Chronic Lung Disease and Relationships: The Emotional Impact for Patients, Partners, Friends & Family
Living with chronic lung disease — such as ABPA, CPA, bronchiectasis, or severe asthma — affects far more than the body.
It alters the emotional landscape between the person with the illness and the people around them.
This isn’t just about physical limitations — it’s about how empathy, energy, guilt, and emotional resilience are shared (or strained) over time.
This guide explores both perspectives — the patient and the healthy person — and offers ways to keep relationships strong.
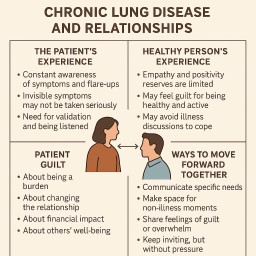
1. The Patient’s Perspective
For the person with the illness, the condition is ever-present:
-
Constant awareness – Every breath, plan, or activity is influenced by symptoms, medication schedules, and the risk of flare-ups.
-
Invisible symptoms – You can feel like you’re drowning without looking or sounding breathless. The absence of obvious signs often means people underestimate how unwell you are.
-
Need for validation – Being listened to, believed, and taken seriously is essential. Dismissive comments such as “you don’t sound wheezy” can feel like a denial of your lived reality.
-
Loss of role – Illness can mean stepping back from work, family responsibilities, or social life, leaving you feeling less “you” and more “the patient.”
2. The Healthy Person’s Perspective
Even the most loving partner, friend, or family member has finite emotional reserves:
-
Empathy fatigue – Offering compassion in a crisis is natural; sustaining it daily for years is emotionally exhausting.
-
Positivity limits – Staying upbeat to encourage the patient can drain energy, sometimes leading to withdrawal.
-
Healthy guilt – Feeling bad for having health, energy, freedom, or the ability to enjoy life.
-
Emotional self-protection – Avoiding deep illness discussions to manage their own fear, helplessness, or sadness.
-
Mismatch of experience – The healthy person dips in and out of illness awareness, while the patient lives in it constantly.
3. Patient Guilt
While healthy guilt is common, patient guilt is just as powerful:
-
Feeling like a burden – Worrying that you limit others’ activities, social life, or freedom.
-
Changing the relationship – Feeling bad that a partner now has to act partly as a carer.
-
Financial strain – Guilt over reduced income or increased expenses.
-
Impact on others’ wellbeing – Feeling responsible for your partner’s, friends’, or family’s stress or fatigue.
-
Mood and personality changes – Guilt about being irritable, anxious, or withdrawn because of the illness or medication effects.
4. Common Relationship Challenges
For partners:
-
Role shift – Moving from equal partnership to a dynamic where one is part-carer.
-
Social imbalance – One may want to go out more than the other can manage.
-
Resentment risk – If needs are unspoken, one may feel abandoned and the other may feel trapped.
For family:
-
Unequal support – Some relatives engage, others withdraw.
-
Generational differences – Older relatives may minimise invisible illness (“just push through”).
-
Positive minimising – Trying to “cheer you up” by downplaying symptoms, which can feel invalidating.
For friends:
-
Friendship drift – Reduced shared activities can lead to less contact.
-
Fear of offending – Friends stop inviting you to events so you won’t have to say no.
-
Discomfort with illness – Some disappear entirely rather than risk awkwardness.
5. The Psychology Behind These Changes
-
Finite empathy and energy – The brain isn’t wired for sustained crisis-mode support.
-
Visible vs. invisible illness gap – We respond more readily to what we can see (limping, coughing) than what we can’t (chest tightness, fatigue).
-
Avoidance coping – Healthy people sometimes step back emotionally to manage their own distress.
-
Healthy guilt – Creates distance when the healthy person hides their joy to avoid hurting you.
-
Patient guilt – Creates distance when you hold back your needs to avoid burdening them.
6. Strategies for Moving Forward Together
For Patients:
-
Be specific – Say what you need: “I need you to just listen” or “Could you help with…?”
-
Make space for non-illness moments – Talk about hobbies, TV shows, shared memories.
-
Recognise recharge needs – Allow healthy people breaks from illness talk without taking it as a lack of care.
-
Value their life too – Encourage them to enjoy activities even if you can’t join.
For Partners, Friends, and Family:
-
Believe them – Accept what the patient says about symptoms, even if they “look fine.”
-
Share your feelings – Guilt, overwhelm, or fear are normal; discussing them prevents silent withdrawal.
-
Keep inviting – Offer options, but no pressure — inclusion matters more than attendance.
-
Balance care with normality – Don’t let every interaction be about the illness.
7. Talking About Guilt (Both Sides)
-
Name it openly – “I feel guilty for being well” or “I feel guilty for needing so much help.”
-
Acknowledge the illness isn’t anyone’s choice – Blame the condition, not each other.
-
Agree on boundaries – Both lives matter, both deserve joy.
