Join our UK Citizen Science Project on Damp Homes and Health

Many people living with aspergillosis, asthma and chronic lung disease tell us they are worried about damp, mould and housing conditions — but often struggle to know:
- whether their home really has a problem
- who to trust for advice
- whether mould testing is reliable
- and what effective remediation should involve.
There is currently considerable uncertainty around indoor mould assessment, air sampling and interpretation of results. Many patients report difficulty obtaining clear, independent advice or meaningful remediation.
At the same time, we still know surprisingly little about the real-life health impact of living in damp homes across the UK.
A UK Citizen Science Project
We are supporting a UK citizen science project exploring how damp homes may affect health, including respiratory health and conditions such as aspergillosis.
Citizen science projects involve members of the public helping researchers and healthcare communities better understand real-world problems by sharing experiences and observations.
You do not need to have diagnosed aspergillosis to take part.
We are interested in hearing from people:
- living in damp or mouldy homes
- living in homes without damp
- with respiratory conditions
- and without respiratory conditions.
The initial registration takes about 1 minute and simply records your interest in the project.
Why this matters
By taking part, you may help improve understanding of:
- damp homes and respiratory disease
- mould exposure
- indoor air quality
- housing conditions
- challenges with mould assessment and remediation
- and the wider health impact of dampness in UK homes.
We hope the project will help patients, clinicians, housing professionals and researchers better understand:
- how people experience damp homes in real life
- the difficulties many people face obtaining reliable advice
- the limitations of current mould assessment approaches
- and what practical interventions may genuinely improve health and quality of life.
Related information
You can also read our practical guide discussing damp homes, mould testing, remediation and tenant support:
Read our guide to damp, mould and aspergillosis
Find out more or register your interest
Damp Homes and Health Study UK
Please share this project with:
- patients and carers
- healthcare professionals
- housing professionals
- damp and mould specialists
- environmental health professionals
- researchers
- and anyone interested in improving understanding of damp homes and health.
Damp, Mould and Aspergillosis: A Practical Guide for Patients Worried About Their Home
People with aspergillosis, asthma, bronchiectasis, chronic lung disease, allergies, or a weakened immune system are often understandably concerned about whether dampness or mould in the home could be affecting their health.
This guide explains:
- what signs to look for
- what practical steps may help
- the limitations of mould air testing
- who is most likely to provide reliable professional help
- and what support may be available for tenants.
Key points
- Dampness and mould can matter for people with respiratory disease.
- The most important question is usually: why is moisture present?
- Air sampling and mould spore counts have major limitations and should not be relied on alone.
- A “normal” air test does not reliably prove that a home is free from damp or hidden mould.
- The best assessments usually focus on building defects, condensation, ventilation, leaks and moisture sources.
- For complex problems, experienced chartered building professionals and occupational/environmental hygienists are often more useful than simple “mould testing” services.
- Dust and dirt accumulation may contribute to mould growth and respiratory irritation, especially in damp environments.
- Recent UK housing guidance increasingly recognises the health impact of damp and mould.
Why damp and mould matter
Fungi are a normal part of the environment. Tiny fungal spores are present in outdoor air, soil, gardens, compost and many indoor spaces. Most people breathe in small numbers of spores every day without becoming ill.
However, persistent dampness indoors can allow mould growth to increase. This may worsen irritation, allergy, asthma symptoms or respiratory symptoms in some people.
People who may be more sensitive include those with:
- Allergic Bronchopulmonary Aspergillosis (ABPA)
- Chronic Pulmonary Aspergillosis (CPA)
- Severe Asthma with Fungal Sensitisation (SAFS)
- bronchiectasis
- Chronic Obstructive Pulmonary Disease (COPD)
- cystic fibrosis
- severe asthma
- significant allergies
- or a weakened immune system.
Signs your home may have a damp problem
Visible signs
- black, green or white mould growth
- condensation on windows
- damp patches
- peeling wallpaper or paint
- bubbling plaster
- staining on walls or ceilings
- warped wood
- persistent condensation
Smell
A persistent musty, earthy or “damp” smell can sometimes indicate hidden moisture or mould growth, even when little is visible.
Possible building causes
- leaks from roofs, gutters or plumbing
- poor ventilation
- condensation
- cold external walls
- thermal bridging
- rising damp
- penetrating damp
- blocked air vents
- drying clothes indoors without enough ventilation.
Can dust and dirt make mould problems worse?
Yes. Accumulated dust and dirt can sometimes contribute to indoor mould problems, especially when combined with moisture or high humidity.
Dust is not simply “dirt” — it often contains:
- skin cells
- textile fibres
- pollen
- bacteria
- fungal spores
- organic material
- and microscopic debris.
When dust accumulates in damp or poorly ventilated areas, it can provide nutrients that allow mould growth to establish more easily on surfaces.
This is particularly common:
- behind furniture placed against cold walls
- around windows
- on curtains and blinds
- inside wardrobes
- under beds
- around ventilation grilles
- and in areas with condensation.
For people with asthma, allergy or aspergillosis, heavy dust accumulation may also worsen irritation or respiratory symptoms independently of visible mould.
Symptoms that may be triggered or worsened
Damp or mould exposure may contribute to:
- coughing
- wheezing
- chest tightness
- breathlessness
- increased sputum
- nasal irritation
- sinus symptoms
- eye irritation
- fatigue
- worsening asthma control
- increased allergy symptoms.
Symptoms may be more noticeable in certain rooms, overnight, during winter, after rainfall, or when ventilation is poor.
However, symptoms alone cannot prove that mould exposure is the cause. Many respiratory conditions can cause similar symptoms, so medical advice is important if symptoms are worsening.
Should you get air testing done?
Many companies offer indoor air sampling, mould spore counts or fungal testing. Patients often hope this will provide reassurance or proof that a home is safe.
Unfortunately, air sampling has important limitations.
Limitations of air sampling
- There are no universally agreed “safe” mould spore levels for homes.
- Results can vary enormously throughout the day.
- Outdoor air can strongly influence indoor results.
- Cleaning, vacuuming, opening windows or walking around can alter results.
