🌿 Will My Body Start Making Cortisol Again After Long-Term Prednisolone?
Many people with Allergic Bronchopulmonary Aspergillosis (ABPA) take prednisolone (a corticosteroid) for long periods to control inflammation and prevent flare-ups.
A common concern is whether the body will ever start producing its own natural steroid hormone, cortisol, again after so many years of treatment.
💡 Why Cortisol Matters
Cortisol is a vital hormone made by your adrenal glands.
It helps your body manage stress, maintain healthy blood pressure, control inflammation, and balance energy levels.
Your brain normally regulates this through the HPA axis (Hypothalamus–Pituitary–Adrenal axis).
When you take prednisolone, your body senses there’s already enough steroid circulating, so your brain switches off the signal that tells the adrenals to make cortisol.
Over time, the adrenal glands can “go to sleep”.
⏳ After Long-Term Prednisolone Use
If you’ve taken prednisolone for months or years, your adrenal glands may not restart immediately — and sometimes not completely.
Recovery depends on several factors:
| Factor | How It Affects Recovery |
|---|---|
| Length of treatment | The longer you’ve been on steroids, the slower recovery tends to be |
| Average daily dose | Higher doses suppress the adrenal glands more strongly |
| Tapering speed | A gradual, careful reduction helps the adrenals “wake up” again |
| Individual differences | Some people recover in months, others may need lifelong steroid replacement (hydrocortisone tablets) |
📅 What to Expect
-
After short courses (a few weeks), cortisol production usually returns quickly.
-
After many months or years, recovery can take months or even years.
-
Some people never regain full adrenal function and need lifelong replacement therapy.
Your specialist will usually assume your adrenal glands are suppressed until tests prove otherwise.
⚠️ Why Adrenal Suppression Is a Safety Concern
If your adrenal glands are not producing cortisol and you suddenly stop prednisolone, or become ill, have an accident, or need surgery, your body can’t produce the extra steroid it needs to handle stress.
This can cause a serious medical emergency called adrenal crisis, which may lead to low blood pressure, collapse, or shock if untreated.
That’s why it’s vital to:
-
Carry a Steroid Emergency Card or Medical Alert bracelet at all times
-
Tell healthcare staff (doctors, dentists, pharmacists, A&E teams) that you’re on or recently stopped steroids
-
Never miss a dose and never stop suddenly without medical advice
-
Use “stress-dose” steroids during illness, surgery, or injury as advised by your doctor
These simple precautions can be life-saving if your body can’t make enough cortisol during stress.
💨 What About Inhaled Steroids?
Many people with ABPA or asthma also use inhaled corticosteroids (such as fluticasone, budesonide, or beclometasone) in combination inhalers like Seretide, Symbicort, or Fostair.
These medicines mainly act in the lungs and only a small amount enters the bloodstream — but at high doses or with long-term use, they can still partly suppress the adrenal glands, especially when combined with oral steroids or certain antifungal medications.
Adrenal suppression is more likely if:
-
You use high-dose inhaled steroids for many months or years (e.g. fluticasone >500 µg/day)
-
You also take oral steroids (even at low doses)
-
You’re on antifungal medicines such as itraconazole, voriconazole, or posaconazole, which slow steroid breakdown
-
You are particularly sensitive to steroid effects
If suppression occurs, you might feel unusually tired, dizzy, or weak — especially when unwell or under stress.
Your doctor may test your morning cortisol or do a Synacthen test if there’s any concern.
In some cases, patients on high-dose inhaled therapy are also advised to carry a steroid card for safety, just like those on oral steroids.
The good news is that inhaled steroids are much safer than long-term oral prednisolone, and the risk of serious adrenal problems remains low when used correctly.
🧪 How Doctors Check for Recovery
Your respiratory or endocrine team may arrange:
-
Morning cortisol blood test (before your usual dose)
-
ACTH stimulation test (Synacthen test) – to see how well your adrenal glands respond
These tests help guide your doctors in determining whether your body is producing enough cortisol naturally or if you require a maintenance or replacement dose.
💊 Why Some Patients Move from Prednisolone to Hydrocortisone
If you’ve been on long-term prednisolone and your body is no longer making enough cortisol, your doctor may switch you to hydrocortisone.
Hydrocortisone is almost identical to the natural cortisol your body should produce.
| Feature | Prednisolone | Hydrocortisone |
|---|---|---|
| Strength | 4–5 times stronger than cortisol | Matches the body’s natural cortisol |
| Duration of action | Long-acting (12–36 hours) | Short-acting (6–8 hours) |
| Typical use | Controls inflammation during flares | Replaces missing cortisol when adrenals are suppressed |
Hydrocortisone is used as replacement therapy, not as an anti-inflammatory drug.
It’s given when your adrenal glands are “asleep” after long-term steroid use — or permanently if they no longer recover.
Doctors may switch to hydrocortisone if:
-
Tests show adrenal suppression (low morning cortisol or poor Synacthen test results)
-
You’ve finished tapering off prednisolone, but still feel unwell or fatigued
-
You have symptoms of adrenal insufficiency, such as dizziness, nausea, or low blood pressure
-
You need more precise stress dosing during illness or surgery
Hydrocortisone more closely mimics the body’s natural rhythm, usually taken two or three times a day, with an increased dose during illness or stress.
If you’re on hydrocortisone:
-
Carry a Steroid Emergency Card and make sure it’s visible to healthcare staff.
-
Never stop suddenly.
-
Increase (“double”) your dose when you’re ill or having surgery, as advised by your doctor.
-
Seek urgent medical help if you vomit and can’t keep tablets down — you may need an injection.
For many ABPA patients, hydrocortisone is temporary, helping to support the body until natural cortisol production recovers.
In others, especially after many years of prednisolone, it may become a lifelong replacement, which is safe and well managed under specialist supervision.
💉 The Future: Reducing Dependence on Prednisolone
The good news is that newer treatments called biologics are changing how ABPA is managed.
