💊 General Strategies to Reduce Antimicrobial Resistance in Clinical Practice
1. IV to Oral Switch (IVOS)
One of the most effective and safe interventions in antimicrobial stewardship.
🔁 Why switch from IV to oral early?
-
Reduces complications (e.g. line infections, thrombosis)
-
Lowers costs and bed-days
-
Improves patient comfort and mobility
-
Oral options (e.g. ciprofloxacin, fluconazole, linezolid) are highly bioavailable, often matching IV efficacy
✅ When is IVOS appropriate?
-
Clinical improvement seen
-
Source controlled
-
Oral route available and tolerated
-
Suitable oral alternative exists
NHS guidance: "Start smart – then focus" encourages early IVOS reviews within 48–72 hours of antibiotic initiation.
2. "Start Smart – Then Focus" (UK NHS Framework)
This key NHS antimicrobial policy includes:
-
Start Smart: Prescribe antibiotics appropriately from the beginning
-
Then Focus:
-
Review at 48–72 hours
-
Consider stop, switch, change, or continue
-
Document clearly in records
-
Supported by NICE guidelines and UKHSA audits
3. Shorter Duration of Therapy
For many infections, shorter courses (e.g. 5–7 days instead of 10–14) are now preferred.
Examples:
-
Community-acquired pneumonia: 5 days
-
Pyelonephritis: 7 days
-
Cellulitis: 5–7 days
This reduces resistance pressure and side effects.
4. Diagnostics-Guided Prescribing
-
Procalcitonin and CRP tests can help distinguish bacterial from viral infections
-
Rapid PCR, MRSA, or blood culture diagnostics guide targeted therapy
The aim is avoid empirical broad-spectrum antibiotics where possible.
5. Restricted Prescribing Policies
-
Certain high-risk drugs (e.g. carbapenems, vancomycin, antifungals) are restricted to ID approval
-
Antimicrobials are tiered by risk (e.g. traffic light systems) to encourage narrow-spectrum use
6. Antimicrobial Stewardship Teams (ASTs)
Multidisciplinary teams:
-
Lead on stewardship strategy
-
Audit antimicrobial use
-
Provide decision support for complex cases
-
Educate staff and update local formularies
In the NHS, stewardship is a CQUIN target (incentivised performance indicator).
7. Education and Behaviour Change
-
Mandatory AMS training for junior doctors and prescribers
-
Behavioural nudges in electronic prescribing systems (e.g. default shorter durations, alert for IVOS)
8. Surveillance and Reporting
-
ePAMS+, ESPAUR, and PHE Fingertips dashboards track:
-
Prescribing by hospital/unit
-
Resistance trends
-
Audit compliance with IVOS, duration, and documentation
-
9. Patient-Facing Initiatives
-
"Antibiotic Guardian" and leaflets explaining viral vs bacterial infections
-
Empowering patients to ask:
"Do I really need antibiotics? When can I switch to tablets?"
📦 Summary Table: Key Interventions
| Strategy | Purpose |
|---|---|
| IV to Oral Switch | Reduce IV duration, speed discharge |
| Review at 48–72 hrs | Reassess need, de-escalate if possible |
| Shorter therapy courses | Lower resistance pressure |
| Targeted diagnostics | Support narrow-spectrum prescribing |
| Prescribing restrictions | Protect last-resort antimicrobials |
| Stewardship teams | Oversee, audit, educate |
| Surveillance & feedback | Monitor trends, guide policy |
🛡️ FFP2/FFP3 Mask Use in Aspergillosis: Summary
| Mask Type | Who Might Use It | When It's Used |
|---|---|---|
| FFP2 (95% filtration) | Some patients with CPA, ABPA, or SAFS, especially during flares or hospital visits | During travel on public transport, clinic waiting rooms, visiting building sites, or dust exposure |
| FFP3 (99% filtration) | Patients who are severely immunocompromised (e.g. post-transplant, on chemotherapy, or high-dose steroids) | In high-risk environments: hospital construction, building work nearby, or heavy dust/mould exposure |
✅ When Masks Might Be Advisable
-
During hospital visits, particularly in winter or during flu/COVID waves
-
If you're immunosuppressed, e.g. taking long-term steroids or biologics
-
When exposed to mouldy buildings, compost, building work, or flood damage
-
In crowded indoor environments where infection risk is high
❌ When They’re Usually Not Needed
-
Day-to-day life in a clean, dry home environment
-
Low-risk outdoor activity (e.g. walking in the park)
-
If your asthma/ABPA/CPA is stable and you're not immunocompromised
🗣️ What the National Aspergillosis Centre Recommends
-
Use FFP2 masks when entering environments likely to have airborne fungal spores
-
FFP3 masks may be offered for high-risk medical procedures or when severely immunocompromised
-
Masks are one part of a broader protection strategy, which includes:
-
Good indoor air quality (HEPA filters, ventilation)
-
Avoidance of dusty environments
-
Prompt treatment of fungal infections
-
🌬️ Living with Asthma and Aspergillosis: Understanding the Overlap, the Immune System, and the Right Treatment
If you live with asthma and have been told you also have aspergillosis, such as ABPA (Allergic Bronchopulmonary Aspergillosis) or SAFS (Severe Asthma with Fungal Sensitisation), your situation is more complex than most people realise.
