🌿 The Different Forms of ABPA
Understanding Your Diagnosis and What It Means
Allergic Bronchopulmonary Aspergillosis (ABPA) is a condition where your immune system overreacts to a fungus called Aspergillus fumigatus, which can be found in air, soil, and compost. This allergic reaction happens mostly in people with asthma or bronchiectasis.
But not everyone with ABPA has the same experience. Doctors now recognise that ABPA can appear in several different forms or stages, depending on how far it has progressed and what’s happening in your lungs.
Here’s a simple guide to help you understand where you might fit — and what it means for your care.
✅ 1. ABPA-S (Serologic ABPA) — The early stage
This is the mildest form of ABPA. It means your immune system is reacting to Aspergillus, but your lungs haven’t been damaged yet.
What’s usually found:
-
High levels of IgE (allergy antibodies)
-
Positive test for Aspergillus-specific IgE
-
Normal or near-normal scans (X-ray or CT)
-
Asthma or mild chest symptoms
🟢 This form is often picked up with blood tests before any permanent changes in the lungs happen.
🟠 2. ABPA-CB — ABPA with Central Bronchiectasis
This is a more typical form of ABPA, where the ongoing allergic reaction has started to damage your airways. “Bronchiectasis” means some airways have become widened and scarred.
What’s usually found:
-
All of the features above plus
-
Changes on a CT scan showing central bronchiectasis
-
More mucus, coughing, or breathlessness
🟠 This form may need regular treatment to reduce inflammation and protect the lungs.
🔴 3. Severe ABPA — ABPA with frequent flares
This isn’t a separate type, but a more active or harder-to-control version of ABPA.
What’s usually happening:
-
Frequent flare-ups (exacerbations)
-
Need for ongoing steroids or antifungals
-
Possible use of biologic medicines (e.g. Xolair/omalizumab)
-
More serious asthma symptoms
🔴 This form can still be well-managed, but needs close monitoring and a good treatment plan.
⚠️ 4. ABPA-CPF — ABPA with Lung Scarring (Fibrosis)
This is the late stage of ABPA, where ongoing inflammation over many years has caused permanent damage to the lungs. It’s now much rarer thanks to earlier diagnosis and treatment.
What’s usually found:
-
Extensive scarring or fibrosis on lung scans
-
Breathlessness or tiredness
-
May overlap with another condition called chronic pulmonary aspergillosis (CPA)
⚠️ This stage needs careful support, but many people can still manage symptoms and improve quality of life.
📈 How doctors track your ABPA
Some doctors will also use stages to describe how your ABPA is behaving, though this does not comply with the most recent guidelines (ISHAM 2024):
-
Stage 0 – No symptoms, but abnormal blood test
-
Stage 1 – Newly diagnosed (active symptoms)
-
Stage 2 – Responding to treatment
-
Stage 3 – In remission (no active disease)
-
Stage 4 – Flare-up
-
Stage 5 – Long-term lung damage (fibrosis)
🩺 Why this matters to you
Knowing what form of ABPA you have helps you and your healthcare team:
-
Choose the right treatments
-
Decide how often you need scans or blood tests
-
Spot early signs of flare-ups
-
Protect your lungs from long-term damage
💬 Final message:
No matter which form you have, there are treatments that work. Many people with ABPA live full lives with the right support.
If you're unsure what form of ABPA you have, ask your doctor — it can help you understand what to expect and how to take care of your lungs.
🧪 Understanding Blood Tests in ABPA-S
How Aspergillus-specific IgE and Eosinophil Counts Help with Diagnosis
If you’ve been told you might have Allergic Bronchopulmonary Aspergillosis – Serologic type (ABPA-S), you’ve probably had blood tests measuring your Aspergillus-specific IgE and your eosinophil count. These markers help doctors understand whether your immune system is reacting unusually to a common fungus called Aspergillus fumigatus.
This article explains what those tests mean — and why normal results don’t always rule out ABPA-S.
🌾 What is Aspergillus-specific IgE?
