🌿 Aspergillosis in the Sinuses (Allergic Fungal Rhinosinusitis – AFRS)
It’s quite possible for Aspergillus to affect both the lungs and the sinuses.
The sinuses are small air-filled spaces behind the nose, eyes, and cheeks that normally drain mucus freely. When Aspergillus spores become trapped there, they can trigger an allergic or inflammatory reaction — rather like ABPA in the lungs.
This allergic form is called Allergic Fungal Rhinosinusitis (AFRS).
It isn’t a contagious infection — it’s an overreaction of the immune system to fungal spores. Over time, it can lead to thick mucus, nasal blockage, and sometimes nasal polyps.
🩵 Common symptoms
-
Persistent nasal congestion or blockage
-
Thick or sticky mucus (sometimes with brown or dark flecks)
-
Reduced or lost sense of smell
-
Facial pressure, pain, or fullness (especially around the eyes or cheeks)
-
Post-nasal drip (mucus running down the throat)
-
Fatigue or worsening asthma symptoms
🔬 Diagnosis
-
CT scan of the sinuses – shows thickened or blocked areas
-
Nasal endoscopy – a tiny camera used to look inside
-
Fungal culture or microscopy from mucus samples
-
Blood tests – sometimes show raised total IgE or Aspergillus-specific IgE
💊 Treatment
-
Topical nasal steroids (sprays or rinses) or short courses of oral steroids to reduce inflammation
-
Saline rinses to help keep the sinuses clear
-
ENT surgery if sinuses are blocked or filled with thick fungal debris
-
Antifungal medication in some cases, especially if fungal growth is confirmed
🌸 The Main Types of Aspergillus Sinus Disease
There are several recognised types of sinus aspergillosis. Most people with ABPA or asthma experience only the allergic form (AFRS).
1️⃣ Allergic Fungal Rhinosinusitis (AFRS)
-
Caused by an allergic reaction to Aspergillus
-
Leads to inflammation, thick mucus, and polyps
-
Non-invasive – the fungus stays on the surface
-
Managed with steroids, nasal rinses, and sometimes surgery
✅ This is the type most relevant for ABPA patients.
2️⃣ Fungal Ball (Mycetoma)
-
A clump of fungus (usually A. fumigatus) in a single sinus, often the cheek (maxillary) sinus
-
Common in otherwise healthy people
-
Causes chronic congestion or facial pain
-
Treated surgically – antifungals rarely needed
-
Not allergic and not invasive
3️⃣ Invasive Aspergillus Sinusitis
-
Rare, seen mostly in people with severely weakened immunity (e.g., chemotherapy, bone marrow transplant, uncontrolled diabetes)
-
The fungus invades surrounding tissue and blood vessels
-
Causes severe facial pain, swelling, fever, sometimes affecting the eyes
-
Needs urgent treatment with antifungal drugs and surgery
⚠️ Very rare in people with ABPA or CPA.
🤝 Specialist care
If you have lung aspergillosis (such as ABPA or CPA) and start noticing more nasal congestion, sinus pressure, or post-nasal drip, it’s sensible to mention it to your respiratory or mycology team.
At the National Aspergillosis Centre (NAC), sinus disease is often co-managed by ENT surgeons, respiratory physicians, and mycology specialists, ensuring coordinated care.
With the right combination of treatments — and early recognition of symptoms — most people find their sinus symptoms improve, and controlling sinus inflammation can even help with overall breathing and energy.
🩵 Coughing and Aspergillosis: Why You Might Still Cough Even When You Feel Well
Many people living with Allergic Bronchopulmonary Aspergillosis (ABPA) or bronchiectasis notice that they still cough regularly — even when their blood tests and scans show their condition is stable. It can be confusing to feel well and yet still have daily coughing or occasional coughing fits.
This article explains why that happens and when you should be concerned.
🌿 Why coughing can continue between flare-ups
ABPA and other forms of aspergillosis can cause long-term changes in the airways. Even when the allergic inflammation has settled and your Immunoglobulin E (IgE) levels are back to baseline, the airways may remain a little widened or scarred. This means:
-
Mucus can collect in the airways more easily.
-
The lining of the bronchi can stay slightly “twitchy” or reactive.
-
Your lungs may continue to produce small amounts of sticky, clear mucus that needs to be cleared out.
