🌿 Biologics when ABPA and CPA overlap: What Patients Need to Know
Understanding how they work, when they’re helpful, and when extra care is needed
Biologic medicines (such as omalizumab, mepolizumab, benralizumab, dupilumab and newer options like tezepelumab) are increasingly used to treat Allergic Bronchopulmonary Aspergillosis (ABPA) and severe asthma. They can be life-changing for some people.
However, their place in Chronic Pulmonary Aspergillosis (CPA) — especially in people who have both ABPA and CPA together — is more complicated and needs careful specialist supervision.
This article explains what we know so far.
🌟 1. ABPA and CPA are different conditions — but some people have both
-
ABPA is mainly an allergic reaction to Aspergillus in the airways.
-
CPA is a chronic fungal infection that causes cavities, scarring, and long-term lung damage.
-
Some people start with ABPA and later develop CPA, or the two conditions overlap.
-
The 2024 international ABPA guidelines now recognise this overlap as real and important.
Because biologics target allergy pathways rather than fungal infection, treatment decisions must look at both sides of the disease.
🌿 2. Biologics in ABPA: the evidence is strong and growing
Biologics can help patients with ABPA or severe asthma by:
-
reducing steroid use
-
improving breathing
-
decreasing mucus plugging
-
lowering flare-ups
-
improving quality of life
Biologics most commonly used in ABPA include:
| Biologic | Target | Notes |
|---|---|---|
| Omalizumab | IgE | Well established, helps many ABPA patients |
| Mepolizumab | IL-5 | Helps eosinophilic inflammation |
| Benralizumab | IL-5Rα | Similar to mepolizumab; long-acting |
| Dupilumab | IL-4Rα | Very promising for allergic disease; growing evidence for ABPA |
| Tezepelumab | TSLP | Very new; limited ABPA data so far |
For many people with ABPA, biologics are safe and effective when monitored.
⚠️ 3. Biologics and CPA: much less evidence
-
CPA is caused by persistent fungal infection and structural lung damage.
-
Biologics do not treat fungal infection, and they do not prevent cavities.
-
In CPA, the mainstay of treatment is still:
-
antifungal medication (usually itraconazole, voriconazole or posaconazole)
-
careful imaging (CT scans)
-
airway clearance
-
sometimes surgery or bronchoscopy
-
There is no strong evidence that biologics help CPA itself.
🔄 4. What about patients who have both ABPA and CPA?
This is where things become more complex.
Biologics may help the allergic part (ABPA), but:
-
they do not treat fungal infection
-
they do not stop fungal cavities from progressing
-
they may reduce inflammation that normally helps the body contain infection
If antifungal treatment is interrupted or not strong enough, fungal activity may increase while the allergic symptoms improve — so regular monitoring is essential.
Specialist centres (like the NAC) now emphasise:
✔️ Continue antifungals if CPA is active
✔️ Watch cavities with regular CT scans
✔️ Monitor Aspergillus IgG/IgE and fungal cultures
✔️ Check whether symptoms are from allergy, infection, or both
✔️ Make joint plans between asthma/airway doctors and mycology specialists
❓ 5. Are some biologics better than others for ABPA/CPA overlap?
There is no official guidance yet, but early observations suggest:
⭐ Most promising for ABPA:
-
Dupilumab seems particularly effective for allergic disease (IgE, mucus, airflow), though still off-label for ABPA.
⭐ Increasing interest:
-
Tezepelumab works outside the eosinophil pathway and may be useful in some asthma types, but research in ABPA is only just starting.
⭐ Useful in selected cases:
-
Anti-IL-5 biologics (mepolizumab, benralizumab) help airway eosinophils but may not help every ABPA patient.
⚠️ Uncertain in CPA:
-
None of the biologics treat fungal infection or cavities directly.
-
Their role in active CPA remains unclear and requires careful oversight.
🧭 6. What this means for patients
If you have ABPA only, biologics may be an excellent option — especially if:
-
steroids cause side-effects
-
your asthma is uncontrolled
-
you have frequent flare-ups
-
your IgE levels are very high
-
mucus plugging or wheezing continues despite treatment
If you have CPA or cavities, treatment needs to be more cautious:
-
antifungal medication usually needs to continue
-
biologics may still help if the allergic component is significant
-
CT scans must be repeated to make sure cavities are not progressing
-
specialists must weigh benefits vs. risk for each patient individually
💬 7. Summary
-
Biologics can be extremely helpful for ABPA.
-
They do not treat CPA, and cannot replace antifungal medicines.
-
In patients with both ABPA and CPA, the approach must be personalised.
-
Dupilumab and (possibly) tezepelumab are emerging biologics with promise, but evidence is still developing.
