Building fitness with Aspergillosis
Last reviewed: 20 March 2026
Audience: Patients, carers, families, and non-specialists
Applies to: Allergic bronchopulmonary aspergillosis (ABPA), chronic pulmonary aspergillosis (CPA), Aspergillus bronchitis, severe asthma with fungal sensitisation (SAFS)
Why it feels so hard — and how to improve safely
Key points
- Feeling exhausted after activity is common in aspergillosis and does not mean you are failing.
- Breathlessness and fatigue are often due to lung changes, not just “lack of fitness”.
- Pushing too hard can make symptoms worse — pacing is essential.
- Small, steady increases in activity are more effective than big efforts.
- Respiratory physiotherapy can make a major difference.
- Some patients (e.g. with cavities or haemoptysis) need tailored, cautious approaches.
Why exercise feels so difficult
Many people with aspergillosis find that even simple activity can feel exhausting.
This is not just about fitness. It is often due to changes in how the lungs and body work, including:
- Inflamed or narrowed airways
- Mucus affecting airflow
- Reduced oxygen transfer
- Increased effort needed to breathe
In addition:
- Long-term illness can reduce muscle strength
- Treatments such as steroids may affect weight and energy
- Many people experience post-exertional fatigue (feeling worse after activity)
This means your body is working harder than it used to — even for everyday tasks.
Why “just doing more” can backfire
It is natural to think that pushing harder will improve fitness. However, in aspergillosis this often leads to a cycle:
- Doing too much on a “good day”
- Feeling exhausted afterwards
- Needing longer recovery
- Losing confidence
This is sometimes called a “boom and bust” cycle.
The goal is not to push harder — it is to build steadily and sustainably.
A safer way to build fitness
1. Find your baseline
Start with what you can do without feeling completely exhausted afterwards.
This may be much less than you expect — and that is normal.
2. Use the 70–80% rule
Only do about 70–80% of what you feel capable of.
This helps prevent setbacks and allows gradual improvement.
3. Break activity into smaller chunks
Short sessions (e.g. 10–15 minutes) with rest in between are often easier than one long effort.
4. Use breathing control
Pursed-lip breathing:
- Breathe in through your nose
- Breathe out slowly through pursed lips
This helps keep airways open and reduces breathlessness.
5. Add gentle strength work
Improving muscle strength can reduce breathlessness and improve stamina.
- Sit-to-stand from a chair
- Light squats (with support)
- Step-ups
Start small — 2–3 times per week is enough.
The role of respiratory physiotherapy
Respiratory physiotherapy can be one of the most helpful supports available.
A respiratory physiotherapist can help with:
- Breathing techniques to reduce breathlessness
- Airway clearance to manage mucus
- Tailored exercise plans at the right pace
- Confidence in what is safe to do
You may be offered this as pulmonary rehabilitation.
If you have not been referred, it is worth asking your GP or specialist team.
⚠️ Important safety advice (including bleeding risk)
Exercise is helpful for many people with aspergillosis — but it is not always appropriate to increase activity without guidance.
Be especially cautious if you have:
- Coughing up blood (haemoptysis) — current or recent
- An aspergilloma (fungal ball)
- Lung cavities
- A recent flare or worsening symptoms
Why this matters
In some forms of aspergillosis, blood vessels in the lungs can become fragile. Strain or increased pressure in the chest can increase the risk of bleeding.
When to stop and seek advice
- Coughing up blood (even small amounts)
- Sudden increase in breathlessness
- Chest pain or tightness
- Feeling significantly worse after activity
How to exercise more safely (if stable)
- Keep activity gentle and controlled
- Avoid heavy lifting or straining
- Avoid holding your breath during exertion
- Build activity gradually
If you are unsure, seek advice from your specialist team or a respiratory physiotherapist before increasing activity.
What progress really looks like
Improvement is rarely a straight line.
- Some days will be better than others
- Setbacks are common
- Progress may be slow but meaningful
This is normal in chronic lung conditions.
When to seek medical advice
Contact your healthcare team if you experience:
- New or worsening breathlessness
- Changes in cough or sputum
- Chest pain
- Coughing up blood
- Severe or persistent fatigue
Final message
Living with aspergillosis changes how your body responds to activity.
But improvement is possible — with the right approach.
Build slowly, pace yourself, and get the right support — especially from a respiratory physiotherapist.
In one sentence
Exercise can help — but it must be paced, personalised, and safe for your type of aspergillosis.
Author: Graham Atherton and ChatGPT draft support
For review by: National Aspergillosis Centre
Note: This article is for general information and does not replace medical advice.
Why Diagnosis Can Take Time — and Why You Are Not Alone
Last reviewed: 18 March 2026
Key points
- Long diagnostic journeys are common in many chronic and rare conditions—not just aspergillosis.
- Delays do not mean your symptoms were not real or important.
- Diagnosis often becomes clear over time, as patterns develop.
- Many patients go through similar experiences before reaching answers.
- Specialist centres play an important role when conditions are complex.
You are not alone in this
One of the most important things to understand is this:
Long and difficult diagnostic journeys are common—especially in chronic or complex illness.
Many people living with conditions such as chronic pulmonary aspergillosis (CPA) or allergic bronchopulmonary aspergillosis (ABPA) describe months or years of symptoms before a clear diagnosis was made.
This experience, while frustrating, is not unusual—and it does not mean your care has failed.
This happens in many conditions
Aspergillosis is not unique in this respect.
Similar diagnostic journeys are seen in:
- chronic lung diseases
- autoimmune conditions
- rare infections
- conditions with overlapping symptoms (e.g. fatigue syndromes)
In all of these, the same pattern often occurs:
- early symptoms are non-specific
- common conditions are treated first
- tests may initially be normal
- the true pattern only becomes clear over time
Why time helps diagnosis
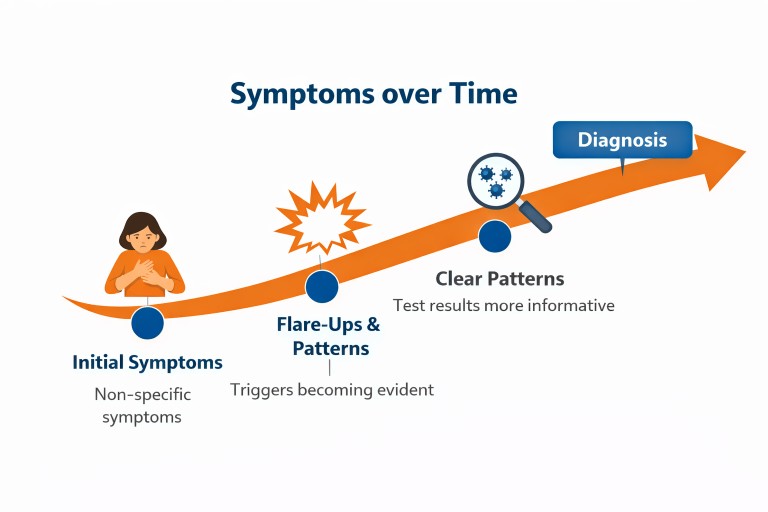
Although it can feel like delay, time often provides essential information.
Patterns emerge
- symptoms become more consistent
- flare-ups follow recognisable triggers
- response to treatment becomes clearer
Tests become more informative
- changes appear on imaging (e.g. CT scans)
- blood markers become more clearly abnormal
- microbiology results become more consistent
What was unclear early on can become much more visible later.
The turning point
Many patients describe a moment when things begin to change:
- symptoms no longer fit common conditions
- treatments stop working as expected
- a clinician recognises a pattern
This is often the point where less common diagnoses—including aspergillosis—are considered.
The role of specialist centres
Complex conditions are often best diagnosed in specialist centres with experience in that field.
In the UK, the National Aspergillosis Centre provides:
- expert multidisciplinary assessment
- access to specialist diagnostics
- experience in recognising patterns of disease
Referral to a specialist centre is often a key step in reaching a diagnosis.
The emotional impact
Long periods without answers can be deeply challenging.
Patients often describe:
- frustration and uncertainty
- feeling unheard or misunderstood
- loss of confidence in their own body
These reactions are entirely understandable.
Your experience is valid—even if the diagnosis took time to emerge.