- A short air sample may not represent usual exposure.
- Hidden damp or mould may not show up in an air sample.
- A “normal” air test does not reliably prove that a building is free from damp or mould problems.
Air sampling may sometimes be useful when carried out by experienced specialists as part of a wider investigation. However, it should not be used as the only basis for deciding whether a home is safe or whether remediation has worked.
What usually matters most?
The key question is usually:
Why is moisture present in the home?
Without moisture, significant mould growth usually cannot continue. Therefore, the most important step is to identify and correct the source of dampness.
This may involve:
- repairing leaks
- improving ventilation
- reducing condensation
- correcting insulation or thermal bridging problems
- repairing gutters, roofs or plumbing
- addressing overcrowding or excessive indoor humidity.
What you can do yourself
Improve ventilation
- Use extractor fans in bathrooms and kitchens.
- Open windows when practical and safe.
- Do not block air vents.
- Ventilate after showering, cooking or drying clothes.
Reduce indoor humidity
- Dry clothes outdoors where possible.
- Use lids on pans while cooking.
- Avoid drying clothes on radiators without ventilation.
- Consider a humidity monitor.
- Aim to avoid persistently high indoor humidity.
A dehumidifier may help reduce humidity in some situations, but it does not fix the underlying cause of dampness if there is a leak, structural defect or ventilation problem.
Reduce dust accumulation
- Clean regularly using methods that minimise dust disturbance.
- Pay particular attention to hidden or poorly ventilated areas.
- Move furniture slightly away from cold external walls where possible.
- Reduce clutter that traps dust and moisture.
- Wash soft furnishings and curtains regularly if practical.
Clean small areas carefully
Small areas of surface mould can sometimes be cleaned carefully using appropriate cleaning products. Avoid dry brushing or actions that disturb mould and release spores into the air.
People with significant lung disease, severe asthma, severe allergy or aspergillosis may prefer somebody else to carry out cleaning to reduce exposure.
Large, recurring or hidden mould problems usually need professional assessment.
Who is most likely to provide reliable help?
The most useful professionals are usually those who investigate the building and the source of moisture, not just the air.
For complex damp or mould problems, more robust help may come from:
- experienced chartered building surveyors
- building pathology specialists
- chartered building engineers
- occupational hygienists
- environmental hygienists with experience in indoor air quality and moisture assessment.
Relevant UK professional bodies
- Royal Institution of Chartered Surveyors (RICS)
- Chartered Institute of Building (CIOB)
- Chartered Association of Building Engineers (CABE)
- British Occupational Hygiene Society (BOHS)
Some damp and remediation companies may also be associated with the Property Care Association (PCA). This may indicate relevant industry training, but membership alone does not guarantee expertise. Experience and independence still matter.
Is impartial advice available?
Sometimes. People are often unsure where to obtain trustworthy, independent advice about damp and mould.
Possible sources of impartial guidance may include:
- local council Environmental Health departments
- housing officers (for tenants)
- Citizens Advice services
- NHS guidance
- UK Health Security Agency (UKHSA) guidance
- recognised professional bodies.
Local councils may sometimes inspect severe housing conditions, particularly where:
- children or vulnerable adults are involved
- landlords are failing to act
- there is extensive visible mould
- or housing conditions may present health hazards.
Support varies considerably between areas, and services are often stretched, but councils can sometimes require landlords to take action where housing conditions are unsafe.
Awaab’s Law and what it may mean for tenants
For people living in rented accommodation, especially social housing, recent changes in UK housing law may provide stronger protection where damp and mould problems are affecting health.
Awaab’s Law was introduced following the death of two-year-old Awaab Ishak in Rochdale after prolonged exposure to severe mould in social housing.
The law strengthens expectations that social landlords:
- investigate damp and mould complaints promptly
- assess potential risks to health
- carry out repairs within defined timescales
- and respond more urgently where vulnerable people are involved.
This is particularly important for people with:
- aspergillosis
- asthma
- bronchiectasis
- Chronic Obstructive Pulmonary Disease (COPD)
- cystic fibrosis
- or weakened immune systems.
What tenants should do
If you are concerned about damp or mould in rented accommodation, it may help to:
- report problems formally and in writing where possible
- keep photographs and dates
- record repeated complaints
- document worsening conditions
- keep copies of correspondence
- retain relevant medical letters if symptoms are worsening.
Where severe respiratory disease is present, medical evidence may help demonstrate vulnerability and the need for urgent action.
Important limitations
Awaab’s Law does not mean that every mould problem becomes an emergency or that all homes can be repaired immediately. Housing shortages, structural problems, funding limitations and contractor delays still affect what can be achieved.
However, the law has strengthened the expectation that damp and mould complaints should be taken seriously and addressed promptly, particularly where vulnerable people are affected.
NICE guidance and UK guidance
The National Institute for Health and Care Excellence (NICE) has increasingly recognised the importance of indoor air quality and housing conditions in respiratory health.
In addition, the UK Health Security Agency (UKHSA) has published major guidance emphasising that:
- damp and mould should be addressed promptly
- visible mould should not be ignored
- people with respiratory disease may be more vulnerable
- and simply blaming lifestyle alone is often inappropriate.
Recent UK guidance has increasingly shifted away from treating damp and mould purely as cosmetic issues, recognising their potential health impacts — especially for vulnerable people.
Questions to ask before paying for an assessment
- What qualifications and experience do you have in damp, mould and building moisture problems?
- Are you independent, or do you also sell remediation work?
- Will you investigate moisture sources, ventilation and building defects?
- Will I receive a written report explaining the likely cause?
- How will you decide whether remediation has worked?
- Will you explain the limitations of any air sampling?
- Do you use air sampling as part of a wider assessment, or as the main test?
Be cautious if...
- the assessment mainly consists of a quick air sample
- dramatic health claims are made
- the report presents spore counts as a simple “safe/unsafe” result
- expensive remediation is recommended immediately
- the company creates pressure to buy treatment packages
- there is little attention to leaks, condensation, ventilation or building defects.
How do you know remediation has worked?
