🌿 Living Well with Aspergillosis: Understanding the Role of Palliative Care
Many people think palliative care is only for those at the very end of life. But that’s a common misconception — especially for people living with aspergillosis, including chronic pulmonary aspergillosis (CPA), ABPA, or aspergillus bronchitis.
Palliative care is not about giving up. It’s about living better, with more comfort, dignity, and control — no matter how far along you are in your illness.
💬 What Is Palliative Care?
Palliative care is specialist medical support for people with serious, long-term, or life-limiting illnesses. It focuses on:
-
Managing symptoms like pain, breathlessness, or fatigue
-
Providing emotional and psychological support
-
Helping you plan ahead for the future
-
Supporting families and carers
✅ It can be given alongside antifungal or active treatments and is not limited to the last weeks or months of life.
🌟 How Can It Help People with Aspergillosis?
People living with aspergillosis often face unpredictable flare-ups, side effects from long-term treatment, hospital admissions, and emotional strain. Palliative care can help with:
✅ 1. Symptom Control
Manage persistent symptoms such as:
-
Breathlessness
-
Chest pain or discomfort
-
Coughing
-
Fatigue
-
Side effects from antifungal or steroid use
✅ 2. Emotional and Mental Health Support
Chronic illness can lead to anxiety, depression, or fear of decline. Palliative teams include trained counsellors and therapists.
✅ 3. Practical Support
Physiotherapists, occupational therapists, and social workers can help with equipment, managing daily tasks, and staying independent.
✅ 4. Family and Carer Support
Caring for someone with aspergillosis can be exhausting and emotionally tough. Palliative care includes carer support, respite advice, and bereavement services.
✅ 5. Planning Ahead
Advance care planning helps you express your wishes for future treatment, care, or emergencies — so your preferences are known and respected.
🧭 Who Can Receive Palliative Care?
Anyone with serious symptoms, emotional distress, or planning needs related to a chronic or progressive illness — even if you’re still on active treatment.
✅ Core criteria include:
-
Ongoing symptoms that are hard to control
-
Emotional or psychological distress
-
Progressive disease or declining health
-
Complex care needs for you or your family
-
Multiple hospital admissions or infections
Tools like the Supportive and Palliative Care Indicators Tool (SPICT) or your GP's Gold Standards Framework register may be used to support a referral, but your experience matters most.
❌ What If You’re Told “You’re Not Ready”?
If you’re told, “you’re not ready for palliative care yet,” remember:
-
Needing help now means you’re ready.
-
Palliative care is about quality of life — not prognosis.
-
It’s common for healthcare professionals to associate palliative care only with end-of-life, but that’s outdated thinking.
💬 What to Say
If dismissed, try:
“I understand palliative care is about improving quality of life at any stage. I’d really value support now with symptoms and planning ahead.”
Or:
“I’m not asking to stop treatment. I want help managing the impact this illness is having on my life.”
If needed, request a second opinion or contact your local hospice directly. Many offer advice even without a referral.
🕰️ When Should I Ask for Palliative Care?
The best time is as early as you feel you need extra support. Don't wait for a crisis.
Research shows that early palliative care:
-
Improves quality of life
-
Reduces hospital visits
-
Can even extend life in some cases
-
Helps you and your loved ones feel more in control
📞 How to Access Palliative Care
| Step | What to Do |
|---|---|
| 1. Talk to your GP or hospital team | Ask if there’s a palliative care or community team you can speak to. You don’t need to be near the end of life. |
| 2. Ask about local services | Find out if there’s a hospice outreach nurse, home visits, or symptom clinic nearby. |
| 3. Contact a hospice directly | Many offer support to people with respiratory conditions, even if you're not staying with them. |
| 4. Ask for a holistic needs assessment | You're entitled to one after being diagnosed with a serious or long-term condition. It can highlight unmet needs. |
| 5. Reach out to charities and support lines | See below for trusted sources of advice and emotional support. |
🧭 Useful Contacts and Resources
-
Marie Curie Support Line: 0800 090 2309 – Emotional and practical advice
-
Macmillan Cancer Support: 0808 808 0000 – Also helps with non-cancer conditions like chronic lung disease
-
Hospice UK Directory: www.hospiceuk.org – Find your local hospice
-
NHS Website: www.nhs.uk – Search “palliative care” for general information
-
Compassion in Dying: www.compassionindying.org.uk – Advance care planning resources
💬 Final Thought
Palliative care is not about giving up — it’s about living well with support. For aspergillosis patients facing ongoing symptoms, uncertainty, or stress, this kind of care can be transformative.
