Fermented Foods & Lung Health: Safety, Infection Risk and Aspergillosis
Last reviewed: April 2026
Many people with lung conditions ask whether foods like kefir, yoghurt or cider vinegar could trigger infections. This article explains what we know — and what we don’t — based on current evidence and patient experience.
Can fermented foods cause lung infections?
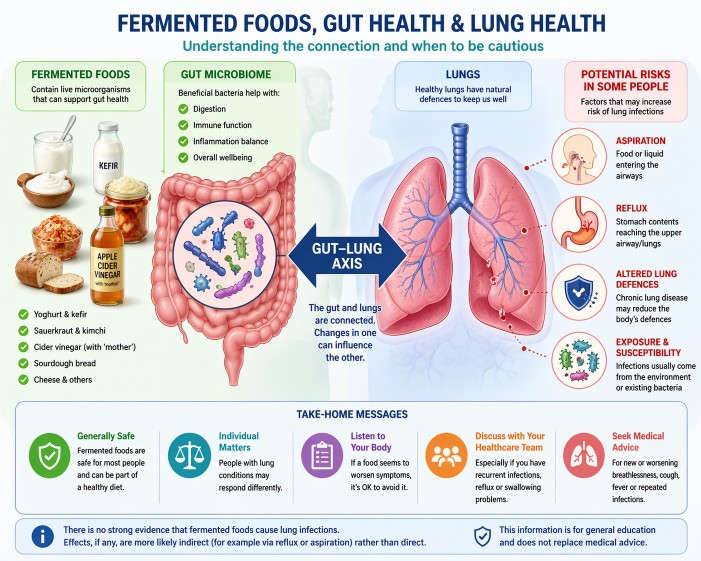
No. There is no strong evidence that fermented foods cause lung infections such as pneumonia. Any effects on the lungs are more likely indirect, for example through reflux or aspiration rather than direct infection.
Quick answer: fermented foods are generally safe, but individual responses vary.
Key Points
- Fermented foods contain live microorganisms, usually beneficial bacteria and yeasts
- For most people, these foods are safe and part of a healthy diet
- There is no strong evidence linking fermented foods to lung infections
- Some people with lung disease may be affected by reflux or aspiration
- If symptoms worsen after certain foods, it is reasonable to avoid them
Table of Contents
- What are fermented foods?
- Are fermented foods safe?
- Can they cause infections?
- Why concerns arise in lung disease
- Who may need caution?
- Practical considerations
- Common questions
- When to seek medical advice
What are fermented foods?
Fermented foods are made using microorganisms (such as bacteria or yeast) to transform food. Examples include yoghurt, kefir, sauerkraut, kimchi, cheese and cider vinegar (including those containing the “mother”).
These microorganisms are generally considered non-harmful or beneficial.
Are fermented foods safe?
For most people, including many with chronic lung conditions, fermented foods are considered safe.
They may support gut health, although evidence varies depending on the product and individual.
You can read more in our
diet and aspergillosis guide
.
Can they cause infections?
There is no clear evidence that eating fermented foods causes lung infections such as pneumonia.
Lung infections usually arise from:
- Microorganisms already present in the airways
- Inhaled organisms from the environment
This is explored further in our article:
Why antibiotics do not always work
.
Why do concerns arise in lung conditions?
People with aspergillosis, bronchiectasis or chronic lung disease may be more sensitive to changes affecting the lungs.
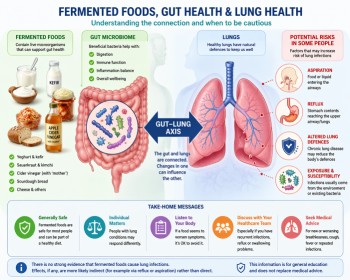
1. Aspiration
If small amounts of food or liquid enter the airway, this can contribute to infection.
2. Reflux
Reflux can reach the upper airway and may play a role in lung irritation.
3. Lung microbiome
The lungs contain their own microbial environment, which can shift during illness.
4. Coincidence vs causation
An infection occurring after a dietary change does not necessarily mean the food caused it.
Evidence in this area is still developing, and most studies focus on gut health rather than direct lung effects.
Who might need to be more cautious?
- Frequent lung infections
- Significant bronchiectasis
- Swallowing difficulties
- Severe reflux
- Weakened immune systems
At specialist centres such as the National Aspergillosis Centre, these factors are considered alongside overall lung health.
Practical considerations
- Avoid foods that appear to worsen symptoms
- Introduce new foods gradually
- Be cautious with unpasteurised products
- Keep a simple symptom diary
Common questions
Are probiotics the same as fermented foods?
No. Probiotics are specific strains studied for health benefits, while fermented foods vary widely.
Should people with aspergillosis avoid fermented foods?
There is no general recommendation to avoid them. Most people tolerate them well.
Can fermented foods affect the lungs directly?
Not usually. Effects, if present, are more likely indirect.
When to seek medical advice
- New or worsening breathlessness
- Persistent cough or sputum changes
- Fever or infection symptoms
- Repeated infections
Summary
Fermented foods are generally safe, but individual responses vary. There is no strong evidence linking them to lung infections, but factors such as reflux or aspiration may be relevant in some people.
Balancing general evidence with personal experience is key.
References
- Marco ML et al. Health benefits of fermented foods.
PMID: 28433791
View on PubMed - Hill C et al. Probiotics consensus.
PMID: 24912386
View on PubMed - Budden KF et al. Gut–lung axis.
PMID: 27694885
View on PubMed - Dickson RP et al. Lung microbiome.
PMID: 26965149
View on PubMed - Marik PE. Aspiration pneumonia.
PMID: 11430328
View on PubMed - NICE Pneumonia guidance
View NICE guidance
Author & Review
This article has been prepared by the National Aspergillosis Centre CARES team for patients and non-specialists.
It is intended for general education and should not replace individual medical advice.
Help us understand how damp homes affect health

We are supporting a UK research project looking at how damp homes may affect health, including respiratory health and conditions such as aspergillosis.
This study is being led by the National Aspergillosis Centre at Manchester University NHS Foundation Trust, and is being shared through aspergillosis.org to support research into damp homes and health.
We are currently inviting people across the UK to register their interest in taking part.
Registering your interest should take less than one minute and does not commit you to taking part.
Why this matters
Damp and mould are often linked to health problems, but there is still limited real-world evidence from people’s homes across the UK.
This project aims to help improve understanding of how home environments may affect health by gathering information from people living in a wide range of housing conditions.
Who can register interest?
We would like to hear from people living in the UK, including:
- people with lung or respiratory conditions
- people without any known lung or breathing condition
- people who have experienced damp or mould at home
- people who have not experienced damp or mould at home
- members of the general public who would like to contribute to the research
We are keen to hear from people with different health backgrounds and a wide range of home environments.
What is the study about?
This research is exploring how damp homes may affect health. The aim is to improve understanding of the relationship between home environments and health symptoms in real-world settings.
This project is for research purposes only and does not provide medical advice or diagnosis.
What might taking part involve later?
If the study opens, some people who register interest may later be invited to:
- complete a short questionnaire about their home and health symptoms
- receive a simple home sampling kit by post
- collect and return a small household sample, for example dust from the home, for research purposes
The home sampling part is intended to be simple and practical. Full instructions would be provided.
Registering your interest now does not commit you to taking part later.
Important information
- Registering interest is voluntary.
- You do not have to take part in the full study later.
- Your details will only be used to contact you about this project.
- Your data will be handled in line with UK data protection regulations.
- You can decide later whether or not to take part.
Frequently asked questions
Am I signing up to take part in the study now?
No. At this stage, you are only registering your interest in hearing more about the study.
Do I need to have a lung condition to register interest?
No. We would like to hear from people with and without lung conditions.
Do I need to have damp or mould in my home?
No. We are interested in hearing from people with a wide range of home environments and experiences.
Will I definitely receive a kit?
Not necessarily. Registering interest helps the research team understand the level of interest and contact people if the study opens.
Will I get personal results about my home or health?
At this stage, no individual results are being promised. More information would be provided if the study proceeds.
What happens after I register interest?
You do not need to do anything further straight away. If the study opens, you may be contacted with more information so you can decide whether you would like to take part.
Register your interest
Ready to help? Complete the form below.
This secure form should take less than one minute to complete.
If the form does not load, you can open it here:
Open the form in a new window
Can People with Aspergillosis Drink Kefir or Take Probiotics?
Many people with aspergillosis ask whether they can safely drink kefir or take probiotics. Kefir is a fermented drink containing live bacteria and yeasts, which raises understandable questions for people with lung conditions. This article explains what is known, what is uncertain, and why advice can differ between chronic pulmonary aspergillosis (CPA), allergic bronchopulmonary aspergillosis (ABPA), and more severe forms of aspergillosis.
Short answer: this is not something with a simple yes-or-no answer. For people with chronic forms of aspergillosis, kefir and probiotic products are not routinely discussed in the same way as they are for people who are severely immunocompromised. However, there is also not enough evidence to say they are helpful for aspergillosis, and people’s experiences vary.
Key Points
- Advice about live foods is often stricter for people with invasive aspergillosis or severe immune suppression
- For chronic pulmonary aspergillosis (CPA), allergic bronchopulmonary aspergillosis (ABPA), and related long-term conditions, the picture is usually less clear-cut
- There is no strong evidence that kefir specifically helps or harms chronic aspergillosis
- Some people feel fine with fermented foods; others feel they do not suit them
- The aim here is to inform, not recommend
What Is Kefir?
