Information on Allergic BronchoPulmonary Aspergillosis (ABPA) / SAFS – For Family and Friends
Print out or share electronically
WHAT IT IS
ABPA (Allergic Bronchopulmonary Aspergillosis) and SAFS (Severe Asthma with Fungal Sensitisation) are allergic reactions to a common fungus, Aspergillus. In some people with asthma, the immune system overreacts to spores in the air, causing inflammation, swelling, and mucus plugs in the lungs.
WHAT IT'S NOT
-
Not contagious – you can't catch it.
-
Not poor hygiene – Aspergillus is everywhere in the air.
-
Not the patient's fault – flare-ups happen because of the condition, not something they did or didn't do.
WHY AREN'T OTHERS AFFECTED?
Most people's lungs clear these spores easily. In ABPA/SAFS the immune system reacts too strongly – more likely with long-standing asthma, severe allergies, damaged airways (e.g., bronchiectasis), or a genetic tendency. It's not weakness or lifestyle choices – often just lung history and bad luck.
TYPICAL SYMPTOMS
-
Wheezing, cough (sometimes with mucus plugs)
-
Breathlessness
-
Severe fatigue
-
Sometimes coughing up blood
WORST SYMPTOMS
-
Mucus plugs – thick, sticky clumps blocking airways, making breathing suddenly harder.
-
Intense coughing – can be exhausting, cause chest pain, and disrupt sleep.
TREATMENT
-
Anti-inflammatory medicines (often steroids)
-
Antifungals to reduce Aspergillus in the airways
-
Biologics for severe asthma/allergic inflammation
-
Monitoring with blood tests, breathing tests, and scans
THE REALITY
This condition can dominate daily life. On bad days the person may not be able to do much at all. Energy and breathing can change day-to-day (even hour-to-hour). If plans are cancelled, it isn't a lack of interest – it's the illness. Flare-ups can also make people feel short-tempered – a natural reaction to frustration, not a lack of care. Many people also live with a constant awareness of environmental risks – weighing up every new place or activity for dust, damp, or spores. This can feel exhausting and may lead them to avoid situations that others wouldn’t think twice about.
LOOKING AHEAD
-
With good control – Many people manage their symptoms well, reduce flare-ups, and keep active with the right treatment and avoidance of triggers.
-
Risks – Without good control, repeated flare-ups can slowly damage the lungs and lead to bronchiectasis.
-
Change over time – Some improve and need less treatment; others have ongoing ups and downs. Early action on flare-ups makes a big difference.
ENVIRONMENTAL TRIGGERS & PROTECTION
Some people with ABPA or SAFS have to avoid dust, mould, strong smells, smoke, and damp places – these can trigger flare-ups. Activities like gardening, compost turning, or DIY can be risky because they release fungal spores into the air. Wearing a well-fitting mask (e.g., FFP2/FFP3) can help reduce exposure – it's about staying well, not being antisocial.
HOW FRIENDS AND FAMILY CAN BEST HELP
-
Be flexible with plans – energy and breathing can change suddenly; last-minute cancellations aren't personal.
-
Help avoid triggers – choose low-dust, low-mould venues and activities.
-
Support treatment routines – lifts to appointments, collecting prescriptions, or reminders if welcome.
-
Listen without judgement – let them share symptoms and frustrations.
-
Encourage safe activities – suggest hobbies and outings with low environmental risk.
-
Show affection and reassurance – a hug, a kind message, or checking in can mean a lot.
MORE INFORMATION & SUPPORT
National Aspergillosis Centre (UK): https://mft.nhs.uk/wythenshawe/services/infectious-diseases/national-aspergillosis-centre/
Patient information & community: https://aspergillosis.org
Chronic Pulmonary Aspergillosis (CPA) – Information For Family and Friends
Print this off or share electronically
WHAT IT IS
CPA (Chronic Pulmonary Aspergillosis) is a long-term lung infection caused by the Aspergillus fungus. It often develops where lungs are already damaged (e.g., TB, COPD, bronchiectasis, sarcoidosis) and may form cavities, sometimes with fungal balls (aspergillomas).
WHAT IT'S NOT
-
Not contagious – you can't catch CPA.
-
Not poor hygiene – spores are everywhere in the air.
-
Not the patient's fault – flare-ups or setbacks happen because of the illness, not something they did wrong.
WHY AREN'T OTHERS AFFECTED?
Most people remove spores without trouble. CPA appears when lungs are already damaged or the immune system can't fight the fungus well – after past infections, chronic lung disease, or weakened defences. It's not about choices; it's lung history and chance.
TYPICAL SYMPTOMS
-
Persistent cough (sometimes with blood)
-
Breathlessness
-
Fatigue and low energy
-
Weight loss
-
Recurring chest infections
WORST SYMPTOMS
-
Coughing up blood – can be small streaks or larger amounts; sudden and frightening; urgent if heavy.
-
Severe fatigue – can stop even simple tasks; not just ‘tiredness’.
