The Power of Keeping a Health Diary When You Have Aspergillosis

Last reviewed: June 2026
Audience: People living with aspergillosis, families and carers
Key points
- A health diary can help you understand symptoms, triggers and changes over time.
- It can be especially useful if you experience fatigue, brain fog or memory problems.
- It can make clinic appointments more focused and productive.
- A diary may show progress that is hard to notice day to day.
- The best diary is simple, quick and realistic to keep using.
Contents
- Why keep a health diary?
- How it can help with aspergillosis
- Brain fog and memory
- Spotting patterns and triggers
- Using your diary at appointments
- The psychological benefit
- Simple diary template
- Common questions
- When to seek medical advice
Why keep a health diary?
Living with aspergillosis often means symptoms change from day to day. Some days may be manageable. Others may involve more coughing, breathlessness, fatigue, sinus symptoms, poor sleep or medication side effects.
Because these changes can happen gradually, it can be difficult to remember exactly when symptoms started, whether they are getting better or worse, or what might have triggered them.
A health diary gives you a simple record of what is happening over time. It can help you, your family and your healthcare team see patterns that may not be obvious from memory alone.
How a diary can help with aspergillosis
People with aspergillosis may find it useful to record:
- Cough
- Breathlessness
- Fatigue
- Sputum or phlegm
- Wheeze
- Sinus symptoms
- Sleep quality
- Exercise or walking distance
- Mood and wellbeing
- Medication changes
- Possible side effects
You may also want to note possible triggers, such as damp or mould exposure, pollen, dusty environments, changes in weather, respiratory infections, stress, travel or changes in medication.
Brain fog and memory
Many people with long-term lung conditions describe episodes of brain fog. This may feel like forgetfulness, poor concentration, difficulty finding words, feeling mentally slower than usual, or feeling as though your head is “empty”.
Brain fog can have many possible causes, including fatigue, poor sleep, infection, inflammation, stress, anxiety, pain, medication side effects, low oxygen levels or other health problems.
A diary acts as an external memory. Instead of trying to remember when something changed, you can look back and see what was happening at the time.
Spotting patterns and triggers
| What you record | What it may help show |
|---|---|
| Symptoms | Whether cough, breathlessness or fatigue are improving or worsening |
| Sleep | Whether poor sleep is linked to worse symptoms |
| Exercise | What level of activity is manageable |
| Weather | Whether heat, humidity, cold air or storms affect symptoms |
| Environment | Possible links with damp, mould, dust or pollen |
| Medication | Possible benefits, side effects or changes during dose reduction |
| Infections | Early warning signs or repeated patterns |
Using your diary at appointments
Healthcare professionals may ask questions such as:
- When did your symptoms start?
- Are they getting better or worse?
- Have you noticed any triggers?
- Have you changed any medication recently?
- How far can you walk now compared with before?
- Have you had any infections or courses of antibiotics?
These questions are not always easy to answer from memory, especially when you are tired or anxious. A diary can help you give clearer, more accurate information.
You may find it useful to bring a short summary to your appointment, such as:
- Three things that have improved
- Three things that have worsened
- Any medication changes
- Your main questions for the appointment
Sometimes the diary tells a different story
When you have had a difficult few days, it can feel as though nothing is improving. A diary may show that the wider picture is more encouraging.
For example, you may feel:
“Nothing has changed.”
But your diary may show:
- You are walking further than three months ago
- You are sleeping better
- You have had fewer chest infections
- You are coughing less at night
- You are doing more social activities
Equally, a diary can show gradual deterioration that might otherwise be missed. Both types of information can be useful.
The psychological benefit
Chronic illness can feel unpredictable. A diary can help restore a sense of control by changing the question from:
“Why do I feel awful?”
to:
“What changed recently?”
This can reduce uncertainty and help you feel more involved in your care.
A diary can also become a record of resilience. It may include difficult days, but it can also capture walks completed, holidays taken, family events attended, personal goals reached and challenges overcome.
Keep it simple
Many people stop keeping a diary because they try to record too much. A simple diary is usually more useful than a complicated one.
A daily entry might take less than two minutes and include:
- Symptoms, scored from 0 to 10
- Energy level, scored from 0 to 10
- Sleep quality
- Exercise or activity
- Medication changes
- Anything unusual
Consistency matters more than detail.
Paper, phone or app?
There is no single correct way to keep a diary. You could use:
- A notebook
- A printed diary sheet
- A phone notes app
- A calendar
- Voice notes
- A spreadsheet
- A symptom tracking app
- A fitness tracker or smartwatch
The best diary is the one you will actually use.
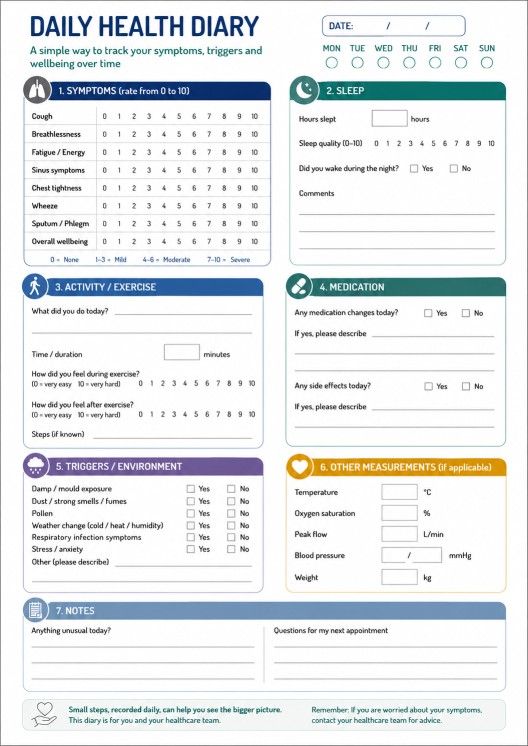
Simple diary template
Daily health diary
Date: __________________________
Symptoms, 0–10
Cough: ______
Breathlessness: ______
Fatigue: ______
Sinus symptoms: ______
Overall wellbeing: ______
Sleep
Hours slept: ______
Sleep quality, 0–10: ______
Activity
Exercise or activity today:
__________________________________________________
Medication
Any medication changes or side effects?