-
Share in two directions – Illness updates and everyday life keep relationships in balance.
8. Final Thought
Chronic illness can strain relationships, but it can also deepen them — if both sides:
-
Understand that empathy, positivity, and energy are finite.
-
Recognise both healthy guilt and patient guilt.
-
Protect space for joy, humour, and connection beyond the illness.
Love doesn’t mean living in the illness 24/7 — it means walking alongside each other, even when the paths look different.
Information on Allergic BronchoPulmonary Aspergillosis (ABPA) / SAFS – For Family and Friends
Print out or share electronically
WHAT IT IS
ABPA (Allergic Bronchopulmonary Aspergillosis) and SAFS (Severe Asthma with Fungal Sensitisation) are allergic reactions to a common fungus, Aspergillus. In some people with asthma, the immune system overreacts to spores in the air, causing inflammation, swelling, and mucus plugs in the lungs.
WHAT IT'S NOT
-
Not contagious – you can't catch it.
-
Not poor hygiene – Aspergillus is everywhere in the air.
-
Not the patient's fault – flare-ups happen because of the condition, not something they did or didn't do.
WHY AREN'T OTHERS AFFECTED?
Most people's lungs clear these spores easily. In ABPA/SAFS the immune system reacts too strongly – more likely with long-standing asthma, severe allergies, damaged airways (e.g., bronchiectasis), or a genetic tendency. It's not weakness or lifestyle choices – often just lung history and bad luck.
TYPICAL SYMPTOMS
-
Wheezing, cough (sometimes with mucus plugs)
-
Breathlessness
-
Severe fatigue
-
Sometimes coughing up blood
WORST SYMPTOMS
-
Mucus plugs – thick, sticky clumps blocking airways, making breathing suddenly harder.
-
Intense coughing – can be exhausting, cause chest pain, and disrupt sleep.
TREATMENT
-
Anti-inflammatory medicines (often steroids)
-
Antifungals to reduce Aspergillus in the airways
-
Biologics for severe asthma/allergic inflammation
-
Monitoring with blood tests, breathing tests, and scans
THE REALITY
This condition can dominate daily life. On bad days the person may not be able to do much at all. Energy and breathing can change day-to-day (even hour-to-hour). If plans are cancelled, it isn't a lack of interest – it's the illness. Flare-ups can also make people feel short-tempered – a natural reaction to frustration, not a lack of care. Many people also live with a constant awareness of environmental risks – weighing up every new place or activity for dust, damp, or spores. This can feel exhausting and may lead them to avoid situations that others wouldn’t think twice about.
LOOKING AHEAD
-
With good control – Many people manage their symptoms well, reduce flare-ups, and keep active with the right treatment and avoidance of triggers.
-
Risks – Without good control, repeated flare-ups can slowly damage the lungs and lead to bronchiectasis.
-
Change over time – Some improve and need less treatment; others have ongoing ups and downs. Early action on flare-ups makes a big difference.
ENVIRONMENTAL TRIGGERS & PROTECTION
Some people with ABPA or SAFS have to avoid dust, mould, strong smells, smoke, and damp places – these can trigger flare-ups. Activities like gardening, compost turning, or DIY can be risky because they release fungal spores into the air. Wearing a well-fitting mask (e.g., FFP2/FFP3) can help reduce exposure – it's about staying well, not being antisocial.
HOW FRIENDS AND FAMILY CAN BEST HELP
-
Be flexible with plans – energy and breathing can change suddenly; last-minute cancellations aren't personal.
-
Help avoid triggers – choose low-dust, low-mould venues and activities.
-
Support treatment routines – lifts to appointments, collecting prescriptions, or reminders if welcome.
-
Listen without judgement – let them share symptoms and frustrations.
-
Encourage safe activities – suggest hobbies and outings with low environmental risk.
-
Show affection and reassurance – a hug, a kind message, or checking in can mean a lot.
MORE INFORMATION & SUPPORT
National Aspergillosis Centre (UK): https://mft.nhs.uk/wythenshawe/services/infectious-diseases/national-aspergillosis-centre/
Patient information & community: https://aspergillosis.org
Chronic Pulmonary Aspergillosis (CPA) – Information For Family and Friends
Print this off or share electronically
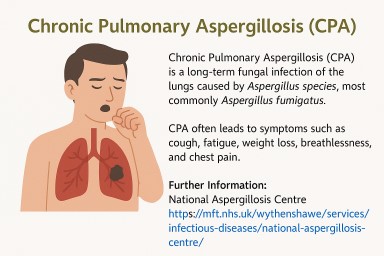
WHAT IT IS
CPA (Chronic Pulmonary Aspergillosis) is a long-term lung infection caused by the Aspergillus fungus. It often develops where lungs are already damaged (e.g., TB, COPD, bronchiectasis, sarcoidosis) and may form cavities, sometimes with fungal balls (aspergillomas).