Biologics such as mepolizumab, benralizumab, dupilumab, and omalizumab target specific immune pathways involved in ABPA rather than suppressing the whole immune system.
For many patients, biologics:
-
Reduce or replace the need for long-term steroids
-
Lower the risk of adrenal suppression
-
Control symptoms more precisely, with fewer side effects
This means more people with ABPA may, in the future, safely taper off prednisolone and give their adrenal glands a chance to recover — always under close medical supervision.
🌤️ In Summary
After many years on prednisolone for ABPA, some people’s adrenal glands do recover, while others remain partially or fully dependent on replacement steroids.
Recovery is slow, varies between individuals, and must be guided by your specialist.
Be aware that both oral and inhaled steroids can suppress the adrenals if used long-term or at high doses.
Carrying a steroid emergency card and knowing what to do in an emergency is essential for safety — especially while your adrenals are still “waking up.”
With newer treatments like biologics and careful follow-up, the goal is to reduce steroid dependence and protect your long-term health.
🌬️ Inhaled Antifungal Treatments for Chronic Pulmonary Aspergillosis (CPA)
Updated: October 2025
💡 Why are inhaled antifungals being developed?
For people living with Chronic Pulmonary Aspergillosis (CPA), treatment usually involves long courses of oral antifungal tablets such as itraconazole, voriconazole, or posaconazole.
These medicines circulate through the whole body to reach the lungs — but sometimes they cause side-effects, interact with other drugs, or fail to reach high enough levels in thick mucus, cavities, or scarred areas of lung tissue.
Inhaled antifungal therapy aims to solve this problem by delivering medicine directly to the lungs using a nebuliser or inhaler device.
This can potentially mean:
-
✅ Higher drug levels exactly where infection is active
-
⚡ Faster local action
-
🚫 Fewer whole-body side-effects
-
🧩 Fewer drug interactions
This approach is especially promising for patients with localized lung disease, such as CPA or aspergillus bronchitis, where the fungus lives in damaged parts of the lung.
💊 Current inhaled antifungal options (used off-label)
🧪 Nebulised Amphotericin B
At the moment, nebulised amphotericin B is the only inhaled antifungal used in hospitals, although it is off-label for CPA.
It is more commonly used to prevent infection in people who have had a lung transplant or who are severely immunocompromised.
In some specialist centres, it may be used as maintenance therapy or an add-on for CPA if other antifungals have not worked or cannot be tolerated.
Advantages
-
High concentration in lung tissue
-
Minimal effects on other organs (especially the kidneys)
Drawbacks
-
Possible airway irritation (cough, tight chest, wheezing)
-
Requires specialist supervision and appropriate nebuliser equipment
🔬 New treatments in development
💨 Opelconazole (also called PC-945)
Opelconazole is a new inhaled triazole antifungal developed by Pulmocide Ltd in the UK.
It works in the same way as existing azole antifungals — by blocking the fungal enzyme CYP51 — but has been specially designed to stay in the lungs and minimise side-effects elsewhere.
In laboratory and early human studies, opelconazole has shown:
-
Strong activity against Aspergillus fumigatus
-
High and lasting drug levels in the lungs
-
Very low blood levels (reducing risk of toxicity and drug interactions)
-
Good tolerability in early trials
Although not yet licensed, it has been used compassionately in small numbers of patients with difficult-to-treat lung aspergillosis at centres such as Manchester and London.
🧾 Current and recent clinical trials
| Trial ID | Treatment | Condition | Purpose / Summary | Status |
|---|---|---|---|---|
| NCT06447402 | Nebulised Amphotericin B vs Saline | Chronic Pulmonary Aspergillosis | Tests whether regular nebulised amphotericin can help prevent CPA relapse compared with saline. | Recruiting |
| NCT03656081 | Itraconazole ± Nebulised Liposomal Amphotericin B | CPA | Compares oral itraconazole alone versus itraconazole plus inhaled amphotericin for symptom and scan improvement. | Completed – results pending |
| NCT05238116 | Inhaled Opelconazole + Standard Therapy | Refractory Invasive Pulmonary Aspergillosis | Phase 3 trial evaluating safety and added benefit of inhaled opelconazole. UK, EU, and US sites. | Recruiting |
| NCT05037851 | Inhaled Opelconazole (PC-945) | Post-Lung Transplant Prophylaxis | Assesses prevention of fungal infection after transplant. Found well tolerated. | Completed |
| PubMed 34058036 | Nebulised Amphotericin B vs Oral Itraconazole | Pulmonary Aspergilloma (CPA subset) | Six-month open study found similar improvement rates between inhaled amphotericin and oral itraconazole. | Completed |
👉 You can look up any of these studies on ClinicalTrials.gov by entering the trial ID (e.g. NCT06447402).
⚠️ Things to keep in mind
-
Not yet routine — Inhaled antifungals are available only in research or specialist centres.
-
Limited evidence — Most data come from transplant or invasive aspergillosis studies, not chronic infection.
-
Delivery challenges — Damaged or scarred areas of lung may be hard for inhaled drugs to reach.
-
Possible side-effects — Coughing or mild bronchospasm are common; pre-treatment with an inhaler may help.
-
Monitoring still needed — Even with inhaled therapy, your care team will continue to check symptoms, lung scans, and blood markers (such as Aspergillus IgG).
🧭 Questions to ask your specialist
If you are interested in this type of therapy, you could ask:
-
Does my centre offer nebulised amphotericin as part of CPA care?
-
Are there any clinical trials nearby (for example NCT06447402 or NCT05238116)?
-
Could an inhaled antifungal be used with my current oral treatment?
-
What are the side-effects and how are they monitored?
-
What nebuliser device is required and how often would I use it?