📢 You have the right to ask for help. Don’t wait until someone tells you it’s time — the right time is when you feel you need it.
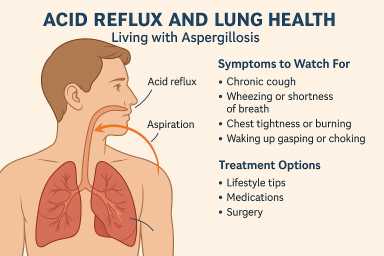
Acid Reflux and Lung Health: What Aspergillosis Patients Should Know
Living with aspergillosis already means managing delicate lung health — so when acid reflux (GERD) or silent reflux (LPR) starts affecting your breathing or causing discomfort, it’s important to know what’s going on and what can be done to help.
This article explains how reflux can impact the lungs, why it may be especially important for aspergillosis patients, and what steps you can take to reduce the risk of further lung irritation or damage.
🔄 What Is Acid Reflux?
GERD (Gastroesophageal Reflux Disease) occurs when stomach acid regularly flows back into the food pipe (esophagus). Sometimes, this acid can reach the throat or even be breathed into the lungs — especially during sleep — causing aspiration. This is more common than people think and is often silent (without heartburn).
🫁 Why Does It Matter for Aspergillosis?
For those with chronic pulmonary aspergillosis (CPA), ABPA, or aspergillus bronchitis, the lungs are already inflamed or damaged. Repeated exposure to stomach acid or bile from reflux can:
-
Worsen coughing and breathlessness
-
Mimic or worsen asthma and wheezing
-
Trigger new infections or inflammation
-
Possibly accelerate lung damage, especially if reflux goes untreated
-
Confuse your diagnosis (e.g. is it infection, inflammation, or reflux?)
In some cases, reflux and aspiration can contribute to lung conditions like bronchiectasis — which is often seen in people with aspergillosis.
🔍 Symptoms to Watch For
If you’re living with aspergillosis and experience any of the following, reflux could be playing a role:
-
Chronic cough or throat clearing
-
Wheezing not relieved by inhalers
-
Chest tightness or “burning” sensation
-
Sour taste in the mouth, especially in the morning
-
Hoarseness or sore throat
-
Waking up gasping or choking
-
Repeated chest infections
These symptoms may be worse after eating or when lying flat.
🧪 Diagnosing Reflux Aspiration
Ask your doctor about the following tests if reflux is suspected:
-
24-hour pH and impedance testing: Measures acid and non-acid reflux
-
Barium swallow or endoscopy: Checks for structural issues
-
Lung function tests: Identify asthma-like patterns
-
CT scan: To detect aspiration-related changes like bronchiectasis
-
Sputum tests: To rule out infection
💊 Treatment Options (and What Helps Most)
Lifestyle Tips
-
Raise the head of your bed 6–8 inches
-
Avoid eating 2–3 hours before lying down
-
Eat smaller meals more frequently
-
Avoid reflux triggers (spicy, fatty, or acidic foods, caffeine, chocolate)
-
Maintain a healthy weight if possible
Medications
-
Proton Pump Inhibitors (PPIs) like omeprazole: reduce stomach acid
-
H2 Blockers like ranitidine or famotidine
-
Prokinetic agents: Improve stomach emptying (check local availability)
-
Always take reflux medications under medical guidance, especially if you’re also taking antifungals (to avoid drug interactions)
Surgical Options
-
Fundoplication: Strengthens the barrier between stomach and esophagus
-
LINX device: A newer, less invasive option using magnetic beads
These may be considered if reflux is proven and not controlled with medications.
🤝 A Joined-Up Approach: Respiratory + Gastro Teams
Many patients benefit most when their respiratory doctor and gastroenterologist work together. For example:
-
Treating reflux may improve cough and wheeze
-
Addressing aspiration may reduce lung infections
-
Reflux control may improve response to antifungal treatment
If you’re under a specialist for aspergillosis and have reflux symptoms, let them know — a referral to a gastroenterologist may be appropriate.