TREATMENT
-
Long-term antifungal medication
-
Regular scans and blood tests
-
Surgery in selected cases
THE REALITY
CPA is a serious, long-term condition. On bad days, people may not be able to do much at all. Symptoms can dominate daily life and limit social plans – cancelled arrangements are the illness talking, not them. It can also make people feel grumpy or irritable – not because they don't care, but because constant symptoms, tiredness, and limits on daily life are frustrating and exhausting. There’s often a mental load too – always thinking about avoiding dust, damp, or mould spores, and sometimes feeling overcautious about activities like going on boats, visiting old buildings, or anywhere that might harbour moisture or mould. This risk-checking is a form of self-protection, even if it means missing out.
It’s important to mention the mood swings and fatigue caused not only by the disease but also by the medication. For some, constant hand tremors are also part of daily life — these are often misunderstood by others.
LOOKING AHEAD
-
With effective treatment – Many people can keep the infection stable for years, control symptoms, and stay independent.
-
Risks – CPA can slowly progress, and severe flare-ups (like coughing large amounts of blood) may need urgent treatment.
-
Change over time – The illness can be stable for long periods, but it often needs lifelong monitoring and treatment changes. Support from specialists helps keep people well for longer.
ENVIRONMENTAL TRIGGERS & PROTECTION
Some people with CPA need to avoid environments with high levels of dust or fungal spores. This includes gardening, composting, building work, or damp/mouldy places. Wearing a protective mask during these activities can help reduce risk. Avoiding these triggers is about preserving lung health – not being fussy or antisocial.
HOW FRIENDS AND FAMILY CAN BEST HELP
-
Respect limits – breathlessness, fatigue, or coughing up blood can stop plans at short notice; it's not a choice.
-
Minimise exposure risks – avoid inviting them to dusty, damp, or mouldy places.
-
Offer practical help – driving to appointments, carrying shopping, or helping at home during flare-ups.
-
Be patient with mood changes – grumpiness can come from exhaustion and constant vigilance against triggers.
-
Talk openly about safety – if you suggest an outing, ask “Would this feel safe for you?”
-
Stay connected – even if they can't join in physically, a call or small gesture keeps them included.
MORE INFORMATION & SUPPORT
National Aspergillosis Centre (UK): https://mft.nhs.uk/wythenshawe/services/infectious-diseases/national-aspergillosis-centre/
Patient information & community: https://aspergillosis.org
Damp, Cold, and Poor Housing – Why It Matters for Lung Health
This briefing from the House of Commons Library (2025) looks at how poor housing conditions—especially damp, mould, and cold homes—affect health and what’s being done about it in the UK.
Main Points
-
Health risks are serious
Living in damp or mouldy homes increases the risk of respiratory problems, particularly for people with existing lung disease like aspergillosis, asthma, COPD, or bronchiectasis. -
Children and vulnerable adults
Young children, older adults, and people with weakened immune systems are most affected. Damp and mould can trigger flare-ups, worsen breathing symptoms, and increase infection risk. -
Mental health impact
Poor housing is linked to stress, anxiety, and depression. Worrying about your home can also worsen physical symptoms, especially if you avoid using rooms with mould or limit heating to save costs. -
Cold homes add to the problem
Cold airways can make breathing more difficult, weaken the immune system, and increase the chance of winter infections. -
Wider health effects
Damp and cold can also affect heart health, bone/joint pain, and overall wellbeing.
What’s Being Done
-
Legal responsibilities: Landlords must keep homes safe and fit to live in under UK law. This includes dealing with serious damp and mould.
-
Government programmes:
-
Funding for improving insulation and heating in social housing.
-
Advice services for tenants.
-
Local councils can take action if landlords fail to address hazards.
-
-
Public health guidance now recognises the link between housing and chronic illness, with stronger advice for early intervention.
What This Means for Aspergillosis Patients
-
Stay alert to symptoms: If your cough, breathlessness, or fatigue worsen at home, check for damp, mould, or poor heating.
-
Act early: Report problems to your landlord or council quickly—prolonged exposure can worsen lung damage.
-
Medical link is recognised: You are more likely to be taken seriously now, as official guidance acknowledges the health risks.
-
Keep records: Photos, symptom diaries, and GP notes can support housing complaints.
For full details see https://commonslibrary.parliament.uk/research-briefings/cdp-2025-0096/
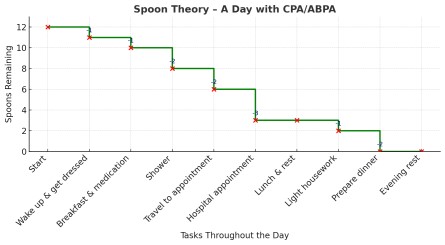
Spoon Theory: Making Sense of Energy Limits in Aspergillosis
The Spoon Theory is a way of explaining what it’s like to live with a long-term illness that affects your energy and stamina. It was first described by Christine Miserandino, who used spoons as a visual metaphor for the limited amount of energy she had each day.
