What a Space-Resistant Fungus Can Teach Us About Aspergillosis
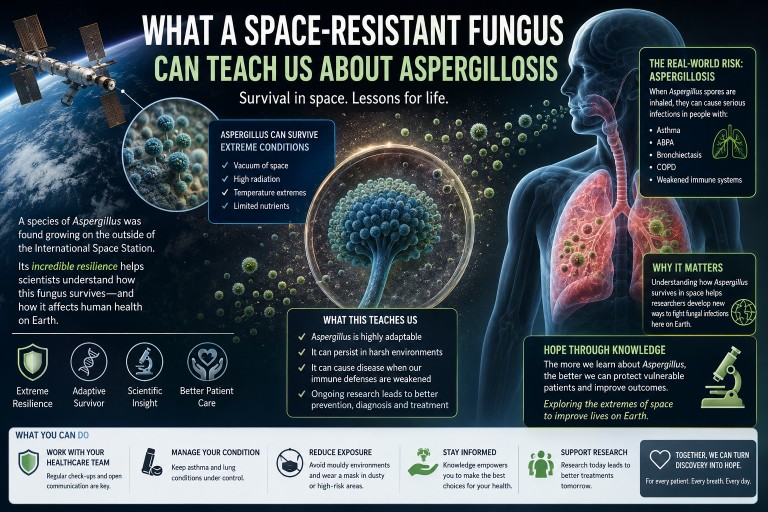
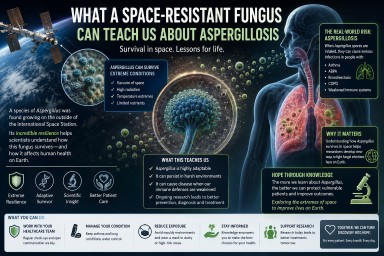
A recent Smithsonian article described how a microscopic fungus survived conditions designed to sterilise spacecraft. At first glance, this might sound like a story about space exploration rather than human health. But for people living with aspergillosis, it carries an important and surprisingly positive message.
Fungi are remarkable survivors
The article describes research showing that some Aspergillus spores can survive extreme conditions, including harsh radiation, dryness and cleaning procedures. This does not mean that aspergillosis patients need to worry about “space fungi”. Instead, it highlights something patients and specialists already understand very well: fungi are extraordinarily resilient organisms.
Aspergillus spores are common in the environment. They can be found in soil, compost, decaying leaves, dust, damp buildings and sometimes even very clean environments. Most people breathe in small numbers of spores every day without becoming ill, because their lungs and immune system clear them effectively.
For people with lung disease, asthma, immune system problems or damaged lung tissue, however, Aspergillus can sometimes cause illness. This includes conditions such as chronic pulmonary aspergillosis, allergic bronchopulmonary aspergillosis and severe asthma with fungal sensitisation.
A positive message for patients
One positive message from this research is that aspergillosis is not caused by weakness, poor hygiene or personal failure. Fungi are genuinely formidable organisms. If some fungal spores can survive environments as extreme as those used in space research, it becomes easier to understand why completely avoiding Aspergillus in everyday life is difficult.
This can be reassuring for patients who feel frustrated when symptoms persist despite doing “everything right”. It is not that they are failing. It is that fungal biology is complex, and fungal exposure is part of the natural world.
Why this matters emotionally
Many people with aspergillosis say they feel misunderstood. They may hear comments such as:
- “It’s only mould.”
- “Surely it should have cleared by now.”
- “Why are you still worrying about it?”
Stories like this help show that fungi are not simple or trivial. They are ancient, adaptable and scientifically fascinating organisms. Aspergillosis is therefore not “just mould exposure”; it is a real medical condition involving a complex interaction between the fungus, the lungs and the immune system.
Science is taking fungi more seriously
Another encouraging message is that fungi are attracting more scientific attention. Researchers are studying fungal survival, environmental spread, resistance to treatment, and the ways fungi interact with humans and indoor environments.
This matters because better understanding can lead to better diagnosis, better treatment and better prevention. In recent years, fungal medicine has already benefited from improvements in CT scanning, fungal blood tests, respiratory samples, antifungal treatments and biologic medicines for some allergic forms of disease.
Resilience goes both ways
The story also offers a useful reflection: fungi are resilient, but so are patients.
Many people living with aspergillosis adapt to long-term symptoms, hospital appointments, uncertainty, fatigue and treatment decisions. They continue to work, care for families, attend support groups, learn about their condition and help others understand fungal disease.
That resilience deserves recognition.
What patients can take from this
- Aspergillus is difficult to avoid completely, so exposure reduction should be realistic rather than perfectionist.
- Persistent symptoms are not a personal failure; fungal diseases can be complex and long-lasting.
- Fungal science is advancing, and aspergillosis is increasingly recognised as an important medical condition.
- Patients’ experiences are valid, even when others do not fully understand them.
When to seek medical advice
People with aspergillosis or suspected aspergillosis should seek medical advice if they develop worsening breathlessness, coughing up blood, unexplained weight loss, persistent fever, chest pain, a major change in sputum, or a significant deterioration in day-to-day symptoms.
Anyone already under specialist care should follow their agreed care plan and contact their clinical team if symptoms change significantly.
Further reading
- Smithsonian Magazine: fungus surviving spacecraft sterilisation conditions
- Aspergillosis.org: patient information and support
Last reviewed: May 2026
What if you can’t tolerate azole antifungal medicines?
Key points
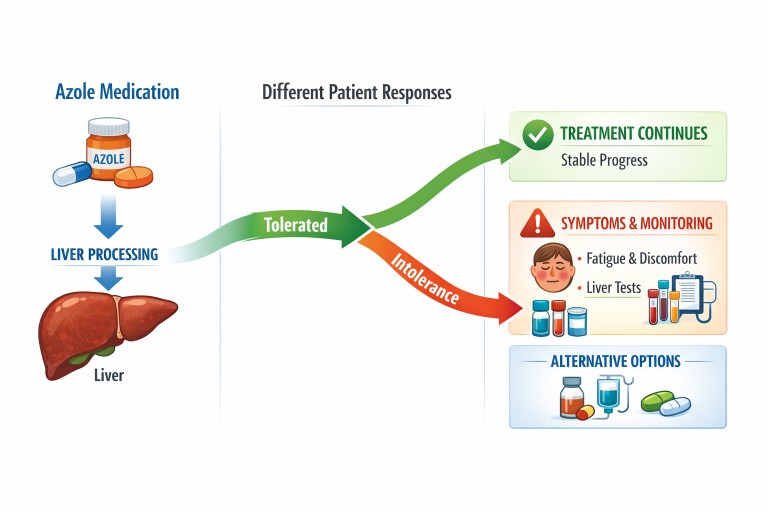
- Azole antifungals are commonly used to treat aspergillosis, but not everyone tolerates them well.
