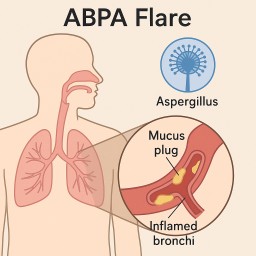
🌬️ When Breathlessness Gets Worse: Understanding What Might Be Happening
Many people with aspergillosis or ABPA (Allergic Bronchopulmonary Aspergillosis) find that their symptoms come and go — some days are better, some worse.
It can feel worrying when you suddenly become more breathless or wheezy, especially if you’ve been doing all the right things: airway clearance, antifungal treatment, and even starting a biologic injection.
This guide explains what might be happening and how you can begin to work out the cause.
💨 1. Why you might feel worse after airway clearance
Airway clearance helps move sticky mucus and plugs out of your lungs — but this can temporarily irritate or narrow the airways, especially if your chest is already inflamed.
You might feel tighter or more wheezy for a short time after a session.
Helpful tips
-
Use your bronchodilator (salbutamol or similar) before starting airway clearance.
-
Keep sessions short and gentle if you feel breathless afterward.
-
Talk to your respiratory physiotherapist about changing the timing or intensity of your airway clearance routine.
-
Nebulisers or inhalers after clearance can help calm things down again.
🧫 2. Could it mean the Aspergillus is becoming more active?
Sometimes it can — but not always.
Symptoms like breathlessness, cough, or fatigue can also be caused by inflammation, infection, or changes in medication.
Signs that might suggest Aspergillus activity is rising include:
-
More sputum, or thicker or darker plugs
-
More coughing or wheezing
-
Tiredness or mild fever
-
A drop in your usual lung function numbers (FEV₁)
These changes are only clues — to be sure, you need blood or sputum tests.
🧪 3. Tests that help you and your team understand what’s going on
| Test | What it shows |
|---|---|
| Total IgE | Rises when allergic inflammation is active (monitored every few months). |
| Aspergillus-specific IgE / IgG | Shows how strongly your immune system is reacting to the fungus. |
| Eosinophil count | Measures allergic immune activity (should fall if your biologic is working). |
| Aspergillus culture or PCR (sputum) | Shows whether fungal growth has increased or returned. |
| Antifungal drug level (itraconazole, voriconazole, etc.) | Confirms whether your medication is at a helpful level in your bloodstream. |
If you feel your symptoms are worsening, you can ask your GP or respiratory nurse if these blood tests can be arranged, even if your specialist clinic is hard to reach.
💉 4. When you’ve just started a biologic
Biologics such as Benralizumab, Mepolizumab, Omalizumab, or Dupilumab work by reducing inflammation in the lungs — but they take time.
What to expect
-
Most people don’t notice big changes after the first dose.
-
Benefits usually appear after 2–3 injections, sometimes longer.
-
You may start to notice less sputum, fewer wheezy days, and more energy over time.
If your breathing still feels difficult after a few doses, your team might review whether this biologic is the best one for you or whether something else is going on.
🧭 5. Keeping track between appointments
When clinic visits are months apart, self-monitoring helps fill the gap.
You can:
-
Keep a symptom diary — note breathlessness, cough, mucus colour, temperature, and how often you need rescue inhalers.
-
Record any oxygen readings if you use a pulse oximeter.
-
Note when you take antifungals and biologic injections.
-
Share this record at your next appointment — it helps your team see the bigger picture.
If you feel abandoned, remember you can still contact your hospital team or ask your GP for basic bloods. These can often be shared with your specialist for advice.
❤️ 6. When you feel alone
Many people with aspergillosis describe long stretches of “self-management.”
That’s why patient support networks (like NAC CARES) exist — to give you a space to talk, ask questions, and share what works.
No one should have to manage this alone.
🕊️ 7. Quick summary
| Possible reason for feeling worse | What you can do |
|---|---|
| Airway irritation after clearance | Use bronchodilator first; ask physio about technique |
| Inflammation or allergic flare | Ask for IgE and eosinophil tests |
| Antifungal not at right level | Ask for a blood level check |
| Early days of biologic treatment | Give it more time; track symptoms |
| Infection or fungal regrowth | Ask for sputum culture or PCR |
🌱 Remember:
Feeling worse doesn’t always mean you’re getting worse — but it’s always worth checking.
The right information (blood tests, drug levels, and a clear plan) can turn a worrying spell into a step forward.