WHAT IT'S NOT
-
Not contagious – you can't catch CPA.
-
Not poor hygiene – spores are everywhere in the air.
-
Not the patient's fault – flare-ups or setbacks happen because of the illness, not something they did wrong.
WHY AREN'T OTHERS AFFECTED?
Most people remove spores without trouble. CPA appears when lungs are already damaged or the immune system can't fight the fungus well – after past infections, chronic lung disease, or weakened defences. It's not about choices; it's lung history and chance.
TYPICAL SYMPTOMS
-
Persistent cough (sometimes with blood)
-
Breathlessness
-
Fatigue and low energy
-
Weight loss
-
Recurring chest infections
WORST SYMPTOMS
-
Coughing up blood – can be small streaks or larger amounts; sudden and frightening; urgent if heavy.
-
Severe fatigue – can stop even simple tasks; not just ‘tiredness’.
TREATMENT
-
Long-term antifungal medication
-
Regular scans and blood tests
-
Surgery in selected cases
THE REALITY
CPA is a serious, long-term condition. On bad days, people may not be able to do much at all. Symptoms can dominate daily life and limit social plans – cancelled arrangements are the illness talking, not them. It can also make people feel grumpy or irritable – not because they don't care, but because constant symptoms, tiredness, and limits on daily life are frustrating and exhausting. There’s often a mental load too – always thinking about avoiding dust, damp, or mould spores, and sometimes feeling overcautious about activities like going on boats, visiting old buildings, or anywhere that might harbour moisture or mould. This risk-checking is a form of self-protection, even if it means missing out.
It’s important to mention the mood swings and fatigue caused not only by the disease but also by the medication. For some, constant hand tremors are also part of daily life — these are often misunderstood by others.
LOOKING AHEAD
-
With effective treatment – Many people can keep the infection stable for years, control symptoms, and stay independent.
-
Risks – CPA can slowly progress, and severe flare-ups (like coughing large amounts of blood) may need urgent treatment.
-
Change over time – The illness can be stable for long periods, but it often needs lifelong monitoring and treatment changes. Support from specialists helps keep people well for longer.
ENVIRONMENTAL TRIGGERS & PROTECTION
Some people with CPA need to avoid environments with high levels of dust or fungal spores. This includes gardening, composting, building work, or damp/mouldy places. Wearing a protective mask during these activities can help reduce risk. Avoiding these triggers is about preserving lung health – not being fussy or antisocial.
HOW FRIENDS AND FAMILY CAN BEST HELP
-
Respect limits – breathlessness, fatigue, or coughing up blood can stop plans at short notice; it's not a choice.
-
Minimise exposure risks – avoid inviting them to dusty, damp, or mouldy places.
-
Offer practical help – driving to appointments, carrying shopping, or helping at home during flare-ups.
-
Be patient with mood changes – grumpiness can come from exhaustion and constant vigilance against triggers.
-
Talk openly about safety – if you suggest an outing, ask “Would this feel safe for you?”
-
Stay connected – even if they can't join in physically, a call or small gesture keeps them included.
MORE INFORMATION & SUPPORT
National Aspergillosis Centre (UK): https://mft.nhs.uk/wythenshawe/services/infectious-diseases/national-aspergillosis-centre/
Patient information & community: https://aspergillosis.org
Damp, Cold, and Poor Housing – Why It Matters for Lung Health
This briefing from the House of Commons Library (2025) looks at how poor housing conditions—especially damp, mould, and cold homes—affect health and what’s being done about it in the UK.
Main Points
-
Health risks are serious
Living in damp or mouldy homes increases the risk of respiratory problems, particularly for people with existing lung disease like aspergillosis, asthma, COPD, or bronchiectasis. -
Children and vulnerable adults
Young children, older adults, and people with weakened immune systems are most affected. Damp and mould can trigger flare-ups, worsen breathing symptoms, and increase infection risk. -
Mental health impact
Poor housing is linked to stress, anxiety, and depression. Worrying about your home can also worsen physical symptoms, especially if you avoid using rooms with mould or limit heating to save costs. -
Cold homes add to the problem
Cold airways can make breathing more difficult, weaken the immune system, and increase the chance of winter infections. -
Wider health effects
Damp and cold can also affect heart health, bone/joint pain, and overall wellbeing.
What’s Being Done
-
Legal responsibilities: Landlords must keep homes safe and fit to live in under UK law. This includes dealing with serious damp and mould.
-
Government programmes:
-
Funding for improving insulation and heating in social housing.
-
Advice services for tenants.
-
Local councils can take action if landlords fail to address hazards.
-
-
Public health guidance now recognises the link between housing and chronic illness, with stronger advice for early intervention.
What This Means for Aspergillosis Patients
-
Stay alert to symptoms: If your cough, breathlessness, or fatigue worsen at home, check for damp, mould, or poor heating.
-
Act early: Report problems to your landlord or council quickly—prolonged exposure can worsen lung damage.
