What drugs are being developed to reduce steroid intake
Here’s a breakdown of what’s already available and what’s on the horizon:
🧬 Biologics – the biggest game-changer
These are antibody-based therapies that target specific immune pathways, rather than suppressing the whole immune system like steroids do.
✅ Already used off-label or in trials for ABPA:
1. Omalizumab (Xolair)
-
Targets IgE (the allergy antibody that’s sky-high in ABPA)
-
Already licensed for severe allergic asthma
-
Studies show it reduces exacerbations, improves lung function, and helps taper off steroids
-
Limitations: expensive, dosing based on IgE levels and weight (difficult in patients with very high IgE)
2. Mepolizumab (Nucala)
-
Targets IL-5, which drives eosinophil activity
-
Approved for eosinophilic asthma
-
Used in some ABPA patients, especially when eosinophils remain high
-
Can help reduce steroid use and fungal exacerbations
3. Benralizumab (Fasenra)
-
Also targets IL-5 receptor – causes direct depletion of eosinophils
-
Similar benefits to mepolizumab but may act faster
-
Small studies and case reports show promise in ABPA and chronic pulmonary aspergillosis with eosinophilia
4. Dupilumab (Dupixent)
-
Blocks IL-4 and IL-13, key drivers of Th2 inflammation
-
Approved for asthma, atopic dermatitis, and nasal polyps
-
Early evidence suggests it may benefit ABPA patients, especially those with co-existing nasal polyps or eczema
-
Could be ideal for steroid-sparing in allergic fungal disease
💊 Antifungals as steroid-sparing agents
Already in use, but still being optimized:
-
Itraconazole
-
Voriconazole
-
Posaconazole
-
Isavuconazole (being explored more recently, better tolerated in some patients)
These reduce fungal burden, which helps turn down the immune overreaction—letting steroids be tapered or even avoided in some patients.
🔬 In Development or Under Investigation
🧪 Tezepelumab
-
Blocks TSLP (thymic stromal lymphopoietin) – an early signal in allergic inflammation
-
In trials for severe asthma
-
May be helpful in ABPA down the line – trials are ongoing
🧪 Anti-IL-33 and Anti-ST2 therapies
-
IL-33 is another "alarmin" involved in allergic responses
-
Still in early stages, but being watched closely for steroid-sparing potential in allergic lung diseases
🌍 Other Strategies Being Studied
-
Inhaled antifungals (e.g., inhaled voriconazole or amphotericin B) – may reduce systemic side effects
-
Vaccines against Aspergillus – still early stage
-
Mucolytics and anti-inflammatory antibiotics (e.g., azithromycin) as steroid-sparing support in some patients
🤔 What You Can Do Now
-
If you’re struggling with steroid side effects or dependency, it’s totally reasonable to ask your respiratory team:
-
“Am I a candidate for a biologic like omalizumab or mepolizumab?”
-
“Is my antifungal therapy optimized?”
-
“Would a switch to inhaled or combination therapy help reduce my steroid use?”
-
🌙 How to Manage Insomnia (Gently and Practically)
🧠 1. Understand the Type
Not all insomnia is the same — and understanding the pattern helps guide what to try.
-
Sleep-onset insomnia = can’t fall asleep
-
Sleep maintenance insomnia = wake up often or too early
-
Mixed = both
This affects what works — e.g., sleep-onset responds well to wind-down rituals, while maintenance might need different support.
🕯️ 2. Evening Wind-Down (Not Just “No Screens”)
Forget rigid rules — the key is sending cues to your nervous system that it’s safe to rest.
✅ Try:
-
Warm drink (caffeine-free herbal tea, warm milk)
-
Warm bath or shower
-
Dim lights, soft music, reading something gentle
-
A short evening walk (light exposure helps your body clock)
❌ Avoid:
-
Stressful news
-
Heavy exercise right before bed
-
Working or arguing in the bedroom
⏰ 3. Rethink the Clock
Insomnia often creates performance anxiety: “I must sleep now.” This makes things worse.
