🧑🤝🧑 Taking Part in Your Own Care: Shared Decision-Making, Self-Management & Advocacy in the NHS
Living with a long-term condition like aspergillosis can be complicated. You may see hospital specialists, your GP, nurses, pharmacists, and sometimes social services too. The NHS is working hard to make sure patients aren’t just “done to,” but are real partners in decisions about their own health.
This approach is called shared decision-making and supported self-management.
🌱 Where did this idea come from?
-
It’s a core part of the NHS Long Term Plan (2019, refreshed 2023/24).
-
The aim: give patients a stronger voice, improve care outside hospital, and reduce emergency admissions.
-
It grew out of earlier “shared care” models, where GPs and hospitals split prescribing or monitoring tasks. Now the focus is much wider: putting patients at the centre of their own care.
💡 What does it mean?
Shared decision-making
-
You and your clinicians decide together.
-
Doctors explain the evidence, options, risks, and benefits.
-
You share what matters most to you — daily life, family, work, fears, and preferences.
-
Example: deciding whether to start biologics, taper steroids, or continue antifungal therapy.
Self-management
-
You are supported to handle your condition day-to-day.
-
This includes recognising early warning signs, having an action plan, knowing when to call for help, and using tools like the NHS App or support groups.
-
Education, pulmonary rehab, peer groups, and digital health apps can all help.
🚧 Barriers patients may face
Even though the NHS wants all patients involved in their care, challenges exist:
-
Short appointments that leave little time for discussion.
-
Medical jargon that is hard to follow.
-
Confidence gaps, especially when you feel unwell.
-
Health inequalities (literacy, language, digital access).
-
Fragmented care, where GP and hospital don’t always join up.
-
Information overload — too much general advice, not enough personalised guidance.
🧑🤝🧑 Can you have an advocate?
Yes. You don’t have to face this alone. Advocacy can come from:
-
Specialist nurses at the National Aspergillosis Centre (NAC) or your local hospital.
-
Family or friends — you are always entitled to bring someone to appointments.
-
Peer groups like NAC CARES, where other patients share practical advice.
-
PALS (Patient Advice and Liaison Service) in every NHS trust.
-
Healthwatch (local branches) or independent advocacy charities.
🔎 Care Coordinators & Link Workers
These are newer NHS roles that help patients navigate complex care.
Care coordinators
-
Support people with complex, long-term conditions.
-
Help organise appointments, blood tests, and follow-up.
-
Make sure GPs, hospitals, and community services talk to each other.
-
Often based in Primary Care Networks (PCNs) or specialist hospital clinics.
Social prescribing link workers
-
Focus on the non-medical side of health.
-
Connect patients to local community support, peer groups, exercise schemes, benefits advice, or housing help.
-
Anyone struggling with isolation, anxiety, or lifestyle issues can be referred.
📋 Criteria for Accessing Care Coordinators & Link Workers
Care Coordinators – who qualifies?
-
Patients with two or more long-term conditions, or one condition requiring complex management (e.g. aspergillosis with antifungals, steroids, biologics, adrenal monitoring).
-
People on multiple medicines or with frequent hospital admissions.
-
Patients needing help to coordinate care between GP, hospital, pharmacy, and community services.
-
Prioritised for those at risk of “falling through the cracks” in the system.
Social Prescribing Link Workers – who qualifies?
-
Any patient whose social or practical situation affects their health.
-
Examples:
-
Feeling isolated or low in mood.
-
Struggling with benefits, housing, or finances.
-
Wanting help with lifestyle changes.
-
Needing connections to peer groups or local activities.
-
-
Usually no strict medical criteria — referral is based on need.
How referrals usually happen
-
GP or practice nurse refers after spotting a need.
-
Hospital team (e.g. NAC or respiratory clinic) may suggest referral back to the GP/PCN.
-
Some PCNs allow self-referral if the service is advertised locally.
📊 How many coordinators are there?
-
As of mid-2025, NHS England data shows:
-
Around 5,000–6,800 full-time equivalent care coordinators employed across Primary Care Networks.
-
Over 3,500 social prescribing link workers active across England.
-
-
Numbers vary by area, and coverage is still expanding as ICSs and PCNs grow their teams.
🧠 Why do people think care coordination is mostly mental health?
-
Historically, most care coordinators were employed in mental health services, where patients often need joined-up support from psychiatry, GPs, housing, benefits, and social care.
-
That’s why many people first hear the term “care coordinator” in relation to community mental health teams.
-
But the NHS is now expanding care coordination into physical long-term conditions, including respiratory diseases like COPD, bronchiectasis, and aspergillosis.
-
Access still varies by region — some areas prioritise cancer, frailty, or diabetes, while others are starting to include respiratory patients.