-
Medical link is recognised: You are more likely to be taken seriously now, as official guidance acknowledges the health risks.
-
Keep records: Photos, symptom diaries, and GP notes can support housing complaints.
For full details see https://commonslibrary.parliament.uk/research-briefings/cdp-2025-0096/
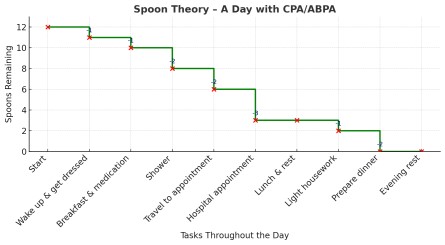
Spoon Theory: Making Sense of Energy Limits in Aspergillosis
The Spoon Theory is a way of explaining what it’s like to live with a long-term illness that affects your energy and stamina. It was first described by Christine Miserandino, who used spoons as a visual metaphor for the limited amount of energy she had each day.
How it works
-
Imagine you start each day with a set number of spoons — maybe 10 or 12.
-
Every task you do “costs” spoons:
-
Getting dressed might cost 1 spoon
-
Cooking a meal might cost 2 spoons
-
A shower could cost 2 spoons on a bad day
-
Going for a walk or attending an appointment might cost 3 or 4 spoons
-
-
When you run out of spoons, that’s it — you don’t have the energy to keep going. If you push yourself, you “borrow” from tomorrow’s spoons, which can leave you feeling worse for days.
 Why CPA and ABPA drain your spoons
Why CPA and ABPA drain your spoons
Both conditions can cause:
-
Breathlessness – even small tasks can feel like hard work.
-
Coughing and mucus production – which can be exhausting physically.
-
Flare-ups – like haemoptysis (coughing blood) in CPA or allergic inflammation in ABPA.
-
Medication side effects – antifungals, steroids, or biologics can also sap your energy.
-
Frequent appointments – travel and hospital visits can eat into your spoon supply.
Why Spoon Theory matters
Understanding Spoon Theory helps you:
-
Plan your day – save enough spoons for the important things.
-
Pace yourself – spread out demanding tasks, rest between them.
-
Explain your limits – it’s an easy way to help friends, family, and employers understand that you’re not being lazy — you’re managing your limited energy.
-
Avoid “boom and bust” – pushing too hard on a good day can leave you with no spoons for the next few days.
Practical tips
-
Prioritise – decide what’s essential today and what can wait.
-
Ask for help – let others “spend” their spoons for you when possible.
-
Rest without guilt – recharging is part of living with a long-term condition.
-
Track your spoons – keeping a symptom diary can help you notice patterns.
Remember: Your number of spoons can change day-to-day, especially if you’ve had a flare-up, infection, or a hospital stay. Learning to work with your spoons instead of against them can help you stay in control and reduce stress.
Being Heard in Healthcare: Confidence, Communication, Gender Bias, and Your Rights
Living with aspergillosis or severe asthma often means frequent contact with healthcare professionals — GPs, hospital specialists, nurses, physiotherapists, pharmacists, and more. Most of these encounters are positive, but sometimes patients leave feeling they weren’t truly listened to. This can be frustrating, especially when symptoms are complex, variable, or invisible to others.
Why Some Patients Feel Unheard
Some patients report that their background, gender, education, or knowledge of their condition seems to affect how clinicians speak to them. If a clinician thinks you are “well informed,” they may change their approach — sometimes giving you more detail, but occasionally becoming defensive or dismissive.
This shouldn’t happen. Every patient deserves the same respect, attention, and clear explanations, regardless of their background or experience.
Occasionally, what feels like “healthcare ego” may actually come from other sources:
-
Time pressure in busy clinics
-
Stress or fatigue
-
Overconfidence in diagnostic skills
-
Unconscious bias about gender, age, or condition severity
The Role of Gender Bias
Research in the UK and internationally shows that gender can sometimes influence how symptoms are interpreted and how seriously they are taken. Women are, on average, more likely to have their symptoms attributed to stress or anxiety, while men may be assumed to under-report pain or discomfort.
In conditions like asthma and aspergillosis — where breathlessness, fatigue, and chest symptoms may not always show clearly on tests — this bias can delay diagnosis, affect treatment urgency, and shape how much explanation is given. Recognising that this bias exists can help you prepare to advocate for yourself more effectively, regardless of gender.
The Women’s Health Strategy for England — A Step Forward
The Women’s Health Strategy for England (gov.uk link) is a landmark initiative aiming to transform how healthcare listens to and serves women. It highlights priorities that matter for anyone with a long-term, complex condition:
-
Women’s Voices Must Be Heard – 84% of women surveyed said they often felt ignored or dismissed by healthcare professionals.
-
More Inclusive Policies and Training – Increased focus on women’s health education for healthcare staff and embedding shared decision-making into routine care.