Moving forward
Once a diagnosis is made, many patients feel a sense of relief—even if treatment is still needed.
A diagnosis provides:
- an explanation for symptoms
- a direction for treatment
- a clearer future plan
Even before diagnosis, it is important to remember:
You are still on a pathway—just not always a straight one.
Common questions
Does a long delay mean something was missed?
Not necessarily. Many conditions are only diagnosable once they have developed further.
Should I have been referred earlier?
Sometimes earlier referral is helpful, but it usually depends on how symptoms evolve over time.
Is this unique to aspergillosis?
No—this pattern is seen across many chronic and rare conditions.
Related pages
When Symptoms Are Real but Answers Are Not: Understanding Uncertainty
Last reviewed: 18 March 2026
Key points
- Many people experience a period where symptoms are real but no clear diagnosis has been made.
- This can sometimes feel like being told “nothing is wrong” or “it is all in your head”.
- In most cases, this reflects uncertainty in the system, not disbelief from clinicians.
- Conditions such as aspergillosis can take time to become recognisable.
- Physical and psychological factors can overlap—but unexplained symptoms are still real symptoms.
- Clear communication and ongoing review are key to moving forward.
The experience many patients describe
During a long diagnostic journey, many people reach a point where they hear phrases such as:
- “Your tests are normal”
- “We can’t find anything serious”
- “It may be stress or anxiety contributing”
Even when these words are carefully chosen, they can feel like:
“Nothing is wrong” or “it’s all in my head”
This can be one of the most difficult parts of the journey—especially when symptoms are ongoing, disruptive, and clearly real.
Why this happens
This situation usually reflects the limits of current medical systems rather than a lack of concern.
Tests do not always give clear answers
Modern medicine relies heavily on tests. But for many conditions—including chronic pulmonary aspergillosis (CPA)—tests may:
- be negative early on
- show unclear or borderline results
- require interpretation over time
This creates a gap between:
- what the patient is experiencing
- what can currently be measured
Medicine is designed to provide answers
Clinicians are trained to explain symptoms and reassure patients. When no clear diagnosis is available, they may turn to explanations such as:
- stress
- anxiety
- functional symptoms
These are real and valid factors—but if introduced too early, they can feel like the search has stopped.
Time pressure
Short consultations can mean:
- less time to explain uncertainty
- less opportunity to validate patient experience
- simplified explanations that lose nuance
What doctors mean vs what patients hear

Often, the issue is not what is said—but how it is understood.
| What may be said | What may be heard |
|---|---|
| “Your tests are normal” | “Nothing is wrong” |
| “We haven’t found a cause yet” | “There is no cause” |
| “Stress may be contributing” | “It’s all in your head” |
Understanding this gap can help both patients and clinicians move forward more constructively.
A critical clarification
Not having a diagnosis is not the same as not having a disease.
Unexplained symptoms are still real symptoms.
Medicine does not always have immediate answers—especially for conditions that develop slowly or do not fit standard patterns.
Physical and psychological overlap
It is important to take a balanced view.
- Physical illness can lead to anxiety, fatigue, and distress
- Anxiety can worsen physical symptoms such as breathlessness
This relationship is two-way, not either/or.
The problem arises when psychological explanations replace further investigation, rather than sitting alongside it.
Why this matters in aspergillosis
Conditions such as aspergillosis often:
- develop gradually
- have non-specific symptoms
- require multiple tests over time
This makes periods of uncertainty more likely, particularly before a diagnosis such as allergic bronchopulmonary aspergillosis (ABPA) or CPA is confirmed.
You can read more about this in Why Aspergillosis Is So Hard to Diagnose.
What patients can do
- Keep a record of symptoms and how they change over time
- Ask what the current working diagnosis is
- Ask when the situation should be reviewed
- Share concerns clearly, but remain open to different explanations
Helpful questions include:
- “What else could this be?”
- “What would make you reconsider the diagnosis?”
- “When should we review this again?”
A shared understanding
This situation is not about:
- patients being dismissed
- clinicians not caring
It reflects a deeper reality:
Medicine does not always have immediate answers—especially for complex or evolving conditions.
The goal is to keep the process open, respectful, and moving forward.
Common questions
Does this mean doctors think I’m imagining symptoms?
No. It usually reflects uncertainty rather than disbelief.
Can stress really affect physical symptoms?
Yes—but this should not stop appropriate medical investigation.
What should I do if I feel dismissed?
Ask for clarification, a review plan, or a second opinion if needed.
Related pages
Managing fatigue and energy in aspergillosis and allergic fungal lung disease
Key points
- Many people with aspergillus-related lung conditions experience extreme tiredness after physical or mental exertion.
- This fatigue can last hours or even several days.
- Breathing, immune activity, inflammation and sometimes hormone imbalance all use extra energy.
- Activity can temporarily increase airway inflammation and mucus.
- Managing energy carefully (“spoon theory”) can help prevent fatigue crashes.
Contents
- Why people with lung disease feel exhausted after exertion
- What is happening in the lungs and body
- Managing energy: the “spoon theory”
- Practical ways to manage energy
- Nutrition and adrenal health
- Warning signs you are running out of energy
- Why fatigue in lung disease is different from normal tiredness
- Daily energy management checklist
- Can this fatigue be treated?
- When to talk to your doctor
Why people with lung disease feel exhausted after exertion
Healthy lungs have a large reserve capacity. When we exercise or do physical work, breathing becomes deeper and faster, but the lungs can usually cope easily.
In people with aspergillosis or allergic airway disease, the airways may already be:
- inflamed
- narrowed
- filled with mucus
- sensitive to allergens such as Aspergillus fumigatus
When the body demands more oxygen during activity, the lungs must work much harder to supply it. Activities that seem minor to other people may therefore require much greater effort from the body.
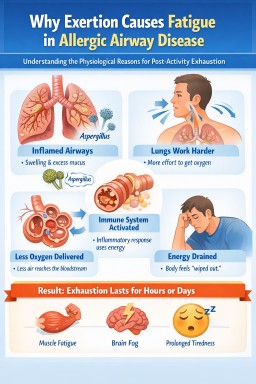
What is happening in the lungs and body?
Inflamed airways
Many aspergillus-related conditions involve inflammation in the airways. The immune system releases chemicals that cause:
- swelling of airway walls
- increased mucus production
- greater airway sensitivity
During exertion, breathing becomes faster and deeper, which can irritate these inflamed airways further.
Mucus affecting airflow
Inflamed airways often produce extra mucus. This mucus can partly block airflow and lead to:
- coughing
- wheezing
- breathlessness
- uneven airflow within the lungs
This may reduce how efficiently oxygen enters the bloodstream. Doctors sometimes refer to this as ventilation–perfusion mismatch.
Breathing uses more energy
In healthy people, breathing uses only a small fraction of the body's energy. In lung disease, breathing may require much more effort.
Additional muscles may assist breathing, including:
- chest muscles
- neck muscles
- shoulder muscles
These muscles can become fatigued during activity, just like leg muscles after exercise.
Immune system activity
If the immune system reacts to fungal proteins or allergens, it releases signalling chemicals called cytokines. These chemicals can produce symptoms similar to mild illness, including fatigue, brain fog and muscle aches.
Delayed inflammation after activity
Some people notice that fatigue appears later rather than immediately. Physical effort can trigger inflammation that develops over 12–48 hours, increasing mucus production, airway irritation and tiredness.
This explains why people sometimes feel worse the day after a busy day.
Managing energy: the “spoon theory”
Many people with chronic illness find it helpful to think about their energy using the idea of spoon theory.
In this idea:
- each spoon represents a small unit of energy
- you start the day with a limited number of spoons
- each activity uses some of those spoons
Because breathing and inflammation already use energy, people with lung disease may begin the day with fewer spoons available.
Example of spoon use
| Activity | Possible energy use |
|---|---|
| Getting dressed | 1 spoon |
| Showering | 2–3 spoons |
| Cooking a meal | 2 spoons |
| Doctor’s appointment | 3–4 spoons |
| Busy social day | Many spoons |
If too many spoons are used early in the day, the body may run out of energy, leading to exhaustion lasting hours or even days.