🏥 UK research centres involved
Current UK involvement is mainly through:
-
National Aspergillosis Centre, Wythenshawe Hospital (Manchester)
-
Royal Brompton and Harefield Hospitals (London)
-
UK transplant centres participating in Pulmocide’s opelconazole studies
🗝️ Key takeaway
Inhaled antifungal medicines are an exciting development that could make CPA treatment safer and more targeted in the future.
For now, they are mainly available through clinical trials or specialist centres, but the early results are promising — especially for those who have struggled with oral antifungal side-effects or limited success.
If you’re interested, speak to your CPA specialist or the National Aspergillosis Centre team about ongoing research and eligibility.
Damp, Mould and Health: Be Careful About Unvalidated Tests and “Detox” Treatments
Updated 2025 – by the NAC CARES team
When you’re desperate for answers
If you live in a damp or mouldy home and your health has suffered, it’s natural to want clear answers. Many people experience coughing, fatigue, sinus trouble or breathing problems and wonder if mould exposure could be the cause.
Unfortunately, the internet is full of misleading claims about “toxic mould”, “biotoxin illness”, or “mould detox”. Some websites and private clinics sell unvalidated medical tests or promote expensive supplements claiming to “flush mould toxins” or “reverse mould illness”.
People often turn to these options out of frustration and desperation when they feel ignored or dismissed by health or housing services. But it’s important to know that these tests and products are not scientifically proven — and in some cases, they may cause harm.
The truth about “mould illness” testing
At present, there is no validated medical test that can prove a person is ill because of mould exposure in their home.
Tests often sold online or through private clinics — such as urine mycotoxin tests, mould antibody panels, or chronic inflammatory response syndrome (CIRS) profiles — are not recognised by the NHS, NICE, or the World Health Organization.
These tests may detect trace amounts of mould-related compounds that appear even in healthy people. There are no agreed normal or abnormal levels, and results can vary dramatically between labs. This means a “positive” test result does not prove illness or guide treatment.
When functional, integrative, or alternative practitioners use these tests
It’s not just online sellers. Some functional medicine, integrative health, or alternative practitioners — including some with medical or allied health qualifications — also use these same mould or mycotoxin tests in private practice.
They may genuinely want to help and believe in “root cause medicine,” but:
-
Many of these tests have never been validated in peer-reviewed clinical studies.
-
Their results cannot reliably distinguish between normal environmental exposure to fungi and actual infection or allergy.
-
People are sometimes told they have “mould toxicity” or “mycotoxin poisoning” without any scientific evidence.
Why this matters
-
It can lead to unnecessary fear and anxiety.
-
Patients may spend hundreds or thousands of pounds on testing, supplements, or “detox” treatments that do not work.
-
Most importantly, genuine medical conditions — like aspergillosis, asthma, or COPD — may be diagnosed late or missed entirely.
Even if the practitioner sounds credible, unvalidated tests remain unvalidated.
If it isn’t approved by NICE, the NHS, or recognised respiratory specialists, it isn’t a reliable diagnostic test.
The risks of “detox” and self-treatment
Many websites and practitioners also recommend “detox” products such as activated charcoal, bentonite clay, chlorella, ozone therapy, or special anti-fungal diets. None of these have been proven to remove mould or mycotoxins from the body.
Some are unsafe or can interact dangerously with prescribed medicines — especially antifungal or steroid treatments used for aspergillosis. Others can damage the gut, lungs or kidneys.
No supplement, spray, or air treatment can replace medical therapy or proper repair of damp housing.
Why these products are still allowed to be sold
These tests and supplements often remain on sale because of regulatory loopholes:
-
They’re marketed as “wellness” or “informational” tests rather than diagnostic tools.
-
Supplements are classed as foods, not medicines — they must be safe, but not proven effective.
-
Many sellers are based overseas, outside UK or EU enforcement.
That’s why public awareness is crucial. Legal does not mean scientifically valid.
If you see misleading health claims, you can report them to:
What is proven to help
Here’s what current evidence supports:
-
Talk to your NHS doctor or respiratory specialist. They can arrange validated tests for fungal disease and lung health.
-
Fix the source of damp or mould. That’s the key to protecting your health — not detox kits.
-
Seek help early from housing officers, environmental health, or Citizens Advice if your home is unsafe.
-
Work with your care team — they can support housing letters or referrals if damp is affecting your condition.
See our practical guides:
If you feel dismissed or desperate
You’re not alone. Many people living in damp conditions feel frustrated and unheard. But unvalidated tests and detox programmes will not provide the answers you deserve.
You will get more meaningful, safer support through:
-
Your GP, respiratory or infectious disease team
-
Housing advocacy services and local councils
-
Peer support groups such as our Aspergillosis Patients & Carers Community
🛡️ Why We Take a Cautious Approach
Some people wonder whether organisations like ours are “allied to big pharma” or dismiss alternative approaches because of financial or legal pressures.
The truth is: we are cautious because of evidence and patient safety, not loyalty to industry.
-
We recommend only treatments or tests that are scientifically proven to be safe and effective.
-
NHS and charity organisations must follow regulatory standards and cannot endorse unvalidated products.
-
Our priority is protecting patients from harm, wasted resources, and delays in care.
Being cautious doesn’t mean rejecting innovation. If a new antifungal therapy, dietary approach, or environmental test is genuinely effective, it will be validated through peer-reviewed research — and we will share it.
Until then, our guidance focuses on evidence-based medicine and environmental interventions, because those are proven to help people with aspergillosis.
Key message
Damp and mould can make you unwell — but there is no quick test, no secret biomarker, and no miracle detox that can prove or cure it.
Stick with evidence-based medicine, protect your living environment, and seek support from trustworthy sources.
Save your money, protect your health, and trust science.
💚 Living With Aspergillus fumigatus and Starting Antifungal Treatment
Question: “I have Aspergillus fumigatus and I’d like to ask a few questions.
After starting antifungal treatment, how long did it take before you noticed improvement or a stop in the bleeding cough?
Has anyone reached a stable condition or full recovery?