Kefir is a fermented drink, usually made from milk, containing a mixture of bacteria and yeasts. It is often described as a probiotic food because it contains live microorganisms.
People may use kefir or probiotic products because of interest in:
- gut health
- recovery after antibiotics
- the microbiome
If you are interested in the wider role of food and nutrition in lung health, see our article on diet and aspergillosis: what helps, what doesn’t, and what matters most.
Why Does This Question Come Up in Aspergillosis?
Different forms of aspergillosis have different risk profiles
It is important not to group all forms of aspergillosis together.
- Invasive aspergillosis usually affects people with very weakened immune systems. In that setting, clinicians are often more cautious about foods or products containing live microorganisms.
- Chronic pulmonary aspergillosis (CPA) usually affects people with underlying lung damage or structural lung disease. Many patients are not severely immunocompromised in the same way.
- Allergic bronchopulmonary aspergillosis (ABPA) and related allergic conditions raise slightly different questions again, because symptom flares may relate more to sensitivity and inflammation than to infection risk.
That distinction matters, because advice that is appropriate for one group may not automatically apply to another.
Chronic vs Invasive Aspergillosis: Why It Matters
For people with chronic pulmonary aspergillosis, the question is usually less about needing to avoid kefir as a rule, and more about recognising that there is no established role for it in treatment. In other words, kefir is not a treatment for CPA, but nor is it routinely listed as something that every patient with CPA must avoid.
For people with ABPA, the picture is slightly different again. Some patients are very aware of foods that seem to trigger symptoms, but that still does not create a universal rule that fermented foods should always be avoided.
What Does the Evidence Say?
At present, there is no strong evidence showing that kefir has a specific benefit for aspergillosis, and there is also no clear evidence that it is harmful in most people with chronic aspergillosis.
Most discussion around kefir and probiotics comes from broader research on:
- the gut microbiome
- antibiotic-associated bowel symptoms
- general digestive health
That is not the same as proving benefit for lung symptoms, fungal disease, or long-term respiratory outcomes.
For related discussion about how antibiotics affect symptoms, infections, and the microbiome, you may also find this helpful: why antibiotics do not always work.
Probiotics and the Gut–Lung Connection
Research into the gut–lung axis suggests that the gut microbiome may influence immune responses elsewhere in the body, including the lungs. This is an active area of research, but it is still early, and it does not yet mean that fermented foods or probiotic supplements should be seen as treatments for aspergillosis.
Some people are interested in probiotics because of repeated antibiotic courses, bowel side effects, or a general wish to support gut health. Those are understandable reasons, but the evidence for a direct lung benefit in chronic aspergillosis remains limited.
Why Do People React Differently?
The main reasons for caution are usually not “aspergillosis” on its own, but the wider clinical picture.
For example, extra caution may be more relevant in people who are:
- severely immunocompromised
- taking high-dose steroids or other immunosuppressive treatment
- acutely unwell
- known to react poorly to fermented foods or probiotic products
In some people, symptoms after kefir may be more about tolerance than infection risk. Patients sometimes describe:
- bloating
- nausea
- abdominal discomfort
- a sense that fermented foods do not suit them
Others report no obvious problems at all. This is one reason it is safer to frame kefir as an individual tolerance issue rather than something routinely recommended or routinely banned.
Kefir in Chronic Pulmonary Aspergillosis (CPA)
For people with CPA, the question is usually less about fungal exposure from kefir and more about whether it suits the individual patient. Many people with CPA have damaged lungs rather than profound immune suppression, so the same dietary warnings used in invasive fungal disease do not automatically apply.
- kefir is not a standard treatment for CPA
- it is not routinely listed as something that must be avoided in all patients with CPA
- individual circumstances, treatments, and tolerance still matter
If you are newly diagnosed or want a broader overview, see our CPA information page.
What About ABPA and Other Allergic Conditions?
In ABPA and related conditions, some people are understandably more alert to foods that seem to trigger symptoms. Fermented products may not suit everyone, but there is not a clear universal rule that they should be avoided.
As with many food-related questions in chronic lung disease, experiences are mixed and difficult to generalise. If you would like a fuller explanation of ABPA itself, visit our ABPA information page.
Homemade vs Shop-Bought Products
Some people also ask whether homemade kefir is different from commercial products. In general terms, homemade fermented products may be less standardised than commercially prepared ones, but that does not automatically mean they will cause a problem. It simply adds another layer of variability.
This is another reason why broad, one-size-fits-all advice is difficult.
How Should This Be Framed for Patients?
A cautious and balanced way to put it is:
Kefir is a fermented drink containing live bacteria and yeasts. Questions about it often come up in aspergillosis because advice is sometimes stricter for people who are severely immunocompromised. For people with chronic conditions such as CPA or ABPA, there is no clear evidence that kefir is either beneficial or harmful for aspergillosis itself. People’s experiences vary, so it is best thought of as an individual tolerance issue rather than something routinely recommended or routinely banned.
When Extra Caution May Be Needed
Extra caution may be more relevant if someone is:
- severely immunocompromised
- on significant immunosuppressive treatment
- recovering from serious illness
- already experiencing ongoing gut symptoms or unexplained food intolerance
In those situations, questions about probiotics, supplements, or fermented foods are often best discussed with a clinician who understands the wider medical picture.
When to Seek Medical Advice
It is sensible to discuss diet or probiotic questions with a clinician or specialist team if:
- you are severely immunocompromised
- you are on significant immunosuppressive treatment
- you develop persistent gut symptoms after using a probiotic product
- you are unsure how advice applies to your particular diagnosis or treatment
Healthcare professionals looking for more formal clinical material can visit our Information for Professionals page.
Common Questions
Can kefir treat aspergillosis?
No. There is no evidence that kefir treats aspergillosis.
Is kefir dangerous with chronic pulmonary aspergillosis?
There is no clear evidence that kefir is harmful in most people with chronic pulmonary aspergillosis, but there is also no evidence that it is beneficial for the condition itself. Tolerance varies between individuals.
Should people with ABPA avoid fermented foods?
Not necessarily. Some people feel certain foods do not suit them, but there is no universal rule that all fermented foods should be avoided in ABPA.
Summary
- Kefir is a fermented probiotic drink containing live bacteria and yeasts
- Advice that applies to invasive aspergillosis does not always apply in the same way to chronic pulmonary aspergillosis or allergic bronchopulmonary aspergillosis
- There is no strong evidence that kefir treats or worsens chronic aspergillosis
- The safest educational position is a neutral one: not a recommendation, not a blanket prohibition
- Individual circumstances, treatments, and tolerance matter
Last reviewed: April 2026
Reviewed by: National Aspergillosis Centre patient information team perspective
Please note: This article is for general education and should not be used as individual medical advice.
Allergy, Intolerance and Wheat Reactions: What Is Actually Going On?
Key points
- You can have real and sometimes severe symptoms without having a classic allergy.
- Allergy, intolerance, and non-IgE reactions involve different biological pathways.
- Similar symptoms (such as wheeze or mucus) do not always mean the same cause.
- The term “intolerance” is often used as a catch-all, which can be confusing.
- For people with lung conditions, triggers may still worsen symptoms even when allergy tests are negative.
This article is general educational information for patients and carers. If you are new to this topic, you may wish to start with our overview of what is aspergillosis or explore common symptoms affecting the lungs and airways.
Contents
- Why this is so confusing
- What is a true allergy?
- What is an intolerance?
- The grey area: non-IgE reactions
- Wheat as an example
- Why “downgraded” feels upsetting
- Why this matters in asthma and aspergillosis
- Why testing is often limited
- What usually happens next?
- Take-home message
- When to seek medical advice
Why this is so confusing
Many people use the word “allergy” to describe any reaction to food or environmental triggers. This is understandable, because the symptoms can feel very similar.
For example:
- wheeze or chest tightness
- increased mucus and respiratory symptoms
- bloating or abdominal discomfort
- fatigue or “brain fog”
However, similar symptoms do not always mean the same biological cause. This is where confusion begins.
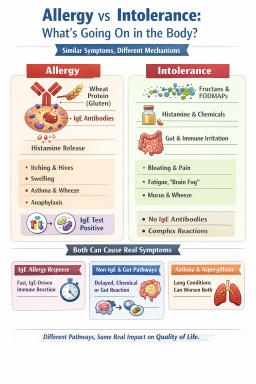
What is a true allergy?
A true allergy usually refers to an IgE-mediated immune reaction.
This means the immune system reacts quickly to a substance, often within minutes to a couple of hours. Symptoms may include:
- itching or hives
- swelling
- wheeze (see asthma and airway symptoms)
- vomiting
- in severe cases, anaphylaxis
This type of reaction is what most allergy clinics are designed to detect, because it can be serious and is usually testable.
What is an intolerance?
An intolerance is a broader term used when symptoms do not follow the classic IgE allergy pathway.
It may involve:
- digestive processes
- food chemicals such as histamine or salicylates
- gut–immune interactions
- non-specific inflammation
Importantly: intolerance does not mean “mild” or “unimportant”. It simply means the mechanism is different and often harder to measure.