Practical ways to manage energy
Plan activities around your best time of day
| Time of day | Suggested activities |
|---|---|
| Morning | Errands or appointments |
| Midday | Light household tasks |
| Afternoon | Quieter activities |
| Evening | Rest and recovery |
Break tasks into smaller steps
Large tasks can overwhelm the lungs and muscles. Instead of doing everything at once:
- clean one room at a time
- cook in stages
- prepare things earlier in the day
Use the 50–70% rule
Try to stop activity when you reach about half to two-thirds of your limit. Stopping early often prevents the fatigue crash that can occur later.
Use breathing techniques
Pursed-lip breathing
- breathe in through your nose
- breathe out slowly through gently pursed lips
Rhythmic breathing
Match breathing with movement, for example when climbing stairs.
Keep mucus moving
Mucus increases the work of breathing. Helpful strategies include:
- airway clearance techniques
- staying well hydrated
- gentle movement
- using inhalers or nebulisers as prescribed
Maintain gentle regular activity
Although exertion can cause fatigue, complete inactivity can worsen the problem. Gentle activity such as walking or pulmonary rehabilitation exercises helps maintain muscle strength.
Protect sleep
- maintain a regular sleep routine
- clear mucus before bedtime if needed
- avoid heavy exertion late in the evening
Nutrition and adrenal health
Nutrition and energy
Good nutrition helps support energy levels. Helpful strategies include:
- eating regular meals
- including protein for muscle repair (eggs, fish, dairy, beans or nuts)
- eating complex carbohydrates for steady energy
- drinking enough fluids
Some people find that smaller, more frequent meals reduce breathlessness compared with large meals.
Important nutrients
- protein
- vitamin D
- iron
- B vitamins
Doctors may check for deficiencies if fatigue is severe.
Adrenal insufficiency
Some patients who have taken long-term steroid medications may develop adrenal insufficiency. The adrenal glands normally produce cortisol, which helps regulate energy and stress responses.
Symptoms may include:
- severe fatigue
- dizziness
- muscle weakness
- difficulty recovering after exertion
Patients with adrenal insufficiency usually take hydrocortisone replacement therapy and should follow their doctor’s advice carefully.
Warning signs you are running out of energy
- breathing becomes faster or more difficult
- increased coughing or mucus
- arms or legs feel heavy
- dizziness or weakness
- difficulty concentrating
- chest tightness or wheezing
When these warning signs appear, it is usually best to stop and rest before continuing.
Why fatigue in lung disease is different from normal tiredness
Fatigue in lung disease is not simply normal tiredness. Several factors occur at the same time:
- breathing requires more energy
- the immune system may be active
- oxygen exchange may be less efficient
- nutrition and hormone balance may influence recovery
Because of this combination, fatigue may appear suddenly and last longer than expected.
Daily energy management checklist
Pacing and activity
- spread activities across the day
- stop before exhaustion
- plan demanding tasks when energy is highest
- allow recovery time after busy days
Breathing and airway care
- use breathing techniques during exertion
- perform airway clearance if needed
- take inhalers or nebulisers as prescribed
- stay well hydrated
Nutrition and medication
- eat regular meals
- include protein for muscle strength
- take medications as prescribed
- follow sick-day rules if you have adrenal insufficiency
Sleep and recovery
- maintain a regular sleep routine
- clear mucus before bedtime
- rest when warning signs appear
Can this fatigue be treated?
Fatigue associated with aspergillosis, allergic fungal airway disease, or severe asthma can sometimes be improved when the underlying causes are treated. Because several different processes contribute to fatigue, treatment usually focuses on improving multiple factors rather than a single cure.
Treating airway inflammation
Inflammation in the airways is one of the major contributors to fatigue. When the airways are inflamed:
- breathing requires more effort
- mucus production increases
- oxygen exchange becomes less efficient
Treatments aimed at reducing airway inflammation may include:
- Inhaled corticosteroids – commonly used in asthma to reduce inflammation directly in the airways.
- Antifungal therapy – in some patients, reducing fungal growth can reduce immune activation and inflammation.
- Biologic therapies – newer treatments that target specific immune pathways involved in allergic and inflammatory lung disease.
Biologic treatments
Biologics are one of the most promising areas of treatment for severe asthma and allergic airway disease. These medications target specific parts of the immune system that drive inflammation.
| Biologic | Target | Effect |
|---|---|---|
| Omalizumab | IgE | Reduces allergic inflammation |
| Mepolizumab / Benralizumab | IL-5 pathway | Reduces eosinophilic inflammation |
| Dupilumab | IL-4 / IL-13 | Reduces type-2 inflammation |
| Tezepelumab | TSLP | Blocks upstream inflammatory signalling |
Some patients with conditions such as allergic bronchopulmonary aspergillosis (ABPA) or severe asthma report improvements in breathlessness, symptoms and overall energy levels when inflammation is better controlled.
Improving mucus clearance
Mucus in the airways increases the work of breathing and can contribute to fatigue. Strategies that may help include:
- airway clearance techniques
- physiotherapy
- maintaining good hydration
- using prescribed inhalers or nebulisers correctly
Treating other contributing factors
Fatigue can also be worsened by other health issues that are common in chronic lung disease, such as:
- iron deficiency
- vitamin deficiencies
- poor sleep
- adrenal insufficiency
- muscle deconditioning
Addressing these factors can sometimes improve overall energy levels.
Pulmonary rehabilitation
Pulmonary rehabilitation programmes combine exercise training, breathing techniques and education about pacing activities. These programmes can improve muscle efficiency and exercise tolerance, and many patients report reduced fatigue and improved quality of life.
Future treatments
Research into inflammatory lung diseases is advancing rapidly. New biologic drugs and other targeted therapies are being developed that may improve control of airway inflammation.
Researchers are also studying how the lung microbiome (bacteria and fungi living in the airways) influences inflammation. In the future, this may lead to more personalised treatments for patients with fungal-related lung disease.
Inflammatory fatigue
Researchers are increasingly recognising that chronic inflammatory diseases can cause a form of fatigue sometimes called “inflammatory fatigue.”
In these conditions, immune signalling chemicals released during inflammation can affect the brain and energy metabolism. Similar patterns of fatigue are seen in diseases such as rheumatoid arthritis and inflammatory bowel disease.
This may help explain why some treatments that reduce inflammation — including biologic therapies — can improve fatigue even when lung function measurements change only modestly.
Interrupting the fatigue cycle
Treatment aims to interrupt the cycle that can develop in chronic lung disease:
Airway inflammation
↓
Breathing requires more effort
↓
More energy used by respiratory muscles
↓
Immune system activity
↓
Reduced overall energy and fatigue
By improving airway inflammation, mucus clearance, muscle strength and overall health, many patients find their energy levels become more manageable.
When to talk to your doctor
Seek medical advice if:
- fatigue becomes progressively worse
- breathlessness increases
- new symptoms appear such as chest pain or coughing up blood
- fatigue prevents normal daily activities
A reassuring message
Many people with aspergillosis or allergic airway disease worry that exhaustion means their condition is worsening.
In most cases it reflects the extra energy required for breathing, inflammation and immune activity. Learning to pace activity can help people live more comfortably with chronic lung disease.
Author: National Aspergillosis Centre information team
Review: Clinical review recommended
Last reviewed: 2026
Does when I eat cause fat gain if I have adrenal insufficiency?
Many people with adrenal insufficiency worry that eating at the “wrong time” — especially later in the day — will automatically cause weight gain or “steroid belly”.
This is understandable, but it’s important to separate myths from what actually happens in the body.