__________________________________________________
Notes
Anything unusual today?
__________________________________________________
__________________________________________________
Daily Diary - PDF downloadable
Common questions
Do I need to write every day?
No. Some people write daily. Others only record changes, flare-ups, medication changes or important events.
What if I forget for a few days?
That is very common. Simply restart when you remember. A diary does not have to be perfect to be useful.
Should I record test results?
You can if you find it helpful. Some people record blood results, oxygen saturations, lung function, weight, clinic letters or medication levels. Do not worry if this feels too much. A simple symptom diary is still useful.
Can a diary replace medical advice?
No. A diary is a tool to support conversations with your healthcare team. It should not be used to diagnose or treat symptoms without medical advice.
When to seek medical advice
Seek medical advice promptly if you experience:
- Sudden or significant worsening of breathlessness
- Coughing up large amounts of blood
- Persistent fever
- Severe chest pain
- New confusion or rapidly worsening brain fog
- Weakness, speech problems, facial drooping or visual changes
- Symptoms that are worsening quickly or feel unusual for you
If you are unsure, contact your healthcare team, NHS 111, your GP, or emergency services depending on severity.
Further information
- Living with aspergillosis
- Fatigue and aspergillosis
- Exercise and aspergillosis
- Mental wellbeing and aspergillosis
Author and review information
This article is provided for general educational support for people affected by aspergillosis. It is not a substitute for medical advice from your own healthcare team.
Prepared for: Aspergillosis.org
Last reviewed: June 2026
Do You Carry Your Aspergillosis Information With You?

New NHS Plans Could Help in Future – But What About Today?
The UK government is currently debating plans for a new NHS “single patient record” system. The aim is to allow authorised healthcare professionals to access important information from GP surgeries, hospitals, community services and other parts of the NHS more easily.
If implemented successfully, this could reduce the need for patients to repeatedly explain their medical history and could help emergency departments, ambulance crews and other healthcare professionals see important information such as diagnoses, medications, allergies and previous treatment.
For people living with aspergillosis and other long-term respiratory conditions, this could be especially valuable. However, these changes will take time to develop and introduce. For now, patients remain one of the most important links between different parts of the healthcare system.
Why This Matters for Aspergillosis Patients
Many people with aspergillosis receive care from several different services, including:
- General Practitioners (GPs)
- Local respiratory teams
- Specialist nurses
- Hospital clinics
- Emergency departments
- Pharmacists
- Community healthcare teams
- Specialist centres such as the National Aspergillosis Centre
Healthcare records are not always immediately available to every professional involved in your care. This means there may be times when you need to explain:
- What type of aspergillosis you have
- Which medications you take
- Any important allergies or serious drug reactions
- Whether you have adrenal insufficiency or take long-term steroids
- Who your specialist team is
- What previous treatments you have received
Having this information readily available can save time and may help healthcare professionals make decisions more quickly and safely.
What Information Should You Carry?
 You do not need to carry your entire medical record. A simple one-page health summary is usually enough.
You do not need to carry your entire medical record. A simple one-page health summary is usually enough.
1. Your Diagnosis
List your main diagnoses clearly. Examples include:
- Allergic Bronchopulmonary Aspergillosis (ABPA)
- Chronic Pulmonary Aspergillosis (CPA)
- Severe Asthma with Fungal Sensitisation (SAFS)
- Aspergillus Bronchitis
- Bronchiectasis
- Severe Asthma
- Chronic Obstructive Pulmonary Disease (COPD)
2. Your Current Medications
Include all current treatments, particularly:
- Antifungal medications, such as itraconazole, voriconazole, posaconazole or isavuconazole
- Steroid tablets
- Hydrocortisone replacement therapy
- Biologic therapies
- Inhalers
- Oxygen therapy
- Antibiotics you are currently taking
Try to keep this list up to date.
3. Drug Allergies and Serious Reactions
This is one of the most important sections. Include any known allergies or serious reactions, for example:
- Penicillin allergy
- Prednisolone allergy
- Previous severe drug reactions
- Medicines you have been told to avoid
4. Steroid or Adrenal Information
If you have adrenal insufficiency or are taking long-term steroid treatment, make this very clear.
I have adrenal insufficiency and may require emergency steroid treatment if seriously unwell.
Many patients already carry a steroid emergency card. If you have been advised to carry one, continue to carry it at all times.
5. Specialist Contact Information
Include:
- Consultant name
- Hospital or specialist centre
- Clinic or specialist nurse contact details, if available
6. Emergency Contact
Include:
- Name
- Relationship
- Telephone number
An Important Extra Note for Aspergillosis Patients
Many antifungal medications interact with other medicines. If you take itraconazole, voriconazole, posaconazole or isavuconazole, consider including the following statement on your health summary:
I take an azole antifungal medication. Please check for potential drug interactions before prescribing new medicines.
This simple statement may help avoid medication-related problems.
If You Are a National Aspergillosis Centre Patient: Using myMFT
If you are a patient of the National Aspergillosis Centre (NAC), you may already have access to some of your hospital information through the myMFT patient portal.
myMFT is the patient portal used by Manchester University NHS Foundation Trust (MFT), which includes Wythenshawe Hospital and the National Aspergillosis Centre.
Depending on the services you use, myMFT may allow you to:
- View MFT appointment details
- Access clinic letters
- Keep track of important test results, letters and health information
- Attend online video consultations
- Use proxy access to help manage a family member’s healthcare, with consent
Many patients find it useful to keep copies of important clinic letters on their phone or tablet. This can be particularly helpful if you attend another hospital, visit your GP, travel away from home or need emergency treatment.
myMFT does not replace a future NHS-wide patient record, but it can provide access to important information that may help you and your healthcare professionals manage your care more effectively.
Find out more about myMFT on the Manchester University NHS Foundation Trust website.