For guidance on managing food-related symptoms, see our diet and nutrition hub.
The grey area: non-IgE reactions
Not all immune reactions involve IgE.
Some reactions involve other parts of the immune system and may be:
- delayed
- longer lasting
- harder to detect with standard tests
This creates a grey area between “allergy” and “intolerance”.
This is why the statement:
“Same symptoms but no IgE = intolerance”
is often an oversimplification.
Wheat as an example
Wheat reactions are often used to illustrate this complexity:
- Wheat allergy → IgE reaction to wheat proteins
- Coeliac disease → autoimmune condition (see NICE guidance)
- Non-coeliac wheat sensitivity → unclear mechanism
- Carbohydrate intolerance → reaction to fructans (FODMAPs)
All of these may cause symptoms, but they require different ways of understanding and managing.
Why “downgraded” feels upsetting
Patients are sometimes told they have been “downgraded” from allergy to intolerance.
In reality, what has usually happened is:
- a classic IgE allergy has been considered unlikely
- testing is unlikely to add further information
- the reaction falls into a less clearly defined category
This is a change in classification, not a judgement about importance or severity.
Why this matters in asthma and aspergillosis
For people with asthma, Allergic Bronchopulmonary Aspergillosis (ABPA), or chronic pulmonary aspergillosis (CPA):
- airways are often more sensitive
- inflammation may already be present
This means that triggers do not always need to be classic allergens to cause problems.
Symptoms such as wheeze, mucus and chest tightness may worsen even when allergy tests are negative.
You may also find it helpful to read why antibiotics do not always work, which explains how non-bacterial causes can drive ongoing symptoms.
Why testing is often limited
Allergy testing works best for IgE-mediated conditions.
For many other reactions:
- there are no simple validated tests
- diagnosis relies more on clinical history and patterns
Further detail for clinicians and advanced readers is available in our information section for patients.
What usually happens next?
After a classic allergy has been ruled out, the process does not stop—it changes direction.
Understanding patterns
The focus often shifts to identifying:
- what triggers symptoms
- how quickly symptoms occur
- whether effects are delayed or cumulative
Identifying the main system involved
- Gut-related → bloating, pain, bowel symptoms
- Airway-related → wheeze, mucus, chest tightness
- Mixed/systemic → fatigue and general symptoms
Different types of support
Depending on the pattern, support may involve:
- dietary approaches (nutrition guidance)
- respiratory care (asthma management)
- specialist review (e.g. CPA services)
This stage is often less clear-cut but can still lead to meaningful improvements over time.
Take-home message
- Allergy and intolerance are not the same.
- “Intolerance” is often used as a broad label.
- Symptoms may be similar, but the underlying pathways differ.
- This affects how conditions are understood and managed.
- Even without a clear label, symptoms remain real and important.
When to seek medical advice
Seek urgent help if you develop:
- sudden breathing difficulty
- swelling of the lips, tongue or throat
- collapse or severe dizziness
Arrange medical review if you have:
- persistent or worsening symptoms
- repeated reactions to foods or triggers
- worsening respiratory symptoms
Related topics
- Asthma and airway inflammation
- Allergic Bronchopulmonary Aspergillosis (ABPA)
- Chronic Pulmonary Aspergillosis (CPA)
- Understanding symptoms
- Diet and food triggers
- Why antibiotics do not always work
References
- NHS – Food allergy and intolerance
- BSACI – Food allergy guidance
- NICE NG20 – Coeliac disease
Last reviewed: April 2026
Author: Aspergillosis Website Team
Review status: Educational content for patients and carers
Inflammation and Aspergillosis: Understanding “Stable”, “Flare”, and “Improving” Disease
Last reviewed: April 2026
Key points
- Inflammation is part of the body’s response to Aspergillus, but it does not always mean damage is actively worsening.
- “Stable” disease means no clear progression over time, not that the condition has disappeared.
- Symptoms in aspergillosis often vary because of other infections, especially in the lungs.
- Test results (such as IgE or CRP) can change without symptoms changing.
- Doctors make decisions based on the overall pattern over time, not a single test result.
Table of contents
- What is inflammation and why does it matter?
- Inflammation in different types of aspergillosis
- Clear definitions: active, flare, stable, improving, remission
- What does “stable disease” mean in practice?
- Why other infections cause flare-ups
- Understanding test results (CRP, IgE, scans)
- When test results worsen but symptoms do not
- How doctors decide what is happening
- Common patient questions
- When to seek medical advice
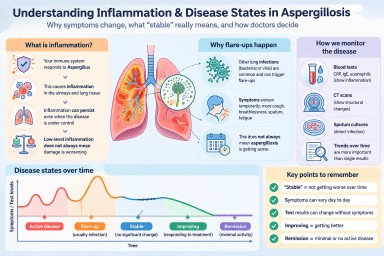
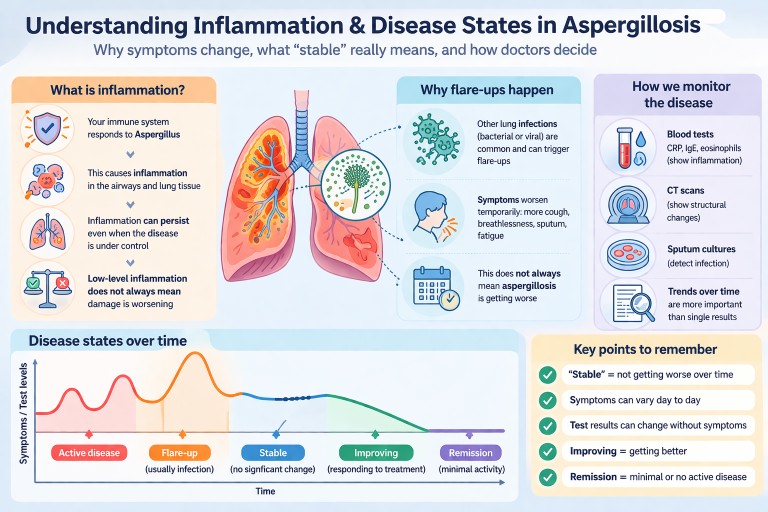
What is inflammation and why does it matter?
Inflammation is the body’s way of responding to something it sees as harmful. In aspergillosis, this is usually the fungus Aspergillus.
This response involves immune cells, chemicals, and changes in the lungs that aim to control the fungus. However, if inflammation continues over a long period (chronic inflammation), it can also contribute to:
- Ongoing symptoms (cough, breathlessness, fatigue)
- Mucus production
- Damage to lung tissue over time
Important: inflammation can be present at a low level without causing active damage. This is common in chronic conditions.
Inflammation in different types of aspergillosis
The type of inflammation depends on the form of aspergillosis:
- Allergic Bronchopulmonary Aspergillosis (ABPA): driven by an overactive allergic response. Blood markers such as IgE and eosinophils are often used to monitor this.
- Chronic Pulmonary Aspergillosis (CPA): caused by long-term infection in damaged lung tissue, leading to ongoing inflammation and structural changes.
- Aspergillus bronchitis: persistent infection with inflammation, often causing chronic cough and sputum.
In all cases, inflammation may improve with treatment but often does not disappear completely.
Clear definitions: disease states
Doctors use the following terms to describe how the disease is behaving:
- Active disease: symptoms, tests, or scans are getting worse over time
- Flare-up: a short-term worsening, often triggered by infection or another stress on the body
- Stable: no clear overall change over time
- Improving / responding to treatment: symptoms and/or tests are getting better
- Remission: minimal or no signs of active disease (used more often in ABPA)
Key point: these states are not fixed — patients may move between them.
What does “stable disease” mean in practice?
“Stable” means that, over a period of time (weeks to months), there is no clear evidence that the disease is progressing.
This usually includes:
- No worsening of key symptoms
- No new complications (e.g. haemoptysis, significant weight loss)
- Imaging (CT scans) showing no progression
- No need to increase treatment
What stable does NOT mean:
- It does not mean symptoms are absent
- It does not mean inflammation is zero
- It does not mean you will feel the same every day
Many patients with stable disease still experience day-to-day variation in symptoms.
Why other infections cause flare-ups
People with aspergillosis are more vulnerable to other lung infections (bacterial or viral).
This is because:
- Lung structure may already be damaged
- Mucus clearance is less effective
- The immune system is already active
When another infection occurs, it can trigger a flare-up, causing:
- Increased cough and breathlessness
- More or thicker sputum
- Fatigue and feeling unwell
- Raised inflammatory markers (e.g. CRP)
Crucial point: this does not necessarily mean the aspergillosis itself is worsening. It is often a temporary additional problem.
Understanding test results
Doctors use several types of tests to monitor inflammation and disease activity:
- CRP / ESR: general markers of inflammation
- IgE: particularly important in ABPA
- Eosinophils: linked to allergic inflammation
- CT scans: show structural changes in the lungs
- Sputum cultures: detect infection
Important limitations:
- No single test gives a complete picture
- Results can fluctuate for many reasons
- Changes must be interpreted over time
When test results worsen but symptoms do not
This situation is common, especially in ABPA.
For example, IgE levels may rise without any noticeable change in symptoms.
This may happen because of:
- Natural biological variation
- Exposure to allergens
- A mild or early flare that has not yet caused symptoms
Key point: a change in a single test result does not automatically mean the disease is worsening.
