🏥 Surgery in Patients with ABPA or CPA: Can It Worsen Symptoms, and Should It Proceed?
Patients with Aspergillus-related lung diseases, such as Allergic Bronchopulmonary Aspergillosis (ABPA) and Chronic Pulmonary Aspergillosis (CPA), sometimes report worsened symptoms after undergoing surgery under general anaesthetic. While this is a recognised clinical pattern, it does not mean surgery should be avoided. Instead, it requires preparation and close perioperative management to reduce risk.
🔍 Can Surgery Worsen Aspergillosis Symptoms?
Yes — and here's why:
✳️ 1. Airway Irritation from Intubation
-
Endotracheal tubes can irritate airways already inflamed by ABPA or structurally altered by CPA.
-
Mechanical ventilation can impair mucus clearance and exacerbate cough or infection.
✳️ 2. Postoperative Immunosuppression
-
Surgery temporarily suppresses immune function.
-
Perioperative corticosteroids or stress-induced immune suppression can permit fungal flare-ups or reactivation.
✳️ 3. Impaired Mucus Clearance
-
Pain, immobility, and sedation reduce the patient’s ability to cough and clear secretions.
-
In CPA or ABPA, this can lead to plugging, fungal regrowth, or secondary bacterial infection.
✳️ 4. Drug Interactions
-
Azole antifungals (e.g. itraconazole, posaconazole) interact with many anaesthetics, opioids, and steroids.
-
These interactions can alter drug levels, reduce antifungal efficacy, or increase toxicity risk.
✳️ 5. Stress and Inflammation
-
Surgical stress may worsen the inflammatory or allergic component of ABPA.
-
CPA-related cavities may bleed or become re-infected post-op.
✅ Should Surgery Still Go Ahead?
Yes — surgery can and often should proceed when it is medically indicated.
Delaying needed procedures (e.g. for cancer, fractures, or pain relief) can lead to worse outcomes than the potential risks related to aspergillosis.
🛡️ Recommended Precautions
🔷 Pre-Operative Planning
-
Ensure all care teams are aware of the diagnosis.
-
Review lung imaging, baseline oxygenation, and current antifungal/steroid regimens.
-
Arrange for pre-op airway clearance if sputum is a concern.
🔷 Antifungal Management
-
Continue antifungal therapy through the perioperative period.
-
Use IV formulations if oral administration isn’t possible.
-
Check for drug interactions with anaesthetic or post-op medications.
🔷 Steroid Cover (ABPA and CPA on steroids)
-
Patients on chronic steroids may need perioperative hydrocortisone supplementation (adrenal cover).
-
Apply “sick day rules” or use the patient’s adrenal insufficiency plan, if applicable.
🔷 Post-Op Monitoring
Watch for:
-
Worsening cough, breathlessness, or sputum
-
Fever or signs of secondary infection
-
Raised IgE (in ABPA) or haemoptysis (in CPA)
-
Any signs of antifungal failure or drug toxicity
⚠️ When Might Surgery Be Delayed?
Consider postponing non-urgent surgery if:
-
There is active haemoptysis
-
The patient has uncontrolled inflammation or fungal burden
-
A recent scan shows expanding cavities or new infiltrates
-
Antifungal resistance is suspected or not yet managed
💬 Key Message for Patients
“Having ABPA or CPA doesn’t mean you can’t have surgery — but we do need to take extra care around your airways, your antifungal treatment, and your recovery. With the right team and planning, we can safely support you through your procedure.”
👅 Geographic Tongue and Aspergillosis: What You Need to Know

Several members have raised concerns about Geographic Tongue — a harmless but uncomfortable condition that affects the surface of the tongue. While it’s not directly caused by aspergillosis, certain factors in people with ABPA, CPA, SAFS, or bronchiectasis may increase their risk of developing or worsening symptoms.
🔍 What is Geographic Tongue?