Please share your experiences — it would really help to hear from you.” 💚
🌿 A Supportive Note
Many people ask this question when they first begin treatment — and it’s a very normal concern. Aspergillus fumigatus can cause a range of lung problems such as chronic pulmonary aspergillosis (CPA), aspergilloma, or Allergic Bronchopulmonary Aspergillosis (ABPA), and each responds differently to antifungal therapy.
Improvement can take time and patience.
Some notice changes within weeks, while for others, it can take several months before symptoms start to ease or stabilise.
💊 Understanding How Antifungal Treatment Works
Antifungal medicines — such as itraconazole, voriconazole, or posaconazole — don’t destroy Aspergillus overnight.
They work by slowing or stopping fungal growth, allowing the body’s immune system and lung healing processes to gradually take over.
Because these infections are often chronic, the goal is usually to:
-
Control symptoms
-
Prevent further damage
-
Reduce inflammation and flare-ups
-
Stabilise lung function
For most patients, this means aiming for long-term stability rather than complete eradication of the fungus.
⏳ How Long Before You Feel Better?
Every patient is different, but this is a general pattern doctors often see:
| Time after starting treatment | What you might notice |
|---|---|
| First few weeks | Some reduction in coughing or mucus; fewer night sweats; side effects settling as your body adjusts. |
| 1–3 months | Energy may start to improve; less coughing or blood in sputum; breathing slightly easier. |
| 3–6 months | Signs of stability — symptoms no longer worsening, CT scans showing improvement, or blood markers (e.g. Aspergillus IgG) falling. |
| 6–12 months | Some people achieve remission or long-term stability. For others, antifungal therapy continues as maintenance. |
If you have a fungal ball (aspergilloma), improvements are often slower, and sometimes bleeding episodes take longer to settle.
🩸 About Bleeding (Haemoptysis)
Coughing up blood can be one of the most distressing symptoms.
It usually improves once antifungals reduce inflammation, but if bleeding continues:
-
Doctors may prescribe tranexamic acid to help the blood clot more easily.
-
In some cases, embolisation (a targeted procedure to seal a bleeding blood vessel) may be needed.
-
Ongoing bleeding should always be reported — even small amounts — so your team can reassess treatment or check for infection changes.
🫁 Why “Stable” Can Be a Positive Outcome
Although “cure” is possible in some early or mild cases, most people live with aspergillosis as a chronic condition.
With consistent antifungal therapy, airway clearance, and monitoring, many reach a stable stage — where symptoms are minimal, life feels more predictable, and flare-ups are rare.
This stability is a real success.
It means your body and treatment are keeping the infection under control, preventing further lung damage.
💚 Real Experiences
Patients often describe:
-
Energy and breathlessness improving slowly
-
Bleeding stopping after several months
-
A new sense of normality once medication side effects settle
Some take antifungals for a set course (e.g. 6–12 months), while others remain on long-term maintenance to stay stable.
It’s common for treatment to be adjusted based on blood levels, side effects, or new sputum results.
💬 Patient Voices
Many people in our community say they wish they’d known:
-
“Improvement isn’t quick — it’s gradual, but it does come.”
-
“Side effects can be managed — don’t stop without advice.”
-
“It’s okay to ask your team what ‘stable’ looks like for you.”
-
“You’re not alone — others have been through this too.”
🧭 Looking After Yourself Along the Way
-
Keep up airway clearance (physiotherapy, saline nebulisers, or airway devices).
-
Attend regular clinic appointments for blood levels and liver tests.
-
Report side effects early — dose adjustments or switching antifungals often helps.
-
Maintain good nutrition and hydration.
-
Reach out for emotional support. Living with a chronic infection can be mentally exhausting; anxiety and fatigue are common.
💬 We’d Love to Hear From You
If you’ve been through antifungal treatment, please share your story:
-
How long it took before you felt a difference
-
What helped you most
-
How you manage side effects or flare-ups
Your experience could make a real difference to someone who’s just starting this journey. 💚
💨 Why Chest Infections Keep Coming Back — and What Can Help
Lisa asks:
“Hi, how do you get rid of chest infections? I had one, and the doctors gave me Clarithromycin. It didn’t clear, so they did a sputum test — it showed Haemophilus influenzae. Then I was given Co-trimoxazole, but that didn’t clear it either. The next test still showed it, so now I’m on Amoxicillin. Is this normal? I’m losing hope of it ever going away.”
💬 You’re Not Alone, Lisa
It’s very common for people with aspergillosis, bronchiectasis, or chronic lung disease to find that chest infections take a long time to clear.
Even with the right antibiotics, infections like Haemophilus influenzae can hang on for weeks or even months — but that doesn’t mean treatment isn’t working.
🦠 Why These Infections Keep Coming Back
-
Thick mucus and biofilms:
In damaged airways, bacteria can hide deep in sticky mucus or biofilms (protective layers). This makes them hard to reach, even with antibiotics. -
Narrow or scarred airways:
In bronchiectasis and aspergillosis, parts of the lung don’t drain properly, so infection pockets linger. -
Reinfection rather than relapse:
Sometimes, you clear one infection but pick up another of the same type from your own airways later. -
Inflammation:
Even when bacteria are gone, airway inflammation can cause ongoing cough and sputum, making it feel as if the infection hasn’t cleared.
💊 Why Doctors Change Antibiotics
Each antibiotic works in a different way.
Your team chooses them based on sputum culture results, which show which antibiotics your bacteria are sensitive to.
It’s quite normal to:
-
Start with a broad antibiotic (e.g. clarithromycin)
-
Switch after sputum results come back
-
Need longer or combination treatment if infection persists
For people with chronic lung conditions, antibiotic courses may last 2–3 weeks, not the usual 5–7 days.
💨 What Can Help You Recover
-
Regular airway clearance:
Using devices like an Acapella, Aerobika, or chest physiotherapy helps move mucus out of the lungs. This allows antibiotics to reach infection sites better. -
Stay hydrated to keep mucus thin.