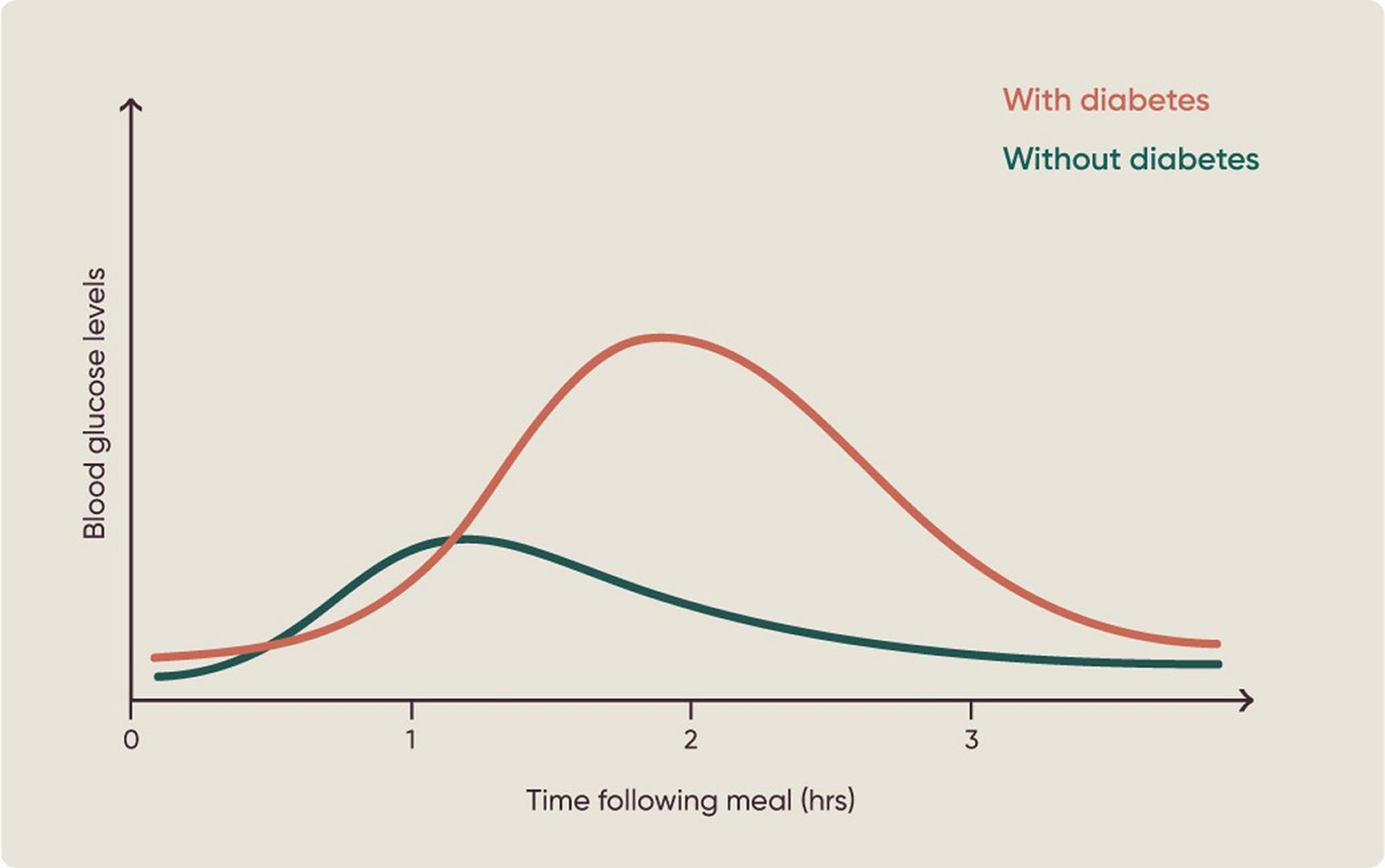

What doctors mean by “glucose response”
When clinicians or researchers talk about glucose response, they mean:
How your blood sugar rises and falls after eating
It does not mean that sugar is instantly being turned into fat.
A rise in blood glucose after eating is normal and happens in everyone.
Does eating later in the day automatically turn food into fat?
No.
Fat gain does not happen because of a single meal or snack — or because you ate at a particular time.
In most people:
-
Carbohydrates are first used for energy
-
Extra glucose is stored as glycogen in muscles and liver
-
Only repeated excess intake over time contributes to fat gain
Eating in the evening does not automatically cause fat storage.
Where insulin fits in (without the fear)
Eating raises blood glucose, which triggers insulin.
Insulin:
-
Helps move glucose into cells
-
Replenishes energy stores
-
Temporarily pauses fat burning
This pause is normal and reversible.
Insulin does not automatically create body fat.
Fat gain happens when:
-
Total calorie intake is consistently higher than needs
-
Steroid replacement is higher than required
-
This pattern continues over weeks or months
Why people with adrenal insufficiency feel confused about this
With adrenal insufficiency:
-
Cortisol replacement is taken in doses, not continuously
-
Symptoms, stress, poor sleep, or illness can affect appetite and energy
-
Some people are prone to low blood sugar, especially later in the day
Because of this:
-
Rigid food timing rules can make symptoms worse
-
Skipping meals or avoiding evening snacks can increase fatigue, dizziness, or night-time symptoms
A safer way to think about meal timing
Instead of strict rules, think in patterns:
-
Some people feel best with:
-
Larger meals earlier in the day
-
Lighter evenings
-
-
Others need:
-
A small evening snack
-
Protein or fat to keep blood sugar stable overnight
-
Both can be correct.
What matters most is:
-
How you feel
-
Whether your energy is stable
-
Whether sleep and symptoms improve
What usually matters more than timing
For people with adrenal insufficiency, weight changes are most often related to:
-
Total daily steroid dose
-
Repeated or prolonged stress dosing
-
Reduced activity due to illness or fatigue
-
Menopause, ageing, or other medical conditions
Food timing plays a much smaller role.
Key reassurance
If a food timing rule makes you feel worse, it is not the right rule for you.
-
A single glucose rise does not cause fat gain
-
Eating later does not automatically lead to weight gain
-
Safety, symptom control, and adequate steroid replacement come first
Please remember
Never change steroid dose or meal patterns intended to prevent hypoglycaemia without medical advice.
Underdosing steroids is far more dangerous than eating at the “wrong” time.
Take-home message
Focus on stability, nourishment, and feeling well — not fear of timing.
Hydrocortisone dosing in adrenal insufficiency
Why adrenal insufficiency can happen in people with aspergillosis
Many people with aspergillosis, particularly those with asthma-related conditions such as allergic bronchopulmonary aspergillosis (ABPA) or more severe chronic lung disease, need treatment with steroid medicines at some point. These treatments — often essential to control inflammation, protect the lungs, and improve breathing — may include repeated or long-term courses of steroids such as prednisolone.
When steroid treatment is used over time, it can reduce the body’s own production of cortisol by the adrenal glands. In some people, the adrenal glands do not fully recover, leading to adrenal insufficiency. Cortisol is a vital hormone that helps the body manage energy, illness, infection, and physical stress. When it cannot be made reliably, hydrocortisone replacement is needed to keep the body safe and functioning.
In this situation, hydrocortisone is prescribed to replace the cortisol your body can no longer make, usually after prednisolone has been reduced or stopped, or when prednisolone is no longer needed to control lung inflammation but adrenal support is still required.
Adrenal insufficiency in people with aspergillosis is not a failure and not something you have caused. It is a recognised consequence of necessary treatment for a serious, long-term condition. With the right information, a personalised dosing plan, and medical support, adrenal insufficiency can be managed safely alongside aspergillosis.
A patient guide to everyday (basal) dosing, higher-dose needs, and short-term stress dosing
If you take hydrocortisone because you have adrenal insufficiency, understanding how your dose works — both day to day and during illness or stress — is essential for your safety and wellbeing.
This guide explains:
-
What your basal (everyday) dose is for
-
Why some people need higher basal doses
-
When and how stress dosing is used — and why it is short term
-
Why some doctors may hesitate — and how to work safely with them
-
Where to find trusted patient and clinician resources
Very important first point ❗
Any changes to your hydrocortisone dose must be agreed in advance with a doctor or specialist nurse who knows your adrenal insufficiency.
This includes:
-
Your usual daily dose
-
Your stress-dosing (“sick day”) plan
-
Emergency injection instructions
This guide does not replace medical advice.
It is designed to help you understand your treatment and communicate clearly with healthcare professionals.
1) Your basal (everyday) hydrocortisone dose
What the basal dose is for
Your basal dose is the hydrocortisone you take on an ordinary day, when you are not ill or under unusual stress. Its purpose is to:
-
Replace the cortisol your body cannot make reliably
-
Support normal daily function (energy, blood pressure, mood)
-
Help your body feel stable and safe
-
Reduce the risk of chronic under-replacement
It is replacement, not treatment for inflammation.