Living Healthier with Aspergillosis: Small Steps That Can Make Life Easier

Living with aspergillosis, whether it is allergic bronchopulmonary aspergillosis (ABPA), chronic pulmonary aspergillosis (CPA), or another form, often means dealing with fatigue, coughing, breathlessness, repeated infections, and the side effects of treatment. Medicines such as antifungals and biologics are central to care, but everyday choices around food, activity, rest, and stress can also make a real difference.
This isn’t about strict rules or being told what you “should” do. It’s about finding small, realistic steps that help you feel stronger and more in control of daily life.
Why healthy habits can feel hard
Many people know what’s “healthy” but still find it difficult to change routines. That’s normal. Habits stick for lots of reasons:
-
Familiar routines feel safe, even if they’re unhelpful.
-
Stress, tiredness, or sadness can make comfort eating or smoking feel like a quick fix.
-
Friends, family, and culture shape our patterns.
-
Healthy food or exercise can seem expensive or time-consuming.
-
Mood and motivation play a huge part — especially if you’re already coping with illness.
Understanding why change is tough is the first step. You’re not failing — you’re human.
The potential benefits of living a little healthier
-
Easier breathing → avoiding smoke and doing gentle activity can help your lungs cope better.
-
Fewer flare-ups and infections → nourishing food, better sleep, and stress control support your immune system.
-
More energy → balanced eating and regular movement often boost stamina and reduce fatigue.
-
Treatments working better → some habits (like smoking or alcohol) interfere with antifungals; avoiding these can make medicines more effective.
-
Improved mood → routines such as exercise, cooking, or group activities can ease anxiety and give a sense of connection.
Diet and weight: it’s about health, not the scales
When weight feels like the focus
Many people are told to lose weight, but strict weight-loss diets rarely succeed in the long term. They can leave people frustrated or feeling worse. For aspergillosis, the aim is not chasing numbers on the scales — it’s about supporting your body so you can feel and function better.
Why diets often fail:
-
Cutting things out makes us crave them more.
-
The body resists weight loss by slowing metabolism.
-
Diets feel temporary, not sustainable.
-
One slip can feel like failure.
-
Stress and emotions drive food choices as much as hunger.
Breaking that cycle
Some people find it more helpful to:
-
Focus on health gains (more stamina, fewer infections, better mood) instead of weight loss.
-
Make small, sustainable swaps they can keep for years.
-
Add nourishing foods (protein, fruit, vegetables) instead of strict restriction.
-
Notice and celebrate everyday wins — walking further, coughing less, sleeping better.
When the struggle is keeping weight on
Not everyone has weight to lose. For some, infections, inflammation, and the effort of breathing can burn through calories, making it hard to maintain weight. In that case, the goal shifts to adding in extra energy and protein:
-
Eat smaller portions more often.
-
Fortify food with milk powder, cheese, cream, nut butters, or olive oil.
-
Keep calorie-rich snacks handy (flapjacks, trail mix, smoothies).
-
Try nutritional drinks (Fortisip, Ensure, or homemade shakes).
-
Ask your team for dietitian support if weight keeps dropping.
When to seek specialist help
General lifestyle tips are a useful starting point, but some people face severe or complex dietary problems. These can include:
-
Ongoing or severe weight loss / malnutrition
-
Difficulty swallowing or digesting food
-
Drug–food interactions (e.g. antifungals with certain juices or stomach acid medicines)
-
Other health conditions (diabetes, coeliac disease, kidney problems)
-
Persistent nausea, diarrhoea, or appetite loss from treatment
If this sounds familiar, the best step is to ask for a referral to a registered dietitian. A dietitian can:
-
Create a personalised nutrition plan to match your energy and protein needs
-
Suggest practical adjustments if eating is difficult
-
Ensure your plan is safe alongside antifungal or steroid treatment
-
Provide access to prescription nutritional supplements if needed
-
Monitor progress and adjust over time
What works for one patient may not be safe for another — professional advice ensures the plan is right for you.
Gut health and the microbiome
There’s growing interest in the link between the gut and the lungs — sometimes called the gut–lung axis. A healthy gut microbiome (the community of bacteria and other microbes in the digestive system) can support overall immunity and help regulate inflammation, which matters in conditions like ABPA and CPA.
-
Fibre feeds healthy gut bacteria → fruits, vegetables, oats, beans, and nuts help your gut produce anti-inflammatory compounds.
-
Probiotics (live “friendly bacteria” in yoghurts or supplements) may help some people, especially after antibiotics, but the evidence in aspergillosis is still limited.
-
Balance is key → too much fibre all at once can cause bloating; start gradually and pair fibre with calorie-rich foods if you struggle with weight.
-
Hydration matters → fibre works best when you’re drinking enough fluids.