This blood test checks whether your immune system is producing allergy antibodies (IgE) against Aspergillus fumigatus. High levels suggest that your body is reacting to this fungus — a key sign in ABPA.
What do the results usually look like in ABPA-S?
-
Above 0.35 kUA/L – this is the minimum level needed for ABPA diagnosis
-
Above 1.5–6.5 kUA/L – this is very common in ABPA-S
-
Above 20 or even 50 kUA/L – these are often seen in more active or severe cases
🔍 Low or normal levels (below 0.35) are rare in ABPA-S unless:
-
You are already receiving treatment
-
You are in remission
-
There was a problem with the test
-
Your condition might be a different type of fungal allergy
So if your Aspergillus-specific IgE is high, that strongly supports the diagnosis. If it’s low, your doctor may retest or look at other factors.
🧬 What is an eosinophil count?
Eosinophils are a type of white blood cell linked to allergic inflammation. In many allergic conditions, including ABPA-S, these levels can go up.
What levels are typical in ABPA-S?
-
Above 500 cells/µL – commonly seen in untreated or active ABPA-S
-
Above 1,500 cells/µL – often seen in flare-ups
-
Below 500 cells/µL – can occur in people with milder disease or if they’ve started treatment
🟡 Normal eosinophils are not rare in ABPA-S
Many people with ABPA-S — especially those already on steroids or antifungals — may have eosinophil levels in the normal range. Up to a third of people with ABPA-S may show normal counts at some point.
🩺 What This Means for You
| Test | What’s Common in ABPA-S | Is It Rare in ABPA-S? |
|---|---|---|
| Aspergillus-specific IgE | High levels (often >1.5 or 6.5) | Low or normal levels are rare |
| Eosinophils | High counts often seen | Normal counts are not rare, especially during treatment |
So if your blood tests show:
-
High Aspergillus-specific IgE → that strongly supports ABPA-S
-
Normal eosinophils → this does not rule it out
💬 What patients often ask:
“Can I have ABPA-S with normal eosinophils?”
Yes. Especially if you’re already on steroids, or your symptoms are mild, your eosinophil count may appear normal.
“Does a low Aspergillus-specific IgE mean I don’t have ABPA?”
Not necessarily. Your doctor will consider your symptoms, scan results, and other blood tests too. Sometimes the test needs repeating.
🤝 Patient voices matter
If you’ve had these tests and been diagnosed with ABPA-S, sharing your experience can help others feel less alone — and more informed when navigating lab results.
Need help understanding your lab report?
Ask your care team:
-
What was my Aspergillus-specific IgE level?
-
What was my eosinophil count?
-
Are these results typical for someone with ABPA-S like mine?
Understanding your blood tests can help you take more confident steps in managing your condition.
🦠 From Baby Guts to Adult Lungs: Why Your Microbiome Matters More Than You Think
We often think of gut bacteria as something that helps with digestion—but new research is showing they do much more than that. In fact, the tiny microbes in your gut may be playing a major role in protecting your lungs, especially from infections and long-term inflammation.
A recent UK study found that newborn babies with a healthy balance of gut bacteria had half the risk of serious lung infections. But what does this mean for people living with chronic lung conditions like aspergillosis?
Let’s take a look.
👶 The Baby Biome Breakthrough
Researchers followed over 1,000 babies in the UK for the first two years of life. They found that those with high levels of Bifidobacterium—a helpful gut bacteria—were far less likely to be hospitalised with chest infections like bronchiolitis.
This protective effect was:
-
Most common in babies born vaginally
-
Linked to how the immune system developed early on
-
Thought to involve chemical signals from the gut to the lungs, helping the lungs prepare for infections
In short: a baby’s gut bacteria helped protect their lungs.
🫁 What Does This Have to Do With Chronic Aspergillosis?
If you have a chronic condition like Chronic Pulmonary Aspergillosis (CPA), Allergic Bronchopulmonary Aspergillosis (ABPA) or aspergillus bronchitis, this research might feel far removed—but it’s actually quite relevant.
