loosen and remove this mucus, reduce chest infections, and improve daily comfort.
🗣️ “Before I started clearing mucus properly, I thought breathlessness was just something I had to live with. But it’s made a big difference.”
🔧 What Techniques Are Available?
| Type | Examples | Purpose | Needs Guidance? |
|---|---|---|---|
| Breathing exercises | ACBT (Active Cycle of Breathing), huffing | Loosens mucus, clears airways | ✅ Yes – to be effective |
| Postural drainage | Lying in specific positions | Uses gravity to drain mucus | ✅ Yes – to avoid reflux or fatigue |
| Devices | Flutter, Acapella, Aerobika (OPEP devices) | Vibrate airways + create back pressure to shift mucus | ✅ Yes – to use correctly |
| Manual techniques | Chest percussion, assisted cough | Help loosen stubborn mucus | ✅ Often needs a helper |
| Mechanical devices | HFCWO (“The Vest”), IPV | Used in severe or complex cases | ✅ Prescribed in specialist settings |
🗣️ “I use the Acapella in the mornings while the kettle boils. It’s part of my routine now – and it really helps.”
🗣️ What Do Other Patients Say?
People with aspergillosis often try more than one method before finding what works best. Here are some common reflections:
On devices:
“The flutter helped a lot once I got the angle and rhythm right – but I needed someone to show me how.”
On ACBT:
“Breathing control and huffing helped me get more up with less effort than coughing all day.”
On adapting to daily life:
“It’s about what fits into your day. If something’s too awkward or tiring, you won’t keep doing it – and that’s okay.”
On trial and error:
“It took me months to find the right technique – but now I can manage my mucus better and avoid antibiotics.”
⚠️ Should I Use a Flutter or Acapella Without Help?
Not at first. These devices are effective only if used correctly. Risks of incorrect use include:
-
Not moving mucus effectively
-
Fatigue or breathlessness
-
Worsening reflux or chest tightness
-
In rare cases, worsening of lung symptoms (e.g., if air trapping occurs)
🗣️ “I bought a device online and started using it myself – but it made me dizzy. A physio later explained I was blowing too hard.”
Always ask your respiratory team or GP for referral to a respiratory physiotherapist before starting.
📝 Patient Decision Guide: Should You Use ACTs?
✅ You may benefit if:
-
You cough up mucus daily or feel it’s “stuck”
-
You’ve had repeated chest infections
-
You live with CPA, ABPA, bronchiectasis, or aspergillus bronchitis
❌ Don’t start without guidance if:
-
You have COPD, asthma, or lung scarring
-
You’ve had haemoptysis (coughing up blood)
-
You experience dizziness, nausea, or chest pain during breathing exercises
-
You have gastric reflux or recent chest surgery
🧑⚕️ What Can I Start Safely at Home?
Without needing equipment, you can begin with:
-
💧 Drink plenty of fluids – thin mucus is easier to clear
-
🪑 Sit upright – especially when coughing or during infections
-
🌬️ Use breathing control – calm, gentle breaths can reduce breathlessness
-
🗣️ Try huffing – like breathing out a mirror; easier than deep coughing
🗣️ “Even on days when I’m tired, I try to stay upright and do a few rounds of breathing exercises. It’s become a habit that helps.”
🧭 Next Steps: What to Ask Your Doctor or Nurse
-
Could I see a respiratory physiotherapist to help with mucus clearance?
-
What technique is best for my condition (e.g., ABPA vs. CPA)?
-
Can I be shown how to use a flutter device or Acapella safely?
-
What should I do if I feel worse after using a technique?
🗣️ “The physio made all the difference – she explained what my lungs were doing and helped me pick something that actually worked.”
💬 Final Word
🗣️ “It’s not just about technique – it’s about what fits your life. Small steps like staying hydrated, using huffing, and getting guidance made a big difference for me.”
There’s no one-size-fits-all approach – but with the right support, airway clearance can help you take control of your lungs, reduce flare-ups, and breathe easier.
Biologics and Long Term Side Effects
✅ What Are Biologics?
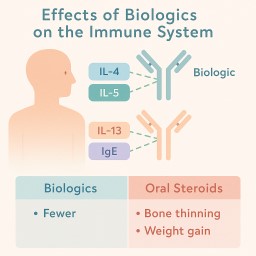
Biologics are targeted treatments made from living cells. They work by blocking parts of the immune system that cause inflammation — for example:
-
IL-4, IL-5, IL-13: linked to eosinophilic inflammation
-
IgE: linked to allergies and ABPA
They are not immunosuppressants like steroids or chemotherapy, but rather immune modulators.
💊 Long-Term Side Effects – What Do We Know?
👨⚕️ What research and experience show:
| Biologic | Used for | Long-term safety known? | Side effects most reported |
|---|---|---|---|
| Omalizumab (Xolair) | Allergic asthma, ABPA | 20+ years of use | Injection site reactions, headache, very rare anaphylaxis |
| Mepolizumab (Nucala) | Eosinophilic asthma, CPA | 10+ years | Fatigue, headache, shingles (rare), mild infections |
| Benralizumab (Fasenra) | Severe asthma, CPA | ~6–7 years | Headache, pharyngitis, injection site issues |
| Dupilumab (Dupixent) | Asthma, eczema, nasal polyps | 6–8 years | Eye dryness/redness, cold sores, joint pain (rare) |
| Tezepelumab (Tezspire) | Severe asthma | ~2 years | Sore throat, joint pain, injection site reactions |
⚠️ Possible Long-Term Concerns (but rare)
-
Infections: Some concern about slightly increased risk of herpes zoster (shingles) or respiratory viruses, but overall risk is very low compared to steroids.
-
Immunogenicity: Your body might develop antibodies to the drug over time, reducing its effect — this is more a loss of benefit, not a dangerous side effect.
-
Cancer risk: No consistent evidence linking asthma/ABPA biologics to cancer.
-
Unknowns: Because some biologics are new (e.g. tezepelumab), we don't yet have 20-year data — but so far the safety profile is reassuring.
🩺 Compared to Oral Steroids
| Treatment | Side Effects Over Time |
|---|---|
| Steroids (e.g. prednisolone) | Weight gain, diabetes, infections, bone thinning, cataracts, adrenal suppression |
| Biologics | Mostly minor – injection site pain, headache, mild infection risk, rare allergic reaction |
So in most cases, biologics reduce the need for steroids and therefore reduce long-term harm.
💬 Patient Experience
Most patients report:
-
Improved quality of life
-
Reduced asthma/ABPA attacks
-
Fewer hospital visits
-
Very few stop due to side effects
✅ Summary
| Question | Answer |
|---|---|
| Do biologics have long-term side effects? | Usually mild and rare; mostly injection reactions or mild infections |
| Are they safer than long-term steroids? | Yes, especially over years |
| Should I be worried? | Not usually — but always monitor with your team |
| How long have they been used? | 6–20+ years, depending on the biologic, with very good safety data |