Drug Safety in the UK: What Aspergillosis Patients Need to Know
Living with aspergillosis often means taking powerful medicines for a long time — antifungals, steroids, antibiotics, or even biologics. These treatments can be life-saving, but they can also cause side effects, especially when used together. It’s natural to wonder: How do we know these drugs are safe? What happens if something goes wrong?
This article explains how drug safety is managed in the UK, what happens when rare problems occur, and what resources patients can use to protect themselves.
How Medicine Safety Works
Before a drug is approved:
Every new medicine goes through several phases of clinical trials. These trials are not just about proving that the drug works (efficacy) — they are also about proving it is safe enough to use in people. Researchers record every possible side effect, monitor blood tests, and look for safety signals as well as improvements in the illness.
However, trials have limits. They usually include only a few thousand participants, so they can reliably detect common side effects but not very rare ones. For example, if a side effect happens in 1 in 100,000 people, and a trial only studies 50,000, it may not appear at all.
After a drug is approved:
Once a medicine is prescribed to thousands or millions of people, those rare side effects start to appear. For example, in the first million patients, perhaps 10 cases may be reported. That’s not manipulation — it’s just the maths of large numbers.
How Do Doctors Link a Side Effect to a Medicine?
When someone develops a new symptom, it isn’t always obvious whether it’s caused by their illness, another condition, or the medicine they’re taking. Linking a side effect to a drug usually involves several steps:
-
Timing – Did the symptom start soon after beginning the medicine? Did it improve when the medicine was stopped? Timing is often the strongest clue.
-
Known side effect profile – Doctors check if the symptom has been reported before in trials, studies, or drug safety updates.
-
Other explanations – Could it be the underlying condition (like aspergillosis) or another drug? All possible causes are reviewed.
-
Drug interactions – Many side effects come from the way medicines interact, rather than one drug alone. Antifungals like itraconazole and voriconazole interact with steroids, antibiotics, and heart drugs.
-
Rechallenge (rarely used) – Sometimes a drug is restarted to see if the side effect returns. This can provide strong evidence but is only done when absolutely necessary.
-
Patient reporting – A single case may not prove much, but when dozens of patients report the same issue, patterns become clear.
🔎 Key message: It’s not always quick or simple to prove a side effect. That’s why your own observations — when it started, how it feels, what other medicines you’re on — are so valuable to your doctors and to the Yellow Card system.
What Happens to Those Patients?
-
Every case is recorded and investigated. Regulators like the MHRA (Medicines and Healthcare products Regulatory Agency) look for patterns.
-
If a link is confirmed, they can issue warnings, add monitoring requirements, restrict use, or withdraw the drug.
-
For the patients affected, the drug is usually stopped, and supportive treatment is given. Sadly, in some cases, harm cannot be reversed.
This is why reporting side effects is so important. Each individual case helps build the full safety picture and protects others in the future.
Is This “Experimenting on Patients”?
It can sometimes feel that way — because new medicines are still watched closely after approval, and some harms are only seen later.
But there’s an important distinction:
-
Clinical trials are the experiments, and they are about safety as much as efficacy. Every trial phase collects safety data, and a medicine cannot be approved unless it is shown to be safe enough for use.
-
Post-marketing monitoring is not an experiment — it’s a safety net that exists for all medicines, because no trial is ever large enough to catch every very rare problem.
Patients aren’t being experimented on after approval, but your experience does matter. Every report adds to knowledge and helps keep medicines safe for everyone.
Who Is Liable If Harm Occurs?
-
Negligence (e.g. wrong dose, ignoring abnormal tests): the prescriber or hospital may be liable.
-
Defective product or hidden data: the manufacturer may be held responsible, sometimes through compensation schemes or legal action.
-
Very rare, unpredictable events despite correct use: liability is often less clear, and compensation is not guaranteed.
This can feel unfair. A few patients may suffer harm without anyone being “at fault.” That’s why strong safety monitoring and reporting are so essential.
Balancing Benefit and Risk
If 10 people out of a million are harmed, 999,990 people may have been helped — often in life-saving ways. That doesn’t make the harm any less real, but it explains why regulators still approve medicines with very rare risks: the benefit to the vast majority outweighs the small chance of harm, as long as those harms are recognised and acted on quickly.
Looking forward, science may allow us to predict who is at risk of those 1-in-a-million harms (through genetics or biomarkers) and screen them out — so that only those who can benefit safely receive the drug.
Key UK Drug Safety Resources
Here are the most useful resources for patients in the UK:
-
Yellow Card Scheme – report any suspected side effect or device problem. Patients, carers, and clinicians can all use it.
-
MHRA – the government body that regulates medicines and devices, publishes safety updates.
-
NHS Medicines A–Z – patient-friendly information on most drugs, including side effects.
-
Electronic Medicines Compendium (eMC) – official patient information leaflets for every licensed UK medicine.
-
British National Formulary (BNF) – the prescribers’ reference, also viewable by patients.
What Aspergillosis Patients Need to Remember
Because aspergillosis often requires long-term, powerful medicines like itraconazole, voriconazole, posaconazole, steroids, or biologics, patients are more likely to:
-
Experience side effects
-
Need regular blood tests to check drug levels
-
Take multiple medicines with possible interactions
Three key takeaways:
-
Know where to look – check NHS Medicines A–Z or your medicine leaflet (eMC) if you’re unsure about a side effect.
