The Power of Keeping a Health Diary When You Have Aspergillosis

Last reviewed: June 2026
Audience: People living with aspergillosis, families and carers
Key points
- A health diary can help you understand symptoms, triggers and changes over time.
- It can be especially useful if you experience fatigue, brain fog or memory problems.
- It can make clinic appointments more focused and productive.
- A diary may show progress that is hard to notice day to day.
- The best diary is simple, quick and realistic to keep using.
Contents
- Why keep a health diary?
- How it can help with aspergillosis
- Brain fog and memory
- Spotting patterns and triggers
- Using your diary at appointments
- The psychological benefit
- Simple diary template
- Common questions
- When to seek medical advice
Why keep a health diary?
Living with aspergillosis often means symptoms change from day to day. Some days may be manageable. Others may involve more coughing, breathlessness, fatigue, sinus symptoms, poor sleep or medication side effects.
Because these changes can happen gradually, it can be difficult to remember exactly when symptoms started, whether they are getting better or worse, or what might have triggered them.
A health diary gives you a simple record of what is happening over time. It can help you, your family and your healthcare team see patterns that may not be obvious from memory alone.
How a diary can help with aspergillosis
People with aspergillosis may find it useful to record:
- Cough
- Breathlessness
- Fatigue
- Sputum or phlegm
- Wheeze
- Sinus symptoms
- Sleep quality
- Exercise or walking distance
- Mood and wellbeing
- Medication changes
- Possible side effects
You may also want to note possible triggers, such as damp or mould exposure, pollen, dusty environments, changes in weather, respiratory infections, stress, travel or changes in medication.
Brain fog and memory
Many people with long-term lung conditions describe episodes of brain fog. This may feel like forgetfulness, poor concentration, difficulty finding words, feeling mentally slower than usual, or feeling as though your head is “empty”.
Brain fog can have many possible causes, including fatigue, poor sleep, infection, inflammation, stress, anxiety, pain, medication side effects, low oxygen levels or other health problems.
A diary acts as an external memory. Instead of trying to remember when something changed, you can look back and see what was happening at the time.
Spotting patterns and triggers
| What you record | What it may help show |
|---|---|
| Symptoms | Whether cough, breathlessness or fatigue are improving or worsening |
| Sleep | Whether poor sleep is linked to worse symptoms |
| Exercise | What level of activity is manageable |
| Weather | Whether heat, humidity, cold air or storms affect symptoms |
| Environment | Possible links with damp, mould, dust or pollen |
| Medication | Possible benefits, side effects or changes during dose reduction |
| Infections | Early warning signs or repeated patterns |
Using your diary at appointments
Healthcare professionals may ask questions such as:
- When did your symptoms start?
- Are they getting better or worse?
- Have you noticed any triggers?
- Have you changed any medication recently?
- How far can you walk now compared with before?
- Have you had any infections or courses of antibiotics?
These questions are not always easy to answer from memory, especially when you are tired or anxious. A diary can help you give clearer, more accurate information.
You may find it useful to bring a short summary to your appointment, such as:
- Three things that have improved
- Three things that have worsened
- Any medication changes
- Your main questions for the appointment
Sometimes the diary tells a different story
When you have had a difficult few days, it can feel as though nothing is improving. A diary may show that the wider picture is more encouraging.
For example, you may feel:
“Nothing has changed.”
But your diary may show:
- You are walking further than three months ago
- You are sleeping better
- You have had fewer chest infections
- You are coughing less at night
- You are doing more social activities
Equally, a diary can show gradual deterioration that might otherwise be missed. Both types of information can be useful.
The psychological benefit
Chronic illness can feel unpredictable. A diary can help restore a sense of control by changing the question from:
“Why do I feel awful?”
to:
“What changed recently?”
This can reduce uncertainty and help you feel more involved in your care.
A diary can also become a record of resilience. It may include difficult days, but it can also capture walks completed, holidays taken, family events attended, personal goals reached and challenges overcome.
Keep it simple
Many people stop keeping a diary because they try to record too much. A simple diary is usually more useful than a complicated one.
A daily entry might take less than two minutes and include:
- Symptoms, scored from 0 to 10
- Energy level, scored from 0 to 10
- Sleep quality
- Exercise or activity
- Medication changes
- Anything unusual
Consistency matters more than detail.
Paper, phone or app?
There is no single correct way to keep a diary. You could use:
- A notebook
- A printed diary sheet
- A phone notes app
- A calendar
- Voice notes
- A spreadsheet
- A symptom tracking app
- A fitness tracker or smartwatch
The best diary is the one you will actually use.
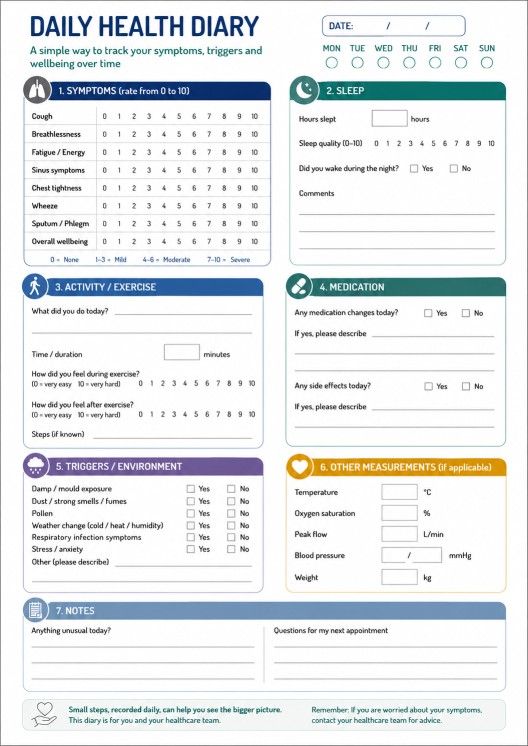
Simple diary template
Daily health diary
Date: __________________________
Symptoms, 0–10
Cough: ______
Breathlessness: ______
Fatigue: ______
Sinus symptoms: ______
Overall wellbeing: ______
Sleep
Hours slept: ______
Sleep quality, 0–10: ______
Activity
Exercise or activity today:
__________________________________________________
Medication
Any medication changes or side effects?
__________________________________________________
Notes
Anything unusual today?
__________________________________________________
__________________________________________________
Daily Diary - PDF downloadable
Common questions
Do I need to write every day?
No. Some people write daily. Others only record changes, flare-ups, medication changes or important events.
What if I forget for a few days?
That is very common. Simply restart when you remember. A diary does not have to be perfect to be useful.
Should I record test results?
You can if you find it helpful. Some people record blood results, oxygen saturations, lung function, weight, clinic letters or medication levels. Do not worry if this feels too much. A simple symptom diary is still useful.
Can a diary replace medical advice?
No. A diary is a tool to support conversations with your healthcare team. It should not be used to diagnose or treat symptoms without medical advice.
When to seek medical advice
Seek medical advice promptly if you experience:
- Sudden or significant worsening of breathlessness
- Coughing up large amounts of blood
- Persistent fever
- Severe chest pain
- New confusion or rapidly worsening brain fog
- Weakness, speech problems, facial drooping or visual changes
- Symptoms that are worsening quickly or feel unusual for you
If you are unsure, contact your healthcare team, NHS 111, your GP, or emergency services depending on severity.
Further information
- Living with aspergillosis
- Fatigue and aspergillosis
- Exercise and aspergillosis
- Mental wellbeing and aspergillosis
Author and review information
This article is provided for general educational support for people affected by aspergillosis. It is not a substitute for medical advice from your own healthcare team.
