Information on Allergic BronchoPulmonary Aspergillosis (ABPA) / SAFS – For Family and Friends
Print out or share electronically
WHAT IT IS
ABPA (Allergic Bronchopulmonary Aspergillosis) and SAFS (Severe Asthma with Fungal Sensitisation) are allergic reactions to a common fungus, Aspergillus. In some people with asthma, the immune system overreacts to spores in the air, causing inflammation, swelling, and mucus plugs in the lungs.
WHAT IT'S NOT
-
Not contagious – you can't catch it.
-
Not poor hygiene – Aspergillus is everywhere in the air.
-
Not the patient's fault – flare-ups happen because of the condition, not something they did or didn't do.
WHY AREN'T OTHERS AFFECTED?
Most people's lungs clear these spores easily. In ABPA/SAFS the immune system reacts too strongly – more likely with long-standing asthma, severe allergies, damaged airways (e.g., bronchiectasis), or a genetic tendency. It's not weakness or lifestyle choices – often just lung history and bad luck.
TYPICAL SYMPTOMS
-
Wheezing, cough (sometimes with mucus plugs)
-
Breathlessness
-
Severe fatigue
-
Sometimes coughing up blood
WORST SYMPTOMS
-
Mucus plugs – thick, sticky clumps blocking airways, making breathing suddenly harder.
-
Intense coughing – can be exhausting, cause chest pain, and disrupt sleep.
TREATMENT
-
Anti-inflammatory medicines (often steroids)
-
Antifungals to reduce Aspergillus in the airways
-
Biologics for severe asthma/allergic inflammation
-
Monitoring with blood tests, breathing tests, and scans
THE REALITY
This condition can dominate daily life. On bad days the person may not be able to do much at all. Energy and breathing can change day-to-day (even hour-to-hour). If plans are cancelled, it isn't a lack of interest – it's the illness. Flare-ups can also make people feel short-tempered – a natural reaction to frustration, not a lack of care. Many people also live with a constant awareness of environmental risks – weighing up every new place or activity for dust, damp, or spores. This can feel exhausting and may lead them to avoid situations that others wouldn’t think twice about.
LOOKING AHEAD
-
With good control – Many people manage their symptoms well, reduce flare-ups, and keep active with the right treatment and avoidance of triggers.
-
Risks – Without good control, repeated flare-ups can slowly damage the lungs and lead to bronchiectasis.
-
Change over time – Some improve and need less treatment; others have ongoing ups and downs. Early action on flare-ups makes a big difference.
ENVIRONMENTAL TRIGGERS & PROTECTION
Some people with ABPA or SAFS have to avoid dust, mould, strong smells, smoke, and damp places – these can trigger flare-ups. Activities like gardening, compost turning, or DIY can be risky because they release fungal spores into the air. Wearing a well-fitting mask (e.g., FFP2/FFP3) can help reduce exposure – it's about staying well, not being antisocial.
HOW FRIENDS AND FAMILY CAN BEST HELP
-
Be flexible with plans – energy and breathing can change suddenly; last-minute cancellations aren't personal.
-
Help avoid triggers – choose low-dust, low-mould venues and activities.
-
Support treatment routines – lifts to appointments, collecting prescriptions, or reminders if welcome.
-
Listen without judgement – let them share symptoms and frustrations.
-
Encourage safe activities – suggest hobbies and outings with low environmental risk.
-
Show affection and reassurance – a hug, a kind message, or checking in can mean a lot.
MORE INFORMATION & SUPPORT
National Aspergillosis Centre (UK): https://mft.nhs.uk/wythenshawe/services/infectious-diseases/national-aspergillosis-centre/
Patient information & community: https://aspergillosis.org
🧵 Why Am I Getting More “Plugs” This July?
