🌦️ Understanding Corticosteroid Mood Swings
Alison shared something that will resonate with many of us:
“Recognising that prednisone mood swings are very unpredictable is a good reminder as I feel like I am up and down so much of late. Yesterday’s swap to half hydrocortisone and half prednisone probably took a bit of adjusting too. Better day today though — I even got out to pick up my campervan that had been in for service. Felt really good to be driving it again and as the weather improves, I live in hope that I might get to use it this year!” 😊🤔
💭 Why mood can change on corticosteroids
Steroid medicines such as prednisone, prednisolone, and hydrocortisone affect many systems in the body — including brain chemistry.
When levels go up or down (for example when changing dose or type), it’s common to feel:
-
Irritable or anxious one day, low or tired the next
-
More emotional than usual — tears or frustration come quickly
-
Sleep disturbance, vivid dreams, or early waking
-
Short bursts of energy or restlessness, followed by a “crash”
These changes don’t mean you’re “losing control” — they reflect how sensitive the brain is to shifts in cortisol, the hormone steroids replace or supplement.
⚖️ Why switching between steroids can feel bumpy
Prednisone and hydrocortisone are both corticosteroids but have different potencies and timings:
| Steroid | Approx. equivalent dose (anti-inflammatory) | Typical duration of action |
|---|---|---|
| Hydrocortisone | 20 mg ≈ 5 mg prednisolone | Short-acting (6–8 hours) |
| Prednisone/Prednisolone | 5 mg | Longer-acting (12–36 hours) |
When switching or mixing them, the body’s rhythm of cortisol can temporarily feel off — like jet lag for your stress hormones. It often settles after a few days.
🌞 Tips that may help
-
Keep a simple mood or energy diary — it helps you and your clinician see patterns.
-
Take doses at consistent times, usually in the morning, unless advised otherwise.
-
Build in gentle activity or time outdoors — small wins, like Alison’s campervan trip, really lift mood.
-
Avoid caffeine or alcohol spikes if feeling restless or irritable.
-
Tell your clinician if mood swings are severe or prolonged — dose adjustment or slower tapering may help.
💬 In Alison’s words
“Better day today.”
Sometimes that’s the victory — one step, one better day, one bit of normality returning.
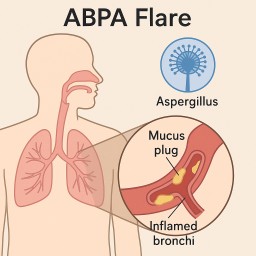
🌿 Why do I get thick, yellow mucus in the morning?
Many people with asthma, ABPA (allergic bronchopulmonary aspergillosis) or sinus problems notice that first thing in the morning they cough up or “hook out” very thick, sticky, yellow mucus from the back of the throat or nose.
It can feel like glue — stringy, rubbery, and slow to move.
The good news is:
👉 This doesn’t automatically mean that Aspergillus fungus is growing in your sinuses.
💧 Why it happens
At night, mucus naturally becomes thicker because:
-
You breathe more through your mouth while sleeping, which dries the nose and throat.
-
Mucus sits still instead of draining, so it concentrates and thickens.
-
If you already have sinus inflammation or allergies, your mucus glands make even more.
-
It often drains down the back of the throat (post-nasal drip), where it collects until morning.
This combination makes for a lumpy, sticky “plug” that only shifts once you’re up and moving around.
🧠 When might fungus be involved?
If the sinuses become colonised with Aspergillus or another fungus, there are usually extra clues, such as:
-
Blocked nose or pressure that doesn’t improve with sprays or rinses
-
One-sided pain or discharge
-
Dark, rubbery, or green-grey plugs rather than yellow mucus
-
Loss of smell
-
CT or endoscopy showing thick debris or “fungal balls”
If these are present, an ENT specialist can look directly into the sinuses and, if needed, take a small sample for fungal culture or order a CT scan.
🩺 What helps most people
You can often manage the morning mucus with simple measures:
-
Saline nasal rinses (like Sterimar, NeilMed, or salt-water sprays) — thin mucus and wash out allergens or fungal dust.
-
Warm fluids or gentle steam to moisten airways.
-
Topical nasal steroid sprays (if prescribed) — reduce swelling and mucus production.
-
Plenty of hydration through the day.
-
Avoid over-using decongestant sprays, which can make congestion worse in the long run.
If mucus stays thick, coloured, or difficult to clear for more than a few weeks — or you develop sinus pressure, pain, or smell loss — ask for a review by your ENT or respiratory team.
🟢 Key message
Thick yellow mucus in the morning is usually a sign of dryness and overnight build-up, not an active fungal infection.
Regular rinsing, good hydration, and controlling sinus inflammation usually keep things under control.