🧠 Summary: Reflux and Aspergillosis
| Concern | Reflux Connection |
|---|---|
| Cough and throat clearing | ✅ Common sign |
| Worsening lung symptoms | ✅ Possible |
| Chest infections | ✅ Aspiration risk |
| Poor response to inhalers | ✅ Reflux-related inflammation |
| Lung scarring/bronchiectasis | ❗ Possible with repeated aspiration |
🫶 You’re Not Alone
Many people with aspergillosis struggle with reflux or silent aspiration without realising it. The good news is that recognising the issue early — and getting the right help — can protect your lungs and improve your quality of life.
Speak to your team, keep a symptom diary, and don’t hesitate to push for answers. Every little improvement in reflux control helps your lungs, too.
Key Shifts to Reinvent the NHS - The 10 Year plan
The plan introduces three radical shifts to modernize the NHS and secure its future:
-
🏥 Hospital → Community
-
Build a Neighbourhood Health Service: community health centres open 6 days/week for 12 hours/day
-
Provide integrated care closer to home—GPs, diagnostics, mental health, rehab, dentists, pharmacists, and even social support
-
Aim to reduce reliance on hospitals and cut waiting lists
-
-
📱 Analogue → Digital
-
Transform the NHS App into a “doctor in your pocket”—for appointments, advice, care plans, and self-referral
-
Embed AI to reduce admin, transcribe consultations, and support clinical decision-making
-
-
🛡️ Sickness → Prevention
-
Emphasize early intervention through more health checks, screenings, vaccines, and public health services
-
Shift funding towards community and preventative care, away from reactive hospital-based services
-
🏗 Underpinning Measures
To support these shifts, the plan introduces:
-
A new operating model & statutory framework to streamline the NHS structure
-
Transparency and accountability through metrics and patient feedback
-
Workforce transformation, including new training and wellbeing support
-
Innovation strategy harnessing genomics, AI, and tech
-
Financial reform via value-based funding—where providers are rewarded for outcomes
🔍 What This Means for You
-
Access to GP advice and care should be faster and more local – with reduced “8 am scramble”
-
More services like scans, mental healthcare, rehab, smoking cessation, and job support delivered at local centres
-
Greater convenience—use the App to manage care, book appointments, or message clinicians
-
Stronger focus on staying healthy—through screening, prevention, and early treatment support
🧩 Challenges & Expert Views
-
Funding & staffing: A £29 billion investment is pledged, but staffing shortages and infrastructure needs remain concerns
-
Implementation: Organisations like the King’s Fund highlight the absence of operational details and worry pilot projects may lead to regional variation
-
Behavioural shift: Success depends on NHS culture evolving—from reactive treatment to proactive, tech-enabled care
✍️ Final Take
The 10‑Year Health Plan represents a transformative vision: bring care closer to home, empower patients digitally, and focus on prevention. With strong backing from Starmer and Health Secretary Streeting, it aims to reshape NHS services by 2035. While optimism is growing, the effectiveness of implementation and securing resources will determine whether it truly delivers for patients and staff.
🌫️ A Life Shaped by Mould: One Person’s Journey with CPA and Lung Disease
Sadly, at the time of writing this story has to be paid for to read the full article. What follows is a summary of the free-to-access abstract.
“It started with damp walls – but it didn’t end there.”
This is the story of someone who spent a lifetime battling the hidden effects of mould exposure and fungal lung disease, from childhood through adulthood. Their experience is a powerful reminder of how long-term exposure to poor indoor environments — especially damp, flood-prone homes — can leave a lasting imprint on lung health.
🧒 Early Clues: Breathing Problems in Childhood
-
The author grew up in mouldy homes, regularly affected by floods.
-
As a teenager, they suffered from collapsed lungs, underwent pleurectomies, and were diagnosed with blebs (small air-filled sacs on the lung lining).
-
No one realised at the time that this could be linked to inhaled fungal spores.
🩺 The Long Road to Diagnosis
-
Years later, symptoms returned: chest infections, breathlessness, persistent coughing.
-
Eventually, doctors diagnosed:
-
Chronic pulmonary aspergillosis (CPA) – a long-term fungal infection
-
Severe bronchiectasis – a condition where the airways become damaged and inflamed
-
The root cause was now clear: years of breathing in airborne mould spores had likely caused permanent lung damage.
💊 Managing CPA: A Complex Balancing Act
The chapter describes the difficulty of living with CPA, including:
-
Strong antifungal medications (like itraconazole or posaconazole) and their side effects
-
Emergency lung procedures
-
Ongoing adjustments in daily life — from avoiding certain environments to managing fatigue
🤝 What Helped Most: Self-Advocacy and Support
This is also a story of resilience and empowerment. The author learned to:
-
Ask better questions at medical appointments
-
Work closely with specialists in fungal lung disease
-
Use trusted online resources to understand their condition
-
Keep going, even when progress was slow
💬 “I had to become my own advocate – not to fight my doctors, but to work with them more effectively.”