-
Decisions should always be made with a specialist centre such as the National Aspergillosis Centre (NAC).
🌬️ Inhaled Antifungal Treatments for Chronic Pulmonary Aspergillosis (CPA)
Updated: October 2025
💡 Why are inhaled antifungals being developed?
For people living with Chronic Pulmonary Aspergillosis (CPA), treatment usually involves long courses of oral antifungal tablets such as itraconazole, voriconazole, or posaconazole.
These medicines circulate through the whole body to reach the lungs — but sometimes they cause side-effects, interact with other drugs, or fail to reach high enough levels in thick mucus, cavities, or scarred areas of lung tissue.
Inhaled antifungal therapy aims to solve this problem by delivering medicine directly to the lungs using a nebuliser or inhaler device.
This can potentially mean:
-
✅ Higher drug levels exactly where infection is active
-
⚡ Faster local action
-
🚫 Fewer whole-body side-effects
-
🧩 Fewer drug interactions
This approach is especially promising for patients with localized lung disease, such as CPA or aspergillus bronchitis, where the fungus lives in damaged parts of the lung.
💊 Current inhaled antifungal options (used off-label)
🧪 Nebulised Amphotericin B
At the moment, nebulised amphotericin B is the only inhaled antifungal used in hospitals, although it is off-label for CPA.
It is more commonly used to prevent infection in people who have had a lung transplant or who are severely immunocompromised.
In some specialist centres, it may be used as maintenance therapy or an add-on for CPA if other antifungals have not worked or cannot be tolerated.
Advantages
-
High concentration in lung tissue
-
Minimal effects on other organs (especially the kidneys)
Drawbacks
-
Possible airway irritation (cough, tight chest, wheezing)
-
Requires specialist supervision and appropriate nebuliser equipment
🔬 New treatments in development
💨 Opelconazole (also called PC-945)
Opelconazole is a new inhaled triazole antifungal developed by Pulmocide Ltd in the UK.
It works in the same way as existing azole antifungals — by blocking the fungal enzyme CYP51 — but has been specially designed to stay in the lungs and minimise side-effects elsewhere.
In laboratory and early human studies, opelconazole has shown:
-
Strong activity against Aspergillus fumigatus
-
High and lasting drug levels in the lungs
-
Very low blood levels (reducing risk of toxicity and drug interactions)
-
Good tolerability in early trials
Although not yet licensed, it has been used compassionately in small numbers of patients with difficult-to-treat lung aspergillosis at centres such as Manchester and London.
🧾 Current and recent clinical trials
| Trial ID | Treatment | Condition | Purpose / Summary | Status |
|---|---|---|---|---|
| NCT06447402 | Nebulised Amphotericin B vs Saline | Chronic Pulmonary Aspergillosis | Tests whether regular nebulised amphotericin can help prevent CPA relapse compared with saline. | Recruiting |
| NCT03656081 | Itraconazole ± Nebulised Liposomal Amphotericin B | CPA | Compares oral itraconazole alone versus itraconazole plus inhaled amphotericin for symptom and scan improvement. | Completed – results pending |
| NCT05238116 | Inhaled Opelconazole + Standard Therapy | Refractory Invasive Pulmonary Aspergillosis | Phase 3 trial evaluating safety and added benefit of inhaled opelconazole. UK, EU, and US sites. | Recruiting |
| NCT05037851 | Inhaled Opelconazole (PC-945) | Post-Lung Transplant Prophylaxis | Assesses prevention of fungal infection after transplant. Found well tolerated. | Completed |
| PubMed 34058036 | Nebulised Amphotericin B vs Oral Itraconazole | Pulmonary Aspergilloma (CPA subset) | Six-month open study found similar improvement rates between inhaled amphotericin and oral itraconazole. | Completed |
👉 You can look up any of these studies on ClinicalTrials.gov by entering the trial ID (e.g. NCT06447402).
⚠️ Things to keep in mind
-
Not yet routine — Inhaled antifungals are available only in research or specialist centres.
-
Limited evidence — Most data come from transplant or invasive aspergillosis studies, not chronic infection.
-
Delivery challenges — Damaged or scarred areas of lung may be hard for inhaled drugs to reach.
-
Possible side-effects — Coughing or mild bronchospasm are common; pre-treatment with an inhaler may help.
-
Monitoring still needed — Even with inhaled therapy, your care team will continue to check symptoms, lung scans, and blood markers (such as Aspergillus IgG).
🧭 Questions to ask your specialist
If you are interested in this type of therapy, you could ask:
-
Does my centre offer nebulised amphotericin as part of CPA care?