Doctors will usually:
- Repeat tests
- Look for consistent trends
- Assess symptoms and scans
If symptoms remain stable and no other changes are seen, the condition may still be considered stable — but monitored more closely.
How doctors decide what is happening
Clinicians do not rely on a single result. Instead, they assess the pattern over time:
- Are symptoms changing?
- Are test results consistently rising or falling?
- Are scans stable or changing?
- Is the patient responding to treatment?
This combined assessment is called the clinical picture.
Common questions
If I feel better, what is that called?
This is usually described as improving or responding to treatment. In some cases (especially ABPA), it may be called remission.
Does inflammation always mean damage?
No. Low-level inflammation can persist without causing further harm.
Why do my symptoms change from day to day?
This is common and often relates to infections, environment, or general health rather than disease progression.
Can aspergillosis affect the whole body?
It can have wider effects, but it mainly affects the lungs in most patients.
When to seek medical advice
Seek medical advice if you notice:
- Persistent worsening of symptoms
- New haemoptysis (coughing up blood)
- Significant weight loss
- Symptoms not improving after a suspected infection
- Concerns about test results
Author and review
Author: Aspergillosis Patient Education Team
Reviewed by: National Aspergillosis Centre (UK)
References
- Denning DW et al. Chronic pulmonary aspergillosis guidelines
- ISHAM ABPA guidelines
This article is for general information only and is not a substitute for medical advice.
Aspergillosis and Diet: coping with weight loss, poor appetite, food avoidance and stomach symptoms
For: patients, carers, general practitioners, specialist nurses and other non-specialists
Last reviewed: 8 April 2026
Important: This page is general information. It does not replace advice from your own clinical team.
Key points
- Eating difficulties are common in aspergillosis, especially in chronic pulmonary aspergillosis (CPA) and in people who also have other lung disease.
- The problem is often not simply “poor appetite”. Breathlessness, cough, fatigue, reflux, nausea, altered taste and medicine side effects can all make eating difficult.
- Some people gradually cut out more and more foods because eating feels uncomfortable or because they have been told certain foods are “bad” for lung symptoms.
- For many patients, the main nutritional goal is not a “perfect” diet. It is getting enough energy, protein and fluids in ways that feel manageable.
- “Little and often”, food fortification and nourishing drinks are often more realistic than trying to eat three large meals a day.
- Ongoing weight loss, a very restricted diet, persistent nausea, reflux or difficulty eating most days should be discussed with a doctor, specialist team or dietitian.
Why diet can become a major problem in aspergillosis
Many people living with aspergillosis find that eating becomes much harder than it used to be. This is particularly important in chronic pulmonary aspergillosis (CPA), where weight loss, fatigue and general ill health are common features of the illness. In practical terms, the body may need more energy while the person is less able to eat comfortably.
Several problems can overlap:
- Breathing takes more effort, which can increase energy needs.
- Coughing or breathlessness can interrupt meals.
- Tiredness can make shopping, cooking and eating feel like hard work.
- Inflammation and chronic illness can reduce appetite and contribute to muscle loss.
- Antifungal treatment and other medicines can cause nausea, altered taste, indigestion or poor appetite.
- Reflux, bloating or early fullness may mean that even small meals feel uncomfortable.
For some patients this creates a vicious circle: eating becomes unpleasant, intake falls, weight drops, strength falls, and eating may then feel even more difficult.
Who is most affected?
Not every patient with aspergillosis has major nutritional problems, but some groups are more likely to struggle. This includes people with:
- Chronic pulmonary aspergillosis (CPA)
- pre-existing lung disease such as chronic obstructive pulmonary disease (COPD), bronchiectasis or previous tuberculosis
- long-term fatigue, breathlessness or coughing
- persistent nausea or reflux symptoms
- a history of recent unplanned weight loss
- side effects from antifungal or other medicines
- anxiety around eating because meals repeatedly trigger symptoms
Some people with allergic bronchopulmonary aspergillosis (ABPA) also report poor intake or nutritional difficulties, although the pattern may differ from CPA. In ABPA, steroid treatment, asthma burden, medicine effects and general symptom load may all influence diet.
How eating can become difficult
People often describe eating problems in ways that do not sound like a classic “nutrition” issue. They may say things like:
- “I get full after a few mouthfuls.”
- “I cannot face a proper meal.”
- “Eating makes me cough.”
- “I feel uncomfortable after food.”
- “Some foods seem to sit badly.”
- “I only eat a few safe foods now.”
These experiences are important. They suggest that the real problem may be a mixture of breathlessness, upper gastrointestinal symptoms, medicine effects and learned food avoidance, not simply a lack of willpower or poor food choices.
When eating shrinks into a “minimal diet”
Some patients end up eating very little, often because that feels safer or more manageable than trying to eat normally. A “minimal diet” may look like:
- very small amounts of food only once or twice a day
- mostly soft or liquid foods
- reliance on tea, toast, soup or yoghurt
- long gaps without eating
- skipping meals because eating feels exhausting
This is understandable, but it can become a serious problem. Small intake over time may lead to:
- weight loss
- loss of muscle mass
- greater weakness and fatigue
- slower recovery from illness
- reduced ability to cope with infections or treatment
If a patient is managing only tiny amounts of food, the first goal is often not to rebuild a “normal” diet immediately. It is to make intake easier, more comfortable and more nourishing.
Avoiding many food types
Another common pattern is gradual food restriction. Patients may stop eating several food groups because they believe these foods worsen mucus, cough, reflux, nausea or fungal disease.
Examples include avoiding:
- dairy products
- sweet foods
- bread or dry foods
- meat
- acidic foods
- foods linked in the mind to a previous bad episode
Sometimes there is a genuine reason for avoiding a particular food. For example, reflux may make acidic or very fatty foods uncomfortable, and a dry crumbly food may clearly trigger coughing. The difficulty is that repeated bad experiences can also lead to over-restriction, where more and more foods are cut out than is really necessary.
That can leave the diet low in calories, low in protein and very repetitive. In practice, the aim is usually to adapt foods rather than cut out whole food groups unless there is a clear reason to avoid them.
Could the stomach or gut be part of the problem?
Yes. This is often overlooked.
Some patients with aspergillosis describe symptoms that sound mainly digestive rather than respiratory, for example:
- nausea
- heartburn or reflux
- bloating
- feeling full very quickly
- upper abdominal discomfort
- reduced appetite after starting or changing medication
- alternating diarrhoea and constipation
There are several possible reasons:
- Medicine side effects, including antifungals
- Gastro-oesophageal reflux disease (GORD), which can also worsen cough
- reduced activity levels and chronic illness
- constipation, especially when intake is poor or medicines contribute
- co-existing gastrointestinal disease that is separate from aspergillosis
If eating repeatedly causes upper abdominal or chest discomfort, or if reflux and nausea are prominent, it is reasonable to think of this as a symptom needing review rather than simply a “fussy eating” problem.
Practical ways to make eating easier
Different things help different people, but these approaches are often more realistic than trying to push through large meals.
1. Think “little and often”
Many people do better with five or six small eating opportunities through the day instead of three big meals. That may mean a small breakfast, a mid-morning snack, a light lunch, a nourishing drink, an evening meal and a supper snack.
2. Lower the effort of eating
Soft, moist foods are often easier than dry, chewy or crumbly foods. Examples include:
- porridge
- yoghurt
- custard or rice pudding
- mashed potato with added butter or cheese
- scrambled eggs
- soup with cream or grated cheese
- stews, casseroles or sauced dishes
3. Use drinks as nutrition
For some patients, drinks are easier to manage than food. Nourishing options can include:
- milky drinks
- smoothies
- milkshakes
- fortified hot drinks
- commercial oral nutritional supplements if prescribed or advised
4. Rest before eating
If fatigue or breathlessness are major barriers, it can help to eat after a rest rather than after exertion. Some people find breakfast or lunch easier than an evening meal.
5. Sit upright and stay upright afterwards
This can be especially helpful when reflux, coughing or chest discomfort are part of the picture.
6. Slow the pace
It is acceptable to eat slowly and pause often. Some patients benefit from smaller mouthfuls and short breathing pauses between them.
7. Look for manageable variety
If the diet has become very narrow, widening it gently may be more successful than trying to overhaul everything at once.
How to support weight maintenance
When keeping weight on is difficult, the most useful approach is often to increase the energy and protein content of what is already being tolerated.
Food-first ideas
- Add butter, cream, cheese, yoghurt, milk powder or olive oil to foods where suitable.
- Choose full-fat products rather than “diet” versions if weight loss is a concern.
- Add grated cheese to soup, mashed potato, scrambled eggs or vegetables.
- Make porridge with milk rather than water.
- Keep easy snacks available, such as yoghurts, cheese and crackers, peanut butter, hummus, custard, rice pudding or milky desserts.
Protein matters
Protein helps preserve muscle. Good sources include:
- milk, yoghurt and cheese
- eggs
- meat, fish and poultry if tolerated
- beans, lentils and other pulses
- nut butters where suitable
Oral nutritional supplements
When food alone is not enough, a doctor or dietitian may suggest oral nutritional supplements. These are often used between meals rather than instead of meals. They can be particularly helpful when appetite is low or meal size is very limited.