- “Azole intolerance” means the body reacts badly to the medication, even if it is otherwise effective.
- Symptoms can include fatigue, flushing, shaking, nausea, and discomfort around the liver area.
- In some cases, blood tests show changes in liver function.
- If azoles are not tolerated, there are often alternative approaches your clinical team can consider.
Contents
- What are azole antifungals?
- What is azole intolerance?
- Why does azole intolerance happen?
- Common symptoms to look out for
- The role of the liver
- What can be done if azoles are not tolerated?
- Why monitoring is important
- Common questions
- When to seek medical advice
What are azole antifungals?
Azole antifungals are a group of medicines used to treat fungal infections such as aspergillosis. They work by interfering with the fungal cell membrane, helping to stop the fungus growing.
Common examples include:
- Fluconazole
- Itraconazole
- Voriconazole
- Posaconazole
They are often used long-term in conditions like chronic pulmonary aspergillosis (CPA) or allergic bronchopulmonary aspergillosis (ABPA).
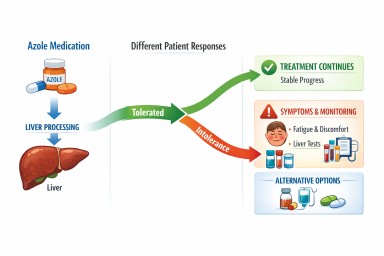
What is azole intolerance?
Azole intolerance means that a person develops unpleasant or harmful side effects when taking these medications, even at standard doses.
This is different from:
- Allergy – an immune reaction (e.g. rash, swelling, breathing difficulty)
- Resistance – when the fungus is not affected by the drug
With intolerance, the drug may still work against the fungus—but the body cannot tolerate its effects.
Why does azole intolerance happen?
There is no single cause. Instead, several factors can contribute:
1. How the body processes the drug
Azoles are broken down in the liver. People vary in how efficiently this happens, which can lead to higher levels of the drug in the body.
2. Effects on liver enzymes
Azoles affect enzymes (called cytochrome P450 enzymes) that are involved in processing many medications. This can:
- Increase drug levels
- Cause interactions with other medications
- Put strain on the liver
3. Individual sensitivity
Some people are simply more sensitive to these drugs, even when blood levels are within the expected range.
4. Other health factors
- Existing liver conditions
- Age
- Other medications
- Nutritional status
Common symptoms to look out for
Patients describe a range of symptoms when azoles are not well tolerated, including:
- Flushed or hot cheeks
- Shaking or tremor
- Severe fatigue
- Nausea or reduced appetite
- Discomfort or pain in the upper abdomen, back, or sides (where the liver sits)
- General feeling of being unwell
These symptoms can appear soon after starting treatment or develop over time.
The role of the liver
The liver plays a central role in processing azole antifungals.
In some cases, this can lead to:
- Raised liver enzymes on blood tests
- Inflammation or irritation of the liver
It is important to note that:
- Some people have abnormal blood tests without symptoms
- Others feel unwell even when tests are only mildly changed
This is why both symptoms and blood tests are considered together.
What can be done if azoles are not tolerated?
If azole intolerance is suspected, your clinical team may consider several approaches:
Adjusting treatment
- Reducing the dose
- Changing how the medication is taken (e.g. with food)
Switching to another azole
Some people tolerate one azole better than another.
Therapeutic drug monitoring (TDM)
Blood tests can measure drug levels to help ensure they are not too high or too low.
Considering non-azole treatments
In some cases, different classes of antifungal medication may be considered.
The best approach depends on the individual, the condition being treated, and how severe the side effects are.
Why monitoring is important
Because azoles affect the liver and interact with other medications, monitoring is a routine part of care.
This may include:
- Regular liver function blood tests
- Drug level monitoring (for some azoles)
- Review of other medications
Monitoring helps detect problems early and allows treatment to be adjusted safely.
Common questions
Does intolerance mean I cannot take any antifungal treatment?
No. Many patients who cannot tolerate one medication can use another, or a different approach may be possible.
Will the symptoms settle if I continue?
In some cases mild symptoms improve, but persistent or worsening symptoms should always be reviewed.
Is this common?
Most people tolerate azoles reasonably well, but intolerance is recognised and not rare in specialist clinics.
When to seek medical advice
You should contact your healthcare team if you experience:
- Persistent or worsening fatigue
- Pain in the upper abdomen, back, or sides
- Nausea affecting eating or drinking
- New or unusual symptoms after starting medication
Seek urgent medical attention if you notice:
- Yellowing of the skin or eyes (jaundice)
- Dark urine or pale stools
- Severe abdominal pain
Summary
Azole antifungals are an important part of treating aspergillosis, but some people experience intolerance.
This is usually related to how the body processes the medication—particularly in the liver—and varies from person to person.
If intolerance occurs, it does not mean that treatment options have run out. With careful monitoring and specialist input, alternative strategies can often be found.
Further reading
- Chronic pulmonary aspergillosis (CPA)
- Allergic bronchopulmonary aspergillosis (ABPA)
- Information for healthcare professionals
Author & review
This article has been prepared for patients and carers using information aligned with UK specialist practice, including the National Aspergillosis Centre (Manchester, UK).
Important: This content is for general educational purposes only and is not a substitute for medical advice. Always speak to your healthcare team about your own situation.
Lung Bleeding (Haemoptysis) in Aspergillosis: What It Means and What to Expect
 Last reviewed: March 2026
Last reviewed: March 2026Audience: Patients, carers, and non-specialist healthcare professionals
Applies to: Chronic Pulmonary Aspergillosis (CPA), bronchiectasis, and related lung conditions
Key Points
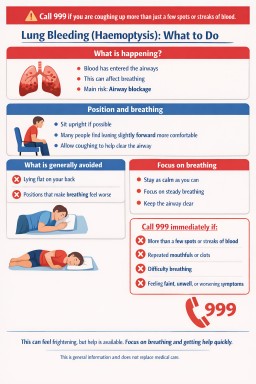
- Coughing up more than a few spots or streaks of blood is a medical emergency
- If bleeding is heavier or affects breathing, call 999 immediately
- The main immediate risk is airway blockage, not just blood loss
- Emergency care focuses on keeping airways clear and protecting breathing
- Some general positioning approaches are commonly used in healthcare settings
- This page provides general information only and is not a substitute for medical care
Table of Contents
- What is haemoptysis?