How it works
-
Imagine you start each day with a set number of spoons — maybe 10 or 12.
-
Every task you do “costs” spoons:
-
Getting dressed might cost 1 spoon
-
Cooking a meal might cost 2 spoons
-
A shower could cost 2 spoons on a bad day
-
Going for a walk or attending an appointment might cost 3 or 4 spoons
-
-
When you run out of spoons, that’s it — you don’t have the energy to keep going. If you push yourself, you “borrow” from tomorrow’s spoons, which can leave you feeling worse for days.
 Why CPA and ABPA drain your spoons
Why CPA and ABPA drain your spoons
Both conditions can cause:
-
Breathlessness – even small tasks can feel like hard work.
-
Coughing and mucus production – which can be exhausting physically.
-
Flare-ups – like haemoptysis (coughing blood) in CPA or allergic inflammation in ABPA.
-
Medication side effects – antifungals, steroids, or biologics can also sap your energy.
-
Frequent appointments – travel and hospital visits can eat into your spoon supply.
Why Spoon Theory matters
Understanding Spoon Theory helps you:
-
Plan your day – save enough spoons for the important things.
-
Pace yourself – spread out demanding tasks, rest between them.
-
Explain your limits – it’s an easy way to help friends, family, and employers understand that you’re not being lazy — you’re managing your limited energy.
-
Avoid “boom and bust” – pushing too hard on a good day can leave you with no spoons for the next few days.
Practical tips
-
Prioritise – decide what’s essential today and what can wait.
-
Ask for help – let others “spend” their spoons for you when possible.
-
Rest without guilt – recharging is part of living with a long-term condition.
-
Track your spoons – keeping a symptom diary can help you notice patterns.
Remember: Your number of spoons can change day-to-day, especially if you’ve had a flare-up, infection, or a hospital stay. Learning to work with your spoons instead of against them can help you stay in control and reduce stress.
💭 Why Some People with Aspergillosis Delay Going to A&E
And Why That Could Be Dangerous
If you live with chronic aspergillosis — whether CPA, ABPA, SAFS, or aspergillus bronchitis — you’ve probably had moments where your symptoms suddenly worsened and you didn’t know what to do. Maybe you’ve thought about going to A&E, or even dialling 999, but something stopped you.
You're not alone. Many people in our community feel reluctant to seek emergency care, even when they’re very unwell.
Here’s why — and why it matters.
🏥 “I’ve Been to A&E Before — and It Wasn’t a Good Experience”
Many patients have told us:
-
“I waited for hours just to be told it’s probably my usual symptoms.”
-
“The staff didn’t seem to know what aspergillosis is.”
-
“They didn’t know how to manage my antifungal treatment or asthma.”
-
“I felt dismissed — like I was being dramatic.”
Experiences like this can leave people feeling humiliated or unsafe, and understandably less likely to go back — even when things are serious.
🛏️ “I Don’t Want to Be Admitted — I’ll Be Stuck There”
A&E can be a gateway to hospital admission, and for someone managing a complex, fluctuating condition at home, this can feel like losing control. You may worry about:
-
Being put on the wrong ward
-
Catching infections
-
Not being given the right antifungal, steroid, or oxygen support
-
Losing time, independence, or confidence
So instead, you might choose to stay home — sometimes too long.
⌛ “I Don’t Want to Waste Anyone’s Time”
We hear this all the time:
“A&E is for people who are really ill — not for someone like me.”
“The NHS is already overwhelmed.”
“I’ll just give it a bit more time.”
But remember: you’re not wasting time by going to A&E if your health is deteriorating. Chronic illness doesn’t make your emergency less urgent — it just makes it harder to spot.
😔 “I’m Tired of Needing Help”
Living with chronic aspergillosis is exhausting. It’s easy to feel like:
-
“I should be able to manage this myself.”
-
“I don’t want to be a burden.”
-
“It’s probably just another bad flare.”
But when symptoms cross a line — from “bad day” to “dangerous” — it’s vital to act. Seeking urgent care isn’t failure. It’s strength.
🌫️ “I Didn’t Know It Was That Serious”
The truth is: even very experienced patients often aren’t sure when symptoms need emergency treatment. You might think:
-
“I’ve had breathlessness before — I’ll just rest.”
-
“The coughing is worse, but it’s happened before.”
-
“I’ll wait until the morning and see.”
But if you’re coughing blood, can’t speak a sentence, can’t stand up, or feel confused or faint, waiting is dangerous.
💬 “I Asked in a Group First”
Support groups are amazing — and a lifeline for many. But no group can diagnose an emergency. If you're:
-
Asking whether to go to A&E
-
Describing symptoms that sound like respiratory failure, sepsis, or adrenal crisis
-
Hoping someone tells you not to worry...
Then it’s already time to act, not wait for replies.
✅ Final Message
If you have severe symptoms, sudden changes, or feel frightened about your health:
Don’t wait. Don’t post. Don’t hope it passes.
Call 999 or go to A&E.