🧑⚕️ Care Coordination: Mental Health vs Physical Health
| Aspect | Mental Health (traditional focus) | Physical Health (expanding role) |
|---|---|---|
| Where based | Community Mental Health Teams | Primary Care Networks (GP groups), hospital specialist clinics |
| Why developed | To join up psychiatry, GPs, social care, housing, and benefits | To support patients with multiple long-term conditions (e.g. COPD, diabetes, aspergillosis) |
| Patient needs | Severe mental illness, complex social problems, frequent crisis episodes | Complex care plans, multiple medicines, hospital visits, difficulty managing appointments |
| Tasks | Coordinate mental health reviews, social support, community referrals | Organise tests and follow-ups, link GP and hospital, ensure medication and monitoring plans are clear |
| Referrals | Usually from psychiatrist or community mental health nurse | Usually from GP practice, sometimes via hospital specialist or self-referral in PCN areas |
| Examples | Patient with schizophrenia needing GP, psychiatrist, housing officer all linked | Patient with aspergillosis on antifungals, steroids, and biologics needing joined-up GP + hospital care |
| Extra support | Peer groups, advocacy, PALS, housing officers | Social prescribing link workers, community health support, peer groups (e.g. NAC CARES) |
✅ What this means for aspergillosis patients
-
If you have complex care needs (antifungal monitoring, biologics, steroid side-effects, adrenal insufficiency, other chronic conditions), you are likely to meet criteria for a care coordinator.
-
If you are struggling with the social and emotional impact of illness (fatigue, isolation, money worries, lifestyle changes), you may benefit from a link worker.
-
These roles are increasingly available in GP networks, though availability may differ locally.
-
Ask both your hospital team and your GP practice what is available in your area.
🔍 Questions to ask at your next appointment
-
Could I be referred to a care coordinator to help manage my appointments and medicines?
-
Is there a link worker who can support me with non-medical needs?
-
What local services are available through my Primary Care Network or ICS?
-
Who is responsible for updating my care plan?
-
What support is there for my carer or family?
💬 In summary:
Shared decision-making and self-management mean you are an active partner in your care. Aspergillosis is complex, but you don’t have to manage it alone. Between your hospital specialists, GP, advocates, and newer NHS roles like care coordinators and link workers, there is growing support available across the NHS to help you live better and feel more in control.
⚠️ Mistakes in NHS Care: Why They Happen & What You Can Do
🔎 Why mistakes happen
-
Heavy workload: Doctors and nurses handle huge numbers of patients and results every day.
-
Fragmented IT systems: GP, hospital, and lab systems don’t always link, so information can get lost.
-
Human error: Fatigue, multitasking, and assumptions all increase the risk of oversight.
-
Defensive culture: Trusts sometimes minimise problems to protect reputation or avoid litigation.
Most errors are not deliberate — but they can cause harm if they are not caught quickly.
Martha’s Rule was created after a young girl died when her family’s concerns were ignored — it’s designed to stop that happening again.
🛡 What safeguards are already in place?
Although mistakes still happen, the NHS has many systems to reduce risk and catch errors early:
-
Critical results alerts: Labs automatically flag dangerously abnormal results so they cannot be overlooked.
-
Early Warning Scores (NEWS2): Vital signs generate a score that prompts urgent review if the patient is deteriorating.
-
Sepsis protocols: Hospitals have rapid-response pathways for suspected sepsis.
-
Cross-checking: High-risk drugs often require two professionals to sign off.
-
Incident reporting: Staff can log “near misses” to help the system learn.
-
Duty of Candour: Trusts must inform patients if serious harm has been caused by an error.
-
Martha’s Rule: Gives patients/families the right to request an urgent independent review if they feel concerns are being ignored.
💻 Are new IT systems making care safer?
The NHS is moving to large electronic patient record (EPR) systems such as Epic, Cerner and Lorenzo. These bring real safety gains:
Safer features
-
Automatic alerts for critical blood results.
-
Built-in early warning score (NEWS2) calculations to detect deterioration.
-
Electronic prescribing with dose, allergy, and interaction checks.
-
Shared records across hospitals, GPs, and community services.
-
Digital audit trails showing who reviewed results and when.
But challenges remain
-
Too many alerts can cause “alert fatigue,” leading staff to dismiss warnings.
-
System crashes or downtime can force staff back to paper, which is less safe.
-
Complexity can slow clinicians down until they are confident with the system.
-
Hospital and GP systems still don’t fully integrate everywhere, so results can still be missed.
Bottom line: New IT has improved safety compared to the old paper-and-fax systems, but it isn’t foolproof. It works best alongside clinical vigilance and patient involvement.
✅ What you can do if you suspect a mistake
Step 1. Check directly with the clinical team
-
Ask: “Can you confirm this result/issue has been reviewed?”