A message for aspergillosis patients
July is often a time when people with aspergillosis feel a bit better — but sometimes, things don’t go quite to plan. If you’ve suddenly started getting more mucus “plugs” or are struggling to clear your chest, here are some possible reasons:
🔍 Common Reasons for More Mucus or Plugs in Summer
| Possible Cause | Why it might affect you now |
|---|---|
| Fungal spores are high | July and August bring very high outdoor levels of Aspergillus, Cladosporium, and other moulds – especially on dry, windy days or after cutting grass. These can trigger inflammation and more mucus. |
| Pollen season continues | Even though tree pollen has gone, grass, weed, and cereal pollen are still in the air. These can worsen symptoms for people with ABPA or asthma. |
| Humidity or storms | Sudden weather changes, humid air, or storms can make breathing more difficult and mucus harder to shift. Some people call this "thunderstorm asthma." |
| Air pollution (ozone) | Sunny weather increases ozone and air pollution – both can irritate your airways. |
| Low-level infection or flare-up | If your mucus is thicker, darker, or smells different, it might be a sign of a fungal or bacterial flare-up, even without a high temperature. |
| Hydration or medication changes | Less water, skipping nebulisers, or changes in routine can make mucus stickier. |
| Blocked sinuses | Post-nasal drip from fungal sinusitis can make it feel like mucus is always sitting in your throat or upper chest. |
✅ What You Can Do
-
Drink more fluids, especially warm water or squash
-
Use saline in your nebuliser to loosen thick mucus
-
Do your chest clearance exercises more often – flutter device, ACBT, or huffing
-
Don’t skip antifungals, inhalers, or mucolytics like carbocisteine
-
Consider a nasal rinse if your sinuses feel blocked
-
Keep windows closed on high spore or high pollen days
-
Speak to your team if things don’t settle – you may need a review or antibiotics
⚠️ When to Get Checked
-
You're coughing up yellow, green or brown mucus
-
Mucus smells bad or has blood in it
-
You feel more breathless or more tired
-
You’ve needed to increase your nebuliser use
💬 You're Not Alone
Many patients with aspergillosis get more mucus at this time of year — even when the sun’s out! Don’t assume it’s “just the weather.” Sometimes it’s a sign that your lungs or sinuses are reacting to invisible spores in the air.
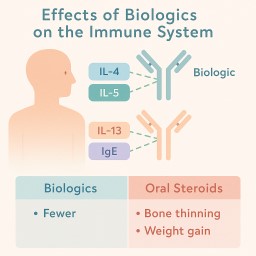
Biologics and Long Term Side Effects
✅ What Are Biologics?
Biologics are targeted treatments made from living cells. They work by blocking parts of the immune system that cause inflammation — for example:
-
IL-4, IL-5, IL-13: linked to eosinophilic inflammation
-
IgE: linked to allergies and ABPA
They are not immunosuppressants like steroids or chemotherapy, but rather immune modulators.
💊 Long-Term Side Effects – What Do We Know?
👨⚕️ What research and experience show:
| Biologic | Used for | Long-term safety known? | Side effects most reported |
|---|---|---|---|
| Omalizumab (Xolair) | Allergic asthma, ABPA | 20+ years of use | Injection site reactions, headache, very rare anaphylaxis |
| Mepolizumab (Nucala) | Eosinophilic asthma, CPA | 10+ years | Fatigue, headache, shingles (rare), mild infections |
| Benralizumab (Fasenra) | Severe asthma, CPA | ~6–7 years | Headache, pharyngitis, injection site issues |
| Dupilumab (Dupixent) | Asthma, eczema, nasal polyps | 6–8 years | Eye dryness/redness, cold sores, joint pain (rare) |
| Tezepelumab (Tezspire) | Severe asthma | ~2 years | Sore throat, joint pain, injection site reactions |
⚠️ Possible Long-Term Concerns (but rare)
-
Infections: Some concern about slightly increased risk of herpes zoster (shingles) or respiratory viruses, but overall risk is very low compared to steroids.
-
Immunogenicity: Your body might develop antibodies to the drug over time, reducing its effect — this is more a loss of benefit, not a dangerous side effect.
-
Cancer risk: No consistent evidence linking asthma/ABPA biologics to cancer.
-
Unknowns: Because some biologics are new (e.g. tezepelumab), we don't yet have 20-year data — but so far the safety profile is reassuring.
🩺 Compared to Oral Steroids
| Treatment | Side Effects Over Time |
|---|---|
| Steroids (e.g. prednisolone) | Weight gain, diabetes, infections, bone thinning, cataracts, adrenal suppression |
| Biologics | Mostly minor – injection site pain, headache, mild infection risk, rare allergic reaction |
So in most cases, biologics reduce the need for steroids and therefore reduce long-term harm.
