🌾 Dietary Fibre and Disease Prevention: Why We Need to Eat More Fibre
Fibre is no longer just about bowel regularity. Modern research shows that dietary fibre plays a fundamental role in overall health, immune regulation, and chronic disease prevention. Low-fibre diets are now being linked to a growing list of physical and mental health conditions, with multiple sclerosis (MS) among the most recent examples.
🔍 What Is Dietary Fibre?
Fibre is the indigestible part of plant-based foods that helps regulate digestion, supports beneficial gut bacteria, and contributes to metabolic and immune function. The two main types are:
- Soluble fibre: dissolves in water, forms a gel-like substance, and helps control blood sugar and cholesterol
- Insoluble fibre: adds bulk to stool and supports bowel regularity
🚨 How Much Fibre Do We Need?
- UK recommendation: 25–30g/day for adults
- Average intake: only around 18g/day
- This means most people are getting 25–40% less fibre than they need
🩺 Diseases Linked to Low Fibre Intake
A growing body of evidence links low-fibre diets to:
Digestive & Gastrointestinal Disorders
- Constipation
- Diverticular disease
- Haemorrhoids
- Irritable bowel syndrome (IBS)
Metabolic and Cardiovascular Diseases
- Type 2 diabetes (via insulin resistance and glucose spikes)
- Obesity (through reduced satiety and changes to the microbiome)
- High cholesterol
- Cardiovascular disease
Cancer
- Colorectal cancer risk is significantly reduced by high-fibre diets (especially cereal fibre)
Inflammatory & Autoimmune Conditions
- Multiple sclerosis (MS): recent research links gut microbial imbalance, worsened by low fibre, to inflammation and autoimmunity
- Inflammatory bowel disease (IBD): fibre can help regulate gut inflammation in some forms
- Rheumatoid arthritis and asthma: animal studies suggest protective roles
Brain and Mental Health
- Anxiety and depression: linked to gut-brain axis disruption when fibre is insufficient
- Neuroinflammation: fibre supports short-chain fatty acid production (e.g. butyrate), which helps reduce inflammation that affects brain and mood
🧬 Why Fibre Matters for the Gut Microbiome
Fibre is the main energy source for beneficial gut bacteria. These microbes ferment fibre into:
- Short-chain fatty acids (SCFAs) like butyrate, propionate, and acetate
- These SCFAs:
- Nourish the gut lining
- Modulate immune responses
- Reduce systemic inflammation
- Influence brain function via the gut–brain axis
Low fibre leads to:
- Less microbial diversity
- More pro-inflammatory bacteria
- Greater permeability of the gut wall ("leaky gut")
🥦 How to Increase Fibre Intake
🥣 Everyday Fibre-Rich Food Ideas
Here are some simple, everyday options to help boost your fibre intake, with estimated fibre content:
| Food Item | Approximate Fibre (g) per Serving |
|---|---|
| Muesli (40g serving with fruit & seeds) | 6–8g |
| Porridge oats (40g) | 4g |
| Wholemeal toast (2 slices) | 5–6g |
| Nut butter (1 tbsp) | 1–2g |
| Lentil or bean soup (1 bowl) | 7–10g |
| Chickpeas in salad (half cup) | 6g |
| Brown rice (1 cup cooked) | 3–4g |
| Quinoa (1 cup cooked) | 5g |
| Berries (1 cup) | 4–8g (depending on type) |
| Apple or pear (with skin) | 3–4g |
| Banana (medium) | 3g |
| Nuts or seeds (30g handful) | 2–4g |
| Air-popped popcorn (3 cups) | 3–4g |
🚫 Common Low-Fibre Foods
Many widely consumed foods contain very little or no dietary fibre, especially if they are highly processed or refined. Examples include:
| Food Item | Approximate Fibre (g) |
| White bread (2 slices) | 1g or less |
| White rice (1 cup cooked) | 0.5–1g |
| White pasta (1 cup cooked) | 1–2g |
| Processed breakfast cereals | 1–2g |
| Biscuits and cakes | <1g per portion |
| Ready meals (typical portion) | 1–2g |
| Crisps / potato chips (25g) | <1g |
| Soft drinks, fruit juice (250ml) | 0g |
| Cheese, meat, and eggs | 0g |
These low-fibre foods dominate many modern diets. Without mindful inclusion of whole plant foods, it is easy to fall well below the recommended fibre intake.
💡 Is It Easy to Reach the Target? These can be rotated across meals and snacks to easily reach your fibre goals without drastic changes.
⚖️ What If Fibre Causes Looser Bowels?
It's not uncommon for people to experience looser stools, more frequent bowel movements, or mild bloating when increasing fibre intake too quickly. This usually happens because:
- The gut bacteria are adjusting to more fermentable material
- Insoluble fibre speeds up gut transit time
The good news:
- These effects are usually temporary and settle within a few days to a couple of weeks
- You can achieve a happy medium by:
- Increasing fibre gradually over 1–2 weeks
- Including both soluble (e.g. oats, pulses, fruit) and insoluble (e.g. wholemeal bread, bran) fibre
- Drinking plenty of water
If symptoms continue, consult a GP or dietitian—especially if you have conditions like IBS or IBD that affect gut sensitivity.
✅ Summary
| Area of Health | Fibre Benefits |
| Gut & digestion | Regularity, reduced IBS/diverticulitis |
| Heart & metabolism | Lower cholesterol, improved glucose control, satiety |
| Immune system | Less inflammation, gut barrier protection |
| Mental health | Gut–brain axis modulation, reduced neuroinflammation |
| Cancer prevention | Lower colorectal cancer risk |
🌿 Special Note for People with Aspergillosis
If you are living with aspergillosis, especially chronic forms like CPA or ABPA, or regularly take medications such as antifungals, corticosteroids, or antibiotics, fibre is particularly important:
- Antibiotics can disrupt gut microbiota, reducing beneficial bacteria and fibre fermentation
- Steroids can impair immune regulation and blood sugar control, both of which benefit from high-fibre diets
- Antifungals and long-term illness may alter digestion or appetite, making a high-quality, fibre-rich diet even more essential
Maintaining a healthy gut environment through a fibre-rich diet may help support immunity, reduce inflammation, and improve resilience to infection and medication side effects.
