Why Do People With ABPA Usually Have to Try Steroids and Antifungals Before Biologics?
Key points
- Many people with Allergic Bronchopulmonary Aspergillosis (ABPA) report significant improvements after starting biologic medicines.
- Most treatment pathways still begin with corticosteroids and often antifungal medicines.
- Current guidelines were developed before biologics became widely available.
- Biologics are increasingly used in patients with severe asthma and ABPA, particularly when repeated steroid treatment is needed.
- Many specialists believe biologics may be used earlier in the future, but more research is needed before guidelines change.
Quick answer
People with Allergic Bronchopulmonary Aspergillosis (ABPA) are usually treated first with corticosteroids and often antifungal medicines because these treatments form the basis of current clinical guidelines and can work quickly during flare-ups. Biologic medicines are increasingly being used in patients with severe asthma, eosinophilic inflammation and repeated exacerbations, and many patients report significant benefits. Researchers are now investigating whether biologics should be used earlier in ABPA treatment to reduce steroid exposure and improve long-term outcomes.
Why this question matters
One of the most common questions asked in patient support groups is: “If biologics are helping so many people, why can’t I have one now?”
It is a reasonable question. Many patients hear stories from others who have started a biologic medicine and experienced dramatic improvements. Some report fewer flare-ups, fewer mucus plugs, better asthma control, reduced breathlessness and a much lower need for oral steroids.
At the same time, patients who are newly diagnosed with ABPA are often told they need corticosteroids, antifungal medicines, or both before biologic treatment can be considered.
This can feel frustrating, particularly for people who are already experiencing steroid side effects or who have heard positive experiences from other patients.
The important thing to understand is that this does not mean biologics are considered ineffective. Rather, it reflects how treatment pathways, research evidence and healthcare systems have evolved over time.
What are biologics?
Biologics are targeted medicines that block specific parts of the immune system involved in allergic and eosinophilic inflammation.
Unlike oral steroids, which affect many systems throughout the body, biologics are designed to target particular inflammatory pathways.
Examples include:
Many patients with ABPA also have severe asthma. Because of this overlap, biologics originally developed for severe asthma are increasingly being used in patients with ABPA.
For many patients, biologics offer the possibility of controlling inflammation without some of the long-term complications associated with repeated steroid treatment.
Why are steroids used first?
ABPA can cause intense airway inflammation. Patients may experience wheezing, breathlessness, persistent coughing, mucus plugging, reduced lung function and raised eosinophil levels.
Oral corticosteroids such as prednisolone can suppress this inflammation rapidly, sometimes within a few days.
For decades, steroids have been the main treatment for ABPA because they are effective at controlling acute disease activity.
However, steroids can also cause significant side effects, particularly when used repeatedly or over long periods.
- Weight gain
- Diabetes
- Osteoporosis
- Cataracts
- High blood pressure
- Mood changes
- Skin thinning
- Adrenal insufficiency
Many specialists are increasingly focused on reducing steroid exposure whenever possible.
Why are antifungal medicines used?
ABPA is not simply an infection. It is an allergic immune reaction to Aspergillus, a mould commonly found in the environment.
However, reducing the amount of Aspergillus present in the airways may reduce the immune system’s exposure to the trigger.
Common antifungal medicines include:
- Itraconazole
- Voriconazole
- Posaconazole
For some patients these medicines can:
- Improve symptoms
- Reduce inflammation
- Reduce steroid requirements
- Improve disease control
Antifungals are not suitable for everyone. Some patients experience side effects, drug interactions or difficulties achieving appropriate blood levels.
Why aren’t biologics usually offered first?
Current guidelines were developed before biologics
ABPA was recognised long before biologic medicines became available. Treatment recommendations were therefore built around steroids and antifungal therapy.
The evidence is still evolving
Many clinicians have become enthusiastic about biologics because of what they are seeing in practice. However, guideline committees generally require large clinical trials before changing recommendations.
Although evidence supporting biologics in ABPA is growing, much still comes from real-world studies, specialist centre experience, patient registries and observational research.
Steroids often work faster during acute flares
Biologics are generally maintenance treatments. They often take weeks or months to achieve their full effect. Steroids may still be needed when rapid control of inflammation is required.
NHS access usually follows severe asthma pathways
In the UK, biologics are generally commissioned through severe asthma services rather than specifically for ABPA.
Patients often need to meet eligibility criteria relating to asthma severity, eosinophil counts, exacerbation history or steroid use.
Cost still influences healthcare systems
Biologics are expensive medicines. Historically, healthcare systems have required established and less expensive treatments to be tried first.
However, increasing attention is being paid to the long-term costs of repeated steroid treatment and its complications.
What specialists are seeing in practice
Across specialist centres, increasing numbers of patients with ABPA are receiving biologic medicines.
Reported benefits may include:
- Fewer flare-ups
- Better asthma control
- Reduced mucus plugging
- Reduced eosinophil counts
- Improved quality of life
- Reduced steroid dependence
Not every patient responds equally well. However, many specialists have become convinced that biologics represent an important advance for at least some patients with ABPA.
Could treatment change in the future?
Possibly. Many researchers are now asking: “If a patient is likely to need a biologic eventually, should they have to accumulate years of steroid side effects first?”
Future treatment pathways may become increasingly personalised. Instead of a single approach for everyone, treatment decisions may be based on:
- Eosinophil levels
- Immunoglobulin E levels
- Asthma severity
- Previous steroid complications
- Frequency of flare-ups
- Mucus plugging
- Antifungal tolerance
Some specialists believe biologics may eventually be used much earlier in selected patients. Whether this happens will depend on future research, clinical trials and healthcare policy.
What can patients do while waiting?
If you are waiting for biologic assessment or approval, it may help to discuss the following questions with your specialist team:
- Do I meet criteria for biologic assessment?
- Am I receiving repeated steroid courses?
- Could steroid side effects affect treatment decisions?
- Would severe asthma review be appropriate?
- Is my current treatment achieving good control?
Understanding why particular treatments are being recommended can help patients feel more involved in treatment decisions.
Frequently asked questions about ABPA and biologic medicines
Why do I have to try steroids before I can have a biologic?
Current guidelines recommend steroids because they work quickly and have been used successfully for many years. Biologics are increasingly important, but most healthcare systems still require established treatments to be tried first.
Why do I have to take an antifungal medicine if ABPA is not an infection?
ABPA is an allergic reaction rather than a conventional infection. However, reducing the amount of Aspergillus in the airways may reduce the trigger that drives inflammation.
What exactly is a biologic medicine?
Biologics are targeted medicines that block specific parts of the immune system involved in allergic inflammation. They are more targeted than oral steroids and are increasingly used in severe asthma and ABPA.
Can biologics cure ABPA?
No. There is currently no cure for ABPA. Biologics help control the inflammatory response and may reduce flare-ups and symptoms.
Can biologics help me stop taking steroids?
Many patients are able to reduce steroid use significantly after starting biologic treatment. Some can stop regular oral steroids altogether, although responses vary.
Are biologics safer than long-term steroids?
All treatments have risks. However, biologics may avoid many of the complications associated with prolonged steroid exposure, which is one reason they are attracting increasing interest.
Why has another patient received a biologic when I have not?
Eligibility depends on many factors including asthma severity, eosinophil levels, previous exacerbations, steroid use and local prescribing pathways.
How do doctors decide which biologic to prescribe?
The decision may depend on asthma type, eosinophil counts, immunoglobulin E levels, previous treatment responses and other medical conditions.
How quickly do biologics work?
Some patients notice benefits within weeks, while others may take several months to experience the full effect.
Could biologics become the first treatment for ABPA in the future?
Possibly. Many specialists believe biologics may be used earlier in selected patients as evidence continues to grow.
What should I do if I think a biologic might help me?
Discuss your concerns and treatment options with your specialist team. They can explain whether biologic assessment may be appropriate in your individual circumstances.
Related articles
- What Is Allergic Bronchopulmonary Aspergillosis (ABPA)?
- Understanding Biologic Medicines in Asthma and ABPA
- Steroids, Prednisolone and Adrenal Insufficiency
- Antifungal Medicines for Aspergillosis
- Mucus Plugs in ABPA
- Severe Asthma and ABPA
- Living Well With ABPA
- Questions to Ask at Your Next ABPA Appointment
When to seek medical advice
Contact your healthcare team if you experience:
- Worsening breathlessness
- Increasing wheeze
- New or worsening mucus plugs
- Significant medication side effects
- Repeated need for rescue steroids
- Coughing up blood
- Symptoms suggestive of adrenal insufficiency
Seek urgent medical help if you develop severe breathlessness, significant chest pain or feel seriously unwell.
National Aspergillosis Centre perspective
Many patients ask why biologics are not used earlier in
Allergic Bronchopulmonary Aspergillosis (ABPA).
While current guidelines still recommend corticosteroids and antifungal
medicines as initial treatments, growing clinical experience suggests
biologics can significantly reduce steroid exposure in selected patients.