-
Closing the Research Gap – Improving female representation in clinical research and analysing data by sex and life stage.
-
System-Level Change – Appointing a Women’s Health Ambassador, setting up women’s health hubs, and introducing women’s health leads for accountability.
For the aspergillosis community, this means a greater push for inclusive research, equal access to treatment, and recognition of symptoms that might otherwise be overlooked.
What to Do if You Feel You Weren’t Heard
If you leave an appointment feeling your concerns weren’t addressed:
-
Restate your main concern politely but firmly, explaining why it matters.
-
Ask the clinician to repeat back what they understood, so you can correct any misunderstandings.
-
Request that your concerns be recorded in your medical notes.
-
Follow up in writing via a patient portal, email, or letter.
-
Bring a trusted supporter (trusted friend, family member, or advocate) to future appointments to help make your case.
Building Confidence in Healthcare Conversations
Confidence in speaking up grows with preparation:
-
Prepare your top two or three key points before the appointment.
-
Practise saying them aloud so they feel natural.
-
Use clear phrases like “I am concerned about…” or “I need to understand…”
-
Remember — you have a right to clear information about your diagnosis, treatment, and risks.
-
If you can’t speak up in the moment, follow up in writing afterwards.
Why This Works — The Evidence
Research shows prepared, assertive patients get clearer, more thorough answers:
-
The “Ask Me 3” approach improves understanding and engagement.
-
Shared decision-making studies show prepared patients are more likely to have concerns addressed and remember what was discussed.
-
BMJ and Patient Education & Counseling studies find that specific, assertive language leads to better explanations and consideration of alternatives.
-
Having an advocate present improves follow-up and adherence to care plans.
Final Thought
In aspergillosis care, where symptoms can be complex and treatments long-term, good communication is as important as good medicine. Speaking up respectfully but confidently helps you get the care you need and supports a culture where every patient — regardless of gender or background — is listened to from the first moment. The Women’s Health Strategy shows there is now national recognition of these issues, and your voice is a vital part of making change happen.
📘 What is CPA? (Chronic Pulmonary Aspergillosis)
Patient handout for A&E staff who are not aware of aspergillosis.
What is CPA?
CPA is a chronic fungal infection of the lungs caused by Aspergillus, most often in people who already have damaged lungs from conditions like tuberculosis, COPD, lung cancer, or sarcoidosis.
Unlike ABPA, CPA is a true infection, not an allergic reaction. It is not contagious but can slowly destroy lung tissue if not treated.
Symptoms
-
Chronic cough, often with mucus
-
Coughing up blood (haemoptysis)
-
Fatigue, low-grade fever
-
Unexplained weight loss
-
Breathlessness
-
Recurrent chest infections not responding to antibiotics
Diagnosis
-
CT scan of the chest showing cavities, nodules, or fungus balls (aspergillomas)
-
Aspergillus IgG antibody (usually raised)
-
Positive sputum PCR or culture for Aspergillus
-
Exclude TB and malignancy
Treatment
-
Long-term antifungal therapy (e.g. itraconazole, voriconazole, posaconazole)
-
Monitor blood levels and liver function
-
Surgery or embolisation if severe bleeding occurs
-
Supportive care: oxygen, nutrition, physiotherapy
Key Points for A&E:
✅ CPA is a progressive fungal infection, not a typical bacterial pneumonia
✅ May present with haemoptysis, respiratory distress, or systemic illness
✅ Review current antifungal treatment and potential drug interactions
✅ Consider urgent chest CT and specialist referral if patient is unwell
📍 For specialist support:
National Aspergillosis Centre (NAC)
🏥 Wythenshawe Hospital, Manchester University NHS Foundation Trust
🌐 NAC homepage on MFT website https://mft.nhs.uk/wythenshawe/services/infectious-diseases/national-aspergillosis-centre/
🌐 www.aspergillosis.org
📞 Daytime contact: 0161 291 2891 or 0161 291 4362
📞 Urgent out-of-hours: Call Wythenshawe switchboard on 0161 998 7070
📢 Ask for the on-call Infectious Diseases Consultant
Debate: Gender Bias in Science and Clinical Trials & Why It Matters to Patients
Introduction: A History of Exclusion For decades, medical research and clinical trials were built around a default male body. Women were routinely excluded from studies out of concern for hormonal variation, pregnancy risks, or assumptions that female responses would mirror male ones. The consequences? Misdiagnoses, incorrect dosing, side effects overlooked in women, and entire conditions dismissed as psychological.
This pattern of systemic gender bias has had real-life consequences for millions of women, especially those living with chronic or misunderstood illnesses like ME/CFS (Myalgic Encephalomyelitis/Chronic Fatigue Syndrome), long COVID, autoimmune diseases — and potentially, aspergillosis.