For Patients Not Under the National Aspergillosis Centre
If you are not an NAC or MFT patient, your local hospital may have its own patient portal or online record system. Ask your hospital clinic, respiratory team or GP surgery whether you can access clinic letters, appointment information or test results online.
You may also be able to use the NHS App to manage parts of your healthcare, depending on your GP surgery and local NHS services.
Find out more about the NHS App.
You may also find it useful to know your NHS number. You do not need to know your NHS number to receive NHS care, but it can be helpful when contacting services or completing forms.
Where Should You Keep Your Information?
Many patients choose to:
- Save a copy on their mobile phone
- Keep a printed copy in their wallet or handbag
- Store it alongside their steroid emergency card
- Keep a copy with travel documents
- Share a copy with family members or carers
- Keep copies of important clinic letters on their phone or tablet
The best system is the one that is easy to access when needed.
Printable options (Word documents):
Looking Ahead
The proposed NHS single patient record could eventually make it easier for healthcare professionals to access important information quickly and safely.
For patients with rare conditions such as aspergillosis, that could improve continuity of care, reduce delays and reduce the need to repeatedly explain complex medical histories.
Until then, carrying a simple summary of your condition remains one of the easiest and most effective ways to help healthcare professionals understand your health needs and provide appropriate care.
Key Points
- Carry a simple one-page health summary.
- Include diagnoses, medications, allergies and specialist contacts.
- Clearly state if you have adrenal insufficiency or take long-term steroids.
- Mention azole antifungal treatment and potential drug interactions.
- National Aspergillosis Centre patients may be able to access clinic information through myMFT.
- Patients outside MFT should ask whether their own hospital has a patient portal.
- Keep important information on your phone and consider carrying a printed copy.
- A future NHS single patient record may improve information sharing, but patients remain an important source of information today.
Common Questions
Do I need to carry all my clinic letters?
No. A concise one-page summary is usually more useful in an emergency. However, keeping copies of important clinic letters on your phone can be helpful.
What if I am treated at more than one hospital?
This is one of the main reasons to carry a health summary. Different healthcare providers may not always have immediate access to the same information.
Is this only useful in emergencies?
No. It can also help during GP appointments, outpatient visits, travel, planned hospital admissions and when seeing healthcare professionals unfamiliar with aspergillosis.
What if I am a National Aspergillosis Centre patient?
Consider registering for myMFT and keeping important clinic letters available on your phone or tablet for easy access.
What if I am not an NAC patient?
Ask your own hospital or respiratory clinic whether they offer a patient portal. You can also check what information is available through the NHS App.
When to Seek Medical Advice
Seek urgent medical advice if you experience:
- Significant worsening of breathlessness
- Chest pain
- Coughing up significant amounts of blood
- Symptoms of adrenal crisis if you have adrenal insufficiency
- Severe allergic reactions to medications
- Rapid deterioration in your respiratory symptoms
If you need emergency help, call 999. For urgent medical advice in the UK, use NHS 111.
Useful Links
- myMFT patient portal – Manchester University NHS Foundation Trust
- NHS App
- Find your NHS number
- Aspergillosis information and support
Frequently Asked Questions
What information should an aspergillosis patient carry in an emergency?
Patients should consider carrying a summary of their diagnosis, medications, allergies, steroid or adrenal information, specialist contacts and emergency contact details.
Should people with aspergillosis carry a medication list?
Yes. Many aspergillosis patients take antifungal medicines, steroids, biologic therapies and inhalers. An up-to-date medication list can help avoid prescribing errors and drug interactions.
What is myMFT?
myMFT is the patient portal used by Manchester University NHS Foundation Trust. It allows eligible patients to access appointments, clinic letters, test results and other healthcare information.
Can aspergillosis patients access their records online?
Some patients can access records through services such as myMFT, local hospital portals or the NHS App, depending on where they receive care.
What is the NHS single patient record?
The proposed NHS single patient record aims to improve information sharing between healthcare providers so patients do not need to repeatedly explain their medical history.
Author: National Aspergillosis Centre Patient Support Team
Reviewed by: National Aspergillosis Centre
Last reviewed: June 2026
Important: This article is intended for information only and should not replace advice from your healthcare team.
Living With Aspergillosis: When Others Do Not Fully Understand How You Feel

Living with aspergillosis can affect far more than the lungs. Many patients have symptoms that are difficult to explain, difficult to measure, and difficult for other people to fully understand.
Breathlessness, fatigue, coughing, chest tightness, sleep disruption, anxiety during flare-ups, medication side effects, and uncertainty about the future can all become part of daily life. These symptoms may fluctuate from day to day, and people may appear well at times even when they are struggling.
This can leave patients feeling misunderstood, dismissed, or even blamed for focusing too much on their health.
Key points
- Symptoms of aspergillosis and chronic lung disease are real, even when they are invisible to others.
- Feeling anxious, frustrated, or preoccupied with health is understandable when symptoms affect daily life.
- Validation from family, friends, and clinicians can reduce distress.
- Finding meaningful things to do beyond illness can also help patients cope.
- The aim is balance: being heard and supported, while also protecting quality of life.
Why aspergillosis can be hard for others to understand
Many people with chronic pulmonary aspergillosis (CPA), allergic bronchopulmonary aspergillosis (ABPA), severe asthma, bronchiectasis, or other long-term lung conditions live with symptoms that are not always visible.
A patient may look well, speak normally, or have reasonable oxygen levels at rest, but still experience severe fatigue, breathlessness on exertion, anxiety during breathing difficulty, or a long recovery after simple activities.
Symptoms may also fluctuate. Someone may manage an activity one day but be unable to do the same thing the next. This inconsistency can be confusing for family, friends, employers, and sometimes even healthcare professionals.
“Stop obsessing” is usually not helpful
Patients with chronic illness are sometimes told to “stop obsessing” about their health. This may be said with good intentions, but it can feel dismissive.
Patients may hear:
“You are making too much of this.”
or:
“It is all in your head.”
