🫁 Understanding ABPA: When and Why It Appears, and Who’s at Risk
Allergic Bronchopulmonary Aspergillosis (ABPA) is a chronic allergic lung condition that’s often misunderstood or misdiagnosed — especially when it appears for the first time in adulthood. This article answers key questions:
-
Why does ABPA usually develop later in life?
-
Can it be diagnosed earlier?
-
What about severe asthma in children — is that an exception?
-
Are there groups at special risk, like those with cystic fibrosis?
This guide is designed for patients, carers, and anyone living with or at risk of ABPA.
🔹 1. What Is ABPA?
ABPA is a hypersensitivity reaction (not a fungal infection) to the fungus Aspergillus fumigatus, which is found in the air we breathe.
In people with asthma, cystic fibrosis (CF), or structurally damaged lungs, Aspergillus can settle in the airways and trigger a strong allergic immune response, causing:
-
Swollen and inflamed airways
-
Mucus build-up that’s hard to clear
-
Worsening of asthma or coughing
-
Irreversible lung damage (e.g. bronchiectasis) if untreated
🔎 2. Why Is ABPA Usually Diagnosed in Adulthood?
Despite being linked to asthma — often a childhood condition — most cases of ABPA are diagnosed in adulthood, typically between ages 20 and 50.
Why? Because ABPA is only diagnosed when several things happen at the same time:
-
High total IgE levels
-
Positive Aspergillus-specific IgE or IgG
-
Lung symptoms like wheezing, cough, mucus
-
CT evidence of mucus plugging or early bronchiectasis
A person might be allergic to Aspergillus (sensitised) for years without having ABPA. Only when their immune system crosses a certain threshold — sometimes after a viral illness, fungal exposure, or change in immune function — does full ABPA emerge.
This helps explain why many people are diagnosed for the first time in their 30s or later, even with a history of asthma.
🧒 3. Is ABPA Ever Diagnosed in Childhood?
✅ Yes — but it’s rare.
There are a few specific exceptions:
🔸 A. Cystic Fibrosis (CF)
-
ABPA is much more common in people with CF — including older children and teenagers.
-
CF causes thick mucus and impaired airway clearance, which promotes persistent exposure to Aspergillus.
-
That’s why CF care guidelines include annual ABPA screening from a young age.
🔸 B. Severe asthma in childhood
-
Children with very severe or poorly controlled asthma may have:
-
High IgE
-
Mucus build-up
-
Sensitisation to Aspergillus
-
-
These children may develop fungal allergic airway disease or be labelled as having SAFS (Severe Asthma with Fungal Sensitisation).
-
Full ABPA may still not be diagnosed until later adolescence or adulthood — but these cases may represent a kind of “pre-ABPA.”
🔸 C. Rare immune disorders
-
Conditions like hyper-IgE syndrome (HIES) or chronic granulomatous disease may cause early ABPA-like features.
-
These are rare and usually managed by immunology specialists.
⚖️ 4. What’s the Difference Between ABPA, SAFS, and Sensitisation?
| Condition | Description | Age group |
|---|---|---|
| Aspergillus sensitisation | Immune system reacts to fungus, but no lung damage or ABPA symptoms | Any age |
| SAFS | Severe asthma + Aspergillus allergy, but does not meet full ABPA criteria | Mostly teens and adults |
| ABPA | Allergy to Aspergillus + lung damage, high IgE, mucus, flare-ups | Usually adults, sometimes teens with CF |
🧪 5. Could a Screening Test Detect ABPA Earlier?
Not currently — but research is ongoing.
Today, ABPA is diagnosed based on a set of criteria (IgE levels, imaging, symptoms), not a single test. That means:
-
Early warning signs may be present for years
-
But ABPA is only diagnosed once enough features appear together
A future screening test for “pre-ABPA” could:
-
Identify at-risk individuals earlier
-
Allow close monitoring
-
Help start treatment at the first signs of disease
This wouldn’t “prevent” ABPA in every case, but could reduce its severity and protect lung function.
💡 6. Can ABPA Be Prevented?
We can’t fully prevent ABPA — but we can reduce risk and prevent long-term damage:
| Strategy | What It Helps Prevent |
|---|---|
| Reduce fungal exposure (damp, compost, hay) | Immune flare-ups, new sensitisation |
| Monitor at-risk patients (CF, severe asthma) | Missed early signs |
| Treat asthma or CF aggressively | Mucus build-up and fungal colonisation |
| Investigate persistent cough/mucus or asthma flares | Delayed ABPA diagnosis |
| Use steroids/antifungals/biologics when needed | Inflammation, progression to bronchiectasis |
📘 7. Summary: Key Takeaways
| Question | Answer |
|---|---|
| Is ABPA a childhood disease? | No, it’s usually diagnosed in adults, even those with childhood asthma |
| Can it appear in children? | Rarely — mostly in CF, severe asthma, or immune disorders |
| Why isn’t it diagnosed earlier? | It requires multiple features to appear at the same time |
| Can it be stopped before it starts? | Possibly in future — early monitoring could reduce damage, even if it doesn’t prevent ABPA |
| What should I do? | Avoid triggers, manage asthma/CF well, seek early specialist input for unexplained symptoms |
🗣️ Patient Tip
“If you’ve just been diagnosed in your 30s, 40s or later — that doesn’t mean it was missed. It means it’s finally been recognised, and now you can get the right treatment.”