📢 Final Note
Fibre is now a front-line defence against modern disease. It's one of the most underconsumed but powerful nutrients for preventing chronic illness, improving resilience, and nurturing a healthy gut microbiome.
Recent links to conditions like multiple sclerosis highlight just how far-reaching fibre’s impact may be—making it more than a digestive aid, but a foundation of systemic health.
💙 Disability Verification and Support for People with Aspergillosis in the UK
Living with aspergillosis—whether it's chronic pulmonary aspergillosis (CPA), allergic bronchopulmonary aspergillosis (ABPA), or another form—can have a significant impact on daily life. Many people find that fatigue, breathlessness, medication side effects, and other long-term symptoms affect their ability to work, care for themselves, or maintain independence.
If your condition is affecting your daily activities, you may be entitled to disability support, financial help, or adjustments at work or home. This guide explains how to get your disability recognised and verified in the UK, who can help, and how this varies across age groups and types of disability.
✅ What Counts as a Disability?
Under the Equality Act 2010, a person is classed as disabled if they have:
“A physical or mental impairment that has a substantial and long-term negative effect on their ability to carry out normal day-to-day activities.”
Many people with aspergillosis meet this definition—especially if they experience breathlessness, fatigue, pain, or recurrent infections over months or years.
📋 How Can You Prove or Verify Your Disability?
There is no single "disability certificate" in the UK. Instead, different systems accept different types of evidence, depending on what support you are applying for.
1. Benefit Award Letters
These are the most commonly accepted form of disability evidence:
- Personal Independence Payment (PIP)
- Disability Living Allowance (DLA) (for under 16s)
- Attendance Allowance (for over State Pension age)
- Employment and Support Allowance (ESA) (Support Group)
- Industrial Injuries Disablement Benefit
Where to get it: Contact the DWP or check your online account for a copy of your award letter.
2. NHS Medical Letters
Ask your GP or consultant to write a letter that:
- Confirms your diagnosis (e.g. CPA, ABPA)
- Describes the symptoms and how they affect your daily life
- Explains any treatments you need (e.g. antifungals, oxygen, steroids)
- States any long-term prognosis or care needs
3. Blue Badge and Disabled Bus Pass
- Blue Badge: Available from your local council for parking needs
- Disabled Bus Pass: Also issued locally; often requires proof of benefits or medical need
4. Occupational Therapy Assessment
- NHS or council-based OTs can assess your ability to manage daily tasks and recommend adaptations or support.
- Access via GP or Adult Social Care team.
5. Workplace or Education Support
- Occupational Health assessments may recommend reasonable adjustments such as flexible hours, remote work, or cleaner air environments.
- You may be eligible for Access to Work grants.
6. PIP and Other Benefit Assessments
- Assessments focus on how your condition affects daily tasks like mobility, personal care, medication management, and communication.
🔢 Do We Get a Disability Percentage?
In the UK, disability is not usually measured as a percentage. Most systems use functional assessments or point-based scoring.
The Exception: Industrial Injuries Disablement Benefit (IIDB)
- Uses a percentage system based on the extent of permanent disablement from a work-related condition.
For Everyone Else:
- PIP, DLA, and ESA use points-based systems.
- Employers, schools, and councils assess need based on impact, not percentage.
🡥 Who Can Help You with Disability Assessment?
| Professional / Service | Role & When to Use |
|---|---|
| GP or Specialist Consultant | Confirm diagnosis and functional impact for letters and forms |
| Occupational Therapist (NHS) | Assess your ability to manage daily tasks, recommend home aids/adaptations |
| Occupational Health (Work) | Recommend workplace adjustments under Equality Act |
| Adult Social Care (Council) | Assess for care support and home adaptation funding |
| Citizens Advice / Disability Charities | Help with forms, appeals, and understanding your rights |
| National Aspergillosis Centre (NAC) | May provide supporting letters for housing or benefits if you're under their care |
👶 Children and Young People
Under 16
- Claim Disability Living Allowance (DLA)
- Apply for an Education, Health and Care Plan (EHCP) if they have learning or developmental needs
- Get support from social care and school SENCOs
Age 16–25
- Transition to PIP for disability benefits
- EHCP can continue to age 25 if still in education
- Access workplace/education adjustments and Access to Work
- Shift from Children’s Services to Adult Social Care at 18
👵 Older Adults (Typically Age 65+)
Attendance Allowance
- For care needs only (not mobility)
- Not means-tested
Care and Support Needs
- Request a Care Act assessment from local council
- May result in home care, adaptations, or care home funding
NHS Continuing Healthcare
- For those with severe, complex needs
- Fully funded by NHS; not means-tested
Blue Badge Scheme
- Still accessible based on breathlessness or mobility limitation
Carer Support
- Carer's Assessment available
- Access to Carer’s Allowance or respite care
🧠 Mental Illness and Long-Term Invisible Disabilities
Mental health conditions and other non-visible disabilities (e.g. chronic fatigue, fibromyalgia, autism, long COVID) are also recognised under the Equality Act if they are long-term and impact daily life.