-
Check before supplements → always discuss probiotic products with your team, especially if you are immunocompromised.
Small steps — like adding an extra piece of fruit or trying a yoghurt with live cultures — can gently support gut balance without overloading.
Starting small (and letting it grow)
Big lifestyle overhauls are rarely realistic. A more helpful approach is:
-
Pick one tiny change — a 10-minute walk, one less sugary drink, or a piece of fruit with breakfast.
-
Celebrate the success — each small step builds confidence and momentum.
-
Notice the ripple effect — walking more may improve sleep; better sleep may give more energy for cooking.
-
Climb the ladder slowly — the first step is hardest, but it makes the next ones easier.
Finding support
-
Share your goals with your medical team — they can suggest safe exercise, eating tips, or referrals.
-
Join pulmonary rehab, exercise groups, or online communities — peer encouragement makes a big difference.
-
Explore local schemes — social prescribing, community cooking, or walking groups can be free and welcoming.
-
Remember: mental health matters too. If low mood or anxiety makes change feel impossible, speaking with a GP or counsellor can help unlock progress.
The bottom line
Treatments like itraconazole and benralizumab are essential in controlling aspergillosis, but they work best when supported by healthy routines.
Living healthier means different things for different people:
-
For some, it’s cutting down alcohol or moving a little more.
-
For others, it’s eating enough to keep strength up.
-
For everyone, it’s about supporting your lungs, your body, your gut, and your wellbeing, not chasing numbers or perfection.
Even small, steady steps — chosen by you, at your pace — can add up to meaningful improvements and make daily life with aspergillosis a little easier.
Winter 2025–26: Flu & Other Respiratory Viruses. Bad Flu Season coming?
Information for people living with aspergillosis (ABPA, CPA and related conditions)
What the evidence says right now
Signals pointing to a tougher flu season
-
Southern Hemisphere “preview.” Australia saw higher-than-usual flu notifications in early 2025 compared with 2024, which often foreshadows a busier winter in the UK and Europe. That doesn’t guarantee the same for us, but it’s a warning sign. ausvaxsafety.org.au
- By September 2025 the numbers of cases in Australia had reached similar levels to those seen in 2024 www.health.gov.au
-
Co-circulation of viruses. In recent winters, influenza, RSV and COVID-19 have circulated together, increasing pressure on people at risk and on health services. WHO continues to flag this pattern in seasonal updates. World Health Organization
-
UK picture (late Sept 2025). UKHSA reports flu and COVID-19 at baseline/low levels for now. Activity can rise quickly as weather cools and schools/universities return. GOV.UK
-
Vaccine effectiveness (VE). Last season’s European interim VE against influenza A was ~32–53%, which is moderate—helpful at preventing severe illness and hospitalisation, especially in higher-risk groups. Effectiveness varies by age, strain and match. PMC
-
Timing. After Southern Hemisphere signals and based on past seasons, an earlier start (late Oct–Nov) with a Dec–Jan peak is plausible, though not certain. Local surveillance will confirm if that pattern emerges.
Why forecasts are uncertain (and what can improve outcomes)
-
Vaccine uptake. Higher uptake = smaller peaks and fewer hospitalisations. GOV.UK
-
Strain match. If circulating strains stay close to vaccine strains, protection is better; drift reduces it. PMC
-
Public behaviour. Ventilation, masks in crowded indoor spaces, and staying home when unwell still reduce spread. NHS Covid
-
Population immunity & health-system readiness. Recent infections and prior vaccines help; NHS readiness also matters.
What this means if you have aspergillosis
People with ABPA/CPA or bronchiectasis can have more severe or longer-lasting symptoms from flu, RSV, or COVID-19. Practical steps:
-
Get your vaccines when invited.
-
Act early if you become unwell.
-
Keep your baseline care tight.
-
Continue airway clearance, inhalers/other prescribed medicines, and your personalised action plan.
-
Ask about a rescue plan (who to call, when to test, when to increase treatments).
-
-
Reduce exposure where you can.
-
Improve ventilation, avoid poorly ventilated crowded spaces during peaks, consider masking indoors when rates rise, and hand hygiene.
-
Bottom line
-
Many experts anticipate a busier-than-average flu season in the UK/Europe this winter, but outcomes are not fixed. What we each do—vaccination, early help if ill, and sensible precautions—can make a big difference.
🧾 Vitamins & Minerals in Aspergillosis: What Patients Should Know
Living with aspergillosis (ABPA, CPA or other forms) and its treatments can affect your body’s levels of certain vitamins and minerals. Some of these nutrients are important for bone strength, energy, and the immune system.
