Last reviewed: April 2026
Many people with lung conditions ask whether foods like kefir, yoghurt or cider vinegar could trigger infections. This article explains what we know — and what we don’t — based on current evidence and patient experience.
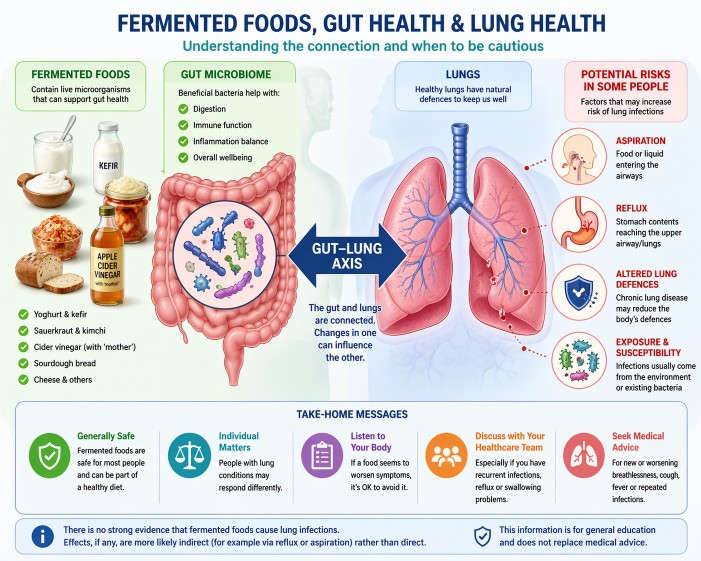
Can fermented foods cause lung infections?
No. There is no strong evidence that fermented foods cause lung infections such as pneumonia. Any effects on the lungs are more likely indirect, for example through reflux or aspiration rather than direct infection.
Quick answer: fermented foods are generally safe, but individual responses vary.
Key Points
- Fermented foods contain live microorganisms, usually beneficial bacteria and yeasts
- For most people, these foods are safe and part of a healthy diet
- There is no strong evidence linking fermented foods to lung infections
- Some people with lung disease may be affected by reflux or aspiration
- If symptoms worsen after certain foods, it is reasonable to avoid them
Table of Contents
- What are fermented foods?
- Are fermented foods safe?
- Can they cause infections?
- Why concerns arise in lung disease
- Who may need caution?
- Practical considerations
- Common questions
- When to seek medical advice
What are fermented foods?
Fermented foods are made using microorganisms (such as bacteria or yeast) to transform food. Examples include yoghurt, kefir, sauerkraut, kimchi, cheese and cider vinegar (including those containing the “mother”).
These microorganisms are generally considered non-harmful or beneficial.
Are fermented foods safe?
For most people, including many with chronic lung conditions, fermented foods are considered safe.
They may support gut health, although evidence varies depending on the product and individual.
You can read more in our
diet and aspergillosis guide
.
Can they cause infections?
There is no clear evidence that eating fermented foods causes lung infections such as pneumonia.
Lung infections usually arise from:
- Microorganisms already present in the airways
- Inhaled organisms from the environment
This is explored further in our article:
Why antibiotics do not always work
.
Why do concerns arise in lung conditions?
People with aspergillosis, bronchiectasis or chronic lung disease may be more sensitive to changes affecting the lungs.
1. Aspiration
If small amounts of food or liquid enter the airway, this can contribute to infection.
2. Reflux
Reflux can reach the upper airway and may play a role in lung irritation.
3. Lung microbiome
The lungs contain their own microbial environment, which can shift during illness.
4. Coincidence vs causation
An infection occurring after a dietary change does not necessarily mean the food caused it.
Evidence in this area is still developing, and most studies focus on gut health rather than direct lung effects.
Who might need to be more cautious?
- Frequent lung infections
- Significant bronchiectasis
- Swallowing difficulties
- Severe reflux
- Weakened immune systems
At specialist centres such as the National Aspergillosis Centre, these factors are considered alongside overall lung health.
Practical considerations
- Avoid foods that appear to worsen symptoms
- Introduce new foods gradually
- Be cautious with unpasteurised products
- Keep a simple symptom diary
Common questions
Are probiotics the same as fermented foods?
No. Probiotics are specific strains studied for health benefits, while fermented foods vary widely.
Should people with aspergillosis avoid fermented foods?
There is no general recommendation to avoid them. Most people tolerate them well.
Can fermented foods affect the lungs directly?
Not usually. Effects, if present, are more likely indirect.
When to seek medical advice
- New or worsening breathlessness
- Persistent cough or sputum changes
- Fever or infection symptoms
- Repeated infections
Summary
Fermented foods are generally safe, but individual responses vary. There is no strong evidence linking them to lung infections, but factors such as reflux or aspiration may be relevant in some people.
Balancing general evidence with personal experience is key.
References
- Marco ML et al. Health benefits of fermented foods.
PMID: 28433791
View on PubMed - Hill C et al. Probiotics consensus.
PMID: 24912386
View on PubMed - Budden KF et al. Gut–lung axis.
PMID: 27694885
View on PubMed - Dickson RP et al. Lung microbiome.
PMID: 26965149
View on PubMed - Marik PE. Aspiration pneumonia.
PMID: 11430328
View on PubMed - NICE Pneumonia guidance
View NICE guidance
Author & Review
This article has been prepared by the National Aspergillosis Centre CARES team for patients and non-specialists.
It is intended for general education and should not replace individual medical advice.
Share this post
Latest News posts
Weekly Aspergillosis Update (2–9 February 2026)(Week 5).
February 9, 2026
Aspergillosis, immunity, and risk
February 2, 2026
Latest Aspergillosis & Related Research Updates (Week 4).
February 2, 2026
Wearable devices and aspergillosis
January 29, 2026
How the Body Handles Chemicals, Medicines, and Antifungals
January 27, 2026
Airways mucus and aspergillosis
January 27, 2026
News archive
- ABPA
- Air Quality
- Airway Clearance, Diagnosis & Physiotherapy
- Antifungals
- Aspergilloma
- Aspergillus Bronchitis
- Biologics
- Blood Tests
- CPA
- Carers & Family
- Communities
- Complementary & Supplements
- Complications
- Conditions
- Diagnostics
- Environment
- Events & Recordings
- GP Guidance
- General interest
- Housing & Damp
- Imaging
- Immune System
- Lifestyle & Coping
- Living with Aspergillosis
- Mental Health
- Monitoring
- Monitoring & Safety
- NAC & Guidance
- NAC Announcements
- Other
- Other Forms Aspergillosis
- Patient Research
- Pets & Animals
- Professional Guidance
- Recordings
- Research
- Research Summaries
- SAFS / Severe Asthma
- Side Effects
- Steroids
- Symptoms
- Travel and Insurance
- Treatment
- Vaccines
- Weekly Updates