Geographic tongue causes red, smooth patches on the surface of the tongue with white or pale borders. These patches may change location from day to day — like a moving map, hence the name. It’s not contagious and usually not dangerous, but it can cause burning or soreness, especially when eating spicy, salty, or acidic foods.
🤔 Why might people with Aspergillosis be affected?
While aspergillosis doesn’t directly cause geographic tongue, the following indirect factors may make it more likely or more bothersome:
1. Inhaled Corticosteroids (ICS)
Used for asthma, ABPA, and bronchiectasis, these can:
-
Alter the balance of bacteria and fungi in the mouth
-
Increase the risk of oral thrush, which can irritate the tongue
-
Cause dryness or sensitivity in the mouth
2. Dry Mouth
Common in patients with:
-
Chronic lung disease
-
Long-term medications
-
Dehydration from breathing difficulties
Dry mouth makes the tongue more prone to irritation and soreness.
3. Mouthwash Sensitivity
Many aspergillosis patients avoid alcohol-based or acidic mouthwashes (like Listerine) — and with good reason:
-
These products can worsen tongue discomfort
-
Your dentist may advise they’re not necessary, especially if they’re harming the delicate lining of your mouth
4. Immune or Nutritional Changes
-
Long-term corticosteroids or other medications may suppress the immune system
-
Vitamin deficiencies (like B12, folate, or iron) can affect the tongue and mouth tissues
✅ Tips to Manage Geographic Tongue
-
Use non-acidic, alcohol-free mouthwashes (or none at all if your dentist agrees)
-
Switch to SLS-free toothpaste (found in many sensitive brands)
-
Avoid spicy, salty, or acidic foods during flare-ups
-
Stay well hydrated
-
Rinse your mouth after using inhalers
-
Speak to your dentist or GP if symptoms are severe or persistent
📜 Etymology: Where does “patient” come from?

The word "patient" has deep historical roots — and its origin gives insight into how medicine used to view people under care.
The word "patient" comes from the Latin:
patiens — meaning "one who suffers" or "one who endures"
It’s related to the verb patior, meaning “to suffer,” “to undergo,” or “to bear.”
So originally, a patient was someone who suffered or endured illness — someone passive, who received care or treatment, rather than someone actively doing something.
🧠 Why is this still used?
Historically, healthcare was something done to a person, often in the context of:
-
Religious or charitable care
-
Limited treatment options (patients mostly endured their illnesses)
-
The role of doctors as “healers,” and patients as the sick who “waited patiently”
Even as medicine advanced, the term persisted — and still reflects:
-
The person receiving care or treatment
-
A distinction from the “professional” (doctor, nurse, etc.)
🩺 Is this changing?
Yes — there's growing awareness that the term "patient" can imply passivity, while many prefer:
-
Person living with [condition]
-
Service user (used in mental health and social care)
-
Client (used in private healthcare)
-
Or just individual / person
That said, “patient” remains standard in medical, legal, and NHS documentation — but the language of healthcare is slowly evolving to be more person-centred.
💉 Best Practices for Self-Injecting Biologics
✅ 1. Choose the Right Injection Site
Biologics are usually given subcutaneously (just under the skin).
Most common sites:
-
Abdomen (at least 2 inches away from the belly button)
-
Thighs (top outer area)
-
Sometimes upper outer arm (if someone else is injecting)
👉 Rotate sites to avoid irritation or lumps.
🧊 2. Warm Up the Medicine First
-
Take it out of the fridge 30–60 minutes before injecting
-
Cold biologics can sting — warming it to room temperature reduces discomfort
❌ Never heat in a microwave or hot water — just let it sit at room temperature.
🧼 3. Prepare Properly
-
Wash your hands
-
Clean the injection site with an alcohol swab — let it dry fully before injecting
-
Check the pen or syringe for:
-
Expiry date
-
Clarity of solution (should be clear, no lumps or particles)
-
💡 4. Use the Right Technique
-
If using a pre-filled syringe:
-
Pinch the skin gently
-
Insert the needle at a 45° angle
-
Inject slowly and steadily
-
-
If using an auto-injector (pen):
-
Place flat against the skin
-
Press firmly until you hear a click
-
Hold for the full time recommended (usually 5–15 seconds)
-
Don’t rub the site afterward — this can increase irritation.