This guide explains:
-
The different types of asthma
-
How aspergillosis complicates asthma
-
The role of eosinophils, IgE, and the immune system
-
Why some people don’t have “typical” symptoms (like wheeze)
-
What treatments are available — and how to personalise your care
🧠 Asthma Isn’t One Disease
Asthma is a condition where the airways (breathing tubes) become:
-
Inflamed (swollen and irritated)
-
Overreactive to certain triggers (allergens, cold air, infection, etc.)
-
Narrowed and often filled with mucus, making breathing difficult
But not everyone with asthma has the same cause, symptoms, or treatment response. Asthma actually includes many subtypes — and understanding your type is key to getting the right care.
🧬 Common Asthma Types in Aspergillosis
| Asthma Type | Cause / Trigger | Key Features |
|---|---|---|
| Allergic asthma | IgE-driven allergy to pollen, dust, pets, fungi | Common in early-life asthma |
| Eosinophilic asthma | High levels of eosinophils (a white blood cell) | Often adult-onset and hard to control |
| SAFS | Allergy to fungi (especially Aspergillus) | Severe, steroid-resistant asthma |
| ABPA | Allergic reaction to Aspergillus growing in lungs | Very high IgE, eosinophils, mucus, lung damage |
| Cough-variant asthma | Inflammation without wheeze | Dry cough as the only symptom |
| “Silent” asthma | Reduced or absent warning signs | No wheeze, may present with fatigue, cough or breathlessness only |
🫢 New Section: What Is “Silent Asthma”?
“Silent asthma” is not an official medical term, but it’s used to describe:
-
Asthma without the classic wheeze (often just cough or tightness)
-
Or where asthma attacks happen suddenly, without clear warning
This is important because:
-
People may not realise they have asthma
-
Diagnosis may be delayed or missed
-
Flare-ups can be severe or even life-threatening
-
It may occur in people with fungal asthma, ABPA, or airway damage
Silent asthma is especially relevant in:
-
Older adults
-
People with ABPA or SAFS
-
People with cough-variant asthma
-
Anyone whose asthma doesn’t “sound” typical
🧪 Tests like FeNO, spirometry, and blood eosinophil counts are vital for confirming what’s really happening inside the lungs — even if symptoms are subtle.
🔬 Why ABPA Adds Complexity
If you have ABPA, the asthma symptoms are made worse by:
-
A hypersensitive immune reaction to Aspergillus fumigatus
-
Mucus plugging and blocked airways
-
Lung damage (bronchiectasis) that doesn’t improve with inhalers alone
-
A mix of allergic and eosinophilic inflammation
Key signs include:
-
Extremely high IgE levels
-
Raised eosinophils
-
Positive blood tests for Aspergillus
-
Lung CT scan changes
💊 Treatment Options Based on Asthma Type
| Treatment | Used For |
|---|---|
| Inhaled corticosteroids (ICS) | All types, first-line |
| Antifungal medications | ABPA, SAFS |
| Oral steroids (e.g. prednisolone) | ABPA flares, severe asthma |
| Biologics (e.g. mepolizumab, omalizumab) | Severe allergic or eosinophilic asthma |
| Chest physiotherapy | Mucus clearance in ABPA or bronchiectasis |
Each treatment is tailored based on whether your asthma is driven by:
-
IgE (allergy)
-
Eosinophils (inflammation)
-
Fungal exposure or colonisation
📍 What to Discuss with Your Healthcare Team
If you:
-
Have asthma that isn’t well controlled
-
Need frequent steroids
-
Have a chronic cough, thick mucus, or lung damage
-
Have high IgE or eosinophils
-
Or don’t wheeze, but still get breathless or fatigued…
… it’s important to ask your doctor:
-
Could I have ABPA or SAFS?
-
Is there a fungal or eosinophilic component to my asthma?
-
Should I be tested for Aspergillus allergy or IgE?
-
Am I a candidate for biologics or antifungals?
✅ Final Takeaway
Asthma with aspergillosis is more than just “bad asthma” — it’s a complex condition involving allergy, inflammation, fungal exposure, and in some cases, permanent airway changes. Some patients don’t experience wheeze — this is called “silent asthma,” and it deserves just as much attention.
You don’t have to manage this alone — and there are now targeted treatments that can help reduce symptoms, prevent damage, and improve quality of life.
Telecare Devices and the UK Digital Switchover: What Aspergillosis Patients and Carers Need to Know
Background By the end of 2025, traditional landline telephone networks in the UK will be phased out and replaced by digital (VoIP) systems delivered via broadband. This national "Digital Switchover" affects anyone using landline-based devices, including many telecare systems vital to people with chronic illnesses like chronic pulmonary aspergillosis (CPA), ABPA, and SAFS.
This document provides clear guidance for aspergillosis patients and carers concerned about how this change affects telecare equipment such as fall alarms, pendant buttons, and GPS trackers.
Why This Matters for Aspergillosis Patients Many people with aspergillosis rely on telecare to remain safe at home. These may include:
- Fall detectors
- Emergency pendant alarms
- Door sensors
- GPS trackers
- Daily wellbeing check-in devices
These systems were typically connected to analogue landlines. Once the switch to digital phone lines is made, some older devices may stop working correctly unless they are upgraded or adapted.
