Exercise and Aspergillosis: How Physical Activity Can Improve Breathing, Strength and Wellbeing
Key points
- Exercise is one of the most helpful non-drug tools for many people living with aspergillosis.
- Regular physical activity can improve breathlessness, strength, stamina, mood, confidence and quality of life.
- The best approach is usually little and often, rather than occasional intensive exercise.
- Do not compare yourself with others. Everyone has different lungs, treatments, fitness levels and limits.
- Respiratory physiotherapists and pulmonary rehabilitation programmes can help you exercise safely and confidently.
- Walking, cycling, swimming, rowing, gentle yoga, Tai Chi and singing can all be useful, depending on the individual.
- People with aspergillosis should take extra care around mould-heavy environments such as compost, leaf mould, sheds and building dust.
Contents
- Why exercise matters in aspergillosis
- The activity and breathlessness cycle
- Benefits of exercise
- Specific issues for aspergillosis patients
- How to start safely
- Activities that may help
- Pulmonary rehabilitation and physiotherapy
- The golden rule: little and often
- What clinicians want patients to know
- Real-life examples
- When to seek medical advice
- Frequently asked questions
- Related articles and further support
Why exercise matters in aspergillosis
Living with aspergillosis can be physically and emotionally challenging. Breathlessness, coughing, fatigue, disturbed sleep, medication side effects and reduced confidence can all make it tempting to become less active.
Unfortunately, becoming less active can make symptoms feel worse over time. Muscles weaken, fitness falls, balance may worsen and everyday activities such as walking, climbing stairs, shopping or playing with grandchildren can become harder.
This process is often called deconditioning. It does not mean the symptoms are imaginary. It means the body has lost some of its ability to cope with activity.
The encouraging news is that exercise can help reverse part of this process.
Exercise cannot cure aspergillosis, but it can help the body use oxygen more efficiently, strengthen muscles, improve confidence and make daily life easier.
Importantly, people may feel better and do more even when their lung function tests do not change very much.
The activity and breathlessness cycle
Many people with chronic lung disease become trapped in a difficult cycle:
The deconditioning cycle
Breathlessness → Less activity → Loss of fitness → More breathlessness → Even less activity
Exercise helps by creating a healthier cycle:
The rebuilding cycle
Gentle activity → Stronger muscles → More confidence → Easier daily tasks → Better quality of life
This is why small, regular activity can be so powerful. The aim is not to force the lungs to work harder. The aim is to help the whole body work better.
Benefits of exercise
Improved breathlessness
Exercise may make you breathless while you are doing it, but regular activity often reduces breathlessness during everyday tasks. This happens because muscles become stronger and more efficient, so they need less effort to perform the same activity.
More energy
Many patients report feeling less tired once they build a regular routine. Exercise uses energy in the short term, but over time it can improve stamina and reduce the effort needed for daily life.
Stronger muscles
Long-term illness, hospital admissions, inactivity and corticosteroid treatment can all contribute to muscle weakness. Strength exercises can help rebuild leg strength, improve balance and support independence.
Better mood and confidence
Living with aspergillosis can affect mental wellbeing. Exercise can help reduce anxiety, stress and low mood. It can also restore a sense of control and achievement.
Improved bone health
This is especially important for people who have taken long-term corticosteroids. Weight-bearing activity and strength training can help protect bone strength and reduce the risk of osteoporosis.
Better daily function
For many patients, the most important benefit is practical: being able to walk further, climb stairs more easily, go shopping, travel, garden, socialise or enjoy family life with more confidence.
Specific issues for aspergillosis patients
Avoiding high mould exposure
Aspergillus is commonly found in soil, compost, decaying vegetation, damp buildings and dust. Some activities can expose people to large numbers of fungal spores.
Activities that may increase exposure include:
- Handling compost
- Turning soil
- Clearing leaf piles
- Wood chipping
- Spreading bark or mulch
- Cleaning sheds, garages, lofts or basements
- Working around mouldy materials
- Construction or demolition environments
Outdoor exercise such as walking, cycling and running is generally encouraged. However, it is sensible to avoid places where mould, compost, dust or decaying vegetation are being heavily disturbed.
Some people may choose to wear a well-fitting FFP2 or FFP3 mask for unavoidable dusty or mould-heavy tasks, but avoidance is usually better where possible.
Haemoptysis: coughing blood
People with Chronic Pulmonary Aspergillosis (CPA), lung cavities or aspergillomas may sometimes cough blood. This is called haemoptysis.
If you have recent, recurrent or significant haemoptysis, discuss exercise with your respiratory team. Most routine activity remains safe for many people, but vigorous exertion may need to be paused or modified during periods of active bleeding.
Oxygen levels
Some people with aspergillosis also have bronchiectasis, Chronic Obstructive Pulmonary Disease (COPD), fibrosis, previous tuberculosis damage or other lung scarring. In these situations, oxygen levels may fall during exertion even when resting oxygen levels are normal.
If breathlessness feels out of proportion, or if you notice unusually low oxygen saturations during activity, discuss this with your respiratory team. You may benefit from an exercise assessment or pulmonary rehabilitation referral.
Fatigue and boom-and-bust activity
Aspergillosis-related fatigue can be different from normal tiredness. It may be influenced by chronic inflammation, active infection, poor sleep, anxiety, medication side effects and reduced fitness.
Many patients experience a boom-and-bust pattern:
Good day → Do too much → Several days recovering
Regular, steady activity is usually more helpful than occasional bursts of intensive effort.
Steroid-related muscle weakness
People who have taken long-term corticosteroids may develop muscle weakness, particularly around the thighs and hips. This can make standing from a chair, climbing stairs and walking uphill more difficult.
Strength exercises such as sit-to-stands, step-ups and resistance band work can be particularly helpful.
Adrenal insufficiency
Some patients who have used long-term corticosteroids develop adrenal insufficiency. These patients should understand their sick day rules and discuss unusually strenuous exercise, endurance events or major hikes with their healthcare team.
Most routine gentle or moderate exercise is safe, but unusually demanding activity may require additional planning.
Asthma, ABPA and exercise symptoms
Many people with Allergic Bronchopulmonary Aspergillosis (ABPA) also have asthma. Exercise can sometimes trigger wheeze, cough or chest tightness.
This does not usually mean exercise should be avoided. Good asthma control, appropriate inhaler use, gradual warm-up and pacing can make a major difference. Speak to your healthcare team if exercise regularly triggers asthma symptoms.
How to start safely
Start from where you are
Your starting point is your starting point. It does not matter what someone else can do. If you can only walk for two or three minutes, that is still a valid place to begin.
Use the talk test
During moderate exercise, you should usually be able to speak in short sentences. If you cannot speak at all, you may be pushing too hard.
Build gradually
Small increases are usually safer and more sustainable than sudden changes. For example, increasing a walk from five minutes to six or seven minutes may be more helpful than trying to double it immediately.
Plan rest periods
Rest is not failure. Many people with lung disease do better with short bursts of activity separated by planned rests.
Track progress gently
Some patients find it motivating to keep a simple record of walks, steps, strength exercises or how breathless they feel. The aim is encouragement, not pressure.
A simple beginner example
Example starter plan
- Week 1–2: Walk for 5 minutes most days, or less if needed.
- Week 3–4: Add one or two minutes when comfortable.
- Week 5–6: Add gentle strength exercises, such as sit-to-stands.
- Ongoing: Continue gradual increases, with rest days when needed.
This is only an example. Some people will need to start lower, while others may safely start higher.
Activities that may help
The best exercise is usually the one you enjoy and can keep doing regularly.
Walking
Walking is one of the simplest and most effective activities. It requires no special equipment, can be adapted to most fitness levels and is easy to build gradually.
Cycling
Cycling, including use of a stationary exercise bike, can improve stamina while placing less strain on the joints than running.
Swimming
Swimming can be helpful because the water supports body weight. However, some people with asthma find chlorinated pools trigger symptoms.
Rowing
Rowing machines can provide both cardiovascular and strength benefits. Start gently and focus on technique.
Strength training
Strength training does not have to mean heavy weights. Useful exercises may include:
- Sit-to-stands from a chair
- Step-ups
- Wall push-ups
- Resistance bands
- Light hand weights
Gentle yoga and Tai Chi
Many patients enjoy gentle yoga or Tai Chi because they combine movement, balance, breathing awareness, posture and relaxation. Chair-based versions may be useful for people with reduced mobility.
Singing
Singing may not sound like exercise, but many people with lung conditions find it helpful. It can support breathing control, posture, confidence, social connection and respiratory muscle coordination.
Some patients enjoy local choirs or Singing for Lung Health groups.
Pulmonary rehabilitation and physiotherapy
You do not have to do this alone.