In general UK nutrition practice, a “food first” approach is usually tried first where appropriate, but oral nutritional supplements are commonly used when someone is at higher risk of malnutrition or is unable to meet needs from food alone.
Food and medicine issues to remember
Food and medicine can interact in two main ways.
1. Medicines can affect eating
Antifungal treatment and other medicines may contribute to:
- nausea
- indigestion
- altered taste
- poor appetite
- bowel upset
If these symptoms started after a medicine was introduced or changed, it is worth discussing that with the prescribing team.
2. Food can affect medicines
Some antifungal medicines have specific instructions about when to take them in relation to food. For example:
- Itraconazole capsules are generally taken with or just after food, while itraconazole liquid is generally taken on an empty stomach.
- Voriconazole is usually taken on an empty stomach.
- Some medicines also have important interactions with antacids or acid-suppressing medicines.
Because formulations differ, and because other medicines may also interact, patients should follow the instructions they have been given for their exact preparation and check with a pharmacist or clinical team if unsure.
Grapefruit and other food interactions: some medicines have clinically important food interactions. Patients should check current advice for each medicine rather than relying on memory or online generalisations.
Common diet myths
Dairy always makes mucus worse
This is a very common belief. Current evidence does not show that dairy routinely increases lung mucus production for most people. Some people do notice a thicker mouth or throat feeling after milk, which may relate to texture rather than extra mucus. If dairy is well tolerated, it can be a useful source of calories and protein.
Sugar “feeds” aspergillosis, so it should be cut out completely
Patients often hear this online, but strict self-imposed restriction can be more harmful than helpful when someone is already struggling to maintain intake. For many patients with weight loss, the immediate nutritional priority is adequate calories and protein, not aggressive dietary exclusion.
There is a special anti-aspergillosis diet
There is no widely accepted specialist diet that treats aspergillosis itself. In routine practice, nutrition advice usually focuses on preventing or treating malnutrition, easing symptoms and managing medicine-related issues.
If eating is difficult, I should just avoid more foods
Sometimes a food really is hard to tolerate, but repeated restriction can shrink the diet too far. Often it is more useful to ask, “Can this be made easier to eat?” rather than “Should I cut this out altogether?”
When to seek medical help
Patients should speak to their doctor, specialist team or another qualified healthcare professional if they have any of the following:
- ongoing unplanned weight loss
- clothes, rings or dentures becoming looser
- difficulty eating most days
- a very narrow diet with only a few “safe” foods
- persistent nausea, reflux, bloating or abdominal discomfort
- increasing weakness or fatigue
- concerns that medicines are worsening appetite or stomach symptoms
It may be appropriate to ask about a dietitian referral, especially if intake has been poor for some time or there are signs of malnutrition.
Seek urgent medical advice if:
- food or fluids are being kept down very poorly
- there are signs of dehydration
- weight loss is rapid or severe
- pain, vomiting, swallowing difficulty or other worrying symptoms are developing
Common questions
Should I force myself to eat full meals?
Usually not. If full meals are consistently overwhelming, smaller and more frequent intake is often more successful.
Are liquid calories “cheating”?
No. For some people, nourishing drinks are one of the most practical ways to protect weight and strength.
What if I only manage a few foods?
That is still worth discussing. A restricted diet may be understandable, but it can increase nutritional risk over time.
What if dairy feels unpleasant?
Individual experience matters. If a food clearly feels uncomfortable, it may help to try alternatives or use smaller amounts in different forms. But many people do not need to exclude dairy automatically.
Could reflux be making my cough worse?
Yes, it can in some people. Reflux can irritate the upper airway and may contribute to cough or discomfort around meals.
When to seek medical advice
Ask for medical advice if you are losing weight, struggling to eat most days, developing a very restricted diet, or think nausea, reflux or medication side effects are affecting your intake. Ask urgently if you are becoming dehydrated, vomiting repeatedly, or your intake has become extremely poor.
Author and review information
Prepared for: aspergillosis.org
Purpose: general educational information for patients and non-specialists
Review note: Because medicine instructions can change between formulations and brands, patients should always check the current advice supplied with their own prescription and confirm uncertainties with a pharmacist or clinical team.
References and further reading
- Carter C, Muldoon EG, Kosmidis C. Chronic pulmonary aspergillosis - a guide for the general physician. 2024.
PubMed - Tashiro M, Takazono T, Izumikawa K. Chronic pulmonary aspergillosis: comprehensive insights into epidemiology, diagnosis, treatment, and unresolved challenges. 2024.
Free full text - Roboubi A, et al. Allergic bronchopulmonary aspergillosis. 2023.
PubMed - Sunman B, et al. Current approach in the diagnosis and management of allergic bronchopulmonary aspergillosis in children with cystic fibrosis. 2020.
Free full text - Madhavan V, et al. Malnutrition in allergic bronchopulmonary aspergillosis complicating asthma. 2023.
Free full text - British Dietetic Association. Spotting and treating malnutrition.
BDA resource - BAPEN. Food first / food enrichment.
BAPEN resource - BAPEN / Malnutrition Pathway. Managing malnutrition in COPD.
PDF - NICE. Managing malnutrition in COPD, The Malnutrition Pathway.
NICE shared learning resource - NHS. Heartburn and acid reflux.
NHS advice - Cambridge University Hospitals NHS Foundation Trust. Dietary and lifestyle advice for adults with gastro-oesophageal reflux disease (GORD).
CUH advice - NICE BNF. Itraconazole.
BNF drug monograph - Manchester University NHS Foundation Trust, National Aspergillosis Centre. Patient Information: Itraconazole.
PDF - Manchester University NHS Foundation Trust, National Aspergillosis Centre. Patient Information: Voriconazole.
PDF - Oxford University Hospitals NHS Foundation Trust. Advice about antifungals.
PDF - Balfour-Lynn IM. Milk, mucus and myths. Archives of Disease in Childhood. 2019.
Article - Pinnock CB, Graham NM, Mylvaganam A. Relationship between milk intake and mucus production in adult volunteers challenged with rhinovirus-2. 1990.
PubMed - ASCIA. Milk, mucus and cough.
Patient resource
Diet and Aspergillosis: What Helps, What Doesn’t, and What Matters Most
Last reviewed: 8 April 2026
Many people living with aspergillosis ask whether diet can help “fight” the fungus, reduce symptoms, or improve recovery. This is completely understandable, particularly given the large amount of advice online suggesting that certain foods, supplements, or diets can control fungal disease.
This article explains what current evidence shows, what diet can and cannot do, and where it genuinely matters for people living with aspergillosis.
Core principle: Aspergillus-related disease is driven by what we breathe in and how the body responds — not by what we eat.
Contents
- Key points
- What do we mean by “no evidence”?
- How Aspergillus disease develops
- The role of airways, mucus and lung structure
- Immune response and inflammation
- Can food treat Aspergillus?
- Diet and ABPA (allergic disease)
- Allergy vs infection: why diet is often misunderstood
- Diet and CPA (chronic infection)
- Why nutrition still matters
- Steroids and diet
- Diet and antifungal medication
- Checking food–drug interactions
- Common diet myths (and why they persist)
- A practical, evidence-based approach
- When to seek help
- References
Key points
- There is no diet that treats aspergillosis.
- Aspergillus-related disease develops through inhalation of spores, changes in the lungs, and immune responses.
- Diet does not control Aspergillus growth in the lungs.
- Diet still matters for strength, weight, recovery, and treatment safety.
- Food can affect how medicines are absorbed and metabolised.
- Many popular online diet claims are based on misunderstood science, oversimplification, or marketing.
What do we mean by “no evidence”?
When this article says there is “no evidence” or “no strong evidence”, this does not mean that we are simply waiting for proof to arrive.
In most cases, it means one of two things:
- the idea has been studied and has not been shown to help real patients, or
- there is only laboratory or theoretical evidence, which does not translate into benefit in real-world disease
For example, fungi can grow in sugar-rich laboratory conditions. That does not mean eating sugar feeds Aspergillus in the lungs. The body tightly regulates blood glucose, and lung disease is far more complex than a laboratory culture dish.
Key message: when clinicians say there is “no evidence”, they usually mean an approach is unlikely to work in practice, not that it is a promising treatment that just has not been tested yet.
How Aspergillus disease develops
Aspergillus is a common environmental mould. People are exposed by breathing in microscopic spores from the air. Most people clear these spores without any problem.
Whether disease develops depends on the interaction between:
- the condition of the lungs
- how well mucus is cleared
- the immune response
In healthy lungs, inhaled spores are trapped in mucus, moved out of the airways, and removed by immune cells. When this system is disrupted, Aspergillus may persist or trigger inflammation. This is described in clinical reviews of pulmonary aspergillosis such as Kosmidis & Denning, 2015.
This process takes place in the respiratory system and is driven by inhalation — not diet.
The role of airways, mucus and lung structure
The lungs have several important defence systems. These include mucus, cilia (tiny hair-like structures that move mucus), and immune cells. Together, they help remove inhaled particles and organisms.
In conditions such as asthma, bronchiectasis, chronic obstructive pulmonary disease (COPD), or other chronic lung diseases:
- mucus may become thicker or harder to clear
- airways may be damaged or widened
- normal clearance may be less effective
This can make it easier for Aspergillus to remain in the lungs. In some people this contributes to allergic disease. In others, especially where there is structural damage, it can contribute to chronic infection.