-
Report problems – use the Yellow Card scheme to flag any suspected reaction.
-
Stay in touch with your team – never stop or change your medicine without advice, but do share new symptoms with your GP or specialist promptly.
✅ Bottom line: Clinical trials test both safety and effectiveness, but no study can capture every rare event. That’s why medicines continue to be monitored after approval, and why patient reporting is so important. By working together — patients, doctors, and regulators — we make medicines safer for everyone.
Medicine Leaflets, Side Effects, and Interactions: Where to Find Reliable Information
When you open a new box of medicine, you’ll usually find a folded sheet of paper inside — the Patient Information Leaflet (PIL). These leaflets are important, but they can be hard to read because of the tiny print and the amount of information squeezed onto the page.
Patients often ask: Where does this information come from? What if I can’t read it? And how do I check for drug interactions as well as side effects?
Here’s what you need to know.
1. Where do leaflets come from?
-
Written by the manufacturer – The drug company that makes the medicine is legally required to prepare the leaflet.
-
Checked by regulators – In the UK, the MHRA (Medicines and Healthcare products Regulatory Agency) reviews and approves the leaflet before the medicine is sold. In Europe, this role is carried out by the EMA.
-
Updated regularly – If new safety information comes to light (for example, through the Yellow Card reporting system), the leaflet must be revised and re-approved.
By law, leaflets must include:
-
What the medicine is for.
-
Who can and cannot take it.
-
How to take it.
-
Side effects and how common they are.
-
Possible drug interactions.
-
Storage instructions.
-
How to report suspected side effects.
2. Why the text is so small
Because there’s so much information to fit into a tiny folded sheet, the print is often very small and difficult to read. For many patients, the leaflet in the box just isn’t practical.
3. Where to find more readable versions
If the leaflet is hard to read, you have better options:
-
Electronic Medicines Compendium (eMC)
-
Up-to-date PILs and professional information for nearly all UK-licensed medicines.
-
Easy to zoom, search, and print in large text.
-
BNF (British National Formulary)
-
Trusted source for doctors and pharmacists, but also useful for patients.
-
Lists side effects, cautions, and drug interactions clearly.
-
NHS.uk
-
Easy-to-read summaries of common medicines.
-
Pharmacist
-
Can print a large-text version of the leaflet.
-
Can check for interactions with other medicines you take.
-
Some companies provide Braille, audio, or large-print versions on request.
-
4. Where to check drug interactions
Drug interactions are just as important as side effects, because they can make medicines stronger, weaker, or more dangerous.
-
BNF online (bnf.nice.org.uk) – the best source in the UK, used by clinicians, with a clear section on interactions.
-
eMC (SmPC section) – each drug’s Summary of Product Characteristics includes detailed interaction data.
-
Pharmacist or GP – the safest and most personal check, since they know your full medication list.
-
Hospital specialists – especially important if you are on antifungals, as these interact with many other medicines.
5. The bottom line
Medicine leaflets are carefully written, regulated documents — but the folded sheet in your box isn’t the only option, and it’s often not the easiest to use.
👉 You don’t have to struggle with tiny print. Reliable, readable versions are available online (eMC, BNF, NHS.uk), and your pharmacist can explain and print large-text copies.
👉 For drug interactions, never rely on random internet sources — use the BNF, eMC, or your healthcare team.
And if you’re ever unsure, ask your doctor or pharmacist before starting anything new, including over-the-counter medicines or supplements.
Side Effects, New Medicines, and Safety Reporting: What Every Patient Should Know
Modern medicines, including antifungals used for aspergillosis, can be life-saving. But they can also have powerful side effects. One patient recently described developing nerve damage (neuropathy) while on treatment, but never mentioned it to their doctor, because they didn’t know it could be a side effect. Sadly, by the time it was recognised, the damage was permanent.
This story shows why patients and doctors need to work together in partnership to spot and report side effects early — especially when medicines are new and real-world safety data is still limited.
1. From passive role to partnership
In the past, healthcare was one-way: the doctor gave instructions, the patient followed. Today the NHS encourages shared responsibility:
-
Doctors bring their expertise about the illness and treatments.
-
Patients bring their daily experience of living with the condition.
-
Together they can make safer, better-informed decisions.
This partnership is essential for powerful drugs like antifungals, where side effect monitoring depends on both sides working together.
2. Why side effect statistics can be misleading
Leaflets list side effects as “common” or “rare,” often with percentages. But these figures don’t always reflect real life because:
-
Trials are limited – only a few thousand people take part, often younger and healthier than typical NHS patients.
-
Under-reporting is common – doctors and patients often fail to report side effects, especially mild ones.
-
Bias exists – severe or unusual reactions are reported more often than everyday ones.
👉 Bottom line: leaflets tell us what can happen, not always how often it happens.
3. The Yellow Card system
The UK’s main tool for detecting safety issues is the Yellow Card Scheme, run by the MHRA.
-
Anyone can report: doctors, nurses, pharmacists, patients, or carers.
-
Reports are vital: patterns in these reports may reveal risks not seen in trials.
-
Action is taken: if needed, leaflets are updated, warnings issued, or drugs restricted/withdrawn.