In reality, many patients are not choosing to focus on illness. The illness is already demanding attention through symptoms, medication routines, appointments, uncertainty, and changes to daily life.
However, there is also a useful point hidden inside the poor wording. Constantly monitoring every symptom can become exhausting and may increase anxiety. The better message is not “stop obsessing”, but:
“Your symptoms are real, but you also deserve space in your life that is not only about illness.”
Validation matters
Validation means recognising that a person’s experience is real and understandable. It does not mean agreeing that every symptom is dangerous, or that every worry needs urgent medical action.
Useful validating phrases include:
- “I believe you.”
- “That sounds exhausting.”
- “I know this affects much more than people can see.”
- “How is today compared with your usual baseline?”
- “What would help you most today?”
Validation can reduce distress. When patients feel dismissed, they may feel driven to repeat themselves, seek reassurance, or prove how unwell they are. When they feel heard, they may find it easier to step back from constant symptom monitoring and focus on other parts of life.
The mind and body interact
Breathlessness is not just a physical sensation. It can trigger fear very quickly. This is a normal human response: breathing difficulty naturally makes the brain more alert to danger.
This does not mean symptoms are imaginary. It means chronic respiratory illness affects the whole person: physically, emotionally, socially, and psychologically.
Anxiety, uncertainty, poor sleep, and repeated flare-ups can all increase awareness of symptoms. At the same time, genuine physical symptoms can increase anxiety. The two can reinforce each other.
Recognising this interaction can help patients and clinicians work together without blame.
Finding something else to think about can help
For many patients, finding meaningful activities beyond illness is genuinely helpful. This might include hobbies, gentle exercise, time outdoors, music, crafts, reading, gardening, photography, volunteering, family activities, or peer support.
This is not the same as ignoring illness. It is a way of protecting identity and quality of life.
The aim is not to deny symptoms, but to prevent illness becoming the only focus of every day.
“Your illness is real, but it should not be allowed to take over every part of who you are.”
What families and friends can do
Family members and friends may not be able to fully understand what chronic aspergillosis feels like. They do not need perfect understanding to be supportive.
Helpful support includes:
- believing the person’s symptoms are real;
- recognising that fatigue and breathlessness may not be visible;
- avoiding dismissive comments;
- asking what would help rather than assuming;
- understanding that symptoms may fluctuate;
- encouraging enjoyable activities without pressuring the person to “push through”.
Less helpful comments include:
- “You look fine.”
- “You were able to do it yesterday.”
- “You need to stop thinking about it.”
- “Everyone gets tired.”
What clinicians may be trying to say
Sometimes clinicians may say things such as “try not to focus on it too much” because they believe further tests or treatments may not currently help. They may be trying to avoid unnecessary antibiotics, steroids, scans, or procedures.
That can be a reasonable clinical concern, but the message needs to be communicated carefully.
A better way to say it might be:
“I believe your symptoms are real and distressing. We will continue to look for changes that need treatment. At the same time, some symptoms may persist despite treatment, so we also need to support your quality of life.”
This keeps the patient heard, while also being honest about the limits of medical treatment.
Practical ways to find balance
- Use structured symptom tracking: a brief daily note may be more helpful than constant checking.
- Know your baseline: understanding what is normal for you makes changes easier to spot.
- Agree an action plan: ask your healthcare team what changes should prompt medical advice.
- Protect non-illness time: plan small, realistic activities that are not centred on health.
- Use peer support carefully: support groups can reduce isolation, but try to avoid constant comparison or fear-based searching.
- Ask for emotional support: counselling, psychological therapies, pulmonary rehabilitation, or breathing physiotherapy may help some people.
When to seek medical advice
This article is general information and does not replace medical advice. Patients should seek medical help if they experience significant or worrying change, especially:
- worsening breathlessness;
- falling oxygen saturations if they monitor them;
- new or worsening chest pain;
- coughing up blood;
- high fever, rigors, or signs of serious infection;
- new confusion, fainting, or severe weakness;
- rapid deterioration from their usual baseline;
- symptoms that feel different from their usual pattern.
If symptoms are severe or rapidly worsening, urgent medical help should be sought.
Final thought
Living with aspergillosis can be physically and emotionally demanding. Patients deserve to be believed, heard, and supported. At the same time, they also deserve help to build a life that is not entirely defined by illness.
A helpful message for patients, families, and clinicians is:
“Your illness is real. Your distress is understandable. You deserve support. And you also deserve a life with meaning, connection, and moments of relief beyond illness.”
Further support and reading
If you are living with aspergillosis and feel that others do not fully understand what you are going through, these resources may help. They offer information about long-term illness, mental wellbeing, breathlessness, invisible symptoms, and patient support.
- Aspergillosis patient support
Information about support meetings, patient resources, and ways to connect with others affected by aspergillosis. - NHS Talking Therapies
NHS support for people experiencing anxiety, depression, or emotional distress, including people living with long-term health conditions. - Asthma + Lung UK: Living with a lung condition
Practical information on living with breathlessness, fatigue, flare-ups, and the emotional effects of lung disease. - Chronic Illness Inclusion
A UK organisation focused on the experiences of people living with chronic, energy-limiting, and often invisible conditions. - The Patients Association: Long-term conditions
Advice and information for people managing long-term health conditions and navigating healthcare conversations.
Important: If your symptoms suddenly worsen, you develop severe breathlessness, chest pain, coughing up blood, confusion, fainting, or signs of serious infection, seek urgent medical advice. In the UK, call NHS 111 for urgent advice or 999 in an emergency.
Why Join an Online Support Group if You Have Aspergillosis?
You are not alone with aspergillosis
Join a friendly online support meeting — no pressure, just listen if you prefer.
Many patients find that even attending once helps them feel more reassured, informed, and supported.
Why Join an Online Support Group if You Have Aspergillosis?
Living with aspergillosis can feel isolating. Many people go for years without meeting another person with the same condition. Family and friends may be supportive, but they may not fully understand what it is like to live with breathlessness, fatigue, treatment side effects, uncertainty, or repeated hospital visits.