🌦️ Staying Safe with Aspergillosis During UK Weather and Health Alerts
People living with aspergillosis—including ABPA, CPA, Aspergillus bronchitis, or those on long-term steroids or antifungals—are especially vulnerable during periods of extreme weather. Understanding official UK weather and health alerts can help you take timely action to protect your lungs and overall health.
🔔 What Are Weather and Health Alerts?
In the UK, two major bodies issue public alerts:
1. Met Office Weather Warnings
-
Focus on immediate weather dangers: storms, heavy rain, wind, snow, ice, and fog
-
Issued in yellow, amber, or red based on severity and risk to life
2. UK Health Security Agency (UKHSA) Health Alerts
-
Focus on health risks from temperature extremes: heatwaves or cold spells
-
Jointly issued with the Met Office as part of the Weather-Health Alerting System
🟨🟧🟥 What the Colours Mean
| Level | What it means | What you should do |
|---|---|---|
| Yellow | Be aware: possible disruption | Stay informed and prepare |
| Amber | Be prepared: likely disruption | Take action to protect health |
| Red | Take action: major risk | Follow emergency advice |
☀️ Heat Alerts and Aspergillosis
Issued from June to September, these alerts warn of high temperatures that may affect health.
🔹 Why Heat Matters:
-
Hot, humid air can worsen breathing in people with lung conditions
-
Ozone and air pollution often rise during heatwaves, irritating airways
-
Aspergillus spores thrive in warm, damp environments, increasing exposure
-
People on antifungals (like voriconazole) may be photosensitive and prone to heat rashes
-
Steroid users may not regulate temperature well, increasing heat stress risk
🔹 What to Do:
-
Stay indoors during the hottest part of the day (11am–3pm)
-
Use fans, cool showers, and keep curtains closed in sunny rooms
-
Drink plenty of fluids (check with your doctor if you have fluid restrictions)
-
Avoid gardening, composting, or opening windows during dry, windy conditions
-
Protect your skin if taking sun-sensitive medications
❄️ Cold Alerts and Aspergillosis
Issued between November and March, these alerts warn of dangerously low temperatures.
🔹 Why Cold Matters:
-
Cold air can tighten airways, leading to coughing or wheezing
-
Cold increases the risk of chest infections in people with CPA or ABPA
-
Damp and mould thrive in unheated homes, raising fungal exposure
-
Cold-related stress can worsen cardiovascular strain and fatigue
🔹 What to Do:
-
Keep indoor temperature at 18°C or above, especially in the bedroom
-
Use dehumidifiers to reduce mould growth
-
Check for leaks or condensation, and ventilate bathrooms and kitchens
-
Wrap up warmly when going outside—wear a scarf over your nose and mouth to warm the air you breathe
-
If you use oxygen or nebulisers, make sure devices are protected from cold damage
🌪️ Storms, Floods & Other Weather Events
The Met Office issues warnings for:
-
Storms (wind, lightning)
-
Heavy rain and flooding
-
Fog
-
Snow and ice
🔹 Risks for Aspergillosis Patients:
-
Flooding or roof damage can promote indoor mould
-
Disrupted power may affect your oxygen concentrator, fridge-stored medication, or nebuliser use
-
Poor air quality may irritate airways
-
Increased fungal exposure after water damage or building repairs
🔹 What to Do:
-
Make a personal emergency plan (backup power for medical equipment, emergency contact list)
-
If your home is damp or recently flooded, ask your local council or housing provider for a mould survey
-
Stay inside during high wind or dust storms
-
Use an FFP2/FFP3 mask if entering dusty or damaged environments
🧭 Who Should Be Extra Cautious?
These alerts are especially important for:
-
People with CPA, ABPA, or bronchiectasis
-
Those on steroids, biologics, or antifungal therapy
-
People with adrenal insufficiency or immune suppression
-
The elderly, babies, or people with mobility or cognitive difficulties
-
People with a history of hospital admissions due to chest infections or exacerbations
📲 How to Get Alerts
You can receive real-time alerts from:
-
Met Office app or website: www.metoffice.gov.uk
-
UKHSA Weather-Health Alerts: often shared via NHS, social care, or local authority newsletters ukhsa-dashboard.data.gov.uk/weather-health-alerts
-
Local news and Twitter/X feeds: follow @metoffice and @UKHSA
-
Sign up for health or vulnerability registers if you receive care at home
✅ Summary: Practical Steps
| Alert Type | Action for Aspergillosis Patients |
|---|---|
| Heat alert | Stay indoors, cool the home, hydrate, reduce spore exposure |
| Cold alert | Heat rooms, reduce damp/mould, stay warm, use respiratory meds as needed |
| Storm/flood | Avoid mould-prone areas, prepare backup power/medication access |
| Air quality | Avoid outdoor exposure, use masks and HEPA filters |
📘 Extra Help & Resources
-
Ask your GP or hospital team if you can be added to a vulnerability list
-
If you’re in social housing, housing officers must act if the home becomes unsafe due to damp or cold
-
For support with mould, damp, or heating costs, contact:
-
Citizens Advice
-
Your local council
-
Your respiratory nurse or hospital’s community support team
-
Understanding the Side Effects of Long-Term Prednisolone Use
Prednisolone is a widely used and effective medication for managing inflammation in aspergillosis. However, when taken for more than 3–4 weeks—especially at moderate or high doses—it can cause unwanted effects in different parts of the body. Knowing what to expect and how to reduce risks can help you feel more in control of your treatment.