A key point many patients are not told
Being consistently under-replaced does not help adrenal recovery.
Ongoing symptoms such as:
-
Constant exhaustion
-
Dizziness or nausea on standing
-
Brain fog or low mood
-
Poor tolerance of everyday stress
-
Frequent “crashes” or infections
can delay recovery, not speed it. Stability supports healing.
What doctors usually mean by a “physiological” dose
Most adults naturally produce the equivalent of about 15–25 mg of hydrocortisone per day.
Doctors aim for a dose in this range and adjust for:
-
Body size
-
Activity level
-
Other medical conditions
-
Individual response
This is replacement, not “high-dose steroids”.
How basal hydrocortisone is usually taken
To mimic the body’s natural rhythm, doses are often split:
-
A larger dose in the morning
-
Smaller doses later in the day
-
Avoiding late evening doses where possible
This supports:
-
Energy and blood pressure
-
Sleep
-
Mood and concentration
Signs your basal dose may be too low
Tell your doctor if you have persistent:
-
Severe fatigue despite rest
-
“Wired but empty” feeling
-
Dizziness, nausea, or salt craving
-
Poor concentration or memory
-
Low mood or anxiety
-
Frequent need for rescue or stress doses
These symptoms matter even if blood tests look reassuring.
Blood tests are only part of the picture
Cortisol and ACTH tests:
-
Help with diagnosis
-
Are less helpful for adjusting daily dose
-
Do not always reflect how well you function
Doctors experienced with adrenal insufficiency rely heavily on how you feel and cope day to day.
The right balance
Rather than “as low as possible,” a safer aim is:
Low enough to avoid overtreatment, but high enough to live a stable, functional life.
Living in constant deficit is not success.
2) When a higher basal dose may be appropriate
Some people with adrenal insufficiency — particularly those with chronic illness — may genuinely need a higher basal hydrocortisone dose (for example 25–30 mg/day).
This does not automatically mean overtreatment.
Well-recognised examples include:
Chronic inflammatory lung disease (including ABPA)
-
Ongoing airway inflammation and immune activation
-
Recurrent infective or inflammatory flares
-
The body may never be in a true “resting” state
-
Standard doses may leave patients under-replaced
-
A stable higher dose can reduce repeated stress dosing and improve daily function
Frequent infections or slow recovery
-
Repeated illness or prolonged recovery
-
Frequent “temporary” stress dosing just to cope with everyday life
Long-standing steroid-induced adrenal insufficiency
-
Years of prednisolone or similar treatment
-
Deep suppression of the adrenal system
Larger body size or higher metabolic demand
-
Cortisol needs vary with body size and activity
Autonomic symptoms or low blood pressure
-
Postural dizziness or faintness
-
Often benefit from a higher morning dose
Clinical clue:
If someone repeatedly needs stress dosing just to manage ordinary days, their basal dose may be too low for their current physiology.
Important reassurance
-
Higher basal doses can be appropriate, temporary, or longer-term
-
They do not automatically prevent recovery
-
Ongoing inflammation and repeated physiological stress suppress recovery more than adequate replacement
-
Doses should always be prescribed, documented, and reviewed
3) Stress dosing — when your body temporarily needs more
What stress dosing means
A healthy body automatically makes more cortisol during:
-
Illness or infection
-
Fever
-
Vomiting or diarrhoea
-
Injury or trauma
-
Severe pain
-
Surgery or medical procedures
-
Major physical stress
If you have adrenal insufficiency:
➡️ your body cannot do this, so doctors prescribe stress dosing in advance as part of your safety plan.
Stress dosing is essential — but it is short term
Stress dosing is meant to last only as long as the stress lasts.
It covers a temporary increase in need, not your everyday requirements.
What “short term” usually means
Stress dosing may last:
-
24–48 hours for minor illness or fever
-
Several days for infections or recovery from injury
-
During and immediately after surgery or procedures
Your doctor should advise:
-
When to increase
-
How much to increase
-
When and how to return to your usual dose
Why stress dosing should not continue indefinitely
If higher doses are needed for longer, something usually needs review:
-
Infection or inflammation has not settled
-
The basal dose may be too low
-
Another medical problem is present
If stress dosing is still needed after the original stress has passed, it’s time to talk to your doctor.
Stepping back down safely
-
Doctors usually advise returning to baseline
-
Sometimes a 1–2 day step-down is used
-
You should not remain on stress doses “just in case”
Stress dosing does NOT:
-
Stop adrenal recovery
-
Mean you are “failing”
-
Cause long-term harm when used correctly
Not stress dosing can:
-
Make you seriously unwell
-
Delay recovery
-
Lead to adrenal crisis


4) Why some doctors seem hesitant
Doctors outside endocrinology (GPs, A&E, ward teams):
-
Are trained to minimise steroid use
-
Often think of steroids only as anti-inflammatory drugs
-
May rarely manage adrenal insufficiency
What they may not realise immediately:
Your hydrocortisone is replacing a missing hormone — it is essential, not extra.
5) How to advocate safely (with medical backing)
It is appropriate to say:
“I have adrenal insufficiency. My doctor has advised stress dosing during illness to prevent adrenal crisis.”
If you have them, show:
-
Your Steroid Emergency Card
-
A written stress-dosing plan
-
A clinic letter or summary
6) Trusted resources & further support (with links)
The following organisations provide reliable, clinician-endorsed information on adrenal insufficiency, hydrocortisone replacement, stress dosing, and emergency care.
They are widely recognised by NHS endocrinology teams and safe to share with patients, families, and healthcare professionals.
UK patient and professional resources
Addison’s Disease Self-Help Group (ADSHG)
Website: https://www.addisonsdisease.org.uk
What it offers:
-
Clear explanations of basal vs stress dosing
-
Patient-friendly sick-day rules
-
Emergency hydrocortisone injection guidance
-
Downloadable patient leaflets used in NHS clinics
-
Webinars, helpline, and peer support
Why it’s useful:
ADSHG explicitly supports individualised dosing and crisis prevention.
Society for Endocrinology
Steroid Emergency Card & adrenal crisis guidance:
https://www.endocrinology.org/clinical-practice/steroid-emergency-card/
Why it’s useful:
-
Highly trusted by doctors, A&E, and ward teams
-
Clear professional wording that reassures non-specialists
-
Supports rapid decision-making in emergencies
NHS (England)
Steroid Emergency Card information:
https://www.nhs.uk/conditions/steroid-emergency-card/
Why it’s useful:
-
Official NHS backing
-
Useful for legitimacy in emergency or inpatient settings
International patient resources (useful supplements)
Endocrine Society
Patient information on adrenal insufficiency:
https://www.endocrine.org/patient-engagement/endocrine-library/adrenal-insufficiency
Why it’s useful:
-
Clear explanations of cortisol physiology
-
Conservative, authoritative tone
-
Helpful for patients seeking international consensus
National Adrenal Diseases Foundation (NADF)
Website: https://www.nadf.us
What it offers:
-
Practical sick-day rules
-
Emergency preparedness guidance
-
Injection training resources
Particularly helpful for patients with long-standing adrenal insufficiency or frequent illness.
Resources especially relevant for ABPA & chronic lung disease
National Aspergillosis Centre
Website: https://mft.nhs.uk/wythenshawe/services/infectious-diseases/national-aspergillosis-centre/
Why it’s relevant:
-
Specialist centre where ABPA and adrenal insufficiency often overlap
-
Supports personalised care plans in complex disease
Aspergillosis Trust
Website: https://www.aspergillosistrust.org
Why it’s useful:
-
Patient-focused education and advocacy
-
Helps explain the chronic physiological stress of ABPA
-
Supports conversations about higher basal hydrocortisone needs
Quick-access patient checklist (phone / wallet)
Patients are encouraged to keep:
-
Steroid Emergency Card
-
Sick-day rules (ADSHG)
-
Personal stress-dosing plan (agreed with doctor)
-
Clinic letter or summary
Many patients keep photos of these documents on their phone for emergencies.
Final reassurance
These resources support — not replace — medical advice.
They exist to help patients stay safe, informed, and confident when managing hydrocortisone and communicating with healthcare professionals.