You are not a burden. You are not overreacting.
You are saving your own life.
When to go to A&E or call 999
🚨 When to Go to A&E or Call 999
A Guide for People with Chronic Aspergillosis, Asthma, and Other Long-Term Conditions
When you live with a long-term health condition like chronic aspergillosis (CPA), allergic bronchopulmonary aspergillosis (ABPA), severe asthma, or immunosuppression, it can be hard to know when a flare-up is “just part of the illness” — and when it’s something more serious that needs emergency medical care.
This guide is designed to help you — or someone you care for — recognise the signs that mean it’s time to stop waiting, stop asking for online advice, and get help immediately.
🧠 A Special Note for People with Aspergillosis
People living with chronic aspergillosis often get used to symptoms like breathlessness, coughing, fatigue, or chest tightness. That makes it easy to miss or downplay serious changes — especially if you're reluctant to make another trip to A&E.
But there are times when acting fast is critical.
If you have CPA, ABPA, SAFS, or aspergillus bronchitis, you should go to A&E or call 999 immediately if you experience:
-
🫁 Sudden or worsening breathlessness, especially if it’s different from your usual
-
💨 Breathing that doesn’t improve after using inhalers, nebulisers, or oxygen
-
💔 New chest pain or tightness — particularly if it spreads or worsens when breathing
-
🌡️ A high fever, shaking chills, or flu-like symptoms
-
🩸 Coughing up blood — especially if it's fresh or in large amounts
-
🧠 Feeling confused, drowsy, or faint
-
❗ Severe weakness, fatigue, or inability to stand or walk
-
💊 Severe reaction to medications (e.g. antifungals, steroids, or biologics) — rash, swelling, dizziness, jaundice
⚠️ Don’t Wait or Ask Online — Act Fast When These Signs Appear
We completely understand why some people — particularly those with severe asthma, CPA, or ABPA — may be hesitant to go to A&E. You may have faced:
-
Long waits
-
Feeling dismissed or misunderstood
-
Fear of hospital admission
-
Exhaustion from too many medical appointments
These are real concerns, but when you're struggling to breathe, disoriented, or deteriorating rapidly, it’s not the time to post in a support group or wait for reassurance. It’s time to act.
In life-threatening moments, what you need isn’t advice — it’s treatment.
No support group — no matter how compassionate — can replace oxygen, IV antibiotics, a steroid boost, or emergency care.
Please don’t delay. You are never wasting anyone’s time by seeking help when something feels wrong.
🔥 Emergency Symptoms That Always Need 999 or A&E
Whether you have a long-term condition or not, there are symptoms that require immediate action:
🫁 Breathing Problems
-
Severe breathlessness, even at rest
-
Struggling to speak or complete sentences
-
Gasping, wheezing, choking
-
Blue or grey lips, face, or fingertips
-
No response to inhalers or nebulisers
-
Sudden onset shortness of breath
❤️ Chest Pain or Heart Symptoms
-
Crushing or heavy chest pain
-
Pain radiating to jaw, neck, arms, or back
-
Palpitations + fainting, dizziness, or breathlessness
-
Fast or irregular heartbeat
-
Suspected heart attack or angina
🧠 Neurological Emergencies
-
Sudden weakness or numbness (especially on one side)
-
Slurred speech, facial droop, or confusion
-
Seizures or fits (especially if new or lasting >5 minutes)
-
Sudden, severe headache
-
Loss of consciousness or collapse
🌡️ Infection / Sepsis Signs
-
High fever with chills or rigors
-
Very fast breathing or heartbeat
-
Cold, mottled, clammy skin
-
Feeling very drowsy, confused, or unable to stay awake
-
Not passing urine or drinking
-
Feeling like something is seriously wrong
🩸 Bleeding or Trauma
-
Heavy bleeding that doesn’t stop
-
Major burns or deep wounds
-
Suspected broken bones
-
Head, neck, or spinal injury
-
Bleeding from eyes, genitals, or rectum
💊 Medication-Related Emergencies
-
Anaphylaxis: swelling, rash, shortness of breath, collapse
-
Adrenal crisis (especially in those on long-term steroids): vomiting, confusion, weakness, fainting
-
Severe side effects to antifungals or biologics: dizziness, liver pain, rash, yellowing skin
-
Sudden change in behaviour or mental state after a new medication
🧭 Not Sure? Here's What to Do
-
If you’re in doubt, but worried: Call NHS 111
-
If symptoms are severe, worsening, or causing distress: Call 999 or go to A&E
-
If you’re alone, unwell, and unsure — you are safer being checked
📘 Summary: When to Get Help Immediately
| Symptom Area | Emergency Signs |
|---|---|
| Aspergillosis-specific | Sudden breathlessness, new chest pain, coughing blood, fever, severe weakness, confusion |
| Breathing | Gasping, cyanosis, wheezing unrelieved by inhalers |
| Heart | Chest pain, palpitations with collapse, irregular pulse |
| Neurological | Stroke signs, seizures, new confusion, severe headache |
| Infection/Sepsis | High fever + confusion or fast breathing, cold mottled skin |
| Trauma/Bleeding | Uncontrolled bleeding, deep wounds, broken bones, burns |
| Medication-related | Anaphylaxis, adrenal crisis, severe side effects, sudden mental health change |
💬 Final Word
If you're experiencing any of these symptoms, this is not the time to post in a support group or wait to see how things go.