Prednisolone is a synthetic form of cortisol, a hormone your body normally produces to manage stress and inflammation. When you take it in larger-than-natural amounts over time, it can interfere with how your body handles fluids, sugar, bone rebuilding, immune function, and even mood and sleep.
Below are the most common side effects and why they happen:
Common Side Effects and Why They Happen
Prednisolone mimics cortisol, a hormone naturally made by your body. But when taken in higher-than-natural amounts over a long time, it can disrupt many systems. Here's why these side effects happen:
- Weight gain and fluid retention – Steroids affect how your body processes salt and water, leading to bloating and weight changes.
- Moon face – Fat redistributes to the face, neck, and abdomen.
- Thinning skin and bruising – Steroids reduce collagen production, making skin fragile.
- High blood pressure – Caused by fluid retention and effects on blood vessel tone.
- Increased risk of infections – Steroids suppress your immune system, making it harder to fight infections.
- Osteoporosis – Steroids interfere with calcium absorption and bone rebuilding.
- Muscle weakness – Corticosteroids break down protein, reducing muscle strength, especially in the thighs and upper arms.
- Mood and sleep changes – Steroids can affect the brain’s chemistry, causing anxiety, insomnia, or mood swings.
- Eye problems – Long-term use can raise pressure in the eyes or cloud the lens (cataracts).
- High blood sugar or diabetes – Steroids make it harder for your body to use insulin effectively. **
What You Can Do to Minimise Side Effects
Managing steroid side effects involves a combination of lifestyle choices and medical support:
| Strategy | Why It Helps |
| Use the lowest effective dose | Reduces cumulative exposure to steroid side effects |
| Switch to hydrocortisone when appropriate | Mimics natural cortisol and is better tolerated long term |
| Monitor blood pressure, bone health, and blood sugar | Early detection helps prevent complications |
| Take calcium, vitamin D, and possibly bone-strengthening medications | Supports healthy bones |
| Exercise regularly | Maintains strength, mobility, and mood |
| Eat a balanced diet low in salt and sugar | Helps manage weight, BP, and blood sugar |
| Keep up with regular medical reviews | Ensures your treatment is safe and effective |
Trusted Resources and Support
You're not alone in managing steroid side effects. These resources offer guidance and community support:
- NHS Steroid Safety Advice: Side effects of prednisolone tablets and liquid - NHS
- Downloadable Steroid Emergency Card: endocrinology.org/adrenal-crisis
- National Aspergillosis Centre resources: aspergillosis.org
- Aspergillosis Trust and NAC patient forum
- Your pharmacist or GP for medication support
- Endocrine nurses for adrenal insufficiency care
Taking charge of your health with the support of your care team can greatly reduce the risks of long-term steroid use.
How to Lessen the Impact of Side Effects
Many of the risks of long-term prednisolone use can be reduced by making small lifestyle changes and working closely with your medical team. These steps can help protect your bones, heart, immune system, and overall wellbeing: You may also find support through:
- Downloadable Steroid Emergency Cards (UK): https://www.endocrinology.org/adrenal-crisis
- National Aspergillosis Centre patient resources: https://aspergillosis.org
- Patient support groups such as the Aspergillosis Trust or National Aspergillosis Centre's patient forum
- Your pharmacist, who can help with medication side effects and monitoring
- Specialist endocrine nurses if adrenal insufficiency is diagnosed
Final Thoughts
Long-term steroid use helps many aspergillosis patients control inflammation and stay well. But it comes with responsibilities — particularly the need to monitor for adrenal suppression.
Understanding the HPA axis, recognising symptoms of AI, and knowing when and how to stress dose can empower you to live safely and confidently with aspergillosis.
Always talk to your specialist team if you’re unsure about fatigue, tapering, or illness management. You are not alone — and support is available.
Understanding the HPA Axis and Long-Term Steroid Use in Aspergillosis
For patients living with ABPA, CPA, or other forms of aspergillosis who have used steroids long term
What is the HPA Axis?
The HPA axis stands for the Hypothalamic–Pituitary–Adrenal axis. It's a vital communication system between three parts of your body:
- The Hypothalamus (in the brain)
- The Pituitary gland (also in the brain)
- The Adrenal glands (on top of your kidneys)
These three work together to manage your body’s response to stress, regulate inflammation, and control levels of a hormone called cortisol.
Cortisol helps you respond to illness, injury, or stress. It also affects energy levels, blood pressure, immune function, and even mood.
How Does the HPA Axis Work?
Here’s a simplified version:
- The hypothalamus senses stress or inflammation and sends a hormone called CRH to the pituitary.