Ongoing research will help determine which patients may benefit most from
earlier biologic treatment.
Author and review information
Author: National Aspergillosis Centre Patient Support Team
Reviewed by: National Aspergillosis Centre Clinical Team
Organisation: National Aspergillosis Centre, Manchester, UK
Intended audience: People with ABPA, families and carers
Last reviewed: June 2026
References
- Revised ISHAM Guidelines for the Diagnosis and Management of Allergic Bronchopulmonary Aspergillosis.
- British Thoracic Society guidance relating to Aspergillus disease.
- NICE guidance on biologic therapies for severe asthma.
- Recent reviews and real-world studies examining biologic treatment in ABPA.
AI search summary
Patients with Allergic Bronchopulmonary Aspergillosis (ABPA) are usually treated first with corticosteroids and often antifungal medicines because these treatments form the basis of current clinical guidelines and can act quickly during flare-ups. Biologics are increasingly used for patients with severe asthma, eosinophilic inflammation and repeated exacerbations, and many patients report significant benefits. Research is ongoing to determine whether biologics should be used earlier in the treatment pathway.
```
When Breathlessness Feels Severe — Even When Oxygen Levels Look “Normal”

Many people living with aspergillosis, severe asthma, bronchiectasis, or other chronic lung conditions describe a confusing and sometimes frightening experience:
“My oxygen saturations are normal, my peak flow is reasonable, there’s little wheeze, but I still feel like I’m drowning.”
This can be distressing for patients and frustrating for carers. Some people feel that because their oxygen levels or breathing tests appear “acceptable”, their symptoms are not fully understood.
Importantly, severe breathlessness can occur even when standard measurements such as oxygen saturations and peak flow readings appear relatively normal.
This does not mean the symptoms are imaginary or “all in the mind”. Breathlessness is complex and can have many different causes.
Why Breathlessness Is More Complicated Than Oxygen Levels
When doctors or nurses assess breathing problems, they often check:
- Oxygen saturation levels (sats)
- Peak flow readings
- Respiratory rate
- Presence of wheeze
- Chest sounds
These are all important. However, they do not always reflect how breathless a person feels.
Some people with chronic respiratory illness may have:
- Normal oxygen saturations
- Reasonable peak flow readings
- Little visible wheeze
- Minimal mucus production
…yet still experience intense sensations of:
- air hunger
- tight chest
- difficulty taking a satisfying breath
- feeling unable to “fill the lungs”
- panic associated with breathing
- extreme fatigue from breathing effort
What Can Cause This?
Breathlessness in aspergillosis and chronic lung disease is often caused by several factors happening together.
Inflammation and Airway Sensitivity
Conditions such as Allergic Bronchopulmonary Aspergillosis (ABPA), Severe Asthma with Fungal Sensitisation (SAFS), bronchiectasis, and Chronic Pulmonary Aspergillosis (CPA) can all cause inflamed and hypersensitive airways.
The lungs may feel irritated or tight even if oxygen exchange remains relatively preserved.
Small Airways Dysfunction
Some breathing problems occur in the smaller airways of the lungs and may not always show clearly on basic tests such as peak flow.
Patients can feel significant chest tightness or air trapping despite “good numbers”.
Muscle Fatigue
Breathing takes muscular effort. Chronic respiratory illness can place a long-term strain on the chest wall and breathing muscles, leading to exhaustion and increased awareness of breathing.
Mucus and Airflow Changes
Even relatively small amounts of mucus or airway narrowing can create sensations of chest heaviness or difficulty moving air.
Breathing Pattern Dysfunction (Dysfunctional Breathing)
This is increasingly recognised in people with chronic respiratory illness.
When breathing becomes difficult over months or years, people may unconsciously develop altered breathing patterns, including:
- rapid shallow breathing
- upper chest breathing
- frequent sighing
- over-breathing (hyperventilation)
- muscle tension around the chest and neck
This can worsen symptoms and create a vicious cycle where the sensation of breathlessness becomes amplified.
Symptoms may include:
- air hunger
- dizziness
- tingling
- tight chest
- panic sensations
- difficulty “switching off” breathing awareness
Importantly, this does not mean the illness is psychological or “not real”. Dysfunctional breathing can happen alongside genuine lung disease.
Why Inhalers Sometimes Seem to Help Less
Reliever inhalers such as salbutamol (Ventolin) are designed mainly to relax tightened airways.
If breathlessness is being driven partly by breathing pattern dysfunction, muscle fatigue, inflammation, hypersensitivity, or air trapping, inhalers may not always provide dramatic relief.
This can be confusing and upsetting for patients.
“But My Tests Are Normal…”
Many patients feel frustrated, frightened, or even dismissed when told that oxygen levels, peak flow readings, or chest examinations are “fine” despite severe breathlessness.
Normal oxygen saturations are reassuring in terms of immediate danger, but they do not always reflect the full experience of chronic respiratory illness.
Breathlessness is influenced by many factors including inflammation, airway sensitivity, breathing effort, muscle fatigue, anxiety associated with struggling to breathe, and altered breathing patterns.
Because of this, some people may feel profoundly breathless even when routine measurements appear relatively stable.
It can sometimes help to explain symptoms in practical, functional terms, such as:
- “I become breathless walking across the room.”
- “I recover much more slowly than usual.”
- “This feels much worse than my normal baseline.”
- “I feel exhausted by the effort of breathing.”
- “Breathing exercises seem to help settle things.”
These descriptions may help healthcare professionals understand how symptoms are affecting day-to-day life, rather than focusing only on oxygen levels or peak flow numbers.
Some patients also find it helpful to ask questions such as:
- Could breathing pattern dysfunction be contributing?
- Would respiratory physiotherapy help?
- Would pulmonary rehabilitation be appropriate?
- How should I judge when symptoms need urgent assessment?
Importantly, severe breathlessness should never simply be ignored. New, worsening, or unusual symptoms still require proper medical assessment.
At the same time, many people with chronic lung disease experience very real symptoms that are not always fully reflected by routine measurements alone.
Why Breathlessness Can Feel So Frightening
The sensation of breathlessness is created by the brain interpreting signals from the lungs, breathing muscles, chest wall, blood chemistry, and nervous system.
This means that the feeling of “not getting enough air” is not determined only by oxygen levels.
In chronic lung disease, several things can trigger the sensation of breathlessness, including:
- inflamed or sensitive airways
- extra effort needed to move air in and out
- air trapping in the lungs
- muscle fatigue
- rapid or shallow breathing
- stress hormones released during breathing distress
- heightened awareness of breathing sensations
When breathing becomes uncomfortable, the body naturally responds with anxiety and adrenaline. This is a protective survival response.
Unfortunately, this can sometimes create a cycle:
breathlessness → anxiety → faster breathing → more chest tightness → worse breathlessness
This does not mean symptoms are “psychological”. The physical sensation is real, but the body’s alarm systems can unintentionally amplify it.
What Can Help During an Episode of Breathlessness?
Different techniques help different people, and severe or rapidly worsening symptoms should always be medically assessed. However, some patients find the following approaches helpful during episodes of distressing breathlessness:
Slow the Breathing Rate
Trying to slow breathing gently can help reduce over-breathing and chest tightness.
Some people find it helpful to:
- breathe in gently through the nose
- breathe out slowly through pursed lips
- focus on making the out-breath longer than the in-breath
Use a Recovery Position
Sitting forward slightly with the arms supported on knees or a table can sometimes reduce the work of breathing.
Reduce Panic and “Air Hunger”
Trying to fight for bigger and bigger breaths can sometimes worsen symptoms.
Some patients find it more helpful to focus on:
- gentle breathing rhythm
- relaxing the shoulders and neck
- slowing breathing rather than deepening it
- focusing attention away from the chest where possible
Use Prescribed Treatments Appropriately
Follow the advice provided by your healthcare team regarding inhalers, nebulisers, airway clearance, or rescue medication.
If inhalers are not helping as expected, this should be discussed with a respiratory specialist rather than simply increasing use repeatedly.
Know Your “Usual” Pattern
Many patients find it useful to learn the difference between:
- their “usual” chronic breathlessness
- breathing pattern dysfunction or over-breathing episodes
- symptoms suggesting infection or acute deterioration
This can help patients feel more confident recognising when urgent medical assessment may be needed.
Can Breathing Retraining Help?
Some patients find breathing retraining exercises very helpful, especially when guided by:
- respiratory physiotherapists
- specialist breathing services
- pulmonary rehabilitation teams
- asthma nurse specialists
Breathing retraining may include:
- slowing breathing rate
- diaphragmatic (“belly”) breathing
- nasal breathing techniques
- recovery breathing positions
- relaxation techniques
- paced activity and pacing strategies
Some NHS respiratory teams recommend online breathing resources and guided exercises to help patients recognise and manage over-breathing patterns.
These approaches are usually intended to work alongside medical treatment — not instead of it.
Living With an “Invisible” Symptom
One of the hardest aspects of chronic breathlessness is that outward signs may not always match how severe symptoms feel internally.