Differences in Assessment
- Focus is on non-physical activities:
- Planning and following journeys
- Managing therapy or medication
- Social interaction
- Decision-making
Key Evidence
- GP letters
- Psychiatrist or psychologist reports
- Occupational therapy or carer evidence
Support Services
- Community mental health teams (CMHT)
- Crisis teams, counselling, and talking therapies
- Supported housing or assisted living
Reasonable Adjustments
- Flexible schedules, quiet spaces, remote work
- Mental health support plans at school, university, or work
Advocacy
- Mind, Rethink, Disability Rights UK, and VoiceAbility provide advocacy, appeals help, and representation
📚 Summary Table
| Area | Physical Disabilities | Mental Health / Invisible Disability | Children | Older Adults |
| Benefit | PIP / ESA | PIP / ESA | DLA | Attendance Allowance |
| Social Care | Adult Social Care assessment | Adult Social Care or MH services | Children’s Services | Adult Social Care |
| Education/Work Support | Access to Work, OH reports | Access to Work, reasonable adjustments | EHCP, SENCO | Retirement/flexible options |
| Blue Badge | Based on mobility | Based on anxiety/severe distress for travel | May be available | Common for respiratory limits |
| Evidence Needed | Consultant, OT, GP | Psychiatrist, GP, carer, advocate | School or paediatric reports | GP, consultant, OT |
| Advocacy Support | Citizens Advice, Scope | Mind, Rethink, Disability Rights UK | IPSEA, Contact | Age UK, Carers UK |
🙏 Final Tips
- Keep copies of all letters, forms, and award notices.
- If your condition fluctuates, keep a symptom diary to show variable impact.
- Apply for assessments early as processes can take time.
- If you need help applying, speak to Citizens Advice or a local disability advocacy service.
- The National Aspergillosis Centre may be able to support patients with evidence for housing, benefit, or support applications.
🤔 Is It Aspergillus or Asthma Causing the Mucus?
It’s often a combination — here’s how they can overlap:
| Condition | What It Might Do |
|---|---|
| Aspergillosis (e.g. ABPA or Aspergillus bronchitis) | Causes thick, sticky mucus with fungal elements and inflammation. Often leads to coughing up plugs or brown mucus. |
| Asthma | Can increase mucus production, especially if poorly controlled or if triggered by allergens (including Aspergillus). |
| Both together | May cause ongoing mucus, irritation, and airway narrowing that makes it harder to clear, despite constant coughing. |
If you're seeing more mucus than usual, it could mean:
-
A flare-up of fungal activity
-
A reaction to something environmental (e.g. pollen, dust, damp)
-
Or simply a bad asthma spell with more inflammation
🧼 The ‘Bottle Brush’ Analogy
An image of wanting to "scrub" the airways is very real — many describe the feeling of:
-
Something stuck that won’t budge
-
Needing a deep clean they can’t reach with coughing
-
Wishing there were tools to physically clear the airways
✅ What You Can Try to Help Clear the Mucus
Here are real methods people find helpful (with advice from a respiratory physio):
-
Airway Clearance Devices (like a ‘brush’ for your lungs!):
-
Flutter or Acapella devices: use vibration and pressure to loosen mucus
-
Positive Expiratory Pressure (PEP) therapy: helps open and clear airways
(You can ask your team for one, or see if your hospital physio provides them.)
-
-
Breathing & Huff Coughing Techniques:
-
Controlled deep breaths, then a huff (a strong open-mouthed exhale like steaming up a mirror) instead of hacking coughs
-
This moves mucus from deep down to the top of the lungs where it’s easier to shift
-
-
Positioning/Gravity Drainage (Postural Drainage):
-
Certain positions help drain mucus from different lobes of the lungs — especially useful for bronchiectasis or ABPA.
-
-
Steam with Caution:
-
Mild steam inhalation (e.g. from a shower) can loosen secretions — just avoid essential oils or herbs if you’re sensitive.
-
-
Hydration and Mucolytics:
-
Staying hydrated helps thin the mucus.
-
Some are prescribed carbocisteine to reduce mucus stickiness.
-
-
Speak to your team if:
-
The mucus is changing in colour or amount
-
You feel more breathless
-
You’re unsure if it’s a fungal flare or asthma spike
-
They might check for infection, offer a sputum test, or tweak your medication.
🗣️ Patient Voices
“I felt like I had cobwebs or glue in my lungs. The flutter device gave me back a sense of control — I still have to work at it, but I don’t feel as helpless.”
“When I learned to huff cough and did it properly, I was amazed at how much came up. It's not a miracle, but it made me feel cleaner inside.”
💊 Staying Safe on Long-Term Treatment for Aspergillosis
(Steroids and Azole Antifungal Medicines)
If you're living with aspergillosis, your treatment plan may include long-term antifungals (e.g. itraconazole, voriconazole, posaconazole, or isavuconazole) and sometimes oral steroids like prednisolone. These medicines can be essential in managing your symptoms and preventing long-term lung damage.
But like all strong medicines, they need to be monitored closely—and you should be part of every treatment decision.
🗣️ You Should Be Involved in Every Medication Decision
NHS and NICE guidance recommend that:
-
Medicines should be reviewed regularly
-
Reviews should include the patient’s voice
-
Decisions to continue, stop, or adjust a medicine should be made together
🔗 NICE Medicines Optimisation Guidance:
https://www.nice.org.uk/guidance/ng5
⚠️ Why Regular Reviews Matter – Especially with Steroids and Azoles
Azole antifungals and steroids are powerful tools for treating aspergillosis, but they can cause side effects—especially if taken for long periods. Regular reviews help ensure you're getting the benefit of treatment without unnecessary risk.
🧪 Azole Antifungals Used in Aspergillosis
| Drug | Brand name(s) | Notes |
|---|---|---|
| Itraconazole | Sporanox | Common first-line; blood level monitoring needed |
| Voriconazole | Vfend | May affect vision, liver; used in severe cases |
| Posaconazole | Noxafil | Often well tolerated; used if others don’t suit |
| Isavuconazole | Cresemba | Newer; fewer interactions and side effects |
These antifungals can interact with many other medicines. The British National Formulary (BNF) lists over 300 interactions for itraconazole alone.
🧠 What About Prednisolone?
