🧠 Struggling to Come Off Prednisolone?
A Guide for Patients with Long-Term Steroid Use (e.g. for ABPA)
If you’ve been on prednisolone or methylprednisolone for a long time — such as for Allergic Bronchopulmonary Aspergillosis (ABPA) — and now feel dreadful while trying to reduce your dose, you’re not alone.
Many people find steroid tapering one of the most difficult parts of treatment. This guide explains what’s happening in your body, why withdrawal symptoms occur, how hydrocortisone may help, and when to pause tapering and seek help.
💡 Why Were You Put on Prednisolone?
Prednisolone is a powerful anti-inflammatory steroid used to control conditions like ABPA. It mimics cortisol, a natural hormone your body produces to:
-
Control inflammation
-
Manage blood sugar, blood pressure, and fluid balance
-
Respond to physical and emotional stress
But after several weeks of steroids, your body stops making cortisol naturally, which leads to dependence and can make tapering very difficult.
🔁 Why Is It So Hard to Come Off Prednisolone?
As you taper:
-
Your dose of artificial cortisol (prednisolone) is reduced
-
But your adrenal glands may not have restarted cortisol production yet
-
This leaves you in a cortisol gap, with symptoms of withdrawal and adrenal insufficiency
😞 Common Symptoms of Cortisol Withdrawal
-
Crippling fatigue or exhaustion
-
Nausea, loss of appetite
-
Light-headedness or dizziness
-
Joint or muscle aches
-
Anxiety, low mood, brain fog
-
Feeling worse in the afternoon (the “crash”)
These symptoms are real and happen because your body is running on too little cortisol.
🛑 Never Taper Without Medical Supervision
Always reduce steroids under a doctor's care. Stopping or tapering too quickly can lead to:
-
Adrenal insufficiency
-
Severe fatigue or collapse
-
Adrenal crisis — a life-threatening emergency
🧪 What Happens to Natural Cortisol?
Your body expects cortisol to rise in the morning and fall by night. Long-term steroids stop this rhythm. As you taper lower (especially <5 mg prednisolone), the brain begins sending signals to “wake up” the adrenal glands — but it takes time.
Doctors monitor recovery using:
-
Morning cortisol tests (8–9am, off steroids for 24 hrs)
-
Synacthen (ACTH stimulation) tests to assess adrenal response
⏱️ Why You Feel Worse Later in the Day
Many people report feeling okay in the morning after their steroid dose, but hit a wall in the afternoon. That’s because:
-
Prednisolone’s effects wear off by then
-
Your body expects a “natural top-up” of cortisol — but it’s not there yet
-
This is often when your brain starts pushing the adrenal glands to restart
So while it feels awful, this may be the point at which your system is trying to recover.
🟡 When to Talk to Your Doctor About Pausing the Taper
If you feel dreadful every day, and your symptoms aren’t improving after 1–2 weeks at a new dose, that’s a sign your body may not be coping.
👉 Tell your doctor if:
-
You can barely get through the day
-
You feel consistently dizzy, nauseated, weak, or mentally “foggy”
-
You are experiencing daily crashes or worsening anxiety
-
You have lost weight, appetite, or sleep due to symptoms
You may need to:
-
Pause the taper and hold your dose longer
-
Increase slightly for symptom control
-
Switch to hydrocortisone for gentler tapering
-
Get retested to see if your adrenal glands are recovering
🗣️ “I think my body is struggling at this dose. Can we pause here and check my cortisol levels?”
🗣️ “Would hydrocortisone be a better option for tapering now?”
These are reasonable, safe, and important questions to ask.
🔄 Could Switching to Hydrocortisone Help?
Yes — hydrocortisone is a short-acting, natural steroid that:
-
Mimics your body’s own cortisol
-
Allows windows for adrenal recovery
-
Is easier to taper in smaller steps
Many people report fewer withdrawal symptoms and a smoother taper after switching from prednisolone.
📈 Prednisolone vs. Hydrocortisone
| Feature | Prednisolone | Hydrocortisone |
|---|---|---|
| Potency | ~4x stronger than cortisol | Equal to cortisol |
| Duration | 12–36 hours | 6–8 hours |
| Suppression risk | High | Lower |
| Recovery support | Slower | Better for adrenal recovery |
| Tapering flexibility | Hard below 5 mg | Easier to reduce gradually |
🛡️ Safety Rules During Tapering
✅ Always taper slowly and with medical guidance
✅ Know your “sick day rules”
During illness, surgery, or stress, you may need higher steroid doses (stress dosing). Ask your doctor for a written plan.
✅ Watch for adrenal crisis:
Seek emergency care if you have:
-
Vomiting or severe nausea
-
Fainting or confusion
-
Collapse, very low blood pressure
-
High fever with fatigue and weakness
✅ Carry a Steroid Emergency Card and/or medical alert ID
-
Especially important if you’re tapering or still on steroids
-
This alerts emergency staff that you may need urgent steroids
🫶 Reassurance
If tapering is making you feel broken — you’re not alone, and you’re not failing. Tapering is about timing, safety, and support. Your adrenal recovery is a process — not a race.
Many people:
-
Recover natural cortisol over months (or longer)
-
Manage long-term steroid replacement safely
-
Return to full lives with the right plan
📋 What You Can Do Next
🗣️ Ask your doctor:
-
“Should we pause tapering and hold my current dose?”
-
“Can we test my morning cortisol or do a Synacthen test?”
-
“Would switching to hydrocortisone help?”
-
“Can I get a steroid emergency card and sick-day instructions?”
🧪 Antibiotics, Fungal Risk, and ABPA: What Patients Need to Know
If you live with Allergic Bronchopulmonary Aspergillosis (ABPA) or another form of aspergillosis, you may be prescribed a range of treatments — including steroids, biologics, and sometimes antibiotics to prevent infections.
But how do these medications interact with each other? Could antibiotics make fungal conditions worse? And when should you use them?
This guide explains how different specialists, especially Infectious Diseases (ID) consultants, approach these questions, and what patients should know when balancing treatments for infections, inflammation, and immunity.
💊 What Are Prophylactic Antibiotics and Why Are They Used?
“Prophylactic” antibiotics are low-dose medications taken regularly to prevent infections, rather than to treat a current one. You may be prescribed them if you:
-
Have frequent chest infections due to asthma, bronchiectasis, or ABPA
-
Are prone to urinary tract infections (UTIs), especially in winter
-
Use long-term steroids, which can reduce your ability to fight bacterial infections
Examples include TRISOL (trimethoprim), azithromycin, or doxycycline.
🦠 Can Antibiotics Make Fungal Problems Worse?
Yes — especially with long-term use. Here's why:
-
Antibiotics disrupt the natural balance of bacteria in the body
-
This allows fungi like Aspergillus (or sometimes Candida) to multiply more easily
-
The risk is higher in people taking steroids, biologics, or who already have fungal colonisation or sensitisation
So while antibiotics may prevent bacterial infections, they can increase the risk of fungal flare-ups — especially in the lungs.
🧠 What Do Infectious Diseases (ID) Specialists Consider?
If you're being seen by an ID team (such as at a specialist aspergillosis clinic), they will carefully assess the balance between preventing bacterial infections and not encouraging fungal overgrowth.
ID specialists tend to:
-
Avoid long-term antibiotics unless absolutely necessary
-
Pause antibiotics to allow accurate cultures to be taken
-
Work with Respiratory and Urology teams to manage infections and inflammation together
-
Consider non-antibiotic options for UTI prevention, such as:
-
Good hydration
-
Methenamine hippurate (Hiprex)
-
Vaginal oestrogen (in post-menopausal women)
-
🧯 What About Steroids and Biologics?
-
Steroids (like prednisolone) are important in controlling allergic inflammation in ABPA
-
But they also suppress the immune system
-
And raise blood sugar, which can fuel fungal growth
-
-
Biologics (like omalizumab or dupilumab) are more targeted
-
They may allow you to use fewer steroids
-
But they still modulate the immune system, so infection risk must be monitored
-
When using steroids or biologics, ID teams may recommend:
-
Close monitoring of fungal markers (e.g. IgE, Aspergillus PCR, sputum culture)
-
Antifungal therapy alongside other treatments if needed
-
Avoiding unnecessary antibiotics to keep fungal balance under control
✅ When Might It Be Safe to Stop Prophylactic Antibiotics?
If you're on long-term antibiotics for UTIs or chest infections, and your infection rate has dropped, it may be safe to pause prophylaxis. This is more likely if:
-
Recent infections have been mild or infrequent
-
Your Urology or Respiratory team agrees
-
Cultures are negative, and symptoms are stable
-
You have access to fast, “test and treat” options if a new infection occurs
In some cases, your doctor may stop antibiotics so blood and urine cultures can be taken without interference — to ensure any future treatment is accurate and appropriate.