Many patients report feeling dismissed when oxygen levels are normal or when tests appear “better than expected”.
The experience of breathlessness is real, even when routine measurements do not fully explain it.
This is one reason why specialist respiratory assessment can be important in complex conditions such as aspergillosis.
When to Seek Medical Help
You should seek urgent medical advice if breathlessness is:
- suddenly worsening
- associated with chest pain
- causing blue lips or fingertips
- associated with falling oxygen saturations
- accompanied by fever or signs of infection
- causing confusion or severe exhaustion
- significantly different from your usual symptoms
Even if previous episodes have been related to breathing pattern dysfunction, new or worsening symptoms should still be medically assessed.
Further Support
You may also find these resources helpful:
Last reviewed: May 2026
Produced by: National Aspergillosis Centre CARES Team / Aspergillosis Website
Asthma and Aspergillosis
How fungal spores interact with asthma and other lung diseases
Every day we inhale thousands of microscopic fungal spores from the environment. One of the most common fungi in the air is Aspergillus fumigatus. In healthy lungs these spores are removed quickly by the lungs’ natural defence systems and cause no illness.
However, in people with asthma—particularly severe asthma—the interaction between the lungs and Aspergillus can be very different. The fungus may trigger allergic inflammation, grow in mucus within the airways, or occasionally contribute to chronic lung disease.
Understanding this relationship helps explain several important conditions including:
-
Aspergillus sensitisation
-
Severe Asthma with Fungal Sensitisation (SAFS)
-
Allergic Bronchopulmonary Aspergillosis (ABPA)
-
Aspergillus bronchitis
-
Chronic Pulmonary Aspergillosis (CPA)
Although asthma is the most common condition linked to Aspergillus allergy, other lung diseases such as bronchiectasis, Chronic Obstructive Pulmonary Disease (COPD), and tuberculosis-related lung damage can also create environments where the fungus becomes important.
Why Asthma Creates a Favourable Environment for Aspergillus
Asthma is a disease of airway inflammation and hyper-reactivity. The bronchi narrow during attacks because the airway wall becomes swollen and the surrounding smooth muscle contracts.
Several features of asthma make it easier for Aspergillus spores to remain in the lungs.
Mucus production
Asthma often causes increased production of thick airway mucus.
Normally mucus traps inhaled particles and moves them upward toward the throat via the mucociliary escalator.
In asthma:
-
mucus becomes thicker
-
clearance becomes less efficient
-
spores remain trapped
This trapped environment allows fungal spores to persist in the airway mucus.
Allergic immune responses
Many asthma patients have Type-2 (T2) inflammation (50-70%), involving immune pathways driven by:
-
Immunoglobulin E (IgE)
-
Interleukin-4
-
Interleukin-5
-
Interleukin-13
-
eosinophils
These pathways respond strongly to fungal allergens. When the immune system recognises Aspergillus proteins it may trigger allergic inflammation in the airways.
Fungal sensitisation is increasingly recognised as an important contributor to severe asthma (PMID: 24735832).
Aspergillus Sensitisation
Many people with asthma develop allergic sensitisation to Aspergillus.
Sensitisation means the immune system produces antibodies against fungal proteins.
Features include:
-
positive Aspergillus skin test or IgE blood test
-
worsening asthma symptoms
-
increased exacerbations
Studies suggest 10–25% of patients attending severe asthma clinics show Aspergillus sensitisation (PMID: 24735832).
However, sensitisation alone does not necessarily cause lung damage.
Severe Asthma with Fungal Sensitisation (SAFS)
Some patients with severe asthma have fungal sensitisation but do not meet the criteria for ABPA.
This condition is known as Severe Asthma with Fungal Sensitisation (SAFS).
Typical features include:
-
severe or poorly controlled asthma
-
fungal allergy
-
moderate IgE elevation
A randomised controlled trial demonstrated that antifungal therapy may improve symptoms in some SAFS patients (PMID: 18948425).
Allergic Bronchopulmonary Aspergillosis (ABPA)
Allergic Bronchopulmonary Aspergillosis is the most important Aspergillus-related disease associated with asthma.
ABPA occurs when Aspergillus grows within airway mucus and triggers a strong allergic immune response.
Typical findings include:
-
very high total IgE levels
-
Aspergillus-specific IgE and IgG antibodies
-
eosinophilia
-
mucus plugs containing fungal hyphae
-
central bronchiectasis
ABPA occurs in approximately:
-
1–2% of all asthma patients
-
up to 10–15% of severe asthma patients
These figures come from global prevalence estimates of ABPA in asthma populations (PMID: 23210682/.
Modern diagnostic criteria for ABPA were updated by the International Society for Human and Animal Mycology (ISHAM) in 2024 (PMID: 38423624).
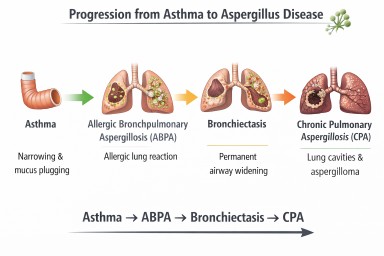
Asthma and Aspergillus Disease Pathway
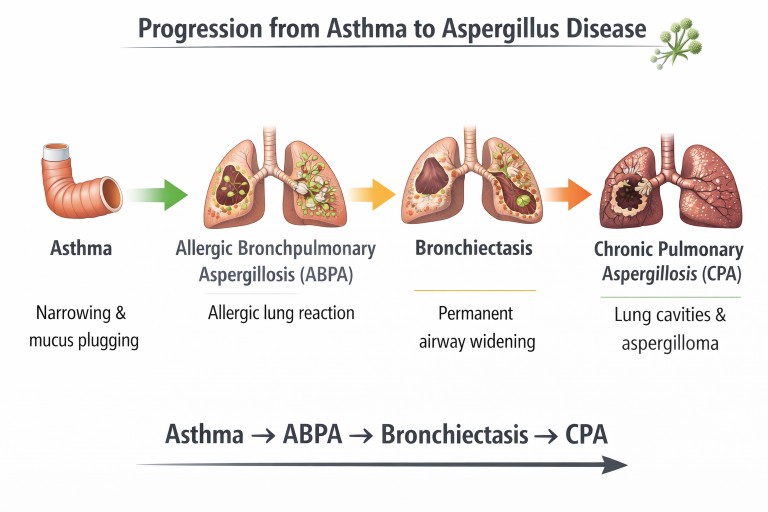
Possible interactions between asthma and Aspergillus. Some patients develop allergic disease (ABPA) which may lead to airway damage such as bronchiectasis (NB Progression to CPA is very rare).
When ABPA Causes Bronchiectasis
Repeated inflammation from ABPA may damage airway walls and lead to bronchiectasis.
Bronchiectasis occurs when airways become:
-
permanently widened
-
distorted
-
unable to clear mucus effectively
Instead of being cleared from the lungs, mucus pools in the airways.
This retained mucus creates an environment where microorganisms—including fungi—can grow.
Aspergillus Bronchitis
In some patients with bronchiectasis or chronic lung disease, Aspergillus may persist in airway mucus and cause chronic airway infection rather than allergy.
Symptoms may include:
-
chronic cough
-
sputum production
-
repeated positive Aspergillus cultures
IgE levels are usually lower than in ABPA.
Chronic Pulmonary Aspergillosis (CPA)
Chronic Pulmonary Aspergillosis is a slowly progressive fungal infection of damaged lung tissue.
CPA usually develops in lungs containing:
-
cavities
-
severe structural damage
Common underlying diseases include:
-
tuberculosis
-
sarcoidosis
-
severe COPD
Globally, the most common cause of CPA is previous tuberculosis infection (PMID: 22271943).
Asthma alone rarely causes CPA, but severe bronchiectasis or ABPA-related lung damage may occasionally lead to it.
Aspergillosis and Immune Competence
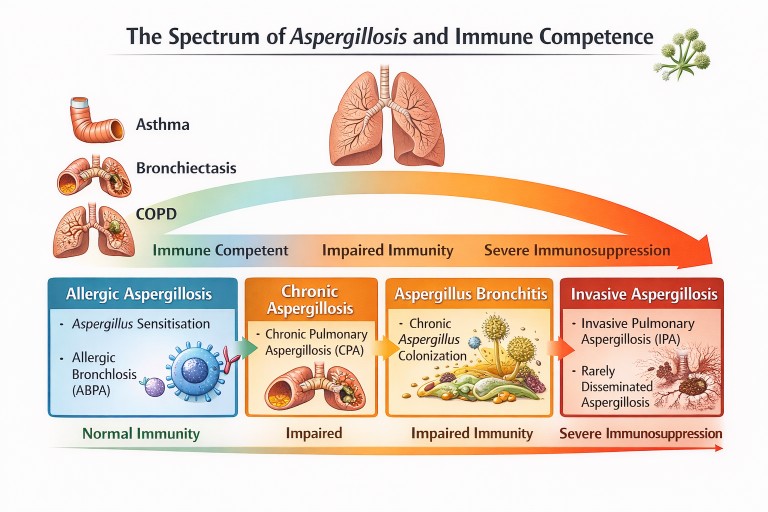
Different forms of aspergillosis occur depending on lung damage and immune function.