Prednisolone is a steroid that helps reduce inflammation but may cause side effects like:
-
Weight gain, diabetes, mood swings
-
Eye problems (e.g. cataracts)
-
Bone thinning (osteoporosis)
-
Adrenal insufficiency—where the body stops making enough natural steroid hormone
This is why lowest dose for the shortest time is best, and stopping should always be gradual and supervised.
🔁 What If You Can’t Stop These Medications?
In ABPA or chronic pulmonary aspergillosis, long-term antifungals or steroids may be the only effective treatment for now. That’s okay—what matters is staying safe and supported.
Here’s how your team should help:
-
✅ Use the lowest effective dose
-
✅ Monitor side effects and blood levels (especially for itraconazole and voriconazole)
-
✅ Watch for liver, nerve, adrenal, or eye problems
-
✅ Consider switching antifungals if side effects develop
-
✅ Look into steroid-sparing options (e.g. biologics like omalizumab or benralizumab for ABPA—though not yet widely approved)
👥 What If You’re Experiencing a Side Effect?
Here’s an example of a positive, patient-led conversation:
Patient:
"Since starting itraconazole, I’ve had tingling in my feet and some burning pain at night. I’m worried it’s the medicine."
Doctor:
"Thank you for bringing this up. That’s important. Let’s review your timing and symptoms. Itraconazole can sometimes cause nerve issues—let’s check your drug level and liver tests, and talk about adjusting the dose or switching antifungals."
Patient:
"Is it dangerous to stop suddenly?"
Doctor:
"No, not if done with supervision from your doctor—we’ll make any changes carefully and monitor you throughout. I’ll schedule follow-up, and please get in touch if anything worsens."
✅ You deserve to be listened to. Never ignore a side effect or worry that you’re being a nuisance—your body knows when something isn’t right.
🔎 Who Should You Talk To?
Here’s who to contact depending on the concern:
| Type of Concern | Best First Contact | Why |
|---|---|---|
| Side effects (e.g. nausea, mood, tingling) | GP or clinical pharmacist | Pharmacists are medication experts and often easier to access than specialists |
| Drug interactions | Pharmacist | They can check for dangerous combinations |
| Monitoring (e.g. blood tests, drug levels) | Specialist team | Usually manages antifungals and steroid tapering |
| Suspected allergy or adrenal issues | GP or endocrinologist referral | For detailed hormone testing or allergy support |
| General concerns or you're unsure who to ask | GP | They can coordinate referrals and advice |
🧩 What If You React Differently Than Expected?
Rare side effects do happen—including steroid allergy or intolerance, or nerve pain from azoles. You might feel dismissed, especially if the reaction is unusual or not in the textbook.
You are entitled to:
-
A proper medication review
-
A second opinion
-
Referral to pharmacy, allergy, or endocrine clinics
-
Kind, respectful care from professionals who take you seriously
True reactions are rare—but not imaginary. Speak up, document what you notice, and ask for help.
📚 Stay Informed with Reliable Sources
-
BNF (British National Formulary): https://bnf.nice.org.uk
-
NICE Guidance: https://www.nice.org.uk
-
Cochrane Reviews (independent evidence summaries):
https://www.cochrane.org/evidence/
🤝 Final Word
If you're on long-term treatment for aspergillosis, you're not failing—you're managing a difficult condition with strength and persistence. What matters is that you’re:
-
Heard
-
Supported
-
Included in every decision
You are the expert in how your body feels—and when your voice is part of the team, the care is always better.
Your Guide to Lung Function Tests: For Patients with Aspergillosis, Severe Asthma, Bronchiectasis, COPD, and Other Lung Conditions
💊 Why Lung Function Testing Matters
Lung function tests (also called pulmonary function tests or PFTs) are vital for understanding how your lungs are working and how your condition is progressing. If you have:
- Aspergillosis (e.g. ABPA, CPA)
- Severe or allergic asthma
- Bronchiectasis
- Chronic Obstructive Pulmonary Disease (COPD)
- or another long-term lung disease
you may be asked to perform one or more of these tests.
Each test looks at a different part of how your lungs function: how well air moves in and out, how oxygen transfers to your blood, how inflamed your airways are, and how your lungs respond to treatment.
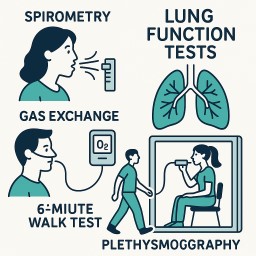
🌬️ Key Lung Function Tests Explained
1. Spirometry
What it does: Measures how much air you can breathe out and how fast you can do it.
Key numbers:
- FEV1: How much air you can blow out in one second
- FVC: Total amount of air you blow out
- FEV1/FVC ratio: Helps detect airflow obstruction
Useful for: Asthma, ABPA, COPD, CPA, bronchiectasis
2. Bronchodilator Reversibility Test
What it does: Compares spirometry before and after taking an inhaler to see if your airways improve.
What it means: A big improvement suggests asthma or ABPA.
3. FeNO (Fractional Exhaled Nitric Oxide)
What it does: Measures airway inflammation by detecting nitric oxide in your breath.
What it means: High levels = eosinophilic inflammation, common in ABPA, asthma.
4. Gas Transfer Test (DLCO/TLCO)
What it does: Measures how well gases like oxygen pass from your lungs into your bloodstream.
What it means: Reduced in CPA, fibrosis, and emphysema. May be normal in asthma or early ABPA.
5. Lung Volume Tests (Plethysmography)
What it does: Estimates total lung capacity and detects air trapping.
How it works: You sit in a sealed cabin and breathe through a tube while pressure and volume are measured (Boyle’s Law).
What it shows:
- High RV/TLC: Air trapping (asthma, CPA)
- Low TLC: Restriction (fibrosis)
6. Peak Flow Monitoring
What it does: Tracks daily variations in how fast you can blow air out.
Useful for: Monitoring asthma, ABPA over time at home.