Prepared for: Aspergillosis.org
Last reviewed: June 2026
ABPA or Steroid Side Effects? Understanding Symptoms During Long-Term Treatment
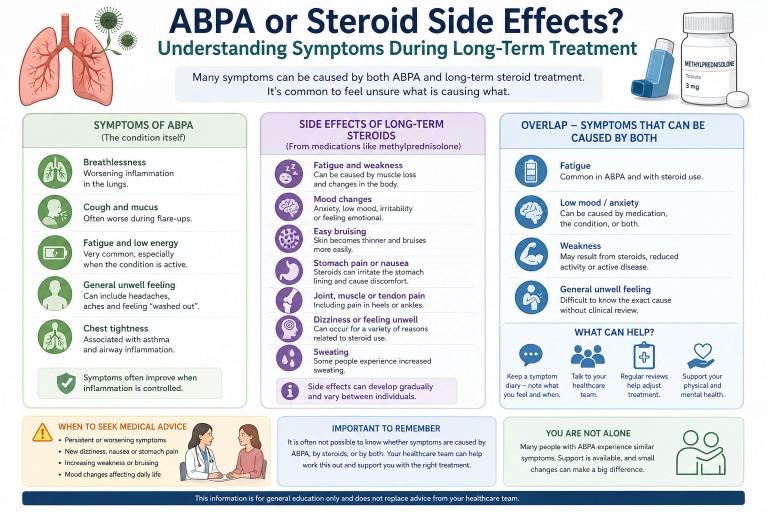

Last reviewed: April 2026
Many people living with Allergic Bronchopulmonary Aspergillosis (ABPA) who take long-term steroids find it difficult to tell whether their symptoms are caused by the condition or the treatment.
Symptoms in ABPA can come from both the condition and long-term steroid treatment. Fatigue, weakness, mood changes, and general unwellness are common to both, making it difficult to identify a single cause without clinical review.
This is especially true for people taking corticosteroids such as methylprednisolone or prednisolone.

---
Key Points
- ABPA and steroid treatment can cause overlapping symptoms.
- Fatigue, low mood, and general unwellness can come from either the condition or medication.
- Long-term corticosteroid use can cause additional side effects.
- It is common to feel unsure what is causing symptoms.
- Ongoing or worsening symptoms should be discussed with your healthcare team.
---
Why is it hard to tell the difference?
ABPA is an immune-driven lung condition that causes inflammation. Treatment often includes corticosteroids such as methylprednisolone or prednisolone, which reduce inflammation but can also affect many systems in the body.
This means that:
- The disease itself can cause symptoms
- The treatment can also cause symptoms
As a result, people often experience a combination of both.
---
Symptoms caused by ABPA
ABPA commonly affects the lungs but can also cause more general symptoms.
- Fatigue and low energy
- Breathlessness
- Cough and mucus production
- Chest tightness
- General feeling of being unwell
Fatigue can be particularly prominent, especially during flare-ups.
---
Side effects of long-term steroids
Corticosteroids such as methylprednisolone are highly effective treatments, but long-term use can lead to a range of side effects.
- Fatigue and weakness (including muscle loss)
- Mood changes (anxiety, low mood, irritability)
- Easy bruising (skin becomes thinner)
- Stomach irritation or pain
- Dizziness or feeling unwell
- Sweating
- Bone or joint discomfort
Learn more about treatment approaches in aspergillosis treatment options.
---
Where symptoms overlap
Some symptoms can be caused by both ABPA and steroid treatment, making them difficult to interpret.
| Symptom | Possible cause |
|---|---|
| Fatigue | ABPA inflammation or steroid effects |
| Low mood / anxiety | Medication effects or impact of chronic illness |
| Weakness | Muscle loss from steroids or reduced activity |
| General unwell feeling | Both |
This overlap is one of the most challenging aspects of long-term management.
🔎 Not sure what’s causing your symptoms?
Many people with ABPA feel exactly the same—this overlap is one of the most common challenges during long-term treatment.
---
Understanding specific symptoms
Some symptoms are more commonly linked to treatment effects:
- Easy bruising – often related to steroid use
- Heel or ankle pain – may relate to tendon or joint effects
- Stomach pain – can be linked to steroid irritation
Other symptoms, such as fatigue, dizziness, and nausea, may have multiple possible causes.
Because of this, it is often not possible to attribute symptoms to a single cause without clinical review.
---
When to seek medical advice
You should contact your healthcare team if you experience:
- Persistent or worsening fatigue
- New dizziness or nausea
- Ongoing stomach pain
- Increasing weakness
- Mood changes affecting daily life
These symptoms do not necessarily indicate a serious problem, but they may mean that treatment or support needs to be reviewed.
---
Summary
In ABPA, symptoms such as fatigue, weakness, and low mood can arise from both the condition and its treatment. Long-term steroid use can add additional effects, making it difficult to distinguish between causes.
If symptoms are persistent or worsening, it is important to discuss them with your healthcare team so that appropriate adjustments or support can be considered.
---
Further Reading
- Allergic Bronchopulmonary Aspergillosis (ABPA)
- Treatment of Aspergillosis
- Weight Loss and Weakness in Aspergillosis
---
Author & Review
Prepared for aspergillosis.org to support patient understanding. Content reflects current clinical knowledge and patient-reported experience.
Disclaimer
This information is for general education only and does not replace advice from your healthcare team.
Weight Loss and Weakness in Aspergillosis: Why It Happens, How It Feels, and What Helps Recovery
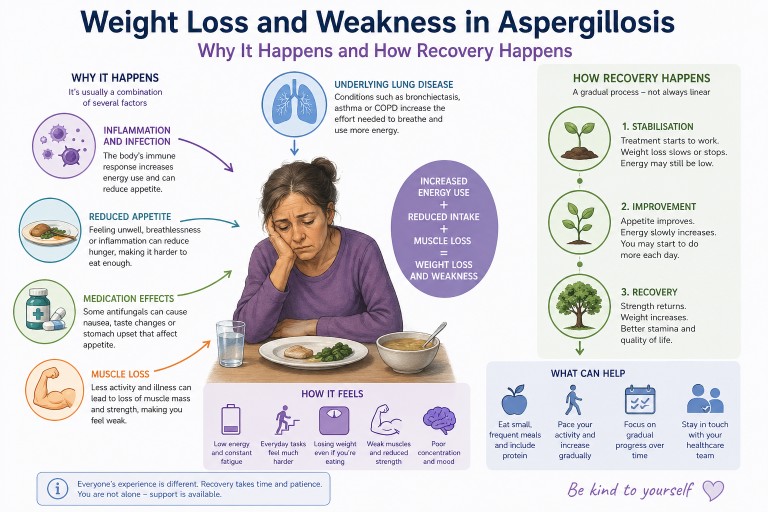
Last reviewed: April 2026
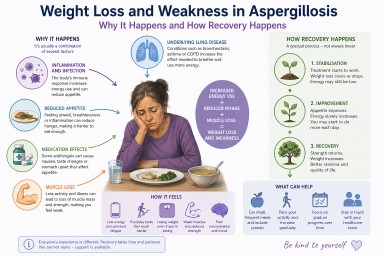
Unexpected weight loss and severe weakness are among the most worrying symptoms people report after being diagnosed with aspergillosis. Many describe feeling unlike themselves—physically drained, thinner than they have ever been, and struggling with everyday activities.
This article explains why this happens, what is going on in the body, and what recovery typically looks like.
---
Key Points
- Weight loss and fatigue are common in aspergillosis, particularly early in the illness or during flare-ups.
- They are usually caused by a combination of inflammation, increased energy use, reduced appetite, and muscle loss.
- Medication side effects can contribute but are rarely the main cause.
- Many people improve over time, but recovery is usually gradual and can take weeks to months.
- Stabilising weight is often the first important step before regaining strength.
---
Contents
- Why does aspergillosis cause weight loss?
- What is happening inside the body?
- Which types of aspergillosis are affected?