Section 1: Real Consequences of Exclusion
Why Gender Bias Matters in Asthma and Aspergillosis
Both asthma and aspergillosis are diseases where gender can influence immune response, disease progression, and side effects of treatment. Women are more likely to develop certain asthma subtypes (e.g., late-onset eosinophilic asthma), which overlap with allergic fungal conditions like ABPA. They may also experience more frequent exacerbations and are more vulnerable to long-term steroid side effects such as adrenal insufficiency and bone loss. Despite this, sex-specific analysis is rare in fungal disease trials, and asthma research has only recently begun to explore these differences.
Is Gender Relevant in Aspergillosis? While aspergillosis affects people of all sexes, some patterns suggest potential sex differences in prevalence, diagnosis, immune response, and treatment side effects:
- Chronic Pulmonary Aspergillosis (CPA) appears more common in men, especially in post-TB or COPD populations, but women may experience more severe fatigue or be underdiagnosed.
- In ABPA (Allergic Bronchopulmonary Aspergillosis), hormonal differences may influence disease severity, and women often report more exacerbations or sensitivity to long-term steroid treatment.
- Invasive aspergillosis is less well studied for sex differences, though some research in animal models suggests hormonal influences on fungal immunity.
- Women may also be more vulnerable to side effects of antifungals and corticosteroids, such as adrenal suppression, hearing loss, or osteoporosis.
Despite these observations, most clinical studies do not stratify by sex or explore gender-specific differences, leaving important questions unanswered.
A Message to Women Living with Aspergillosis
If you're reading this as a woman affected by aspergillosis, please don’t feel discouraged. While we highlight gaps in past research, the goal is to push for better inclusion, not to suggest you're being overlooked in care. You are not alone. Clinicians are becoming more aware of these issues, and researchers — especially in the UK — are actively working to close the gender gap. Patient groups and specialist centres like the NAC are also strong advocates for fair, personalised treatment. Your voice matters, and being informed is a powerful step in making future care better for everyone.
Clinical trials that exclude or underrepresent women have led to:
- Drugs that stay longer in women's bodies (e.g., Zolpidem) causing next-day drowsiness and driving risk
- Heart medications being under-prescribed to women, because early trials only studied men
- Misunderstanding of how autoimmune diseases develop and respond to treatment
- Failure to understand symptoms unique to women, such as how heart attacks present differently
Historically, women were also more likely to have their physical symptoms dismissed as anxiety or "hysteria." ME/CFS, a condition affecting mostly women, was dismissed for decades as psychological. When patients with ME later caught COVID-19, many were again left behind as new post-viral syndromes took priority.
For patients with aspergillosis, particularly chronic forms like CPA or ABPA, the relevance is clear. These conditions are under-researched and under-recognised, and early studies may not fully reflect how they impact women. Steroid-related side effects like osteoporosis, adrenal suppression, and hearing loss may differ by sex — yet sex-stratified data is rarely available.
Section 2: Has Anything Changed?
Yes. In the UK, the National Institute for Health and Care Research (NIHR) and the Medical Research Council (MRC) have taken steps to improve inclusion:
- NIHR-funded studies are expected to include representative populations and report on diversity
- UK Research and Innovation (UKRI) promotes equality in trial design, including sex and gender analysis
- The DecodeME study (the world’s largest ME/CFS genetics study, based in the UK) is actively engaging with female participants
But gaps remain — especially in rare diseases, chronic illnesses, and reproductive health. For fungal disease and aspergillosis specifically, many trials still do not analyse sex-specific outcomes, despite women forming a significant proportion of the affected population.
Section 3: Are Women Now Being Protected Too Much? Some worry that extra precautions — like excluding women from early-phase trials — may backfire:
- Delaying access to life-changing drugs
- Forcing women to wait until post-marketing surveillance to be included
- Excluding pregnant and breastfeeding women entirely, even when they are at high risk (e.g., in pandemics)
This creates a paradox: either women are harmed by being ignored, or excluded "for their safety."
The solution is not to avoid studying women — but to design smarter, safer, inclusive trials from the beginning.
Section 4: Will We Need Two Trials — One for Men, One for Women? This concern is understandable. Stratifying data by sex, running subgroup analyses, and including both pre- and post-menopausal women does cost more.
But it's not about running two separate trials. It's about:
- Recruiting balanced numbers of men and women
- Analysing sex-specific outcomes from one trial
- Designing adaptive trials or pooled data studies
Neglecting sex differences costs more in the long run — through failed drugs, recalls, and harm to patients.