🧾 Key Takeaways
| Situation | What to Consider |
|---|---|
| You’ve been on TRISOL or another antibiotic | Reassess whether infections are still frequent/severe enough to justify it |
| You’re starting steroids or biologics | Watch for fungal flare-ups — you may need antifungal support |
| You’ve been told to stop antibiotics temporarily | This may be to allow clear diagnosis (cultures, IgE, sputum tests) |
| You’re not sure what to do next | Ask for your care to be coordinated between ID, Urology, and Respiratory teams |
🩺 A Word on Coordination
If multiple specialists are involved in your care (e.g. GP, Urology, Infectious Diseases, Respiratory), it's important they communicate clearly. You may want to ask:
-
“Can you confirm this plan with my other specialists?”
-
“Do I need a fungal check-up before restarting antibiotics?”
-
“Could we use a non-antibiotic prevention strategy instead?”
This will help avoid overlapping risks, conflicting advice, or missed infections.
🗣️ Final Thought
In ABPA and other fungal conditions, it's not a matter of choosing between bacteria or fungi — it's about managing both carefully.
Antibiotics, steroids, and biologics all have a role — but they need to be used in balance, with infection risk, fungal exposure, and immune suppression monitored as a whole.
Understanding the Side Effects of Long-Term Prednisolone Use
Prednisolone is a widely used and effective medication for managing inflammation in aspergillosis. However, when taken for more than 3–4 weeks—especially at moderate or high doses—it can cause unwanted effects in different parts of the body. Knowing what to expect and how to reduce risks can help you feel more in control of your treatment.
Prednisolone is a synthetic form of cortisol, a hormone your body normally produces to manage stress and inflammation. When you take it in larger-than-natural amounts over time, it can interfere with how your body handles fluids, sugar, bone rebuilding, immune function, and even mood and sleep.
Below are the most common side effects and why they happen:
Common Side Effects and Why They Happen
Prednisolone mimics cortisol, a hormone naturally made by your body. But when taken in higher-than-natural amounts over a long time, it can disrupt many systems. Here's why these side effects happen:
- Weight gain and fluid retention – Steroids affect how your body processes salt and water, leading to bloating and weight changes.
- Moon face – Fat redistributes to the face, neck, and abdomen.
- Thinning skin and bruising – Steroids reduce collagen production, making skin fragile.
- High blood pressure – Caused by fluid retention and effects on blood vessel tone.
- Increased risk of infections – Steroids suppress your immune system, making it harder to fight infections.
- Osteoporosis – Steroids interfere with calcium absorption and bone rebuilding.
- Muscle weakness – Corticosteroids break down protein, reducing muscle strength, especially in the thighs and upper arms.
- Mood and sleep changes – Steroids can affect the brain’s chemistry, causing anxiety, insomnia, or mood swings.
- Eye problems – Long-term use can raise pressure in the eyes or cloud the lens (cataracts).
- High blood sugar or diabetes – Steroids make it harder for your body to use insulin effectively. **
What You Can Do to Minimise Side Effects
Managing steroid side effects involves a combination of lifestyle choices and medical support:
| Strategy | Why It Helps |
| Use the lowest effective dose | Reduces cumulative exposure to steroid side effects |
| Switch to hydrocortisone when appropriate | Mimics natural cortisol and is better tolerated long term |
| Monitor blood pressure, bone health, and blood sugar | Early detection helps prevent complications |
| Take calcium, vitamin D, and possibly bone-strengthening medications | Supports healthy bones |
| Exercise regularly | Maintains strength, mobility, and mood |
| Eat a balanced diet low in salt and sugar | Helps manage weight, BP, and blood sugar |
| Keep up with regular medical reviews | Ensures your treatment is safe and effective |
Trusted Resources and Support
You're not alone in managing steroid side effects. These resources offer guidance and community support:
- NHS Steroid Safety Advice: Side effects of prednisolone tablets and liquid - NHS
- Downloadable Steroid Emergency Card: endocrinology.org/adrenal-crisis
- National Aspergillosis Centre resources: aspergillosis.org
- Aspergillosis Trust and NAC patient forum
- Your pharmacist or GP for medication support
- Endocrine nurses for adrenal insufficiency care
Taking charge of your health with the support of your care team can greatly reduce the risks of long-term steroid use.
How to Lessen the Impact of Side Effects
Many of the risks of long-term prednisolone use can be reduced by making small lifestyle changes and working closely with your medical team. These steps can help protect your bones, heart, immune system, and overall wellbeing: You may also find support through:
- Downloadable Steroid Emergency Cards (UK): https://www.endocrinology.org/adrenal-crisis
- National Aspergillosis Centre patient resources: https://aspergillosis.org
- Patient support groups such as the Aspergillosis Trust or National Aspergillosis Centre's patient forum
- Your pharmacist, who can help with medication side effects and monitoring
- Specialist endocrine nurses if adrenal insufficiency is diagnosed
Final Thoughts
Long-term steroid use helps many aspergillosis patients control inflammation and stay well. But it comes with responsibilities — particularly the need to monitor for adrenal suppression.
Understanding the HPA axis, recognising symptoms of AI, and knowing when and how to stress dose can empower you to live safely and confidently with aspergillosis.
Always talk to your specialist team if you’re unsure about fatigue, tapering, or illness management. You are not alone — and support is available.
Understanding the HPA Axis and Long-Term Steroid Use in Aspergillosis
For patients living with ABPA, CPA, or other forms of aspergillosis who have used steroids long term
What is the HPA Axis?
The HPA axis stands for the Hypothalamic–Pituitary–Adrenal axis. It's a vital communication system between three parts of your body:
- The Hypothalamus (in the brain)
- The Pituitary gland (also in the brain)
- The Adrenal glands (on top of your kidneys)
These three work together to manage your body’s response to stress, regulate inflammation, and control levels of a hormone called cortisol.
Cortisol helps you respond to illness, injury, or stress. It also affects energy levels, blood pressure, immune function, and even mood.
How Does the HPA Axis Work?
Here’s a simplified version:
- The hypothalamus senses stress or inflammation and sends a hormone called CRH to the pituitary.
- The pituitary gland then sends ACTH to the adrenal glands.
- The adrenal glands release cortisol, which acts throughout your body to reduce inflammation and keep your systems balanced.
Once enough cortisol is in the blood, it signals the brain to stop releasing more. This keeps the system in balance.
Why Aspergillosis Patients Need to Understand This
Many people with aspergillosis—especially those with ABPA (Allergic Bronchopulmonary Aspergillosis)—are treated with oral corticosteroids such as prednisolone. These steroids reduce inflammation but can also interfere with the HPA axis.
Over time, the body may stop producing natural cortisol because it detects enough from medication. This condition is called adrenal insufficiency (AI) or HPA axis suppression.
Symptoms of Adrenal Insufficiency (AI)
If your adrenal glands are underactive, especially after long-term steroid use, you may experience:
- Extreme fatigue or feeling drained
- Muscle weakness
- Joint pain
- Feeling dizzy or faint, especially when standing
- Low blood pressure
- Nausea, vomiting, or abdominal pain
- Loss of appetite
- Worsening of general health during mild illnesses
In severe cases, a lack of cortisol can lead to an adrenal crisis, which is a medical emergency.
What to Do if You Suspect Adrenal Insufficiency
- Never stop steroids suddenly. Your dose should always be tapered under medical supervision.
- If you’ve been on steroids for several weeks or more, ask your doctor whether you should be tested for adrenal insufficiency using a short Synacthen test, which checks how well your adrenal glands respond to a synthetic version of ACTH (not cortisol itself). Synacthen is not your natural corticosteroid, but it helps doctors assess whether your adrenal glands are producing enough natural cortisol..
- You may be switched from prednisolone to hydrocortisone, which is a more natural replacement for cortisol and easier to adjust during illness.
When to Stress Dose (and Why It Matters)
Your stress dosing plan must always be agreed with your doctor. It should be tailored to your specific needs and medical history. If your body is under stress (e.g., illness, surgery, trauma), it needs more cortisol. If your adrenal glands aren’t working properly, this extra cortisol must come from medication.
Common stress dosing scenarios include:
- Fever over 38°C
- Vomiting or diarrhoea
- Dental surgery or minor operations
- Respiratory infections or flare-ups
- Emotional trauma or physical injury
Typical stress dosing guidance:
- Double your usual dose for 2–3 days during mild illness
- Seek emergency care immediately if you can’t keep down tablets or feel seriously unwell. In some cases, emergency medical staff may need to inject hydrocortisone (100 mg intramuscularly) to stabilise you. This should only be done by trained professionals unless you have been specifically trained and advised to self-administer by your specialist.