🧭 Advice for Others
The author shares practical tips that could help anyone dealing with CPA, bronchiectasis, or long-term lung illness:
-
Track your symptoms and treatments
-
Stay informed – but avoid misinformation online
-
Get help from respiratory physiotherapists
-
Don’t ignore your environment – especially damp, mouldy places
-
Keep asking questions until the answers make sense
🌟 A Message of Hope
This chapter isn’t just a medical account – it’s a message of hope and strength. It shows how understanding your own health, building a good medical team, and staying proactive can make a big difference, even in the face of serious illness.
Taking Charge: How to Get Involved in Decisions About Your Treatment
When you live with a long-term condition like aspergillosis, ABPA, CPA, or severe asthma, you may face tough decisions about medication, side effects, and quality of life. Treatments like biologics can offer huge benefits—but they also carry risks, and no one knows your body, lifestyle, or priorities better than you do.
The NHS is clear in its long-term plan: you should be involved in every major decision about your care. This is known as shared decision-making (SDM), and it means clinicians and patients working together to make the best choices—not just being told what to do.
Here’s how you can become more confident in taking part in your own care—and how to help your clinical team include you.
🪜 Step-by-Step: How to Join the Decision-Making Process
✅ 1. Know You Have a Right to Be Involved
You are not being "difficult" by asking questions or wanting to be part of the decision. The NHS encourages shared decision-making—and it’s your health.
🗣 “I’d like to understand the options and be involved in deciding what’s best for me.”
✅ 2. Ask for the Options – Including None
Sometimes we are only offered one treatment, but most decisions have at least 2 or 3 choices. For example:
-
Start or delay biologics?
-
Try antifungals again or monitor symptoms?
-
Continue with current care or make a change?
Ask:
🗣 “What are my options, including the option of not doing anything right now?”
✅ 3. Talk About What Matters Most to You
Doctors often focus on test results or scan findings. But you may be more concerned about fatigue, side effects, work, travel, or caring for family.
Let them know what your priorities are:
🗣 “My top goal is to stay out of hospital and manage breathlessness so I can keep working.”
🗣 “I can live with minor side effects, but I don’t want something that weakens my immune system too much.”
✅ 4. Understand the Risks and Benefits
Every treatment, including biologics, is a balance—they reduce inflammation but may make you more vulnerable to infection. That doesn’t mean you shouldn’t take them, but it’s important to understand the trade-offs.
Ask:
🗣 “What are the likely benefits of this treatment for someone like me? What are the possible side effects?”
🗣 “How will this affect my overall health and day-to-day life?”
✅ 5. Ask for Time to Reflect
You don’t need to make big decisions in a 10-minute appointment.
🗣 “Can I take this information home and think about it? I’d like to talk with family or other patients before I decide.”
It’s okay to not decide straight away.
✅ 6. Keep Track of Questions and Progress
Write things down before your appointment. You can even bring someone with you, or ask to record the discussion on your phone.
Apps and treatment diaries help you track side effects, symptoms, and goals, so you and your team can review how well things are working later.
✅ 7. Use Supportive Tools and People
Ask for:
-
Leaflets, videos, or trusted websites to read later
-
A follow-up call with a specialist nurse
You could say:
🗣 “Can you recommend a trusted place to read more about this? I’d like to understand it in my own time.”
🧠 A Shift in Thinking: It’s Not About a Quick Fix
We’ve all grown up with advertising that tells us “This treatment will fix the problem.” But in reality, every treatment is a trade-off—between the benefits it brings and the side effects or limitations it may cause.
Even doctors can fall into the trap of focusing only on what they can treat in their specialty—lungs, infections, skin—and miss how treatments affect the whole person.
You can help by:
-
Gently reminding them of the bigger picture
-
Asking them to explain in plain language
-
Saying honestly how things are affecting your life, not just your lungs
🌈 Your Quality of Life Is the Priority
In the end, what matters is how you feel and function. For some, a small side effect might be worth the gain in lung function or fewer flare-ups. For others, it may not. Only you can make that call—with the right information and support.
📌 Good care means making decisions with you, not for you.