-
Request a written explanation or clinic letter.
-
Keep notes of the conversation.
Step 2. Escalate to a senior doctor/clinical lead
-
Ask who the consultant in charge is.
-
Write your concern clearly and factually.
Step 3. If your loved one is deteriorating: use Martha’s Rule
-
You can request an urgent review by a critical care team, separate from the ward team.
-
Available 24/7 in hospitals where introduced.
-
Say: 👉 “We want a review under Martha’s Rule.”
-
If not yet in your hospital, ask for the critical care outreach team.
Step 4. Contact PALS (Patient Advice & Liaison Service)
-
They can chase answers and log concerns.
Step 5. Make a formal complaint to the Trust
-
Keep it factual (what happened, why it matters, what outcome you want).
-
The Trust must acknowledge within 3 working days.
Step 6. Escalate outside the Trust
-
If unsatisfied, go to the Parliamentary and Health Service Ombudsman (PHSO).
🧭 Tips to protect yourself & your family
-
Keep copies of all results and letters.
-
Track your results in a simple log.
-
Bring support (family, advocate, charity like AvMA).
-
Stay factual: stick to dates, facts, and impact.
🔑 Key message
Mistakes in healthcare happen for many reasons — but the NHS has safeguards and new IT systems to reduce risk, and Martha’s Rule adds an extra urgent safety net.
Patients and families still play a vital role by asking questions, checking results, and speaking up.
You are not being difficult — you are being safe.
Misinformation on Social Media: Health and Beyond
Social media helps us stay connected, share experiences, and find support. But it also spreads false or misleading stories — about health, politics, money, and world events. These stories can cause unnecessary fear, confusion, and sometimes real harm if people act on them.
Understanding why misinformation spreads, what’s being done about it, and how to spot it helps keep you and your loved ones safe.
🚩 Why do false stories spread?
-
Algorithms reward attention
Platforms are designed to keep you scrolling. Content that shocks (“miracle cure discovered!”), scares (“hidden danger you’re not being told about!”), or excites spreads the fastest — even if it isn’t true. -
Anyone can post anything
Unlike newspapers, medical journals, or BBC/NHS websites, most social media posts aren’t checked by editors or experts before going live. -
Echo chambers
Platforms show you more of what you already click on. If you read about miracle diets or political conspiracies, you’ll see more of them — true or not. -
Deliberate misinformation
Some people spread falsehoods deliberately:-
To sell fake health products
-
To make money from clicks
-
To influence politics or sow division
-
-
Speed beats accuracy
False stories can go viral in minutes. Corrections are slower and rarely reach as many people.
⚖️ What’s being done about it?
Legal approaches
-
UK: The Online Safety Act (2023) requires platforms to remove illegal or harmful misinformation, including dangerous health advice.
-
EU: The Digital Services Act (DSA) makes large platforms responsible for acting faster against harmful content.
-
Extreme cases: Fraud, scams, defamation, or incitement of violence are not protected speech and can be prosecuted.
Technical approaches
-
Algorithms: AI flags suspicious posts.
-
Labelling: Content can be marked as “false” or “missing context.”
-
Bot control: Platforms limit fake accounts that spread stories at scale.
-
Digital nudges: Some apps ask “Do you want to read before sharing?” or warn if a post is outdated.
The limits
-
Freedom of speech protects many misleading opinions unless they cause direct harm.
-
Global reach makes it hard to police.
-
Volume — billions of posts daily are impossible to check one by one.
-
Trust — some people ignore fact-check labels, believing platforms are biased.
🧐 How to know what’s real
Five quick checks:
-
Who is posting it? NHS, WHO, BBC, or Reuters → reliable. Unknown influencer or “miracle cure” shop → beware.
-
Is it reported elsewhere? Real news appears in multiple reputable outlets.
-
Does it use scare tactics or hype? “Doctors don’t want you to know this secret cure!” → red flag.
-
Can you fact-check it? Try NHS.uk, Full Fact (UK), Snopes, Reuters Fact Check or BBC Verify.
-
Check dates and pictures — old or unrelated content is often recycled to look new.
🚦 The traffic-light test
-
🟢 Green – from official sources, confirmed, calm tone → likely true.
-
🟡 Amber – source unclear, dramatic style, no confirmation elsewhere → pause, check.
-
🔴 Red – sensational, “miracle” claims, conspiracy, or urging you to share → almost certainly false.
💡 Should we avoid social media completely?
Not necessarily. Social media has real value for support, awareness, and connection. The key is using it wisely:
-
Follow trusted organisations for health and news.
-
Unfollow or mute accounts that regularly spread falsehoods.
-
Balance social media with direct trusted sources (NHS, GP, recognised news).