A respiratory physiotherapist can help assess your current ability and design a programme that suits your symptoms, fitness level and goals.
A specialist physiotherapist may help with:
- Breathlessness management
- Pacing strategies
- Strength and stamina building
- Airway clearance techniques where appropriate
- Confidence around movement
- Safe return to activity after illness
Pulmonary rehabilitation
Pulmonary rehabilitation is a structured programme that usually combines supervised exercise, education, breathing techniques and self-management advice.
Many people with chronic lung disease describe pulmonary rehabilitation as one of the most helpful interventions they have received.
If you have ongoing breathlessness, reduced exercise tolerance or loss of confidence, ask your GP, respiratory consultant, specialist nurse or physiotherapist whether pulmonary rehabilitation may be suitable for you.
The golden rule: little and often
Exercise with aspergillosis: the golden rule
Little and often is usually better than a lot all at once.
Do not compare yourself with other people, including other aspergillosis patients.
Everyone has different lungs, different treatments, different ages and different levels of fitness.
Focus on your own starting point and your own progress.
Do not try to keep up with others. You do you.
One of the biggest traps is comparing yourself with other patients. Someone else may complete a long-distance walk, climb a mountain, run a race or cycle hundreds of miles. That can be inspiring, but it should not become your target.
Instead, ask yourself:
Am I a little stronger, fitter or more confident than I was a few months ago?
Success may mean:
- Walking for five minutes when previously you could only manage three
- Climbing stairs more comfortably
- Shopping with less breathlessness
- Doing light gardening safely
- Enjoying a holiday more easily
- Playing with children or grandchildren
- Needing fewer rests during ordinary daily tasks
These achievements matter.
For most people living with aspergillosis, consistency beats intensity.
What clinicians want patients to know
Exercise is not about pushing through at all costs
Healthcare professionals usually want patients to remain as active as safely possible, but that does not mean ignoring symptoms or forcing yourself to keep up with others.
The safest approach is usually to build gradually, pace yourself and ask for help when symptoms change.
Exercise should support your life, not punish your body.
Real-life examples
The person who walks five minutes a day
For someone recovering from illness or a hospital admission, a five-minute daily walk may be a major achievement. If that becomes six minutes, then eight minutes, that is progress.
The person who completes a long-distance walk
Some people with aspergillosis manage major challenges such as long-distance walking routes. These stories can be inspiring, but they are not a standard everyone else must meet.
The person who joins a singing group
For some patients, a singing group may be more enjoyable and sustainable than a gym. Singing can support breathing control and confidence while also providing social contact.
The person who returns to gardening carefully
Gardening can be enjoyable and active, but compost, leaf mould and disturbed soil may contain high levels of fungal spores. Some patients adapt by avoiding compost handling, asking for help with mould-heavy tasks, wearing protective masks where appropriate, and choosing lower-risk gardening activities.
When to seek medical advice
Stop exercising and seek medical advice if you experience:
- Chest pain
- Severe or unusual breathlessness
- Dizziness or fainting
- Significant haemoptysis, meaning coughing blood
- Sudden worsening of symptoms
- New palpitations or heart rhythm symptoms
- Oxygen levels much lower than usual, if you monitor them
- Exercise tolerance that suddenly falls without an obvious reason
Always speak to your healthcare team if you are unsure whether exercise is safe for you, especially if your symptoms have recently changed.
Frequently asked questions
Can I exercise if I have aspergillosis?
Yes, many people with aspergillosis benefit from regular physical activity. Exercise should be adapted to your symptoms, fitness level and medical conditions. Ask your healthcare team for advice if you have severe breathlessness, recent haemoptysis or unstable symptoms.
Can exercise improve breathlessness?
Yes. Exercise can improve muscle efficiency, stamina and confidence. This can reduce breathlessness during everyday activities, even if lung function test results do not change significantly.
What is the best exercise for Allergic Bronchopulmonary Aspergillosis?
There is no single best exercise for Allergic Bronchopulmonary Aspergillosis. Walking, cycling, swimming, gentle yoga, strength training and pulmonary rehabilitation can all be helpful. The best activity is one you can do safely and regularly.
Can pulmonary rehabilitation help aspergillosis patients?
Many people with chronic respiratory symptoms, bronchiectasis or reduced exercise tolerance benefit from pulmonary rehabilitation. It combines supervised exercise, education, breathing techniques and self-management support.
Should people with aspergillosis avoid gardening?
Not necessarily, but some gardening activities can expose people to high levels of Aspergillus spores. Handling compost, turning soil, clearing leaves and working with mulch may carry higher exposure. Lower-risk gardening activities may be more suitable for some patients.
Can exercise help steroid-related muscle weakness?
Yes. Strength exercises can help rebuild muscle strength lost through long-term corticosteroid treatment, illness or inactivity. Simple exercises such as sit-to-stands, step-ups and resistance bands can be useful.
Is singing useful for people with lung disease?
Many people with lung disease find singing helpful for breathing control, posture, confidence and social connection. Some areas offer Singing for Lung Health groups.
Should I exercise when I am tired?
Gentle movement may help on some tired days, but severe fatigue may mean your body needs rest. Pacing is important. Try to avoid repeated boom-and-bust cycles where you do too much on a good day and then need several days to recover.
Take-home message
Exercise is one of the most powerful tools available to help people living with aspergillosis maintain independence, strength and quality of life.
Move more, but move at your own pace.
Find something you enjoy.
Ask for help when you need it.
Little and often beats heroic efforts.
Do not compare yourself with others.
You do you.
Related articles
You may also find these aspergillosis.org articles helpful:
- Why Am I Breathless When My Oxygen Levels Are Normal?
- Physiotherapy for Aspergillosis
- Living with Aspergillosis
- Managing Fatigue in Aspergillosis
- Steroids and Adrenal Insufficiency
- Bronchiectasis and Aspergillosis
- What is Allergic Bronchopulmonary Aspergillosis (ABPA)?
- What is Chronic Pulmonary Asprgillosis (CPA)?
Further support and information
Author and review information
Author: Graham Atherton, National Aspergillosis Centre
Medical review: National Aspergillosis Centre Clinical Team
Last reviewed: June 2026
This article provides general information and should not replace advice from your own healthcare team.
Physiotherapy for Aspergillosis: Breathing, Mucus Clearance and Keeping Active
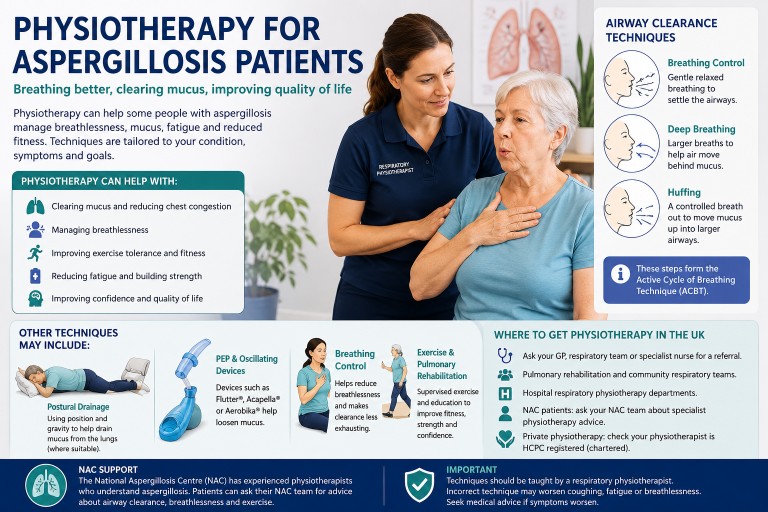
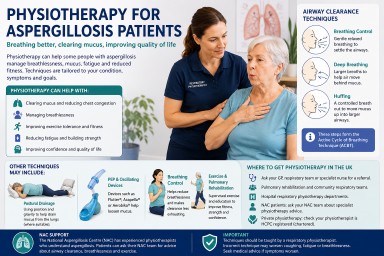
Physiotherapy can be an important part of supportive care for some people living with aspergillosis. It does not treat the fungal infection itself, but it can help with breathlessness, mucus clearance, strength, fitness, posture, fatigue and confidence with activity.
This may be especially helpful for people with Chronic Pulmonary Aspergillosis (CPA), Allergic Bronchopulmonary Aspergillosis (ABPA), Severe Asthma with Fungal Sensitisation (SAFS), Aspergillus bronchitis, bronchiectasis, asthma, Chronic Obstructive Pulmonary Disease (COPD), or lung damage from previous infection.
Key points
- Physiotherapy can help some aspergillosis patients manage mucus, breathlessness and reduced activity.
- Airway clearance techniques may be useful when mucus is difficult to clear.
- The Active Cycle of Breathing Technique (ACBT) is commonly used in respiratory physiotherapy.