💬 Patient Experience
Most patients report:
-
Improved quality of life
-
Reduced asthma/ABPA attacks
-
Fewer hospital visits
-
Very few stop due to side effects
✅ Summary
| Question | Answer |
|---|---|
| Do biologics have long-term side effects? | Usually mild and rare; mostly injection reactions or mild infections |
| Are they safer than long-term steroids? | Yes, especially over years |
| Should I be worried? | Not usually — but always monitor with your team |
| How long have they been used? | 6–20+ years, depending on the biologic, with very good safety data |
😷 Coping With Masks: Advice for People With Aspergillosis Who Struggle to Wear One
For people living with aspergillosis, asthma, or other lung conditions, wearing a facemask can sometimes feel uncomfortable — even frightening. You may feel like you can’t breathe properly, become hot or anxious, or feel claustrophobic. Some patients avoid masks altogether, even when they want to wear one to protect themselves from spores, pollution, or infection.
This guide is here to reassure you: you are not alone, and there are ways to make mask-wearing safer and more comfortable.
🫁 "I Can’t Breathe in a Mask" – Is This Normal?
Yes — many people with respiratory conditions feel this way. But here’s what the science tells us:
✅ For most people, even those with chronic lung disease, oxygen levels are not reduced by wearing a mask
❌ The feeling of not getting enough air is often caused by:
-
Anxiety or shallow breathing
-
The heat and humidity under the mask
-
The sensation of restricted airflow, not actual oxygen deprivation
💡 Helpful Tips If You Find Masks Difficult to Wear
1. Practise in a calm setting
Start wearing your mask for short periods at home, where you feel safe. Use calming breathing (slow in through the nose, out through the mouth). This helps your brain and lungs get used to the sensation.
2. Choose a mask that suits your needs
Different types of masks feel very different to wear.
| Problem | Suggested Mask |
|---|---|
| Feels suffocating or hot | Structured FFP2 or duckbill-style masks (keep shape off your face) |
| Claustrophobic | Surgical masks (lighter and looser fitting) |
| Strong reactions to smells or pollution | FFP2/FFP3 masks or Vogmask with carbon filter |
| Sweat or overheating | Lightweight cotton or disposable masks with cooling fabric or filter inserts |
3. Use your inhaler beforehand (if prescribed)
Some people with asthma or ABPA find wearing a mask easier after using their reliever inhaler (blue) 10–15 minutes beforehand.
4. Take breaks when needed
If you’re in a safe place (like outdoors, away from people), it’s okay to briefly lift your mask and take a few calm breaths — especially if you're struggling. You don't need to wear it all the time to benefit.
5. Try alternatives in low-risk settings
If you genuinely can’t tolerate a mask:
-
Wear one only in crowded indoor areas (shops, clinics, transport)
-
Consider using a face shield over a mask or in short exposures (note: shields protect others less)
-
Maintain distance and ventilation in mask-free spaces
🔁 Don’t Let One Bad Experience Stop You
Struggling to wear a mask doesn’t mean you’ve failed — it just means you need to try something different. Many patients find that with the right mask and some breathing strategies, they can use one when it matters most.
Remember, even wearing a mask for short periods (e.g. clinic waiting room, pharmacy queue) offers valuable protection.
🧠 Why It Matters for Aspergillosis
People with aspergillosis often need to avoid airborne risks like:
-
Fungal spores (especially Aspergillus fumigatus)
-
Pollution and chemicals
-
Viral infections that could worsen lung damage
Wearing a well-fitting FFP2 or FFP3 mask, especially in higher-risk situations, is one of the best ways to reduce exposure.
🤝 You're Not Alone
If you feel overwhelmed, isolated, or panicked when wearing a mask — you are not alone. Many others in the aspergillosis community feel the same way. With time, support, and the right mask, it often gets easier.
📝 Summary: What You Can Try
-
✅ Practise wearing a mask at home for short periods
-
✅ Try structured masks (like FFP2 duckbill) for better airflow
-
✅ Use a reliever inhaler beforehand if needed
-
✅ Take short breaks if it becomes too uncomfortable
-
✅ Don’t wear a mask all the time — just when it matters most
🛡️ FFP2/FFP3 Mask Use in Aspergillosis: Summary
| Mask Type | Who Might Use It | When It's Used |
|---|---|---|
| FFP2 (95% filtration) | Some patients with CPA, ABPA, or SAFS, especially during flares or hospital visits | During travel on public transport, clinic waiting rooms, visiting building sites, or dust exposure |
| FFP3 (99% filtration) | Patients who are severely immunocompromised (e.g. post-transplant, on chemotherapy, or high-dose steroids) | In high-risk environments: hospital construction, building work nearby, or heavy dust/mould exposure |
✅ When Masks Might Be Advisable
-
During hospital visits, particularly in winter or during flu/COVID waves
-
If you're immunosuppressed, e.g. taking long-term steroids or biologics
-
When exposed to mouldy buildings, compost, building work, or flood damage
-
In crowded indoor environments where infection risk is high
❌ When They’re Usually Not Needed
-
Day-to-day life in a clean, dry home environment
-
Low-risk outdoor activity (e.g. walking in the park)
-
If your asthma/ABPA/CPA is stable and you're not immunocompromised
🗣️ What the National Aspergillosis Centre Recommends
-
Use FFP2 masks when entering environments likely to have airborne fungal spores
-
FFP3 masks may be offered for high-risk medical procedures or when severely immunocompromised
-
Masks are one part of a broader protection strategy, which includes:
-
Good indoor air quality (HEPA filters, ventilation)
-
Avoidance of dusty environments
-
Prompt treatment of fungal infections
-
🌬️ Living with Asthma and Aspergillosis: Understanding the Overlap, the Immune System, and the Right Treatment
If you live with asthma and have been told you also have aspergillosis, such as ABPA (Allergic Bronchopulmonary Aspergillosis) or SAFS (Severe Asthma with Fungal Sensitisation), your situation is more complex than most people realise.