Coughing is your body’s way of keeping those airways clear — so a light, regular cough can actually be a sign that your lungs are doing their job.
💨 Why you might not cough during exercise
Many patients notice something surprising:
“I can walk or exercise in the gym for a couple of hours without coughing at all — but later, I get a coughing fit and bring up mucus.”
This is quite normal. When you exercise, you breathe more deeply and more rapidly. This helps:
-
Keep the airways open
-
Move mucus towards the larger airways
-
Reduce the irritation that triggers coughing
When you stop exercising, mucus that’s been loosened can settle again — and that’s often when a coughing fit happens to clear it out. It’s part of your lungs’ natural “housekeeping” system.
🌬️ What you can do to help
-
Stay active: Gentle exercise is good for your lungs. It keeps the airways open and improves mucus clearance.
-
Hydration helps: Drinking enough water or warm fluids keeps mucus less sticky.
-
Airway-clearance techniques: Ask your physiotherapist about huff coughing or devices like the Aerobika or Acapella, which help loosen and move mucus.
-
Watch for changes:
-
Mucus turning yellow, green, or brown
-
Increased shortness of breath or fatigue
-
A rise in IgE or worsening symptoms
-
If any of these occur, contact your respiratory or mycology team — it might mean an infection or early flare-up.
💙 The key message
A mild, regular cough between flare-ups is normal for many ABPA or bronchiectasis patients.
It doesn’t mean your condition is worsening — it’s often your lungs simply clearing secretions.
If your IgE levels are stable and you feel well, that’s a strong sign your disease is under good control.
💚 Living With Aspergillus fumigatus and Starting Antifungal Treatment
Question: “I have Aspergillus fumigatus and I’d like to ask a few questions.
After starting antifungal treatment, how long did it take before you noticed improvement or a stop in the bleeding cough?
Has anyone reached a stable condition or full recovery?
Please share your experiences — it would really help to hear from you.” 💚
🌿 A Supportive Note
Many people ask this question when they first begin treatment — and it’s a very normal concern. Aspergillus fumigatus can cause a range of lung problems such as chronic pulmonary aspergillosis (CPA), aspergilloma, or Allergic Bronchopulmonary Aspergillosis (ABPA), and each responds differently to antifungal therapy.
Improvement can take time and patience.
Some notice changes within weeks, while for others, it can take several months before symptoms start to ease or stabilise.
💊 Understanding How Antifungal Treatment Works
Antifungal medicines — such as itraconazole, voriconazole, or posaconazole — don’t destroy Aspergillus overnight.
They work by slowing or stopping fungal growth, allowing the body’s immune system and lung healing processes to gradually take over.
Because these infections are often chronic, the goal is usually to:
-
Control symptoms
-
Prevent further damage
-
Reduce inflammation and flare-ups
-
Stabilise lung function
For most patients, this means aiming for long-term stability rather than complete eradication of the fungus.
⏳ How Long Before You Feel Better?
Every patient is different, but this is a general pattern doctors often see:
| Time after starting treatment | What you might notice |
|---|---|
| First few weeks | Some reduction in coughing or mucus; fewer night sweats; side effects settling as your body adjusts. |
| 1–3 months | Energy may start to improve; less coughing or blood in sputum; breathing slightly easier. |
| 3–6 months | Signs of stability — symptoms no longer worsening, CT scans showing improvement, or blood markers (e.g. Aspergillus IgG) falling. |
| 6–12 months | Some people achieve remission or long-term stability. For others, antifungal therapy continues as maintenance. |
If you have a fungal ball (aspergilloma), improvements are often slower, and sometimes bleeding episodes take longer to settle.
🩸 About Bleeding (Haemoptysis)
Coughing up blood can be one of the most distressing symptoms.
It usually improves once antifungals reduce inflammation, but if bleeding continues:
-
Doctors may prescribe tranexamic acid to help the blood clot more easily.
-
In some cases, embolisation (a targeted procedure to seal a bleeding blood vessel) may be needed.
-
Ongoing bleeding should always be reported — even small amounts — so your team can reassess treatment or check for infection changes.
🫁 Why “Stable” Can Be a Positive Outcome
Although “cure” is possible in some early or mild cases, most people live with aspergillosis as a chronic condition.