**Pain Perception and Aspergillosis:
Why It Matters — and What Help Is Available**
Living with aspergillosis—whether Chronic Pulmonary Aspergillosis (CPA), Allergic Bronchopulmonary Aspergillosis (ABPA), Aspergillus bronchitis, or Severe Asthma with Fungal Sensitivity (SAFS)—can mean coping with symptoms that change day to day.
Pain, breathlessness, muscle aches, fatigue and joint discomfort are common. What many people don’t realise is that how the body perceives and processes pain plays a major role in how these symptoms feel — and how well they can be managed.
Understanding pain perception doesn’t mean your symptoms aren’t real. It means understanding why pain behaves the way it does in chronic illness — and how to gain more control.
1. Why pain perception matters in aspergillosis
Pain is produced by the nervous system, and is influenced by:
-
Inflammation in the lungs or sinuses
-
Muscle strain from coughing or altered breathing
-
Reduced fitness after flare-ups
-
Long-term corticosteroid use
-
Adrenal insufficiency
-
Stress, uncertainty, poor sleep, and emotional load
Pain is therefore a mix of bodily changes and how the brain interprets signals.
Both are real. Both deserve attention.
2. Muscle changes and increased sensitivity
People with aspergillosis may experience:
-
Weakened rib, back, and shoulder muscles
-
Reduced leg strength
-
Joint instability
-
Muscle fatigue leading to higher pain sensitivity
Everyday movements can feel more painful, and pain can worsen breathlessness. Many people fall into a cycle: flare-up → rest → muscle weakening → more pain → more breathlessness → more rest.
Understanding this cycle helps break it.
3. Stress, sleep and emotions influence pain
Pain becomes stronger when:
-
You are tired
-
You feel anxious, unsafe, or overwhelmed
-
Your symptoms are unpredictable
-
You have recently been in hospital
-
You are caring for someone who is unwell
This does not mean pain is psychological.
It means the nervous system becomes more alert, so signals feel louder.
Carers experience this too.
4. Why understanding pain helps you manage symptoms
Learning about pain perception helps you:
-
Pace activity wisely
-
Avoid panic when symptoms spike
-
Identify muscular vs inflammatory discomfort
-
Communicate clearly with clinicians
-
Reduce stress-driven symptom amplification
-
Prevent flare-ups by calming the nervous system
It’s not about ignoring symptoms — it’s about understanding them so you can respond safely and confidently.
5. NHS resources that can help
Below are useful links recommended across NHS pain services.
🔹 NHS self-help guidance on long-term pain
These pages offer practical advice on managing persistent pain, pacing, movement, and everyday strategies:
How to get NHS help for your pain
https://www.nhs.uk/live-well/pain/how-to-get-nhs-help-for-your-pain/
10 ways to reduce pain
https://www.nhs.uk/live-well/pain/10-ways-to-ease-pain/
These guides are suitable for people with chest pain, muscular pain, fatigue and inflammation linked to lung disease.
🔹 NHS Pain Management Programmes (PMP)
Many NHS Trusts run Pain Management Programmes. These provide a combination of physiotherapy, psychology, pacing education, flare-up planning, and medication review.
Examples of NHS PMP resources:
Royal Orthopaedic Hospital – PMP information
https://roh.nhs.uk/services-information/pain-management/pain-management-programme
Ashford & St Peter’s Hospitals – Pain Management Programme
https://www.ashfordstpeters.nhs.uk/the-pain-management-programme
Gloucestershire Hospitals – Pain Management Options
https://www.gloshospitals.nhs.uk/our-services/services-we-offer/pain-management-service/management-options-pain/
Speak to your GP or specialist team if you want a referral.
🔹 The Pain Toolkit (NHS-endorsed self-management booklet)
Widely used by NHS pain services and physiotherapy teams.
PDF:
https://www.nhsfife.org/media/c349s6xo/nhs-fife-pain-toolkit.pdf
This guide covers pacing, flare-up planning, problem-solving, emotional wellbeing and shared decision-making.
🔹 NHS Talking Therapies (for stress-related pain amplification)
If stress, anxiety or sleep disturbance are worsening your pain, NHS Talking Therapies services can help.
Find your local service here:
https://www.nhs.uk/service-search/mental-health/find-a-psychological-therapies-service/
These services support people with long-term physical conditions as well as mood and anxiety problems.
🔹 Physiotherapy & pulmonary rehabilitation
These services help with:
-
Breathing pattern retraining
-
Strengthening ribs, shoulders, back, hips, and knees
-
Improving stamina and reducing breathlessness
-
Reducing muscle pain and improving posture
Ask your GP, respiratory consultant, or specialist nurse for a referral.
6. What patients and carers can start today
✔ Notice pain patterns
Track fatigue, sleep, activity, stress, and symptoms.
✔ Practice pacing
Spread tasks through the day. Avoid pushing hard on “good days” — it often leads to flare-ups.
✔ Gentle strengthening
Even small daily exercises protect joints, support breathing and lower pain sensitivity.
✔ Reduce nervous-system overload
Breathing exercises, grounding, relaxation and mindfulness calm the system that amplifies pain.
✔ Seek help early
If pain changes or worries you, involve your GP or specialist team.
✔ Carers: protect your wellbeing
Carers benefit from pacing, strengthening and psychological support just as much as patients.
7. When to seek medical review
Contact your GP or specialist team urgently if you experience:
-
Sudden new chest pain
-
Pain with fever or coughing up blood
-
Pain that stops you breathing normally
-
Severe muscle weakness
-
Persistent flare-ups despite treatment
-
Symptoms suggesting adrenal problems
Pain in aspergillosis is real, but also manageable. With the right understanding and NHS-supported tools, you can reduce flare-ups, regain confidence, and improve daily life.
Why do some people with aspergillosis lose weight on the hips and thighs, but gain around the waist?
Many people living with aspergillosis, bronchiectasis or ABPA notice their body shape changing as they get older — especially after 60.
A very common pattern is:
-
Thinner hips and legs
-
More weight around the waist or tummy
This can feel confusing, but there are clear reasons why it happens.
1. Chronic lung conditions make it harder to keep leg and hip muscle
When you live with a long-term lung condition, you often have:
-
Breathlessness
-
Fatigue
-
Repeated chest infections
-
Less ability to walk long distances or climb stairs
Because the legs work harder than any other muscles, they are the first to lose strength and size when activity drops.
This is why many people notice:
-
Slimmer thighs
-
Smaller hips
-
Feeling weaker when getting out of a chair
This is partly due to age, but it happens faster in people with chronic lung disease.
2. Steroids can move weight from the limbs to the waist
Many aspergillosis patients have had:
-
Several courses of prednisolone over the years
-
High-dose inhaled steroids
-
Hydrocortisone replacement for adrenal problems
Even short or occasional courses can cause fat redistribution, where:
-
Fat and muscle reduce in the arms, hips and legs
-
More fat settles around the stomach area
-
The centre of the body becomes rounder even if the overall weight hasn’t changed much
This effect can continue long after stopping steroids.
3. Ageing naturally shifts fat towards the waist
After about age 60, the body changes how it stores fat:
-
Less around the hips and thighs
-
More around the waist
-
More “internal” fat around organs (visceral fat)
This happens to everyone, but can be more noticeable in people with aspergillosis because illness already reduces leg muscle.
4. You can lose muscle even if weight on the scales stays the same
Many patients say,
“I feel thinner and thicker at the same time.”
That’s because:
-
Muscle in the legs may be lost
-
Fat around the waist may increase
-
The total body weight doesn’t always change much
This is a normal pattern in long-term lung disease.
5. Illness, flare-ups, infections and poor appetite add to this
During flare-ups or infections, it’s common to:
-
Eat less
-
Feel exhausted
-
Lose muscle faster
-
Keep or gain tummy fat
The body burns muscle first when unwell, not fat — especially not tummy fat.
Is this dangerous?
Not usually on its own — but it does mean:
-
Legs may feel weaker
-
Balance and stamina can reduce
-
It may be harder to stay active
Strength and gentle exercise (within your limits) can help rebuild some leg muscle.
If weight changes are sudden or unexplained, they should always be discussed with your GP or specialist.
In summary
This body-shape change is very common in people with aspergillosis over 60.