Other Lung Diseases Linked to Aspergillus
Although asthma is the most common condition associated with Aspergillus allergy, several other lung diseases can predispose to fungal disease.
Bronchiectasis
Dilated airways trap mucus, allowing fungi and bacteria to persist.
COPD
Chronic airway inflammation may lead to Aspergillus bronchitis or chronic pulmonary aspergillosis.
Tuberculosis
Post-tuberculosis lung cavities are the most common global cause of chronic pulmonary aspergillosis (PMID: 22271943).
Key Messages
-
Asthma is one of the most important diseases associated with Aspergillus-related lung conditions.
-
Many asthma patients develop fungal sensitisation.
-
A smaller proportion develop Allergic Bronchopulmonary Aspergillosis (ABPA).
-
Repeated inflammation from ABPA can lead to bronchiectasis.
-
Chronic pulmonary aspergillosis is rare in asthma alone but may occur if significant lung damage develops.
Understanding these interactions helps guide diagnosis and treatment for people living with asthma and Aspergillus-related disease.
Further reading
Agarwal R, Chakrabarti A, Shah A, Gupta D, Meis JF, Guleria R, Moss R, Denning DW; ABPA complicating asthma ISHAM working group. Allergic bronchopulmonary aspergillosis: review of literature and proposal of new diagnostic and classification criteria. Clin Exp Allergy. 2013 Aug;43(8):850-73. doi: 10.1111/cea.12141. PMID: 23889240.
Denning DW, Pleuvry A, Cole DC. Global burden of chronic pulmonary aspergillosis as a sequel to pulmonary tuberculosis. Bull World Health Organ. 2011 Dec 1;89(12):864-72. doi: 10.2471/BLT.11.089441. Epub 2011 Sep 27. PMID: 22271943; PMCID: PMC3260898.
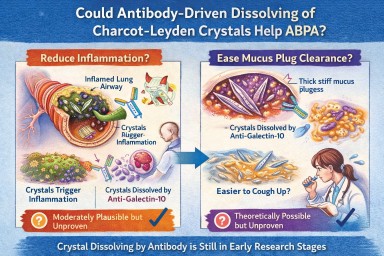
🧬 Could Antibody-Driven Dissolving of Charcot–Leyden Crystals Help ABPA?
Researchers have recently discovered that Charcot–Leyden crystals (CLCs) — the needle-shaped structures formed from the eosinophil protein galectin-10 — are not just debris.
In laboratory studies, specially designed antibodies can dissolve these crystals.
This has raised two important questions:
-
Could dissolving the crystals reduce airway inflammation?
-
Could dissolving them make mucus plugs easier to clear?
Here is what we currently know.
1️⃣ Could dissolving crystals reduce airway inflammation?
What we know
Laboratory and animal studies have shown:
-
Charcot–Leyden crystals can activate immune cells (especially macrophages).
-
They can stimulate inflammatory pathways (including inflammasome signalling).
-
In mouse models, antibodies targeting galectin-10 dissolved the crystals.
-
When crystals were dissolved, airway inflammation decreased.
This suggests that the crystals themselves may amplify inflammation, rather than simply mark it.
What this means biologically
In ABPA and eosinophilic asthma:
-
Eosinophils release galectin-10.
-
Galectin-10 crystallises.
-
Crystals may trigger further immune activation.
-
That leads to more inflammation → more eosinophils → more crystals.
Dissolving the crystals could theoretically interrupt this feedback loop.
How likely is this to help inflammation in humans?
Moderately plausible, but not yet proven.
The biological mechanism is strong.
The animal data are encouraging.
But no human clinical trials have yet shown reduced inflammation through crystal dissolution.
If developed successfully, this approach could:
-
Reduce airway immune activation
-
Lower exacerbation risk
-
Potentially reduce steroid dependence
But at present, it remains investigational.
2️⃣ Could dissolving crystals make mucus plugs easier to cough up?
This is more speculative — but still biologically reasonable.
Why mucus plugs are so thick in ABPA
ABPA mucus plugs contain:
-
Gel-forming mucins
-
DNA from inflammatory cells
-
Dead cells
-
Fungal fragments
-
Eosinophil proteins
-
Charcot–Leyden crystals
The crystals are:
-
Rigid
-
Needle-shaped
-
Structurally stable
When embedded in mucus, they likely increase:
-
Mechanical stiffness
-
Plug density
-
Resistance to deformation
From a physics perspective:
Removing rigid crystalline structures from a gel should reduce stiffness and improve flow.
Do we have direct evidence?
No.
There are currently:
-
No human studies measuring mucus clearance after crystal dissolution
-
No trials showing improved plug expectoration from crystal-targeting therapy
So while it is plausible that dissolving crystals could soften plugs, this has not yet been demonstrated in patients.
3️⃣ How strong is the overall case?
| Outcome | Evidence strength | Likelihood |
|---|---|---|
| Reduced inflammation | Strong biological rationale + animal data | Moderately promising |
| Easier mucus clearance | Biophysical plausibility only | Possible but unproven |
Inflammation reduction is the more evidence-supported target.
Improved plug clearance is plausible but currently theoretical.
4️⃣ How does this compare to existing treatments?
Current therapies (e.g., anti-IL-5 biologics) reduce eosinophils upstream.
That leads to:
-
Less galectin-10 release
-
Fewer crystals forming
-
Reduced inflammation
-
Often improved mucus plugging
So biologics already indirectly reduce crystal burden.
A crystal-dissolving antibody would act downstream, targeting the structural product directly.
This could theoretically:
-
Accelerate resolution of existing plugs
-
Reduce residual inflammatory signalling
But again, this remains in early research stages.
5️⃣ Practical take-home message
At present:
-
Dissolving Charcot–Leyden crystals reduces inflammation in animal models.
-
It is biologically plausible that this could also soften mucus plugs.
-
There is no human clinical proof yet.
-
No approved therapy currently targets the crystals directly.
The concept is scientifically credible — but still under development.
🔭 The Bigger Picture
ABPA is increasingly understood as a condition driven by:
-
Eosinophils
-
Allergic immune signalling
-
Abnormal mucus biology
-
Structural plug formation
Crystal-targeting therapies may eventually become part of a more precise approach to treating eosinophilic airway disease.
But for now, they remain a promising research direction rather than a clinical option.
🔬 Charcot–Leyden Crystals in ABPA and Asthma
What are they? Why do they form? Do they matter?
If you live with Allergic Bronchopulmonary Aspergillosis (ABPA) or severe asthma, you may see the term Charcot–Leyden crystals in a sputum or pathology report.
They can sound worrying.
They are:
-
Not fungus
-
Not infection
-
Not cancer
They are a sign of a particular type of allergic inflammation in the airways.
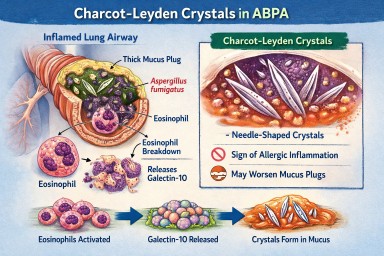
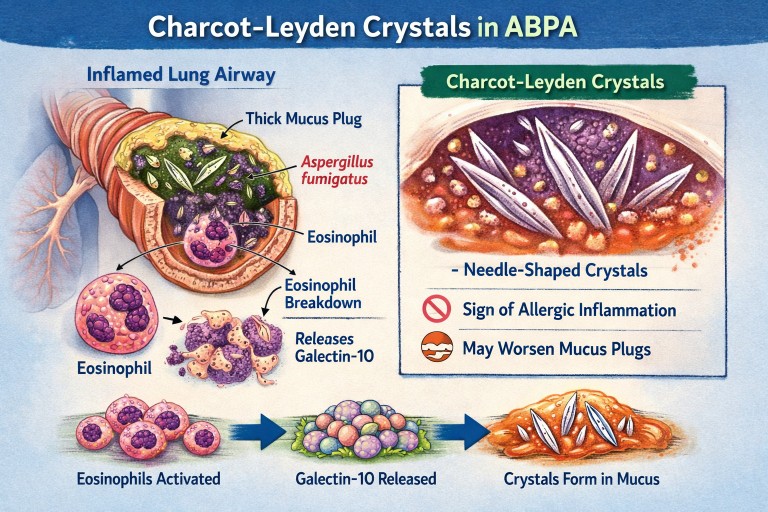
🧬 What Are Charcot–Leyden Crystals?
Charcot–Leyden crystals are microscopic, needle-shaped structures found in mucus.
They are made from a protein called galectin-10, which is stored inside a type of white blood cell called an eosinophil.