📥 Want to Take This Further?
Ask your clinic or GP about:
-
Shared Decision-Making tools (they’re part of NICE guidelines)
-
Getting written summaries of discussions and next steps
And remember: you’re not just a patient—you’re a partner in your care.
Best Types of Cleaning Products for Chemical Sensitivities
For people with chemical sensitivities—such as Multiple Chemical Sensitivity (MCS), asthma, or other respiratory conditions—it's important to use gentle, non-toxic cleaning products that don't contain harsh chemicals, fragrances, or volatile organic compounds (VOCs). Here's an overview:
✅ Best Types of Cleaning Products for Chemical Sensitivities
🧴 1. Fragrance-Free and Dye-Free Products
-
Look for labels that say “fragrance-free,” “unscented,” and “free and clear.”
-
Avoid products labeled "natural" if they still contain essential oils or botanical fragrances (these can still trigger reactions).
🌿 2. Simple, Non-toxic Ingredients
Safer cleaning agents often include:
-
White vinegar – natural disinfectant, but avoid if the smell is bothersome.
-
Baking soda – gentle abrasive cleaner, excellent for scrubbing.
-
Castile soap – a mild, vegetable-based soap (e.g. Dr. Bronner’s).
-
Hydrogen peroxide (3%) – for disinfecting and stain removal.
-
Rubbing alcohol (70%) – effective on surfaces, but test for sensitivity.
🔄 3. DIY Cleaning Solutions
Many people with sensitivities prefer to make their own:
-
All-purpose cleaner: 1 part vinegar + 1 part water (optional: a drop of castile soap).
-
Glass cleaner: 2 cups water + 2 tablespoons vinegar + 1 tablespoon rubbing alcohol.
-
Soft scrub: Baking soda + a small amount of water or castile soap.
👩⚕️ Recommendations from Support Groups and Allergy Specialists
-
Choose products that are certified by:
-
EcoLogo
-
Green Seal
-
Safer Choice (US EPA)
-
Allergy UK’s Seal of Approval
-
-
Common brands used by sensitive individuals:
-
Ecover Zero
-
Attitude (Sensitive line)
-
Seventh Generation Free & Clear
-
Molly’s Suds
-
Clean Living
-
Simple Truth Free & Clear
-
(Always patch test new products first.)
🧠 Tips from People Living with Sensitivities
-
Ventilate well during and after cleaning.
-
Use microfiber cloths and steam mops to reduce the need for chemical cleaners.
-
Avoid air fresheners, candles, and essential oils, even if labeled “natural.”
-
Store cleaning products away from living spaces to limit fumes.
🌡️ How to Store Your Medicines Safely in Hot Weather
Many prescription medicines must be stored below 25°C to remain safe and effective. During summer or heatwaves, especially when temperatures rise above 30°C, you need to take extra care.
This guide explains what to do to keep your medicines safe at home or while travelling.
❓ Why It Matters
Medicines exposed to too much heat can:
-
Lose effectiveness
-
Change in appearance or texture
-
Become unsafe to use
This is especially true for:
-
Antibiotics
-
Inhalers
-
Liquid medicines
-
Hormone tablets (e.g. thyroxine)
-
Biologics or injectables (some require refrigeration)
📦 What "Store Below 25°C" Means
-
This refers to room temperature – ideally between 15°C and 25°C.
-
Some medicines may tolerate brief periods above 25°C, but prolonged heat can degrade them.
-
Do not refrigerate medicines unless specifically instructed – cold can also damage some drugs.
🏠 At Home: Tips for Keeping Medicines Cool
| ✅ Do | ❌ Avoid |
|---|---|
| Store in a cool, dark place | Windowsills or near radiators |
| Use a shaded cupboard or wardrobe | Kitchen cupboards near ovens |
| Consider an insulated box (without ice) | Bathrooms (can get hot and humid) |
| Monitor the temperature with a small digital thermometer | Leaving in direct sunlight |
You can buy inexpensive thermometers online to check storage temperatures.
🌞 In a Heatwave
If indoor temperatures go above 25°C for more than a few hours:
-
Move medicines to the coolest part of your home (e.g. north-facing room or basement).
-
Close blinds and curtains during the day to keep rooms cooler.
-
Use fans or portable air conditioners if available.
-
Keep medicines away from heat-generating electronics.
✈️ Travelling or on Holiday
-
Never leave medicine in a hot car, especially glove boxes or boots.