These airway and lung-structure problems are not altered by avoiding particular foods.
Immune response and inflammation
In many people, particularly those with allergic forms of Aspergillus disease, symptoms are driven more by the immune system than by direct tissue invasion from the fungus.
For example, in allergic bronchopulmonary aspergillosis (ABPA), the body mounts an exaggerated allergic response to Aspergillus. This typically involves:
- raised IgE antibodies
- eosinophilic inflammation
- airway swelling and mucus production
Reviews of ABPA describe these immune processes in more detail, including the overlap with asthma and cystic fibrosis-related airway disease, for example Knutsen & Slavin, ABPA review.
These immune pathways are complex and are not controlled by specific foods.
Can food treat Aspergillus?
No specific food has been shown to treat Aspergillus-related lung disease.
You may come across claims about garlic, turmeric, coconut oil, probiotics, herbs, or “anti-fungal” foods. Some of these have shown antifungal effects in laboratory settings, but there is no reliable clinical evidence that eating them improves aspergillosis outcomes.
This is because:
- food is processed in the digestive system, not the lungs
- active compounds may not reach the lungs in useful amounts
- the biology of lung disease is much more complex than simple fungal growth in a dish
Diet can support the body, but it is not a treatment for Aspergillus disease.
Diet and ABPA (allergic disease)
In ABPA, the main problem is an allergic or immune reaction to Aspergillus. Diet does not switch that reaction on or off.
That means:
- food does not “feed” ABPA
- there is no evidence that an “anti-fungal diet” controls ABPA
- restrictive diets do not treat the underlying immune process
However, diet can become more important because many patients with ABPA are treated with prednisolone or other corticosteroids. These medicines can affect appetite, weight, blood sugar, and bone health. NHS information on prednisolone describes common effects such as weight gain, increased appetite, and longer-term bone risks: NHS Prednisolone guidance.
So in ABPA, diet often matters more in relation to treatment effects than in relation to the fungal trigger itself.
Allergy vs infection: why diet is often misunderstood
Many patients understandably ask whether a certain food might be “triggering” symptoms. This can be confusing because aspergillosis includes both allergic and infectious forms.
What matters here is the route of exposure:
- Aspergillus-related lung disease is driven by inhaled spores
- food enters the body through the digestive tract
Symptoms that seem to occur after eating may actually relate to:
- acid reflux
- throat irritation
- airway sensitivity
- coincidental fluctuation in symptoms
These may be real and troublesome, but they are not the same thing as diet directly driving Aspergillus disease.
Key message: Aspergillus-related lung symptoms are driven by what you breathe in and how your immune system responds — not by what you eat.
Diet and CPA (chronic infection)
Chronic pulmonary aspergillosis (CPA) is different from ABPA. CPA tends to occur in lungs that are already damaged or structurally abnormal, for example after tuberculosis, with bronchiectasis, or with COPD.
In CPA, the key issue is not food intake but the presence of abnormal lung tissue where Aspergillus can persist. This broader clinical picture is outlined in reviews such as Kosmidis & Denning, 2015.
Diet does not alter fungal growth directly, but it can matter because some people with CPA experience:
- weight loss
- fatigue
- low appetite
- reduced physical strength
In CPA, diet is therefore mainly about maintaining strength, resilience, and recovery — not about “starving” the fungus.
Why nutrition still matters
Although diet does not treat Aspergillus directly, nutrition still matters a great deal. Good nutrition supports the whole body, including the respiratory system.
Good nutrition can help support:
- muscle strength, including the muscles used for breathing
- energy levels
- general immune function
- recovery from illness and treatment
Poor nutrition, by contrast, can contribute to:
- tiredness
- lower resilience
- reduced strength
- slower recovery
This is one reason why very restrictive diets can be unhelpful, especially for patients already coping with chronic disease, breathlessness, or weight loss.
Steroids and diet
For patients taking corticosteroids such as prednisolone, diet becomes particularly relevant.
Important issues can include:
- increased appetite
- weight gain
- raised blood sugar
- fluid retention
- longer-term bone health
From a practical point of view, this is one of the strongest reasons to think carefully about diet in aspergillosis care. Here, diet is not being used to treat the fungus; it is helping patients cope with the effects of treatment and maintain overall health.
For longer-term steroid use, adequate calcium intake and attention to bone health may also be important. This is particularly relevant for people already at risk of osteoporosis.
Diet and antifungal medication
The clearest and most important direct link between diet and aspergillosis care is through medication.
Food can affect how medicines are absorbed, broken down, or cleared from the body.
Food–drug interactions
Some foods and drinks affect enzymes in the liver that metabolise drugs. A well-known example is grapefruit, which can interfere with CYP3A4 and change drug levels in the body.
Taking antifungals correctly
Some antifungal medicines are affected by food. For example, voriconazole is usually taken on an empty stomach so that absorption is more reliable. This is described in professional guidance such as the British National Formulary (BNF).
Supplements and herbal products
Supplements are often marketed as “natural”, but they can still interact with prescription medicines. Some herbal products may alter drug metabolism and therefore affect antifungal treatment.
Key message: diet rarely affects Aspergillus directly, but it can be very important in how your medicines work.
Checking food–drug interactions
Reliable sources for checking medicine and food interactions include:
- British National Formulary (BNF)
- patient information leaflets supplied with medicines
- Patient.info interaction checker
It is also important to understand the limits of specialist tools. Drug-interaction tools designed specifically for antifungals are very useful for drug–drug interactions, but they do not usually include food interactions in a comprehensive way.
The safest source of advice remains your pharmacist or clinical team.
Common diet myths (and why they persist)
Many people with aspergillosis come across strong claims online about diet and fungal disease. These often sound convincing, especially when symptoms are difficult to control and people understandably want something practical they can do.
However, most of these claims are based on misunderstandings of biology, laboratory research taken out of context, or commercial promotion.
Below are some of the most common myths, along with what current evidence suggests.
“Sugar feeds fungus”
This is one of the most common claims.
It comes from the fact that fungi can grow in sugar-rich laboratory conditions. However, this does not reflect what happens in the human body.
- blood sugar is tightly regulated
- Aspergillus in the lungs is not directly exposed to dietary sugar in the way people often imagine
- there are no clinical studies showing that reducing dietary sugar improves aspergillosis outcomes
Why it persists: it sounds intuitive, it is easy to repeat, and it fits with heavily marketed “anti-fungal” diet programmes.
“Milk and dairy increase mucus”
This is a very common concern in respiratory disease generally.
Research does not show that dairy increases mucus production in the lungs. Some people notice a thicker or coated feeling in the mouth and throat after milk, but that is different from producing more mucus in the airways.
- no good evidence of increased lung mucus
- no evidence that dairy worsens Aspergillus disease itself
Why it persists: the mouth and throat sensation after dairy can easily be mistaken for a lung effect.
“Yeast in food causes fungal infection”
Foods such as bread or fermented products may contain yeast, but yeast used in food is not the same thing as Aspergillus.
- food yeast and Aspergillus are different organisms
- Aspergillus-related lung disease is linked to inhalation of environmental spores, not eating yeast-containing foods
Why it persists: the word “fungus” is used broadly, which can blur important differences between very different organisms.
“Avoid foods made with mould”
Some patients are advised online to avoid blue cheese, mushrooms, or other foods associated with moulds.
There is no good evidence that eating these foods changes Aspergillosis in the lungs.
- the digestive and respiratory systems are separate
- food moulds are not the same thing as inhaled environmental Aspergillus exposure
Why it persists: when a disease involves mould, it feels logical to avoid all mould-associated foods, even though the biology does not support that approach.
“Low-carb or ketogenic diets can starve the fungus”
This idea grows out of the “sugar feeds fungus” claim.
However:
- the body keeps glucose within a narrow range
- lung infections are not directly altered by short-term dietary carbohydrate restriction
- there is no clinical evidence that low-carb or ketogenic diets improve aspergillosis outcomes
Why it persists: it sounds more scientific than it is, and it is frequently promoted in wellness and biohacking communities.
“Anti-fungal foods such as garlic, turmeric or coconut oil can treat aspergillosis”
Some of these substances show antifungal activity in laboratory experiments.
That is not the same as treating disease in people. The concentrations used in experiments are often very different from what is achievable through normal eating, and human lung disease is far more complex than a petri dish.
Why it persists: laboratory findings are often presented online as though they were proven clinical treatments.
“Detox diets or cleanses remove fungal infection”
There is no biological mechanism by which detox diets or juice cleanses remove Aspergillus from the lungs.
- the lungs are not “cleansed” through the digestive tract
- there is no clinical evidence supporting detox approaches in aspergillosis
Why it persists: detox language is emotionally appealing, especially when people feel unwell and want a sense of control.
“Candida overgrowth” diets apply to aspergillosis
Many patients come across “anti-Candida” diets and wonder whether the same advice applies to Aspergillus.
These diets often recommend:
- cutting out sugar
- avoiding carbohydrates
- removing yeast-containing foods
- following restrictive “anti-fungal” eating plans
However, these ideas are based on a different organism and a different part of the body.
Candida vs Aspergillus: important differences
- Candida is a yeast commonly found on the skin and in the gut
- Aspergillus is a mould in the environment that is inhaled into the lungs
Aspergillus-related disease such as ABPA or CPA affects the lungs and is driven by inhaled spores, not by changes in the gut.