Here’s why:
1. The gut and lungs are connected
Known as the gut-lung axis, this two-way communication means that what’s happening in your digestive system can affect how your lungs respond to inflammation, infection, and allergens.
2. Long-term medications can harm gut balance
People with aspergillosis often need antifungal medicines, steroids, or antibiotics—all of which can disturb the natural balance of gut bacteria. This may weaken the immune system’s ability to manage fungal growth or increase inflammation in the lungs.
3. A healthier gut may support immune stability
Although the research is still developing, supporting a healthy gut microbiome might help reduce flare-ups, inflammation, or secondary infections—especially if you’ve had lots of antibiotics or are steroid-dependent.
🌿 What Can You Do?
While we don’t yet have a proven probiotic "treatment" for aspergillosis, there are safe and practical steps you can take to support your microbiome and, potentially, your lung health:
-
Eat more plant fibre (e.g. oats, vegetables, legumes)
-
Limit ultra-processed foods
-
Consider fermented foods like kefir, sauerkraut or yoghurt—only if tolerated and not contraindicated (important in ABPA)
-
Ask your doctor if a probiotic supplement might help you—especially if you’ve had frequent antibiotics or digestive symptoms
-
Avoid unnecessary antibiotic use
⚠️ Always check with your healthcare team before starting new supplements, especially if you're on antifungals or immunosuppressants.
🧪 What’s Next?
Researchers are already testing whether giving newborns the right bacteria (like Bifidobacterium longum) in the first few weeks of life can prevent infections. Similar trials may follow in older children and adults with chronic lung conditions.
For now, the message is clear:
Looking after your gut health isn’t just about digestion—it could be an important part of protecting your lungs too.
🧠 Understanding Health Evidence: A Guide for Patients
This guide helps patients and the public understand how to judge the quality of health information, especially around treatments, supplements, and medical claims.
📚 Menu
- How Science Works
- Assessing the Strength of Evidence
- Trusting Online Medical Information
- Scientific Journal Quality and Bias
- Herbal Remedies and Industry Influence
- Unrecognised Syndromes and Clinics
- Predatory Journals and Peer Review
🔬 How Science Works
Medical advice and treatments are ideally based on well-tested science. Here’s how that process usually works:
- Research is done by scientists who ask questions and collect data.
- Peer review: Experts examine the study to ensure it’s fair and thorough.
- Publication: If it passes peer review, it's published.
- Replication: Other researchers try to repeat it. If they can't, confidence in the findings drops.
One study rarely proves something on its own. Medical certainty comes when multiple high-quality studies agree.
📊 Assessing the Strength of Evidence
🔎 Use these steps to check whether a claim is solid or uncertain:
- Is it based on one study or a pattern of studies?
- Has the result been replicated by others?
- Is it a randomised controlled trial, or a weaker type (like a case report)?
- Does it appear in a systematic review or meta-analysis?
- Was it published in a known, peer-reviewed journal?
Always check with a trusted clinician if unsure.
🌐 Trusting Online Medical Information
Look out for:
✅ NHS, NICE, university, or respected charity sources ✅ References to studies or expert guidelines ✅ Recently published or reviewed content ❌ Claims that sound too good to be true ❌ Articles trying to sell you something
Good places to check information:
🧾 Scientific Journal Quality and Bias
Even good journals may publish studies with industry funding. That’s not wrong by itself, but look out for signs of bias:
- Conflict of interest statements (often near the beginning or end)
- Funding sources: Drug companies vs. independent organisations
- How results are framed: Are benefits overstated? Risks ignored?
- Compare with other studies: Are the results too good to be true?
The strongest evidence comes from independent replication.
🌿 Herbal Remedies and Industry Influence
Some believe herbal treatments are suppressed by drug companies. In truth:
- Most herbal products haven’t had large, well-run trials.
- Companies don’t fund them because they can’t be patented.
- It’s not suppression — it’s a lack of commercial incentive.
Even if early research looks good, we need repeatable, well-controlled studies to ensure safety and effectiveness.
Doctors can’t recommend unproven treatments — not because they don’t work, but because we don’t yet know enough.