What Changes with the Digital Switchover?
| Feature | Current (Analogue Landline) | Future (Digital via Broadband) |
|---|---|---|
| Phone line works during power cuts | Yes | No (unless battery backup is added) |
| Telecare devices plug into phone socket | Yes | Only with compatible router or adapter |
| Works independently of broadband | Yes | No, relies on internet connection |
Common Concerns and Solutions
- "Will my current telecare alarm still work?"
- Possibly not. Many older alarms won't function over digital broadband lines.
- Solution: Ask your alarm provider if your device is VoIP compatible or if they can supply a digital-ready or cellular version.
- "Will full fibre broadband stop my telecare from working?"
- Not automatically, but older devices may be incompatible.
- Solution: If switching to full fibre, ensure your telecare system can plug into the new router or ask about an analogue telephone adapter (ATA) with battery backup.
- "What happens during a power cut?"
- Digital lines go down unless you have a UPS (Uninterruptible Power Supply) or the telecare device is cellular-based.
- "Can I upgrade to something more future-proof?"
- Yes. Many councils and private providers now offer mobile-enabled alarms with built-in SIM cards and GPS.
- These do not rely on landlines or home Wi-Fi.
What You Should Do Now
- Contact your telecare provider
- Ask if your current device is digital-compatible.
- Request upgrade options if needed.
- Speak to your broadband provider
- Let them know you use telecare. Ask about battery backup or compatibility.
- Contact your local Adult Social Care team
- Many councils are offering free or subsidised upgrades to digital or mobile telecare.
- Test your system
- Before and after switching broadband providers, run a test call with your alarm provider.
Summary As the UK phases out analogue landlines, it's essential for patients and carers to act early. Ensuring your telecare system is compatible with digital broadband will help maintain your independence and safety. Monitoring your oxygen saturation may also support early detection of lung health changes.
Resources for Further Help
- Aspergillosis Patient Support
- Aspergillus & Aspergillosis Resources
- Ofcom Digital Switchover Advice
- Your local council’s Adult Social Care department
If you have questions or need help contacting the right services, the National Aspergillosis Centre support team can guide you.
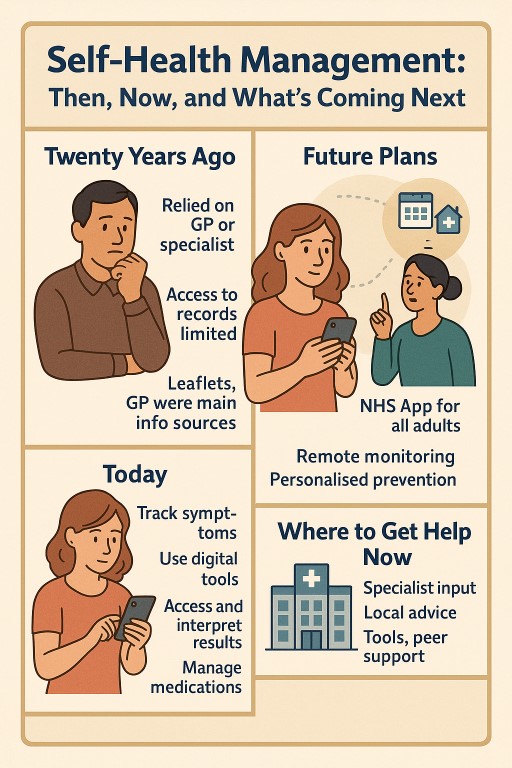
🧭 Self-Health Management: Then, Now, and What’s Coming Next
🧭 Self-Health Management: Then, Now, and What’s Coming Next
Over the past 20 years, the way people manage their health in the UK has changed dramatically — and more changes are on the horizon. For people living with long-term or complex conditions like aspergillosis, asthma, or chronic lung disease, this shift has brought both new opportunities and new burdens.
This article explains what’s changed, what the government is planning, what benefits are hoped for — and what happens if you can’t or don’t want to use online tools.
🕰️ What Was Self-Health Management Like 20 Years Ago?
In the early 2000s:
-
Patients relied heavily on their GP or hospital specialist for every decision.
-
Access to records was limited or non-existent.
-
Health information came from leaflets, GPs, or occasional TV programmes.
-
Appointments were mostly face-to-face and arranged by phone.
-
There was less expectation for people to self-manage complex conditions.
📲 What’s Different Today?
Patients today are expected to:
-
Track symptoms themselves and know when to seek help.
-
Use digital tools like the NHS App, online consultations, and health monitoring apps.
-
Interpret test results, medication side effects, and care plans with less direct support.
-
Coordinate care between services — sometimes across different hospitals or systems.
-
Understand and act on complex health advice, often with less contact from clinicians.
For people with chronic respiratory conditions like CPA or ABPA, this can sometimes improve control — but it can also feel overwhelming, especially when care is fragmented or specialists are hard to reach.
🧑⚕️ How Are Healthcare Staff Adapting?
Many GPs, nurses, and hospital teams are trying to:
-
Embrace shared decision-making and educate patients more directly.
-
Offer video, phone, or online consultations when appropriate.
-
Provide tools like self-monitoring diaries, peak flow meters, or oxygen saturation monitors.
-
Rely on electronic triage systems and limit in-person appointments to the most complex cases.
But many are also under pressure. Staff shortages, long waiting lists, and increased demand mean clinicians have less time per patient, making it harder to offer the detailed guidance many people still need.
🏛️ What Is the UK Government Planning for the Future?