But ⚠️ taking supplements without advice can be harmful. Always check with your doctor or specialist team before buying or using vitamins or minerals.
🌟 Common Deficiencies in Aspergillosis
1. Vitamin D & Calcium
-
Why important: Strong bones, healthy immune system.
-
Why low: Long-term steroids and less sunlight.
-
Problems if low: Weak bones, higher risk of fractures, tiredness.
-
⚠️ Too much can cause kidney damage — only take on medical advice.
2. Magnesium
-
Why important: Muscle strength, energy, nerve function.
-
Why low: Some antifungal or reflux medicines reduce levels.
-
Problems if low: Muscle cramps, weakness, tiredness.
-
⚠️ High doses can upset the heart and kidneys — medical supervision is essential.
3. Iron
-
Why important: Carries oxygen in the blood.
-
Why low: Chronic illness, poor appetite, blood loss.
-
Problems if low: Tiredness, breathlessness, pale skin.
-
⚠️ Aspergillus uses iron to grow — taking iron when you don’t need it can make infection worse.
4. Zinc
-
Why important: Healing, immunity, skin health.
-
Why low: Chronic illness or poor diet.
-
Problems if low: Slow wound healing, infections, taste changes.
-
⚠️ High zinc can block copper absorption and damage health.
5. B Vitamins (B12, Folate, B6)
-
Why important: Energy, blood health, nerve function.
-
Why low: Poor absorption, weight loss, some medicines.
-
Problems if low: Fatigue, pins and needles, anemia.
-
⚠️ Over-supplementation can also cause problems — needs testing first.
6. Vitamin A
-
Why important: Keeps lung lining healthy.
-
Why low: Poor diet, chronic illness.
-
Problems if low: Weaker lung defences, more infections.
-
⚠️ Too much vitamin A can be toxic (especially to the liver).
7. Vitamin K
-
Why important: Normal blood clotting.
-
Why low: Gut bacteria disruption from antibiotics/antifungals.
-
Problems if low: Easy bruising, bleeding gums, nosebleeds.
-
⚠️ Vitamin K can interfere with warfarin and other blood thinners.
🩺 Safe Steps for Patients
-
✅ Ask your doctor about vitamin D and calcium checks (especially if on steroids).
-
✅ Routine blood tests can check iron, B12, folate, magnesium, zinc.
-
✅ Take supplements only if prescribed — many interact with antifungal medicines.
-
✅ Don’t buy “high-dose” vitamins or minerals online or in shops without advice.
-
✅ Ask your team about a dietitian referral if you are struggling with appetite or weight.
-
✅ Bone scans (DEXA) may be needed to monitor steroid-related bone loss.
📌 Key message
People with aspergillosis are more likely to have low levels of vitamin D, calcium, magnesium, iron, zinc, and B vitamins.
These can affect your energy, bones, and immune system.
👉 Supplements can help — but only when checked, prescribed, and monitored by your healthcare team.
Steroid Use and Your Eyesight: What Patients Need to Know
Steroids (such as prednisolone, inhaled corticosteroids, eye drops, or steroid injections) are important medicines for conditions like asthma, allergic bronchopulmonary aspergillosis (ABPA), and other inflammatory illnesses. But they can also affect your eyesight — sometimes in subtle ways day-to-day, and sometimes with long-term risks.
This guide explains what may happen, why vision can fluctuate, and what you can do to protect your eyes.
How steroids can affect the eyes
-
Cataracts
Long-term steroids may cause a type of cataract at the back of the lens (posterior subcapsular). This can cause glare, blurred vision, or difficulty seeing in bright light. -
Glaucoma (raised eye pressure)
Steroids can increase pressure inside the eye, potentially damaging the optic nerve if untreated. This is more common with steroid eye drops, but tablets and inhalers can also contribute. -
Central Serous Retinopathy (CSR)
Fluid may build up under the retina, causing blurred or distorted central vision. Usually reversible when steroids are reduced or stopped, but it can recur. -
Blood sugar and fluid changes
Steroids raise blood sugar and shift body fluids. This can temporarily alter the eye lens, making vision sharper one day and blurrier the next. -
Delayed healing and infection risk
Steroids can make eye infections worse or delay healing after injury or surgery.
Why vision changes from day to day
Some patients notice that their glasses seem to “work” differently depending on their steroid dose. Reasons include:
-
Time of day: Vision may blur a few hours after taking a dose, when steroid levels peak.
-
Dose level: Higher doses cause more fluctuation; tapering can also make vision variable.
-
Delivery method:
-
Tablets: most likely to cause daily swings.
-
Eye drops: may raise eye pressure within hours.