Success should usually be judged by practical outcomes, including:
- visible mould has been removed safely
- the source of moisture has been corrected
- damp patches are drying out
- musty smells have reduced
- ventilation has improved
- humidity is better controlled
- mould does not quickly return
- symptoms improve over time, where mould exposure was contributing.
Repeat air sampling alone is not a reliable way to prove that a home is safe.
When to seek medical advice
People with aspergillosis or other lung conditions should seek medical advice if they experience:
- worsening breathlessness
- coughing blood
- rapidly worsening asthma symptoms
- fever or signs of infection
- unexplained weight loss
- significant deterioration in chest symptoms
- new or worsening fatigue with chest symptoms.
If symptoms appear linked to a damp or mouldy environment, discuss this with your healthcare team. They may not be able to assess the building, but they can help assess your health and whether your respiratory condition is changing.

Related information on Aspergillosis.org
- Reducing mould exposure
- Damp homes and health study
- What is aspergillosis?
- Living with aspergillosis
- Patient information hub
Useful resources
- UK Health Security Agency: Damp and mould guidance
- NICE: Indoor air quality at home
- NICE: Excess winter deaths and illness and the health risks associated with cold homes
- UK Government: Awaab’s Law factsheet
- Shelter UK: Damp and mould in rented homes
- Citizens Advice: Housing disrepair
Reducing Exposure to Mould (Aspergillus) at Home
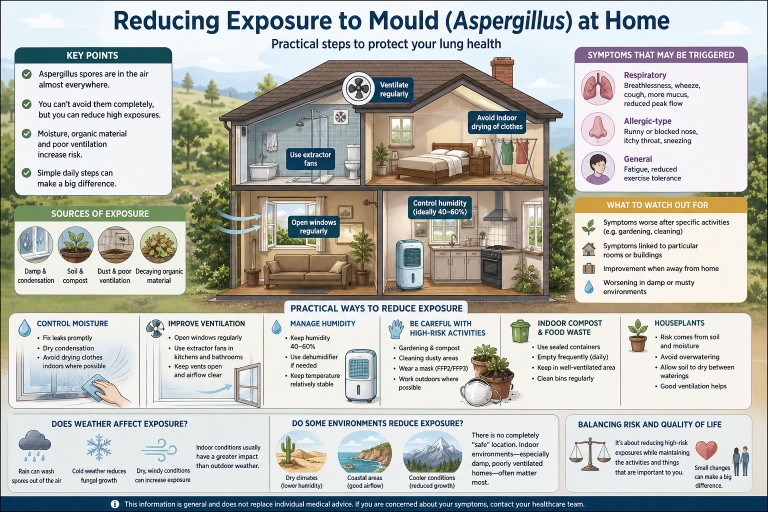
Audience: Patients with aspergillosis (including Allergic Bronchopulmonary Aspergillosis and Chronic Pulmonary Aspergillosis), carers, and non-specialist cliniciansIf you have aspergillosis, reducing exposure to environmental moulds such as Aspergillus can help minimise symptoms and reduce the risk of flare-ups.This guide brings together practical, evidence-informed advice based on environmental studies and clinical experience at specialist centres such as the National Aspergillosis Centre (Manchester, UK).
🔑 Key Points
- Aspergillus spores are present in the air almost everywhere.
- Complete avoidance is not possible—focus on reducing higher-level exposures.
- The most important drivers are moisture, organic decay, and disturbance.
- Indoor exposure is often more important than outdoor exposure.
- Simple environmental and behavioural changes can significantly reduce risk.
🌍 Where does mould exposure come from?
Aspergillus is a common environmental mould. It grows on organic material and releases microscopic spores into the air.
Common sources include:
- Damp walls, ceilings, and condensation
- Soil, compost, and plant material
- Dust and poorly ventilated spaces
- Food waste and decaying organic matter
Spores are always present at low levels. Problems arise when concentrations increase, particularly in enclosed or damp environments.
⚖️ Who is most affected?
Reducing exposure is particularly relevant for people with:
- Allergic Bronchopulmonary Aspergillosis (ABPA)
- Chronic Pulmonary Aspergillosis (CPA)
- Asthma or bronchiectasis
- Reduced immune function
Individual sensitivity varies. Some people notice clear environmental triggers, while others are less affected by day-to-day variation.
⚠️ What symptoms can mould exposure trigger?
Exposure may trigger or worsen symptoms by increasing airway inflammation or allergic responses.
Respiratory symptoms
- Increased breathlessness
- Wheezing or chest tightness
- Persistent or worsening cough
- Increased or thicker mucus
- Reduced peak flow (if monitored)
Allergic-type symptoms
- Nasal congestion or runny nose
- Itchy throat
- Sneezing
General symptoms
- Fatigue
- Reduced exercise tolerance
In ABPA, exposure may contribute to flare-ups. In CPA, changes may be more gradual.
👀 What should you watch out for?
Patterns are often more informative than single exposures.
- Symptoms worsening after specific activities (e.g. gardening, cleaning)
- Symptoms linked to particular rooms or buildings
- Improvement when away from home
- Worsening in damp or musty environments
Keeping a simple symptom diary can sometimes help identify triggers.
Important: Not all symptoms are due to mould exposure—other factors such as infection or asthma control may also play a role.
🏠 Reducing mould in your home
1. Control moisture (most important factor)
- Fix leaks promptly (pipes, roofs, windows)
- Dry condensation from windows and walls
- Avoid prolonged indoor drying of clothes where possible
Moisture is the key driver of mould growth—reducing it addresses the root cause.
2. Improve ventilation
- Open windows regularly (even short periods can help)
- Use extractor fans in kitchens and bathrooms
- Avoid blocking vents or airflow pathways
Ventilation removes spores and reduces humidity at the same time.
3. Manage condensation
- Maintain a relatively stable indoor temperature
- Use lids when cooking
- Consider dehumidifiers in problem areas
🌬️ Ventilation, filtration and humidity
Ventilation (first priority)
Ventilation is usually the most effective intervention because it removes airborne spores and reduces moisture.
Dehumidifiers
Dehumidifiers reduce indoor humidity (target around 40–60%), making conditions less favourable for mould growth.