The government’s current plans aim to make the NHS more digital, preventative, and self-directed. This is laid out in the NHS Long Term Plan, the Digital Health and Care Strategy, and the Data Saves Lives policy.
| Goal | Target |
|---|---|
| Make the NHS App the main access point for care | 2025–2026 |
| Move more routine care to remote monitoring and self-management | By 2026–2029 |
| Personalise prevention and reduce avoidable illness | By 2029 |
| Reduce reliance on face-to-face appointments | Ongoing since 2021 |
| Digitise health records across all services | By 2025–2027 |
Patients with long-term conditions are expected to:
-
Manage their own prescriptions
-
Monitor symptoms at home
-
Use digital tools to stay informed and in control
-
Access care only when needed, rather than by default
🎯 What Are the Hoped-For Benefits?
The government promotes these changes as delivering:
✅ Better Outcomes
-
Early intervention, better symptom tracking, and fewer complications.
-
Personalised care plans based on your data and condition.
✅ More Convenient Care
-
Fewer unnecessary visits
-
More control over your own information and appointments
✅ NHS Cost Savings
-
Reducing face-to-face appointments and hospital stays frees up staff time.
-
Less duplication, fewer unnecessary tests, better resource use.
⚠️ But Is It Better for Everyone?
Not necessarily. These benefits are not equally felt by all patients.
🧓 Digital Exclusion Is a Real Problem
-
Around 1 in 5 UK adults struggle with using digital health services.
-
Older adults, people on low incomes, and those with disabilities or learning needs are most affected.
-
Some patients simply don’t feel confident, or don’t trust digital systems.
🧭 What Happens If You’re Left Behind?
Government guidance insists that non-digital options must remain — but this isn’t always consistent. Some patients report:
-
Difficulty reaching practices by phone
-
Online-only booking or consultations
-
Fewer letters and face-to-face reviews
Patients with complex, fluctuating, or rare conditions like aspergillosis may find it harder to get appropriate support without a strong digital presence — especially if care crosses multiple departments or regions.
🧠 So What Needs to Happen?
To make this shift work for everyone, the system must:
-
Protect non-digital access routes (e.g. phone, letter, face-to-face)
-
Offer digital training and support to those who want it
-
Make sure apps and online tools are inclusive and easy to use
-
Involve patients in designing these services — especially those with long-term conditions
-
Keep monitoring for harm or exclusion, and respond quickly
📍 Where Can Patients Get Help Today?
| Support Type | Where to Find It |
|---|---|
| 🔬 Specialist advice | National Aspergillosis Centre, hospital respiratory clinics |
| 👨⚕️ Local support | GP, pharmacist, practice nurse |
| 📱 Digital tools | NHS App, condition-specific apps, NHS websites |
| 🤝 Peer support | Online groups, charities, forums (e.g. Asthma + Lung UK, aspergillosis.org) |
| 💬 Advice lines | NHS 111, condition-specific helplines |
✅ In Summary
The NHS is changing — and patients are expected to change with it. Over 20 years, self-management has gone from optional to expected, and digital care is being rapidly expanded.
For some, this means more control and quicker help. For others, it can feel isolating, confusing, or unsafe. The challenge is to design systems that support everyone — not just the tech-savvy or well-connected.
If you’re living with a long-term condition like aspergillosis, you should never be left managing alone.
🧾 Getting a Second Opinion for Aspergillosis: What If Your Hospital Refuses?
Many patients living with aspergillosis or allergic bronchopulmonary aspergillosis (ABPA) ask for a second opinion — often from a national centre like the National Aspergillosis Centre (NAC) in Manchester or from another specialist elsewhere in the UK. But sometimes, hospitals resist sending your case outside their own department.
Here’s what’s happening, why it might occur, and what you can do.
🤔 Why Would a Hospital Refuse an Outside Opinion?
It’s understandably frustrating when you’ve asked for expert help and your local hospital insists on keeping things “in-house.” Here are some reasons this might happen:
1. Internal Referral Rules
Hospitals sometimes have a policy to refer to another consultant within their own department first. They may consider this a “second opinion,” even if it’s not truly independent.
2. Cost and Complexity
Referrals to another NHS trust — especially across health boards or into England (e.g. to NAC) — can involve extra steps and costs. Some hospitals prefer to avoid that unless they feel there’s no choice.
3. Professional Sensitivities
Some doctors may feel a national second opinion implies criticism of their care, even if your request is made respectfully.
4. Lack of Awareness
Some clinicians aren’t fully aware of what the National Aspergillosis Centre offers — or may underestimate how complex aspergillosis, ABPA, or recurrent fungal infections can be.
🧑⚕️ But Isn’t a Specialist Opinion My Right as an NHS Patient?
Yes. If your GP or hospital team believes it’s clinically appropriate, you have the right to be referred to another NHS consultant — including one outside your local area.
The NAC is nationally commissioned by NHS England to provide care for people with chronic aspergillosis. They accept referrals from across the UK.
💷 Why Private Care Might Not Be an Option
Some patients consider going private when local NHS referrals are blocked — but private care often means:
-
Paying for new scans, blood tests, and sputum cultures
-
No direct access to previous NHS records
-
Higher costs than expected, especially for complex tests
If you can’t afford this, you are not alone, and there are still NHS options available.
🧭 What You Can Do Next
Here are practical steps if you're being blocked from getting a second opinion:
✅ 1. Restate Your Request Clearly
Ask your GP (or write yourself) to reply to the hospital and explain:
-
You are specifically asking for an opinion from a national expert service (e.g. NAC or Dr Iain Page in Edinburgh).