- Other approaches include huffing, breathing control, postural drainage, airway clearance devices, exercise training and pulmonary rehabilitation.
- Technique matters — airway clearance should ideally be taught by a respiratory physiotherapist.
- National Aspergillosis Centre (NAC) patients can ask for advice from experienced physiotherapists who understand aspergillosis.
Contents
- Why physiotherapy matters in aspergillosis
- Airway clearance and mucus management
- Active Cycle of Breathing Technique (ACBT)
- Other physiotherapy techniques
- Pulmonary rehabilitation and exercise
- Breathing retraining and breathlessness
- Where to get physiotherapy in the UK
- Useful NHS videos and guides
- When to seek medical advice
Why physiotherapy matters in aspergillosis
Many people with aspergillosis have underlying lung conditions that affect how the lungs clear mucus, expand during breathing and cope with exertion. Long-term illness can also lead to muscle weakness, reduced fitness and loss of confidence with activity.
Common problems include:
- thick or persistent mucus
- frequent coughing
- breathlessness on exertion
- fatigue
- reduced walking distance
- weakness after illness or hospital admission
- poor posture from chronic breathlessness or coughing
- anxiety around breathing
- dysfunctional breathing patterns
Physiotherapy aims to improve function and quality of life. It is often most useful when it is personalised to the patient’s lung condition, symptoms, fitness level and treatment plan.
Airway clearance and mucus management
Some people with aspergillosis produce mucus every day. This is particularly common in people who also have bronchiectasis, asthma, Aspergillus bronchitis or repeated chest infections.
Mucus that remains in the lungs can contribute to:
- blocked or narrowed airways
- more coughing
- chest tightness
- breathlessness
- fatigue
- recurrent infections
Respiratory physiotherapists can teach airway clearance techniques to help move mucus from smaller airways towards larger airways, where it can be cleared more easily by huffing or coughing.
Active Cycle of Breathing Technique (ACBT)
ACBT stands for Active Cycle of Breathing Technique. It is one of the most commonly used airway clearance methods in respiratory physiotherapy.
It usually includes three parts:
- Breathing control – gentle relaxed breathing to settle the airways.
- Deep breathing exercises – larger breaths to help air move behind mucus.
- Huffing – a controlled breath out through an open mouth to move mucus upwards.
ACBT can often be adapted depending on symptoms, oxygen levels, energy, breathlessness and the amount of mucus being produced.
Other physiotherapy techniques
Huffing
A huff is a controlled breath out through an open mouth and throat. It can move mucus without the effort of repeated hard coughing. Many patients find huffing less exhausting than forceful coughing.
Postural drainage
Postural drainage uses body position and gravity to help drain mucus from different parts of the lungs. It may not be suitable for everyone, especially people with reflux, severe breathlessness, frailty, oxygen requirements or certain heart and lung complications.
Positive Expiratory Pressure and oscillating devices
Some patients may be advised to use airway clearance devices such as Flutter®, Acapella® or Aerobika®. These devices create resistance or vibration during breathing out, helping to loosen mucus and keep the airways open.
Breathing control
Breathing control can help settle the breathing pattern, reduce panic during breathlessness and make airway clearance less tiring.
Posture and mobility work
Chronic coughing and breathlessness can affect posture. Physiotherapy may include stretching, shoulder mobility, chest wall movement, gentle strengthening and exercises to improve comfort when breathing.
Fatigue management and pacing
Fatigue is common in aspergillosis. Physiotherapists may help patients pace activities, avoid “boom and bust” patterns, and gradually rebuild function without triggering prolonged exhaustion.
Pulmonary rehabilitation and exercise
Pulmonary rehabilitation is a structured programme of exercise and education for people with long-term lung disease who experience breathlessness. NHS England describes pulmonary rehabilitation as an exercise and education programme for people with lung disease who have symptoms of breathlessness.
Programmes may include:
- supervised exercise
- walking or cycling
- strength training
- breathing advice
- education about managing long-term lung disease
- confidence-building around activity
For aspergillosis patients, pulmonary rehabilitation may be particularly useful when breathlessness, weakness or reduced activity are affecting daily life.
Breathing retraining and breathlessness
Some people feel very breathless even when oxygen levels are normal or near normal. This can happen because breathlessness is influenced by airway inflammation, muscle effort, anxiety, breathing pattern, air trapping and the brain’s perception of breathing discomfort.
Breathing retraining may include:
- slower, calmer breathing
- diaphragmatic breathing
- pursed-lip breathing
- relaxation techniques
- coordinating breathing with walking, stairs or other activity
These techniques can be especially useful for patients who feel frightened by breathlessness or who have developed an inefficient breathing pattern.
Where to get physiotherapy in the UK
Access to physiotherapy varies across the UK, but patients with long-term lung disease may be able to obtain support through several routes.
1. Through your GP or respiratory team
Your GP, respiratory consultant, specialist nurse or hospital team may be able to refer you to a respiratory physiotherapist, community respiratory team or pulmonary rehabilitation service.
2. Through pulmonary rehabilitation services
Many local NHS pulmonary rehabilitation services accept referrals for people with chronic respiratory disease, including conditions such as Chronic Obstructive Pulmonary Disease (COPD), bronchiectasis, asthma, interstitial lung disease and other long-term breathing problems. Some services accept GP referrals, hospital referrals or self-referrals, but criteria vary locally.
3. Through community respiratory teams
Some areas have community respiratory teams that provide assessment, education, pulmonary rehabilitation, breathlessness support, oxygen-related advice and airway clearance support.
4. Through hospital respiratory physiotherapy departments
Hospital respiratory physiotherapists often support patients during admissions, after exacerbations, or through specialist outpatient respiratory clinics.
5. Through the National Aspergillosis Centre
National Aspergillosis Centre (NAC) patients can ask their NAC team whether specialist physiotherapy advice would be helpful. NAC has experienced physiotherapists who understand aspergillosis and the particular problems patients may face, including mucus clearance, breathlessness, fatigue, reduced fitness and co-existing lung disease.
6. Private physiotherapy
Some patients choose to see a private physiotherapist. The NHS advises that private physiotherapists should be chartered and registered with the Health and Care Professions Council (HCPC). The Chartered Society of Physiotherapy provides a “Find a Physio” directory that can be searched by location and specialty.
Useful UK links:
- National Aspergillosis Centre Physiotherapy
- NHS: Physiotherapy
- NHS England: Pulmonary rehabilitation
- Chartered Society of Physiotherapy: Find a physiotherapist
- Association of Chartered Physiotherapists in Respiratory Care
Useful NHS videos and guides
The following NHS resources may help patients understand airway clearance techniques. They should not replace individual advice from a respiratory physiotherapist.
Royal Free London NHS Foundation Trust – Active Cycle of Breathing
A clear patient-focused demonstration of ACBT.
Watch: Active Cycle of Breathing – Royal Free London NHS Foundation Trust
NHS Greater Glasgow & Clyde – Active Cycle of Breathing
A detailed demonstration from respiratory physiotherapy services.
Watch: Respiratory Physiotherapy Service – Active Cycle of Breathing
University College London Hospitals NHS Foundation Trust – breathing and airway clearance videos
UCLH has a useful set of patient information videos covering breathing exercises and airway clearance.
Watch: UCLH patient information videos – breathing exercises
UCLH – How to clear phlegm from your chest
A short, practical NHS video explaining how ACBT can help clear phlegm.
Watch: How to clear phlegm from your chest – ACBT
Cambridge University Hospitals NHS Foundation Trust
A patient information page explaining airway clearance and ACBT.
Read: Airway clearance – Active Cycle of Breathing Technique
Hull University Teaching Hospitals NHS Trust
A detailed patient leaflet on ACBT as a secretion clearance technique.
Read: Active Cycle of Breathing Technique – secretion clearance
University Hospitals Plymouth NHS Trust
A step-by-step patient guide to breathing control, thoracic expansion exercises and huffing.
Read: Active Cycle of Breathing Technique
When to seek medical advice
Airway clearance techniques should ideally be taught by a respiratory physiotherapist. Incorrect technique may sometimes worsen coughing, fatigue, airway irritation or breathlessness.
Seek medical advice urgently if you develop:
- new or worsening coughing of blood
- sudden worsening breathlessness
- chest pain
- fever or signs of infection
- dizziness or fainting
- significant oxygen desaturation
- rapid deterioration after starting a new exercise or airway clearance routine
Summary
Physiotherapy can be an important supportive treatment for some people with aspergillosis. It may help with mucus clearance, breathlessness, posture, fatigue, strength, confidence and activity levels.
Techniques such as ACBT, huffing, breathing control, postural drainage, airway clearance devices and pulmonary rehabilitation can all help selected patients. The best approach depends on the person’s symptoms, underlying lung condition and overall health.