7. 6-Minute Walk Test + Oxygen Monitoring
What it does: Checks how well you maintain oxygen during activity.
What it shows: Exercise capacity, oxygen needs in CPA, ABPA, fibrosis.
🤔 Are the Numbers Something to Worry About?
Not in isolation. These numbers are pieces of the puzzle, not the whole story.
Your doctor will consider:
- Your symptoms
- Scan results
- Blood markers (e.g. IgE, eosinophils)
- Trends over time
Even if a number seems low, it may not be a concern unless it’s worsening, linked with new symptoms, or part of a larger change.
The key is the pattern over time, and how well you’re functioning in daily life.
🚀 How These Tests Guide Your Treatment
These tests help your team:
- Decide whether your condition is asthma, ABPA, CPA, bronchiectasis, etc.
- Monitor response to inhalers, antifungals, biologics, or steroids
- Adjust or escalate treatment
- Plan oxygen support, pulmonary rehab, or surgery if needed
📊 Summary Table
| Test | What it Measures | Helpful in... |
|---|---|---|
| Spirometry | Airflow (FEV1, FVC) | Asthma, ABPA, CPA, COPD, bronchiectasis |
| Bronchodilator Test | Reversibility of obstruction | Asthma, ABPA |
| FeNO | Airway inflammation (eosinophils) | ABPA, allergic asthma |
| Gas Transfer (DLCO) | Oxygen movement from lungs to blood | CPA, fibrosis, emphysema |
| Lung Volumes | Air trapping, hyperinflation | CPA, asthma, bronchiectasis |
| Peak Flow | Daily airflow changes | Asthma, ABPA |
| 6-Min Walk + O2 | Oxygen levels during activity | CPA, ABPA, fibrosis |
✨ Final Word
Lung function tests can feel unfamiliar, but they are powerful tools for understanding your condition and improving your care. They help build a clearer picture — not of how "bad" your lungs are, but of how they are changing and what support you need.
Always ask your team to explain your results and what they mean for your treatment. You are the expert in how your body feels — and these tests help your team support you better.
Other forms of aspergillosis:🌿 Allergic Fungal Rhinosinusitis (AFRS), A Complete Patient Guide
👃 What Is AFRS?
Allergic Fungal Rhinosinusitis (AFRS) is a rare, non-invasive allergic condition affecting the sinuses. It occurs when a person develops a strong allergic reaction to fungal spores — most often Aspergillus or other environmental moulds.
This allergic reaction causes:
-
Chronic sinus inflammation
-
Nasal polyps
-
Thick, sticky mucus (called allergic mucin)
-
Blocked sinus drainage
-
In some cases, bone changes due to pressure from the build-up
Importantly, the fungus does not invade tissues, unlike more serious forms of aspergillosis.
🧬 AFRS and ABPA: Similar Diseases in Different Places
AFRS is very similar in nature to Allergic Bronchopulmonary Aspergillosis (ABPA), which affects the lungs.
| Feature | AFRS | ABPA |
|---|---|---|
| Location | Sinuses (nose, face) | Lungs (airways) |
| Cause | Allergy to fungi (e.g. Aspergillus, Bipolaris) | Allergy to Aspergillus fumigatus |
| Type of condition | Allergic (non-invasive) | Allergic (non-invasive) |
| Main symptoms | Nasal blockage, thick mucus, polyps, facial pressure | Cough, wheeze, mucus plugs, breathlessness |
| Seen in | People with chronic rhinosinusitis, nasal polyps, allergic rhinitis | People with asthma or cystic fibrosis |
| IgE levels | Often raised | Typically >1000 IU/mL |
| Inflammatory cells | Eosinophils in sinus mucin | Eosinophils in sputum and blood |
| Treatment | Sinus surgery, nasal steroids, biologics (sometimes) | Oral steroids, antifungals, biologics (sometimes) |
🧠 In short:
AFRS is to the sinuses what ABPA is to the lungs — both are allergic responses to inhaled fungal spores.
In fact, some patients may have both conditions if fungal sensitivity affects multiple airways.
📉 How Common Is AFRS?
AFRS is uncommon, but may be underdiagnosed. It occurs mostly in people with long-standing sinus problems or fungal allergies.
| Group | Estimated prevalence |
|---|---|
| General population | Less than 1 in 10,000 |
| People with chronic rhinosinusitis | 5–10% |
| Sinus surgery patients | 6–9% |
| Humid climates (India, Southern US) | Up to 25–30% of CRS cases |
In the UK, AFRS is less common than in tropical areas — but awareness is growing.
🛑 Why Is It Often Missed?
-
Looks just like chronic rhinosinusitis with nasal polyps (CRSwNP)
-
Most patients have symptoms like blocked nose, facial pressure, and mucus
-
Doctors may treat these as routine infections without testing for fungal allergy
-
Diagnosis requires ENT, allergy testing, imaging, and often surgery
🧬 Who’s at Risk?
People most at risk of AFRS typically:
-
Have asthma, nasal polyps, or severe allergic rhinitis
-
Experience long-term or recurring sinus infections
-
Have elevated IgE levels or known allergies to fungi
-
Live in damp or mould-prone environments
-
May have other fungal allergic conditions, including ABPA
🧪 How Is AFRS Diagnosed?
Diagnosis is based on the Bent and Kuhn criteria, which include:
-
Chronic rhinosinusitis with nasal polyps
-
Characteristic "allergic mucin" seen on CT or during surgery
-
Positive fungal test (PCR or culture)
-
Evidence of IgE-mediated allergy (skin test or blood test)
-
CT scan showing sinus opacification, expansion, or bone thinning
A diagnosis is usually made by an ENT specialist, sometimes with support from allergists and microbiologists.