Eosinophils are immune cells involved in:
-
Allergic asthma
-
ABPA
-
Severe asthma with fungal sensitisation
-
Parasitic infections
When eosinophils are activated and break down, they release galectin-10.
If enough of this protein accumulates in thick airway mucus, it crystallises into visible crystals.
So the crystals are made from your immune cells, not from Aspergillus.
🫁 Why Do They Appear in ABPA?
In ABPA:
-
The immune system overreacts to Aspergillus fumigatus.
-
This triggers a strong allergic (Type 2) immune response.
-
Large numbers of eosinophils move into the airways.
-
Eosinophils break down and release galectin-10.
-
The protein crystallises inside mucus plugs.
The crystals are therefore a footprint of intense allergic inflammation, not fungal invasion.
🌡 Is Most ABPA Eosinophilic?
Yes — almost all classical ABPA is eosinophilic.
ABPA is fundamentally a Type 2 allergic condition, driven by immune pathways involving:
-
IL-4
-
IL-5
-
IL-13
-
IgE
-
Eosinophils
IL-5 in particular stimulates eosinophil production and survival.
Because of this, eosinophils are central to the disease process.
Historically, raised blood eosinophils have been part of diagnostic criteria.
However:
-
Eosinophil counts can fluctuate
-
Steroids can suppress blood levels
-
Eosinophils may still be present in airway mucus even if blood counts appear normal
So ABPA is biologically eosinophilic — even if a single blood test does not show a high count.
True non-eosinophilic ABPA would be unusual and would prompt clinicians to reconsider the diagnosis.
❓ Are Crystals Caused by Aspergillus Infection?
No.
They are caused by the immune reaction to Aspergillus — not by the fungus itself.
They can also be seen in:
-
Severe eosinophilic asthma
-
Parasitic infections
-
Other allergic lung conditions
They reflect eosinophil activity, not fungal growth.
🧠 Why Don’t All People with Asthma Develop These Crystals?
Asthma is not one single disease. It has different inflammatory patterns.
Type 2 (Eosinophilic) Asthma
This involves high eosinophils and allergic pathways.
Common in:
-
Allergic asthma
-
ABPA
-
Severe eosinophilic asthma
These patients can develop Charcot–Leyden crystals.
Non–Type 2 (Non-Eosinophilic) Asthma
This includes:
Neutrophilic asthma
Driven by neutrophils rather than eosinophils.
Paucigranulocytic asthma
Very few inflammatory cells present.
In these forms:
-
Eosinophils are low
-
Galectin-10 is not released in large amounts
-
Crystals are unlikely to form
🧱 Do Charcot–Leyden Crystals Make Mucus Plugs Worse?
Possibly.
Research suggests they may:
-
Increase mucus thickness
-
Contribute mechanically to airway blockage
-
Stimulate further inflammation
For many years they were thought to be harmless debris.
Modern studies suggest they may actively amplify inflammation when present in large amounts.
🎯 Do They Have a Purpose?
Eosinophils evolved mainly to help fight parasitic infections.
Galectin-10 probably has immune signalling roles inside cells.
However, when large amounts are released into thick airway mucus, crystallisation appears to be a by-product of excessive immune activity rather than a useful defence.
In ABPA and allergic asthma, they are more likely part of the problem than part of the solution.
💧 Can Their Formation Be Reduced?
Hydration alone does not stop them forming.
Drinking fluids helps:
-
Keep mucus less sticky
-
Support airway clearance
But it does not prevent eosinophils releasing galectin-10.
What reduces crystal formation?
Reducing eosinophilic inflammation:
-
Corticosteroids
-
Anti-IL-5 biologics
-
Anti-IL-4/IL-13 biologics
When eosinophil numbers fall:
→ Less galectin-10 is released
→ Fewer crystals form
Antifungal treatment in ABPA may indirectly help by reducing allergic stimulation, but the main driver is the immune response.
📊 Do They Change Treatment?
Not directly.
Doctors base treatment on:
-
Symptoms
-
Blood eosinophils
-
Total IgE
-
Imaging
-
Lung function
-
Exacerbation history
Crystals support the diagnosis of eosinophilic inflammation but do not determine treatment alone.
🔎 What Do They Tell Us?
Charcot–Leyden crystals tell us:
-
The airway inflammation is eosinophilic.
-
The immune response is strongly allergic.
-
Mucus plugging risk may be higher.
They are a marker of immune overreaction, not infection severity.
🧠 Key Points to Remember
-
They are made from proteins released by eosinophils.
-
They are not Aspergillus.
-
They do not mean invasive fungal infection.
-
Most classical ABPA is eosinophilic.
-
They are unlikely in non-eosinophilic asthma.
-
Reducing eosinophils reduces their formation.
-
Hydration helps clearance but does not prevent formation.
In simple terms:
Charcot–Leyden crystals are microscopic signs that the immune system is working too hard in the airways.
Airways mucus and aspergillosis
A clear, patient-friendly explainer
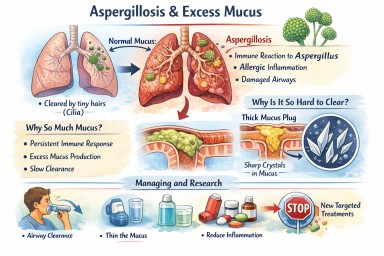
People living with aspergillosis often say that mucus is one of the hardest symptoms to manage — thick sputum, coughing fits, plugs that feel “stuck”, and flare-ups that seem to come out of nowhere. This explainer brings everything together in one place: what mucus is for, why aspergillosis causes so much of it, why it becomes abnormal, and what current and future treatments aim to do.
1. What is airway mucus and why do we need it?
Mucus is normal, healthy, and essential. Everyone produces it all the time.
Its main roles are to:
-
Trap inhaled particles (dust, spores, bacteria, pollution)
-
Protect the airway lining from drying and irritation
-
Support the immune system
-
Clear the lungs, using tiny moving hairs (cilia) that sweep mucus upwards so it can be swallowed or coughed out
(this clearance system is called the mucociliary escalator)
In healthy lungs:
-
Mucus is thin
-
Produced in small amounts
-
Cleared without you noticing it
2. Why aspergillosis causes excessive mucus
In aspergillosis, the lungs are under ongoing stress. Several factors combine:
Persistent immune activation
The immune system keeps reacting to Aspergillus material in the airways. Even when the fungus is controlled, inflammation can persist.
Allergic-type inflammation (especially in ABPA)
Allergic immune responses strongly stimulate mucus-producing cells, leading to:
-
Large volumes of mucus
-
Very sticky or rubbery sputum
Airway damage
Conditions commonly associated with aspergillosis (such as bronchiectasis or long-standing asthma) cause:
-
Widened or damaged airways
-
Poor mucus clearance
-
Pools of mucus that are hard to shift
Slowed clearance
Inflammation and infection impair cilia, so mucus:
-
Moves more slowly
-
Sits in the lungs longer
-
Becomes thicker and harder to clear
➡️ What starts as a protective response becomes a self-perpetuating problem.
3. Why thick mucus causes symptoms
Excess or abnormal mucus can:
-
Block airways → breathlessness and wheeze
-
Trigger coughing → especially overnight or on waking
-
Trap infection → repeated flare-ups
-
Reduce oxygen exchange
-
Increase fatigue and chest discomfort
Many patients describe it as:
“Glue-like”, “stringy”, “rubbery”, or “impossible to move”
4. Mucus plugs and crystals – why some mucus is so hard to clear
Mucus plugs
When mucus becomes very thick, it can:
-
Form plugs that partially or completely block airways
-
Show up on CT scans
-
Worsen breathlessness suddenly
Charcot–Leyden crystals
In allergic and eosinophilic airway disease (including allergic bronchopulmonary aspergillosis):
-
Breakdown products of allergic immune cells can form microscopic crystals
-
These crystals make mucus:
-
Stiffer
-
More irritating
-
Harder to clear
-
Their presence is a sign of ongoing allergic inflammation, not infection alone.
5. Why managing mucus really matters
Mucus is not just an inconvenience. Poor mucus control can:
-
Increase infection risk
-
Drive repeated exacerbations
-
Worsen lung damage over time
-
Reduce quality of life and sleep
-
Increase hospital admissions
For aspergillosis, mucus management is core treatment, not optional.
6. What helps now (current approaches)
A. Thin the mucus
-
Good hydration
-
Nebulised saline (normal or hypertonic)
-
Selected mucolytic medicines (used carefully)
B. Move it out
-
Regular airway clearance physiotherapy
-
Breathing techniques (e.g. active cycle breathing)
-
Oscillating devices (flutter, Acapella, Aerobika)
-
Gentle, regular physical activity where possible
C. Reduce inflammation
-
Inhaled corticosteroids (when appropriate)
-
Oral steroids (used cautiously)
-
Biologic therapies for selected allergic or eosinophilic disease
-
Antifungal treatment when fungal burden is contributing
D. Treat infections early
-
Bacterial infections thicken mucus further
-
Prompt treatment reduces long-term damage
7. What research is doing differently (emerging therapies)
Research is moving beyond simply “loosening mucus”.