- Why can it happen in aspergillosis?
- Why does it feel so frightening?
- When is it an emergency?
- What happens during emergency care?
- While waiting for help (general guidance)
- Why positioning matters
- Understanding airway safety
- What is generally avoided
- What happens after hospital care?
- Medications such as tranexamic acid
- Common questions
- When to seek medical help
What is haemoptysis?
Haemoptysis means coughing up blood from the lungs or airways. This can range from small streaks in sputum to larger bleeds.
In people with Chronic Pulmonary Aspergillosis (CPA) and related lung conditions, haemoptysis can occur due to changes in lung structure and blood vessels.
Why can it happen in aspergillosis?
- Areas of lung damage (such as cavities) may develop
- Blood vessels in these areas can become fragile
- Inflammation may increase susceptibility to bleeding
Not all patients will experience haemoptysis, but awareness is important.
Why does it feel so frightening?
Many patients describe a strong sensation of being unable to breathe during a lung bleed.
This can occur because blood enters the airways, which may interfere with airflow. Even small amounts in the wrong place can feel overwhelming.
This reaction is common and understandable.
When is it an emergency?
NHS guidance advises calling 999 if you are coughing up more than just a few spots or streaks of blood.
Call 999 immediately if:
- You are coughing up more than just a few spots or streaks of blood
- You are coughing up repeated mouthfuls or clots
- You have difficulty breathing
- You feel faint, unwell, or symptoms are worsening
Small streaks or flecks of blood should still be checked by a healthcare professional, but larger or increasing amounts should be treated as an emergency.
What happens during emergency care?
Emergency responders and hospital teams focus on:
- Supporting breathing (for example, with oxygen)
- Monitoring vital signs
- Identifying the source of bleeding
- Protecting unaffected areas of the lung where possible
In some cases, procedures such as bronchial artery embolisation may be used to control bleeding.
While waiting for help (general guidance)
If you are waiting for emergency services to arrive, general first-aid principles often focus on maintaining comfort and supporting breathing.
- If possible, try to remain in a position that feels easiest for breathing
- Many patients find that being upright or slightly forward is more comfortable
- Try to keep the airway clear by allowing coughing if needed
The priority is to seek urgent medical help rather than attempting to manage the situation alone.
In an emergency, it may not be possible to adopt an “ideal” position—focus on calling for help.
Why positioning matters
In healthcare settings, positioning is sometimes used to help:
- Keep airways as clear as possible
- Reduce the spread of blood within the lungs
- Maintain breathing while further treatment is arranged
This is based on general principles of lung anatomy and airflow. The aim is not to stop bleeding, but to support breathing.
Many people find it easier to breathe when upright or leaning slightly forward. This may help fluid move out through the mouth rather than further back into the main airways.
Understanding airway safety
In situations where there is bleeding (or sometimes vomiting), the main concern is keeping the airway clear so that air can move in and out of the lungs.
Fluid in the airway can interfere with breathing, which is why emergency care focuses on maintaining airway clearance as well as treating the underlying cause.
Positions that allow fluid to move out of the mouth rather than back into the airway are generally preferred. Many people find being upright or slightly forward helps with this.
If someone becomes unable to remain upright, is very drowsy, or is vomiting, placing them on their side (recovery position) may help keep the airway clear while waiting for emergency services.
This information is general and does not replace emergency care. Always call 999 if symptoms are severe.
What is generally avoided
In clinical practice, certain positions are usually avoided because they may make breathing more difficult.
- Lying flat on the back
- Positions that feel like they worsen breathing
If you feel unsure, prioritise comfort and breathing while waiting for help.
What happens after hospital care?
After an episode of haemoptysis, your clinical team may:
- Investigate the cause of bleeding
- Review your current treatment
- Discuss whether any preventative measures are appropriate
If you have experienced haemoptysis, it may be helpful to ask your team whether you need an individualised plan.
Medications such as tranexamic acid
Some patients may be prescribed tranexamic acid to help reduce bleeding.
If you have been given this medication with clear instructions, it may be intended for use during bleeding episodes. It should only be taken exactly as directed by your clinical team.
Tranexamic acid does not replace the need to seek urgent medical help. If you are coughing up more than a few spots or streaks of blood, or feel unwell or breathless, call 999.
If you are unsure whether to take it during an episode, seek urgent medical advice.
Common Questions
Is coughing up blood always serious?
Any new or unexplained bleeding should be assessed. Larger amounts require urgent attention.
Can I manage this at home?
Significant haemoptysis should not be managed at home. Always seek urgent medical help.
Will it happen again?
This varies between individuals. Your specialist team can advise based on your condition.
When to seek medical help
Call 999 immediately if:
- You are coughing up more than just a few spots or streaks of blood
- You have difficulty breathing
- You feel faint, unwell, or symptoms are worsening
Seek medical advice urgently (NHS 111 or GP) if:
- You notice new or increasing blood in sputum
- You have recurrent or ongoing minor bleeding
Important safety note
This information is for general education only and does not replace medical advice. In an emergency, always seek immediate professional care.
References
- NHS. Coughing up blood (haemoptysis): https://www.nhs.uk/symptoms/coughing-up-blood/
- European Respiratory Society and interventional radiology guidance on haemoptysis
Author and review
Author: National Aspergillosis Centre (Patient Education Team)
Review: Specialist clinicians, Manchester University NHS Foundation Trust
Next review due: March 2027
Why Join an Online Support Group if You Have Aspergillosis?
You are not alone with aspergillosis
Join a friendly online support meeting — no pressure, just listen if you prefer.
Many patients find that even attending once helps them feel more reassured, informed, and supported.
Why Join an Online Support Group if You Have Aspergillosis?
Living with aspergillosis can feel isolating. Many people go for years without meeting another person with the same condition. Family and friends may be supportive, but they may not fully understand what it is like to live with breathlessness, fatigue, treatment side effects, uncertainty, or repeated hospital visits.
That is one reason online support groups can be so valuable. They bring people together who understand, often immediately, many of the challenges that aspergillosis can bring.
Key points
- Online support groups reduce isolation and help patients feel understood
- They offer shared experience alongside emotional support
- They improve confidence and understanding of the condition
- They help patients feel better prepared for appointments
- They are flexible — you can simply listen if you prefer
What changes when people join a support group?