Fungal colonisation is much less common — and when it happens, there are usually other warning signs that your clinician can check.
🌬️ When Breathlessness Gets Worse: Understanding What Might Be Happening
Many people with aspergillosis or ABPA (Allergic Bronchopulmonary Aspergillosis) find that their symptoms come and go — some days are better, some worse.
It can feel worrying when you suddenly become more breathless or wheezy, especially if you’ve been doing all the right things: airway clearance, antifungal treatment, and even starting a biologic injection.
This guide explains what might be happening and how you can begin to work out the cause.
💨 1. Why you might feel worse after airway clearance
Airway clearance helps move sticky mucus and plugs out of your lungs — but this can temporarily irritate or narrow the airways, especially if your chest is already inflamed.
You might feel tighter or more wheezy for a short time after a session.
Helpful tips
-
Use your bronchodilator (salbutamol or similar) before starting airway clearance.
-
Keep sessions short and gentle if you feel breathless afterward.
-
Talk to your respiratory physiotherapist about changing the timing or intensity of your airway clearance routine.
-
Nebulisers or inhalers after clearance can help calm things down again.
🧫 2. Could it mean the Aspergillus is becoming more active?
Sometimes it can — but not always.
Symptoms like breathlessness, cough, or fatigue can also be caused by inflammation, infection, or changes in medication.
Signs that might suggest Aspergillus activity is rising include:
-
More sputum, or thicker or darker plugs
-
More coughing or wheezing
-
Tiredness or mild fever
-
A drop in your usual lung function numbers (FEV₁)
These changes are only clues — to be sure, you need blood or sputum tests.
🧪 3. Tests that help you and your team understand what’s going on
| Test | What it shows |
|---|---|
| Total IgE | Rises when allergic inflammation is active (monitored every few months). |
| Aspergillus-specific IgE / IgG | Shows how strongly your immune system is reacting to the fungus. |
| Eosinophil count | Measures allergic immune activity (should fall if your biologic is working). |
| Aspergillus culture or PCR (sputum) | Shows whether fungal growth has increased or returned. |
| Antifungal drug level (itraconazole, voriconazole, etc.) | Confirms whether your medication is at a helpful level in your bloodstream. |
If you feel your symptoms are worsening, you can ask your GP or respiratory nurse if these blood tests can be arranged, even if your specialist clinic is hard to reach.
💉 4. When you’ve just started a biologic
Biologics such as Benralizumab, Mepolizumab, Omalizumab, or Dupilumab work by reducing inflammation in the lungs — but they take time.
What to expect
-
Most people don’t notice big changes after the first dose.
-
Benefits usually appear after 2–3 injections, sometimes longer.
-
You may start to notice less sputum, fewer wheezy days, and more energy over time.
If your breathing still feels difficult after a few doses, your team might review whether this biologic is the best one for you or whether something else is going on.
🧭 5. Keeping track between appointments
When clinic visits are months apart, self-monitoring helps fill the gap.
You can:
-
Keep a symptom diary — note breathlessness, cough, mucus colour, temperature, and how often you need rescue inhalers.
-
Record any oxygen readings if you use a pulse oximeter.
-
Note when you take antifungals and biologic injections.
-
Share this record at your next appointment — it helps your team see the bigger picture.
If you feel abandoned, remember you can still contact your hospital team or ask your GP for basic bloods. These can often be shared with your specialist for advice.
❤️ 6. When you feel alone
Many people with aspergillosis describe long stretches of “self-management.”
That’s why patient support networks (like NAC CARES) exist — to give you a space to talk, ask questions, and share what works.
No one should have to manage this alone.
🕊️ 7. Quick summary
| Possible reason for feeling worse | What you can do |
|---|---|
| Airway irritation after clearance | Use bronchodilator first; ask physio about technique |
| Inflammation or allergic flare | Ask for IgE and eosinophil tests |
| Antifungal not at right level | Ask for a blood level check |
| Early days of biologic treatment | Give it more time; track symptoms |
| Infection or fungal regrowth | Ask for sputum culture or PCR |
🌱 Remember:
Feeling worse doesn’t always mean you’re getting worse — but it’s always worth checking.
The right information (blood tests, drug levels, and a clear plan) can turn a worrying spell into a step forward.
Understanding and Controlling Your Immune System
How your immune system works
Your immune system is your body’s built-in defence and repair network.
It protects you from infection, clears away damaged cells, and helps you heal after illness or injury. But it’s also connected to almost every part of the body — your brain, gut, hormones, and even mood.
When finely balanced, it keeps you healthy. When it becomes over- or under-active, it can cause inflammation, allergies, or long-term conditions such as ABPA or asthma.
🧠 1. Brain and nerves
-
Normal role: Immune cells in the brain (called microglia) keep nerve circuits healthy and remove damaged cells.