Always carry:
- A Steroid Emergency Card
- A medical alert bracelet
- An emergency hydrocortisone injection kit if advised
Why Doctors May Switch You to Hydrocortisone
Even though prednisolone can be used to replace cortisol, some patients still experience symptoms of adrenal insufficiency while on it. This can happen because:
- The dose might be too low for your needs
- Prednisolone doesn’t follow the body’s natural cortisol rhythm, which peaks in the early morning and drops throughout the day
- During illness or stress, the body needs more cortisol, and prednisolone doesn’t automatically increase
- Individuals metabolise steroids differently, so a standard dose may not be right for everyone
Common symptoms despite taking prednisolone may include:
- Ongoing fatigue, especially in the morning or late afternoon
- Poor stress tolerance
- Dizziness or weakness during illness
- Slow recovery after infections
For these reasons, your doctor may switch you to hydrocortisone, which is:
- Shorter-acting and better mimics natural cortisol rhythms
- Easier to adjust during illness or stress
- Often better tolerated long term with fewer side effects Hydrocortisone is shorter-acting and more closely mimics the natural rhythm of cortisol. It is usually taken in two or three doses throughout the day — for example, a larger dose in the morning, a smaller dose at lunchtime, and sometimes a final small dose in the early afternoon. This schedule helps replicate the natural daily rise and fall of cortisol and may improve energy levels, mood, and overall well-being.. It may be preferred if:
- You’re tapering from long-term prednisolone
- You’ve developed confirmed adrenal insufficiency
- You need a safer long-term maintenance dose
- You experience steroid-related side effects
Key Reminders for Aspergillosis Patients
| Do This | Why It Matters |
|---|---|
| Follow your tapering plan | Prevents adrenal crisis |
| Ask about adrenal testing if fatigued | Catches suppressed adrenal function early |
| Know your sick-day rules | Allows for stress dosing during illness |
| Consider switching to hydrocortisone | Safer, more natural for long-term hormone replacement |
| Carry emergency ID and hydrocortisone | Life-saving in a crisis |
Final Thoughts
Long-term steroid use helps many aspergillosis patients control inflammation and stay well. But it comes with responsibilities — particularly the need to monitor for adrenal suppression.
Understanding the HPA axis, recognising symptoms of AI, and knowing when and how to stress dose can empower you to live safely and confidently with aspergillosis.
Always talk to your specialist team if you’re unsure about fatigue, tapering, or illness management. You are not alone — and support is available.
🧪 Are Multiple CT Scans Safe? A Guide for Aspergillosis Patients
If you’re living with aspergillosis — whether ABPA, CPA, SAFS, or another form — your doctors may recommend CT scans (or other types of imaging) to monitor your lungs over time. You might be wondering:
“Is it safe to have several CT scans? What about the radiation?”
This article explains when scans are needed, how much radiation they involve, and why they are considered safe — especially when used for chronic lung conditions like aspergillosis.
📷 Why CT Scans Are Used in Aspergillosis
CT scans (especially HRCT or high-resolution CT) are important tools for:
-
Diagnosing or confirming fungal infection
-
Detecting lung cavities, inflammation, or mucus plugging
-
Monitoring disease progression or improvement
-
Checking for complications (e.g. bleeding, infection, fibrosis)
-
Deciding on or adjusting treatment (e.g. antifungals or biologics)
For people with CPA, ABPA, or other long-term lung problems, CT scans provide much more detail than standard chest X-rays.
☢️ How Much Radiation Does a CT Scan Use?
| Scan Type | Typical Radiation Dose | Equivalent Exposure |
|---|---|---|
| Chest X-ray | 0.1 mSv | ~10 days of natural background radiation |
| HRCT Chest | 3–7 mSv | ~1–2 years of background radiation |
| Low-Dose CT (LDCT) | 1–2 mSv | Often used for regular lung monitoring |
✈️ For comparison, a return flight from the UK to New York gives you about 0.1 mSv — the same as one chest X-ray.
✅ Are Multiple Scans Safe?
Yes — when medically necessary, repeated CT scans are considered safe, even over the course of many years. Doctors weigh the small potential risk of radiation against the very real risk of missing important changes in your lungs.
Key points:
-
There is no strict lifetime limit on CT scans
-
Low-dose CT is often used to reduce exposure
-
Your medical team will track your history and avoid unnecessary scans
-
The benefit of accurate diagnosis and monitoring far outweighs the theoretical risk
📈 When Are Repeat CT Scans Recommended in Aspergillosis?
| Situation | Why Scanning Helps |
|---|---|
| CPA monitoring | Track cavities, check for fungal growth or bleeding |
| ABPA flare-up | Look for mucus impaction or bronchiectasis changes |
| New or unexplained symptoms | Rule out co-infections, pneumonia, or embolism |
| Post-treatment review | See if antifungals or biologics are working |
| Surgery planning or lung transplant screening | Required for safety and precision |
🤔 Can You Ask for Fewer Scans?
You can always talk to your healthcare team and ask:
-
"Can this be done with a low-dose CT?"
-
"Is there a recent scan that covers this already?"
-
"How will this scan change my care?"
However, don't delay or refuse a scan out of fear. CT scans are one of the best tools to catch problems early, which can avoid complications, hospital stays, or irreversible lung damage.
🧠 Summary: What You Need to Know
Yes, CT scans use radiation — but in controlled amounts, and only when needed. The information they provide is often vital for treating aspergillosis safely and effectively.
✅ Safe — especially when medically justified
✅ Used with care by your clinical team
✅ Often available in low-dose versions for repeat use
If you have concerns, always feel free to ask your doctor. It’s okay to be curious — and it's even better to be informed.
🌿 Complementary Therapies and Aspergillosis: What Helps, What Doesn’t
Living with aspergillosis — whether it's ABPA, CPA, SAFS, or another form — can be physically and emotionally challenging. While medical treatments like antifungals, steroids, or biologics remain essential, many people ask:
“Can alternative or complementary therapies help with my symptoms or recovery?”
The short answer is: some can support your wellbeing, but they must be used safely and alongside your prescribed care. This guide helps you understand what’s worth exploring — and what to avoid.
🟢🟡🔴 Traffic Light Guide to Complementary Therapies
This guide helps you navigate the wide range of alternative treatments — showing what’s generally safe, what to approach with caution, and what may cause harm.
🟢 GREEN – Generally Safe & Often Helpful
| Therapy | Benefit | Notes |
|---|---|---|
| Airway clearance (ACTs, postural drainage) | Clears mucus, reduces infection risk | Best when guided by physiotherapy |
| Mindfulness / breathing exercises | Helps anxiety, reduces flare-ups | Supports emotional balance |
| Vitamin D (with testing) | May improve immune regulation | Deficiency is common in chronic conditions |
| Yoga / tai chi / gentle stretching | Improves lung mobility, energy | Avoid overexertion during flares |
| CBT / talking therapy | Helps manage fear, fatigue, trauma | Often underused but effective |
| Steam inhalation (plain or saline) | Loosens mucus | Avoid if you’re chemically sensitive |
| Probiotics (capsules or pasteurised products) | Rebuilds gut after antibiotics | Avoid live cultures if immunocompromised |
🟡 AMBER – Use with Caution
These may offer some support, but need discussion with your doctor or asthma nurse.
| Therapy | Claimed Use | Caution |
|---|---|---|
| Curcumin (turmeric extract) | Anti-inflammatory | May interact with meds; avoid high doses |
| Ginger, green tea | Mild antioxidant effect | Some people are sensitive or intolerant |
| Salt therapy (halotherapy) | Loosens mucus | May irritate lungs if dry or unregulated |
| Essential oils (external use only) | Relaxation | May trigger asthma or MCS |
| Acupuncture | Pain or immune balance | Choose practitioners familiar with lung disease |
| Herbal teas (e.g. liquorice, chamomile) | Stress relief | Liquorice can raise BP and potassium levels |
🔴 RED – Avoid These
These therapies are unproven, unsafe, or known to cause harm — especially in people with respiratory or immune-related illness.
| Therapy | Risk |
|---|---|
| Homeopathy | No evidence of effectiveness; delays real treatment |
| Unregulated antifungal herbs (e.g. oregano oil, pau d’arco) | Potential liver damage, interactions |
| Colloidal silver | Can damage organs, build up in body |
| Ingesting essential oils | Toxic to lungs and digestive system |
| Raw unpasteurised probiotics | Unsafe for immunocompromised patients |
| Detox diets / extreme fasting | Can lead to weakness, adrenal crash (especially if on steroids) |
💬 What About "Immune Boosting"?