Please don’t delay — even if you’ve had difficult A&E experiences in the past. The risk of waiting is far greater than the discomfort of being seen.
You are never wasting anyone’s time by protecting your health or saving your life.
🌾 Dietary Fibre and Disease Prevention: Why We Need to Eat More Fibre
Fibre is no longer just about bowel regularity. Modern research shows that dietary fibre plays a fundamental role in overall health, immune regulation, and chronic disease prevention. Low-fibre diets are now being linked to a growing list of physical and mental health conditions, with multiple sclerosis (MS) among the most recent examples.
🔍 What Is Dietary Fibre?
Fibre is the indigestible part of plant-based foods that helps regulate digestion, supports beneficial gut bacteria, and contributes to metabolic and immune function. The two main types are:
- Soluble fibre: dissolves in water, forms a gel-like substance, and helps control blood sugar and cholesterol
- Insoluble fibre: adds bulk to stool and supports bowel regularity
🚨 How Much Fibre Do We Need?
- UK recommendation: 25–30g/day for adults
- Average intake: only around 18g/day
- This means most people are getting 25–40% less fibre than they need
🩺 Diseases Linked to Low Fibre Intake
A growing body of evidence links low-fibre diets to:
Digestive & Gastrointestinal Disorders
- Constipation
- Diverticular disease
- Haemorrhoids
- Irritable bowel syndrome (IBS)
Metabolic and Cardiovascular Diseases
- Type 2 diabetes (via insulin resistance and glucose spikes)
- Obesity (through reduced satiety and changes to the microbiome)
- High cholesterol
- Cardiovascular disease
Cancer
- Colorectal cancer risk is significantly reduced by high-fibre diets (especially cereal fibre)
Inflammatory & Autoimmune Conditions
- Multiple sclerosis (MS): recent research links gut microbial imbalance, worsened by low fibre, to inflammation and autoimmunity
- Inflammatory bowel disease (IBD): fibre can help regulate gut inflammation in some forms
- Rheumatoid arthritis and asthma: animal studies suggest protective roles
Brain and Mental Health
- Anxiety and depression: linked to gut-brain axis disruption when fibre is insufficient
- Neuroinflammation: fibre supports short-chain fatty acid production (e.g. butyrate), which helps reduce inflammation that affects brain and mood
🧬 Why Fibre Matters for the Gut Microbiome
Fibre is the main energy source for beneficial gut bacteria. These microbes ferment fibre into:
- Short-chain fatty acids (SCFAs) like butyrate, propionate, and acetate
- These SCFAs:
- Nourish the gut lining
- Modulate immune responses
- Reduce systemic inflammation
- Influence brain function via the gut–brain axis
Low fibre leads to:
- Less microbial diversity
- More pro-inflammatory bacteria
- Greater permeability of the gut wall ("leaky gut")
🥦 How to Increase Fibre Intake
🥣 Everyday Fibre-Rich Food Ideas
Here are some simple, everyday options to help boost your fibre intake, with estimated fibre content:
| Food Item | Approximate Fibre (g) per Serving |
|---|---|
| Muesli (40g serving with fruit & seeds) | 6–8g |
| Porridge oats (40g) | 4g |
| Wholemeal toast (2 slices) | 5–6g |
| Nut butter (1 tbsp) | 1–2g |
| Lentil or bean soup (1 bowl) | 7–10g |
| Chickpeas in salad (half cup) | 6g |
| Brown rice (1 cup cooked) | 3–4g |
| Quinoa (1 cup cooked) | 5g |
| Berries (1 cup) | 4–8g (depending on type) |
| Apple or pear (with skin) | 3–4g |
| Banana (medium) | 3g |
| Nuts or seeds (30g handful) | 2–4g |
| Air-popped popcorn (3 cups) | 3–4g |
🚫 Common Low-Fibre Foods
Many widely consumed foods contain very little or no dietary fibre, especially if they are highly processed or refined. Examples include:
| Food Item | Approximate Fibre (g) |
| White bread (2 slices) | 1g or less |
| White rice (1 cup cooked) | 0.5–1g |
| White pasta (1 cup cooked) | 1–2g |
| Processed breakfast cereals | 1–2g |
| Biscuits and cakes | <1g per portion |
| Ready meals (typical portion) | 1–2g |
| Crisps / potato chips (25g) | <1g |
| Soft drinks, fruit juice (250ml) | 0g |
| Cheese, meat, and eggs | 0g |
These low-fibre foods dominate many modern diets. Without mindful inclusion of whole plant foods, it is easy to fall well below the recommended fibre intake.