With consistent antifungal therapy, airway clearance, and monitoring, many reach a stable stage — where symptoms are minimal, life feels more predictable, and flare-ups are rare.
This stability is a real success.
It means your body and treatment are keeping the infection under control, preventing further lung damage.
💚 Real Experiences
Patients often describe:
-
Energy and breathlessness improving slowly
-
Bleeding stopping after several months
-
A new sense of normality once medication side effects settle
Some take antifungals for a set course (e.g. 6–12 months), while others remain on long-term maintenance to stay stable.
It’s common for treatment to be adjusted based on blood levels, side effects, or new sputum results.
💬 Patient Voices
Many people in our community say they wish they’d known:
-
“Improvement isn’t quick — it’s gradual, but it does come.”
-
“Side effects can be managed — don’t stop without advice.”
-
“It’s okay to ask your team what ‘stable’ looks like for you.”
-
“You’re not alone — others have been through this too.”
🧭 Looking After Yourself Along the Way
-
Keep up airway clearance (physiotherapy, saline nebulisers, or airway devices).
-
Attend regular clinic appointments for blood levels and liver tests.
-
Report side effects early — dose adjustments or switching antifungals often helps.
-
Maintain good nutrition and hydration.
-
Reach out for emotional support. Living with a chronic infection can be mentally exhausting; anxiety and fatigue are common.
💬 We’d Love to Hear From You
If you’ve been through antifungal treatment, please share your story:
-
How long it took before you felt a difference
-
What helped you most
-
How you manage side effects or flare-ups
Your experience could make a real difference to someone who’s just starting this journey. 💚
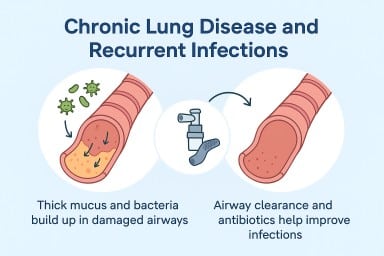
💨 Why Chest Infections Keep Coming Back — and What Can Help
Lisa asks:
“Hi, how do you get rid of chest infections? I had one, and the doctors gave me Clarithromycin. It didn’t clear, so they did a sputum test — it showed Haemophilus influenzae. Then I was given Co-trimoxazole, but that didn’t clear it either. The next test still showed it, so now I’m on Amoxicillin. Is this normal? I’m losing hope of it ever going away.”
💬 You’re Not Alone, Lisa
It’s very common for people with aspergillosis, bronchiectasis, or chronic lung disease to find that chest infections take a long time to clear.
Even with the right antibiotics, infections like Haemophilus influenzae can hang on for weeks or even months — but that doesn’t mean treatment isn’t working.
🦠 Why These Infections Keep Coming Back
-
Thick mucus and biofilms:
In damaged airways, bacteria can hide deep in sticky mucus or biofilms (protective layers). This makes them hard to reach, even with antibiotics. -
Narrow or scarred airways:
In bronchiectasis and aspergillosis, parts of the lung don’t drain properly, so infection pockets linger. -
Reinfection rather than relapse:
Sometimes, you clear one infection but pick up another of the same type from your own airways later. -
Inflammation:
Even when bacteria are gone, airway inflammation can cause ongoing cough and sputum, making it feel as if the infection hasn’t cleared.
💊 Why Doctors Change Antibiotics
Each antibiotic works in a different way.
Your team chooses them based on sputum culture results, which show which antibiotics your bacteria are sensitive to.
It’s quite normal to:
-
Start with a broad antibiotic (e.g. clarithromycin)
-
Switch after sputum results come back
-
Need longer or combination treatment if infection persists
For people with chronic lung conditions, antibiotic courses may last 2–3 weeks, not the usual 5–7 days.
💨 What Can Help You Recover
-
Regular airway clearance:
Using devices like an Acapella, Aerobika, or chest physiotherapy helps move mucus out of the lungs. This allows antibiotics to reach infection sites better. -
Stay hydrated to keep mucus thin.
-
Nebulised saline (if prescribed) can help loosen secretions.
-
Avoid skipping doses — consistent antibiotic levels help stop bacteria from regrowing.
-
Regular sputum tests guide your doctors in choosing the next best treatment.
-
See your specialist team if infections return frequently — they might check for fungal infection, resistant bacteria, or airway blockages.