-
When things go wrong: Too much inflammation can cause fatigue, “brain fog,” anxiety, or depression — feelings many people experience during infection or flare-ups. Long-term inflammation is linked to memory problems and slower recovery after illness.
❤️ 2. Heart and blood vessels
-
Normal role: Immune cells repair vessel walls and help wounds heal.
-
When things go wrong: Chronic inflammation can thicken arteries (atherosclerosis) or cause rare problems like vasculitis, which affects blood flow. Balancing inflammation helps protect heart and circulation health.
🫁 3. Lungs and airways
-
Normal role: The immune system protects your lungs from germs, clears dust, and repairs tissue after irritation.
-
When things go wrong:
-
In asthma or ABPA, the immune system overreacts to harmless triggers such as Aspergillus spores, pollen, or dust, causing airway swelling, mucus build-up, and breathlessness.
-
In CPA, parts of the immune system struggle to clear fungal infection effectively, leading to chronic inflammation and tissue damage.
Keeping the immune response balanced — not too weak, not too strong — is the key to long-term lung health.
-
🍽️ 4. Gut and digestion
-
Normal role: About 70% of your immune cells live in the gut, where they keep a healthy balance of bacteria and prevent harmful microbes leaking into the bloodstream.
-
When things go wrong: Stress, poor diet, or antibiotics can disrupt this balance, increasing inflammation.
A varied, fibre-rich diet and, in some cases, probiotics can help the gut “educate” the immune system.
💪 5. Muscles, joints, and repair
-
Normal role: Immune cells clear damaged tissue and stimulate repair after exercise or illness.
-
When things go wrong: If the immune system stays “switched on,” joints and muscles can ache or feel weak.
Fatigue in aspergillosis may be partly due to ongoing low-level inflammation.
🧬 6. Hormones and metabolism
-
Normal role: Hormones like cortisol and adrenaline help keep inflammation under control.
-
When things go wrong:
-
Overactive inflammation can worsen insulin resistance, weight changes, and tiredness.
-
Autoimmune problems can affect glands like the thyroid or adrenal glands (Addison’s disease).
Managing stress, sleep, and diet all help the immune-hormonal balance.
-
🩸 7. Blood and bone marrow
-
Normal role: The immune system is built in the bone marrow, producing white cells, red cells, and platelets.
-
When things go wrong: Excessive inflammation raises blood markers such as CRP or eosinophils, often seen during ABPA flare-ups or infection.
Monitoring these levels helps your specialist adjust treatment safely.
🦴 8. Skin and mucous membranes
-
Normal role: Acts as the body’s first barrier, with immune cells ready to seal wounds or fight germs.
-
When things go wrong: Eczema, psoriasis, and slow-healing wounds can occur when immune balance is disturbed — sometimes as side effects of steroids or other medications.
⚖️ 9. The balance between defence and tolerance
The most important job of your immune system is to tell friend from foe — to destroy invaders but leave your own body unharmed.
-
If it overreacts, you get allergies or autoimmune disease.
-
If it underreacts, infections can take hold more easily.
-
In aspergillosis, both problems can occur together: too little defence against fungus, but too much inflammation once the fungus is detected.
🧩 How Medicine Is Learning to Control the Immune System Better
In the past, we only had blunt tools — like steroids — to “calm” inflammation. These saved lives but also caused side effects.
Today, science is learning to control the immune system more precisely, using targeted treatments, cell therapies, and even lifestyle tools that work with your body’s own defences.
🎯 1. Targeted biologic drugs
These are antibodies made in the lab that block one specific immune signal instead of suppressing everything.
Examples used in asthma and ABPA:
-
Mepolizumab and benralizumab block interleukin-5 (IL-5), reducing eosinophil-driven inflammation.
-
Dupilumab blocks IL-4 and IL-13 pathways, calming allergic inflammation.
Other biologics (like infliximab, tocilizumab, and omalizumab) target immune messengers involved in arthritis, eczema, or autoimmune disease.
💉 2. Vaccines and immune training
Vaccines “teach” the immune system to respond safely and efficiently.
New approaches — such as mRNA vaccines — can be updated quickly and may in future be used to retrain the immune system in chronic diseases, allergies, and even cancer.
⚙️ 3. Immune cell therapies and genetic repair
Researchers can now rebuild parts of the immune system:
-
CAR-T cell therapy modifies a patient’s own T cells to find and destroy cancer.
-
T-reg therapy expands the body’s natural “peacekeeping” cells to prevent autoimmune attack.
-
Gene editing (CRISPR) aims to correct inherited immune problems or fine-tune overactive responses.
🧠 4. Neuro-immune and stress control
Because the brain and immune system constantly talk, therapies that reduce stress or stimulate specific nerves can influence inflammation.