-
This is not a rejection of their care, but a request for specialist reassurance, diagnosis support, or treatment planning.
✅ 2. Ask for a Tertiary Centre Referral
Use the term “tertiary referral” — this means a referral to a national or highly specialised NHS service.
✅ 3. Raise It with PALS
If you're still being blocked, contact your local Patient Advice and Liaison Service (PALS) or NHS complaints team. Explain:
-
You have a rare/complex condition,
-
You’ve asked for a national review,
-
And you’ve been offered only an internal opinion.
✅ 4. Get support on NAC Support Facebook Group
- https://www.facebook.com/groups/aspergillussupport/
💬 In Summary
-
You’re not being difficult — you’re advocating for your health.
-
It is reasonable and often necessary to seek input from specialists like those at the NAC.
-
If you’ve been told “no,” it may be due to policies or misunderstandings — not a reflection on your need for better care.
-
Keep asking, and if needed, involve your GP, or PALS.
🌿 Living with Chronic Pulmonary Aspergillosis (CPA):
Hope, Setbacks, and What “Cure” Really Means
Being diagnosed with chronic pulmonary aspergillosis (CPA) is often overwhelming. You may be on treatment with antifungals like itraconazole (Sporanox) and have already gone through ups and downs — early improvement, then a period of stagnation, and now you're facing a new CT scan with anxiety.
You’re not alone — and this guide brings together the key questions patients often ask, along with helpful real-life insights.
✅ “I Felt Better at First — Then It Stalled. Why?”
This is very common in CPA. In the first few months:
-
Symptoms like cough, breathlessness, and fatigue may improve.
-
CT scans may show fungal balls shrinking or disappearing.
But then: -
Symptoms return or stay the same.
-
Scans show little change.
-
Anxiety grows.
This doesn’t mean treatment has failed.
It may just mean you've reached a slower phase of healing. Here's why:
| Reason | What’s Happening |
|---|---|
| Antifungal success at first | Fungal load drops, but scarring and inflammation remain. |
| Itraconazole is working | But drug levels may be too low — monitoring is essential. |
| Other lung conditions coexist | Like bronchiectasis or NTM, which antifungals don’t treat. |
| Ongoing exposure to mould | Especially from damp buildings, compost, or dust. |
| Immune response adapts | Symptoms may persist even if fungus is under control. |
🔁 “Can Things Improve Again?”
Yes — many people improve again after a plateau or setback.
What helps:
-
✅ Check your itraconazole blood level — low levels = poor response.
-
✅ Consider a switch to another antifungal, like voriconazole or posaconazole.
-
✅ Ask your team about co-infections, inhaled therapies, or lung physiotherapy.
-
✅ Monitor your vitamin D, weight, and steroid use (to rule out other causes of symptoms).
-
✅ Keep going — many people improve again with time, adjustments, and support.
🗣️ “I had a dip after three months. We checked my drug levels — they were low. After a small dose change, I felt better again.” — Patient story
💬 “Can CPA Be Cured?”
🩺 What Do We Mean by “Cure”?
In medicine, a cure usually means:
-
The disease is gone,
-
Treatment is no longer needed,
-
There’s no sign of the illness coming back.
But in CPA, a full cure is rare — because the conditions that allowed it to take hold usually remain.
⚠️ Why CPA Is Rarely “Cured” in the Traditional Sense
-
CPA often happens in lungs already damaged by:
-
Tuberculosis (TB)
-
COPD or emphysema
-
Bronchiectasis
-
Allergic bronchopulmonary aspergillosis (ABPA)
These conditions are chronic and don’t disappear, even if the fungus is controlled.
-
-
Scars, cavities, and weakened lung tissue remain, and symptoms can return if antifungal treatment is stopped too soon or if reinfection occurs.
✅ So What’s a More Accurate Way to Think About It?
Instead of talking about a cure, specialists use words like:
| Term | What It Means |
|---|---|
| Clinical improvement | You feel better, symptoms reduce, scans look more stable. |
| Stability | The disease is under control — not progressing. |
| Remission | The infection is quiet or inactive — with or without treatment. |
| Disease control | Long-term treatment is helping manage the condition safely. |
📌 Think of CPA like asthma or diabetes — not "gone," but often well controlled.
🟢 Sometimes — CPA can be cured
In a small number of people:
-
The fungus is cleared completely,
-
Symptoms resolve,
-
Antifungals are stopped and not needed again.
This is more likely when:
-
CPA is caught early,
-
The disease is limited to one area,
-
The person has otherwise healthy lungs.
🟡 For Most — CPA is treatable but long-term
You may not fully “get rid of it” — but you can:
-
Live well with it,
-
Keep symptoms under control,
-
Avoid major complications.
🔴 If untreated, CPA can progress
-
Damage spreads,
-
Bleeding may worsen,
-
General health may decline.
That’s why staying on treatment and having regular check-ups is so important.
🔪 What About Surgery?
Surgery can help in some cases — but it depends on your specific situation.
🟢 Surgery may help if:
-
You have a single aspergilloma (fungal ball).
-
You're experiencing repeated bleeding (haemoptysis).
-
The lesion is growing or pressing on nearby structures.
-
Antifungals haven’t worked, or aren’t tolerated.
In these cases, removing part of the lung may stop bleeding, reduce symptoms, and improve quality of life.