❤️ The Take-Home Message
Yes — it’s quite normal for lung infections like Haemophilus influenzae to need several antibiotics and take time to clear when you have chronic lung disease.
It doesn’t mean your body isn’t fighting — it just means your lungs need a bit more help.
Keep in touch with your specialist nurse or clinic, and don’t lose hope — with good airway care, the right antibiotics, and patience, things usually improve.
🌟 Vitamin B12 (Cobalamin) and Iron – What Patients Should Know
People living with chronic lung or fungal conditions sometimes develop low vitamin B12 or iron, especially if appetite, diet, or absorption are affected.
Here’s how to understand your results and treatment options.
🌟 Vitamin B12 (Cobalamin)
✅ What’s a Normal B12 Level?
| Level (pmol/L) | What It Means |
|---|---|
| > 300 | Normal |
| 200–300 | Borderline – may need extra tests (e.g. MMA or homocysteine) |
| < 200 | Deficiency likely |
Some labs report B12 in ng/L — the ranges are similar. Your doctor will interpret them based on the lab reference range.
⚠️ What Happens If B12 Is Low?
Low B12 can cause:
-
Fatigue and weakness
-
Brain fog or memory issues
-
Numbness or tingling in hands or feet
-
Low mood or irritability
-
In severe cases, nerve damage
💉 B12 Treatment
| Cause | Typical Treatment |
|---|---|
| Dietary deficiency (e.g. vegan diet) | High-dose oral B12 tablets or injections |
| Pernicious anaemia (autoimmune) | Lifelong B12 injections every 8–12 weeks |
| Malabsorption (gut issues) | Long-term injections often required |
In the UK, injections are usually hydroxocobalamin 1 mg every 2–3 months for maintenance, after an initial “loading phase” (several doses over 2 weeks).
🌟 Iron (Ferritin and Haemoglobin)
✅ Key Iron Markers
| Test | Normal Range (Women) | What Low Levels Mean |
|---|---|---|
| Ferritin | 30–200 µg/L (some doctors prefer >50) | Reflects iron stores — low = iron deficiency |
| Haemoglobin | 120–160 g/L | Measures oxygen-carrying capacity — low = anaemia |
You can have low iron without anaemia (low ferritin, normal Hb) or both together.
💉 Iron Infusions (e.g. Ferinject)
Used when:
-
Iron tablets don’t work or cause side effects
-
Iron levels are very low or symptoms severe
-
Ongoing blood or iron loss (e.g. heavy periods, inflammatory bowel disease)
Iron infusions raise levels more quickly than tablets. Some people need repeat infusions every 6–12 months depending on the cause.
🔄 Ongoing Monitoring and Follow-Up
| Condition | Typical Follow-Up |
|---|---|
| Low B12 (pernicious anaemia) | Injections for life; blood tests yearly |
| Low B12 (diet-related) | May stop if diet improves and levels remain stable |
| Iron deficiency (no bleeding cause) | Tablets for 3–6 months, then reassess |
| Chronic iron loss (e.g. periods, IBD) | Maintenance iron or repeat infusions |
✅ Reliable Information Sources
📣 Final Advice
If you’re unsure about your test results or treatment:
-
Ask your GP for a copy of your blood test results
-
Request a referral to a dietitian or haematologist
-
Agree a treatment plan and review dates
Always let your healthcare team know if you’re feeling more tired, dizzy, or unwell — sometimes simple tests and supplements make a big difference.
💬 Healthwatch: Your Local Voice in the NHS
Living with a long-term lung condition such as aspergillosis, asthma, or bronchiectasis often means regular contact with hospitals, GPs, and community clinics.
Sometimes things work well — and sometimes they don’t.
That’s where Healthwatch comes in.
Healthwatch is an independent organisation that represents patients and the public.
It exists to make sure your experiences help shape the way NHS and social-care services are delivered.
🏛️ What is Healthwatch?
Healthwatch was set up by law to be the official voice of patients and the public in health and social care.
There are two levels:
-
Healthwatch England – works nationally to influence NHS and government policy
-
Local Healthwatch – works in every local authority area across England, gathering feedback from people using local services
Healthwatch is not part of the NHS, and it’s not a complaints service, but it does have statutory powers to:
-
Listen to people’s experiences of care
-
Report issues and make recommendations to the NHS, local councils, and care providers
-
Request responses from organisations it investigates
-
Escalate serious concerns to the Care Quality Commission (CQC)
Learn more on the Healthwatch website.