For NAC patients, specialist physiotherapy advice is available from professionals experienced in aspergillosis care. If mucus clearance, breathlessness or reduced activity are becoming difficult, it is worth asking the NAC team whether physiotherapy input may help.
Medical note: This article is for general information only. It does not replace advice from your doctor, specialist nurse or respiratory physiotherapist. Airway clearance and exercise plans should be tailored to the individual patient.
Last reviewed: May 2026
When Breathlessness Feels Severe — Even When Oxygen Levels Look “Normal”

Many people living with aspergillosis, severe asthma, bronchiectasis, or other chronic lung conditions describe a confusing and sometimes frightening experience:
“My oxygen saturations are normal, my peak flow is reasonable, there’s little wheeze, but I still feel like I’m drowning.”
This can be distressing for patients and frustrating for carers. Some people feel that because their oxygen levels or breathing tests appear “acceptable”, their symptoms are not fully understood.
Importantly, severe breathlessness can occur even when standard measurements such as oxygen saturations and peak flow readings appear relatively normal.
This does not mean the symptoms are imaginary or “all in the mind”. Breathlessness is complex and can have many different causes.
Why Breathlessness Is More Complicated Than Oxygen Levels
When doctors or nurses assess breathing problems, they often check:
- Oxygen saturation levels (sats)
- Peak flow readings
- Respiratory rate
- Presence of wheeze
- Chest sounds
These are all important. However, they do not always reflect how breathless a person feels.
Some people with chronic respiratory illness may have:
- Normal oxygen saturations
- Reasonable peak flow readings
- Little visible wheeze
- Minimal mucus production
…yet still experience intense sensations of:
- air hunger
- tight chest
- difficulty taking a satisfying breath
- feeling unable to “fill the lungs”
- panic associated with breathing
- extreme fatigue from breathing effort
What Can Cause This?
Breathlessness in aspergillosis and chronic lung disease is often caused by several factors happening together.
Inflammation and Airway Sensitivity
Conditions such as Allergic Bronchopulmonary Aspergillosis (ABPA), Severe Asthma with Fungal Sensitisation (SAFS), bronchiectasis, and Chronic Pulmonary Aspergillosis (CPA) can all cause inflamed and hypersensitive airways.
The lungs may feel irritated or tight even if oxygen exchange remains relatively preserved.
Small Airways Dysfunction
Some breathing problems occur in the smaller airways of the lungs and may not always show clearly on basic tests such as peak flow.
Patients can feel significant chest tightness or air trapping despite “good numbers”.
Muscle Fatigue
Breathing takes muscular effort. Chronic respiratory illness can place a long-term strain on the chest wall and breathing muscles, leading to exhaustion and increased awareness of breathing.
Mucus and Airflow Changes
Even relatively small amounts of mucus or airway narrowing can create sensations of chest heaviness or difficulty moving air.
Breathing Pattern Dysfunction (Dysfunctional Breathing)
This is increasingly recognised in people with chronic respiratory illness.
When breathing becomes difficult over months or years, people may unconsciously develop altered breathing patterns, including:
- rapid shallow breathing
- upper chest breathing
- frequent sighing
- over-breathing (hyperventilation)
- muscle tension around the chest and neck
This can worsen symptoms and create a vicious cycle where the sensation of breathlessness becomes amplified.
Symptoms may include:
- air hunger
- dizziness
- tingling
- tight chest
- panic sensations
- difficulty “switching off” breathing awareness
Importantly, this does not mean the illness is psychological or “not real”. Dysfunctional breathing can happen alongside genuine lung disease.
Why Inhalers Sometimes Seem to Help Less
Reliever inhalers such as salbutamol (Ventolin) are designed mainly to relax tightened airways.
If breathlessness is being driven partly by breathing pattern dysfunction, muscle fatigue, inflammation, hypersensitivity, or air trapping, inhalers may not always provide dramatic relief.
This can be confusing and upsetting for patients.
“But My Tests Are Normal…”
Many patients feel frustrated, frightened, or even dismissed when told that oxygen levels, peak flow readings, or chest examinations are “fine” despite severe breathlessness.
Normal oxygen saturations are reassuring in terms of immediate danger, but they do not always reflect the full experience of chronic respiratory illness.
Breathlessness is influenced by many factors including inflammation, airway sensitivity, breathing effort, muscle fatigue, anxiety associated with struggling to breathe, and altered breathing patterns.
Because of this, some people may feel profoundly breathless even when routine measurements appear relatively stable.
It can sometimes help to explain symptoms in practical, functional terms, such as:
- “I become breathless walking across the room.”
- “I recover much more slowly than usual.”
- “This feels much worse than my normal baseline.”
- “I feel exhausted by the effort of breathing.”
- “Breathing exercises seem to help settle things.”
These descriptions may help healthcare professionals understand how symptoms are affecting day-to-day life, rather than focusing only on oxygen levels or peak flow numbers.
Some patients also find it helpful to ask questions such as:
- Could breathing pattern dysfunction be contributing?
- Would respiratory physiotherapy help?
- Would pulmonary rehabilitation be appropriate?
- How should I judge when symptoms need urgent assessment?
Importantly, severe breathlessness should never simply be ignored. New, worsening, or unusual symptoms still require proper medical assessment.
At the same time, many people with chronic lung disease experience very real symptoms that are not always fully reflected by routine measurements alone.
Why Breathlessness Can Feel So Frightening
The sensation of breathlessness is created by the brain interpreting signals from the lungs, breathing muscles, chest wall, blood chemistry, and nervous system.
This means that the feeling of “not getting enough air” is not determined only by oxygen levels.
In chronic lung disease, several things can trigger the sensation of breathlessness, including:
- inflamed or sensitive airways
- extra effort needed to move air in and out
- air trapping in the lungs
- muscle fatigue
- rapid or shallow breathing
- stress hormones released during breathing distress
- heightened awareness of breathing sensations
When breathing becomes uncomfortable, the body naturally responds with anxiety and adrenaline. This is a protective survival response.
Unfortunately, this can sometimes create a cycle:
breathlessness → anxiety → faster breathing → more chest tightness → worse breathlessness
This does not mean symptoms are “psychological”. The physical sensation is real, but the body’s alarm systems can unintentionally amplify it.
What Can Help During an Episode of Breathlessness?
Different techniques help different people, and severe or rapidly worsening symptoms should always be medically assessed. However, some patients find the following approaches helpful during episodes of distressing breathlessness:
Slow the Breathing Rate
Trying to slow breathing gently can help reduce over-breathing and chest tightness.
Some people find it helpful to:
- breathe in gently through the nose
- breathe out slowly through pursed lips
- focus on making the out-breath longer than the in-breath
Use a Recovery Position
Sitting forward slightly with the arms supported on knees or a table can sometimes reduce the work of breathing.
Reduce Panic and “Air Hunger”
Trying to fight for bigger and bigger breaths can sometimes worsen symptoms.
Some patients find it more helpful to focus on:
- gentle breathing rhythm
- relaxing the shoulders and neck
- slowing breathing rather than deepening it
- focusing attention away from the chest where possible
Use Prescribed Treatments Appropriately
Follow the advice provided by your healthcare team regarding inhalers, nebulisers, airway clearance, or rescue medication.
If inhalers are not helping as expected, this should be discussed with a respiratory specialist rather than simply increasing use repeatedly.
Know Your “Usual” Pattern
Many patients find it useful to learn the difference between:
- their “usual” chronic breathlessness
- breathing pattern dysfunction or over-breathing episodes
- symptoms suggesting infection or acute deterioration
This can help patients feel more confident recognising when urgent medical assessment may be needed.
Can Breathing Retraining Help?
Some patients find breathing retraining exercises very helpful, especially when guided by:
- respiratory physiotherapists
- specialist breathing services
- pulmonary rehabilitation teams
- asthma nurse specialists
Breathing retraining may include:
- slowing breathing rate
- diaphragmatic (“belly”) breathing
- nasal breathing techniques
- recovery breathing positions
- relaxation techniques
- paced activity and pacing strategies
Some NHS respiratory teams recommend online breathing resources and guided exercises to help patients recognise and manage over-breathing patterns.
These approaches are usually intended to work alongside medical treatment — not instead of it.
Living With an “Invisible” Symptom
One of the hardest aspects of chronic breathlessness is that outward signs may not always match how severe symptoms feel internally.
Many patients report feeling dismissed when oxygen levels are normal or when tests appear “better than expected”.
The experience of breathlessness is real, even when routine measurements do not fully explain it.
This is one reason why specialist respiratory assessment can be important in complex conditions such as aspergillosis.