Section 5: Positive Examples of Progress
- UK heart disease research now includes female-specific risk factors and symptom profiles in NICE guidance
- Autoimmune research increasingly uses female animal models and stratifies analysis by sex
- Endometriosis, menopause, and menstrual health are finally getting targeted research funding in the UK
- DecodeME is helping uncover the genetic basis of ME/CFS with full inclusion of women
- Long COVID clinics in the NHS are building on lessons from women-led ME/CFS research
- New studies on asthma and fungal allergy (e.g., ABPA) are beginning to explore hormonal and immunological factors that may differ by sex
Section 6: Where Patients Fit In Patients have led many of these changes:
- Women with ME, long COVID, POTS, or fibromyalgia have insisted their experiences are real
- Advocacy groups in the UK (e.g. Action for M.E., LongCovidSOS, National Aspergillosis Centre support groups) have pushed for sex-specific research
- Patient-led data collection and patient involvement in trial design are now expected in NIHR-funded studies
- In rare fungal diseases like CPA, SAFS, and ABPA, patients can support research by contributing to trials that welcome women and report on sex-specific outcomes
Conclusion: A Call to Patients This isn’t just a scientific issue — it’s a patient rights issue. Without full inclusion of women in research, we can't expect safe, effective, and equitable treatments.
Ask questions. Share your stories. Advocate for better science. And when possible, participate in trials that commit to transparency and inclusivity.
For patients with aspergillosis, the message is clear: We need sex-aware, inclusive research to understand this complex disease in all its forms — and that means including and reporting on women properly.
Medicine must work for everyone — not just the default male.
💭 Why Some People with Aspergillosis Delay Going to A&E
And Why That Could Be Dangerous
If you live with chronic aspergillosis — whether CPA, ABPA, SAFS, or aspergillus bronchitis — you’ve probably had moments where your symptoms suddenly worsened and you didn’t know what to do. Maybe you’ve thought about going to A&E, or even dialling 999, but something stopped you.
You're not alone. Many people in our community feel reluctant to seek emergency care, even when they’re very unwell.
Here’s why — and why it matters.
🏥 “I’ve Been to A&E Before — and It Wasn’t a Good Experience”
Many patients have told us:
-
“I waited for hours just to be told it’s probably my usual symptoms.”
-
“The staff didn’t seem to know what aspergillosis is.”
-
“They didn’t know how to manage my antifungal treatment or asthma.”
-
“I felt dismissed — like I was being dramatic.”
Experiences like this can leave people feeling humiliated or unsafe, and understandably less likely to go back — even when things are serious.
🛏️ “I Don’t Want to Be Admitted — I’ll Be Stuck There”
A&E can be a gateway to hospital admission, and for someone managing a complex, fluctuating condition at home, this can feel like losing control. You may worry about:
-
Being put on the wrong ward
-
Catching infections
-
Not being given the right antifungal, steroid, or oxygen support
-
Losing time, independence, or confidence
So instead, you might choose to stay home — sometimes too long.
⌛ “I Don’t Want to Waste Anyone’s Time”
We hear this all the time:
“A&E is for people who are really ill — not for someone like me.”
“The NHS is already overwhelmed.”
“I’ll just give it a bit more time.”
But remember: you’re not wasting time by going to A&E if your health is deteriorating. Chronic illness doesn’t make your emergency less urgent — it just makes it harder to spot.
😔 “I’m Tired of Needing Help”
Living with chronic aspergillosis is exhausting. It’s easy to feel like:
-
“I should be able to manage this myself.”
-
“I don’t want to be a burden.”
-
“It’s probably just another bad flare.”
But when symptoms cross a line — from “bad day” to “dangerous” — it’s vital to act. Seeking urgent care isn’t failure. It’s strength.
🌫️ “I Didn’t Know It Was That Serious”
The truth is: even very experienced patients often aren’t sure when symptoms need emergency treatment. You might think:
-
“I’ve had breathlessness before — I’ll just rest.”
-
“The coughing is worse, but it’s happened before.”
-
“I’ll wait until the morning and see.”
But if you’re coughing blood, can’t speak a sentence, can’t stand up, or feel confused or faint, waiting is dangerous.
💬 “I Asked in a Group First”
Support groups are amazing — and a lifeline for many. But no group can diagnose an emergency. If you're:
-
Asking whether to go to A&E
-
Describing symptoms that sound like respiratory failure, sepsis, or adrenal crisis
-
Hoping someone tells you not to worry...
Then it’s already time to act, not wait for replies.
✅ Final Message
If you have severe symptoms, sudden changes, or feel frightened about your health:
Don’t wait. Don’t post. Don’t hope it passes.
Call 999 or go to A&E.
You are not a burden. You are not overreacting.
You are saving your own life.
When to go to A&E or call 999
🚨 When to Go to A&E or Call 999
A Guide for People with Chronic Aspergillosis, Asthma, and Other Long-Term Conditions
When you live with a long-term health condition like chronic aspergillosis (CPA), allergic bronchopulmonary aspergillosis (ABPA), severe asthma, or immunosuppression, it can be hard to know when a flare-up is “just part of the illness” — and when it’s something more serious that needs emergency medical care.
This guide is designed to help you — or someone you care for — recognise the signs that mean it’s time to stop waiting, stop asking for online advice, and get help immediately.