Be careful with products or diets claiming to "boost" your immune system. In ABPA and SAFS, the immune system is already overreacting. Instead, the goal is to calm or rebalance inflammation — often through medications like biologics, not immune stimulants.
📌 Tips for Safe Use of Complementary Therapies
-
Always tell your doctor about anything new you’re trying
-
Check for interactions with antifungals, steroids, or blood pressure medication
-
Watch for chemically sensitive reactions (some ABPA patients are triggered by fragrances, sprays, or supplements)
-
Focus on whole-body support: rest, nutrition, lung clearance, and emotional wellbeing
🧠 Key Takeaway
Complementary therapies can help you feel better, breathe easier, and cope with the mental toll of chronic illness — but they are not a substitute for medical treatment.
Choose therapies that are:
-
Evidence-informed
-
Used alongside your prescribed care
-
Safe for your specific condition
🫁 ABPA Treatment: Why Are Steroids First, Even if They Can Increase Fungal Growth?

If you've been diagnosed with Allergic Bronchopulmonary Aspergillosis (ABPA), you may have heard that treatment often starts with oral steroids like prednisolone. But ABPA is triggered by a reaction to the Aspergillus fungus — so why use a treatment that might actually let that fungus grow more?
It’s a great question. This guide explains why steroids are still often the first step, what other treatments are available, and when they might be used.
🌿 What Is ABPA?
ABPA is not an infection — it’s an allergic immune reaction in the lungs to the fungus Aspergillus fumigatus. This overreaction causes:
-
Lung inflammation
-
Mucus plugging
-
Breathlessness and wheezing
-
Possible long-term lung damage (e.g., bronchiectasis)
People with asthma or cystic fibrosis are more likely to develop ABPA.
💊 Why Are Steroids Usually the First Treatment?
🔥 The key problem in ABPA is inflammation, not the fungus itself.
Steroids like prednisolone are often used first because they:
-
Act quickly to calm the allergic immune reaction
-
Reduce inflammation and mucus
-
Help relieve symptoms fast (wheezing, tight chest, breathlessness)
-
Prevent long-term damage if started early
Even though steroids may allow some fungal growth, their fast action against inflammation is often more important — especially in flare-ups.
🍄 What About Antifungal Treatments?
Antifungals like itraconazole or posaconazole reduce the amount of Aspergillus in the lungs. This helps to:
-
Reduce allergic triggers
-
Prevent future flare-ups
-
Lower the need for steroids
However, antifungals:
-
Take weeks to work
-
Don’t control inflammation well on their own during a flare
-
Can have side effects and interact with other medications
➡️ That’s why they are often used after steroids, or alongside them — especially in people who flare up often or need steroids long term.
🧬 What About Biologics?
Biologic therapies like:
-
Omalizumab (anti-IgE)
-
Dupilumab (blocks IL-4 and IL-13)
-
Mepolizumab (anti-IL-5)
…are used to help regulate the immune system in patients who:
-
Can’t tolerate steroids
-
Have frequent relapses
-
Need ongoing treatment despite antifungals
Biologics can help:
-
Reduce steroid use
-
Lower flare frequency
-
Improve asthma control
But they’re not yet approved as first-line treatments and are generally reserved for more complex or persistent cases.
✅ What Happens If My Symptoms Are Mild?
Good question. In mild ABPA (e.g. stable breathing, low IgE, no major lung damage), specialists may:
-
Monitor closely before starting any treatment
-
Try antifungals alone, especially if steroid use is risky
However, regular follow-up is essential to make sure inflammation doesn’t silently worsen.
🔄 Typical ABPA Treatment Steps
| Stage | Treatment |
|---|---|
| First flare or moderate symptoms | Steroids (short course) ± antifungals |
| Steroid side effects or long-term use | Add antifungals |
| Recurrent or steroid-dependent ABPA | Add or switch to biologics |
| Mild symptoms and stable lungs | Possibly antifungals first (specialist decision) |
🧘 Staying Well with ABPA
-
Follow your treatment plan closely
-
Keep lungs clear with mucus clearance techniques
-
Avoid damp, mouldy environments
-
Keep up with regular check-ups and lung tests
-
Let your team know if symptoms return
🗨️ In Summary
Steroids are still first-line because they work fast to stop inflammation.
Antifungals and biologics are important longer-term options that help reduce fungal triggers and flare-ups — and may reduce or even replace steroids over time.
Every ABPA patient is different, and your care should be tailored to you.
Managing ABPA: How to Protect Your Lungs and Stay Well
If you’ve been diagnosed with ABPA (Allergic Bronchopulmonary Aspergillosis), you’re probably already working to control inflammation and clear mucus from your lungs. These are essential steps—but there’s more you can do to protect your lung function and prevent long-term damage.
This guide will help you understand what matters most in managing ABPA and feeling your best.
✅ The Basics: What You're Probably Already Doing
1. Keep Inflammation Low
-
This means reducing your IgE levels and calming the immune system.
-
Your doctor may prescribe:
-
Steroids (like prednisolone)
-
Antifungal medication (like itraconazole or voriconazole)
-
In some cases, biologic treatments like omalizumab or mepolizumab
-
2. Clear Mucus Regularly
-
Mucus can trap infection and block your airways.
-
You might be using:
-
Airway clearance techniques (like chest physiotherapy or postural drainage)
-
Nebulised medications (saline or bronchodilators)
-
Mucus-thinning medicines (like carbocisteine or NAC)
-
These two steps are essential, but they’re not the whole picture.
💡 What Else Can Help You Stay Well?
3. Prevent Chest Infections
ABPA can lead to bronchiectasis, a condition where your airways get scarred and damaged. To help prevent this:
-
Treat infections early
-
Get regular chest scans to monitor changes
-
Stay up to date with vaccines (flu, pneumonia, COVID, etc.)
-
Your doctor may consider low-dose antibiotics if infections are frequent
4. Avoid Fungal Exposure
Aspergillus is a fungus found in the environment, especially in:
-
Compost, soil, or damp leaves (gardening can be risky)
-
Mouldy or damp areas in homes
-
Older buildings with water damage
Use air filters, wear a mask when needed, and keep your living space clean and dry.
5. Look After Your Overall Lung Health
-
Pulmonary rehabilitation (specialist-guided breathing and exercise therapy) can improve your stamina and lung function.
-
Practice breathing exercises daily.
-
Stay physically active in ways that are manageable for you.
6. Take Care of Your Body
Steroids can cause side effects over time, like bone thinning and fragile skin.
-
Make sure you're getting enough calcium and vitamin D
-
Ask your doctor about a bone density (DEXA) scan
-
Eat a balanced, anti-inflammatory diet and stay hydrated
7. Look After Your Mental Health
Living with ABPA can be exhausting. Fatigue, breathlessness, and medical side effects can affect your mood and confidence.
-
Track how you’re feeling—physically and emotionally
-
Talk to your care team about fatigue or mental health support if needed
-
You’re not alone—support groups and patient communities can really help
🗣️ Talk to Your Doctor About:
-
Biologic treatments (like omalizumab or mepolizumab) — these may help reduce steroid use
-
Sputum testing to catch early infections
-
Specialist referral to a severe asthma or lung clinic if needed
🧭 Summary: What to Focus On
| What to Manage | Why It Matters |
|---|---|
| Inflammation (IgE levels) | Reduces flare-ups and long-term damage |
| Mucus clearance | Keeps airways open and lowers infection risk |
| Chest infections | Slows or prevents bronchiectasis |
| Environmental exposure | Reduces fungal triggers |
| Exercise & breathing | Supports stronger lungs and energy levels |
| Bone and general health | Counters effects of long-term steroid use |
| Mental wellbeing | Helps you stay strong and supported |
Final Tip
Managing ABPA is a long-term journey, but you're not alone. With the right care, medications, and lifestyle changes, many people with ABPA are able to stabilise their condition and keep their lungs as healthy as possible.
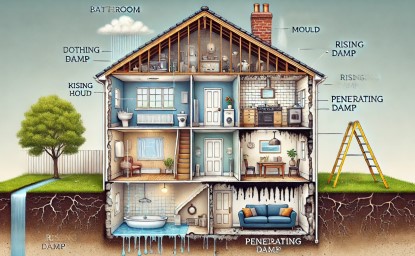
Living Safely in a Damp or Mould-Prone Home: A Complete Guide for Patients and Families
Introduction
Damp and mould in homes are more than a nuisance — they can cause serious health risks, especially for people with existing lung conditions such as asthma, Allergic Bronchopulmonary Aspergillosis (ABPA), Chronic Pulmonary Aspergillosis (CPA), or weakened immune systems. This guide combines essential knowledge, practical steps, and trusted resources to help you protect your home and your health.