-
Inhalers: usually small risk, unless high dose over many years.
-
-
Other factors in asthma/aspergillosis: Nebulisers, oxygen, antifungal medicines (like voriconazole), fatigue, and infections can all add to vision changes.
What patients can do
Day-to-day management
-
Drink plenty of water to help with fluid balance.
-
Eat regularly and limit sugary snacks to reduce blood sugar swings.
-
Use good lighting and take regular breaks from close work.
-
Try to take steroids at the same time each day for more predictable effects.
-
Keep a diary of when blurred vision happens in relation to your dose.
Eye care
-
Tell your optician and GP you are on long-term steroids.
-
Ask for regular eye checks (pressure and cataract screening every 6–12 months).
-
Don’t rush to buy new glasses if your prescription seems to keep changing — vision often settles once steroid doses stabilise.
-
Lubricating eye drops can help if dryness is a problem.
When to seek urgent help
-
Sudden or severe blurred vision
-
Dark spots, flashing lights, or distorted shapes
-
Eye pain, halos around lights, or redness
-
Rapid worsening of eyesight
These could be signs of glaucoma, cataract progression, or retinal changes and need prompt medical attention.
Key message
Not everyone on steroids will notice eyesight problems, but it is a well-recognised side effect. The changes are often temporary and reversible, especially the day-to-day fluctuations, but long-term use does carry risks.
By being aware, monitoring regularly, and working with both your doctor and optician, you can catch problems early and protect your sight.
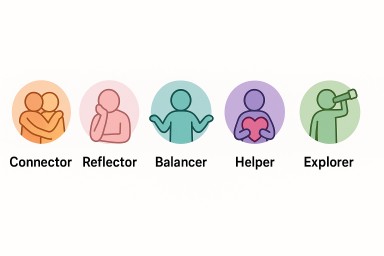
Personality, Connection, and Mental Health

Everyone has different ways of keeping emotionally balanced. Some people need lots of contact with others, while some need quiet time to recharge. Others feel best when they mix both. Recognising your “type” isn’t about putting yourself in a box — it’s about understanding what you need to stay well.
1. The Connector
-
How they thrive: by spending time with friends, family, or groups.
-
Mental health benefit: being around others boosts mood, reduces anxiety, and gives a sense of belonging.
-
Challenges: isolation or long stretches without company can lead to loneliness, low mood, or feeling cut off.
-
Helpful strategies:
-
Build regular contact into your week (calls, visits, online groups).
-
Explain to family/friends that contact isn’t a “nice extra” but an essential for your wellbeing.
-
Use support groups (like NAC CARES) to stay connected if health limits travel.
-
2. The Reflector
-
How they thrive: by having quiet, personal space to recharge after socialising.
-
Mental health benefit: time alone helps calm the nervous system, reduce stress, and spark creativity.
-
Challenges: may feel drained if pressured into constant social contact. Can appear “distant” to others when actually just recharging.
-
Helpful strategies:
-
Protect quiet time without guilt — see it as fuel, not selfishness.
-
Use calming practices (journaling, meditation, walks, hobbies).
-
Communicate with loved ones: “I need some downtime, then I’ll rejoin.”
-
3. The Balancer
-
How they thrive: with a healthy mix of both social contact and private time.
-
Mental health benefit: balance allows them to enjoy connection without becoming overstimulated.
-
Challenges: may tip too far one way — overbooking social time and burning out, or retreating too much and feeling lonely.
-
Helpful strategies:
-
Notice your signals — irritability might mean you need rest, loneliness means you need contact.
-
Plan weeks with both connection (calls, visits) and rest (quiet evenings, gentle hobbies).
-
4. The Helper
-
How they thrive: by supporting and caring for others. Helping gives meaning and boosts self-worth.
-
Mental health benefit: gives purpose and strengthens relationships.
-
Challenges: may neglect their own needs, leading to burnout or resentment.
-
Helpful strategies:
-
Follow the “oxygen mask rule” — you can only help others if you look after yourself.
-
Schedule self-care alongside care for others.
-
Accept help when offered — balance is key.
-
5. The Explorer
-
How they thrive: through novelty, discovery, and learning. They love trying new things, meeting new people, or exploring new ideas.
-
Mental health benefit: curiosity and new experiences can reduce boredom, lift mood, and spark resilience.
-
Challenges: chronic illness can limit physical adventures, which may feel like a loss of identity.
-
Helpful strategies:
-
Adapt “exploring” to your situation — online learning, virtual tours, new books or creative hobbies.
-
Set small, achievable challenges so you still get a sense of growth.