-
Nebulised saline (if prescribed) can help loosen secretions.
-
Avoid skipping doses — consistent antibiotic levels help stop bacteria from regrowing.
-
Regular sputum tests guide your doctors in choosing the next best treatment.
-
See your specialist team if infections return frequently — they might check for fungal infection, resistant bacteria, or airway blockages.
❤️ The Take-Home Message
Yes — it’s quite normal for lung infections like Haemophilus influenzae to need several antibiotics and take time to clear when you have chronic lung disease.
It doesn’t mean your body isn’t fighting — it just means your lungs need a bit more help.
Keep in touch with your specialist nurse or clinic, and don’t lose hope — with good airway care, the right antibiotics, and patience, things usually improve.
🧬 The Story of Brensocatib: A New Way to Calm Lung Inflammation
What Is Brensocatib?
Brensocatib is a new type of anti-inflammatory medicine being developed to protect the lungs from long-term damage caused by overactive immune cells, especially neutrophils.
It is being tested by the company Insmed in people with bronchiectasis, but it may also help those with aspergillosis and other chronic lung diseases where inflammation is a major problem.
Brensocatib is taken as a once-daily tablet—not an injection.
Why Was It Developed?
In conditions like ABPA (Allergic Bronchopulmonary Aspergillosis) and CPA (Chronic Pulmonary Aspergillosis), inflammation is often persistent.
The lungs attract neutrophils, which are immune cells that normally destroy germs.
However, when too many neutrophils gather, they release enzymes that damage healthy lung tissue, thicken mucus, and make infection easier for fungi and bacteria.
Researchers realised that if they could turn down the destructive part of neutrophil activity—without turning off the immune system completely—they might be able to break the cycle of inflammation and infection.
How Brensocatib Works
Brensocatib blocks a switch inside the bone marrow called DPP1 (dipeptidyl peptidase-1).
DPP1’s job is to “activate” enzymes inside newly formed neutrophils before they enter the bloodstream.
By blocking DPP1, brensocatib stops neutrophils from producing harmful enzymes such as neutrophil elastase.
These neutrophils can still travel to the lungs and fight infection, but they cause less collateral damage.
👉 In short: brensocatib reduces lung injury caused by over-active immune cells, not by suppressing immunity itself.
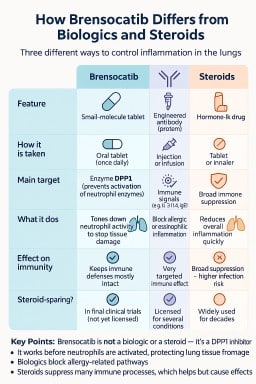
Not a Biologic – A Different Type of Treatment
It’s important to understand that brensocatib is not a biologic.
| Feature | Biologic drugs (e.g. mepolizumab, dupilumab) | Brensocatib |
|---|---|---|
| Made from | Complex proteins or antibodies | Small chemical molecule |
| How it’s given | Injection or infusion | Oral tablet |
| What it targets | Specific immune pathways (e.g. IL-5, IL-4) | Enzyme activation in neutrophils |
| Purpose | Block inflammatory signals | Reduce tissue-damaging enzymes |
| Typical use | Severe asthma, ABPA, autoimmune diseases | Bronchiectasis, chronic airway inflammation |
So, while biologics act by targeting immune messengers in the bloodstream, brensocatib works deeper—at the level of neutrophil development.
The two approaches are different but potentially complementary.
Some people in future may benefit from a combination, depending on their pattern of inflammation.
The Development Story
-
Early research (2010s): Scientists found that blocking DPP1 prevented lung injury in animal studies.
-
Insmed’s discovery: Brensocatib was developed as an oral, selective DPP1 inhibitor.
-
Phase 2 WILLOW trial (2020): In people with bronchiectasis, brensocatib significantly reduced flare-ups and lowered airway inflammation.
-
Phase 3 ASPEN trial (2022–2025): A large international study now nearing completion; results are expected soon.
If successful, brensocatib could become the first approved DPP1 inhibitor for long-term inflammatory lung disease.
Why This Matters for Aspergillosis Patients
People living with aspergillosis often also have bronchiectasis, where inflammation causes persistent mucus, infection, and breathlessness.
Current treatments such as steroids, antifungals, and biologics can help, but each has limits.
Brensocatib could:
-
Reduce airway inflammation without steroid side-effects
-
Protect lung tissue from further damage
-
Possibly lower the number of flare-ups or infections
-
Work safely alongside antifungals or biologics
It represents a new way of calming inflammation—by modifying neutrophil behaviour rather than blocking the immune system.
What Happens Next
The ASPEN Phase 3 results are expected soon. If positive, Insmed plans to apply for approval in the UK, EU, and USA.
Researchers are also studying brensocatib in:
-
COPD (Chronic Obstructive Pulmonary Disease)
-
Cystic fibrosis
-
Nontuberculous mycobacterial (NTM) infections
If licensed, it could mark the first new oral anti-inflammatory class for chronic lung disease in decades.
Key Take-Home Messages
-
Brensocatib reduces harmful lung inflammation by blocking the enzyme DPP1.
-
It is a small-molecule tablet, not a biologic injection.
-
It aims to protect the lungs by preventing damage from overactive neutrophils.
-
It may offer a steroid-sparing option for chronic airway diseases like bronchiectasis and aspergillosis.
-
It’s currently in final clinical trials, with results expected soon.
💬 Find Out More
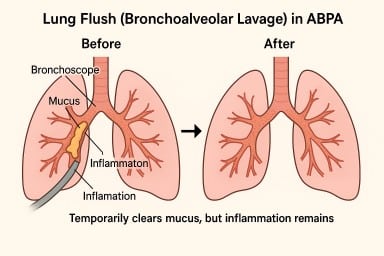
🫁 “Lung Flush” (Bronchoalveolar Lavage) in ABPA – What It Is and Why It Brings Only Short-Term Relief
A lung flush (also called a bronchoalveolar lavage, or BAL) isn’t a regular treatment for Allergic Bronchopulmonary Aspergillosis (ABPA), but it’s sometimes used selectively in NHS hospitals.