You can report suspected side effects at yellowcard.mhra.gov.uk.
4. Why reporting matters
Poor reporting leads to harm:
-
Delayed warnings – e.g. photosensitivity with voriconazole took years to be recognised.
-
Biased safety data – drugs may seem safer than they are.
-
Preventable harm – patients may suffer permanent injury before action is taken.
For new medicines (marked with a ▼ black triangle in the BNF and leaflets), the MHRA asks for all side effects to be reported, no matter how small.
5. Extra protections for new medicines
When a drug is new, safety systems are stronger than usual:
-
Black triangle (▼) – signals “additional monitoring” so all suspected ADRs should be reported.
-
Specialist prescribing – new antifungals are usually limited to centres like NAC.
-
Closer monitoring – frequent blood tests, drug levels, eye or skin checks depending on risk.
-
Risk Management Plans – agreed with regulators, spelling out what to watch for.
-
Post-marketing studies – Phase 4 trials track safety in real-world patients.
These safeguards are extensive, but not fool-proof. Rare or long-term effects may still emerge only after years of wider use.
6. The NHS challenge
Despite the systems:
-
Only a small percentage of doctors file Yellow Card reports each year.
-
Most GPs never prescribe brand-new drugs — so reporting falls heavily on specialist centres like NAC.
-
Under-reporting risks harm, increases NHS costs, and erodes trust.
7. Who sets the rules?
Several organisations provide guidance on reporting and safety:
-
MHRA (UK regulator): runs Yellow Card, monitors new and established drugs, and issues safety updates.
-
BNF (British National Formulary): highlights side effects, black triangle drugs, and links to reporting tools.
-
GMC (General Medical Council): obliges doctors to report serious ADRs and all reactions to ▼ drugs.
-
EMA (European Medicines Agency): operates EudraVigilance, pooling reports from across Europe.
-
Global standards: the UK follows international rules (ICH E2B) so data is shared worldwide.
8. What patients can do
You are central to this safety net:
-
Be observant – notice anything new or unusual.
-
Keep a record – note when it started, how often, and any changes with medication.
-
Report promptly – tell your team and consider submitting a Yellow Card yourself.
-
Ask questions – “What side effects should I look out for? Which are urgent? How will we monitor this drug?”
-
Use trusted sources – NHS.uk, bnf.nice.org.uk, NAC, or your pharmacist.
9. The reality of side effects
For many, side effects are not “minor inconveniences.” They can mean:
-
Permanent disability (e.g. nerve or vision damage).
-
Loss of independence or mobility.
-
Social isolation and depression.
That’s why side effect monitoring is not just bureaucracy — it’s about protecting real lives.
Key message
The systems around new medicines are extensive but not fool-proof. That’s why patients and doctors must work as partners.
👉 If you notice something new, strange, or worrying while on antifungal medication — however small — tell your healthcare team and consider reporting it. Your report may be the missing piece that protects you and others.
Working With Your Medical Team: What Every Patient With Aspergillosis Needs to Know
Modern antifungal treatments, and many of the medicines used alongside them, can be life-saving. They help control infections that would otherwise cause severe damage to the lungs and other organs. But these medicines are also powerful, and like all strong treatments, they sometimes carry risks.
One patient recently shared that they developed nerve damage (neuropathy) while taking antifungal medication, but did not mention it to their doctor because they did not know it could be a side effect. Sadly, problems like this can sometimes become permanent if not spotted early.
This raises an important question: what do patients need to know about their responsibilities when taking medicines like antifungals, and more broadly, when living with aspergillosis?
From passive role to partnership
In the past, healthcare often worked in one direction: the doctor gave instructions, and the patient was expected to follow them. Patients were mostly passive, with little chance to ask questions or take part in decisions.
The NHS is now moving towards a very different way of working: partnership.
This means:
-
Doctors and nurses share their medical knowledge.
-
Patients share their experiences of living with their condition.
-
Together, both sides decide what treatment and care will work best.
Why doctors sometimes hesitate about side effects
Some patients are surprised to learn that not all doctors automatically tell patients about possible side effects. Why is this?
-
Some worry about causing anxiety or putting patients off treatment.
-
Others fear the nocebo effect — where simply knowing about a side effect can make someone more likely to notice it.
-
They may also feel that handing over a long list of possible effects is overwhelming.
But when it comes to antifungals and other long-term, powerful medicines, not knowing can be dangerous. If patients do not know what to look for, they may ignore early signs of serious problems until it is too late.
The best approach is balance:
-
Patients don’t need to memorise an endless list.
-
They do need a clear, short list of the most important and urgent symptoms to look out for — and to know what to do if they appear.
Medicines: what patients should do
-
Take medicines as prescribed – antifungals, inhalers, steroids, or biologics must be taken on schedule. Missing doses can reduce effectiveness or drive resistance.
-
Do not stop suddenly – especially steroids. Always follow tapering advice.
-
Check for interactions – antifungals can clash with common medicines such as statins, blood pressure tablets, and painkillers. Always tell your team about new prescriptions, over-the-counter drugs, or supplements.
-
Use the same pharmacy if possible – so interactions are checked consistently.
Monitoring your health
-
Attend all scheduled tests – blood work, lung function, CT scans. These can reveal hidden changes before you feel them.