🔴 Surgery may not be suitable if:
-
Disease affects both lungs or multiple areas.
-
Your lung function is too low.
-
The lesion is too close to vital structures.
-
You have underlying conditions like COPD, bronchiectasis, or ABPA that wouldn’t improve after surgery.
🩺 If surgery isn’t an option:
You may still benefit from:
-
Bronchial artery embolisation (BAE) — a non-surgical way to stop bleeding.
-
Ongoing antifungal therapy.
-
Symptom management through breathing support and physiotherapy.
💬 What Other Patients Say
| Patient Story | Outcome |
|---|---|
| “My fungal ball vanished after 6 months. I’m still on meds but doing well.” | Stable with long-term itraconazole |
| “I plateaued, then improved again after switching drugs.” | Switched to posaconazole |
| “I had surgery after coughing up blood for months. It made a huge difference.” | Surgery successful |
| “I live with scarring, but I’m off meds now and stable.” | Clinical remission |
🧾 What You Can Do
-
✅ Ask your doctor to check your itraconazole level if not already done.
-
✅ Record weekly symptoms — cough, fatigue, breathlessness.
-
✅ Ask about sputum tests for fungi or bacteria.
-
✅ Discuss surgery or embolisation if you’re coughing up blood.
-
✅ Stay hopeful — CPA is manageable, and some people do recover.
❤️ Final Thoughts
CPA is rarely curable in the strictest sense, but that doesn’t mean it’s hopeless.
Many people live full lives with the disease under control. Even if CT scans show lasting changes, what really matters is:
How you feel. How well you breathe. How stable your condition stays.
With antifungal therapy, expert care, and the right support, you are not alone — and you can feel better again.
🛡️ Choosing the Best Air Filter for Aspergillosis – Day & Night
Living with aspergillosis (such as ABPA, CPA, aspergillus bronchitis, or SAFS) means taking extra care to avoid airborne Aspergillus spores, which can be found both outdoors and indoors. One of the most effective ways to protect yourself at home is by using a high-quality air purifier.
This guide will help you choose a purifier that works for you — especially for bedroom use at night, where quiet operation is just as important as clean air.
🎯 Why Use an Air Filter?
-
Aspergillus spores are tiny (2–3 microns), invisible to the eye, and can remain airborne for long periods.
-
Indoor sources include dust, damp areas, stored food, compost, or even indoor plants.
-
A HEPA air purifier can trap these particles, helping reduce airway irritation, infections, or allergic reactions.
✅ What to Look For
| Feature | Why It Matters |
|---|---|
| True HEPA Filter | Captures ≥99.97% of particles ≥0.3 microns — includes Aspergillus spores |
| Activated Carbon Filter | Helps remove odours, gases, VOCs (optional bonus) |
| Room Size & CADR | Clean Air Delivery Rate (CADR) should match or exceed your room’s size |
| Quiet Operation | For night-time use, look for ≤25–30 dB (whisper-quiet) |
| Sleep Mode / Dim Lights | Prevents disturbance from lights or fan noise overnight |
| Filter Replacement | Easy to change, ideally with indicator for when to replace |
| No Ozone or Ionisers | Avoids irritation to sensitive lungs — stick with mechanical HEPA filtration |
🌙 Night-Time Friendly Options
| Model | Noise (dB) | Room Size | Notes |
|---|---|---|---|
| Blueair Blue Pure 411 Auto | 17 dB | Up to 35 m² | Super-quiet, ideal for small bedrooms |
| Levoit Core 300S | 24 dB | Up to 40 m² | Quiet, smart controls, affordable |
| Philips 3000i AC3033 | 25 dB | Up to 104 m² | Excellent for larger spaces, smart app |
| IQAir Atem Desk | <22 dB | Personal zone | Ultra-quiet, high-quality for desks/bedsides |
| Dyson Purifier Cool | ~24–32 dB | Medium–large | Stylish, also a fan, more expensive |
Tip: Choose a unit slightly larger than your room size for best effect.
💡 Extra Tips for Aspergillosis Patients
-
✅ Vacuum with a HEPA filter weekly
-
✅ Keep humidity below 50% (use a dehumidifier if needed)
-
✅ Avoid ionizers or ozone generators — these can irritate your lungs
-
✅ Close windows at night during high pollen or spore seasons
-
✅ Clean or change filters regularly (check manufacturer’s guide)
🛏 Night Setup Checklist
-
Place the purifier 1–2 metres from your bed (not right next to your face)
-
Use “Sleep Mode” or low fan for silent overnight cleaning
-
Turn off indicator lights (if bright)
-
Close doors and windows to keep clean air contained
-
Replace filters every 6–12 months or as prompted
📌 Summary
| Must-Have Features | Optional but Useful |
|---|---|
| ✅ True HEPA filtration | 🌫 Activated carbon filter |
| ✅ Quiet night mode (<25 dB) | 📱 Smart controls or auto mode |
| ✅ Right room size / CADR rating | 🌡 Monitor for humidity or air quality |
| ✅ No ozone, no ionizers | 🔁 Filter change indicator |
🗨️ Final Thought
For aspergillosis patients, an air purifier is a worthwhile investment in long-term lung health — especially in sleeping areas where your body is most vulnerable. Choosing the right device helps reduce exposure to fungal spores and improves quality of life, one breath at a time.