💡 Is It Easy to Reach the Target? These can be rotated across meals and snacks to easily reach your fibre goals without drastic changes.
⚖️ What If Fibre Causes Looser Bowels?
It's not uncommon for people to experience looser stools, more frequent bowel movements, or mild bloating when increasing fibre intake too quickly. This usually happens because:
- The gut bacteria are adjusting to more fermentable material
- Insoluble fibre speeds up gut transit time
The good news:
- These effects are usually temporary and settle within a few days to a couple of weeks
- You can achieve a happy medium by:
- Increasing fibre gradually over 1–2 weeks
- Including both soluble (e.g. oats, pulses, fruit) and insoluble (e.g. wholemeal bread, bran) fibre
- Drinking plenty of water
If symptoms continue, consult a GP or dietitian—especially if you have conditions like IBS or IBD that affect gut sensitivity.
✅ Summary
| Area of Health | Fibre Benefits |
| Gut & digestion | Regularity, reduced IBS/diverticulitis |
| Heart & metabolism | Lower cholesterol, improved glucose control, satiety |
| Immune system | Less inflammation, gut barrier protection |
| Mental health | Gut–brain axis modulation, reduced neuroinflammation |
| Cancer prevention | Lower colorectal cancer risk |
🌿 Special Note for People with Aspergillosis
If you are living with aspergillosis, especially chronic forms like CPA or ABPA, or regularly take medications such as antifungals, corticosteroids, or antibiotics, fibre is particularly important:
- Antibiotics can disrupt gut microbiota, reducing beneficial bacteria and fibre fermentation
- Steroids can impair immune regulation and blood sugar control, both of which benefit from high-fibre diets
- Antifungals and long-term illness may alter digestion or appetite, making a high-quality, fibre-rich diet even more essential
Maintaining a healthy gut environment through a fibre-rich diet may help support immunity, reduce inflammation, and improve resilience to infection and medication side effects.
📢 Final Note
Fibre is now a front-line defence against modern disease. It's one of the most underconsumed but powerful nutrients for preventing chronic illness, improving resilience, and nurturing a healthy gut microbiome.
Recent links to conditions like multiple sclerosis highlight just how far-reaching fibre’s impact may be—making it more than a digestive aid, but a foundation of systemic health.
💙 Disability Verification and Support for People with Aspergillosis in the UK
Living with aspergillosis—whether it's chronic pulmonary aspergillosis (CPA), allergic bronchopulmonary aspergillosis (ABPA), or another form—can have a significant impact on daily life. Many people find that fatigue, breathlessness, medication side effects, and other long-term symptoms affect their ability to work, care for themselves, or maintain independence.
If your condition is affecting your daily activities, you may be entitled to disability support, financial help, or adjustments at work or home. This guide explains how to get your disability recognised and verified in the UK, who can help, and how this varies across age groups and types of disability.
✅ What Counts as a Disability?
Under the Equality Act 2010, a person is classed as disabled if they have:
“A physical or mental impairment that has a substantial and long-term negative effect on their ability to carry out normal day-to-day activities.”
Many people with aspergillosis meet this definition—especially if they experience breathlessness, fatigue, pain, or recurrent infections over months or years.
📋 How Can You Prove or Verify Your Disability?
There is no single "disability certificate" in the UK. Instead, different systems accept different types of evidence, depending on what support you are applying for.
1. Benefit Award Letters
These are the most commonly accepted form of disability evidence:
- Personal Independence Payment (PIP)
- Disability Living Allowance (DLA) (for under 16s)
- Attendance Allowance (for over State Pension age)
- Employment and Support Allowance (ESA) (Support Group)
- Industrial Injuries Disablement Benefit
Where to get it: Contact the DWP or check your online account for a copy of your award letter.
2. NHS Medical Letters
Ask your GP or consultant to write a letter that:
- Confirms your diagnosis (e.g. CPA, ABPA)
- Describes the symptoms and how they affect your daily life
- Explains any treatments you need (e.g. antifungals, oxygen, steroids)
- States any long-term prognosis or care needs
3. Blue Badge and Disabled Bus Pass
- Blue Badge: Available from your local council for parking needs
- Disabled Bus Pass: Also issued locally; often requires proof of benefits or medical need
4. Occupational Therapy Assessment
- NHS or council-based OTs can assess your ability to manage daily tasks and recommend adaptations or support.
- Access via GP or Adult Social Care team.
5. Workplace or Education Support
- Occupational Health assessments may recommend reasonable adjustments such as flexible hours, remote work, or cleaner air environments.
- You may be eligible for Access to Work grants.
6. PIP and Other Benefit Assessments
- Assessments focus on how your condition affects daily tasks like mobility, personal care, medication management, and communication.
🔢 Do We Get a Disability Percentage?
In the UK, disability is not usually measured as a percentage. Most systems use functional assessments or point-based scoring.
The Exception: Industrial Injuries Disablement Benefit (IIDB)
- Uses a percentage system based on the extent of permanent disablement from a work-related condition.