-
Step away if scrolling leaves you anxious, angry, or confused.
✨ Bottom line
False stories spread online because the system rewards attention, not accuracy. Laws and technology help, but they can’t stop misinformation entirely.
The best defence is awareness. Before acting on or sharing any post — whether about health, politics, or world events — pause, check, and if in doubt, don’t share.
👉 Protecting yourself from misinformation means protecting your community too.
When Caring for a Loved One Becomes Overwhelming: A Guide for Family Carers
Caring for a spouse, parent, or child is one of the most loving things you can do — but it can also be one of the hardest. Many family carers feel torn: wanting to give the very best care, yet struggling with exhaustion, isolation, and the feeling that “no one else can do it as well as me.”
This guide brings together insights to help you recognise when caring is becoming too heavy, why it feels so difficult to let go, and how to build a sustainable balance that protects both you and the person you love.
Why caring feels so demanding with family
-
Loss of independence: Illness often leaves people feeling powerless. Demanding behaviour can be a way of trying to regain control.
-
Role reversal stress: When a child becomes a parent’s carer, or a spouse becomes more like a nurse, both sides can feel uncomfortable.
-
Emotional safety: Patients often hold back with professionals but show raw feelings at home. That can come across as extra demanding.
-
Blurred boundaries: With family, it’s harder to say “no.” A patient may expect more than they ever would from an outsider.
When the caring role becomes unreasonable
Caring is no longer sustainable when:
-
Your health breaks down from exhaustion or stress.
-
You are completely isolated, with no time for friends, rest, or hobbies.
-
The caree’s demands exceed real need, and everything revolves around them.
-
Boundaries disappear and you can’t say no without conflict.
-
You are the only source of support, with no outside help.
These are warning signs that it’s time to rebalance the situation.
Why it doesn’t mean “defeat”
Asking for help can feel like admitting failure — but it isn’t.
-
Caring is a marathon, not a sprint. Protecting your health means you can keep caring longer.
-
Strength means knowing your limits. Bringing in help shows foresight, not weakness.
-
Love isn’t replaced. Professional carers can take tasks off your hands, but your relationship and bond remain uniquely yours.
Think of it not as “stepping back” but as building a care team. You remain the anchor, but you don’t carry everything alone.
Why it’s hard to let others help
Many carers say: “They don’t do it as well as I do.” This is natural — you know your loved one’s habits and needs better than anyone. Professionals may work differently, and that can feel uncomfortable.
But:
-
Different doesn’t always mean worse — just not “your way.”
-
Perfection isn’t sustainable if it destroys your health.
-
Your role as spouse/child/friend is irreplaceable — letting others handle routine care may free you to keep that role.
Start small: allow someone else to take over one task or cover for a short period. Gradually, trust can build.
Can problems be predicted?
Yes — carers often see the signs early:
-
Constant exhaustion or resentment
-
Dropping their own health needs or appointments
-
Losing touch with friends and community
-
Feeling guilty if they take any time for themselves
If these signs appear, it’s time to bring in extra support before crisis strikes.
Practical steps to make caring sustainable
-
Have early, honest conversations about what you can and cannot do.
-
Ask for a Carer’s Assessment (in the UK) — this can open up respite care, day services, and financial support.
-
Bring in professional support early so it feels like teamwork, not abandonment.
-
Protect your own time — even short, regular breaks keep you healthier.
-
Seek peer support — carers’ groups and counselling reduce isolation.
Final thought
Caring is an act of deep love. But love alone cannot carry the whole weight forever. Sharing the load is not defeat — it is the wisest way to ensure that both you and your loved one remain safe, cared for, and connected.
You are not failing. You are leading a team, protecting your own well-being, and preserving the relationship that matters most.
📚 New Children’s Book Helps Families Understand Aspergillosis
Launch Event at Affinity Outlet, Fleetwood – 13th September 2025
The Aspergillosis Trust is delighted to announce the launch of a brand-new children’s book, Dad and the Sneaky Spores, written by award-winning author Christina Gabbitas and beautifully illustrated by Ursula Hurst.
This story has been specially commissioned to raise awareness of aspergillosis, a serious lung condition caused by the Aspergillus fungus. Through gentle storytelling and colourful illustrations, the book helps children and families understand what it means to live with a parent affected by aspergillosis.
✨ About the Event
📅 Date: Saturday 13th September 2025
📍 Location: Affinity Outlet, Fleetwood
The launch event will be a fun and informative day for all the family.
-
✍️ Meet the Author: Christina Gabbitas will be signing copies of the book between 12pm and 2pm.
-
👩⚕️ Ask the Experts: A qualified nurse will be available to answer medical questions or offer advice.