🌿 Why Healthwatch matters to aspergillosis patients
People living with chronic lung disease often face delays, limited understanding, or difficulties accessing ongoing support.
Healthwatch helps make sure those experiences aren’t ignored.
1. Raising the patient voice
You can share your experience of healthcare — good or bad — with your local Healthwatch.
They collect stories from across the community and use them to:
-
Identify patterns (for example, problems with accessing respiratory clinics or antifungal monitoring)
-
Produce reports and recommendations for local NHS decision-makers
-
Push for improvements to long-term care pathways and community support
2. Helping to improve new neighbourhood health hubs
As NHS care moves into the community, Healthwatch plays a key role in making sure new Neighbourhood Health Hubs are:
-
Accessible for people with limited mobility or oxygen needs
-
Located where public transport and parking work for patients
-
Designed with chronic-illness patients in mind, not just short-term care
You can feed in your ideas through Healthwatch about what’s working and what isn’t in new NHS community models.
3. Providing information and signposting
If you’re unsure where to go for care — GP, hospital, or new health hub — or how to complain or appeal a service decision, Healthwatch can point you in the right direction.
They offer clear, local information about:
-
NHS patient transport
-
The Healthcare Travel Costs Scheme (HTCS)
-
Local support groups and community services
4. Supporting patient involvement
Healthwatch works with NHS organisations to include patients and carers in planning and reviewing services.
If you’d like to get involved as a patient representative or share your experience of aspergillosis services, Healthwatch can help you join local working groups or consultations.
5. Spotlighting inequalities
Healthwatch highlights where certain groups are left behind — for example:
-
People with rare or complex conditions
-
Patients in rural or deprived areas
-
Those unable to use digital appointment systems
This helps ensure people with chronic lung conditions are not overlooked when new community-care models are designed.
⚖️ What Healthwatch can — and can’t — do
| ✅ Healthwatch can | 🚫 Healthwatch can’t |
|---|---|
| Collect and report your experience to NHS leaders | Fix individual clinical problems directly |
| Influence NHS and council decisions | Guarantee faster treatment or appointments |
| Provide advice on local services and support | Replace legal or complaints services |
| Escalate major safety concerns to the CQC | Act as your personal advocate in disputes |
Even so, their influence can be powerful — many improvements in NHS access and transport have started with patient stories collected by Healthwatch.
📍 How to contact your local Healthwatch
Every local area has its own Healthwatch website and phone number.
You can find yours at:
👉 Find your local Healthwatch
When you contact them, you can:
-
Fill in a short online form to share your story
-
Ask to join a focus group or consultation
-
Request accessible information or help finding services
-
Subscribe to local updates and reports
If you’d like support from the aspergillosis community, NAC CARES can also help you write or submit your feedback.
💬 Why this matters
“Nothing about us without us.”
Healthwatch exists so that patients — including those with rare and chronic conditions like aspergillosis — can make their experiences count.
By telling your story and feeding back to Healthwatch, you help shape better care for yourself and for others who will face similar challenges in future.
🎢 Life as a Patient

Living with chronic illness is often described as a journey, but that word can feel far too calm. In truth, it’s more like a modern roller coaster — fast, unpredictable, and full of twists that catch you off guard.
There are the high climbs, when medication works, energy returns, and hope builds quietly in your chest. Then there are the sudden drops, when symptoms flare, infections hit, or test results turn against you. But what really defines the experience are the loops and spirals — the disorienting moments that spin you upside down, when you’re not sure which way is forward, or how long it will take to steady yourself again.
Each turn tests your courage, your patience, and your ability to keep holding on. Sometimes you’re screaming inside while smiling on the outside. Other times, you find small moments of stillness even as the track twists beneath you — the deep breath between the storms.
And through it all, you learn:
-
To adapt rather than control.
-
To brace and breathe rather than fight every turn.
-
To appreciate those who stay beside you in the carriage, even when the ride is rough.
The roller coaster of illness is not one anyone chooses to board. But it teaches something profound — that strength isn’t about never being scared; it’s about showing up, again and again, when the world flips upside down.