Do “anti-Candida diets” affect Aspergillus?
There is no clinical evidence that diets designed to reduce Candida:
- affect Aspergillus in the lungs
- reduce allergic responses to Aspergillus
- improve outcomes in aspergillosis
These diets often rely on the same assumptions as other myths, especially the idea that “sugar feeds fungus”. Those assumptions do not fit how Aspergillus lung disease works.
What about the gut microbiome?
There is real scientific interest in the gut microbiome and its role in health. However, there is currently no evidence that changing diet to target gut fungi alters aspergillosis outcomes.
This is an area of research interest, but it is not a basis for dietary treatment at present.
Why these diets can be unhelpful
Restrictive anti-Candida or “anti-fungal” diets can sometimes lead to:
- reduced calorie intake
- weight loss
- nutritional imbalance
- anxiety around food
This can be particularly unhelpful in people with chronic lung disease who need to maintain strength and energy.
Key message: diets designed for “Candida overgrowth” are not relevant to aspergillosis and are not supported by evidence in this context.
“If symptoms improve after changing diet, the diet must be working”
This is a very understandable conclusion, but it can be misleading.
Symptoms in aspergillosis often fluctuate because of:
- natural variation in disease activity
- environmental exposure
- allergy activity
- medication changes
An improvement may happen at the same time as a dietary change without being caused by that change.
Advice from non-mainstream or alternative sources
Many people with long-term or difficult-to-control conditions look beyond standard medical care for additional answers. This is entirely understandable, especially when symptoms are persistent or uncertain.
You may come across advice from practitioners or online sources who describe themselves as offering “functional”, “integrative”, or “alternative” approaches. These often include:
- strict or highly restrictive diets
- “anti-fungal” or “detox” protocols
- long lists of supplements
- tests or diagnoses that are not widely used in NHS practice
Some of this advice may sound detailed or scientific. However, it is important to understand that:
- many of these approaches are not supported by clinical evidence in aspergillosis
- they may be based on theories that do not reflect how lung disease develops
- they are often not part of standard respiratory or infectious disease care
In some cases, following this advice can lead to:
- unnecessary dietary restriction
- weight loss or nutritional problems
- delays in receiving appropriate medical treatment
- confusion about symptoms and diagnosis
This does not mean that all non-mainstream approaches are harmful, but it does mean they should be approached with care.
Key message: if you are considering advice outside standard medical guidance, it is usually helpful to discuss it with your clinical team or pharmacist so it can be considered safely alongside your current treatment.
Overall message: many diet claims are based on ideas that sound plausible but do not reflect how aspergillosis works in the body.
A practical, evidence-based approach
For most people with aspergillosis, the most sensible and evidence-based approach is:
- eat a balanced diet
- maintain weight and strength
- include regular sources of protein
- avoid unnecessarily restrictive diets
- follow medicine-specific instructions carefully
- check food–drug interactions rather than relying on social media advice
Focus on supporting your body and treatment — not trying to treat Aspergillus through diet.
When to seek help
It may be worth asking for extra support if you are experiencing:
- unintentional weight loss
- poor appetite
- difficulty managing steroid-related appetite or weight changes
- concerns about blood sugar or bone health
- questions about food–drug interactions
Pharmacists, GPs, specialist teams, and where appropriate dietitians can all help with these issues.
References
- Kosmidis C, Denning DW. The clinical spectrum of pulmonary aspergillosis. Thorax. 2015.
- Warris A, Bercusson A, Armstrong-James D. Aspergillus colonization and antifungal immunity in cystic fibrosis patients. Med Mycol. 2019.
- Knutsen AP, Slavin RG. Reviews on allergic bronchopulmonary aspergillosis.
- NHS. Prednisolone guidance.
- British National Formulary (BNF).
- Patient.info interaction checker.
This article is for general information and should not replace advice from your own clinical team.
Why Headaches Can Occur in Aspergillosis
Last reviewed: March 2026
Key Points
- Headaches are relatively common in people living with aspergillosis, but they usually have multiple contributing causes.
- Common causes include sinus involvement, inflammation, sleep disturbance, and medication effects.
- Antifungal medicines such as itraconazole may improve some symptoms indirectly but can also occasionally cause headaches.
- Patterns (timing, location, triggers) can help identify likely causes, but headaches are rarely due to one factor alone.
- New, severe, or unusual headaches should always be assessed by a healthcare professional.
Table of Contents
- Overview
- Sinus involvement (common cause)
- Inflammation and immune response
- Allergic-type responses (e.g. ABPA)
- Medication effects
- Sleep disturbance and night symptoms
- Breathing and oxygen levels
- General health factors
- Understanding headache patterns
- Common questions
- When to seek medical advice
- Summary
- Author and review
- References
Overview
Many people living with aspergillosis report headaches at some point during their illness. These headaches can vary in type, severity, and timing, and may be confusing—especially when they change over time or seem linked to treatment.
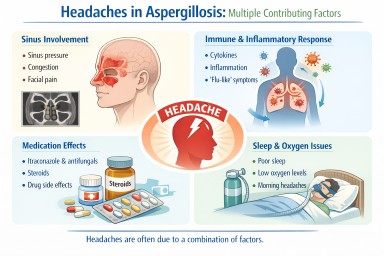
In most cases, headaches are not caused by a single factor. Instead, they reflect a combination of:
- local effects (such as sinus pressure)
- immune system activity
- medication effects
- sleep and general health factors
Understanding these different contributors can help make sense of symptoms and support more informed discussions with your clinical team.
Sinus involvement (common cause)
When Aspergillus affects the sinuses (sometimes called fungal sinusitis), this can directly cause headaches.
This happens because:
- sinus drainage becomes blocked
- pressure builds up in the sinus cavities
- the lining of the sinuses becomes inflamed
Typical features:
- pain or pressure in the forehead, cheeks, or behind the eyes
- worsening when bending forward
- a feeling of fullness or congestion
This is one of the most direct ways aspergillosis can lead to headaches.
Inflammation and immune response
Even when the sinuses are not directly involved, the body’s immune response to fungal material can cause systemic effects.
The immune system releases signalling molecules (such as cytokines) that can:
- increase inflammation
- affect blood vessels
- trigger headache pathways
This type of headache can feel similar to a “flu-like” or inflammatory headache.
Allergic-type responses (e.g. ABPA)
In conditions such as Allergic Bronchopulmonary Aspergillosis (ABPA), the immune system reacts strongly to Aspergillus.
This may involve:
- allergic pathways
- histamine and related mediators
- ongoing airway inflammation
Possible symptoms:
- head pressure or discomfort
- fluctuating headaches
- a “foggy” or unwell feeling
These headaches are often less clearly localised than sinus-related pain.
Medication effects
Some treatments used in aspergillosis can contribute to headaches.
Antifungal medications (e.g. itraconazole):
- headache is a recognised side effect in some people
- effects vary between individuals
Steroids (if prescribed):
- can affect sleep and mood
- may influence blood pressure
- can indirectly contribute to headaches
Medication effects can sometimes overlap with disease-related symptoms, making patterns harder to interpret.
Sleep disturbance and night symptoms
Sleep disruption is common in chronic lung conditions.
Possible contributors include:
- night-time coughing
- breathlessness
- discomfort or anxiety
Poor sleep can lead to:
- morning headaches
- increased sensitivity to pain
- fatigue-related headaches
Breathing and oxygen levels
In some people with more advanced lung involvement:
- oxygen levels may be slightly reduced
- breathing effort may increase
This can contribute to:
- morning headaches
- fatigue and cognitive symptoms
Not all patients experience this, but it is an important factor in some cases.
General health factors
Headaches can also be influenced by general aspects of living with a long-term condition:
- dehydration
- fatigue
- reduced activity levels
- stress or anxiety
These factors can contribute to tension-type headaches or make other headache types more noticeable.
Understanding headache patterns
Looking at patterns can sometimes help identify likely contributors.
- Facial pressure worse on bending: may suggest sinus involvement
- Early morning headaches: may relate to sleep or breathing patterns
- Fluctuating or “wave-like” symptoms: may reflect inflammation or immune activity
- New headaches after starting medication: may be treatment-related
However, these are general observations only and do not replace clinical assessment.
Headaches in Aspergillosis: Interactive Decision Aid
This tool helps patients and carers think about common patterns that can contribute to headaches in aspergillosis. It does not diagnose the cause of a headache.
It is designed to support discussion with a healthcare professional and highlight possible contributors such as sinus involvement, inflammation, medication effects, sleep disturbance, and breathing-related factors.
1. Where is the pain mainly felt?
2. When is it most noticeable?
3. What does it feel like?
4. What other features are present?
5. Are there any red flags?
Possible contributors
This panel highlights common patterns only. It is not a diagnosis and does not replace medical assessment.
Common questions
Are headaches a recognised symptom of aspergillosis?
They can occur, but are usually indirect and caused by associated factors such as sinus disease or inflammation.
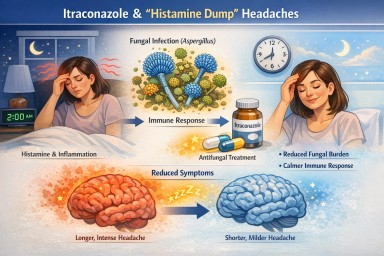
Can antifungal treatment improve headaches?