-
Vagus nerve stimulation devices can reduce gut and joint inflammation.
-
Mindfulness, relaxation, and gentle exercise lower stress hormones and improve immune balance — especially in asthma or ABPA, where stress can trigger flares.
🌿 5. Microbiome and metabolic balance
Your gut bacteria, diet, and metabolism shape immune health.
-
A high-fibre, plant-based diet produces short-chain fatty acids that calm inflammation.
-
Probiotic and prebiotic therapies are being studied to restore immune tolerance.
-
Metabolic drugs such as metformin are showing anti-inflammatory effects beyond diabetes care.
🧩 6. Re-teaching immune tolerance
The ultimate goal is to re-educate the immune system so it stops attacking harmless things.
-
Allergen immunotherapy exposes the body to small, increasing doses of allergens to reduce sensitivity.
-
Nanoparticle and peptide therapies are being developed to signal to immune cells that “this is safe,” switching off allergic or autoimmune responses without weakening defences.
👤 7. Personalised immune medicine
Every person’s immune system behaves differently.
-
New blood and genetic tests (“immune phenotyping”) help doctors match patients to the best biologic or antifungal treatment.
-
Artificial intelligence is being used to model individual immune systems — predicting who will respond best to certain drugs.
-
In the future, “immune profiles” may be as common as cholesterol or blood pressure checks.
💬 Living with Aspergillosis: What This Means for You
-
You’re not powerless. Understanding your immune system helps you work with your doctors to find the best balance of antifungal, biologic, and anti-inflammatory treatments.
-
Lifestyle still matters. Stress control, exercise, nutrition, and infection avoidance (e.g. clean air, low mould exposure) all influence immune stability.
-
New hope. Research is rapidly advancing — turning immune control from a guessing game into a precise science.
The same breakthroughs that transformed cancer and autoimmune care are now informing treatments for allergic and fungal lung disease.
🩺 In summary
Your immune system touches every part of your body — lungs, gut, brain, hormones, and skin.
In aspergillosis, it can become both under-protective and over-reactive, creating the delicate balance specialists are trying to restore.
Modern medicine is learning to tune the immune system like an orchestra, not silence it — calming inflammation when it harms you, and strengthening defence when you need it most.
The future of aspergillosis care lies in immune precision — treating not just infection, but the whole system that responds to it.
💨 Airway Clearance and Nebulised Saline
(for ABPA, severe allergic asthma, and bronchiectasis)
Why mucus clearance matters
If you have ABPA (allergic bronchopulmonary aspergillosis), severe allergic asthma, or bronchiectasis:
-
The airways can produce thick, sticky mucus.
-
Mucus may form plugs that block airflow.
-
Trapped mucus increases the risk of flare-ups and infections.
Nebulised saline loosens mucus, but it must be followed by airway clearance to move it out of your lungs.
Airway clearance methods
1. Active Cycle of Breathing Technique (ACBT)
-
A structured cycle of relaxed breathing, deep breaths, and “huffing” (forced breaths out).
-
Very effective when combined with nebulised saline.
2. Devices (Acapella, Flutter, Aerobika, etc.)
-
Use vibrations and back pressure to shake mucus loose.
-
Often recommended alongside ACBT.
3. Traditional physiotherapy techniques
-
Postural drainage – lying in certain positions to use gravity to drain mucus.
-
Chest percussion (clapping) – rhythmic tapping on the chest/back.
-
Assisted coughing – for those who can’t cough strongly.
All these techniques remain valid. The key is choosing the one that works for you.
The role of the respiratory physiotherapist
Your respiratory physiotherapist is central to airway clearance care:
-
They assess your condition (ABPA, asthma, bronchiectasis pattern).
-
They teach and supervise techniques so you can use them safely.
-
They tailor a plan – deciding whether ACBT, a device, drainage, or a mix is best.
-
They adjust your plan over time – for example:
-
During a flare-up with extra mucus
-
If new treatments (like biologics or antifungals) change your symptoms
-
If you develop new bronchiectasis or infections
-
👉 The physio is your partner in protecting your lungs.
How nebulised saline helps
-
Comes in sterile vials (normal 0.9% or stronger “hypertonic” 3–7%).
-
Hydrates and thins sticky mucus.
-
Prepares mucus for clearance with ACBT, devices, or drainage.
-
Sometimes used with a bronchodilator first to avoid wheeze or tightness.
Putting it together
-
Nebulised saline to loosen mucus
-
Airway clearance technique (ACBT, device, drainage) guided by your physio
-
Regular review with your physio to keep the plan up to date
✅ Key takeaway:
For ABPA, severe allergic asthma, and bronchiectasis, the combination of nebulised saline + airway clearance is one of the most effective ways to keep your lungs clearer and healthier. The respiratory physiotherapist will help you find the right method for your lungs and adjust it as your condition changes.