-
Are there any clinical trials nearby (for example NCT06447402 or NCT05238116)?
-
Could an inhaled antifungal be used with my current oral treatment?
-
What are the side-effects and how are they monitored?
-
What nebuliser device is required and how often would I use it?
🏥 UK research centres involved
Current UK involvement is mainly through:
-
National Aspergillosis Centre, Wythenshawe Hospital (Manchester)
-
Royal Brompton and Harefield Hospitals (London)
-
UK transplant centres participating in Pulmocide’s opelconazole studies
🗝️ Key takeaway
Inhaled antifungal medicines are an exciting development that could make CPA treatment safer and more targeted in the future.
For now, they are mainly available through clinical trials or specialist centres, but the early results are promising — especially for those who have struggled with oral antifungal side-effects or limited success.
If you’re interested, speak to your CPA specialist or the National Aspergillosis Centre team about ongoing research and eligibility.
Chronic Pulmonary Aspergillosis (CPA) – Information For Family and Friends
Print this off or share electronically
WHAT IT IS
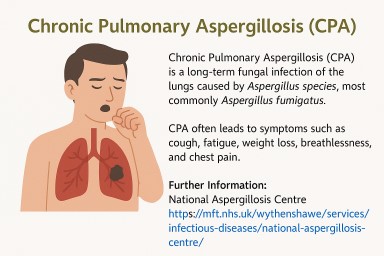
CPA (Chronic Pulmonary Aspergillosis) is a long-term lung infection caused by the Aspergillus fungus. It often develops where lungs are already damaged (e.g., TB, COPD, bronchiectasis, sarcoidosis) and may form cavities, sometimes with fungal balls (aspergillomas).
WHAT IT'S NOT
-
Not contagious – you can't catch CPA.
-
Not poor hygiene – spores are everywhere in the air.
-
Not the patient's fault – flare-ups or setbacks happen because of the illness, not something they did wrong.
WHY AREN'T OTHERS AFFECTED?
Most people remove spores without trouble. CPA appears when lungs are already damaged or the immune system can't fight the fungus well – after past infections, chronic lung disease, or weakened defences. It's not about choices; it's lung history and chance.
TYPICAL SYMPTOMS
-
Persistent cough (sometimes with blood)
-
Breathlessness
-
Fatigue and low energy
-
Weight loss
-
Recurring chest infections
WORST SYMPTOMS
-
Coughing up blood – can be small streaks or larger amounts; sudden and frightening; urgent if heavy.
-
Severe fatigue – can stop even simple tasks; not just ‘tiredness’.
TREATMENT
-
Long-term antifungal medication
-
Regular scans and blood tests
-
Surgery in selected cases
THE REALITY
CPA is a serious, long-term condition. On bad days, people may not be able to do much at all. Symptoms can dominate daily life and limit social plans – cancelled arrangements are the illness talking, not them. It can also make people feel grumpy or irritable – not because they don't care, but because constant symptoms, tiredness, and limits on daily life are frustrating and exhausting. There’s often a mental load too – always thinking about avoiding dust, damp, or mould spores, and sometimes feeling overcautious about activities like going on boats, visiting old buildings, or anywhere that might harbour moisture or mould. This risk-checking is a form of self-protection, even if it means missing out.
It’s important to mention the mood swings and fatigue caused not only by the disease but also by the medication. For some, constant hand tremors are also part of daily life — these are often misunderstood by others.
LOOKING AHEAD
-
With effective treatment – Many people can keep the infection stable for years, control symptoms, and stay independent.
-
Risks – CPA can slowly progress, and severe flare-ups (like coughing large amounts of blood) may need urgent treatment.
-
Change over time – The illness can be stable for long periods, but it often needs lifelong monitoring and treatment changes. Support from specialists helps keep people well for longer.
ENVIRONMENTAL TRIGGERS & PROTECTION
Some people with CPA need to avoid environments with high levels of dust or fungal spores. This includes gardening, composting, building work, or damp/mouldy places. Wearing a protective mask during these activities can help reduce risk. Avoiding these triggers is about preserving lung health – not being fussy or antisocial.
HOW FRIENDS AND FAMILY CAN BEST HELP
-
Respect limits – breathlessness, fatigue, or coughing up blood can stop plans at short notice; it's not a choice.
-
Minimise exposure risks – avoid inviting them to dusty, damp, or mouldy places.
-
Offer practical help – driving to appointments, carrying shopping, or helping at home during flare-ups.
-
Be patient with mood changes – grumpiness can come from exhaustion and constant vigilance against triggers.
-
Talk openly about safety – if you suggest an outing, ask “Would this feel safe for you?”