1. Understanding Damp and Mould
Damp and mould are common problems in homes and workplaces, particularly in the UK’s colder, wetter climate. While often seen as cosmetic or minor issues, they can cause significant damage to buildings and pose serious health risks if left untreated. Understanding what causes damp and mould is the first step toward preventing them.
🌧️ What Is Damp?
Damp refers to the presence of unwanted moisture in the structure of a building. It can affect walls, ceilings, floors, windows, and even furniture. Damp conditions create the ideal environment for mould, mildew, rot, and structural damage.
There are several types of damp:
-
Condensation: The most common form, caused by excess moisture in the air settling on cold surfaces. Often seen on windows, external walls, and bathrooms.
-
Rising Damp: Caused by moisture moving up through walls from the ground due to a failed or missing damp-proof course (DPC).
-
Penetrating Damp: Occurs when water enters through defects in the building fabric, such as leaking roofs, broken gutters, or cracked walls.
-
Plumbing Leaks/Internal Damp: Caused by leaking pipes, appliances, or internal fixtures.
🍄 What Is Mould?
Mould is a type of fungus that thrives in damp, humid conditions. It grows on a wide range of surfaces, including plaster, wallpaper, wood, tiles, and fabric. Mould reproduces by releasing microscopic spores into the air.
-
Common indoor moulds include Aspergillus, Cladosporium, and Stachybotrys (black mould).
-
Mould can appear as black, green, brown, or white patches.
-
It often produces a musty or earthy smell, even before it’s visibly noticeable.
🧪 The Damp-Mould Cycle
-
Excess moisture enters or forms in the property (e.g., from condensation or leaks).
-
Surfaces stay damp for extended periods—especially where airflow is poor.
-
Mould spores settle on damp surfaces and begin to grow.
-
If not cleaned and the cause not addressed, mould spreads and becomes a persistent issue.
🔍 Signs of Damp and Mould
-
Water marks or discoloured patches on walls and ceilings
-
Peeling paint or wallpaper
-
Condensation on windows, especially in the mornings
-
Musty, damp smell
-
Visible mould growth—black, green, or brown spots
-
Damp or humid feeling in the air
✅ Summary: Key Points
-
Damp is caused by excess moisture and can be structural or lifestyle-related
-
Mould thrives in damp environments and spreads via airborne spores
-
Condensation is the most common trigger for mould in UK homes
-
Spotting early signs and understanding causes is essential for effective prevention
Understanding the basics of damp and mould helps you act quickly, avoid costly damage, and create a healthier living or working space.
2. Health Risks of Damp and Mould
Damp and mould in homes and workplaces aren’t just unpleasant—they can pose serious health risks, especially to vulnerable individuals. Prolonged exposure to mould spores and damp environments can affect respiratory health, worsen existing medical conditions, and contribute to overall poor indoor air quality.
🦠 How Damp and Mould Affect Health
Mould releases microscopic spores and mycotoxins into the air. When inhaled, these particles can irritate the lungs, eyes, skin, and immune system. Damp conditions also encourage the growth of dust mites and bacteria, further contributing to health problems.
👶🧓 Who is Most at Risk?
While mould exposure can affect anyone, certain groups are more vulnerable:
-
Babies and young children – developing lungs are more sensitive to airborne irritants
-
Older adults – weakened immune systems or existing conditions increase risk
-
People with asthma or other respiratory conditions – mould can trigger or worsen symptoms
-
Individuals with weakened immune systems – due to illness or treatment
-
Pregnant individuals – due to changes in immune response
-
People with allergies or skin conditions – may experience worsened symptoms
😷 Common Health Effects
Respiratory Issues
-
Coughing, wheezing, shortness of breath
-
Asthma attacks or worsening asthma symptoms
-
Increased risk of chest infections and bronchitis
-
Irritation of the throat and nasal passages
Allergic Reactions
-
Sneezing, runny or blocked nose
-
Red, itchy, or watery eyes
-
Skin rashes and irritation
-
Sinus congestion and headaches
Other Health Concerns
-
Fatigue and difficulty concentrating – linked to poor indoor air quality
-
Fungal infections – in severe cases, especially in immunocompromised individuals
-
Mental health effects – prolonged exposure to poor living conditions, including mould and damp, can contribute to stress, anxiety, and depression
🏥 When to Seek Medical Help
You should consult a doctor if:
-
You or someone in your household experiences persistent coughing, wheezing, or breathing difficulties
-
Asthma symptoms are worsening or becoming harder to control
-
Allergic symptoms appear or intensify after spending time indoors
-
A child, elderly person, or immunocompromised individual is exposed to mould regularly
Doctors may recommend medications, allergy testing, or home environment assessments.
🧼 Prevention Is the Best Protection
-
Fix leaks and ventilate regularly to reduce moisture
-
Clean mould promptly and safely
-
Monitor humidity and condensation levels
-
Use dehumidifiers or air purifiers if needed
-
Act quickly—even small patches of mould can pose a risk
✅ Summary: Health Risks at a Glance
-
Mould can trigger asthma, allergies, and infections
-
Damp environments encourage dust mites and bacteria
-
Vulnerable individuals are at higher risk of health complications
-
Long-term exposure may affect mental wellbeing and indoor air quality
-
Early prevention and treatment are key to protecting health
Maintaining a dry, well-ventilated home is not just about comfort—it's a vital part of protecting your family’s health.
3. Prevention: Keeping Your Home Warm, Dry, and Clean
The most effective way to tackle damp and mould is to stop it before it starts. Prevention focuses on managing moisture, improving airflow, and maintaining a clean, warm environment. Whether you live in a new build or an older property, these proactive steps can greatly reduce the risk of damp and mould developing.
🔥 Keep Your Home Warm
A warm home helps prevent condensation, which is a key cause of mould in colder months.
-
Maintain a consistent temperature (ideally 18–21°C) throughout the day, especially in bedrooms and living areas.
-
Use thermostats and timers to control heating efficiently without wasting energy.
-
Avoid letting rooms get very cold, even when unoccupied—this can cause moisture to condense on cold surfaces.
-
If heating only certain rooms, keep doors closed to retain warmth.
💨 Improve Ventilation
Proper ventilation helps remove moist air generated from daily activities like cooking, bathing, and drying clothes.
-
Open windows for short periods each day, even in winter, to allow fresh air in and moisture out.
-
Use extractor fans in kitchens and bathrooms—and leave them running for 10–15 minutes after use.
-
Install trickle vents or leave window vents open to allow passive airflow.
-
Avoid blocking air bricks or ventilation grilles.
If natural ventilation isn’t enough, consider mechanical ventilation systems, especially in properties prone to damp.
💧 Manage Indoor Moisture
Daily activities release moisture into the air. Limiting and controlling this moisture is key:
-
Dry clothes outside when possible. If indoors, use a room with good ventilation and keep the door closed.
-
Cover pots and pans when cooking, and use extractor fans or open windows.
-
Wipe condensation off windows and walls daily, especially in the mornings.
-
Avoid overfilling wardrobes and cupboards—allow air to circulate around furniture and stored items.
-
Consider using dehumidifiers in damp-prone rooms such as basements or poorly ventilated areas.
🧽 Clean Regularly and Act Early
-
Clean bathrooms and kitchens frequently, focusing on areas where moisture builds up—tiles, window frames, behind furniture.
-
Use anti-mould sprays or vinegar to clean areas prone to black mould.
-
Check hidden spots regularly—behind sofas, in wardrobes, and under windowsills.
-
Tackle early signs of mould as soon as you see them. Small patches can often be safely cleaned before they spread (see Section 4).
🔧 Carry Out Routine Maintenance
Preventing structural damp is just as important as managing daily moisture.
-
Inspect and repair leaks in roofs, windows, gutters, and pipes.
-
Keep gutters and downpipes clear of leaves and debris to avoid overflow.
-
Seal windows and doors to stop rain from entering.
-
Ensure your home’s damp-proof course (DPC) is intact and unobstructed by soil, decking, or external paving.
✅ Summary: Top Prevention Tips
-
Keep rooms consistently warm
-
Ventilate daily—even in cold weather
-
Dry clothes carefully and wipe down condensation
-
Clean high-moisture areas regularly
-
Repair leaks and inspect your home’s exterior
-
Use dehumidifiers and anti-mould products where necessary
By keeping your home warm, dry, and clean, you’ll create an environment where damp and mould are far less likely to thrive. Prevention is always easier—and cheaper—than cure.