📁 Coping with Steroid Side Effects and Finding Balance: A Guide for Aspergillosis Patients
Living with chronic forms of aspergillosis—such as chronic pulmonary aspergillosis (CPA), allergic bronchopulmonary aspergillosis (ABPA), severe asthma with fungal sensitisation (SAFS), or Aspergillus bronchitis—often means taking corticosteroids like prednisolone or hydrocortisone. These powerful medicines can be life-saving, but they also come with physical and emotional side effects, especially at high doses or when taken over long periods.
This guide is here to support you with practical tips, patient stories, and advice on reducing steroids while maintaining your quality of life.
🔊 What Do Steroids Do?
Steroids reduce inflammation and calm overactive immune responses. They're commonly used in aspergillosis to:
- Manage allergic reactions (e.g. in ABPA)
- Control lung inflammation
- Treat adrenal insufficiency or steroid withdrawal symptoms
🔁 Why Reducing Steroids Can Be So Difficult
Steroids are very effective but also powerful. Tapering the dose can cause:
- Return of pain, fatigue, breathing problems, or inflammation
- Steroid withdrawal symptoms (fatigue, low mood, joint pain)
- Adrenal suppression if the body has stopped making its own cortisol
Many patients report:
“I reduced by 1mg and everything fell apart.” “I want to be on less, but life is unbearable when I try.”
You are not failing. Finding the right dose is a balance between lowering risks and keeping your life manageable.
🛋 Common Side Effects and What You Can Do
| Side Effect | Tips to Cope |
|---|---|
| Increased appetite | Plan balanced meals, high-fibre snacks, drink water, be kind to yourself |
| Weight gain / swelling | Gentle movement, reduce salt, try pressotherapy (discuss with your team) |
| Mood swings or anxiety | Talk about it, track your feelings, ask about counselling or peer support |
| Insomnia | Avoid caffeine late, consider timing of dose, try a calming bedtime routine |
| "Moon face" / puffiness | Often fades when dose is reduced; hydrate and moisturise |
| Muscle/joint pain or weakness | Gentle stretches, walking, low-impact activity, speak to a physio if needed |
| Bruising/thin skin | Moisturise, protect from bumps, avoid strong detergents |
| Raised blood sugar | Eat regularly, reduce sugary drinks, ask about monitoring if concerned |
| Bone thinning | Ask about calcium, vitamin D, or bone-protecting medications |
| Adrenal suppression | Never stop suddenly; always taper with a doctor's guidance |
👥 Real Patient Stories and Analogies
🐻 Alison's Bears
“There are two bears inside me. Prednisone Bear is wild and wants to eat and sleep and snap. But Rusty McTravel Bear is my real self—gentle, curious, slowly trying to get back on the road. I’ve learned to recognise the first and nurture the second.”
🏎️ The Revving Car
“Being on steroids sometimes feels like a car with the engine revving but the brakes on. You’re buzzing, but you’re stuck. Try easing the brakes: take a walk, make tea, do something simple to use the energy.”
🚩 Finding Your Balance: When Less Isn't Always Better
✅ Go slow
- Taper in small steps—as little as 0.5–1mg at a time
- Wait several weeks between reductions
✅ Keep a steroid diary
- Note dose, mood, sleep, symptoms, activity
- This helps identify your "minimum effective dose"
✅ Accept that a small maintenance dose may be necessary
- You are not failing if you need 2mg, 5mg, or 7.5mg long-term
- The goal is a life worth living, not perfection
✅ Ask about alternatives
- Inhaled steroids, antifungals, or biologics might help reduce systemic steroid use
✅ Consider adrenal testing
- Especially if you feel unwell during tapering or on low doses
🛏️ Other Strategies That May Help
- Pressotherapy for leg pain and swelling
- Mindfulness or breathing exercises for anxiety or insomnia
- Peer support (online or in person)
- Short-term plans: some patients use a "rescue dose" plan for flare-ups
- Talk to your care team: never reduce on your own without guidance
💼 Summary
Reducing or living with steroids is not just about doses. It’s about protecting your body and your sense of self. If a small daily dose keeps you functioning, that is not weakness—it’s balance.
You are not alone. Many in the aspergillosis community are navigating this same path.
“The right dose is the one where I can breathe, move, smile — and still feel like myself.”
🛡️ Staying Safe with Self-Treatment and Complementary Therapies: A Guide for Aspergillosis Patients
Living with a chronic condition like aspergillosis — whether chronic pulmonary aspergillosis (CPA), allergic bronchopulmonary aspergillosis (ABPA), severe asthma with fungal sensitisation (SAFS), or aspergillus bronchitis — can be exhausting. Many patients explore over-the-counter (OTC) products, natural remedies, or complementary therapies to gain a sense of control.
But how can you be sure a product or therapy is safe, effective, and not a waste of money?
This guide aims to help.
🔍 Why Do Patients Try Things on Their Own?
In many countries, it’s common to self-medicate or explore alternative treatments without consulting a healthcare professional. Reasons include:
-
Limited access to specialist care
-
Cultural norms that favour self-management
-
Easy access to remedies and supplements online or in shops
-
Feeling unheard or unsupported in mainstream medical care
Even in the UK, patients with aspergillosis may turn to:
-
Herbal products
-
Nutritional supplements
-
Creams or gels with capsaicin (chilli), turmeric, or menthol
-
Breathing techniques, steam inhalation
-
“Immune-boosting” diets or over-the-counter fungal cleanses
Some of these may be helpful — but not all are safe or worthwhile.