That is one reason online support groups can be so valuable. They bring people together who understand, often immediately, many of the challenges that aspergillosis can bring.
Key points
- Online support groups reduce isolation and help patients feel understood
- They offer shared experience alongside emotional support
- They improve confidence and understanding of the condition
- They help patients feel better prepared for appointments
- They are flexible — you can simply listen if you prefer
What changes when people join a support group?
Before joining
- Feeling alone with the condition
- Uncertainty about symptoms
- Limited practical advice
- Low confidence at appointments
- Worry about the future
After joining
- Connection with others who understand
- Better understanding of the condition
- Practical day-to-day coping ideas
- More confidence asking questions
- Feeling more supported and reassured
Why aspergillosis can feel so isolating
Aspergillosis is a relatively rare condition, and many patients never meet someone else with the same diagnosis. Online support groups help bridge that gap by creating a shared space for understanding and connection.
1. You realise you are not alone
Hearing others describe similar symptoms and challenges can be immediately reassuring and reduce feelings of isolation.
2. Shared experience can be deeply reassuring
Support groups provide practical, real-world insight into managing fatigue, pacing, work, and daily life.
3. You may understand your condition better
Listening to others and accessing shared resources helps build confidence and understanding.
4. It can help you feel more confident at appointments
Patients often feel better prepared and more able to ask the right questions.
5. Emotional support matters too
These groups provide encouragement, understanding, and a sense of belonging.
What happens in a typical online support session?
- Friendly welcome — no pressure to speak
- Open discussion — share or listen
- Optional topics — such as fatigue or treatment experiences
- Flexible participation — camera and microphone optional
- Safe, moderated space
Many people attend their first session just to listen — and that is completely fine.
What patients often say
“I wish I had joined sooner. Just hearing others talk made a huge difference.”
“I didn’t speak in my first meeting, but it really helped just listening.”
“It helped me understand my condition and feel more confident.”
Thinking of joining?
You can attend once, listen, and decide if it feels helpful. There is no obligation to continue.
View meeting times and book here:
https://aspergillosis.org/support-meetings/
Meetings are held online using Microsoft Teams. You will receive a joining link after booking.
Bottom line
Online support groups offer connection, reassurance, and understanding. They cannot replace medical care, but they can make living with aspergillosis feel more manageable and less lonely.
Please note: These groups are for support and shared experience. They do not replace advice from your own doctor or specialist team.
Donating Your Body for Medical Research in the UK
This is an uncommon request, but it can be very helpful to researchers. There is no compulsion at all to consider body donation. It is entirely a personal choice. Many people will decide that it is not for them, and that is completely understandable. For those who do wish to explore it, however, body donation can make an important contribution to medical education, training, and research.
What does body donation mean?
In the UK, donating your body means leaving it after death to a medical school or other appropriately licensed institution for anatomical examination, education, training, or research.
You cannot usually donate your body specifically to “aspergillosis research” alone. However, donation may still support work that is highly relevant to people affected by aspergillosis, including:
- lung disease
- infection
- immune responses
- medical training in complex respiratory illness
The most important point: consent must be given in advance
Under UK law, body donation must be arranged before death. This means:
- you must give written consent
- the consent must usually be witnessed
- your family cannot normally make this decision for you after you die
How to arrange body donation
- Choose a medical school
You need to contact a medical school directly. Most only accept donations from their local area. - Request an information pack
The school will explain its process, send consent forms, and set out any restrictions. - Complete the consent forms
Keep copies with your important papers and let your family know your wishes. - Tell your next of kin or executor
They will usually need to contact the medical school promptly after death.
Important to understand
- Not every donation can be accepted. Even if you have registered, a medical school may not be able to accept the body in every circumstance.
- A backup funeral plan is important.
- Body donation is separate from organ donation. They are different systems and require separate arrangements.
Can I ask for donation to help lung or aspergillosis-related research?
You can certainly explain that your interest is in supporting research and education relevant to lung disease, infection, or aspergillosis. However, you cannot usually guarantee exactly how a donated body will be used. Even so, donation may still support education and research that benefits future patients with complex respiratory and fungal conditions.
Where to start: Human Tissue Authority
The best first step is the Human Tissue Authority (HTA), which provides UK guidance and a way to identify the correct medical school for your postcode.
Examples of medical school body donation pages
Please note: contact details and catchment arrangements can change, so it is wise to confirm current information directly on each medical school’s website.
- University of Manchester
Body donation / bequeathals information - University of Liverpool
Human Anatomy Resource Centre body donation page
Email: [email protected]
Tel: 0151 794 5442 - University of Leeds
Bequests information
Email: [email protected]
Tel: 0113 343 4297
Final thought
Donating your body for medical education or research is an unusual and deeply personal decision. There is absolutely no obligation to consider it. But for those who do, it can be a generous and lasting way to support future learning, better care, and research that may help people living with serious conditions, including aspergillosis.
Last reviewed: March 2026
Why Aspergillosis Is So Hard to Diagnose
Last reviewed: 18 March 2026
Key points
- Aspergillosis is often difficult to diagnose because its symptoms can look very similar to those of more common conditions.
- Diagnosis usually depends on several pieces of evidence being brought together, rather than one simple test.
- Doctors are trained to consider common conditions first, because this is usually the safest and most efficient approach.
- This approach works well for many patients, but it can delay recognition of conditions such as aspergillosis.
- Delays are often caused by the way healthcare systems are organised, not by lack of care or effort from individual clinicians.
- Patients can help by keeping a clear record of symptoms, tests, treatments, and how things have changed over time.
Why diagnosis can be difficult
Aspergillosis is not a single illness but a group of conditions caused by Aspergillus, a mould commonly found in the environment. These include:
- Allergic bronchopulmonary aspergillosis (ABPA)
- Chronic pulmonary aspergillosis (CPA)
- Other airway and colonisation-related conditions
Diagnosis usually depends on combining:
- symptoms over time
- CT scan findings
- blood tests (including immunological tests)
- sputum microbiology
- clinical history
There is rarely a single “yes or no” test, which is why diagnosis can take time.