-
📚 Learn Together: Families can explore how storytelling can make complex health conditions easier to understand.
📖 About Dad and the Sneaky Spores
The book follows a family’s journey with aspergillosis in a way that children can relate to. It not only explains the illness but also encourages empathy, resilience, and understanding within families.
“The narrative not only educates readers about aspergillosis but is also thoughtfully crafted to foster empathy and understanding.” – Aspergillosis Trust
Published by Poems & Pictures, Dad and the Sneaky Spores is available from 1st August 2025.
💜 Why This Matters
Aspergillosis is a rare and often misunderstood condition. By raising awareness through creative storytelling, this initiative provides a new way to start important conversations with children, families, and the wider community.
🔗 Find out more at: www.aspergillosistrust.org
Prednisone, Hydrocortisone, and Adrenal Function – What Patients Need to Know
Why Aspergillosis Patients Are Often Given Prednisolone
Prednisolone is often prescribed for patients with aspergillosis (especially Allergic Bronchopulmonary Aspergillosis – ABPA) because it helps to reduce lung inflammation and allergic reactions triggered by Aspergillus spores. It can be life-changing in controlling breathlessness, wheeze, and repeated flare-ups. However, using steroids for weeks or months can affect the body’s own natural hormone production.
How Do I Know If I Might Need Adrenal Testing While on Prednisolone?
Prednisolone is a corticosteroid medicine. If you take it for more than a few weeks, it can “switch off” your adrenal glands, which normally make the hormone cortisol. Cortisol is essential for coping with stress, fighting infection, and maintaining energy.
You might need adrenal testing if you notice:
-
Extreme tiredness or weakness, especially if it worsens when tapering your pred dose.
-
Excessive sleepiness or difficulty staying awake, even when rested.
-
Feeling much worse during stress or illness (for example, flu, chest infection, or surgery).
-
Dizziness or fainting on standing (low blood pressure symptoms).
-
Nausea, vomiting, or stomach pain that isn’t explained by infection or medicines.
-
Unexplained weight loss or poor appetite.
Why Might Patients Stop Making Cortisol?
The adrenal glands may temporarily stop producing cortisol if they have been “switched off” by long-term steroid treatment. This is called secondary adrenal insufficiency. It is usually reversible, but recovery can take months or even years.
In contrast, primary adrenal insufficiency (Addison’s disease) is when the adrenal glands are damaged and stop working permanently. This is not caused by steroids, but by autoimmune or other diseases.
Symptoms of Low DHEA
The adrenal glands also produce DHEA, a weak sex hormone that contributes to mood, energy, and libido — particularly important in women. Long-term steroid use or secondary adrenal insufficiency may reduce DHEA levels.
Possible signs of low DHEA:
-
Ongoing low energy or fatigue, even when cortisol is replaced
-
Low mood, depression, or “flat” emotions
-
Reduced libido (sex drive)
-
Thinning of underarm or pubic hair (especially in women)
-
Lower resilience or general sense of well-being
Not all patients with adrenal insufficiency need DHEA replacement, but in some, it can make a difference. This is assessed by specialists.
How to Tell the Difference Between Causes of Fatigue
Because fatigue can come from several overlapping sources, it helps to compare:
| Symptom | Cortisol deficiency (Adrenal Insufficiency) | Prednisolone Side Effect | Low DHEA |
|---|---|---|---|
| Sudden exhaustion during stress/illness | ✅ | ❌ | ❌ |
| Sleepiness, can’t stay awake | ✅ | ❌ | ❌ |
| Dizziness or fainting | ✅ | ❌ | ❌ |
| Nausea, vomiting, stomach upset | ✅ | ❌ | ❌ |
| Insomnia, wired-but-tired feeling | ❌ | ✅ | ❌ |
| Mood swings, irritability | ❌ | ✅ | ❌ |
| Weight gain, bloating, “puffy face” | ❌ | ✅ | ❌ |
| Ongoing low energy despite treatment | ❌ | ❌ | ✅ |
| Low mood, “flat” emotions | ❌ | ❌ | ✅ |
| Reduced libido | ❌ | ❌ | ✅ |
| Thinning pubic/underarm hair (women) | ❌ | ❌ | ✅ |
✅ = typical feature
Prednisolone, Hydrocortisone and Fatigue
-
If a patient is on prednisolone and feels extremely fatigued during stress or illness, it may mean their body is not making enough natural cortisol.
-
If they are tapering prednisolone and develop fatigue or sleepiness, this can mean the taper is too fast and the adrenal glands have not “woken up” yet.
-
If a patient feels tired while still on prednisolone, it could be due to:
-
Side effects of prednisolone itself,
-
Lack of natural cortisol (adrenal suppression),
-
Or low DHEA.