- The pituitary gland then sends ACTH to the adrenal glands.
- The adrenal glands release cortisol, which acts throughout your body to reduce inflammation and keep your systems balanced.
Once enough cortisol is in the blood, it signals the brain to stop releasing more. This keeps the system in balance.
Why Aspergillosis Patients Need to Understand This
Many people with aspergillosis—especially those with ABPA (Allergic Bronchopulmonary Aspergillosis)—are treated with oral corticosteroids such as prednisolone. These steroids reduce inflammation but can also interfere with the HPA axis.
Over time, the body may stop producing natural cortisol because it detects enough from medication. This condition is called adrenal insufficiency (AI) or HPA axis suppression.
Symptoms of Adrenal Insufficiency (AI)
If your adrenal glands are underactive, especially after long-term steroid use, you may experience:
- Extreme fatigue or feeling drained
- Muscle weakness
- Joint pain
- Feeling dizzy or faint, especially when standing
- Low blood pressure
- Nausea, vomiting, or abdominal pain
- Loss of appetite
- Worsening of general health during mild illnesses
In severe cases, a lack of cortisol can lead to an adrenal crisis, which is a medical emergency.
What to Do if You Suspect Adrenal Insufficiency
- Never stop steroids suddenly. Your dose should always be tapered under medical supervision.
- If you’ve been on steroids for several weeks or more, ask your doctor whether you should be tested for adrenal insufficiency using a short Synacthen test, which checks how well your adrenal glands respond to a synthetic version of ACTH (not cortisol itself). Synacthen is not your natural corticosteroid, but it helps doctors assess whether your adrenal glands are producing enough natural cortisol..
- You may be switched from prednisolone to hydrocortisone, which is a more natural replacement for cortisol and easier to adjust during illness.
When to Stress Dose (and Why It Matters)
Your stress dosing plan must always be agreed with your doctor. It should be tailored to your specific needs and medical history. If your body is under stress (e.g., illness, surgery, trauma), it needs more cortisol. If your adrenal glands aren’t working properly, this extra cortisol must come from medication.
Common stress dosing scenarios include:
- Fever over 38°C
- Vomiting or diarrhoea
- Dental surgery or minor operations
- Respiratory infections or flare-ups
- Emotional trauma or physical injury
Typical stress dosing guidance:
- Double your usual dose for 2–3 days during mild illness
- Seek emergency care immediately if you can’t keep down tablets or feel seriously unwell. In some cases, emergency medical staff may need to inject hydrocortisone (100 mg intramuscularly) to stabilise you. This should only be done by trained professionals unless you have been specifically trained and advised to self-administer by your specialist.
Always carry:
- A Steroid Emergency Card
- A medical alert bracelet
- An emergency hydrocortisone injection kit if advised
Why Doctors May Switch You to Hydrocortisone
Even though prednisolone can be used to replace cortisol, some patients still experience symptoms of adrenal insufficiency while on it. This can happen because:
- The dose might be too low for your needs
- Prednisolone doesn’t follow the body’s natural cortisol rhythm, which peaks in the early morning and drops throughout the day
- During illness or stress, the body needs more cortisol, and prednisolone doesn’t automatically increase
- Individuals metabolise steroids differently, so a standard dose may not be right for everyone
Common symptoms despite taking prednisolone may include:
- Ongoing fatigue, especially in the morning or late afternoon
- Poor stress tolerance
- Dizziness or weakness during illness
- Slow recovery after infections
For these reasons, your doctor may switch you to hydrocortisone, which is:
- Shorter-acting and better mimics natural cortisol rhythms
- Easier to adjust during illness or stress
- Often better tolerated long term with fewer side effects Hydrocortisone is shorter-acting and more closely mimics the natural rhythm of cortisol. It is usually taken in two or three doses throughout the day — for example, a larger dose in the morning, a smaller dose at lunchtime, and sometimes a final small dose in the early afternoon. This schedule helps replicate the natural daily rise and fall of cortisol and may improve energy levels, mood, and overall well-being.. It may be preferred if:
- You’re tapering from long-term prednisolone
- You’ve developed confirmed adrenal insufficiency
- You need a safer long-term maintenance dose
- You experience steroid-related side effects
Key Reminders for Aspergillosis Patients
| Do This | Why It Matters |
|---|---|
| Follow your tapering plan | Prevents adrenal crisis |
| Ask about adrenal testing if fatigued | Catches suppressed adrenal function early |
| Know your sick-day rules | Allows for stress dosing during illness |
| Consider switching to hydrocortisone | Safer, more natural for long-term hormone replacement |
| Carry emergency ID and hydrocortisone | Life-saving in a crisis |
Final Thoughts
Long-term steroid use helps many aspergillosis patients control inflammation and stay well. But it comes with responsibilities — particularly the need to monitor for adrenal suppression.
Understanding the HPA axis, recognising symptoms of AI, and knowing when and how to stress dose can empower you to live safely and confidently with aspergillosis.
Always talk to your specialist team if you’re unsure about fatigue, tapering, or illness management. You are not alone — and support is available.