💧 What Happens During a Lung Flush
It’s done during a bronchoscopy, where a thin, flexible tube is passed through the nose or mouth into the lungs.
A small amount of sterile saline is washed into part of the lung and then gently suctioned back out.
The fluid is tested for:
-
Aspergillus growth or DNA
-
Other infections (bacteria, fungi, viruses)
-
Signs of inflammation or allergic activity
You’re given local anaesthetic and light sedation, so you stay comfortable but sleepy. Most people go home the same day.
🧪 Main Purpose – Diagnosis
In most ABPA cases, a lavage is done to find out what’s causing symptoms – whether they’re due to Aspergillus, another infection, or ongoing inflammation.
The results help doctors fine-tune treatment, such as adjusting antifungal doses or deciding if a biologic drug might help.
🫁 Sometimes Used to Clear Mucus
In certain situations – especially when thick mucus plugs are blocking airways or causing part of a lung to collapse – doctors may use lavage as a therapeutic “flush.”
This can wash out sticky secretions and temporarily improve airflow, helping physiotherapy and medication work more effectively.
It’s usually a short, day-case procedure, and most people feel back to normal after a day or two.
⚠️ Why It’s Only Short-Term Relief
Although lavage can clear mucus, ABPA is caused by an allergic immune reaction, not by the mucus itself.
Unless that reaction is controlled with:
-
Corticosteroids (to reduce inflammation),
-
Antifungal drugs (to lower the fungal load), or
-
Biologic injections (to block allergy pathways),
…the lungs will continue to produce thick, sticky mucus, which can re-accumulate within days or weeks.
So while a “lung flush” can make breathing easier in the short term, the effect is temporary – like clearing a blocked drain while the tap is still running.
⚠️ Risks and After-Effects
A bronchoscopy with lavage is generally safe, but it is still an invasive procedure. Possible effects include:
-
Temporary sore throat, cough, or hoarseness (common)
-
Mild bleeding or streaks of blood in sputum for a short time
-
Low oxygen levels during or after the procedure (monitored carefully)
-
Chest tightness, infection, or fever – uncommon but possible
-
Bronchospasm (airway narrowing) in people with very sensitive lungs, which is why it’s done in a hospital with respiratory support available
Because of these small but real risks, the NHS uses lavage only when the benefits outweigh the downsides – for example, when mucus is causing serious blockage or when test results will change management.
💬 In Summary
A “lung flush” can temporarily clear mucus and ease breathing, but it doesn’t stop ABPA’s underlying allergic inflammation.
The mucus often returns unless that inflammation is brought under control with long-term medical treatment.
It’s a useful tool when needed, but not something done regularly or lightly.
💬 Healthwatch: Your Local Voice in the NHS
Living with a long-term lung condition such as aspergillosis, asthma, or bronchiectasis often means regular contact with hospitals, GPs, and community clinics.
Sometimes things work well — and sometimes they don’t.
That’s where Healthwatch comes in.
Healthwatch is an independent organisation that represents patients and the public.
It exists to make sure your experiences help shape the way NHS and social-care services are delivered.
🏛️ What is Healthwatch?
Healthwatch was set up by law to be the official voice of patients and the public in health and social care.
There are two levels:
-
Healthwatch England – works nationally to influence NHS and government policy
-
Local Healthwatch – works in every local authority area across England, gathering feedback from people using local services
Healthwatch is not part of the NHS, and it’s not a complaints service, but it does have statutory powers to:
-
Listen to people’s experiences of care
-
Report issues and make recommendations to the NHS, local councils, and care providers
-
Request responses from organisations it investigates
-
Escalate serious concerns to the Care Quality Commission (CQC)
Learn more on the Healthwatch website.
🌿 Why Healthwatch matters to aspergillosis patients
People living with chronic lung disease often face delays, limited understanding, or difficulties accessing ongoing support.
Healthwatch helps make sure those experiences aren’t ignored.
1. Raising the patient voice
You can share your experience of healthcare — good or bad — with your local Healthwatch.
They collect stories from across the community and use them to:
-
Identify patterns (for example, problems with accessing respiratory clinics or antifungal monitoring)
-
Produce reports and recommendations for local NHS decision-makers
-
Push for improvements to long-term care pathways and community support
2. Helping to improve new neighbourhood health hubs
As NHS care moves into the community, Healthwatch plays a key role in making sure new Neighbourhood Health Hubs are:
-
Accessible for people with limited mobility or oxygen needs
-
Located where public transport and parking work for patients
-
Designed with chronic-illness patients in mind, not just short-term care
You can feed in your ideas through Healthwatch about what’s working and what isn’t in new NHS community models.
3. Providing information and signposting
If you’re unsure where to go for care — GP, hospital, or new health hub — or how to complain or appeal a service decision, Healthwatch can point you in the right direction.
They offer clear, local information about:
-
NHS patient transport
-
The Healthcare Travel Costs Scheme (HTCS)
-
Local support groups and community services
4. Supporting patient involvement
Healthwatch works with NHS organisations to include patients and carers in planning and reviewing services.
If you’d like to get involved as a patient representative or share your experience of aspergillosis services, Healthwatch can help you join local working groups or consultations.
5. Spotlighting inequalities
Healthwatch highlights where certain groups are left behind — for example:
-
People with rare or complex conditions
-
Patients in rural or deprived areas
-
Those unable to use digital appointment systems
This helps ensure people with chronic lung conditions are not overlooked when new community-care models are designed.