For Everyone Else:
- PIP, DLA, and ESA use points-based systems.
- Employers, schools, and councils assess need based on impact, not percentage.
🡥 Who Can Help You with Disability Assessment?
| Professional / Service | Role & When to Use |
|---|---|
| GP or Specialist Consultant | Confirm diagnosis and functional impact for letters and forms |
| Occupational Therapist (NHS) | Assess your ability to manage daily tasks, recommend home aids/adaptations |
| Occupational Health (Work) | Recommend workplace adjustments under Equality Act |
| Adult Social Care (Council) | Assess for care support and home adaptation funding |
| Citizens Advice / Disability Charities | Help with forms, appeals, and understanding your rights |
| National Aspergillosis Centre (NAC) | May provide supporting letters for housing or benefits if you're under their care |
👶 Children and Young People
Under 16
- Claim Disability Living Allowance (DLA)
- Apply for an Education, Health and Care Plan (EHCP) if they have learning or developmental needs
- Get support from social care and school SENCOs
Age 16–25
- Transition to PIP for disability benefits
- EHCP can continue to age 25 if still in education
- Access workplace/education adjustments and Access to Work
- Shift from Children’s Services to Adult Social Care at 18
👵 Older Adults (Typically Age 65+)
Attendance Allowance
- For care needs only (not mobility)
- Not means-tested
Care and Support Needs
- Request a Care Act assessment from local council
- May result in home care, adaptations, or care home funding
NHS Continuing Healthcare
- For those with severe, complex needs
- Fully funded by NHS; not means-tested
Blue Badge Scheme
- Still accessible based on breathlessness or mobility limitation
Carer Support
- Carer's Assessment available
- Access to Carer’s Allowance or respite care
🧠 Mental Illness and Long-Term Invisible Disabilities
Mental health conditions and other non-visible disabilities (e.g. chronic fatigue, fibromyalgia, autism, long COVID) are also recognised under the Equality Act if they are long-term and impact daily life.
Differences in Assessment
- Focus is on non-physical activities:
- Planning and following journeys
- Managing therapy or medication
- Social interaction
- Decision-making
Key Evidence
- GP letters
- Psychiatrist or psychologist reports
- Occupational therapy or carer evidence
Support Services
- Community mental health teams (CMHT)
- Crisis teams, counselling, and talking therapies
- Supported housing or assisted living
Reasonable Adjustments
- Flexible schedules, quiet spaces, remote work
- Mental health support plans at school, university, or work
Advocacy
- Mind, Rethink, Disability Rights UK, and VoiceAbility provide advocacy, appeals help, and representation
📚 Summary Table
| Area | Physical Disabilities | Mental Health / Invisible Disability | Children | Older Adults |
| Benefit | PIP / ESA | PIP / ESA | DLA | Attendance Allowance |
| Social Care | Adult Social Care assessment | Adult Social Care or MH services | Children’s Services | Adult Social Care |
| Education/Work Support | Access to Work, OH reports | Access to Work, reasonable adjustments | EHCP, SENCO | Retirement/flexible options |
| Blue Badge | Based on mobility | Based on anxiety/severe distress for travel | May be available | Common for respiratory limits |
| Evidence Needed | Consultant, OT, GP | Psychiatrist, GP, carer, advocate | School or paediatric reports | GP, consultant, OT |
| Advocacy Support | Citizens Advice, Scope | Mind, Rethink, Disability Rights UK | IPSEA, Contact | Age UK, Carers UK |
🙏 Final Tips
- Keep copies of all letters, forms, and award notices.
- If your condition fluctuates, keep a symptom diary to show variable impact.
- Apply for assessments early as processes can take time.
- If you need help applying, speak to Citizens Advice or a local disability advocacy service.
- The National Aspergillosis Centre may be able to support patients with evidence for housing, benefit, or support applications.
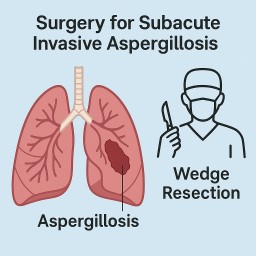
When Antifungals Fail: One Patient’s Recovery from Subacute Invasive Aspergillosis After Surgery
Subacute Invasive Aspergillosis (SAIA) is a rare and serious lung infection caused by the Aspergillus fungus. It often affects people who are immunocompromised—whether due to illness or medications like immunosuppressants—and typically sits between chronic and acute invasive forms in severity.
🧬 A Patient's Story from Australia
“I was diagnosed with SAIA after being treated with immunosuppressants for an autoimmune condition. Over seven months, I tried three different antifungal medications—but the infection persisted. I was still producing thick mucus and felt systemically unwell, almost like I had a constant infection running through me.
Four weeks ago, I underwent a wedge resection—a type of surgery where the affected part of my lung was removed. Since then, my symptoms have completely resolved. I’m no longer coughing or feeling septic.