-
Use a cool bag, insulated travel pouch, or medication wallet with a cooling gel pack.
-
In hotels, store medicines in a shaded cupboard or the fridge only if the label allows it.
-
Avoid storing medicines in your luggage if it may be left in the sun or overheated.
✅ Signs Your Medicine May Be Affected
Contact your pharmacist if:
-
The medicine looks or smells different
-
Tablets have melted, crumbled or discoloured
-
Liquids have separated or changed consistency
-
You’re unsure whether the medicine has been exposed to prolonged heat
🗨️ What the NHS and UK Pharmacists Say
-
Short-term exposure to temperatures slightly above 25°C is usually not harmful.
-
Medicines stored above 25°C for several days may need to be replaced – ask your pharmacist.
-
Pharmacies use temperature-controlled storage and monitor heat during hot weather – you can do the same at home.
Sources include NHS Trusts, SPS (Specialist Pharmacy Service), and Royal Pharmaceutical Society guidance.
📋 Quick Tips Checklist
✅ Keep medicines in their original packaging
✅ Avoid windowsills, kitchens, and bathrooms
✅ Use a shaded, cool cupboard or wardrobe
✅ Monitor room temperatures during heatwaves
✅ Carry medicines in a cool bag when travelling
✅ Check for changes in medicine appearance
✅ Ask a pharmacist if in doubt
📞 Need advice?
Speak to your pharmacist or GP if you're unsure whether a medicine has been affected by heat or if it still seems safe to use.
🧬 Are Vaccines for Aspergillosis on the Horizon?
If you live with aspergillosis—whether it's ABPA (Allergic Bronchopulmonary Aspergillosis), CPA (Chronic Pulmonary Aspergillosis), or invasive aspergillosis—you’ve probably wondered if a vaccine might one day help prevent or control this condition. As of 2025, there is no licensed vaccine for any form of aspergillosis, but scientists are actively working on it.
This article explains where things stand, what’s being developed, and what it could mean for people like you.
🦠 What is Aspergillosis?
Aspergillosis is a group of illnesses caused by the fungus Aspergillus fumigatus. It’s very common in the environment, especially in soil, dust, and decaying vegetation. Most people breathe in the spores without getting sick, but if you have:
-
Damaged lungs (due to asthma, COPD, or TB)
-
A weakened immune system
-
An allergic reaction to fungal spores
…you may develop a form of aspergillosis, such as:
-
ABPA – a severe allergic lung condition
-
CPA – long-term fungal infection in damaged lungs
-
Invasive aspergillosis – a fast-moving, life-threatening infection in immunocompromised people
💉 Why Develop a Vaccine?
A vaccine could:
-
Prevent serious illness in high-risk people (like cancer or transplant patients)
-
Reduce allergic sensitisation in ABPA
-
Lower the need for long-term antifungal drugs, which can have side effects and lose effectiveness
-
Protect against lung damage caused by repeated infections
But making a vaccine isn’t easy—especially for a disease that behaves differently depending on a person’s immune system.
🧪 Vaccines in Development (2025)
While none are yet available for patients, several experimental vaccines are being tested in laboratories and early-stage trials. Here are the most promising ones:
1. NDV-3A Vaccine
-
Originally developed for a yeast infection (Candida albicans)
-
Found to trigger cross-protection against Aspergillus fumigatus
-
Uses a protein called Als3p, shared between fungi
-
Completed early safety trials for Candida
-
Being explored for people with weak immune systems, like transplant recipients
2. AF.KEX1 DNA Vaccine
-
Uses a fungal protein called Kexin 1
-
Delivered as a DNA vaccine to help the body produce protective immune cells
-
Shown to work well in animal models
-
Designed to help high-risk patients, such as those having chemotherapy
3. Asp f3 Protein Vaccine
-
Focuses on a specific Aspergillus protein (Asp f3)
-
Stimulates T-helper cells (Th1 and Th17), important for fighting fungal infections
-
Still in preclinical stages, but results in mice are promising
4. Nasal Spray Vaccine with Nanoparticles
-
Uses chitosan (a natural substance) to deliver the vaccine via the nose
-
Aims to stimulate mucosal immunity (lining of the lungs and airways)
-
Could be useful for people with ABPA or cystic fibrosis, who often have fungal colonisation in the lungs
5. Exploratory mRNA Vaccines
-
Inspired by COVID-19 vaccine technology
-
Still experimental, but may offer faster, more targeted vaccine design
-
No clinical trials yet, but research is underway
🚧 Why Don’t We Have a Vaccine Yet?