-
Stay connected – even if they can't join in physically, a call or small gesture keeps them included.
MORE INFORMATION & SUPPORT
National Aspergillosis Centre (UK): https://mft.nhs.uk/wythenshawe/services/infectious-diseases/national-aspergillosis-centre/
Patient information & community: https://aspergillosis.org
📘 What is CPA? (Chronic Pulmonary Aspergillosis)
Patient handout for A&E staff who are not aware of aspergillosis.
What is CPA?
CPA is a chronic fungal infection of the lungs caused by Aspergillus, most often in people who already have damaged lungs from conditions like tuberculosis, COPD, lung cancer, or sarcoidosis.
Unlike ABPA, CPA is a true infection, not an allergic reaction. It is not contagious but can slowly destroy lung tissue if not treated.
Symptoms
-
Chronic cough, often with mucus
-
Coughing up blood (haemoptysis)
-
Fatigue, low-grade fever
-
Unexplained weight loss
-
Breathlessness
-
Recurrent chest infections not responding to antibiotics
Diagnosis
-
CT scan of the chest showing cavities, nodules, or fungus balls (aspergillomas)
-
Aspergillus IgG antibody (usually raised)
-
Positive sputum PCR or culture for Aspergillus
-
Exclude TB and malignancy
Treatment
-
Long-term antifungal therapy (e.g. itraconazole, voriconazole, posaconazole)
-
Monitor blood levels and liver function
-
Surgery or embolisation if severe bleeding occurs
-
Supportive care: oxygen, nutrition, physiotherapy
Key Points for A&E:
✅ CPA is a progressive fungal infection, not a typical bacterial pneumonia
✅ May present with haemoptysis, respiratory distress, or systemic illness
✅ Review current antifungal treatment and potential drug interactions
✅ Consider urgent chest CT and specialist referral if patient is unwell
📍 For specialist support:
National Aspergillosis Centre (NAC)
🏥 Wythenshawe Hospital, Manchester University NHS Foundation Trust
🌐 NAC homepage on MFT website https://mft.nhs.uk/wythenshawe/services/infectious-diseases/national-aspergillosis-centre/
🌐 www.aspergillosis.org
📞 Daytime contact: 0161 291 2891 or 0161 291 4362
📞 Urgent out-of-hours: Call Wythenshawe switchboard on 0161 998 7070
📢 Ask for the on-call Infectious Diseases Consultant
🧾 Rezafungin: A New Antifungal Being Trialled for CPA
Some people with chronic pulmonary aspergillosis (CPA) have trouble tolerating standard antifungal medications. Commonly used drugs like voriconazole and posaconazole can cause serious side effects such as hallucinations, liver enzyme disturbances, or gut problems. When these medications can’t be used, options become limited.
A new antifungal, rezafungin, is now being studied as a possible treatment for CPA — especially in people who can't tolerate azoles. It is not yet approved for aspergillosis, but a major clinical trial is under way.
🧬 What Is Rezafungin?
Rezafungin is part of a newer group of antifungal drugs called echinocandins. These work by weakening the fungal cell wall — a very different mechanism to azole drugs like itraconazole or voriconazole.
Key features:
-
Given as a weekly intravenous (IV) drip
-
Long-acting: stays in the body for days after each dose
-
Designed to provide high drug levels in the lungs and bloodstream
-
Early studies show less frequent side effects than with some older antifungals
It is already licensed for treatment of Candida bloodstream infections but is being studied now for CPA.
🧪 Current Research: Trial for CPA
A clinical trial is currently recruiting people with CPA who:
-
Cannot take azole antifungals because of side effects or resistance
-
Need alternative or combination therapy
This trial (called REZAFUNGin Efficacy and Safety for Aspergillus – CPA) is being conducted in the UK and internationally. The goal is to test whether rezafungin is safe and effective in CPA patients who have few remaining options.
🔗 View the clinical trial (NCT06794554)
📊 What Have Previous Studies Found?
While studies in CPA are just beginning, previous trials in other fungal infections provide important clues:
✅ Phase 2 & 3 Studies (Candida Infections)
-
Rezafungin was found to be as effective as daily echinocandins (like caspofungin)
-
Once-weekly dosing worked just as well as daily treatment
-
Side effects were mild, and liver toxicity was rare
-
No CNS side effects (like hallucinations) were reported
🧫 Laboratory Evidence
-
Rezafungin is active against Aspergillus fumigatus, including some azole-resistant strains
-
It reaches good levels in lung tissue — an important feature for CPA
-
May be used alone or with another antifungal in complex cases
🩺 Case Example
A recent case report described successful treatment of chronic pulmonary aspergillosis using rezafungin plus voriconazole in a patient with resistant infection (Oxford University Press, 2024).