When to Seek Medical Help
You should seek urgent medical advice if breathlessness is:
- suddenly worsening
- associated with chest pain
- causing blue lips or fingertips
- associated with falling oxygen saturations
- accompanied by fever or signs of infection
- causing confusion or severe exhaustion
- significantly different from your usual symptoms
Even if previous episodes have been related to breathing pattern dysfunction, new or worsening symptoms should still be medically assessed.
Further Support
You may also find these resources helpful:
Last reviewed: May 2026
Produced by: National Aspergillosis Centre CARES Team / Aspergillosis Website
Airways mucus and aspergillosis
A clear, patient-friendly explainer
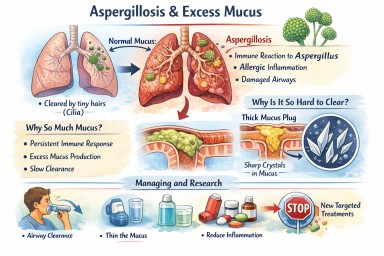
People living with aspergillosis often say that mucus is one of the hardest symptoms to manage — thick sputum, coughing fits, plugs that feel “stuck”, and flare-ups that seem to come out of nowhere. This explainer brings everything together in one place: what mucus is for, why aspergillosis causes so much of it, why it becomes abnormal, and what current and future treatments aim to do.
1. What is airway mucus and why do we need it?
Mucus is normal, healthy, and essential. Everyone produces it all the time.
Its main roles are to:
-
Trap inhaled particles (dust, spores, bacteria, pollution)
-
Protect the airway lining from drying and irritation
-
Support the immune system
-
Clear the lungs, using tiny moving hairs (cilia) that sweep mucus upwards so it can be swallowed or coughed out
(this clearance system is called the mucociliary escalator)
In healthy lungs:
-
Mucus is thin
-
Produced in small amounts
-
Cleared without you noticing it
2. Why aspergillosis causes excessive mucus
In aspergillosis, the lungs are under ongoing stress. Several factors combine:
Persistent immune activation
The immune system keeps reacting to Aspergillus material in the airways. Even when the fungus is controlled, inflammation can persist.
Allergic-type inflammation (especially in ABPA)
Allergic immune responses strongly stimulate mucus-producing cells, leading to:
-
Large volumes of mucus
-
Very sticky or rubbery sputum
Airway damage
Conditions commonly associated with aspergillosis (such as bronchiectasis or long-standing asthma) cause:
-
Widened or damaged airways
-
Poor mucus clearance
-
Pools of mucus that are hard to shift
Slowed clearance
Inflammation and infection impair cilia, so mucus:
-
Moves more slowly
-
Sits in the lungs longer
-
Becomes thicker and harder to clear
➡️ What starts as a protective response becomes a self-perpetuating problem.
3. Why thick mucus causes symptoms
Excess or abnormal mucus can:
-
Block airways → breathlessness and wheeze
-
Trigger coughing → especially overnight or on waking
-
Trap infection → repeated flare-ups
-
Reduce oxygen exchange
-
Increase fatigue and chest discomfort
Many patients describe it as:
“Glue-like”, “stringy”, “rubbery”, or “impossible to move”
4. Mucus plugs and crystals – why some mucus is so hard to clear
Mucus plugs
When mucus becomes very thick, it can:
-
Form plugs that partially or completely block airways
-
Show up on CT scans
-
Worsen breathlessness suddenly
Charcot–Leyden crystals
In allergic and eosinophilic airway disease (including allergic bronchopulmonary aspergillosis):
-
Breakdown products of allergic immune cells can form microscopic crystals
-
These crystals make mucus:
-
Stiffer
-
More irritating
-
Harder to clear
-
Their presence is a sign of ongoing allergic inflammation, not infection alone.
5. Why managing mucus really matters
Mucus is not just an inconvenience. Poor mucus control can:
-
Increase infection risk
-
Drive repeated exacerbations
-
Worsen lung damage over time
-
Reduce quality of life and sleep
-
Increase hospital admissions
For aspergillosis, mucus management is core treatment, not optional.
6. What helps now (current approaches)
A. Thin the mucus
-
Good hydration
-
Nebulised saline (normal or hypertonic)
-
Selected mucolytic medicines (used carefully)
B. Move it out
-
Regular airway clearance physiotherapy
-
Breathing techniques (e.g. active cycle breathing)
-
Oscillating devices (flutter, Acapella, Aerobika)
-
Gentle, regular physical activity where possible
C. Reduce inflammation
-
Inhaled corticosteroids (when appropriate)
-
Oral steroids (used cautiously)
-
Biologic therapies for selected allergic or eosinophilic disease
-
Antifungal treatment when fungal burden is contributing
D. Treat infections early
-
Bacterial infections thicken mucus further
-
Prompt treatment reduces long-term damage
7. What research is doing differently (emerging therapies)
Research is moving beyond simply “loosening mucus”.
1. Reducing mucus production at source
Scientists are developing drugs that aim to:
-
Switch off excessive mucus secretion
-
Preserve normal protective mucus
This targets the mucus-producing cells directly.
2. Blocking the signals that drive over-production
Inflammation sends chemical signals telling airways to make more mucus. New treatments aim to:
-
Calm allergic and immune pathways
-
Prevent expansion of mucus-producing cells
Some current biologic therapies already reduce mucus indirectly; future drugs will be more precise.
3. Changing mucus structure
Instead of thinning everything, researchers are studying ways to:
-
Loosen the internal “mesh” of mucus
-
Prevent dense plugs from forming
-
Restore normal movement by cilia
4. Targeting mucus crystals
In allergic aspergillosis, research is exploring how to:
-
Reduce crystal formation
-
Calm the specific immune responses that create them
5. New inhaled and physical approaches
Early trials are testing:
-
Inhaled therapies designed to mobilise secretions
-
Treatments that improve airflow behind mucus plugs
6. Precision medicine
Future mucus treatments are likely to be:
-
Personalised
-
Based on inflammation type, fungal involvement, airway damage, and immune markers
Two people with aspergillosis may have very different mucus drivers — and need different solutions.
8. What this means for patients today
-
There is no single “anti-mucus cure” yet
-
Promising therapies are in research and early trials
-
Safety and long-term effects must be proven first
For now:
-
Regular airway clearance remains essential
-
Treating inflammation and infection promptly is crucial
-
Understanding why your mucus behaves as it does helps guide treatment
Key messages to remember
-
Mucus is normally protective
-
Aspergillosis turns a helpful system into a problem
-
Thick, sticky mucus reflects ongoing inflammation and airway damage
-
Crystals signal allergic involvement, not just infection
-
Research is moving toward preventing abnormal mucus formation, not just thinning it
Why do some people cough up long, tube-shaped pieces of mucus?
In several chronic lung conditions, the airways can become inflamed and produce thick mucus.
When this mucus sits in the bronchial tubes, it can sometimes harden into a cast shaped exactly like the airway.
People often describe these casts as:
-
long, ribbon-like or “snakeskin” pieces
-
rubbery or stretchy
-
white, yellow, or green
-
shaped like the inside of a tube
Coughing one up can feel dramatic but is usually a sign that your lungs are finally able to clear a blockage.
What does it mean if a cast has black flecks or dark spots?
This can look alarming, but several common, mostly harmless explanations exist.
1. Old or dried blood
Tiny amounts of bleeding from irritated airways can dry and turn:
red → brown → black
This often appears as tiny black dots or threads.
2. Inhaled particles
Dust, soot, pollution, or smoke can get trapped in mucus deeper in the lungs and show up as dark specks.
3. Debris from infection or inflammation
Long-standing inflammation can cause:
-
darkened mucus fragments
-
tiny bits of fungal, bacterial or biofilm material
-
oxidised (darkened) mucus layers
These often look like pepper-like flecks and are not dangerous on their own.
4. Oxidation or ageing of thick mucus
When mucus sits for a long time before it is coughed out, it can become darker in spots.
When this is usually not worrying
Black flecks are often harmless when:
-
the amount is small
-
the colour change is occasional
-
you feel better after coughing the cast out
-
there is no new increase in blood, fever, or breathlessness
-
this fits your usual pattern of mucus plugging
Most people with chronic airway disease experience occasional colour changes in mucus.
When to mention it to your doctor
You should let your team know if:
-
black flecks keep appearing repeatedly
-
you cough up more blood than usual
-
your breathing worsens suddenly
-
your sputum smells different
-
you have fever or chest pain
-
casts become bigger, more frequent, or harder to clear
These changes do not always mean something serious, but they are worth checking.
Why do casts form in the first place?
Conditions that can cause airway casts include:
-
Bronchiectasis
-
ABPA (Allergic Bronchopulmonary Aspergillosis)
-
Severe or eosinophilic asthma
-
Chronic infections, including fungal or bacterial
-
COPD with mucus hypersecretion
Inflammation makes mucus thicker, and narrowed airways make it harder to clear.