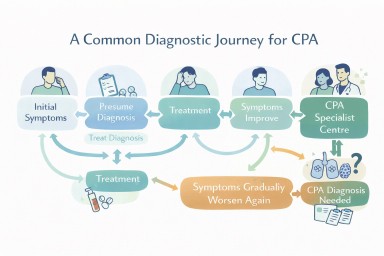
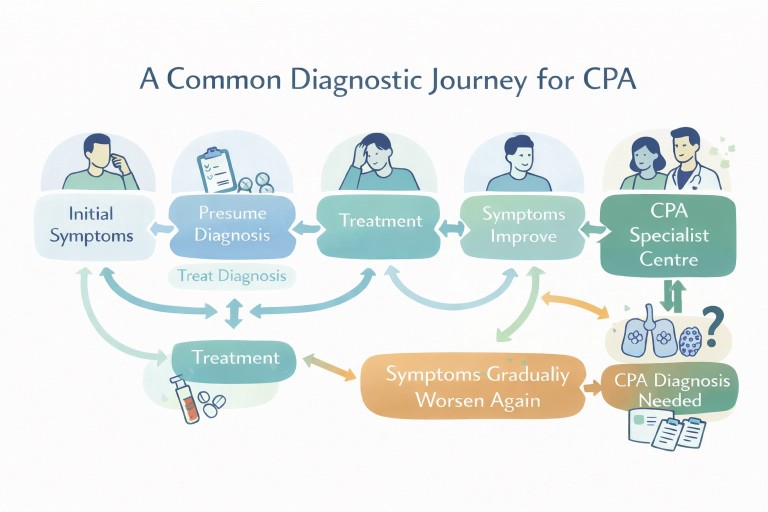
What the patient journey often looks like
Early symptoms
Symptoms such as cough, breathlessness, fatigue, or sputum are common across many conditions including bronchiectasis, asthma, and infection.
Treatment for common conditions
Initial treatment often includes antibiotics, inhalers, or steroids. These are appropriate first steps based on clinical guidelines such as those from the British Thoracic Society (BTS).
Ongoing symptoms
When symptoms persist or return, further investigation is usually needed.
The turning point
At some stage, fungal disease may be considered and tests for Aspergillus are performed.
Why doctors tackle common conditions first
Why do doctors start with common conditions?
Doctors treat common diseases first, prioritizing efficiency, patient safety, and high-probability outcomes. This approach, considering the most likely diagnosis first, helps manage patient health efficiently and effecctively before investigating rare or complex conditions.
This approach is safe and effective for most people, but conditions like aspergillosis can sit outside these usual pathways.
Where delays can happen
Overlap of symptoms
Symptoms overlap with many conditions, including tuberculosis and lung cancer.
No single definitive test
Diagnosis often requires combining multiple test results rather than relying on one.
Gradual disease progression
Conditions such as CPA may evolve over months or years.
Multiple conditions
Patients may have more than one lung condition at the same time.
Why this is often about the system, not the individual doctor
Healthcare systems are designed to manage large numbers of patients efficiently and safely. This means prioritising common conditions first.
However, aspergillosis often requires specialist input. In the UK, this may include referral to the National Aspergillosis Centre, which provides expert assessment and management.
International guidance from organisations such as ESCMID (European Society of Clinical Microbiology and Infectious Diseases) also highlights the complexity of fungal diseases.
What patients can do
- Keep a record of symptoms and treatments
- Ask when diagnosis should be reviewed
- Discuss whether further tests are needed
- Use trusted information sources such as our diagnosis guide
A more balanced way to think about delay
Diagnosis is often not a single event but a process that unfolds over time.
The goal is to recognise patterns earlier and ensure patients who need specialist input are identified sooner.
Common questions
Why was I treated for other conditions first?
Because those conditions are more common and more likely.
Should I ask about aspergillosis?
Yes, especially if symptoms are persistent or unusual—but it should be part of a broader discussion.
When to seek medical advice
- Persistent or worsening symptoms
- Coughing up blood
- Unexplained weight loss
References and further reading
When Symptoms Are Real but Answers Are Not: Understanding Uncertainty
Last reviewed: 18 March 2026
Key points
- Many people experience a period where symptoms are real but no clear diagnosis has been made.
- This can sometimes feel like being told “nothing is wrong” or “it is all in your head”.
- In most cases, this reflects uncertainty in the system, not disbelief from clinicians.
- Conditions such as aspergillosis can take time to become recognisable.
- Physical and psychological factors can overlap—but unexplained symptoms are still real symptoms.
- Clear communication and ongoing review are key to moving forward.
The experience many patients describe
During a long diagnostic journey, many people reach a point where they hear phrases such as:
- “Your tests are normal”
- “We can’t find anything serious”
- “It may be stress or anxiety contributing”
Even when these words are carefully chosen, they can feel like:
“Nothing is wrong” or “it’s all in my head”
This can be one of the most difficult parts of the journey—especially when symptoms are ongoing, disruptive, and clearly real.
Why this happens
This situation usually reflects the limits of current medical systems rather than a lack of concern.
Tests do not always give clear answers
Modern medicine relies heavily on tests. But for many conditions—including chronic pulmonary aspergillosis (CPA)—tests may:
- be negative early on
- show unclear or borderline results
- require interpretation over time
This creates a gap between:
- what the patient is experiencing
- what can currently be measured
Medicine is designed to provide answers
Clinicians are trained to explain symptoms and reassure patients. When no clear diagnosis is available, they may turn to explanations such as:
- stress
- anxiety
- functional symptoms
These are real and valid factors—but if introduced too early, they can feel like the search has stopped.
Time pressure
Short consultations can mean:
- less time to explain uncertainty
- less opportunity to validate patient experience
- simplified explanations that lose nuance
What doctors mean vs what patients hear

Often, the issue is not what is said—but how it is understood.
| What may be said | What may be heard |
|---|---|
| “Your tests are normal” | “Nothing is wrong” |
| “We haven’t found a cause yet” | “There is no cause” |
| “Stress may be contributing” | “It’s all in your head” |
Understanding this gap can help both patients and clinicians move forward more constructively.