This guide explains:
-
The different types of asthma
-
How aspergillosis complicates asthma
-
The role of eosinophils, IgE, and the immune system
-
Why some people don’t have “typical” symptoms (like wheeze)
-
What treatments are available — and how to personalise your care
🧠 Asthma Isn’t One Disease
Asthma is a condition where the airways (breathing tubes) become:
-
Inflamed (swollen and irritated)
-
Overreactive to certain triggers (allergens, cold air, infection, etc.)
-
Narrowed and often filled with mucus, making breathing difficult
But not everyone with asthma has the same cause, symptoms, or treatment response. Asthma actually includes many subtypes — and understanding your type is key to getting the right care.
🧬 Common Asthma Types in Aspergillosis
| Asthma Type | Cause / Trigger | Key Features |
|---|---|---|
| Allergic asthma | IgE-driven allergy to pollen, dust, pets, fungi | Common in early-life asthma |
| Eosinophilic asthma | High levels of eosinophils (a white blood cell) | Often adult-onset and hard to control |
| SAFS | Allergy to fungi (especially Aspergillus) | Severe, steroid-resistant asthma |
| ABPA | Allergic reaction to Aspergillus growing in lungs | Very high IgE, eosinophils, mucus, lung damage |
| Cough-variant asthma | Inflammation without wheeze | Dry cough as the only symptom |
| “Silent” asthma | Reduced or absent warning signs | No wheeze, may present with fatigue, cough or breathlessness only |
🫢 New Section: What Is “Silent Asthma”?
“Silent asthma” is not an official medical term, but it’s used to describe:
-
Asthma without the classic wheeze (often just cough or tightness)
-
Or where asthma attacks happen suddenly, without clear warning
This is important because:
-
People may not realise they have asthma
-
Diagnosis may be delayed or missed
-
Flare-ups can be severe or even life-threatening
-
It may occur in people with fungal asthma, ABPA, or airway damage
Silent asthma is especially relevant in:
-
Older adults
-
People with ABPA or SAFS
-
People with cough-variant asthma
-
Anyone whose asthma doesn’t “sound” typical
🧪 Tests like FeNO, spirometry, and blood eosinophil counts are vital for confirming what’s really happening inside the lungs — even if symptoms are subtle.
🔬 Why ABPA Adds Complexity
If you have ABPA, the asthma symptoms are made worse by:
-
A hypersensitive immune reaction to Aspergillus fumigatus
-
Mucus plugging and blocked airways
-
Lung damage (bronchiectasis) that doesn’t improve with inhalers alone
-
A mix of allergic and eosinophilic inflammation
Key signs include:
-
Extremely high IgE levels
-
Raised eosinophils
-
Positive blood tests for Aspergillus
-
Lung CT scan changes
💊 Treatment Options Based on Asthma Type
| Treatment | Used For |
|---|---|
| Inhaled corticosteroids (ICS) | All types, first-line |
| Antifungal medications | ABPA, SAFS |
| Oral steroids (e.g. prednisolone) | ABPA flares, severe asthma |
| Biologics (e.g. mepolizumab, omalizumab) | Severe allergic or eosinophilic asthma |
| Chest physiotherapy | Mucus clearance in ABPA or bronchiectasis |
Each treatment is tailored based on whether your asthma is driven by:
-
IgE (allergy)
-
Eosinophils (inflammation)
-
Fungal exposure or colonisation
📍 What to Discuss with Your Healthcare Team
If you:
-
Have asthma that isn’t well controlled
-
Need frequent steroids
-
Have a chronic cough, thick mucus, or lung damage
-
Have high IgE or eosinophils
-
Or don’t wheeze, but still get breathless or fatigued…
… it’s important to ask your doctor:
-
Could I have ABPA or SAFS?