Over time, mucus can mould itself into the shape of the airway — becoming a cast.
What to do if you cough one up
-
Stay calm — this often brings relief.
-
Take note of its colour and size.
-
Hydrate well to thin mucus.
-
Continue your usual airway-clearance technique (physio, nebulisers, saline, etc.)
-
Let your team know if it is unusual for you.
Final reassurance
Coughing up a long, tube-like piece of mucus can feel shocking, but in most cases it simply means your lungs are clearing a blocked area.
Black flecks are usually:
-
old blood
-
trapped dust or soot
-
dried mucus debris
Most of the time, these findings are not dangerous, but they can give useful clues about airway inflammation.
Physiotherapy and Aspergillosis: Why It Matters
Physiotherapy is an important part of care for many people with aspergillosis, including allergic bronchopulmonary aspergillosis (ABPA), chronic pulmonary aspergillosis (CPA), aspergillus bronchitis, and severe asthma with fungal sensitisation (SAFS).
It doesn’t diagnose the disease on its own, but physiotherapists play a key role in detecting symptoms, collecting good sputum samples, and helping patients stay stable.
1. How Physiotherapy Helps With Diagnosis
🔍 A. Spotting patterns of sputum, breathlessness, and airway clearance problems
Respiratory physiotherapists often notice:
-
Thick, sticky mucus that is difficult to clear
-
Recurrent phlegm plugs
-
Wheeze, crackles, or airflow changes
-
Reduced ability to clear secretions after infection
These patterns can be early clues pointing toward ABPA, aspergillus bronchitis, or bronchiectasis linked to Aspergillus.
🔍 B. Supporting high-quality sputum collection
A good sputum sample is essential for:
-
Fungal culture
-
PCR
-
Galactomannan tests
-
Antibiotic/antifungal susceptibility testing
Techniques like huff coughing, breathing control, postural drainage, or using devices such as Acapella or Aerobika help ensure the sample comes from deep in the lungs, not just saliva.
🔍 C. Identifying airway collapsibility or dysfunctional breathing
Physiotherapists can pick up:
-
Tracheobronchomalacia
-
Inducible laryngeal obstruction
-
Breathing pattern disorder
These are often overlooked and can mimic or worsen aspergillosis symptoms.
If a physio notices these features, they feed findings back to the medical team, supporting a faster, more accurate diagnosis.
2. How Physiotherapy Helps With Treatment
🫁 A. Airway clearance
One of the biggest challenges in aspergillosis—especially ABPA, CPA, and bronchiectasis—is mucus.
Physiotherapy helps patients learn techniques to keep the lungs clear:
-
Active Cycle of Breathing Techniques (ACBT)
-
Huffing
-
Directed huff / forced expiration technique
-
Gravity-assisted drainage
-
Oscillating PEP devices (Acapella/Aerobika)
-
Autogenic drainage
-
Saline nebulisers to thin mucus
Keeping the airways clear:
-
Reduces cough and breathlessness
-
Helps antifungal treatment reach affected areas
-
Lowers risk of infection and flare-ups
-
Improves quality of life
💨 B. Managing breathlessness and fatigue
Physiotherapists teach:
-
Breathing control
-
Pacing techniques
-
Positions of ease
-
Diaphragmatic breathing
-
Inspiratory muscle training (if appropriate)
This is especially valuable for patients with:
-
ABPA flare-ups
-
CPA with reduced lung capacity
-
COPD or asthma overlap
-
Deconditioning after illness
🏃 C. Exercise, strength, and rehabilitation
Long-term aspergillosis can reduce fitness due to:
-
Repeated infections
-
Inflammation
-
Steroid side-effects
-
Time spent resting
Physios provide personalised rehab plans to rebuild:
-
Strength
-
Endurance
-
Balance
-
Activity levels
-
Confidence
🧠 D. Managing the “vicious cycle” of breathlessness and anxiety
Breathlessness naturally triggers anxiety, which then worsens breathlessness.
Physiotherapists help break this cycle through:
-
Breathing retraining
-
Relaxation strategies
-
Education on pacing and control
This also reduces the number of A&E visits for “flare-ups” that are actually driven by breathlessness-anxiety spirals.
3. Supporting Long-Term Stability
Regular physiotherapy follow-up helps patients:
-
Spot flare-ups early
-
Adjust airway clearance routines
-
Stay active despite chronic illness
-
Prevent hospital admissions
-
Maintain independence
For many patients with aspergillosis, physio becomes a key part of long-term disease management, just like antifungals, inhalers, and specialist review.
4. When Should Patients See a Physiotherapist?
Physiotherapy is particularly helpful if you have:
-
ABPA with repeated mucus plugging
-
CPA with sputum, breathlessness, or reduced activity
-
Bronchiectasis
-
Frequent chest infections
-
Difficulty producing sputum for testing
-
Breathing pattern disorder
-
Muscle weakness from steroids or long illness
-
Unexplained breathlessness
-
Tracheal or airway collapsibility
Summary
Physiotherapy is not just an “add-on” to aspergillosis care—it is a core part of both diagnosis and treatment.
Physiotherapists help:
-
Identify airway issues
-
Support accurate testing
-
Improve breathing control
-
Clear mucus
-
Build strength and stamina
-
Stabilise long-term disease
This combination leads to better outcomes, fewer infections, and a better quality of life.
🫁 Mucus Plugging in Aspergillosis: What It Is, Why It Happens, and What It Means
For patients with ABPA, CPA, Aspergillus bronchitis, or asthma
🔍 What Is a Mucus Plug?
A mucus plug is a thick clump of sticky mucus that becomes trapped in your lungs. It can block airways, cause coughing, and make breathing more difficult. In people with aspergillosis, this is common — but the type, location, and cause of the mucus can vary.
🧪 What Causes Mucus Plugging?
Your lungs naturally make mucus to protect against germs and irritants. But in fungal or allergic lung disease, this mucus may:
-
Be produced in excess
-
Become too thick or sticky
-
Get trapped due to airway damage
Aspergillosis-related causes include:
-
ABPA (Allergic Bronchopulmonary Aspergillosis) – inflammation causes thick, sticky mucus
-
Aspergillus bronchitis – fungus lives in mucus, producing biofilms
-
CPA (Chronic Pulmonary Aspergillosis) – may lead to mucus due to structural damage
-
Bronchiectasis – airways are widened and can no longer clear mucus properly
🧬 Are All Mucus Plugs the Same?
No. Mucus plugs vary in colour, texture, cause, and treatment. Here's how they differ:
| Type of Plug | What You Might See | What It Could Mean | Common in... |
|---|---|---|---|
| Sticky, stringy | Clear/yellow, like glue | Allergic inflammation | ABPA, asthma |
| Rubbery or solid | Brown, rubbery, “slug-like” | Allergic + fungal mix | ABPA, Aspergillus bronchitis |
| Green or smelly | Thick, foul-smelling | Infection (bacteria) | Bronchiectasis |
| Foamy or frothy | Clear/white, bubbly | Non-infectious irritation | COPD, asthma |
| Black or speckled | May contain fungal specks | Fungal growth | CPA, fungal bronchitis |
🖼️ What Do Mucus Plugs Look Like on a CT Scan?
Below are real examples of CT scan findings showing mucus plugging in different forms of aspergillosis and related conditions.
🧷 1. Finger-in-glove sign (ABPA)
Mucus in large airways appears like fingers inside a glove. This is common in allergic fungal airway disease.
➡ Seen in: ABPA, bronchiectasis with fungal colonisation
📍 Note: Branching tubular opacities filled with mucus.
🌿 2. Tree-in-bud pattern
Small airway blockage — plugs in the tiniest branches of the lungs. Common in infection, inflammation, and Aspergillus bronchitis.
➡ Seen in: Aspergillus bronchitis, asthma, CPA with superinfection
📍 Note: Tiny dots and lines in a tree-like shape.
🧱 3. Lung collapse (atelectasis) from plug
A large mucus plug can block a main airway, causing collapse of part of the lung.
➡ Seen in: Severe ABPA, CPA, patients with weakened cough reflex
📍 Note: Whiteout of part of lung where plug is blocking airflow.
📸 Example CT Findings

1. Bronchiectasis + mucus plug
Area in the left lower lung shows dilated bronchi filled with mucus—classic for bronchiectasis with mucoid impaction

2. Extensive bronchiectasis with plugs
Widespread thick-walled airway dilatation accompanied by mucus plugs (black arrows) and consolidation (black arrowheads)

3. Luminal plugging in small airways
Subtle luminal opacities in peripheral bronchi—the “tree‑in‑bud” pattern common in asthma, COPD, and infections.