- Why does it feel so severe?
- Does it get better?
- What can help day to day?
- Nutrition and rebuilding strength
- When to seek medical advice
- Common questions
---
Why does aspergillosis cause weight loss?
Weight loss in aspergillosis is rarely due to a single cause. Instead, it is usually the result of several overlapping processes.
1. Increased energy use (hypermetabolism)
When the body is dealing with infection or inflammation, it requires more energy. This is sometimes described as a hypermetabolic state.
- The immune system is active and consumes energy
- The body produces inflammatory signals
- Breathing effort may increase
This means you may be burning more calories than usual—even at rest.
2. Reduced appetite
Many people notice they are eating less, sometimes without realising it. This may be due to:
- Feeling unwell or fatigued
- Shortness of breath when eating
- Changes in appetite driven by inflammation
3. Medication effects
Some treatments can affect appetite or digestion. For example:
- Antifungal medications such as itraconazole or voriconazole may cause nausea or taste changes
- Steroids may increase appetite but can also contribute to muscle weakness over time
Medication effects vary widely and are usually only part of the overall picture.
4. Muscle breakdown
During illness, the body may break down muscle to meet energy needs. This can happen quickly, especially if activity levels fall.
This leads to:
- Loss of strength
- Reduced stamina
- A feeling of being “weak” rather than just lighter
5. Underlying lung disease
Many people with aspergillosis also have conditions such as bronchiectasis, asthma, or chronic obstructive pulmonary disease (COPD). These can increase the effort required for breathing and contribute to ongoing energy use.
---
What is happening inside the body?
Several biological processes contribute to weight loss and fatigue:
- Inflammatory signalling: The immune system releases chemical signals that affect metabolism and appetite
- Catabolism: The body breaks down tissues (including muscle) to release energy
- Energy imbalance: More energy is used than consumed
This combination can make weight loss feel rapid and difficult to control.
---
Which types of aspergillosis are affected?
These symptoms are most commonly seen in:
- Chronic Pulmonary Aspergillosis (CPA)
- Allergic Bronchopulmonary Aspergillosis (ABPA), particularly during flare-ups
However, not everyone experiences weight loss, and severity varies.
---
Why does it feel so severe?
Many people describe this stage as one of the most difficult parts of their illness. This is because several factors are happening at once:
- Physical energy is reduced
- Muscle strength has declined
- The body is under ongoing stress
- Recovery has not yet begun
This can make everyday activities—such as walking, cooking, or even eating—feel unusually difficult.
---
Does it get better?
In many cases, yes—there is gradual improvement over time, especially once treatment begins to control the condition.
Recovery often follows a pattern:
- Initial phase: weight loss and severe fatigue
- Stabilisation: weight loss slows or stops
- Recovery: gradual return of strength and energy
This process is usually slow and uneven, with good and bad days.
---
What can help day to day?
1. Focus on maintaining nutrition
- Eat small amounts regularly rather than large meals
- Choose foods that are easy to prepare and eat
- Include protein to support muscle maintenance
2. Pace activity carefully
- Gentle movement can help maintain strength
- Avoid pushing too hard, as this can worsen fatigue
- Increase activity gradually as energy improves
3. Look at trends over time
It can be helpful to focus on gradual changes such as:
- Weight stabilising
- Small improvements in energy
---
Nutrition and rebuilding strength
Recovery often happens in stages:
- Stage 1: Stabilising weight
- Stage 2: Gradually increasing intake
- Stage 3: Rebuilding muscle and strength
Regaining muscle mass takes time and usually follows once the underlying condition is better controlled.
---
When to seek medical advice
You should contact your healthcare team if you experience:
- Continued or rapid weight loss
- Increasing weakness
- Difficulty eating or swallowing
- New or worsening symptoms
This may indicate the need for additional support or adjustment of treatment.
---
Common questions
Is weight loss just due to poor appetite?
No. Reduced appetite is only one factor. Increased energy use and muscle loss are also important contributors.
Are medications the main cause?
Medications can contribute, but they are rarely the main reason for weight loss.
Will I regain my strength?
Many people do regain strength over time, although recovery is usually gradual.
Why does recovery take so long?
The body needs time to reduce inflammation, restore energy balance, and rebuild muscle.
---
Summary
Weight loss and weakness in aspergillosis are common and can feel severe, particularly early in the illness. They are usually caused by a combination of increased energy use, reduced appetite, muscle loss, and underlying lung disease.
Although recovery can take time, many people improve gradually as treatment takes effect.
---
Further Reading
- Chronic Pulmonary Aspergillosis (CPA)
- Allergic Bronchopulmonary Aspergillosis (ABPA)
- Treatment of Aspergillosis
---
Author & Review
Prepared for aspergillosis.org to support patient understanding. Content reflects current clinical knowledge and patient-reported experience.
Disclaimer
This page is for general information only and does not replace advice from your healthcare team.
What if you can’t tolerate azole antifungal medicines?
Key points
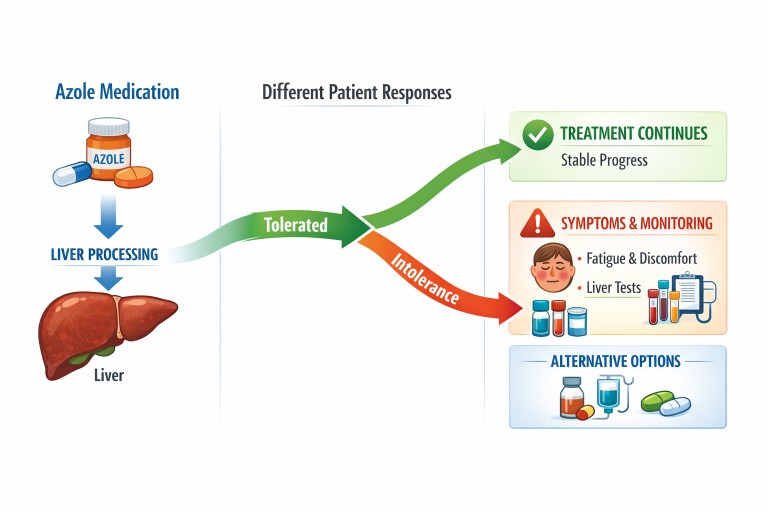
- Azole antifungals are commonly used to treat aspergillosis, but not everyone tolerates them well.
- “Azole intolerance” means the body reacts badly to the medication, even if it is otherwise effective.
- Symptoms can include fatigue, flushing, shaking, nausea, and discomfort around the liver area.
- In some cases, blood tests show changes in liver function.
- If azoles are not tolerated, there are often alternative approaches your clinical team can consider.
Contents
- What are azole antifungals?
- What is azole intolerance?
- Why does azole intolerance happen?
- Common symptoms to look out for
- The role of the liver
- What can be done if azoles are not tolerated?
- Why monitoring is important
- Common questions
- When to seek medical advice
What are azole antifungals?
Azole antifungals are a group of medicines used to treat fungal infections such as aspergillosis. They work by interfering with the fungal cell membrane, helping to stop the fungus growing.
Common examples include:
- Fluconazole
- Itraconazole
- Voriconazole
- Posaconazole
They are often used long-term in conditions like chronic pulmonary aspergillosis (CPA) or allergic bronchopulmonary aspergillosis (ABPA).
What is azole intolerance?
Azole intolerance means that a person develops unpleasant or harmful side effects when taking these medications, even at standard doses.
This is different from:
- Allergy – an immune reaction (e.g. rash, swelling, breathing difficulty)
- Resistance – when the fungus is not affected by the drug
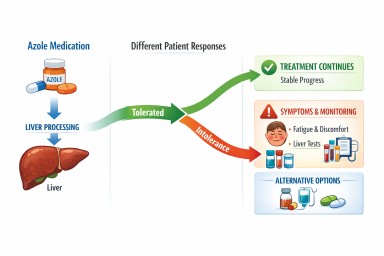
With intolerance, the drug may still work against the fungus—but the body cannot tolerate its effects.