⚠️ Unrecognised Syndromes and Clinics
Some private clinics promote treatments for self-defined syndromes. They often:
- Rely on a few early or small studies
- Use unrecognised diagnostic tools
- Sell unproven or expensive treatments
Mainstream medicine needs strong, repeated evidence before accepting a new condition or treatment. It’s about safety and evidence, not disbelief or conspiracy.
⚖️ Is It Legal — and Ethical?
In many countries, including the UK, it is legal for clinics to offer non-mainstream treatments if they do not break safety, advertising, or professional conduct laws. However, legality does not always mean ethical acceptability.
Offering treatments that are unsupported by high-quality evidence may be seen by many as amoral or unethical, especially when:
- Patients are vulnerable or desperate
- Treatments are expensive
- Claims are overstated or misleading
- Alternatives with better evidence are not discussed
Healthcare professionals are expected to put patient welfare before profit, be transparent about evidence limitations, and avoid offering false hope. Patients should always ask questions, seek second opinions, and verify claims with trusted sources.
Some private clinics promote treatments for self-defined syndromes.
They often:
- Rely on a few early or small studies
- Use unrecognised diagnostic tools
- Sell unproven or expensive treatments
Mainstream medicine needs strong, repeated evidence before accepting a new condition or treatment. It’s about safety and evidence, not disbelief or conspiracy.
Other examples of self-defined or poorly validated syndromes promoted by certain clinics include:
- Adrenal fatigue (not the same as adrenal insufficiency)
- Leaky gut syndrome (distinct from recognised intestinal permeability disorders)
- Multiple chemical sensitivity (MCS)
- Chronic Lyme disease (as distinct from recognised post-treatment Lyme syndrome)
- Sick building syndrome (& similar relating to treating those in a damp home)
These conditions are often treated with:
- Specialised tests with unclear scientific validity
- Supplements, detox regimes, or off-label drug use
- Expensive personalised programmes with limited oversight
📉 Predatory Journals and Peer Review
Some journals publish low-quality or unreviewed research for money. Warning signs:
❌ Generic names, vague editorial boards, fast publication ✅ Indexed in PubMed, Web of Science, or Scopus ✅ Member of COPE or listed in DOAJ
Peer-reviewed journals differ in quality. Just because something is published doesn’t mean it’s reliable.
📜 Etymology: Where does “patient” come from?

The word "patient" has deep historical roots — and its origin gives insight into how medicine used to view people under care.
The word "patient" comes from the Latin:
patiens — meaning "one who suffers" or "one who endures"
It’s related to the verb patior, meaning “to suffer,” “to undergo,” or “to bear.”
So originally, a patient was someone who suffered or endured illness — someone passive, who received care or treatment, rather than someone actively doing something.
🧠 Why is this still used?
Historically, healthcare was something done to a person, often in the context of:
-
Religious or charitable care
-
Limited treatment options (patients mostly endured their illnesses)
-
The role of doctors as “healers,” and patients as the sick who “waited patiently”
Even as medicine advanced, the term persisted — and still reflects:
-
The person receiving care or treatment
-
A distinction from the “professional” (doctor, nurse, etc.)
🩺 Is this changing?
Yes — there's growing awareness that the term "patient" can imply passivity, while many prefer:
-
Person living with [condition]
-
Service user (used in mental health and social care)
-
Client (used in private healthcare)
-
Or just individual / person
That said, “patient” remains standard in medical, legal, and NHS documentation — but the language of healthcare is slowly evolving to be more person-centred.
⚠️ Summer 2025 Travel Warning: Fungal Lung Infections a Hidden Risk
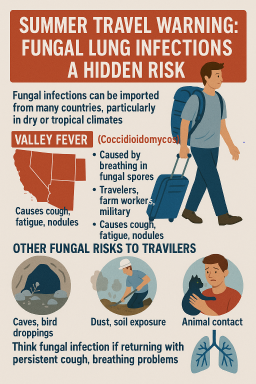
Important information for UK travellers, GPs and patients with chronic lung conditions
As more UK residents prepare to travel this summer — whether for holidays, charity work, military duty, or visiting family abroad — it’s important to raise awareness of a growing health risk that is often overlooked: fungal lung infections.