Understanding ABPA: A Patient Guide to Managing Allergic Bronchopulmonary Aspergillosis
Being newly diagnosed with ABPA (Allergic Bronchopulmonary Aspergillosis) can feel overwhelming, especially when faced with complicated information online. You may hear about disease stages, possible complications, and unfamiliar terms. This guide is here to reassure you: ABPA is a manageable condition, and with the right treatment and monitoring, many people live full and active lives.
What Is ABPA?
ABPA is an allergic reaction in your lungs caused by a fungus called Aspergillus fumigatus. It's more likely to affect people with existing lung conditions such as:
- Asthma
- Bronchiectasis
- Cystic fibrosis (in some cases)
The immune system overreacts to the presence of Aspergillus, leading to inflammation, mucus buildup, and sometimes long-term lung changes.
Can ABPA Become CPA?
Some people worry that ABPA might turn into CPA (Chronic Pulmonary Aspergillosis), a separate fungal lung infection.
- This only happens in a small number of people, usually those with severe lung damage or cavities.
- If ABPA is well-managed early, the chances of developing CPA are very low.
- Your care team can monitor for this with scans and blood tests.
The 5 Stages of ABPA: What Do They Mean?
The stages of ABPA are used by doctors to describe how the disease behaves, not to predict life expectancy.
| Stage | What It Means |
|---|---|
| 1 | Acute: Flare-up with symptoms and high IgE |
| 2 | Response to treatment |
| 3 | Remission: Symptoms and inflammation settle |
| 4 | Relapse: New flare-up after remission |
| 5 | Fibrotic: Long-term scarring in the lungs |
Even Stage 5 is not a death sentence. Some people live in this stage for many years with stable symptoms. It just means that some lung changes have become permanent.
Key Goals of ABPA Management
With the right care, people with ABPA can:
- Prevent long-term lung damage
- Reduce flare-ups
- Stay active and independent
Your treatment may include:
- Corticosteroids to reduce inflammation
- Antifungal medications (like itraconazole) to reduce fungal burden
- Biologics (like omalizumab or dupilumab) in some cases
- Mucus clearance physiotherapy
- Environmental control to reduce exposure to mould and dust
What You Can Do to Stay Well
- Stick to your treatment plan and attend regular check-ups
- Monitor symptoms like coughing, mucus, breathlessness or chest pain
- Practice good airway clearance techniques
- Avoid triggers: e.g., mould, compost, damp areas
- Seek support: Patient groups, nurses, respiratory therapists can help
Final Reassurance
Being diagnosed in February means you are still early in your journey, and that’s a good thing. You have time to learn, adapt, and manage your condition.
ABPA does not mean you are dying — it means you are living with a chronic condition that can be controlled with the right tools and knowledge.
You are not alone, and with support, you can live well with ABPA.
🌿 Complementary Therapies and Aspergillosis: What Helps, What Doesn’t
Living with aspergillosis — whether it's ABPA, CPA, SAFS, or another form — can be physically and emotionally challenging. While medical treatments like antifungals, steroids, or biologics remain essential, many people ask:
“Can alternative or complementary therapies help with my symptoms or recovery?”
The short answer is: some can support your wellbeing, but they must be used safely and alongside your prescribed care. This guide helps you understand what’s worth exploring — and what to avoid.
🟢🟡🔴 Traffic Light Guide to Complementary Therapies
This guide helps you navigate the wide range of alternative treatments — showing what’s generally safe, what to approach with caution, and what may cause harm.
🟢 GREEN – Generally Safe & Often Helpful
| Therapy | Benefit | Notes |
|---|---|---|
| Airway clearance (ACTs, postural drainage) | Clears mucus, reduces infection risk | Best when guided by physiotherapy |
| Mindfulness / breathing exercises | Helps anxiety, reduces flare-ups | Supports emotional balance |
| Vitamin D (with testing) | May improve immune regulation | Deficiency is common in chronic conditions |
| Yoga / tai chi / gentle stretching | Improves lung mobility, energy | Avoid overexertion during flares |
| CBT / talking therapy | Helps manage fear, fatigue, trauma | Often underused but effective |
| Steam inhalation (plain or saline) | Loosens mucus | Avoid if you’re chemically sensitive |
| Probiotics (capsules or pasteurised products) | Rebuilds gut after antibiotics | Avoid live cultures if immunocompromised |
🟡 AMBER – Use with Caution
These may offer some support, but need discussion with your doctor or asthma nurse.
| Therapy | Claimed Use | Caution |
|---|---|---|
| Curcumin (turmeric extract) | Anti-inflammatory | May interact with meds; avoid high doses |
| Ginger, green tea | Mild antioxidant effect | Some people are sensitive or intolerant |
| Salt therapy (halotherapy) | Loosens mucus | May irritate lungs if dry or unregulated |
| Essential oils (external use only) | Relaxation | May trigger asthma or MCS |
| Acupuncture | Pain or immune balance | Choose practitioners familiar with lung disease |
| Herbal teas (e.g. liquorice, chamomile) | Stress relief | Liquorice can raise BP and potassium levels |
🔴 RED – Avoid These
These therapies are unproven, unsafe, or known to cause harm — especially in people with respiratory or immune-related illness.
| Therapy | Risk |
|---|---|
| Homeopathy | No evidence of effectiveness; delays real treatment |
| Unregulated antifungal herbs (e.g. oregano oil, pau d’arco) | Potential liver damage, interactions |
| Colloidal silver | Can damage organs, build up in body |
| Ingesting essential oils | Toxic to lungs and digestive system |
| Raw unpasteurised probiotics | Unsafe for immunocompromised patients |
| Detox diets / extreme fasting | Can lead to weakness, adrenal crash (especially if on steroids) |
💬 What About "Immune Boosting"?