⚠️ Is Rezafungin Available Now?
Not yet. Rezafungin is only available for CPA:
-
Through a clinical trial, or
-
By special approval for compassionate use in selected cases
It is not currently licensed for aspergillosis in the UK or elsewhere.
💬 What Should I Discuss with My Doctor?
If you're considering participation in a clinical trial or if standard treatments have failed, you might ask:
-
Am I eligible for the rezafungin CPA trial?
-
What are the benefits and risks of trying this treatment?
-
Will I still need other antifungals (e.g. azoles or amphotericin)?
-
How often will I need blood tests and hospital visits?
-
Will this help if I have azole resistance or liver side effects?
📌 Summary
Rezafungin is a new antifungal drug being tested for people with chronic pulmonary aspergillosis who cannot take older treatments. It offers once-weekly dosing and early signs suggest a favourable safety profile, including in patients with liver concerns or those who had side effects from azoles.
Although not yet widely available, it may offer hope for people with limited options. If you or someone you know is struggling with antifungal intolerance, you may wish to speak to your medical team about the CPA clinical trial or explore compassionate access routes.
👉 Learn more or check trial sites:
🔗 https://clinicaltrials.gov/study/NCT06794554
🌿 Living with Chronic Pulmonary Aspergillosis (CPA):
Hope, Setbacks, and What “Cure” Really Means
Being diagnosed with chronic pulmonary aspergillosis (CPA) is often overwhelming. You may be on treatment with antifungals like itraconazole (Sporanox) and have already gone through ups and downs — early improvement, then a period of stagnation, and now you're facing a new CT scan with anxiety.
You’re not alone — and this guide brings together the key questions patients often ask, along with helpful real-life insights.
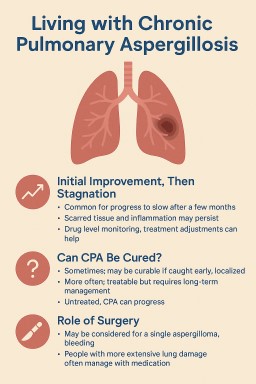
✅ “I Felt Better at First — Then It Stalled. Why?”
This is very common in CPA. In the first few months:
-
Symptoms like cough, breathlessness, and fatigue may improve.
-
CT scans may show fungal balls shrinking or disappearing.
But then: -
Symptoms return or stay the same.
-
Scans show little change.
-
Anxiety grows.
This doesn’t mean treatment has failed.
It may just mean you've reached a slower phase of healing. Here's why:
| Reason | What’s Happening |
|---|---|
| Antifungal success at first | Fungal load drops, but scarring and inflammation remain. |
| Itraconazole is working | But drug levels may be too low — monitoring is essential. |
| Other lung conditions coexist | Like bronchiectasis or NTM, which antifungals don’t treat. |
| Ongoing exposure to mould | Especially from damp buildings, compost, or dust. |
| Immune response adapts | Symptoms may persist even if fungus is under control. |
🔁 “Can Things Improve Again?”
Yes — many people improve again after a plateau or setback.
What helps:
-
✅ Check your itraconazole blood level — low levels = poor response.
-
✅ Consider a switch to another antifungal, like voriconazole or posaconazole.
-
✅ Ask your team about co-infections, inhaled therapies, or lung physiotherapy.
-
✅ Monitor your vitamin D, weight, and steroid use (to rule out other causes of symptoms).
-
✅ Keep going — many people improve again with time, adjustments, and support.
🗣️ “I had a dip after three months. We checked my drug levels — they were low. After a small dose change, I felt better again.” — Patient story
💬 “Can CPA Be Cured?”
🩺 What Do We Mean by “Cure”?
In medicine, a cure usually means:
-
The disease is gone,
-
Treatment is no longer needed,
-
There’s no sign of the illness coming back.
But in CPA, a full cure is rare — because the conditions that allowed it to take hold usually remain.
⚠️ Why CPA Is Rarely “Cured” in the Traditional Sense
-
CPA often happens in lungs already damaged by:
-
Tuberculosis (TB)
-
COPD or emphysema
-
Bronchiectasis
-
Allergic bronchopulmonary aspergillosis (ABPA)
These conditions are chronic and don’t disappear, even if the fungus is controlled.
-
-
Scars, cavities, and weakened lung tissue remain, and symptoms can return if antifungal treatment is stopped too soon or if reinfection occurs.
✅ So What’s a More Accurate Way to Think About It?