A critical clarification
Not having a diagnosis is not the same as not having a disease.
Unexplained symptoms are still real symptoms.
Medicine does not always have immediate answers—especially for conditions that develop slowly or do not fit standard patterns.
Physical and psychological overlap
It is important to take a balanced view.
- Physical illness can lead to anxiety, fatigue, and distress
- Anxiety can worsen physical symptoms such as breathlessness
This relationship is two-way, not either/or.
The problem arises when psychological explanations replace further investigation, rather than sitting alongside it.
Why this matters in aspergillosis
Conditions such as aspergillosis often:
- develop gradually
- have non-specific symptoms
- require multiple tests over time
This makes periods of uncertainty more likely, particularly before a diagnosis such as allergic bronchopulmonary aspergillosis (ABPA) or CPA is confirmed.
You can read more about this in Why Aspergillosis Is So Hard to Diagnose.
What patients can do
- Keep a record of symptoms and how they change over time
- Ask what the current working diagnosis is
- Ask when the situation should be reviewed
- Share concerns clearly, but remain open to different explanations
Helpful questions include:
- “What else could this be?”
- “What would make you reconsider the diagnosis?”
- “When should we review this again?”
A shared understanding
This situation is not about:
- patients being dismissed
- clinicians not caring
It reflects a deeper reality:
Medicine does not always have immediate answers—especially for complex or evolving conditions.
The goal is to keep the process open, respectful, and moving forward.
Common questions
Does this mean doctors think I’m imagining symptoms?
No. It usually reflects uncertainty rather than disbelief.
Can stress really affect physical symptoms?
Yes—but this should not stop appropriate medical investigation.
What should I do if I feel dismissed?
Ask for clarification, a review plan, or a second opinion if needed.
Related pages
How to Ask Fewer, Better Questions in Appointments
Focusing on what matters most to you—without feeling you’re wasting time
Many patients and carers worry about “asking too much” in clinic. Appointments are short, clinicians are busy, and you may already have a long list of questions in your head. The aim isn’t to stop asking questions—it’s to ask the right ones, at the right time, in the right way.
Here are practical strategies that help you stay focused, feel heard, and make the most of limited time.
1. Decide your Top 3 priorities before you go
Before the appointment, write down everything you’re thinking about. Then circle just three things that matter most right now.
Good priorities are usually:
-
A symptom that is new, worsening, or frightening
-
A treatment issue that affects daily life (side-effects, adherence, cost, function)
-
A decision you need to make soon
If it doesn’t change what happens in the next few weeks, it may not need airtime today.
If you remember only one thing: appointments are for decisions, not encyclopaedias.
2. Separate “need to know” from “nice to know”
It’s easy to mix curiosity with urgency.
Need to know (ask now):
-
Is this symptom important?
-
Is this treatment still right for me?
-
What should I do if X happens?
-
Are we monitoring the right things?
Nice to know (park for later):
-
Mechanisms, pathways, emerging research
-
Rare side-effects without symptoms
-
“What if” scenarios far in the future
Keep a “parking list” for later reading or discussion.
3. Frame questions around impact, not theory
Clinicians work best when questions are grounded in real life.
Instead of:
-
“I read a paper saying X might affect Y…”
Try:
-
“I’m noticing X in daily life—does that change what we do?”
-
“Is this symptom something you’d want to investigate?”
This signals relevance and helps clinicians triage quickly.
4. Ask one question at a time
Long, multi-part questions feel overwhelming and are easy to partially answer.
Break them down:
-
First: Is this important?
-
Then (if yes): What do we do about it?
-
Then (if needed): What should I watch for?
You’ll often find later questions become unnecessary once the first is answered.
5. Use the “Is this something we should…” test
This single phrase keeps questions concise and respectful of time:
-
“Is this something we should investigate?”
-
“Is this something that changes treatment?”
-
“Is this something I should worry about?”
A clear yes/no (or not yet) is often all you need.
6. Accept that not everything fits in one appointment
It’s okay—and normal—to say:
-
“I know we may not have time today—what should I prioritise?”
-
“Which of these matters most from your point of view?”
This shows partnership, not passivity.
If something needs more time, ask how best to handle it:
-
Another appointment
-
A nurse specialist
-
Written advice
-
Monitoring and review later
7. Bring written notes (but don’t read them all out)
A short list helps you stay focused under pressure.
Tip:
-
Highlight your top 3
-
Tick them off as they’re addressed
-
If time runs out, you still covered what mattered most
8. For carers: ask on behalf, not over
Carers often worry about dominating the conversation.
Helpful approaches:
-
Ask the patient first: “What do you most want answered today?”
-
Step in only if something important is being missed
-
Offer to follow up questions outside the appointment if possible
9. Reassure yourself: clinicians don’t expect perfection
You are not expected to:
-
Understand everything
-
Ask the “right” questions every time
-
Cover your entire condition in one visit
Good clinicians prefer:
a focused conversation
over
a rushed, overloaded one
10. A simple closing question that saves time
If time is tight, end with:
-
“Is there anything you think I should have asked but didn’t?”
This often surfaces the most important point of all.
The takeaway
You are not wasting time by asking questions—you’re wasting time by asking too many unfocused ones.
Clarity, prioritisation, and relevance help everyone:
-
You leave with answers that matter
-
Clinicians can make better decisions
-
Anxiety is reduced, not fuelled
When Caring for a Loved One Becomes Overwhelming: A Guide for Family Carers
Caring for a spouse, parent, or child is one of the most loving things you can do — but it can also be one of the hardest. Many family carers feel torn: wanting to give the very best care, yet struggling with exhaustion, isolation, and the feeling that “no one else can do it as well as me.”
This guide brings together insights to help you recognise when caring is becoming too heavy, why it feels so difficult to let go, and how to build a sustainable balance that protects both you and the person you love.