🧘♀️ 5. Reduce Pain and Anxiety
-
Breathe out slowly as you inject — this reduces muscle tension
-
Use distraction (music, cold pack, or mental focus techniques)
-
If nervous, consider numbing the skin with an ice pack for 30 seconds before cleaning with alcohol
-
Inject slowly with syringes — fast injection = more sting
🧴 Aftercare
-
Apply light pressure with a cotton ball or tissue
-
Avoid rubbing or massaging
-
Use a cold pack if sore or bruised
-
Report any ongoing redness, swelling, or allergic reaction
🛠️ Tools That Help
-
Needle-free injection devices (limited availability)
-
Numbing creams like lidocaine/prilocaine (available OTC or by GP)
-
Sharps disposal bin — request one from your pharmacy or consultant team
-
Injection reminder apps if on a schedule (e.g. MyTherapy, Medisafe)
🧑⚕️ When to Speak to Your Team
-
If injections remain very painful
-
If you're unsure about technique
-
If you develop redness, swelling, or lumps that last more than 24–48 hours
-
If you feel light-headed or allergic afterward
⚠️ Summer 2025 Travel Warning: Fungal Lung Infections a Hidden Risk
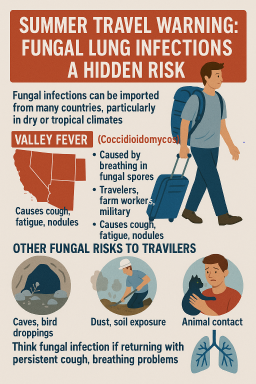
Important information for UK travellers, GPs and patients with chronic lung conditions
As more UK residents prepare to travel this summer — whether for holidays, charity work, military duty, or visiting family abroad — it’s important to raise awareness of a growing health risk that is often overlooked: fungal lung infections.
These conditions can be serious, persistent, and easily mistaken for other illnesses — including long COVID, TB, or bacterial pneumonia.
🌍 Fungal Infections Can Be Acquired Abroad — and Not Just in the Tropics
Fungal spores live in soil, compost, dust, and decaying organic matter. In many parts of the world, especially dry or tropical climates, travellers can unknowingly inhale spores that can cause long-term lung disease — often weeks or months after returning to the UK.
🧳 Key Risk Regions and Infections
🇺🇸 Valley Fever (Coccidioidomycosis)
-
Endemic to the southwestern United States — including Arizona, California, Nevada, Texas, and New Mexico
-
Caused by inhaling Coccidioides spores from dry, dusty soil
-
Affects travellers, farm workers, and military personnel
-
Can cause chronic cough, fatigue, joint pain, and lung nodules
❗ UK patients with unexplained lung symptoms should be asked about travel to these areas — Valley Fever can mimic CPA or even lung cancer.
🌎 Other Endemic Fungal Risks for Travellers
| Disease | Region(s) | Typical Exposure |
|---|---|---|
| Histoplasmosis | Central/South America, Africa, Asia | Caves, bird/bat droppings, demolition sites |
| Blastomycosis | Central USA (Great Lakes, Mississippi) | Soil, wood, riverside areas |
| Paracoccidioidomycosis | Brazil, Colombia | Rural farming dust |
| Talaromycosis | SE Asia, Southern China, India | Dusty environments (esp. in immunocompromised) |
| Sporotrichosis | Latin America, Africa, Japan | Plant thorns, soil, cat scratches |
| Cryptococcosis | Worldwide | Bird droppings, tree bark |
🌾 UK Risks Still Apply at Home
Even without travel, UK residents can develop Aspergillus-related conditions (CPA, ABPA) through:
-
Gardening (esp. with compost)
-
Farming or stables
-
Building or renovation work
-
Damp housing
Drug-resistant Aspergillus fumigatus is also rising in the UK — partly due to the use of agricultural fungicides.