Be careful with products or diets claiming to "boost" your immune system. In ABPA and SAFS, the immune system is already overreacting. Instead, the goal is to calm or rebalance inflammation — often through medications like biologics, not immune stimulants.
📌 Tips for Safe Use of Complementary Therapies
-
Always tell your doctor about anything new you’re trying
-
Check for interactions with antifungals, steroids, or blood pressure medication
-
Watch for chemically sensitive reactions (some ABPA patients are triggered by fragrances, sprays, or supplements)
-
Focus on whole-body support: rest, nutrition, lung clearance, and emotional wellbeing
🧠 Key Takeaway
Complementary therapies can help you feel better, breathe easier, and cope with the mental toll of chronic illness — but they are not a substitute for medical treatment.
Choose therapies that are:
-
Evidence-informed
-
Used alongside your prescribed care
-
Safe for your specific condition
🫁 Do Lung Cavities Ever Heal? A Guide for People with Aspergillosis

If you’ve been diagnosed with aspergillosis and have lung cavities (also called cavitary lesions), you may be wondering:
Will these cavities go away? Can lungs heal from this?
The answer isn’t simple — but with the right care and monitoring, you and your medical team can understand what’s likely in your case.
🧬 What Causes Lung Cavities in Aspergillosis?
Lung cavities are hollow spaces in lung tissue. In people with aspergillosis, they can develop for different reasons:
-
In Chronic Pulmonary Aspergillosis (CPA), cavities are often long-standing and may contain a fungal ball (aspergilloma)
-
In Allergic Bronchopulmonary Aspergillosis (ABPA), they may follow an episode of severe infection like pneumonia or result from long-term inflammation and airway damage
-
In invasive aspergillosis, especially in people with weak immune systems, rapid tissue damage can lead to new cavities
Sometimes, cavities form in people who already have underlying conditions like:
-
Tuberculosis
-
Sarcoidosis
-
COPD
-
Bronchiectasis
✅ When Lung Cavities Might Heal
Some lung cavities can heal or shrink over time — especially if:
-
The original infection (e.g. pneumonia or invasive aspergillosis) has fully cleared
-
There is no ongoing fungal infection
-
The cavity is thin-walled and small
-
Your body is able to mount a good healing response
In these cases, the lung may scar over, and the cavity can slowly close or shrink over several months.
🟡 When Cavities Are Less Likely to Heal
Cavities may persist or even worsen if:
-
There is ongoing infection with Aspergillus fumigatus or another fungus
-
You have CPA, where cavities are part of the disease
-
The cavity contains an aspergilloma (fungal ball)
-
You have long-term inflammation or damage from previous diseases like TB or ABPA
-
You're on long-term steroids or immunosuppressants, which affect healing
In these situations, cavities often remain and may need long-term monitoring or treatment.
🔍 How Are Cavities Monitored in Aspergillosis?
Your team will usually monitor lung cavities with:
| Test | Purpose |
|---|---|
| Chest CT scans | To see if the cavity is stable, shrinking, or changing shape |
| Blood tests (Aspergillus IgG, CRP, etc.) | To check for signs of infection or inflammation |
| Sputum or BAL cultures | To detect fungal growth in the lungs |
| Regular symptom checks | To track signs like cough, chest pain, fatigue, or coughing blood |
💡 How Can You Support Healing?
Although not all cavities heal completely, you can take steps to support your lung health:
| Action | Why It Matters |
|---|---|
| Treat infection early | Reduces the chance of further lung damage |
| Follow antifungal treatment if prescribed | Controls fungal colonisation and CPA |
| Keep inflammation down | Essential in ABPA or CPA to limit tissue injury |
| Minimise steroid use when safe | Steroids can delay healing and increase risk of fungal growth |
| Quit smoking & avoid pollutants | Gives your lungs the best chance to recover |
| Attend follow-ups | CT scans and blood tests help catch changes early |
⚠️ When to Get Urgent Help
Contact your medical team if you notice:
-
Sudden worsening of cough or shortness of breath
-
Blood in your sputum (even small amounts)
-
Fever or weight loss
-
Chest pain or fatigue that’s getting worse
These could be signs of complications like bleeding or progression of CPA.
🧠 Summary
Lung cavities caused by aspergillosis can sometimes heal — especially if they’re small, caused by a short-term infection, and not colonised by fungus. But many people with chronic forms like CPA will have cavities that remain and need careful management.
Staying informed, sticking to your treatment plan, and attending regular check-ups give you the best chance of protecting your lung health.
🫁 ABPA Treatment: Why Are Steroids First, Even if They Can Increase Fungal Growth?