It’s caused by a combination of:
-
Reduced activity due to breathlessness
-
Loss of leg and hip muscle
-
Steroid effects on fat distribution
-
Natural age-related changes
-
Appetite changes during illness
It doesn’t mean you’re doing anything wrong — it’s simply a pattern seen in many people with long-term lung disease.
FINDING COMFORT & PURPOSE ON LOW-ENERGY DAYS
A Gentle, Resource-Rich Handbook for Aspergillosis, Asthma, Bronchiectasis & COPD Patients
Many people living with aspergillosis (ABPA/CPA), asthma, bronchiectasis and COPD experience unpredictable energy levels, breathlessness, coughing, pain, flare-ups, treatment effects and fatigue.
On these days, large tasks feel impossible — but gentle activities can still offer comfort, focus, pleasure and calm.
This handbook brings together low-energy, low-breathing-demand hobbies and micro-activities, with recommended resources for every ability and symptom level.
Table of Contents
- 1. Understanding Fluctuating Energy
- 2. Creative Hobbies (with resources)
- 3. Music, Singing & Breath-Friendly Voice Work
- 4. Gentle Movement
- 5. Quiet Mind–Body Practices
- 6. Low-Effort Cognitive Hobbies (Puzzles & Jigsaws)
- 7. Social Connection (Low-Energy Options)
- 8. Good / Medium / Bad Day Plans
- 9. When Rest Is the Right Choice
- 10. Final Thoughts
1. Understanding Fluctuating Energy & Breathlessness
Living with lung disease means your available energy changes daily. You may move between:
-
Good days (stable breathing, clearer head)
-
Medium days (ok but fragile)
-
Bad days (breathless, fatigued, flaring, coughing)
This is normal.
Helpful Resources
-
The Spoon Theory by Christine Miserandino
-
The Energy Envelope approach – ME Association
-
NHS Lothian – “Managing Breathlessness”
-
NAC Facebook Community – patient-to-patient pacing strategies
2. Creative Hobbies (All low-energy & breath-friendly)
Creativity calms the mind without increasing breathlessness. Most activities below can be done sitting or reclining.
🎨 Watercolour Painting
Why it helps: slow movements, calming colours, short bursts (5–10 min), easy to pause.
Beginner Tutorials (YouTube)
-
Sarah Burns Studio – gentle landscapes
-
Steven Cronin – skies & mist
-
Watercolor Misfit – textures, blending
-
Liron Yanconsky – excellent for beginners
Materials
-
100% cotton paper: Etchr, Saunders Waterford, Arches
-
Paints: Winsor & Newton Cotman, Daniel Smith
-
Brushes: Da Vinci / Escoda size 6–8 round + 1" flat
✏️ Drawing & Colouring
Resources
-
Colouring apps: Lake, Pigment, Happy Color
-
Colouring books: Johanna Basford, Millie Marotta
-
Drawing tutorials: Draw With Shiba, Art for Kids Hub
Materials
-
Staedtler Noris pencils
-
Faber-Castell Polychromos
-
Smooth sketchpad
-
Sakura Micron pens
💻 Digital Art
Apps
-
Procreate / Procreate Pocket
-
Ibis Paint X
-
Sketchbook (free)
Tutorials
-
Bardot Brush (digital watercolour)
-
Stayf Draws
-
Genevieve’s Design Studio
🧵 Crafts (very low breath demand)
Knitting, crochet, loom bands, origami, scrapbooking.
Tutorials
-
Bella Coco Crochet
-
VeryPink Knits
-
Jo Nakashima (origami)
Beginner Kits
-
Hobbycraft
-
Etsy
-
The Works
📝 Writing, Journalling, Story Snippets
Apps
-
Day One
-
Penzu
-
Bear Notes
-
Gratitude App
Prompt Sources
-
Pinterest: “Journal prompts chronic illness”
-
Reddit r/Journaling
3. Music, Singing & Breath-Friendly Voice Work
Music is deeply calming and very compatible with breathlessness.
🎧 Listening to Music
Playlists (Spotify)
-
Peaceful Piano
-
Lo-Fi Beats
-
Deep Focus
-
Calming Acoustic
-
Rain Sounds / Ocean Waves
YouTube Channels
-
Ambient World
-
Nature Healing Society
-
Lofi Girl
🎤 Gentle Singing (VERY breath-friendly)
Guided Sessions
-
Singing for Lung Health – British Lung Foundation
-
Sidcot Singing for Breathing (YouTube)
-
Breath-Supported Vocal Warmups – Carolyn Grace Music
Why it's helpful
-
controls exhale
-
relaxes throat
-
reduces panic around breathlessness
😌 Humming
One of the most effective breathing tools:
-
lengthens exhale
-
improves nasal airflow
-
calms upper airway
-
reduces anxiety
🎶 Breathing With Music
Apps:
-
Calm
-
Breathing Zone
-
Insight Timer: “Breathing With Music” tracks
🎹 Easy Instruments
-
Kalimba
-
Tongue/Handpan drum
-
Small keyboard
-
Tablet piano apps: FlowKey, Simply Piano, Yousician
🫁 Singing for Lung Health Groups
Available through:
-
British Lung Foundation
-
Local NHS respiratory teams
-
Online Zoom groups (search “singing for breathing UK”)
-
NAC Facebook events
4. Gentle Movement (Breath-aware & low strain)
🪑 Chair-Based Stretching
Videos
-
NHS Sitting Exercises
-
BLF Chair Exercises
-
Jenny Wren Chair Yoga
-
HasFit Senior Chair Workouts
🛏️ Bed-Based Mini Yoga
Videos
-
Yoga With Adriene (Gentle series, Bedtime)
-
Gentle Yoga for Chronic Illness
-
Sleepy Slow Stretching
🏥 Pulmonary Rehab Mini Exercises
-
NHS PR worksheets
-
BLF Pulmonary Rehab Home Sessions
-
“Living Well With Breathlessness” (NHS Ayrshire)
🥋 Seated Tai Chi / Qigong
Videos
-
Dr Paul Lam – Tai Chi for Health
-
Qigong With Mimi Kuo-Deemer
-
Tai Chi for Seniors (seated)
5. Quiet Mind–Body Practices
🫁 Breathing Techniques
Resources
-
NHS Breathlessness Support
-
BLF Breathing Control
-
4-7-8 Breathing (guided)
-
Apps: Breathe2Relax, Breathing Zone, Oak
🧘 Guided Relaxation
Apps
-
Calm
-
Headspace
-
Insight Timer
-
Aura
YouTube
-
Michael Sealey
-
The Honest Guys
-
Guided Sleep Meditation channels
🌿 Sensory Grounding
Tools:
-
lavender/chamomile inhaler stick
-
warm mug
-
textured blanket
-
grounding cards (“5-4-3-2-1”)
**6. Low-Effort Cognitive Hobbies
(DAILY PUZZLES, JIGSAWS & BRAIN GAMES)**
Cognitive activities are perfect for breathless or fatigued days because they require almost no physical energy.