-
Is there a fungal or eosinophilic component to my asthma?
-
Should I be tested for Aspergillus allergy or IgE?
-
Am I a candidate for biologics or antifungals?
✅ Final Takeaway
Asthma with aspergillosis is more than just “bad asthma” — it’s a complex condition involving allergy, inflammation, fungal exposure, and in some cases, permanent airway changes. Some patients don’t experience wheeze — this is called “silent asthma,” and it deserves just as much attention.
You don’t have to manage this alone — and there are now targeted treatments that can help reduce symptoms, prevent damage, and improve quality of life.
🛡️ Choosing the Best Air Filter for Aspergillosis – Day & Night
Living with aspergillosis (such as ABPA, CPA, aspergillus bronchitis, or SAFS) means taking extra care to avoid airborne Aspergillus spores, which can be found both outdoors and indoors. One of the most effective ways to protect yourself at home is by using a high-quality air purifier.
This guide will help you choose a purifier that works for you — especially for bedroom use at night, where quiet operation is just as important as clean air.
🎯 Why Use an Air Filter?
-
Aspergillus spores are tiny (2–3 microns), invisible to the eye, and can remain airborne for long periods.
-
Indoor sources include dust, damp areas, stored food, compost, or even indoor plants.
-
A HEPA air purifier can trap these particles, helping reduce airway irritation, infections, or allergic reactions.
✅ What to Look For
| Feature | Why It Matters |
|---|---|
| True HEPA Filter | Captures ≥99.97% of particles ≥0.3 microns — includes Aspergillus spores |
| Activated Carbon Filter | Helps remove odours, gases, VOCs (optional bonus) |
| Room Size & CADR | Clean Air Delivery Rate (CADR) should match or exceed your room’s size |
| Quiet Operation | For night-time use, look for ≤25–30 dB (whisper-quiet) |
| Sleep Mode / Dim Lights | Prevents disturbance from lights or fan noise overnight |
| Filter Replacement | Easy to change, ideally with indicator for when to replace |
| No Ozone or Ionisers | Avoids irritation to sensitive lungs — stick with mechanical HEPA filtration |
🌙 Night-Time Friendly Options
| Model | Noise (dB) | Room Size | Notes |
|---|---|---|---|
| Blueair Blue Pure 411 Auto | 17 dB | Up to 35 m² | Super-quiet, ideal for small bedrooms |
| Levoit Core 300S | 24 dB | Up to 40 m² | Quiet, smart controls, affordable |
| Philips 3000i AC3033 | 25 dB | Up to 104 m² | Excellent for larger spaces, smart app |
| IQAir Atem Desk | <22 dB | Personal zone | Ultra-quiet, high-quality for desks/bedsides |
| Dyson Purifier Cool | ~24–32 dB | Medium–large | Stylish, also a fan, more expensive |
Tip: Choose a unit slightly larger than your room size for best effect.
💡 Extra Tips for Aspergillosis Patients
-
✅ Vacuum with a HEPA filter weekly
-
✅ Keep humidity below 50% (use a dehumidifier if needed)
-
✅ Avoid ionizers or ozone generators — these can irritate your lungs
-
✅ Close windows at night during high pollen or spore seasons
-
✅ Clean or change filters regularly (check manufacturer’s guide)
🛏 Night Setup Checklist
-
Place the purifier 1–2 metres from your bed (not right next to your face)
-
Use “Sleep Mode” or low fan for silent overnight cleaning
-
Turn off indicator lights (if bright)
-
Close doors and windows to keep clean air contained
-
Replace filters every 6–12 months or as prompted
📌 Summary
| Must-Have Features | Optional but Useful |
|---|---|
| ✅ True HEPA filtration | 🌫 Activated carbon filter |
| ✅ Quiet night mode (<25 dB) | 📱 Smart controls or auto mode |
| ✅ Right room size / CADR rating | 🌡 Monitor for humidity or air quality |
| ✅ No ozone, no ionizers | 🔁 Filter change indicator |
🗨️ Final Thought
For aspergillosis patients, an air purifier is a worthwhile investment in long-term lung health — especially in sleeping areas where your body is most vulnerable. Choosing the right device helps reduce exposure to fungal spores and improves quality of life, one breath at a time.