💡 Try:
-
Cover the clock or put it out of view
-
Get out of bed if you're awake >20–30 mins, and do something boring or calming (puzzle, stretching, audiobook)
-
Go back to bed only when sleepy
📆 4. Consistency is King
Even if you sleep badly, try to:
-
Wake up at the same time every day
-
Don’t “make up” for poor sleep with long naps or sleeping in — it confuses your body clock
This retrains your circadian rhythm.
🧘♀️ 5. Calm the Mind (Not Force Sleep)
Racing thoughts? Try:
-
Box breathing or 4-7-8 breathing
-
Body scan meditation (many free ones on YouTube or Calm app)
-
Journaling before bed to “park” worries
-
CBT for Insomnia (CBT-I) — best evidence-based therapy
Apps like Sleepio, Pzizz, Insight Timer, or Headspace have helpful guided sessions.
🌿 6. Gentle Natural Aids
These aren’t cures, but they can help some people feel drowsier:
-
Magnesium glycinate
-
Valerian root, passionflower, ashwagandha
-
Melatonin (best for circadian issues like shift work or jet lag — less effective for general insomnia)
Always check for interactions, especially with other meds.
🗣️ 7. When to Get Help
See a GP or sleep specialist if:
-
It’s lasting more than 3 months
-
It’s impacting daily functioning or mood
-
You have signs of sleep apnea, restless legs, or depression/anxiety
They can guide you through structured therapy or rule out hidden causes.
Swimming for people with aspergillosis
How could you advise someone with aspergillosis who wants to swim but finds the local pool triggers their asthma?
Great question — and can be really important for quality of life. For someone with aspergillosis (especially ABPA or CPA) and asthma that worsens in chlorinated pools, here’s a tailored guide that balances safety with enjoyment:
🏊♀️ Swimming with Aspergillosis + Chlorine Sensitivity: A Practical Guide
💡 1. Choose the Right Pool Environment
Goal: Minimise chloramine exposure (which irritates airways).
✅ Best options:
-
Ozone- or UV-treated pools: These significantly reduce chloramine levels.
-
Saltwater pools: Gentler, although still chlorinated (just less harsh).
-
Natural pools or lidos: Often free from chlorine, especially in outdoor settings.
-
Seawater swimming: The ultimate in chlorine-free options if you're near the coast and it's safe.
🚫 Avoid:
-
Indoor pools with poor ventilation
-
Pools that "smell strongly of chlorine" — this usually means high chloramines
🕗 2. Swim at Low-Traffic Times
-
Early morning swims are ideal — before other swimmers add organic matter (sweat, sunscreen, etc.), which reacts with chlorine to form irritants.
-
Ask the pool when they clean/shock it — swimming after that is usually better.
🧤 3. Protect Your Airways
-
Use a nose clip to avoid inhaling water vapor directly through the nasal passages.
-
Consider wearing a light face mask (e.g., FFP2) on the poolside until just before entering, to avoid breathing chloramines in enclosed spaces.
-
Ventolin (salbutamol) or another rescue inhaler should always be close by — even poolside if staff are aware.
💊 4. Pre-medicate if Needed
With your doctor’s advice, consider:
-
Short-acting bronchodilator 15–30 mins before swimming (e.g., salbutamol)
-
Leukotriene receptor antagonists (like montelukast) for added airway protection
-
Nasal rinses or corticosteroid sprays post-swim if you’re prone to sinus issues
🚿 5. Shower Immediately After
To reduce any skin or airway irritation:
-
Warm shower straight after
-
Nasal rinse or saline spray
-
Clean/dry clothes quickly to avoid damp mold exposure
🏞️ 6. Explore Alternative Swimming Options
-
Outdoor pools or lidos
-
Swimming lakes or sea-based pools (like Bude Sea Pool)
-
Private or spa pools with alternative sanitisation systems
-
Aquatherapy centres: Often use lower chemical levels and may cater to sensitive lungs
💬 7. Talk to Pool Staff
Many pools are willing to help. Try:
“I have a medical lung condition that reacts to chloramines — can you tell me when chlorination is lowest or if you use UV systems?”
You might be surprised how supportive they are.
Help Us Explore a New Treatment for Chronic Pulmonary Aspergillosis (CPA)
We’re Recruiting for a Clinical Trial of Interferon-Gamma (IFNγ)
We’re looking for people with chronic pulmonary aspergillosis (CPA) to take part in an exciting clinical trial testing a new treatment approach using interferon-gamma (IFNγ) — a substance that could help the immune system fight the Aspergillus infection more effectively.