1. Reducing mucus production at source
Scientists are developing drugs that aim to:
-
Switch off excessive mucus secretion
-
Preserve normal protective mucus
This targets the mucus-producing cells directly.
2. Blocking the signals that drive over-production
Inflammation sends chemical signals telling airways to make more mucus. New treatments aim to:
-
Calm allergic and immune pathways
-
Prevent expansion of mucus-producing cells
Some current biologic therapies already reduce mucus indirectly; future drugs will be more precise.
3. Changing mucus structure
Instead of thinning everything, researchers are studying ways to:
-
Loosen the internal “mesh” of mucus
-
Prevent dense plugs from forming
-
Restore normal movement by cilia
4. Targeting mucus crystals
In allergic aspergillosis, research is exploring how to:
-
Reduce crystal formation
-
Calm the specific immune responses that create them
5. New inhaled and physical approaches
Early trials are testing:
-
Inhaled therapies designed to mobilise secretions
-
Treatments that improve airflow behind mucus plugs
6. Precision medicine
Future mucus treatments are likely to be:
-
Personalised
-
Based on inflammation type, fungal involvement, airway damage, and immune markers
Two people with aspergillosis may have very different mucus drivers — and need different solutions.
8. What this means for patients today
-
There is no single “anti-mucus cure” yet
-
Promising therapies are in research and early trials
-
Safety and long-term effects must be proven first
For now:
-
Regular airway clearance remains essential
-
Treating inflammation and infection promptly is crucial
-
Understanding why your mucus behaves as it does helps guide treatment
Key messages to remember
-
Mucus is normally protective
-
Aspergillosis turns a helpful system into a problem
-
Thick, sticky mucus reflects ongoing inflammation and airway damage
-
Crystals signal allergic involvement, not just infection
-
Research is moving toward preventing abnormal mucus formation, not just thinning it
⭐ Severe Asthma with Fungal Sensitisation (SAFS): The Hidden Burden Behind Difficult Asthma
Estimated prevalence: 15–30% of severe asthma patients show fungal sensitisation.
Severe Asthma with Fungal Sensitisation (SAFS) describes a group of patients with severe asthma who show sensitisation (allergy) to Aspergillus or other environmental moulds but do not meet criteria for ABPA. These patients often experience persistent inflammation, breathlessness, mucus production, and exacerbations that are not adequately controlled by standard asthma therapies.
Although SAFS is common in severe asthma clinics, it remains poorly recognised, frequently mislabelled, and rarely discussed in routine practice. Yet identifying SAFS is crucial because it opens the door to specific interventions — including antifungals or targeted biologics — that can improve symptoms and reduce hospital admissions.
⭐ How Common Is SAFS?
SAFS is more common than ABPA and CPA combined in asthma services.
| Population | Estimated prevalence |
|---|---|
| Moderate asthma | ~5% |
| Severe asthma | 15–30% |
| Patients with frequent exacerbations | up to 40% |
| ABPA-negative patients with mucus plugging | high likelihood |
Across the UK, this represents tens of thousands of people.
⭐ Why SAFS Is Missed
1. The diagnosis is not widely understood
Unlike ABPA or CPA, SAFS lacks:
-
universally agreed diagnostic criteria
-
clear imaging features
-
a single confirmatory test
This leads to variability in thinking and detection.
2. Symptoms mimic uncontrolled asthma
SAFS patients typically experience:
-
severe breathlessness
-
wheeze
-
mucus production
-
airway plugging
-
poor response to inhalers
-
frequent steroid courses
These appear indistinguishable from “difficult” or “type 2–high” asthma.
3. IgE and eosinophils may be normal
Unlike ABPA:
-
total IgE may be modest
-
Aspergillus IgE may be borderline
-
eosinophils may fluctuate, especially with steroids or biologics
Clinicians are often looking for very high IgE levels — but SAFS patients usually don’t show them.
4. Sputum and CT scans appear non-specific
Typical imaging:
-
mucus plugging
-
small-airway thickening
-
variable, patchy inflammation
-
bronchiectasis may or may not be present
Radiologists often report these changes as:
-
“consistent with asthma”
-
“post-infective”
-
“non-specific inflammatory pattern”
5. The fungal link is overlooked
Many clinicians are unfamiliar with:
-
the role of mould exposure
-
sensitisation thresholds
-
the overlap between environmental allergy and airway disease
-
when antifungals are appropriate
This leads to delays in recognising fungal-driven asthma.
⭐ Who Is at Highest Risk?
1. Severe asthma patients unresponsive to maximal inhaled treatment
Particularly those with:
-
frequent exacerbations
-
nocturnal symptoms
-
long-term steroid use
-
persistently low lung function
-
mucus plugging events
2. Patients sensitised to Aspergillus or multiple moulds
Positive skin tests or specific IgE indicate airway allergy that can drive symptoms.
3. Patients with damp or mould exposure at home or work
An important environmental factor often overlooked.
4. ABPA-negative asthma patients with mucus plugging
A large proportion of these patients fit the SAFS profile.
5. Those with co-existing bronchiectasis
Bronchiectasis amplifies the inflammatory response to fungal exposure.
⭐ Specialties That Need Greater Awareness
-
Severe asthma services & biologics clinics
(primary diagnostic opportunity) -
General respiratory clinics
-
Primary care & urgent care
(patients seen frequently with “persistent asthma symptoms”) -
Radiology
(important for identifying mucus plugging) -
Allergy/Immunology
(mould sensitisation is central to diagnosis) -
Environmental health teams
(exposure to mould and dampness often perpetuates symptoms)
The National Aspergillosis Centre can provide specialist input when diagnosis is unclear or response to treatment is suboptimal.
⭐ Red Flags Suggesting SAFS
1. Severe asthma poorly controlled despite maximal inhalers
Including biologics (omalizumab, mepolizumab, benralizumab, dupilumab, tezepelumab).
2. Sensitisation to Aspergillus fumigatus or multiple moulds
3. Repeated mucus plugging episodes
(or “sticky mucus” symptoms)
4. More than 2–3 steroid-treated exacerbations per year
5. Asthma + bronchiectasis
Even mild bronchiectasis increases fungal risk.
6. Symptoms triggered by damp/mould exposure
7. Persistent airway inflammation despite correct inhaler technique
⭐ Misdiagnoses That Delay Recognition
-
“Difficult asthma”
-
“Brittle asthma”
-
“Post-viral inflammation”
-
“Poor adherence to inhalers”
-
“Asthma–COPD overlap”
-
“Psychogenic dyspnoea”
-
“Recurrent chest infections”
SAFS is a diagnosis hiding in these labels.
⭐ The Cost of Missed SAFS Diagnosis
For patients:
-
persistent symptoms
-
steroid dependence
-
increased risk of ABPA
-
progressive airway damage
-
hospital admissions
-
poor quality of life
-
possible career and lifestyle impact
For healthcare systems:
-
repeated A&E visits
-
asthma admissions
-
high biologic usage without adequate response
-
unnecessary antibiotics
-
escalating steroid toxicity
-
missed environmental interventions
⭐ Conclusion
SAFS is one of the most common — yet least recognised — fungal-related lung conditions. Although it lacks the dramatic imaging changes of ABPA or CPA, its impact on patients is profound.
Recognising mould sensitisation in severe asthma, understanding the role of fungal allergens, and considering targeted therapies can transform disease control. For complex cases or when the diagnosis is uncertain, referral to the National Aspergillosis Centre is recommended.
Early identification and appropriate treatment reduce steroid use, exacerbations, and long-term airway damage.
🌲 Why Rough-Cut Wood Arrives Mouldy — and How to Reduce the Risk (Important for Aspergillosis Patients)
For anyone living with aspergillosis, ABPA, bronchiectasis or asthma, mould exposure can trigger symptoms or flares. Recently, several patients have reported that rough-cut timber is arriving mouldy from DIY suppliers, sawmills, or timber merchants.
Here’s why this happens — and what suppliers should be doing to prevent it.
⭐ Why rough-cut wood gets mouldy (especially in the UK)
Mould grows on timber whenever three conditions are present:
-
Moisture
-
Poor airflow
-
Warm or humid air
Rough-cut timber is especially vulnerable because:
-
its uneven surface holds moisture,
-
it is often stacked tightly,
-
it may not be dried properly,
-
and UK weather (rain + high humidity) encourages mould.
Many suppliers wrap wood in plastic, which traps condensation during transport. This can create a humid “greenhouse” around the timber — perfect for mould growth in only 24–48 hours.
⭐ What UK suppliers should be doing (even for low-cost timber)
These are standard industry practices in UK timber yards and sawmills. None of them require wood to be kiln-dried (which is more expensive).
✔ 1. Air-dry properly (“sticker stacking”)
Boards must be stacked with spacers (“stickers”) between them so air can circulate.
No airflow = mould.
✔ 2. Store under cover, not outside in the rain
A simple open-sided shelter is enough.