✅ Step 1: How to Check if a Product or Therapy Is Safe
Before trying anything new, ask:
1. Is it approved or regulated in the UK?
Medicines and certain creams should have a Product Licence (PL) number, issued by the Medicines and Healthcare products Regulatory Agency (MHRA).
You can check the licence on the MHRA product registry.
2. Could it interact with your prescribed medications?
-
Some herbal remedies affect azole antifungal drugs (like itraconazole or voriconazole) or oral steroids.
-
Ask your GP (General Practitioner), specialist, or pharmacist before combining treatments.
3. Is it safe to apply or inhale?
-
Never use essential oils, menthol, or herbal mixtures in a nebuliser unless clearly intended for lung use.
-
Avoid applying hot or irritating creams to broken or sensitive skin.
4. Is it mentioned in NHS guidance?
Stick to advice on:
-
Your local hospital trust’s respiratory or infectious disease guidelines
-
National Institute for Health and Care Excellence (NICE) recommendations
-
Cochrane Reviews or published clinical trials
⚠️ Watch Out for Red Flags
Be cautious of any product, practitioner, or website that:
| 🚩 Red Flag | ⚠️ Why It’s a Concern |
|---|---|
| Claims to “cure” aspergillosis | There is no cure — only long-term management |
| Says it’s “100% natural with no side effects” | Natural products can still be harmful |
| Uses high-pressure sales tactics | Legitimate care is never urgent or fear-based |
| Recommends stopping your prescribed treatment | Stopping antifungals or steroids can be dangerous |
🧪 Step 2: Look for Evidence, Not Just Testimonials
Some treatments are promising — but we need solid evidence to know they work.
✅ Good sources of trustworthy evidence:
-
Cochrane Library (systematic reviews of healthcare studies)
-
Electronic Medicines Compendium (EMC): www.medicines.org.uk
-
NHS Trust guidelines or clinical leaflets
-
Published studies on PubMed, ClinicalTrials.gov, or from recognised research institutions
💬 Can You Trust a Pharmacist?
Yes — in most cases, UK pharmacists are highly trained and regulated. However, there are two kinds to be aware of:
| Type of Pharmacist | What to Know |
|---|---|
| Retail Pharmacist | May sell you products directly; still bound by safety standards |
| Clinical Pharmacist (in GP surgeries or hospitals) | Focused entirely on clinical care and not sales-driven |
Both are regulated by the General Pharmaceutical Council (GPhC) and must put patient safety first, regardless of sales.
🟢 Ask them:
-
“Will this interact with my medications?”
-
“Is this supported by NHS or NICE?”
-
“Would this be suitable for someone with CPA or ABPA?”
🧘 What About Complementary Therapies?
Some patients explore:
-
Acupuncture
-
Herbal medicine
-
Osteopathy or chiropractic
-
Reflexology or massage
-
Nutritional therapy
-
Mindfulness and yoga
These may help with:
-
Muscle or joint pain
-
Fatigue and sleep problems
-
Emotional stress or anxiety
They can complement your medical treatment — but should never replace it.
✅ Safe if:
-
Practitioner is registered with a reputable UK body
-
The therapy does not interfere with prescribed medications
-
It is used for symptom relief, not for “cleansing” or treating the infection
❌ Risky if:
-
It’s marketed as a cure for aspergillosis
-
It encourages you to stop medical treatment
-
It is expensive, secretive, or vague about its effects
Reputable UK Registers:
| Practitioner Type | Regulator / Body |
|---|---|
| Acupuncturists | British Acupuncture Council (BAcC) |
| Herbalists | National Institute of Medical Herbalists (NIMH) |
| Osteopaths | General Osteopathic Council (GOsC) |
| Chiropractors | General Chiropractic Council (GCC) |
| Nutritionists | Association for Nutrition (AfN) |
🧾 Summary: A Safer Way to Explore New Treatments
| ✅ Do This | ❌ Avoid This |
|---|---|
| Check the MHRA or NHS website | Trusting social media or forums alone |
| Look for a PL number and regulated status | Using unlicensed creams, drops, or nebuliser fluids |
| Ask your pharmacist or GP about interactions | Assuming “natural” means harmless |
| Use one new treatment at a time | Trying multiple new remedies together |
| Start with low doses or small trial sessions | Buying expensive long-term “packages” up front |
📘 Real Example: Using Capsaicin Cream for Pain
Some patients with back pain or joint discomfort have tried capsaicin cream (chilli-based), especially if they cannot tolerate non-steroidal anti-inflammatory drugs (NSAIDs) like ibuprofen.
✅ It’s safe for many people when:
-
Applied in small amounts to intact skin
-
Hands are washed after use
-
Used up to 4 times daily
-
Product is licensed (e.g. Zacin® 0.025%)
⚠️ It may cause a burning feeling for the first few days.
Avoid contact with eyes, mouth, or mucous membranes.
Ask a pharmacist before use — especially if you’re on steroids, have skin thinning, or are very sensitive to heat or irritation.
🗂️ Want to Learn More?
-
Visit www.aspergillosis.org
-
Contact the National Aspergillosis Centre (NAC) in Manchester
-
Speak to your GP or hospital respiratory specialist
-
Ask in trusted support groups like the Aspergillosis Support Facebook Group