HEPA air purifiers
HEPA filters can remove airborne particles, including fungal spores. However, they do not address the source of mould and are best used alongside other measures.
Practical approach: address moisture and ventilation first, then consider additional filtration if needed.
🌦️ Does weather affect mould exposure?
- Rain can reduce airborne spores by washing them out of the air
- Cold conditions reduce fungal growth
- Dry, windy weather can increase exposure by disturbing dust and soil
However, indoor conditions usually have a greater impact than outdoor weather.
🌍 Do some environments reduce exposure?
Some environments may be associated with lower exposure:
- Dry climates (lower humidity)
- Coastal areas (good airflow and dilution)
- Cooler conditions (reduced fungal growth)
There is no completely “safe” location, and indoor conditions often matter more than geography.
🌿 Activities and exposure
Some activities can temporarily increase exposure:
- Gardening or handling compost
- Cleaning dusty areas
- Handling stored materials
Precautions:
- Wear a well-fitted mask (FFP2 or FFP3)
- Carry out dusty tasks outdoors where possible
- Avoid enclosed, poorly ventilated spaces
🗑️ Indoor compost bins and food waste
Food waste provides an ideal environment for mould growth.
Risk increases when waste is stored indoors for prolonged periods, particularly in warm conditions.
- Empty bins frequently (ideally daily)
- Use sealed containers
- Keep in well-ventilated areas
- Clean bins regularly
🌱 Houseplants
The main risk comes from soil and moisture rather than the plant itself.
👉 Read full guide on houseplants and aspergillosis
⚖️ Balancing risk and quality of life
It is important to balance exposure reduction with maintaining normal daily activities.
- Gardening can often continue with precautions
- Houseplants can often be kept safely
- Focus on reducing higher-risk exposures rather than avoiding everything
⚠️ When to seek medical advice
- Increasing breathlessness
- Worsening cough or mucus
- Reduced peak flow
- Symptoms clearly linked to environment
Seek urgent advice for:
- Rapid breathlessness
- Chest pain
- Coughing blood
📚 Further reading
👩⚕️ Author & Review
Developed using patient questions and reviewed in line with National Aspergillosis Centre practice (Manchester, UK).
This information is general and does not replace individual medical advice.
Houseplants and Aspergillosis: Do You Need to Get Rid of Them?

Audience: Patients with aspergillosis (including Allergic Bronchopulmonary Aspergillosis), carers, and non-specialist cliniciansHouseplants are a common concern for people with
aspergillosis, particularly those with
Allergic Bronchopulmonary Aspergillosis (ABPA).If you’ve asked this question, you’re not alone—many patients raise it in our
patient questions and discussions.
🔑 Key Points
- Houseplants can be a source of Aspergillus spores, mainly from soil.
- Most people with ABPA do not need to remove all plants.
- The main risk comes from damp soil and disturbance.
- Simple precautions can significantly reduce exposure.
- How plants are cared for matters more than the type of plant.
Contents
- Why houseplants can be a problem
- How big is the risk?
- Do houseplants clean the air?
- Can I safely keep my plants?
- How to reduce risk
- Are some plants lower risk?
- When to consider removing plants
- Common questions
- When to seek medical advice
- References
🌱 Why can houseplants be a problem?
Aspergillus is a common environmental mould found in:
- Soil and compost
- Decaying plant material
- Damp indoor environments
For people with Allergic Bronchopulmonary Aspergillosis (ABPA), inhaling spores can trigger airway inflammation, wheeze, cough, and breathlessness.
The main risk comes from soil rather than the plant itself.
⚖️ How big is the risk?
The risk varies depending on:
- How stable your condition is
- The number of plants
- Ventilation in your home
- How plants are maintained
Specialist centres such as the National Aspergillosis Centre (NAC) recommend a
risk reduction approach rather than complete avoidance.
You can read more in our guide to
reducing mould exposure.
Important: There is limited direct research linking houseplants to worsening ABPA. Advice is based on environmental studies and clinical experience.
🌿 Do houseplants clean the air?
You may have heard that houseplants “clean the air.” This idea comes from laboratory studies, including research by
:contentReference[oaicite:0]{index=0}, conducted in sealed environments.
In real homes, the effect is minimal.
- Very large numbers of plants would be needed
- Ventilation has a much greater impact
- Soil may introduce Aspergillus spores
For a broader explanation, see our
aspergillosis overview.
Bottom line: Plants may improve wellbeing, but they are not an effective air-cleaning strategy.
🌿 Can I safely keep my houseplants?
In many cases, yes.
Many people with ABPA keep houseplants without problems when their condition is stable and plants are well maintained.
However, some individuals are more sensitive, so a personalised approach is important.
✅ How to reduce your risk
1. Manage the soil carefully
- Avoid constantly damp compost
- Allow the top layer to dry between watering
- Consider lower-organic substrates (e.g. clay pebbles)
Tip from patients: Adding a layer of stones or gravel on top of the soil can reduce disturbance during watering and may help limit release of fungal spores.
2. Avoid disturbing soil indoors
- Repot plants outside if possible
- Wear a well-fitted mask (FFP2 or FFP3)
3. Maintain good plant hygiene
- Remove dead leaves promptly
- Avoid visible mould growth
- Do not allow stagnant water
4. Choose locations carefully
- Keep plants out of bedrooms
- Ensure good ventilation
5. Personal hygiene after handling plants
- Wash hands after handling soil or compost
- Avoid touching your face before cleaning hands
- Consider changing clothes after heavy gardening
- Ventilate the area after indoor plant work
These steps form part of a wider approach to
reducing environmental exposure.
🌿 Are some plants lower risk for ABPA?
There is no strong evidence that specific plants are “safe” or “unsafe.” The main risk comes from soil and moisture.
Some setups may be lower risk in practice:
- Hydroponic or semi-hydroponic plants
- Plants that prefer drier conditions (e.g. succulents)
- Well-maintained plants with minimal decaying material
Important: Any plant can become higher risk if soil becomes damp or mouldy.