⚖️ What Healthwatch can — and can’t — do
| ✅ Healthwatch can | 🚫 Healthwatch can’t |
|---|---|
| Collect and report your experience to NHS leaders | Fix individual clinical problems directly |
| Influence NHS and council decisions | Guarantee faster treatment or appointments |
| Provide advice on local services and support | Replace legal or complaints services |
| Escalate major safety concerns to the CQC | Act as your personal advocate in disputes |
Even so, their influence can be powerful — many improvements in NHS access and transport have started with patient stories collected by Healthwatch.
📍 How to contact your local Healthwatch
Every local area has its own Healthwatch website and phone number.
You can find yours at:
👉 Find your local Healthwatch
When you contact them, you can:
-
Fill in a short online form to share your story
-
Ask to join a focus group or consultation
-
Request accessible information or help finding services
-
Subscribe to local updates and reports
If you’d like support from the aspergillosis community, NAC CARES can also help you write or submit your feedback.
💬 Why this matters
“Nothing about us without us.”
Healthwatch exists so that patients — including those with rare and chronic conditions like aspergillosis — can make their experiences count.
By telling your story and feeding back to Healthwatch, you help shape better care for yourself and for others who will face similar challenges in future.
🏥 NHS Neighbourhood Health Hubs: How Community Care Will Work for People with Aspergillosis and Asthma
The NHS is changing how healthcare is delivered — with more care moving closer to home and fewer hospital visits.
A new model called Neighbourhood Health Services (or Neighbourhood Health Hubs) is being rolled out across England from late 2025, and it could make a real difference for people living with aspergillosis, asthma, bronchiectasis, and other long-term respiratory conditions.
🌍 Why care is moving into the community
The goal is to:
-
Bring care to where people live, not just in large hospitals
-
Reduce waiting times by shifting routine tests and reviews out of hospital clinics
-
Join up GPs, nurses, pharmacists, and hospital specialists into one local team
-
Focus on prevention, self-management, and early support
These reforms come from the government’s Healthcare on Your Doorstep announcement (September 2025), supported initially by £10 million across 43 pilot areas in England.
🧑⚕️ What a “Neighbourhood Health Hub” looks like
A one-stop local health centre bringing together:
-
GPs and practice nurses
-
Respiratory nurses, physiotherapists, and pharmacists
-
Mental-health and wellbeing workers
-
Dietitians, occupational therapists, and social-prescribing link staff
-
Voluntary and community organisations (e.g. NAC CARES, Asthma + Lung UK)
Some hubs will connect directly to Community Diagnostic Centres (CDCs) – local sites providing CT, MRI, X-ray, lung-function and blood tests through the NHS England diagnostics programme.
The aim is for one joined-up team to share your records and plan your care locally.
🩺 How hubs work with your GP and A&E
The new hubs are designed to fill the gap between GP surgeries and hospitals – giving extra support when you’re too unwell to manage alone but don’t need emergency care.
Home → GP Practice → Neighbourhood Health Hub → Hospital / A&E
🏠 Your GP surgery
You’ll stay registered with your usual GP. They remain in charge of your prescriptions, results, and overall care.
Your GP can now refer you to a Neighbourhood Health Hub for things that need a wider team – for example:
-
Antifungal monitoring or blood tests
-
Lung-function or CT scans
-
Flare-up review by respiratory nurses
-
Fatigue or wellbeing support
🧑⚕️ The Neighbourhood Health Hub
You might go here instead of hospital for:
-
Same-day assessment of an infection or flare-up
-
Bloods, ECGs, or scans ordered by your GP
-
Physiotherapy, airway-clearance or rehabilitation
-
Medication reviews with a pharmacist
-
Appointments with dietitians or mental-health staff
-
Practical help from link workers (see below)
🚨 A&E (Emergency Department)
Still essential for serious problems such as:
-
Sudden or severe breathlessness not relieved by treatment
-
Coughing up blood
-
Chest pain, fainting, or collapse
-
High fever with confusion
If unsure, call NHS 111 or 999 in an emergency.
🔁 When to use which service
| Situation | Who decides | Where you’ll be seen |
|---|---|---|
| Routine check-up or repeat prescription | You / GP | GP surgery |
| Specialist review or complex medication | GP / consultant | Neighbourhood Hub |
| Mild flare-up needing same-day care | NHS 111 / GP | Hub or GP |
| Emergency or life-threatening symptoms | NHS 111 / 999 | A&E / hospital |
| Diagnostic tests | GP / hospital referral | Community Diagnostic Centre |
All sites will share your digital care record so results and updates reach your GP and hospital team automatically.
🧑🤝🧑 Link workers and care coordinators – local help through your GP
Every GP practice and neighbourhood team now has link workers (also called care coordinators or social prescribers).
They’re there to help you navigate healthcare and community support. They can:
-
Arrange or advise on transport for appointments
-
Help complete travel cost reimbursement or benefit forms
-
Connect you with volunteer driver schemes or local charities
-
Find exercise, wellbeing, or peer-support groups
-
Support with fatigue, isolation, or anxiety
Ask your GP reception or Neighbourhood Hub to refer you to the link worker, or request a call-back via the NHS App.
🚗 Transport and accessibility
🚐 NHS Patient Transport Service (PTS)
If you can’t use public transport for medical reasons (for example, oxygen use, mobility difficulties, or severe fatigue), you may qualify for free NHS transport.
Your GP, link worker, or hospital can book this for you through the regional PTS (for example, NWAS in the North West).
💷 Healthcare Travel Costs Scheme (HTCS)
If you’re on a low income or certain benefits, you can reclaim travel expenses under the HTCS.
Bring your appointment letter and proof of eligibility, or ask your link worker to help with the form.
🚙 Community & volunteer transport
Each Integrated Care System (ICS) works with local councils and charities such as Age UK, Mind, or Good Neighbour schemes to run community minibuses and volunteer driver services.
Ask your link worker or hub team for local options.