Living Healthier with Aspergillosis: Small Steps That Can Make Life Easier

Living with aspergillosis, whether it is allergic bronchopulmonary aspergillosis (ABPA), chronic pulmonary aspergillosis (CPA), or another form, often means dealing with fatigue, coughing, breathlessness, repeated infections, and the side effects of treatment. Medicines such as antifungals and biologics are central to care, but everyday choices around food, activity, rest, and stress can also make a real difference.
This isn’t about strict rules or being told what you “should” do. It’s about finding small, realistic steps that help you feel stronger and more in control of daily life.
Why healthy habits can feel hard
Many people know what’s “healthy” but still find it difficult to change routines. That’s normal. Habits stick for lots of reasons:
-
Familiar routines feel safe, even if they’re unhelpful.
-
Stress, tiredness, or sadness can make comfort eating or smoking feel like a quick fix.
-
Friends, family, and culture shape our patterns.
-
Healthy food or exercise can seem expensive or time-consuming.
-
Mood and motivation play a huge part — especially if you’re already coping with illness.
Understanding why change is tough is the first step. You’re not failing — you’re human.
The potential benefits of living a little healthier
-
Easier breathing → avoiding smoke and doing gentle activity can help your lungs cope better.
-
Fewer flare-ups and infections → nourishing food, better sleep, and stress control support your immune system.
-
More energy → balanced eating and regular movement often boost stamina and reduce fatigue.
-
Treatments working better → some habits (like smoking or alcohol) interfere with antifungals; avoiding these can make medicines more effective.
-
Improved mood → routines such as exercise, cooking, or group activities can ease anxiety and give a sense of connection.
Diet and weight: it’s about health, not the scales
When weight feels like the focus
Many people are told to lose weight, but strict weight-loss diets rarely succeed in the long term. They can leave people frustrated or feeling worse. For aspergillosis, the aim is not chasing numbers on the scales — it’s about supporting your body so you can feel and function better.
Why diets often fail:
-
Cutting things out makes us crave them more.
-
The body resists weight loss by slowing metabolism.
-
Diets feel temporary, not sustainable.
-
One slip can feel like failure.
-
Stress and emotions drive food choices as much as hunger.
Breaking that cycle
Some people find it more helpful to:
-
Focus on health gains (more stamina, fewer infections, better mood) instead of weight loss.
-
Make small, sustainable swaps they can keep for years.
-
Add nourishing foods (protein, fruit, vegetables) instead of strict restriction.
-
Notice and celebrate everyday wins — walking further, coughing less, sleeping better.
When the struggle is keeping weight on
Not everyone has weight to lose. For some, infections, inflammation, and the effort of breathing can burn through calories, making it hard to maintain weight. In that case, the goal shifts to adding in extra energy and protein:
-
Eat smaller portions more often.
-
Fortify food with milk powder, cheese, cream, nut butters, or olive oil.
-
Keep calorie-rich snacks handy (flapjacks, trail mix, smoothies).
-
Try nutritional drinks (Fortisip, Ensure, or homemade shakes).
-
Ask your team for dietitian support if weight keeps dropping.
When to seek specialist help
General lifestyle tips are a useful starting point, but some people face severe or complex dietary problems. These can include:
-
Ongoing or severe weight loss / malnutrition
-
Difficulty swallowing or digesting food
-
Drug–food interactions (e.g. antifungals with certain juices or stomach acid medicines)
-
Other health conditions (diabetes, coeliac disease, kidney problems)
-
Persistent nausea, diarrhoea, or appetite loss from treatment
If this sounds familiar, the best step is to ask for a referral to a registered dietitian. A dietitian can:
-
Create a personalised nutrition plan to match your energy and protein needs
-
Suggest practical adjustments if eating is difficult
-
Ensure your plan is safe alongside antifungal or steroid treatment
-
Provide access to prescription nutritional supplements if needed
-
Monitor progress and adjust over time
What works for one patient may not be safe for another — professional advice ensures the plan is right for you.
Gut health and the microbiome
There’s growing interest in the link between the gut and the lungs — sometimes called the gut–lung axis. A healthy gut microbiome (the community of bacteria and other microbes in the digestive system) can support overall immunity and help regulate inflammation, which matters in conditions like ABPA and CPA.
-
Fibre feeds healthy gut bacteria → fruits, vegetables, oats, beans, and nuts help your gut produce anti-inflammatory compounds.
-
Probiotics (live “friendly bacteria” in yoghurts or supplements) may help some people, especially after antibiotics, but the evidence in aspergillosis is still limited.