In some cases, yes—if symptoms are linked to fungal-related inflammation. However, antifungals can also occasionally cause headaches as a side effect.
Are “histamine-type” headaches part of aspergillosis?
Some patients describe symptoms in this way, but the underlying mechanism is often more complex than histamine alone.
Why do my headaches change over time?
This is common and may reflect changes in inflammation, treatment, sleep, or overall health.
When to seek medical advice
You should seek medical advice if you experience:
- new or unusually severe headaches
- headaches that are worsening over time
- neurological symptoms (e.g. vision changes, weakness, confusion)
- fever, neck stiffness, or other concerning symptoms
If you are unsure whether your headaches are related to aspergillosis, treatment, or another cause, it is important to discuss this with your healthcare team.
Summary
Headaches in people with aspergillosis are usually caused by a combination of factors rather than a single issue.
The most common contributors include:
- sinus involvement
- immune and inflammatory responses
- sleep disturbance
- medication effects
Understanding patterns and changes over time can be helpful, but medical assessment is important if symptoms are new, severe, or concerning.
Author and review
Prepared for: aspergillosis.org
Audience: Patients and non-specialist readers
Important: This article is for general information only and does not replace individual medical advice.
References
- Patterson TF et al. (2016). Practice Guidelines for the Diagnosis and Management of Aspergillosis.
PMID: 27365388 - Denning DW et al. (2016). Chronic pulmonary aspergillosis guidelines.
PMID: 26699723 - Chakrabarti A et al. (2009). Fungal sinusitis: a categorization and definitional schema.
PMID: 19522756
Why Do My “Histamine” Headaches Improve on Itraconazole?
Last reviewed: March 2026
Key Points
- Itraconazole is an antifungal medicine. It is not an antihistamine.
- Some people notice that symptoms such as headaches, flushing, or a “histamine-type” feeling become shorter or less intense after starting treatment.
- This is most likely because itraconazole reduces the fungal burden and the immune response it triggers, rather than blocking histamine directly.
- Symptoms that happen in the early hours of the morning may also be influenced by the body’s natural day-night rhythm.
- Changes in symptoms can be helpful clues, but headaches can have more than one cause.
Table of Contents
- Overview
- What is itraconazole and how does it work?
- What do people mean by “histamine dump” headaches?
- Why might symptoms improve on itraconazole?
- Why do symptoms often happen at night?
- Does this mean histamine is the main problem?
- Common questions
- When to seek medical advice
- Summary
- Author and review
- References
Overview
Some people taking itraconazole for non-lung or lung forms of aspergillosis notice that symptoms they describe as “histamine-type” symptoms, such as headaches, flushing, pressure, or a general sense of inflammatory overload, become shorter or less severe.
A typical pattern might be:
- Symptoms start overnight, for example, around 2 am
- Symptoms previously lasted most of the day
- Symptoms are now settling much earlier after starting treatment
This can be confusing, especially when the symptoms feel similar to a histamine reaction. The important point is that itraconazole does not work like an antihistamine, but it can reduce symptoms indirectly if a fungal process is contributing to them.
What is itraconazole and how does it work?
Itraconazole is an antifungal medicine used to treat infections caused by fungi such as Aspergillus.
It works by interfering with the production of ergosterol, an essential part of the fungal cell membrane. This weakens the fungus and helps reduce fungal growth and survival in the body.
As the fungal burden falls, the immune system may be less strongly stimulated, and that can lead to a reduction in inflammation-related symptoms.
So although itraconazole does not block histamine directly, it may reduce the underlying trigger that is causing the body to react.
What do people mean by “histamine dump” headaches?
“Histamine dump” is not a formal medical diagnosis, but some patients use it as a practical way of describing symptoms such as:
- sudden headaches, especially overnight or early in the morning
- flushing or a feeling of heat
- pressure in the head or sinuses
- a sense of being “wired”, agitated, or unwell
These symptoms may involve histamine, but they can also reflect broader inflammation, immune activation, mast cell activity, or other signalling chemicals in the body.
Why might symptoms improve on itraconazole?
If itraconazole is helping, it is most likely doing so indirectly. There are several possible reasons for this.
1. Reduced fungal burden
If fungal material in the body is reduced, there may be less for the immune system to react to. That can mean less inflammatory signalling overall.
2. Reduced immune activation
Fungi can stimulate the immune system in ways that lead to inflammation and, in some people, histamine-related symptoms. If antifungal treatment lowers that stimulus, symptoms may become less intense or settle more quickly.
3. Shorter inflammatory response
Some people find that the symptom still begins, but does not “run on” for as long. For example, a headache that used to last from 2am until late afternoon may now settle by 5am.
Why do symptoms often happen at night?
The body has a natural circadian rhythm, a 24-hour cycle that affects hormones, inflammation, sleep, and immune activity.
- Some inflammatory signals can be more noticeable overnight
- Cortisol rises in the early morning, and helps suppress inflammation
Does this mean histamine is the main problem?
Not necessarily. Symptoms may involve multiple pathways, including immune response to fungi, general inflammation, mast cell activity, and sinus pressure.
Common questions
Does itraconazole act like an antihistamine?
No. It does not block histamine receptors.
Why are my symptoms improving but not gone?
This is common and may reflect partial control of the underlying trigger.
Does this prove Aspergillus is the cause?
No. It suggests a possible link but does not confirm causation.
Will symptoms continue to improve?
Possibly, but responses vary between individuals.
When to seek medical advice
- new or severe headaches
- neurological symptoms (vision, speech, balance)
- worsening or persistent symptoms
- concerns about medication side effects
Summary
Itraconazole does not directly affect histamine but may reduce symptoms by lowering fungal burden and immune activation.
Author and review
Prepared for: aspergillosis.org
Audience: Patients and non-specialist readers
Important: This does not replace individual medical advice.
References
- Patterson TF, Thompson GR 3rd, Denning DW, et al. (2016).
Practice Guidelines for the Diagnosis and Management of Aspergillosis.
View on PubMed (PMID: 27365388) - Denning DW et al. (2016).
Chronic pulmonary aspergillosis guidelines.
View on PubMed (PMID: 26699723) - Barnes PJ, Adcock IM (2009).
Circadian rhythm in airway disease.
View on PubMed (PMID: 19336589) - Stone KD et al. (2010).
IgE, mast cells, and eosinophils.
View on PubMed (PMID: 20176269)
Why Join an Online Support Group if You Have Aspergillosis?
You are not alone with aspergillosis
Join a friendly online support meeting — no pressure, just listen if you prefer.
Many patients find that even attending once helps them feel more reassured, informed, and supported.
Why Join an Online Support Group if You Have Aspergillosis?
Living with aspergillosis can feel isolating. Many people go for years without meeting another person with the same condition. Family and friends may be supportive, but they may not fully understand what it is like to live with breathlessness, fatigue, treatment side effects, uncertainty, or repeated hospital visits.
That is one reason online support groups can be so valuable. They bring people together who understand, often immediately, many of the challenges that aspergillosis can bring.
Key points
- Online support groups reduce isolation and help patients feel understood
- They offer shared experience alongside emotional support
- They improve confidence and understanding of the condition
- They help patients feel better prepared for appointments
- They are flexible — you can simply listen if you prefer
What changes when people join a support group?
Before joining
- Feeling alone with the condition
- Uncertainty about symptoms
- Limited practical advice
- Low confidence at appointments
- Worry about the future
After joining
- Connection with others who understand
- Better understanding of the condition
- Practical day-to-day coping ideas
- More confidence asking questions
- Feeling more supported and reassured
Why aspergillosis can feel so isolating
Aspergillosis is a relatively rare condition, and many patients never meet someone else with the same diagnosis. Online support groups help bridge that gap by creating a shared space for understanding and connection.
1. You realise you are not alone
Hearing others describe similar symptoms and challenges can be immediately reassuring and reduce feelings of isolation.
2. Shared experience can be deeply reassuring
Support groups provide practical, real-world insight into managing fatigue, pacing, work, and daily life.
3. You may understand your condition better
Listening to others and accessing shared resources helps build confidence and understanding.
4. It can help you feel more confident at appointments
Patients often feel better prepared and more able to ask the right questions.
5. Emotional support matters too
These groups provide encouragement, understanding, and a sense of belonging.
What happens in a typical online support session?
- Friendly welcome — no pressure to speak
- Open discussion — share or listen
- Optional topics — such as fatigue or treatment experiences
- Flexible participation — camera and microphone optional
- Safe, moderated space
Many people attend their first session just to listen — and that is completely fine.
What patients often say
“I wish I had joined sooner. Just hearing others talk made a huge difference.”
“I didn’t speak in my first meeting, but it really helped just listening.”
“It helped me understand my condition and feel more confident.”
Thinking of joining?
You can attend once, listen, and decide if it feels helpful. There is no obligation to continue.
View meeting times and book here:
https://aspergillosis.org/support-meetings/
Meetings are held online using Microsoft Teams. You will receive a joining link after booking.
Bottom line
Online support groups offer connection, reassurance, and understanding. They cannot replace medical care, but they can make living with aspergillosis feel more manageable and less lonely.
Please note: These groups are for support and shared experience. They do not replace advice from your own doctor or specialist team.