If unsure, you may wish to review
clinical guidance or discuss with your care team.
🚩 When should I consider removing plants?
- Symptoms worsen after watering or handling plants
- Visible mould in soil
- Frequent flare-ups
- Clinical advice recommends stricter avoidance
Some people remove plants temporarily during unstable periods and reintroduce them later.
❓ Common questions
Are leaves dangerous?
No—the main risk comes from soil and decaying material.
Is outdoor gardening riskier?
Yes, due to higher exposure. Wearing a mask is recommended.
Do air purifiers help?
HEPA filters may reduce airborne particles, but evidence specific to ABPA is limited.
⚠️ When to seek medical advice
- Increasing breathlessness or wheeze
- Worsening cough or mucus
- Reduced peak flow
- Symptoms linked to specific environments
Do not change treatment without medical advice.
📚 References & Further Reading
- What is aspergillosis?
- Reducing exposure to mould
- World Health Organization – Indoor air quality guidance
- UK Health Security Agency – Damp and mould health risks
👩⚕️ Author & Review
Developed for patient education in line with UK specialist practice (National Aspergillosis Centre, Manchester).
This information is general and does not replace individual medical advice.
Looking for more answers? Visit our
patient questions hub.
Damp Homes, Indoor Air and Health: What a Recent Evidence Review Tells Us

Summary: A recent rapid review by researchers from the Health and Safety Executive examined evidence on microbiological hazards in buildings, including moulds, bacteria and viruses. The review highlights that dampness, poor ventilation and building design can all affect indoor air quality and respiratory health.
Key points
- People spend much of their time indoors, so indoor air quality can strongly affect health.
- Damp indoor conditions increase the risk of mould growth and musty odours.
- Common indoor moulds include Aspergillus, Penicillium and Cladosporium.
- Dampness and visible or hidden mould are linked with asthma, rhinitis, wheeze and other respiratory symptoms.
- Ventilation is one of the most important ways to reduce moisture and dilute airborne contaminants.
- Improving energy efficiency is important, but very airtight homes still need adequate ventilation.
Contents
- Why indoor air matters
- What the review found
- Damp, mould and lung health
- Aspergillus and aspergillosis
- Ventilation and building design
- What can help reduce risk?
- Help us understand damp homes and health
- When to seek medical advice
Why indoor air matters
Most of us spend a large amount of time indoors — at home, at work, or in public buildings. The air inside buildings can contain particles from many sources, including dust, mould spores, bacteria, viruses, cooking, cleaning products, pets and outdoor air entering the home.
The recent review, Exposure Risks from Microbiological Hazards in Buildings and Their Control — A Rapid Review of the Evidence, looked at evidence for harmful microorganisms in indoor air and on surfaces, and how building design, ventilation and moisture affect exposure.
What the review found
The review found strong evidence that microorganisms can be present in indoor air and on surfaces. These include fungi, bacteria and viruses. The evidence was strongest for the role of dampness and poor ventilation in increasing the risk of indoor mould growth and respiratory health effects.
The review’s main conclusions included:
- Airborne allergenic fungi are well documented in indoor air.
- Damp conditions increase mould growth and mouldy odours indoors.
- Dampness and mould are associated with respiratory ill health, including asthma, rhinitis and wheezing.
- Penicillium, Aspergillus and Cladosporium are commonly detected in damp buildings.
- Infectious viruses and bacteria can also be detected in indoor air and on surfaces.
- Ventilation is a key control measure for reducing moisture and diluting airborne contaminants.
Damp, mould and lung health
Dampness is one of the most important drivers of indoor mould growth. Moisture can come from leaks, condensation, flooding, poor insulation, inadequate heating, drying clothes indoors, cooking, showering, or poor ventilation.
When dampness persists, mould can colonise indoor materials such as plasterboard, wallpaper, wood, carpets, soft furnishings and settled dust. Mould may be visible, but it can also grow in hidden areas such as behind furniture, inside wall cavities, behind wallpaper, under flooring, or around poorly ventilated cold surfaces.
Exposure to damp and mould has been linked with:
- Wheezing
- Asthma symptoms or asthma worsening
- Rhinitis and nasal symptoms
- Cough
- Respiratory infections
- Worsening symptoms in people with existing lung disease
Importantly, the review notes that the relationship between indoor microorganisms and health is complex. Risk depends on the type of organism, the level of exposure, the building conditions and the susceptibility of the person exposed.
Aspergillus and aspergillosis
Aspergillus is a common mould found in the environment. Most people inhale Aspergillus spores every day without becoming ill. However, some people are more vulnerable, including those with asthma, bronchiectasis, chronic lung disease, weakened immune systems, or previous lung damage.
In susceptible people, exposure to Aspergillus may contribute to conditions such as allergic bronchopulmonary aspergillosis (ABPA), severe asthma with fungal sensitisation (SAFS), aspergillus bronchitis, or chronic pulmonary aspergillosis (CPA). The home environment is not the only source of exposure, but damp indoor spaces may increase the amount of fungal material a person breathes in.
This does not mean that every damp home causes aspergillosis, or that every person exposed to mould will become ill. It does mean that reducing dampness, improving ventilation and addressing visible or hidden mould are sensible steps for respiratory health.
Ventilation and building design
One of the strongest messages from the review is that ventilation is central to controlling indoor microbiological risk. Ventilation helps by:
- Removing moisture from indoor air
- Reducing condensation
- Diluting airborne mould spores and other particles
- Reducing the build-up of infectious aerosols
- Improving overall indoor air quality
The review also highlights an important modern problem. Homes are increasingly designed or retrofitted to be more airtight and energy efficient. This can improve warmth and reduce energy use, but if ventilation is inadequate, moisture and airborne contaminants may accumulate indoors.
In other words, insulation and energy efficiency are important, but they need to be balanced with effective ventilation and moisture control.
What can help reduce risk?
The review does not suggest that one single action solves all indoor air problems. Instead, it supports a combined approach.
1. Reduce moisture
- Repair leaks promptly.
- Check roofs, gutters, pipes and window seals.
- Use extractor fans in kitchens and bathrooms where available.