-
Balance is key → too much fibre all at once can cause bloating; start gradually and pair fibre with calorie-rich foods if you struggle with weight.
-
Hydration matters → fibre works best when you’re drinking enough fluids.
-
Check before supplements → always discuss probiotic products with your team, especially if you are immunocompromised.
Small steps — like adding an extra piece of fruit or trying a yoghurt with live cultures — can gently support gut balance without overloading.
Starting small (and letting it grow)
Big lifestyle overhauls are rarely realistic. A more helpful approach is:
-
Pick one tiny change — a 10-minute walk, one less sugary drink, or a piece of fruit with breakfast.
-
Celebrate the success — each small step builds confidence and momentum.
-
Notice the ripple effect — walking more may improve sleep; better sleep may give more energy for cooking.
-
Climb the ladder slowly — the first step is hardest, but it makes the next ones easier.
Finding support
-
Share your goals with your medical team — they can suggest safe exercise, eating tips, or referrals.
-
Join pulmonary rehab, exercise groups, or online communities — peer encouragement makes a big difference.
-
Explore local schemes — social prescribing, community cooking, or walking groups can be free and welcoming.
-
Remember: mental health matters too. If low mood or anxiety makes change feel impossible, speaking with a GP or counsellor can help unlock progress.
The bottom line
Treatments like itraconazole and benralizumab are essential in controlling aspergillosis, but they work best when supported by healthy routines.
Living healthier means different things for different people:
-
For some, it’s cutting down alcohol or moving a little more.
-
For others, it’s eating enough to keep strength up.
-
For everyone, it’s about supporting your lungs, your body, your gut, and your wellbeing, not chasing numbers or perfection.
Even small, steady steps — chosen by you, at your pace — can add up to meaningful improvements and make daily life with aspergillosis a little easier.
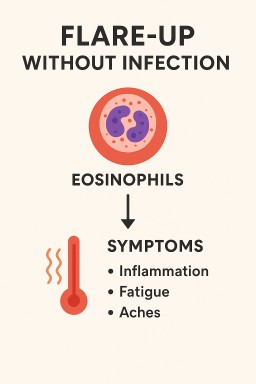
🌿 Why Do Flare-Ups Happen Without an Obvious Infection?
Many people with asthma, ABPA (Allergic Bronchopulmonary Aspergillosis), or other eosinophilic lung conditions describe sudden “crashes” where they feel feverish, inflamed, and completely drained — even when tests don’t show an infection. This can be confusing and worrying, but there is a clear explanation.
🔬 The role of eosinophils
-
Eosinophils are a type of white blood cell that drive allergic and inflammatory reactions.
-
When too many become activated, they release chemicals and proteins that cause:
-
Inflammation in the airways and body
-
Fatigue and muscle aches
-
“Flu-like” symptoms
-
-
In eosinophilic diseases such as ABPA, severe asthma, or EGPA, these episodes are often described as flare-ups.
🧩 Common triggers of flares
-
Stress – both emotional and physical stress can tip the immune system into overdrive.
-
Biologic not yet started – until a biologic (e.g. mepolizumab, benralizumab, tezepelumab) calms eosinophil activity, your immune system may stay “over-reactive.”
-
Mechanical strain – back pain, muscle strain, or other physical problems can amplify inflammation.
-
Minor viral infections – even a tiny cold virus, too mild to register on tests, can trigger eosinophil-driven inflammation.
📉 Why symptoms come and go
-
Many patients feel very unwell at home (fever, aches, exhaustion), but by the time they see a doctor, their vital signs look normal again.
-
This doesn’t mean the flare wasn’t real. Eosinophil flares often burn out quickly, leaving behind fatigue and soreness that can last for days.
⚠️ When to seek medical advice
Contact your healthcare team if you notice:
-
Persistent or high fever
-
Worsening shortness of breath
-
New or increased cough
-
Chest pain
These may signal an infection or another complication that needs treatment.
✅ Key message
Yes — high eosinophils can cause flare-ups that feel like sudden illness without infection. Many patients describe exactly this: sudden feverishness, inflammation, aches, and feeling “knocked flat” for a few days.
Biologic medicines are designed to reduce eosinophil activity, helping to cut down the number and severity of these flares.
🌿 Covid-19 and ABPA / Bronchiectasis: What Patients Need to Know
Many patients with ABPA, bronchiectasis, and asthma ask:
“If I test positive for Covid, am I at higher risk, and do I need antivirals or steroids?”
“Is Covid still a dangerous infection now that everyone has had it many times?”
Here’s what’s important right now.
🎯 Why you may be at higher risk
Having ABPA, bronchiectasis, or asthma doesn’t guarantee severe illness, but it does put you at higher risk compared to the average healthy adult. This means you are more likely to experience:
-
More severe Covid illness – infections can trigger worse chest symptoms (wheeze, shortness of breath, cough).
