Last reviewed: April 2026
Key points
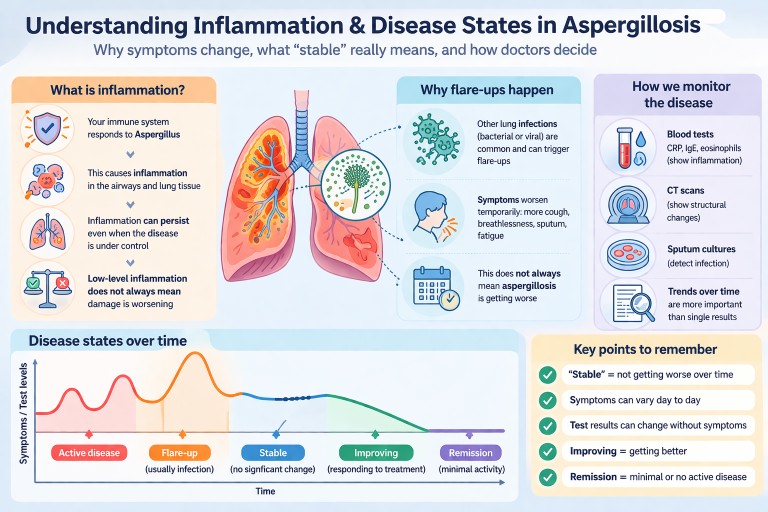
- Inflammation is part of the body’s response to Aspergillus, but it does not always mean damage is actively worsening.
- “Stable” disease means no clear progression over time, not that the condition has disappeared.
- Symptoms in aspergillosis often vary because of other infections, especially in the lungs.
- Test results (such as IgE or CRP) can change without symptoms changing.
- Doctors make decisions based on the overall pattern over time, not a single test result.
Table of contents
- What is inflammation and why does it matter?
- Inflammation in different types of aspergillosis
- Clear definitions: active, flare, stable, improving, remission
- What does “stable disease” mean in practice?
- Why other infections cause flare-ups
- Understanding test results (CRP, IgE, scans)
- When test results worsen but symptoms do not
- How doctors decide what is happening
- Common patient questions
- When to seek medical advice
What is inflammation and why does it matter?
Inflammation is the body’s way of responding to something it sees as harmful. In aspergillosis, this is usually the fungus Aspergillus.
This response involves immune cells, chemicals, and changes in the lungs that aim to control the fungus. However, if inflammation continues over a long period (chronic inflammation), it can also contribute to:
- Ongoing symptoms (cough, breathlessness, fatigue)
- Mucus production
- Damage to lung tissue over time
Important: inflammation can be present at a low level without causing active damage. This is common in chronic conditions.
Inflammation in different types of aspergillosis
The type of inflammation depends on the form of aspergillosis:
- Allergic Bronchopulmonary Aspergillosis (ABPA): driven by an overactive allergic response. Blood markers such as IgE and eosinophils are often used to monitor this.
- Chronic Pulmonary Aspergillosis (CPA): caused by long-term infection in damaged lung tissue, leading to ongoing inflammation and structural changes.
- Aspergillus bronchitis: persistent infection with inflammation, often causing chronic cough and sputum.
In all cases, inflammation may improve with treatment but often does not disappear completely.
Clear definitions: disease states
Doctors use the following terms to describe how the disease is behaving:
- Active disease: symptoms, tests, or scans are getting worse over time
- Flare-up: a short-term worsening, often triggered by infection or another stress on the body
- Stable: no clear overall change over time
- Improving / responding to treatment: symptoms and/or tests are getting better
- Remission: minimal or no signs of active disease (used more often in ABPA)
Key point: these states are not fixed — patients may move between them.
What does “stable disease” mean in practice?
“Stable” means that, over a period of time (weeks to months), there is no clear evidence that the disease is progressing.
This usually includes:
- No worsening of key symptoms
- No new complications (e.g. haemoptysis, significant weight loss)
- Imaging (CT scans) showing no progression
- No need to increase treatment
What stable does NOT mean:
- It does not mean symptoms are absent
- It does not mean inflammation is zero
- It does not mean you will feel the same every day
Many patients with stable disease still experience day-to-day variation in symptoms.