4. Atelectasis (part of the lung has collapsed or isn’t fully inflating) due to mucus plugging
Consolidation and small airway blockage leading to lung collapse, highlighted by arrows in the upper lobe.
💡 Clinical Takeaways
| Feature | What it indicates |
|---|---|
| Mucoid impaction | Large airway fungal/allergic plugs (e.g., ABPA) or bronchiectasis |
| Tree‑in‑bud | Small-airway infection/inflammation (e.g., TB, PCD, asthma) |
| Atelectasis | Complete blockage, leading to collapse and consolidation |
| Persistent luminal plugs | Associated with worse airflow obstruction and symptoms in COPD/asthma |
✅ Next Steps / Applications
-
These CT examples are valuable for educational use—they illustrate the different patterns seen in mucus plugging across disease types.
-
Radiologists often use these signs to help diagnose and tailor management (infection, allergy, structural lung disease).
-
If your patients or students need simplified visuals, these scans paired with annotations (e.g., arrows, labels) can make great teaching tools.
🧠 What Does It Feel Like?
People often say:
“It felt like something was stuck and wouldn’t come out.”
“I finally coughed up a rubbery strand — like glue.”
“Once it cleared, I could breathe better instantly.”
🧼 How Are Mucus Plugs Treated?
Treatment depends on the underlying cause:
✅ Medications
-
Steroids – reduce inflammation in ABPA and asthma
-
Antifungals – lower fungal load (e.g., itraconazole, posaconazole)
-
Mucolytics – thin mucus (e.g., carbocisteine, hypertonic saline)
-
Antibiotics – treat bacterial infections
✅ Airway Clearance Techniques
-
Respiratory physio – helps you learn how to shift mucus
-
Devices – flutter valve, PEP mask, Acapella
-
Inhaled/nebulised therapy – opens airways and loosens plugs
⚠️ Always speak to your clinical team before starting a new technique.
🧪 Can Coughing Up a Plug Help Diagnosis?
Yes! If you cough up a rubbery, large, or unusual plug, it can be:
-
Tested for fungus, bacteria, or allergy cells (eosinophils)
-
Sent for culture to detect Aspergillus
-
Helpful in guiding or confirming diagnosis of ABPA or Aspergillus bronchitis
👣 Key Points for Aspergillosis Patients
| Question | Answer |
|---|---|
| Is mucus plugging common? | Yes, especially in ABPA, CPA, and bronchiectasis |
| Are all mucus plugs the same? | No – they vary in size, shape, colour, and cause |
| What should I do if I cough one up? | Tell your doctor – it may be useful to test |
| Can it be seen on scans? | Yes – CT can show where plugs are and how severe |
| Can it be treated? | Yes – treatments include steroids, antifungals, mucolytics, and physio |
🫁 Understanding Bronchiectasis, COPD, and Aspergillosis: What Patients Need to Know
Living with a lung condition can be confusing — especially when the symptoms of bronchiectasis, COPD, and aspergillosis are so similar. This guide explains the differences, how they are diagnosed, and why many people are wrongly diagnosed (or underdiagnosed) at first.
🌬️ What Are These Conditions?
Bronchiectasis
A condition where the airways become damaged, widened, and scarred, often from past infections, immune problems, or conditions like ABPA or CPA. This makes it hard to clear mucus, leading to regular infections.
COPD (Chronic Obstructive Pulmonary Disease)
A group of conditions — including emphysema and chronic bronchitis — that cause narrowed airways and damaged air sacs. Most often caused by smoking or long-term exposure to fumes or dust.
Aspergillosis
An infection or allergic reaction caused by the fungus Aspergillus. Types include:
-
ABPA (allergic bronchopulmonary aspergillosis) — mostly in asthma or bronchiectasis
-
CPA (chronic pulmonary aspergillosis) — causes lung cavities and fungal balls
-
Aspergillus bronchitis — low-grade infection in people with bronchiectasis
🔄 Shared Symptoms
All three can cause:
| Symptom | Bronchiectasis | COPD | Aspergillosis |
|---|---|---|---|
| Chronic cough | ✅ | ✅ | ✅ |
| Sputum (phlegm) | ✅ (often a lot) | ✅ (varies) | ✅ (sticky, sometimes brown) |
| Breathlessness | ✅ | ✅ | ✅ |
| Recurrent infections | ✅ | ✅ | ✅ |
| Fatigue | ✅ | ✅ | ✅ |
| Wheezing | Sometimes | ✅ | ✅ in ABPA |
| Coughing blood (haemoptysis) | ✅ | ⚠️ | ✅ (especially in CPA) |
Because the symptoms are so similar, many people with aspergillosis are first told they have COPD or bronchiectasis until further tests are done.
🖥️ How Are They Diagnosed?
🧪 Tests Used
| Test | Helps Diagnose |
|---|---|
| Spirometry (lung function) | COPD or asthma (airflow obstruction) |
| High-resolution CT scan | Bronchiectasis, CPA, emphysema |
| Aspergillus IgG & IgE blood tests | CPA (IgG), ABPA (IgE) |
| Sputum culture or PCR | Finds Aspergillus or bacterial infections |
| Eosinophil count | High in ABPA |
| Chest X-ray | May show cavities, but CT is better |
🫁 CT Scan Signs: What Do Radiologists Look For?
| Feature | Bronchiectasis | COPD | CPA / Aspergillosis |
|---|---|---|---|
| Airway shape | Widened, thickened (signet-ring sign) | Narrowed or normal | May have overlapping bronchiectasis |
| Lung tissue | Scarring, mucus plugging | Blackened areas (emphysema) | Cavities, fungal balls, fibrosis |
| Mucus | Often present | Sometimes present | Mucus or fungus in airways |
| Other signs | Tree-in-bud, cystic changes | Air trapping, flattened diaphragm | Thickened cavity walls, pleural changes |
💨 What Are Air Trapping and Hyperinflation?
These are signs that air is getting stuck in the lungs — common in asthma, COPD, ABPA, and sometimes CPA.
🔹 Air trapping
Air gets into the lungs but can’t get out fully. You may feel like you can’t finish exhaling.
-
Seen on CT scan as dark areas during breathing out.
-
Lung function tests show high residual volume (RV).
-
Common in asthma, ABPA, bronchiectasis, and COPD.
🔹 Hyperinflation
The lungs are permanently overfilled with air, even when you’re not trying to breathe in.
-
Seen on CT/X-ray as large lungs, flattened diaphragm, and horizontal ribs.
-
Lung function shows high total lung capacity (TLC).
-
Common in emphysema, severe asthma, and ABPA.
Why it matters: Both conditions make breathing harder and less efficient, especially when active. Treatment like inhalers, antifungals, airway clearance, or biologics may help.
💊 Treatment Approaches
| Treatment | Bronchiectasis | COPD | Aspergillosis |
|---|---|---|---|
| Airway clearance physiotherapy | ✅ Essential | Sometimes | ✅ Often vital |
| Antibiotics | ✅ Regularly used | During flares | ✅ For Aspergillus bronchitis/CPA |
| Inhalers (bronchodilators) | Sometimes helpful | ✅ Core treatment | ✅ In ABPA if asthma is present |
| Steroids | In flares or ABPA | ✅ Often | ✅ In ABPA |
| Antifungals (e.g. itraconazole, voriconazole) | ❌ Not routine | ❌ | ✅ Main treatment for CPA/ABPA |
| Pulmonary rehab | ✅ | ✅ | ✅ May help fatigue/breathlessness |
| Oxygen | Rare | ✅ In advanced disease | ✅ In some advanced cases |
🧠 Why It’s Complicated
Many patients are misdiagnosed at first:
-
Aspergillosis can develop on top of COPD or bronchiectasis
-
A long delay in diagnosis is common
-
Some people have all three conditions, or overlapping features (e.g. COPD + ABPA)
That’s why blood tests and CT scans are so important — symptoms alone aren’t enough.
✅ Summary Table
| Feature | Bronchiectasis | COPD | Aspergillosis |
|---|---|---|---|
| Cause | Infection, immune issues | Smoking, pollutants | Fungal allergy or infection |
| Airway problem | Widened, mucus-filled | Narrowed, damaged sacs | Cavities, fungus growth or allergy |
| Diagnostic test | CT scan | Spirometry | CT + Aspergillus IgG/IgE |
| Key treatment | Clearance + antibiotics | Inhalers, steroids | Antifungals ± steroids |
💬 What Should I Ask My Doctor?
-
Could my symptoms be due to more than one condition?
-
Have I had a CT scan and Aspergillus blood tests?
-
Should I be seen by a specialist centre (e.g. for ABPA or CPA)?
-
Am I using the right inhalers or physiotherapy?