-
Know your “normal” – keep track of oxygen levels (if you use a pulse oximeter), peak flow, sputum colour, cough, and breathlessness.
-
Spot infections early – worsening cough, fever, or new sputum colour may mean infection or flare-up. Report these quickly.
Communication with your team
-
Bring notes to clinic – write down questions and symptoms so nothing is forgotten.
-
Be open and honest – if you’ve missed doses, struggled with side effects, or found treatment difficult, let your team know.
-
Keep contact details handy – know who to call if problems arise (specialist nurse, hospital helpline, GP).
Lifestyle and prevention
-
Reduce exposure to moulds – avoid compost heaps, rotting leaves, damp basements, and building dust. If you cannot avoid them, wear an FFP2/3 mask.
-
Protect your lungs – keep up with vaccinations (flu, COVID-19, pneumococcal).
-
Support your overall health – eat well, stay as active as you can, and rest when needed.
-
Look after your mental health – chronic illness is stressful. Patient groups, counselling, or peer support can make a big difference.
Self-management skills
-
Recognise flare-ups – learn the difference between ABPA flare, CPA progression, and bacterial infection symptoms.
-
Know your rescue plan – what to do if you suddenly worsen (extra inhalers, antibiotics, or emergency help).
-
Keep records – note symptoms, hospital visits, and medication changes. This helps spot long-term patterns.
-
Be part of decisions – ask about benefits, risks, and alternatives of treatments. Care should fit your life as well as your lungs.
Where to find reliable information on medicines
Many patients say the leaflet in the medicine box is written in tiny print or feels overwhelming. You do have other options:
-
Ask your clinical team or pharmacist — they can give you a short list of the most important side effects to watch for and explain what’s urgent.
-
Check the BNF (British National Formulary) online — the NHS makes this trusted reference free to the public at bnf.nice.org.uk. It lists side effects, drug:drug interactions, and safety notes.
-
Use NHS.uk — clear pages on most medicines, written in plain English.
-
Patient support organisations — such as the National Aspergillosis Centre or relevant charities, which often provide tailored advice.
If you’re unsure, it’s always safer to ask rather than guess.
The bigger picture: partnership
In the past, doctors made decisions and patients followed instructions. Today, with complex conditions like aspergillosis, patients are central members of the care team.
-
You notice problems first.
-
You take daily responsibility for medication.
-
You decide when to seek help.
This isn’t about shifting the whole burden onto patients — it’s about recognising that care works best when it is a true partnership.
Key message
👉 If you notice something new, strange, or worrying while on antifungal medication — however small — tell your healthcare team. Don’t assume it’s not important.
And remember: safe, effective treatment is a two-way street. Your role as a patient is not just to take medicines, but to observe, record, communicate, and partner with your team. That partnership is what keeps you safe and makes your treatment work.
⚠️ Mistakes in NHS Care: Why They Happen & What You Can Do
🔎 Why mistakes happen
-
Heavy workload: Doctors and nurses handle huge numbers of patients and results every day.
-
Fragmented IT systems: GP, hospital, and lab systems don’t always link, so information can get lost.
-
Human error: Fatigue, multitasking, and assumptions all increase the risk of oversight.
-
Defensive culture: Trusts sometimes minimise problems to protect reputation or avoid litigation.
Most errors are not deliberate — but they can cause harm if they are not caught quickly.
Martha’s Rule was created after a young girl died when her family’s concerns were ignored — it’s designed to stop that happening again.
🛡 What safeguards are already in place?
Although mistakes still happen, the NHS has many systems to reduce risk and catch errors early:
-
Critical results alerts: Labs automatically flag dangerously abnormal results so they cannot be overlooked.
-
Early Warning Scores (NEWS2): Vital signs generate a score that prompts urgent review if the patient is deteriorating.
-
Sepsis protocols: Hospitals have rapid-response pathways for suspected sepsis.
-
Cross-checking: High-risk drugs often require two professionals to sign off.
-
Incident reporting: Staff can log “near misses” to help the system learn.
-
Duty of Candour: Trusts must inform patients if serious harm has been caused by an error.
-
Martha’s Rule: Gives patients/families the right to request an urgent independent review if they feel concerns are being ignored.
💻 Are new IT systems making care safer?
The NHS is moving to large electronic patient record (EPR) systems such as Epic, Cerner and Lorenzo. These bring real safety gains:
Safer features
-
Automatic alerts for critical blood results.
-
Built-in early warning score (NEWS2) calculations to detect deterioration.
-
Electronic prescribing with dose, allergy, and interaction checks.
-
Shared records across hospitals, GPs, and community services.
-
Digital audit trails showing who reviewed results and when.
But challenges remain
-
Too many alerts can cause “alert fatigue,” leading staff to dismiss warnings.
-
System crashes or downtime can force staff back to paper, which is less safe.
-
Complexity can slow clinicians down until they are confident with the system.
-
Hospital and GP systems still don’t fully integrate everywhere, so results can still be missed.
Bottom line: New IT has improved safety compared to the old paper-and-fax systems, but it isn’t foolproof. It works best alongside clinical vigilance and patient involvement.
✅ What you can do if you suspect a mistake
Step 1. Check directly with the clinical team
-
Ask: “Can you confirm this result/issue has been reviewed?”
-
Request a written explanation or clinic letter.