-
Why this matters for mental health
-
There is no “right” type. Each way of recharging is valid. Problems arise when we don’t recognise or honour our needs.
-
Stress comes when needs aren’t met. A Connector without contact feels lonely; a Reflector without quiet feels overwhelmed.
-
Self-awareness protects wellbeing. Knowing your type helps you explain your needs to family, friends, and even your healthcare team.
Key message for aspergillosis patients
Chronic illness can magnify these needs. Fatigue, isolation, or hospital visits may disrupt your usual coping style. Recognising whether you’re a Connector, Reflector, Balancer, Helper, or Explorer can guide you to the right kinds of support.
👉 In short: protect what restores you. Whether it’s people, quiet, balance, helping, or exploring, these are not luxuries — they are the building blocks of good mental health.
Grief and the Loss of Health in Aspergillosis
Understanding grief
Grief is usually thought of as the response to the death of a loved one, but it is more than that. Grief is the natural human reaction to any major loss — whether of a person, a role, a relationship, or one’s health.
For people living with aspergillosis, grief often arises not only from bereavement but also from the daily reality of lost health, independence, and certainty about the future. This type of grief is sometimes overlooked by others, yet it is just as valid and just as painful.
Bereavement grief vs. health-related grief
Grieving a loved one
When a person we love dies, the grief process involves:
-
Remembering and honouring the relationship.
-
Finding ways to carry that memory forward through photos, anniversaries, stories, or rituals.
-
Adjusting to life in their absence while keeping a continuing bond.
The work of bereavement grief is therefore about preserving connection to memory and integrating loss into our life story.
Grieving health
By contrast, grieving the loss of health is about adapting to change in the present and future:
-
Our body no longer works as it once did.
-
Activities and roles that defined us may no longer be possible.
-
Identity and self-image shift as illness reshapes daily life.
The task here is not to “hold on” to a memory, but to rebuild life around a new reality. Patients often grieve the loss of their “old self” — the person who could climb stairs, walk long distances, work, or join in family activities without limitation.
👉 Put simply:
-
Bereavement grief = finding ways to remember.
-
Health-related grief = finding ways to adapt.
Why health loss grief is particularly difficult
For people with aspergillosis (and other long-term conditions), this grief is uniquely challenging because:
-
The loss is ongoing – illness can fluctuate, relapse, or progress, so grief is re-triggered many times.
-
It is invisible – others may not see how devastating the loss of health feels, which adds loneliness.
-
It is about the self – we mourn not just someone else but the person we used to be.
-
It holds uncertainty – unlike death, health loss sits in a space between grief and hope, as treatments may stabilise or improve things, but may not restore the past.
How to adapt and live with health-related grief
1. Recognise it for what it is
-
Naming these feelings as grief helps reduce guilt and self-blame. You are not “weak” or “failing” — you are adjusting to a major life change.
2. Give space for feelings
-
Sadness, anger, frustration, and even envy are normal. Suppressing them often prolongs the pain.
3. Use safe outlets
-
Talk with others who understand — family, friends, support groups, or counsellors.
-
Write in a journal, make art, or use rituals (like lighting a candle or planting a tree) to symbolise change.
4. Maintain connection and meaning
-
Illness may limit old roles, but it does not erase identity. People often rediscover purpose through hobbies, creativity, peer support, or volunteering.
5. Focus on what’s possible now
-
Set small, realistic goals — e.g. walking to the garden, preparing a simple meal, joining a call.
-
Celebrate these achievements, rather than only comparing yourself to your old abilities.
6. Care for your body
-
Sleep, nutrition, and gentle movement (as tolerated) improve energy and resilience.
7. Seek professional support if needed
-
If grief leads to ongoing despair, anxiety, or hopelessness, ask your GP about counselling or NHS Talking Therapies. Support is available, and you don’t have to carry this alone.
Resources
UK-based
-
NHS Talking Therapies – free counselling/CBT for anxiety and depression.
-
MIND – support for mental health and loss.
-
Asthma + Lung UK – helpline and groups for lung disease.
-
Cruse Bereavement Support – guidance on grief that can apply to non-death losses.
-
NAC CARES (aspergillosis.org) – patient meetings, forums, and tailored educational resources.
International / Online
-
What’s Your Grief – blogs, courses, and podcasts on different types of grief.
-
The Mighty – online community sharing experiences of chronic illness and loss.
Books
-
How to Live Well with Chronic Pain and Illness – Toni Bernhard.
-
When the Body Says No – Gabor Maté.
-
On Grief and Grieving – Elisabeth Kübler-Ross & David Kessler.