4. Safe Mould Cleaning
Cleaning mould safely and effectively is essential to protect your health and prevent it from returning. If mould is not dealt with properly, it can spread quickly and worsen underlying damp problems. This guide outlines how to clean small areas of mould safely and when to call in professional help.
⚠️ Before You Start: Assess the Situation
-
Size Matters: If the mould covers an area larger than 1 square metre, or if it returns frequently, it’s best to consult a professional.
-
Hidden Mould: If you suspect mould behind walls, under floors, or in insulation, do not disturb it—this can release large amounts of spores into the air.
-
Health Warning: People with respiratory conditions (asthma, COPD), allergies, weakened immune systems, or pregnant individuals should avoid cleaning mould themselves.
🧰 What You’ll Need
-
Protective gear:
-
Disposable gloves
-
N95/FFP2 mask or equivalent
-
Safety goggles or protective glasses
-
-
Cleaning tools:
-
Soft scrubbing brush or cloth
-
Bucket of warm water
-
Spray bottle (optional)
-
-
Cleaning solution:
-
Mild detergent and warm water, or
-
White vinegar (undiluted), or
-
A mould and mildew remover approved for domestic use (avoid mixing chemicals)
-
Avoid bleach for porous surfaces—it may remove staining but often doesn’t kill mould roots.
🧼 Step-by-Step Cleaning Process
1. Ventilate the Area
-
Open windows and keep the room well-ventilated during and after cleaning.
-
Close internal doors to prevent spores spreading to other parts of the home.
2. Prepare Safely
-
Put on all protective gear before entering the mould-affected area.
-
Remove or cover nearby soft furnishings and valuables.
3. Apply the Cleaning Solution
-
Spray or apply your chosen cleaning solution directly onto the mouldy surface.
-
Let it sit for a few minutes to loosen the mould.
4. Gently Scrub the Area
-
Use a cloth or soft brush to scrub the area gently.
-
Don’t scrape or use excessive force, as this can damage surfaces and spread spores.
5. Rinse and Wipe
-
Wipe the cleaned area with a clean damp cloth, then again with a dry one.
-
Dispose of all cloths or rags used in a sealed plastic bag.
6. Dry the Area Thoroughly
-
Use fans, heaters, or natural airflow to dry the area completely.
-
Mould will return quickly if surfaces remain damp.
🗑️ Disposal and Clean-Up
-
Double-bag all disposable items (gloves, cloths, etc.) and throw them away in your household rubbish.
-
Wash hands thoroughly after cleaning, even if gloves were worn.
-
Clean tools used in hot soapy water or dispose of them if heavily contaminated.
🧯 Prevent Mould from Returning
-
Address the source of moisture (leaks, condensation, poor ventilation).
-
Use a dehumidifier if humidity remains high.
-
Repaint affected areas with anti-mould paint or sealant.
-
Monitor the space over the following weeks for any signs of return.
👷♀️ When to Call in Professionals
You should seek professional help if:
-
The mould covers more than 1m² or appears in multiple rooms
-
The mould returns after cleaning
-
You suspect hidden damp or structural causes
-
The property has vulnerable occupants (elderly, babies, or those with health issues)
Certified mould remediation specialists can safely remove large infestations and identify underlying issues that DIY methods can’t reach.
✅ Summary: Safe Mould Cleaning Tips
-
Wear protective gear and ventilate the room
-
Use mild detergent, vinegar, or mould-specific cleaner—never mix chemicals
-
Clean small areas gently and dispose of contaminated materials safely
-
Dry the area completely after cleaning
-
Address moisture sources to stop mould from returning
By following safe cleaning practices and staying vigilant, you can tackle small-scale mould before it becomes a bigger—and more expensive—problem.
5. Structural Causes of Damp and Mould
Damp and mould are often the result of underlying structural issues in a building. Identifying and addressing these causes is crucial for long-term prevention. Common structural causes include:
-
Roof Leaks: Broken or missing roof tiles and damaged flashing can allow water to seep into the property, leading to damp ceilings and walls.
-
Faulty Gutters and Downpipes: Blocked or leaking gutters and downpipes can overflow, allowing water to run down exterior walls and soak into the structure.
-
Rising Damp: This occurs when moisture from the ground travels up through walls due to a damaged or missing damp-proof course (DPC).
-
Penetrating Damp: Caused by water entering through external walls due to cracks, porous bricks, or faulty rendering.
-
Poor Insulation: Inadequate insulation can lead to cold surfaces inside the home, encouraging condensation and mould growth.
-
Broken Seals Around Windows and Doors: Damaged seals can let in rainwater and allow moisture to build up around frames.
-
Plumbing Issues: Leaking or burst pipes inside walls or under floors can cause hidden damp spots that lead to mould growth.
Regular maintenance and early repairs can help prevent structural damp problems and reduce the risk of mould developing in your home.
6. How to Recognise a Good Damp Surveyor
When dealing with persistent damp or mould problems, hiring a qualified and trustworthy damp surveyor is one of the most important steps you can take. A good surveyor doesn’t just offer a quick fix—they diagnose the root cause and recommend long-term solutions based on evidence, not sales incentives.
👷♂️ What is a Damp Surveyor?
A damp surveyor is a building specialist trained to assess the causes and extent of damp, mould, and moisture-related problems in a property. Their role is to:
-
Inspect the building thoroughly
-
Identify the type of damp (e.g., rising, penetrating, condensation)
-
Detect hidden moisture using professional tools
-
Recommend the most appropriate, cost-effective remedy
🏅 Key Qualities of a Good Damp Surveyor
✅ Relevant Qualifications
Look for surveyors with recognised professional credentials, such as:
-
CSRT (Certified Surveyor in Remedial Treatment) – Focused on damp, timber decay, and treatment solutions
-
CSSW (Certified Surveyor in Structural Waterproofing) – For diagnosing and specifying waterproofing systems in below-ground structures
-
Membership with the Property Care Association (PCA) or the Royal Institution of Chartered Surveyors (RICS) is a strong indicator of professionalism and adherence to standards.
✅ Independence and Impartiality
-
Choose an independent surveyor—not one linked to a damp-proofing company.
-
Be cautious of "free surveys" from companies whose main goal is selling you expensive treatments.
-
A good surveyor provides an unbiased assessment based on the building’s condition, not on commission-driven sales.
✅ Experience and Reputation
-
Look for someone with proven experience in diagnosing a range of damp problems, especially in buildings similar to yours (e.g., period properties, flats, basements).
-
Check online reviews, ask for references, or seek recommendations from local homeowners, tradespeople, or your local authority.
✅ Thorough and Methodical Approach
A good damp surveyor will:
-
Inspect the entire property, including loft spaces, basements, and external walls
-
Use a range of diagnostic tools, such as:
-
Moisture meters
-
Thermal imaging cameras
-
Hygrometers (to measure humidity levels)
-
-
Take time to explain findings clearly and answer your questions
-
Identify not just the symptoms, but the underlying cause of the damp
✅ Detailed Written Report
-
Expect a comprehensive report, not just a brief summary.
-
A quality report should include:
-
Photographic evidence
-
Moisture readings and data
-
Clear explanation of the type(s) of damp
-
Root causes and contributing factors
-
Tailored recommendations for repairs, ventilation, or treatment
-
Estimated costs and timelines (if applicable)
-
❌ Warning Signs of a Poor Surveyor
-
Overly quick inspections that miss key areas
-
Vague recommendations or pushy sales tactics
-
Offering only one "solution" (usually chemical damp-proofing) without explaining other options
-
No formal qualifications or unclear professional background
-
Inability or refusal to answer technical questions clearly
📍 Where to Find a Good Surveyor
-
Property Care Association (PCA): www.property-care.org
-
Royal Institution of Chartered Surveyors (RICS): www.rics.org
-
Ask your local council, especially if you’re in social or rented housing—they may recommend or provide qualified assessors.
✅ Summary: What to Look for
-
Recognised qualifications (ISSE, CSRT, CSSW, PCA, RICS)
-
Independent, unbiased advice
-
Experience with similar properties
-
Full inspection with professional tools
-
Detailed, clear written report
-
Willingness to answer your questions
Hiring the right damp surveyor can save you from unnecessary work, high costs, and ongoing problems. Take the time to choose someone you can trust—your home and health are worth it.
7. Remediation and Repairs
Once damp or mould has been identified in a property, it's crucial to go beyond surface cleaning and address the root causes. Proper remediation and repair work not only removes visible damage but also prevents future problems, protecting both the building and the health of its occupants.