🅿️ Accessibility
All new and refurbished hubs must include:
-
Blue Badge parking and drop-off zones
-
Wheelchair-friendly entrances and toilets
-
Seating and oxygen-safe waiting areas
-
Negotiated free or reduced parking in shared sites
🧭 At a glance
| Issue | What’s planned | What to do now |
|---|---|---|
| Public transport | Sites chosen to be local, but not always central | Check routes before your visit |
| NHS Patient Transport | Still available for medical need | Ask GP or link worker to book |
| Travel-cost reimbursement | Continue via HTCS | Keep proof of benefit |
| Community / volunteer drivers | Expanding under ICB–VCS partnerships | Request info via link worker |
| Disabled parking / drop-off | Required at new sites | Confirm when booking |
🪶 A message from the aspergillosis community
For many people with lung disease, “local care” only works if it’s accessible care.
Groups such as NAC CARES, Asthma + Lung UK, and Healthwatch are urging NHS leaders to:
-
Design transport and parking into every new site
-
Ask about mobility and oxygen needs when booking
-
Fund local volunteer schemes
-
Provide dedicated link workers at every hub and GP practice
If you struggle to reach appointments, tell your clinic or Healthwatch — your feedback shapes how services develop.
🧾 Questions to ask before your first visit
-
🚗 Is there Blue Badge or patient parking on site?
-
🚌 What public-transport links serve the hub?
-
🚐 Can the clinic arrange NHS Patient Transport?
-
💷 Can I claim travel costs under the HTCS scheme?
-
♿ Is the building accessible for wheelchairs or oxygen users?
-
💨 Are there rest areas for people who get breathless?
-
🧑🤝🧑 Can my carer or partner attend with me?
-
👩💼 Is there a link worker who can help with transport or forms?
-
🕓 Are there quiet waiting spaces to reduce infection risk?
Having these answers before your appointment makes your visit smoother and safer.
💬 Final thought
“Neighbourhood care” isn’t about replacing your GP or A&E — it’s about bridging the gap.
The new hubs aim to bring together your GP, hospital specialists, and community teams in one local setting, providing earlier help, fewer hospital journeys, and care designed around your life, not your postcode.
🔎 Behind the Headlines: Is this an NHS Expansion or a Shift?
Many people wonder whether this is new investment or a reshuffle of existing NHS services.
🧱 What’s really happening
-
The Neighbourhood Health Service is not a new tier of the NHS, but a redesign of how GP, hospital, and community teams work together.
-
The focus is on moving care out of hospitals and into local clinics, using the same staff and budgets more effectively.
-
Hospitals will still handle emergencies and complex cases, but routine tests, reviews, and education will move into the hubs.
⚖️ Expansion or movement?
| Area | Expansion | Reorganisation |
|---|---|---|
| Buildings | Some new or refurbished hubs and diagnostics centres | Many reusing existing GP or community facilities |
| Staffing | Some new link workers, pharmacists, and AHPs | Most existing NHS staff redeployed across neighbourhoods |
| Funding | £10m pilot investment + diagnostic capital | No major long-term new funding yet announced |
| Patient benefit | Easier access, joined-up records | May reduce hospital appointments rather than add capacity |
💬 What this means
For patients, it should feel like an expansion — more care, closer to home —
but in reality it’s a shift of where and how NHS services are delivered, not a large-scale increase in total NHS resources.
⚠️ Risks and opportunities
| Opportunities | Risks |
|---|---|
| Easier local access | Risk of hospital clinics closing before hubs fully staffed |
| Joined-up records | Depends on IT integration |
| Focus on prevention | May feel like hospital services are being reduced |
| Better continuity | Needs clear accountability (GP vs hub) |
🧩 Summary
The new neighbourhood model is a reorganisation within the NHS, not a separate expansion.
It aims to use existing staff, buildings, and budgets more efficiently — giving patients with chronic conditions like aspergillosis and asthma easier access to care and support in their own communities.
🌦️ Understanding Corticosteroid Mood Swings
Alison shared something that will resonate with many of us:
“Recognising that prednisone mood swings are very unpredictable is a good reminder as I feel like I am up and down so much of late. Yesterday’s swap to half hydrocortisone and half prednisone probably took a bit of adjusting too. Better day today though — I even got out to pick up my campervan that had been in for service. Felt really good to be driving it again and as the weather improves, I live in hope that I might get to use it this year!” 😊🤔
💭 Why mood can change on corticosteroids
Steroid medicines such as prednisone, prednisolone, and hydrocortisone affect many systems in the body — including brain chemistry.
When levels go up or down (for example when changing dose or type), it’s common to feel:
-
Irritable or anxious one day, low or tired the next
-
More emotional than usual — tears or frustration come quickly
-
Sleep disturbance, vivid dreams, or early waking
-
Short bursts of energy or restlessness, followed by a “crash”
These changes don’t mean you’re “losing control” — they reflect how sensitive the brain is to shifts in cortisol, the hormone steroids replace or supplement.
⚖️ Why switching between steroids can feel bumpy
Prednisone and hydrocortisone are both corticosteroids but have different potencies and timings:
| Steroid | Approx. equivalent dose (anti-inflammatory) | Typical duration of action |
|---|---|---|
| Hydrocortisone | 20 mg ≈ 5 mg prednisolone | Short-acting (6–8 hours) |
| Prednisone/Prednisolone | 5 mg | Longer-acting (12–36 hours) |
When switching or mixing them, the body’s rhythm of cortisol can temporarily feel off — like jet lag for your stress hormones. It often settles after a few days.
🌞 Tips that may help
-
Keep a simple mood or energy diary — it helps you and your clinician see patterns.
-
Take doses at consistent times, usually in the morning, unless advised otherwise.
-
Build in gentle activity or time outdoors — small wins, like Alison’s campervan trip, really lift mood.
-
Avoid caffeine or alcohol spikes if feeling restless or irritable.
-
Tell your clinician if mood swings are severe or prolonged — dose adjustment or slower tapering may help.
💬 In Alison’s words
“Better day today.”
Sometimes that’s the victory — one step, one better day, one bit of normality returning.