Videos
-
Grieving with a Chronic Illness (YouTube).
-
Living with Loss: Navigating Grief in Chronic Illness (YouTube).
-
Letting Go of Grief and Guilt with Chronic Illness (YouTube).
Final message for patients
Grief from health loss is real, human, and normal. It is not about weakness, nor about giving up. It is about learning how to live differently — with compassion for yourself, space for your feelings, and courage to rebuild purpose in new ways.
While bereavement grief holds on to memory, health grief asks us to adapt. Both are valid, both are painful, and both can soften with time, support, and self-kindness.
👉 You are not alone — others with aspergillosis and chronic illness are walking the same path, and support is out there to help you carry it. 💙
Autumn 2025 COVID-19 Booster – What Aspergillosis Patients Need to Know
The UK Health Security Agency (UKHSA) has updated who will be offered the COVID-19 booster this autumn. The programme is now more limited than in 2024, so it’s important to know if you qualify.
Who will be offered the booster?
You can get a free COVID-19 booster this autumn if you are:
-
Aged 75 or over
-
Living in a care home for older adults
-
Aged 6 months or older and immunosuppressed
This is a change from 2024, when everyone aged 65+ and many other clinical risk groups were included.
What “immunosuppressed” means
Many people with aspergillosis fall into this category. You may be considered immunosuppressed if you are:
-
Taking systemic steroids for more than a month
-
Receiving biologic therapy or other immunomodulatory medication
-
Living with a condition that affects your immune system
-
Having had chemotherapy, radiotherapy, or a transplant
If you’re unsure whether this applies to you, check with your GP or hospital specialist.
Timing of the booster
-
Boosters are usually offered at least 6 months after your last dose, including the spring booster.
-
Even if you’ve never had a COVID-19 vaccine before, you can still get one this autumn if you are in one of the eligible groups.
Why this matters for aspergillosis patients
People with aspergillosis often have weaker lungs and higher risks from infections. If your immune system is also suppressed by medication or illness, COVID-19 can be more severe. The booster offers added protection during the winter months.
💙 Key advice:
-
If you are immunosuppressed or over 75, you should be offered the vaccine.
-
If you think you qualify but haven’t received an invitation, speak to your GP or specialist.
-
Don’t delay — protecting yourself against COVID-19 is especially important when living with aspergillosis.
📌 Full details from UKHSA: Who’s eligible for the 2025 COVID-19 vaccine or autumn booster
Inhaled Mycotoxins and Testing: What Patients Need to Know
Many patients ask about mould, mycotoxins, and private test panels — especially when symptoms overlap with conditions like aspergillosis, asthma, or MCAS (see glossary). The science is complex, and there’s a lot of misinformation online. Here’s what we know.
Can inhaled mycotoxins cause illness?
-
High exposure at work: In farming, animal feed, waste handling, or recycling, workers can breathe in dusts that contain fungal fragments and mycotoxins. At these levels, people may develop work-related asthma, cough, or “organic dust toxic syndrome.”
-
Homes and offices: Damp and mouldy buildings are consistently linked to worse asthma and respiratory symptoms. But experts (WHO, Institute of Medicine, CDC, MHRA) stress that it’s not just mycotoxins — spores, allergens, β-glucans, and bacteria all play a role.
-
Bottom line: Dampness and mould are unhealthy, but there’s limited proof that airborne mycotoxins alone at household levels cause chronic illness. The key intervention is always fixing damp and mould, improving ventilation, and managing lung conditions properly.
Why are private mycotoxin tests offered?
Despite the limited evidence, urine and blood “mycotoxin panels” are marketed by private labs (often in the US). They detect tiny traces of toxins that almost everyone has — mostly from food.
Why they exist:
-
People with real symptoms want answers, and commercial labs meet that demand.
-
It is technically possible to measure mycotoxins, even if the meaning is unclear.
-
Some alternative practitioners use them because patients want something tangible.
Why are these tests unreliable?
-
Everyone has some exposure – Sensitive tests will almost always find traces from normal diet, even in healthy people.
-
No agreed cut-offs – No international standards for what level in blood/urine is “safe” or “unsafe.”
-
Not validated for diagnosis – NHS, WHO, CDC, EMA do not accept these tests as diagnostic.
-
Can’t show source – They can’t distinguish whether the toxin came from food, dust, or infection.
-
Risk of unnecessary treatment – May push people toward costly, unproven therapies.
👉 Bottom line: A positive result usually reflects diet, not disease. That’s why NHS doctors don’t use these tests.
Why validation matters
For any medical test to be trusted, it must go through validation:
-
Analytical validation – does the test reliably measure what it claims?