Instead of talking about a cure, specialists use words like:
| Term | What It Means |
|---|---|
| Clinical improvement | You feel better, symptoms reduce, scans look more stable. |
| Stability | The disease is under control — not progressing. |
| Remission | The infection is quiet or inactive — with or without treatment. |
| Disease control | Long-term treatment is helping manage the condition safely. |
📌 Think of CPA like asthma or diabetes — not "gone," but often well controlled.
🟢 Sometimes — CPA can be cured
In a small number of people:
-
The fungus is cleared completely,
-
Symptoms resolve,
-
Antifungals are stopped and not needed again.
This is more likely when:
-
CPA is caught early,
-
The disease is limited to one area,
-
The person has otherwise healthy lungs.
🟡 For Most — CPA is treatable but long-term
You may not fully “get rid of it” — but you can:
-
Live well with it,
-
Keep symptoms under control,
-
Avoid major complications.
🔴 If untreated, CPA can progress
-
Damage spreads,
-
Bleeding may worsen,
-
General health may decline.
That’s why staying on treatment and having regular check-ups is so important.
🔪 What About Surgery?
Surgery can help in some cases — but it depends on your specific situation.
🟢 Surgery may help if:
-
You have a single aspergilloma (fungal ball).
-
You're experiencing repeated bleeding (haemoptysis).
-
The lesion is growing or pressing on nearby structures.
-
Antifungals haven’t worked, or aren’t tolerated.
In these cases, removing part of the lung may stop bleeding, reduce symptoms, and improve quality of life.
🔴 Surgery may not be suitable if:
-
Disease affects both lungs or multiple areas.
-
Your lung function is too low.
-
The lesion is too close to vital structures.
-
You have underlying conditions like COPD, bronchiectasis, or ABPA that wouldn’t improve after surgery.
🩺 If surgery isn’t an option:
You may still benefit from:
-
Bronchial artery embolisation (BAE) — a non-surgical way to stop bleeding.
-
Ongoing antifungal therapy.
-
Symptom management through breathing support and physiotherapy.
💬 What Other Patients Say
| Patient Story | Outcome |
|---|---|
| “My fungal ball vanished after 6 months. I’m still on meds but doing well.” | Stable with long-term itraconazole |
| “I plateaued, then improved again after switching drugs.” | Switched to posaconazole |
| “I had surgery after coughing up blood for months. It made a huge difference.” | Surgery successful |
| “I live with scarring, but I’m off meds now and stable.” | Clinical remission |
🧾 What You Can Do
-
✅ Ask your doctor to check your itraconazole level if not already done.
-
✅ Record weekly symptoms — cough, fatigue, breathlessness.
-
✅ Ask about sputum tests for fungi or bacteria.
-
✅ Discuss surgery or embolisation if you’re coughing up blood.
-
✅ Stay hopeful — CPA is manageable, and some people do recover.
❤️ Final Thoughts
CPA is rarely curable in the strictest sense, but that doesn’t mean it’s hopeless.
Many people live full lives with the disease under control. Even if CT scans show lasting changes, what really matters is:
How you feel. How well you breathe. How stable your condition stays.
With antifungal therapy, expert care, and the right support, you are not alone — and you can feel better again.
🌫️ A Life Shaped by Mould: One Person’s Journey with CPA and Lung Disease
Sadly, at the time of writing this story has to be paid for to read the full article. What follows is a summary of the free-to-access abstract.
“It started with damp walls – but it didn’t end there.”
This is the story of someone who spent a lifetime battling the hidden effects of mould exposure and fungal lung disease, from childhood through adulthood. Their experience is a powerful reminder of how long-term exposure to poor indoor environments — especially damp, flood-prone homes — can leave a lasting imprint on lung health.
🧒 Early Clues: Breathing Problems in Childhood
-
The author grew up in mouldy homes, regularly affected by floods.
-
As a teenager, they suffered from collapsed lungs, underwent pleurectomies, and were diagnosed with blebs (small air-filled sacs on the lung lining).
-
No one realised at the time that this could be linked to inhaled fungal spores.
🩺 The Long Road to Diagnosis
-
Years later, symptoms returned: chest infections, breathlessness, persistent coughing.
-
Eventually, doctors diagnosed:
-
Chronic pulmonary aspergillosis (CPA) – a long-term fungal infection
-
Severe bronchiectasis – a condition where the airways become damaged and inflamed
-
The root cause was now clear: years of breathing in airborne mould spores had likely caused permanent lung damage.