Before joining
- Feeling alone with the condition
- Uncertainty about symptoms
- Limited practical advice
- Low confidence at appointments
- Worry about the future
After joining
- Connection with others who understand
- Better understanding of the condition
- Practical day-to-day coping ideas
- More confidence asking questions
- Feeling more supported and reassured
Why aspergillosis can feel so isolating
Aspergillosis is a relatively rare condition, and many patients never meet someone else with the same diagnosis. Online support groups help bridge that gap by creating a shared space for understanding and connection.
1. You realise you are not alone
Hearing others describe similar symptoms and challenges can be immediately reassuring and reduce feelings of isolation.
2. Shared experience can be deeply reassuring
Support groups provide practical, real-world insight into managing fatigue, pacing, work, and daily life.
3. You may understand your condition better
Listening to others and accessing shared resources helps build confidence and understanding.
4. It can help you feel more confident at appointments
Patients often feel better prepared and more able to ask the right questions.
5. Emotional support matters too
These groups provide encouragement, understanding, and a sense of belonging.
What happens in a typical online support session?
- Friendly welcome — no pressure to speak
- Open discussion — share or listen
- Optional topics — such as fatigue or treatment experiences
- Flexible participation — camera and microphone optional
- Safe, moderated space
Many people attend their first session just to listen — and that is completely fine.
What patients often say
“I wish I had joined sooner. Just hearing others talk made a huge difference.”
“I didn’t speak in my first meeting, but it really helped just listening.”
“It helped me understand my condition and feel more confident.”
Thinking of joining?
You can attend once, listen, and decide if it feels helpful. There is no obligation to continue.
View meeting times and book here:
https://aspergillosis.org/support-meetings/
Meetings are held online using Microsoft Teams. You will receive a joining link after booking.
Bottom line
Online support groups offer connection, reassurance, and understanding. They cannot replace medical care, but they can make living with aspergillosis feel more manageable and less lonely.
Please note: These groups are for support and shared experience. They do not replace advice from your own doctor or specialist team.
Understanding the Journey to Diagnosis (Start Here)
Last reviewed: 18 March 2026
Key points
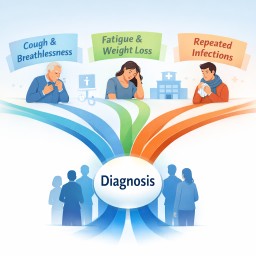
- Aspergillosis can be difficult to diagnose because symptoms often overlap with more common illnesses.
- Long diagnostic journeys are common in many chronic and uncommon conditions, not just aspergillosis.
- Uncertainty does not mean symptoms are unreal.
- Diagnosis often becomes clearer over time, as symptoms, scans, tests, and patterns build up.
- Good communication, ongoing review, and specialist input can make a major difference.
Why we created this series
People living with aspergillosis often tell us that the hardest part was not only the illness itself, but the time before they had an answer. Many describe repeated symptoms, multiple appointments, courses of treatment that only partly helped, and a growing sense that something still did not fit.
This experience is common in conditions such as chronic pulmonary aspergillosis (CPA) and allergic bronchopulmonary aspergillosis (ABPA), but it is also seen much more widely across medicine.
We created this series to help make sense of that process in a way that is:
- clear and accessible for patients and carers
- respectful of clinicians working within complex systems
- honest about uncertainty, delay, and emotional impact
- useful for improving understanding on both sides
The articles in this series
1. Why Aspergillosis Is So Hard to Diagnose
This article explains why aspergillosis can be difficult to recognise, why medicine usually starts with more common explanations, and how diagnosis often depends on patterns building up over time rather than one single test.
Best for: understanding the overall process and why delays can happen.
2. When Symptoms Are Real but Answers Are Not: Understanding Uncertainty
This article looks at the emotional and communication side of the diagnostic journey, including why patients may feel unheard, what clinicians may mean when they speak cautiously, and why unexplained symptoms are still real symptoms.
Best for: understanding uncertainty, communication gaps, and the experience of not yet having answers.
3. Why Diagnosis Can Take Time — and Why You Are Not Alone
This article places the diagnostic journey in a wider context, showing that long paths to diagnosis are common in many chronic and complex conditions, and offering reassurance that patients are not alone in this experience.
Best for: reassurance, perspective, and recognising that this journey is shared by many others.
Who may find this series helpful
This series may be useful if you are:
- a patient with ongoing respiratory symptoms and no clear diagnosis yet
- a carer or family member trying to understand what your loved one is going through
- a person recently diagnosed with aspergillosis and looking back on a long journey
- a general practitioner, respiratory clinician, nurse, or allied health professional wanting to better understand the patient perspective
It may also help people with other chronic conditions, because many of the same themes—uncertainty, overlap of symptoms, repeated reassessment, and eventual recognition—are seen across a wide range of illnesses.
When to seek medical advice
Seek medical advice if you have ongoing or worsening symptoms that are not improving as expected, especially if they keep returning or no longer fit the original explanation.
Seek urgent medical advice if you have symptoms such as:
- coughing up blood
- rapidly worsening breathlessness
- new chest pain
- significant unexplained weight loss
- high fever or signs of severe infection
If you already have an underlying lung condition and your usual treatment no longer seems to be working, it is reasonable to ask whether the diagnosis needs to be reviewed.
Related resources
Using AI Safely When You Have Aspergillosis
Artificial intelligence (AI) tools (for example, ChatGPT and other “medical chatbots”) can help people living with aspergillosis understand information, prepare for appointments, and feel more confident asking questions.
Used well, AI can be like a helpful explainer.
Used badly, it can be misleading — especially for conditions like aspergillosis where treatment decisions are complex.
This page explains what is safe, what is not safe, and how to use AI in a way that supports (not replaces) your clinical team.
Who is this page for?
This guidance is for people affected by:
-
Chronic Pulmonary Aspergillosis (CPA)
-
Allergic Bronchopulmonary Aspergillosis (ABPA)
-
Severe Asthma with Fungal Sensitisation (SAFS)
-
Aspergillus bronchitis
-
Other long-term Aspergillus-related lung problems
A simple rule that keeps you safe
AI should improve your understanding — it should not change your treatment.
If an AI tool suggests starting, stopping, or changing medication, do not act on it without speaking to your clinician.
What AI is good for
AI tools are usually helpful for:
Explaining medical words in plain language
Examples:
-
“What is Aspergillus Immunoglobulin G (IgG)?”