-
Treatment and Monitoring
-
Doctors may recommend slowing or pausing tapering if adrenal insufficiency is suspected.
-
Some patients are switched to hydrocortisone, which more closely mimics natural cortisol.
-
In situations of stress (infection, surgery, trauma), patients may need extra “stress doses” of steroids.
-
Patients at risk should carry a steroid emergency card or medical alert bracelet.
👉 Key message:
Aspergillosis patients often need steroids, but long-term use can suppress natural adrenal function. Fatigue can come from:
-
Low cortisol,
-
Prednisolone side effects,
-
Or low DHEA.
Since these overlap, specialist endocrine advice is often needed to work out the cause.
Other forms of aspergillosis: Aspergilloma (Fungal Ball in the Lung)
Aspergilloma (Fungal Ball in the Lung)
An aspergilloma is a clump of fungus (usually Aspergillus) that grows inside an old cavity in the lung. These cavities often form after conditions like tuberculosis (TB), other lung infections, or lung disease. The fungus does not usually invade healthy lung tissue, but it uses the cavity as a space to grow.
How common is aspergilloma?
-
Aspergillomas are uncommon overall, but they are more likely to appear in people who have had tuberculosis in the past.
-
In some countries where TB is (or was) common, aspergillomas are found quite frequently.
-
In countries like the UK, they are rare, but can still happen in people with conditions such as COPD, sarcoidosis, or after lung surgery.
-
Doctors often describe aspergilloma as part of the wider group of conditions called chronic pulmonary aspergillosis (CPA).
What are the symptoms?
-
Many people with an aspergilloma have very few symptoms at first – sometimes only a cough.
-
The most serious problem is bleeding from the lungs (haemoptysis). This can range from small streaks of blood in the sputum to heavy, life-threatening bleeding.
-
Some people may also have chest infections, breathlessness, or tiredness if other lung problems are present.
How is it found?
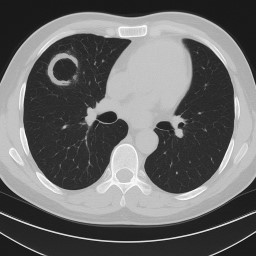
-
An aspergilloma usually shows up on a chest scan (X-ray or CT).
-
It often looks like a round “ball” inside a cavity in the upper part of the lung.
-
Sometimes it can move around a little inside the space.
-
Important note: Aspergillomas are not cancer, but they can sometimes be mistaken for cancer on scans. For this reason, doctors may arrange extra tests (such as blood tests, repeat scans, or sometimes biopsy) and may refer patients to the National Aspergillosis Centre (NAC) to be certain of the diagnosis.
Who looks after you?
-
At your local hospital, aspergillomas are usually managed by a respiratory (chest) specialist doctor.
-
Depending on your situation, they may also work with:
-
Thoracic surgeons (for possible surgery)
-
Radiologists (for scans or embolisation)
-
Infectious diseases doctors (for antifungal treatment)
-
-
If your case is complex, unclear, or high-risk, your local team can refer you to the National Aspergillosis Centre (NAC) at Wythenshawe Hospital, Manchester. NAC is the UK’s only NHS specialist centre for aspergillosis and provides expert diagnosis, advanced testing, and treatment advice, often working alongside your local hospital team.
What is the outlook (prognosis)?
-
Some aspergillomas remain stable for years and cause very few problems.
-
A small number may even disappear on their own, although this is unusual.
-
The main risk is serious bleeding, which can be sudden. This is why regular check-ups are important.
-
Surgery to remove the part of lung with the aspergilloma is usually the most effective treatment and can be curative in suitable patients.
-
For people who cannot have surgery, treatments such as blocking bleeding vessels (embolisation) or instilling antifungal medicine into the cavity can sometimes help, but problems may return.
🚨 Emergency: If you cough up blood 🚨
-
Small streaks of blood (mild):
-
Stay calm – these often stop by themselves.
-
Contact your hospital team promptly to let them know.
-
Keep a record of how much and how often it happens.
-
-
More than a few teaspoons, clots, or ongoing bleeding (moderate to heavy):
-
Call 999 (UK) or go to A&E immediately.
-
Sit upright to help protect the other lung.
-
Take this leaflet or your aspergillosis care details with you.
-
-
Very heavy bleeding (life-threatening):
-
Treat this as an emergency.
-
Emergency doctors may use medicine to help blood clot, a procedure to block the bleeding vessel (embolisation), or surgery if possible.
-
⚠️ Always report any bleeding to your doctor, even if it seems small.
Treatment options
-
No treatment may be needed if the aspergilloma is small, not causing bleeding, and the person feels well. Regular monitoring is important.
-
Surgery is the most effective treatment if the fungal ball is causing repeated or heavy bleeding.