Living Between What My Body Needs and What the World Expects

Sometimes it feels as if people grow tired of hearing about illness or fatigue. They encourage us to “think positively,” as if mindset alone could repair the body or quiet exhaustion.
But chronic illness doesn’t work like that. It’s a daily negotiation between two inner voices — one saying, “You need to rest,” and the other whispering, “You still have responsibilities.” That constant tug-of-war leaves many of us feeling trapped between what our body needs and what life demands.
Even small things — such as changes in weather, sleep patterns, or stress — can tip the balance. We learn to pace ourselves, to weigh every decision, to ration energy. And still, the world around us often sees only the surface: “You look well.”
The Other Side of Positivity
For those who don’t live with chronic illness, this can be difficult to face. Often, people cling to optimism not because they’re unkind, but because they don’t want to confront the truth — that illness can be long-term, unpredictable, and out of anyone’s control.
Positivity can become a shield: a way of keeping the world steady and reassuring when faced with something that can’t be fixed. Saying “You’ll be fine” or “Stay strong” helps them feel hopeful, even if it leaves us feeling unseen.
Understanding that this comes from discomfort, fear, or helplessness rather than indifference can make those moments a little easier.
Where Real Connection Starts
Real empathy sits somewhere between positivity and honesty — where people can acknowledge pain without losing hope.
Most of the world won’t fully understand chronic fatigue or the mental gymnastics it takes to stay balanced until they experience it themselves. But by sharing what it’s really like, we give others the chance to learn — just as society learns to understand invisible struggles like dyslexia or digital exclusion.
Understanding begins when we listen without needing to fix. Sometimes the greatest kindness is simply to say, “That sounds hard — how are you managing today?”
Aspergillus Saga — July 2024 to June 2025: Searching for the Invisible
In this compelling personal account, a patient describes her year-long journey battling what ultimately was identified as subacute invasive aspergillosis. She walks us through months of worsening symptoms, repeated rounds of antifungals, diagnostic uncertainty, and the pivotal decision to undergo lung surgery. The turning point: removal of a single lesion led to a rapid resolution of systemic infection signs, with follow-up therapy and monitoring guided by her infectious disease team. Her story highlights how, with very little precedent in medical literature, patients and clinicians sometimes must walk together on uncharted ground.
👉 Read the full article here:
“Aspergillus Saga – July 2024 to June 2025: Searching for the Invisible” Beauty for Ashes
🧩 NAC Aspergillosis Research Digest — Focus: Chronic Aspergillosis (October 2025: week 42)
🧬 Focus Review — Chronic Aspergillosis (October 2025)
Here are peer-reviewed papers on chronic aspergillosis published in the last month:
1. Improving Diagnostic Sensitivity Using Species-Specific IgG (Sep 2025)
-
This study investigated better blood tests to diagnose CPA by measuring IgG antibodies not just to Aspergillus fumigatus but also to other common Aspergillus species.
-
They found adding antibodies against non-fumigatus species identified more CPA cases that would have been missed by the standard A. fumigatus test alone.
-
The treatment results were similar regardless of which Aspergillus species was involved.
-
This means broader antibody testing improves diagnosis without changing expected outcomes.
- Read full paper on PubMed
2. Prevalence and Impact of Bacterial Co-infections in CPA (April 2025)
-
This study looked at how often bacterial infections occur alongside CPA and their effect on patients.
-
About 21% of CPA patients had bacterial co-infections.
-
However, having a bacterial co-infection did not significantly change mortality rates compared to those without.
-
This highlights the need to assess for bacteria but suggests it may not worsen long-term outcomes.
- Read full paper on PMC
3. Non-invasive Monitoring Using Serology and HRCT Imaging (June 2025)
-
Researchers combined blood antibody tests and high-resolution chest CT scans to identify active Aspergillus infections in chronic lung disease patients.
-
This method distinguished active infections from colonization without invasive procedures.
-
It supports using combined non-invasive tests to decide who needs further invasive diagnostics or antifungal treatment.
-
This approach helps avoid unnecessary treatments and invasive tests.
- Read full paper on Frontiers
In short: these studies improve how doctors diagnose and monitor CPA — by expanding antibody testing beyond classic targets, recognizing the role but limited impact of bacterial co-infections, and using combined non-invasive testing strategies to guide management safely and effectively.