💊 Treatment and Management in 2025
1. Endoscopic Sinus Surgery (ESS)
-
Clears out mucin and polyps
-
Restores drainage and reduces symptoms
-
Often the first step in diagnosis and treatment
2. Nasal Corticosteroids
-
Long-term sprays or rinses to keep inflammation down
3. Short Courses of Oral Steroids
-
Reduce inflammation after surgery or during flare-ups
4. Biologic Medications
-
For recurrent or severe cases:
-
Anti-IgE (omalizumab)
-
Anti-IL-5 (mepolizumab, benralizumab)
-
Anti-IL-4/IL-13 (dupilumab)
-
5. Antifungals?
-
Not usually needed
-
Oral antifungals have not consistently helped in trials
🔁 Will It Come Back?
AFRS can recur, especially if polyps return or inflammation flares up. Most patients need ongoing care from an ENT team and occasional follow-up imaging or treatment adjustments.
✅ Key Takeaways
-
AFRS is a rare, allergic form of sinus disease caused by hypersensitivity to fungi like Aspergillus.
-
It shares similarities with ABPA, which affects the lungs.
-
It is non-invasive, but can be severe and persistent without treatment.
-
Diagnosis requires a combination of ENT evaluation, allergy testing, and imaging.
-
Most people improve with surgery, nasal steroids, and in some cases, biologic therapy.
🫁 Mucus Plugging in Aspergillosis: What It Is, Why It Happens, and What It Means
For patients with ABPA, CPA, Aspergillus bronchitis, or asthma
🔍 What Is a Mucus Plug?
A mucus plug is a thick clump of sticky mucus that becomes trapped in your lungs. It can block airways, cause coughing, and make breathing more difficult. In people with aspergillosis, this is common — but the type, location, and cause of the mucus can vary.
🧪 What Causes Mucus Plugging?
Your lungs naturally make mucus to protect against germs and irritants. But in fungal or allergic lung disease, this mucus may:
-
Be produced in excess
-
Become too thick or sticky
-
Get trapped due to airway damage
Aspergillosis-related causes include:
-
ABPA (Allergic Bronchopulmonary Aspergillosis) – inflammation causes thick, sticky mucus
-
Aspergillus bronchitis – fungus lives in mucus, producing biofilms
-
CPA (Chronic Pulmonary Aspergillosis) – may lead to mucus due to structural damage
-
Bronchiectasis – airways are widened and can no longer clear mucus properly
🧬 Are All Mucus Plugs the Same?
No. Mucus plugs vary in colour, texture, cause, and treatment. Here's how they differ:
| Type of Plug | What You Might See | What It Could Mean | Common in... |
|---|---|---|---|
| Sticky, stringy | Clear/yellow, like glue | Allergic inflammation | ABPA, asthma |
| Rubbery or solid | Brown, rubbery, “slug-like” | Allergic + fungal mix | ABPA, Aspergillus bronchitis |
| Green or smelly | Thick, foul-smelling | Infection (bacteria) | Bronchiectasis |
| Foamy or frothy | Clear/white, bubbly | Non-infectious irritation | COPD, asthma |
| Black or speckled | May contain fungal specks | Fungal growth | CPA, fungal bronchitis |
🖼️ What Do Mucus Plugs Look Like on a CT Scan?
Below are real examples of CT scan findings showing mucus plugging in different forms of aspergillosis and related conditions.
🧷 1. Finger-in-glove sign (ABPA)
Mucus in large airways appears like fingers inside a glove. This is common in allergic fungal airway disease.
➡ Seen in: ABPA, bronchiectasis with fungal colonisation
📍 Note: Branching tubular opacities filled with mucus.
🌿 2. Tree-in-bud pattern
Small airway blockage — plugs in the tiniest branches of the lungs. Common in infection, inflammation, and Aspergillus bronchitis.
➡ Seen in: Aspergillus bronchitis, asthma, CPA with superinfection
📍 Note: Tiny dots and lines in a tree-like shape.
🧱 3. Lung collapse (atelectasis) from plug
A large mucus plug can block a main airway, causing collapse of part of the lung.
➡ Seen in: Severe ABPA, CPA, patients with weakened cough reflex
📍 Note: Whiteout of part of lung where plug is blocking airflow.
📸 Example CT Findings

1. Bronchiectasis + mucus plug
Area in the left lower lung shows dilated bronchi filled with mucus—classic for bronchiectasis with mucoid impaction

2. Extensive bronchiectasis with plugs
Widespread thick-walled airway dilatation accompanied by mucus plugs (black arrows) and consolidation (black arrowheads)

3. Luminal plugging in small airways
Subtle luminal opacities in peripheral bronchi—the “tree‑in‑bud” pattern common in asthma, COPD, and infections.

4. Atelectasis (part of the lung has collapsed or isn’t fully inflating) due to mucus plugging
Consolidation and small airway blockage leading to lung collapse, highlighted by arrows in the upper lobe.
💡 Clinical Takeaways
| Feature | What it indicates |
|---|---|
| Mucoid impaction | Large airway fungal/allergic plugs (e.g., ABPA) or bronchiectasis |
| Tree‑in‑bud | Small-airway infection/inflammation (e.g., TB, PCD, asthma) |
| Atelectasis | Complete blockage, leading to collapse and consolidation |
| Persistent luminal plugs | Associated with worse airflow obstruction and symptoms in COPD/asthma |
✅ Next Steps / Applications
-
These CT examples are valuable for educational use—they illustrate the different patterns seen in mucus plugging across disease types.
-
Radiologists often use these signs to help diagnose and tailor management (infection, allergy, structural lung disease).
-
If your patients or students need simplified visuals, these scans paired with annotations (e.g., arrows, labels) can make great teaching tools.
🧠 What Does It Feel Like?
People often say:
“It felt like something was stuck and wouldn’t come out.”
“I finally coughed up a rubbery strand — like glue.”
“Once it cleared, I could breathe better instantly.”
🧼 How Are Mucus Plugs Treated?