-
“What does ‘eosinophils’ mean?”
-
“What is a CT scan finding such as ‘cavity’ or ‘bronchiectasis’?”
Understanding medicines (general information)
AI can explain:
-
What a medicine is for
-
How it works in the body
-
Common side effects (in general terms)
-
Why monitoring is needed
This can be helpful for antifungal medicines such as itraconazole, voriconazole, posaconazole, and isavuconazole.
Preparing for appointments
AI can help you create a list of questions, for example:
-
“What monitoring do I need while on antifungals?”
-
“What symptoms should prompt urgent review?”
-
“How do we judge whether treatment is working?”
Summarising research articles
If you paste a paragraph from a paper (or describe it), AI can often translate it into patient-friendly language.
(Always remember: AI can sometimes get details wrong — see below.)
Organising your story
Many people find it useful to ask AI to format:
-
A timeline of symptoms
-
A list of medicines and dates
-
A short “what I want from this appointment” summary
This can make consultations more productive.
What AI is NOT safe for
AI should not be used for:
Diagnosis
Aspergillosis diagnosis usually depends on a careful combination of:
-
Symptoms and clinical history
-
Imaging (often computed tomography, CT)
-
Blood tests
-
Sputum tests / microbiology
-
Sometimes bronchoscopy results
AI cannot reliably “diagnose” from symptoms or a single test result.
Treatment decisions
Do not use AI to decide:
-
Whether you should start or stop antifungals
-
Steroid doses or tapering plans
-
Whether you “should” try biologics (for example, omalizumab)
-
Whether a side effect is safe to ignore
These decisions must be individualised and clinician-led.
Urgent situations
If you have worsening breathlessness, fever, chest pain, or coughing blood (haemoptysis), seek medical advice urgently.
AI is not an emergency service.
Why aspergillosis needs extra caution
Aspergillosis care can be complicated because:
-
Some antifungal medicines have important drug interactions
-
Blood levels may need monitoring (therapeutic drug monitoring)
-
Side effects can overlap with symptoms of lung disease
-
Different Aspergillus-related conditions can look similar but need different management
AI tools can also:
-
Over-generalise from asthma guidance
-
Confuse chronic disease with invasive disease
-
“Hallucinate” (invent) facts, references, or confident-sounding explanations
-
Be out of date
Privacy and confidentiality: what not to share with AI
To protect your privacy, avoid typing in:
-
Your full name
-
Date of birth
-
NHS number
-
Home address
-
Phone number
-
Identifiable clinic letters or reports (unless anonymised)
A safer way to write questions
Instead of pasting an entire letter, use a summary like:
“Adult with chronic lung disease, on itraconazole 200 mg daily, recent CT shows cavities, asking about monitoring and side effects.”
That’s usually enough for education and planning questions.
A safe “4-step” way to use AI
-
Ask AI to explain (terms, tests, general concepts)
-
Ask AI to help you prepare questions
-
Discuss those questions with your clinician
-
Only change treatment after clinical advice
A quick safety checklist
Before trusting an AI answer, ask:
-
Is this general education, or is it telling me what I should do?
-
Does it recommend changing my medicine or dose?
-
Does it mention checking interactions or monitoring?
-
Does it conflict with my current plan?
-
Is this situation urgent?
If any answer worries you: pause and ask your care team.
Example prompts patients can use safely
You can copy/paste these into an AI tool:
-
“Explain Chronic Pulmonary Aspergillosis (CPA) in plain language.”
-
“What questions should I ask about long-term itraconazole treatment?”
-
“What monitoring is commonly recommended for antifungal medicines?”
-
“Can you help me write a one-page symptom and medication summary for my clinic appointment?”
-
“Here is a paragraph from a research paper — can you summarise it in patient-friendly language and list any uncertainties?”
Tip: If you want a more cautious response, add:
“Please be conservative and tell me what you’re unsure about.”
Signs an AI answer may be unreliable
Be cautious if the AI:
-
Sounds very confident but gives no clear reasoning
-
Gives exact doses or taper schedules
-
Claims “this is definitely ABPA/CPA” from limited information
-
Provides references you cannot find elsewhere
-
Dismisses side effects, interactions, or monitoring
-
Encourages you to delay medical care
Final reminder
AI can be a helpful tool for understanding and preparing — but it is not a substitute for a specialist team.
If you are unsure, or something feels wrong, it is always reasonable to contact your clinician, specialist nurse, or GP.
Medical disclaimer
This page is for general information only and is not medical advice. Always follow the guidance of your healthcare team, especially regarding diagnosis, medicines, and urgent symptoms.
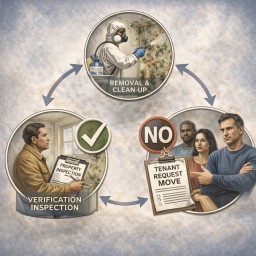
Remediation, verification, and refusal to move you
Home › Knowledge Hub › Damp, mould and aspergillosis › Remediation & refusal to move
If remediation is done but symptoms persist or worsen, the key question becomes: has the home been demonstrated to be safe to occupy?
What “good remediation” should include
- Cause fixed: leak/ingress/defect repaired, not just cleaned.
- Drying: adequate drying time and moisture checks.
- Material decisions: water-damaged porous materials removed where needed.
- Safe work: dust/spore spread controlled (important for medically vulnerable households).
- Verification: documented checks that work is complete and the home is safe.
Red flags (“bad remediation”)
- Paint over staining or “mould spray” only
- No drying plan, no moisture measurements
- No documentation of what was removed/replaced
- Work that creates dust without protection/containment
- Refusal to provide any meaningful post-remediation checks
If symptoms worsen after remediation
Worsening symptoms can occur if contaminated materials were disturbed or if damp persists behind walls/floors. This is a strong indicator that the hazard may not be resolved.
Actions:
- Document symptoms and healthcare visits (Page 3 template).
- Ask landlord for written evidence of safety and remediation details.
- Request escalation to Environmental Health if unresolved.
If the landlord refuses to move you (decant)
Use this framing:
- The issue is not “repairs completed” — it is safety and health risk.
- Ask: “What evidence shows the home is safe to occupy?”