📄 Why Have Asthma Rates Risen Despite Cleaner Air?
It might seem surprising, but even though outdoor air pollution has fallen a lot since the 1970s, asthma is more common today — especially in children. Here's why:
🧼 1. Cleaner Isn’t Always Better for the Immune System
Modern lifestyles mean children are exposed to fewer germs early in life. This can cause the immune system to become over-sensitive, making allergies and asthma more likely. This is called the "hygiene hypothesis."
👩⚕️ 2. Better Diagnosis
Asthma is diagnosed much more often now than in the past. In the 1970s, many children with wheezy breathing weren't given a diagnosis. Today, doctors recognise and treat asthma early. That means the numbers look higher — but some of it is due to better awareness.
🏠 3. Indoor Pollution
While outdoor air has improved, indoor air can be a problem:
- Gas cookers, damp and mould
- Dust mites and cleaning sprays
- Less fresh air due to sealed homes These things can all affect breathing and trigger asthma.
🚗 4. Modern Air Pollution Still Affects Us
Pollution from traffic (especially nitrogen dioxide and tiny particles called PM2.5) is still a problem — especially near busy roads. These can irritate lungs and make asthma worse, even at low levels.
⚖️ 5. Lifestyle Factors
Obesity increases the risk of asthma, and more children are now overweight. Children also spend more time indoors and less time being active, which may affect lung health.
🧬 6. Genetics and Early Exposures
Family history matters, and things like antibiotics, pollution, or infections during pregnancy or early life can influence a child’s risk of developing asthma.
✅ Good News
Even though more people have asthma, it’s much better managed today:
- Inhalers are more effective
- Fewer people die from asthma
- Most children and adults with asthma can live full, active lives with the right support
🩺 Has Cleaning Our Air Been Worth It?
Despite the rise in asthma diagnoses, cleaning up the air has been a major public health success:
✔️ Major Benefits:
- Huge drop in bronchitis, pneumonia, and childhood chest infections
- Far fewer hospital admissions for acute respiratory illness
- Respiratory deaths due to coal smoke, sulphur dioxide, and black soot have plummeted
- Safer air for people with long-term lung conditions like COPD, ABPA, and CPA
🤔 Why Asthma Went Up Anyway:
As the section above explains, asthma is influenced by more than just air pollution:
- Indoor air, allergens, obesity, early-life exposures, and genetic factors all matter
- Better detection and survival also increase the number of people living with asthma
🔍 The Bigger Picture:
Even though asthma became more common, the severity of lung disease has dropped for many people thanks to:
- Better inhalers and treatments
- Early diagnosis
- Cleaner air and less exposure to smoke and harmful chemicals
So yes — cleaning the air has been worth it. It’s saved lives and made breathing easier for millions. But like most things in health, it's one part of a much bigger story.
Let your healthcare team know if you have questions — understanding your environment and your own triggers can help you breathe easier, wherever you live.
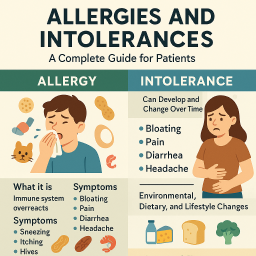
🌿 Allergies and Intolerances: A Complete Guide for Patients
Reactions to foods, pollen, mould, animals, or chemicals are increasingly common. But many people don't realise there’s a difference between allergies and intolerances — and that understanding this difference can help protect your health and guide treatment.
This guide explains:
-
What allergies and intolerances are
-
How they develop
-
How they differ
-
Why more people are affected than in the past
-
What to do if you’re experiencing symptoms
🤧 What Is an Allergy?
An allergy happens when your immune system overreacts to a harmless substance (called an allergen). Instead of ignoring the substance, your body sees it as a threat and releases histamine and other chemicals, causing inflammation and symptoms.
✅ Common Allergy Symptoms
-
Sneezing, runny or blocked nose
-
Itchy eyes or throat
-
Wheezing or coughing
-
Rashes or hives
-
Swelling of lips, face, or throat
-
Nausea or vomiting
-
In severe cases: anaphylaxis, a life-threatening reaction that requires emergency treatment
🧴 Common Allergy Triggers
-
Pollen
-
Mould spores
-
Dust mites
-
Pet dander
-
Foods (e.g., peanuts, shellfish, eggs)
-
Insect stings
-
Latex
-
Medications (e.g., penicillin)
Onset: Usually within minutes to 2 hours
Severity: Can range from mild to life-threatening
🍞 What Is an Intolerance?