-
Antifungal tablets are sometimes used before or after surgery, but on their own they are usually not very effective.
-
Tranexamic acid – a medicine that helps the blood clot – is sometimes prescribed to reduce or control bleeding. It can be taken by mouth or given in hospital if bleeding is significant. It does not remove the aspergilloma but can help keep bleeding under control.
-
Other treatments for people who cannot have surgery include:
-
Blocking the bleeding blood vessels (embolisation) – this can stop bleeding, but the effect may not last.
-
Instilling antifungal medicine directly into the cavity – less common, results vary.
-
Key points for patients
-
An aspergilloma is not cancer, but because it can sometimes look like cancer on scans, careful checks and sometimes referral to the NAC are needed.
-
The main risk is bleeding, which may require urgent treatment.
-
Surgery offers the best chance of cure, but only if lung function allows.
-
If you have an aspergilloma, you should:
-
Attend regular hospital check-ups.
-
Report any coughing up of blood immediately.
-
Take tranexamic acid if prescribed for bleeding, but also inform your doctor if bleeds occur.
-
Avoid blood-thinning medicines (like aspirin, ibuprofen, or some herbal remedies) unless your doctor prescribes them.
-
🩺 NHS Data Sharing: How It Will Improve Your Care
🌍 The Problem Today
At the moment, your health information is stored in many different places:
-
Your GP (General Practitioner) has one record.
-
Hospitals keep their own records.
-
Community services (like district nurses or physiotherapists) have separate notes.
-
Social care also keeps its own information.
This can cause problems:
-
You may be asked to repeat your story again and again.
-
Doctors don’t always see the full picture (medications, allergies, past test results).
-
Sometimes tests are repeated unnecessarily.
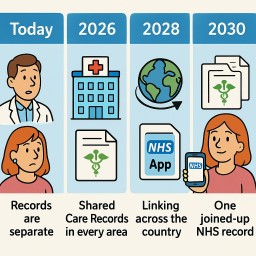
📅 The Timeline for Change
Today (2025)
-
Records are mostly separate.
-
Some areas already share basic information like your medicines and allergies through a “Summary Care Record.”
👉 What it means for you: You still have to repeat information at most appointments.
2026 – Shared Care Records in Every Area
-
Every region (called an Integrated Care System, or ICS) will have a Shared Care Record.
-
This links together information from GPs, hospitals, community teams, and social care.
-
Hospitals using modern systems like Epic (a type of electronic patient record - MFT has installed this already) can also start sharing directly with other Epic hospitals.
👉 What it means for you: Doctors can see more of your health record without asking you to repeat everything.
2028 – Linking Across the Country
-
Regional Shared Care Records will start to connect with each other.
-
Epic hospitals across the UK will share records more easily using Care Everywhere (Epic’s sharing tool).
-
Community services and “virtual wards” (hospital care at home) will be fully connected.
👉 What it means for you: If you are treated in another part of the country, staff there will be able to see important parts of your health record straight away.
2030 – One Joined-Up NHS Record
-
The NHS plans to give every patient a longitudinal record – one joined-up health and care record that follows you everywhere.
-
This will combine information from GPs, hospitals, community services, mental health teams, and social care.
-
Patients will also be able to see much more of their own record through the NHS App.
👉 What it means for you: Wherever you go in the NHS, staff can see your medical history safely. You’ll feel your care is joined-up, and you can also check your record yourself.
✅ Your Patient Journey: Step by Step
-
Today: “I have to explain my medication list every time. I’m not sure my hospital knows what my GP prescribed.”
-
2026: “When I go into hospital, the doctor can already see my GP record and community nurse notes.”
-
2028: “I was treated far from home, and the hospital could see my recent test results straight away.”
-
2030: “Wherever I go, the NHS staff have the full picture. I can see my record too on the NHS App.”
Why It Can Be Hard to Clear Carbon Dioxide (CO₂) From the Lungs in Aspergillosis
When we breathe, oxygen comes in and carbon dioxide (CO₂) goes out. For people living with aspergillosis (ABPA or CPA), and sometimes with other conditions like severe asthma, COPD, or bronchiectasis, this process can be much more difficult.
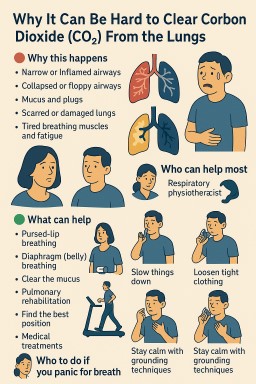
🔴 Why this happens
-
Narrow or inflamed airways
In ABPA or asthma, swelling and tightening of the breathing tubes can trap air inside. -
Collapsed or floppy airways
In COPD and bronchiectasis, airways may close too soon when you breathe out, leaving CO₂ stuck in the lungs. -
Mucus and plugs
Thick or sticky mucus — common in ABPA, bronchiectasis, and COPD — blocks airways and reduces airflow. -
Scarred or damaged lungs
CPA can create cavities and scarring that make air movement less efficient. -
Tired breathing muscles and fatigue
Long-term illness, steroid use, or simple exhaustion can weaken the diaphragm and chest muscles, making it harder to breathe out fully.