What is CPA?
CPA is a long-term lung infection caused by the fungus Aspergillus. It usually affects people with chronic lung diseases like COPD or those who’ve had tuberculosis (TB) in the past. Over time, CPA can cause:
-
Enlarging cavities in the lungs
-
Recurrent chest infections
-
Persistent coughing and fatigue
-
Worsening breathlessness and reduced quality of life
It’s a progressive condition and can be hard to diagnose early. Around 3,600 people are living with CPA in the UK. Without effective treatment, CPA can be life-limiting — up to 4 in 10 people may die within five years of diagnosis.
Current Treatment Challenges
Treatment typically involves long-term antifungal medication, but:
-
Only about 60% of patients improve
-
Treatment can be lifelong, with relapses common
-
There is only one class of oral antifungals available
-
Side effects and high costs are frequent problems
This is why we urgently need better treatment options.
Why Interferon-Gamma?
Our research suggests that many CPA patients may have a weakened immune response, particularly a lower production of interferon-gamma (IFNγ) — a natural substance that helps the body fight fungal infections like Aspergillus.
In small studies, giving IFNγ to patients who didn’t respond to antifungals showed fewer lung flares, fewer hospital stays, and better quality of life. It’s already used safely in other NHS treatments — now we want to explore its role in CPA.
What This Trial Involves
We’re running a randomised clinical trial to test IFNγ in CPA. Here’s what to expect:
-
You must be starting antifungal treatment for CPA
-
You’ll be randomly placed in one of two groups:
-
One group receives IFNγ + antifungals for 12 weeks
-
The other group receives antifungals only
-
-
We’ll monitor:
-
Changes in lung CT scans
-
Quality-of-life scores
-
Any side effects or problems with tolerability
-
The trial will include 50 participants in total (25 in each group) and is expected to run until August 2026.
Why Your Participation Matters
By joining this study, you’ll help us find out whether IFNγ could:
-
Improve treatment outcomes
-
Shorten the duration of therapy
-
Prevent relapses
-
Potentially benefit others with chronic lung diseases
If successful, this could lead to a larger trial and possibly a new standard treatment for CPA.
Interested in Taking Part?
You may be eligible if you:
-
Have been diagnosed with CPA
-
Are about to start antifungal treatment
-
Are willing to attend follow-up appointments for 12 weeks
👉 Click here for full details and how to take part
Steroid-induced insomnia
Steroid-induced insomnia is a common and frustrating side effect of corticosteroid medications like prednisolone, dexamethasone, or hydrocortisone — especially when taken for conditions like aspergillosis, adrenal insufficiency, or inflammatory diseases.
🧠 Why it Happens
Corticosteroids affect the brain’s sleep-wake cycle and increase levels of cortisol-like hormones, which can make you feel:
-
Wired or overstimulated
-
Restless or anxious
-
Unable to fall asleep or stay asleep
Even low-to-moderate doses can affect sensitive sleepers, especially when taken in the afternoon or evening.
🕒 Tips to Manage It
1. Take Steroids in the Morning (if possible - discuss with your doctor)
Mimics the body’s natural cortisol rhythm and reduces sleep disruption.
2. Create a Wind-Down Routine
Try calming activities in the evening — reading, gentle music, warm bath, breathing exercises.
3. Avoid Stimulants After 2 PM
That includes caffeine, nicotine, and even long naps.
4. Sleep Hygiene Helps
Keep your room cool and dark
Avoid screens at least an hour before bed
Stick to a regular sleep schedule
5. Melatonin (with caution)
Some doctors may suggest melatonin to reset sleep patterns — but always ask first, especially if you're on multiple meds.
💊 Medical Support
If insomnia is severe or long-lasting:
-
Your doctor might adjust your steroid dose or timing
-
A short course of sleep aids may be prescribed if needed
-
Sometimes adding a mood stabilizer or sedating medication at night (like mirtazapine or a low-dose antihistamine) is helpful
Managing the stress of having a chronic disease, could it even be PTSD?