Why does azole intolerance happen?
There is no single cause. Instead, several factors can contribute:
1. How the body processes the drug
Azoles are broken down in the liver. People vary in how efficiently this happens, which can lead to higher levels of the drug in the body.
2. Effects on liver enzymes
Azoles affect enzymes (called cytochrome P450 enzymes) that are involved in processing many medications. This can:
- Increase drug levels
- Cause interactions with other medications
- Put strain on the liver
3. Individual sensitivity
Some people are simply more sensitive to these drugs, even when blood levels are within the expected range.
4. Other health factors
- Existing liver conditions
- Age
- Other medications
- Nutritional status
Common symptoms to look out for
Patients describe a range of symptoms when azoles are not well tolerated, including:
- Flushed or hot cheeks
- Shaking or tremor
- Severe fatigue
- Nausea or reduced appetite
- Discomfort or pain in the upper abdomen, back, or sides (where the liver sits)
- General feeling of being unwell
These symptoms can appear soon after starting treatment or develop over time.
The role of the liver
The liver plays a central role in processing azole antifungals.
In some cases, this can lead to:
- Raised liver enzymes on blood tests
- Inflammation or irritation of the liver
It is important to note that:
- Some people have abnormal blood tests without symptoms
- Others feel unwell even when tests are only mildly changed
This is why both symptoms and blood tests are considered together.
What can be done if azoles are not tolerated?
If azole intolerance is suspected, your clinical team may consider several approaches:
Adjusting treatment
- Reducing the dose
- Changing how the medication is taken (e.g. with food)
Switching to another azole
Some people tolerate one azole better than another.
Therapeutic drug monitoring (TDM)
Blood tests can measure drug levels to help ensure they are not too high or too low.
Considering non-azole treatments
In some cases, different classes of antifungal medication may be considered.
The best approach depends on the individual, the condition being treated, and how severe the side effects are.
Why monitoring is important
Because azoles affect the liver and interact with other medications, monitoring is a routine part of care.
This may include:
- Regular liver function blood tests
- Drug level monitoring (for some azoles)
- Review of other medications
Monitoring helps detect problems early and allows treatment to be adjusted safely.
Common questions
Does intolerance mean I cannot take any antifungal treatment?
No. Many patients who cannot tolerate one medication can use another, or a different approach may be possible.
Will the symptoms settle if I continue?
In some cases mild symptoms improve, but persistent or worsening symptoms should always be reviewed.
Is this common?
Most people tolerate azoles reasonably well, but intolerance is recognised and not rare in specialist clinics.
When to seek medical advice
You should contact your healthcare team if you experience:
- Persistent or worsening fatigue
- Pain in the upper abdomen, back, or sides
- Nausea affecting eating or drinking
- New or unusual symptoms after starting medication
Seek urgent medical attention if you notice:
- Yellowing of the skin or eyes (jaundice)
- Dark urine or pale stools
- Severe abdominal pain
Summary
Azole antifungals are an important part of treating aspergillosis, but some people experience intolerance.
This is usually related to how the body processes the medication—particularly in the liver—and varies from person to person.
If intolerance occurs, it does not mean that treatment options have run out. With careful monitoring and specialist input, alternative strategies can often be found.
Further reading
- Chronic pulmonary aspergillosis (CPA)
- Allergic bronchopulmonary aspergillosis (ABPA)
- Information for healthcare professionals
Author & review
This article has been prepared for patients and carers using information aligned with UK specialist practice, including the National Aspergillosis Centre (Manchester, UK).
Important: This content is for general educational purposes only and is not a substitute for medical advice. Always speak to your healthcare team about your own situation.
Why Headaches Can Occur in Aspergillosis
Last reviewed: March 2026
Key Points
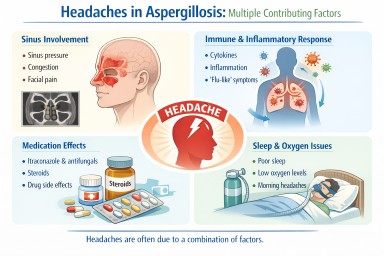
- Headaches are relatively common in people living with aspergillosis, but they usually have multiple contributing causes.
- Common causes include sinus involvement, inflammation, sleep disturbance, and medication effects.
- Antifungal medicines such as itraconazole may improve some symptoms indirectly but can also occasionally cause headaches.
- Patterns (timing, location, triggers) can help identify likely causes, but headaches are rarely due to one factor alone.
- New, severe, or unusual headaches should always be assessed by a healthcare professional.
Table of Contents
- Overview
- Sinus involvement (common cause)
- Inflammation and immune response
- Allergic-type responses (e.g. ABPA)
- Medication effects
- Sleep disturbance and night symptoms
- Breathing and oxygen levels
- General health factors
- Understanding headache patterns
- Common questions
- When to seek medical advice
- Summary
- Author and review
- References
Overview
Many people living with aspergillosis report headaches at some point during their illness. These headaches can vary in type, severity, and timing, and may be confusing—especially when they change over time or seem linked to treatment.
In most cases, headaches are not caused by a single factor. Instead, they reflect a combination of:
- local effects (such as sinus pressure)
- immune system activity
- medication effects
- sleep and general health factors
Understanding these different contributors can help make sense of symptoms and support more informed discussions with your clinical team.
Sinus involvement (common cause)
When Aspergillus affects the sinuses (sometimes called fungal sinusitis), this can directly cause headaches.
This happens because:
- sinus drainage becomes blocked
- pressure builds up in the sinus cavities
- the lining of the sinuses becomes inflamed
Typical features:
- pain or pressure in the forehead, cheeks, or behind the eyes
- worsening when bending forward
- a feeling of fullness or congestion
This is one of the most direct ways aspergillosis can lead to headaches.
Inflammation and immune response
Even when the sinuses are not directly involved, the body’s immune response to fungal material can cause systemic effects.
The immune system releases signalling molecules (such as cytokines) that can:
- increase inflammation
- affect blood vessels
- trigger headache pathways
This type of headache can feel similar to a “flu-like” or inflammatory headache.
Allergic-type responses (e.g. ABPA)
In conditions such as Allergic Bronchopulmonary Aspergillosis (ABPA), the immune system reacts strongly to Aspergillus.
This may involve:
- allergic pathways
- histamine and related mediators
- ongoing airway inflammation
Possible symptoms:
- head pressure or discomfort
- fluctuating headaches
- a “foggy” or unwell feeling
These headaches are often less clearly localised than sinus-related pain.
Medication effects
Some treatments used in aspergillosis can contribute to headaches.
Antifungal medications (e.g. itraconazole):
- headache is a recognised side effect in some people
- effects vary between individuals
Steroids (if prescribed):
- can affect sleep and mood
- may influence blood pressure
- can indirectly contribute to headaches
Medication effects can sometimes overlap with disease-related symptoms, making patterns harder to interpret.
Sleep disturbance and night symptoms
Sleep disruption is common in chronic lung conditions.
Possible contributors include:
- night-time coughing
- breathlessness
- discomfort or anxiety
Poor sleep can lead to:
- morning headaches
- increased sensitivity to pain
- fatigue-related headaches
Breathing and oxygen levels
In some people with more advanced lung involvement:
- oxygen levels may be slightly reduced
- breathing effort may increase
This can contribute to:
- morning headaches
- fatigue and cognitive symptoms
Not all patients experience this, but it is an important factor in some cases.
General health factors
Headaches can also be influenced by general aspects of living with a long-term condition:
- dehydration
- fatigue
- reduced activity levels
- stress or anxiety
These factors can contribute to tension-type headaches or make other headache types more noticeable.