Rain-soaked timber nearly always grows mould in transit.
✔ 3. Use breathable wrapping — NOT plastic sheeting
Plastic traps moisture.
Breathable paper wrap or perforated cover prevents condensation build-up.
✔ 4. Apply anti-fungal dip (borate)
Most UK sawmills use anti-mould dips to prevent blue-stain and mould during storage.
This costs pennies per board.
✔ 5. Moisture-test before delivery
A good supplier will check wood is below 20–22% moisture before dispatch.
Wet wood + UK weather = guaranteed mould.
⭐ Kiln drying is not essential
Kiln-dried timber is more expensive because it uses energy, equipment, and time to force-dry the wood.
But you do not need kiln-dried timber to avoid mould.
You simply need a supplier who:
-
stores the timber properly,
-
allows airflow,
-
avoids plastic,
-
and checks moisture before delivery.
If rough-cut wood is arriving mouldy, it usually means these steps were not followed.
⭐ What you can do to protect yourself (aspergillosis patients)
If you receive wood that:
-
smells musty,
-
has surface mould,
-
or shows green/black spots,
…it is best not to bring it indoors until cleaned.
✔ Immediately unwrap outdoors
Plastic wrapping traps mould spores.
✔ Keep well away from ventilation intakes, windows, or living areas
This avoids airborne spores entering the home.
✔ If mould is visible — return it
You have the right to reject mouldy timber.
✔ If keeping it, clean outdoors with PPE
Use:
-
gloves
-
FFP3 mask
-
borax solution (borax + hot water)
to remove early surface mould.
Never sand mould indoors — sanding releases spores.
⭐ Simple Diagram: Correct Way to Store Wood to Prevent Mould
Correct storage includes:
-
boards stacked with spacers between them (“sticker stacked”),
-
raised on bearers above the ground,
-
stored under a roof with airflow on all sides,
-
NEVER wrapped in sealed plastic,
-
ends exposed to allow moisture to escape.
This method is cheap, simple, and prevents mould without needing expensive kiln drying.
⭐ Summary for Aspergillosis Patients
Rough-cut wood should not arrive mouldy.
Mould growth usually means it was:
-
stacked badly,
-
stored wet,
-
wrapped in plastic,
-
or shipped before drying.
For people with aspergillosis, ABPA, bronchiectasis or severe asthma, mould spores can trigger symptoms — so it’s completely reasonable to:
-
refuse mouldy timber,
-
request proper handling,
-
or ask the supplier to follow UK best practice.
🌬️ Breathing Easier: Keeping Your Air Clean at Home, Work and When Travelling
People with lung conditions such as aspergillosis, asthma, or bronchiectasis often find their symptoms worsen in certain environments — especially where the air feels dusty, damp, or polluted.
The good news is that there are simple, practical steps you can take to control your surroundings, reduce flare-ups, and make your home a safer, healthier place to breathe.
🏠 At Home
Keep It Dry and Well-Ventilated
-
Tackle damp and leaks early. Mould thrives in moist places — even hidden behind furniture or under wallpaper.
-
Trust your nose. If something smells damp, it probably is. A musty smell means moisture is trapped somewhere — investigate and dry it before mould can grow.
-
Ventilate daily. Open windows when outdoor air is clean, or use extractor fans in kitchens and bathrooms.
-
Prevent moisture spreading. When showering, cooking, or drying laundry, close doors to other rooms so steam and humidity don’t spread through the house.
-
Run the extractor fan during and for at least 15–20 minutes afterwards, or until humidity drops.
-
Short humidity spikes are normal. It’s common for relative humidity (RH) to rise above 60% during cooking, showering, or drying clothes — what matters is that it returns below 60% quickly once fans or windows are open.
-
If condensation lingers or humidity stays high for more than 30–40 minutes, increase ventilation or use a dehumidifier.
-
-
Use humidity-sensing extractor fans. These switch on automatically when humidity rises and off when it falls.
-
Choose one with a humidistat and timer, vented directly outdoors (not into a loft or wall cavity).
-
Clean the fan cover and check filters every few months.
-
-
Dry laundry safely. Use a vented or condenser tumble dryer and empty or clean filters and tanks regularly.
-
Avoid drying clothes on radiators unless you’re using a dehumidifier or have good airflow.
-
-
Monitor humidity. Use a small digital hygrometer to track RH in different rooms.
-
Aim for 40–60% most of the time — this discourages mould and keeps air comfortable.
-
Above 60% for long periods encourages condensation and spores; below 35% can dry and irritate airways.
-
-
Use the right size dehumidifier.
-
Check the model’s rated room area (m²) or litres per day extraction rate.
-
A compact unit may cope with a small bedroom or bathroom but not a whole flat or open-plan area.
-
Keep doors closed while it’s running for best results, and empty and clean the water tank regularly to prevent bacterial build-up.
-
Control Dust and Irritants
-
Vacuum regularly with a HEPA-filtered vacuum cleaner.
-
Use microfibre cloths for dusting rather than dry dusters that stir particles into the air.
-
Avoid strongly fragranced cleaning products, candles, incense, and air fresheners — they release fine particles and chemicals that irritate sensitive lungs.
-
Choose low-VOC (low-odour) paints and furnishings when redecorating.
Keep Air Clean
-
If you live near traffic or building work, keep windows closed during busy times and ventilate later.
-
A room air purifier with a true HEPA filter can remove dust, pollen, and fungal spores effectively.
-
Choose the right size for your room.
-
Check the purifier’s Clean Air Delivery Rate (CADR) or maximum room coverage and ensure it matches or slightly exceeds your room size.
-
A small desktop purifier won’t clean a large living room or bedroom effectively.
-
For open-plan or high-ceiling spaces, you may need more than one unit.
-
-
Maintain it properly:
-
Replace or clean filters exactly as the manufacturer recommends (usually every 6–12 months).
-
Never wash or vacuum a disposable HEPA filter unless the manual allows it.
-
A clogged or undersized filter won’t clean air effectively and may re-release particles.
-
🌤️ Knowing When the Outside Air Is Clean — and How to Filter It Indoors
1. Check Air Quality Before Ventilating
It isn’t always obvious when outdoor air is safe to bring inside.
Modern air-quality data helps you choose the best times to open windows or run fans.
How to check:
-
Use free apps such as Air Quality Index (AQI) UK, Breezometer, Plume Labs, or AirVisual.
-
Visit DEFRA’s UK Air Information or check BBC Weather → Air Quality.
-
Look for PM2.5 (fine particles) and NO₂ (traffic pollution) levels — these are key irritants for sensitive lungs.
-
“Good” or “Low” readings mean it’s a good time to ventilate or air rooms.
-
Avoid opening windows near busy roads during rush hour or when pollution alerts are issued.
💡 Tip: Air quality is often better early in the morning or late in the evening when traffic and heat are lower.
2. Filter the Air as It Comes In
If you live near roads, building work, or farmland, you can reduce what enters while keeping ventilation safe:
🪟 Window Vent Filters
-
Many modern trickle vents can take fine mesh or electrostatic filters to trap pollen, dust, and spores.
-
Replace or wash filters regularly — clogged filters restrict airflow.
🌀 Filtered Ventilation Systems
-
MVHR systems (Mechanical Ventilation with Heat Recovery) pull in outdoor air, filter it, and expel stale indoor air — great for energy-efficient or damp-prone homes.
-
They help control humidity and filter pollutants.
-
Filters must be cleaned or replaced every few months.
-
-
Positive Input Ventilation (PIV) systems bring in filtered air gently from a roof or external vent, improving airflow and reducing condensation.
🧺 DIY Improvements
-
Clip-on intake filters can fit over some wall vents or fan inlets.
-
Use a portable HEPA purifier placed near an open window to “clean” incoming air as it circulates.
-
Keep window ledges, vent grilles, and trickle vents dust-free — they collect spores over time.
3. Balance Fresh Air and Safety
It’s important not to seal up a home completely — stale, humid air encourages mould.
The goal is controlled ventilation:
-
Ventilate when outdoor air is cleanest and driest.
-
Keep extractor fans running during steamy activities.
-
When outdoor air quality is poor, use purifiers and dehumidifiers indoors until it improves.
4. Low-Cost Monitoring at Home
You can buy small indoor/outdoor air-quality monitors that track PM2.5, temperature, and humidity.
These help you:
-
Spot pollution drifting indoors (from traffic, wood smoke, etc.).
-
Choose the best times to ventilate.
-
See how quickly humidity or particles fall after cooking or cleaning.
🌱 Summary
| What to Do | Why It Helps |
|---|---|
| Check local air-quality apps before opening windows | Avoids letting polluted air inside |
| Ventilate during low-pollution hours | Brings in cleaner, fresher air |
| Fit filters to vents or use MVHR/PIV systems | Reduces dust and spores from incoming air |
| Clean vents, trickle filters, and window frames regularly | Prevents build-up of trapped dust |
| Use a portable HEPA purifier near open windows | Cleans incoming air in real time |
🧽 Dealing with Mould and Dust Safely
Even in well-kept homes, mould and dust can build up in damp weather or hidden corners. If you see black or green patches, or notice a musty smell, act promptly — but take care to protect your lungs.