These conditions can be serious, persistent, and easily mistaken for other illnesses — including long COVID, TB, or bacterial pneumonia.
🌍 Fungal Infections Can Be Acquired Abroad — and Not Just in the Tropics
Fungal spores live in soil, compost, dust, and decaying organic matter. In many parts of the world, especially dry or tropical climates, travellers can unknowingly inhale spores that can cause long-term lung disease — often weeks or months after returning to the UK.
🧳 Key Risk Regions and Infections
🇺🇸 Valley Fever (Coccidioidomycosis)
-
Endemic to the southwestern United States — including Arizona, California, Nevada, Texas, and New Mexico
-
Caused by inhaling Coccidioides spores from dry, dusty soil
-
Affects travellers, farm workers, and military personnel
-
Can cause chronic cough, fatigue, joint pain, and lung nodules
❗ UK patients with unexplained lung symptoms should be asked about travel to these areas — Valley Fever can mimic CPA or even lung cancer.
🌎 Other Endemic Fungal Risks for Travellers
| Disease | Region(s) | Typical Exposure |
|---|---|---|
| Histoplasmosis | Central/South America, Africa, Asia | Caves, bird/bat droppings, demolition sites |
| Blastomycosis | Central USA (Great Lakes, Mississippi) | Soil, wood, riverside areas |
| Paracoccidioidomycosis | Brazil, Colombia | Rural farming dust |
| Talaromycosis | SE Asia, Southern China, India | Dusty environments (esp. in immunocompromised) |
| Sporotrichosis | Latin America, Africa, Japan | Plant thorns, soil, cat scratches |
| Cryptococcosis | Worldwide | Bird droppings, tree bark |
🌾 UK Risks Still Apply at Home
Even without travel, UK residents can develop Aspergillus-related conditions (CPA, ABPA) through:
-
Gardening (esp. with compost)
-
Farming or stables
-
Building or renovation work
-
Damp housing
Drug-resistant Aspergillus fumigatus is also rising in the UK — partly due to the use of agricultural fungicides.
🩺 Advice for GPs and Respiratory Teams
Ask:
-
Have you travelled to dry, dusty regions or tropical countries this year?
-
Have you been exposed to soil, caves, animals, compost, or renovation dust?
-
Do you have underlying lung disease (e.g. asthma, COPD, bronchiectasis)?
Consider:
-
Fungal testing (Aspergillus IgG/IgE, fungal cultures)
-
CT imaging for persistent nodules or cavitations
-
Early referral to respiratory or infectious disease specialists
-
Contacting the National Aspergillosis Centre for persistent or complex cases
✅ What Travellers Can Do
-
Wear a dust mask when gardening, hiking, or working around soil
-
Avoid enclosed spaces with bird or bat droppings
-
Seek help if you return from travel and develop:
-
A cough that won’t go away
-
Fatigue, fever, or weight loss
-
Chest tightness or unexplained breathlessness
-
📌 Final Reminder
Fungal infections are not rare — they’re under-recognised.
This summer, think fungal if you or your patient return from travel with persistent lung symptoms. Early diagnosis can make all the difference.
🫁 Why Is CPA Called a Long-Term Condition — Not a Lifelong One?

Chronic Pulmonary Aspergillosis (CPA) is often described as a long-term condition, but people sometimes wonder why it isn’t called a “lifelong” disease — especially since many people need antifungal treatment and regular monitoring for years.
Here’s what we know:
🩺 CPA Affects Everyone Differently
CPA is a complex condition that includes several forms — some people have a single fungal ball (aspergilloma), while others have more widespread or progressive disease. For many, CPA needs long-term treatment, such as antifungal tablets, oxygen, physiotherapy, or hospital care.