Let’s look at some of the best ways patients can manage chronic illness-related stress, especially when it edges into PTSD territory:
🧠 1. Acknowledge It’s Trauma
-
First: you’re not overreacting. Living with the constant threat of something like a lung bleed is traumatic.
-
Repeated hospital visits, coughing up blood, uncertainty—it can leave a person hypervigilant, anxious, and emotionally worn out.
🗣️ 2. Trauma-Informed Therapy
-
PTSD-like symptoms (flashbacks, panic, avoidance) can respond really well to therapies like:
-
CBT (Cognitive Behavioural Therapy)
-
EMDR (Eye Movement Desensitisation and Reprocessing) – especially useful for medical trauma
-
ACT (Acceptance & Commitment Therapy) – often used in chronic illness
-
-
Ask for a therapist familiar with chronic illness or health-related trauma.
🧾 You can usually request a referral from your GP, or seek out private therapy if accessible.
🧘 3. Mind-Body Practices
Some proven stress-reducing tools:
-
Breathwork (even just gentle box breathing: in 4s, hold 4s, out 4s, hold 4s)
-
Mindfulness (not just meditation, but moment-by-moment grounding)
-
Yoga or tai chi (adapted for lung health if needed)
-
Trauma-informed movement: gentle, non-triggering physical activity can help discharge stress.
💬 4. Peer Support (Online or In Person)
-
Talking to people who get it can massively reduce isolation.
-
Look for groups for:
-
Chronic lung disease / aspergillosis
-
Rare disease communities
-
Health anxiety or chronic illness PTSD
-
🌐 Aspergillosis Trust and NTM Patient Care UK sometimes link patients to support forums.
📖 5. Create a Health Toolkit or “Plan”
One big part of PTSD is the loss of control. Building a personal toolkit helps:
-
Written action plan for what to do during a flare or bleed (with your doctor)
-
Keep emergency contacts + hospital info handy
-
Have a “go bag” ready if hospital visits are frequent
-
Set up a small win routine (e.g., meds, hydration, small walk, rest)
💊 6. Medication Support (If Needed)
-
If panic, anxiety, or intrusive thoughts are severe, short-term or long-term medication can help.
-
SSRIs, low-dose beta blockers for panic symptoms, or sleep support may be part of care.
-
Work with a GP or psychiatrist who understands both mental health and chronic disease.
🧡 7. Give Yourself Credit and Kindness
This is hard. You’re surviving a reality most people can’t imagine. The fear is real. The strength it takes to keep going with all that fear is real too.
If you’d like, I can help you draft a personal “resilience plan” based on your needs—something tangible to refer to when you’re overwhelmed.
Let’s create a Personal Resilience Plan tailored to someone living with a chronic lung condition (like ABPA or CPA), with anxiety around lung bleeds and possible PTSD-like stress. This plan is meant to help you feel more grounded, supported, and in control, even when things feel overwhelming.
🛡️ Your Personal Resilience Plan
For Managing Chronic Illness, Lung Bleed Anxiety, and PTSD-Related Stress
🧭 1. Grounding Statement (Your “North Star”)
“I live with a serious condition, but I am not alone. I have tools, people, and plans that help me stay steady, even in scary moments.”
Use this when panic or flashbacks arise.
🧰 2. Emergency Action Plan
Having a clear plan for “what to do if…” takes the edge off the unknown.
✅ In case of a suspected lung bleed:
-
Stay calm, sit upright, lean slightly forward.
-
Call 999 (or your emergency contact) if bleeding is profuse or you feel faint.
-
Notify hospital/clinic (add number here:
__________) -
Use oxygen if prescribed. Avoid lying flat.
-
Bring your go bag with essentials (see below).