Developing a vaccine for aspergillosis is challenging:
-
The immune response needed varies between allergic, chronic, and invasive forms
-
Many people most at risk (e.g. after organ transplant) are too immunocompromised to respond well to vaccines
-
Aspergillus has many different proteins—no single target works for everyone
-
Research funding is often limited, because aspergillosis is considered rare
👥 Who Might Benefit Most?
A future vaccine could be life-changing for:
-
People with weakened immune systems (e.g. after stem cell or organ transplant)
-
People with long-term lung disease, including ABPA and CPA
-
Children and adults with cystic fibrosis
-
People undergoing chemotherapy or immune-suppressing treatment
🗣️ What Can Patients Do?
You can help push this research forward:
-
Join a registry or research study if asked by your hospital
-
Share your story with groups like the National Aspergillosis Centre (NAC) or Rare Disease UK
-
Support advocacy efforts calling for better funding of fungal research
-
Stay up to date with trial opportunities on trusted sites like aspergillosis.org
📌 Key Takeaways
| Question | Answer |
|---|---|
| Is there a vaccine for ABPA or CPA? | Not yet — but several are in development. |
| Who might benefit from a vaccine? | People with asthma, CF, CPA, ABPA, or weakened immunity |
| When will it be available? | Likely several more years away — still early in trials |
| What’s the biggest challenge? | Complex immunity, rare disease status, limited funding |
🧭 Looking Ahead
Although no vaccine is available yet, the science is moving forward — thanks to global research teams who see the impact aspergillosis has on patients’ lives. Even small steps now could lead to major breakthroughs in future care.
Your voice matters. Stay connected, stay informed — and keep asking for more focus on this important condition.
How can we, as patients, support or raise our voices to bring more focus to ABPA in the medical and research world?
You're absolutely right that ABPA (Allergic Bronchopulmonary Aspergillosis) often sits in the shadow of more widely recognised diseases like asthma, cystic fibrosis, and even chronic pulmonary aspergillosis (CPA), despite the daily impact it has on breathing, energy, and quality of life for those affected. Here's a comprehensive response to your two key questions:
👉 Is more active research or clinical development happening specifically for ABPA therapies?
✅ Some research is happening — but it's limited and fragmented.
-
ABPA is considered a rare disease (likely fewer than 10,000 diagnosed in the UK), so it doesn’t attract the same commercial research attention as asthma, cystic fibrosis (CF) or chronic obstructive pulmonary disease (COPD)..
-
ABPA overlaps with asthma, cystic fibrosis, and bronchiectasis, which means treatments often come from those areas — but are not tailored to ABPA patients.
💊 Existing therapies are adapted, not designed for ABPA:
-
Steroids (oral or inhaled) remain first-line, but long-term use has harmful side effects.
-
Azole antifungals (like itraconazole or voriconazole) are used to reduce fungal burden — but responses vary, side effects are common, and resistance is rising.
-
Biologics (like omalizumab, mepolizumab, dupilumab, and now tezepelumab) are showing promise in small studies and real-world experience — but none are licensed specifically for ABPA, which means access is inconsistent and often requires individual funding requests (IFRs).
🔬 Ongoing research and development (as of 2025):
-
Japan and India are leading some ABPA-specific studies, especially around imaging, IgE trends, and steroid-sparing strategies.
-
Small studies and case series are evaluating biologic therapies in ABPA, particularly in:
-
Asthma + ABPA overlap
-
CF + ABPA overlap
-
Bronchiectasis + ABPA cases with poor control
-
-
No current large-scale Phase 3 trials for ABPA-specific therapies are active in the UK or Europe, though there is growing academic interest at centres like Manchester (NAC) and Royal Brompton and specialist centres across Europe.
👉 How can we, as patients, raise our voices to bring more focus to ABPA?
🗣️ 1. Share your story
-
Personal experiences — like the one you just shared — are powerful advocacy tools. NAC and Aspergillosis Trust are regularly asked to provide volunteers to talk about their experiences for national media stories - when they happen there is usually little time to respond so leaving your contact details with Aspergillosis Trust or NAC can be a way to help raise awareness.
-
Blogs, social media, patient interviews, or videos can humanize the condition for researchers, clinicians, and policymakers.
-
You could contribute to aspergillosis.org, BLF, or Rare Disease UK platforms.