-
Keep notes of the conversation.
Step 2. Escalate to a senior doctor/clinical lead
-
Ask who the consultant in charge is.
-
Write your concern clearly and factually.
Step 3. If your loved one is deteriorating: use Martha’s Rule
-
You can request an urgent review by a critical care team, separate from the ward team.
-
Available 24/7 in hospitals where introduced.
-
Say: 👉 “We want a review under Martha’s Rule.”
-
If not yet in your hospital, ask for the critical care outreach team.
Step 4. Contact PALS (Patient Advice & Liaison Service)
-
They can chase answers and log concerns.
Step 5. Make a formal complaint to the Trust
-
Keep it factual (what happened, why it matters, what outcome you want).
-
The Trust must acknowledge within 3 working days.
Step 6. Escalate outside the Trust
-
If unsatisfied, go to the Parliamentary and Health Service Ombudsman (PHSO).
🧭 Tips to protect yourself & your family
-
Keep copies of all results and letters.
-
Track your results in a simple log.
-
Bring support (family, advocate, charity like AvMA).
-
Stay factual: stick to dates, facts, and impact.
🔑 Key message
Mistakes in healthcare happen for many reasons — but the NHS has safeguards and new IT systems to reduce risk, and Martha’s Rule adds an extra urgent safety net.
Patients and families still play a vital role by asking questions, checking results, and speaking up.
You are not being difficult — you are being safe.
Misinformation on Social Media: Health and Beyond
Social media helps us stay connected, share experiences, and find support. But it also spreads false or misleading stories — about health, politics, money, and world events. These stories can cause unnecessary fear, confusion, and sometimes real harm if people act on them.
Understanding why misinformation spreads, what’s being done about it, and how to spot it helps keep you and your loved ones safe.
🚩 Why do false stories spread?
-
Algorithms reward attention
Platforms are designed to keep you scrolling. Content that shocks (“miracle cure discovered!”), scares (“hidden danger you’re not being told about!”), or excites spreads the fastest — even if it isn’t true. -
Anyone can post anything
Unlike newspapers, medical journals, or BBC/NHS websites, most social media posts aren’t checked by editors or experts before going live. -
Echo chambers
Platforms show you more of what you already click on. If you read about miracle diets or political conspiracies, you’ll see more of them — true or not. -
Deliberate misinformation
Some people spread falsehoods deliberately:-
To sell fake health products
-
To make money from clicks
-
To influence politics or sow division
-
-
Speed beats accuracy
False stories can go viral in minutes. Corrections are slower and rarely reach as many people.
⚖️ What’s being done about it?
Legal approaches
-
UK: The Online Safety Act (2023) requires platforms to remove illegal or harmful misinformation, including dangerous health advice.
-
EU: The Digital Services Act (DSA) makes large platforms responsible for acting faster against harmful content.
-
Extreme cases: Fraud, scams, defamation, or incitement of violence are not protected speech and can be prosecuted.
Technical approaches
-
Algorithms: AI flags suspicious posts.
-
Labelling: Content can be marked as “false” or “missing context.”
-
Bot control: Platforms limit fake accounts that spread stories at scale.
-
Digital nudges: Some apps ask “Do you want to read before sharing?” or warn if a post is outdated.
The limits
-
Freedom of speech protects many misleading opinions unless they cause direct harm.
-
Global reach makes it hard to police.
-
Volume — billions of posts daily are impossible to check one by one.
-
Trust — some people ignore fact-check labels, believing platforms are biased.
🧐 How to know what’s real
Five quick checks:
-
Who is posting it? NHS, WHO, BBC, or Reuters → reliable. Unknown influencer or “miracle cure” shop → beware.
-
Is it reported elsewhere? Real news appears in multiple reputable outlets.
-
Does it use scare tactics or hype? “Doctors don’t want you to know this secret cure!” → red flag.
-
Can you fact-check it? Try NHS.uk, Full Fact (UK), Snopes, Reuters Fact Check or BBC Verify.
-
Check dates and pictures — old or unrelated content is often recycled to look new.
🚦 The traffic-light test
-
🟢 Green – from official sources, confirmed, calm tone → likely true.
-
🟡 Amber – source unclear, dramatic style, no confirmation elsewhere → pause, check.
-
🔴 Red – sensational, “miracle” claims, conspiracy, or urging you to share → almost certainly false.
💡 Should we avoid social media completely?
Not necessarily. Social media has real value for support, awareness, and connection. The key is using it wisely:
-
Follow trusted organisations for health and news.
-
Unfollow or mute accounts that regularly spread falsehoods.
-
Balance social media with direct trusted sources (NHS, GP, recognised news).
-
Step away if scrolling leaves you anxious, angry, or confused.
✨ Bottom line
False stories spread online because the system rewards attention, not accuracy. Laws and technology help, but they can’t stop misinformation entirely.
The best defence is awareness. Before acting on or sharing any post — whether about health, politics, or world events — pause, check, and if in doubt, don’t share.
👉 Protecting yourself from misinformation means protecting your community too.