✅ Go Bag Checklist:
-
Hospital letters
-
Medication list
-
Emergency contact numbers
-
Water, charger, snacks, headphones
-
Comfort item (photo, small item that grounds you)
💬 3. People to Call/Text When You’re Struggling
| Name | Contact | Role |
|---|---|---|
| GP / Specialist Nurse | [Name] – [Number] | Medical support |
| Friend or Family Member | [Name] – [Number] | Emotional support |
| Therapist / Mental Health Contact | [Name] – [Number] | Grounding and talking it through |
| Crisis Line | 116 123 (Samaritans, 24/7 UK) | Non-judgmental emotional support |
🧠 4. PTSD & Anxiety Coping Tools
Choose 2–3 from each category that resonate with you:
🌬️ In-the-Moment Grounding Techniques:
-
Box breathing: In for 4, hold 4, out 4, hold 4
-
5-4-3-2-1 grounding: Name 5 things you see, 4 you feel, 3 you hear, 2 you smell, 1 you taste
-
Hold a cold item (ice cube or chilled bottle) — physical sensation brings you back to the present
✍️ Ongoing Processing Tools:
-
Keep a “bad day journal” just to vent — no need for polish
-
Write letters to your past self (“You got through that.”) or future self (“Here’s what helps next time.”)
📱 Helpful Apps:
-
Insight Timer (free guided breathing + trauma-sensitive meditations)
-
MindShift CBT (helps reframe anxious thoughts)
-
PTSD Coach (developed by clinicians, good for triggers + tracking)
🧘 5. Daily Resilience Routine (Small Wins Only)
Design this with chronic illness in mind — flexible and compassionate:
-
🌞 Wake up + check-in (1–10: how’s body/mind today?)
-
💊 Meds + hydration
-
👣 Gentle movement (walk to garden, stretch, or none if flaring)
-
📓 1 thing I’m grateful for, 1 thing I’m proud of
-
🌙 Wind-down: calm music, bath, story podcast
💡 6. Medical Empowerment
-
Keep a written copy of your diagnosis, meds, and hospital plan
-
Ask your doctor for a specific protocol for what to do if bleeding recurs
-
Track symptoms via app or paper log — this helps you feel seen and them spot patterns
🧑🤝🧑 7. Support Network
Consider joining:
-
Aspergillosis Trust Facebook Group: very active and supportive
-
Try finding PTSD supportive groups that suit your situation (many on Facebook and Reddit)
For more general guidance, try NHS PTSD webpages
HEPA filters & heat to reduce exposure to allergens
Patients with forms of aspergillosis like ABPA can be highly allergic to fungal and many other airborne allergens. For some, relief can be found by ensuring the levels of airborne allergens in the home are as low as possible—this means removing as much dust as possible and removing sources of dust in the home.
Fungal spore fragments can be extremely small so air filters and vacuum cleaners have to have HEPA-grade filtration systems in order to be effective. NB there are some air cleaning systems that do not use filtration as a means to remove particles, instead they use heat (see bottom of page).
For those that use HEPA filters it is important that the correct grade of HEPA filtration is provided:
HEPA (High-Efficiency Particulate Air) filters are classified into different grades based on their filtration efficiency. The most commonly used classification is from ISO 29463 (based on EN 1822-1), which divides HEPA filters into E (Efficiency), H (High Efficiency), and U (Ultra-Low Penetration Air - ULPA) categories.
HEPA Filter Grades and Their Uses
| Filter Class | Efficiency (MPPS - Most Penetrating Particle Size, ~0.1-0.3 μm) | Common Applications |
|---|---|---|
| E10 | ≥ 85% | Pre-filters in air purification systems |
| E11 | ≥ 95% | Air conditioning systems, HVAC filters |
| E12 | ≥ 99.5% | General air filtration, residential HEPA vacuum cleaners |
| H13 | ≥ 99.95% | Medical facilities, clean rooms, operating theaters |
| H14 | ≥ 99.995% | Pharmaceutical industry, laboratories, high-end medical applications |
| U15 | ≥ 99.9995% | Semiconductor manufacturing, critical research labs |
| U16 | ≥ 99.99995% | Nuclear and hazardous material containment |
| U17 | ≥ 99.999995% | Highly sensitive biological or radioactive environments |
Key Uses of Different HEPA Grades
- E10-E12: Used in standard HVAC systems, air purifiers, and vacuum cleaners.
- H13-H14: Common in hospitals, clean rooms, and biosafety labs where high air purity is needed.
- U15-U17 (ULPA): Found in pharmaceutical manufacturing, semiconductor industries, and nuclear facilities.
For medical conditions like ABPA, HEPA H13 or H14 filters are recommended in home air purifiers and hospital settings to reduce airborne Aspergillus spores.