💬 2. Engage with research centres
-
The National Aspergillosis Centre (NAC) is uniquely placed to drive research.
-
Ask to be part of patient advisory panels, surveys, or focus groups — your lived experience helps shape research priorities. There is currently a Europe-wide group run by the European Lung Foundation (Aspergillosos PAG) that is designed to do exactly this, and here at NAC we periodically ask for volunteers to help run clinical trials in the UK, usually via our Facebook or Telegram groups.. The Aspergillosis Trust are also occasionally asked to suggest volunteers for trials, so it is well worth engaging with them too. There is no obligation, just join to see what is going on! Every extra person in advocacy groups gives the group more awareness power.
-
Inquire whether NAC is seeking trial participants, or if they plan to study ABPA-specific uses of biologics.
✍️ 3. Support and pressure through policy
-
Add your voice to calls for biologic licensing for ABPA.
-
Back campaigns like Accelerating Access to Rare Disease Therapies (via Genetic Alliance or Rare Disease UK).
-
Contact your local MP or ICB (Integrated Care Board) to raise access issues — such as Individual Funding Request (IFR) delays or biologic refusals.
🤝 4. Connect with others
-
ABPA-specific support groups (e.g. through NAC, Facebook groups, or Zoom meetups) allow patients to:
-
Share coping strategies
-
Create collective pressure
-
Support research studies via recruitment or funding
-
📈 5. Help build data
-
ABPA is under-diagnosed and under-coded in NHS data — meaning we don’t know how many people truly have it.
-
Participating in registries, audits, or quality-of-life research helps build a case for investment and clinical guidelines.
✨ Final Thoughts
You are right to point out that the scale of suffering from ABPA is real — even if it doesn't generate headlines. That makes patient voices even more essential. The good news is: the more we talk about ABPA, the more momentum we can build. Already, biologics are gaining attention — but formal ABPA trials, compassionate-use programs, and NHS funding clarity are still needed.
Let me know if you'd like help writing a patient statement, connecting with a researcher, or forming a focus group to bring these issues forward. You could help shape the next chapter of ABPA care.
You're doing more than you realise by speaking out. 👏
🌿 Practical Steps for Managing Steroid-Related Facial Swelling
🧊 1. Cold Compresses
-
Applying a cool, damp cloth or cold gel mask to your face and neck for 10–15 minutes may help reduce inflammation and redness, especially in the evening.
-
Avoid ice directly on the skin.
🛌 2. Elevation and Sleep Position
-
Try sleeping with your head elevated on an extra pillow. This helps reduce overnight fluid pooling in the face.
-
During the day, keep your head upright when sitting or resting.
💧 3. Fluid Management
-
Paradoxically, drinking plenty of water helps your body excrete excess salt and reduce fluid retention.
-
Consider reducing your sodium intake, as salt encourages water retention and worsens facial puffiness.
🍽️ 4. Diet Adjustments
-
Avoid high-carb and sugary foods, which can worsen fluid retention and blood sugar instability (already affected by steroids).
-
Add potassium-rich foods (e.g. bananas, spinach, sweet potatoes), which help balance fluid levels.
🚶 5. Gentle Movement
-
Short walks or mild activity during the day help circulation and prevent dependent edema (swelling that increases as the day goes on).
🧴 6. Skin Soothing and Anti-Inflammatory Topicals
-
Use fragrance-free soothing moisturisers containing niacinamide or aloe vera.
-
Redness may also respond to mild over-the-counter hydrocortisone cream for short use — though caution is advised since you're already on systemic steroids.
💊 7. Medication Review
-
Diuretics (water tablets) are rarely used for steroid-induced swelling, but in some cases, a clinician may consider it if fluid retention is severe.
-
Tapering your corticosteroids (if appropriate and under supervision) can gradually improve symptoms — discuss this with your prescriber.
🩺 8. Consult a Specialist
-
If the swelling is asymmetric, very painful, or associated with new symptoms (e.g., visual changes, difficulty swallowing, skin tightness), you should be checked promptly for other causes.
-
A referral to a dermatologist or endocrinologist may help if cosmetic or systemic effects are severe or long-term.
⚠️ When to Seek Urgent Medical Advice
Call your GP or attend an urgent care clinic if you have:
-
Sudden, painful swelling
-
Shortness of breath
-
Swelling spreading rapidly
-
New rash, fever, or visual disturbance