🟢 What can help
-
Pursed-lip breathing
Inhale gently through your nose, then breathe out slowly through pursed lips (like blowing out a candle). This keeps airways open longer so CO₂ can escape. -
Diaphragm (belly) breathing
Using your stomach muscles for slower, deeper breaths improves oxygen and CO₂ exchange. -
Clear the mucus
Daily airway clearance (physio techniques, huff coughing, or devices like Acapella, Flutter, Aerobika) can stop mucus building up and blocking airways. -
Pulmonary rehabilitation
Specialist exercise and breathing training improve stamina, breathing control, and lung efficiency. -
Find the best position
Sitting upright or leaning forward slightly often makes it easier to breathe out during flare-ups. -
Medical treatments
Your team may use antifungals, steroids, inhalers, or nebulisers to reduce inflammation and mucus.
If CO₂ levels remain too high, oxygen therapy or breathing support machines (like BiPAP or CPAP) may be needed.
👩⚕️ Who can help most
The best place for personalised advice is usually a respiratory physiotherapist.
They can:
-
Teach you the right breathing techniques
-
Show you how to clear your airways effectively
-
Support you with safe exercise and pacing strategies
🟦 What to do if you panic for breath
Feeling panic when breathless is common — but panic can make breathing even harder. Try these steps:
-
Stop and sit upright — lean slightly forward with your arms supported on a table or your knees.
-
Focus on breathing out — use pursed-lip breathing (in through the nose, out slowly through pursed lips).
-
Slow things down — count “in for 2, out for 4” to calm breathing.
-
Loosen tight clothing — open collars or waistbands to ease pressure on the chest.
-
Use your reliever inhaler or nebuliser if prescribed.
-
Stay calm with grounding techniques — focus on your surroundings (e.g. name things you see or hear) to reduce panic.
⚠️ When to seek urgent help
-
If your breathing does not improve after following these steps.
-
If you are too breathless to speak in full sentences.
-
If you feel faint, confused, or unusually drowsy.
-
If you have sudden chest pain or start coughing up a lot of blood.
➡️ Call 999 or go to A&E immediately in these situations.
✅ Key message
For patients with aspergillosis, especially when combined with asthma, COPD, or bronchiectasis, clearing CO₂ can be harder because of blocked or damaged airways, mucus, and fatigue.
-
Learning breathing techniques
-
Clearing mucus regularly
-
Seeking advice from a respiratory physiotherapist
-
Knowing what to do if you panic for breath
…can all make a big difference in helping you breathe more easily and safely.
Why Does Prednisolone Affect Energy Differently?
If you live with aspergillosis, you may be prescribed prednisolone, a type of steroid medicine that reduces inflammation in the lungs. Many patients notice changes in their energy levels — but not everyone experiences the same effects.
Why some feel “full of energy”
-
Boosting effect: Prednisolone can act a bit like adrenaline, raising blood sugar and speeding up metabolism.
-
Improved breathing: When inflammation in the lungs is brought under control, it may feel easier to breathe, which can make you more energetic.
-
Mood lift: In some people, steroids can trigger feelings of alertness or even mild euphoria.
Why others feel very tired
-
Sleep disturbance: Prednisolone can interfere with your normal sleep pattern, especially if taken later in the day. Poor sleep = daytime fatigue.
-
Body effects: Steroids can cause muscle breakdown, fluid changes, or blood sugar swings, which may leave you feeling drained.
-
Adrenal suppression: If you’ve been on steroids for a while, your body’s own cortisol production may slow down, leading to tiredness, especially during dose reductions.
-
Underlying illness: Even if the steroid helps, aspergillosis itself (with coughing, infections, or bleeding) can still leave you exhausted.
What you can do
-
Take in the morning: This reduces the chance of sleep problems.
-
Plan rest breaks: Listen to your body if you’re feeling tired.
-
Track your symptoms: Notice if your energy changes when doses go up or down.
-
Talk to your doctor: If you feel extremely fatigued or “too wired to sleep,” your team may be able to adjust your dose, timing, or taper.
✅ Key message for patients:
It is normal for people with aspergillosis to respond differently to prednisolone — some feel more energetic, while others feel exhausted. Both reactions are common. If the effects are troubling, discuss them with your medical team so your treatment can be adjusted safely.