Heat-based filtration
Some domestic air purifiers use heat-based filtration to neutralize airborne contaminants. These typically work by heating air to a high temperature to kill bacteria, viruses, mould spores, and other pathogens before cooling them down and releasing them into the room.
Types of Heat-Based Air Cleaners
-
Thermodynamic Sterilization (TSS) Air Purifiers
- Uses a ceramic core heated to ~200°C (392°F) to destroy airborne microorganisms.
- No filters, so there’s no need for replacements.
- Example: Airfree air purifiers (popular in allergy-sensitive households).
-
Hybrid Heat & Filtration Systems
- Combines heat sterilization with HEPA filters or activated carbon.
- Example: Some high-end medical-grade air purifiers integrate thermal disinfection.
Advantages
✔ Kills mold, bacteria, and viruses rather than just trapping them.
✔ No filter replacements (TSS models).
✔ Silent operation (as some don’t use fans).
Disadvantages
❌ Limited particle filtration—doesn’t remove dust, pet dander, or allergens like a HEPA filter does.
❌ Slower purification compared to fan-driven systems.
Best Use Cases
- Allergy and asthma sufferers (e.g., ABPA) who want a maintenance-free solution.
- People sensitive to mold and bacteria in humid environments.
- Homes with immunocompromised individuals needing sterile air.
How the UK evaluates new drugs for use in the NHS
The UK evaluates expensive drugs for cost-effectiveness primarily through the National Institute for Health and Care Excellence (NICE) and other bodies like the Scottish Medicines Consortium (SMC). The evaluation is based on clinical effectiveness, cost-effectiveness, and impact on NHS resources.
Key Aspects of Evaluation
1. Cost-Effectiveness Analysis (CEA) using QALYs
- NICE uses the Quality-Adjusted Life Year (QALY) as a measure to assess whether a drug provides sufficient health benefits relative to its cost.

- If the ICER is below £20,000–£30,000 per QALY, the drug is typically considered cost-effective.
- For certain severe or rare diseases, NICE may allow a higher cost per QALY threshold (e.g., up to £100,000 for very rare conditions under the Highly Specialised Technologies (HST) program).
2. Budget Impact Test
- If a drug is expected to cost the NHS more than £20 million per year, NICE may negotiate with the manufacturer for a Managed Access Agreement (MAA) or phased introduction to spread costs.
3. Clinical Evidence & Real-World Data
- NICE considers clinical trial data, real-world effectiveness, and patient-reported outcomes.
- The NHS Commercial Medicines Directorate may negotiate confidential pricing agreements (e.g., rebates or discounts).
4. NHS England & Special Cases
- For cancer drugs, the Cancer Drugs Fund (CDF) allows faster access while gathering more real-world data.
- The Innovative Medicines Fund (IMF) supports non-cancer drugs with promising early data but uncertain long-term benefits.
5. Scotland & Wales
- The Scottish Medicines Consortium (SMC) and the All Wales Medicines Strategy Group (AWMSG) perform similar cost-effectiveness evaluations for their health systems.
Example: Cost-Effectiveness Evaluation of Omalizumab in the UK
Omalizumab (Xolair) is a monoclonal antibody used for severe allergic asthma and chronic spontaneous urticaria (CSU). Its cost-effectiveness for NHS use was evaluated by NICE based on clinical benefit, quality of life improvement, and economic impact.
1. How is the benefit of Omalizumab calculated?
A. Clinical Benefits (Health Gains)
- Clinical trials show reduced asthma exacerbations, hospitalizations, and improved symptom control.
- Fewer oral corticosteroid (OCS) bursts, reducing side effects (osteoporosis, diabetes risk).
- Improved quality of life due to fewer symptoms and better lung function.
B. Quality-Adjusted Life Years (QALY) Calculation
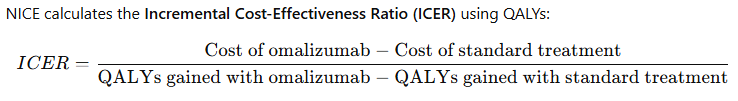
- Without treatment: Patients may experience frequent asthma attacks, reliance on oral corticosteroids, and reduced quality of life (e.g., QALY score = 0.50).