🧠 A Special Note for People with Aspergillosis
People living with chronic aspergillosis often get used to symptoms like breathlessness, coughing, fatigue, or chest tightness. That makes it easy to miss or downplay serious changes — especially if you're reluctant to make another trip to A&E.
But there are times when acting fast is critical.
If you have CPA, ABPA, SAFS, or aspergillus bronchitis, you should go to A&E or call 999 immediately if you experience:
-
🫁 Sudden or worsening breathlessness, especially if it’s different from your usual
-
💨 Breathing that doesn’t improve after using inhalers, nebulisers, or oxygen
-
💔 New chest pain or tightness — particularly if it spreads or worsens when breathing
-
🌡️ A high fever, shaking chills, or flu-like symptoms
-
🩸 Coughing up blood — especially if it's fresh or in large amounts
-
🧠 Feeling confused, drowsy, or faint
-
❗ Severe weakness, fatigue, or inability to stand or walk
-
💊 Severe reaction to medications (e.g. antifungals, steroids, or biologics) — rash, swelling, dizziness, jaundice
⚠️ Don’t Wait or Ask Online — Act Fast When These Signs Appear
We completely understand why some people — particularly those with severe asthma, CPA, or ABPA — may be hesitant to go to A&E. You may have faced:
-
Long waits
-
Feeling dismissed or misunderstood
-
Fear of hospital admission
-
Exhaustion from too many medical appointments
These are real concerns, but when you're struggling to breathe, disoriented, or deteriorating rapidly, it’s not the time to post in a support group or wait for reassurance. It’s time to act.
In life-threatening moments, what you need isn’t advice — it’s treatment.
No support group — no matter how compassionate — can replace oxygen, IV antibiotics, a steroid boost, or emergency care.
Please don’t delay. You are never wasting anyone’s time by seeking help when something feels wrong.
🔥 Emergency Symptoms That Always Need 999 or A&E
Whether you have a long-term condition or not, there are symptoms that require immediate action:
🫁 Breathing Problems
-
Severe breathlessness, even at rest
-
Struggling to speak or complete sentences
-
Gasping, wheezing, choking
-
Blue or grey lips, face, or fingertips
-
No response to inhalers or nebulisers
-
Sudden onset shortness of breath
❤️ Chest Pain or Heart Symptoms
-
Crushing or heavy chest pain
-
Pain radiating to jaw, neck, arms, or back
-
Palpitations + fainting, dizziness, or breathlessness
-
Fast or irregular heartbeat
-
Suspected heart attack or angina
🧠 Neurological Emergencies
-
Sudden weakness or numbness (especially on one side)
-
Slurred speech, facial droop, or confusion
-
Seizures or fits (especially if new or lasting >5 minutes)
-
Sudden, severe headache
-
Loss of consciousness or collapse
🌡️ Infection / Sepsis Signs
-
High fever with chills or rigors
-
Very fast breathing or heartbeat
-
Cold, mottled, clammy skin
-
Feeling very drowsy, confused, or unable to stay awake
-
Not passing urine or drinking
-
Feeling like something is seriously wrong
🩸 Bleeding or Trauma
-
Heavy bleeding that doesn’t stop
-
Major burns or deep wounds
-
Suspected broken bones
-
Head, neck, or spinal injury
-
Bleeding from eyes, genitals, or rectum
💊 Medication-Related Emergencies
-
Anaphylaxis: swelling, rash, shortness of breath, collapse
-
Adrenal crisis (especially in those on long-term steroids): vomiting, confusion, weakness, fainting
-
Severe side effects to antifungals or biologics: dizziness, liver pain, rash, yellowing skin
-
Sudden change in behaviour or mental state after a new medication
🧭 Not Sure? Here's What to Do
-
If you’re in doubt, but worried: Call NHS 111
-
If symptoms are severe, worsening, or causing distress: Call 999 or go to A&E
-
If you’re alone, unwell, and unsure — you are safer being checked
📘 Summary: When to Get Help Immediately
| Symptom Area | Emergency Signs |
|---|---|
| Aspergillosis-specific | Sudden breathlessness, new chest pain, coughing blood, fever, severe weakness, confusion |
| Breathing | Gasping, cyanosis, wheezing unrelieved by inhalers |
| Heart | Chest pain, palpitations with collapse, irregular pulse |
| Neurological | Stroke signs, seizures, new confusion, severe headache |
| Infection/Sepsis | High fever + confusion or fast breathing, cold mottled skin |
| Trauma/Bleeding | Uncontrolled bleeding, deep wounds, broken bones, burns |
| Medication-related | Anaphylaxis, adrenal crisis, severe side effects, sudden mental health change |
💬 Final Word
If you're experiencing any of these symptoms, this is not the time to post in a support group or wait to see how things go.
Please don’t delay — even if you’ve had difficult A&E experiences in the past. The risk of waiting is far greater than the discomfort of being seen.
You are never wasting anyone’s time by protecting your health or saving your life.