- Avoid drying clothes indoors where possible, or ventilate well if you do.
- Reduce condensation on windows and cold walls.
2. Improve ventilation
- Use trickle vents if fitted.
- Open windows when safe and practical.
- Use mechanical ventilation systems correctly.
- Keep air bricks and vents clear.
- Make sure extractor fans are working effectively.
3. Deal with mould safely
- Small areas of surface mould may be cleaned carefully using appropriate household methods.
- Large, persistent or recurring mould usually needs the underlying damp problem fixed.
- People with significant lung disease, immune suppression or severe symptoms should avoid heavy mould disturbance and seek advice.
4. Reduce dust reservoirs
- Regular cleaning can reduce settled dust and spores.
- HEPA-filter vacuum cleaners may be helpful for some households.
- Hard flooring may be easier to keep dust-free than carpets in high-risk situations.
5. Consider air filtration where appropriate
Portable high-efficiency particulate air (HEPA) filters may help reduce airborne particles in some settings. They are not a substitute for fixing damp or improving ventilation, but they may be a useful additional measure for some people.
Help us understand damp homes and health
The evidence linking damp homes, mould and respiratory health is strong, but there are still important unanswered questions. We need to better understand how different homes, building types, ventilation patterns and damp conditions affect people’s health in real life.
The National Aspergillosis Centre is running a UK citizen science study looking at damp homes and health.
We are inviting people to register their interest in taking part.
The study is open to people with and without lung conditions, and to people living in homes with or without damp or mould. This comparison is important because it helps researchers understand which factors are most strongly linked with health outcomes.
Register your interest in the damp homes and health study
Taking part may involve completing a questionnaire and, at a later stage, providing a dust sample from your home. The information gathered will help improve understanding of indoor environments and respiratory health.
When to seek medical advice
Please seek medical advice if you have:
- New or worsening breathlessness
- Chest pain
- Coughing up blood
- Persistent fever
- Repeated chest infections
- Rapidly worsening asthma symptoms
- Unexplained weight loss or severe fatigue
If you already have aspergillosis, asthma, bronchiectasis, chronic obstructive pulmonary disease (COPD), immune suppression, or another lung condition, it is worth discussing any significant damp or mould exposure with your healthcare team.
Common questions
Can mould affect health even if I cannot see it?
Yes. Hidden mould or dampness may still affect indoor air quality. A musty smell, persistent condensation or symptoms that worsen in a particular room may suggest a problem.
Does all mould cause aspergillosis?
No. Mould exposure is common, and most people do not develop aspergillosis. Aspergillosis usually occurs when exposure combines with individual susceptibility, such as asthma, bronchiectasis, immune suppression or existing lung damage.
Is ventilation always good?
Ventilation is usually important for reducing moisture and improving indoor air quality. However, the best approach depends on the building, outdoor conditions and the person’s health. Ventilation should not replace fixing leaks or removing sources of damp.
Can air purifiers solve damp and mould problems?
No. Air purifiers may reduce airborne particles, but they do not remove the source of moisture or mould growth. Damp problems need to be addressed at source.
Summary
This recent evidence review reinforces a practical message: indoor air quality matters. Dampness, poor ventilation and mould growth are not simply cosmetic housing problems — they can affect respiratory health, especially in people with asthma, aspergillosis or other lung conditions.
The most effective approach is to reduce moisture, improve ventilation, remove mould sources where possible and understand how buildings influence exposure. Research such as the UK damp homes and health study will help build better evidence for patients, clinicians, housing providers and policymakers.
References and further reading
- Beswick A, Crook B, Gosling B, et al. Exposure Risks from Microbiological Hazards in Buildings and Their Control — A Rapid Review of the Evidence. Atmosphere. 2025;16:1243. doi:10.3390/atmos16111243.
- Damp homes and health study — register your interest
- Aspergillosis.org — patient and carer information
Article type: Patient and public information
Last reviewed: April 2026
Based on: Recent evidence review of microbiological hazards in buildings and their control.
Help us understand how damp homes affect health

We are supporting a UK research project looking at how damp homes may affect health, including respiratory health and conditions such as aspergillosis.
This study is being led by the National Aspergillosis Centre at Manchester University NHS Foundation Trust, and is being shared through aspergillosis.org to support research into damp homes and health.
We are currently inviting people across the UK to register their interest in taking part.
Registering your interest should take less than one minute and does not commit you to taking part.
Why this matters
Damp and mould are often linked to health problems, but there is still limited real-world evidence from people’s homes across the UK.
This project aims to help improve understanding of how home environments may affect health by gathering information from people living in a wide range of housing conditions.
Who can register interest?
We would like to hear from people living in the UK, including:
- people with lung or respiratory conditions
- people without any known lung or breathing condition
- people who have experienced damp or mould at home
- people who have not experienced damp or mould at home
- members of the general public who would like to contribute to the research
We are keen to hear from people with different health backgrounds and a wide range of home environments.
What is the study about?
This research is exploring how damp homes may affect health. The aim is to improve understanding of the relationship between home environments and health symptoms in real-world settings.
This project is for research purposes only and does not provide medical advice or diagnosis.
What might taking part involve later?
If the study opens, some people who register interest may later be invited to:
- complete a short questionnaire about their home and health symptoms
- receive a simple home sampling kit by post
- collect and return a small household sample, for example dust from the home, for research purposes
The home sampling part is intended to be simple and practical. Full instructions would be provided.
Registering your interest now does not commit you to taking part later.
Important information
- Registering interest is voluntary.
- You do not have to take part in the full study later.
- Your details will only be used to contact you about this project.
- Your data will be handled in line with UK data protection regulations.
- You can decide later whether or not to take part.
Frequently asked questions
Am I signing up to take part in the study now?
No. At this stage, you are only registering your interest in hearing more about the study.
Do I need to have a lung condition to register interest?
No. We would like to hear from people with and without lung conditions.
Do I need to have damp or mould in my home?
No. We are interested in hearing from people with a wide range of home environments and experiences.
Will I definitely receive a kit?
Not necessarily. Registering interest helps the research team understand the level of interest and contact people if the study opens.