-
Secondary infections – bronchiectasis makes it easier for bacteria to grow in mucus after a viral infection.
-
Flares of existing disease – Covid can set off asthma attacks or ABPA flare-ups.
-
Slower recovery – fatigue, breathlessness, and extra sputum can last longer.
⚠️ Important: “Higher risk” does not mean you will definitely become very unwell. Many people with chronic lung disease still have mild Covid and recover fully at home.
✅ Current Covid treatments in the UK (2025)
-
Antivirals / monoclonal antibodies
-
People with conditions like ABPA, bronchiectasis, or severe asthma may be eligible for medicines such as Paxlovid or Molnupiravir.
-
These must usually be started within 5 days of symptoms or a positive test.
-
Access is through the NHS Covid Medicines Delivery Unit (CMDU), often arranged via NHS 111 or your GP.
-
-
Steroids
-
Oral steroids (prednisolone) are not routinely given for Covid unless oxygen levels drop, or you already take them for your lung condition.
-
If your asthma/ABPA flares, follow your specialist’s guidance on when to start rescue steroids.
-
-
Antibiotics
-
Covid is viral, so antibiotics don’t treat it directly.
-
But if your doctor suspects a bacterial infection (e.g. in bronchiectasis), they may prescribe something like doxycycline.
-
🧾 Practical steps if you test positive
-
Call NHS 111 or your GP: Tell them you have ABPA/bronchiectasis/asthma and ask about referral for antivirals.
-
Monitor symptoms closely:
-
Use a pulse oximeter if you have one (seek help if oxygen ≤94%).
-
Watch for worsening breathlessness, chest pain, or confusion.
-
-
Keep safe at home: Ventilate rooms, use masks if possible, and wash hands often — though once exposed, focus mainly on monitoring and treatment.
🚨 When to seek urgent help
-
Severe shortness of breath
-
Oxygen levels ≤92–94%
-
Chest pain, confusion, or sudden collapse
→ Call 999
❓ Is Covid still dangerous in 2025?
Why it feels less dangerous now
-
Vaccination and immunity: Most people have had jabs and multiple infections, so later bouts are usually milder.
-
Variants: Current strains spread more easily but often cause less pneumonia than the original virus.
-
Better treatments: Antivirals and steroids (when needed) are widely available.
Why it can still be dangerous
-
Vulnerable groups: People with lung disease, weakened immunity, or older age are still more likely to need hospital care.
-
Exacerbations: Even mild Covid can set off asthma or ABPA flares, or worsen bronchiectasis infections.
-
Long Covid: Some people continue to develop fatigue, breathlessness, or brain fog lasting weeks to months.
-
Hospital admissions: Lower than during the pandemic, but NHS hospitals still see severe cases every winter.
👉 In summary: For most healthy people, Covid now feels like a bad cold or flu. For people with ABPA, bronchiectasis, or severe asthma, it can still be a dangerous infection — which is why monitoring and access to antivirals remain important.
✅ Key message
With ABPA and bronchiectasis, you are more vulnerable to complications from Covid. Most people still recover at home, but you may be eligible for antivirals. Steroids are only used if your underlying condition flares or if your oxygen drops. Stay alert, act quickly if symptoms worsen, and reach out for NHS support as soon as you test positive.
🌿 Coping with Exhaustion When Tapering Prednisolone
Coming off prednisolone can leave you feeling unusually tired. This happens because:
-
Your body’s own adrenal glands have been “asleep” while steroids did the work.
-
As the dose drops, your body needs time to start making its own cortisol again.
-
Tiredness and low energy are the most common symptoms during this adjustment.
✅ Tips that may help
1. Pace yourself
-
Don’t expect full energy straight away.
-
Break tasks into smaller chunks, with rests in between.
-
Use a “little and often” approach for activities.
2. Prioritise rest and sleep
-
Listen to your body: extra rest is part of recovery, not weakness.
-
Try to keep a regular bedtime routine to support natural hormone rhythms.
3. Gentle movement
-
Light activity (walking, stretching) can actually boost energy and mood.
-
Avoid pushing too hard — overexertion can worsen fatigue.
4. Balanced diet
-
Aim for regular meals with protein, whole grains, fruit/veg.
-
Stay hydrated — dehydration makes fatigue worse.
-
Limit caffeine or sugar “quick fixes” that lead to energy crashes.
5. Monitor stress
-
Emotional stress increases your body’s demand for cortisol.
-
Try calming activities: breathing exercises, mindfulness, or gentle hobbies.
6. Stay in touch with your team
-
If exhaustion is severe, worsening, or you develop dizziness, faintness, low blood pressure, or nausea → contact your doctor urgently.