My infectious diseases specialist plans to keep me on posaconazole for 12 months, with monthly galactomannan blood tests to catch any recurrence early.
I’ve found there’s very little published about surgery for SAIA, so I hope my experience might help others.”
🧪 What Is SAIA?
SAIA is a slowly progressive lung infection that develops over weeks to months. Unlike acute invasive aspergillosis, which moves quickly, SAIA often occurs in people with some degree of immune suppression but who aren’t completely immunocompromised.
It can present with:
-
Persistent cough
-
Low-grade fever
-
Fatigue
-
Mucus production
-
Progressive lung damage
Standard treatment involves long-term antifungal therapy, often with drugs like:
-
Itraconazole
-
Voriconazole
-
Posaconazole
But in some cases—like this patient’s—antifungal therapy alone isn’t enough.
🛠️ When Is Surgery Used for SAIA?
Surgery, including wedge resection, may be considered when:
-
Antifungal medications are not effective
-
The infection is localized to one part of the lung
-
There is persistent or worsening lung damage
-
Patients are fit enough to undergo surgery
🔍 What Does the Evidence Say?
Although not commonly performed, surgery for aspergillosis is documented in medical literature, especially in cases of:
-
Chronic pulmonary aspergillosis (CPA)
-
Fungal nodules
-
Subacute forms like SAIA
Key studies:
-
A U.S. study of >100,000 aspergillosis cases found that only 4.8% underwent surgery, usually for treatment failure or severe complications.
-
A Chinese study of 85 CPA patients showed a relapse rate of only 7% post-surgery, with most patients improving dramatically.
-
A UK case series described 30 patients having lung resections over 15 years, showing surgery is safe and effective when performed in experienced centres.
🔄 What Happens After Surgery?
Even after a successful resection, follow-up antifungal treatment is often continued to prevent recurrence. Monitoring usually includes:
-
Regular imaging (CT scans)
-
Galactomannan blood tests (to detect fungal components)
-
Symptom tracking
This is typically guided by a multidisciplinary team involving infectious diseases, respiratory, and thoracic surgery specialists.
🎯 Key Takeaways
-
SAIA is uncommon, and when antifungals fail, surgery can be life-changing.
-
Wedge resection is a lung-sparing procedure that removes just the infected portion, offering good outcomes when the disease is localised.
-
Ongoing antifungal therapy and monitoring are critical to long-term success.
-
Your story adds to a growing but still limited body of knowledge and may help inform future treatment decisions and encourage further research.
If you are a patient or clinician navigating SAIA and struggling with antifungal treatment, this story may offer hope—and a reminder that surgical options, though rarely needed, can be effective when used judiciously.
🧵 Why Am I Getting More “Plugs” This July?
A message for aspergillosis patients
July is often a time when people with aspergillosis feel a bit better — but sometimes, things don’t go quite to plan. If you’ve suddenly started getting more mucus “plugs” or are struggling to clear your chest, here are some possible reasons:
🔍 Common Reasons for More Mucus or Plugs in Summer
| Possible Cause | Why it might affect you now |
|---|---|
| Fungal spores are high | July and August bring very high outdoor levels of Aspergillus, Cladosporium, and other moulds – especially on dry, windy days or after cutting grass. These can trigger inflammation and more mucus. |
| Pollen season continues | Even though tree pollen has gone, grass, weed, and cereal pollen are still in the air. These can worsen symptoms for people with ABPA or asthma. |
| Humidity or storms | Sudden weather changes, humid air, or storms can make breathing more difficult and mucus harder to shift. Some people call this "thunderstorm asthma." |
| Air pollution (ozone) | Sunny weather increases ozone and air pollution – both can irritate your airways. |
| Low-level infection or flare-up | If your mucus is thicker, darker, or smells different, it might be a sign of a fungal or bacterial flare-up, even without a high temperature. |
| Hydration or medication changes | Less water, skipping nebulisers, or changes in routine can make mucus stickier. |
| Blocked sinuses | Post-nasal drip from fungal sinusitis can make it feel like mucus is always sitting in your throat or upper chest. |
✅ What You Can Do
-
Drink more fluids, especially warm water or squash
-
Use saline in your nebuliser to loosen thick mucus
-
Do your chest clearance exercises more often – flutter device, ACBT, or huffing
-
Don’t skip antifungals, inhalers, or mucolytics like carbocisteine
-
Consider a nasal rinse if your sinuses feel blocked
-
Keep windows closed on high spore or high pollen days
-
Speak to your team if things don’t settle – you may need a review or antibiotics
⚠️ When to Get Checked
-
You're coughing up yellow, green or brown mucus
-
Mucus smells bad or has blood in it
-
You feel more breathless or more tired
-
You’ve needed to increase your nebuliser use
💬 You're Not Alone
Many patients with aspergillosis get more mucus at this time of year — even when the sun’s out! Don’t assume it’s “just the weather.” Sometimes it’s a sign that your lungs or sinuses are reacting to invisible spores in the air.