Template request for temporary alternative accommodation
Subject: Request for temporary alternative accommodation (health risk / damp and mould) Hello [Name/Team], Despite remediation work, we are experiencing ongoing damp/mould concerns and worsening health symptoms in a clinically vulnerable household. Please provide written evidence that the home is safe to occupy, including: - confirmation the moisture source has been resolved, - evidence of drying/moisture checks, - what materials were removed/replaced, - what post-remediation checks were completed. Given the uncertainty around safety and the health impacts, we are requesting temporary alternative accommodation until the property can be demonstrated to be safe to occupy. Kind regards, [Name]
If you return “under protest”
If you have no alternative but to return, keep it in writing:
We are returning to the property due to lack of alternative accommodation. We do not accept that the damp/mould hazard has been resolved and will continue to document health impacts and seek independent assessment.
❤️ Thinking About Donating Blood After Aspergillosis or Lung Treatment?
A supportive message for people living with ABPA, CPA, SAFS, and related lung conditions
When you live with aspergillosis or a long-term lung condition, you know what it means to go through difficult treatments, long recoveries, and moments of uncertainty.
So when someone says, “Once I’m well, I’d like to donate blood to help others,” it is an incredibly generous and hopeful act.
Many people in our community wonder whether blood donation is possible after lung surgery, long-term inhalers, antifungals, or biologics. The reassuring answer is:
👉 Yes — some aspergillosis patients can donate blood once fully recovered, but it depends on individual treatments and health status.
And even if you can’t donate, the spirit behind the idea is powerful and meaningful.
🌱 1. Recovery comes first — your health is the priority
Whether you’ve had:
-
ABPA flare-ups
-
CPA treatment
-
bronchoscopy
-
long-term antifungals
-
biologics
-
a lobectomy or wedge resection
…the NHS will want you to be:
-
fully healed
-
breathing comfortably
-
stable in your lung condition
-
free from infection
-
strong enough to safely donate
For major surgery like a lobectomy, this often means several months of recovery before you can even be reviewed for donation.
This protects your health, not just the receiver’s.
💊 2. Medications commonly used for aspergillosis can affect eligibility
NHS Blood and Transplant will look closely at what you’re taking.
Here’s a simple guide:
Often NOT permitted
-
Biologics (e.g., mepolizumab, benralizumab, dupilumab)
-
Long-term immunosuppressants
-
Regular systemic steroids
May require a delay after stopping
-
Itraconazole / voriconazole / posaconazole
-
Recent antibiotic courses
-
Short steroid bursts
Usually fine
-
Inhalers
-
Nebulised saline
-
Montelukast
-
Airway clearance treatments
-
Most pain medicines
Every case is assessed individually — there is no automatic “yes” or “no” for all aspergillosis patients.
🫁 3. Your lung condition does not automatically exclude you
Having ABPA, CPA, bronchiectasis, or SAFS does not automatically prevent blood donation.
What matters is:
-
your condition is stable
-
your oxygen levels are good
-
you are not prone to sudden flare-ups
-
you feel well and strong
Many people with asthma or mild-to-moderate bronchiectasis still donate safely.
🩸 4. Your blood type is always valuable
Whether you’re a universal donor type (O-negative) or any other type, your blood can help save lives.
Even wanting to donate is something to be proud of — especially after everything you’ve been through.
🌟 5. The intention to donate speaks volumes about your strength
People living with aspergillosis know:
-
what it means to struggle for breath
-
how it feels to wait for test results
-
the exhaustion of flare-ups
-
the courage needed for surgery
-
the patience required for long-term treatment
So when someone in this community says:
“If I recover well, I want to donate blood to help someone else.”
…it’s a truly inspiring message of recovery and generosity.
🌈 6. Even if you can’t donate — your kindness still matters
Because of medications or long-term conditions, some people with aspergillosis will be told they can’t donate blood. This is completely normal.
You can still help others by:
-
encouraging friends or family to donate
-
sharing your story to raise awareness
-
supporting patient groups, campaigns, and research
-
simply being there for someone newly diagnosed
Your contribution to the world is not measured by a needle — it’s measured by your compassion.
❤️ Takeaway message
If you want to donate blood after aspergillosis treatment or lung surgery, that’s a beautiful intention. When you’re fully recovered, the NHS can review your health and medications. Whether you can donate or not, the willingness to help others already makes a real difference.
⭐ How to Avoid Being Fooled by Misleading Products, Private Tests and Health Claims
A practical, evidence-based guide for people living with aspergillosis, asthma, bronchiectasis and COPD
People with long-term lung conditions are often targeted by persuasive marketing, “health influencers”, alternative practitioners, and private test companies.
These services frequently exploit fear, frustration, and the very understandable desire for answers.
This expanded guide explains why certain products look scientific, why most are biologically impossible, and how you can protect yourself from being misled or spending money on things that cannot help your condition.
This is about empowerment — never about blaming patients.
🧩 1. Why misleading products look convincing
Companies deliberately use wording and imagery that trigger trust:
-
lab coats
-
microscopes
-
graphs and biological diagrams
-
words like “antifungal”, “immune”, “toxins”, “wellness”, “clinical strength”
These features make a product appear evidence-based — but appearance is not evidence.
Many claims contain a grain of truth, e.g.:
-
“Tea tree oil kills fungus in the lab”
-
“Silver has antimicrobial properties”
-
“This herbal extract reduces inflammation in laboratory tests”
But the missing information is the critical part:
⭐ The lab conditions have nothing to do with the human body.
To “kill fungus in a dish”, companies use concentrations that:
-
would be toxic in humans
-
cannot reach the lung tissue
-
would be broken down in the gut or bloodstream
-
do not survive into the airways
Companies rely on the fact that most customers don’t know this.
🧬 2. “Plausibility comes before testing” — the rule companies hope you don’t know
Scientists follow a simple chain:
1️⃣ Is it plausible?
Can the substance reach the lung?
Does the pathway make sense?
2️⃣ If yes — test it.
If not — don’t.
Products sold online almost always fail at Step 1.
Examples:
Turmeric supplements
Even at huge oral doses, only a tiny amount enters the bloodstream — nowhere near the lung in meaningful levels.
Oregano oil
Kills fungi on metal plates in labs — but the amount needed inside the lung would be toxic.
Silver products
Irritate the lungs and accumulate in tissues — highly implausible as therapy.
Essential oils
Break down long before reaching the airways in meaningful amounts.
Herbal antifungals
Often metabolised by the gut and liver — never reach airways at therapeutic levels.
This is why clinical trials don’t happen —
not because no one has tried,
but because there’s no scientific reason to bother.
🛍️ 3. How companies use “allowed” claims to sound medical
Because these products are not classed as medicines, they must not claim to “treat disease”.