- With Omalizumab: Patients have fewer exacerbations, reduced hospital stays, and improved daily function (e.g., QALY score = 0.72).
- QALYs gained = 0.72 - 0.50 = 0.22**
**NOTE that for Omalizumab initial ICER calculation would have been £8000/26000 (ie. cost of drug) divided by 0.22 (QALY gained) which equals £40-100 000 ie. well above the usual approval threshold of £20-30 000. NHS presumably negotiated a way around that problem to allow approval of Omalizumab.
2. Cost-Effectiveness of Omalizumab
A. NHS Cost Evaluation
- Omalizumab cost: ~£8,000–£26,000 per patient per year (depending on dosage).
- Cost savings: Fewer hospitalizations, ICU admissions, and OCS-related complications.
- NICE’s ICER threshold is £20,000–£30,000 per QALY.
B. NICE Decision on Cost-Effectiveness
- For severe allergic asthma: Approved, as the ICER was ~£28,000 per QALY, within the acceptable NHS threshold.
- For chronic urticaria: Initially not approved due to an ICER > £50,000 per QALY, but later funded under special circumstances.
3. Special NHS Funding Mechanisms
- Managed Access Agreements (MAA): Discounted pricing for eligible patients.
- Real-World Data Collection: Continued monitoring of benefits via the Severe Asthma Registry.
ABPA & CPA: Patient priorities
We have launched a new section that lists the commonest symptoms reported by our patient groups and offers tips on how to manage them.
In Their Words: CPA & ABPA
I Have ABPA and feel worse if I sleep with windows open
- Increased Allergen Exposure Outdoor Allergens: Opening windows can allow pollen, mould spores, and other allergens to enter, triggering respiratory symptoms. This is especially true during certain seasons (e.g., spring and fall).
Mould Growth: If mould levels are high outdoors, particularly in damp or humid conditions, this can worsen symptoms in sensitive individuals. - Temperature and Humidity Changes Cold Air: Cooler air at night can constrict airways, leading to increased asthma or allergy symptoms in some individuals.
Humidity Levels: Increased humidity can promote mold growth and worsen respiratory issues, particularly for those with ABPA. - Air Quality Pollution and Irritants: Urban areas may have higher levels of pollutants or other irritants at night, affecting respiratory health.
Odours: Nighttime activities (e.g., grilling, yard work) may introduce smoke or other irritants into the air. - Nighttime Symptoms Circadian Rhythms: Some people experience more pronounced respiratory symptoms at night due to natural variations in body functions and hormone levels.
Increased Sensitivity: Allergic individuals may be more sensitive to changes in their environment during the night when they are less distracted by daily activities. - Exposure to Pets or Dust Mites Indoor Allergens: Opening windows can stir up dust or expose individuals to pet dander and dust mites, exacerbating symptoms.Recommendations If opening windows leads to discomfort:
Keep Windows Closed: Especially during high pollen or mold seasons.
Use Air Purifiers: HEPA filters can help reduce allergens indoors.
Monitor Air Quality: Check local air quality indexes, particularly for mold and pollen counts eg. IQAir- Install an APP on your phone that tracks where you are and tells you what the local levels of pollution are.
Consult a Healthcare Provider: Discuss symptoms and management strategies, including potential adjustments to medication. If you’re experiencing significant discomfort, it may be helpful to maintain a controlled indoor environment to minimize exposure to allergens.In the UK, allergy season typically runs from March to November, with different types of pollen causing symptoms at different times.
Tree pollen
- The first wave of symptoms for some people, usually from late March to mid-May
- Hazel and birch trees are common culprits
Grass pollen
- The main cause of pollen in the UK from mid-May to July
- There are usually two peaks, one in early June and another in early July
Weed pollen
- It can start in June and last into autumn
- Dock and mugwort are common weeds that cause pollen
Other allergens
- Mould can be a problem in late summer/autumn until the first frosts
- House dust mites and pet allergens can cause year-round symptoms
Factors affecting pollen
- Weather conditions like temperature, wind, and rainfall can affect pollen counts
- Where you live can affect when and how severe symptoms are
- Urban areas tend to have lower pollen counts than rural areas
You can check the pollen forecast on the Met Office website.