🩺 Advice for GPs and Respiratory Teams
Ask:
-
Have you travelled to dry, dusty regions or tropical countries this year?
-
Have you been exposed to soil, caves, animals, compost, or renovation dust?
-
Do you have underlying lung disease (e.g. asthma, COPD, bronchiectasis)?
Consider:
-
Fungal testing (Aspergillus IgG/IgE, fungal cultures)
-
CT imaging for persistent nodules or cavitations
-
Early referral to respiratory or infectious disease specialists
-
Contacting the National Aspergillosis Centre for persistent or complex cases
✅ What Travellers Can Do
-
Wear a dust mask when gardening, hiking, or working around soil
-
Avoid enclosed spaces with bird or bat droppings
-
Seek help if you return from travel and develop:
-
A cough that won’t go away
-
Fatigue, fever, or weight loss
-
Chest tightness or unexplained breathlessness
-
📌 Final Reminder
Fungal infections are not rare — they’re under-recognised.
This summer, think fungal if you or your patient return from travel with persistent lung symptoms. Early diagnosis can make all the difference.
🫁 Why Is CPA Called a Long-Term Condition — Not a Lifelong One?

Chronic Pulmonary Aspergillosis (CPA) is often described as a long-term condition, but people sometimes wonder why it isn’t called a “lifelong” disease — especially since many people need antifungal treatment and regular monitoring for years.
Here’s what we know:
🩺 CPA Affects Everyone Differently
CPA is a complex condition that includes several forms — some people have a single fungal ball (aspergilloma), while others have more widespread or progressive disease. For many, CPA needs long-term treatment, such as antifungal tablets, oxygen, physiotherapy, or hospital care.
But not everyone has the same experience:
-
Some people are stable for years
-
Some respond well to treatment and no longer need antifungals
-
Others may live with occasional flare-ups or long-term health problems
🔁 Why It’s Not Always Called Lifelong
CPA is called a “long-term condition” because:
-
It typically lasts at least a year, often longer
-
It may come and go in phases
-
It needs regular follow-up and may affect daily life
But not everyone will have it for the rest of their life — and that’s why we don’t use the word “lifelong” for everyone.
🔬 We Don’t Yet Know Who is Truly ‘Cured’
To say whether CPA is curable, we would need to:
-
Follow a large group of patients
-
For many decades
-
To see who stays well and never relapses
That kind of long-term research is still ongoing — so at the moment, doctors can’t say for sure when or if someone is permanently cured.
Some people stay well for years after stopping treatment — but it’s too early to know if the infection is truly gone, or just sleeping.
💬 What This Means for You
-
CPA is a condition that can be managed — sometimes very successfully
-
You might not need treatment forever — but regular check-ups help catch any changes early
-
Your team will work with you to find the right balance of treatment and independence
-
If you feel well, that's a good sign — but it's still important to keep an eye on things
📍In short: CPA is a serious, long-term condition, but it’s not always lifelong. We still have more to learn, and long-term studies are helping us understand it better every year.
BBC Food Nutrition Calculator – Summary for Patients and Public

The BBC Food Nutrition Calculator is an easy-to-use, interactive tool designed to help you understand whether your diet is meeting your nutritional needs. By entering your age and sex, the calculator evaluates your intake of key nutrients and highlights any you might be under- or over-consuming. It also suggests foods rich in those nutrients to help you make healthy dietary adjustments.
Key Features
-
Personalised Assessment: Calculates your nutritional needs based on age and sex.
-
Food Recommendations: Suggests nutrient-rich foods if your intake is too low or too high.
-
Supplement Guidance: Explains when supplements might be useful—e.g. vitamin D in winter months or when housebound.
-
Immune System Support: Highlights nutrients that support immune health (vitamins A, C, D, B6, B9, B12, zinc, and iron).