Understanding headache patterns
Looking at patterns can sometimes help identify likely contributors.
- Facial pressure worse on bending: may suggest sinus involvement
- Early morning headaches: may relate to sleep or breathing patterns
- Fluctuating or “wave-like” symptoms: may reflect inflammation or immune activity
- New headaches after starting medication: may be treatment-related
However, these are general observations only and do not replace clinical assessment.
Headaches in Aspergillosis: Interactive Decision Aid
This tool helps patients and carers think about common patterns that can contribute to headaches in aspergillosis. It does not diagnose the cause of a headache.
It is designed to support discussion with a healthcare professional and highlight possible contributors such as sinus involvement, inflammation, medication effects, sleep disturbance, and breathing-related factors.
1. Where is the pain mainly felt?
2. When is it most noticeable?
3. What does it feel like?
4. What other features are present?
5. Are there any red flags?
Possible contributors
This panel highlights common patterns only. It is not a diagnosis and does not replace medical assessment.
Common questions
Are headaches a recognised symptom of aspergillosis?
They can occur, but are usually indirect and caused by associated factors such as sinus disease or inflammation.
Can antifungal treatment improve headaches?
In some cases, yes—if symptoms are linked to fungal-related inflammation. However, antifungals can also occasionally cause headaches as a side effect.
Are “histamine-type” headaches part of aspergillosis?
Some patients describe symptoms in this way, but the underlying mechanism is often more complex than histamine alone.
Why do my headaches change over time?
This is common and may reflect changes in inflammation, treatment, sleep, or overall health.
When to seek medical advice
You should seek medical advice if you experience:
- new or unusually severe headaches
- headaches that are worsening over time
- neurological symptoms (e.g. vision changes, weakness, confusion)
- fever, neck stiffness, or other concerning symptoms
If you are unsure whether your headaches are related to aspergillosis, treatment, or another cause, it is important to discuss this with your healthcare team.
Summary
Headaches in people with aspergillosis are usually caused by a combination of factors rather than a single issue.
The most common contributors include:
- sinus involvement
- immune and inflammatory responses
- sleep disturbance
- medication effects
Understanding patterns and changes over time can be helpful, but medical assessment is important if symptoms are new, severe, or concerning.
Author and review
Prepared for: aspergillosis.org
Audience: Patients and non-specialist readers
Important: This article is for general information only and does not replace individual medical advice.
References
- Patterson TF et al. (2016). Practice Guidelines for the Diagnosis and Management of Aspergillosis.
PMID: 27365388 - Denning DW et al. (2016). Chronic pulmonary aspergillosis guidelines.
PMID: 26699723 - Chakrabarti A et al. (2009). Fungal sinusitis: a categorization and definitional schema.
PMID: 19522756
Why Do My “Histamine” Headaches Improve on Itraconazole?
Last reviewed: March 2026
Key Points
- Itraconazole is an antifungal medicine. It is not an antihistamine.
- Some people notice that symptoms such as headaches, flushing, or a “histamine-type” feeling become shorter or less intense after starting treatment.
- This is most likely because itraconazole reduces the fungal burden and the immune response it triggers, rather than blocking histamine directly.
- Symptoms that happen in the early hours of the morning may also be influenced by the body’s natural day-night rhythm.
- Changes in symptoms can be helpful clues, but headaches can have more than one cause.
Table of Contents
- Overview
- What is itraconazole and how does it work?
- What do people mean by “histamine dump” headaches?
- Why might symptoms improve on itraconazole?
- Why do symptoms often happen at night?
- Does this mean histamine is the main problem?
- Common questions
- When to seek medical advice
- Summary
- Author and review
- References
Overview
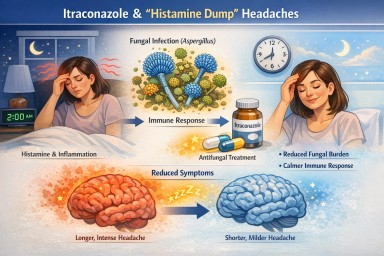
Some people taking itraconazole for non-lung or lung forms of aspergillosis notice that symptoms they describe as “histamine-type” symptoms, such as headaches, flushing, pressure, or a general sense of inflammatory overload, become shorter or less severe.
A typical pattern might be:
- Symptoms start overnight, for example, around 2 am
- Symptoms previously lasted most of the day
- Symptoms are now settling much earlier after starting treatment
This can be confusing, especially when the symptoms feel similar to a histamine reaction. The important point is that itraconazole does not work like an antihistamine, but it can reduce symptoms indirectly if a fungal process is contributing to them.
What is itraconazole and how does it work?
Itraconazole is an antifungal medicine used to treat infections caused by fungi such as Aspergillus.
It works by interfering with the production of ergosterol, an essential part of the fungal cell membrane. This weakens the fungus and helps reduce fungal growth and survival in the body.
As the fungal burden falls, the immune system may be less strongly stimulated, and that can lead to a reduction in inflammation-related symptoms.
So although itraconazole does not block histamine directly, it may reduce the underlying trigger that is causing the body to react.
What do people mean by “histamine dump” headaches?
“Histamine dump” is not a formal medical diagnosis, but some patients use it as a practical way of describing symptoms such as:
- sudden headaches, especially overnight or early in the morning
- flushing or a feeling of heat
- pressure in the head or sinuses
- a sense of being “wired”, agitated, or unwell
These symptoms may involve histamine, but they can also reflect broader inflammation, immune activation, mast cell activity, or other signalling chemicals in the body.
Why might symptoms improve on itraconazole?
If itraconazole is helping, it is most likely doing so indirectly. There are several possible reasons for this.
1. Reduced fungal burden
If fungal material in the body is reduced, there may be less for the immune system to react to. That can mean less inflammatory signalling overall.
2. Reduced immune activation
Fungi can stimulate the immune system in ways that lead to inflammation and, in some people, histamine-related symptoms. If antifungal treatment lowers that stimulus, symptoms may become less intense or settle more quickly.
3. Shorter inflammatory response
Some people find that the symptom still begins, but does not “run on” for as long. For example, a headache that used to last from 2am until late afternoon may now settle by 5am.
Why do symptoms often happen at night?
The body has a natural circadian rhythm, a 24-hour cycle that affects hormones, inflammation, sleep, and immune activity.
- Some inflammatory signals can be more noticeable overnight
- Cortisol rises in the early morning, and helps suppress inflammation
Does this mean histamine is the main problem?
Not necessarily. Symptoms may involve multiple pathways, including immune response to fungi, general inflammation, mast cell activity, and sinus pressure.
Common questions
Does itraconazole act like an antihistamine?
No. It does not block histamine receptors.
Why are my symptoms improving but not gone?
This is common and may reflect partial control of the underlying trigger.
Does this prove Aspergillus is the cause?
No. It suggests a possible link but does not confirm causation.
Will symptoms continue to improve?
Possibly, but responses vary between individuals.
When to seek medical advice
- new or severe headaches
- neurological symptoms (vision, speech, balance)
- worsening or persistent symptoms
- concerns about medication side effects
Summary
Itraconazole does not directly affect histamine but may reduce symptoms by lowering fungal burden and immune activation.
Author and review
Prepared for: aspergillosis.org
Audience: Patients and non-specialist readers
Important: This does not replace individual medical advice.
References
- Patterson TF, Thompson GR 3rd, Denning DW, et al. (2016).
Practice Guidelines for the Diagnosis and Management of Aspergillosis.
View on PubMed (PMID: 27365388) - Denning DW et al. (2016).
Chronic pulmonary aspergillosis guidelines.
View on PubMed (PMID: 26699723) - Barnes PJ, Adcock IM (2009).
Circadian rhythm in airway disease.