So companies use vague, legally safe wording:
-
“Supports immunity”
-
“Maintains wellness”
-
“Promotes respiratory health”
-
“Contains antifungal botanicals”
-
“Helps with mould exposure”
-
“Advanced detox science”
All of these sound medical but say nothing measurable.
Example:
A supplement cannot say:
-
“Improves aspergillosis symptoms”
But it can say:
-
“Supports healthy immune response”
This tricks the viewer into mentally connecting the dots without the company making any illegal claims.
🧊 4. Air filters — the rare partial exception
Air purifiers can help some people, because they reduce:
-
dust
-
pollen
-
irritants
-
pet dander
-
airborne particulate matter
These changes may ease coughing or wheezing in sensitive people.
BUT…
most devices sold online are far too weak.
A purifier needs:
-
True HEPA H13 filter (not “HEPA-type”)
-
CADR 250–350+ for most rooms
-
Strong fan to turn over room air 4–5 times per hour
Without these, a purifier is just an expensive fan.
What they cannot do:
-
cure aspergillosis
-
remove Aspergillus from the lungs
-
prevent exposure
-
substitute for ventilation
-
fix damp or mould in walls
They improve comfort, not disease.
👩⚕️ 5. Why alternative practitioners are so persuasive
Alternative practitioners often:
-
speak with confidence
-
promise personalised care
-
provide long consultations
-
listen sympathetically
-
use scientific-sounding language
-
offer simple explanations for complex symptoms
Their tests and treatments look legitimate, but the problems include:
❌ No training in lung disease
❌ Misunderstanding of immunology
❌ Misuse of lab dish studies
❌ Incorrect interpretation of “toxins”
❌ Selling supplements with no evidence
❌ Recommending dangerous inhaled substances (e.g., oils, peroxide)
❌ Relying on anecdotes, not data
Even well-meaning practitioners can unintentionally cause:
-
lung irritation
-
drug interactions
-
adrenal effects
-
delays in proper NHS treatment
-
unnecessary fear
🧪 6. Private test companies — why their results look real but mean nothing
Common private tests include:
-
mycotoxin urine tests
-
“mould illness panels”
-
detox pathway testing
-
food IgG tests
-
fungal metabolite tests
-
heavy metal hair analysis
-
“immune balance” panels
-
testosterone finger-prick kits
These results are presented with:
-
charts
-
colour-coded ranges
-
expert-sounding commentary
But the key issue is:
⭐ The reference ranges are invented by the company.
Often “high” simply means:
-
“higher than the average of people who bought this test”
Not:
-
higher than healthy people
-
higher than unwell people
-
linked to disease
GPs and consultants cannot act on these results because they are not medically interpretable.
👨⚕️ 7. Testosterone tests — a perfect illustration of misleading health screening
Companies advertise:
-
“Tired? Low mood? Low motivation?”
-
“Check your testosterone at home”
-
“Feel younger again”
They use US-style messaging that implies easy treatment.
But in the UK, testosterone treatment requires:
-
symptoms consistent with hypogonadism
-
two morning venous blood tests
-
validated hospital labs
-
endocrine specialist interpretation
-
ruling out multiple other causes
- testosterone levels fall slowly as part of ageing - it is normal
Finger-prick tests do not meet NHS criteria,
so patients end up:
-
anxious
-
misinformed
-
sold supplements
-
not eligible for NHS treatment
This perfectly mirrors the broader pattern of private testing.
🔍 8. The “curiosity gap”: why people buy tests that GPs won’t order
Patients understandably feel:
-
frustrated
-
curious
-
confused
-
not listened to
-
desperate for answers
When a GP says “That test won’t help,” it can feel like:
-
rejection
-
dismissal
-
obstruction
But the reality is:
⭐ GPs are following evidence-based pathways to protect you.
Most private tests:
-
do not answer a clinical question
-
have false positives
-
trigger unnecessary follow-up scans
-
cause anxiety
-
cannot be interpreted
-
do not influence treatment
Private companies exploit:
-
curiosity
-
frustration
-
the desire for answers
-
the emotional gap left by long waits or unexplained symptoms
But a meaningless test result is worse than no test at all.
🧾 9. Real-world examples: 15 common traps to avoid
1. Mould settle plates
All rooms grow mould on plates — totally meaningless for health.
2. IgG food sensitivity tests
Measure normal immune exposure, not allergies.
3. Finger-prick vitamin tests
Often inaccurate and label normal levels as “borderline”.
4. Lung detox drinks
Nothing you drink detoxes the lungs.
5. Hydrogen peroxide / silver nebulisers
Dangerous. Irritate lungs. Risk chemical burns and pneumonitis.
6. Essential oil diffusers marketed as “antifungal”
Irritate airways; no delivery to lung tissue.
7. Mycotoxin detox programmes
Based on non-diagnoses; push expensive supplements.
8. Immune-boosting products
No supplement boosts immunity in a useful way for aspergillosis.
9. “Black mould blood tests”
No such test exists; ranges are invented.
10. Ozone machines and air ionisers
Harmful to lungs; zero evidence.
11. Anti-mould paint additives
Mask damp; do not impact indoor fungal counts long term.
12. Red-light therapy devices
Cannot penetrate tissue; no lung benefit.
13. Detox foot patches
Turn brown from sweat; total scam.
14. Anti-mould laundry boosters
Irrelevant to aspergillus exposure.
15. Humidifiers sold for “lung support”
Raise humidity → increase mould risk.
🛡️ 10. The Anti-Fooling Checklist
Before you buy anything, ask:
✔ Has this been tested in people with aspergillosis?
✔ Can it physically reach the lungs?
✔ Does NHS medicine recognise or use it?
✔ Are the claims vague? (“supports immunity”)
✔ Are the reference ranges medically valid?
✔ Would my consultant recommend this?
✔ Is this a simple answer to a complex condition?
If any answer is no, it’s a red flag.
⭐ 11. Golden rule
If a treatment or test genuinely helped aspergillosis, your consultant would already be using it —
not influencers, Amazon sellers, or unregulated US labs.
🌟 12. Final message: It’s not foolishness — it’s human
You are not being “tricked” because you’re naïve.
These products are engineered to be emotionally irresistible.
People with chronic illness are targeted because they are thoughtful, curious, and trying hard to get better.
If you are ever unsure about a product or test:
-
ask NAC/CARES
-
ask your specialist
-
or bring it to your next appointment
You deserve real answers — not false hope.