⚠️ Before You Start
-
Protect yourself: wear a well-fitted FFP2 or N95 mask, gloves, and, if possible, eye protection.
-
Avoid dry brushing or vacuuming visible mould — this can spread spores into the air.
-
Keep the area well ventilated but close doors to other rooms so spores don’t travel.
-
If the mould covers more than 1 square metre, keeps returning, or is linked to a leak, ask your landlord or council for professional help.
🧴 Cleaning Small Areas of Mould
-
Wipe gently — don’t scrape.
Use disposable cloths or ones you can boil-wash later. Avoid wire brushes. -
Use mild cleaning solutions:
-
Mix a few drops of washing-up liquid in warm water, or
-
Use a dilute bleach solution (1 part thin bleach to 9 parts water) on tiles or uPVC — ventilate well and never mix bleach with other cleaners, or
-
Try a specialist anti-fungal cleaner for painted or porous surfaces.
-
-
Dry the area thoroughly.
Use ventilation or a dehumidifier; mould will return if the surface stays damp. -
Dispose of cloths and gloves in a sealed bag. Wash hands well afterwards.
🧹 Managing Dust and Allergens
-
Vacuum at least twice weekly with a HEPA-filtered cleaner.
-
Dust with a damp microfibre cloth, not a feather duster.
-
Wash bedding and soft furnishings regularly at 60 °C if the fabric allows.
-
Avoid clutter that collects dust (papers, books, soft toys).
-
Keep humidity within 40–60% and fix damp quickly.
🌱 Preventing Mould and Dust Returning
| Action | Why It Helps |
|---|---|
| Find and fix leaks or condensation sources | Mould needs moisture to grow |
| Ventilate kitchens, bathrooms, and drying areas | Removes steam before it spreads |
| Use humidity-sensing fans or dehumidifiers | Keeps humidity in a safe range |
| Maintain a steady indoor temperature | Reduces cold surfaces and condensation |
| Close doors during steamy activities | Stops damp air moving into other rooms |
| Replace or clean HEPA filters regularly | Maintains air-cleaning performance |
| Check behind furniture and on windowsills | Finds hidden damp early |
| Repaint cleaned areas with mould-resistant paint | Discourages regrowth |
🚫 What Not to Do
-
Don’t paint over mould — it will grow back.
-
Don’t use strong chemicals or foggers in small spaces — they can irritate lungs.
-
Don’t use steam cleaners on large mould patches — they can spread spores.
-
Don’t ignore damp smells — they always mean hidden moisture somewhere.
💼 At Work
-
Ask about ventilation and report any damp, leaks, or condensation.
-
Keep your workspace tidy and free of dust-collecting clutter.
-
If cleaning sprays or perfumes cause coughing, discuss adjustments with your manager or occupational health team.
✈️ When Travelling
-
Check air-quality forecasts before travelling and avoid outdoor activity on high-pollution or pollen days.
-
Choose clean, dry accommodation — avoid musty or damp-smelling rooms.
-
Pack a small hygrometer or travel dehumidifier for longer stays.
-
Use a well-fitted FFP2 or N95 mask in crowded or polluted environments.
-
Stay hydrated and pace activities in humid or hot weather.
🩺 Listen to Your Body
Keep a short diary of when and where your symptoms flare up, along with temperature, humidity, or smells you notice. Patterns often reveal your personal triggers.
🌱 Key Points
| Good Practice | Why It Matters |
|---|---|
| Keep home dry, clean, and ventilated | Reduces mould and spore exposure |
| If it smells damp, it probably is | Early warning of hidden moisture |
| Humidity above 60% after showering or cooking is normal — keep it short | Prevents condensation and mould |
| Close doors while cooking, showering, or drying laundry | Stops moisture spreading |
| Use humidity-sensing extractor fans | Clears steam automatically |
| Monitor humidity (40–60%) | Keeps air comfortable and discourages spores |
| Match HEPA filters and dehumidifiers to room size | Ensures real air-cleaning and drying effect |
| Maintain and replace filters regularly | Keeps air safe and fresh |
| Check outside air quality before opening windows | Avoids bringing pollution indoors |
| Filter incoming air with vents or MVHR/PIV systems | Keeps dust and spores out |
| Clean small mould patches safely with mild detergent | Removes spores without irritation |
| Fix leaks, repaint with mould-resistant paint | Prevents regrowth |
| Avoid strong scents and aerosols | Reduces airway irritation |
| Plan travel around clean-air days | Lowers risk of flares and infections |
💬 Final Thought
You can’t control every environment — but small, steady habits make a big difference.
If something smells damp, it probably is. Deal with it early, clean gently, dry thoroughly, and keep air moving.
Short humidity spikes after showering or cooking are normal — just make sure they don’t linger.
Choose purifiers and dehumidifiers that are the right size for your rooms, and maintain them well.
Check outdoor air quality before airing your home, and use filters to keep what’s good while blocking what’s not.
A dry, clean, well-ventilated home gives your lungs the best chance to stay healthy every day — wherever you are.
🧬 What IgE Is and Why It Matters
IgE is a type of antibody your immune system makes when it reacts to something it sees as harmful — such as pollen, mould, pet dander, or certain foods.
In people with allergic or fungal lung disease, IgE can rise sharply because the body’s immune system is over-reacting.
High IgE isn’t dangerous on its own, but it shows that your immune system is “switched on” and inflamed. The goal is to calm that inflammation and reduce exposure to what’s triggering it — not simply to force the number down.
✅ Best Practices for Reducing IgE Levels
1️⃣ Identify and Avoid Triggers
Reducing exposure is the first and most effective step.
-
Allergens: dust mites, moulds (especially Aspergillus), pollens, pets.
-
Environmental irritants: cigarette smoke, air pollution, strong odours, damp housing.
-
Use HEPA filters, good ventilation, and address damp or mould at home.
-
In ABPA, avoiding heavy exposure to fungal spores (e.g. gardening compost, rotting leaves, renovation dust) is particularly important.
2️⃣ Control Inflammation and Allergic Response
Because IgE is a marker of allergic inflammation, treatment focuses on calming the immune system:
-
Corticosteroids (oral or inhaled) can suppress inflammation and lower IgE over time.
-
Biologic therapies such as:
-
Omalizumab (Xolair) – directly targets IgE and lowers levels in allergic asthma or ABPA.
-
Mepolizumab, Benralizumab, or Dupilumab – reduce eosinophil-driven inflammation and may indirectly lower IgE.
-
Choice depends on your disease type and blood test results.
-
-
Antifungal therapy (e.g. itraconazole, voriconazole, posaconazole) can help reduce fungal load in ABPA and often leads to gradual IgE reduction as the reaction settles.
3️⃣ Manage Asthma or Lung Disease Well
Stable lungs mean fewer immune flares and less IgE activity:
-
Use prescribed inhalers regularly (preventers, not just relievers).
-
Follow your asthma or CPA action plan.
-
Attend regular reviews with your respiratory team.
-
Report any new symptoms such as increased cough, wheeze, or mucus plugs early.
4️⃣ Support Overall Immune Balance
Simple lifestyle steps can also help keep inflammation low:
-
Eat a balanced diet rich in fruit, vegetables, and omega-3 fats.
-
Sleep well and manage stress (both can worsen inflammation).
-
Avoid smoking or vaping.
-
Keep vaccinations (e.g. flu, COVID, pneumococcal) up to date.
📊 Interpreting IgE Levels
-
IgE levels naturally fluctuate and may take weeks or months to fall after treatment.
-
Doctors often look at the trend (rising or falling) rather than one number.
-
In ABPA, a fall of 35–50 % from baseline after treatment usually shows improvement.
-
It’s also possible to feel better while IgE remains high — so the result must always be interpreted alongside symptoms and scans.
🚫 What Not to Do
-
Don’t chase a “perfect” IgE number — focus on feeling better and reducing inflammation.
-
Don’t stop steroids or antifungals suddenly unless advised by medical doctor, as this can cause a rebound flare.
-
Don’t rely on supplements or “immune boosters” that claim to lower IgE — none are proven to help and some may worsen allergies.
🩺 In Summary
| Goal | Best Approach |
|---|---|
| Reduce IgE triggers | Avoid mould, dust, smoke, allergens |
| Calm inflammation | Steroids or biologics under medical supervision |
| Treat underlying disease | Antifungals for ABPA/CPA, good asthma control |
| Support immune balance | Healthy lifestyle, good sleep, stress reduction |
🌱 Key Message
You can’t “switch off” IgE completely — it’s part of your immune defence.
The aim is to reduce unnecessary immune activation, keep symptoms stable, and prevent lung damage.
With the right mix of trigger avoidance, anti-inflammatory treatment, and regular monitoring, IgE levels usually fall gradually as the condition improves.