💊 Managing CPA: A Complex Balancing Act
The chapter describes the difficulty of living with CPA, including:
-
Strong antifungal medications (like itraconazole or posaconazole) and their side effects
-
Emergency lung procedures
-
Ongoing adjustments in daily life — from avoiding certain environments to managing fatigue
🤝 What Helped Most: Self-Advocacy and Support
This is also a story of resilience and empowerment. The author learned to:
-
Ask better questions at medical appointments
-
Work closely with specialists in fungal lung disease
-
Use trusted online resources to understand their condition
-
Keep going, even when progress was slow
💬 “I had to become my own advocate – not to fight my doctors, but to work with them more effectively.”
🧭 Advice for Others
The author shares practical tips that could help anyone dealing with CPA, bronchiectasis, or long-term lung illness:
-
Track your symptoms and treatments
-
Stay informed – but avoid misinformation online
-
Get help from respiratory physiotherapists
-
Don’t ignore your environment – especially damp, mouldy places
-
Keep asking questions until the answers make sense
🌟 A Message of Hope
This chapter isn’t just a medical account – it’s a message of hope and strength. It shows how understanding your own health, building a good medical team, and staying proactive can make a big difference, even in the face of serious illness.
Understanding the Different Types of Chronic Pulmonary Aspergillosis (CPA)
CPA is a long-term lung condition caused by a common fungus called Aspergillus. It usually affects people who already have lung damage — from infections like tuberculosis (TB), conditions like COPD or asthma, or diseases such as sarcoidosis.
There are five main types of CPA. Knowing which one you have can help guide your treatment and follow-up.
🟠 1. Chronic Cavitary Pulmonary Aspergillosis (CCPA)
Most common form
-
Caused by Aspergillus growing in one or more cavities in the lungs
-
Cavities may slowly get larger or thicker
-
Often develops in people with previous lung disease
Symptoms:
-
Long-term cough
-
Fatigue and weight loss
-
Breathlessness
-
Sometimes mild or moderate coughing up blood
Treatment: Long-term antifungal tablets (e.g. itraconazole or voriconazole)
⚠️ 2. Chronic Fibrosing Pulmonary Aspergillosis (CFPA)
Advanced stage of CPA
-
Happens when long-term infection causes lung scarring (fibrosis)
-
Lungs become stiff, making breathing harder
Symptoms:
-
Worsening breathlessness
-
Low oxygen levels
-
Severe fatigue
Treatment: Focuses on antifungals, symptom relief, and oxygen if needed
🟢 3. Simple Aspergilloma
A single fungal ball in a lung cavity
-
A round ball of fungus (aspergilloma) forms in an existing lung cavity
-
Often found during scans done for other reasons
-
Some people have no symptoms at all
Main risk: Coughing up blood (sometimes serious)
Treatment:
-
Monitoring if mild
-
Surgery or embolisation if bleeding occurs
🔴 4. Subacute Invasive Aspergillosis (SAIA or CNPA)
Faster-moving form of CPA
-
Occurs over weeks to months
-
Often seen in people with weaker immune systems (e.g. due to diabetes, steroids, or alcohol dependence)
-
Infection starts to invade deeper lung tissue
Symptoms:
-
Fever
-
Worsening breathlessness
-
Severe weight loss
Treatment: Prompt antifungal treatment and close medical monitoring
🟡 5. Aspergillus Nodules
Small lumps caused by Aspergillus
-
These are solid nodules in the lungs, often found by chance on a CT scan
-
They may be mistaken for cancer at first
-
Often cause no symptoms
Treatment:
-
Usually watch and wait
-
Sometimes surgery or biopsy if uncertain
🩺 Why Knowing Your CPA Type Matters
Understanding your CPA type helps your medical team:
-
Choose the best treatment for you
-
Monitor for bleeding or lung damage
-
Decide when to repeat scans or adjust medication
💬 Questions to Ask Your Doctor
-
Which type of CPA do I have?
-
Will I need long-term antifungal treatment?
-
How often should I have scans or blood tests?
-
What should I do if I cough up blood?
🧘 Final Note
CPA is a chronic condition, but many people manage it well with the right treatment and regular check-ups. You are not alone — support and information are available.
🏥 Surgery in Patients with ABPA or CPA: Can It Worsen Symptoms, and Should It Proceed?
Patients with Aspergillus-related lung diseases, such as Allergic Bronchopulmonary Aspergillosis (ABPA) and Chronic Pulmonary Aspergillosis (CPA), sometimes report worsened symptoms after undergoing surgery under general anaesthetic. While this is a recognised clinical pattern, it does not mean surgery should be avoided. Instead, it requires preparation and close perioperative management to reduce risk.
🔍 Can Surgery Worsen Aspergillosis Symptoms?
Yes — and here's why:
✳️ 1. Airway Irritation from Intubation
-
Endotracheal tubes can irritate airways already inflamed by ABPA or structurally altered by CPA.