Will I get personal results about my home or health?
At this stage, no individual results are being promised. More information would be provided if the study proceeds.
What happens after I register interest?
You do not need to do anything further straight away. If the study opens, you may be contacted with more information so you can decide whether you would like to take part.
Register your interest
Ready to help? Complete the form below.
This secure form should take less than one minute to complete.
If the form does not load, you can open it here:
Open the form in a new window
Mould, “Toxins” and Aspergillus: Understanding What’s True and What Isn’t
Last reviewed: April 2026
Key points
- Exposure to mould is not the same as having aspergillosis.
- Aspergillus is a common environmental fungus that most people inhale daily.
- “Mycotoxin” and “detox” explanations are common online but are not part of standard diagnosis.
- Symptoms usually arise from a combination of lung disease, infection, inflammation, and environment.
- Diagnosis relies on clinical tests (scans, blood tests, microbiology), not environmental testing alone.
- Specialist home testing is sometimes used—but only in specific clinical situations.
A guide for patients and carers
Many people with lung conditions come across information linking mould exposure, toxins, and Aspergillus infections. Some of this information can be helpful—but much of it can also be confusing.
This article explains the most common misunderstandings and what current medical practice actually relies on.
Important: Some tests measure exposure—but medical diagnosis requires evidence of disease.
Contents
- Why this topic is confusing
- Mould exposure vs Aspergillus disease
- Mycotoxins and “detox” claims
- Why “mould toxin tests” are not used diagnostically
- Why symptoms don’t have one single cause
- How Aspergillus conditions are actually diagnosed
- When home testing may be used
- What matters most for patients
Why this topic is confusing
- Mould is visible and easy to focus on
- Symptoms (fatigue, cough, breathlessness) are non-specific
- Online information often mixes different conditions together
This can lead to the idea that one single cause—such as “mould toxicity”—explains everything. In practice, respiratory conditions are usually more complex.
Mould exposure vs Aspergillus disease
Mould exposure
- Common in homes and outdoor air
- Can irritate airways
- May worsen symptoms
Aspergillus disease
- Occurs in specific medical contexts
- Related to lung structure and immune response
- Requires clinical diagnosis
Important context: Aspergillus spores are present in the air we breathe every day. Most people inhale them without developing disease.
Mycotoxins and “detox” claims
You may see references to:
- “Mycotoxin illness”
- “Die-off reactions”
- “Binders” to remove toxins
These ideas are widely discussed online, but they are not part of standard medical diagnosis or treatment for Aspergillus lung conditions.
This does not mean symptoms are not real. It means they are usually explained through:
- Inflammation
- Infection
- Underlying lung disease
Why “mould toxin tests” are not used diagnostically
Exposure is common
Many people have detectable environmental exposure, so results are not specific.
Results do not match symptoms reliably
Levels do not consistently correlate with disease or severity.
Lack of standardisation
Different labs use different methods, making interpretation difficult.
Not part of clinical guidelines
Major respiratory guidelines do not include these tests in diagnosing Aspergillus conditions.
Risk of confusion
- May cause unnecessary concern
- May lead to unproven treatments
Why symptoms don’t have one single cause
Symptoms often arise from a combination of:
- Underlying lung disease
- Inflammation
- Infection (fungal or bacterial)
- Environmental triggers (pollution, damp)
This is why symptoms can fluctuate and may not respond to a single explanation or treatment.
How Aspergillus conditions are actually diagnosed
Diagnosis is based on a combination of:
- CT imaging
- Blood tests (e.g. IgE, IgG)
- Microbiology (sputum or bronchoscopy)
Environmental testing alone is not sufficient to diagnose disease.
When home testing may be used
In some cases, specialist teams (for example via the Mycology Reference Centre Manchester) may arrange targeted environmental sampling.
This is different from commercial testing and focuses on:
- Specific clinically relevant fungi (e.g. Aspergillus species)
- Known allergens or pathogens
Why it is done
- Established Aspergillus-related disease
- Unexplained or persistent symptoms
- Concern about ongoing exposure
This testing is used to answer specific clinical questions and is interpreted alongside medical findings.
What matters most for patients
- Work with your clinical team for diagnosis and treatment
- Address damp and mould in your home
- Focus on practical steps that improve symptoms
- Avoid relying on a single explanation for complex symptoms
Final takeaway
Mould, environment, and Aspergillus are connected—but not in a simple cause-and-effect way.
Understanding this helps you focus on what is most likely to improve your health: appropriate treatment, good living conditions, and ongoing monitoring.
Author: aspergillosis.org
Note: Educational content only – not medical advice.
Indoor Air Quality, Damp, Mould and Aspergillus
Last reviewed: April 2026
Key points
- Indoor air problems usually relate to pollution, damp, or mould—these are different but can overlap.
- Aspergillus is a normal part of the environment and not automatically a sign of a problem indoors.
- Damp and mould can worsen breathing symptoms and should be taken seriously.
- Fixing the underlying moisture problem is more important than cleaning visible mould.
- Knowing who to contact (GP, landlord, council) is key to resolving problems.
Indoor Air Quality, Damp, Mould and Aspergillus
A practical guide for patients
Many people with aspergillosis or other lung conditions are concerned about the air inside their home. This article explains how indoor air quality works, how to recognise problems, and what steps you can take to improve your environment.
Contents
- What affects indoor air?
- Three common problems
- Aspergillus in the home
- Damp and mould
- Symptoms and health effects
- Identifying problems
- Getting the right help
- Practical steps
- Air purifiers
What affects indoor air?
Indoor air quality is influenced by both indoor and outdoor factors. People spend most of their time indoors, so even small issues can have a noticeable effect on health. :contentReference[oaicite:0]{index=0}
Indoor air can be affected by:
- Outdoor pollution entering the building
- Damp and moisture
- Mould growth
- Cooking, heating, and cleaning products
- Dust and particles
Three common indoor air problems
1. Indoor air pollution
- Particles from cooking, heating, and candles
- Outdoor pollution enters indoors
2. Damp (moisture)
- Condensation, leaks, poor ventilation
- Creates conditions for mould growth
3. Mould
- Visible fungal growth on surfaces
- Releases spores into the air
Aspergillus in the home
Aspergillus is a common environmental fungus found in air, dust, and soil.