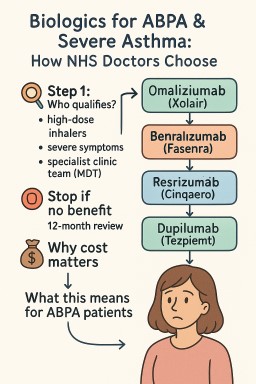
💊 Biologics for ABPA & Severe Asthma: How NHS Doctors Choose
Biologics are modern injection or infusion treatments that target the immune system. They can help people with Allergic Bronchopulmonary Aspergillosis (ABPA) by reducing inflammation, cutting down on steroid use, and lowering flare-ups.
In the UK, consultants must follow NICE (National Institute for Health and Care Excellence) guidance, which sets both clinical criteria and cost-effectiveness rules.
🔎 Step 1: Who qualifies?
-
You must already be on high-dose inhalers and still have severe symptoms.
-
Decisions are made by a specialist severe asthma / ABPA clinic team (MDT).
-
Blood tests, flare history, and steroid use are all considered.
🧭 Step 2: Which biologic?
Consultants match the drug to the type of inflammation you have:
| Pathway / Clues | Possible Biologic | Notes |
|---|---|---|
| IgE-allergic (allergic tests positive, high IgE) | Omalizumab (Xolair) | Works best if perennial allergies are driving symptoms. |
| Eosinophilic (high eosinophil counts, frequent flare-ups, or long-term steroid use) | Mepolizumab (Nucala) or Benralizumab (Fasenra) | NHS requires doctors to choose the least-expensive if both fit. |
| Eosinophils ≥400 + frequent flare-ups | Reslizumab (Cinqaero, IV drip) | Less used, but an option if IV therapy is acceptable. |
| Still severe after above / not eligible | Dupilumab (Dupixent) | Also helps if you have eczema or nasal polyps. |
| Any type, severe with ≥3 flare-ups or on daily steroids | Tezepelumab (Tezspire) | Works even if blood tests don’t show high eosinophils or IgE. |
🛑 Step 3: Stop if no benefit
NICE requires a 12-month review.
-
If your flare-ups or daily steroid dose haven’t fallen enough (usually by ≥50%), treatment should stop.
💷 Why cost matters
-
The NHS only funds biologics judged “cost-effective.”
-
If two drugs are equally suitable, consultants must use the least-expensive one.
-
This doesn’t mean you won’t get the right drug — but sometimes doctors must justify why one biologic is better for you personally.
📌 What this means for ABPA patients
-
ABPA is not directly covered by NICE guidance, but the same biologics are often used if you also meet asthma criteria.
-
Main goals:
-
Reduce oral steroids (prednisolone) and their side-effects.
-
Control flare-ups and lung damage.
-
-
Evidence supports omalizumab, mepolizumab, benralizumab, and dupilumab in ABPA; tezepelumab has less data so far.
✅ Bottom line:
Biologics can be life-changing for ABPA patients, but the NHS pathway means the choice depends on your blood results, flare history, steroid needs — and cost-efficiency rules. If one option doesn’t work, another may still be possible.
Prednisone, Hydrocortisone, and Adrenal Function – What Patients Need to Know
Why Aspergillosis Patients Are Often Given Prednisolone
Prednisolone is often prescribed for patients with aspergillosis (especially Allergic Bronchopulmonary Aspergillosis – ABPA) because it helps to reduce lung inflammation and allergic reactions triggered by Aspergillus spores. It can be life-changing in controlling breathlessness, wheeze, and repeated flare-ups. However, using steroids for weeks or months can affect the body’s own natural hormone production.
How Do I Know If I Might Need Adrenal Testing While on Prednisolone?
Prednisolone is a corticosteroid medicine. If you take it for more than a few weeks, it can “switch off” your adrenal glands, which normally make the hormone cortisol. Cortisol is essential for coping with stress, fighting infection, and maintaining energy.
You might need adrenal testing if you notice:
-
Extreme tiredness or weakness, especially if it worsens when tapering your pred dose.
-
Excessive sleepiness or difficulty staying awake, even when rested.
-
Feeling much worse during stress or illness (for example, flu, chest infection, or surgery).
-
Dizziness or fainting on standing (low blood pressure symptoms).
-
Nausea, vomiting, or stomach pain that isn’t explained by infection or medicines.
-
Unexplained weight loss or poor appetite.
Why Might Patients Stop Making Cortisol?
The adrenal glands may temporarily stop producing cortisol if they have been “switched off” by long-term steroid treatment. This is called secondary adrenal insufficiency. It is usually reversible, but recovery can take months or even years.
In contrast, primary adrenal insufficiency (Addison’s disease) is when the adrenal glands are damaged and stop working permanently. This is not caused by steroids, but by autoimmune or other diseases.
Symptoms of Low DHEA
The adrenal glands also produce DHEA, a weak sex hormone that contributes to mood, energy, and libido — particularly important in women. Long-term steroid use or secondary adrenal insufficiency may reduce DHEA levels.
Possible signs of low DHEA:
-
Ongoing low energy or fatigue, even when cortisol is replaced
-
Low mood, depression, or “flat” emotions
-
Reduced libido (sex drive)
-
Thinning of underarm or pubic hair (especially in women)
-
Lower resilience or general sense of well-being
Not all patients with adrenal insufficiency need DHEA replacement, but in some, it can make a difference. This is assessed by specialists.