🛠️ Step-by-Step Remediation Process
1. Identify the Source of Moisture
Before any repairs begin, determine where the moisture is coming from. Common sources include:
-
Leaking pipes or roofs
-
Condensation from poor ventilation
-
Rising or penetrating damp due to structural issues
-
Faulty guttering or downpipes
A professional damp surveyor can help accurately diagnose the problem.
2. Stop the Moisture at Its Source
-
Fix Leaks: Repair plumbing, roofs, windows, and gutters to stop water ingress.
-
Improve Ventilation: Install extractor fans in kitchens and bathrooms, unblock air vents, and ensure windows can be opened.
-
Install or Repair Damp-Proofing: Address rising damp with a working damp-proof course (DPC) or membrane.
-
Insulate and Heat: Add insulation to cold walls, and maintain a consistent indoor temperature to reduce condensation.
3. Dry Out the Affected Areas
Once the source has been controlled, thoroughly dry out the space:
-
Use dehumidifiers and fans to remove moisture from the air.
-
Keep windows open when safe to do so, or use trickle vents to maintain airflow.
-
Drying may take several days to weeks, depending on the extent of the damp.
4. Remove Damaged or Contaminated Materials
Mould can penetrate porous materials, which often need to be replaced:
-
Remove and safely dispose of contaminated carpets, wallpaper, insulation, or plasterboard.
-
Use sealed plastic bags for disposal and avoid spreading spores.
-
In severe cases, professional removal may be required to ensure safe handling and containment.
5. Clean and Treat Surfaces
Once dry, clean all affected hard surfaces with suitable mould-killing products:
-
Use antifungal sprays, vinegar, or specialised cleaners (avoid bleach on porous surfaces).
-
Wear protective gear—gloves, mask, goggles—when cleaning.
-
Apply mould-resistant sealants or primers before repainting or refinishing.
6. Repair and Refinish
After cleaning and removal:
-
Replaster walls where necessary
-
Repaint with mould-resistant paint
-
Replace floorboards, skirting boards, or ceiling tiles that were removed
These repairs help restore your home and improve its long-term resistance to moisture.
🧰 Preventive Upgrades to Consider
To reduce the risk of recurrence:
-
Install Humidistats: These monitor humidity and automatically trigger ventilation.
-
Improve Insulation: Especially on external walls and in loft spaces.
-
Add Cavity Wall or Loft Insulation: This helps regulate temperature and reduces condensation.
-
Use Anti-Mould Paints and Finishes: Especially in kitchens, bathrooms, and basements.
⚠️ When to Call in Professionals
You should hire professional damp and mould remediation specialists when:
-
The mould covers a large area (more than 1 square metre)
-
You suspect hidden damp behind walls or under floors
-
Occupants have persistent health symptoms related to mould
-
DIY cleaning hasn’t solved the problem, or mould keeps returning
Look for certified professionals (e.g., PCA members or surveyors with CSRT/CSSW credentials) who offer comprehensive diagnostics and long-term solutions.
✅ Summary: Key Remediation Steps
-
Find and fix the source of moisture
-
Dry out affected areas thoroughly
-
Remove damaged materials
-
Clean and treat all surfaces
-
Repair and refinish the space
-
Upgrade ventilation and insulation to prevent return
Proper remediation and repairs are critical to protecting both your property and your health. Don’t settle for cosmetic fixes—deal with damp and mould at the source for long-lasting results.
8. Special Winter Advice
Winter is the most challenging season for managing damp and mould. Cold weather, increased indoor moisture, and reduced ventilation all contribute to the perfect conditions for mould growth. However, with the right preventative steps, you can keep your home or workplace warm, dry, and healthy throughout the colder months.
❄️ Why Winter Increases Risk
-
Condensation: Warm, moist indoor air hits cold surfaces (like windows and external walls), turning into water droplets that can soak into building materials.
-
Limited Ventilation: People tend to keep windows closed in winter, trapping moisture from cooking, showering, and breathing.
-
Higher Humidity Indoors: Drying clothes inside, using heaters, and running hot water increases humidity.
-
Poor Insulation: Cold spots and draughts can cause uneven temperatures and condensation buildup.
🧣 Essential Winter Prevention Tips
🔥 Keep the Home Consistently Warm
-
Set your thermostat to maintain a steady temperature between 18°C and 21°C, even at night.
-
Avoid sudden drops in temperature, which increase condensation.
-
Use programmable timers on your heating system to manage energy use efficiently.
🌬️ Ventilate Without Losing Too Much Heat
-
Open windows briefly (10–15 minutes) each day to refresh stale, humid air—especially in bathrooms and kitchens.
-
Use extractor fans when cooking or bathing, and keep them running for at least 15 minutes after use.
-
Keep internal doors closed while ventilating to contain warm air in other areas.
👕 Dry Clothes with Caution
-
Avoid drying clothes on radiators, which releases large amounts of moisture into the air.
-
If you must dry indoors, use a dedicated room with windows open or use a dehumidifier to absorb the extra moisture.
💧 Monitor and Control Humidity
-
Use a hygrometer to track indoor humidity (ideal range: 40–60%).
-
Place moisture absorbers in corners, wardrobes, or poorly ventilated spaces.
-
Use a dehumidifier in high-risk areas like basements or bathrooms.
🚪 Eliminate Cold Spots and Draughts
-
Seal gaps around doors and windows with draught excluders or weather stripping.
-
Use thick curtains and thermal blinds to keep heat in and cold out.
-
Insulate cold walls where possible to reduce surface condensation.
🧼 Routine Maintenance in Winter
-
Check Gutters and Downpipes: Clear leaves and debris to prevent blockages that can lead to water ingress.
-
Inspect Roofs and Windows: Look for signs of leaks or damage before snow and rain make them worse.
-
Wipe Down Surfaces: Remove condensation from windows and sills every morning with a dry cloth or window vacuum.
-
Keep Furniture Away from Walls: Leave a gap to allow air to circulate and prevent mould from forming behind items.
🚨 Act Quickly at First Signs of Trouble
-
Don’t ignore cold, damp smells or early signs of mould.
-
Clean small patches using safe methods (see Section 7), and address the cause immediately.
-
If problems persist, consider getting a damp survey to check for hidden issues.
✅ Summary: Winter Damp Defence
-
Maintain consistent warmth
-
Ventilate, even in cold weather
-
Control humidity levels
-
Dry laundry carefully
-
Carry out regular inspections
-
Act early if problems develop
By combining good habits with simple adjustments, you can keep damp and mould at bay—even during the coldest months of the year.
9. Damp and Mould at Work
Damp and mould problems can have serious consequences in the workplace, affecting the health and wellbeing of staff, damaging property, and even leading to legal and financial liabilities for employers. Recognising and addressing these issues promptly is essential for maintaining a safe and compliant working environment.
🛠️ Common Causes in the Workplace
-
Poor Ventilation: Many office and commercial buildings rely on sealed environments with artificial climate control. Without proper airflow, moisture builds up—especially in kitchens, toilets, basements, and storage areas.
-
Leaks and Water Ingress: Leaking roofs, faulty windows, damaged plumbing, and burst pipes can introduce moisture into the building’s fabric, leading to persistent damp patches and hidden mould.
-
Condensation: Poor heating and ventilation management can lead to high humidity and condensation, particularly around windows and in cold areas of the building.
-
Structural Defects: Cracks in walls, missing roof tiles, broken guttering, and failed damp-proofing can all allow water to penetrate the structure, especially during heavy rain or freezing conditions.
🩺 Health Risks to Employees
Exposure to damp and mould in the workplace can cause or worsen a range of health conditions, especially for those with asthma, allergies, or weakened immune systems. Common symptoms and issues include:
-
Coughing, wheezing, or shortness of breath
-
Nasal congestion and sinus infections
-
Eye, nose, and throat irritation
-
Headaches, fatigue, and reduced concentration
-
Skin rashes or irritation
-
Aggravation of pre-existing respiratory conditions
Persistent exposure can result in absenteeism, reduced productivity, and long-term health issues for affected staff.
⚖️ Employer Responsibilities (UK)
Under UK health and safety law, employers are legally required to provide a safe, healthy workplace. Relevant legislation includes:
-
Health and Safety at Work etc. Act 1974
-
Workplace (Health, Safety and Welfare) Regulations 1992
-
Control of Substances Hazardous to Health (COSHH) Regulations 2002
Employers must:
-
Carry out regular health and safety risk assessments
-
Address hazards promptly, including damp and mould
-
Provide clean, ventilated, and dry working conditions
-
Respond to employee complaints about indoor air quality
-
Engage professional help if needed to investigate and resolve the issue
Failing to act can result in enforcement action, fines, or compensation claims.