Why Exposure to Young Children Can Increase Illness in Aspergillosis, ABPA, and Bronchiectasis — and How to Track Viral Outbreaks
Many patients with Allergic Bronchopulmonary Aspergillosis (ABPA), aspergillus-related asthma, or bronchiectasis notice that they become ill far more often when spending time around younger children. This applies whether you work with them, live with them, or spend time with grandchildren or family groups. Here’s why it happens, what other patients experience, and how to monitor viral outbreaks so you can protect yourself.
Why Young Children Increase Illness Risk
1. Young children spread far more respiratory infections
Children under 11:
-
Carry more colds, viruses, and respiratory bugs
-
Shed viruses for longer periods
-
Have high viral loads
-
Are still learning hygiene habits
-
Spend a lot of time in close physical contact with adults
Even small viral infections can cause major lung flares in ABPA and bronchiectasis.
2. Viral infections trigger flare-ups, exacerbations, and pneumonia
With:
-
Bronchiectasis → mucus doesn’t clear properly, so infections “stick”
-
ABPA → airways are inflamed, reactive, and mucus-filled
-
Asthma → viruses are the most common exacerbation trigger
A simple cold in a child can turn into:
-
Fever
-
Chest infection
-
Need for antibiotics
-
Pneumonia
-
Weeks of recovery
This pattern is extremely common.
3. Children spread viruses even when only mildly ill
Some viruses (RSV, adenovirus, flu) spread before symptoms, or for many days after a child appears well.
Adults with lung conditions may experience far more severe symptoms from these same infections.
4. Any indoor, close-contact time increases risk
This includes:
-
Teaching music or classroom work
-
Caring for grandchildren
-
Sitting in cars together
-
Birthday parties, playgroups, soft play
-
Family gatherings
-
Living in the same household
Even short exposures can be enough in winter months.
What Other Aspergillosis Patients Report
Across support groups and clinics:
-
Many patients stay well until grandchildren reach nursery/school age.
-
Switching from high school to primary/elementary teaching often leads to repeated infections.
-
People frequently report more pneumonias in winter when around young children.
This is very common and not your fault.
How to Reduce Risk (Realistically)
1. Improve ventilation
-
Open windows/doors during visits or lessons
-
Use a HEPA air purifier at home or work
-
Avoid long stays in small rooms
2. Control exposure without avoiding children
Shorter visits with good ventilation are safer than long indoor contact.
3. Keep up with airway clearance routines
Vital for preventing infections from settling.
4. Mask during periods of high virus circulation
Especially when RSV, flu, COVID, or “winter bugs” are rising.
5. Stay vaccinated
Flu, pneumococcal, COVID (if eligible), and pertussis if around infants.
6. Get medical review if you're repeatedly unwell
Your team may consider:
-
Prophylactic antibiotics
-
Nebulised saline
-
Optimising inhalers/biologics
-
Checking ABPA control
7. Use Occupational Health if exposure is workplace-related
Ask for:
-
Teaching older groups
-
Ventilation improvements
-
Reduced winter exposure
Where to Get Reliable Information on Viral Outbreaks
Tracking viral activity can help you plan safer weeks and reduce the chance of flare-ups.
1. UK Health Security Agency (UKHSA)
Weekly reports on:
-
Flu
-
COVID
-
RSV
-
Measles and other outbreaks
-
Regional activity levels
Best official national overview. Link
2. GOV.UK Infectious Disease Reports
Lists:
-
Confirmed outbreaks
-
Public health warnings
-
School/nursery clusters
-
Localised alerts
3. Local NHS Trust or ICB Websites
Many publish:
-
Weekly respiratory dashboards
-
Local flu/RSV alerts
-
Outbreak notices for schools and care settings
(Example: Greater Manchester ICB has regular respiratory activity updates.)
4. GP Surgeries & NHS App Alerts
GPs can push:
-
Local viral alerts
-
Flu surges
-
Measles/strep notifications
Often one of the earliest local signals.
5. School/Nursery Letters and Newsletters
Schools must notify families about:
-
Flu/strep outbreaks
-
High absence levels
-
Confirmed clusters
Very useful if you work with or spend time around children.
6. Zoe Health Study App
Crowd-sourced, real-time data on:
-
Colds
-
Flu-like illness
-
COVID
-
Regional spikes
Good for early warning.
7. Local Council Public Health
Check:
[Your council] + “Public Health”
They often post:
-
Local outbreak alerts
-
Enhanced infection-control notices
-
Community virus trends
8. NHS 111 Online Data
Shows real-time spikes in:
-
Cough
-
Fever
-
Chest infections
-
Sore throat or strep symptoms
A useful snapshot of local trends.
Key Message
Yes — any exposure to young children can raise infection risk when you have aspergillosis, ABPA, or bronchiectasis.
Tracking viral outbreaks helps you plan safer contact, adjust your activities, and reduce the chance of pneumonia or flare-ups.
Resources
Here are direct links to trusted resources you can use to monitor viral outbreaks and infection risk (especially helpful for those with ABPA, bronchiectasis, asthma, and other lung conditions):
-
UK Health Security Agency (UKHSA) “Influenza and Respiratory Viruses” dashboard — UK data on influenza, RSV, COVID-19, ICU/hospital admission rates.
https://ukhsa-dashboard.data.gov.uk/ -
UKHSA / GOV.UK “National flu and COVID-19 surveillance reports” — weekly/bi-weekly reports summarising community, primary care, hospital and mortality data.
https://www.gov.uk/government/statistics/national-flu-and-covid-19-surveillance-reports-2025-to-2026-season -
GOV.UK “Outbreaks under monitoring” — current outbreaks of various infectious diseases in the UK.
https://www.gov.uk/government/publications/outbreaks-under-monitoring-in-2025/outbreaks-under-monitoring-week-41-week-ending-12-october-2025 -
GOV.UK “Infectious diseases: detailed information” — data, guidance, and analysis for a wide range of infections (flu, RSV, scarlet-fever, etc.).
https://www.gov.uk/government/collections/infectious-diseases-detailed-information -
Public Health Wales “Weekly influenza and acute respiratory infection report” — regional data including GP consultations and infection trends.
https://www.phw.nhs.wales/topics/immunisation-and-vaccines/fluvaccine/weekly-influenza-and-acute-respiratory-infection-report/ -
GOV.UK “Prepare – infectious disease outbreaks” — advice for the public on how to stay prepared for outbreaks, with hygiene and vaccination guidance.
https://prepare.campaign.gov.uk/be-informed-about-hazards/health-infectious-disease-outbreaks/