How to Tell the Difference Between Causes of Fatigue
Because fatigue can come from several overlapping sources, it helps to compare:
| Symptom | Cortisol deficiency (Adrenal Insufficiency) | Prednisolone Side Effect | Low DHEA |
|---|---|---|---|
| Sudden exhaustion during stress/illness | ✅ | ❌ | ❌ |
| Sleepiness, can’t stay awake | ✅ | ❌ | ❌ |
| Dizziness or fainting | ✅ | ❌ | ❌ |
| Nausea, vomiting, stomach upset | ✅ | ❌ | ❌ |
| Insomnia, wired-but-tired feeling | ❌ | ✅ | ❌ |
| Mood swings, irritability | ❌ | ✅ | ❌ |
| Weight gain, bloating, “puffy face” | ❌ | ✅ | ❌ |
| Ongoing low energy despite treatment | ❌ | ❌ | ✅ |
| Low mood, “flat” emotions | ❌ | ❌ | ✅ |
| Reduced libido | ❌ | ❌ | ✅ |
| Thinning pubic/underarm hair (women) | ❌ | ❌ | ✅ |
✅ = typical feature
Prednisolone, Hydrocortisone and Fatigue
-
If a patient is on prednisolone and feels extremely fatigued during stress or illness, it may mean their body is not making enough natural cortisol.
-
If they are tapering prednisolone and develop fatigue or sleepiness, this can mean the taper is too fast and the adrenal glands have not “woken up” yet.
-
If a patient feels tired while still on prednisolone, it could be due to:
-
Side effects of prednisolone itself,
-
Lack of natural cortisol (adrenal suppression),
-
Or low DHEA.
-
Treatment and Monitoring
-
Doctors may recommend slowing or pausing tapering if adrenal insufficiency is suspected.
-
Some patients are switched to hydrocortisone, which more closely mimics natural cortisol.
-
In situations of stress (infection, surgery, trauma), patients may need extra “stress doses” of steroids.
-
Patients at risk should carry a steroid emergency card or medical alert bracelet.
👉 Key message:
Aspergillosis patients often need steroids, but long-term use can suppress natural adrenal function. Fatigue can come from:
-
Low cortisol,
-
Prednisolone side effects,
-
Or low DHEA.
Since these overlap, specialist endocrine advice is often needed to work out the cause.
Brensocatib for Aspergillosis Patients: A New Approach to Managing Bronchiectasis and Inflammation
Brensocatib is a promising investigational medication currently under evaluation for the treatment of non-cystic fibrosis bronchiectasis (NCFBE) and other neutrophil-driven diseases, including conditions related to Aspergillus infections like aspergillosis. This article explores how brensocatib may benefit patients with aspergillosis, particularly those dealing with bronchiectasis and other complications that arise from chronic Aspergillus infections.
Note that brensocatib is NOT a cure for bronchiectasis or aspergillosis.
What is Brensocatib?
Brensocatib is an oral Dipeptidyl Peptidase 1 (DPP-1) inhibitor, a new class of drugs that targets neutrophil serine proteases, which are enzymes involved in the inflammation and tissue damage seen in chronic respiratory diseases. By inhibiting DPP-1, brensocatib reduces the activation of these destructive enzymes, leading to less inflammation and potentially slowing disease progression.
In clinical trials, brensocatib has shown significant promise in reducing the frequency of pulmonary exacerbations and slowing the decline in lung function for patients with bronchiectasis. This makes it an intriguing treatment option for individuals with Aspergillus-related diseases like chronic pulmonary aspergillosis (CPA), allergic bronchopulmonary aspergillosis (ABPA), and other forms of aspergillosis.
How Brensocatib May Benefit Aspergillosis Patients
1. Impact on Bronchiectasis in Aspergillosis
For many aspergillosis patients, bronchiectasis—a condition characterized by the permanent dilation of the bronchi—is a significant complication. In ABPA and CPA, Aspergillus infection contributes to chronic inflammation in the lungs, which can lead to bronchial damage and bronchiectasis. This increases the risk of frequent exacerbations and lung function decline.
Brensocatib works by reducing neutrophil-driven inflammation in the lungs, which could help prevent further lung damage and progression of bronchiectasis. By reducing inflammation and improving airway function, brensocatib may offer significant benefits for aspergillosis patients with bronchiectasis or chronic lung damage from fungal infections.
2. Reducing Pulmonary Exacerbations
One of the key benefits of brensocatib is its ability to reduce exacerbations, which are common in both ABPA and CPA. These flare-ups can lead to increased inflammation, infection, and lung tissue damage, further complicating the disease. The ASPEN trial (Phase 3 study) demonstrated that brensocatib significantly reduced the annualized rate of pulmonary exacerbations in patients with non-cystic fibrosis bronchiectasis. This benefit may extend to patients with aspergillosis, as frequent exacerbations can worsen lung function and overall health.
3. Slowing the Decline in Lung Function
Brensocatib also helps slow the decline in lung function, which is crucial for aspergillosis patients whose lung health may already be compromised by the infection. In chronic pulmonary aspergillosis (CPA), lung function decline can be progressive and irreversible without effective management. By reducing inflammation and exacerbations, brensocatib may help stabilize lung function and improve long-term outcomes for these patients.