🧩 Daily Puzzle Sites
New York Times Games
-
Wordle
-
Connections
-
Mini Crossword
-
Spelling Bee
-
Letter Boxed
Others
-
Guardian Puzzles
-
Telegraph Puzzles
-
BBC Puzzle Hub
-
Washington Post Crosswords
-
AARP Games (gentle)
📱 Puzzle Apps (by energy level)
Very Low Energy
-
Zen Match
-
Tiles
-
Color Sort
-
Simple digital jigsaws
-
Solitaire
Medium Energy
-
Flow Free
-
Nonograms (easy mode)
-
Wordscapes
-
Easy Sudoku
-
NYT Mini Crossword
High Energy
-
NYT Crossword
-
Good Sudoku
-
Lumosity
-
Elevate
-
Brilliant.org
🧠 Tiny “Brain Snacks” (1–2 minutes)
-
Brainful
-
Left vs Right
-
Peak (1-minute games)
-
Picture matching
-
Memory card apps
🧩 Jigsaws
Digital Jigsaws
-
Ravensburger Puzzle App
-
Microsoft Jigsaw
-
Magic Jigsaw
-
Jigidy
Physical Jigsaws
-
100–500 pieces (fatigue-friendly)
-
1000+ pieces for long-term projects
-
Use a puzzle roll mat
⭐ Puzzle Difficulty Ladder
(To match breathing & fatigue level)
Level 1 — very low energy / flare
Matching games, colour sort, easy jigsaws, Wordle
Level 2 — low energy, stable
Word searches, Flow Free, easy Sudoku, Mini Crossword
Level 3 — medium
Connections, Spelling Bee, medium Sudoku, trivia
Level 4 — good day
Cryptic crosswords, hard Sudoku, logic puzzles, Brilliant.org
7. Social Connection (without exhaustion)
Low-Effort Options
-
WhatsApp voice notes
-
NAC Facebook & Telegram groups
-
“Photo-a-day” messages
-
5-minute video chats
-
Online craft or puzzle groups
Apps
-
Telegram
-
WhatsApp
-
Discord “chill lounge” servers
-
Facebook Messenger Lite
8. Good / Medium / Bad Day Plans
Good Day
-
1 creative hobby
-
1 gentle movement
-
some music
-
small social contact
Medium Day
-
1 light creative or cognitive activity
-
breathing practice
-
sensory grounding
Bad Day
-
full rest
-
breathing support
-
soft music
-
low-sensory comfort
9. When Rest Is the Right Choice
Good rest-day resources
-
Calm Sleep Stories
-
BBC Sounds (audiobooks, drama)
-
Bob Ross – The Joy of Painting
-
Nature documentaries (slow paced)
-
Gentle ASMR channels
-
Ambient rain / ocean playlists
10. Final Thoughts
Your worth is not measured by productivity.
On low-energy days, you deserve calm, comfort, connection and kindness toward yourself.
This handbook gives you choices — not obligations.
Pick whatever feels gentle today, and leave the rest for tomorrow.
Why Exposure to Young Children Can Increase Illness in Aspergillosis, ABPA, and Bronchiectasis — and How to Track Viral Outbreaks
Many patients with Allergic Bronchopulmonary Aspergillosis (ABPA), aspergillus-related asthma, or bronchiectasis notice that they become ill far more often when spending time around younger children. This applies whether you work with them, live with them, or spend time with grandchildren or family groups. Here’s why it happens, what other patients experience, and how to monitor viral outbreaks so you can protect yourself.
Why Young Children Increase Illness Risk
1. Young children spread far more respiratory infections
Children under 11:
-
Carry more colds, viruses, and respiratory bugs
-
Shed viruses for longer periods
-
Have high viral loads
-
Are still learning hygiene habits
-
Spend a lot of time in close physical contact with adults
Even small viral infections can cause major lung flares in ABPA and bronchiectasis.
2. Viral infections trigger flare-ups, exacerbations, and pneumonia
With:
-
Bronchiectasis → mucus doesn’t clear properly, so infections “stick”
-
ABPA → airways are inflamed, reactive, and mucus-filled
-
Asthma → viruses are the most common exacerbation trigger
A simple cold in a child can turn into:
-
Fever
-
Chest infection
-
Need for antibiotics
-
Pneumonia
-
Weeks of recovery
This pattern is extremely common.
3. Children spread viruses even when only mildly ill
Some viruses (RSV, adenovirus, flu) spread before symptoms, or for many days after a child appears well.
Adults with lung conditions may experience far more severe symptoms from these same infections.
4. Any indoor, close-contact time increases risk
This includes:
-
Teaching music or classroom work
-
Caring for grandchildren
-
Sitting in cars together
-
Birthday parties, playgroups, soft play
-
Family gatherings
-
Living in the same household
Even short exposures can be enough in winter months.
What Other Aspergillosis Patients Report
Across support groups and clinics:
-
Many patients stay well until grandchildren reach nursery/school age.
-
Switching from high school to primary/elementary teaching often leads to repeated infections.
-
People frequently report more pneumonias in winter when around young children.
This is very common and not your fault.
How to Reduce Risk (Realistically)
1. Improve ventilation
-
Open windows/doors during visits or lessons
-
Use a HEPA air purifier at home or work
-
Avoid long stays in small rooms
2. Control exposure without avoiding children
Shorter visits with good ventilation are safer than long indoor contact.
3. Keep up with airway clearance routines
Vital for preventing infections from settling.
4. Mask during periods of high virus circulation
Especially when RSV, flu, COVID, or “winter bugs” are rising.
5. Stay vaccinated
Flu, pneumococcal, COVID (if eligible), and pertussis if around infants.
6. Get medical review if you're repeatedly unwell
Your team may consider:
-
Prophylactic antibiotics
-
Nebulised saline
-
Optimising inhalers/biologics
-
Checking ABPA control
7. Use Occupational Health if exposure is workplace-related
Ask for:
-
Teaching older groups
-
Ventilation improvements
-
Reduced winter exposure
Where to Get Reliable Information on Viral Outbreaks
Tracking viral activity can help you plan safer weeks and reduce the chance of flare-ups.
1. UK Health Security Agency (UKHSA)
Weekly reports on:
-
Flu
-
COVID
-
RSV
-
Measles and other outbreaks
-
Regional activity levels
Best official national overview. Link
2. GOV.UK Infectious Disease Reports
Lists:
-
Confirmed outbreaks
-
Public health warnings
-
School/nursery clusters
-
Localised alerts
3. Local NHS Trust or ICB Websites
Many publish:
-
Weekly respiratory dashboards
-
Local flu/RSV alerts
-
Outbreak notices for schools and care settings
(Example: Greater Manchester ICB has regular respiratory activity updates.)
4. GP Surgeries & NHS App Alerts
GPs can push:
-
Local viral alerts
-
Flu surges
-
Measles/strep notifications
Often one of the earliest local signals.
5. School/Nursery Letters and Newsletters
Schools must notify families about:
-
Flu/strep outbreaks
-
High absence levels
-
Confirmed clusters
Very useful if you work with or spend time around children.
6. Zoe Health Study App
Crowd-sourced, real-time data on:
-
Colds
-
Flu-like illness
-
COVID
-
Regional spikes
Good for early warning.
7. Local Council Public Health
Check:
[Your council] + “Public Health”
They often post:
-
Local outbreak alerts
-
Enhanced infection-control notices
-
Community virus trends
8. NHS 111 Online Data
Shows real-time spikes in:
-
Cough
-
Fever
-
Chest infections
-
Sore throat or strep symptoms
A useful snapshot of local trends.
Key Message
Yes — any exposure to young children can raise infection risk when you have aspergillosis, ABPA, or bronchiectasis.
Tracking viral outbreaks helps you plan safer contact, adjust your activities, and reduce the chance of pneumonia or flare-ups.
Resources
Here are direct links to trusted resources you can use to monitor viral outbreaks and infection risk (especially helpful for those with ABPA, bronchiectasis, asthma, and other lung conditions):
-
UK Health Security Agency (UKHSA) “Influenza and Respiratory Viruses” dashboard — UK data on influenza, RSV, COVID-19, ICU/hospital admission rates.
https://ukhsa-dashboard.data.gov.uk/ -
UKHSA / GOV.UK “National flu and COVID-19 surveillance reports” — weekly/bi-weekly reports summarising community, primary care, hospital and mortality data.
https://www.gov.uk/government/statistics/national-flu-and-covid-19-surveillance-reports-2025-to-2026-season -
GOV.UK “Outbreaks under monitoring” — current outbreaks of various infectious diseases in the UK.
https://www.gov.uk/government/publications/outbreaks-under-monitoring-in-2025/outbreaks-under-monitoring-week-41-week-ending-12-october-2025 -
GOV.UK “Infectious diseases: detailed information” — data, guidance, and analysis for a wide range of infections (flu, RSV, scarlet-fever, etc.).
https://www.gov.uk/government/collections/infectious-diseases-detailed-information -
Public Health Wales “Weekly influenza and acute respiratory infection report” — regional data including GP consultations and infection trends.
https://www.phw.nhs.wales/topics/immunisation-and-vaccines/fluvaccine/weekly-influenza-and-acute-respiratory-infection-report/ -
GOV.UK “Prepare – infectious disease outbreaks” — advice for the public on how to stay prepared for outbreaks, with hygiene and vaccination guidance.
https://prepare.campaign.gov.uk/be-informed-about-hazards/health-infectious-disease-outbreaks/