-
These can be signs your body is struggling with adrenal insufficiency, and your taper may need adjusting.
⚠️ Important reminders
-
Never stop prednisolone suddenly unless your doctor tells you to.
-
Carry a steroid card or alert bracelet if you are tapering — in case of emergencies.
-
If you get unwell (infection, surgery, severe stress), you may temporarily need a higher steroid dose.
👉 Key message:
Tiredness during tapering is very common. Self-care, pacing, and staying in close contact with your healthcare team can help you get through this phase more smoothly.
Why Medicines in the UK Come in Blister Packs – and What’s Being Done About the Waste
Many patients with aspergillosis (or other long-term conditions) notice something frustrating when they collect prescriptions: medicines often come in tiny blister packs, with only a few tablets per box. For example, azithromycin often arrives in boxes of just three tablets. When a longer course is needed, the pharmacy has to give you several boxes – leading to mountains of card and plastic waste.
So why does the UK stick with blister packs instead of using larger recyclable bottles? And is anything being done to cut down on the waste?
Why the UK prioritises blister packs
Blister packs are not just a packaging choice – they are built into how medicines are licensed and regulated in the UK and Europe. The main reasons are:
-
Safety and tamper protection
-
Each tablet is sealed in its own compartment, so it’s clear if a dose has been tampered with.
-
Bottles are harder to secure once opened.
-
-
Stability of the medicine
-
Some drugs break down if exposed to moisture, air, or light.
-
A blister pack protects each tablet until the moment it’s taken, which can extend shelf-life.
-
-
Dosing and adherence
-
Blisters help patients (and carers) see how many doses have been taken.
-
For short antibiotic courses, blister packs help doctors prescribe “one strip = one course.”
-
-
Child safety
-
Blisters are harder for small children to open compared with bottles, even those with child-resistant caps.
-
-
Regulatory approval
-
When a company licenses a medicine, the tests are carried out on that specific packaging.
-
To switch to bottles, companies would have to repeat expensive stability tests and resubmit to the MHRA.
-
These factors explain why UK pharmacies almost always supply the manufacturer’s blister pack, rather than re-dispensing tablets into bottles (as is common in the US).
The problem: waste and inefficiency
While blisters have advantages, they cause problems for patients and the NHS:
-
Waste of card and plastic: multiple boxes and layers of packaging for what could fit into one small bottle.
-
Cost and storage: pharmacies spend time opening and combining packs; patients are left with unnecessary clutter.
-
Recycling difficulties: blister packs are made of mixed plastic and foil, which are very hard to recycle in normal household systems.
What’s being done to reduce packaging waste
There is now a growing effort across the NHS, regulators, and industry to tackle this problem. Key developments include:
1. Greener NHS programme
-
The NHS has pledged to reach net zero by 2040.
-
Medicines are a big part of its carbon footprint, and packaging is specifically highlighted as an area for improvement.
-
Suppliers will increasingly be judged on how sustainable their packaging is when the NHS decides what to buy.
2. Original Pack Dispensing (OPD) reform (England, 2025)
-
From January 2025, pharmacists in England will be allowed to dispense up to 10% more or less than prescribed if it allows them to give patients the full original pack.
-
This reduces the need to cut up blister strips or re-package tablets, helping both safety and efficiency.
3. Extended Producer Responsibility (EPR) for packaging (2025)
-
All large companies must start reporting on the recyclability of their packaging.
-
Packs that are harder to recycle (like plastic-foil blisters) will face higher fees, pushing manufacturers to redesign them.
4. Industry innovation (CiPPPA)
-
A group called the Circularity in Primary Pharmaceutical Packaging Accelerator (CiPPPA) is working with the MHRA and industry to test new blister materials that are easier to recycle.
5. Pharmacy leadership
-
The Royal Pharmaceutical Society and local NHS teams are producing guides for “greener pharmacies,” encouraging steps to reduce medicine and packaging waste.
What this means for patients
Right now, the small packs are still the norm – especially for antibiotics and antifungals. But over the next few years we may start to see:
-
Larger, recyclable pack sizes becoming available.
-
Pharmacies having more flexibility to supply original packs instead of splitting them.
-
New materials being trialled to replace mixed-plastic blisters.
In the meantime, patients can:
-
Return unused medicines (and their packaging) to the pharmacy for safe disposal.
-
Ask their pharmacist if combining packs is possible (sometimes they can reduce excess boxes).
-
Support “greener pharmacy” initiatives by raising awareness of the waste problem.
✅ In short: The UK prioritises blister packs for safety, stability, and child protection, but the waste they generate is a real issue. Change is coming slowly, through NHS net zero commitments, new regulations, and industry projects – but for now, patients still see the frustration of multiple half-empty boxes.