If you've been diagnosed with Allergic Bronchopulmonary Aspergillosis (ABPA), you may have heard that treatment often starts with oral steroids like prednisolone. But ABPA is triggered by a reaction to the Aspergillus fungus — so why use a treatment that might actually let that fungus grow more?
It’s a great question. This guide explains why steroids are still often the first step, what other treatments are available, and when they might be used.
🌿 What Is ABPA?
ABPA is not an infection — it’s an allergic immune reaction in the lungs to the fungus Aspergillus fumigatus. This overreaction causes:
-
Lung inflammation
-
Mucus plugging
-
Breathlessness and wheezing
-
Possible long-term lung damage (e.g., bronchiectasis)
People with asthma or cystic fibrosis are more likely to develop ABPA.
💊 Why Are Steroids Usually the First Treatment?
🔥 The key problem in ABPA is inflammation, not the fungus itself.
Steroids like prednisolone are often used first because they:
-
Act quickly to calm the allergic immune reaction
-
Reduce inflammation and mucus
-
Help relieve symptoms fast (wheezing, tight chest, breathlessness)
-
Prevent long-term damage if started early
Even though steroids may allow some fungal growth, their fast action against inflammation is often more important — especially in flare-ups.
🍄 What About Antifungal Treatments?
Antifungals like itraconazole or posaconazole reduce the amount of Aspergillus in the lungs. This helps to:
-
Reduce allergic triggers
-
Prevent future flare-ups
-
Lower the need for steroids
However, antifungals:
-
Take weeks to work
-
Don’t control inflammation well on their own during a flare
-
Can have side effects and interact with other medications
➡️ That’s why they are often used after steroids, or alongside them — especially in people who flare up often or need steroids long term.
🧬 What About Biologics?
Biologic therapies like:
-
Omalizumab (anti-IgE)
-
Dupilumab (blocks IL-4 and IL-13)
-
Mepolizumab (anti-IL-5)
…are used to help regulate the immune system in patients who:
-
Can’t tolerate steroids
-
Have frequent relapses
-
Need ongoing treatment despite antifungals
Biologics can help:
-
Reduce steroid use
-
Lower flare frequency
-
Improve asthma control
But they’re not yet approved as first-line treatments and are generally reserved for more complex or persistent cases.
✅ What Happens If My Symptoms Are Mild?
Good question. In mild ABPA (e.g. stable breathing, low IgE, no major lung damage), specialists may:
-
Monitor closely before starting any treatment
-
Try antifungals alone, especially if steroid use is risky
However, regular follow-up is essential to make sure inflammation doesn’t silently worsen.
🔄 Typical ABPA Treatment Steps
| Stage | Treatment |
|---|---|
| First flare or moderate symptoms | Steroids (short course) ± antifungals |
| Steroid side effects or long-term use | Add antifungals |
| Recurrent or steroid-dependent ABPA | Add or switch to biologics |
| Mild symptoms and stable lungs | Possibly antifungals first (specialist decision) |
🧘 Staying Well with ABPA
-
Follow your treatment plan closely
-
Keep lungs clear with mucus clearance techniques
-
Avoid damp, mouldy environments
-
Keep up with regular check-ups and lung tests
-
Let your team know if symptoms return
🗨️ In Summary
Steroids are still first-line because they work fast to stop inflammation.
Antifungals and biologics are important longer-term options that help reduce fungal triggers and flare-ups — and may reduce or even replace steroids over time.
Every ABPA patient is different, and your care should be tailored to you.
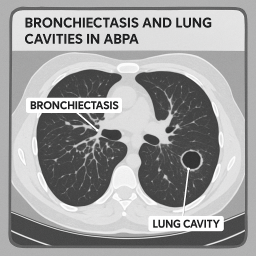
🫁 Understanding ABPA, Bronchiectasis & Lung Cavities
A Patient’s Guide to What Happens in the Lungs – and What You Can Do About It
🌿 What is ABPA?
Allergic Bronchopulmonary Aspergillosis (ABPA) is a condition where the lungs react strongly to a common fungus called Aspergillus. This overreaction causes inflammation in the airways, making it harder to clear mucus and increasing the risk of flare-ups.
Many people with asthma or cystic fibrosis are more likely to develop ABPA, but it can affect others too.
🌀 What Happens to the Lungs?
Over time, repeated inflammation and mucus build-up can affect the structure of the airways. Here’s what can happen:
1. Bronchiectasis
-
The airways (bronchi) become widened and thickened.
-
This makes it harder to clear mucus, which can lead to more infections.
-
In ABPA, this usually affects the central parts of the lungs.
🔸 Bronchiectasis is not the same as a lung cavity. It’s a change in the shape of the airways, not a hole in the lung.
2. Lung Cavities (Less Common)
-
These are air-filled spaces that form when a small area of lung tissue is damaged or infected.
-
Cavities are less common in ABPA but can happen after repeated inflammation or infection.
-
They may look worrying on a scan, but often they are just monitored and don’t cause major issues unless they become infected.
🩺 What About Lung Function?
ABPA and bronchiectasis can affect lung function, especially if not caught early.