4. Managing Chronic Inflammation in ABPA and CPA
Both ABPA and CPA are characterized by chronic inflammation in the airways. Brensocatib targets the underlying cause of much of this inflammation—neutrophil serine proteases—by inhibiting their activation. This could help reduce the chronic inflammation that causes damage to the airways and makes symptoms like cough, wheezing, and mucus production worse. For patients with aspergillosis and related respiratory complications, controlling this inflammation is key to managing symptoms and improving quality of life.
Clinical Evidence Supporting Brensocatib
The ASPEN trial, which included patients with bronchiectasis, demonstrated that brensocatib not only reduced exacerbations but also slowed the progression of lung function decline, as measured by forced expiratory volume in one second (FEV₁). Patients on brensocatib had a higher proportion of exacerbation-free days and better overall lung function than those on a placebo.
Although this trial did not focus solely on aspergillosis, its positive results suggest that brensocatib could be a valuable option for managing the lung damage and inflammation caused by Aspergillus infections, particularly in patients who have developed bronchiectasis as a result of the infection.
Safety and Side Effects
Like any medication, brensocatib can have side effects. The most common side effects observed in clinical trials included:
-
Hyperkeratosis (thickening of the skin)
-
Periodontal issues (such as gum inflammation)
-
Headache
-
Cough
-
Nasopharyngitis (inflammation of the nasal passages)
These side effects were generally mild to moderate. As brensocatib is still being evaluated for regulatory approval, ongoing monitoring and further clinical studies will help clarify its long-term safety profile.
Regulatory Status
Brensocatib has received FDA Priority Review for the treatment of non-cystic fibrosis bronchiectasis, and a decision is expected by August 12, 2025. If approved, it could become the first FDA-approved treatment for bronchiectasis and the first DPP-1 inhibitor for neutrophil-driven diseases. In the UK, Insmed, the manufacturer of brensocatib, has submitted a marketing authorization application to the MHRA. Pending approval, brensocatib could be available to patients in the UK by late 2025 or early 2026.
Conclusion
For aspergillosis patients, particularly those with bronchiectasis and chronic inflammation, brensocatib represents an exciting new treatment option. By targeting neutrophil-driven inflammation, reducing exacerbations, and slowing the decline in lung function, brensocatib offers hope for managing the long-term complications of Aspergillus infections. While it is still undergoing regulatory review, the clinical evidence supporting its efficacy suggests that it could become a valuable addition to the treatment arsenal for patients with aspergillosis.
🦠 Understanding Antibiotic Use in Aspergillosis: A Guide to Antimicrobial Stewardship (AMS)
This information is provided to help you understand your treatment. Always follow your medical team's advice. They will make the best decision for your care based on your individual health needs.
⚖️ What is Antimicrobial Stewardship (AMS)?
Antimicrobial stewardship means using antibiotics responsibly — only when needed, and choosing the most appropriate one for each infection. This helps protect patients from side effects and helps ensure antibiotics remain effective in the future.
For people with chronic lung conditions like chronic pulmonary aspergillosis (CPA), ABPA, or aspergillus bronchitis, this balance is especially important.
🔍 Why Is This Important for Aspergillosis Patients?
-
Antibiotics don’t work for fungal infections, but they may be prescribed if a bacterial infection is also present.
-
Using unnecessary antibiotics can lead to side effects, gut upset, or drug interactions (especially with antifungal medicines).
-
Overuse of broad-spectrum antibiotics can make future infections harder to treat.
Your clinical team carefully considers all of this when prescribing.
🔴 Broad-Spectrum Antibiotics
Broad-spectrum antibiotics target a wide range of bacteria, including helpful ones in your body. They are sometimes necessary, but their use is carefully monitored.
| Examples | Common Uses |
|---|---|
| Co-amoxiclav | Chest infections, dental issues |
| Ciprofloxacin, Levofloxacin | Serious or hospital infections |
| Doxycycline | Chest infections, acne |
| Azithromycin | Atypical pneumonia |
| Meropenem | Resistant or hospital-acquired infections |
🧠 These antibiotics may be used only if clearly needed. Doctors will often review and adjust the treatment after tests.
🟢 Narrow-Spectrum Antibiotics
These target specific bacteria and are usually first choice when the infection source is known.
| Examples | Common Uses |
|---|---|
| Penicillin V | Sore throats, dental infections |
| Flucloxacillin | Skin infections (e.g. infected eczema) |
| Nitrofurantoin | Urinary tract infections |
| Vancomycin (IV) | Resistant bacterial infections |
| Fosfomycin | Resistant urinary infections |
✅ These are often preferred because they reduce the risk of resistance and protect your body’s healthy bacteria.
🤝 What You Can Do
-
Trust your clinical team’s decisions — they are based on guidelines, test results, and your health history.
-
Tell your doctor or pharmacist about all medications you are taking — especially antifungals like itraconazole or voriconazole.
-
Report any side effects or concerns, especially if you notice gut problems or unexpected symptoms.
⚠️ A Note on Drug Interactions
Some antibiotics (like clarithromycin or rifampicin) can reduce how well azole antifungals work. Your doctor will avoid these combinations or adjust treatment accordingly.
✅ Final Reminder
This article is for general understanding only.
Your doctors are trained to choose the safest and most effective treatments for your condition. If you’re ever unsure about why a medication has been prescribed, ask — they’ll be happy to explain.