View on PubMed (PMID: 19336589) - Stone KD et al. (2010).
IgE, mast cells, and eosinophils.
View on PubMed (PMID: 20176269)
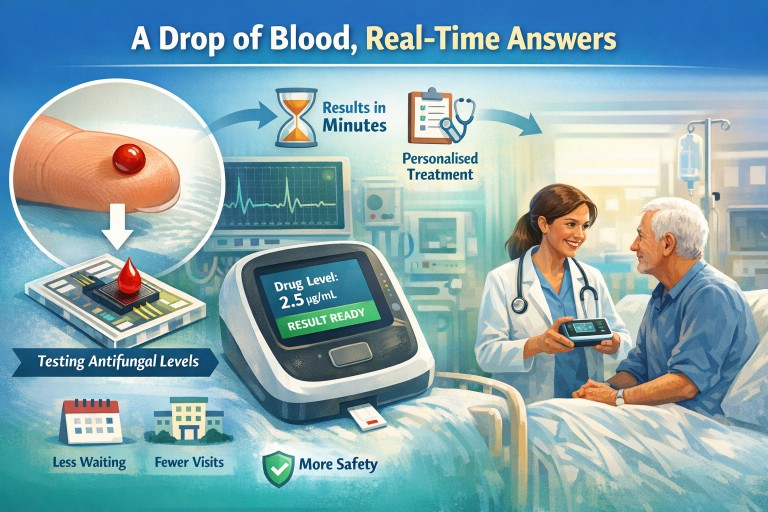
A Drop of Blood, Real-Time Answers
Last reviewed: 20 March 2026
Audience: Patients, carers, families, and non-specialists
Topic: Point-of-care monitoring of antifungal drug levels
New bedside testing for antifungal drugs — and why patients welcome it
For many people taking antifungal medicines, blood tests are an important part of care. These tests help doctors check whether the amount of medicine in the body is too low, too high, or about right.
A new type of technology is being developed to do this much more quickly, using just a single drop of blood placed onto a specialised chip. Instead of sending blood away to a laboratory and waiting days for a result, this kind of test may be able to provide an answer much more quickly, sometimes during the clinic visit itself.
Patients in a recent focus group responded very positively to this idea. They welcomed not only the technology itself, but also what it could mean for their care: less waiting, less uncertainty, fewer trips to hospital, and more personalised treatment.
Key points
- A new test can measure antifungal drug levels from a drop of blood.
- The blood is placed on a specialised chip containing tiny sensors.
- Results may be available much faster than standard laboratory testing.
- This could help doctors adjust treatment more quickly and more precisely.
- Patients in a focus group strongly welcomed the technology.
- Reported benefits included less anxiety, fewer hospital visits, and more confidence in treatment decisions.
What is this new test?
This is a type of point-of-care test. That means it is designed to be used close to the patient, such as in a clinic or at the bedside, rather than sending the sample away to a central laboratory.
In this case, the aim is to measure the level of an antifungal drug in the blood from a very small sample, sometimes just a finger-prick drop. The drop of blood is placed onto a specialised chip. That chip contains tiny channels and sensors that can detect the amount of drug present.
People sometimes describe this type of system as a “lab on a chip” because it performs some of the work of a laboratory in a very small device.
How does the technology work?
The exact science varies between devices, but the general idea is similar.
- A small blood sample is taken.
This may be from a finger prick rather than a larger blood draw. - The blood is placed onto a specialised chip.
The chip is designed to handle a tiny volume of blood. - The blood moves through microscopic channels.
These channels guide the sample to the parts of the chip that do the measurement. - Sensors on the chip detect the antifungal drug.
These sensors are designed to recognise the drug or react to it in a measurable way. - A reader produces a result.
A connected device reads the signal from the chip and estimates the drug level.
Some systems use electrical signals, some use light, and some use chemical reactions. Patients do not need to understand all the engineering details to understand the main point: the chip is acting like a mini laboratory.
A simple way to think about it is this:
Instead of sending your blood sample to a distant laboratory, this technology brings part of the laboratory to your fingertip.
Why do antifungal drug levels matter?
Some antifungal medicines need careful monitoring because the “right” level can be quite important.
If the drug level is too low, the medicine may not work well enough. If the drug level is too high, side effects may become more likely.
This can be especially relevant for antifungal drugs such as:
- itraconazole
- voriconazole
- posaconazole
Drug levels can vary from person to person for many reasons, including:
- how well the body absorbs the medicine
- interactions with other medicines
- differences in liver function and metabolism
- changes in health over time
At present, monitoring usually involves sending blood to a laboratory. That works, but it can mean delays. Results may not come back quickly enough to guide decisions during the clinic appointment itself.
A faster bedside test could help clinicians make treatment decisions more quickly and could support more personalised care.
What did patients say about it?
In the patient focus group, this technology was widely welcomed. Patients were not only interested in the novelty of the test. They also recognised several practical benefits that could make day-to-day care easier and safer.
1. Faster results could reduce anxiety
Many patients described the stress of waiting for test results. Waiting can create a sense of uncertainty: Is the treatment working? Is the dose correct? Are side effects more likely?
A test that gives much quicker results was seen as reassuring. Instead of waiting days, patients liked the idea of getting answers much sooner, possibly while still in clinic.
2. Fewer visits could reduce the burden of care
For many people with chronic lung conditions or long-term illness, going to hospital is not a small task. Travel, parking, breathlessness, fatigue, mobility problems, and long waits can make even a short appointment exhausting.
Patients felt that a faster and simpler test could reduce some of this burden, especially if it could be built into a normal appointment or eventually be offered closer to home.
3. More personalised dosing felt important
Patients often understand from experience that medicines do not affect everyone in the same way. One person may tolerate a treatment well, while another may have side effects or absorb the medicine differently.
Because of this, patients valued the idea that treatment could be adjusted based on their own measured drug level, rather than relying only on standard dosing. This gave a stronger sense that care was being tailored to the individual.
4. Closer monitoring gave reassurance about safety
Antifungal drugs can be very helpful, but patients also know that some of them can have side effects and interactions. That can make treatment feel worrying, especially over longer periods.
Patients said that being able to check drug levels more quickly and more easily could help them feel safer. It suggested that treatment was being watched closely rather than left unchecked between appointments.
5. Immediate results could help patients feel more involved
Another important theme was involvement. Patients often feel that blood is taken, results disappear into the system, and decisions come later without much real-time discussion.
By contrast, a bedside result creates the possibility of discussing the number there and then. Patients felt this could help them better understand their treatment and feel more involved in decisions about dose changes and ongoing care.
6. It seemed to fit better with real life
Patients repeatedly emphasised that long-term treatment has to fit around real lives, not just clinic systems. Many welcomed the idea of a test that was quicker, simpler, and potentially more convenient.
In that sense, what patients welcomed was not just a chip or a machine, but a model of care that felt more responsive and more human-centred.
What could this mean for future care?
If this technology proves accurate, reliable, and affordable, it could support a different way of monitoring antifungal treatment.
Possible future benefits could include:
- drug level testing during the clinic appointment itself
- faster dose adjustment when levels are too high or too low
- closer monitoring when starting or changing treatment
- fewer repeat visits just to check blood levels
- potential future use in community settings or, one day, at home
It is important to be realistic. New technologies must be carefully tested before they become routine. They need to be shown to be accurate, dependable, and practical in real healthcare settings.
Even so, patients clearly recognised the potential. For them, this is not just about speed. It is about moving toward care that is:
- more responsive
- more personalised
- more convenient
- less anxiety-provoking
Common questions
Is this available now?
Usually not as a routine test in most healthcare settings. It is still being developed and studied, although interest in this type of monitoring is growing.
Will this replace ordinary blood tests?