-
Spirometry tests may show lower results if the airways are blocked or inflamed.
-
Some people improve after treatment; others may see a gradual decline.
-
Most patients still breathe well at rest, and many stay active with proper care.
🌬️ Will Cavities Leak Air?
This is a common worry. The answer is: usually not.
-
Most cavities in ABPA are not at risk of bursting or leaking.
-
Sudden breathlessness or chest pain should always be checked, but leaks (pneumothorax) are rare in ABPA.
📉 Does Everyone Get Cavities?
Not at all.
-
Around 50–90% of ABPA patients get some bronchiectasis.
-
Only a minority go on to develop true cavities.
-
Early treatment and regular check-ups help reduce the risk of further lung changes.
🧪 What About Oxygen Levels?
Many people with ABPA — even with bronchiectasis — still have normal oxygen levels (SpO₂):
-
Most rest between 95–98%
-
During a flare or infection, it might dip a little
-
If oxygen drops below 92%, your team may check more closely
🧘 What Can I Do to Stay Well?
-
🩺 Stick to your treatment plan – antifungals, inhalers, or steroids if prescribed
-
💨 Clear mucus regularly – ask about airway clearance techniques
-
🧼 Avoid damp, mouldy environments
-
🍎 Stay active and eat well
-
📆 Attend check-ups and lung function tests
-
🚭 Avoid smoking or vaping (these can worsen damage)
💬 A Final Word
Having ABPA and some lung changes doesn’t mean life has to stop. Many people continue to live active, fulfilling lives. Even with bronchiectasis or small cavities, the focus is on prevention, staying stable, and getting support when needed.
Managing ABPA: How to Protect Your Lungs and Stay Well
If you’ve been diagnosed with ABPA (Allergic Bronchopulmonary Aspergillosis), you’re probably already working to control inflammation and clear mucus from your lungs. These are essential steps—but there’s more you can do to protect your lung function and prevent long-term damage.
This guide will help you understand what matters most in managing ABPA and feeling your best.
✅ The Basics: What You're Probably Already Doing
1. Keep Inflammation Low
-
This means reducing your IgE levels and calming the immune system.
-
Your doctor may prescribe:
-
Steroids (like prednisolone)
-
Antifungal medication (like itraconazole or voriconazole)
-
In some cases, biologic treatments like omalizumab or mepolizumab
-
2. Clear Mucus Regularly
-
Mucus can trap infection and block your airways.
-
You might be using:
-
Airway clearance techniques (like chest physiotherapy or postural drainage)
-
Nebulised medications (saline or bronchodilators)
-
Mucus-thinning medicines (like carbocisteine or NAC)
-
These two steps are essential, but they’re not the whole picture.
💡 What Else Can Help You Stay Well?
3. Prevent Chest Infections
ABPA can lead to bronchiectasis, a condition where your airways get scarred and damaged. To help prevent this:
-
Treat infections early
-
Get regular chest scans to monitor changes
-
Stay up to date with vaccines (flu, pneumonia, COVID, etc.)
-
Your doctor may consider low-dose antibiotics if infections are frequent
4. Avoid Fungal Exposure
Aspergillus is a fungus found in the environment, especially in:
-
Compost, soil, or damp leaves (gardening can be risky)
-
Mouldy or damp areas in homes
-
Older buildings with water damage
Use air filters, wear a mask when needed, and keep your living space clean and dry.
5. Look After Your Overall Lung Health
-
Pulmonary rehabilitation (specialist-guided breathing and exercise therapy) can improve your stamina and lung function.
-
Practice breathing exercises daily.
-
Stay physically active in ways that are manageable for you.
6. Take Care of Your Body
Steroids can cause side effects over time, like bone thinning and fragile skin.
-
Make sure you're getting enough calcium and vitamin D
-
Ask your doctor about a bone density (DEXA) scan
-
Eat a balanced, anti-inflammatory diet and stay hydrated
7. Look After Your Mental Health
Living with ABPA can be exhausting. Fatigue, breathlessness, and medical side effects can affect your mood and confidence.
-
Track how you’re feeling—physically and emotionally
-
Talk to your care team about fatigue or mental health support if needed
-
You’re not alone—support groups and patient communities can really help
🗣️ Talk to Your Doctor About:
-
Biologic treatments (like omalizumab or mepolizumab) — these may help reduce steroid use
-
Sputum testing to catch early infections
-
Specialist referral to a severe asthma or lung clinic if needed
🧭 Summary: What to Focus On
| What to Manage | Why It Matters |
|---|---|
| Inflammation (IgE levels) | Reduces flare-ups and long-term damage |
| Mucus clearance | Keeps airways open and lowers infection risk |
| Chest infections | Slows or prevents bronchiectasis |
| Environmental exposure | Reduces fungal triggers |
| Exercise & breathing | Supports stronger lungs and energy levels |
| Bone and general health | Counters effects of long-term steroid use |
| Mental wellbeing | Helps you stay strong and supported |
Final Tip
Managing ABPA is a long-term journey, but you're not alone. With the right care, medications, and lifestyle changes, many people with ABPA are able to stabilise their condition and keep their lungs as healthy as possible.