This means:
- Everyone breathes in Aspergillus spores regularly
- Indoor exposure is not unusual
Important: Exposure does not equal disease. Aspergillosis depends on lung health and immune response—not just environment.
Damp and mould
Damp and mould are important because they can affect respiratory health. Damp homes are linked with increased respiratory symptoms and illness. :contentReference[oaicite:1]{index=1}
UK guidance highlights that damp and mould can produce irritants and spores that affect the lungs and should be addressed promptly. :contentReference[oaicite:2]{index=2}
Symptoms and health effects
Indoor air problems may contribute to:
- Cough
- Breathlessness
- Wheeze
- Chest tightness
- Fatigue
These symptoms often overlap with infection or underlying disease, making them difficult to interpret.
Identifying problems
Signs of damp
- Condensation on windows
- Cold or damp walls
- Peeling paint or wallpaper
- Musty smell
Signs of mould
- Black or green patches
- Mould returning after cleaning
- Growth behind furniture or in corners
Hidden issues
- Persistent damp smell
- Symptoms are worse in certain rooms
Getting the right help
1. Your healthcare team
- If symptoms worsen
- If you suspect your environment is affecting your health
2. Landlord or housing provider
- Report problems early
- Keep records (photos, dates)
UK guidance makes clear that damp and mould should be addressed promptly and not ignored.
3. Local council
- If landlord does not act
- If health is affected
Further reading
See more detailed guidance and support resources here:
Housing, damp and mould articles (aspergillosis.org)
Practical steps
- Improve ventilation (especially kitchens and bathrooms)
- Reduce moisture
- Address leaks quickly
- Clean small mould areas safely
Air purifiers
Air purifiers can reduce airborne particles, but:
- They do not fix damp
- They do not remove mould from surfaces
- They do not treat aspergillosis
Final takeaway
Indoor air problems are common and often manageable. The key is to:
- Recognise the signs early
- Address moisture and mould properly
- Seek help when needed
Author: aspergillosis.org
Note: This article is for general education and does not replace medical advice.
Damp & Mould Health Evidence Monitor: 4 March 2026
Date of check
4 March 2026
🆕 New papers since last check
Early-life indoor mould exposure and lung function
Journal: Environmental Research: Health
Published: Feb 2026
Summary
Children exposed to serious indoor mould in early life showed:
-
reduced lung function in adolescence
-
increased risk of asthma during childhood
This study used long-term cohort data and objective lung function testing, strengthening the evidence that early mould exposure can have lasting respiratory consequences.
PMID: 39162373
PubMed link:
https://pubmed.ncbi.nlm.nih.gov/39162373/
Damp and mouldy homes: impact on lung health in childhood
Authors: Moorcroft C, Whitehouse A, Grigg J
Journal: Archives of Disease in Childhood (2025)
Summary
This clinical review explains how damp housing contributes to:
-
childhood asthma
-
recurrent respiratory infections
-
allergic disease
It emphasises that paediatric clinicians frequently encounter children whose symptoms are linked to poor housing conditions.
PMID: 39814530
PubMed link:
https://pubmed.ncbi.nlm.nih.gov/39814530/
Damp housing and mental health effects
Journal: Environmental Health Perspectives
Summary
A major review examining whether damp and mould exposure affects mental health.
Evidence suggests associations with:
-
anxiety
-
depression
-
psychological stress
Mechanisms may include chronic illness, housing insecurity, and inflammatory responses to mould exposure.
PMID: 39162373
PubMed link:
https://pubmed.ncbi.nlm.nih.gov/39162373/
📊 Summary
New or important items identified
• Evidence continues to strengthen the link between damp housing and respiratory disease
• Long-term cohort data show effects on lung development
• Emerging research also suggests mental health impacts
Health effects: why aspergillosis patients are higher-risk
Home › Knowledge Hub › Damp, mould and aspergillosis › Health effects
This page explains what damp and mould can do to the lungs and how to recognise patterns that suggest your home is contributing to symptoms.
How damp buildings can affect the lungs
Damp homes can increase exposure to airborne particles including fungal spores and fragments. For many people this causes irritation; for people with chronic lung disease it can trigger significant exacerbations.
- Worsening cough, wheeze, breathlessness
- Increased mucus and reduced airway clearance
- More frequent chest infections / antibiotic courses
- Allergic-type reactions in sensitised individuals
Why aspergillosis and severe airways disease are different
If you have Aspergillus-related disease or severe asthma/bronchiectasis, your airways may react strongly to fungal material and irritants. Some patients also require systemic or inhaled corticosteroids, which can increase susceptibility to infections and complicate symptom control.
Important nuance: a damp home does not automatically “cause” aspergillosis, but it can be a powerful driver of persistent symptoms and repeated flares.
Patterns that support a housing contribution
- Time-and-place pattern: symptoms worsen at home and improve when away (even partially).
- Multi-person effects: more than one household member develops respiratory/allergic symptoms.
- Post-disturbance worsening: symptoms worsen after “repairs” or “remediation”.
- Escalating medication use: increased reliever inhaler/nebuliser use, repeated steroid bursts, more antibiotics.
Simple symptom timeline template (copy/paste)
Keeping a short, factual timeline helps clinicians and councils understand risk.
Date(s): Where damp/mould is present: What changed (rain event, leak, repair work, return after decant): Symptoms (breathlessness/wheeze/cough/fever/skin/eyes/nose): Medication change (inhalers, steroids, antibiotics): Healthcare use (GP/A&E/hospital): Improves when away from home? (yes/no, how quickly):
What to ask your clinician to document
- Diagnosis (e.g., Chronic pulmonary aspergillosis, allergic bronchopulmonary aspergillosis, asthma, bronchiectasis)
- That symptoms are consistent with environmental triggers or worsened by damp/mould exposure (they do not need to prove causation)
- Any vulnerability factors (steroid use, immunosuppression, reduced lung function)