An intolerance is when your body has difficulty processing or digesting a substance. It does not involve the immune system and is not life-threatening, though it can be very uncomfortable.
✅ Common Intolerance Symptoms
-
Bloating
-
Abdominal pain
-
Gas or diarrhoea
-
Nausea
-
Headaches or migraines
-
Fatigue or “brain fog”
🧂 Common Intolerance Triggers
-
Lactose (milk sugar)
-
Gluten (in non-coeliac cases)
-
Food additives (e.g. sulphites, MSG)
-
Caffeine or alcohol
-
Certain fruits and vegetables (e.g., those high in FODMAPs)
Onset: Often delayed – hours after eating
Severity: Not dangerous, but can affect quality of life
🛑 What About Coeliac Disease?
Coeliac disease is different from both allergies and intolerances. It is an autoimmune condition triggered by gluten (in wheat, rye, barley), where the immune system damages the small intestine.
-
Can lead to nutrient deficiencies, fatigue, bone loss, and other complications
-
Requires strict lifelong gluten-free diet
-
Diagnosed by blood tests and intestinal biopsy
🩺 Allergy vs Intolerance: Side-by-Side Comparison
| Feature | Allergy | Intolerance |
|---|---|---|
| System involved | Immune system (IgE antibodies) | Digestive, metabolic, or chemical sensitivity |
| Speed of reaction | Fast (minutes to 2 hours) | Slower (can take hours or be delayed until next day) |
| Common symptoms | Hives, sneezing, swelling, wheeze, anaphylaxis | Bloating, cramps, diarrhoea, fatigue, headache |
| Life-threatening? | Yes | No |
| Diagnosis available? | Yes: skin prick or blood tests (IgE) | Often by elimination diet or breath testing |
| Treatment | Avoid allergens, antihistamines, adrenaline pens | Avoid triggers, enzyme supplements, dietary management |
⏳ Can They Develop Over Time?
Yes — both allergies and intolerances can develop at any age, even in adulthood.
-
Allergies may appear after repeated exposure, a change in environment, infection, or hormone shift.
-
Intolerances may emerge gradually and worsen over time, especially after illness or with changes in gut health.
Can They Go Away?
-
Some childhood allergies (e.g., to milk or egg) may fade with age.
-
Intolerances can sometimes improve if the gut heals or the irritant is removed temporarily.
🧬 Why Do Some People Get Allergies or Intolerances?
Several factors increase the risk:
| Factor | How It Plays a Role |
|---|---|
| Genetics | Family history of allergies or intolerances |
| Environment | Pollution, damp housing, early-life exposures |
| Immune sensitivity | Some people’s immune systems are more reactive |
| Gut microbiome | A diverse gut protects against food sensitivities |
| Stress and anxiety | Can worsen or trigger symptoms in sensitive people |
🔬 Why Are These Conditions Becoming More Common?
Over recent decades, both allergies and intolerances have become more widespread — especially in industrialised countries. Here's why:
1. Hygiene Hypothesis
-
Cleaner environments mean fewer early exposures to bacteria and parasites.
-
Immune systems may become overreactive, mistaking harmless things like food or pollen for threats.
2. Environmental Changes
-
More pollution, chemical exposure, and indoor living.
-
Increased use of cleaning products, synthetic fragrances, and pesticides.
3. Modern Diets
-
More processed foods, additives, and preservatives
-
Less fibre and fermented food = poorer gut microbiome diversity
4. Changes in Early Childhood Exposure
-
Less breastfeeding
-
More Caesarean births (altering gut flora)
-
Delayed introduction of allergens (now reversed in guidelines)
5. Better Awareness and Diagnosis
-
People are more likely to report symptoms
-
Testing and knowledge have improved, leading to more diagnoses
6. Stress and Modern Lifestyle
-
Stress may worsen sensitivity to foods, chemicals, or allergens
-
Stress can also influence gut function and immune balance
🧪 How Are Allergies and Intolerances Diagnosed?
Allergy Testing:
-
Skin prick tests
-
Blood tests for IgE antibodies
-
Oral food challenge (done in hospital if risk of anaphylaxis)
-
Referral to an allergy specialist
Intolerance Testing:
-
Elimination and reintroduction diets
-
Hydrogen breath tests (e.g., for lactose or fructose)
-
Intolerances often require trial and error
Never self-diagnose based on internet lists — mislabeling a symptom could lead to unnecessary food avoidance or missed health risks.