🗣️ What Employees Should Do
-
Report It: Notify a supervisor, facilities manager, or health and safety representative if you notice damp smells, mould growth, or symptoms linked to poor air quality.
-
Document It: Take photos and note dates, symptoms, and any patterns in exposure. Keep a record if problems persist.
-
Know Your Rights: If an employer fails to act, contact your union representative or external bodies such as the Health and Safety Executive (HSE) or Citizens Advice.
-
Look After Your Health: If you experience symptoms, seek medical advice and mention potential workplace exposure.
👷♀️ When to Get Professional Help
Employers should engage qualified professionals if:
-
The source of damp is unknown or extensive
-
The mould is widespread (covering more than 1m²)
-
The issue returns after basic cleaning or repairs
-
Staff health complaints are increasing
Professional damp surveyors and remediation contractors can identify structural issues, recommend repairs, and safely remove mould.
✅ Summary: Best Practices for Workplaces
-
Regularly inspect building interiors and exteriors for signs of damp
-
Maintain heating, ventilation, and air conditioning (HVAC) systems
-
Address leaks and maintenance issues immediately
-
Ensure cleaning teams are trained to spot and report mould
-
Keep staff informed and encourage early reporting
Tackling damp and mould in the workplace isn't just about comfort—it's a health and legal responsibility. A proactive approach protects both people and property.
10. Trusted Resources
If you're dealing with damp and mould in your home or workplace, it's important to get accurate information and support from reliable sources. Below are trusted organisations and resources that offer guidance, assistance, and further reading:
Government and Public Health
-
NHS – Offers health advice on symptoms and treatment related to mould exposure.
www.nhs.uk -
UK Government (GOV.UK) – Guidance on housing standards, tenants’ rights, and landlord responsibilities.
www.gov.uk -
Public Health England (now UKHSA) – Information on the health impacts of damp and mould in indoor environments.
www.gov.uk/government/organisations/uk-health-security-agency
Housing and Tenant Support
-
Shelter – Offers legal advice and support for tenants facing housing issues, including damp and mould.
www.shelter.org.uk -
Citizens Advice – Free guidance on resolving disputes with landlords and understanding your rights.
www.citizensadvice.org.uk
Technical and Surveyor Support
- Institute of Specialist Surveyors and Engineers- ISSE run their own specialised high-quality certification & validation www.isse.org.uk
-
Property Care Association (PCA) – Find certified damp and timber specialists, including surveyors with CSRT and CSSW qualifications.
www.property-care.org -
Royal Institution of Chartered Surveyors (RICS) – Directory of accredited surveyors and building professionals.
www.rics.org
Additional Help
-
Local Councils – Many councils offer environmental health services to inspect and act on damp issues in rental properties.
Using these trusted sources can help you make informed decisions and get the right support to effectively manage and resolve damp and mould problems.
✅Summary Checklist: Top Actions for Damp and Mould Prevention
Use this quick-reference guide to stay on top of the most effective ways to prevent and manage damp and mould in your home or workplace:
🏠 Keep Your Home Warm and Dry
-
Maintain a consistent indoor temperature (18–21°C)
-
Insulate walls, roofs, and floors properly
-
Use thermostats and timers to manage heating efficiently
💨 Improve Ventilation
-
Open windows regularly, even in winter
-
Use extractor fans in bathrooms and kitchens
-
Install trickle vents or air bricks if needed
🚿 Manage Moisture and Humidity
-
Wipe down windows and cold surfaces daily
-
Use a dehumidifier in high-moisture rooms
-
Dry clothes outside or in a ventilated room
🔧 Fix Structural and Maintenance Issues
-
Repair leaks in roofs, pipes, gutters, and windows promptly
-
Check for cracks in walls and faulty damp-proofing
-
Clean and maintain gutters and downpipes
🧼 Clean Safely and Act Early
-
Clean mould as soon as it appears using safe methods
-
Wear gloves, mask, and eye protection when cleaning
-
Discard mouldy materials that can't be cleaned
🧑🔧 Seek Professional Help When Needed
-
Hire a qualified, independent damp surveyor (CSRT/CSSW)
-
Use trusted contractors for repairs and remediation
-
Contact local council or tenants' support if landlord is unresponsive
📅 Be Proactive in Winter
-
Increase ventilation despite colder weather
-
Monitor condensation and damp-prone areas closely
-
Check insulation and seal drafts before winter starts
Regular checks, early action, and good habits are your best defence against damp and mould.
📘 Managing IgE Levels in ABPA: What Happens After Treatment?
If you have ABPA (Allergic Bronchopulmonary Aspergillosis), you’ve likely been told your IgE levels are high. Many patients ask:
“Once my IgE goes down with treatment, how do I keep it down without staying on steroids or antifungals forever?”
This guide explains why IgE is important, how it’s treated, and what long-term steps you can take to stay well.
🧪 What is IgE and Why Is It High in ABPA?
IgE (Immunoglobulin E) is an antibody your immune system makes in response to allergens. In ABPA, your immune system overreacts to Aspergillus, a common fungus, causing inflammation in the lungs. This leads to:
-
High total IgE levels (often over 1,000–10,000 IU/mL)
-
Symptoms like coughing, wheezing, and mucus plugs
-
Lung changes on scans, if untreated
🎯 Treatment Goals
Treatment aims to:
-
Lower inflammation
-
Reduce the fungal burden
-
Bring IgE levels down (a marker that your inflammation is settling)
-
Prevent long-term lung damage
You might be treated with:
-
Oral steroids (e.g. prednisolone)
-
Antifungal tablets (e.g. itraconazole or voriconazole)
These medications help bring IgE levels down, sometimes dramatically. But they can’t usually be taken forever — long-term use may cause side effects.
🔄 After IgE Drops – What Next?
Even after successful treatment, ABPA can flare up again. So the key questions become:
How do we keep IgE low?
How do we prevent future flare-ups?
🧭 Long-Term Management Options
1. Close Monitoring
-
IgE is checked every 2–6 months
-
Doctors look for a doubling in IgE — this can mean a flare is starting
-
Regular chest scans and lung function tests are also used to spot changes early
2. Tapering Medication
-
Steroids are slowly reduced, not stopped suddenly
-
Your doctor will watch for any return of symptoms or rise in IgE
3. Biologic Treatments
Some newer medications can help long-term, especially if you:
-
Have frequent flare-ups
-
Can’t reduce steroids safely
-
Have asthma or eosinophilic inflammation
These include:
-
Omalizumab (anti-IgE antibody)
-
Mepolizumab / Benralizumab (target eosinophils)
-
Dupilumab (blocks part of the allergy pathway)
Biologics are usually injections given every 2–4 weeks, and can help reduce relapses and steroid need.
🏡 Lifestyle & Environmental Tips
Reducing your exposure to Aspergillus can help keep IgE from rising again.
🔹 Avoid:
-
Damp or moldy areas
-
Compost, rotting leaves, hay, or soil dust
-
Rooms with poor ventilation
🔹 Use:
-
Ventilate your home well (eg open windows/extractor fans)
-
A HEPA-filter air purifier at home
-
An FFP2/FFP3 mask when doing dusty activities (gardening, cleaning mold)
🥗 Eat for Immune Support:
-
Anti-inflammatory foods (vegetables, oily fish, berries)
-
Reduce sugar (high sugar may promote inflammation)
-
Stay well hydrated
-
Ask your doctor about vitamin D — it may help regulate immunity
📅 Follow-up Schedule (General examples, yours may differ)
| Time Since Treatment | What to Expect |
|---|---|
| 1–3 months | Blood tests (IgE, eosinophils), lung check |
| 3–6 months | Check for symptoms, possibly repeat IgE |
| 6–12 months | CT scan or lung function, if needed |
| After 1 year | Stable patients may have annual reviews |
Let your team know if any symptoms return — even if your last IgE result was stable.
🧠 Final Thoughts
-
You may always have “elevated” IgE compared to someone without ABPA — that’s okay. The goal is stability, not “zero IgE”.
-
Many patients live well with ABPA for years by learning to manage flare-ups early and avoiding fungal exposure.
-
Ask your clinic about your personal IgE pattern — some people flare with small changes; others don’t.
-
Support groups and educational resources (like aspergillosis.org) can help you stay informed and confident.
📩 Have questions for your team?
Bring these up at your next appointment:
-
Can I reduce my medication safely?
-
Could I benefit from a biologic?
-
How often should I check my IgE?
-
How can I reduce exposure at home?