Not immediately. Standard laboratory testing is still important. New bedside systems may first be used alongside existing methods while they are being evaluated and introduced.
Would this work for every antifungal drug?
Not necessarily. Some devices may be designed for specific drugs first. Wider use would depend on the technology and the evidence supporting it.
Could this be used at home?
Possibly one day, but that is likely to depend on how reliable, affordable, and easy to use the technology becomes. For now, clinic or bedside use is the more immediate possibility.
Why is a drop-of-blood test appealing to patients?
Because it may mean quicker answers, less uncertainty, fewer hospital trips, and more confidence that treatment decisions are based on what is happening in their own body.
When to seek medical advice
You should contact your healthcare team if you:
- develop new or worsening side effects from your antifungal medicine
- feel your treatment is not helping
- have concerns about drug interactions with other medicines
- are unsure whether to continue, stop, or change your medication
A new bedside test could support treatment decisions, but it would not replace medical advice. Symptoms, scans, blood tests, and clinical review would still matter.
Final thoughts
This new chip-based bedside technology may sound futuristic, but the reason patients welcomed it is very straightforward.
They saw the possibility of care that is faster, clearer, safer, and better adapted to real life.
In other words, this is about more than measuring a drug level from a drop of blood. It is about moving away from delayed, one-size-fits-all monitoring and toward real-time, personalised, patient-centred care.
In one sentence
A tiny chip and a drop of blood could help doctors adjust antifungal treatment more quickly — and patients believe that could make care less stressful, less burdensome, and more personal.
Author: Graham Atherton and ChatGPT draft support
For review by: National Aspergillosis Centre / relevant clinical or research reviewer
Note: This article is for general information and should not be used as a substitute for medical advice.
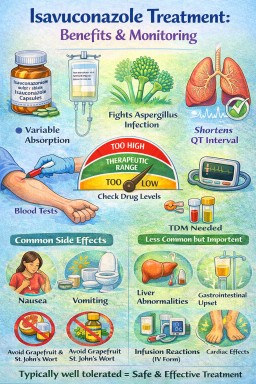
Isavuconazole in Aspergillosis
A balanced guide for patients and clinicians
Isavuconazole (given as the prodrug isavuconazonium sulfate) is a newer broad-spectrum triazole antifungal used in:
-
Chronic pulmonary aspergillosis (CPA)
-
Invasive aspergillosis
-
Patients who cannot tolerate other azoles
-
Selected refractory Allergic bronchopulmonary aspergillosis (ABPA) cases
It is available as oral capsules and intravenous (IV) formulation and is often chosen for its favourable tolerability profile.
1️⃣ What Isavuconazole Does
Like other azoles, isavuconazole inhibits fungal CYP51 (14-α-demethylase), blocking ergosterol synthesis and impairing fungal cell membrane formation.
It:
-
Suppresses Aspergillus growth
-
Reduces fungal burden
-
Helps stabilise lung disease
-
Provides systemic antifungal coverage
Clinical improvement is gradual over weeks.
2️⃣ How Long Is Treatment?
In CPA
-
Often 6–12 months or longer
-
May be used when other azoles cause side effects
-
Sometimes used as long-term suppressive therapy
In Invasive Aspergillosis
-
Duration depends on immune recovery and response
-
Often several months
In ABPA
-
Used selectively when other azoles are not tolerated
As with all azoles, stopping too early may lead to relapse.
3️⃣ Pharmacokinetics – Why It’s Different
Isavuconazole has more predictable pharmacokinetics than itraconazole or voriconazole.
Key features:
-
High oral bioavailability
-
Not dependent on gastric acidity
-
Food has minimal impact
-
Linear pharmacokinetics (dose–level relationship more predictable)
-
Long half-life (~100–130 hours)
Importantly:
It shortens the QT interval (unlike other azoles, which may prolong it).
This can make it preferable in patients with QT prolongation risk.
4️⃣ Do We Need Blood Level Monitoring?
Therapeutic Drug Monitoring (TDM) is not routinely required in all patients.
However, levels may be considered in:
-
Treatment failure
-
Drug interactions
-
Extreme body weight
-
Severe liver disease
-
Long-term therapy
This is a practical advantage compared with voriconazole.
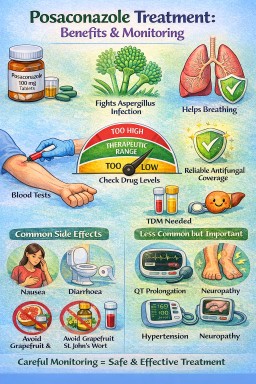
5️⃣ Common Side Effects (Usually Mild)
-
Nausea
-
Vomiting
-
Diarrhoea
-
Headache
Generally fewer visual or skin-related effects compared with voriconazole.
6️⃣ Less Common but Important Effects
Liver Abnormalities
Routine liver monitoring is recommended.
Most abnormalities are mild and reversible.
Gastrointestinal Upset
Can occur early in therapy but often settles.
Infusion Reactions (IV Form)
Occasional mild reactions with IV administration.
Cardiac Effects
Unlike other azoles:
-
Isavuconazole may shorten QT interval
-
It is not associated with QT prolongation
This makes it attractive in patients with:
-
Existing QT prolongation
-
Multiple QT-prolonging drugs
However, ECG review may still be prudent in complex cardiac patients.
7️⃣ Drug Interactions
Isavuconazole:
-
Moderately inhibits CYP3A4
-
Has fewer interactions than some other azoles
Still review carefully, especially with:
-
Immunosuppressants
-
Statins
-
Certain anticoagulants
Avoid:
-
St John’s Wort
-
Strong enzyme inducers
Grapefruit has less impact than with other azoles but is generally avoided as a precaution.
8️⃣ Comparison Snapshot
| Feature | Itraconazole | Voriconazole | Posaconazole | Isavuconazole |
|---|---|---|---|---|
| Acid-dependent absorption | Yes (capsules) | No | No (tablet) | No |
| Genetic metabolism impact | Low | High (CYP2C19) | Low | Low |
| QT prolongation | Minimal | Possible | Possible | No (shortens QT) |
| Visual side effects | Rare | Common | Rare | Rare |
| TDM required | Yes | Essential | Recommended | Usually not |
| Long-term tolerability | Moderate | Sometimes limited | Often good | Often very good |
Balanced Summary for Patients
Isavuconazole is a newer antifungal that is often easier to tolerate and has more predictable levels in the body. Blood tests and monitoring help ensure treatment remains safe and effective.
Clinician Checklist
-
Confirm indication and prior azole exposure
-
Baseline liver function tests
-
Review interacting medications
-
Consider ECG if complex cardiac history
-
Consider TDM only if clinically indicated
Posaconazole in Aspergillosis
A balanced guide for patients and clinicians
-
Chronic pulmonary aspergillosis (CPA)
-
Allergic bronchopulmonary aspergillosis (ABPA) (selected or refractory cases)
-
Invasive aspergillosis
-
Patients intolerant of itraconazole or voriconazole
-
Antifungal prophylaxis in high-risk immunocompromised patients
It is generally well tolerated and often used when other azoles cause side effects.
1️⃣ What Posaconazole Does
Like other azoles, posaconazole blocks fungal ergosterol synthesis (CYP51 inhibition), preventing fungal growth.
It:
-
Suppresses Aspergillus replication
-
Reduces fungal burden
-
Helps stabilise lung disease in CPA
-
Can reduce steroid need in some ABPA cases
It works gradually over weeks.
2️⃣ How Long Is Treatment?
In CPA
-
Often 6–12 months or longer
-
Sometimes long-term suppressive therapy
-
Used if other azoles are ineffective or not tolerated
In ABPA
-
Used in refractory or steroid-dependent disease
In prophylaxis
-
Duration depends on immune suppression status
As with other azoles, premature discontinuation may lead to relapse.