-
Mechanical ventilation can impair mucus clearance and exacerbate cough or infection.
✳️ 2. Postoperative Immunosuppression
-
Surgery temporarily suppresses immune function.
-
Perioperative corticosteroids or stress-induced immune suppression can permit fungal flare-ups or reactivation.
✳️ 3. Impaired Mucus Clearance
-
Pain, immobility, and sedation reduce the patient’s ability to cough and clear secretions.
-
In CPA or ABPA, this can lead to plugging, fungal regrowth, or secondary bacterial infection.
✳️ 4. Drug Interactions
-
Azole antifungals (e.g. itraconazole, posaconazole) interact with many anaesthetics, opioids, and steroids.
-
These interactions can alter drug levels, reduce antifungal efficacy, or increase toxicity risk.
✳️ 5. Stress and Inflammation
-
Surgical stress may worsen the inflammatory or allergic component of ABPA.
-
CPA-related cavities may bleed or become re-infected post-op.
✅ Should Surgery Still Go Ahead?
Yes — surgery can and often should proceed when it is medically indicated.
Delaying needed procedures (e.g. for cancer, fractures, or pain relief) can lead to worse outcomes than the potential risks related to aspergillosis.
🛡️ Recommended Precautions
🔷 Pre-Operative Planning
-
Ensure all care teams are aware of the diagnosis.
-
Review lung imaging, baseline oxygenation, and current antifungal/steroid regimens.
-
Arrange for pre-op airway clearance if sputum is a concern.
🔷 Antifungal Management
-
Continue antifungal therapy through the perioperative period.
-
Use IV formulations if oral administration isn’t possible.
-
Check for drug interactions with anaesthetic or post-op medications.
🔷 Steroid Cover (ABPA and CPA on steroids)
-
Patients on chronic steroids may need perioperative hydrocortisone supplementation (adrenal cover).
-
Apply “sick day rules” or use the patient’s adrenal insufficiency plan, if applicable.
🔷 Post-Op Monitoring
Watch for:
-
Worsening cough, breathlessness, or sputum
-
Fever or signs of secondary infection
-
Raised IgE (in ABPA) or haemoptysis (in CPA)
-
Any signs of antifungal failure or drug toxicity
⚠️ When Might Surgery Be Delayed?
Consider postponing non-urgent surgery if:
-
There is active haemoptysis
-
The patient has uncontrolled inflammation or fungal burden
-
A recent scan shows expanding cavities or new infiltrates
-
Antifungal resistance is suspected or not yet managed
💬 Key Message for Patients
“Having ABPA or CPA doesn’t mean you can’t have surgery — but we do need to take extra care around your airways, your antifungal treatment, and your recovery. With the right team and planning, we can safely support you through your procedure.”
🫁 Why Is CPA Called a Long-Term Condition — Not a Lifelong One?

Chronic Pulmonary Aspergillosis (CPA) is often described as a long-term condition, but people sometimes wonder why it isn’t called a “lifelong” disease — especially since many people need antifungal treatment and regular monitoring for years.
Here’s what we know:
🩺 CPA Affects Everyone Differently
CPA is a complex condition that includes several forms — some people have a single fungal ball (aspergilloma), while others have more widespread or progressive disease. For many, CPA needs long-term treatment, such as antifungal tablets, oxygen, physiotherapy, or hospital care.
But not everyone has the same experience:
-
Some people are stable for years
-
Some respond well to treatment and no longer need antifungals
-
Others may live with occasional flare-ups or long-term health problems
🔁 Why It’s Not Always Called Lifelong
CPA is called a “long-term condition” because:
-
It typically lasts at least a year, often longer
-
It may come and go in phases
-
It needs regular follow-up and may affect daily life
But not everyone will have it for the rest of their life — and that’s why we don’t use the word “lifelong” for everyone.
🔬 We Don’t Yet Know Who is Truly ‘Cured’
To say whether CPA is curable, we would need to:
-
Follow a large group of patients
-
For many decades
-
To see who stays well and never relapses
That kind of long-term research is still ongoing — so at the moment, doctors can’t say for sure when or if someone is permanently cured.
Some people stay well for years after stopping treatment — but it’s too early to know if the infection is truly gone, or just sleeping.
💬 What This Means for You
-
CPA is a condition that can be managed — sometimes very successfully
-
You might not need treatment forever — but regular check-ups help catch any changes early
-
Your team will work with you to find the right balance of treatment and independence
-
If you feel well, that's a good sign — but it's still important to keep an eye on things
📍In short: CPA is a serious, long-term condition, but it’s not always lifelong. We still have more to learn, and long-term studies are helping us understand it better every year.