Treatment depends on the underlying cause:
✅ Medications
-
Steroids – reduce inflammation in ABPA and asthma
-
Antifungals – lower fungal load (e.g., itraconazole, posaconazole)
-
Mucolytics – thin mucus (e.g., carbocisteine, hypertonic saline)
-
Antibiotics – treat bacterial infections
✅ Airway Clearance Techniques
-
Respiratory physio – helps you learn how to shift mucus
-
Devices – flutter valve, PEP mask, Acapella
-
Inhaled/nebulised therapy – opens airways and loosens plugs
⚠️ Always speak to your clinical team before starting a new technique.
🧪 Can Coughing Up a Plug Help Diagnosis?
Yes! If you cough up a rubbery, large, or unusual plug, it can be:
-
Tested for fungus, bacteria, or allergy cells (eosinophils)
-
Sent for culture to detect Aspergillus
-
Helpful in guiding or confirming diagnosis of ABPA or Aspergillus bronchitis
👣 Key Points for Aspergillosis Patients
| Question | Answer |
|---|---|
| Is mucus plugging common? | Yes, especially in ABPA, CPA, and bronchiectasis |
| Are all mucus plugs the same? | No – they vary in size, shape, colour, and cause |
| What should I do if I cough one up? | Tell your doctor – it may be useful to test |
| Can it be seen on scans? | Yes – CT can show where plugs are and how severe |
| Can it be treated? | Yes – treatments include steroids, antifungals, mucolytics, and physio |
👁️ Other forms of Aspergillosis: Aspergillus Endophthalmitis, A Rare Eye Infection
🧐 What Is It?
Aspergillus endophthalmitis is a severe fungal infection that affects the inside of the eye — specifically the vitreous (gel) or retina — caused by Aspergillus. It can lead to:
-
Red, painful eye
-
Blurred or lost vision
-
Eye inflammation, sometimes with “filamentous” fungal growth on the lens if post-surgery
-
Both exogenous (from cataract surgery or injury) and endogenous (spread through the blood, often in immunocompromised patients) forms exist
📉 How Rare Is It?
| Condition | Cases per 100,000 | Commonality |
|---|---|---|
| ABPA | 40–60 | Moderately common |
| CPA | 3–4 | Uncommon |
| Aspergilloma | 0.5–1 | Rare |
| Empyema | <0.1 | Very rare |
| Endocarditis | <0.05 | Extremely rare |
| Endophthalmitis | Estimated < 0.05 | Extremely rare |
-
Aspergillus causes fewer than 1% of postoperative eye infections
-
Even among fungal cases, it’s a leading but still uncommon cause
🧬 Who Is at Risk?
-
Immunocompromised individuals (e.g., transplant, high-dose steroids, cancer infusion, diabetes, HIV)
-
Post-operative or post-trauma eye patients, especially cataract surgery
-
IV drug users, or people with systemic aspergillosis
Despite these risk factors, it remains an uncommon complication.
🩺 Symptoms
-
Eye pain and redness
-
Blurry or reduced vision
-
Sensation of “floaters” or shadows
-
Often unilateral, but can be bilateral, especially after surgery or in immunosuppressed patients
🧪 Diagnosis
-
Eye examination by an ophthalmologist with slit lamp or ultrasound
-
Sampling of vitreous or aqueous fluid for culture, PCR, or galactomannan tests
💊 Current Treatment Guidelines
Based on 2022–2025 evidence:
-
Prompt vitrectomy (surgical removal of infected gel) improves outcomes Intravitreal voriconazole injections (directly into the eye) enhance recovery
-
Systemic antifungals: voriconazole or isavuconazole are preferred; amphotericin B or combination therapy may be used if resistant
-
Prognosis: Vision ≥20/400 in <50% of cases; globe preserved in ~66% of eyes
🧭 Summary for Patients
-
Aspergillus endophthalmitis is extremely rare — it affects a tiny fraction of aspergillosis patients.
-
It’s often linked to eye surgeries, trauma, or severe immunosuppression.
-
Symptoms include pain, redness, floaters, and vision loss — if any appear, seek urgent ophthalmology care.
-
Best outcomes result from early vitrectomy, intravitreal antifungals, and systemic treatment.
✅ Bottom Line
While Aspergillus can affect many parts of the body, eye infections (endophthalmitis) are among the rarest forms. Most patients with respiratory forms (ABPA, CPA, or aspergilloma) will never develop this.
But awareness matters — especially for those who are immunocompromised or have had eye surgery. With swift, specialist treatment, many eyes can be saved, though vision recovery is often limited.
❤️🩹 Other forms of Aspergillosis: Aspergillus Endocarditis, Understanding a Rare Heart Infection
🫀 What Is It?
Aspergillus endocarditis is a rare infection of the heart’s inner lining (endocardium) caused by the fungus Aspergillus. This condition affects the heart valves (native or prosthetic), the inner wall of the heart, or even devices such as pacemaker leads. The fungus forms large masses called vegetations and can spread to the brain or other organs.
📉 How Rare Is It?
This is among the rarest forms of aspergillosis:
| Type of Aspergillosis | Estimated Cases per 100k | Commonality |
|---|---|---|
| ABPA | 40–60 | Moderately common |
| CPA | 3–4 | Uncommon |
| Aspergilloma | 0.5–1 | Rare |
| Aspergillus Empyema | <0.1 | Very rare |
| Aspergillus Endocarditis (AE) | <0.05 | Extremely rare |
⚠️ Who Is at Risk?
AE usually occurs in individuals who:
-
Are immunocompromised (e.g., cancer chemotherapy, transplant recipients, high-dose steroids)
-
Have heart valve abnormalities or a prosthetic valve
-
Had cardiac surgery or devices placed
-
Are critically ill or have severe fungus in the bloodstream
Even with these factors, AE remains extremely uncommon, but its rapid progression makes awareness and early treatment crucial.