But not everyone has the same experience:
-
Some people are stable for years
-
Some respond well to treatment and no longer need antifungals
-
Others may live with occasional flare-ups or long-term health problems
🔁 Why It’s Not Always Called Lifelong
CPA is called a “long-term condition” because:
-
It typically lasts at least a year, often longer
-
It may come and go in phases
-
It needs regular follow-up and may affect daily life
But not everyone will have it for the rest of their life — and that’s why we don’t use the word “lifelong” for everyone.
🔬 We Don’t Yet Know Who is Truly ‘Cured’
To say whether CPA is curable, we would need to:
-
Follow a large group of patients
-
For many decades
-
To see who stays well and never relapses
That kind of long-term research is still ongoing — so at the moment, doctors can’t say for sure when or if someone is permanently cured.
Some people stay well for years after stopping treatment — but it’s too early to know if the infection is truly gone, or just sleeping.
💬 What This Means for You
-
CPA is a condition that can be managed — sometimes very successfully
-
You might not need treatment forever — but regular check-ups help catch any changes early
-
Your team will work with you to find the right balance of treatment and independence
-
If you feel well, that's a good sign — but it's still important to keep an eye on things
📍In short: CPA is a serious, long-term condition, but it’s not always lifelong. We still have more to learn, and long-term studies are helping us understand it better every year.
BBC Food Nutrition Calculator – Summary for Patients and Public

The BBC Food Nutrition Calculator is an easy-to-use, interactive tool designed to help you understand whether your diet is meeting your nutritional needs. By entering your age and sex, the calculator evaluates your intake of key nutrients and highlights any you might be under- or over-consuming. It also suggests foods rich in those nutrients to help you make healthy dietary adjustments.
Key Features
-
Personalised Assessment: Calculates your nutritional needs based on age and sex.
-
Food Recommendations: Suggests nutrient-rich foods if your intake is too low or too high.
-
Supplement Guidance: Explains when supplements might be useful—e.g. vitamin D in winter months or when housebound.
-
Immune System Support: Highlights nutrients that support immune health (vitamins A, C, D, B6, B9, B12, zinc, and iron).
Common Nutrient Gaps in the UK
According to UK dietary surveys, many people do not get enough of the following nutrients:
-
Fibre – under-consumed across all age groups
-
Vitamin D – commonly low year-round
-
Iron – especially low in girls and women aged 11–49
-
Calcium – often low in girls aged 11–18
-
Selenium – low among most females and older males
-
Zinc – insufficient in teenagers and adults over 75
Additionally, many people exceed recommended levels of free sugars, saturated fats, and salt.
Is the Information Verified?
Yes. The nutritional guidance in the BBC Food Nutrition Calculator is based on verified and reliable sources, including:
-
NHS and Public Health England recommendations
-
National Diet and Nutrition Survey (NDNS) data
-
Scientific consensus on daily nutrient requirements and health effects
While the BBC may not cite sources on every page, its content is regularly reviewed and reflects the current public health standards in the UK. You can trust this tool as a credible and evidence-based guide to dietary health.
Try the Calculator
You can access the BBC Nutrition Calculator here:
🔗 bbc.co.uk/food/articles/nutrition_calculator
💊 How Medicines Are Approved — and What “Off-Label” Means
🔹 1. What Is “Licensed” or “Approved” Medication Use?
Before a medicine can be prescribed in the UK (or any country), it goes through a formal approval process:
| Step | What Happens |
|---|---|
| Clinical trials | The medicine is tested for safety, effectiveness, and quality. |
| Regulatory review | In the UK, the Medicines and Healthcare products Regulatory Agency (MHRA) or the European Medicines Agency (EMA) reviews trial data. |
| Marketing authorisation | If approved, the medicine is “licensed” for specific conditions, doses, age groups, and methods of use. |
🟢 A licensed use means the drug has been judged safe and effective for that specific use, based on strong clinical evidence.
🔹 2. What Is “Off-Label” Use?
Off-label use means a doctor prescribes a medicine in a way that is not covered by its official license.
This could include:
-
Using a medicine for a different condition
-
Giving it at a different dose or frequency
-
Using a different route (e.g. inhaled instead of injected)
-
Giving it to a different age group (e.g. in children)
This is legal, but it means the prescriber is using their clinical judgement outside the official licensing terms.