Why other infections cause flare-ups
People with aspergillosis are more vulnerable to other lung infections (bacterial or viral).
This is because:
- Lung structure may already be damaged
- Mucus clearance is less effective
- The immune system is already active
When another infection occurs, it can trigger a flare-up, causing:
- Increased cough and breathlessness
- More or thicker sputum
- Fatigue and feeling unwell
- Raised inflammatory markers (e.g. CRP)
Crucial point: this does not necessarily mean the aspergillosis itself is worsening. It is often a temporary additional problem.
Understanding test results
Doctors use several types of tests to monitor inflammation and disease activity:
- CRP / ESR: general markers of inflammation
- IgE: particularly important in ABPA
- Eosinophils: linked to allergic inflammation
- CT scans: show structural changes in the lungs
- Sputum cultures: detect infection
Important limitations:
- No single test gives a complete picture
- Results can fluctuate for many reasons
- Changes must be interpreted over time
When test results worsen but symptoms do not
This situation is common, especially in ABPA.
For example, IgE levels may rise without any noticeable change in symptoms.
This may happen because of:
- Natural biological variation
- Exposure to allergens
- A mild or early flare that has not yet caused symptoms
Key point: a change in a single test result does not automatically mean the disease is worsening.
Doctors will usually:
- Repeat tests
- Look for consistent trends
- Assess symptoms and scans
If symptoms remain stable and no other changes are seen, the condition may still be considered stable — but monitored more closely.
How doctors decide what is happening
Clinicians do not rely on a single result. Instead, they assess the pattern over time:
- Are symptoms changing?
- Are test results consistently rising or falling?
- Are scans stable or changing?
- Is the patient responding to treatment?
This combined assessment is called the clinical picture.
Common questions
If I feel better, what is that called?
This is usually described as improving or responding to treatment. In some cases (especially ABPA), it may be called remission.
Does inflammation always mean damage?
No. Low-level inflammation can persist without causing further harm.
Why do my symptoms change from day to day?
This is common and often relates to infections, environment, or general health rather than disease progression.
Can aspergillosis affect the whole body?
It can have wider effects, but it mainly affects the lungs in most patients.
When to seek medical advice
Seek medical advice if you notice:
- Persistent worsening of symptoms
- New haemoptysis (coughing up blood)
- Significant weight loss
- Symptoms not improving after a suspected infection
- Concerns about test results
Author and review
Author: Aspergillosis Patient Education Team
Reviewed by: National Aspergillosis Centre (UK)
References
- Denning DW et al. Chronic pulmonary aspergillosis guidelines
- ISHAM ABPA guidelines
This article is for general information only and is not a substitute for medical advice.
Share this post
Latest News posts
Do you need a Patient Information Leaflet for your medication?
September 26, 2023
Understanding Sepsis: A Patient’s Guide
September 26, 2023
Martha’s Rule: A Lifeline for Patients and Families in the NHS
September 6, 2023
NHS Complaint Procedures
September 4, 2023
Accessing GP Services: A Detailed Overview
August 31, 2023
Unvalidated Laboratory Testing
August 2, 2023
Osteoporosis (Thinning bones)
August 1, 2023
Understanding a Fever
July 31, 2023
Living with & Managing Chronic Illness
July 27, 2023
News archive
- ABPA
- Air Quality
- Airway Clearance, Diagnosis & Physiotherapy
- Antifungals
- Aspergilloma
- Aspergillus Bronchitis
- Biologics
- Blood Tests
- CPA
- Carers & Family
- Communities
- Complementary & Supplements
- Complications
- Conditions
- Diagnostics
- Environment
- Events & Recordings
- GP Guidance
- General interest
- Housing & Damp
- Imaging
- Immune System
- Lifestyle & Coping
- Living with Aspergillosis
- Mental Health
- Monitoring
- Monitoring & Safety
- NAC & Guidance
- NAC Announcements
- Other
- Other Forms Aspergillosis
- Patient Research
- Pets & Animals
- Professional Guidance
- Recordings
- Research
- Research Summaries
- SAFS / Severe Asthma
- Side Effects
- Steroids
- Symptoms
- Travel and Insurance
- Treatment
- Vaccines
- Weekly Updates