3️⃣ Formulations Matter
Posaconazole comes in:
-
Delayed-release tablets
-
Oral suspension
-
Intravenous formulation
Tablets (preferred)
-
Good, reliable absorption
-
Less affected by food
-
More predictable levels
Oral suspension
-
Absorption highly dependent on food (especially fatty meals)
-
Greater variability
In most CPA practice, tablets are preferred.
4️⃣ Why Blood Level Monitoring Is Still Important
Posaconazole has more predictable pharmacokinetics than itraconazole or voriconazole, but monitoring is still recommended.
Reasons:
-
Interpatient variability
-
Drug interactions
-
Severe infection requires adequate exposure
-
Toxicity avoidance
If Levels Are Too Low
-
Inadequate fungal suppression
-
Ongoing disease activity
-
Risk of resistance
If Levels Are Too High
-
Liver abnormalities
-
Gastrointestinal symptoms
-
Rare cardiac effects
Typical Target (Trough)
-
1 mg/L for treatment
-
0.7 mg/L often sufficient for prophylaxis
(Laboratory guidance varies.)
Levels are typically checked:
-
After 5–7 days
-
After dose adjustments
-
If response is suboptimal
-
If toxicity suspected
5️⃣ Common Side Effects (Usually Mild)
-
Nausea
-
Diarrhoea
-
Abdominal discomfort
-
Headache
These are often less troublesome than with voriconazole.
6️⃣ Less Common but Important Effects
Liver Abnormalities
Routine monitoring required.
Most are mild and reversible.
QT Interval Prolongation
Posaconazole can prolong QT interval.
Caution in patients with:
-
Known arrhythmias
-
Electrolyte imbalance
-
Other QT-prolonging drugs
ECG monitoring may be appropriate in higher-risk individuals.
Hypertension & Mineralocorticoid Effect (Rare)
High levels can rarely cause:
-
Elevated blood pressure
-
Low potassium
More common with long-term or high exposure.
Neuropathy
Much less commonly reported than with other azoles, but peripheral symptoms should still be assessed carefully if they occur.
7️⃣ Food & Drug Advice
-
Tablets: can be taken with or without food (follow prescribing guidance)
-
Suspension: take with food (preferably fatty meal)
Avoid:
-
Grapefruit
-
St John’s Wort
Posaconazole inhibits CYP3A4 and interacts with:
-
Statins
-
Certain immunosuppressants
-
Some anticoagulants
Medication review is essential.
8️⃣ Comparison Snapshot
| Feature | Itraconazole | Voriconazole | Posaconazole |
|---|---|---|---|
| Absorption variability | High | Moderate | Low–Moderate (tablet) |
| Visual side effects | Rare | Common | Rare |
| Photosensitivity | Rare | Common | Rare |
| QT prolongation | Minimal | Possible | Possible |
| TDM needed | Yes | Essential | Recommended |
| Long-term tolerability | Moderate | Sometimes limited | Often good |
Balanced Summary for Patients
Posaconazole is a newer azole that is often well tolerated and provides reliable antifungal coverage. Blood tests help ensure the level is effective and safe. Most patients complete treatment without major difficulties.
Clinician Checklist
-
Confirm formulation (tablet preferred in CPA)
-
Baseline LFTs
-
Review ECG if cardiac risk present
-
Check electrolytes (especially potassium)
-
Arrange trough level after initiation
-
Review full medication list
Voriconazole in Aspergillosis
A balanced guide for patients and clinicians
-
Chronic pulmonary aspergillosis (CPA)
-
Allergic bronchopulmonary aspergillosis (ABPA) (selected cases)
-
Invasive aspergillosis
-
Azole-resistant or itraconazole-intolerant cases
It is available orally and intravenously and is often used when a stronger or more reliably absorbed azole is required.
1️⃣ What Voriconazole Does
Voriconazole works by blocking fungal ergosterol synthesis (CYP51 inhibition), which disrupts the fungal cell membrane.
Compared with itraconazole:
-
More potent against Aspergillus
-
More predictable oral absorption
-
More central nervous system penetration
It often produces symptom improvement over weeks, though some effects (e.g. visual symptoms) may occur quickly.
2️⃣ How Long Is Treatment?
In CPA
-
Often 6–12 months or longer
-
Sometimes used as second-line or after intolerance to itraconazole
-
Long-term suppressive therapy may be required
In ABPA
-
Used in selected steroid-dependent or refractory cases
In invasive disease
-
Typically several months depending on response and immune status
3️⃣ Why Blood Level Monitoring Is Essential
Voriconazole has non-linear pharmacokinetics.
Small dose changes can cause large blood level shifts.
Two patients on the same dose may have very different levels due to:
-
Liver metabolism (CYP2C19 genetic variation is important)
-
Drug interactions
-
Age
-
Weight
-
Liver function
If Levels Are Too Low
-
Treatment failure
-
Persistent fungal activity
-
Risk of resistance
If Levels Are Too High
-
Liver toxicity
-
Neurological side effects
-
Visual disturbances
-
Increased interaction risk
Typical Target (Trough)
-
Generally 1–5.5 mg/L (lab dependent)
-
Toxicity risk increases >5–6 mg/L
Levels are usually checked:
-
5–7 days after starting
-
After dose adjustments
-
If side effects occur
-
If clinical response is inadequate
4️⃣ Common Side Effects (Often Mild & Reversible)
Visual Disturbances (Very Common but Usually Harmless)
-
Blurred vision
-
Altered colour perception
-
Light sensitivity
-
“Wavy” vision
These typically:
-
Occur within 30–60 minutes of dosing
-
Last less than an hour
-
Reduce over time
Patients should avoid night driving initially until they understand their response.
Photosensitivity
-
Increased sensitivity to sunlight
-
Sunburn risk
-
Long-term risk of skin damage with prolonged therapy
Sun protection is important.
Gastrointestinal
-
Nausea
-
Abdominal discomfort
5️⃣ Less Common but Important Effects
Neurological
-
Headache
-
Vivid dreams
-
Hallucinations (usually at high levels)
-
Confusion (dose-related)
These are generally reversible with dose adjustment.
Liver Abnormalities
Routine liver function monitoring is required.
Most abnormalities are mild and resolve with dose modification.
Cardiac Effects
Voriconazole can prolong the QT interval.
Caution in patients with:
-
Known arrhythmias
-
Electrolyte imbalance
-
Other QT-prolonging drugs
ECG monitoring may be appropriate in higher-risk patients.
Skin Cancer Risk (Long-Term Use)
With prolonged use (especially >1–2 years):
-
Increased risk of skin squamous cell carcinoma
-
Particularly in transplant recipients
Sun protection and dermatology review are advised for long-term therapy.
6️⃣ Food & Drug Advice
-
Avoid grapefruit
-
Avoid St John’s Wort
-
Take tablets at least 1 hour before or after meals (food reduces absorption)
Voriconazole has many CYP-mediated interactions and requires careful medication review.
7️⃣ Comparison With Itraconazole (Simple Overview)
| Feature | Itraconazole | Voriconazole |
|---|---|---|
| Absorption variability | High | More predictable |
| Visual side effects | Rare | Common but mild |
| Photosensitivity | Rare | More common |
| QT prolongation | Minimal | Possible |
| TDM needed | Yes | Yes (essential) |
Balanced Summary for Patients
Voriconazole is a strong antifungal used when more reliable or potent treatment is needed. Most side effects are manageable and reversible, and blood monitoring keeps treatment safe.
Clinician Checklist
-
Confirm indication and prior azole exposure
-
Check baseline LFTs
-
Review ECG if cardiac risk present
-
Assess drug interactions (CYP2C19, 2C9, 3A4)
-
Arrange trough level at day 5–7
-
Counsel regarding visual symptoms and sun protection