-
Could I benefit from a sputum test or antifungal treatment?
🫁 Airway Clearance in Aspergillosis: A Patient Guide
Managing mucus to breathe easier, stay healthier, and feel more in control
💡 Why Is Mucus Clearance Important?
If you’re living with a condition like chronic pulmonary aspergillosis (CPA), allergic bronchopulmonary aspergillosis (ABPA), or aspergillus bronchitis, you may experience ongoing mucus build-up in your lungs. This can:
-
Make breathing harder
-
Trap infection
-
Cause inflammation and damage
-
Trigger coughing, wheeze or breathlessness
Airway clearance techniques (ACTs) help loosen and remove this mucus, reduce chest infections, and improve daily comfort.
🗣️ “Before I started clearing mucus properly, I thought breathlessness was just something I had to live with. But it’s made a big difference.”
🔧 What Techniques Are Available?
| Type | Examples | Purpose | Needs Guidance? |
|---|---|---|---|
| Breathing exercises | ACBT (Active Cycle of Breathing), huffing | Loosens mucus, clears airways | ✅ Yes – to be effective |
| Postural drainage | Lying in specific positions | Uses gravity to drain mucus | ✅ Yes – to avoid reflux or fatigue |
| Devices | Flutter, Acapella, Aerobika (OPEP devices) | Vibrate airways + create back pressure to shift mucus | ✅ Yes – to use correctly |
| Manual techniques | Chest percussion, assisted cough | Help loosen stubborn mucus | ✅ Often needs a helper |
| Mechanical devices | HFCWO (“The Vest”), IPV | Used in severe or complex cases | ✅ Prescribed in specialist settings |
🗣️ “I use the Acapella in the mornings while the kettle boils. It’s part of my routine now – and it really helps.”
🗣️ What Do Other Patients Say?
People with aspergillosis often try more than one method before finding what works best. Here are some common reflections:
On devices:
“The flutter helped a lot once I got the angle and rhythm right – but I needed someone to show me how.”
On ACBT:
“Breathing control and huffing helped me get more up with less effort than coughing all day.”
On adapting to daily life:
“It’s about what fits into your day. If something’s too awkward or tiring, you won’t keep doing it – and that’s okay.”
On trial and error:
“It took me months to find the right technique – but now I can manage my mucus better and avoid antibiotics.”
⚠️ Should I Use a Flutter or Acapella Without Help?
Not at first. These devices are effective only if used correctly. Risks of incorrect use include:
-
Not moving mucus effectively
-
Fatigue or breathlessness
-
Worsening reflux or chest tightness
-
In rare cases, worsening of lung symptoms (e.g., if air trapping occurs)
🗣️ “I bought a device online and started using it myself – but it made me dizzy. A physio later explained I was blowing too hard.”
Always ask your respiratory team or GP for referral to a respiratory physiotherapist before starting.
📝 Patient Decision Guide: Should You Use ACTs?
✅ You may benefit if:
-
You cough up mucus daily or feel it’s “stuck”
-
You’ve had repeated chest infections
-
You live with CPA, ABPA, bronchiectasis, or aspergillus bronchitis
❌ Don’t start without guidance if:
-
You have COPD, asthma, or lung scarring
-
You’ve had haemoptysis (coughing up blood)
-
You experience dizziness, nausea, or chest pain during breathing exercises
-
You have gastric reflux or recent chest surgery
🧑⚕️ What Can I Start Safely at Home?
Without needing equipment, you can begin with:
-
💧 Drink plenty of fluids – thin mucus is easier to clear
-
🪑 Sit upright – especially when coughing or during infections
-
🌬️ Use breathing control – calm, gentle breaths can reduce breathlessness
-
🗣️ Try huffing – like breathing out a mirror; easier than deep coughing
🗣️ “Even on days when I’m tired, I try to stay upright and do a few rounds of breathing exercises. It’s become a habit that helps.”
🧭 Next Steps: What to Ask Your Doctor or Nurse
-
Could I see a respiratory physiotherapist to help with mucus clearance?
-
What technique is best for my condition (e.g., ABPA vs. CPA)?
-
Can I be shown how to use a flutter device or Acapella safely?
-
What should I do if I feel worse after using a technique?
🗣️ “The physio made all the difference – she explained what my lungs were doing and helped me pick something that actually worked.”
💬 Final Word
🗣️ “It’s not just about technique – it’s about what fits your life. Small steps like staying hydrated, using huffing, and getting guidance made a big difference for me.”
There’s no one-size-fits-all approach – but with the right support, airway clearance can help you take control of your lungs, reduce flare-ups, and breathe easier.
🗣️ Managing Cough in Aspergillosis: A Patient Guide
Cough is one of the most common and exhausting symptoms of aspergillosis. Whether you have ABPA, CPA, Aspergillus bronchitis, or co-existing bronchiectasis, coughing can:
-
Disrupt sleep
-
Cause fatigue, pain, or incontinence
-
Trigger bleeding (haemoptysis)
-
Affect emotional wellbeing
The good news: many strategies can help reduce cough, loosen mucus, and protect your lungs.
🧪 First: Understand Why You're Coughing
| Underlying cause | Why it triggers cough |
|---|---|
| Inflammation (e.g. ABPA) | Airways swell and become hyperreactive |
| Mucus overproduction | Thick secretions irritate airway linings |
| Fungal burden or infection | Triggers immune response and inflammation |
| Bronchiectasis | Traps mucus and fosters infection |
| Dry air, scents, reflux | External triggers aggravate coughing reflex |
🧹 1. Clear Your Airways Safely and Effectively
Clearing mucus gently can reduce irritation and risk of infection.
✅ Best techniques:
-
Postural drainage (lying in positions to let mucus drain out)
-
Active cycle of breathing technique (ACBT):
-
Relaxed breathing
-
Deep breaths in
-
Gentle "huff" to move mucus up
-
-
Autogenic drainage (controlled breathing at different depths)
⚠️ Caution after haemoptysis:
Pause airway clearance or get medical advice first.
💧 2. Keep Mucus Thin
Thick mucus worsens cough and is harder to clear.
-
Stay hydrated – aim for 6–8 glasses of water a day
-
Nebulised saline (0.9% or 3% hypertonic) – prescribed for some patients to thin secretions
-
Humidifiers (cool mist) – especially in dry indoor environments
-
Warm showers/steam – unless they trigger coughing
💊 3. Medications to Control Cough (Prescription only)
| Type | Purpose | Notes |
|---|---|---|
| Steroids (oral or inhaled) | Reduces inflammation in ABPA | Short-term or long-term |
| Antifungals (e.g. itraconazole) | Reduce fungal burden in CPA, ABPA | May take weeks to improve cough |
| Bronchodilators (e.g. salbutamol) | Open airways and relieve tightness | Can help with productive coughing |
| Macrolide antibiotics (e.g. azithromycin) | Anti-inflammatory for bronchiectasis | Prescribed long-term in some cases |
| Antitussives (e.g. low-dose codeine) | Suppress dry, irritating cough | Use with care — consult doctor |
🧘 4. Gentle Breathing to Calm Cough Reflex
Some coughs are partly reflexive — especially in ABPA and fungal bronchitis.
Try:
-
Pursed-lip breathing
-
Diaphragmatic (belly) breathing
-
Silent counting breath cycles
-
Box breathing (inhale 4, hold 4, exhale 4, hold 4)
✅ These can reduce throat tension and break cough–irritation cycles.
🍃 5. Avoid Triggers
Many patients notice patterns — keep a cough diary to spot yours.
Common triggers:
-
Dust, damp, mould, perfumes, cleaning sprays
-
Sudden changes in temperature
-
Acid reflux (especially at night)
-
Lying flat without elevation
Tip: Try HEPA air purifiers, keep rooms ventilated, and elevate your pillow at night.
🛌 6. Manage Night-time Cough
-
Use two pillows or a wedge to keep your head elevated
-
Avoid eating or drinking large amounts just before bed
-
Use humidified air
-
Try a warm, non-irritating drink (e.g. water with honey) if safe for you
-
Consider a bedside lozenge or mild cough suppressant on bad nights (with GP approval)
🫁 7. When to Seek Help
Speak to your specialist if:
-
Cough worsens suddenly
-
You develop fever, chest pain, or breathlessness
-
You start coughing up blood or clots
-
You are losing sleep or weight due to cough
-
Current treatments no longer help
You may need:
-
Repeat chest imaging
-
Change in antifungal or steroid dose
-
Additional airway clearance support (e.g. physiotherapy)
-
Blood or sputum tests for infection
🤝 Support Is Available
-
National Aspergillosis Centre (UK) – offers advice and remote support
-
Respiratory physiotherapists – can teach breathing and mucus clearance techniques
-
Patient support groups – many share cough coping strategies