-
Clinical validation – does it correctly identify people with the disease and exclude those without it?
-
Clinical utility – does it actually help doctors make better treatment decisions?
-
Regulatory approval – bodies like the MHRA (UK), FDA (US), and EMA (EU) ensure tests are safe and meaningful before routine use.
Without validation, a test can give results that look scientific but don’t guide care. That’s why the NHS doesn’t accept mycotoxin blood or urine testing — they haven’t been shown to make diagnoses more accurate or treatments more effective.
What if your mycotoxin test is positive, but you don’t live in a damp home?
This is very common.
-
Food is the main source: Mycotoxins are often found in grains, nuts, coffee, and dried fruit.
-
Exposure ≠ illness: A positive only shows contact, not harm.
-
No NHS role: Since the tests can’t separate harmless from harmful exposure, they aren’t used.
-
What matters most: If you’re unwell, validated NHS tests (CT scans, Aspergillus IgE/IgG, sputum cultures) guide proper diagnosis and treatment.
Foods that can contain mycotoxins
-
Aflatoxins – peanuts, maize, tree nuts, dried fruit, spices.
-
Ochratoxin A – coffee, dried fruit, wine, cereals.
-
Fumonisins, zearalenone, DON – maize, wheat, cereals.
-
Patulin – apples and apple juice.
-
Gliotoxin – made by Aspergillus fumigatus; occasionally found in mouldy cereals/silage, but mainly important when produced inside the body during invasive aspergillosis.
👉 In the UK/EU, foods are routinely monitored and regulated to keep levels very low.
What this means for patients
-
If you have aspergillosis or asthma, mould can worsen symptoms — but NHS doctors use validated tests, not private toxin panels.
-
If you feel unwell in a mouldy home, focus on fixing damp and talking to your GP or specialist.
-
A positive mycotoxin test without damp exposure almost always reflects normal diet.
-
Be cautious about spending money on unvalidated tests, which don’t change safe NHS treatment.
💙 Key message: Damp and mould can harm health, and sometimes mycotoxins are part of that story. But unvalidated mycotoxin blood/urine tests are unreliable and not used by the NHS. The safest approach is to fix damp, protect your lungs, and rely on NHS-approved diagnostics and treatments.
Glossary of Terms
-
WHO – World Health Organization, the UN’s global health authority.
-
CDC – Centers for Disease Control and Prevention, the main US public health body.
-
EMA – European Medicines Agency, which regulates medicines across the European Union.
-
MHRA – Medicines and Healthcare products Regulatory Agency, the UK body that regulates medicines and devices.
-
NHS – National Health Service, the publicly funded health system in the UK.
-
IgE / IgG – Immunoglobulin E and Immunoglobulin G, types of antibodies measured in blood tests to check for allergy or immune response.
-
CT scan – Computed Tomography scan, a detailed type of X-ray that shows cross-sections of the body.
-
MCAS – Mast Cell Activation Syndrome, a condition where mast cells release too many chemicals, causing allergic-type symptoms.
-
ABPA – Allergic Bronchopulmonary Aspergillosis, an allergic lung condition caused by reaction to Aspergillus.
-
CPA – Chronic Pulmonary Aspergillosis, a long-term fungal infection of the lungs caused by Aspergillus.
Voriconazole and Sun Sensitivity: What Patients Can Do
Voriconazole is an important antifungal, but it can make your skin much more sensitive to sunlight. Some people develop mild rashes, while others can get severe sunburn even after only a few minutes outdoors.
🌞 Protect your skin every day
-
High-factor sunscreen (SPF 50+) on all exposed skin, even in winter or cloudy weather.
-
Lip balm with SPF for lips, which are often affected.
-
Protective clothing: hats, long sleeves, UV-blocking fabrics if possible.
-
Avoid peak sun (11am–3pm) and try to stay in shade when outdoors.
👀 Watch your skin closely
-
Report any new rashes, blisters, lumps, or patches to your specialist team.
-
Regular skin checks may be offered if you are on long-term voriconazole.
💊 Medication review
-
If severe reactions develop, your doctors may:
-
Adjust the dose
-
Switch you to another antifungal (e.g. posaconazole, isavuconazole)
-
Add specialist dermatology follow-up
-
🚨 When to act fast
Seek medical advice urgently if you develop:
-
Blistering burns after short sun exposure
-
Painful or rapidly changing skin lesions
-
Any signs of infection in damaged skin
💙 Key message for patients: Sun sensitivity on voriconazole is common enough that everyone should take precautions. Don’t wait until your skin is badly affected — protect daily, and tell your team about any changes.