Common Nutrient Gaps in the UK
According to UK dietary surveys, many people do not get enough of the following nutrients:
-
Fibre – under-consumed across all age groups
-
Vitamin D – commonly low year-round
-
Iron – especially low in girls and women aged 11–49
-
Calcium – often low in girls aged 11–18
-
Selenium – low among most females and older males
-
Zinc – insufficient in teenagers and adults over 75
Additionally, many people exceed recommended levels of free sugars, saturated fats, and salt.
Is the Information Verified?
Yes. The nutritional guidance in the BBC Food Nutrition Calculator is based on verified and reliable sources, including:
-
NHS and Public Health England recommendations
-
National Diet and Nutrition Survey (NDNS) data
-
Scientific consensus on daily nutrient requirements and health effects
While the BBC may not cite sources on every page, its content is regularly reviewed and reflects the current public health standards in the UK. You can trust this tool as a credible and evidence-based guide to dietary health.
Try the Calculator
You can access the BBC Nutrition Calculator here:
🔗 bbc.co.uk/food/articles/nutrition_calculator
💊 How Medicines Are Approved — and What “Off-Label” Means
🔹 1. What Is “Licensed” or “Approved” Medication Use?
Before a medicine can be prescribed in the UK (or any country), it goes through a formal approval process:
| Step | What Happens |
|---|---|
| Clinical trials | The medicine is tested for safety, effectiveness, and quality. |
| Regulatory review | In the UK, the Medicines and Healthcare products Regulatory Agency (MHRA) or the European Medicines Agency (EMA) reviews trial data. |
| Marketing authorisation | If approved, the medicine is “licensed” for specific conditions, doses, age groups, and methods of use. |
🟢 A licensed use means the drug has been judged safe and effective for that specific use, based on strong clinical evidence.
🔹 2. What Is “Off-Label” Use?
Off-label use means a doctor prescribes a medicine in a way that is not covered by its official license.
This could include:
-
Using a medicine for a different condition
-
Giving it at a different dose or frequency
-
Using a different route (e.g. inhaled instead of injected)
-
Giving it to a different age group (e.g. in children)
This is legal, but it means the prescriber is using their clinical judgement outside the official licensing terms.
🔹 3. Why Might a Doctor Use a Medicine Off-Label?
| Reason | Example |
|---|---|
| There is no licensed treatment for a rare condition | e.g. inhaled amphotericin B for CPA or ABPA |
| The licensed treatment doesn’t work or causes side effects | e.g. switching antifungal drugs |
| New evidence supports another use, but the company hasn’t applied for a new licence | e.g. old drugs used in new ways based on research |
| Medicines used in children or elderly often lack specific licensing data |
🔹 4. Is Off-Label Use Safe?
It can be, but it requires:
-
Good clinical judgement
-
Use of the best available evidence
-
Often, discussion with a multidisciplinary team
-
Informed consent from the patient (especially important in high-risk cases)
The prescriber takes more responsibility, because the use hasn’t been formally approved by regulators.
🔹 5. Who Oversees This in the UK?
-
The MHRA licenses medicines.
-
The General Medical Council (GMC) and NHS allow doctors to prescribe off-label when it’s in the patient’s best interest.
-
NICE guidelines sometimes include off-label use if evidence supports it.
🔹 6. Real-World Example: Inhaled Amphotericin
-
Licensed: Amphotericin B is approved for injection to treat fungal infections.
-
Off-label: Nebulised (inhaled) use is not officially licensed, but it is used in some centres to treat or prevent fungal lung disease (e.g. CPA, ABPA) where evidence and specialist experience supports it.
🔹 Summary: Key Points
| Term | Meaning |
|---|---|
| Licensed use | The use of a medicine that has been approved for a specific purpose by a regulator. |
| Off-label use | Prescribing a medicine in a different way than officially licensed — legal, but used with clinical caution. |
| Who decides? | Ultimately, the prescribing clinician, supported by evidence, guidance, and the needs of the individual patient. |
🌍 Fungal Spore Release in Different Climates
Climate has a major impact on fungal spore patterns. The types of fungi, timing of spore release, and health risks vary greatly between temperate, tropical, arid, and cold climates.