💊 How Are They Treated?
| Condition | Treatment |
|---|---|
| Allergy | Avoidance, antihistamines, nasal sprays, inhalers, adrenaline pens (EpiPen) |
| Intolerance | Avoid trigger foods, enzyme supplements, low-FODMAP diet |
| Coeliac disease | Lifelong gluten-free diet, monitoring, dietitian support |
🩺 When to See a Doctor
You should speak to your GP if:
-
You experience repeated symptoms after certain foods or environmental exposures
-
You’ve had severe reactions like swelling, wheezing, or fainting
-
You’re unsure whether your reaction is allergy or intolerance
-
You’re planning to reintroduce foods or need support with diet changes
🧭 Final Summary
| Key Takeaways |
|---|
| Allergies involve the immune system and can be life-threatening |
| Intolerances do not involve the immune system and are not dangerous |
| Both can develop at any age and may change over time |
| Environmental, dietary, and lifestyle changes have contributed to rising rates |
| Diagnosis and management depend on proper testing and support |
Understanding the difference between allergies and intolerances can help you:
-
Stay safe
-
Manage your symptoms
-
Avoid unnecessary restrictions
-
Get the care and advice you need
You are not alone — and support is available.
Severe Asthma with Fungal Sensitisation (SAFS) for Expert Patients and non-Specialist Clinicians
Expert Information for Patients, GPs, and Specialist Nurses
🔎 What Is SAFS?
SAFS describes a clinical subgroup of patients with severe asthma who are sensitised to environmental fungi, particularly Aspergillus fumigatus, but who do not meet criteria for ABPA (i.e. no high total IgE or central bronchiectasis).
Fungal sensitisation may contribute to poor asthma control, airway inflammation, and increased exacerbations.
🧬 Pathophysiology
-
IgE-mediated sensitisation to fungi in the airways
-
Chronic airway inflammation exacerbated by fungal allergens
-
Unlike ABPA, no eosinophilia, mucus plugging, or significant IgE rise
👥 Who Is at Risk?
SAFS affects adults or children with:
-
Severe asthma (high-dose ICS + additional controller medication)
-
Recurrent exacerbations or persistent symptoms
-
Evidence of IgE sensitisation to fungi, especially A. fumigatus, Alternaria, Cladosporium
It may overlap with ABPA, and some patients may transition between the two.
⚠️ Common Symptoms
-
Poor asthma control despite optimal treatment
-
Frequent exacerbations
-
Airflow limitation (FEV1 often <80%)
-
Increased oral corticosteroid use
-
Wheeze, cough, chest tightness
🧪 Diagnosis
SAFS is a diagnosis of exclusion in patients with severe asthma and fungal sensitisation, but without ABPA.
Required Features:
-
Severe asthma, typically on BTS Step 4–5 therapy
-
Positive fungal-specific IgE (skin prick or blood) to at least one fungus
-
Aspergillus fumigatus most common
-
-
No ABPA: i.e., total IgE <1000 IU/mL, no eosinophilia, no central bronchiectasis
Investigations:
-
Skin prick testing or specific IgE blood test
-
Total IgE to exclude ABPA
-
CT chest to rule out ABPA or CPA
-
Sputum culture for A. fumigatus (not required for diagnosis)
💊 Treatment
Antifungal Therapy:
-
Itraconazole (first-line): 3–6 months may improve asthma control, reduce exacerbations
-
Posaconazole (alternative)
-
Liver function and drug levels must be monitored
The EVITA 3 and Fungal Asthma trials suggest modest benefit with antifungal therapy in SAFS.
Asthma Management:
-
High-dose inhaled corticosteroids + LABA
-
Leukotriene receptor antagonists
-
Macrolides in selected patients (anti-inflammatory benefit)
-
Biologics:
-
Omalizumab (anti-IgE)
-
Mepolizumab, Benralizumab (anti-IL-5)
-
Dupilumab (anti-IL-4/13)
-
🧾 Monitoring
-
Asthma control questionnaires (ACT, ACQ)
-
Exacerbation frequency
-
Spirometry
-
Fungal IgE titres (do not typically change with treatment)
-
LFTs and drug levels if on antifungals
📚 More Information
-
SAFS patients often benefit from review in a specialist asthma clinic or severe asthma network centre.
-
Overlap with ABPA: patients should be periodically reassessed to detect transition to ABPA.
-
Patient resources: aspergillosis.org, Asthma + Lung UK, BTS asthma guidelines
- Resource: SAFS