Why caring feels so demanding with family
-
Loss of independence: Illness often leaves people feeling powerless. Demanding behaviour can be a way of trying to regain control.
-
Role reversal stress: When a child becomes a parent’s carer, or a spouse becomes more like a nurse, both sides can feel uncomfortable.
-
Emotional safety: Patients often hold back with professionals but show raw feelings at home. That can come across as extra demanding.
-
Blurred boundaries: With family, it’s harder to say “no.” A patient may expect more than they ever would from an outsider.
When the caring role becomes unreasonable
Caring is no longer sustainable when:
-
Your health breaks down from exhaustion or stress.
-
You are completely isolated, with no time for friends, rest, or hobbies.
-
The caree’s demands exceed real need, and everything revolves around them.
-
Boundaries disappear and you can’t say no without conflict.
-
You are the only source of support, with no outside help.
These are warning signs that it’s time to rebalance the situation.
Why it doesn’t mean “defeat”
Asking for help can feel like admitting failure — but it isn’t.
-
Caring is a marathon, not a sprint. Protecting your health means you can keep caring longer.
-
Strength means knowing your limits. Bringing in help shows foresight, not weakness.
-
Love isn’t replaced. Professional carers can take tasks off your hands, but your relationship and bond remain uniquely yours.
Think of it not as “stepping back” but as building a care team. You remain the anchor, but you don’t carry everything alone.
Why it’s hard to let others help
Many carers say: “They don’t do it as well as I do.” This is natural — you know your loved one’s habits and needs better than anyone. Professionals may work differently, and that can feel uncomfortable.
But:
-
Different doesn’t always mean worse — just not “your way.”
-
Perfection isn’t sustainable if it destroys your health.
-
Your role as spouse/child/friend is irreplaceable — letting others handle routine care may free you to keep that role.
Start small: allow someone else to take over one task or cover for a short period. Gradually, trust can build.
Can problems be predicted?
Yes — carers often see the signs early:
-
Constant exhaustion or resentment
-
Dropping their own health needs or appointments
-
Losing touch with friends and community
-
Feeling guilty if they take any time for themselves
If these signs appear, it’s time to bring in extra support before crisis strikes.
Practical steps to make caring sustainable
-
Have early, honest conversations about what you can and cannot do.
-
Ask for a Carer’s Assessment (in the UK) — this can open up respite care, day services, and financial support.
-
Bring in professional support early so it feels like teamwork, not abandonment.
-
Protect your own time — even short, regular breaks keep you healthier.
-
Seek peer support — carers’ groups and counselling reduce isolation.
Final thought
Caring is an act of deep love. But love alone cannot carry the whole weight forever. Sharing the load is not defeat — it is the wisest way to ensure that both you and your loved one remain safe, cared for, and connected.
You are not failing. You are leading a team, protecting your own well-being, and preserving the relationship that matters most.
🧾 Getting a Second Opinion for Aspergillosis: What If Your Hospital Refuses?
Many patients living with aspergillosis or allergic bronchopulmonary aspergillosis (ABPA) ask for a second opinion — often from a national centre like the National Aspergillosis Centre (NAC) in Manchester or from another specialist elsewhere in the UK. But sometimes, hospitals resist sending your case outside their own department.
Here’s what’s happening, why it might occur, and what you can do.
🤔 Why Would a Hospital Refuse an Outside Opinion?
It’s understandably frustrating when you’ve asked for expert help and your local hospital insists on keeping things “in-house.” Here are some reasons this might happen:
1. Internal Referral Rules
Hospitals sometimes have a policy to refer to another consultant within their own department first. They may consider this a “second opinion,” even if it’s not truly independent.
2. Cost and Complexity
Referrals to another NHS trust — especially across health boards or into England (e.g. to NAC) — can involve extra steps and costs. Some hospitals prefer to avoid that unless they feel there’s no choice.
3. Professional Sensitivities
Some doctors may feel a national second opinion implies criticism of their care, even if your request is made respectfully.
4. Lack of Awareness
Some clinicians aren’t fully aware of what the National Aspergillosis Centre offers — or may underestimate how complex aspergillosis, ABPA, or recurrent fungal infections can be.
🧑⚕️ But Isn’t a Specialist Opinion My Right as an NHS Patient?
Yes. If your GP or hospital team believes it’s clinically appropriate, you have the right to be referred to another NHS consultant — including one outside your local area.
The NAC is nationally commissioned by NHS England to provide care for people with chronic aspergillosis. They accept referrals from across the UK.
💷 Why Private Care Might Not Be an Option
Some patients consider going private when local NHS referrals are blocked — but private care often means:
-
Paying for new scans, blood tests, and sputum cultures
-
No direct access to previous NHS records
-
Higher costs than expected, especially for complex tests
If you can’t afford this, you are not alone, and there are still NHS options available.
🧭 What You Can Do Next
Here are practical steps if you're being blocked from getting a second opinion:
✅ 1. Restate Your Request Clearly
Ask your GP (or write yourself) to reply to the hospital and explain:
-
You are specifically asking for an opinion from a national expert service (e.g. NAC or Dr Iain Page in Edinburgh).
-
This is not a rejection of their care, but a request for specialist reassurance, diagnosis support, or treatment planning.
✅ 2. Ask for a Tertiary Centre Referral
Use the term “tertiary referral” — this means a referral to a national or highly specialised NHS service.
✅ 3. Raise It with PALS
If you're still being blocked, contact your local Patient Advice and Liaison Service (PALS) or NHS complaints team. Explain:
-
You have a rare/complex condition,
-
You’ve asked for a national review,
-
And you’ve been offered only an internal opinion.
✅ 4. Get support on NAC Support Facebook Group
- https://www.facebook.com/groups/aspergillussupport/
💬 In Summary
-
You’re not being difficult — you’re advocating for your health.
-
It is reasonable and often necessary to seek input from specialists like those at the NAC.
-
If you’ve been told “no,” it may be due to policies or misunderstandings — not a reflection on your need for better care.
-
Keep asking, and if needed, involve your GP, or PALS.