🩺 How It’s Diagnosed
Diagnosis is challenging due to:
-
Negative blood cultures (blood tests usually don’t detect Aspergillus)
-
Symptoms often include fever, new heart murmur, or emboli (e.g., stroke)
-
Echocardiograms (TTE/TEE) may reveal large vegetations or abscesses
-
Valve or embolus tissue tested via PCR or galactomannan confirms diagnosis
⏳ Prognosis
-
AE has a very high mortality rate, ranging from 50–90%, often due to delayed diagnosis
-
Even with treatment, survival is around 50–60% with surgery and antifungals; without surgery, survival falls below 5–10%
💊 Current Treatment Guidelines
🛠️ 1. Early Surgical Intervention + Antifungal Therapy
-
Surgery to remove infected tissue and replace valves is essential
-
Voriconazole (an antifungal) is the preferred medication; liposomal amphotericin B is an alternative
-
Combined therapy (two antifungals) may improve outcomes in certain cases
🕰️ 2. Long-Term or Lifelong Antifungal Treatment
-
Lifelong antifungals may be needed to prevent recurrence, especially when prosthetic valves are involved
🧪 3. Monitoring and Follow-Up
-
Regular monitoring through clinical exams, echocardiograms, and possibly biomarkers
-
Watch for signs of relapse or emboli (e.g., neurological symptoms)
📘 Case Insights
-
A patient with a prosthetic aortic valve had ≥60% survival with surgery + voriconazole and long-term suppressive treatment
-
Another recovered from native valve involvement with combined antifungal therapy and surgery, despite being previously healthy
-
Without surgery and antifungals, AE is almost always fatal — mortality approaches 100%
✅ What This Means for Patients
-
AE is extremely rare, particularly compared to other forms like ABPA or CPA.
-
It occurs mostly in people with significant risk factors — immunosuppression, prior heart surgery, or invasive devices.
-
If suspected, early recognition and referral to a specialist center is urgent.
-
Treatment combines surgery and antifungals, and usually requires long-term care.
🧭 Bottom Line
Aspergillus endocarditis is a serious and rare complication. While most people with aspergillosis (like ABPA or CPA) will never develop it, anyone with heart valve issues and severe immune weakness should be vigilant.
With early, specialist treatment, recovery is possible — but only if the condition is identified and treated quickly.
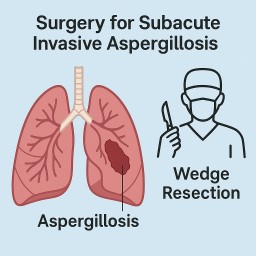
When Antifungals Fail: One Patient’s Recovery from Subacute Invasive Aspergillosis After Surgery
Subacute Invasive Aspergillosis (SAIA) is a rare and serious lung infection caused by the Aspergillus fungus. It often affects people who are immunocompromised—whether due to illness or medications like immunosuppressants—and typically sits between chronic and acute invasive forms in severity.
🧬 A Patient's Story from Australia
“I was diagnosed with SAIA after being treated with immunosuppressants for an autoimmune condition. Over seven months, I tried three different antifungal medications—but the infection persisted. I was still producing thick mucus and felt systemically unwell, almost like I had a constant infection running through me.
Four weeks ago, I underwent a wedge resection—a type of surgery where the affected part of my lung was removed. Since then, my symptoms have completely resolved. I’m no longer coughing or feeling septic.
My infectious diseases specialist plans to keep me on posaconazole for 12 months, with monthly galactomannan blood tests to catch any recurrence early.
I’ve found there’s very little published about surgery for SAIA, so I hope my experience might help others.”
🧪 What Is SAIA?
SAIA is a slowly progressive lung infection that develops over weeks to months. Unlike acute invasive aspergillosis, which moves quickly, SAIA often occurs in people with some degree of immune suppression but who aren’t completely immunocompromised.
It can present with:
-
Persistent cough
-
Low-grade fever
-
Fatigue
-
Mucus production
-
Progressive lung damage
Standard treatment involves long-term antifungal therapy, often with drugs like:
-
Itraconazole
-
Voriconazole
-
Posaconazole
But in some cases—like this patient’s—antifungal therapy alone isn’t enough.
🛠️ When Is Surgery Used for SAIA?
Surgery, including wedge resection, may be considered when:
-
Antifungal medications are not effective
-
The infection is localized to one part of the lung
-
There is persistent or worsening lung damage
-
Patients are fit enough to undergo surgery
🔍 What Does the Evidence Say?
Although not commonly performed, surgery for aspergillosis is documented in medical literature, especially in cases of:
-
Chronic pulmonary aspergillosis (CPA)
-
Fungal nodules
-
Subacute forms like SAIA
Key studies:
-
A U.S. study of >100,000 aspergillosis cases found that only 4.8% underwent surgery, usually for treatment failure or severe complications.
-
A Chinese study of 85 CPA patients showed a relapse rate of only 7% post-surgery, with most patients improving dramatically.
-
A UK case series described 30 patients having lung resections over 15 years, showing surgery is safe and effective when performed in experienced centres.
🔄 What Happens After Surgery?
Even after a successful resection, follow-up antifungal treatment is often continued to prevent recurrence. Monitoring usually includes:
-
Regular imaging (CT scans)
-
Galactomannan blood tests (to detect fungal components)
-
Symptom tracking
This is typically guided by a multidisciplinary team involving infectious diseases, respiratory, and thoracic surgery specialists.
🎯 Key Takeaways
-
SAIA is uncommon, and when antifungals fail, surgery can be life-changing.
-
Wedge resection is a lung-sparing procedure that removes just the infected portion, offering good outcomes when the disease is localised.
-
Ongoing antifungal therapy and monitoring are critical to long-term success.
-
Your story adds to a growing but still limited body of knowledge and may help inform future treatment decisions and encourage further research.
If you are a patient or clinician navigating SAIA and struggling with antifungal treatment, this story may offer hope—and a reminder that surgical options, though rarely needed, can be effective when used judiciously.