🌦️ Temperate Climates (e.g. UK, Northern Europe, Pacific Northwest USA)
-
Seasonal peaks: late summer to early autumn
-
Cladosporium, Alternaria, Aspergillus, Penicillium dominate
-
Triggers: humidity, rain, decaying vegetation, compost
-
Evening/night peaks for many spore types
🧠 Health risk: ABPA, asthma, SAFS, especially after garden work or composting
🌴 Tropical and Subtropical Climates (e.g. SE Asia, Central America, parts of Africa)
-
High year-round spore loads
-
Fungi: Aspergillus, Rhizopus, Mucor, Curvularia, Basidiomycetes, tropical molds
-
Daily rain cycles promote spore germination and release
-
Basidiospores and hyaline molds surge during evening and after rainfall
🧠 Higher incidence of fungal sinusitis, allergic fungal rhinosinusitis, and invasive infections in immunocompromised patients
🏜️ Arid and Semi-Arid Climates (e.g. Southwest USA, parts of the Middle East, Northern Africa)
-
Lower general spore burden, but dust storms can release huge amounts
-
Fungi: Coccidioides spp. (Valley fever), Aspergillus, dryland molds
-
Dry conditions favour small, dry spores that aerosolise easily
-
Wind and soil disturbance (construction, farming) are major triggers
🧠 Coccidioidomycosis, aspergillosis, dust-related asthma
❄️ Cold or Alpine Climates (e.g. Scandinavia, Alps, Canadian north)
-
Lower fungal biodiversity
-
Short seasonal spore peaks (spring–summer)
-
Indoor exposure more relevant: Penicillium, Cladosporium, Aspergillus
-
Mold growth occurs in poorly ventilated buildings (e.g. after snow melts)
🧠 Winter indoor mould exposure can worsen asthma, ABPA, SAFS
📌 Key Takeaway:
Different climates = different fungal threats.
The more humid, warm, or plant-rich the environment, the more active and diverse the fungal spore release — but indoor mould exposure is relevant in every climate.
Types of Window Screens for Allergen Protection
Yes — there are specialised window screens designed specifically to block allergens, including fungal spores, pollen, and dust. These can be a practical and effective solution for patients with ABPA, SAFS, asthma, CPA, or other respiratory allergies.
✅ 1. Pollen and Allergen Screens (Micromesh / Allergy Mesh)
-
Made from ultrafine polyester or polypropylene mesh
-
Pore size: typically 0.3–0.5 mm, small enough to block:
-
Pollen
-
Fungal spores (like Aspergillus and Cladosporium)
-
Insect particles
-
-
Allows air flow while reducing allergen load
🛒 UK Brands / Products to Look For:
-
Poll-Tex®: Proven in European studies to block >99% of airborne pollen and fine particles.
-
Neat Pleat® or Flyscreen UK Allergy Mesh
-
Tesa® Insect Stop Pollen Protection
-
Amazon or B&Q: Offer DIY-fit mesh kits
✅ 2. HEPA-Filtered Window Units
-
Some products combine an extractor fan + HEPA filter, ideal for:
-
Rooms needing airflow without outdoor contaminants
-
Urban or high-spore environments
-
-
More expensive but very effective
Examples:
-
Vent-Axia PureAir Room Ventilator
-
Aereco HRV or HEPA filter units
🛠️ Installation Tips
-
Choose removable or magnetic frames for rented homes
-
Ensure tight seal around edges to prevent gaps
-
Use with dehumidifiers or HEPA air purifiers indoors for extra control
💡 Bonus Tip:
-
Leave windows open early morning or midday if you must ventilate — avoid dusk/night when fungal spore levels rise.
-
Don’t open windows near compost heaps, sheds, or leafy overgrowth.