🔹 3. Why Might a Doctor Use a Medicine Off-Label?
| Reason | Example |
|---|---|
| There is no licensed treatment for a rare condition | e.g. inhaled amphotericin B for CPA or ABPA |
| The licensed treatment doesn’t work or causes side effects | e.g. switching antifungal drugs |
| New evidence supports another use, but the company hasn’t applied for a new licence | e.g. old drugs used in new ways based on research |
| Medicines used in children or elderly often lack specific licensing data |
🔹 4. Is Off-Label Use Safe?
It can be, but it requires:
-
Good clinical judgement
-
Use of the best available evidence
-
Often, discussion with a multidisciplinary team
-
Informed consent from the patient (especially important in high-risk cases)
The prescriber takes more responsibility, because the use hasn’t been formally approved by regulators.
🔹 5. Who Oversees This in the UK?
-
The MHRA licenses medicines.
-
The General Medical Council (GMC) and NHS allow doctors to prescribe off-label when it’s in the patient’s best interest.
-
NICE guidelines sometimes include off-label use if evidence supports it.
🔹 6. Real-World Example: Inhaled Amphotericin
-
Licensed: Amphotericin B is approved for injection to treat fungal infections.
-
Off-label: Nebulised (inhaled) use is not officially licensed, but it is used in some centres to treat or prevent fungal lung disease (e.g. CPA, ABPA) where evidence and specialist experience supports it.
🔹 Summary: Key Points
| Term | Meaning |
|---|---|
| Licensed use | The use of a medicine that has been approved for a specific purpose by a regulator. |
| Off-label use | Prescribing a medicine in a different way than officially licensed — legal, but used with clinical caution. |
| Who decides? | Ultimately, the prescribing clinician, supported by evidence, guidance, and the needs of the individual patient. |
🌍 Fungal Spore Release in Different Climates
Climate has a major impact on fungal spore patterns. The types of fungi, timing of spore release, and health risks vary greatly between temperate, tropical, arid, and cold climates.
🌦️ Temperate Climates (e.g. UK, Northern Europe, Pacific Northwest USA)
-
Seasonal peaks: late summer to early autumn
-
Cladosporium, Alternaria, Aspergillus, Penicillium dominate
-
Triggers: humidity, rain, decaying vegetation, compost
-
Evening/night peaks for many spore types
🧠 Health risk: ABPA, asthma, SAFS, especially after garden work or composting
🌴 Tropical and Subtropical Climates (e.g. SE Asia, Central America, parts of Africa)
-
High year-round spore loads
-
Fungi: Aspergillus, Rhizopus, Mucor, Curvularia, Basidiomycetes, tropical molds
-
Daily rain cycles promote spore germination and release
-
Basidiospores and hyaline molds surge during evening and after rainfall
🧠 Higher incidence of fungal sinusitis, allergic fungal rhinosinusitis, and invasive infections in immunocompromised patients
🏜️ Arid and Semi-Arid Climates (e.g. Southwest USA, parts of the Middle East, Northern Africa)
-
Lower general spore burden, but dust storms can release huge amounts
-
Fungi: Coccidioides spp. (Valley fever), Aspergillus, dryland molds
-
Dry conditions favour small, dry spores that aerosolise easily
-
Wind and soil disturbance (construction, farming) are major triggers
🧠 Coccidioidomycosis, aspergillosis, dust-related asthma
❄️ Cold or Alpine Climates (e.g. Scandinavia, Alps, Canadian north)
-
Lower fungal biodiversity
-
Short seasonal spore peaks (spring–summer)
-
Indoor exposure more relevant: Penicillium, Cladosporium, Aspergillus
-
Mold growth occurs in poorly ventilated buildings (e.g. after snow melts)
🧠 Winter indoor mould exposure can worsen asthma, ABPA, SAFS
📌 Key Takeaway:
Different climates = different fungal threats.
The more humid, warm, or plant-rich the environment, the more active and diverse the fungal spore release — but indoor mould exposure is relevant in every climate.

